Abstract
Objectives
Tumor glycolytic activity as determined by 2-deoxy-2-[F-18]fluoro-d-glucose-positron emission tomography (FDG-PET) imaging is an important marker of tumor biology and provides critical information about the behavior of most malignancies at different stages of the disease. This study was undertaken to determine whether the degree of FDG uptake differs between the primary breast lesions with varying disease burden at diagnosis in proven cases of breast carcinoma.
Materials and Methods
Among 250 patients enrolled for this prospective study, 174 patients with newly diagnosed breast carcinoma at different disease stages who had undergone dual time point FDG-PET before any therapeutic or surgical interventions were considered for inclusion in this analysis. These patients prospectively underwent multimodality imaging techniques, such as magnetic resonance imaging (MRI), ultrasonography, digital mammography, computed tomography (CT), and dual time point FDG-PET, as a component of a National Institutes of Health-funded project for characterizing primary breast lesions and local–regional staging. The slice with maximum FDG uptake in the region of interest (ROI) was chosen for the first time point and the second time point images for quantitative measurement of the metabolic activity of the tracer (SUVmax1 and SUVmax2, respectively). Furthermore, the percent change in SUVmax (%ΔSUVmax) between SUVmax1 and SUVmax2 was calculated.
Results
The patient population (n = 174) were divided into three groups for the purposes of this study. Sixty-four patients with primary and metastatic axillary lymphadenopathy (designated as group I) and 18 patients with both axillary and distant metastases (designated as group II) met the inclusion criteria for this analysis. The third group (group III) comprised of a population of 92 patients without any metastasis either at the lymph nodes or at distant sites. The mean SUVmax1, SUVmax2, and the %ΔSUVmax in the early and delayed FDG-PET in group I (n = 64) patients were as follows: primary lesion 4.8 ± 3.9, 5.3 ± 4.5, and 9.4 ± 12.8%, respectively, and axillary lesions 3 ± 2.6, 3 ± 2.7, and 1.1 ± 21.3%, respectively. Among the group II patients (n = 18), the mean values of the primary lesion with regard to the SUVmax1, SUVmax2, and the %ΔSUVmax were 7.7 ± 6.2, 8.9 ± 7.1, and 15.7 ± 10.8%, respectively. The corresponding figures for the axillary lesions were 3.5 ± 3.1, 3.7 ± 3.1, and 6.3 ± 20.9%, respectively, and those for the distant metastatic lesions were 3 ± 1.4, 3.1 ± 1.2, and 8.5 ± 21.2%, respectively. The mean SUVmax1, SUVmax2, and the %ΔSUVmax of the primary lesion of group III patients (n = 92) without any metastasis were 2.9 ± 2.7, 3.4 ± 2.4, and 4.5 ± 4.2%, respectively. Unifactorial ANOVA of the three parameters among the primary lesions of these three groups were statistically significant with regard to the mean SUVmax1 (p = 0.01) and SUVmax2 (p = 0.01). These values in the primary lesions were highest in group II (those with both axillary and distant metastases), followed by group I (those with only metastatic axillary adenopathy) and group III (patients without any metastasis), and could be related to the more aggressive tumor biology in group II.
Conclusion
The findings provide evidence that among the lesions with varying disease burden at diagnosis, the FDG uptake is highest in cases with both axillary and distant metastasis, followed by those with axillary metastasis and then by those with no metastatic disease. These provide in vivo insight into tumor biology as FDG uptake is regarded as a surrogate marker of the same.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
2-Deoxy-2-[F-18]fluoro-d-glucose-positron emission tomography (FDG-PET) imaging is a promising noninvasive modality for assessing regional and global metabolic activity of an organ or a diseased site in the entire body [1]. The tumoral FDG accumulation is based upon enhanced glycolysis, a phenomenon known as the “Warburg effect” [2]. There is now ample evidence in the literature that the degree of FDG uptake in the cancer cells correlates with tumor growth rate and the potential for aggressive behavior and prediction of prognosis [3–10]. The prognostic significance of FDG uptake has been demonstrated in several malignancies [3–10]. However, the reported studies in the literature are primarily based upon the degree of metabolic activity of the primary tumors. Therefore, we undertook this study to determine whether the FDG uptake parameters in the primary tumor could forecast potential for locoregional and distant site and whether the tendency for metastases differs between the groups with tumors that have high metabolic activity compared to those with relatively hypometabolic tumors. Comparison was also made with regard to these parameters among the primary and metastatic lesions in the same group of patients. This prospective study examined patients with newly diagnosed breast carcinoma by utilizing FDG-PET imaging along with other imaging modalities for characterizing primary lesions and also determining the disease stage at diagnosis. For the purposes of this research, we analyzed the following parameters obtained from the dual time point FDG-PET studies: (a) tumor metabolism at the initial single time point (SUVmax1), (b) at the second time point (SUVmax2), and (c) the rate of change over time at the primary and the metastatic sites (%ΔSUVmax).
