Abstract
Retinal hypoxia is a major condition of the chronic inflammatory disease age-related macular degeneration. Extracellular ATP is a danger signal which is known to activate the NLRP3 inflammasome in various cell systems. We investigated in cultured human retinal pigment epithelial (RPE) cells whether hypoxia alters the expression of inflammasome-associated genes and whether purinergic receptor signaling contributes to the hypoxic expression of key inflammatory (NLRP3) and angiogenic factor (VEGF) genes. Hypoxia and chemical hypoxia were induced by a 0.2%-O2 atmosphere and addition of CoCl2, respectively. Gene expression was determined with real-time RT-PCR. Cytosolic NLRP3 and (pro-) IL-1β levels, and the extracellular VEGF level, were evaluated with Western blot and ELISA analyses. Cell culture in 0.2% O2 induced expression of NLRP3 and pro-IL-1β genes but not of the pro-IL-18 gene. Hypoxia also increased the cytosolic levels of NLRP3 and (pro-) IL-1β proteins. Inflammasome activation by lysosomal destabilization decreased the cell viability under hypoxic, but not control conditions. In addition to activation of IL-1 receptors, purinergic receptor signaling mediated by a pannexin-dependent release of ATP and a release of adenosine, and activation of P2Y2 and adenosine A1 receptors, was required for the full hypoxic expression of the NLRP3 gene. P2Y2 (but not A1) receptor signaling also contributed to the hypoxic expression and secretion of VEGF. The data indicate that hypoxia induces priming and activation of the NLRP3 inflammasome in cultured RPE cells. The hypoxic NLRP3 and VEGF gene expression and the secretion of VEGF are in part mediated by P2Y2 receptor signaling.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Age-related macular degeneration (AMD) is the main cause of visual impairment and blindness in people aged over 65 years in developed countries [1, 2]. The majority of patients suffer from the dry form of AMD which is, in the late stage, characterized by geographic atrophy, i.e., a degeneration of the retinal pigment epithelium (RPE) associated with a degeneration of photoreceptors [3]. The remaining patients suffer from the neovascular form characterized by choroidal neovascularization and subretinal edema. Normal aging and AMD are associated with a decrease in the choroidal blood flow [4, 5] and a dysfunction of the RPE. The dysfunction of RPE cells results in an impaired degradation of peroxidized photoreceptor lipoproteins, accumulation of lipofuscin in the RPE [6, 7], and deposition of drusen beneath the RPE [8, 9]. Accumulated lipoproteins constitute a hydrophobic barrier that adversely affects the transport of oxygen and nutrients from the choriocapillaris to the photoreceptors [10]. Inadequate choroidal perfusion and accumulation of lipoproteins lead to hypoglycemia and hypoxia of the outer retina resulting in overproduction of angiogenic factors by RPE cells that stimulate the growth of choroidal vessels [10]. Vascular endothelial growth factor (VEGF) is the most relevant angiogenic factor induced by retinal hypoxia [11]. In addition to glial cells and macrophages, RPE cells are a source of VEGF [12].
AMD was shown to be associated with chronic local and systemic inflammation [13,14,15,16]. Inflammatory processes are initiated by activation of inflammasomes which are cytosolic protein-signaling complexes that recognize pathogen- and damage-associated molecular patterns [17]. The activated inflammasome mediates the proteolytic activation of caspase-1 that catalyzes the maturation of the inflammatory cytokines interleukin (IL)-1β and IL-18 [17]. The RPE of patients with geographic atrophy or neovascular AMD contains the NLRP3 (nucleotide-binding oligomerization domain receptors-like receptor protein 3) inflammasome [18]. Activation of the NLRP3 inflammasome is assumed to be involved in mediating the degeneration of the RPE and the development of choroidal neovascularization [19,20,21].
Activation of the inflammasome is a two-step process triggered by a priming signal followed by the action of an activation signal [17]. Priming of the inflammasome involves the gene expression and production of inflammasome receptor and pro-IL-1β proteins [17]. The NLRP3 inflammasome in RPE cells was shown to be activated by different factors that are assumed to be implicated in the pathogenesis of AMD like complement factors, lipofuscin-mediated photooxidative damage, peroxidized lipids, lysosomal destabilization, and overexpressed VEGF [18,19,20,21,22,23,24,25]. The NLRP3 inflammasome in RPE cells is also transiently primed and activated by elevation of the extracellular osmolarity; the hyperosmotic activation of the NLRP3 inflammasome is associated with a decrease of the RPE cell viability [26]. Among other factors like advanced age, race, genetic factors, sunlight exposure, and cigarette smoking, systemic hypertension is a risk factor of AMD [27, 28]. The main condition that causes acute hypertension is increased extracellular osmolarity following intake of dietary salt (NaCl) [29].
Retinal hypoxia is a major pathogenic condition of AMD; however, it is not known whether hypoxia also induces priming and activation of the NLRP3 inflammasome in RPE cells. Therefore, the first aim of the present study was to determine whether the gene expression of inflammasome-associated proteins in cultured human RPE cells is altered under hypoxic conditions. We found that the expression levels of NLRP3 and pro-IL-1β genes are elevated under low-O2 conditions, suggesting that hypoxia induces priming of the NLRP3 inflammasome in cultured RPE cells. We also found a hypoxic increase of the cytosolic level of (pro-) IL-1β, suggesting that hypoxia may also induce activation of the inflammasome in RPE cells. The hyperosmotic priming of the NLRP3 inflammasome in RPE cells was shown to be in part dependent on autocrine/paracrine purinergic (P2) receptor signaling induced by a pannexin-mediated release of adenosine 5′-triphosphate (ATP) [26]. Extracellular ATP is a danger signal that is released in large amounts by stressed cells, e.g., in response to inflammation, oxidative stress, nutrient starvation, ischemia-hypoxia, and cell injury [30]. However, it is not known whether the hypoxic and hyperosmotic activation of the inflammasome in RPE cells is mediated by similar or different signal transduction mechanisms including extracellular ATP signaling. The second aim of the present study was to determine whether autocrine/paracrine purinergic receptor signaling contributes to the hypoxia-induced expression of key inflammatory (NLRP3) and angiogenic factor (VEGF) genes in cultured RPE cells.
Materials and methods
Human material
The use of human material was approved by the Ethics Committee of the University of Leipzig (approval #745, 07/25/2011) and was performed according to the Declaration of Helsinki. Postmortem eyes from human cornea donors without reported eye disease were obtained within 48 h of death; the written informed consent for the use of retinal tissue in basic science was obtained from the relatives of each donor.
Cell lines from a total of 26 donors (14 females, 12 males) were used. The age of the donors ranged from 38 to 90 years (means ± SD, 60.8 ± 14.8 years for females and 59.6 ± 15.1 years for males). The donors suffered from following end-stage diseases: multiple organ failure (n = 9), subarachnoid hemorrhage (n = 4), cerebral hemorrhage (n = 4), cardiac infarction (n = 3), pulmonary embolism (n = 2), lung failure and hepatocerebral syndrome due to chronic liver cirrhosis (n = 1), traumatic brain injury (n = 1), cerebral edema (n = 1), and heparin-induced thrombocytopenia, renal failure, and bronchopneumonia (n = 1). Data obtained with cells of younger and aged donors, and with cells of females and males, were not significantly different (not shown).
