Abstract
Purpose
Obstructive sleep apnea syndrome (OSAS) has been recognized as an important risk factor for cardiovascular morbidity and mortality. However, the underlying mechanisms are poorly understood. Present study aimed to investigate the role of NF-κB-dependent inflammation pathways in pathophysiological responses of cardiovascular system in OSAS.
Methods
Thirty male specific pathogen-free (SPF) Sprague-Dawley rats were randomly assigned to normoxia (N) group, continual hypoxia (CH) group, and intermittent hypoxia (IH) group (n = 10) and were exposed to N (21 % O2), CH (8 % O2), or IH (6–11 % O2 for 10 s and 21 % O2 for 80 s in every 90 s) for 8 h/day for 35 days. The hemodynamic and pathomorphologic effects of IH and CH exposure were investigated as well as the expression of NF-κB-dependent inflammation factors.
Results
Chronic IH or CH significantly increased mean pulmonary arterial pressure (mPAP) in rats, while no significant changes occurred in mean carotid arterial pressure (mCAP). The ratio of right ventricle (RV) to left ventricle (LV) + septum (S) was significantly increased by both IH and CH, suggesting RV hypertrophy was induced by IH or CH. Elastic fiber staining showed an irregular pattern of elastic fiber distribution after hypoxia, and aortic tunica media thickness was increased. Both chronic IH and CH upregulated the expressions of transcription factor NF-κB and related pro-inflammatory cytokines and adhesion molecules.
Conclusions
The current study expands our understanding that both IH and CH could activate the expression of NF-κB and related inflammatory factors as well as cause pathophysiologic damage to the cardiovascular system in OSAS. All these results provide further support to an emerging hypothesis that activation of NF-κB-dependent inflammation may play a central role in the pathophysiology of cardiovascular dysfunction in OSAS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea syndrome (OSAS) is one of the most common public health problems, characterized by frequently recurrent intermittent hypoxia/reoxygenation as the obvious pathological trait, and affects an increasing number of population in the both developed and developing countries all around the world [1]. Accumulating evidences have indicated that OSAS is clearly associated with an increased risk of cardiovascular disorders and is an important risk factor for cardiovascular morbidity and mortality [2]. The major contributing factor to OSAS-associated cardiovascular disorders is thought to be exposure to intermittent hypoxia (IH), which in turn results in oxidative stress, inflammation, endothelial dysfunction, and hypertension [3]. These proposed mechanisms have been drawn from clinical studies and basic research in both animal and human models of IH.
The IH is responsible for many of the cardiovascular consequences of OSAS [4], and a greater understanding of the cellular response to IH and reoxygenation may provide insight into pathophysiological pathways in OSAS [5]. The experimental animal and human models of acute and chronic IH have been developed to evaluate potential mechanisms for the association between OSAS and cardiovascular disease. Murine models may be particularly useful to examine how IH causes cardiovascular dysfunction. Recurrent short cycles of normoxia-hypoxia, when administered to rats for 35 days, allow examination of the chronic cardiovascular response to IH patterned after the episodic desaturation in humans with sleep apnea [6]. Exposure of mouse to acute or chronic IH causes systemic hypertension [7] and systemic and vascular inflammation [8–10, 5]. However, the potential mechanism by which intermittent hypoxia leads to cardiovascular disease in OSAS is still unknown.
Previous evidences suggest that OSAS appears to be associated with systemic inflammation, and OSAS should be considered as a chronic and low-grade systemic inflammatory disease [11, 12]. IH is thought to cause vessel inflammation and is hypothesized to upregulate transcription factor production and adhesion molecule expression, which can aid in the production of reactive oxygen species (ROS) and exacerbate endothelial dysfunction [3]. However, the precise mechanisms through which OSAS promotes systemic inflammation have not been fully explored.
