Abstract
Shikonin, a major effective component in the Chinese herbal medicine Lithospermum erythrorhizon Sieb., exhibits an anti-inflammatory property towards rheumatoid arthritis (RA), but the potential mechanism is unclear. Our aim was to investigate the mechanism of shikonin on the lipopolysaccharide (LPS)-induced fibroblast-like synoviocyte (LiFLS) inflammation model. Fibroblast-like synoviocytes (FLSs) were treated with 200 μg/ml of LPS for 24 h to establish the RA-like model, LiFLS. FLSs were pretreated with shikonin (0.1–1 μM) for 30 min in the treatment groups. Quantitative real-time polymerase chain reaction and enzyme-linked immunosorbent assays were used to detect mRNA and protein levels of interleukin (IL)-10 and tumor necrosis factor (TNF)-α. Signal proteins involved in IL-10 production were analyzed by Western blotting. Shikonin significantly reversed the inhibitory effects of LPS on IL-10 expression in FLSs by inactivating the PKC-NF-κB pathway. In addition, shikonin inhibited LPS-induced TNF-α expression in FLSs, and this effect was markedly diminished by IL-10-neutralizing antibody. The IL-10-mediated suppression of TNF-α transcription was demonstrated by no response to the protein synthesis inhibitor cyclohexamide and no mRNA decay. Shikonin inhibits LPS-induced TNF-α production in FLSs through suppressing the PKC-NF-κB-dependent decrease in IL-10, and this study also highlights the potential application of shikonin in the treatment of RA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA), one of the most common chronic autoimmune diseases, is characterized by chronic inflammation, articular destruction and abnormal immune response [1]. Fibroblast-like synoviocytes (FLSs) are key cellular participants in RA and are crucial in initiating and driving RA in concert with inflammatory cells [2,3,4]. The principal treatment for arthritis patients is non-steroidal anti-inflammatory drugs (NSAIDs), such as indomethacin, which has been shown to reduce the expression of inflammatory factors in lipopolysaccharide (LPS)-induced FLSs (LiFLSs) [5]. However, anti-inflammatory agents have the risk of gastrointestinal toxicity, heart failure, etc. [6, 7], and therefore new anti-inflammatory drugs urgently need to be discovered.
Shikonin, the major active substance in Lithospermum erythrorhizon Sieb., has been reported to mediate multiple pharmacological activities such as antioxidation, antiviral, cardiovascular protection, antineoplastic and anti-inflammation [8,9,10,11]. In RA, researchers found that shikonin could inhibit inflammation, regulate immunity and relieve pathological joint lesions in a mouse RA model which was induced by collagen type II in the late period [12].
In the collagen type II-induced murine arthritis model, shikonin was found to induce interleukin (IL)-10 production through a GATA-3-dependent mechanism in vivo [13]. IL-10 is an immunosuppressive cytokine in inflammatory responses [14]. Increasing evidence shows that IL-10 is elevated in peripheral blood and synovial joints of RA patients [15,16,17]. In addition, Shikonin was also found to inhibit tumor necrosis factor (TNF)-α production in human macrophage and murine cells [8, 9]. TNF-α is a proinflammatory cytokine that plays a pivotal role in enhancing the inflammatory response in RA, and is abundantly presented in RA patients’ serum and the arthritic synovium [18]. Inhibitors specific for TNF-α have demonstrated efficacy as monotherapy or in combination with NSAIDs in the treatment of RA. Based on these observations, we speculated that shikonin inhibits TNF-α production through induction of IL-10 expression, but no data has fully demonstrated this pathway.
In the present study, we further investigated the effect of shikonin on IL-10 and TNF-α production in a RA-like model, LiFLSs. Our results showed that shikonin could induce the expression of IL-10 and inhibit protein kinase C (PKC) and NF-κBp65 protein in LiFLSs. Moreover, inhibition of either PKC or NF-κB increased shikonin-induced IL-10 production, and the induction of IL-10 further promoted the down-regulation of TNF-α mRNA. This study provides novel insight into the anti-inflammatory mechanisms of shikonin, and suggests the application of shikonin in the treatment of RA.