Materials
Cell culture components and solutions were obtained from Gibco BRL (Paisley, UK). The recombinant human IL-1 receptor antagonist was purchased from R&D Systems (Abingdon, UK). Stattic was from Enzo Life Science (Lörrach, Germany). 666-15, A-438079, AR-C 118925XX, ARL-67156, caffeic acid phenethyl ester (CAPE), MRS2179, the pannexin-blocking peptide 10panx, the scrambled control peptide 10panxScr, and SR11302 were obtained from Tocris (Ellisville, MO). 8-Cyclopentyl-1,3-dipropylxanthine (DPCPX), 8-(3-chlorostyryl) caffeine (CSC), the hypoxia-inducible transcription factor (HIF)-1 inhibitor 3-[2-(4-adamantan-1-yl-phenoxy)-acetylamino]-4-hydroxybenzoic acid methyl ester, and SU1498 were obtained from Calbiochem (Bad Soden, Germany). Ac-YVAD-CMK was obtained from Enzo (Lausen, Switzerland). L-Leucyl-L-leucine methyl ester was from Bachem (Weil am Rhein, Germany). Adenosine-5′-O-(α,β-methylene)-diphosphate (AOPCP), apyrase, and all other agents used were from Sigma-Aldrich (Taufkirchen, Germany), unless stated otherwise. Human-specific small interfering RNA (siRNA) against nuclear factor of activated T cell 5 (NFAT5) and non-targeted control siRNA were obtained from Santa Cruz (Dallas, TX). The following antibodies were used: a mouse anti-human NLRP3 (1:1000; #ALX-804-819, Enzo), a rabbit anti-human β-actin (1:1000; #8457, Cell Signaling, Frankfurt/M., Germany), an anti-mouse IgG conjugated with alkaline phosphatase (1:2000; #7056, Cell Signaling), and an anti-rabbit IgG conjugated with alkaline phosphatase (1:2000; #7054, Cell Signaling).
Cell culture
Preparation and culture of RPE cells were previously described [31]. Cell lines of passages 2–5 were used; each line was used in 3–10 different experiments. When a confluency of approximately 90% was achieved, the cells were cultured in serum-free medium for 16 h. During this time period, the cultures reached 100% confluency. Thereafter, test substances were added to the serum-free medium. Hypoxia was induced by two methods: cell culture in a 0.2%-O2 atmosphere and addition of CoCl2 (150 μM) to the culture medium. The hyperosmotic medium was made up by addition of 100 mM NaCl to the culture medium. The cells were preincubated with pharmacological inhibitors for 30 min.
RT-PCR analysis
The RNeasy Mini Kit (Qiagen, Hilden, Germany) was used to extract the total RNA. The quality of the RNA was analyzed with agarose gel electrophoresis. The A260/A280 ratio of the optical density was measured using the GeneQuantpro device (Pharmacia, Uppsala, Sweden), and was between 2.0 and 2.2 for all RNA samples, indicating sufficient quality. After treatment with DNase I (Roche, Mannheim, Germany), cDNA was synthesized from 1 μg of total RNA using the RevertAid H Minus First Strand cDNA Synthesis kit (Fermentas, St. Leon-Roth, Germany). PCR was performed with the Taq PCR Master Mix kit (Qiagen) and the primer pairs described in Table 1. One microliter of the first-strand mixture and 0.25 μM of each gene-specific sense and anti-sense primers were used for amplification in a final volume of 20 μl. Amplification was done for 40 cycles with the PTC-200 Thermal Cycler (MJ Research, Watertown, MA). Each cycle consisted of 30 s at 94 °C, 60 s at 58 °C, and 1 min at 72 °C.
Real-time RT-PCR analysis
Semi-quantitative real-time RT-PCR analysis was performed with the Single-Color Real-Time PCR Detection System (BioRad, Munich, Germany) and the primer pairs described in Table 1. The PCR solution contained 1 μl cDNA, specific primer set (0.2 μM each), and 10 μl of a 2x mastermix (QuantiTect SYBR Green PCR Kit; Qiagen) in a final volume of 20 μl. The following conditions were used: initial denaturation and enzyme activation (1 cycle at 95 °C for 15 min); denaturation, amplification, and quantification (45 cycles at 95 °C for 30 s, 58 °C for 30 s, and 72 °C for 1 min); and melting curve (55 °C with the temperature gradually increased (0.5 °C) up to 95 °C). The amplified samples were analyzed with standard agarose gel electrophoresis. The mRNA expression levels were normalized to the level of β-actin mRNA. Changes in mRNA expression were calculated according to the 2-ΔΔCT method [32].
siRNA transfection
Cells were seeded at 7 × 104 cells per well in 12-well culture plates and were allowed to grow up to a confluency of 60–80%. Thereafter, the cells were transfected with NFAT5 siRNA and non-targeted siRNA (5 nM each), respectively, using HiPerfect reagent (Qiagen) in F-10 medium containing 10% fetal bovine serum (Invitrogen, Paisley, UK) according to the manufacturer’s instructions. After 48 h (a time point at which the cultures were confluent), the medium was removed and fresh medium without serum was added for 2 h. Thereafter, CoCl2 (150 μM) was added for further 6 h. Total RNA was extracted, and the NLRP3 mRNA level was determined with real-time RT-PCR analysis.
Western blot analysis
Cells were seeded at 5 × 105 cells per well in 6-well plates in 2 ml complete medium and were allowed to grow up in serum-containing medium. After cell culture in serum-free medium for 16 h, the cells were cultured in the presence of CoCl2 (150 μM) for 6, 16, and 24 h, respectively. Then, the medium was removed, the cells were washed twice with prechilled phosphate-buffered saline (pH 7.4; Invitrogen), scraped into 150 μl of lysis buffer (50 mM Tris-HCl pH 8.0, 5 mM EDTA, 150 mM NaCl, 0.5% NP-40, 1% protease inhibitor cocktail), and agitated at 4 °C for 30 min. Cell lysates were centrifuged at 13,000×g for 10 min, and supernatants were analyzed with immunoblotting. Equal amounts of protein (35 μg) were separated by 10% SDS-polyacrylamide gel electrophoresis. Immunoblots were probed with primary and secondary antibodies; immunoreactive bands were visualized with 5-bromo-4-chloro-3-indolyl phosphate/nitro blue tetrazolium.
ELISA
Cells were cultured at 3 × 103 cells per well in 12-well plates. At a confluency of about 90%, the cells were cultured in serum-free medium for 16 h; within this time period, the cultures reached 100% confluency. Subsequently, the medium was changed, and the cells were cultured in 0.2% O2 or treated with CoCl2 (150 μM). Culture supernatants (1 ml) and cell lysates (150 μl) were collected after 6 and 24 h. The cytosolic level of IL-1β (which may include both pro-IL-1β and mature IL-1β) and the level VEGF-A165 in the culture supernatants (100 μl) were determined with ELISA (#HSLB00C; DVE00; R&D Systems).
Cell viability
A trypan blue exclusion assay was used to investigate the cell viability. The cells were seeded at 5 × 104 cells per well in 6-well plates. After reaching a confluency of about 90%, the cells were cultured in serum-free medium for 16 h; during this period, the cultures reached 100% confluency. Thereafter, the cells were cultured for 24 h in serum-free medium in a 0.2%-O2 atmosphere or in the presence of CoCl2 (150 μM). After trypsinization, the cells were stained with trypan blue (0.4%). The numbers of viable (non-stained) and dead (stained) cells were counted using a hemocytometer.