As a pivotal transcription factor in chronic inflammatory diseases, nuclear factor-kappa B (NF-κB) appears to play a key role in mediating the inflammatory and cardiovascular consequences of OSAS [13]. The experimental repetitive hypoxia/reoxygenation that mimics OSAS activates NF-κB-dependent inflammatory pathways [9, 5]. Patients with OSAS had increased NF-κB activities [14], as well as elevated serum levels of NF-κB-dependent pro-inflammatory cytokine and adhesion molecules, such as tumor necrosis factor-α (TNF-α) [15], monocyte chemotactic protein-1 (MCP-1) [16], vascular cell adhesion molecule-1 (VCAM-1) [14], and regulated upon activation normal T cell expressed and secreted factor (RANTES) [17]. However, despite all this evidence, the pathophysiologic events orchestrating the activation of NF-κB-dependent pathway that leads to cardiovascular dysfunction remain largely unexplored. The present study aimed to investigate the effects of chronic IH on the cardiovascular dysfunction and the NF-κB-dependent pathways in rats.
Materials and methods
Animals
Thirty male specific pathogen-free (SPF) Sprague-Dawley (SD) rats, weighed 180–220 g, were obtained from the experimental animal center of Wenzhou Medical College, Wenzhou, Zhejiang, China, and were randomly assigned to three groups: normoxia (N) group, continual hypoxia (CH) group, and intermittent hypoxia (IH) group (n = 10). Rats were housed in controlled conditions and provided with standard rat chow. All animal care and procedures were approved by the Ethics Committee of Wenzhou Medical University.
Continuous and intermittent hypoxia protocol
Animals were exposed to normoxic, intermittent, or continual hypoxic conditions according to group destinations. Briefly, rats were housed in customized steel chambers equipped with air control to deliver an intermittent or continuous hypoxic stimulus. An automated nitrogen/oxygen gas delivery system, provided by Scientific Research Center of Wenzhou Medical College, was used to maintain hypoxia/reoxygenation or continuous hypoxia. IH rat chambers were flushed with nitrogen to rapidly achieve hypoxia (a nadir of 6–11 % O2), stabilized at that level for 10 s, and then infused with oxygen to restore normoxia (21 % O2). The cycle was repeated every 90 s for 8 h/day (from 9:00 to 17:00) during the animals’ diurnal sleep period for 35 days using a computer-controlled system. Rats in the CH chambers and N chambers were exposed to similar handling except that O2 concentrations were continuously maintained at 8 and 21 %, at approximately the same liter flow, respectively, which simulated the same noise and airflow disturbance. Anhydrous calcium chloride and sodium hydroxide was used for water vapor absorption and carbon dioxide absorption, respectively.
Hemodynamic assessment and pathomorphologic analysis
After 35 days of exposure, the rats were weighed and anesthetized by intraperitoneal injection of 5 % chloral hydrate (400 mg/kg body weight), and a polyethylene catheter was slowly inserted into the pulmonary artery through the right jugular vein. The mean pulmonary arterial pressure (mPAP) was then recorded. At the meantime, the mean carotid arterial pressure (mCAP) was also recorded via a polyethylene catheter inserted into the carotid artery.
Next, the heart was dissected out of the chest cavity immediately after the animal was killed. After removal of the atria, the free wall of the right ventricle was carefully dissected from the remainder of the heart. The right ventricle (RV), left ventricle (LV), and septum (S) were weighed individually for each rat. The RV/(LV + S) ratio was calculated as an index of RV hypertrophy (RVHI) [18].
Elastic fiber staining
The aorta and left ventricle of each rat were separated and fixed in 4 % paraformaldehyde for 24 h. The samples were embedded in paraffin and cut in 4 μm cross sections. The elastic fiber in the aorta and left ventricular tissues were stained, and one aorta and left ventricle sections per animal were used for analysis. After deparaffinization, sections were oxidized with potassium permanganate, oxalic acid-bleached for 1–2 min, followed by ethanol dehydration, and then elastic fibers were stained for about 1–2 h (Brilliant Green and Ponceau Red, Shanghai Source Biological Technology Co., Ltd., Shanghai, China). Stained cross sections were captured on a Leica microscope, and the tunica media thickness of aorta (ATMT) was determined.