Materials and methods
Establishment of RA-like model
Fibroblast-like synoviocytes (FLSs) were isolated from knees of rats. Synovial membranes were minced and digested with 1 mg/ml collagen type II (Sigma) in DMEM (Hyclone) at 37 °C for 1 h in 5% CO2. After centrifugation and washing, the cells were resuspended in DMEM supplemented with 10% fetal bovine serum (Gibco), 100 U/ml penicillin and 100 U/ml streptomycin (Beyotime Institute of Biotechnology, Haimen, China). Non-adherent cells were removed after 24 h and adherent cells were trypsinized with 0.25% trypsin (Hyclone) at confluence and then plated in culture flasks. To obtain a homogeneous population of synoviocytes, confluent cultures from passages 3–7 were used. FLSs were verified by immunocytochemistry (BOSTER) as a homogeneous population (phenotype: >99% vimentin and <1% CD68, data not shown). FLSs were treated with 200 μg/ml of LPS for 24 h to establish the RA-like model, LiFLSs.
Western blot analysis
LiFLSs were lysed in RIPA [50 mM Tris (pH 7.4), 150 mM NaCl, 1% Triton X-100, 1% sodium deoxycholate, 0.1% SDS] buffer containing protease inhibitor mixture (0.1% CTAB, Sigma). Cytoplasmic and nuclear extraction was performed using the protocol reported by Jobin [19]. Lysate (50 µg of protein) was separated on 5–12% SDS–polyacrylamide gel and transferred onto polyvinylidene difluoride membranes (Millipore) using a Mini Tank Transfer System (Bio-Rad Laboratories, Hercules, CA, USA) at 200 mA for 2 h. The blots were blocked with 5% skim milk, followed by incubation with antibodies anti-p-NF-κBp65 (cat. no. ab86299; 1:2000; Abcam, Cambridge, MA, USA), anti-NF-κBp65 (cat. no. ab16502; 1:2000; Abcam), anti-pIκBα (cat. no. ab92700; 1:1000; Abcam), anti-IκBα (cat. no. ab97783; 1:1000; Abcam), anti-pIKKα (cat. no. ab38515; 1:500; Abcam), anti-IKKα (cat. no. ab32041; 1:10,000; Abcam), anti-PKCβ (cat. no. ab32026; 1:1000; Abcam) and anti-GAPDH (cat. no. 5174; 1:1500, Cell Signaling Technology, Inc., Danvers, MA, USA) overnight at 4 °C. Blots were then incubated with goat anti-mouse or anti-rabbit horseradish peroxidase-conjugated IgG antibodies (cat. nos. A0208 and A0216; 1:1000; Beyotime) for 1 h at 37 °C. Proteins were detected using Western blotting and visualized by chemiluminescence (Pierce, SuperSignal West Pico Chemiluminescent Substrate).
Quantitative real-time polymerase chain reaction (qRT-PCR)
mRNA expression of TNF-α and IL-10 was analyzed by using the ABI 7300 real-time PCR system (Foster City, CA, USA). Primer pairs were TNF-α [20]: 5′-TTCTCATTCCTGCTCGTGG-3′ and 5′-TTTGGTGGTTCGCCTCCT-3′; IL-10 [21]: 5′-TGCCAAGCCTTGTCAGAAATGATCAAG-3′ and 5′-GTATCCAGAGGGTCTTCAGCTTCTCTC-3′; and GAPDH [22]: 5′-TGGCCTCCAAGGAGTAAGAAAC-3′ and 5′-GGCCTCTCC CTCTCAGTATC-3′. The reverse transcription reaction was performed with 1 µg total RNA. cDNAs were amplified using SYBR Green Real-time PCR Master Mix (Takara) and 0.4 µmol/L of each primer pair. The reaction was carried out with an initial step at 94 °C for 30 s, followed by 40 cycles of amplification step (94 °C for 30 s, 60 °C for 60 s, and 72 °C for 1 min). Each sample was analyzed in triplicate and the averages of the threshold cycles were used to interpolate curves using 7300 System SDS software. Results were expressed as the relative expression to the internal control GAPDH.
Enzyme-linked immunosorbent assays
Culture medium was harvested at the indicated time. The concentrations of TNF-α and IL-10 in the supernatant of cultured cells were detected by sandwich enzyme-linked immunosorbent assay (ELISA) kits (Dingguo, Beijing, China) according to the manufacturer’s protocol.
Statistical analysis
Results are expressed as mean ± SD. The data were analyzed by one-way ANOVA followed by the Student–Newman–Keuls test for multiple comparisons. Results were considered statistically significant at p < 0.05.
