Abstract
Objectives
To develop an intermittent hypoxia/reoxygenation (IH/ROX) rabbit carotid artery model and then investigate the inflammation status of rabbit carotid artery endothelium after IH exposure and its relationship with leptin.
Materials and methods
After anesthetization, rabbit’s right common carotid artery was cleared of surrounding tissue with anatomic microscope, cannulated to its distal part and the proximal part was ligated. Preparations were challenged by changing the PO2 of the gas mixture equilibrating the perfusate. Alternate perfusing (2 mL/min) of equilibrated perfusate bubbled with normoxia or hypoxia gas mixtures formed IH/ROX cycles in the right carotid common artery, simulating the pattern of hypoxic episodes seen in obstructive sleep apnea (OSA), or continuous perfusing of hypoxia perfusate to form continuous hypoxia (CH) modes. Sixty adult male New Zealand White rabbits (2.5–3.0 kg) were separated into six groups, ten per group. Groups were: A, intermittent normoxia (IN) group, perfused with perfusion equilibrated with 21% O2 [PO2 about 141 ± 2.87 mmHg] for 15 s and 21% O2 for 1 min 45 s, 60 cycles; B, severe IH group, 5% O2 [PO2 about 35.2 ± 1.27 mmHg] 15 s and 21% O2 1 min 45 s, 60 cycles; C, mild IH group, 10% O2 [PO2 about 54.3 ± 3.31 mmHg] 15 s and 21% O2 1 min 45 s, 60 cycles; D, severe IH+Lep group, protocol was the same with severe IH group; E, CH group, IN for 1 h 45 min and then 5% O2 for 15 min; and F, Lep group, the same with IN group. Right common carotid artery parts distal to the cannula were harvested after exposure, and endothelial cell layers were gotten from longitudinal outspread vessels. Nuclear factor κB (NFκB) DNA binding activities of partial cell layers were measured with electrophoretic mobility shift assay in the IN group, severe IH group, mild IH group, and CH group nuclear extracts. The other part of the cell layers in the IN group, severe IH group, severe IH+Lep group, and Lep group were cultured for 2 h, and during the culture procedure, recombinated human leptin solutions were added to culture dishes of severe IH+Lep group and Lep group (resulted concentration, 10 ng/mL). Enzyme-linked immunosorbent assay was used to analyze medium interleukin-6 (IL-6) concentrations, reverse transcription polymerase chain reaction was used to analyze endothelial cell Ras homology A (RhoA) mRNA expression levels. Statistical analysis was done with SPSS 11.5 software package.
Results
NFκB DNA binding activities were significantly different between groups (F = 112.428, P < 0.001). This activity in the severe IH group (4.27 ± 0.64) was higher than that in the mild IH group (2.33 ± 0.45, P < 0.001), IN group (1.00 ± 0.26, P < 0.001), and CH group (1.15 ± 0.36, P < 0.001). RhoA mRNA expression levels were different in groups (F = 26.634, P < 0.001).This level in the severe IH+Lep group (2.54 ± 0.53) was higher than that in the severe IH group (1.57 ± 0.44, P = 0.002), IN group (1.00 ± 0.31, P < 0.001), and Lep group (1.31 ± 0.30, P < 0.001). IL-6 concentrations were different in groups (F = 79.922, P < 0.001). IL-6 concentration in the severe IH+Lep group (1591.50 ± 179.57 pg/mL) was higher than that in the severe IH group (1217.20 ± 320.62 pg/mL, P = 0.036), IN group (325.40 ± 85.26 pg/mL, P < 0.001), and Lep group (517.40 ± 183.09 pg/mL, P < 0.001).
Conclusions
IH/ROX activated the inflammation pathway significantly in the endothelium, which was more intensive than CH and intensity-dependent. When exposed to both IH/ROX and leptin, inflammation occurs more dramatically. It means that synergic activating roles were performed by IH/ROX and leptin. This study may have a clinical implication that IH can cause endothelial damage through activated inflammation in OSA patients, and if the OSA patients have obesity at the same time, the endothelial damage or the inflammation would be more significant because of elevated leptin level as a synergic factor.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea (OSA), characterized by frequently recurrent intermittent hypoxia/reoxygenation (IH/ROX) as its obvious pathological trait, is clearly associated with an increased risk of cardiovascular disorders, particularly atherosclerosis [1]. On cell culture level, IH/ROX produces reactive oxygen species (ROS), which induce inflammation and damage endothelial cells [2, 3], and consequently complicates atherosclerosis [4].