Materials and Methods
Patient Population
Newly diagnosed patients with breast carcinoma with and without axillary or distant metastases at presentation underwent dual time point FDG-PET before any therapeutic or major surgical intervention provided the basis for this analysis. All patients underwent multimodality imaging techniques, including magnetic resonance imaging (MRI), ultrasonography, digital mammography, computed tomography (CT), and FDG-PET, as a component of this National Institutes of Health-funded project for characterizing primary breast lesions and local–regional staging. After FDG-PET imaging, all of these patients underwent surgical intervention, which was scaled according to the stage of the disease. Histopathological results provided the definitive diagnosis in this population against which the PET findings were compared.
FDG-PET Imaging Protocol
FDG-PET was performed with a dedicated whole-body PET scanner (Allegro; Philips Medical Systems). All patients fasted for at least six hours before the PET scan and had blood glucose levels of <140 mg/dl at the time of injection. The first scan was performed as whole-body images from head to midthigh with acquisition of four to five emission scans, resulting in a complete axial length of 64–76.8 cm. The second scan included the chest alone with acquisition of one or two emission scans, resulting in a complete axial length of 25.6–38.4 cm. The approximate mean time intervals between the injection of FDG and the first and second scans were 63 minutes (range, 60–70 minutes) and 101 minutes (range, 95–105 minutes), respectively. Transmission scans were performed for all patients to provide attenuation correction with a 137Cs point source. The patients did not leave the scanning table between the two acquisitions, minimizing patient motion artifacts. The ordered-subsets expectation maximization method was used to reconstruct all PET images.
Study Analysis
In the present study, comparative evaluation of the standardized uptake value (SUV) indices was carried out among the primary lesions of various groups with varying disease burden at diagnosis. Two nuclear medicine physicians analyzed the data independently for this study. The SUVs were identical in most cases with both of the observers. In cases where the numbers were different, the mean value was calculated for the final SUVmax analysis. After image reconstruction, a 2-D region of interest (ROI) was carefully drawn around the site of the primary breast lesion and the metastatic lesion on the consequent four to six PET scan slices. The slice with the maximum FDG uptake in the ROI was chosen for the first time point and the second time point images for quantitative measurement of the metabolic activity of the tracer (SUVmax1 and SUVmax2). We then determined the percent change in SUVmax (%SUVmax) between SUVmax1 and SUVmax2.
Statistical Analysis
All of the quantitative values were expressed in terms of the mean±SD. Groups were compared by using the Student’s t test and unifactorial analysis of variance (ANOVA) test, wherever applicable.
Results
Among the entire population who underwent multimodality imaging protocol, 64 patients had evidence of axillary metastases at the time of FDG-PET with clear visualization of both primary and axillary lesions on each of the dual time point scans. These patients had no prior history of any therapeutic or surgical intervention at the time of PET imaging and metastatic involvement was proven subsequently on all cases when they underwent biopsy or surgical excision. These 64 patients formed group I of the study population. There were a total of 68 breast lesions and 159 metastatic axillary nodes.
Group II of the study population comprised of 18 cases of breast carcinoma that had both axillary and evidence for distant metastasis at the time of FDG-PET in addition to the primary breast lesion. They either had subsequent proof of disease involvement by histopathology (in case of axillary disease) or by any other imaging modality (in case of distant metastasis). There were a total of 19 breast lesions, 41 metastatic axillary nodes, and 18 distant metastatic lesions.
