Abstract
Organophosphorus insecticides toxicity is still considered a major global health problem. Malathion is one of the most commonly used organophosphates nowadays, as being considered to possess relatively low toxicity compared with other organophosphates. However, widespread use may lead to excessive exposure from multiple sources. Mechanisms of MAL toxicity include inhibition of acetylcholinesterase enzyme, change of oxidants/antioxidants balance, DNA damage, and facilitation of apoptotic cell damage. Exposure to malathion has been associated with different toxicities that nearly affect every single organ in our bodies, with CNS toxicity being the most well documented. Malathion toxic effects on liver, kidney, testis, ovaries, lung, pancreas, and blood were also reported. Moreover, malathion was considered as a genotoxic and carcinogenic chemical compound. Evidence exists for adverse effects associated with prenatal and postnatal exposure in both animals and humans. This review summarizes the toxic data available about malathion in mammals and discusses new potential therapeutic modalities, with the aim to highlight the importance of increasing awareness about its potential risk and reevaluation of the allowed daily exposure level.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In the past decades, the pesticides were utilized to enhance agricultural productivity and minimize losses by controlling unwanted insects, worms, and animals, in addition to eradicating disease vectors in different parts of the world (Bhardwaj and Saraf 2014). However, they are not totally beneficial; they are important sources of environmental pollution and exert adverse health consequences, some of which are irreversible (LaVerda et al. 2015; Navarrete-Meneses et al. 2017). Pesticides induce both acute and chronic toxic effects including neurological manifestations, respiratory diseases, genetic damage, and reproductive disorders in various organisms (Bhardwaj and Saraf 2014; Bhardwaj et al. 2018). Pesticide poisoning is being considered as an important cause of morbidity and mortality, especially in developing countries. Nevertheless, every year there are three million cases of acute poisoning and 220,000 deaths; the majority of these poisoning and 49% of the resulting death occur in third world countries (Seth et al. 2001).
Organophosphate synthetic pesticides (OPs) are being widely used since the mid-1940s for controlling pest (Ozsoy et al. 2016; Esen and Uysal 2018). They are highly toxic to humans and are considered potential hazards to human health (El-Bini Dhouib et al. 2015). Epidemiological studies investigated the relationship between a high level of OP exposure and adverse health effects (Navarrete-Meneses et al. 2017). They act by inhibiting acetylcholinesterase (AChE), an enzyme hydrolyzing acetylcholine in cholinergic synapses and neuromuscular junctions, by phosphorylating it. They are thus called AChE inhibitors (El-Bini Dhouib et al. 2015). Inhibition of AChE causes accumulation of acetylcholine, with subsequent increased activity of cholinergic muscarinic, in addition to nicotinic receptors (Velmurugan et al. 2017; Esen and Uysal 2018). Despite anticholinergic treatment and sophisticated intensive care facilities, severe OP poisoning has a high mortality rate (~ 25–40%) (Kang et al. 2009). Therefore, a better understanding of the pathophysiology caused by OPs and the development of new treatment modalities are of great importance in OP toxicity (Esen and Uysal 2018; Vanova et al. 2018).
Malathion
Malathion (MAL) (S-(1,2-dicarbethoxyethyl) O,O-dimethyl dithiophosphate) (Fig. 1), is being used, since 1980, in agriculture, industry, and veterinary medicine. As MAL is considered to have relatively lower acute toxicity as compared with other OPs, it is now one of the most extensively used pesticides (Ozsoy et al. 2016; Bogen and Singhal 2017). Even though commonly named as a pesticide, it is still used therapeutically for pediculosis (Varol et al. 2015). This widespread use leads to environmental pollution and increases the extent of exposure, and almost any individual may be exposed to MAL through different routes (dos Santos et al. 2016; Navarrete-Meneses et al. 2017). Moreover, traces of MAL have been detected in the blood, urine, and hair of pregnant women (Bossi et al. 2013; Navarrete-Meneses et al. 2017). Thus, OPs, including MAL, remain a serious health hazard.
Chemical structure of malathion (Naughton and Terry 2018)
MAL exposure may cause subacute, acute, or chronic toxicity, and both incidental and intentional MAL toxicity were recorded especially in developing countries (Varol et al. 2015). Occupational and nonoccupational exposures to MAL have been reported in adults and children (Eskenazi et al. 2007; Salvatore et al. 2008; Fenske et al. 2013; Voorhees et al. 2016; Smith et al. 2017). Workers of MAL manufactories, people who work in agriculture and their families, those living near farms, and those performing the home application of pesticides or eating food highly contaminated with pesticides are highly susceptible to MAL intoxication (Jaga and Dharmani 2003; Waheed et al. 2017). MAL toxicity is mainly caused by its metabolites and is affected by different variables including product purity (as contaminants may aggravate MAL toxicity), route of exposure, nutritional status, genetics, and gender (Moore et al. 2011).
Malathion pharmacokinetics and pharmacodynamics
MAL may represent a greater risk than it would be expected. The toxicity of malathion is highly correlated with its metabolites and affected by MAL contaminants (Baiomy et al. 2015). Therefore, with the aim to understand MAL toxicity, we first have to understand the pharmacokinetics of MAL, as well as its pharmacodynamics.
Pharmacokinetics of malathion
Mammals can be adversely affected by MAL through nearly any route of exposure, including the oral ingestion of food and drinking water contaminated with MAL (Sapbamrer and Hongsibsong 2014; Akbel et al. 2018), dermal absorption (Geng et al. 2015b), conjunctival (Kamanyire and Karalliedde 2004), and respiratory exposure through occupational or nonoccupational during contact with contaminated soil and plants, working at pesticides factories, handling and applying of MAL, or from accidental spills (Machera et al. 2003; Ozsoy et al. 2016). Acute MAL toxicity occurs mostly orally (Esen and Uysal 2018); however, the major route of occupational exposure is the dermal one (Tchounwou et al. 2015).
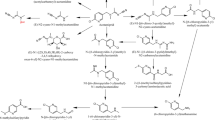
Generally, OPs are relatively rapidly absorbed, metabolized, and excreted in the form of more hydrophilic metabolites in both animals and humans (Chambers and Levi 2013). Similarly, due to its lipophilic nature, MAL is rapidly absorbed, through different routes, and distributed to different body organs, thus leads to several pathologies (Selmi et al. 2018). Like other OPs, MAL requires cytochrome P-450-mediated metabolic activation for cholinergic toxicity (Abdollahi et al. 2004). It is metabolized through desulfuration to an active metabolite, malaoxon, that strongly inhibits AChE (Guyton et al. 2015) (Fig. 2). At low MAL concentration, malaoxon formation is catalyzed by CYP1A2 and 2B6 (to a lesser extent); however, 3A4 plays a relevant role only at high MAL concentrations (Buratti et al. 2005). The metabolites, produced by MAL oxidation, are considered the primary source of its toxicity and malaoxon is found to be 40 times more toxic than MAL (Baiomy et al. 2015).
Major pathways of MAL metabolism. Figure modified from that of Buratti and Testai (2005). DMPT dimethyltiophosphate, MMA malathion (malaoxon)-monocarboxylic acid, MDA malathion (malaoxon)-dicaroxylic acid
On the other hand, MAL and malaoxon can be rapidly and effectively detoxified by carboxylesterases to form monocarboxylic acid (MMA), which also competes with malaoxon for the cytochrome P-450s (Fig. 2) (Buratti and Testai 2005; Chen et al. 2013). Carboxylesterases are widely distributed in mammalian tissue, with the highest levels exist in the liver, the gastrointestinal tract, and the brain (Brodeur and DuBois 1967; Buratti and Testai 2005). However, some contaminants of commercial MAL formulations are potent inhibitors of carboxylesterase, thus shifting the balance toward a significant increase in malaoxon formation; this may explain the role of contaminants in aggravating MAL toxicity (Buratti et al. 2005). In 1976, an epidemic of MAL poisonings occurred in Pakistan, emphasizing the role of impurities in the commercial formulations. Actually, at a level of exposure, which should not produce adverse effects on humans, about 2800 workers (spraymen and mixer operators) suffered from variable degrees of toxicity and five died (Hosokawa et al. 1990). The unexplained toxicity was related to isomalathion contaminant that inhibits carboxylesterases, with subsequently increased malaoxon formation (Hosokawa et al. 1995; Josse et al. 2014).
Regarding excretion, MAL and its metabolites have relatively low accumulation potential and are excreted primarily by the kidney, followed by the lung and the intestinal route (Waldron Lechner and Abdel-Rahman 1986; Tchounwou et al. 2015). The metabolites excreted in the urine can be convenient biomarkers of occupational exposure since they represent an internal or absorbed dose and they require only few measurements to reliably estimate workers’ exposure (Ross et al. 2008). MAL is also excreted in breast milk and can inhibit AChE of the offspring and thus was associated with various psychological and biological outcomes in exposed offspring (da Silva et al. 2006).
Pharmacodynamics of malathion
Acute, subchronic and chronic toxicity reports concluded that MAL is toxic to mammals (Wang et al. 2014; Ozsoy et al. 2016). It has toxic effects on experimental animals and exposed workers. MAL exposure was correlated with the dysfunction of several organs, including the liver, kidney, pancreas, testis, and brain (Ozsoy et al. 2016; Esen and Uysal 2018). MAL can also lead to metabolic disorders (Esen and Uysal 2018). Toxic mechanisms include inhibition of AChE, oxidative stress, induction of inflammatory response, promotion of apoptosis, genotoxicity, and immunomodulation (Nicholas et al. 1979; Geng et al. 2015b; Guyton et al. 2015; Ince et al. 2017). Toxicity depends on many factors including the level and duration of exposure, the route of exposure, age, and health status (Rosas and Eskenazi 2008; Sánchez-Santed et al. 2016).
The main mechanism of MAL toxic effects is the inhibition of AChE (Esen and Uysal 2018), with subsequent accumulation of acetylcholine, leading to excessive stimulation of both muscarinic and nicotinic receptors in the muscles and nerves of either the central, peripheral, or autonomic nervous system, evoking a wide array of cholinergic toxic manifestations (Mileson et al. 1998; Sapbamrer and Hongsibsong 2019). Acute toxicity signs and symptoms may include salivation, lacrimation, urination, and defecation (the SLUD syndrome), dyspnea, vomiting, bradycardia, abdominal pain, pinpoint pupil, and anorexia, which are caused by acetylcholine over excitation of the muscarinic receptors. Other signs of toxicity include muscle weakness, tremors, and rigidity, convulsions, and paralysis are induced as a result of acetylcholine excessive stimulation of nicotinic receptors. Finally, respiratory depression may take place, which characterizes the “cholinergic syndrome” (Kwong 2002; Takahashi and Hashizume 2014).
AChE inhibition alone cannot explain the wide range of toxic effects that were correlated with MAL exposure. Recently, oxidative stress has been proposed as the key player in accounting for both acute and chronic MAL toxic effects. Due to its lipophilic nature, MAL directly interacts with the phospholipid bilayer of cellular membranes, which causes disturbances in their structure and induces the production of free radicals (Ozsoy et al. 2016). This was experimentally studied by Rieger et al., who used pralidoxime, an AChE reactivator, to protect against cytotoxic effects of MAL in rat cortical cells. They found that pralidoxime significantly protected against MAL-induced AChE blockade; however, pralidoxime did not affect MAL-induced decrease in cellular viability, indicating that other mechanisms contribute to MAL toxic effects. They also found that MAL-induced cell death was directly linked to the increase in superoxide anion production and that antioxidant substance like ascorbic acid significantly counteracted the decrease of cell viability with no effect on AChE activity. This provides evidence of the role of oxidative stress in MAL-induced toxicity (Rieger et al. 2017).
Many other in vivo and in vitro studies in animals supported the oxidative stress theory (Moridi et al. 2018; Arab et al. 2018); MAL-induced oxidative stress was also recently observed in many types of human cells (Durak et al. 2009; Tuzcu et al. 2014; Yan et al. 2019; Shieh et al. 2019). They found that MAL treatment leads to enhanced production of reactive oxygen species (ROS) and subsequent lipid peroxidation (Durak et al. 2009; Bhardwaj et al. 2018). It is evident that lipid peroxidation is accompanied by an alteration, either inhibition or activation, of the antioxidant defense system in different organs (Flehi-Slim et al. 2015). Different studies revealed that MAL decreased the activity of cellular antioxidant defenses, superoxide dismutase (SOD), reduced glutathione (GSH), and glutathione peroxidase (GPx), thus disrupting the oxidant-antioxidant balance in the body (Akhgari et al. 2003; Franco et al. 2009; Ozsoy et al. 2016; Ullah et al. 2018; Thakur et al. 2018). Other studies showed that the activities of antioxidant enzymes were induced by MAL as a compensatory protective mechanism (El-Bini Dhouib et al. 2015).
ROS directly or indirectly adversely affects cell membrane integrity and may even cause failure in mitochondrial function (Fortunato et al. 2006; Said et al. 2014). They can also cause oxidation of cellular molecules: lipids, proteins, and DNA (Cooke et al. 2003). DNA damage may lead to the activation of the apoptotic factors or being a putative source of genetic neoplastic mutations (Syng-Ai et al. 2004; Fouad et al. 2019). Accordingly, upregulation of apoptotic markers was also reported in association with MAL toxicity in different tissues (Masoud et al. 2003; dos Santos et al. 2016). ROS can also damage DNA leading genotoxic mutagenic and carcinogenic effects (Bagchi et al. 1995; Ojha et al. 2013). Oxidative stress–induced cell damage caused by MAL exposure affects many tissues including liver, kidney, pancreas, erythrocytes, and brain (Durak et al. 2009; Selmi et al. 2012, 2015; Tuzcu et al. 2014; Ullah et al. 2018; Shieh et al. 2019). Other mechanisms of MAL-induced toxicity were discussed later.
Toxic effects of malathion in mammals
Neurotoxicity
Many studies document the correlation between high-level OP exposure and neurological or neuropsychological impairments (Naughton and Terry 2018; Glass et al. 2018). Neurological and psychological effects of OPs can be associated with either acute or chronic exposure and may include motor dysfunction and extrapyramidal symptoms, psychosis, anxiety, depression, as well as defects in attention, memory, problem-solving, cognition, and delayed polyneuropathy (Pereira et al. 2014; Naughton and Terry 2018). In cases of chronic toxicity, these symptoms are referred to collectively as chronic OP-induced neuropsychiatric disorders (COPIND) (Singh and Sharma 2000; Naughton and Terry 2018). Moreover, OP exposure has also been linked to the pathogenesis of neurodegenerative disorders like Parkinson’s disease and Alzheimer’s disease (Belin et al. 2012; Mohammadzadeh et al. 2020). Additionally, there is great evidence that suggests that prenatal and early postnatal exposure to OPs is implicated in the development of neurodevelopmental disorders in various stages, including behavioral abnormalities and deficits in attention, learning, and memory (Sapbamrer and Hongsibsong 2019).
Among mostly used pesticides, MAL is ranked fourth in targeting the nervous system (Bhardwaj et al. 2018). Manuscripts reported that it may have neurotoxic effects in both animals and humans that include a wide variety of neuromotoric, cholinergic, affective, and cognitive disorders, in addition to impairment of memory and discrimination (Komori et al. 1991; Abdel-Rahman et al. 2004; Brocardo et al. 2005; dos Santos et al. 2016). Rats treated with MAL showed neuronal degeneration in the cortex and the hippocampus that is associated with a significant decrease in the density of viable neurons in different brain regions (Sánchez-Santed et al. 2016; Abdel-Salam et al. 2017). This may be directly related to MAL-induced depressive and Parkinsonian-like behaviors (Saeedi Saravi et al. 2016; Mohammadzadeh et al. 2018). Moreover, MAL toxicity can cause muscle weakness and easy fatigability, which are associated with damage to the nervous system and the brain (Karami-Mohajeri et al. 2014; Rezg et al. 2015).