The interrelationships between obesity and OSA are complex and bidirectional [5]. Significant OSA is present in about 40% of obese individuals, and about 70% of OSA patients are obese [6]. Body mass index (BMI) increase results in the development and progression of OSA, confirmed by the Sleep Heart Health Study, the Wisconsin Sleep Cohort Study, and the Cleveland Family Study [7–9], while weight loss reduces OSA severity in spite of what means they used for losing weight [10, 11].
So, the study on vascular level for whether IH/ROX can cause vascular endothelium inflammation and the relationships with leptin, a main cytokine coded by obesity gene and secreted by adipocytes, especially higher level in obese patients [12, 13], is essential. Leptin, a 167-amino acid peptidic hormone secreted by adipose tissue, acts not only in the arcuate hypothalamus nucleus as a satiety signal, but also in the inflammatory and endothelial systems [14]. It has been proved about the relationship between leptin and obesity that most of obesity patients have an elevated serum leptin level and an energy metabolism disorder because of leptin and its receptor dysfunction [12, 13], and blood levels of leptin were correlated with all measures of adiposity [15]. However, hypoxia is another leptin-inductive factor [16, 17]. So, the study about the cross-reaction between IH/ROX and leptin, the production of obesity gene, can shed light on the relationship of obesity and OSA.
In this study, we developed an IH/ROX rabbit carotid artery model, and then with the de novo model, we investigated the inflammation status of the rabbit carotid artery endothelium after IH exposure and its relationship with leptin. The aim for this study was to investigate the inflammatory status in the rabbit carotid artery endothelium caused by IH/ROX and if leptin can further accelerate this inflammation effects. We think that the results of this study can give some explanations to the pathophysiology of endothelial damage in patients with OSA and obesity at the same time.
Materials and methods
Perfusion system
Visual C++ computer language was used in coding a control program (Breath-Simulating system 1.0) which regulated the delivery system as previously described [2, 3]. Briefly, a personal computer drove singlechip through serial port communicating protocol, and with this system, solid relay was adjusted to modulate a peristaltic pump controlling whether the prefab perfusion with different oxygen partial pressure (PO2) was given or not. The composition of the perfusion medium in 36.5°C was as follows: 125 mM NaCl, 5.3 mM KCl, 1.8 mM CaCl2, 2 mM MgSO4, 1.2 mM NaH2PO4, 25 mM NaHCO3, 10 mM d-glucose, 5 mM sucrose, and pH value was 7.4. The gas mixture we used was produced by Tianjin Liu-fang Gas Limited Company, and this mixture was consisted of O2 in particular concentration, 5% CO2 and balanced N2. Perfusate was continuously bubbled in a custom-made cabin for 30 min to make it saturated with hypoxia or normoxia gas mixture [18]. O2, CO2 partial pressure, and pH value of saturated perfusate were sampled and monitored by oxygen electrode (American Lazar) and blood gas analyzer (Swiss AVL OMNI).
Animal model development
Adult male New Zealand White rabbit (2.5–3.0 kg) was anesthetized with pentobarbitone sodium (20 mg/kg) via an ear vein without muscle relaxant and respirator, and voluntary breathing was reserved with a functional airway. The animal presented with well live status and physiological condition relatively. In supine position, hair was removed from the neck and the right carotid sinus region was exposed. With an anatomic microscope, right carotid arterial bifurcation was identified and cleared of surrounding tissue without touching the left side of the carotid region. The right common carotid artery was cannulated to the distal part and its proximal part was ligated. Preparations were challenged by changing the PO2 of the gas mixture, equilibrating the perfusate. Alternate perfusing (2 mL/min) of equilibrated perfusate bubbled with normoxia or hypoxia gas mixtures formed IH/ROX cycles in the right carotid common artery, simulating the pattern of hypoxic episodes seen in OSA, or with continuous perfusing of hypoxia perfusate to form continuous hypoxia (CH) modes (Fig. 1). The study was approved by the Medical Ethics Committee of the Chinese Medical Association.