Among the group I patients (n = 64), the mean values for the SUVmax1, SUVmax2, and the %ΔSUVmax were 4.8 ± 3.9, 5.3 ± 4.5, and 9.4 ± 12.8%, respectively, while those of axillary nodes were 3 ± 2.6, 3 ± 2.7, and 1.1 ± 21.3%, respectively. The data are presented in Table 1.
Among the group II patients (n = 14), the mean values of the primary lesion with regard to for the SUVmax1, SUVmax2, and the %ΔSUVmax were 7.7 ± 6.2, 8.9 ± 7.1, and 15.7 ± 10.8%, respectively. The corresponding figures for the axillary nodes were 3.5 ± 3.1, 3.7 ± 3.1, 6.3 ± 20.9%, respectively, and for the distant metastatic lesions were 3 ± 1.4, 3.1 ± 1.2, and 8.5 ± 21.2%, respectively. It is interesting to note that among the metastatic sites, the distal metastases had a higher mean %ΔSUVmax than that of the axillary ones. The data are presented in Table 2.
Finally, we selected 92 patients with 92 primary lesions without any nodal or distant metastasis as the group III for this analysis. All lesions in this group were proven to be malignant by histopathological examination subsequent to surgical excision. The mean SUVmax1, SUVmax2, and the %ΔSUVmax were 2.9 ± 2.7, 3.4 ± 2.4, and 4.5 ± 4.2%, respectively.
Unifactorial ANOVA of the three parameters among the primary lesions of these three groups were statistically significant with regard to the mean SUVmax1 (p = 0.01) and SUVmax2 (p = 0.01). Among the primary lesions, the highest values were noted in group II (those with both axillary and distant metastases), followed by group I (those with only metastatic axillary adenopathy) and group III (patients with no metastasis). The results of this analysis are depicted in Table 3.
Discussion
Currently, standardized uptake value (SUV) is the most commonly used semiquantitative parameter for assessing the degree of FDG accumulation in a variety of clinical settings [1]. It is calculated by dividing the activity in the ROI drawn around the lesion (MBq/ml) by the injected dose (MBq) divided by the body weight (g). This is usually an automated procedure and is available on the current PET workstations. The SUV of the tissue has a linear relationship with the rate of glucose metabolism as measured by kinetic modeling [11, 12].
Several approaches have been explored to enhance the specificity of FDG-PET in several malignancies of which dual time point FDG-PET imaging has been explored in the recent literature in a wide variety of malignancies including those of the head and neck [13], lung [14], breast [15–17], gall bladder [18], cervix [19], and glioma [20]. The theoretical basis of this approach stems from the fact that the dephosphorylation in malignant tumor cells is either absent or is very slow compared to that of normal cells because of low glucose-6-phosphatase content in the former group. This results in building up a contrast between the malignant lesions and surrounding normal tissues with time, which further enhances lesion detectability. Also, this has been successfully exploited in distinguishing malignant from benign lesions where changes in SUV over time are significantly different between these two distinct pathologic states. In one of the earliest reports, Hamberg et al. [21] documented that the equilibrium time in bronchial carcinoma varied from 256 to 340 minutes post injection, and this changed after therapy, when it varied from 123 to 185 minutes post injection. They concluded that the time interval of 45–60 minutes lead to significant underestimation of the true SUV because, in most tumors, FDG uptake continues to rise beyond this period and typically does not reach a plateau for several hours. To date, there has not been any well-designed study in the literature investigating the potential of dual time point imaging in predicting disease burden in cancer.
