Abstract
There are inconsistent reports on the association between air pollution and cancers. This systematic review was, therefore, conducted to ascertain the relationship between air pollution and some cancers. This is a systematic review study, which all articles published in this area were extracted from January 1, 1950 to December 31, 2018 from Web of Science, PubMed, Scopus, Cochrane Library, MEDLINE, EMBASE, Science Direct, Google scholar. Searching was performed independently by two search-method experts. The required data were extracted from the articles by an author-made questionnaire. Forty-eight articles were investigated. Evidence linking air pollution to some cancers is limited. Leukemia had the highest association with exposure to various air pollutants and bladder cancer had the lowest association. It is noteworthy that the specific type of pollutants in all studies was not specified. Based on the findings, the results are contradictory, and the role of air pollution in some cancers cannot be supported. Accordingly, studies are recommended to be performed at the individual level or multifactorial studies to specifically investigate the relationship between air pollution and these types of cancers. In this way, the role of air pollution in the incidence of these cancers can be determined more accurately.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
With the industrialization of the countries around the world, air pollution has increased over the recent decades, to such an extent that in some cases, it has threatened the life of human beings (Newby et al. 2015; Pourvakhshoori et al. 2020; Straif et al. 2013). The main factors influencing air pollution include the use of motor vehicles, industrial activities, mining activities, power plants, and the use of fossil fuels. Human beings are exposed to air pollutants at all kinds of places, including home, work, public areas, public transport vehicles, and open air. They can be introduced through breathing, foods, and skin contact, which may ultimately lead to various types of respiratory and cardiac morbidities and cancers (Bazyar et al. 2019; Bräuner et al. 2010; Weng et al. 2008). Investigation of the disease burden resulting from the air pollution in 2016 by the World Health Organization (WHO) showed that 4.2 million fatalities have been recorded due to global air pollution, 262,000 of which have been due to lung cancer (Ha et al. 2017).
Cancer is the second cause of increased disease burden and fatality in the world. Every year, there are many fatalities from cancer worldwide, such that, according to the WHO report from 185 countries, in 2018, 18.1 million new cases of cancer and 9.6 fatalities due to the disease occurred. Most of the cases were related to lung, breast, colorectal, prostate, and gastric cancers. Also, lung and breast cancers were the leading cause of mortality in men and women, respectively (Janitz et al. 2016). According to the World Health Organization (WHO), various factors have contributed to the increase in cancer incidence and its resulting mortality including population growth, population aging, development and industrialization of countries, and lifestyle changes (de Smith et al. 2017).
Although genetic and environmental factors play a role in the incidence of cancer, environmental factors play a more important role, such that some references have reported up to 80% of the influence of the environmental factors. The most important environmental factors affecting cancer include exposure to radiation, heavy metals, chemical compounds, contaminated water, infections, and air pollution (Straif et al. 2013). One of the factors that have been taken into consideration in recent years is the role of air pollution in the incidence of cancer. According to the International Agency for Research on Cancer (IARC), and other studies elsewhere (Fiebelkorn and Meredith 2018; Janitz et al. 2017; Raaschou-Nielsen et al. 2016; Straif et al. 2013), the role of air pollution and its compounds including benzene, polycyclic aromatic hydrocarbons (PHAS), asbestosis, radon, formaldehyde, sulfur dioxide, ozone, and carbon monoxide has been proved in the incidence of cancer (Parodi et al. 2015; Winters et al. 2015). According to Nielsen et al.’s review, exposure to air pollution has increased the incidence of cancer in childhood (Farioli et al. 2014). Some studies have also shown that exposure to air pollution increases the fatality resulting from cancer (Gao et al. 2014). Studies have suggested that exposure to air pollution results in oxidative damage to DNA and ultimately cellular damage and cancer (Badaloni et al. 2013). Also, in biological studies, carcinogens that are present in the air pollutants have been extracted from human body tissues. All these indicate the role of air pollution in the incidence of cancer (Bailey et al. 2011).
Worldwide, a large number of cancer cases are reported every year, most of which lead to mortality and morbidity. Air pollution is one of the environmental factors associated with cancers. It has been associated with lung, breast, and stomach cancers; however, there is not enough evidence for the association between air pollutants and some other cancers (Magnani et al. 2016; Mattioli et al. 2014). This systematic review aims at investigating the relationship between air pollution and some cancers not attributable to air pollution. This will help improve our understanding of the role of air pollution in the control of these cancers.