Mechanisms of malathion-induced neurotoxicity
OPs including MAL are known to modulate the expression and activity of hundreds of enzymes and proteins that may be especially relevant to the COPIND and developmental neurotoxicity. In addition to AChE inhibition, MAL-induced neurotoxicity may involve various additional non-cholinergic mechanisms including oxidative stress, neuroinflammation, axonal transport malfunctions, and apoptosis (Sánchez-Santed et al. 2016; Abdel-Salam et al. 2017) (Fig. 3).
Non-cholinergic mechanism of malathion-induced neurotoxicity. Malathion induces oxidative stress by unbalancing oxidants: reactive oxygen species (ROS), reactive nitrogen species (RNS), and others; and antioxidants: glutathione peroxidase (GPx), glutathione reductase (GRed), superoxide dismutase (SOD), and catalase. Malathion can also activate microglia to release inflammatory mediators: tumor necrosis factor-α (TNF-α), interleukin-1 (IL-1), IL-6, and nitric oxide (NO); and induce neuroinflammation. ROS can induce apoptotic pathways by inducing mitochondrial damage, with subsequent increased Bax/Bcl-2 ratio, release of cytochrome C, and the resultant activation of lethal caspase-3. ROS and caspases can induce DNA breaks and damage. Other postulated mechanisms include increased phosphorylation of TAU and reduced level of brain-derived neurotrophic factor (BDNF)
Inhibition of AChE
MAL-induced neurotoxicity can be explained in terms of increased acetylcholine following AChE inhibition (Kwong 2002). This is especially important in cases of acute MAL toxicity. However, it is worthy to note that COPIND does not appear to be dependent on AChE inhibition alone (Naughton and Terry 2018). It was also found that MAL affects brain AChE rats and mice pubs exposed during lactation (da Silva et al. 2006; Selmi et al. 2012). Although AChE inhibition certainly plays a key role in MAL-induced neurotoxicity, but when alone cannot explain the wide range of neurological signs and symptoms that have been reported (Venkatesan et al. 2017). Therefore, different non-cholinergic mechanisms have been proposed.
Oxidative stress and inflammation
Unlikely, the brain has the propensity to suffer a significant oxidative injury due to its lipid composition, which is easily oxidized due to its high oxygen consumption rate and relatively low concentration of antioxidant substances. As induction of oxidative stress plays an important role in MAL toxic effects, MAL-induced oxidative stress appears to be directly correlated to MAL-associated neurotoxicity. This was emphasized by the consistent MAL-induced alterations in endogenous enzymatic and nonenzymatic antioxidant activities in brain tissues that was associated with subsequent disruption in mitochondrial functions and enhanced incidence of free radical-mediated injury such as lipid peroxidation (Fortunato et al. 2006; Abdel-Salam et al. 2017). MAL increased oxidative stress markers, total oxidative status, and malondialdehyde (MDA) levels and reduced activity of antioxidant protective machinery, total antioxidant capacity (TAC), and SOD in brains of MAL-treated groups compared with that of the control group (Fortunato et al. 2006; Yu et al. 2013; Varol et al. 2015; Mohammadzadeh et al. 2020) (Fig. 3). Mohammadzadeh et al. (2018) found that subchronic MAL exposure induced Parkinsonian-like behavior with oxidative stress being considered to play an important role in its development (Mohammadzadeh et al. 2018).
MAL-induced oxidative stress in the brain was reported to be mediated through increased endogenous nitric oxide (NO) biosynthesis and inducible NO synthase (iNOS) expression in the rat brain. This was concluded when neuronal damage was minimized by the use of a nonselective NOS antagonist, (l-NAME), and the selective neuronal NOS antagonist, 7-NI (Abdel-Salam et al. 2017). A further contributor to MAL-induced neurotoxicity is the Paraoxonase enzyme (PON-1), an enzyme of marked interest in the view of its ability to modulate OP toxicity. PON-1 possesses arylesterase and lactonase activities and thus hydrolyzes the active metabolites of many OPs, including MAL (Primo-Parmo et al. 1996; Hosseini et al. 2019). The antioxidant and anti-inflammatory properties of PON-1 has also been proposed (Lou-Bonafonte et al. 2015). Sufficient evidence has revealed that serum PON-1 activity can be inhibited by OPs (Costa et al. 2005). Thus, this may decrease the protective ability of PON-1 against free radicals (Shih et al. 1998). A decrease in PON-1 activity in rat brain exposed to MAL was found, and the effect was dose-dependent (Varol et al. 2015; Abdel-Salam et al. 2017).
Santos et al. (2012) proposed a potential link between AChE activity and oxidative stress in experimental models of neurotoxicity (Santos et al. 2012). However, Rieger et al. (2017) proved experimentally that MAL-induced oxidative stress in cortical cell culture does not involve AChE inhibition. They found that MAL-induced decreased cell viability was directly correlated with a significant increase in superoxide anion production and that the use of an antioxidant significantly protected against MAL-induced cytotoxic effects and proceeded with the decrease in superoxide anion level; however, it did not affect MAL-induced AChE inhibition. Thus, they provided a good evidence of the significant role of oxidative stress in MAL-induced neurotoxicity (Rieger et al. 2017).
On the other hand, some studies have indicated that the activities of antioxidant enzymes are unchanged in the brains of animals treated with MAL (da Silva et al. 2006; dos Santos et al. 2011). The differences found may be related to the dose and duration of MAL exposure that were employed (Brocardo et al. 2005).
Neuroinflammation also plays a role in neurotoxicity induced by OPs. The proinflammatory cytokines play a magnificent role in mediating neuronal damage (Banks and Lein 2012). Oxidative stress and inflammation are usually interconnected, and chronic oxidative stress is usually connected with inflammation. In parallel to oxidative stress, MAL induced increase in inflammatory cytokines TNF-α and IL-6 in rat brains (Mohammadzadeh et al. 2020). Chronic exposure to MAL in mice was also associated with increased microglial cell count in parallel with increased microglial activation (Ahmed et al. 2017; Naughton and Terry 2018). Microglia are brain macrophages that protects the brain and release inflammatory mediators when activated by noxious stimulus. The role of neuroinflammation was further supported by the ameliorative role of anti-inflammatory drugs against MAL-induced behavioral changes and dopaminergic neurons loss (Ahmed et al. 2017; Naughton and Terry 2018) (Fig. 3).
Mitochondrial dysfunction, DNA damage, and apoptosis
MAL-induced oxidative stress can induce mitochondrial dysfunction, DNA breaks, autophagy, and finally apoptosis (dos Santos et al. 2016). MAL-increased O2•− formation in submitochondrial particles in the hippocampus was associated with the inhibition of mitochondrial complex I, II, and IV activities, which would have major effects on cellular energy production and may further induce oxidant-antioxidant imbalance (Delgado et al. 2006; Karami-Mohajeri et al. 2014). Defective mitochondrial function is reported to be closely related to Parkinsonism (Binukumar et al. 2010) and Alzheimer’s disease (Reddy and Beal 2008). Moreover, MAL was also found to induce DNA damage of cerebral tissues (Réus et al. 2008).
Both, mitochondrial disturbances and DNA damage may lead to the activation of apoptotic pathways. MAL treatment was found to increase proapoptotic and apoptotic proteins in the brain (Brocardo et al. 2005), such as Bax, Bak (dos Santos et al. 2016), and caspase-3 (Varol et al. 2015; Salama et al. 2019), and reduce antiapoptotic proteins, such as Bcl-2 and p-Akt (Venkatesan et al. 2017). Imbalance of proapoptotic and antiapoptotic proteins stimulates the mitochondrial release of cytochrome c and induction of caspase-dependent DNA fragmentation. MAL also induced autophagy and lysosomal membrane permeabilization in neuroblastoma cells. Lysosomal membrane permeabilization induces cathepsin B release, which may intensify apoptotic insults via its proteolytic effect (Venkatesan et al. 2017). The effect of mitochondrial disturbance and apoptosis was supported by Dos Santos et al. who showed that chronic malathion exposure, at a dose that does not inhibit AChE, induced spatial memory impairment and discrimination in mice and that the effects were correlated to mitochondrial dysfunctional and apoptosis (dos Santos et al. 2016) (Fig. 3).
Other possible mechanisms of MAL-induced neurotoxicity
MAL was also reported to induce TAU hyperphosphorylation at multiple Alzheimer disease–related sites, via activation of glycogen synthase kinase-3β and inhibition of protein phosphatase-2A; this may support the role of MAL in Alzheimer’s pathogenesis (Mohammadzadeh et al. 2020). Moreover, MAL was found to inhibit brain-derived neurotrophic factor, which plays a magnificent role in cognitive behaviors and its inhibition plays a crucial role in the development of depressive symptoms (Dorri et al. 2015) (Fig. 3).
Other mechanisms may be involved in MAL-induced neurotoxicity. Some are reported with other OPs; however, it was not clearly studied with MAL. One of these is the impairment of axonal transport by alteration of motor proteins, e.g., kinesin, or neuronal cytoskeleton proteins, such as microtubules (Naughton and Terry 2018). Another possible mechanism may involve the induction of autoimmune response in some individuals; some evidence do exist that such mechanism plays a role in other OP neurotoxic effects (El Rahman et al. 2018).
More studies are still needed to explore different mechanisms of MAL-induced neurotoxicity, with the aim to identify effective measures that help to protect high-risk populations.
Neurotoxic dose of MAL
The neurotoxic dose of MAL in humans is not specified, only data is available about MAL neurotoxic dose was collected from studies in experimental animals. Acutely, MAL induced oxidative stress in rat brain at a dose as low as 25 mg/kg (Fortunato et al. 2006). Chronically, MAL induced cerebral oxidative stress and increased caspase-3 at very small doses (5 and 10 mg/kg daily for 28 days), and the effect was dose-dependent (Varol et al. 2015). Additionally, Abdel-Rahman et al. showed that MAL also induced neurobehavioral changes and neuronal loss after subacute dermal exposure (44 mg/kg, for 30 days) (Abdel-Rahman et al. 2004). Other experimental studies used higher doses of MAL (ranging from 35 to 100 mg/kg), either daily or every other day for about 2–4 weeks or more (Coban et al. 2015; Saeedi Saravi et al. 2016).
Malathion-induced hepatotoxicity
The liver is one of the important organs that are affected by MAL toxicity. MAL causes hepatocellular damage in liver tissue and increases the activity of liver enzymes. MAL hepatotoxicity was even reported in rat pups exposed to MAL through lactation (Selmi et al. 2015). Histopathologically, MAL treatment induces hepatic degenerative changes in the form of necrosis, congestion of the central vein, hemorrhage, and focal areas of leucocytic infiltration (Abdel-Salam et al. 2017). As expected, the decrease of AChE in the liver was reported (Ince et al. 2017). In homology with cerebral effects of MAL, several studies also documented that MAL-induced changes in oxidant-antioxidant balance in hepatic tissue, and it was believed that the affection of liver tissues caused by MAL exposure is mainly a function of the overall balance between the degree of oxidative stress and the antioxidant capacity (Baiomy et al. 2015). MAL exposure resulted in the reduction of hepatic GSH, TAC, SOD, and catalase and increment of lipid peroxidation (Lasram et al. 2014a; Selmi et al. 2015). Abdel-Salam et al. found that MAL increases NO production and induces iNOS in the liver, and thus the use of NOS inhibitors minimize MAL-induced hepatotoxicity (Abdel-Salam et al. 2017).
ROS production might cause cell damage by failure in mitochondrial function due to an increase in membrane permeability and disturbance in mitochondrial function, which consequently triggers apoptotic cell death (Ranjbar et al. 2010). Esen and Uysal found increased apoptotic proteins, Bax and caspase-3, in liver tissues exposed to MAL (Esen and Uysal 2018). In addition to the oxidative damage, the inhibition of mitochondrial respiratory complexes by OPs may also be an additional intrinsic factor that triggers apoptosis (Delgado et al. 2006; Karami-Mohajeri et al. 2014). The mitochondrial injury results in a damaged oxidative pathway, and this situation may increase the use of glucose by the way of glycolysis (Karami-Mohajeri and Abdollahi 2011).
Another possible mechanism of MAL-induced hepatocellular injury leads to inflammation and the activation of the innate immune system (El-Bini Dhouib et al. 2015). Dhouib et al. reported increased total white blood cells (WBC) following MAL administration (9). WBCs are an essential part of the innate immunity, and their increase seems to concern particularly neutrophils and could result from an inflammation caused by MAL toxicity (Lasram et al. 2014b, a). The inflammatory response was associated with increased inflammatory cytokines production, as MAL increased hepatic expression of interferon-γ, interleukin (IL) 1-β, tumor necrosis factor-α, and nuclear factor-ĸB (NF-kB) in rats (Ince et al. 2017). Inflammatory mediators play a significant role in hepatic injury and activation of stellate cells, with a wide spectrum of hepatic damage including steatohepatitis and apoptosis (Fujii and Kawada 2012; Lasram et al. 2014a) (Fig. 4).
Mechanisms of malathion-induced hepatotoxicity. MAL acts on hepatocytes, inducing cell damage and oxidative stress. Tissue damage stimulates hepatic Kupffer cells to release inflammatory cytokines, IL-1β, IL-6, and INF-γ. Inflammatory cytokines affect the function of hepatocytes and stellate cells, leading to various hepatic damaging effects, e.g., hepatitis, steatosis, or apoptotic cell death. Figure adapted and modified from Lasram et al. (2014a)
MAL exposure can also affect the metabolic functions of the liver. Dhouib et al. and Selmi et al. reported reduced albumin levels in rats treated with MAL and suggested the possibility of the alteration of protein and free amino acid metabolism and their synthesis in the liver by MAL (Akbel et al. 2018; Fenske et al. 2013). Moreover, MAL exposure has been also associated with altered glucose and metabolic syndromes by inducing hepatosteatosis (Lasram et al. 2009, 2014a) (Fig. 4). This may be partially caused by changes in glucose, protein, and lipid metabolism in association with MAL exposure (Wang et al. 2014). MAL induced changes of lipid metabolism; it increased total cholesterol, low-density lipoprotein-cholesterol, and triglycerides and reduced high-density lipoprotein-cholesterol; thus, MAL exposure may be related to increased risk of atherosclerosis (Selmi et al. 2015).
Changes of glucose metabolism was evident by documents reporting a strong correlation between both blood glucose level and insulin resistance and MAL blood concentration (Pournourmohammadi et al. 2007; Lasram et al. 2008; Raafat et al. 2012; Ramirez-Vargas et al. 2018), and thus OPs have been considered as potential diabetogenic (Lassiter et al. 2008; Lasram et al. 2009). MAL-induced hyperglycemia may be mediated via activation of hepatic glycogenolysis and gluconeogenesis. MAL-induced hyperglycemia can be also explained in terms of its hepatic toxic inflammatory effects (Aboul-Soud et al. 2011; Al-Othman et al. 2012). There is actually increasing evidence of the role of chronic inflammation, especially increased hepatic IKK and NF-kB, in the development of insulin resistance (Cai et al. 2005). Thus, MAL has a considerable significant effect on hepatic pathogenesis.