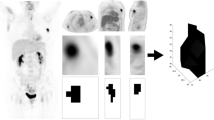
In this study, we observed an increase in the SUVs in both the primary and metastatic lesions regardless of the population groups selected for analysis; this is in agreement with other studies using similar or identical approaches and reiterates the fact that the FDG uptake increases over time in both the primary and metastatic lesions irrespective of the site of the lesion. The results obtained in this study reiterate the fact that the various SUV parameters obtained in the dual-time-point approach correlate well with the disease burden at diagnosis. The finding of significantly higher SUVmax values (at both time points) in the primary breast malignancies of patients with both axillary and distant metastatic disease, followed by those with only axillary disease, and finally by individuals with breast cancer without any metastasis reflects the degree of the relative aggressiveness of the primary tumor among these three subgroups (Figs. 1 and 2). This can explain the relatively poor prognosis of the primary tumors with higher SUVs as reported in literature [3–10] and reflects the greater aggressiveness of the malignancy in patients with both axillary and distant metastases than in those with only axillary adenopathy. This is consistent with the hypothesis that we proposed in undertaking this analysis. One of the shortcomings of this study was we did not make a subclassification of the individual histological subtypes as most of our patients harbored infiltrating ductal carcinoma. We believe it will be worthwhile to examine individual subtypes when we have a larger patient population in each subcategory of histopathological type to investigate whether there is any differential behavior among these groups. Metastatic lesions at the distant sites (in our series all were skeletal metastases) demonstrated higher %ΔSUVmax than that of the axillary adenopathies. Although this did not reach a statistical significance (p > 0.05), we believe that this could be because of the relatively smaller number of patients in this group (n = 18). The higher %ΔSUVmax values at the distant metastatic sites (in our series skeletal metastasis) compared to the axillary nodes could be related to the differential cell proliferation among these different sites and this in turn might be because of the different local homeostatic factors that the tumor cells can usurp. One of the observations made in this study was that in both groups the SUVmax1 and SUVmax2 were significantly higher in the primary tumors than in the metastatic sites. Among the metastases, the corresponding values were significantly higher in the axillary metastases than the distant ones. We believe this difference in SUV parameters between the primary and the metastatic lesions need to be evaluated after partial volume correction of the SUV with regard to the size of the individual lesions [22], and this analysis will be reported in a different study.
Conclusion
The findings from this study provide evidence that among the primary lesions with varying disease burden at diagnosis, the FDG uptake is highest in cases with both axillary and distant metastasis, followed by those with axillary metastasis, and then by those with no metastatic disease. These provide an in vivo insight into tumor biology as FDG uptake is regarded as a surrogate marker for the degree of tumor aggressiveness in a multitude of malignancies.
References
Basu S, Zaidi H, Houseni M, Bural G, Udupa J, Acton P, Torigian DA, Alavi A (2007) Novel quantitative techniques for assessing regional and global function and structure based on modern imaging modalities: implications for normal variation, aging and diseased states. Semin Nucl Med 37:223–239
Warburg O, Posener K, Negelein E (1924) Uber den stoffwechsel der carcinomzelle. Biochem Z 152:309–335
Nguyen XC, Lee WW, Chung JH, Park SY, Sung SW, Kim YK, So Y, Lee DS, Chung JK, Lee MC, Kim SE (2007) FDG uptake, glucose transporter type 1, and Ki-67 expressions in non-small-cell lung cancer: correlations and prognostic values. Eur J Radiol 62:214–219
Ohtsuka T, Nomori H, Watanabe K, Kaji M, Naruke T, Suemasu K, Uno K (2006) Prognostic significance of [(18)F]fluorodeoxyglucose uptake on positron emission tomography in patients with pathologic stage I lung adenocarcinoma. Cancer 107:2468–2473
