Abstract
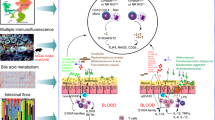
Quantitative metagenomic studies have linked the gut microbiota to autoimmune disorders. Here, we performed deep shotgun metagenomic sequencing of fecal samples from 99 immune thrombocytopenia (ITP) patients and 52 healthy controls. Dysbiosis in the gut microbiome of ITP was detected phylogenetically and functionally, and classifier based on species markers distinguished individuals with ITP from healthy controls. In particular, the abundance of Ruminococcus gnavus, Bifidobacterium longum and Akkermansia muciniphila was markedly increased in treatment-naïve ITP patients, and the alterations of microbial species were correlated with clinical indices. Functionally, the secondary bile acid biosynthesis and flagellar assembly were depleted in the gut microbiota of ITP, which may contribute to the onset of ITP by affecting the immune system. Furthermore, we found that corticosteroid treatment affected the gut microbiome of ITP. Compared with corticosteroid-sensitive ITP patients, we identified that the corticosteroid-resistant ITP patients displayed a distinct gut microbiome, which was different from that of the treatment-naïve ITP patients. Together, we provided support for the critical role of gut microbiota in the development of ITP and established a foundation for further research characterizing gut microbiota in relation to corticosteroid resistance of ITP.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Albertsen, M., Hugenholtz, P., Skarshewski, A., Nielsen, K.L., Tyson, G. W., and Nielsen, P.H. (2013). Genome sequences of rare, uncultured bacteria obtained by differential coverage binning of multiple metagenomes. Nat Biotechnol 31, 533–538.
Asahi, A., Nishimoto, T., Okazaki, Y., Suzuki, H., Masaoka, T., Kawakami, Y., Ikeda, Y., and Kuwana, M. (2008). Helicobacter pylori eradication shifts monocyte Fcy receptor balance toward inhibitory FcγRIIB in immune thrombocytopenic purpura patients. J Clin Invest 118, 2939–2949.
Audia, S., Mahévas, M., Samson, M., Godeau, B., and Bonnotte, B. (2017). Pathogenesis of immune thrombocytopenia. Autoimmun Rev 16, 620–632.
Azzouz, D., Omarbekova, A., Heguy, A., Schwudke, D., Gisch, N., Rovin, B.H., Caricchio, R., Buyon, J.P., Alekseyenko, A.V., and Silverman, G. J. (2019). Lupus nephritis is linked to disease-activity associated expansions and immunity to a gut commensal. Ann Rheum Dis 78, 947–956.
Bettaieb, A., Oksenhendler, E., Duedari, N., and Bierling, P. (1996). Cross-reactive antibodies between HIV-gp120 and platelet gpIIIa (CD61) in HIV-related immune thrombocytopenic purpura. Clin Exp Immunol 103, 19–23.
Borody, T., Campbell, J., Torres, M., Nowak, A., and Leis, S. (2011). Reversal of idiopathic thrombocytopenic purpura [ITP] with fecal microbiota transplantation [FMT]. Am J Gastroenterol 106, S352.
Brandt, L.J., Aroniadis, O.C., Mellow, M., Kanatzar, A., Kelly, C., Park, T., Stollman, N., Rohlke, F., and Surawicz, C. (2012). Long-term follow-up of colonoscopic fecal microbiota transplant for recurrent Clostridium difficile infection. Am J Gastroenterol 107, 1079–1087.
Breunis, W.B., van Mirre, E., Bruin, M., Geissler, J., de Boer, M., Peters, M., Roos, D., de Haas, M., Koene, H.R., and Kuijpers, T.W. (2008). Copy number variation of the activating FCGR2C gene predisposes to idiopathic thrombocytopenic purpura. Blood 111, 1029–1038.
Chiang, J.Y.L. (2009). Bile acids: regulation of synthesis. J Lipid Res 50, 1955–1966.
Chua, H.H., Chou, H.C., Tung, Y.L., Chiang, B.L., Liao, C.C., Liu, H.H., and Ni, Y.H. (2018). Intestinal dysbiosis featuring abundance of Ruminococcus gnavus associates with allergic diseases in infants. Gastroenterology 154, 154–167.