Malathion-induced nephrotoxicity
The kidney is one of the target organs that are attacked by OP compounds’ toxicity. MAL-treated rats showed upregulation of renal function tests, serum creatinine, urea, and uric acid (Zidan 2015; Selmi et al. 2015). Histopathologically, MAL treatment induced renal degenerative changes including cloudy swelling and cellular desquamations, as well as swollen and pleomorphic mitochondria (Keadtisuke et al. 1989; Al-Attar 2010). It was also found that MAL induces an oxidative stress status in the renal tissues, which mostly accounts for increased lipid peroxidation and depletion of GSH, GPx, catalase, and SOD (Baiomy et al. 2015; Coban et al. 2015; Yokota et al. 2017; Selmi et al. 2018).
Recently, Yokota et al. 2017 reported a case of acute renal injury and nephrotic syndrome in a man 15 days after MAL inhalation, associated with proteinuria, abnormality in serum creatinine, and glomerular and tubular damage. Recovery took about 6 weeks under steroid therapy (Yokota et al. 2017). A similar case report of acute renal failure associated with MAL inhalation was previously reported by Albright et al. (1983). These cases represent an evidence of MAL nephrotoxicity in humans and the need to be included in the differential diagnosis of nephrotoxicity.
Effects of malathion on endocrine system
Many OPs, including MAL, have been identified as endocrine disruptors, which can disturb hormone levels through different mechanisms including inhibition of hormonal secretion (MAL was found to inhibit secretion of catecholamine) or binding to and activation of hormonal receptors, e.g., thyroid hormone, estrogen, and androgen receptors (Ishihara et al. 2003; Mnif et al. 2011; Geng et al. 2015b; Schang et al. 2016).
Effects of malathion on reproductive systems
Pesticides are known to induce reproductive toxicity in animals and humans, and many studies have documented the role of pesticides in mediating infertility (Runkle et al. 2017; Sifakis et al. 2017). The adverse effects of pesticides and OPs were reported to affect the reproductive system of both males and females (Mehrpour et al. 2014; Messerlian et al. 2018).
Effects of malathion on male reproductive system
Toxicological studies suggest that excessive use of MAL causes serious harmful effects on the male reproductive system and reduces male fertility. Choudhary et al. (2008) reported that MAL-treated experimental animals exhibited a significant decrease in the weight of the testis, seminal vesicle, epididymis, and prostate, in addition to diminished testicular and epididymal sperm count, and decreased values of fertility test by about 80% (Choudhary et al. 2008). This was supported by several studies reporting reduced motility and number of sperms and increased sperm abnormality in response to MAL treatment (Akbarsha et al. 2000; Giri et al. 2002; Geng et al. 2016; Jamal et al. 2016). Similar results were reported in adolescent male mice treated with MAL (500 mg/kg for 3 days) at the pubertal age (Slimen et al. 2014).
Histopathologically, MAL induced degenerative changes, necrosis, and edema in the interstitial tissues and seminiferous tubules (Uzun et al. 2009). In vitro effects of MAL treatment, using spermatogonial cells, showed a significant reduction of testicular germ cells viability, with histopathological changes like pyknosis, vacuolization, empty spaces, tubular degeneration, and condensed or fragmented chromatin (Bhardwaj et al. 2018). Biochemical tests were also affected, showing a significant decrease in testicular content of glycogen and sialic acid, in addition to a significant increase in testicular protein and cholesterol. The enzymatic profile was also modified, with increased activity of lactate dehydrogenase and testicular acid phosphatase, and reduced activity of testicular alkaline phosphatase and γ-glutamyl transferase (Choudhary et al. 2008). The change of enzymatic activity by MAL may be a direct consequence of MAL-induced damage of seminiferous epithelium (Uzun et al. 2009; Slimen et al. 2014). Moreover, Contreras and Bustos-Obregón suggested that MAL has a teratogenic effect on mice spermatid differentiation, perhaps due to an alkylating effect that disturbs the normal assembling of tail structural protein components (Contreras and Bustos-Obregón 1999). Furthermore, exposure to MAL was associated with reduced levels of FSH, LH, and testosterone (Uzun et al. 2009; Slimen et al. 2014).
The effect of MAL on the male reproductive system may be explained in terms of MAL capacity to induce an oxidative stress condition, by enhancing ROS production and lipid peroxidation, and reducing ferric reducing antioxidant power (FRAP) activity within testicular tissue (Bhardwaj et al. 2018). ROS may induce DNA damage and activates apoptotic pathways. It has been found that MAL disrupts the seminiferous epithelium proliferation, by impairing steroidogenesis, and that induces DNA fragmentation and apoptosis (Penna-Videau et al. 2012; Bhardwaj et al. 2018). MAL-induced increase in spermatogenic apoptosis rate was confirmed by modified protein expression of p53, Bax, and Bcl-2, which facilitate apoptosis initiation (Penna-Videau et al. 2012; Bhardwaj et al. 2018). Although it has been documented that MAL exerts its cytotoxic outcomes, via direct effects on mitochondria by the induction of apoptosis, which may be due to increased ROS activating apoptotic pathways, the apoptotic effects may also be explained in terms of MAL-genotoxic effects that alter gene expression without mutation (Geng et al. 2015a, 2016). Another possible mechanism may be the induction of RNA and DNA alkylation, leading to mutagenesis, sperm morphology disruption, or teratozoospermia (associated with a high risk of apoptosis) (Agarwal and Said 2005; Penna-Videau et al. 2012). Thus, the decreased number of sperm cells and spermatozoon may be caused by increased apoptosis associated with MAL exposure (Geng et al. 2015a, 2015b).
The abnormal levels of reproductive hormones induced by MAL may also play important roles (Yu et al. 2011). MAL was found to probably affect the hypothalamic-pituitary-gonadal axis leading to a consequent reduction in pituitary gonadotrophins, follicular stimulating hormone (FSH) and luteinizing hormone (LH), and testosterone (Uzun et al. 2009; Slimen et al. 2014). Krause and Homola (1974) proposed that the decreased testosterone level might be due to direct damage of Leydig cell or to lowered stimulation of these cells by LH (Krause and Homola 1974). The probable effect of MAL on the male reproductive system needs further study and reconsideration of the daily allowed dose of MAL, especially in developed countries with extensive use of pesticides.
Female reproductive system
OP-specific effect on the female reproductive system is not clear. It is believed that OPs, including MAL, disturb normal ovarian function resulting in a high incidence of atresia and apoptosis of granulosa cell that may consequently lead to loss and atresia of ovarian follicles (Bhardwaj and Saraf 2014). Koc. et al. reported that MAL exposure reduced the ovarian size of adult Wistar rats, and the effect was dose-dependent (Koc et al. 2009). In 2016, Ozsoy et al. and Bhardwaj and Saraf studied biochemical, histological alterations induced by MAL on ovarian tissues. They concluded that acute MAL exposure significantly reduced ovarian antioxidant defenses, SOD, and catalase activity, as compared with the control group (Ozsoy et al. 2016; Bhardwaj and Saraf 2016). Increased MDA and reduced GSH were also observed, confirming the role of oxidative stress in MAL-induced toxicities (Koc et al. 2009; Arab et al. 2018). In addition, MAL exposure was associated with histopathological alterations in the ovarian tissue, such as hemorrhage, edema, decreased number of healthy follicles, increased number of atretic follicles, follicular degeneration, and infiltration of inflammatory cells (Koc et al. 2009; Ozsoy et al. 2016). Moreover, granulosa cells showed highly condensed or marginated chromatin with a fragmented nucleus, pyknosis, loss of membrane integrity, increased empty spaces, and vacuolization in response to MAL treatment (Bhardwaj and Saraf 2016). Additionally, MAL exposure caused a significant decrease in mice oocyte survival and affected genes encoding proteins involved in transcription (BP75), translation (ribosomal protein S5), and mitochondrial function (cytochrome oxidase subunits I and III), in such a way that provides an evidence for MAL toxicity on mammal oocytes during the early oogenesis (Bonilla et al. 2008).
In addition to oxidative stress, the effect of MAL on the ovarian tissue may be induced by a change in hypothalamus-pituitary-gonadal axis. Uluitu et al. reported that chronic administration of MAL in female rats was associated with increased cerebral serotonin levels, during the active phases of the gonadal cycle (proestrus + oestrus), and this was accompanied with a decrease of LH synthesis and release and increase of the FSH release. Thus, MAL effect on the ovaries may involve affecting the reproductive encephalic regulatory serotoninergic and acetylcholinergic, in addition to affecting pituitary gland hormones (Uluitu et al. 1981). Other studies suggested that oxidative stress is the key player that mediates MAL-induced ovarian toxicity by changing the physiology of ovarian follicles, inducing apoptosis and follicular atresia (Koc et al. 2009; Ozsoy et al. 2016). Bhardwaj and Saraf found a negative relationship between follicular apoptotic incidence and the activity of antioxidant enzymes, highlighting the role of oxidative stress in MAL-induced ovarian damage (Bhardwaj and Saraf 2016). Another possibility may be that MAL mediates apoptosis by distinct mechanisms such as inhibiting compensatory ovarian hypertrophy (Asmathbanu and Kaliwal 1997).
The effect on humans was supported by only one clinical study documenting that a high level of MAL, in the follicular fluid in women, was correlated with thinner endometrial thickness and lower retrieval and fertilization. Thus pesticide exposure may also adversely affect embryological intracytoplasmic sperm injection outcomes (Al-Hussaini et al. 2018).
Effect of malathion on the thyroid gland
MAL is not listed as a primary thyroid toxic chemical. However, recent evidence found that MAL affected thyroperoxidase catalyzed iodide oxidation, which affected thyroid hormone transportation and increased incidence of parathyroid hyperplasia (Mora et al. 2016; Xiong et al. 2018). The effect of MAL on the thyroid gland in humans was supported by a study reporting the association between hypothyroidism and MAL in male applicators (Goldner et al. 2013). Akhtar et al. reported decreased T3 and T4, which was accompanied by increased TSH in rats treated with MAL (Akhtar et al. 1996). Subsequently, Xiong et al. investigated the effects of MAL, on the thyroid gland, using Fischer rat thyroid follicular cell line. They found that both mRNA and protein expression of thyroglobulin were significantly inhibited, and cAMP level and thyroid stimulating hormone (TSH) receptor expression were reduced by MAL (6.0 μg/ml). The results suggested that MAL disrupts the synthesis of thyroid hormone, probably by downregulating TSH receptor and cellular cAMP. This led to the inhibition of TSH-dependent signal transduction, thyroglobulin transcription, and thyroid hormone biosynthesis (Xiong et al. 2018). This explains reduced T3 and T4 level, with an increase of TSH as a feedback mechanism, observed by Ghisari et al. (2015). Another mechanism that may be involved in MAL-induced thyroid affection is by antagonizing aryl hydrocarbon receptors (Ghisari et al. 2015).
Mutagenic and carcinogenic potential
Pesticide exposure was correlated with genotoxicity and carcinogenicity in human and nonhuman subjects. Case control analyses of occupational exposures to OPs concluded positive correlations with non-Hodgkin lymphoma in the USA (Waddell et al. 2001), Canada (McDuffie et al. 2001), and Sweden (Eriksson et al. 2008). Occupational exposure was also correlated with increased risk of prostate cancer in Canada (Band et al. 2011). Furthermore, it was reported that in-utero environmental exposure to pesticides is associated with the development of childhood leukemia (Ferri et al. 2018; Hyland et al. 2018).
MAL is an already known mutagenic agent targeting DNA (Rupa et al. 1988; Lu et al. 2012). MAL was classified as “probably carcinogenic to humans” (Group 2A) by the International Agency for Research on Cancer (IARC) (Guyton et al. 2015). It was found to increase hepatocellular adenoma and carcinoma in mice and rats (Reuber 1985; Guyton et al. 2015). Moreover, one study found an evidence of a positive correlation between MAL exposure and thyroid cancer (Brasil et al. 2018). MAL exposure was also associated with increased risk of lung cancer in rats and the risk increased by cofactors, such as estrogen (Echiburú-Chau and Calaf 2008). Epidemiological studies and meta-analysis found a positive association between exposure to MAL and increased risk of leukemia and lymphoma, and the risk increases when MAL is used in combination with other pesticides (Hohenadel et al. 2011; Navarrete-Meneses et al. 2017). On the other hand, a relatively recent AHS analysis of male applicators found null associations with MAL use and non-Hodgkin lymphoma (Alavanja and Bonner 2012; Hu et al. 2017).
In addition, several studies reported the role of MAL in breast cancer. One of these studies was conducted by Cabello et al., who found that MAL increased cell proliferation of terminal end buds of the mammary glands of 44-day old rats, followed by the formation of mammary adenocarcinomas, after about 28 months (Cabello et al. 2001). Similar results were observed by Omran and Omar, in which MAL induced breast atypical hyperplasia and malignant changes (Omran and Omer 2015). A correlation between MAL exposure and breast cancer in Hispanic agricultural workers in California was also documented (Mills and Yang 2005).
The carcinogenicity of MAL may be directly related to MAL-induced genotoxicity (Fig. 5). The genotoxicity of MAL had been previously studied, and it is suggested that MAL and its metabolite, malaoxon, can induce DNA breaks, micronuclei, chromosomal aberrations, and sister chromatid exchanges, with malaoxon being more damaging than MAL (Moore et al. 2011; Josse et al. 2014; Navarrete-Meneses et al. 2017; Abdel-Salam et al. 2018). Genotoxicity was observed in both animals and humans (Moore et al. 2010; Bianchi et al. 2015). They may induce DNA breakage at sites of oncogenes or tumor suppressor genes, thus explain the mutagenicity and carcinogenic potential (Salvadori et al. 1988; Błasiak et al. 1999). It was found that MAL induces aberrations in KMT2A-AFF1 and ETV6-RUNX1 genes involved in the etiology of leukemia and lymphoma (Navarrete-Meneses et al. 2018). Furthermore, in vitro studies showed that MAL induced malignant transformation of breast epithelial cell lines, through genomic instability altering p53 (tumor suppressor gene) and oncogenes (Calaf and Roy 2008; Calaf et al. 2009).
Mechanisms of malathion-induced carcinogenicity. Malathion can induce carcinogenicity via its genotoxic effect. Malathion may induce genotoxicity through reactive oxygen species (ROS); ROS has the potential to induce DNA breaks and chromosomal aberrations. Other neurotoxic mechanisms include DNA methylation and/or acetylcholine esterase (AChE) inhibition. Malathion carcinogenicity may be also mediated through modulation of gene expression, modification of endocrine hormones or receptors, and immunotoxicity
Most probably, MAL-induced DNA breaks may be mediated through ROS, especially NO or its reactive metabolites, e.g., ONOO−, as the effect of MAL was minimized by 7-NI (a NOS inhibitor) (Blasiak and Stańkowska 2001; Abdel-Salam et al. 2017). Another possible genotoxic mechanism is through modifying gene promoter DNA methylation levels, thus acting via an epigenetic mechanism, and this may contribute to MAL carcinogenic potential (Zhang et al. 2012); malaoxon was found to methylate DNA bases (Blasiak and Stańkowska 2001). Others suggest that MAL induces genotoxicity and carcinogenicity through the inhibition of AChE as it was partially antagonized with atropine (Cabello et al. 2001; Calaf and Echiburú-Chau 2012) (Fig. 5). The genotoxicity of MAL was reported in Hepa RG (Josse et al. 2014), HepG (2) cells (Moore et al. 2010), blood lymphocytes (Ojha and Gupta 2015), and human choriocarcinoma cell line (Galántai et al. 2011), in addition to liver, brain, kidney, and spleen (Ojha et al. 2013).
MAL was also found to modify gene expression, which also plays a role in carcinogenicity, e.g., it was found to suppress proapoptotic Bax in breast tissues (Omran and Omer 2015). Recently, Anjitha et al. found that MAL upregulated or downregulated about 600 and 3500 genes in human lymphocytes, and about 57 of these genes are implicated in the etiology of cancer, such as genes involved in cell growth and differentiation, oncogenes, and signal transduction pathways like MAPK and RAS (Anjitha et al. 2020).