The right common carotid artery was cannulated to the distal part and its proximal part was ligated. Preparations were challenged by changing the PO2 of the gas mixture equilibrating the perfusate. Alternate perfusion (2 mL/min) of equilibrated perfusate bubbled with normoxia or hypoxia gas mixtures formed IH/ROX cycles in right carotid common artery, simulating the pattern of hypoxic episodes seen in OSA, or with continuous perfusing hypoxia perfusate to form CH modes
Experimental protocols
Sixty rabbits (2.5–3.0 kg, provided by the Model Animal Center of Radiological Medicine Research Institute, Chinese Academy of Medical Science, license no. SCXK Tianjin 2005-0001) were separated into six groups, ten per group, according to exposure conditions. Groups were: A, intermittent normoxia group (IN group), preparations were perfused with perfusion equilibrated with 21% O2 [PO2 about 141 ± 2.87 mmHg] for 15 s and 21% O2 for 1 min 45 s until 60 cycles; B, severe IH group, 5% O2 [PO2 about 35.2 ± 1.27 mmHg] 15 s and 21% O2 1 min 45 s, 60 cycles; C, mild IH group, 10% O2 [PO2 about 54.3 ± 3.31 mmHg] 15 s and 21% O2 1 min 45 s, 60 cycles; D, severe IH+Lep group, protocol was the same with that in the severe IH group; E, CH group, IN for 1 h 45 min and then 5% O2 for 15 min; and F, Lep group, the same with that in the IN group. Right common carotid artery parts distal to the cannula were harvested after systematic exposures, and endothelial cell layers were gotten with cell-scraper from longitudinal-cut outspread vessels. Endothelial cells scraped from each preparation were divided into two parts: One part was washed twice with ice-cold phosphate-buffered saline (PBS) and the cell suspension was transferred into a centrifuge tube. Cells were collected by centrifugation at 600×g for 5 min at 4°C, and then cytosol extraction reagent A (Active Motif, USA) was added to the cell pellet. The tube was vigorously vortexed to fully resuspend the cell pellet, and then after incubating the tube on ice, cytosol extraction reagent B was added into the tube. The tube was centrifuged for 5 min at maximum speed in a microcentrifuge (∼16,000×g) and the supernatant was removed. The insoluble (pellet) fraction produced in last step, which contains nuclei, was resuspended in ice-cold nuclear extraction reagent (Active Motif, USA). The tube was centrifuged at maximum speed (∼16,000×g) in a microcentrifuge and then the supernatant (nuclear extract) fraction was immediately transferred to a clean prechilled tube; all extracts were stored at −80°C until use. Nuclear protein concentrations were determined with bicinchoninic acid (BCA) protein assay for standardization. Nuclear factor κB (NFκB) DNA binding reaction of nuclear extract was performed with nonradiolabeled electrophoretic mobility shift assay (EMSA, Weiao, China Ningbo) in the IN group, mild IH group, severe IH group, and CH group, four groups totally [Double-stranded oligonucleotide containing the consensus sequence of the binding site for NFκB was 5′-AGTTGAGGGGACTTTCCCAGGC-3′, which was labeled with biotin. Reaction system: labeled probe 0.5 μL; 10X binding solution 1.0 μL; poly(dI:dC)(dI:dC) 1.0 μL; nuclear extract 0.4 μL–0.4 μg; total volume was regulated with distilled water till 10 μL.) The other part of the endothelial cells scraped from each preparation in the IN group, severe IH group, severe IH+Lep group, and Lep group was resuspended with RPMI-1640 medium, and cell concentration was adjusted to 3 × 106/mL. Endothelial cells were transplanted to Petri dishes with 1 mL per well and cultured for 2 h in standard incubator, and during the culture procedure, human recombinant leptin (final concentration 10 ng/mL; Promega) was added to the wells of the severe IH+Lep group and Lep group. Interleukin-6 (IL-6) concentration of the culture medium was measured with enzyme-linked immunosorbent assay kit (ELISA, Jingmei, China Shenzhen). Total RNA was extracted from adherent cells pellet centrifuged after resuspending and PBS washing. Reverse transcription polymerase chain reaction (RT-PCR) was used to analyze endothelial cell Ras homology A (RhoA) mRNA expression levels [RhoA: sense primer, 5′-ATGTGCCCACAGTGTTTGAGAAC-3′, antisense primer, 5′-TCAGTTCGTAAAGACAGGGTTGC-3′; β-actin: sense primer, 5′-GACTACCTCATGAAGATC-3′, antisense primer, 5′-GATCCACATCTGCTGGAA-3′ (Invitrogen); RhoA cDNA product, 345 bp; β-actin cDNA product, 265 bp]. RhoA is a member of RhoGTPase family, and its role was to regulate eukaryotic endothelial permeability [19] with the mechanism that switching between GTP binding (activated) and GDP binding (deactivated) will trigger downstream kinase cascade. Optical density values of RT-PCR and EMSA results were all standardized with related IN group’s results.