Clemente, J.C., Ursell, L.K., Parfrey, L.W., and Knight, R. (2012). The impact of the gut microbiota on human health: an integrative view. Cell 148, 1258–1270.
Collison, J. (2019). Gut microbiota linked to kidney disease in SLE. Nat Rev Rheumatol 15, 188.
Cooper, N., and Ghanima, W. (2019). Immune thrombocytopenia. N Engl J Med 381, 945–955.
Dao, M.C., Everard, A., Aron-Wisnewsky, J., Sokolovska, N., Prifti, E., Verger, E.O., Kayser, B.D., Levenez, F., Chilloux, J., Hoyles, L., et al. (2016). Akkermansia muciniphila and improved metabolic health during a dietary intervention in obesity: relationship with gut microbiome richness and ecology. Gut 65, 426–436.
Derrien, M., Belzer, C., and de Vos, W.M. (2017). Akkermansia muciniphila and its role in regulating host functions. Microb Pathogenesis 106, 171–181.
Eckburg, P.B., Bik, E.M., Bernstein, C.N., Purdom, E., Dethlefsen, L., Sargent, M., Gill, S.R., Nelson, K.E., and Relman, D.A. (2005). Diversity of the human intestinal microbial flora. Science 308, 1635–1638.
Fiorucci, S., and Distrutti, E. (2015). Bile acid-activated receptors, intestinal microbiota, and the treatment of metabolic disorders. Trends Mol Med 21, 702–714.
Forslund, K., Hildebrand, F., Nielsen, T., Falony, G., Le Chatelier, E., Sunagawa, S., Prifti, E., Vieira-Silva, S., Gudmundsdottir, V., Krogh Pedersen, H., et al. (2015). Disentangling type 2 diabetes and metformin treatment signatures in the human gut microbiota. Nature 528, 262–266.
Francis, O.E., Bendall, M., Manimaran, S., Hong, C., Clement, N.L., Castro-Nallar, E., Snell, Q., Schaalje, G.B., Clement, M.J., Crandall, K. A., et al. (2013). Pathoscope: Species identification and strain attribution with unassembled sequencing data. Genome Res 23, 1721–1729.
Franzosa, E.A., Sirota-Madi, A., Avila-Pacheco, J., Fornelos, N., Haiser, H. J., Reinker, S., Vatanen, T., Hall, A.B., Mallick, H., McIver, L.J., et al. (2019). Gut microbiome structure and metabolic activity in inflammatory bowel disease. Nat Microbiol 4, 293–305.
Frydman, G.H., Davis, N., Beck, P.L., and Fox, J.G. (2015). Helicobacter pylori eradication in patients with immune thrombocytopenic purpura: A review and the role of biogeography. Helicobacter 20, 239–251.
Fu, L., Niu, B., Zhu, Z., Wu, S., and Li, W. (2012). CD-HIT: accelerated for clustering the next-generation sequencing data. Bioinformatics 28, 3150–3152.
Furumitsu, Y., Yukioka, K., Yukioka, M., Ochi, T., Morishima, Y., Matsui-Yuasa, I., Otani, S., Inaba, M., Nishizawa, Y., and Morii, H. (2000). Interleukin-1beta induces elevation of spermidine/spermine N1-acetyl-transferase activity and an increase in the amount of putrescine in synovial adherent cells from patients with rheumatoid arthritis. J Rheumatol 27, 1352–1357.
Furusawa, Y., Obata, Y., Fukuda, S., Endo, T.A., Nakato, G., Takahashi, D., Nakanishi, Y., Uetake, C., Kato, K., Kato, T., et al. (2013). Commensal microbe-derived butyrate induces the differentiation of colonic regulatory T cells. Nature 504, 446–450.
Goleva, E., Harris, J.K., Robertson, C.E., Jackson, L.P., Martin, R.J., and Leung, D.Y.M. (2017). Airway microbiome and responses to corticosteroids in corticosteroid-resistant asthma patients treated with acid suppression medications. J Allergy Clin Immunol 140, 860–862.e1.