Other postulated mechanisms of MAL-associated carcinogenic potential may include immunotoxicity (Galloway and Handy 2003; Battaglia et al. 2010) and endocrine-disturbing effects. MAL exhibited weak estrogen receptor induction effect, caused changes in sex hormones circulation levels, and thus can promote the proliferation of hormone-related cancers (Kjeldsen et al. 2013; Lerro et al. 2015) (Fig. 5).
Immunomodulation
The immune system is very sensitive to a variety of environmental chemical and physical stressors, such as pesticides, which interfere with its function. The outcome of immune dysfunction may appear as a reduction in the resistance to infectious diseases and cancer or induction, facilitation, or exacerbation of allergy and autoimmune disorders (Jorsaraei et al. 2014). Increased incidence of immune-related disorders due to exposure to chemicals has been observed, including OPs and MAL (Corsini et al. 2013). Mechanisms include genotoxicity that may end with mutations in the genes coding for immunoregulatory factors, modification of immune tolerance, and activation of implicated pathways, such as inflammatory and apoptotic pathways (Corsini et al. 2013).
Experimental studies proved that OP compounds can directly increase the secretion of pro-inflammatory cytokines. The increase in pro-inflammatory cytokines such as NF-kB, TNF-α, INFγ, IL-6, IL-4, IL-1β, and IL-10 was observed in rats treated with MAL (Ince et al. 2017; Mohammadzadeh et al. 2018). Dhouib et al. found that MAL also enhanced the expression of IFN- δ in the liver of MAL-treated rats, which causes increased proliferation of immune cells such as leukocytes, neutrophils, and lymphocytes, as a direct consequence. Cytokine levels returned to control values 1–2 days after exposure, but a second increase in cytokine levels was observed in some rats 1 month later, indicating that inflammation can persist long after the initial exposure. MAL-induced leucocytosis may also be caused by the release of catecholamine as a stress hormone, which causes demargination of neutrophils, and is accompanied by lymphocytosis and by monocytosis (El-Bini Dhouib et al. 2015). In addition, MAL increased the number of total CD4+ and CD8+ T cells in the spleens of exposed rats. The increase in T cell indicates an activation of the immune system in response to a xenobiotic and proves that MAL induces inflammation. It is possible that MAL may act directly on T lymphocytes, inducing activation of cell proliferation (El-Bini Dhouib et al. 2015).
Moreover, Johnson et al. reported an increased antibody production following immunization with a T lymphocyte–dependent antigen in female mice treated with MAL at doses as low as 0.018 mg/kg, which is below the human allowable daily intake (0.02 mg/kg) (Johnson et al. 2002); their results were in agreement with those of Flipo et al. (Flipo et al. 1992). This may explain the report of Sozeri et al. of 2 children with generalized cutaneous sclerosis, with signs correlated to exposure to pesticides containing MAL (Sozeri et al. 2012). Another study revealed that weekly administration (> 33 mg/kg) elevated the level of serum rheumatoid factor at 19 weeks of age, and a higher dose (> 100 mg/kg) also increased the level of anti-anti-DNA antibodies in the serum of MRL-lpr mice (mice genetically predisposed to autoimmune disease) (Rodgers 1997). Malathion thus may be a possible player in development of an autoimmune disease, especially in predisposed individuals. However, further data still need to be collected.
On the other hand, many studies in rats showed that MAL induced immunosuppression (Zabrodskii et al. 2015; Ramadan et al. 2017). Mechanisms include the decrease of the count of blood leukocytes, granulocytes or agranulocytes, weights and cellularity of lymphoid organs, and humoral and cellular immune responses (as indicated by the decrease in the serum γ-globulin concentration and the delayed-type of hypersensitivity response, respectively) (Zabrodskii et al. 2015; Ramadan et al. 2017). In addition, it was found that MAL induced shrinkage and distortion of lymphatic follicles of the spleen and degeneration of most bone marrow cells (Ramadan et al. 2017). Moreover, Zabrodskii et al. reported that subacute exposure of rats to MAL suppressed both humoral and cellular immune responses and reduced the function of Type 1 helper cells (Th1) and to a lesser extent Th2 lymphocyte, as well as significantly decreased the level of blood cytokines: TNFα, IL-1β and IL-6, IFN-γ, IL-2, and IL-4 (Zabrodskii et al. 2015). Additionally, MAL was found to induce lymphocytes’ DNA adduct formation, which leads to apoptosis that is partially mediated by activation of intracellular caspases (Ojha and Gupta 2017). Seth et al. (2001) found changes in GSH and γ-glutamyl transpeptidase level in lymphocytes in humans intoxicated with MAL (Seth et al. 2001).
Thus, the effect of MAL on the immune system is well documented in experimental animals; the alteration between either immunosuppression or immunostimulation may be a factor of the dose and duration of exposure, experimental design, nutritional status, and innate immunity. However, the available studies on the effects of MAL on human’s immune system is not sufficient, and further studies are necessary (Corsini et al. 2013).
Other malathion-related toxic effects
Effect on blood cells
MAL was shown to induce normocytic normochromic anemia, thrombocytopenia, and prolongation of the clotting time (Ramadan et al. 2017). Hematotoxic activity may be attributed to the decrease in hematopoiesis due to bone marrow suppression, an increase in the rate of erythrocytes breakdown, internal hemorrhage, and a reduction in clotting factors production resulting from liver toxicity (Durak et al. 2009; Kundu and Roychoudhury 2009). Under normal conditions, erythrocytes are resistant to hemolysis resulting from peroxidative reactions, by the help of antioxidant enzymes and molecules; SOD, GPx, catalase, and GSH. Excessive ROS production, associated with MAL-induced oxidative stress and reduction in antioxidant defenses, may be associated with increased hemolytic oxidative injury of erythrocytes (Fakhri-Bafghi et al. 2016; Farag and Alagawany 2018). MAL was found to increase lipid peroxidation and deplete antioxidant defenses in rats and human erythrocytes (Uzun et al. 2009; Ramadan et al. 2017). Akhgari et al. found that oxidative stress and the degree of erythrocyte lipid peroxidation was correlated with the degree of inhibition of erythrocytes AChE (Akhgari et al. 2003; Farag and Alagawany 2018).
Acute pancreatitis
Previous reports have suggested that acute pancreatitis may follow the oral ingestion of several OPs (Hsiao et al. 1996). MAL may also induce pancreatic-β-cells injury, hyperglycemia, temporary hyperinsulinemia, and oxidative stress (Tuzcu et al. 2014). A case report of a combination of acute pancreatitis and toxic hepatitis, which developed in a 30-year-old farmworker, was provided by Fındıklı et al. (2018). The possible pathogeneses of the pancreatic injury may be excessive cholinergic stimulation of the pancreas and ductular hypertension (Hsiao et al. 1996).
Lung injury
Many OPs are implicated in the development of pulmonary injury in both humans and experimental animals (Atiş et al. 2002; Nambiar et al. 2007; Moin-Azad Tehrani et al. 2011; Angelini et al. 2013). It is possible that these chemicals are directly affecting the viability of the pulmonary epithelium resulting in pulmonary distress (Angelini et al. 2015). Uysal and Karaman (2018) revealed that acute oral MAL administration increased oxidative stress and apoptosis in the lung tissue of rats. Tissue GPx and SOD activities decreased and MDA level and the expression of proapoptotic proteins Bax and caspase-3 significantly increased in the MAL-treated group (Uysal and Karaman 2018). Furthermore, thickened lung epithelium was also observed (Saadi et al. 2008). In another study, malaoxone (the toxic metabolite of MAL) induced apoptotic cytotoxicity of primary cultured human large and small airway cells, associated with the upregulation of caspases (Angelini et al. 2015). Thus, there is evidence of pulmonary risk associated with MAL not only in animals but also in human.
Pre- and post-natal exposure toxicity
In recent years, a growing body of evidence indicates the high vulnerability of pregnant/lactating women concerning pesticide exposures (Berkowitz et al. 2003; Salas et al. 2003). Many studies report neurotoxicity to be linked to perinatal exposure to OPs in animals (Slotkin et al. 2005; da Silva et al. 2006). Both high and low levels of OP exposure may have a serious impact on pregnant women and children (Sapbamrer and Hongsibsong 2019). Children are more vulnerable than adults because of the incomplete nature of the detoxification process, the age-related speed of neurologic development, the increased exposure relative to the body weight, and the undeveloped immune system (Eskenazi et al. 1999; Fiedler et al. 2015). The major concerns related to prenatal and postnatal exposure in children is neurodevelopmental impact. Exposure to pesticides in a period of great vulnerability is a major factor in causing dysfunction in the nervous system and neurodevelopmental disorders (Landrigan et al. 1999; Heyer and Meredith 2017).
Bossi et al. found that both MAL and its metabolite appear in the amniotic fluid of female rats, and thus the fetus is exposed to them (Bossi et al. 2013). Several studies reported the effect of prenatal and postnatal exposure to MAL. Prabhakaran et al. found that MAL exposure during pregnancy induces maternal toxicity in mice and causes fetal growth retardation. MAL effects were aggravated with protein-deficient diet, GSH depletion, and decreased activities of GPx, glutathione reductase, and glucose-6-phosphate dehydrogenase (Prabhakaran et al. 1993).
Da Silva et al. studied the effect of MAL exposure through lactation in mice. They found that MAL exposure induced significantly high inhibitory effect on AChE in the brain of the offspring even at the lowest dose (20 mg/kg); however, AChE activity in the mother was inhibited only at the higher dose (200 mg/kg) (da Silva et al. 2006). This may be explained by reduced metabolizing detoxifying capacity in neonates. Similarly, Selmi et al. reported that MAL exposure during lactation induced a high inhibitory effect on the brain, plasma, and erythrocyte AChE activities in rat pups and was also associated with increased oxidative stress (Selmi et al. 2012). MAL was also detected in human milk in women from Bhopal, India, who used MAL as a pesticide. The offspring were found to receive 4 times more MAL than the average daily intake recommended by the World Health Organization (Sanghi et al. 2003). Gunier et al. found an adverse relationship between the agricultural use of neurotoxic pesticides near maternal residences during pregnancy and the IQ of 7-year-old children (Gunier et al. 2017). The effect of MAL on the reproductive function and neurodevelopment in young rats is more pronounced when combined with other pesticides (synergism) (Moser et al. 2006; Yu et al. 2013).
Since ACh plays important trophic roles in brain development, thus excessive exposure during the developmental period can lead to abnormal neurodevelopment by modifying the timing or the intensity of ACh neurotrophic actions (Slotkin 2004). Moreover, MAL has direct effects on cellular processes, such as oxidative stress, which can affect brain development and are unrelated to the inhibition of AChE (Slotkin 2004; Selmi et al. 2012). Hepatotoxicity and nephrotoxicity were also observed by Selmi et al. in rat pups exposed to MAL through breastfeeding (Selmi et al. 2015).
Therefore, the state of knowledge of pregnant women and nursing mothers should be updated to help them protect themselves and their children from exposure to pesticides.
Protection and management of MAL toxic exposures
Treatment of MAL toxicity
Classical measures
Acute MAL toxicity can be treated as ordinary OP toxicity; however, acute toxicity incidence is relatively low. The primary cause of death after an AChE inhibitor poisoning is respiratory failure and hypoxemia due to muscarinic effects on the cardiovascular and pulmonary systems (i.e., bronchospasm, aspiration, bradycardia, or hypotension), nicotinic effects on skeletal muscles (weakness and paralysis), loss of central respiratory drive, and seizures (rare). Initial treatment for acute MAL toxicity is mainly concerned with ensuring an adequate airway, oxygenation, and ventilation and stabilizing patient hemodynamics by reversing excessive muscarinic effects, mainly by using atropine (Eddleston et al. 2008; Eddleston 2019). Once the patient is stable, the administration of an AChE-reactivating drug, such as pralidoxime or obidoxime, should be considered along with skin and/or gastric decontamination (Roberts and Aaron 2007) (Fig. 6). Benzodiazepines are to be used for patients with agitation and seizures.
Planned recommendation for the management of patients presenting with a history of acute organophosphorus poisoning. Figure modified from that of Roberts and Aaron (2007). AChE acetyl cholinesterase, CNS central nervous system, ICU intensive care unit, OPs organophosphates
Novel treatments for MAL poisoning
Lipid emulsions
Intralipid is the brand name of the first safe fat emulsion developed for human use and was introduced in 1962. Intravenous lipid emulsion (ILE) is always used in parenteral nutrition therapy. ILE has proved to be an effective treatment for local anesthetic systemic toxicity in humans and animals and is promising as a novel antidote for a wide range of other lipophilic drug poisonings (Ozsoy et al. 2016). ILE seriously improved TAC in rats with MAL-induced neurotoxicity (Basarslan et al. 2014), restored SOD activity considerably in the ovarian tissue, partially improved histopathological changes, and inhibited MAL-induced upregulation of caspase-3 (Ozsoy et al. 2016). Uysal and Karaman (2018) study suggests that ILE has treatment efficacy on MAL-induced lung toxicity (Uysal and Karaman 2018). Evidence of protective effects on pancreatic (minimized pancreatic- β-cells) and hepatic damage caused by MAL, using intralipid fat emulsion, was also found (Tuzcu et al. 2014; Esen and Uysal 2018). That ILE is a promising safe therapy for acute MAL intoxication. Beside lipid sink theory, the use of fatty acids contained within the ILE as a good source of energy might have provided a protective mechanism against apoptosis by further increasing the ATP levels in the cells (Esen and Uysal 2018).
Magnesium and calcium channel blockers
The use of magnesium or calcium channel blockers such as nifedipine in OP poisoning has long been advocated (Petroianu et al. 1998; Brvar et al. 2018). Both preclinical and clinical data suggest that they might be promising adjunct treatments. However, the evidence is currently insufficient to recommend their use, and the precise mechanism of how they might work remains unclear (Brvar et al. 2018; Eddleston 2019). Mohammadi et al. found that magnetic isotopes of magnesium significantly recovered MAL-induced arrhythmia and cardiac failure in rats (Mohammadi et al. 2011). Recently, Hsu et al. revealed that MAL toxicity in glial cells was associated with the stimulation of Ca2+-signal transduction and induction of Ca2+-associated cytotoxicity (Hsu et al. 2019). This may explain the role of calcium channel blockers in OP toxicities.
Potential protective measures against long-term effects of MAL exposure
Several studies document the protective effect of different antioxidants and minerals against toxic effects associated with MAL exposure. Treatment with antioxidants or mineral substances can decrease lipid peroxidation and oxidative stress related to MAL-induced toxicity (Ince et al. 2017; Akbel et al. 2018). Among those are N-acetyl cysteine (Bhardwaj et al. 2018), vitamin E and C, selenium (Durak et al. 2009; Uzun et al. 2009; Aboul-Soud et al. 2011; Lu et al. 2012), α-lipoic acid (Omran and Omer 2015), and taurine amino acid (Ince et al. 2017), which have shown promising protective effects against different organs’ toxicity that was induced by MAL.