Methods
The present study was conducted as a systematic review of the relationship between air pollution and cancer in the world. In this study, all relevant English articles published from the beginning of 1950 to the end of 2018 were extracted from MEDLINE, EMBASE, Scopus, Web of Science, PubMed, Cochrane Library, Science Direct, and Google Scholar. The searching process was performed via the keywords of “cancer,” “neoplasm,” “malignancy,” “tumor,” “carcinoma,” and “air pollution,” either individually and in combination and using “and” or “or” operators.
By this method, all articles related to air pollution and cancers were gathered, and a list of the summary section of the articles was prepared. Then, the profile of the articles, such as the name of the author and journal, along with the articles full text, was given to two researchers trained in the literature review. Every article was independently analyzed by the two researchers. In case any of the articles were rejected, the researchers mentioned the reason for the rejection. If there was a disagreement on the rejected articles between the researchers, the article was judged by a third person. To evaluate the quality of the articles, the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) checklist was used (Boers et al. 2005). This checklist contained 22 items, and scoring was performed considering the significance of every item and the studied choices. In examining the quality of studies, the minimum acceptable score was 15 (Pedersen et al. 2017). The required data were extracted by a pre-authored checklist which included the location and time of the study, type of cancer, community, and air pollution.
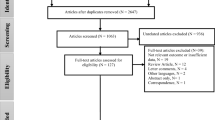
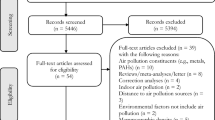
Finally, all English articles on air pollution, in which the word cancer was mentioned and had the required criteria, were included in the study. The exclusion criteria were poor quality studies, those that only discussed air pollution or cancer, interventional studies, case reports, or case series. The primary goal of this study was to ascertain the relationship between all types of cancers and air pollution. After a primary search, we found that there are many cancers with a clear association with air pollution, whereas, for some cancers, this associated has not been well investigated, so the association between air pollution and these cancers was further investigated by the research team in this study. A total of 4982 articles were found which were related to air pollution and cancer, of which 1810 were duplicates, 1551 were irrelevant, and 213 were indistinguishable, and thus were eliminated. After reviewing the abstract section of the articles, 796 of them were eliminated because as they did not include the required information. After reviewing the full text of the articles, 42 of them were eliminated because as they did not include the required information. Finally, 91 articles had the inclusion criteria and were included in the study. Our search yielded 43 articles which contained information related to cancers with a strong association with air pollution, such as lung, breast, and stomach cancers, and 48 articles related to cancers with less evidence of air pollution association. Studies containing information on cancers with an established strong association with air pollution (43 articles) were excluded from the study, and the remaining 48 articles were further investigated for a possible association (Fig. 1).
Results
Air pollution and leukemia
Leukemia is one of the most common cancers in childhood and adultness, with 200,000 to 400,000 new cases every year worldwide. The 5-year survival rate of leukemia is low and causes fatality in many patients every year (Bray et al. 2018). The cause of leukemia is currently unknown, although some sources have mentioned genetic and transgenic mutations due to environmental factors (Gao et al. 2014; Lien et al. 2016). Many studies have been conducted in recent years on the role of air pollution and its constituents, including benzene, formaldehyde, and PHA in the incidence of cancer in children and adults. They have found that exposure to air pollution causes leukemia in children and adults (Table 1).
Air pollution and prostate cancer
Prostate cancer is one of the most popular cancers in men afflicting an estimated 60 to 112 cases out of 100,000 men. It causes an annual 310,000 deaths in the world (6). Various factors including family history, smoking, race, diet, physical activity, sexual activity, prostate inflammation, and obesity are related to prostate cancer. Air pollution is one of the factors that has been studied about prostate cancer in recent years (Garcia-Perez et al. 2016) (Table 2).