Goleva, E., Jackson, L.P., Harris, J.K., Robertson, C.E., Sutherland, E.R., Hall, C.F., Good Jr., J.T., Gelfand, E.W., Martin, R.J., and Leung, D.Y. M. (2013). The effects of airway microbiome on corticosteroid responsiveness in asthma. Am J Respir Crit Care Med 188, 1193–1201.
He, Y., Xu, L.L., Feng, F.E., Wang, Q.M., Zhu, X.L., Wang, C.C., Zhang, J. M., Fu, H.X., Xu, L.P., Liu, K.Y., et al. (2018). Mesenchymal stem cell deficiency influences megakaryocytopoiesis through the TNFAIP3/NF-κB/SMAD pathway in patients with immune thrombocytopenia. Br J Haematol 180, 395–411.
Hevia, A., Milani, C., López, P., Cuervo, A., Arboleya, S., Duranti, S., Turroni, F., Gonzàlez, S., Suàrez, A., Gueimonde, M., et al. (2014). Intestinal dysbiosis associated with systemic lupus erythematosus. mBio 5.
Huson, D.H., Auch, A.F., Qi, J., and Schuster, S.C. (2007). MEGAN analysis of metagenomic data. Genome Res 17, 377–386.
Imhann, F., Bonder, M.J., Vich Vila, A., Fu, J., Mujagic, Z., Vork, L., Tigchelaar, E.F., Jankipersadsing, S.A., Cenit, M.C., Harmsen, H.J.M., et al. (2016). Proton pump inhibitors affect the gut microbiome. Gut 65, 740–748.
Iwamura, C., Bouladoux, N., Belkaid, Y., Sher, A., and Jankovic, D. (2017). Sensing of the microbiota by NOD1 in mesenchymal stromal cells regulates murine hematopoiesis. Blood 129, 171–176.
Jackson, M.A., Goodrich, J.K., Maxan, M.E., Freedberg, D.E., Abrams, J. A., Poole, A.C., Sutter, J.L., Welter, D., Ley, R.E., Bell, J.T., et al. (2016). Proton pump inhibitors alter the composition of the gut microbiota. Gut 65, 749–756.
Jackson, S., Beck, P.L., Pineo, G.F., and Poon, M.C. (2005). Helicobacter pylori eradication: novel therapy for immune thrombocytopenic purpura? A review of the literature. Am J Hematol 78, 142–150.
Jie, Z., Xia, H., Zhong, S.L., Feng, Q., Li, S., Liang, S., Zhong, H., Liu, Z., Gao, Y., Zhao, H., et al. (2017). The gut microbiome in atherosclerotic cardiovascular disease. Nat Commun 8, 845.
Kinnebrew, M.A., Buffie, C.G., Diehl, G.E., Zenewicz, L.A., Leiner, I., Hohl, T.M., Flavell, R.A., Littman, D.R., and Pamer, E.G. (2012). Interleukin 23 production by intestinal CD103 CD11b dendritic cells in response to bacterial flagellin enhances mucosal innate immune defense. Immunity 36, 276–287.
Kong, Y., Cao, X.N., Zhang, X.H., Shi, M.M., Lai, Y.Y., Wang, Y., Xu, L.P., Chang, Y.J., and Huang, X.J. (2018). Atorvastatin enhances bone marrow endothelial cell function in corticosteroid-resistant immune thrombocytopenia patients. Blood 131, 1219–1233.
Kuwana, M., Asahi, A., Suzuki, H., Okazaki, Y., and Ikeda, Y. (2006). Eradication of Helicobacter pylori shifts the balance of Fcy receptors on monocytes toward the inhibitory FcyRIIB in patients with chronic ITP. Blood 108, 1082.
Le Chatelier, E., Nielsen, T., Qin, J., Prifti, E., Hildebrand, F., Falony, G., Almeida, M., Arumugam, M., Batto, J.M., Kennedy, S., et al. (2013). Richness of human gut microbiome correlates with metabolic markers. Nature 500, 541–546.
Lewis, J.D., Chen, E.Z., Baldassano, R.N., Otley, A.R., Griffiths, A.M., Lee, D., Bittinger, K., Bailey, A., Friedman, E.S., Hoffmann, C., et al. (2015). Inflammation, antibiotics, and diet as environmental stressors of the gut microbiome in pediatric Crohn’s disease. Cell Host Microbe 18, 489–500.