Natural compounds are gaining much attention, as being considered safer and can be used daily on highly exposed personals. Many natural compounds showed potential protective activity against various types of toxicities (Madrigal-Santillán et al. 2014; Wu et al. 2017). Polyphenols, such as flavonoids, anthocyanins, and phenolic acids, are powerful antioxidant substances (Madrigal-Santillán et al. 2014), and many of them approved efficacy against MAL-induced tissue damage. Akbel et al. found that resveratrol reduced the level of malaoxon in different tissues and counteracted the toxic effects of MAL and maintained antioxidant defenses (Akbel et al. 2018). Ginger and zinc mixture ameliorated the toxic effect of MAL in the liver and the kidney due to its antioxidant effect (Baiomy et al. 2015). Mohammadzadeh and his colleagues found that crocin, saffron active components, exhibited protective effects against MAL-induced Parkinson-like behavior through reducing lipid peroxidation, improving motor deficits and anti-inflammatory effects (Mohammadzadeh et al. 2018). Other natural products that approved efficacy include aged garlic extract (Ramadan et al. 2017), grape seed extract (Abdel-Salam et al. 2018), Aloe vera (Gupta et al. 2019), caffeic acid (Rezg et al. 2015), thymoquinone (Abdel-Daim et al. 2020), and curcumin (Alp et al. 2012). Recommendations for increasing the use of these antioxidants on a daily basis, especially those working in pesticides’ factories or agriculture, may be warranted.
Few data support the possible effectiveness of anti-inflammatory drugs in ameliorating MAL toxicity; one study used acetylsalicylic acid and dexamethasone to ameliorate MAL-induced neurotoxicity. The use of anti-inflammatory drugs was associated with improved neurobehavioral performance and reduced neurodegeneration in the nigrostriatal system (Ahmed et al. 2017). Another study showed that the use of dexamethasone improved a case of nephrotic syndrome that was associated with MAL (Yokota et al. 2017). Further studies regarding the effectiveness of anti-inflammatory drugs against MAL-induced toxicity are needed.
One new trend in therapy, which is still not investigated in OP toxicity, is probiotics. Trinder et al. reported that lactobacilli are able to degrade some pesticides and reduce the accumulation of mercury and arsenic. So, they assume that similar effects may take place with OPs including MAL, given that the lactobacilli can also attenuate ROS production, enhance gastrointestinal barrier function, reduce inflammation, and modulate host xenobiotic metabolism (Trinder et al. 2015). Probiotics, if proven effective, will represent a convenient and cost-effective protective measure against MAL toxicity, especially neurotoxicity (as the gut-brain axis is being extensively studied nowadays). I thus recommend the use of probiotics in MAL-induced toxic experimental models to assess their potential protective value.
Conclusion
MAL toxicity is well documented, affecting nearly every tissue in the body. Special consideration to prenatal and postnatal exposure and those exposed during occupation may be needed. MAL toxicity was reported to occur experimentally at doses lower than the daily allowed ones, so reconsideration of the allowed level may be necessary. Nutritional status and the combined use of pesticides play a significant role in amelioration or potentiation of toxic effects. Further studies are needed regarding the carcinogenic and genotoxic effects in humans and potential protective measures.
References
Abdel-Daim MM, Abushouk AI, Bungău SG et al (2020) Protective effects of thymoquinone and diallyl sulphide against malathion-induced toxicity in rats. Environ Sci Pollut Res Int. https://doi.org/10.1007/s11356-019-07580-y
Abdel-Rahman A, Dechkovskaia AM, Goldstein LB et al (2004) Neurological deficits induced by malathion, DEET, and permethrin, alone or in combination in adult rats. J Toxicol Environ Health A 67:331–356
Abdel-Salam OME, Youness ER, Mohammed NA et al (2017) Nitric oxide synthase inhibitors protect against brain and liver damage caused by acute malathion intoxication. Asian Pac J Trop Med 10:773–786. https://doi.org/10.1016/j.apjtm.2017.07.018
Abdel-Salam OME, Galal AF, Hassanane MM et al (2018) Grape seed extract alone or combined with atropine in treatment of malathion induced neuro- and genotoxicity. J Nanosci Nanotechnol 18:564–575. https://doi.org/10.1166/jnn.2018.13943
Abdollahi M, Ranjbar A, Shadnia S et al (2004) Pesticides and oxidative stress: a review. Med Sci Monit 10:RA141–RA147
Aboul-Soud MAM, Al-Othman AM, El-Desoky GE et al (2011) Hepatoprotective effects of vitamin E/selenium against malathion-induced injuries on the antioxidant status and apoptosis-related gene expression in rats. J Toxicol Sci 36:285–296
Agarwal A, Said TM (2005) Oxidative stress, DNA damage and apoptosis in male infertility: a clinical approach. BJU Int 95:503–507. https://doi.org/10.1111/j.1464-410X.2005.05328.x
Ahmed D, Abdel-Rahman RH, Salama M et al (2017) Malathion neurotoxic effects on dopaminergic system in mice: role of inflammation. J Biomed Sci 6. https://doi.org/10.4172/2254-609X.100074
Akbarsha MA, Latha PN, Murugaian P (2000) Retention of cytoplasmic droplet by rat cauda epididymal spermatozoa after treatment with cytotoxic and xenobiotic agents. J Reprod Fertil 120:385–390. https://doi.org/10.1530/jrf.0.1200385
Akbel E, Arslan-Acaroz D, Demirel HH et al (2018) The subchronic exposure to malathion, an organophosphate pesticide, causes lipid peroxidation, oxidative stress, and tissue damage in rats: the protective role of resveratrol. Toxicol Res (Camb) 7:503–512. https://doi.org/10.1039/c8tx00030a
Akhgari M, Abdollahi M, Kebryaeezadeh A et al (2003) Biochemical evidence for free radical-induced lipid peroxidation as a mechanism for subchronic toxicity of malathion in blood and liver of rats. Hum Exp Toxicol 22:205–211. https://doi.org/10.1191/0960327103ht346oa
Akhtar N, Kayani SA, Ahmad MM, Shahab M (1996) Insecticide-induced changes in secretory activity of the thyroid gland in rats. J Appl Toxicol 16:397–400. https://doi.org/10.1002/(SICI)1099-1263(199609)16:5<397::AID-JAT362>3.0.CO;2-Y
Al-Attar AM (2010) Physiological and histopathological investigations on the effects of alpha-lipoic acid in rats exposed to malathion. J Biomed Biotechnol 2010:203503. https://doi.org/10.1155/2010/203503
Alavanja MCR, Bonner MR (2012) Occupational pesticide exposures and cancer risk: a review. J Toxicol Environ Health B Crit Rev 15:238–263. https://doi.org/10.1080/10937404.2012.632358
Albright RK, Kram BW, White RP (1983) Malathion exposure associated with acute renal failure. JAMA 250:2469–2469. https://doi.org/10.1001/jama.1983.03340180031010
Al-Hussaini TK, Abdelaleem AA, Elnashar I et al (2018) The effect of follicullar fluid pesticides and polychlorinated biphenyls concentrations on intracytoplasmic sperm injection (ICSI) embryological and clinical outcome. Eur J Obstet Gynecol Reprod Biol 220:39–43. https://doi.org/10.1016/j.ejogrb.2017.11.003
Al-Othman AM, Al-Othman ZA, El-Desoky GE et al (2012) Ameliorative effect of α-tocopherol and selenium on effects of malathion on plasmatic biochemical indices and lesions in the liver of rats. Curr Pharm Anal 8:214–218
Alp H, Aytekin I, Hatipoglu NK et al (2012) Effects of sulforophane and curcumin on oxidative stress created by acute malathion toxicity in rats. Eur Rev Med Pharmacol Sci 16(Suppl 3):144–148
Angelini DJ, Dorsey RM, Willis KL et al (2013) Chemical warfare agent and biological toxin-induced pulmonary toxicity: could stem cells provide potential therapies? Inhal Toxicol 25:37–62. https://doi.org/10.3109/08958378.2012.750406
Angelini DJ, Moyer RA, Cole S et al (2015) The pesticide metabolites paraoxon and malaoxon induce cellular death by different mechanisms in cultured human pulmonary cells. Int J Toxicol 34:433–441. https://doi.org/10.1177/1091581815593933
Anjitha R, Antony A, Shilpa O et al (2020) Malathion induced cancer-linked gene expression in human lymphocytes. Environ Res 182:109131. https://doi.org/10.1016/j.envres.2020.109131
Arab SA, Nikravesh MR, Jalali M, Fazel A (2018) Evaluation of oxidative stress indices after exposure to malathion and protective effects of ascorbic acid in ovarian tissue of adult female rats. Electron Physician 10:6789–6795. https://doi.org/10.19082/6789
Asmathbanu I, Kaliwal BB (1997) Temporal effect of methyl parathion on ovarian compensatory hypertrophy, follicular dynamics and estrous cycle in hemicastrated albino rats. J Basic Clin Physiol Pharmacol 8:237–254
Atiş S, Cömelekoğlu U, Coşkun B et al (2002) Electrophysiological and histopathological evaluation of respiratory tract, diaphragm, and phrenic nerve after dichlorvos inhalation in rats. Inhal Toxicol 14:199–215. https://doi.org/10.1080/089583701753403999
Bagchi D, Bagchi M, Hassoun EA, Stohs SJ (1995) In vitro and in vivo generation of reactive oxygen species, DNA damage and lactate dehydrogenase leakage by selected pesticides. Toxicology 104:129–140. https://doi.org/10.1016/0300-483x(95)03156-a
Baiomy AA, Attia HF, Soliman MM, Makrum O (2015) Protective effect of ginger and zinc chloride mixture on the liver and kidney alterations induced by malathion toxicity. Int J Immunopathol Pharmacol 28:122–128. https://doi.org/10.1177/0394632015572083
Band PR, Abanto Z, Bert J et al (2011) Prostate cancer risk and exposure to pesticides in British Columbia farmers. Prostate 71:168–183. https://doi.org/10.1002/pros.21232
Banks CN, Lein PJ (2012) A review of experimental evidence linking neurotoxic organophosphorus compounds and inflammation. Neurotoxicology 33:575–584. https://doi.org/10.1016/j.neuro.2012.02.002
Basarslan SK, Alp H, Senol S et al (2014) Is intralipid fat emulsion a promising therapeutic strategy on neurotoxicity induced by malathion in rats? Eur Rev Med Pharmacol Sci 18:471–476
Battaglia CLR, Gogal RM, Zimmerman K, Misra HP (2010) Malathion, lindane, and piperonyl butoxide, individually or in combined mixtures, induce immunotoxicity via apoptosis in murine splenocytes in vitro. Int J Toxicol 29:209–220. https://doi.org/10.1177/1091581809357954
Belin AC, Ran C, Anvret A et al (2012) Association of a protective paraoxonase 1 (PON1) polymorphism in Parkinson’s disease. Neurosci Lett 522:30–35. https://doi.org/10.1016/j.neulet.2012.06.007
Berkowitz GS, Obel J, Deych E et al (2003) Exposure to indoor pesticides during pregnancy in a multiethnic, urban cohort. Environ Health Perspect 111:79–84. https://doi.org/10.1289/ehp.5619
Bhardwaj JK, Saraf P (2014) Malathion-induced granulosa cell apoptosis in caprine antral follicles: an ultrastructural and flow cytometric analysis. Microsc Microanal 20:1861–1868. https://doi.org/10.1017/S1431927614013452
Bhardwaj JK, Saraf P (2016) Granulosa cell apoptosis by impairing antioxidant defense system and cellular integrity in caprine antral follicles post malathion exposure. Environ Toxicol 31:1944–1954. https://doi.org/10.1002/tox.22195
Bhardwaj JK, Saraf P, Kumari P et al (2018) N-acetyl-cysteine mediated inhibition of spermatogonial cells apoptosis against malathion exposure in testicular tissue. J Biochem Mol Toxicol 32:e22046. https://doi.org/10.1002/jbt.22046
Bianchi J, Mantovani MS, Marin-Morales MA (2015) Analysis of the genotoxic potential of low concentrations of Malathion on the Allium cepa cells and rat hepatoma tissue culture. J Environ Sci (China) 36:102–111. https://doi.org/10.1016/j.jes.2015.03.034
Binukumar BK, Bal A, Kandimalla RJL, Gill KD (2010) Nigrostriatal neuronal death following chronic dichlorvos exposure: crosstalk between mitochondrial impairments, α synuclein aggregation, oxidative damage and behavioral changes. Mol Brain 3:35. https://doi.org/10.1186/1756-6606-3-35
Blasiak J, Stańkowska D (2001) Genotoxicity of malaoxon: induction of oxidized and methylated bases and protective effect of α-tocopherol. Pestic Biochem Physiol 71:88–96. https://doi.org/10.1006/pest.2001.2557
Błasiak J, Jałoszynski P, Trzeciak A, Szyfter K (1999) In vitro studies on the genotoxicity of the organophosphorus insecticide malathion and its two analogues. Mutat Res 445:275–283. https://doi.org/10.1016/s1383-5718(99)00132-1
Bogen KT, Singhal A (2017) Malathion dermal permeability in relation to dermal load: assessment by physiologically based pharmacokinetic modeling of in vivo human data. J Environ Sci Health B 52:138–146. https://doi.org/10.1080/03601234.2016.1248150
Bonilla E, Hernández F, Cortés L et al (2008) Effects of the insecticides malathion and diazinon on the early oogenesis in mice in vitro. Environ Toxicol 23:240–245. https://doi.org/10.1002/tox.20332
Bossi R, Vinggaard AM, Taxvig C et al (2013) Levels of pesticides and their metabolites in Wistar rat amniotic fluids and maternal urine upon gestational exposure. Int J Environ Res Public Health 10:2271–2281. https://doi.org/10.3390/ijerph10062271
Brasil VLM, Ramos Pinto MB, Bonan RF et al (2018) Pesticides as risk factors for head and neck cancer: a review. J Oral Pathol Med 47:641–651. https://doi.org/10.1111/jop.12701
Brocardo PS, Pandolfo P, Takahashi RN et al (2005) Antioxidant defenses and lipid peroxidation in the cerebral cortex and hippocampus following acute exposure to malathion and/or zinc chloride. Toxicology 207:283–291. https://doi.org/10.1016/j.tox.2004.09.012
Brodeur J, DuBois KP (1967) Studies on factors influencing the acute toxicity of malathion and malaoxon in rats. Can J Physiol Pharmacol 45:621–631. https://doi.org/10.1139/y67-075
Brvar M, Chan MY, Dawson AH et al (2018) Magnesium sulfate and calcium channel blocking drugs as antidotes for acute organophosphorus insecticide poisoning - a systematic review and meta-analysis. Clin Toxicol (Phila) 56:725–736. https://doi.org/10.1080/15563650.2018.1446532
Buratti FM, Testai E (2005) Malathion detoxification by human hepatic carboxylesterases and its inhibition by isomalathion and other pesticides. J Biochem Mol Toxicol 19:406–414. https://doi.org/10.1002/jbt.20106