Enzyme-linked immunosorbent assay
After the hemodynamic data were recorded, blood samples were collected from the right jugular vein. Serum level of C-reaction protein (CRP), NF-κB, TNF-α, MCP-1, VCAM-1, and RANTES were detected using commercially available enzyme-linked immunosorbent assay (ELISA) kits (Shanghai Source Biological Technology Co., Ltd., Shanghai, China) according to the manufacturer’s directions.
Immunohistochemical staining
Additional aortic and left ventricular sections were processed as described above and blocked at room temperature followed by incubation with rabbit anti-rat NF-κB p65 antibody (1:50, Abcam, UK) and rabbit anti-rat MCP-1 antibody (1:50, Abcam, UK) diluted in PBS containing 5 % of bovine serum albumin (BSA), respectively, and then incubated with horse reddish peroxidase (HRP)-labeled second antibodies after being washed by PBS. The aortic and left ventricular specimens, incubated with 5 % BSA to replace the specific primary antibody, served as negative controls. Immune reaction was visualized using 3,30-diaminobenzidine (DAB). Five fields of vision were randomly selected from each section for analyses. The expressions of NF-κB and MCP-1 were quantified by Image Pro Plus 6.0 (Media Cybernetics, Bethesda, MD, USA) and that in N group were set as 1 to indicate the basal level.
Statistical analyses
All data were expressed as mean ± standard deviation (SD). All statistical analyses were performed with SPSS, version 17.0 (SPSS Inc., Chicago, IL, USA). Statistical tests for distribution (QQ plots) were performed. Comparison between the groups was performed by one-way analysis of variance (ANOVA). A level of P < 0.05 was considered as statistically significant; a level of P < 0.01 as highly significant.
Results
The hemodynamic and pathomorphologic effects of chronic IH or CH
All data were shown to be normally distributed by QQ plot analysis. After 35 days of hypoxia, the mean pulmonary arterial pressure (mPAP) in both groups were significantly elevated when compared with the N group (P = 0.00 and 0.01, respectively, F = 10.94, Table 1). The mPAP in the IH group was higher than that in the CH group, although the difference did not reach the statistical significance (P = 0.29). However, the variation tendency of mean carotid arterial pressure (mCAP) among groups was quite different from that of mPAP. The mCAP were slightly higher in N group than in either IH or CH group, and there was no distinct difference of the mCAP between each group (P = 0.93 and 0.29, respectively, F = 1.31, Table 1).
The RV/(LV + S) ratio was used as an index for RV hypertrophy (RVHI). As shown in Table 1, hypoxia exposure caused RV hypertrophy. RVHI in IH and CH groups were statistically higher than that in N group (P = 0.03 and P = 0.02 respectively, F = 5.56). No significant difference was found between the IH and CH groups (P = 0.97).
Effects of chronic IH and CH on the aorta and left ventricle
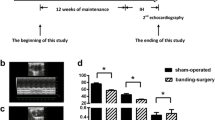
Elastic fiber staining showed obvious changes in the elastic fiber structure of the aorta and left ventricle (Fig. 1). After exposure to hypoxia for 35 days, the aorta in the IH and CH group showed an irregular elastic fiber pattern of distribution compared with the N group, and elastic fibers in the aorta were discontinued and disordered (Fig. 1a). Meanwhile, the left ventricle in the IH and CH groups showed some pathological alterations of the left ventricular muscle cells, which were swollen and arranged irregularly (Fig. 1a). The thicknesses of the aortic tunica media were also measured and were found to be significantly increased in IH and CH groups, when compared with the N group (P = 0.004 and P = 0.01, respectively, Fig. 1b). On the other hand, the aortic tunica media thickness was similar between the IH and CH groups (P = 0.24).