Air pollution and liver cancer
Liver cancer is the fifth most popular cancer in men and the ninth most popular cancer in women, which causes an annual 746,000 deaths in the world (Pedersen et al. 2017). Hepatocellular carcinoma, alcohol consumption, smoking, and hepatitis B and C are the main causes of liver cancer. Smoke and air pollution include complex compounds such as polycyclic aromatic hydrocarbons, nickel, heterocyclic hydrocarbons, and cadmium that which carcinogenic to humans (Altekruse et al. 2009). Liver cancer is another type of cancer supposed to be affected by air pollution. Few studies have been performed on this subject (Table 2).
Air pollution and bladder cancer
Bladder cancer is the ninth most popular cancer in the world. Smoking, exposure to aniline dyes, employment in rubber and battery industries, and driving vehicles such as busses and trucks are the risk factors associated with bladder cancer (Bray et al. 2018). Exposure to air pollution caused by vehicle exhaust, and combinations such as polycyclic aromatic hydrocarbons and volatile organic compounds, can cause bladder cancer (Cumberbatch et al. 2016) (Table 2).
Air pollution and colorectal cancer
Colorectal cancer is one of the most popular types of cancers among men and women worldwide, with about 1,400,000 new cases per year. Various factors such as obesity, sedentary lifestyle, red meat consumption, and smoking are associated with colorectal cancer (Bray et al. 2018). Air pollution is one of the factors associated with colorectal cancer and has been considered in recent years (Table 3).
Air pollution and mouth cancer
Mouth cancer is one of the most common types of cancer in the world and affects many people per year. This cancer has only a 5-year survival rate and causes a large number of fatalities. Smoking, alcohol, and exposure to tobacco smoke are related to mouth cancer. There have been few studies on exposure to air pollution and mouth cancer worldwide (Table 3).
Air pollution and brain cancer
Brain cancer has increased in recent years due to industrialization such that its incidence rate in Europe (2012) has risen to 6.6/100.000. Various factors such as ionizing radiation, aging, being Caucasoid, exposure to infectious agents, working in petrochemical and agricultural industries, and exposure to compounds in the polluted air are related to the incidence of this cancer. Some studies have examined the relationship between air pollution and brain cancer (Table 4).
Air pollution and cervical cancer
Cervical cancer is the fourth most popular cancer in women with 528,000 new cases per year and 266,000 fatalities. Infection with human papillomavirus, multiple sexual partners, and sexual activity at a young age and multiple pregnancies are risk factors related to cervical cancer (Makuza et al. 2015). Air pollution is one of the other factors which can be related to cervical cancer. This has been investigated in a few studies (Table 4).
After reviewing the articles, the relationship between different pollutants and types of cancers was also examined, as shown in Table 5.
Discussion
Today, cancer claims the second rank among the morbidities in the world, which annually causes millions of fatalities (Bailey et al. 2011). Several risk factors are involved in cancer. One of these risk factors, which has recently been considered by global communities, is the carcinogenic role of air pollution and its compounds, which has been widely studied around the globe (Jerrett et al. 2017). This study reviewed the role of air pollution in the incidence of, blood, prostate, bladder, liver, colorectal, oral, brain, and cervical cancers. The International Agency for Research on Cancer (IARC) has classified outdoor air pollution as a cancer-causing agent (a carcinogen). The IARC is part of the World Health Organization and is one of the primary sources for information on cancer-causing substances for the American Cancer Society and other organizations. In its evaluation, the IARC concluded that outdoor air pollution causes lung cancer and is also linked to an increased risk for bladder cancer (Simon 2013). “The air we breathe is filled with cancer-causing substances,” said Kurt Straif, Ph.D., head of the IARC Monographs Section. “Outdoor air pollution is not only a major environmental risk to health in general; it is the most important environmental cancer killer due to the large number of people exposed.” The IARC based its report on a review of more than 1000 scientific papers from studies on 5 continents. The studies analyzed the cancer risk caused by various pollutants present in outdoor air pollution, especially particulate matter and transportation-related pollution. The findings came from large epidemiologic studies that included millions of people living in Europe, North and South America, and Asia. “Classifying outdoor air pollution as carcinogenic to humans is an important step,” said IARC Director Christopher Wild, PhD. “Given the scale of the exposure, it sends a strong signal that it is vital to implement efficient policies to reduce exposure to pollution worldwide”(Simon 2013). The findings from studies on the relationship between prostate, liver, bladder, colorectal, oral, blood, brain, and cervical cancers, and the air pollution were inconsistent, where there was a