Statistical analysis
RT-PCR and EMSA data were standardized with associated IN group’s values, and all data were represented as the mean±SE (\(\bar x \pm s\)) and analyzed with the SPSS 11.5 software package. After one-way analysis of variance (ANOVA) for whole difference, Tamhane’s T2 was used for post hoc analysis.
Results
NFκB DNA binding reactions were significantly different between IN group, mild IH group, severe IH group, and CH group (F = 112.428, P < 0.001). This activity in the severe IH group (4.27 ± 0.64) was higher than in the IN group (1.00 ± 0.26) (standard error = 0.2191, P < 0.001), mild IH group (2.33 ± 0.45) (standard error = 0.2481, P < 0.001), and CH group (1.15 ± 0.36) (standard error = 0.2329, P < 0.001). Mild IH group’s activity was higher than the IN group (standard error = 0.1641, P < 0.001) and CH group (standard error = 0.1821, P < 0.001), and there was no statistical difference between the IN group and CH group (standard error = 0.1401, P = 0.882) (Fig. 2).
NFκB DNA binding reaction of nuclear extract was performed with nonradiolabeled EMSA. NFκB DNA binding reactions of nuclear extract were significantly different between the IN group, mild IH group, severe IH group, and CH group. In this figure, the difference was significant (P < 0.05) between groups without the same symbol
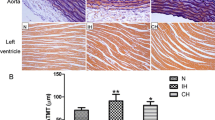
Endothelial cell RhoA mRNA expression levels were different in the IN group, severe IH group, severe IH+Lep group, and Lep group (F = 26.634, P < 0.001). This level in the severe IH+Lep group (2.54 ± 0.53) was higher than in the IN group (1.00 ± 0.31) (standard error = 0.1937, P < 0.001), severe IH group (1.57 ± 0.44) (standard error = 0.2183, P = 0.002), and Lep group (1.31 ± 0.30) (standard error = 0.1930, P < 0.001). Severe IH group’s level was higher than in the IN group (standard error = 0.1710, P = 0.025) but not different with that in the Lep group (standard error = 0.1701, P = 0.613), and there was no difference between the IN group and Lep group (standard error = 0.1373, P = 0.200) (Fig. 3).
Culture medium IL-6 concentrations were different in the IN group, severe IH group, severe IH+Lep group, and Lep group (F = 79.922, P < 0.001). IL-6 concentration in the severe IH+Lep group (4.89 ± 0.55, real value = 1,591.50 ± 179.57 pg/mL) was higher than in the IN group (1.00 ± 0.26, real value = 325.40 ± 85.26 pg/mL) (standard error = 0.1931, P < 0.001), severe IH group (3.74 ± 0.99, real value = 1217.20 ± 320.62 pg/mL) (standard error = 0.3572, P = 0.036), and Lep group (1.59 ± 0.56, real value = 517.40 ± 183.09 pg/mL) (standard error = 0.2491, P < 0.001). Severe IH group’s IL-6 concentration was higher than the IN group (standard error = 0.3225, P < 0.001) and Lep group (standard error = 0.3589, P < 0.001), and there was no difference between the IN group and Lep group (standard error = 0.1963, P = 0.060) (Fig. 4).
Discussion
Atherosclerosis evolves from the activation of the inflammatory cascade [20], and the inflammation in the endothelium would result in endothelial layer damage and more permeability, as included in the pathologic basis of atherosclerosis during which NFκB acts the key role and its binding activity is the initiative factor [21]. IH induces vascular inflammation and pathology by activating the NFκB pathway [22]. Activated NFκB translocates into the nucleus, will bind to the DNA promoter in the reaction element, and regulate the transactivation of downstream proinflammatory genes which will produce proinflammatory proteins like IL-6. These chemical reactions will result in dramatic inflammation in the endothelium and initiate atherosclerosis procedure [23, 24]. In this study, total hypoxia duration (severe IH group, 15 s × 60 cycles = 15 min; CH, 15 min), total exposure duration, and hypoxia intensity (both 2 h, both 5% PO2) were the same between the severe IH group and CH group, but NFκB DNA binding activity in the severe IH group, even in the mild IH group, was greater than that in the CH group, and there was no statistical difference between the CH group and IN group about this binding activity. This is evidence that 15 min of CH perfusion is not necessary to activate the endothelial inflammatory pathway at our rabbit common carotid artery; however, 15 min in total of IH/ROX perfusion activates inflammatory reaction significantly. This kind of activation is intensity-dependent, more intensity of hypoxia, more significant in activation. What makes IH more effective in activating NFκB than CH? The feature that distinguishes IH from CH is the intervening periods of normoxia. In CH, the mitochondria consume almost all of the O2, and rapid stabilization of hypoxia-inducible factor-1 (HIF-1) occurs, which leads to increased activation of the adaptive pathway [25]. In IH/ROX, the extent of hypoxia is not sufficient to allow HIF-1 stabilization; however, possibly through mitochondrial dysfunction induced by ROX, it results in oxidative stress and then inflammatory stimulation which activates NFκB, with the downstream consequence of intensity-dependent activation of the inflammatory pathway that depends on NFκB translocating into the nucleus [2, 3].