Effects of chronic hypoxia (CH) and intermittent hypoxia (IH) on the aorta and left ventricle. Elastic fiber staining of the aorta and left ventricle after the chronic IH and CH (a); the thicknesses of the aortic tunica media (ATMT) were found to be significantly increased in IH and CH groups (b); and the value in the IH group was lower than that of CH group although the difference did not reach statistical significance. N normoxia, IH intermittent hypoxia, CH continual hypoxia. *P < 0.05, **P < 0.01 vs the N group
Effect of chronic IH and CH on serum inflammatory factors
To investigate the influence of hypoxia and hypoxia/reoxygenation on systemic inflammation, serum levels of CRP, NF-κB, TNF-α, MCP-1, VCAM-1, and RANTES were detected using ELISA method. Compared with normoxia, hypoxia notably increased the serum levels of transcript factor NF-κB and other aforementioned inflammatory factors (Fig. 2). In the IH group, CRP, NF-κB, MCP-1, and RANTES levels showed statistically significant differences (P < 0.01), and TNF-α and VCAM-1 showed statistical differences (P < 0.05), as compared with the N group. Whereas, in the CH group, the increase in serum inflammatory factor levels had statistical differences (P < 0.05), except that for RANTES (P = 0.213). However, there was no significant difference in the serum inflammatory factor levels between the IH and CH groups.
ELISA analysis of the serum levels of inflammatory factors, including CRP, NF-κB, TNF-α, MCP-1, VCAM-1, and RANTES, after chronic IH or CH. ELISA enzyme-linked immunosorbent assay, CRP C-reaction protein, NF-κB nuclear factor-kappa B, TNF-α tumor necrosis factor-α, MCP-1 monocyte chemotactic protein-1, VCAM-1 vascular cell adhesion molecule-1, RANTES regulated upon activation normal T cell expressed and secreted factor, N normoxia, IH intermittent hypoxia, CH continual hypoxia. *P < 0.05, **P < 0.01 ***p < 0.001 vs the N group
Effects of chronic IH and CH on NF-κB and MCP-1 in the aorta and left ventricle
The expressions of NF-κB (Fig. 3) and MCP-1 (Fig. 4) in the aorta and left ventricle were determined immunohistochemically. In the IH and CH groups, positive immunohistochemical staining of NF-κB and MCP-1 showed dark brown particle sediment, as well as the blue-stained nucleus of the smooth muscle cells that distributed loosely and irregularly in the aorta and left ventricle (Figs. 3 and 4). By contrast, there were low NF-κB and MCP-1 expressions in the N group without hypoxia exposure. Both NF-κB and MCP-1 expressions were upregulated by chronic IH or CH in the aorta and left ventricle (Figs. 3 and 4b).
Immunohistochemical analysis of NF-κB expressions in the aorta and left ventricle after chronic IH or CH (a), and the expressions of NF-κB were showed to be upregulated by IH or CH exposure (b). NF-κB nuclear factor-kappa B, N normoxia, IH intermittent hypoxia, CH continual hypoxia. *P < 0.05 vs the N group
Immunohistochemical analysis of MCP-1 expressions in the aorta and left ventricle after chronic IH or CH (a), and the expressions of MCP-1 were showed to be upregulated by IH or CH exposure (b). MCP-1 monocyte chemotactic protein-1, N normoxia, IH intermittent hypoxia, CH continual hypoxia. *P < 0.05, **P < 0.01 vs the N group
Discussions
Previous studies evidenced that even small increase in blood pressure is associated with significant increases in cardiovascular morbidity and mortality, and sleep-related diseases that induce increased blood pressure would be anticipated to substantially affect cardiovascular risk [19]. The results of our study showed that exposure of SD rats to chronic IH or CH for 35 days stimulated the changes in cardiopulmonary hemodynamics and morphology of the RV. The mPAP in our OSAS rat models was significantly increased by either IH or CH, while mCAP was not significantly different between normoxic group and hypoxic groups, corroborating the results of previous researches, which suggested pulmonary hypertension developed by 4 weeks of chronic hypoxia [20]. In addition, the RV/(LV/S) ratio of hypoxia groups was also increased significantly compared with the normal oxygen control group, indicating the existence of RV hypertrophy induced by chronic IH or CH. This observation is in partial agreement with the previous studies, which reported significant increases in the mPAP, and RV hypertrophy in hypoxia rats when compared with the normoxia ones [21, 22]. Furthermore, we also found the obvious changes in the elastic fiber structure of the aorta and left ventricle after 35 days of continuous or intermittent hypoxia. The thicknesses of the aortic tunica media were significantly increased by IH or CH, consistent with previous results, which indicated that patients with OSAS have a significantly increased intima-media thickness compared with matched controls [23]. All the above results showed evidence that suggested rat model of OSAS with cardiovascular complication was successfully established, and both IH and CH can result in the similar effects on cardiopulmonary hemodynamics and morphology of the RV.