Results
Shikonin induced the up-regulation of IL-10 and down-regulation of TNF-α
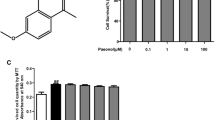
IL-10, an important immunosuppressive mediator, is usually down-regulated in RA. In LiFLSs, IL-10 was reduced by LPS, while shikonin reversed the mRNA expression of IL-10 in a dose-dependent manner (Fig. 1a). In particular, 1 μM of shikonin showed similar potency to the positive control indomethacin, an anti-inflammatory agent for RA. We then detected the production of IL-10 protein, as shown in Fig. 2a; shikonin also significantly reversed the IL-10 production which was decreased by LPS. TNF-α is the major macrophage-derived inflammatory cytokine in the rheumatoid joint of RA patients and induces the synthesis and secretion of various proinflammatory cytokines, such as IL-6 and IL-8 in synovial fibroblasts [23]. In our results, shikonin markedly decreased the mRNA and protein level of TNF-α in LiFLSs (Figs. 1b, 2b). As for the inhibitory effect on TNF-α, shikonin showed similar potency to the positive control indomethacin. However, shikonin had no effects on the mRNA expression and production of IL-10 and TNF-α under LPS-free conditions (p > 0.05; data not shown).
Effect of shikonin on mRNA expression of TNF-α and IL-10 in LiFLSs. Fibroblast-like synoviocytes were treated with LPS (200 μg/ml) for 24 h to establish the RA-like model, LiFLSs. a IL-10 and b TNF-α mRNA expression were quantified by qRT-PCR and normalized to GAPDH. Values are mean ± SD (n = 3). **p < 0.01 and ***p < 0.001
Effect of shikonin on protein production of TNF-α and IL-10 in LiFLSs. Fibroblast-like synoviocytes were treated with LPS (200 μg/ml) for 24 h to establish the RA-like model, LiFLSs. a IL-10 and b TNF-α protein production in supernatant were quantified by ELISA. Values are mean ± SD (n = 3). *p < 0.05 and ***p < 0.0001, NS no significant difference
Shikonin induced the expression of IL-10 through the PKC-NF-κB pathway
In order to determine how shikonin increased the expression of IL-10, we pretreated with various signal protein inhibitors and then carried out shikonin treatment. As shown in Fig. 3a, IL-10 production was promoted by LY333531 (10 nM, protein kinase C inhibitor) and pyrrolidine dithiocarbamate (PDTC; 10 μM, NF-κB inhibitor), but not by JNK inhibitor (40 nM, SP600125), MEK1 inhibitor (2 μM, PD98059), PI3 K inhibitor (1 μM, LY294002), P38 inhibitor (0.5 μM, SB203580) or AP1 inhibitor (100 nM, BMS-536924). However, these inhibitors had no effects on the production of IL-10 under shikonin but LPS-free conditions (p > 0.05; data not shown). According to the previous report, PKC was found to be involved in IL-10 production in an LPS-induced endotoxemia model [24], and promoted the downstream activation of NF-κB in mice melanoma cells [25]. Based on these clues, we further examined the protein expression of PKCβ, NF-κBp65 and its upstream components IKKα and IκB [26] in shikonin-treated LiFLSs. The result showed that pretreatment with shikonin could dramatically decrease the expression of pNF-κBp65, pIκB, pIKKα and PKCβ, but increase the expression of IκB (Fig. 3b). However, shikonin had no effect on expressions of NF-κB, pIκB, pIKKα, IKKα and PKCβ under LPS-free conditions (p > 0.05; data not shown). These results demonstrated that shikonin induced the expression of IL-10 through inactivating the PKC-NF-κB pathway.
Shikonin induces IL-10 production through PKC-NF-κB pathway in LiFLSs. a All signal protein inhibitors (10 nM LY333531, 10 μM PDTC, 40 nM SP600125, 2 μM PD98059, 1 μM LY294002, 0.5 μM SB203580 and 100 nM BMS-536924) treated LiFLSs 1 h before shikonin treatment; 0.1% DMSO was solvent control to inhibitors. IL-10 protein in supernatant was quantified by ELISA. Values are mean ± SD (n = 3). b Cells were pretreated with shikonin for 30 min at different indicated concentrations. Proteins were quantified by Western blotting and normalized to GAPDH. ***p < 0.0001
Shikonin decreased TNF-α expression through IL-10
It was reported that IL-10 inhibits the transcription of TNF-α [27, 28], so we investigated whether there is a connection between IL-10 and TNF-α that is induced by shikonin. LiFLSs were pretreated with IL-10 antibody, as shown in Fig. 4; the decrease in TNF-α protein secretion and mRNA expression induced by shikonin was reversed by the addition of IL-10 neutralizing antibody (Fig. 4a, b).
