Abstract
Purpose
Few studies have examined the co-morbidity between insomnia and sleep-disordered breathing in the clinical setting. This study evaluated treatment-seeking insomnia patients and their self-report of sleep breathing complaints.
Methods
A retrospective chart review was conducted on 1,035 consecutive treatment-seeking, chronic insomnia patients who reported insomnia as their primary problem upon seeking care at a private, community-based sleep medical center. Measurements included the insomnia severity index, standard subjective sleep measures as well as rankings, attributions, and self-reports about sleep breathing disorders, problems, and symptoms.
Results
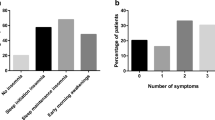
A total of 1,035 adult, treatment-seeking insomnia patients indicated insomnia interfered with daytime functioning, and their average insomnia severity was in the range of a clinically relevant problem: total sleep time (5.50 h, SD = 1.60), sleep efficiency (71.05 %, SD = 18.26), wake time after sleep onset (120.70 min, SD = 92.56), and an insomnia severity index (18.81, SD = 5.09). Of these 1,035 insomnia patients, 42 % also ranked a sleep breathing disorder among their list of reasons for seeking treatment, another 13 % revealed a concern about a sleep breathing problem, and another 26 % reported awareness of sleep breathing symptoms. Only 19 % of this clinical insomnia sample reported no awareness or concerns about sleep breathing disorders, problems, or symptoms. A greater proportion of men than women reported significantly more sleep breathing disorders, problems, or symptoms.
Conclusions
Sleep breathing complaints were extremely common among a large sample of treatment-seeking, self-identified, adult chronic insomnia patients. Prospective prevalence research is needed to corroborate or revise these findings, and polysomnography should be considered in appropriate cohorts to determine the clinical relevance of treatment-seeking chronic insomnia patients' sleep breathing complaints.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Research dating back to the late 1980s demonstrated utility for polysomnography (PSG) in the evaluation of treatment-seeking chronic insomnia patients [1, 2]. Edinger et al. demonstrated at least one third of chronic insomnia patients' sleep tests yielded important objective data [1]. Jacobs et al. demonstrated pertinent objective findings in 49 % of treatment-seeking insomnia patients [2]. Only a small proportion of these patients were diagnosed with sleep apnea, but testing was conducted with thermistor technology which would have severely underestimated the frequency of hypopneas on PSG [3]. Regardless, Edinger noted the potential importance of the findings: “[insomnia] patients showing clinical evidence of possible sleep apnea….should clearly receive a PSG evaluation in order to confirm the clinical diagnosis” [1]. These two studies have been cited for more than two decades to support both the need for testing at-risk insomnia patients with sleep breathing complaints as well as to discourage routine testing of all insomnia patients [4, 5].
Few studies have replicated or expanded upon these earlier works to test for sleep apnea in clinical samples of treatment-seeking insomnia patients or to even screen for sleep breathing symptoms. In a 1999 study by Lichstein et al. [6], individuals ≥59 years of age with primary insomnia symptoms were recruited through media announcements. Of the 386 patients who volunteered for the study, 226 were excluded for medical reasons. Of the remaining 160 patients, 67 (41.9 %) were excluded during telephone and in-person interviews for subjective symptoms suggestive of sleep-disordered breathing. In 2001, Krakow et al.[7] evaluated a consecutive series of 44 crime victims with the combination of insomnia and nightmares that were self-referred in response to media announcements or by rape crisis centers or private therapists. Sleep-disordered breathing (SDB) symptoms were not reported in the study; however, unpublished data revealed 75 % of the sample (33 of 44) reported the presence of at least one SDB symptom (snoring; choking, gasping, or struggling for breath at night; or witnessed cessation of breathing by bed partner). In 2002, Guilleminault et al. looked at a population of community-recruited and sleep clinic-referred postmenopausal women with complaints of primary insomnia without major psychiatric or medical disorders and without symptoms consistent with obstructive sleep apnea (OSA) [8]. Of the 501 patients who passed initial screening and completed an extensive sleep questionnaire, 41 or 8 % of the sample were excluded due to symptoms suggestive of OSA. Last, in 2010, Krakow et al. [9] completed a retrospective chart review of 218 chronic insomniacs presenting to a sleep medical clinic with persistent insomnia complaints despite nightly use of prescription sleep medication. Unpublished data showed that only 60 of the 218 patients did not report SDB symptoms (snoring, choking, gasping, or struggling for breath at night, or witnessed cessation of breathing by bed partner). Thus, 72 % of these insomnia patients reported sleep breathing symptoms. From these four studies, we may surmise that a very wide range of insomnia patients (8 to 75 %) may present with sleep breathing complaints.