The pathogenesis of cardiovascular disease in OSAS is not yet completely understood and is thought to be multifactorial in origin [24]. Increasing evidence suggests that OSAS is a systemic inflammatory disease, and inflammatory processes play a pivotal role in the pathogenesis of cardiovascular disease in OSA [25, 10]. The increased levels of inflammatory cytokines, adhesion molecules, and activation of circulating neutrophils have been reported in OSAS patients and were suggested to be linked to the pathogenesis of systemic inflammation that directly contribute to cardiovascular diseases [14, 26]. IH may play a role in the pathobiology of cardiovascular complications in OSAS through activation of pro-inflammatory pathways [27]. Our results showed the activation of CRP, NF-κB, TNF-α, MCP-1, VCAM-1, and RANTES by hypoxia exposure.
As an important circulating marker of inflammation, CRP is suggested to be one of the best predictors for future cardiovascular morbidity directly participating in atheromatous lesion formation [28]. One possible mechanism for the CRP-induced gene expression is suggested to be through the activation of NF κB that results in the expression of profibrotic plasminogen activator inhibitor-1 (PAI-1), known atherothrombogenic factor [29]. Chronic hypoxia exposure in our study did result in significantly elevated levels of CRP, suggesting inflammatory reaction was caused and potential effect on the cardiovascular system.
Activated NF-κB is a key transcription factor in chronic inflammatory diseases [30], and accumulating findings that OSAS and chronic IH were associated with activation of NF-κB and its downstream products implicated NF-κB as a key factor in the link between OSAS and cardiovascular diseases [26, 27]. This observation seemed potentially relevant to reports in OSAS populations of increased circulating cytokines and proteins in the downstream pathways from NF-κB activation, including plasma levels of TNF-α [15], CRP, and MCP-1 [31], and increased VCAM-1 [32]. Our data are consistent with these studies, in addition to the pulmonary hypertension and RV hypertrophy identified in our OSAS rat model, the results of our study also clearly demonstrated the activation of NF-κB and its downstream products after IH or CH exposure.
Pro-inflammatory cytokine TNF-α modulated the physiological sleep, and the level of TNF-α was found to correlate with the severity of OSAS [15]. TNF-α is produced by monocytes and T cells through a transcriptional pathway involving NF-κB and upregulates VCAM-1 expression [33]. NF-κB can also activate the overexpression of VCAM-1, MCP-1, and RANTES involved in leukocyte recruitment and migration to the inflammatory site [14, 34, 35].