IL-10 induced by shikonin inhibited TNF-α production in LiFLSs at least in part by down-regulated expression of TNF-α mRNA. a Cells were treated with 1 μM shikonin 30 min before LPS treatment with or without 4 μg/ml IL-10 antibody. TNF-α protein production in supernatant was quantified by ELISA. Values are mean ± SD (n = 3). b In addition to some groups the same as a, cells were treated with recombinant IL-10 (50 U/ml) with or without cycloheximide (5 μg/ml) 1 h before LPS treatment; supernatant means medium used to culture FLSs was replaced by supernatant from shikonin-treated LiFLSs before the addition of cycloheximide. TNF-α mRNA expression was quantified by qRT-PCR and normalized to GAPDH. c Shikonin with or without IL-10-antibody-treated cells 30 min before LPS treatment. Following incubation with LPS for 1 h, 5 μg/ml actinomycin D was added and cells were lysed at 1, 2, 4, 6 and 8 h following the addition of actinomycin D. TNF-α mRNA expression was quantified by qRT-PCR and normalized to GAPDH. Values are mean ± SD (n = 3). **p < 0.01 and ***p < 0.0001
To determine whether protein synthesis was involved in the IL-10-mediated suppression of TNF-α, the protein synthesis inhibitor cycloheximide was used. However, considering that cycloheximide inhibits all protein synthesis, as shown in Fig. 4b, cycloheximide totally blocked the inhibitory effect of shikonin on TNF-α transcription. This may be due to cycloheximide inhibiting IL-10 production induced by shikonin, so we added recombinant IL-10 (50 U/ml) or replaced the medium with the supernatant from shikonin-treated LiFLSs to exclude the inhibitory effect of cycloheximide on IL-10 production. In the presence of cycloheximide (5 μg/ml), which at this dose has been shown to have an inhibitory effect on translation [29], IL-10 decreased TNF-α mRNA levels (Fig. 4b). In other words, in the presence of cycloheximide, the supernatant from shikonin-treated LiFLSs also down-regulated TNF-α expression, which might be caused by IL-10 or other inhibitory molecules in the supernatant of shikonin-treated LiFLSs. Overall, these data demonstrated that IL-10 induced by shikonin suppresses the transcription of TNF-α independent of protein synthesis, and other substances induced by shikonin may also be involved in the inhibition of TNF-α mRNA expression.
In order to exclude the possibility that IL-10 could shorten the half-life of TNF-α mRNA and thus decrease TNF-α production, we also assessed the half-life of TNF-α mRNA in the presence of 5 μg/ml actinomycin D, which at this dose has been shown to inhibit translation [30, 31]. Following actinomycin D treatment, mRNA was extracted at different time points. No significant difference was seen in the rate of TNF-α mRNA decay in the shikonin-treated groups with or without IL-10 antibody (Fig. 4c). This result indicated that TNF-α was not reduced by IL-10 through increasing its mRNA decay.
Discussion
RA is characterized by the proliferation of the synovial membrane into a pannus, which includes resident fibroblast-like synoviocytes (FLSs) and infiltrating mononuclear cells capable of producing inflammatory cytokines [32]. Prompt treatment is the key to preventing joint destruction and organ damage; traditionally RA has been treated with disease-modifying anti-rheumatic drugs, NSAIDs, but NSAID tablets can increase the risk of serious stomach problems, and thus new drugs urgently need to be found.
Shikonin, a major active chemical component isolated from the dried root of Lithospermum erythrorhizon (LE), possesses numerous pharmacological properties, including anti-inflammatory and antitumor properties and promotion of wound healing activity [33]. It was reported that shikonin significantly inhibits the concentrations of TNF-α, IL-6 and IL-1β in bronchoalveolar lavage fluid and primary macrophage cultures induced by LPS [10, 11, 34]. In RA, shikonin also exerts beneficial effects on collagen-induced arthritis (CIA), a mouse RA model, and markedly reduces joint swelling and cartilage destruction [12, 13].