Li, J., Ma, S., Shao, L., Ma, C., Gao, C., Zhang, X.H., Hou, M., and Peng, J. (2017). Inflammation-related gene polymorphisms associated with primary immune thrombocytopenia. Front Immunol 8.
Li, R., Yu, C., Li, Y., Lam, T.W., Yiu, S.M., Kristiansen, K., and Wang, J. (2009). SOAP2: an improved ultrafast tool for short read alignment. Bioinformatics 25, 1966–1967.
Li, W., and Godzik, A. (2006). Cd-hit: a fast program for clustering and comparing large sets of protein or nucleotide sequences. Bioinformatics 22, 1658–1659.
Liu, C., Cheng, L., Ji, L., Li, F., Zhan, Y., Wu, B., Ke, Y., Chen, P., Hua, F., Yuan, L., et al. (2020). Intestinal microbiota dysbiosis play a role in pathogenesis of patients with primary immune thrombocytopenia. Thromb Res 190, 11–19.
Liu, R., Hong, J., Xu, X., Feng, Q., Zhang, D., Gu, Y., Shi, J., Zhao, S., Liu, W., Wang, X., et al. (2017). Gut microbiome and serum metabolome alterations in obesity and after weight-loss intervention. Nat Med 23, 859–868.
Luo, Y., Chen, G.L., Hannemann, N., Ipseiz, N., Krönke, G., Bäuerle, T., Munos, L., Wirtz, S., Schett, G., and Bozec, A. (2015). Microbiota from obese mice regulate hematopoietic stem cell differentiation by altering the bone niche. Cell Metab 22, 886–894.
Malnick’ S.D.H., Oppenheim, A., and Melzer, E. (2015). Immune thrombocytopenia caused by fecal microbial transplantation in a patient with severe recurrent clostridium difficile infection. J Clin Gastroenterol 49, 888–889.
Manzo, V.E., and Bhatt, A.S. (2015). The human microbiome in hematopoiesis and hematologic disorders. Blood 126, 311–318.
Maynard, C.L., Elson, C.O., Hatton, R.D., and Weaver, C.T. (2012). Reciprocal interactions of the intestinal microbiota and immune system. Nature 489, 231–241.
McMillan, R., and Nugent, D. (2005). The effect of antiplatelet autoantibodies on megakaryocytopoiesis. Int J Hematol 81, 94–99.
Miquel, S., Martín, R., Rossi, O., Bermúdez-Humaràn, L.G., Chatel, J.M., Sokol, H., Thomas, M., Wells, J.M., and Langella, P. (2013). Faecalibacterium prausnitzii and human intestinal health. Curr Opin Microbiol 16, 255–261.
Moreno, B., Fernandez-Diez, B., Di Penta, A., and Villoslada, P. (2010). Preclinical studies of methylthioadenosine for the treatment of multiple sclerosis. Mult Scler 16, 1102–1108.
Nielsen, H.B., Almeida, M., Juncker, A.S., Rasmussen, S., Li, J., Sunagawa, S., Plichta, D.R., Gautier, L., Pedersen, A.G., Le Chatelier, E., et al. (2014). Identification and assembly of genomes and genetic elements in complex metagenomic samples without using reference genomes. Nat Biotechnol 32, 822–828.
Nomura, S., Matsuzaki, T., Ozaki, Y., Yamaoka, M., Yoshimura, C., Katsura, K., Xie, G.L., Kagawa, H., Ishida, T., and Fukuhara, S. (1998). Clinical significance of HLA-DRB1*0410 in Japanese patients with idiopathic thrombocytopenic purpura. Blood 91, 3616–3622.
Patil, K.R., and Nielsen, J. (2005). Uncovering transcriptional regulation of metabolism by using metabolic network topology. Proc Natl Acad Sci USA 102, 2685–2689.
Plaza-Díaz, J., Ruiz-Ojeda, F.J., Vilchez-Padial, L.M., and Gil, A. (2017). Evidence of the anti-inflammatory effects of probiotics and synbiotics in intestinal chronic diseases. Nutrients 9, 555.