significant relationship between air pollution and these cancers, but this relationship was not significant in some cases. Scheurer et al. (2014) in Texas reported that exposure to benzene from air pollution causes uterine dysplasia (Scheurer et al. 2014). Mahalingaiah et al. (2014) studied the relationship between air pollution and the risk of Uterine Leiomyomata. They concluded chronic exposure to PM2.5 may be associated with a modestly increased risk of uterine leiomyomata (Mahalingaiah et al. 2014). In a study by Zheng et al. (2013), exposure to PM2.5 could incur biological damages to liver tissue and lead to liver cancer (Zheng et al. 2013). Deng et al. (2017) in their study found adverse effects of pm 2.5 exposure after diagnosis on liver cancer survival. Not only were such effects more profoundly for those diagnosed with early stage, but they also increased strongly with concentration, suggesting that reductions in high pm 2.5 exposure could increase survival for a no respiratory system cancer (Deng et al. 2017). The hypothesis-generating study of Raaschou-Nielsen et al. (2011) indicates that traffic-related air pollution might increase the risks for cervical and brain cancer. Their results also showed a weak, insignificant association between traffic-related air pollution and bladder cancer. Their results showed no significant relationship between the type of occupation and alcohol consumption as well as smoking and liver cancer (OR: 2.14, 95% CI: 0.96–4.75)(Raaschou-Nielsen et al. 2011). The evidence of an association between ambient air pollution and bladder cancer in the general population is not conclusive (Castaño-Vinyals et al. 2008; Liu et al. 2009; Visser et al. 2004). In the study of Visser et al. (2004) in the Netherlands, there was no significant correlation between exposure to air pollution, NOx, traffic density and PAHs, and bladder cancer (Visser et al. 2004). Also, in the study of Fu et al. (2013), exposure to cigarette smoke increased the incidence of colorectal polyps (Fu et al. 2013). In a meta-analysis by Carlos-Wallace et al. (2016), exposure to benzene from air pollution increased the incidence of leukemia in children (Carlos-Wallace et al. 2016). There was an inverse correlation between the amount of benzene in the blood and the number of red blood cells in the study of Koh et al. (2015), where the elevation of the amount of benzene reduced the number of blood cells (Koh et al. 2015). The results of some studies show inconsistencies; for instance, the results from a large prospective study suggest that ambient air pollution was not associated with death from most non-lung cancers, but associations with kidney, bladder, and colorectal cancer death warrant further investigation (Turner et al. 2017).
Conclusions
In general, the lack of evidence of the link between air pollution and these cancers is not due to their low importance because the incidence of cancers is increasing. The lack of studies investigating this relationship can be attributed to the multifactorial nature of these cancers. The majority of studies are likely to address the role of the main cancer risk factors than air pollution, which may be one of the silent risks and/or exacerbating factors of these cancers. Therefore, it is recommended that multifactorial studies measure the different risk factors in the form of regression, and model them to see how much pollution contributes to the epidemiology of these cancers. According to the results of this and other studies on the relationship between air pollution and lung, gastric, and breast cancers, it was observed that exposure to air pollution has an impact on these cancers, but in terms of prostate, bladder, brain, cervical, and liver cancers, the results are contradictory and the role of the air pollution in these types of cancer cannot be determined accurately. Accordingly, it is recommended that studies are performed at the individual level by controlling the confounding factors to more accurately determine the role of air pollution in the incidence of these types of cancer.
However, it is recommended that groups that have direct long-term exposure to air pollution, such as police officers, take measures to reduce their exposure, and have more care than their health. It may be useful for policymakers to implement appropriate strategies toward the reduction of these risks. According to the results, it cannot be stated that exposure to air pollutants increases the incidence of prostate, liver, bladder, colorectal, oral, blood, brain, and cervical cancers. Regarding the relationship between exposure to air pollution and the incidence of these types of cancer, although some studies showed a significant statistical relationship since the source of air pollution is different which may be due to fossil fuels, motor vehicles, mining activities, industries, dust, and smoke, various carcinogens from these sources are brought to the air, each of which has a different effect on the tissues of the body. Other factors such as age, sex, and lifestyle are also related to cancer, so it is recommended that studies are performed at the individual level by controlling the confounding factors and identifying air pollutant carcinogens to accurately determine the role of air pollution in the development of cancer.