Buratti FM, D’Aniello A, Volpe MT et al (2005) Malathion bioactivation in the human liver: the contribution of different cytochrome P450 isoforms. Drug Metab Dispos 33:295–302. https://doi.org/10.1124/dmd.104.001693
Cabello G, Valenzuela M, Vilaxa A et al (2001) A rat mammary tumor model induced by the organophosphorous pesticides parathion and malathion, possibly through acetylcholinesterase inhibition. Environ Health Perspect 109:471–479. https://doi.org/10.1289/ehp.01109471
Cai D, Yuan M, Frantz DF et al (2005) Local and systemic insulin resistance resulting from hepatic activation of IKK-beta and NF-kappaB. Nat Med 11:183–190. https://doi.org/10.1038/nm1166
Calaf GM, Echiburú-Chau C (2012) Synergistic effect of malathion and estrogen on mammary gland carcinogenesis. Oncol Rep 28:640–646. https://doi.org/10.3892/or.2012.1817
Calaf GM, Roy D (2008) Cancer genes induced by malathion and parathion in the presence of estrogen in breast cells. Int J Mol Med 21:261–268. https://doi.org/10.3892/ijmm.21.2.261
Calaf GM, Echiburu-Chau C, Roy D (2009) Organophosphorous pesticides and estrogen induce transformation of breast cells affecting p53 and c-Ha-ras genes. Int J Oncol 35:1061–1068. https://doi.org/10.3892/ijo_00000421
Chambers JE, Levi PE (2013) Organophosphates chemistry, fate, and effects: chemistry, fate, and effects. Elsevier
Chen L, Zhao T, Pan C et al (2013) Absorption and excretion of organophosphorous insecticide biomarkers of malathion in the rat: implications for overestimation bias and exposure misclassification from environmental biomonitoring. Regul Toxicol Pharmacol 65:287–293. https://doi.org/10.1016/j.yrtph.2012.12.010
Choudhary N, Goyal R, Joshi SC (2008) Effect of malathion on reproductive system of male rats. J Environ Biol 29:259–262
Coban FK, Ince S, Kucukkurt I et al (2015) Boron attenuates malathion-induced oxidative stress and acetylcholinesterase inhibition in rats. Drug Chem Toxicol 38:391–399. https://doi.org/10.3109/01480545.2014.974109
Contreras HR, Bustos-Obregón E (1999) Morphological alterations in mouse testis by a single dose of malathion. J Exp Zool 284:355–359
Cooke MS, Evans MD, Dizdaroglu M, Lunec J (2003) Oxidative DNA damage: mechanisms, mutation, and disease. FASEB J 17:1195–1214. https://doi.org/10.1096/fj.02-0752rev
Corsini E, Sokooti M, Galli CL et al (2013) Pesticide induced immunotoxicity in humans: a comprehensive review of the existing evidence. Toxicology 307:123–135. https://doi.org/10.1016/j.tox.2012.10.009
Costa LG, Cole TB, Vitalone A, Furlong CE (2005) Measurement of paraoxonase (PON1) status as a potential biomarker of susceptibility to organophosphate toxicity. Clin Chim Acta 352:37–47. https://doi.org/10.1016/j.cccn.2004.09.019
da Silva AP, Meotti FC, Santos ARS, Farina M (2006) Lactational exposure to malathion inhibits brain acetylcholinesterase in mice. Neurotoxicology 27:1101–1105. https://doi.org/10.1016/j.neuro.2006.04.002
Delgado EHB, Streck EL, Quevedo JL, Dal-Pizzol F (2006) Mitochondrial respiratory dysfunction and oxidative stress after chronic malathion exposure. Neurochem Res 31:1021–1025. https://doi.org/10.1007/s11064-006-9111-1
Dorri SA, Hosseinzadeh H, Abnous K et al (2015) Involvement of brain-derived neurotrophic factor (BDNF) on malathion induced depressive-like behavior in subacute exposure and protective effects of crocin. Iran J Basic Med Sci 18:958–966
dos Santos AA, dos Santos DB, Ribeiro RP et al (2011) Effects of K074 and pralidoxime on antioxidant and acetylcholinesterase response in malathion-poisoned mice. Neurotoxicology 32:888–895. https://doi.org/10.1016/j.neuro.2011.05.008
dos Santos AA, Naime AA, de Oliveira J et al (2016) Long-term and low-dose malathion exposure causes cognitive impairment in adult mice: evidence of hippocampal mitochondrial dysfunction, astrogliosis and apoptotic events. Arch Toxicol 90:647–660. https://doi.org/10.1007/s00204-015-1466-0
Durak D, Uzun FG, Kalender S et al (2009) Malathion-induced oxidative stress in human erythrocytes and the protective effect of vitamins C and E in vitro. Environ Toxicol 24:235–242. https://doi.org/10.1002/tox.20423
Echiburú-Chau C, Calaf GM (2008) Rat lung cancer induced by malathion and estrogen. Int J Oncol 33:603–611
Eddleston M (2019) Novel clinical toxicology and pharmacology of organophosphorus insecticide self-poisoning. Annu Rev Pharmacol Toxicol 59:341–360. https://doi.org/10.1146/annurev-pharmtox-010818-021842
Eddleston M, Buckley NA, Eyer P, Dawson AH (2008) Management of acute organophosphorus pesticide poisoning. Lancet 371:597–607. https://doi.org/10.1016/S0140-6736(07)61202-1
El Rahman HAA, Salama M, Gad El-Hak SA et al (2018) A panel of autoantibodies against neural proteins as peripheral biomarker for pesticide-induced neurotoxicity. Neurotox Res 33:316–336. https://doi.org/10.1007/s12640-017-9793-y
El-Bini Dhouib I, Lasram MM, Annabi A et al (2015) A comparative study on toxicity induced by carbosulfan and malathion in Wistar rat liver and spleen. Pestic Biochem Physiol 124:21–28. https://doi.org/10.1016/j.pestbp.2015.03.012
Eriksson M, Hardell L, Carlberg M, Åkerman M (2008) Pesticide exposure as risk factor for non-Hodgkin lymphoma including histopathological subgroup analysis. In: International Journal of Cancer. https://onlinelibrary.wiley.com/doi/abs/10.1002/ijc.23589. Accessed 24 Sep 2019
Esen M, Uysal M (2018) Protective effects of intravenous lipid emulsion on malathion-induced hepatotoxicity. Bratisl Lek Listy 119:373–378. https://doi.org/10.4149/BLL_2018_069
Eskenazi B, Bradman A, Castorina R (1999) Exposures of children to organophosphate pesticides and their potential adverse health effects. Environ Health Perspect 107(Suppl 3):409–419. https://doi.org/10.1289/ehp.99107s3409
Eskenazi B, Marks AR, Bradman A et al (2007) Organophosphate pesticide exposure and neurodevelopment in young Mexican-American children. Environ Health Perspect 115:792–798. https://doi.org/10.1289/ehp.9828
Fakhri-Bafghi MS, Ghasemi-Niri SF, Mostafalou S et al (2016) Protective effect of selenium-based medicines on toxicity of three common organophosphorus compounds in human erythrocytes in vitro. Cell J 17:740–747
Farag MR, Alagawany M (2018) Erythrocytes as a biological model for screening of xenobiotics toxicity. Chem Biol Interact 279:73–83. https://doi.org/10.1016/j.cbi.2017.11.007
Fenske RA, Lu C, Negrete M, Galvin K (2013) Breaking the take home pesticide exposure pathway for agricultural families: workplace predictors of residential contamination. Am J Ind Med 56:1063–1071. https://doi.org/10.1002/ajim.22225
Ferri GM, Guastadisegno CM, Intranuovo G et al (2018) Maternal exposure to pesticides, paternal occupation in the army/police force, and CYP2D6*4 polymorphism in the etiology of childhood acute leukemia. J Pediatr Hematol Oncol 40:e207–e214. https://doi.org/10.1097/MPH.0000000000001105
Fiedler N, Rohitrattana J, Siriwong W et al (2015) Neurobehavioral effects of exposure to organophosphates and pyrethroid pesticides among Thai children. Neurotoxicology 48:90–99. https://doi.org/10.1016/j.neuro.2015.02.003
Fındıklı HA, Bilge Z, Aydın H et al (2018) The combination of acute pancreatitis and toxic hepatitis developing secondary to exposure to malathion: a case report. Acta Gastroenterol Belg 81:333–335
Flehi-Slim I, Chargui I, Boughattas S et al (2015) Malathion-induced hepatotoxicity in male Wistar rats: biochemical and histopathological studies. Environ Sci Pollut Res Int 22:17828–17838. https://doi.org/10.1007/s11356-015-5014-5
Flipo D, Bernier J, Girard D et al (1992) Combined effects of selected insecticides on humoral immune response in mice. Int J Immunopharmacol 14:747–752. https://doi.org/10.1016/0192-0561(92)90071-r
Fortunato JJ, Feier G, Vitali AM et al (2006) Malathion-induced oxidative stress in rat brain regions. Neurochem Res 31:671–678. https://doi.org/10.1007/s11064-006-9065-3
Fouad D, Badr A, Attia HA (2019) Hepatoprotective activity of raspberry ketone is mediated via inhibition of the NF-κB/TNF-α/caspase axis and mitochondrial apoptosis in chemically induced acute liver injury. Toxicol Res. https://doi.org/10.1039/C9TX00068B
Franco JL, Posser T, Mattos JJ et al (2009) Zinc reverses malathion-induced impairment in antioxidant defenses. Toxicol Lett 187:137–143. https://doi.org/10.1016/j.toxlet.2009.02.015
Fujii H, Kawada N (2012) Inflammation and fibrogenesis in steatohepatitis. J Gastroenterol 47:215–225. https://doi.org/10.1007/s00535-012-0527-x
Galántai R, Emody-Kiss B, Somosy Z et al (2011) Does malaoxon play a role in the geno- and cytotoxic effects of malathion on human choriocarcinoma cells? J Environ Sci Health B 46:773–779. https://doi.org/10.1080/03601234.2012.597703
Galloway T, Handy R (2003) Immunotoxicity of organophosphorous pesticides. Ecotoxicology 12:345–363
Geng X, Bo C, Han G, Shao H (2015a) Effects of malathion on testicular spermatogenic function in rats. Zhonghua Lao Dong Wei Sheng Zhi Ye Bing Za Zhi 33:180–185
Geng X, Shao H, Zhang Z et al (2015b) Malathion-induced testicular toxicity is associated with spermatogenic apoptosis and alterations in testicular enzymes and hormone levels in male Wistar rats. Environ Toxicol Pharmacol 39:659–667. https://doi.org/10.1016/j.etap.2015.01.010
Geng X, Bo CX, Shao H (2016) Effects of malathion on testicular enzyme activities and sperm quality of male rats. Zhonghua Lao Dong Wei Sheng Zhi Ye Bing Za Zhi 34:329–332. https://doi.org/10.3760/cma.j.issn.1001-9391.2016.05.003
Ghisari M, Long M, Tabbo A, Bonefeld-Jørgensen EC (2015) Effects of currently used pesticides and their mixtures on the function of thyroid hormone and aryl hydrocarbon receptor in cell culture. Toxicol Appl Pharmacol 284:292–303. https://doi.org/10.1016/j.taap.2015.02.004
Giri S, Prasad SB, Giri A, Sharma GD (2002) Genotoxic effects of malathion: an organophosphorus insecticide, using three mammalian bioassays in vivo. Mutat Res 514:223–231. https://doi.org/10.1016/s1383-5718(01)00341-2
Glass T, Dalvie MA, Holtman Z et al (2018) DNA variants and organophosphate neurotoxicity among emerging farmers in the Western Cape of South Africa. Am J Ind Med 61:11–20. https://doi.org/10.1002/ajim.22790
Goldner WS, Sandler DP, Yu F et al (2013) Hypothyroidism and pesticide use among male private pesticide applicators in the agricultural health study. J Occup Environ Med 55:1171–1178. https://doi.org/10.1097/JOM.0b013e31829b290b
Gunier RB, Bradman A, Harley KG et al (2017) Prenatal residential proximity to agricultural pesticide use and IQ in 7-year-old children. Environ Health Perspect 125:057002. https://doi.org/10.1289/EHP504
Gupta VK, Siddiqi NJ, Ojha AK, Sharma B (2019) Hepatoprotective effect of Aloe vera against cartap- and malathion-induced toxicity in Wistar rats. J Cell Physiol 234:18329–18343. https://doi.org/10.1002/jcp.28466
Guyton KZ, Loomis D, Grosse Y et al (2015) Carcinogenicity of tetrachlorvinphos, parathion, malathion, diazinon, and glyphosate. Lancet Oncol 16:490–491. https://doi.org/10.1016/S1470-2045(15)70134-8
Heyer DB, Meredith RM (2017) Environmental toxicology: sensitive periods of development and neurodevelopmental disorders. Neurotoxicology 58:23–41. https://doi.org/10.1016/j.neuro.2016.10.017
Hohenadel K, Harris SA, McLaughlin JR et al (2011) Exposure to multiple pesticides and risk of non-Hodgkin lymphoma in men from six Canadian provinces. Int J Environ Res Public Health 8:2320–2330. https://doi.org/10.3390/ijerph8062320
Hosokawa M, Maki T, Satoh T (1990) Characterization of molecular-species of liver microsomal carboxylesterases of several animal species and humans. Arch Biochem Biophys 277:219–227. https://doi.org/10.1016/0003-9861(90)90572-G
Hosokawa M, Endo T, Fujisawa M et al (1995) Interindividual variation in carboxylesterase levels in human liver microsomes. Drug Metab Dispos 23:1022–1027
Hosseini SA, Saidijam M, Karimi J et al (2019) Cerium oxide nanoparticle effects on paraoxonase-1 activity and oxidative toxic stress induced by malathion: a potential antioxidant compound, yes or no? Indian J Clin Biochem 34:336–341. https://doi.org/10.1007/s12291-018-0760-z
Hsiao CT, Yang CC, Deng JF et al (1996) Acute pancreatitis following organophosphate intoxication. J Toxicol Clin Toxicol 34:343–347. https://doi.org/10.3109/15563659609013800
Hsu S-S, Jan C-R, Liang W-Z (2019) Uncovering malathion (an organophosphate insecticide) action on Ca2+ signal transduction and investigating the effects of BAPTA-AM (a cell-permeant Ca2+ chelator) on protective responses in glial cells. Pestic Biochem Physiol 157:152–160. https://doi.org/10.1016/j.pestbp.2019.03.015
Hu L, Luo D, Zhou T et al (2017) The association between non-Hodgkin lymphoma and organophosphate pesticides exposure: a meta-analysis. Environ Pollut 231:319–328. https://doi.org/10.1016/j.envpol.2017.08.028
Hyland C, Gunier RB, Metayer C et al (2018) Maternal residential pesticide use and risk of childhood leukemia in Costa Rica. Int J Cancer 143:1295–1304. https://doi.org/10.1002/ijc.31522
Ince S, Arslan-Acaroz D, Demirel HH et al (2017) Taurine alleviates malathion induced lipid peroxidation, oxidative stress, and proinflammatory cytokine gene expressions in rats. Biomed Pharmacother 96:263–268. https://doi.org/10.1016/j.biopha.2017.09.141
Ishihara A, Nishiyama N, Sugiyama S, Yamauchi K (2003) The effect of endocrine disrupting chemicals on thyroid hormone binding to Japanese quail transthyretin and thyroid hormone receptor. Gen Comp Endocrinol 134:36–43. https://doi.org/10.1016/s0016-6480(03)00197-7
Jaga K, Dharmani C (2003) Sources of exposure to and public health implications of organophosphate pesticides. Rev Panam Salud Publica 14:171–185. https://doi.org/10.1590/s1020-49892003000800004
Jamal F, Haque QS, Singh S, Rastogi SK (2016) The influence of organophosphate and carbamate on sperm chromatin and reproductive hormones among pesticide sprayers. Toxicol Ind Health 32:1527–1536. https://doi.org/10.1177/0748233714568175
Johnson VJ, Rosenberg AM, Lee K, Blakley BR (2002) Increased T-lymphocyte dependent antibody production in female SJL/J mice following exposure to commercial grade malathion. Toxicology 170:119–129. https://doi.org/10.1016/s0300-483x(01)00515-7