In this study, we investigated the potential beneficial effects of shikonin in an RA-like model: LPS (200 μg/ml)-induced fibroblast-like synoviocyte (LiFLS) inflammation. However, others have reported that LPS at a lower concentration of 1 μg/ml could also induce IL-6 secretion, but activated FLSs did not release any detectable amount of mature IL-18 [35]. Similarly, increased IL-6 and CXCL-10 production and p38 phosphorylation were found in LPS (1 μg/ml)-activated RA LiFLSs [36]. Our result showed that shikonin significantly increased the level of the anti-inflammatory cytokine IL-10. IL-10 can effectively block the production of the proinflammatory cytokines TNF-α, IL-1 and IL-8 in synovial macrophages and synoviocytes [37,38,39]. IL-10 was also found to inhibit TNF-α production in interferon-γ-activated macrophages [40], and has been used in the treatment of RA in clinical trials [41, 42]. In this study, we found that shikonin inhibited TNF-α production through IL-10 in LiFLSs, and exerted a similar potency to indomethacin. These results suggested that shikonin may serve as an effective candidate for the treatment of RA.
We investigated which pathway is involved in the shikonin-induced up-regulation of IL-10. In bone marrow-derived dendritic cells, glycogen synthase kinase-3 inhibition has been shown to induce PKC and ERK1/2 activation, and thus provoke the production of IL-10 [24]. NF-κB activation is normally correlated with the production of proinflammatory cytokines, such as IL-6 and IL-8 [43], and mediates inflammation [44]. To date, only one report on HIV transactivating Tat protein found that Tat protein [45] induces NF-κB activation and thus promotes production of IL-10 through at least three signaling pathways concurrently, including the classical and alternative IKKa pathways. However, we demonstrated IL-10 production in shikonin-treated LiFLSs in the presence of seven signal protein inhibitors; this result showed that PKC inhibitor and NF-κB inhibitor both significantly enhanced this effect. Decreased NF-κB phosphorylation could increase the expression of IL-10 and is associated with PKC signaling [46, 47]. In our study, shikonin also markedly decreased PKC expression, IKKα phosphorylation and NF-κBp65 translocation.
It was found that IL-10 could inhibit TNF-α production in synoviocytes [37], and that shikonin suppresses the basal transcription and activator-regulated transcription of TNF-α by inhibiting the binding of transcription factor IID protein complex (TATA box-binding protein) to the TATA box [8]. In our results, we found that IL-10 antibody markedly reduced the inhibitory function of shikonin on TNF-α, though still less than the concentration of TNF-α in LiFLSs. Before adding cycloheximide into the medium of FLSs, we replaced the medium with the supernatant from shikonin-treated LiFLSs. Compared with the exogenous IL-10-treated group, the supernatant inhibited TNF-α transcription more effectively than exogenous IL-10, implying that shikonin may have other ways to down-regulate TNF-α production. mRNA half-life analysis showed that IL-10 has no influence on TNF-α mRNA degradation. Taken together, these results demonstrated that IL-10 inhibits TNF-α through its transcription level.
In summary, this study demonstrated the mechanism of shikonin in the treatment of RA. By using a RA-like cell model, LiFLSs, we found that shikonin has anti-inflammatory effects on LiFLSs by targeting IL-10 and TNF-α, two key cytokines in the development of RA pathogenesis. Shikonin inhibited TNF-α transcription by suppressing the PKC-NF-κB-dependent decrease in IL-10 production. Our work highlights the potential application of shikonin in the treatment of RA in future.