Limitations
Only English language articles included.
References
Altekruse SF, McGlynn KA, Reichman ME (2009) Hepatocellular carcinoma incidence, mortality, and survival trends in the United States from 1975 to 2005. J Clin Oncol Off J Am Soc Clin Oncol 27:1485–1491
Andersen ZJ, Pedersen M, Weinmayr G, Stafoggia M, Galassi C, Jorgensen JT et al (2018) Long-term exposure to ambient air pollution and incidence of brain tumor: the European study of cohorts for air pollution effects (escape). Neuro-oncology 20:420–432
Badaloni C, Ranucci A, Cesaroni G, Zanini G, Vienneau D, Al-Aidrous F et al (2013) Air pollution and childhood leukaemia: a nationwide case-control study in Italy. Occup Environ Med 70:876–883
Bailey HD, de Klerk NH, Fritschi L, Attia J, Daubenton JD, Armstrong BK, Milne E, for the Aus-ALL Consortium (2011) Refueling of vehicles, the use of wood burners, and the risk of acute lymphoblastic leukaemia in childhood. Paediatr Perinat Epidemiol 25:528–539
Bazyar J, Pourvakhshoori N, Khankeh H, Farrokhi M, Delshad V, Rajabi E (2019) A comprehensive evaluation of the association between ambient air pollution and adverse health outcomes of major organ systems: a systematic review with a worldwide approach. Environ Sci Pollut Res Int 26:12648–12661
Boers D, Zeegers MP, Swaen GM, Kant I, van den Brandt PA (2005) The influence of occupational exposure to pesticides, polycyclic aromatic hydrocarbons, diesel exhaust, metal dust, metal fumes, and mineral oil on prostate cancer: a prospective cohort study. Occup Environ Med 62:531–537
Bräuner EV, Andersen CE, Andersen HP, Gravesen P, Lind M, Ulbak K, Hertel O, Schüz J, Raaschou-Nielsen O (2010) Is there any interaction between domestic radon exposure and air pollution from traffic in relation to childhood leukemia risk? Cancer Causes Control 21:1961–1964
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Carlos-Wallace FM, Zhang L, Smith MT, Rader G, Steinmaus C (2016) Parental, in utero, and early-life exposure to benzene and the risk of childhood leukemia: a meta-analysis. Am J Epidemiol 183:1–14
Castano-Vinyals G, Cantor KP, Malats N, Tardon A, Garcia-Closas R, Serra C, Carrato A, Rothman N, Vermeulen R, Silverman D, Dosemeci M, Kogevinas M (2008) Air pollution and risk of urinary bladder cancer in a case-control study in Spain. Occup Environ Med 65:56–60
Cicalese L, Curcuru G, Montalbano M, Shirafkan A, Georgiadis J, Rastellini C (2017) Hazardous air pollutants and primary liver cancer in Texas. PLoS One 12:e0185610
Cumberbatch MG, Rota M, Catto JW, La Vecchia C. 2016. The role of tobacco smoke in bladder and kidney carcinogenesis: a comparison of exposures and meta-analysis of incidence and mortality risks. Eur Urol 70:458–466
de Smith AJ, Kaur M, Gonseth S, Endicott A, Selvin S, Zhang L, Roy R, Shao X, Hansen HM, Kang AY, Walsh KM, Dahl GV, McKean-Cowdin R, Metayer C, Wiemels JL (2017) Correlates of prenatal and early-life tobacco smoke exposure and frequency of common gene deletions in childhood acute lymphoblastic leukemia. Cancer Res 77:1674–1683
De Verdier MG, Plato N, Steineck G, Peters JM (1992) Occupational exposures and cancer of the colon and rectum. Am J Ind Med 22:291–303
Deng H, Eckel SP, Liu L, Lurmann FW, Cockburn MG, Gilliland FD (2017) Particulate matter air pollution and liver cancer survival. Int J Cancer 141:744–749
Eitan O, Yuval BM, Dubnov J, Linn S, Carmel Y et al (2010) Spatial analysis of air pollution and cancer incidence rates in Haifa bay, Israel. Sci Total Environ 408:4429–4439