Jorsaraei SGA, Maliji G, Azadmehr A et al (2014) Immunotoxicity effects of carbaryl in vivo and in vitro. Environ Toxicol Pharmacol 38:838–844. https://doi.org/10.1016/j.etap.2014.09.004
Josse R, Sharanek A, Savary CC, Guillouzo A (2014) Impact of isomalathion on malathion cytotoxicity and genotoxicity in human HepaRG cells. Chem Biol Interact 209:68–76. https://doi.org/10.1016/j.cbi.2013.12.002
Kamanyire R, Karalliedde L (2004) Organophosphate toxicity and occupational exposure. Occup Med - Oxford 54:69–75. https://doi.org/10.1093/occmed/kqh018
Kang E-J, Seok S-J, Lee K-H et al (2009) Factors for determining survival in acute organophosphate poisoning. Korean J Intern Med 24:362–367. https://doi.org/10.3904/kjim.2009.24.4.362
Karami-Mohajeri S, Abdollahi M (2011) Toxic influence of organophosphate, carbamate, and organochlorine pesticides on cellular metabolism of lipids, proteins, and carbohydrates: a systematic review. Hum Exp Toxicol 30:1119–1140. https://doi.org/10.1177/0960327110388959
Karami-Mohajeri S, Hadian MR, Fouladdel S et al (2014) Mechanisms of muscular electrophysiological and mitochondrial dysfunction following exposure to malathion, an organophosphorus pesticide. Hum Exp Toxicol 33:251–263. https://doi.org/10.1177/0960327113493300
Keadtisuke S, Dheranetra W, Fukuto TR (1989) Detection of kidney damage by malathion impurities using a microdissection technique. Toxicol Lett 47:53–59. https://doi.org/10.1016/0378-4274(89)90085-4
Kjeldsen LS, Ghisari M, Bonefeld-Jørgensen EC (2013) Currently used pesticides and their mixtures affect the function of sex hormone receptors and aromatase enzyme activity. Toxicol Appl Pharmacol 272:453–464. https://doi.org/10.1016/j.taap.2013.06.028
Koc ND, Kayhan FE, Sesal C, Muslu MN (2009) Dose-dependent effects of endosulfan and malathion on adult Wistar albino rat ovaries. Pak J Biol Sci 12:498–503
Komori T, Yamane K, Nagayama T et al (1991) A case of delayed myeloneuropathy due to malathion intoxication. No To Shinkei 43:969–974
Krause W, Homola S (1974) Alterations of the seminiferous epithelium and the Leydig cells of the mouse testis after the application of dichlorvos (DDVP). Bull Environ Contam Toxicol 11:429–433. https://doi.org/10.1007/bf01685299
Kundu CR, Roychoudhury S (2009) Malathion-induced sublethal toxicity on the hematology of cricket frog (Fejervarya limnocharis). J Environ Sci Health B 44:673–680. https://doi.org/10.1080/10934520902847794
Kwong T (2002) Organophosphate pesticides: biochemistry and clinical toxicology. Ther Drug Monit 24:144–149
Landrigan PJ, Claudio L, Markowitz SB et al (1999) Pesticides and inner-city children: exposures, risks, and prevention. Environ Health Perspect 107(Suppl 3):431–437. https://doi.org/10.1289/ehp.99107s3431
Lasram MM, Annabi AB, Rezg R et al (2008) Effect of short-time malathion administration on glucose homeostasis in Wistar rat. Pestic Biochem Physiol 92:114–119. https://doi.org/10.1016/j.pestbp.2008.06.006
Lasram MM, Annabi AB, Elj NE et al (2009) Metabolic disorders of acute exposure to malathion in adult Wistar rats. J Hazard Mater 163:1052–1055. https://doi.org/10.1016/j.jhazmat.2008.07.059
Lasram MM, Dhouib IB, Bouzid K et al (2014a) Association of inflammatory response and oxidative injury in the pathogenesis of liver steatosis and insulin resistance following subchronic exposure to malathion in rats. Environ Toxicol Pharmacol 38:542–553. https://doi.org/10.1016/j.etap.2014.08.007
Lasram MM, Lamine AJ, Dhouib IB et al (2014b) Antioxidant and anti-inflammatory effects of N-acetylcysteine against malathion-induced liver damages and immunotoxicity in rats. Life Sci 107:50–58. https://doi.org/10.1016/j.lfs.2014.04.033
Lassiter TL, Ryde IT, Mackillop EA et al (2008) Exposure of neonatal rats to parathion elicits sex-selective reprogramming of metabolism and alters the response to a high-fat diet in adulthood. Environ Health Perspect 116:1456–1462. https://doi.org/10.1289/ehp.11673
LaVerda NL, Goldsmith DF, Alavanja MCR, Hunting KL (2015) Pesticide exposures and body mass index (BMI) of pesticide applicators from the agricultural health study. J Toxicol Environ Health A 78:1255–1276. https://doi.org/10.1080/15287394.2015.1074844
Lerro CC, Koutros S, Andreotti G et al (2015) Organophosphate insecticide use and cancer incidence among spouses of pesticide applicators in the agricultural health study. Occup Environ Med 72:736–744. https://doi.org/10.1136/oemed-2014-102798
Lou-Bonafonte JM, Gabás-Rivera C, Navarro MA, Osada J (2015) PON1 and Mediterranean diet. Nutrients 7:4068–4092. https://doi.org/10.3390/nu7064068
Lu XT, Ma Y, Wang C et al (2012) Cytotoxicity and DNA damage of five organophosphorus pesticides mediated by oxidative stress in PC12 cells and protection by vitamin E. J Environ Sci Health B 47:445–454. https://doi.org/10.1080/03601234.2012.663312
Machera K, Goumenou M, Kapetanakis E et al (2003) Determination of potential dermal and inhalation operator exposure to malathion in greenhouses with the whole body dosimetry method. Ann Occup Hyg 47:61–70. https://doi.org/10.1093/annhyg/mef097
Madrigal-Santillán E, Madrigal-Bujaidar E, Álvarez-González I et al (2014) Review of natural products with hepatoprotective effects. World J Gastroenterol 20:14787–14804. https://doi.org/10.3748/wjg.v20.i40.14787
Masoud L, Vijayasarathy C, Fernandez-Cabezudo M et al (2003) Effect of malathion on apoptosis of murine L929 fibroblasts: a possible mechanism for toxicity in low dose exposure. Toxicology 185:89–102. https://doi.org/10.1016/s0300-483x(02)00596-6
McDuffie HH, Pahwa P, McLaughlin JR et al (2001) Non-Hodgkin’s lymphoma and specific pesticide exposures in men: cross-Canada study of pesticides and health. Cancer Epidemiol Biomark Prev 10:1155–1163
Mehrpour O, Karrari P, Zamani N et al (2014) Occupational exposure to pesticides and consequences on male semen and fertility: a review. Toxicol Lett 230:146–156. https://doi.org/10.1016/j.toxlet.2014.01.029
Messerlian C, Williams PL, Mínguez-Alarcón L et al (2018) Organophosphate flame-retardant metabolite concentrations and pregnancy loss among women conceiving with assisted reproductive technology. Fertil Steril 110:1137–1144.e1. https://doi.org/10.1016/j.fertnstert.2018.06.045
Mileson BE, Chambers JE, Chen WL et al (1998) Common mechanism of toxicity: a case study of organophosphorus pesticides. Toxicol Sci 41:8–20. https://doi.org/10.1006/toxs.1997.2431
Mills PK, Yang R (2005) Breast cancer risk in Hispanic agricultural workers in California. Int J Occup Environ Health 11:123–131. https://doi.org/10.1179/oeh.2005.11.2.123
Mnif W, Hassine AIH, Bouaziz A et al (2011) Effect of endocrine disruptor pesticides: a review. Int J Environ Res Public Health 8:2265–2303. https://doi.org/10.3390/ijerph8062265
Mohammadi H, Karimi G, Rezayat SM et al (2011) Benefit of nanocarrier of magnetic magnesium in rat malathion-induced toxicity and cardiac failure using non-invasive monitoring of electrocardiogram and blood pressure. Toxicol Ind Health 27:417–429. https://doi.org/10.1177/0748233710387634
Mohammadzadeh L, Hosseinzadeh H, Abnous K, Razavi BM (2018) Neuroprotective potential of crocin against malathion-induced motor deficit and neurochemical alterations in rats. Environ Sci Pollut Res Int 25:4904–4914. https://doi.org/10.1007/s11356-017-0842-0
Mohammadzadeh L, Abnous K, Razavi BM, Hosseinzadeh H (2020) Crocin-protected malathion-induced spatial memory deficits by inhibiting TAU protein hyperphosphorylation and antiapoptotic effects. Nutr Neurosci 23:221–236. https://doi.org/10.1080/1028415X.2018.1492772
Moin-Azad Tehrani M-S, Soltaninejad K, Yazdani S et al (2011) Bilateral loculated pleural effusion as a manifestation of acute parenteral organophosphate intoxication: a case report. J Emerg Med 41:630–634. https://doi.org/10.1016/j.jemermed.2010.11.028
Moore PD, Yedjou CG, Tchounwou PB (2010) Malathion-induced oxidative stress, cytotoxicity, and genotoxicity in human liver carcinoma (HepG2) cells. Environ Toxicol 25:221–226. https://doi.org/10.1002/tox.20492
Moore PD, Patlolla AK, Tchounwou PB (2011) Cytogenetic evaluation of malathion-induced toxicity in Sprague-Dawley rats. Mutat Res 725:78–82. https://doi.org/10.1016/j.mrgentox.2011.07.007
Mora JDS, Hurtado DA, Sandoval OLR (2016) Prediction of endocrine system affectation in fisher 344 rats by food intake exposed with malathion, applying Naïve Bayes classifier and genetic algorithms. Int J Prev Med 7:111. https://doi.org/10.4103/2008-7802.190611
Moridi H, Hosseini SA, Shateri H et al (2018) Protective effect of cerium oxide nanoparticle on sperm quality and oxidative damage in malathion-induced testicular toxicity in rats: an experimental study. Int J Reprod Biomed (Yazd) 16:261–266
Moser VC, Simmons JE, Gennings C (2006) Neurotoxicological interactions of a five-pesticide mixture in preweanling rats. Toxicol Sci 92:235–245. https://doi.org/10.1093/toxsci/kfj189
Nambiar MP, Gordon RK, Rezk PE et al (2007) Medical countermeasure against respiratory toxicity and acute lung injury following inhalation exposure to chemical warfare nerve agent VX. Toxicol Appl Pharmacol 219:142–150. https://doi.org/10.1016/j.taap.2006.11.002
Naughton SX, Terry AV (2018) Neurotoxicity in acute and repeated organophosphate exposure. Toxicology 408:101–112. https://doi.org/10.1016/j.tox.2018.08.011
Navarrete-Meneses MP, Salas-Labadía C, Sanabrais-Jiménez M et al (2017) Exposure to the insecticides permethrin and malathion induces leukemia and lymphoma-associated gene aberrations in vitro. Toxicol in Vitro 44:17–26. https://doi.org/10.1016/j.tiv.2017.06.013
Navarrete-Meneses MP, Pedraza-Meléndez AI, Salas-Labadía C et al (2018) Low concentrations of permethrin and malathion induce numerical and structural abnormalities in KMT2A and IGH genes in vitro. J Appl Toxicol 38:1262–1270. https://doi.org/10.1002/jat.3638
Nicholas AH, Vienne M, van den Berghe H (1979) Induction of sister-chromatid exchanges in cultured human cells by an organophosphorous insecticide: malathion. Mutat Res Genet Toxicol 67:167–172. https://doi.org/10.1016/0165-1218(79)90128-9
Ojha A, Gupta YK (2015) Evaluation of genotoxic potential of commonly used organophosphate pesticides in peripheral blood lymphocytes of rats. Hum Exp Toxicol 34:390–400. https://doi.org/10.1177/0960327114537534
Ojha A, Gupta YK (2017) Study of commonly used organophosphate pesticides that induced oxidative stress and apoptosis in peripheral blood lymphocytes of rats. Hum Exp Toxicol 36:1158–1168. https://doi.org/10.1177/0960327116680273
Ojha A, Yaduvanshi SK, Pant SC et al (2013) Evaluation of DNA damage and cytotoxicity induced by three commonly used organophosphate pesticides individually and in mixture, in rat tissues. Environ Toxicol 28:543–552. https://doi.org/10.1002/tox.20748
Omran OM, Omer OH (2015) The effects of alpha-lipoic acid on breast of female albino rats exposed to malathion: histopathological and immunohistochemical study. Pathol Res Pract 211:462–469. https://doi.org/10.1016/j.prp.2015.02.006
Ozsoy AZ, Nursal AF, Karsli MF et al (2016) Protective effect of intravenous lipid emulsion treatment on malathion-induced ovarian toxicity in female rats. Eur Rev Med Pharmacol Sci 20:2425–2434
Penna-Videau S, Bustos-Obregón E, Cermeño-Vivas JR, Chirino D (2012) Malathion affects spermatogenic proliferation in mouse. Int J Morphol 30:1399–1407. https://doi.org/10.4067/S0717-95022012000400023
Pereira EFR, Aracava Y, DeTolla LJ et al (2014) Animal models that best reproduce the clinical manifestations of human intoxication with organophosphorus compounds. J Pharmacol Exp Ther 350:313–321. https://doi.org/10.1124/jpet.114.214932
Petroianu G, Toomes LM, Petroianu A et al (1998) Control of blood pressure, heart rate and haematocrit during high-dose intravenous paraoxon exposure in mini pigs. J Appl Toxicol 18:293–298. https://doi.org/10.1002/(sici)1099-1263(199807/08)18:4<293::aid-jat509>3.0.co;2-p
Pournourmohammadi S, Ostad SN, Azizi E et al (2007) Induction of insulin resistance by malathion: evidence for disrupted islets cells metabolism and mitochondrial dysfunction. Pestic Biochem Physiol 88:346–352. https://doi.org/10.1016/j.pestbp.2007.02.001
Prabhakaran S, Shameem F, Devi KS (1993) Influence of protein deficiency on hexachlorocyclohexane and malathion toxicity in pregnant rats. Vet Hum Toxicol 35:429–433
Primo-Parmo SL, Sorenson RC, Teiber J, Du BNL (1996) The human serum paraoxonase/arylesterase gene (PON1) is one member of a multigene family. Genomics 33:498–507. https://doi.org/10.1006/geno.1996.0225
Raafat N, Abass MA, Salem HM (2012) Malathion exposure and insulin resistance among a group of farmers in Al-Sharkia governorate. Clin Biochem 45:1591–1595. https://doi.org/10.1016/j.clinbiochem.2012.07.108
Ramadan G, El-Beih NM, Ahmed RSA (2017) Aged garlic extract ameliorates immunotoxicity, hematotoxicity and impaired burn-healing in malathion- and carbaryl-treated male albino rats. Environ Toxicol 32:789–798. https://doi.org/10.1002/tox.22279
Ramirez-Vargas MA, Flores-Alfaro E, Uriostegui-Acosta M et al (2018) Effects of exposure to malathion on blood glucose concentration: a meta-analysis. Environ Sci Pollut Res Int 25:3233–3242. https://doi.org/10.1007/s11356-017-0890-5
Ranjbar A, Ghahremani MH, Sharifzadeh M et al (2010) Protection by pentoxifylline of malathion-induced toxic stress and mitochondrial damage in rat brain. Hum Exp Toxicol 29:851–864. https://doi.org/10.1177/0960327110363836
Reddy PH, Beal MF (2008) Amyloid beta, mitochondrial dysfunction and synaptic damage: implications for cognitive decline in aging and Alzheimer’s disease. Trends Mol Med 14:45–53. https://doi.org/10.1016/j.molmed.2007.12.002
Reuber MD (1985) Carcinogenicity and toxicity of malathion and malaoxon. Environ Res 37:119–153. https://doi.org/10.1016/0013-9351(85)90054-4
Réus GZ, Valvassori SS, Nuernberg H et al (2008) DNA damage after acute and chronic treatment with malathion in rats. J Agric Food Chem 56:7560–7565. https://doi.org/10.1021/jf800910q