Leptin is a peripheral inflammatory cytokine-like hormone that causes atherosclerosis, a mechanism that needs a long period of time [26]. But exposing scraped endothelial cells to leptin purely for 2 h cannot cause significant RhoA and IL-6 changing, while IH/ROX exposure activates RhoA transcription and then produces inflammatory proteins like IL-6 through translation. However, when exposing to both IH/ROX and leptin, inflammation occurs more dramatically, which means that synergic activating roles were performed by IH/ROX and leptin. Vascular endothelium damage and increased permeability are extremely correlated with inflammatory factors activating RhoA [27]. Activated RhoA participates filament actin remodeling and dynamic regulating [28], involves in the structure of lamellipodia, membrane ruffles, and cytoskeleton [29] and stresses endothelial cells, all of which are involved in the formation of arteriosclerosis [30]. Activated RhoA anastoles endothelial cells and increases cell permeability, making it more feasible for inflammatory cells, like leukocyte, to pass through the endothelium barrier when it combines with elevated adhesive capability caused by cell’s IH exposure [2, 3]. So, most of the needed pathologic basis for arteriosclerosis like inflammation, increased adherent leukocytes, and more permeability is available. This study may have a clinical implication that IH can cause endothelial damage through activated inflammation in OSA patients, and if the OSA patients have obesity at the same time, the endothelial damage or the inflammation would be more significant because of elevated leptin level as a synergic factor.
References
McNicholas WT, Bonsignore MR, Management Committee of EU COST ACTION B26 (2007) Sleep apnoea as an independent risk factor for cardiovascular disease: current evidence, basic mechanisms and research priorities. Eur Respir J 29:156–178
Feng J, Chen BY, Guo MN, Cao J, Zhao HY, Liang DC, Zuo AJ (2007) Interleukin-6 and tumor necrosis factor-alpha levels of endothelial cells in different hypoxia modes: in vitro experiment. Zhonghua Yi Xue Za Zhi 87:774–777
Feng J, Chen BY, Guo MN, Cao J, Zhao HY, Liang DC, Zuo AJ (2007) Changes of nuclear factor-kappaB and intercellular adhesion molecule-1 in endothelial cells exposed to various intermittent hypoxia. Zhonghua Jie He He Hu Xi Za Zhi 30:202–206
Shamsuzzaman AS, Gersh BJ, Somers VK (2003) Obstructive sleep apnea: implications for cardiac and vascular disease. JAMA 290:1906–1914
Punjabi NM, Polotsky VY (2005) Disorders of glucose metabolism in sleep apnea. J Appl Physiol 99:1998–2007
Vgontzas AN, Tan TL, Bixler EO, Martin LF, Shubert D, Kales A (1994) Sleep apnea and sleep disruption in obese patients. Arch Intern Med 154:1705–1711
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J (2000) Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA 284:3015–3021
Newman AB, Foster G, Givelber R, Nieto FJ, Redline S, Young T (2005) Progression and regression of sleep-disordered breathing with changes in weight: the Sleep Heart Health Study. Arch Intern Med 165:2408–2413
Tishler PV, Larkin EK, Schluchter MD, Redline S (2003) Incidence of sleep-disordered breathing in an urban adult population: the relative importance of risk factors in the development of sleep-disordered breathing. JAMA 289:2230–2237
Fritscher LG, Mottin CC, Canani S, Chatkin JM (2007) Obesity and obstructive sleep apnea–hypopnea syndrome: the impact of bariatric surgery. Obes Surg 17:95–99
Grunstein RR, Stenlöf K, Hedner JA, Peltonen M, Karason K, Sjöström L (2007) Two year reduction in sleep apnea symptoms and associated diabetes incidence after weight loss in severe obesity. Sleep 30:703–710