Fang R, Le N, Band P (2011) Identification of occupational cancer risks in British Columbia, Canada: a population-based case-control study of 1,155 cases of colon cancer. Int J Environ Res Public Health 8:3821–3843
Farioli A, Legittimo P, Mattioli S, Miligi L, Benvenuti A, Ranucci A, Salvan A, Rondelli R, Conter V, Magnani C (2014) Tobacco smoke and risk of childhood acute lymphoblastic leukemia: findings from the SETIL case-control study. Cancer Causes Control 25:683–692
Fiebelkorn S, Meredith C (2018) Estimation of the leukemia risk in human populations exposed to benzene from tobacco smoke using epidemiological data. Risk Anal 38:1490–1501
Fu Z, Shrubsole MJ, Li G, Smalley WE, Hein DW, Cai Q, Ness RM, Zheng W (2013) Interaction of cigarette smoking and carcinogen-metabolizing polymorphisms in the risk of colorectal polyps. Carcinogenesis 34:779–786
Gao Y, Zhang Y, Kamijima M, Sakai K, Khalequzzaman M, Nakajima T et al (2014) Quantitative assessments of indoor air pollution and the risk of childhood acute leukemia in shanghai. Environ Pollut (Barking, Essex : 1987) 187:81–89
Garcia-Perez J, Perez-Abad N, Lope V, Castello A, Pollan M, Gonzalez-Sanchez M et al (2016) Breast and prostate cancer mortality and industrial pollution. Environ Pollut (Barking, Essex : 1987) 214:394–399
Goldberg MS, Parent ME, Siemiatycki J, Desy M, Nadon L, Richardson L, et al. 2001. A case-control study of the relationship between the risk of colon cancer in men and exposures to occupational agents. Am J Ind Med 39:531–546
Ha M, Hwang SS, Kang S, Park NW, Chang BU, Kim Y (2017) Geographical correlations between indoor radon concentration and risks of lung cancer, non-Hodgkin’s lymphoma, and leukemia during 1999–2008 in Korea. Int J Environ Res Public Health 14
He B, Chen F, Yan L, Huang J, Liu F, Qiu Y, Lin L, Zhang Z, Cai L (2016) Independent and joint exposure to passive smoking and cooking oil fumes on oral cancer in Chinese women: a hospital-based case-control study. Acta Otolaryngol 136:1074–1078
Ho CK, Peng CY, Yang CY (2010) Traffic air pollution and risk of death from bladder cancer in Taiwan using petrol station density as a pollutant indicator. J Toxicol Environ Health A 73:23–32
Janitz AE, Campbell JE, Magzamen S, Pate A, Stoner JA, Peck JD (2016) Traffic-related air pollution and childhood acute leukemia in Oklahoma. Environ Res 148:102–111
Janitz AE, Campbell JE, Magzamen S, Pate A, Stoner JA, Peck JD (2017) Benzene and childhood acute leukemia in Oklahoma. Environ Res 158:167–173
Jerrett M, Turner MC, Beckerman BS, Pope CA, van Donkelaar A, Martin RV et al (2017) Comparing the health effects of ambient particulate matter estimated using ground-based versus remote sensing exposure estimates. Environ Health Perspect 125:552–559
Kachuri L, Villeneuve PJ, Parent ME, Johnson KC, Harris SA (2016) Workplace exposure to diesel and gasoline engine exhausts and the risk of colorectal cancer in Canadian men. Environ Health 15:4
Koh DH, Jeon HK, Lee SG, Ryu HW (2015) The relationship between low-level benzene exposure and blood cell counts in Korean workers. Occup Environ Med 72:421–427
Lien S-YA, Young L, Gau B-S, Shiao SPK (2016) Meta-prediction of mthfr gene polymorphism-mutations, air pollution, and risks of leukemia among world populations. Oncotarget 8:4387–4398
Liu C-C, Tsai S-S, Chiu H-F, Wu T-N, Chen C-C, Yang C-Y (2009) Ambient exposure to criteria air pollutants and risk of death from bladder cancer in Taiwan. Inhal Toxicol 21:48–54