Rezg R, Mornagui B, Santos JSO et al (2015) Protective effects of caffeic acid against hypothalamic neuropeptides alterations induced by malathion in rat. Environ Sci Pollut Res Int 22:6198–6207. https://doi.org/10.1007/s11356-014-3824-5
Rieger DK, Dos Santos AA, Suñol C, Farina M (2017) Involvement of superoxide in malaoxon-induced toxicity in primary cultures of cortical neurons. J Toxic Environ Health A 80:1106–1115. https://doi.org/10.1080/15287394.2017.1357305
Roberts DM, Aaron CK (2007) Management of acute organophosphorus pesticide poisoning. BMJ 334:629–634. https://doi.org/10.1136/bmj.39134.566979.BE
Rodgers KE (1997) Effects of oral administration of malathion on the course of disease in MRL-lpr mice. J Autoimmun 10:367–373. https://doi.org/10.1006/jaut.1997.0145
Rosas L, Eskenazi B (2008) Pesticides and child neurodevelopment. Curr Opin Pediatr 20:191–197. https://doi.org/10.1097/MOP.0b013e3282f60a7d
Ross J, Chester G, Driver J et al (2008) Comparative evaluation of absorbed dose estimates derived from passive dosimetry measurements to those derived from biological monitoring: validation of exposure monitoring methodologies. J Expo Sci Environ Epidemiol 18:211–230. https://doi.org/10.1038/sj.jes.7500591
Runkle J, Flocks J, Economos J, Dunlop AL (2017) A systematic review of Mancozeb as a reproductive and developmental hazard. Environ Int 99:29–42. https://doi.org/10.1016/j.envint.2016.11.006
Rupa DS, Rita P, Reddy PP, Reddi OS (1988) Screening of chromosomal aberrations and sister chromatid exchanges in peripheral lymphocytes of vegetable garden workers. Hum Toxicol 7:333–336
Saadi L, Lebaili N, Benyoussi M (2008) Exploration of cytotoxic effect of malathion on some rat organs structure. Commun Agric Appl Biol Sci 73:875–881
Saeedi Saravi SS, Amirkhanloo R, Arefidoust A et al (2016) On the effect of minocycline on the depressive-like behavior of mice repeatedly exposed to malathion: interaction between nitric oxide and cholinergic system. Metab Brain Dis 31:549–561. https://doi.org/10.1007/s11011-015-9764-z
Said RS, Badr AM, Nada AS, El-Demerdash E (2014) Sodium selenite treatment restores long-lasting ovarian damage induced by irradiation in rats: impact on oxidative stress and apoptosis. Reprod Toxicol 43:85–93. https://doi.org/10.1016/j.reprotox.2013.11.005
Salama OA, Attia MM, Abdelrazek MAS (2019) Modulatory effects of swimming exercise against malathion induced neurotoxicity in male and female rats. Pestic Biochem Physiol 157:13–18. https://doi.org/10.1016/j.pestbp.2019.01.014
Salas JH, González MM, Noa M et al (2003) Organophosphorus pesticide residues in Mexican commercial pasteurized milk. J Agric Food Chem 51:4468–4471. https://doi.org/10.1021/jf020942i
Salvadori DM, Ribeiro LR, Pereira CA, Beçak W (1988) Cytogenetic effects of malathion insecticide on somatic and germ cells of mice. Mutat Res 204:283–287. https://doi.org/10.1016/0165-1218(88)90101-2
Salvatore AL, Bradman A, Castorina R et al (2008) Occupational behaviors and farmworkers’ pesticide exposure: findings from a study in Monterey County, California. Am J Ind Med 51:782–794. https://doi.org/10.1002/ajim.20622
Sánchez-Santed F, Colomina MT, Herrero Hernández E (2016) Organophosphate pesticide exposure and neurodegeneration. Cortex 74:417–426. https://doi.org/10.1016/j.cortex.2015.10.003
Sanghi R, Pillai MKK, Jayalekshmi TR, Nair A (2003) Organochlorine and organophosphorus pesticide residues in breast milk from Bhopal, Madhya Pradesh, India. Hum Exp Toxicol 22:73–76. https://doi.org/10.1191/0960327103ht321oa
Santos D, Milatovic D, Andrade V et al (2012) The inhibitory effect of manganese on acetylcholinesterase activity enhances oxidative stress and neuroinflammation in the rat brain. Toxicology 292:90–98. https://doi.org/10.1016/j.tox.2011.11.017
Sapbamrer R, Hongsibsong S (2014) Organophosphorus pesticide residues in vegetables from farms, markets, and a supermarket around Kwan Phayao Lake of Northern Thailand. Arch Environ Contam Toxicol 67:60–67. https://doi.org/10.1007/s00244-014-0014-x
Sapbamrer R, Hongsibsong S (2019) Effects of prenatal and postnatal exposure to organophosphate pesticides on child neurodevelopment in different age groups: a systematic review. Environ Sci Pollut Res 26:18267–18290. https://doi.org/10.1007/s11356-019-05126-w
Schang G, Robaire B, Hales BF (2016) Organophosphate flame retardants act as endocrine-disrupting chemicals in MA-10 mouse tumor Leydig cells. Toxicol Sci 150:499–509. https://doi.org/10.1093/toxsci/kfw012
Selmi S, El-Fazaa S, Gharbi N (2012) Oxidative stress and cholinesterase inhibition in plasma, erythrocyte and brain of rats’ pups following lactational exposure to malathion. Environ Toxicol Pharmacol 34:753–760. https://doi.org/10.1016/j.etap.2012.09.012
Selmi S, El-Fazaa S, Gharbi N (2015) Oxidative stress and alteration of biochemical markers in liver and kidney by malathion in rat pups. Toxicol Ind Health 31:783–788. https://doi.org/10.1177/0748233713475507
Selmi S, Rtibi K, Grami D et al (2018) Malathion, an organophosphate insecticide, provokes metabolic, histopathologic and molecular disorders in liver and kidney in prepubertal male mice. Toxicol Rep 5:189–195. https://doi.org/10.1016/j.toxrep.2017.12.021
Seth V, Banerjee BD, Bhattacharya A et al (2001) Pesticide induced alterations in acetylcholine esterase and gamma glutamyl transpeptidase activities and glutathione level in lymphocytes of human poisoning cases. Clin Biochem 34:427–429. https://doi.org/10.1016/s0009-9120(01)00232-6
Shieh P, Jan C-R, Liang W-Z (2019) The protective effects of the antioxidant N-acetylcysteine (NAC) against oxidative stress-associated apoptosis evoked by the organophosphorus insecticide malathion in normal human astrocytes. Toxicology 417:1–14. https://doi.org/10.1016/j.tox.2019.02.004
Shih DM, Gu L, Xia YR et al (1998) Mice lacking serum paraoxonase are susceptible to organophosphate toxicity and atherosclerosis. Nature 394:284–287. https://doi.org/10.1038/28406
Sifakis S, Androutsopoulos VP, Tsatsakis AM, Spandidos DA (2017) Human exposure to endocrine disrupting chemicals: effects on the male and female reproductive systems. Environ Toxicol Pharmacol 51:56–70. https://doi.org/10.1016/j.etap.2017.02.024
Singh S, Sharma N (2000) Neurological syndromes following organophosphate poisoning. Neurol India 48:308–313
Slimen S, Saloua EF, Najoua G (2014) Oxidative stress and cytotoxic potential of anticholinesterase insecticide, malathion in reproductive toxicology of male adolescent mice after acute exposure. Iran J Basic Med Sci 17:522–530
Slotkin TA (2004) Guidelines for developmental neurotoxicity and their impact on organophosphate pesticides: a personal view from an academic perspective. NeuroToxicology 25:631–640. https://doi.org/10.1016/S0161-813X(03)00050-0
Slotkin TA, Oliver CA, Seidler FJ (2005) Critical periods for the role of oxidative stress in the developmental neurotoxicity of chlorpyrifos and terbutaline, alone or in combination. Dev Brain Res 157:172–180. https://doi.org/10.1016/j.devbrainres.2005.04.001
Smith MN, Workman T, McDonald KM et al (2017) Seasonal and occupational trends of five organophosphate pesticides in house dust. J Expo Sci Environ Epidemiol 27:372–378. https://doi.org/10.1038/jes.2016.45
Sozeri B, Gulez N, Aksu G et al (2012) Pesticide-induced scleroderma and early intensive immunosuppressive treatment. Arch Environ Occup Health 67:43–47. https://doi.org/10.1080/19338244.2011.564231
Syng-Ai C, Kumari AL, Khar A (2004) Effect of curcumin on normal and tumor cells: role of glutathione and bcl-2. Mol Cancer Ther 3:1101–1108
Takahashi N, Hashizume M (2014) A systematic review of the influence of occupational organophosphate pesticides exposure on neurological impairment. BMJ Open 4:e004798–e004798. https://doi.org/10.1136/bmjopen-2014-004798
Tchounwou PB, Patlolla AK, Moore CGY and PD (2015) Environmental exposure and health effects associated with malathion toxicity. Toxicity and Hazard of Agrochemicals. https://doi.org/10.5772/60911
Thakur S, Dhiman M, Mantha AK (2018) APE1 modulates cellular responses to organophosphate pesticide-induced oxidative damage in non-small cell lung carcinoma A549 cells. Mol Cell Biochem 441:201–216. https://doi.org/10.1007/s11010-017-3186-7
Trinder M, Bisanz JE, Burton JP, Reid G (2015) Probiotic lactobacilli: a potential prophylactic treatment for reducing pesticide absorption in humans and wildlife. Benef Microbes 6:841–847. https://doi.org/10.3920/BM2015.0022
Tuzcu K, Alp H, Ozgur T et al (2014) Oral intralipid emulsion use: a novel therapeutic approach to pancreatic β-cell injury caused by malathion toxicity in rats. Drug Chem Toxicol 37:261–267. https://doi.org/10.3109/01480545.2013.838780
Ullah S, Li Z, Hasan Z et al (2018) Malathion induced oxidative stress leads to histopathological and biochemical toxicity in the liver of rohu (Labeo rohita, Hamilton) at acute concentration. Ecotoxicol Environ Saf 161:270–280. https://doi.org/10.1016/j.ecoenv.2018.06.002
Uluitu M, Boca A, Petec G et al (1981) The influence of malathion on the brain serotonin and reproductive function in rats. Physiologie 18:167–174
Uysal M, Karaman S (2018) In vivo effects of intravenous lipid emulsion on lung tissue in an experimental model of acute malathion intoxication. Toxicol Ind Health 34:110–118. https://doi.org/10.1177/0748233717748080
Uzun FG, Kalender S, Durak D et al (2009) Malathion-induced testicular toxicity in male rats and the protective effect of vitamins C and E. Food Chem Toxicol 47:1903–1908. https://doi.org/10.1016/j.fct.2009.05.001
Vanova N, Pejchal J, Herman D et al (2018) Oxidative stress in organophosphate poisoning: role of standard antidotal therapy. J Appl Toxicol 38:1058–1070. https://doi.org/10.1002/jat.3605
Varol S, Başarslan SK, Fırat U et al (2015) Detection of borderline dosage of malathion intoxication in a rat’s brain. Eur Rev Med Pharmacol Sci 19:2318–2323
Velmurugan G, Ramprasath T, Swaminathan K et al (2017) Gut microbial degradation of organophosphate insecticides-induces glucose intolerance via gluconeogenesis. Genome Biol 18:8. https://doi.org/10.1186/s13059-016-1134-6
Venkatesan R, Park YU, Ji E et al (2017) Malathion increases apoptotic cell death by inducing lysosomal membrane permeabilization in N2a neuroblastoma cells: a model for neurodegeneration in Alzheimer’s disease. Cell Death Discov 3:17007. https://doi.org/10.1038/cddiscovery.2017.7
Voorhees JR, Rohlman DS, Lein PJ, Pieper AA (2016) Neurotoxicity in preclinical models of occupational exposure to organophosphorus compounds. Front Neurosci 10:590. https://doi.org/10.3389/fnins.2016.00590
Waddell BL, Zahm SH, Baris D et al (2001) Agricultural use of organophosphate pesticides and the risk of non-Hodgkin’s lymphoma among male farmers (United States). Cancer Causes Control 12:509–517. https://doi.org/10.1023/A:1011293208949
Waheed S, Halsall C, Sweetman AJ et al (2017) Pesticides contaminated dust exposure, risk diagnosis and exposure markers in occupational and residential settings of Lahore, Pakistan. Environ Toxicol Pharmacol 56:375–382. https://doi.org/10.1016/j.etap.2017.11.003
Waldron Lechner D, Abdel-Rahman MS (1986) Kinetics of carbaryl and malathion in combination in the rat. J Toxicol Environ Health 18:241–256
Wang P, Wang H-P, Xu M-Y et al (2014) Combined subchronic toxicity of dichlorvos with malathion or pirimicarb in mice liver and serum: a metabonomic study. Food Chem Toxicol 70:222–230. https://doi.org/10.1016/j.fct.2014.05.027
Wu J-C, Lai C-S, Tsai M-L et al (2017) Chemopreventive effect of natural dietary compounds on xenobiotic-induced toxicity. J Food Drug Anal 25:176–186. https://doi.org/10.1016/j.jfda.2016.10.019
Xiong J, Tian L, Qiu Y et al (2018) Evaluation on the thyroid disrupting mechanism of malathion in Fischer rat thyroid follicular cell line FRTL-5. Drug Chem Toxicol 41:501–508. https://doi.org/10.1080/01480545.2017.1397162
Yan J, Xiang B, Wang D et al (2019) Different toxic effects of racemate, enantiomers, and metabolite of malathion on HepG2 cells using high-performance liquid chromatography-quadrupole-time-of-flight-based metabolomics. J Agric Food Chem 67:1784–1794. https://doi.org/10.1021/acs.jafc.8b04536
Yokota K, Fukuda M, Katafuchi R, Okamoto T (2017) Nephrotic syndrome and acute kidney injury induced by malathion toxicity. BMJ Case Rep 2017. https://doi.org/10.1136/bcr-2017-220733
Yu Y, Yang A-M, Zhang J-H et al (2011) Synergistic effect of dichlorvos, dimethoate and malathion mixture on reproduction toxicity in male mice. Zhonghua Yu Fang Yi Xue Za Zhi 45:810–814. https://doi.org/10.3760/cma.j..issn.0253-9624.2011.09.010
Yu Y, Yang A, Zhang J, Hu S (2013) Maternal exposure to the mixture of organophosphorus pesticides induces reproductive dysfunction in the offspring. Environ Toxicol 28:507–515. https://doi.org/10.1002/tox.20741
Zabrodskii PF, Maslyakov VV, Gromov MS (2015) Changes in the function of lymphocytes and cytokine concentration in blood caused by the action of atropine under conditions of acute malathion intoxication. Eksp Klin Farmakol 78:20–23
Zhang X, Wallace AD, Du P et al (2012) DNA methylation alterations in response to pesticide exposure in vitro. Environ Mol Mutagen 53:542–549. https://doi.org/10.1002/em.21718
Zidan NE-HA (2015) Hepato- and nephrotoxicity in male albino rats exposed to malathion and spinosad in stored wheat grains. Acta Biol Hung 66:133–148. https://doi.org/10.1556/018.66.2015.2.1
Funding
The Deanship of Scientific Research at King Saud University funded this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that she has no conflict of interest.
Ethical approval
Not applicable.
Informed consent
Not Applicable.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Badr, A.M. Organophosphate toxicity: updates of malathion potential toxic effects in mammals and potential treatments. Environ Sci Pollut Res 27, 26036–26057 (2020). https://doi.org/10.1007/s11356-020-08937-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-020-08937-4