Statistical analysis
At least three independent experiments with cell lines from different donors were performed for each test. Data are shown as means ± SEM. Statistical analysis was made with Prism (Graphpad Software, San Diego, CA). Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test and with Mann-Whitney U test, respectively, and were accepted at p < 0.05.
Results
Expression of inflammasome-associated genes
We investigated with RT-PCR analysis whether cultured human RPE cells contain gene transcripts of inflammasome-associated proteins. We found in agreement with a previous study [26] that the cells contained transcripts of the inflammasome sensor proteins NLRP2, NLRP3, and absent in melanoma 2 (AIM2), of the adaptor protein apoptosis-associated speck-like protein containing a caspase-recruitment domain (ASC), of pro-IL-1β, pro-IL-18, and the procaspases 1 and 4 (Fig. 1a). Transcripts of other inflammasome sensor proteins (NLRP1, NLRP6, NLRP7, NLRP12, NLRC4) were not detected in the RNAs extracted from different cell lines cultured under control and hypoxic conditions (not shown).
Hypoxic regulation of the gene expression of inflammasome-associated proteins in cultured human RPE cells. mRNA levels were determined with real-time RT-PCR analysis in cells cultured 2, 6, and 24 h (as indicated by the panels of the bars) and are expressed as folds of unstimulated control. a Presence of gene transcripts of inflammasome-associated proteins in RPE cells. The correct lengths of PCR products were confirmed with agarose gel electrophoresis using products obtained from cell lines of two different donors (1, 2). Negative controls (0) were done with double-distilled water instead of cDNA as template. ACTB mRNA was used as loading control. b, c Effects of cell culture in 0.2% O2 (b) and of addition of CoCl2 (150 μM; c), respectively, on the gene expression of inflammasome-associated proteins. d Effects of CoCl2 (150 μM) on the expression of NLRP3 in iso- and hyperosmotic media. Hyperosmolarity was induced by addition of 100 mM NaCl to the culture medium. The numbers of independent experiments using cell lines from different donors are indicated in or above the bars. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference between two groups (as indicated by the brackets): ●p < 0.05
Hypoxic regulation of inflammasome-associated gene expression
Real-time RT-PCR analysis was carried out to investigate whether hypoxia induces alterations in the expression of inflammasome-associated genes in cultured RPE cells. Hypoxia was induced by cell culture in a 0.2%-O2 atmosphere or by addition of the hypoxia mimetic CoCl2 [33]. Cell culture in 0.2% O2 induced significant (p < 0.05) increases in the expression levels of NLRP3 and pro-IL-1β genes (Fig. 1b). Addition of CoCl2 to the culture medium resulted in significant (p < 0.05) increases in the expression of NLRP3, AIM2, ASC, and caspase-4 genes, while the level of caspase-1 gene transcripts was time-dependently decreased; the expression of the pro-IL-1β gene remained unaltered (Fig. 1c). The expression levels of NLRP2 and IL-18 genes did not change under both conditions (Fig. 1b, c). Extracellular hyperosmolarity was shown to induce priming of the NLRP3 inflammasome in RPE cells [26]. We found that the effects of high NaCl-induced extracellular hyperosmolarity and CoCl2-induced hypoxia on the expression of the NLRP3 gene were additive (Fig. 1d). The time-dependencies of the NLRP3 gene expression under both conditions were also different; the CoCl2-induced expression of the NLRP3 gene was highest after 24 h of stimulation (Fig. 1c), whereas the hyperosmotic expression of the NLRP3 gene was shown to peak after 6 h of stimulation [26]. The data may support the assumption that different signal transduction mechanisms mediate the transcriptional induction of the NLRP3 gene under hypoxic and hyperosmotic conditions.
Hypoxia-induced increases of NLRP3 and IL-1β protein levels
Western blot analysis was performed to investigate whether hypoxia also increases the level of NLRP3 protein in cultured RPE cells. Under unstimulated control conditions, the level of NLRP3 protein in the cells was low (Fig. 2a). The cellular level of NLRP3 protein increased time-dependently in the presence, but not in the absence, of the hypoxia mimetic CoCl2 (Fig. 2a, b). Increases of the cellular NLRP3 protein level were observed after 16 and 24 h of stimulation (Fig. 2a, b); this time dependency fits well with that of the CoCl2-induced expression of the NLRP3 gene (Fig. 1c).
Hypoxia-induced increases of the cytosolic levels of NLRP3 (a, b) and (pro-) IL-1β proteins (c) in cultured RPE cells. a The cells were cultured 6, 16, and 24 h in the absence (control) and presence of the hypoxia mimetic CoCl2 (150 μM). The level of NLRP3 protein (110 kDa) in cell lysates was determined with Western blot analysis (above). Equal amounts of total protein (35 μg) were used for separation. β-Actin (45 kDa) was used as loading control. Negative controls were done by omission of the first antibodies (below). b Cytosolic level of the NLRP3 protein, as determined by densitometric analysis of Western blot data. The data were normalized to the level of β-actin protein and are expressed as percent of unstimulated control measured after 6 h of stimulation (100%). c The cytosolic level of (pro-) IL-1β protein of cells which were cultured 6 and 24 h in 0.2% O2. The protein level was determined with ELISA and is expressed as percent of unstimulated control (100%; 3.20 ± 0.67 pg/ml). Means ± SEM of 3 (b) and 4 (c) independent experiments using cell lines from different donors. Significant difference vs. unstimulated 6-h control (evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test): *p < 0.05. Significant difference between 6-h and 24-h groups (evaluated with Mann-Whitney U test): ●p < 0.05
In order to investigate whether hypoxia also induces activation of the NLRP3 inflammasome in cultured RPE cells, we determined with ELISA the cytosolic level of (pro-) IL-1β protein. Cell culture in 0.2% O2 had a biphasic effect on the (pro-) IL-1β protein level in cultured RPE cells; it induced a small but significant (p < 0.05) decrease after 6 h and a high increase after 24 h (Fig. 2c). In agreement with a previous study [26], the concentration of IL-1β in the media obtained from cells cultured 6 or 24 h under control and CoCl2-stimulated conditions was below the detection threshold of the ELISA used (not shown).
RPE cell viability
It was suggested that activation of the NLRP3 inflammasome contributes to the degeneration of the RPE in patients with AMD [19, 21]. We investigated whether activation of the NLRP3 inflammasome under hypoxic conditions is associated with a decrease in the viability of cultured RPE cells. In addition to hypoxia, inflammasome activation was induced by addition of L-leucyl-L-leucine methyl ester which produces permeabilization of lysosome membranes [34] and activation of the NLRP3 inflammasome in RPE cells [18, 35]. We found that cell culture for 24 h in a 0.2%-O2 atmosphere induced a significant (p < 0.05) decrease in the viability of RPE cells (Fig. 3). The decrease in cell viability after 24 h of hypoxia corresponds with the time period of inflammasome activation as indicated by the increase of the cytosolic (pro-) IL-1β level (Fig. 2c). In agreement with a previous study [26], the presence of L-leucyl-L-leucine methyl ester in the culture medium did not alter the cell viability under control conditions. However, under hypoxic conditions, additional activation of the NLRP3 inflammasome by L-leucyl-L-leucine methyl ester was associated with a significant (p < 0.05) decrease of the RPE cell viability (Fig. 3). The decrease of the cell viability induced by cell culture in 0.2%-O2 was significantly (p < 0.05) greater in the presence than in the absence of L-leucyl-L-leucine methyl ester (Fig. 3). The data may suggest that inflammasome activation might be one factor that mediates the hypoxic decrease of the cell viability.