Proinflammatory chemokines MCP-1, RANTES are believed to be responsible for cell recruitment [36]. Activation of the MCP-1 and RANTES genes was found to be controlled by NF-κB [34, 35]. As a chemoattractant for inflammatory cells, RANTES is also associated with cardiovascular diseases risk [37] and is critically and early involved in the atherogenesis [38]. An increased aortic intima-media thickness with inflammation was demonstrated in the IH induced inflammatory pre-atherosclerotic remodeling of C57BL6 mouse, and this effect was attenuated by neutralizing the RANTES/CCL5 activity during IH exposure [8]. The present study showed that serum levels of RANTES, a pro-atherosclerotic chemokine, and MCP-1 increased in our IH-induced OSAS rat models, along with the aforementioned chemokine TNF-α, CRP, and VCAM-1, along with the elevated NF-κB level. All these results provide further support for the NF-κB-dependent inflammatory pathways involving in the pathophysiology of both OSAS and cardiovascular diseases.
The evidence for the difference in the response of physiological systems between IH and CH has been mentioned previously [39]. Chronic exposure to IH has been generally used as an animal model for studying IH during sleep. However, it is worth noting that in our study, both chronic IH and CH resulted in pulmonary hypertension and RV hypertrophy, as well as significantly increased expressions of the aforementioned cytokines, and CH showed no statistically different effect than the IH, corroborating the results of recent study, which indicated that chronic CH for 2 weeks can also significantly increase mPAP, as well as elicited significantly RV hypertrophy [40].
In summary, the current study expanding our previous findings indicates that both IH and CH could activate the expression of NF-κB and related inflammatory factors, as well as cause the pathophysiologic damage to cardiovascular system. All these results provide further support to an emerging hypothesis that activation of NF-κB may play a central role in linking the pathophysiology of OSAS with cardiovascular disease.
References
Mbata G, Chukwuka J (2013) Obstructive sleep apnea hypopnea syndrome. Arch Med Health Sci 2(1):74–77
McNicholas W, Bonsignore M (2007) Sleep apnoea as an independent risk factor for cardiovascular disease: current evidence, basic mechanisms and research priorities. Eur Respir J 29(1):156–178
Foster GE, Poulin MJ, Hanly PJ (2007) Intermittent hypoxia and vascular function: implications for obstructive sleep apnoea. Exp Physiol 92(1):51–65
Campen M, Shimoda L, O’Donnell C (2005) Acute and chronic cardiovascular effects of intermittent hypoxia in C57BL/6J mice. J Appl Physiol 99(5):2028–2035
Ryan S, Taylor CT, McNicholas WT (2005) Selective activation of inflammatory pathways by intermittent hypoxia in obstructive sleep apnea syndrome. Circulation 112(17):2660–2667
Fletcher EC (2001) Physiological consequences of intermittent hypoxia: systemic blood pressure. J Appl Physiol 90(4):1600–1605
de Frutos S, Duling L, Alò D, Berry T, Jackson-Weaver O, Walker M, Kanagy N, Bosc LG (2008) NFATc3 is required for intermittent hypoxia-induced hypertension. Am J Physiol Heart Circ 294(5):H2382–H2390
Arnaud C, Beguin PC, Lantuejoul S, Pepin J-L, Guillermet C, Pelli G, Burger F, Buatois V, Ribuot C, Baguet J-P (2011) The inflammatory preatherosclerotic remodeling induced by intermittent hypoxia is attenuated by RANTES/CCL5 inhibition. Am J Respir Crit Care Med 184(6):724–731