Given this wide range, we wanted to conduct a study with a much larger sample of clinical and chronic insomnia patients—seeking treatment at a sleep medical center—to determine their prevalence of sleep breathing symptoms. As part of our ongoing research efforts to examine the relationships between insomnia and sleep-disordered breathing [7, 9–14], the following retrospective case series attempts to shed light on this question by assessing more than a thousand consecutive chronic insomnia patients presenting for treatment at a private, community-based sleep medical center. In future studies, we will evaluate objective data on these patients, whereas this preliminary study is restricted to the subjective data from patient self-reports about their awareness of breathing complaints. We hypothesized that sleep breathing complaints would be common when elicited through various types of questions.
Methods
Informed consent and sample
The study was reviewed and approved by the Los Alamos Medical Center Institutional Review Board. Patients provided consent upon completion of their intake at Maimonides Sleep Arts & Sciences (MSAS) to use their information anonymously for research purposes. Patients at MSAS complete a standard intake set of questionnaires assessing sleep symptoms based on the nosology for sleep disorders in the International Classification of Sleep Disorders [15]. The intake is an online program, and patients must complete all surveys. Once completed, the patient must list and rank their main reasons for seeking treatment.
For this retrospective chart review conducted for the period between March 2004 and February 2010, we examined only those patients who denoted chronic insomnia as their primary or chief complaint for which they were seeking treatment, suffered from insomnia for at least 6 months, and linked insomnia to daytime impairment, thus meeting criteria for a chronic insomnia disorder. The complaint of insomnia was construed in one of two ways: either insomnia was ranked as the first disorder (chief complaint) or insomnia was ranked as the second disorder in combination with nonrestorative sleep ranked as the first disorder. Those not meeting these criteria were excluded.
Once this main insomnia sub-group (group A) was identified, we sub-divided the sample into four additional subgroups. When the patients rank their chief complaint, they also rank other sleep problems or disorders for which they are concerned. Thus, we selected those insomnia patients who also ranked a sleep breathing problem to form group B. Next, for those who did not rank a sleep breathing problem, we reviewed four attribution questions that were completed about their perceptions on sleep breathing, which included: (1) the need to eliminate snoring, (2) awareness of awakenings due to breathing problems at night, (3) the potential need for a sleep breathing machine, and (4) an outright declaration of a sleep breathing problem (despite not ranking SDB as a disorder). Any affirmative endorsement of these factors suggested awareness of or concerns about sleep breathing symptoms (group C). Of the remaining patients, we reviewed their intake for the presence or absence of classic sleep breathing symptoms (snoring, loud snoring, gasping or choking, witnessed apnea) (group D). Once these reviews were completed, we also examined those remaining patients who reported no indications of any type of awareness or concern about sleep breathing symptoms, problems, or disorders (group E). Finally, from the online surveys completed by the patient at intake, information was extracted on standard self-reported sleep measures for insomnia, including sleep onset latency, total sleep time, total time in bed, and wake time after sleep onset from which sleep efficiency was calculated. Total scores on the insomnia severity index were also recorded [16].