Effect of lysosomal destabilization with L-leucyl-L-leucine methyl ester (Leu-Leu-OMe; 1 mM) on the viability of cultured RPE cells under hypoxic conditions. The cells were cultured 6 and 24 h in 0.2% O2 and in the presence of CoCl2 (150 μM), respectively. Means ± SEM of 4 independent experiments using cell lines from different donors. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference between two groups (as indicated by the brackets; evaluated with Mann-Whitney U test): ●p < 0.05
Transcription factor activities involved in mediating the hypoxia-induced expression of the NLRP3 gene
Pharmacological blockers were tested in CoCl2-stimulated cell cultures to investigate which transcription factors are involved in mediating the hypoxic expression of the NLRP3 gene. The CoCl2-induced expression of the NLRP3 gene was significantly (p < 0.05) decreased by a HIF-1 inhibitor [36] and the inhibitor of the cAMP response element-binding protein (CREB), 666-15 (Fig. 4a). The CoCl2-induced expression of the NLRP3 gene was not altered in the presence of inhibitors of signal transducer and activator of transcription 3 (STAT3), Stattic [37], nuclear factor (NF)-κB, CAPE [38], and activator protein-1 (AP-1), SR11302 (Fig. 4a).
Transcription factor activities involved in mediating the hypoxic expression of the NLRP3 gene in cultured RPE cells. The mRNA levels were determined with real-time RT-PCR analysis in cells cultured 6 h in the absence (control) and presence of CoCl2 (150 μM; as indicated by the panels of the bars), and are expressed as folds of unstimulated control. a The following pharmacological agents were tested: a HIF-1 inhibitor (HIF-Inh; 5 μM), the STAT3 inhibitor Stattic (1 μM), the NF-κB inhibitor CAPE (5 μM), the AP-1 inhibitor SR11302 (5 μM), and the CREB inhibitor 666-15 (250 nM). b Transfection of RPE cells with NFAT5 siRNA (siNFAT5; 5 nM) resulted in a reduction of the NFAT5 mRNA level in cells cultured 48 h in control medium. As negative control, non-targeted siRNA (siNon; 5 nM) was used. c Knocking down the gene expression of NFAT5 with siRNA (siNFAT5; 5 nM) did not alter the level of NLRP3 mRNA in cells cultured 6 h in the presence of CoCl2 (150 μM) compared to non-transfected cells (control). siRNA transfection was done 50 h before addition of CoCl2. The numbers of independent experiments using cell lines from different donors are indicated in the bars. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference vs. CoCl2 control: ●p < 0.05
In order to investigate whether the hypoxic expression of the NLRP3 gene in cultured RPE cells might be also dependent on the transcriptional activity of NFAT5, we knocked down NFAT5 with siRNA. Transfection of the cells with NFAT5 siRNA resulted in a decrease of the NFAT5 mRNA level by approximately 50% under unstimulated control conditions (Fig. 4b). On the other hand, knocking down NFAT5 had no effect on the CoCl2-induced expression of the NLRP3 gene (Fig. 4c). The data may suggest that the hypoxic expression of the NLRP3 gene in cultured RPE cells is (in part) dependent on the activities of HIF-1 and CREB.
Receptor signaling implicated in the regulation of the hypoxic expression of NLRP3 and VEGF genes
Inflammasome activation results in the production of IL-1β [17]. An IL-1 receptor antagonist was tested in CoCl2-stimulated cell cultures to investigate whether autocrine/paracrine IL-1 receptor activation is required for the hypoxic expression of the NLRP3 gene. The CoCl2-induced expression of the NLRP3 gene was significantly (p < 0.05) decreased in the presence of the IL-1 receptor antagonist (Fig. 5a). On the other hand, the caspase-1 inhibitor Ac-YVAD-CMK (as well as the inhibitor of VEGF receptor-2, SU1498) did not alter the CoCl2-induced expression of the NLRP3 gene (Fig. 5a). The data may support the assumption that hypoxia induces a release of IL-1β from cultured RPE cells; autocrine/paracrine activation of IL-1 receptors is likely involved in mediating the hypoxic expression of the NLRP3 gene.
Effects of IL-1 and VEGF receptor signaling on the hypoxic expression of NLRP3 (a) and VEGF genes (b, c) in cultured RPE cells. The mRNA levels were determined with real-time RT-PCR analysis in cells cultured 6 (a, b) and 24 h (c) in the absence (control) and presence of CoCl2 (150 μM; as indicated by the panels of the bars), and are expressed as folds of unstimulated control. The following agents were tested: a recombinant human IL-1 receptor antagonist (IL-1RA; 1 μg/ml), the inhibitor of VEGF receptor-2, SU1498 (10 μM), and the caspase-1 inhibitor Ac-YVAD-CMK (Ac-Y; 500 nM). Vehicle control was made with dimethyl sulfoxide (DMSO; 1:1000). The numbers of independent experiments using cell lines from different donors are indicated in or above the bars. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference vs. CoCl2 control: ●p < 0.05
VEGF is the most relevant hypoxia-induced angiogenic factor of the retina [11]. The expression of the VEGF gene in cultured RPE cells was significantly (p < 0.05) increased in the presence of the VEGF receptor-2 antagonist SU1498 under both control and CoCl2-stimulated conditions (Fig. 5b). The IL-1 receptor antagonist increased the VEGF gene expression under unstimulated control conditions (Fig. 5b) and after 24 h of stimulation with CoCl2 (Fig. 5c). The data may support the assumption that autocrine/paracrine VEGF and IL-1β signaling inhibits the VEGF gene expression in cultured RPE cells. The caspase-1 inhibitor Ac-YVAD-CMK had no effects on the levels of NLRP3 and VEGF mRNAs under control and CoCl2-stimulated conditions (Fig. 5a, b). The caspase-1 inhibitor did also not alter the VEGF gene expression and secretion during a 24-h culture in a 0.2%-O2 atmosphere (not shown).
Purinergic receptor signaling is involved in mediating the hypoxic expression of the NLRP3 gene
It has been shown in various cell systems that ATP released from stressed cells is a danger signal which contributes to the activation of the NLRP3 inflammasome [39]. RPE cells express multiple purinergic receptor subtypes including metabotropic P2Y and ionotropic P2X receptors, as well as adenosine receptors [19, 26, 40]. Pharmacological receptor antagonists were tested in CoCl2-stimulated cell cultures to investigate whether purinergic receptor signaling is involved in mediating the hypoxic NLRP3 gene expression in cultured RPE cells. The control and CoCl2-induced expression of the NLRP3 gene was significantly (p < 0.05) decreased in the presence of the ATP-hydrolyzing enzyme apyrase (Fig. 6a). This finding may support the assumption that a release of endogenous ATP is required for the full induction of the constitutive and hypoxic transcription of the NLRP3 gene in cultured RPE cells. We found in agreement with a previous study [26] that the constitutive expression of the NLRP3 gene is significantly (p < 0.05) decreased in the presence of the P2Y1 receptor antagonist MRS2179 (Fig. 6a). This finding might indicate that the transcription of the NLRP3 gene under control conditions is (at least in part) induced by autocrine/paracrine activation of P2Y1 receptors. However, the CoCl2-induced expression of the NLRP3 gene was not altered by the P2Y1 receptor antagonist MRS2179 but was significantly (p < 0.05) decreased by the P2Y2 receptor antagonist AR-C 118925XX and by the adenosine A1 receptor antagonist DPCPX (Fig. 6a).