Greenberg H, Ye X, Wilson D, Htoo AK, Hendersen T, Liu SF (2006) Chronic intermittent hypoxia activates nuclear factor-κB in cardiovascular tissues in vivo. Biochem Biophys Res Commun 343(2):591–596
Ryan S, Taylor C, McNicholas W (2009) Systemic inflammation: a key factor in the pathogenesis of cardiovascular complications in obstructive sleep apnoea syndrome? Thorax 64(7):631–636
Bhattacharjee R, Kim J, Kheirandish‐Gozal L, Gozal D (2011) Obesity and obstructive sleep apnea syndrome in children: a tale of inflammatory cascades. Pediatr Pulmonol 46(4):313–323
Kim J, Hakim F, Kheirandish-Gozal L, Gozal D (2011) Inflammatory pathways in children with insufficient or disordered sleep. Respir Physiol Neurobiol 178(3):465–474
Garvey J, Taylor C, McNicholas W (2009) Cardiovascular disease in obstructive sleep apnoea syndrome: the role of intermittent hypoxia and inflammation. Eur Respir J 33(5):1195–1205
Htoo AK, Greenberg H, Tongia S, Chen G, Henderson T, Wilson D, Liu SF (2006) Activation of nuclear factor κB in obstructive sleep apnea: a pathway leading to systemic inflammation. Sleep Breathing 10(1):43–50
Minoguchi K, Tazaki T, Yokoe T, Minoguchi H, Watanabe Y, Yamamoto M, Adachi M (2004) Elevated production of tumor necrosis factor-α by monocytes in patients with obstructive sleep apnea syndrome. Chest J 126(5):1473–1479
Ohga E, Tomita T, Wada H, Yamamoto H, Nagase T, Ouchi Y (2003) Effects of obstructive sleep apnea on circulating ICAM-1, IL-8, and MCP-1. J Appl Physiol 94(1):179–184
Zoja C, Donadelli R, Colleoni S, Figliuzzi M, Bonazzola S, Morigi M, Remuzzi G (1998) Protein overload stimulates RANTES production by proximal tubular cells depending on NF-κB activation. Kidney Int 53(6):1608–1615
Zuckerbraun BS, Shiva S, Ifedigbo E, Mathier MA, Mollen KP, Rao J, Bauer PM, Choi JJ, Curtis E, Choi AM (2010) Nitrite potently inhibits hypoxic and inflammatory pulmonary arterial hypertension and smooth muscle proliferation via xanthine oxidoreductase–dependent nitric oxide generation. Circulation 121(1):98–109
Calhoun DA, Harding SM (2010) Sleep and hypertension. Chest J 138(2):434–443
Gong Y, Fan X, Wu X, Hu L, Tang C, Pang Y, Qi Y (2007) Changes of intermedin/adrenomedullin 2 and its receptors in the right ventricle of rats with chronic hypoxic pulmonary hypertension. Sheng Li Xue Bao Acta Physiologica Sinica 59(2):210–214
Peng P, Ly H, Li J, Fan R, Zhang SM, Wang YM, Hu YZ, Sun X, Kaye AD, Pei JM (2009) Distribution of κ-opioid receptor in the pulmonary artery and its changes during hypoxia. Anat Rec 292(7):1062–1067
Li J, Zhang P, Zhang Q-y, Zhang S-m, Guo H-t, Bi H, Wang Y-m, Sun X, Liu J-c, Cheng L (2009) Effects of U50, 488H on hypoxia pulmonary hypertension and its underlying mechanism. Vasc Pharmacol 51(2):72–77
Drager LF, Bortolotto LA, Lorenzi MC, Figueiredo AC, Krieger EM, Lorenzi-Filho G (2005) Early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med 172(5):613–618
Bagai K (2010) Obstructive sleep apnea, stroke, and cardiovascular diseases. Neurologist 16(6):329–339
Almendros I, Farré R, Torres M, Bonsignore MR, Dalmases M, Ramírez J, Navajas D, Montserrat JM (2011) Early and mid-term effects of obstructive apneas in myocardial injury and inflammation. Sleep Med 12(10):1037–1040
Yamauchi M, Tamaki S, Tomoda K, Yoshikawa M, Fukuoka A, Makinodan K, Koyama N, Suzuki T, Kimura H (2006) Evidence for activation of nuclear factor kappaB in obstructive sleep apnea. Sleep Breathing 10(4):189–193
Williams A, Scharf SM (2007) Obstructive sleep apnea, cardiovascular disease, and inflammation—is NF-κB the key? Sleep Breathing 11(2):69–76