All data were analyzed with SPSS version 11.0.1. ANOVA and contingency coefficient analyses were performed for continuous and dichotomous variables, respectively. Cohen's d effect sizes, the standardized mean difference, were calculated from the difference in two means divided by the pooled standard deviation. The differences in proportions test was calculated to determine effect sizes for dichotomous variables. Pearson correlation coefficients were analyzed for relationships among BMI and SDB symptoms. Statistical significance was .05.
Results
Sample characteristics and insomnia severity
The Fig. 1 flow chart shows the original sample comprising 4,355 patients at our sleep center, of which 1,035 or 24 % reported a chief complaint of insomnia as their primary reason for seeking treatment (656, insomnia first; 379, insomnia second with nonrestorative sleep first). The insomnia sample consisted of predominantly female (56.8 %), overweight [BMI mean (SD) = 29.64 (12.07)], Caucasian (63.8 %), married (68.6 %) individuals with bachelor degrees or higher (52.6 %). The chronicity of their insomnia was a mean (SD) of 10.17 ± 9.52 years.
Flow chart of five subgroups, filtered per awareness of insomnia plus sleep breathing disorders, problems, or symptoms. The initial cohort included 4,355 patients of which 3,215 reported no insomnia, leaving 24 % in the main insomnia sub-group. aRanked insomnia #1 or insomnia #2 with nonrestorative sleep #1 on list of chief complaints. bRanked sleep-disordered breathing (SDB) on list of chief complaints. c SDB Attributes include: (1) snoring, (2) breathing-induced awakenings, (3) use of a breathingmachine, and (4) declared sleep breathing problem. d SDB Symptoms include: (1) snoring, (2) loud snoring, (3) choking or gasping, and (4) witnessed apneas
In addition to meeting the criteria for an insomnia disorder, among the entire insomnia sub-group (group A) of 1,035 adult insomnia patients, insomnia severity was consistent with a clinically relevant insomnia problem: total sleep time (5.50 h, SD = 1.60), sleep efficiency (71.05 %, SD = 18.26), wake time after sleep onset (120.70 min, SD = 92.56), and an insomnia severity index (18.81, SD = 5.09) above the conservative cutoff of 15 (Table 1) [16]. Comparing those ranking insomnia first vs ranking insomnia second (when ranking nonrestorative sleep first) demonstrated subjective sleep indices for the nonrestorative group consistent with a clinical insomnia problem: [total sleep time (5.85 h, SD = 1.44), sleep efficiency (74. 57 %, SD = 15.28), wake time after sleep onset (99.80 min, SD = 76.78), and an insomnia severity index (18.04, SD = 4.61)], but which were all significantly (p = .001) less severe than those in the insomnia first group [total sleep time (5.30 h, SD = 1.44), sleep efficiency (69.02 %, SD = 19.49), wake time after sleep onset (132.70 min, SD = 98.58), and an insomnia severity index (19.25, SD = 5.30)]; however, the overall mean effect size between groups was 0.32, indicative of small clinical differences. When comparing men to women, there were no significant differences in subjective sleep indices or total ISI scores.
Presentation of sleep breathing complaints and related effects
From the 1,035 insomnia patients (Fig. 1,group A), the initial sub-division comprised 431 patients (group B) who ranked a sleep breathing disorder. Of the remaining 604 patients, the next sub-group was 135 patients (group C) who endorsed at least one of four attribution questions about sleep breathing problems (snoring, breathing-induced awakenings, use of a breathing machine, or a declared sleep breathing problem), decreasing our sample to 469 patients. Last, we examined these 469 patients for the presence or absence of classic sleep breathing complaints (snoring, loud snoring, choking or gasping, witnessed apneas) and found 272 (group D) reporting one or more symptoms. Thus, our final sub-group of chronic insomnia patients without any awareness of or concerns about sleep breathing symptoms, problems, or disorders comprised 197 patients (group E) or 19 % of the total insomnia sample. In sum, on presentation of 1,035 patients who declared that insomnia was their chief complaint, 81 % exhibited awareness of sleep breathing disorders, problems, or symptoms. Comparing our two types of insomniacs, the nonrestorative sleep first group reported significantly (p = .01) higher levels of awareness of breathing symptoms (snoring, moving from bedroom due to snoring, and witnessed apneas) than the insomnia first group, but effect sizes as measured by difference of proportions were less than 10 %.