Magnani C, Ranucci A, Badaloni C, Cesaroni G, Ferrante D, Miligi L, Mattioli S, Rondelli R, Bisanti L, Zambon P, Cannizzaro S, Michelozzi P, Cocco P, Celentano E, Assennato G, Merlo DF, Mosciatti P, Minelli L, Cuttini M, Torregrossa MV, Lagorio S, Haupt R, Forastiere F, Magnani C, Mattioli S, Farioli A, Miligi L, Ranucci A, Ferrante D, Rondelli R, Salvan A, Masera G, Rizzari C, Bisanti L, Zambon P, Greco Veneto A, Cannizzaro S, Gafà L, Luzzatto LL, Benvenuti A, Michelozzi P, Kirchmayer U, Cocco P, Galassi C, Celentano E, Guarino E, Assennato G, de Nichilo G, Merlo DF, Bocchini V, Mosciatti P, Minelli L, Chiavarini M, Cuttini M, Casotto V, Torregrossa MV, Valenti RM, Forastiere F, Haupt R, Lagorio S, Risica S, Polichetti A, Bochicchio F, Nuccetelli C, Biddau P, Aricò M, DeSalvo GL, Locatelli F, Pession A, Varotto S, Poggi V, Massaglia P, Monetti D, Targhetta R, Bernini G, Pannelli F, Sampietro G, Schilirò G, Pulsoni A, Parodi S (2016) Road traffic pollution and childhood leukemia: a nationwide case-control study in Italy. Arch Med Res 47:694–705
Mahalingaiah S, Hart JE, Laden F, Terry KL, Boynton-Jarrett R, Aschengrau A, Missmer SA (2014) Air pollution and risk of uterine leiomyomata. Epidemiology 25:682–688
Mahalingaiah S, Hart JE, Laden F, Farland LV, Hewlett MM, Chavarro J et al (2016) Adult air pollution exposure and risk of infertility in the nurses’ health study ii. Hum Reprod (Oxford, England) 31:638–647
Makuza JD, Nsanzimana S, Muhimpundu MA, Pace LE, Ntaganira J, Riedel DJ (2015) Prevalence and risk factors for cervical cancer and pre-cancerous lesions in Rwanda. Pan Afr Med J 22:26
Mattioli S, Farioli A, Legittimo P, Miligi L, Benvenuti A, Ranucci A, Salvan A, Rondelli R, Magnani C, on behalf of the SETIL Study Group (2014) Tobacco smoke and risk of childhood acute non-lymphocytic leukemia: findings from the SETIL study. PLoS One 9:e111028
McKean-Cowdin R, Calle EE, Peters JM, Henley J, Hannan L, Thurston GD, Thun MJ, Preston-Martin S (2009) Ambient air pollution and brain cancer mortality. Cancer Causes Control 20:1645–1651
Newby DE, Mannucci PM, Tell GS, Baccarelli AA, Brook RD, Donaldson K et al (2015) Expert position paper on air pollution and cardiovascular disease. Eur Heart J 36:83–93b
Parent ME, Goldberg MS, Crouse DL, Ross NA, Chen H, Valois MF, Liautaud A (2013) Traffic-related air pollution and prostate cancer risk: a case-control study in Montreal, Canada. Occup Environ Med 70:511–518
Parodi S, Santi I, Casella C, Puppo A, Montanaro F, Fontana V, Pescetto M, Stagnaro E (2015) Risk of leukaemia and residential exposure to air pollution in an industrial area in northern Italy: a case-control study. Int J Environ Health Res 25:393–404
Pedersen M, Andersen ZJ, Stafoggia M, Weinmayr G, Galassi C, Sorensen M et al (2017) Ambient air pollution and primary liver cancer incidence in four European cohorts within the escape project. Environ Res 154:226–233
Pedersen M, Stafoggia M, Weinmayr G, Andersen ZJ, Galassi C, Sommar J, Forsberg B, Olsson D, Oftedal B, Krog NH, Aamodt G, Pyko A, Pershagen G, Korek M, de Faire U, Pedersen NL, Östenson CG, Fratiglioni L, Sørensen M, Eriksen KT, Tjønneland A, Peeters PH, Bueno-de-Mesquita B, Vermeulen R, Eeftens M, Plusquin M, Key TJ, Jaensch A, Nagel G, Concin H, Wang M, Tsai MY, Grioni S, Marcon A, Krogh V, Ricceri F, Sacerdote C, Ranzi A, Cesaroni G, Forastiere F, Tamayo I, Amiano P, Dorronsoro M, Stayner LT, Kogevinas M, Nieuwenhuijsen MJ, Sokhi R, de Hoogh K, Beelen R, Vineis P, Brunekreef B, Hoek G, Raaschou-Nielsen O 2018. Is there an association between ambient air pollution and bladder cancer incidence? Analysis of 15 European cohorts. Eur Urol Focus 4:113–120