Involvement of purinergic receptor signaling in mediating the hypoxic expression of NLRP3 (a) and VEGF genes (b) in cultured RPE cells. mRNA levels were determined with real-time RT-PCR analysis. mRNA levels are expressed as folds of unstimulated control. a The cells were cultured 6 h in the absence (control) and presence of CoCl2 (150 μM). b The cells were cultured 24 h in a 0.2%-O2 atmosphere and in the presence of CoCl2 (150 μM), respectively. The following agents were tested: the ATP/ADP phosphohydrolase apyrase (10 U/ml), the P2Y1 receptor antagonist MRS2179 (30 μM), the P2Y2 receptor antagonist AR-C 118925XX (AR-C; 10 μM), the P2X7 receptor antagonist A-438079 (50 nM), the adenosine A1 receptor antagonist DPCPX (50 nM), the adenosine A2A receptor antagonist CSC (200 nM), the ecto-ATPase inhibitor ARL-67156 (50 μM), the ectonucleotidase inhibitor AOPCP (250 μM), the pannexin-blocking peptide 10panx (200 μM), and the scrambled control peptide 10panxScr (200 μM). Vehicle control was made with dimethyl sulfoxide (DMSO; 1:1000). The numbers of independent experiments using cell lines from different donors are indicated in or above the bars. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference vs. low-O2 and CoCl2 control, respectively: ●p < 0.05
The P2X7 receptor antagonist A-438079, the ecto-ATPase inhibitor ARL-67156, and the ectonucleotidase inhibitor AOPCP had also no effects on the CoCl2-induced expression of the NLRP3 gene (Fig. 6a). The data could be explained with the assumption that a release of ATP and adenosine from cultured RPE cells and autocrine/paracrine activation of P2Y2 and adenosine A1 receptors contribute to the induction of the NLRP3 gene expression under hypoxic conditions. The adenosine A2A receptor antagonist CSC increased significantly (p < 0.05) the expression level of the NLRP3 gene under CoCl2-induced conditions (Fig. 6a). We found that the pannexin-blocking peptide 10panx decreased the CoCl2-induced expression of the NLRP3 gene to a similar extent like apyrase, while a scrambled control peptide had no effect (Fig. 6a). The data might indicate that hypoxia induces a pannexin-dependent release of ATP from cultured RPE cells.
Purinergic receptor signaling is involved in the hypoxic expression of the VEGF gene
The hypoxic expression of the VEGF gene was significantly (p < 0.05) suppressed by the ATP/ADP phosphohydrolase apyrase and the P2Y2 receptor antagonist AR-C 118925XX (Fig. 6b). In addition, the pannexin-blocking peptide 10panx decreased significantly (p < 0.05) the hypoxic expression of the VEGF gene (Fig. 6b). The adenosine A2A receptor antagonist CSC increased the hypoxic expression of the VEGF gene under low-O2 conditions, but not in the presence of CoCl2 (Fig. 6b). The data may support the assumption that a pannexin-dependent release of ATP and autocrine/paracrine P2Y2 receptor signaling also contribute to the full induction of the VEGF gene expression in cultured RPE cells under hypoxic conditions.
Purinergic receptor signaling is involved in the hypoxic secretion of VEGF
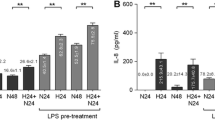
In order to investigate whether purinergic receptor signaling is required for the hypoxic secretion of VEGF from cultured RPE cells, the level of VEGF protein in the cultured media was measured with ELISA. As shown in Fig. 7, hypoxia induced by a 0.2%-O2 atmosphere or by addition of CoCl2 to the medium induced significant (p < 0.05) increases in the VEGF content of the cultured media. The hypoxic secretion of VEGF was significantly (p < 0.05) decreased in the presence of the ATP/ADP phosphohydrolase apyrase and the P2Y2 receptor antagonist AR-C 118925XX, respectively (Fig. 7). The hypoxic secretion of VEGF was not altered in the presence of the adenosine A1 receptor antagonist DPCPX, an IL-1 receptor antagonist, and the caspase-1 inhibitor Ac-YVAD-CMK (Fig. 7). The data may be consistent with the assumption that autocrine/paracrine P2Y2 receptor activation is required for the full secretion of VEGF from cultured RPE cells under hypoxic conditions.
Involvement of P2Y2 receptor signaling in mediating the hypoxic secretion of VEGF from cultured RPE cells. The cells were cultured 24 h in a 0.2%-O2 atmosphere and in the presence of CoCl2 (150 μM), respectively. The level of VEGF-A165 protein in the cultured media was determined with ELISA and is expressed in percent of the unstimulated control (100%). The following agents were tested: the ATP/ADP phosphohydrolase apyrase (10 U/ml), the P2Y2 receptor antagonist AR-C 118925XX (AR-C; 10 μM), the adenosine A1 receptor antagonist DPCPX (50 nM), a recombinant human IL-1 receptor antagonist (IL-1RA; 1 μg/ml), and the caspase-1 inhibitor Ac-YVAD-CMK (Ac-Y; 500 nM). Vehicle control was made with dimethyl sulfoxide (DMSO; 1:1000). The numbers of independent experiments using cell lines from different donors are indicated in the bars. Significant differences were evaluated with one-way ANOVA followed by Bonferroni’s multiple comparison test. Significant difference vs. unstimulated control: *p < 0.05. Significant difference vs. low-O2 and CoCl2 control, respectively: ●p < 0.05
Discussion
It was suggested that activation of the NLRP3 inflammasome, which is expressed in the RPE of patients with AMD [18], is implicated in mediating the degeneration of the RPE in geographic atrophy [19, 21] and the development of choroidal neovascularization [20]. A main pathogenic condition of AMD is hypoxia of the outer retina resulting from the decrease of the choroidal blood flow and accumulation of lipoproteins in and beneath the RPE [4,5,6,7,8,9]. Hypoxia of the outer retina stimulates the production of angiogenic factors by the RPE that induce choroidal neovascularization [10]. In the present study, we investigated whether hypoxia induces priming and activation of the NLRP3 inflammasome in cultured RPE cells. We found that cell culture in a low-O2 atmosphere is associated with a priming of the NLRP3 inflammasome, i.e., expression of NLRP3 and pro-IL-1β genes (Fig. 1b). In addition, the gene of the adaptor protein ASC (which binds procaspase-1 during inflammasome formation) is transcriptionally activated under hypoxic conditions (Fig. 1b, c). The expression of NLRP2 and pro-IL-18 genes was not altered (Fig. 1b). The finding that the IL-18 gene expression was not altered under hypoxic conditions (Fig. 1b, c) is in agreement with various studies which showed that IL-18, but not IL-1β, is constitutively expressed in RPE cells [41] and that NLRP3 inflammasome activation in a RPE cell line results in a production of IL-1β, but not of IL-18 [42]. The finding that hypoxia does not induce expression of the procaspase-1 gene (Fig. 1b) is consistent with a study in macrophages which showed that lipopolysaccharide-induced priming is characterized by NLRP3 and pro-IL-1β gene expression, but no alteration of the procaspase-1 mRNA level [43].