Png, C.W., Linden, S.K., Gilshenan, K.S., Zoetendal, E.G., McSweeney, C. S., Sly, L.I., McGuckin, M.A., and Florin, T.H.J. (2010). Mucolytic bacteria with increased prevalence in IBD mucosa augment in vitro utilization of mucin by other bacteria. Am J Gastroenterol 105, 2420–2428.
Provan, D., Arnold, D.M., Bussel, J.B., Chong, B.H., Cooper, N., Gernsheimer, T., Ghanima, W., Godeau, B., Gonzàlez-López, T.J., Grainger, J., et al. (2019). Updated international consensus report on the investigation and management of primary immune thrombocytopenia. Blood Adv 3, 3780–3817.
Provan, D., Stasi, R., Newland, A.C., Blanchette, V.S., Bolton-Maggs, P., Bussel, J.B., Chong, B.H., Cines, D.B., Gernsheimer, T.B., Godeau, B., et al. (2010). International consensus report on the investigation and management of primary immune thrombocytopenia. Blood 115, 168–186.
Qi, X., Li, X., Zhao, Y., Wu, X., Chen, F., Ma, X., Zhang, F., and Wu, D. (2018). Treating steroid refractory intestinal acute graft-vs.-host disease with fecal microbiota transplantation: A pilot study. Front Immunol 9, 2195.
Qin, J., Li, Y., Cai, Z., Li, S., Zhu, J., Zhang, F., Liang, S., Zhang, W., Guan, Y., Shen, D., et al. (2012). A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature 490, 55–60.
Qin, J., Li, R., Raes, J., Arumugam, M., Burgdorf, K.S., Manichanh, C., Nielsen, T., Pons, N., Levenez, F., Yamada, T., et al. (2010). A human gut microbial gene catalogue established by metagenomic sequencing. Nature 464, 59–65.
Qin, N., Yang, F., Li, A., Prifti, E., Chen, Y., Shao, L., Guo, J., Le Chatelier, E., Yao, J., Wu, L., et al. (2014). Alterations of the human gut microbiome in liver cirrhosis. Nature 513, 59–64.
Rooks, M.G., and Garrett, W.S. (2016). Gut microbiota, metabolites and host immunity. Nat Rev Immunol 16, 341–352.
Satoh, T., Miyazaki, K., Shimohira, A., Amano, N., Okazaki, Y., Nishimoto, T., Akahoshi, T., Munekata, S., Kanoh, Y., Ikeda, Y., et al. (2013). Fcy receptor IIB gene polymorphism in adult Japanese patients with primary immune thrombocytopenia. Blood 122, 1991–1992.
Sokol, H., Pigneur, B., Watterlot, L., Lakhdari, O., Bermúdez-Humaràn, L. G., Gratadoux, J.J., Blugeon, S., Bridonneau, C., Furet, J.P., Corthier, G., et al. (2008). Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proc Natl Acad Sci USA 105, 16731–16736.
Stat, M., Pochon, X., Franklin, E.C., Bruno, J.F., Casey, K.S., Selig, E.R., and Gates, R.D. (2013). The distribution of the thermally tolerant symbiont lineage (Symbiodinium clade D) in corals from Hawaii: correlations with host and the history of ocean thermal stress. Ecol Evol 3, 1317–1329.
Suzuki, T., Matsushima, M., Masui, A., Watanabe, K., Takagi, A., Ogawa, Y., Shirai, T., and Mine, T. (2005). Effect of Helicobacter pylori eradication in patients with chronic idiopathic thrombocytopenic purpura—A randomized controlled trial. Am J Gastroenterol 100, 1265–1270.
Takahashi, T., Yujiri, T., Shinohara, K., Inoue, Y., Sato, Y., Fujii, Y., Okubo, M., Zaitsu, Y., Ariyoshi, K., Nakamura, Y., et al. (2004). Molecular mimicry by Helicobacter pylori CagA protein may be involved in the pathogenesis of H. pylori-associated chronic idiopathic thrombocytopenic purpura. Br J Haematol 124, 91–96.