Poulsen AH, Sorensen M, Andersen ZJ, Ketzel M, Raaschou-Nielsen O. 2016. Air pollution from traffic and risk for brain tumors: a nationwide study in Denmark. Cancer Causes Control 27:473–480
Pourvakhshoori N, Poursadeghiyan M, Khankeh HR, Harouni GG, Farrokhi M (2020) The simultaneous effects of thermal stress and air pollution on the body temperature of Tehran traffic officers. J Environ Health Sci Eng
Raaschou-Nielsen O, Andersen ZJ, Hvidberg M, Jensen SS, Ketzel M, Sorensen M et al (2011) Air pollution from traffic and cancer incidence: a Danish cohort study. Environ Health 10:67
Raaschou-Nielsen O, Ketzel M, Harbo Poulsen A, Sorensen M (2016) Traffic-related air pollution and risk for leukaemia of an adult population. Int J Cancer 138:1111–1117
Scheurer ME, Danysh HE, Follen M, Lupo PJ (2014) Association of traffic-related hazardous air pollutants and cervical dysplasia in an urban multiethnic population: a cross-sectional study. Environ Health 13:52
Siemiatycki J, Gerin M, Stewart P, Nadon L, Dewar R, Richardson L. 1988. Associations between several sites of cancer and ten types of exhaust and combustion products. Results from a case-referent study in Montreal. Scand J Work Environ Health 14:79–90
Silverman D, Dosemeci M, Castaño-Vinyals G, Kogevinas M, Cantor KP, Malats N, Tardón A, Real FX, Garcia-Closas R, Serra C, Carrato A, Rothman N (2004) Air pollution and bladder cancer risk in Spain. Epidemiology 15:S80
Simon S (2013) World health organization: outdoor air pollution causes cancer. In: The American Cancer Society medical and editorial content team
Straif K, Cohen A, Samet J (2013) Air pollution and cancer. International Agency for Research on Cancer 150
Tsai SS, Tiao MM, Kuo HW, Wu TN, Yang CY (2009) Association of bladder cancer with residential exposure to petrochemical air pollutant emissions in Taiwan. J Toxicol Environ Health A 72:53–59
Turner MC, Krewski D, Diver WR, Pope CA, Burnett RT, Jerrett M et al (2017) Ambient air pollution and cancer mortality in the cancer prevention study ii. Environ Health Perspect 125:087013
Visser O, van Wijnen JH, van Leeuwen FE (2004) Residential traffic density and cancer incidence in Amsterdam, 1989-1997. Cancer Causes Control 15:331–339
Weng H-H, Tsai S-S, Chiu H-F, Wu T-N, Yang C-Y (2008) Childhood leukemia and traffic air pollution in Taiwan: petrol station density as an indicator. J Toxic Environ Health A 72:83–87
Winkelstein W Jr, Kantor S (1969) Prostatic cancer: relationship to suspended particulate air pollution. Am J Public Health Nation's Health 59:1134–1138
Winters N, Goldberg MS, Hystad P, Villeneuve PJ, Johnson KC (2015) Exposure to ambient air pollution in Canada and the risk of adult leukemia. Sci Total Environ 526:153–176
Zheng Z, Xu X, Zhang X, Wang A, Zhang C, Huttemann M et al (2013) Exposure to ambient particulate matter induces a NASH-like phenotype and impairs hepatic glucose metabolism in an animal model. J Hepatol 58:148–154
Funding
This article is funded by the “Iran National Science Foundation” and the “The University of Social Welfare and Rehabilitation Sciences.”
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Responsible editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pourvakhshoori, N., Khankeh, H.R., Stueck, M. et al. The association between air pollution and cancers: controversial evidence of a systematic review. Environ Sci Pollut Res 27, 38491–38500 (2020). https://doi.org/10.1007/s11356-020-10377-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-020-10377-z