Caspase-1, which cleaves pro-IL-1β, might be activated by various molecular pathways mediated, for example, by the activated NLRP3 inflammasome, the AIM2 inflammasome, and by a direct interaction of caspase-4 and procaspase-1 [17, 44,45,46]. Caspase-4 may be also essential for efficient NLRP3 inflammasome-dependent production of IL-1β [44]. We found that hypoxia also activates the transcription of AIM2 and procaspase-4 genes (Fig. 1b, c). Further research is required to investigate whether hypoxia also induces AIM2 inflammasome- and caspase-4-mediated production of IL-1β in RPE cells and whether these pathways play a role in mediating the retinal inflammation in AMD.
We found that hypoxia had a biphasic effect on the (pro-) IL-1β protein level in cultured RPE cells, i.e., a decrease after 6 h and a strong increase after 24 h of hypoxia (Fig. 2c). Because the increase of the NLRP3 protein level was observed after 16 and 24 h of hypoxic stimulation (Fig. 2a, b), we assume that the increase in the cytosolic (pro-) IL-1β level (Fig. 2c) is caused by both production of pro-IL-1β and inflammasome-mediated production of mature IL-1β. The decrease in the cytosolic (pro-) IL-1β level after 6 h of hypoxia (Fig. 2c) might be caused by the secretion of stored preformed IL-1β. Hypoxia-mediated secretion of IL-1β from RPE cells is also suggested by the effects of an IL-1 receptor antagonist on the expression of VEGF and NLRP3 genes (Fig. 5a, c). We did not detect IL-1β in the media obtained from cells cultured 6 or 24 h under control and CoCl2-stimulated conditions with the ELISA (not shown). Because we found effects of an IL-1 receptor antagonist on the hypoxic gene expression (Fig. 5a, c), we assume that the main part of the secreted IL-1β reentered the cells via receptor-mediated endocytosis and was degraded intracellularly. The effect of the IL-1 receptor antagonist on the gene expression of VEGF under control conditions (Fig. 5b) may suggest that there is a constitutive secretion of IL-1β from the cells. This may correspond with our finding that there is a low level of NLRP3 protein in the cells under unstimulated control conditions (Fig. 2a).
We found that the caspase-1 inhibitor Ac-YVAD-CMK had no effects on the levels of NLRP3 and VEGF mRNAs under control and hypoxic conditions (Fig. 5a, b). It might be conceivable that the effects of the IL-1 receptor antagonist on the hypoxic expression of VEGF and NLRP3 genes (Fig. 5a, c) are caused by the secretion of stored preformed IL-1β and that IL-1β produced by newly formed inflammasome protein complexes does not contribute to the regulation of the NLRP3 and VEGF gene expression under the present study conditions. Whether newly formed IL-1β regulates the NLRP3 and VEGF gene expression during longer time periods remains to be proven in future investigations. It was described that NLRP3 inflammasome activation in RPE cells induced by lysosomal membrane permeabilization is associated with a reduction of the constitutive secretion of VEGF from RPE cells [35]. We found that the IL-1 receptor antagonist increased the level of VEGF mRNA under control and hypoxic conditions (Fig. 5b, c). This suggests that autocrine/paracrine IL-1 receptor signaling induced by a release of IL-1β suppresses the expression of the VEGF gene. On the other hand, the secretion of VEGF is independent on both inflammasome activation and IL-1 receptor signaling (Fig. 7).
Both cell culture in a low-O2 atmosphere and chemical hypoxia stimulated the expression of the NLRP3 gene (Fig. 1c). However, there were various differences in the effects of both conditions, e.g., on the expression of pro-IL-1β and procaspase-1 genes (Fig. 1b, c). We also found that the level of VEGF mRNA is lower in the presence of a low-O2 atmosphere than in the presence of CoCl2 (Fig. 6b). The reasons for the differences are unclear but could be explained partially with the assumptions that CoCl2 induces (in addition to hypoxia) oxidative stress and that it also interacts with calcium channels and calcium-dependent enzymes. Oxidative stress was shown to activate the NLRP3 inflammasome in RPE cells [23, 47]. Further investigations are required to explore the (partially different) mechanisms of low-O2 and CoCl2 on the priming and activation of the NLRP3 inflammasome in RPE cells.
We described recently that the NLRP3 inflammasome in cultured RPE cells is primed and activated following elevation of the extracellular osmolarity [26]. As suggested by the additive effects of extracellular hyperosmolarity and hypoxia on the expression level of the NLRP3 gene (Fig. 1d) and the different time-dependencies of both effects, it is likely that the hyperosmotic and hypoxic expressions of the NLRP3 gene in cultured RPE cells are mediated by different signal transduction mechanisms. The hypoxic expression of the NLRP3 gene is (at least in part) dependent on the transcriptional activities of HIF-1 and CREB (Fig. 4a), whereas the hyperosmotic expression of the NLRP3 gene is dependent on the activities of HIF-1 and NFAT5 [26]. The present data are in agreement with previous studies which showed in various cell systems that HIF activity is implicated in the induction of NLRP3 inflammasome activation [48, 49]. In addition, we found that an IL-1 receptor antagonist decreased the hypoxic expression of the NLRP3 gene (Fig. 5a), suggesting that autocrine/paracrine IL-1β signaling is a priming signal for hypoxic RPE cells.
The findings that apyrase and a pannexin-blocking peptide decreased the hypoxic expression of the NLRP3 gene (Fig. 6a) may support the assumption that hypoxia induces a pannexin-mediated release of ATP from cultured RPE cells. Similar effects of both compounds were found in respect to the hyperosmotic expression of the NLRP3 gene [26]. Autocrine/paracrine activation of P2Y1 receptors is implicated in mediating both the constitutive and the hyperosmotic expression of the NLRP3 gene [26]. On the other hand, the present data may indicate that activation of P2Y2 receptors contributes to the induction of NLRP3 gene expression under hypoxic conditions (Fig. 6a). The decreasing effect of the A1 receptor antagonist DPCPX on the expression of the NLRP3 gene (Fig. 6a) may support the assumption that hypoxia also induces a release of adenosine from cultured RPE cells. Apparently, adenosine has contrary effects under hypoxic conditions; via activation of A1 receptors, it stimulates the expression of the NLRP3 gene, and via activation of A2A receptors, it decreases the expression of the NLRP3 gene (Fig. 6a). Because inhibition of the ecto-ATPase and ectonucleotidase did not alter the expression level of the NLRP3 gene under hypoxic conditions (Fig. 6a), it is assumed that adenosine is not formed by extracellular degradation of ATP. Interestingly, we found that autocrine/paracrine P2Y2 receptor signaling also contributes to the stimulation of the expression of the VEGF gene (Fig. 6b) and the secretion of VEGF from cultured RPE cells under hypoxic conditions (Fig. 7). Because inhibition of adenosine A1 receptors by DPCPX had no effects on the hypoxic expression of the VEGF gene (Fig. 6b), it may be conceivable that the effects of P2Y2 receptor activation on the expression of NLRP3 and VEGF genes are mediated by different intracellular signal transduction pathways.
In summary, we show that hypoxia induces priming and activation of the NLRP3 inflammasome in cultured RPE cells. Because outer retinal hypoxia is a pathogenic condition of AMD which also stimulates the progression of AMD to the neovascular stage [10], hypoxic priming and activation of the NLRP3 inflammasome in RPE cells could represent a mechanism which contributes to the development of dry and neovascular AMD. Hypoxic inflammasome activation may render RPE cells more susceptible to inflammatory stimuli and other pathogenic factors involved in mediating the degeneration of the RPE. This assumption is supported by the finding that inflammasome activation resulting from lysosomal destabilization induces RPE cell death under hypoxic but not under control conditions (Fig. 3). We found that autocrine/paracrine purinergic receptor signaling is involved in mediating the hypoxic priming of the NLRP3 inflammasome in RPE cells and the gene expression and secretion of VEGF. Because both effects may contribute to the development and progression of AMD, P2Y receptors may represent a target for the development of pharmacological approaches to treat age-related retinal inflammation and degeneration. However, because the present data were obtained in cultured, dedifferentiated RPE cells, the data must be confirmed with differentiated cells or in vivo experiments.