Table 1 revealed no significant differences among any of the breathing-delineated subgroups for subjective sleep measures or insomnia severity. As a further analysis, we compared the no-breathing-awareness group (group E) as a reference against each of the other three groups. We found that group E had significantly longer SOL [84.77 (78.06)] than group B [72.70 (65.33), p = .04, d = .17] and group C [68.38 (66.09), p = .05, d = .22]. Group E also had a significantly higher total ISI score [19.36 (5.43)] than group C [18.06 (4.93), p = .03, d = .25] and group D [17.92 (5.05), p = .003, d = .28]. And lastly, group E had a lower SE [69.15 (18.08)] than group C [74.48 (18.22), p = .01, d = .29]. However, the average effect size for these differences as measured with Cohen's d was in the small range (d = 0.24).
Socio-demographic influences on breathing symptoms
Supplemental analyses with socio-demographic variables revealed expected findings for gender. First, there were fewer men than women in the full insomnia sample (group A, 43.2 vs 56.8 %, respectively). The proportion of women in group B was slightly lower than the proportion of men (48.7 vs 51.3 %, respectively) but was higher in the remaining groups and increased significantly (p = .001) in each sub-group from group C (54.1 vs 45.9 %) to group D (61.8 vs 38.2 %) and finally to group E (66.5 vs 33.5 %) consistent with published data showing women report fewer breathing symptoms than men [17]. The proportion of men was significantly greater than that of women endorsing snoring (74.6 vs 68.9 %, p = .03), witnessed apneas (44.5 vs 29.9 %, p = .001), choking, gasping, or struggling for breath (40.4 vs 28.6 %, p = .001), and moving from the bedroom due to snoring (36.0 vs 23.4 %, p = .001). Overall, men endorsed an average of 1.95 SDB symptoms of the four listed while women endorsed an average of 1.50 symptoms (p = .001). There were no significant differences in BMI between men and women in each of the four subgroups, and BMI did not correlate with number of reported breathing symptoms (p = .55).
Discussion
The relationships between chronic insomnia and sleep-disordered breathing have been the subject of recent review articles [18–22]. Evidence suggests insomnia is common in patients with sleep-disordered breathing, while others note a higher than expected prevalence of sleep-disordered breathing among chronic insomniacs. Some researchers have raised the possibility that the relationship is simply an epiphenomenon based on the fact that the two most commonly diagnosed sleep disorders are insomnia and sleep-disordered breathing [23, 24]. Other viewpoints suggest that the relationship represents a strong association in which sleep-disordered breathing may contribute to sleep maintenance insomnia and, more speculatively, insomnia and resultant sleep fragmentation may serve as a substrate for respiratory instability that leads to sleep breathing events [25, 26].
The current study is the first to demonstrate a high prevalence of self-reported sleep breathing complaints, symptoms, or problems in a large clinical sample of 1,035 adult chronic insomnia patients presenting to a sleep medical center for insomnia treatment and who met the criteria for an insomnia disorder. The vast majority of patients (81 %) reported awareness or a concern about sleep breathing problems or symptoms. Although it is unknown whether these patients merit PSG, the numbers suggest that a sizeable proportion needs further workup for potential SDB. Our future investigations to analyze objective data in these patients will clarify the presence or absence of sleep breathing disorders, and this diagnostic information may shed light on the relationship between chronic insomnia and sleep breathing complaints.