Schot BW, Zijlstra JM, Sluiter WJ, van Imhoff GW, Pruim J, Vaalburg W, Vellenga E (2007) Early FDG-PET assessment in combination with clinical risk scores determines prognosis in recurring lymphoma. Blood 109:486–491
Querellou S, Valette F, Bodet-Milin C, Oudoux A, Carlier T, Harousseau JL, Chatal JF, Couturier O (2006) FDG-PET/CT predicts outcome in patients with aggressive non-Hodgkin’s lymphoma and Hodgkin’s disease. Ann Hematol 85:759–767
Choi JY, Jang KT, Shim YM, Kim K, Ahn G, Lee KH, Choi Y, Choe YS, Kim BT (2006) Prognostic significance of vascular endothelial growth factor expression and microvessel density in esophageal squamous cell carcinoma: comparison with positron emission tomography. Ann Surg Oncol 13:1054–1062
Capirci C, Rubello D, Chierichetti F, Crepaldi G, Fanti S, Mandoliti G, Salviato S, Boni G, Rampin L, Polico C, Mariani G (2006) Long-term prognostic value of 18F-FDG PET in patients with locally advanced rectal cancer previously treated with neoadjuvant radiochemotherapy. AJR Am J Roentgenol 87:W202–W208
Alavi JB, Alavi A, Chawluk J, Kushner M, Powe J, Hickey W, Reivich M (1988) Positron emission tomography in patients with glioma. A predictor of prognosis. Cancer 62:1074–1078
Cachin F, Prince HM, Hogg A, Ware RE, Hicks RJ (2006) Powerful prognostic stratification by [18F]fluorodeoxyglucose positron emission tomography in patients with metastatic breast cancer treated with high-dose chemotherapy. J Clin Oncol 24:3026–3031
Minn H, Leskinen-Kallio S, Lindholm P, et al. (1993) [18F]fluorodeoxyglucose uptake in tumors: kinetic vs. steady-state methods with reference to plasma insulin. J Comput Assist Tomogr 17:115–123
Kole A, Nieweg O, Pruim J, et al. (1997) Standardized uptake value and quantification of metabolism for breast cancer imagin with FDG and L-[1-11C]tyrosine PET. J Nucl Med 38:692–696
Hustinx R, Smith RJ, Benard F, et al. (1999) Dual time point fluorine-18 fluorodeoxyglucose positron emission tomography: a potential method to differentiate malignancy from inflammation and normal tissue in the head and neck. Eur J Nucl Med 26:1345–1348
Matthies A, Hickeson M, Cuchiara A, Alavi A (2002) Dual-time-point 18F-FDG PET for the evaluation of pulmonary nodules. J Nucl Med 43:871–875
Kumar R, Loving VA, Chauhan A, Zhuang H, Mitchell S, Alavi A (2005) Potential of dual-time-point imaging to improve breast cancer diagnosis with (18)F-FDG PET. J Nucl Med 46:1819–1824
Mavi A, Urhan M, Yu JQ, et al. (2006) Dual time point 18F-FDG PET imaging detects breast cancer with high sensitivity and correlates well with histologic subtypes. J Nucl Med 47:1440–1446
Boerner AR, Weckesser M, Herzog H, et al. (1999) Optimal scan time for fluorine-18 fluorodeoxyglucose positron emission tomography in breast cancer. Eur J Nucl Med 26:226–230
Nishiyama Y, Yamamoto Y, Fukunaga K, et al. (2006) Dual-time-point 18F-FDG PET for the evaluation of gallbladder carcinoma. J Nucl Med 47:633–638
Ma SY, See LC, Lai CH, et al. (2003) Delayed 18F-FDG PET for detection of paraaortic lymph node metastases in cervical cancer patients. J Nucl Med 44:1775–1783
Spence M, Muzi M, Mankoff DA, et al. (2004) 18F-FDG PET of gliomas at delayed intervals: improved distinction between tumor and normal gray matter. J Nucl Med 45:1653–1659
Hamberg LM, Hunter GJ, Alpert NM, Choi NC, Babich JW, Fischman AJ (1994) The dose uptake ratio as an index of glucose metabolism: useful parameter or oversimplification? J Nucl Med 35:1308–1312
Basu S, Alavi A (2007) Partial volume correction of standardized uptake values and the dual-time-point in FDG-PET imaging: should these be routinely employed in assessing patients with cancer? Eur J Nucl Med Mol Imaging 34:1527–1529
Acknowledgements
This work was supported in part by the International Union against Cancer (UICC), Geneva, Switzerland, under the ACSBI fellowship.
Declaration.
A part of this work was presented in the 2007 Annual Meeting of the Society of Nuclear Meeting at Washington DC.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Basu, S., Mavi, A., Cermik, T. et al. Implications of Standardized Uptake Value Measurements of the Primary Lesions in Proven Cases of Breast Carcinoma with Different Degree of Disease Burden at Diagnosis: Does 2-Deoxy-2-[F-18]fluoro-d-glucose-Positron Emission Tomography Predict Tumor Biology?. Mol Imaging Biol 10, 62–66 (2008). https://doi.org/10.1007/s11307-007-0121-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-007-0121-4