Münzberg H, Björnholm M, Bates SH, Myers MG Jr (2005) Leptin receptor action and mechanisms of leptin resistance. Cell Mol Life Sci 62:642–652
Cinaz P, Bideci A, Camurdan MO, Güven A, Gönen S (2005) Leptin and soluble leptin receptor levels in obese children in fasting and satiety states. J Pediatr Endocrinol Metab 18:303–307
Fouillioux C, Contreras F, Lares M, Cano R, Leal E, Arraiz N, Bermúdez V, Velasco M (2008) Metabolic and hemodynamic markers of endothelial dysfunction in patients with hypertension and patients with type 2 diabetes during the cold pressor test. Am J Ther 15:389–396
Kim K, Valentine RJ, Shin Y, Gong K (2008) Associations of visceral adiposity and exercise participation with C-reactive protein, insulin resistance, and endothelial dysfunction in Korean healthy adults. Metabolism 57:1181–1189
Grosfeld A, Andre J, Hauguel-De Mouzon S, Berra E, Pouyssegur J, Guerre-Millo M (2002) Hypoxia-inducible factor transactivates the human leptin gene promoter. J Biol Chem 277:42953–42957
Meissner U, Hänisch C, Ostreicher I, Knerr I, Hofbauer KH, Blum WF, Allabauer I, Rascher W, Dötsch J (2005) Differential regulation of leptin synthesis in rats during short-term hypoxia and short-term carbon monoxide inhalation. Endocrinology 146:215–220
Cummings KJ, Wilson RJ (2005) Time-dependent modulation of carotid body afferent activity during and after intermittent hypoxia. Am J Physiol Regul Integr Comp Physiol 288:R1571–R1580
Etienne-Manneville S, Hall A (2002) Rho GTPase in cell biology. Nature 420:629–635
Yamauchi M, Tamaki S, Tomoda K, Yoshikawa M, Fukuoka A, Makinodan K, Koyama N, Suzuki T, Kimura H (2006) Evidence for activation of nuclear factor kappaB in obstructive sleep apnea. Sleep Breath 10:189–193
Williams A, Scharf SM (2007) Obstructive sleep apnea, cardiovascular disease, and inflammation—is NF-kappaB the key? Sleep Breath 11:69–76
Greenberg H, Ye X, Wilson D, Htoo AK, Hendersen T, Liu SF (2006) Chronic intermittent hypoxia activates nuclear factor-kappaB in cardiovascular tissues in vivo. Biochem Biophys Res Commun 343:591–596
Lentsch AB, Ward PA (2000) The NFkappaBb/IkappaB system in acute inflammation. Arch Immunol Ther Exp (Warsz) 48:59–63
Savransky V, Nanayakkara A, Vivero A, Li J, Bevans S, Smith PL, Torbenson MS, Polotsky VY (2007) Chronic intermittent hypoxia predisposes to liver injury. Hepatology 45:1007–1013
Schofield CJ, Ratcliffe PJ (2004) Oxygen sensing by HIF hydroxylases. Nat Rev Mol Cell Biol 5:343–354
Matarese G, Mantzoros C, La Cava A (2007) Leptin and adipocytokines: bridging the gap between immunity and atherosclerosis. Curr Pharm Des 13:3676–3680
Wójciak-Stothard B, Potempa S, Eichholtz T, Ridley AJ (2001) Rho and Rac but not Cdc42 regulate endothelial cell permeability. J Cell Sci 114:1343–1355
Liu HW, Halayko AJ, Fernandes DJ, Harmon GS, McCauley JA, Kocieniewski P, McConville J, Fu Y, Forsythe SM, Kogut P, Bellam S, Dowell M, Churchill J, Lesso H, Kassiri K, Mitchell RW, Hershenson MB, Camoretti-Mercado B, Solway J (2003) The RhoA/Rho kinase pathway regulates nuclear localization of serum response factor. Am J Respir Cell Mol Biol 29:39–47
Wettschureck N, Offermanns S (2002) Rho/Rho kinase mediated signaling in physiology and pathophysiology. J Mol Med 80:629–638
Bishop AL, Hall A (2000) Rho GTPases and their effector proteins. Biochem J 348(Pt 2):241–255
Acknowledgements
This study was supported by grants from the National Natural Science Foundation of China (no. 30800507).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Feng, J., Chen, By., Cui, Ly. et al. Inflammation status of rabbit carotid artery model endothelium during intermittent hypoxia exposure and its relationship with leptin. Sleep Breath 13, 277–283 (2009). https://doi.org/10.1007/s11325-009-0246-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-009-0246-6