Abbreviations
- AIM:
-
absent in melanoma
- AMD:
-
age-related macular degeneration
- AOPCP:
-
adenosine-5′-O-(α,β-methylene)-diphosphate
- AP:
-
activator protein
- ASC:
-
apoptosis-associated speck-like protein containing a caspase-recruitment domain
- ATP:
-
adenosine 5′-triphosphate
- CAPE:
-
caffeic acid phenethyl ester
- CREB:
-
cAMP response element-binding protein
- DPCPX:
-
8-cyclopentyl-1,3-dipropylxanthine
- HIF:
-
hypoxia-inducible transcription factor
- IL:
-
interleukin
- NFAT:
-
nuclear factor of activated T cell
- NLRC:
-
NLR family CARD domain-containing protein
- NLRP:
-
nucleotide-binding oligomerization domain receptors-like receptor protein
- RPE:
-
retinal pigment epithelium
- siRNA:
-
small interfering RNA
- STAT:
-
signal transducer and activator of transcription
- VEGF:
-
vascular endothelial growth factor
References
Van Leeuwen R, Klaver CC, Vingerling JR, Hofman A, de Jong PT (2003) Epidemiology of age-related maculopathy: a review. Eur J Epidemiol 18(9):845–854
Klein R, Klein BE, Knudtson MD, Meuer SM, Swift M, Gangnon RE (2007) Fifteen-year cumulative incidence of age-related macular degeneration: the Beaver Dam Eye Study. Ophthalmology 114(2):253–262
Gehrs KM, Anderson DH, Johnson LV, Hageman GS (2006) Age-related macular degeneration – emerging pathogenetic and therapeutic concepts. Ann Med 38(7):450–471
Dallinger S, Findl O, Strenn K, Eichler HG, Wolzt M, Schmetterer L (1998) Age dependence of choroidal blood flow. J Am Geriatr Soc 46(4):484–487
Ehrlich R, Kheradiya NS, Winston DM, Moore DB, Wirostko B, Harris A (2009) Age-related ocular vascular changes. Graefes Arch Clin Exp Ophthalmol 247(5):583–591
Kaarniranta K, Sinha D, Blasiak J, Kauppinen A, Vereb Z, Salminen A, Boulton ME, Petrovski G (2013) Autophagy and heterophagy dysregulation leads to retinal pigment epithelium dysfunction and development of age-related macular degeneration. Autophagy 9(7):973–984
Ferrington DA, Sinha D, Kaarniranta K (2016) Defects in retinal pigment epithelial cell proteolysis and the pathology associated with age-related macular degeneration. Prog Retin Eye Res 51:69–89
Feeney-Burns L, Berman ER, Rothman H (1980) Lipofuscin of human retinal pigment epithelium. Am J Ophthalmol 90(6):783–791
Anderson DH, Mullins RF, Hageman GS, Johnson LV (2002) A role for local inflammation in the formation of drusen in the aging eye. Am J Ophthalmol 134(3):411–431
Schlingemann RO (2004) Role of growth factors and the wound healing response in age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol 242(1):91–101
Witmer AN, Vrensen GF, Van Noorden CJ, Schlingemann RO (2003) Vascular endothelial growth factors and angiogenesis in eye disease. Prog Retin Eye Res 22(1):1–29
Ishibashi T, Hata Y, Yoshikawa H, Nakagawa K, Sueishi K, Inomata H (1997) Expression of vascular endothelial growth factor in experimental choroidal neovascularization. Graefes Arch Clin Exp Ophthalmol 235(3):159–167
Xu H, Chen M, Forrester JV (2009) Para-inflammation in the aging retina. Prog Retin Eye Res 28(5):348–368
Cheung CM, Wong TY (2014) Is age-related macular degeneration a manifestation of systemic disease? New prospects for early intervention and treatment. J Intern Med 276(2):140–153
Nita M, Grzybowski A, Ascaso FJ, Huerva V (2014) Age-related macular degeneration in the aspect of chronic low-grade inflammation (pathophysiological parainflammation). Mediat Inflamm 2014:930671
Kauppinen A, Paterno JJ, Blasiak J, Salminen A, Kaarniranta K (2016) Inflammation and its role in age-related macular degeneration. Cell Mol Life Sci 73(9):1765–1786
Latz E, Xiao TS, Stutz A (2013) Activation and regulation of the inflammasomes. Nat Rev Immunol 13(6):397–411
Tseng WA, Thein T, Kinnunen K, Lashkari K, Gregory MS, D'Amore PA, Ksander BR (2013) NLRP3 inflammasome activation in retinal pigment epithelial cells by lysosomal destabilization: implications for age-related macular degeneration. Invest Ophthalmol Vis Sci 54(1):110–120
Kerur N, Hirano Y, Tarallo V, Fowler BJ, Bastos-Carvalho A, Yasuma T, Yasuma R, Kim Y, Hinton DR, Kirschning CJ, Gelfand BD, Ambati J (2013) TLR-independent and P2X7-dependent signaling mediate Alu RNA-induced NLRP3 inflammasome activation in geographic atrophy. Invest Ophthalmol Vis Sci 54(12):7395–7401
Marneros AG (2013) NLRP3 inflammasome blockade inhibits VEGF-A-induced age-related macular degeneration. Cell Rep 4(5):945–958
Fowler BJ, Gelfand BD, Kim Y, Kerur N, Tarallo V, Hirano Y, Amarnath S, Fowler DH, Radwan M, Young MT, Pittman K, Kubes P, Agarwal HK, Parang K, Hinton DR, Bastos-Carvalho A, Li S, Yasuma T, Mizutani T, Yasuma R, Wright C, Ambati J (2014) Nucleoside reverse transcriptase inhibitors possess intrinsic anti-inflammatory activity. Science 346(6212):1000–1003
Doyle SL, Campbell M, Ozaki E, Salomon RG, Mori A, Kenna PF, Farrar GJ, Kiang AS, Humphries MM, Lavelle EC, O'Neill LA, Hollyfield JG, Humphries P (2012) NLRP3 has a protective role in age-related macular degeneration through the induction of IL-18 by drusen components. Nat Med 18(5):791–798
Kauppinen A, Niskanen H, Suuronen T, Kinnunen K, Salminen A, Kaarniranta K (2012) Oxidative stress activates NLRP3 inflammasomes in ARPE-19 cells – implications for age-related macular degeneration (AMD). Immunol Lett 147(1–2):29–33
Anderson OA, Finkelstein A, Shima DT (2013) A2E induces IL-1ß production in retinal pigment epithelial cells via the NLRP3 inflammasome. PLoS One 8(6):e67263
Brandstetter C, Mohr LK, Latz E, Holz FG, Krohne TU (2015) Light induces NLRP3 inflammasome activation in retinal pigment epithelial cells via lipofuscin-mediated photooxidative damage. J Mol Med (Berl) 93(8):905–916
Prager P, Hollborn M, Steffen A, Wiedemann P, Kohen L, Bringmann A (2016) P2Y1 receptor signaling contributes to high salt-induced priming of the NLRP3 inflammasome in retinal pigment epithelial cells. PLoS One 11(10):e0165653
Klein R, Klein BE, Tomany SC, Cruickshanks KJ (2003) The association of cardiovascular disease with the long-term incidence of age-related maculopathy: the Beaver Dam Eye Study. Ophthalmology 110(6):1273–1280