Thomas, T.J., Meryhew, N.L., and Messner, R.P. (1990). Enhanced binding of lupus sera to the polyamine-induced left-handed Z-DNA form of polynucleotides. Arthritis Rheum 33, 356–365.
Tsutsumi, Y., Kanamori, H., Yamato, H., Ehira, N., Kawamura, T., Umehara, S., Mori, A., Obara, S., Ogura, N., Tanaka, J., et al. (2005). Randomized study of Helicobacter pylori eradication therapy and proton pump inhibitor monotherapy for idiopathic thrombocytopenic purpura. Ann Hematol 84, 807–811.
Wang, Q., Li, J., Yu, T.S., Liu, Y., Li, K., Liu, S., Liu, Y., Feng, Q., Zhang, L., Li, G.S., et al. (2019). Disrupted balance of CD4+ T-cell subsets in bone marrow of patients with primary immune thrombocytopenia. Int J Biol Sci 15, 2798–2814.
Wang, T., Zhao, H., Ren, H., Guo, J., Xu, M., Yang, R., and Han, Z.C. (2005). Type 1 and type 2 T-cell profiles in idiopathic thrombocytopenic purpura. Haematologica 90, 914–923.
Wen, C., Zheng, Z., Shao, T., Liu, L., Xie, Z., Le Chatelier, E., He, Z., Zhong, W., Fan, Y., Zhang, L., et al. (2017). Quantitative metagenomics reveals unique gut microbiome biomarkers in ankylosing spondylitis. Genome Biol 18, 142.
Wu, H., Esteve, E., Tremaroli, V., Khan, M.T., Caesar, R., Mannerås-Holm, L., Ståhlman, M., Olsson, L.M., Serino, M., Planas-Fèlix, M., et al. (2017). Metformin alters the gut microbiome of individuals with treatment-naive type 2 diabetes, contributing to the therapeutic effects of the drug. Nat Med 23, 850–858.
Xing, J., Ying, Y., Mao, C., Liu, Y., Wang, T., Zhao, Q., Zhang, X., Yan, F., and Zhang, H. (2018). Hypoxia induces senescence of bone marrow mesenchymal stem cells via altered gut microbiota. Nat Commun 9, 2020.
Zhang, J.M., Feng, F.E., Wang, Q.M., Zhu, X.L., Fu, H.X., Xu, L.P., Liu, K. Y., Huang, X.J., and Zhang, X.H. (2016). Platelet-derived growth factor-BB protects mesenchymal stem cells (MSCs) derived from immune thrombocytopenia patients against apoptosis and senescence and maintains MSC-mediated immunosuppression. Stem Cells Transl Med 5, 1631–1643.
Zhang, W., Nardi, M.A., Borkowsky, W., Li, Z., and Karpatkin, S. (2009). Role of molecular mimicry of hepatitis C virus protein with platelet GPIIIa in hepatitis C-related immunologic thrombocytopenia. Blood 113, 4086–4093.
Zhang, X., Zhang, D., Jia, H., Feng, Q., Wang, D., Liang, D., Wu, X., Li, J., Tang, L., Li, Y., et al. (2015). The oral and gut microbiomes are perturbed in rheumatoid arthritis and partly normalized after treatment. Nat Med 21, 895–905.
Zhu, W., Lomsadze, A., and Borodovsky, M. (2010). Ab initio gene identification in metagenomic sequences. Nucleic Acids Res 38, e132.
Acknowledgements
This work was supported by Beijing Municipal Science and Technology Commission (Z171100001017084), Natural Science Foundation of Beijing Municipality (7171013 and H2018206423), Key Program of National Natural Science Foundation of China (81730004), the National Natural Science Foundation of China (81670116 and 81970113), and National Key Research and Development Program of China (2017YFA0105503).
Author information
Authors and Affiliations
Corresponding author
Additional information
Compliance and ethics
The author(s) declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, Y., Liu, F., Zhang, G. et al. Gut microbiome alterations and its link to corticosteroid resistance in immune thrombocytopenia. Sci. China Life Sci. 64, 766–783 (2021). https://doi.org/10.1007/s11427-020-1788-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11427-020-1788-2