References
Filippin LI, Vercelino R, Marroni N, Xavier RM (2008) Redox signalling and the inflammatory response in rheumatoid arthritis. Clin Exp Immunol 152:415–422
Cheon H, Yu SJ, Yoo D, Chae I, Song G, Sohn J (2002) Increased expression of pro-inflammatory cytokines and metalloproteinase-1 by TGF-β1 in synovial fibroblasts from rheumatoid arthritis and normal individuals. Clin Exp Immunol 127:547–552
Xu H, He Y, Yang X, Liang L, Zhan Z, Ye Y, Sun L (2007) Anti-malarial agent artesunate inhibits TNF-α-induced production of proinflammatory cytokines via inhibition of NF-κB and PI3 kinase/Akt signal pathway in human rheumatoid arthritis fibroblast-like synoviocytes. Rheumatology 46:920–926
Bartok B, Firestein GS (2010) Fibroblast-like synoviocytes: key effector cells in rheumatoid arthritis. Immunol Rev 233:233–255
Kawashima M, Ogura N, Akutsu M, Ito K, Kondoh T (2013) The anti-inflammatory effect of cyclooxygenase inhibitors in fibroblast-like synoviocytes from the human temporomandibular joint results from the suppression of PGE2 production. J Oral Pathol Med 42:499–506
Henry D, Lim LL, Rodriguez LAG, Gutthann SP, Carson JL, Griffin M, Savage R, Logan R, Moride Y, Hawkey C, Hill S, Fries JT (1996) Variability in risk of gastrointestinal complications with individual non-steroidal anti-inflammatory drugs: results of a collaborative meta-analysis. BMJ 312:1563–1566
MacDonald T, Morant S, Robinson GC, Shield MJ, McGilchrist MM, Murray FE, McDevitt DG (1997) Association of upper gastrointestinal toxicity of non-steroidal anti-inflammatory drugs with continued exposure: cohort study. BMJ 315:1333–1337
Staniforth V, Wang SY, Shyur LF, Yang NS (2004) Shikonins, phytocompounds from Lithospermum erythrorhizon, inhibit the transcriptional activation of human tumor necrosis factor α promoter in vivo. J Biol Chem 279:5877–5885
Chiu SC, Yang NS (2007) Inhibition of tumor necrosis factor-α through selective blockade of pre-mRNA splicing by shikonin. Mol Pharmacol 71:1640–1645
Lu L, Qin A, Huang H, Zhou P, Zhang C, Liu N, Li S, Wen G, Zhang C, Dong W, Wang X, Dou P, Liu J (2011) Shikonin extracted from medicinal Chinese herbs exerts anti-inflammatory effect via proteasome inhibition. Eur J Pharmacol 658:242–247
Liang D, Sun Y, Shen Y, Li F, Song X, Zhou E, Zhao F, Liu Z, Fu Y, Guo M, Zhang N, Yang Z, Cao Y (2013) Shikonin exerts anti-inflammatory effects in a murine model of lipopolysaccharide-induced acute lung injury by inhibiting the nuclear factor-kappaB signaling pathway. Int Immunopharmacol 16:475–480
Kim YO, Hong SJ, Yim SV (2010) The efficacy of shikonin on cartilage protection in a mouse model of rheumatoid arthritis. Korean J Physiol Pharmacol 14:199–204
Dai Q, Fang J, Zhang FS (2009) Dual role of shikonin in early and late stages of collagen type II arthritis. Mol Biol Rep 36:1597–1604
Asadullah K, Sterry W, Volk H (2003) Interleukin-10 therapy-review of a new approach. Pharmacol Rev 55:241–269
Katsikis PD, Chu CQ, Brennan FM, Maini RN, Feldmann M (1994) Immunoregulatory role of interleukin 10 in rheumatoid arthritis. J Exp Med 179:1517–1527
Llorente L, Richaud-Patin Y, Fior R, Alcocer-Varela J, Wijdenes J, Fourrier BM, Galanaud P, Emilie D (1994) In vivo production of interleukin-10 by non-T cells in rheumatoid arthritis, Sjögren’s syndrome, and systemic lupus erythematosus. Arthritis Rheum 37:1647–1655
Cush JJ, Splawski JB, Thomas R, Mcfarlin JE, Schulze-Koops H, Schulze-Koops H, Davis LS, Fujita K, Lipsky PE (1995) Elevated interleukin-10 levels in patients with rheumatoid arthritis. Arthritis Rheum 38:96–104