Van Leeuwen R, Ikram MK, Vingerling JR, Witteman JC, Hofman A, de Jong PT (2003) Blood pressure, atherosclerosis, and the incidence of age-related maculopathy: the Rotterdam Study. Invest Ophthalmol Vis Sci 44(9):3771–3777
Lifton RP, Gharavi AG, Geller DS (2001) Molecular mechanisms of human hypertension. Cell 104(4):545–556
Reichenbach A, Bringmann A (2016) Purinergic signaling in retinal degeneration and regeneration. Neuropharmacology 104:194–211
Chen R, Hollborn M, Grosche A, Reichenbach A, Wiedemann P, Bringmann A, Kohen L (2014) Effects of the vegetable polyphenols epigallocatechin-3-gallate, luteolin, apigenin, myricetin, quercetin, and cyanidin in retinal pigment epithelial cells. Mol Vis 20:242–258
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2−ΔΔCT method. Methods 25(4):402–408
An WG, Kanekal M, Simon MC, Maltepe E, Blagosklonny MV, Neckers LM (1998) Stabilization of wild-type p53 by hypoxia-inducible factor 1α. Nature 392(6674):405–408
Thiele DL, Lipsky PE (1990) The action of leucyl-leucine methyl ester on cytotoxic lymphocytes requires uptake by a novel dipeptide-specific facilitated transport system and dipeptidyl peptidase I-mediated conversion to membranolytic products. J Exp Med 172(1):183–194
Mohr LK, Hoffmann AV, Brandstetter C, Holz FG, Krohne TU (2015) Effects of inflammasome activation on secretion of inflammatory cytokines and vascular endothelial growth factor by retinal pigment epithelial cells. Invest Ophthalmol Vis Sci 56(11):6404–6413
Lee K, Lee JH, Boovanahalli SK, Jin Y, Lee M, Jin X, Kim JH, Hong YS, Lee JJ (2007) (Aryloxyacetylamino) benzoic acid analogues: a new class of hypoxia-inducible factor-1 inhibitors. J Med Chem 50(7):1675–1684
Schust J, Sperl B, Hollis A, Mayer TU, Berg T (2006) Stattic: a small-molecule inhibitor of STAT3 activation and dimerization. Chem Biol 13(11):1235–1242
Natarajan K, Singh S, Burke TR Jr, Grunberger D, Aggarwal BB (1996) Caffeic acid phenethyl ester is a potent and specific inhibitor of activation of nuclear transcription factor NF-κB. Proc Natl Acad Sci U S A 93(17):9090–9095
Bours MJ, Dagnelie PC, Giuliani AL, Wesselius A, Di Virgilio F (2011) P2 receptors and extracellular ATP: a novel homeostatic pathway in inflammation. Front Biosci (Schol Ed) 3:1443–1456
Housley GD, Bringmann A, Reichenbach A (2009) Purinergic signaling in special senses. Trends Neurosci 32:128–141
Shi G, Chen S, Wandu WS, Ogbeifun O, Nugent LF, Maminishkis A, Hinshaw SJ, Rodriguez IR, Gery I (2015) Inflammasomes induced by 7-ketocholesterol and other stimuli in RPE and in bone marrow-derived cells differ markedly in their production of IL-1β and IL-18. Invest Ophthalmol Vis Sci 56(3):1658–1664
Piippo N, Korkmaz A, Hytti M, Kinnunen K, Salminen A, Atalay M, Kaarniranta K, Kauppinen A (2014) Decline in cellular clearance systems induces inflammasome signaling in human ARPE-19 cells. Biochim Biophys Acta 1843(12):3038–3046
Bauernfeind F, Bartok E, Rieger A, Franchi L, Núñez G, Hornung V (2011) Cutting edge: reactive oxygen species inhibitors block priming, but not activation, of the NLRP3 inflammasome. J Immunol 187(2):613–617
Sollberger G, Strittmatter GE, Kistowska M, French LE, Beer HD (2012) Caspase-4 is required for activation of inflammasomes. J Immunol 188(4):1992–2000
Cheung KT, Sze DM, Chan KH, Leung PH (2018) Involvement of caspase-4 in IL-1β production and pyroptosis in human macrophages during dengue virus infection. Immunobiology 223(4–5):356–364
Lugrin J, Martinon F (2018) The AIM2 inflammasome: sensor of pathogens and cellular perturbations. Immunol Rev 281(1):99–114
Piippo N, Korhonen E, Hytti M, Kinnunen K, Kaarniranta K, Kauppinen A (2018) Oxidative stress is the principal contributor to inflammasome activation in retinal pigment epithelium cells with defunct proteasomes and autophagy. Cell Physiol Biochem 49(1):359–367
Nicholas SA, Bubnov VV, Yasinska IM, Sumbayev VV (2011) Involvement of xanthine oxidase and hypoxia-inducible factor 1 in Toll-like receptor 7/8-mediated activation of caspase 1 and interleukin-1β. Cell Mol Life Sci 68(1):151–158
Tannahill GM, Curtis AM, Adamik J, Palsson-McDermott EM, McGettrick AF, Goel G, Frezza C, Bernard NJ, Kelly B, Foley NH, Zheng L, Gardet A, Tong Z, Jany SS, Corr SC, Haneklaus M, Caffrey BE, Pierce K, Walmsley S, Beasley FC, Cummins E, Nizet V, Whyte M, Taylor CT, Lin H, Masters SL, Gottlieb E, Kelly VP, Clish C, Auron PE, Xavier RJ, O'Neill LA (2013) Succinate is an inflammatory signal that induces IL-1β through HIF-1α. Nature 496(7444):238–242
Acknowledgments
The authors thank Ute Weinbrecht for excellent technical assistance.
Funding
This research was supported by grants from the Deutsche Forschungsgemeinschaft (KO 1547/7-1 to L.K.) and the Geschwister Freter Stiftung (Hannover, Germany) to P.W.
Author information
Authors and Affiliations
Contributions
LK, AB, and MH conceived and designed the experiments. FD, PP, and MH performed the experiments. FD, AB, and MH analyzed and interpreted the data. PW, LK, and MH supervised research personnel. FD, AB, and MH drafted the manuscript. PW and LK made critical revision of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Fabian Doktor declares that he has no conflict of interest.
Philipp Prager declares that he has no conflict of interest.
Peter Wiedemann declares that he has no conflict of interest.
Leon Kohen declares that he has no conflict of interest.
Andreas Bringmann declares that he has no conflict of interest.
Margrit Hollborn declares that she has no conflict of interest.
Ethical approval
All experimental protocols in this study were approved by the Ethics Committee of the University of Leipzig (approval #745, 07/25/2011).
Rights and permissions
About this article
Cite this article
Doktor, F., Prager, P., Wiedemann, P. et al. Hypoxic expression of NLRP3 and VEGF in cultured retinal pigment epithelial cells: contribution of P2Y2 receptor signaling. Purinergic Signalling 14, 471–484 (2018). https://doi.org/10.1007/s11302-018-9631-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11302-018-9631-6