Ridker PM, Hennekens CH, Buring JE, Rifai N (2000) C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med 342(12):836–843
Nakakuki T, Ito M, Iwasaki H, Kureishi Y, Okamoto R, Moriki N, Kongo M, Kato S, Yamada N, Isaka N (2005) Rho/Rho-kinase pathway contributes to C-reactive protein–induced plasminogen activator inhibitor-1 expression in endothelial cells. Arterioscler Thromb Vasc Biol 25(10):2088–2093
Monaco C, Paleolog E (2004) Nuclear factor κB: a potential therapeutic target in atherosclerosis and thrombosis. Cardiovasc Res 61(4):671–682
Hayashi M, Fujimoto K, Urushibata K, Takamizawa A, Kinoshita O, Kubo K (2006) Hypoxia-sensitive molecules may modulate the development of atherosclerosis in sleep apnoea syndrome. Respirology 11(1):24–31
Chin K, Nakamura T, Shimizu K, Mishima M, Nakamura T, Miyasaka M, Ohi M (2000) Effects of nasal continuous positive airway pressure on soluble cell adhesion molecules in patients with obstructive sleep apnea syndrome. Am J Med 109(7):562–567
Quercioli A, Mach F, Montecucco F (2010) Inflammation accelerates atherosclerotic processes in obstructive sleep apnea syndrome (OSAS). Sleep Breathing 14(3):261–269
Nelson PJ, Kim H, Manning W, Goralski T, Krensky A (1993) Genomic organization and transcriptional regulation of the RANTES chemokine gene. J Immunol 151(5):2601–2612
Ueda A, Okuda K, Ohno S, Shirai A, Igarashi T, Matsunaga K, Fukushima J, Kawamoto S, Ishigatsubo Y, Okubo T (1994) NF-kappa B and Sp1 regulate transcription of the human monocyte chemoattractant protein-1 gene. J Immunol 153(5):2052–2063
Lloyd CM, Minto AW, Dorf ME, Proudfoot A, Wells TN, Salant DJ, Gutierrez-Ramos J-C (1997) RANTES and monocyte chemoattractant protein–1 (MCP-1) play an important role in the inflammatory phase of crescentic nephritis, but only MCP-1 is involved in crescent formation and interstitial fibrosis. J Exp Med 185(7):1371–1380
Koh SJ, Kim JY, Hyun YJ, Park SH, Chae JS, Park S, Kim J-S, Youn JC, Jang Y, Lee JH (2009) Association of serum RANTES concentrations with established cardiovascular risk markers in middle-aged subjects. Int J Cardiol 132(1):102–108
Borel J-C, Roux-Lombard P, Tamisier R, Arnaud C, Monneret D, Arnol N, Baguet J-P, Levy P, Pepin J-L (2009) Endothelial dysfunction and specific inflammation in obesity hypoventilation syndrome. PLoS One 4(8):e6733
Feng J, Wu Q, Zhang D, Chen B (2012) Hippocampal impairments are associated with intermittent hypoxia of obstructive sleep apnea. Chin Med J 125(4):696–701
Wu Q, Wang H-Y, Li J, Zhou P, Wang Q-L, Zhao L, Fan R, Wang Y-M, Xu X-Z, Yi D-H (2013) κ-opioid receptor stimulation improves endothelial function in hypoxic pulmonary hypertension. PLoS One 8(5):e60850
Acknowledgments
This work was supported by the Wenzhou Technology Project Foundation of China (No. Y20090125). The authors want to thank the teachers at the Department of Animal Experiment and Path Physiology for expert technical assistance, and the teachers and students who had participated in this study.
Conflict of interest
All coauthors certify that they have no affiliations with or involvement in any organization or entity with any financial interest, or non-financial interest in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, XM., Yao, D., Cai, XD. et al. Effect of chronic continual- and intermittent hypoxia-induced systemic inflammation on the cardiovascular system in rats. Sleep Breath 19, 677–684 (2015). https://doi.org/10.1007/s11325-014-1075-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-014-1075-9