Other studies examining this issue on a smaller scale often recruited patients from outside the clinical environment [6, 7]. The data retrieved in these studies were relevant in so far as sleep breathing symptoms were an exclusion category, not the main variable of interest. Yet, these works also showed unexpectedly high rates of sleep breathing disorders even among those without sleep breathing symptoms [6–9]. Thus, our findings probably generalize to other sleep centers that represent community-based, health-insured patients who present for insomnia treatment, albeit our work may not generalize to other types of sleep centers serving different populations. Regardless, the actual proportion of insomnia patients at other centers who report sleep breathing problems or symptoms is unlikely to be small.
Last, the most pressing clinical question raised by this work is whether or not sleep centers routinely inquire about sleep breathing complaints in diverse ways among their chronic insomnia patients. It is essential that sleep clinics utilize multiple ways of eliciting information in order to accurately assess potential sleep breathing complaints in patients presenting with an insomnia disorder [21]. Otherwise, it is conceivable that diagnostic testing for sleep-disordered breathing may be underutilized, because the failure to recognize sleep breathing symptoms in a presenting insomnia patient is likely to steer the treatment plan towards psychological or pharmacological therapy and away from physiological assessments.
The main limitation of this research is that it only provides epidemiological information from subjective reports. More intensive interviews of each individual patient would have yielded greater clarity about the specifics of their insomnia or nonrestorative sleep complaints [27] as well as the potential impact of their sleep breathing complaints on their sleep. Thus, the precise clinical utility of our dataset cannot be determined without completion of a thorough sleep medical workup. Although our findings further demonstrate the frequent co-occurrence of chronic insomnia and sleep breathing symptoms, it does not address issues about the causality of this co-morbidity. Research investigations must not only determine how to explain and treat presenting complaints of sleep breathing symptoms among insomnia patients, but also whether or not sleep breathing symptoms impact insomnia disorders and vice versa. While this study clearly supports the view that sleep breathing symptoms are more common among insomnia patients than previously documented, it remains a question for further study to determine whether or not routine polysomnography in these chronic insomnia patients is warranted.
References
Edinger JD, Hoelscher TJ, Webb MD, Marsh GR, Radtke RA, Erwin CW (1989) Polysomnographic assessment of DIMS: empirical evaluation of its diagnostic value. Sleep 12:315–322
Jacobs EA, Reynolds CF III, Kupfer DJ, Lovin PA, Ehrenpreis AB (1988) The role of polysomnography in the differential diagnosis of chronic insomnia. Am J Psychiatry 145:346–349
Iber C, A-ISCAQS (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester
Cronlein T, Geisler P, Langguth B, Eichhammer P, Jara C, Pieh C, Zulley J, Hajak G (2012) Polysomnography reveals unexpectedly high rates of organic sleep disorders in patients with prediagnosed primary insomnia. Sleep Breath (in press)
Littner M, Hirshkowitz M, Kramer M, Kapen S, Anderson WM, Bailey D, Berry RB, Davila D, Johnson S, Kushida C, Loube DI, Wise M, Woodson BT (2003) Practice parameters for using polysomnography to evaluate insomnia: an update. Sleep 26:754–760
Lichstein KL, Riedel BW, Lester KW, Aquillard RN (1999) Occult sleep apnea in a recruited sample of older adults with insomnia. J Consult Clin Psychol 67:405–410
Krakow B, Melendrez D, Pedersen B, Johnston L, Hollifield M, Germain A, Koss M, Warner TD, Schrader R (2001) Complex insomnia: insomnia and sleep-disordered breathing in a consecutive series of crime victims with nightmares and PTSD. Biol Psychiatry 49:948–953