Moelants EA, Mortier A, Van Damme J, Proost P (2013) Regulation of TNF-α with a focus on rheumatoid arthritis. Immunol Cell Biol 91:393–401
Jobin C, Haskill S, Mayer L, Panja A, Sartor RB (1997) Evidence for altered regulation of I kappa B alpha degradation in human colonic epithelial cells. J Immunol 158:226–234
Song SS, Huang B, Wang QT, Wu YJ, Fu JJ, Zhang YF, Chang Y, Chen ZY, Wu HX, Wang D, Zhang LL, Wei W (2013) BF02, a recombinant TNFR2 fusion protein, alleviates adjuvant arthritis by regulating T lymphocytes in rats. Acta Pharmacol Sin 34:414–423
Matsuda S, Uchikawa R, Yamada M, Arizono N (1995) Cytokine mRNA expression profiles in rats infected with the intestinal nematode Nippostrongylus brasiliensis. Infect Immun 63:4653–4660
Padegimas L, Kowalczyk TH, Adams S, Gedeon CR, Oette SM, Dines K, Hyatt SL, Sesenoglu-Laird O, Tyr O, Moen RC, Cooper MJ (2012) Optimization of hCFTR lung expression in mice using DNA nanoparticles. Mol Ther 20:63–72
Matsuno H, Yudoh K, Katayama R, Nakazawa F, Uzuki M, Sawai T, Yonezawa T, Saeki Y, Panayi GS, Pitzalis C (2002) The role of TNF-α in the pathogenesis of inflammation and joint destruction in rheumatoid arthritis (RA): a study using a human RA/SCID mouse chimera. Rheumatology 41:329–337
Noh KT (2014) Protein kinase C delta (PKCδ)- extracellular-signal regulated kinase 1/2 (ERK1/2) signaling cascade regulates glycogen synthase kinase-3 (GSK-3) inhibition- mediated interleukin-10 (IL-10) expression in lipopolysaccharide (LPS)-induced endotoxemia (IRM5P. 704). J Immunol 192:62–65
La Porta C, Comolli R (1997) PKC-dependent modulation of IkB alpha-NFkB pathway in low metastatic B16F1 murine melanoma cells and in highly metastatic BL6 cells. Anticancer Res 18:2591–2597
Lee JW, Cheong IY, Kim HS, Lee JJ, Lee YS, Kwon YS, Kim MJ, Lee HJ, Kim SS, Chun W (2011) Anti-inflammatory activity of 1-docosanoyl cafferate isolated from Rhus verniciflua in LPS-stimulated BV2 microglial cells. Korean J Physiol Pharmacol 15:9–15
Armstrong L, Jordan N, Millar A (1996) Interleukin 10 (IL-10) regulation of tumour necrosis factor alpha (TNF-alpha) from human alveolar macrophages and peripheral blood monocytes. Thorax 51:143–149
Smallie T, Ricchetti G, Horwood NJ, Feldmann M, Clark AR, Williams LM (2010) IL-10 inhibits transcription elongation of the human TNF gene in primary macrophages. J Exp Med 207:2081–2088
Schneider-Poetsch T, Ju J, Eyler DE, Jewett JC, Bhat S, Rawal VH, Green R, Liu JO (2010) Inhibition of eukaryotic translation elongation by cycloheximide and lactimidomycin. Nat Chem Biol 6:209–217
Leclerc GJ, Leclerc GM, Barredo JC (2002) Real-time RT-PCR analysis of mRNA decay: half-life of Beta-actin mRNA in human leukemia CCRF-CEM and Nalm-6 cell lines. Cancer Cell Int 2:1
Weidensdorfer D, Stöhr N, Baude A, Lederer M, Köhn M, Schierhorn A, Buchmeier S, Wahle E, Hüttelmaier S (2009) Control of c-myc mRNA stability by IGF2BP1-associated cytoplasmic RNPs. RNA 15:104–115
Hur GM, Hwang YB, Lee JH, Bae SH, Park JS, Lee CJ, Seok JH (2003) Caffeic acid phenethyl ester inhibits the PKC-induced IL-6 gene expression in the synoviocytes of rheumatoid arthritis patients. Korean J Physiol Pharmacol 7:363–368
Chen X, Yang L, Oppenheim JJ, Howard O (2002) Cellular pharmacology studies of shikonin derivatives. Phytother Res 16:199–209
Bai GZ, Yu HT, Ni YF, Li XF, Zhang ZP, Su K, Lei J, Liu BY, Ke CK, Zhong DX (2013) Shikonin attenuates lipopolysaccharide-induced acute lung injury in mice. J Surg Res 182:303–311
Alsaleh G, Suffert G, Semaan N, Juncker T, Frenzel L, Gottenberg JE, Sibilia J, Pfeffer S, Wachsmann D (2009) Bruton’s tyrosine kinase is involved in miR-346-related regulation of IL-18 release by lipopolysaccharide-activated rheumatoid fibroblast-like synoviocytes. J Immunol 182:5088–5097