Guilleminault C, Palombini L, Poyares D, Chowdhuri S (2002) Chronic insomnia, postmenopausal women, and sleep disordered breathing: part 1. Frequency of sleep disordered breathing in a cohort. J Psychosom Res 53:611–615
Krakow B, Ulibarri VA, Romero EA (2010) Patients with treatment-resistant insomnia taking nightly prescription medications for sleep: a retrospective assessment of diagnostic and treatment variables. Prim Care Companion J Clin Psychiatry 12(4)
Krakow B, Melendrez D, Ferreira E, Clark J, Warner TD, Sisley B, Sklar D (2001) Prevalence of insomnia symptoms in patients with sleep-disordered breathing. Chest 120:1923–1929
Krakow B, Melendrez D, Lee SA, Warner TD, Clark JO, Sklar D (2004) Refractory insomnia and sleep-disordered breathing: a pilot study. Sleep Breath 8:15–29
Krakow B (2004) An emerging interdisciplinary sleep medicine perspective on the high prevalence of co-morbid sleep-disordered breathing and insomnia. Sleep Med 5:431–433
Krakow B, Melendrez D, Sisley B, Warner TD, Krakow J, Leahigh L, Lee S (2006) Nasal dilator strip therapy for chronic sleep-maintenance insomnia and symptoms of sleep-disordered breathing: a randomized controlled trial. Sleep Breath 10:16–28
Krakow B, Ulibarri VA, Romero E (2010) Persistent insomnia in chronic hypnotic users presenting to a sleep medical center: a retrospective chart review of 137 consecutive patients. J Nerv Ment Dis 198:734–741
American Academy of Sleep Medicine (2005) International classification of sleep disorders: diagnostic and coding manual, 2nd edn. American Academy of Sleep Medicine, Westchester, pp 51–55
Bastien CH, Vallieres A, Morin CM (2001) Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2:297–307
Larsson LG, Lindberg A, Franklin KA, Lundback B (2003) Gender differences in symptoms related to sleep apnea in a general population and in relation to referral to sleep clinic. Chest 124:204–211
Luyster FS, Buysse DJ, Strollo PJ Jr (2010) Comorbid insomnia and obstructive sleep apnea: challenges for clinical practice and research. J Clin Sleep Med 6:196–204
Wickwire EM, Collop NA (2010) Insomnia and sleep-related breathing disorders. Chest 137:1449–1463
Beneto A, Gomez-Siurana E, Rubio-Sanchez P (2009) Comorbidity between sleep apnea and insomnia. Sleep Med Rev 13:287–293
Al Jawder SE, Bahammam AS (2011) Comorbid insomnia in sleep-related breathing disorders: an under-recognized association. Sleep Breath 16:295–304
Subramanian S, Guntupalli B, Murugan T, Bopparaju S, Chanamolu S, Casturi L, Surani S (2011) Gender and ethnic differences in prevalence of self-reported insomnia among patients with obstructive sleep apnea. Sleep Breath 15:711–715
Krell SB, Kapur VK (2005) Insomnia complaints in patients evaluated for obstructive sleep apnea. Sleep Breath 9:104–110
Lavie P (2007) Insomnia and sleep-disordered breathing. Sleep Med 8(Suppl 4):S21–S25
Krakow B, Melendrez D, Warner TD, Dorin R, Harper R, Hollifield M (2002) To breathe, perchance to sleep: sleep-disordered breathing and chronic insomnia among trauma survivors. Sleep Breath 6:189–202
Series F (2009) Can improving sleep influence sleep-disordered breathing? Drugs 69(Suppl 2):77–91
Ohayon MM (1997) Prevalence of DSM-IV diagnostic criteria of insomnia: distinguishing insomnia related to mental disorders from sleep disorders. J Psychiatr Res 31:333–346
Acknowledgments
This is not an industry-supported study. Dr. Krakow operates six websites providing education and offering products and services for sleep disorder patients, markets and sells three books for sleep disorder patients, owns and operates a commercial sleep center, and is the president of a non-profit sleep research center which has received support from ConAlma, Respironics, GlaxoSmithKlein, and Covidien. He has participated in speaking engagements supported by ResMed and Respironics. Mr. Ulibarri has indicated no financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Krakow, B., Ulibarri, V.A. Prevalence of sleep breathing complaints reported by treatment-seeking chronic insomnia disorder patients on presentation to a sleep medical center: a preliminary report. Sleep Breath 17, 317–322 (2013). https://doi.org/10.1007/s11325-012-0694-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0694-2