Philippe L, Alsaleh G, Pichot A, Ostermann E, Zuber G, Frisch B, Sibilia J, Pfeffer S, Bahram S, Wachsmann D (2013) MiR-20a regulates ASK1 expression and TLR4-dependent cytokine release in rheumatoid fibroblast-like synoviocytes. Ann Rheum Dis 72:1071–1079
Chomarat P, Vannier E, Dechanet J, Rissoan MC, Banchereau J, Dinarello CA, Miossec P (1995) Balance of IL-1 receptor antagonist/IL-1 beta in rheumatoid synovium and its regulation by IL-4 and IL-10. J Immunol 154:1432–1439
Hart P, Ahern M, Smith M, Finlay-Jones J (1995) Comparison of the suppressive effects of interleukin-10 and interleukin-4 on synovial fluid macrophages and blood monocytes from patients with inflammatory arthritis. Immunology 84:536
Hart PH, Hunt EK, Bonder CS, Watson CJ, Finlay-Jones JJ (1996) Regulation of surface and soluble TNF receptor expression on human monocytes and synovial fluid macrophages by IL-4 and IL-10. J Immunol 157:3672–3680
Oswald IP, Wynn TA, Sher A, James SL (1992) Interleukin 10 inhibits macrophage microbicidal activity by blocking the endogenous production of tumor necrosis factor alpha required as a costimulatory factor for interferon gamma-induced activation. Proc Natl Acad Sci USA 89:8676–8680
Chernoff AE, Granowitz EV, Shapiro L, Vannier E, Lonnemann G, Angel JB, Kennedy JS, Rabson AR, Wolff SM, Dinarello CA (1995) A randomized, controlled trial of IL-10 in humans. Inhibition of inflammatory cytokine production and immune responses. J Immunol 154:5492–5499
St Clair EW (1999) Interleukin 10 treatment for rheumatoid arthritis. Ann Rheum Dis 58:I99–I102
Matsusaka T, Fujikawa K, Nishio Y, Mukaida N, Matsushima K, Kishmoto T, Akira S (1993) Transcription factors NF-IL6 and NF-kappa B synergistically activate transcription of the inflammatory cytokines, interleukin 6 and interleukin 8. Proc Natl Acad Sci USA 90:10193–10197
Tak PP, Firestein GS (2001) NF-κB: a key role in inflammatory diseases. J Clin Invest 107:7–11
Leghmari K, Bennasser Y, Bahraoui E (2008) HIV-1 Tat protein induces IL-10 production in monocytes by classical and alternative NF-κB pathways. Eur J Cell Biol 87:947–962
Correa F, Hernangomez M, Mestre L, Loria F, Spagnolo A, Docagne F, Di Marzo V, Guaza C (2010) Anandamide enhances IL-10 production in activated microglia by targeting CB(2) receptors: roles of ERK1/2, JNK, and NF-kappaB. Glia 58:135–147
Zhang J, Ping P, Vondriska TM, Tang XL, Wang GW, Cardwell EM, Bolli R (2003) Cardioprotection involves activation of NF-kappa B via PKC-dependent tyrosine and serine phosphorylation of I kappa B-alpha. Am J Physiol Heart Circ Physiol 285:H1753–H1758
Acknowledgements
This work was supported by grants from the Science and Technology Planning Natural Scientific Foundation of Hubei Province of China (2010CDB07501).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that no conflict of interests exists.
Additional information
W.-X. Sun and Y. Liu contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
11418_2016_1064_MOESM1_ESM.tif
Supplementary Fig. 1. Identification of FLSs by microscope and flow cytometry. LiFLSs was identified by (a) microscopy (200× and 400×) or (b) flow cytometry using antibodies anti-vimentin and anti-CD68. (TIFF 556 kb)
Rights and permissions
About this article
Cite this article
Sun, WX., Liu, Y., Zhou, W. et al. Shikonin inhibits TNF-α production through suppressing PKC-NF-κB-dependent decrease of IL-10 in rheumatoid arthritis-like cell model. J Nat Med 71, 349–356 (2017). https://doi.org/10.1007/s11418-016-1064-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-016-1064-3