Abstract
Background
It is common for Chinese American breast cancer survivors to believe that having cancer is a stigmatizing condition. Little research exists on how this might affect their quality of life (QoL) and through which psychological processes.
Objective
In the present study, we examined the association between self-stigma and QoL in a sample of Chinese American breast cancer survivors and tested the potential mediating roles of intrusive thoughts and posttraumatic growth in this relationship.
Methods
One hundred and thirty-six Chinese American breast cancer survivors completed a questionnaire packet assessing their levels of self-stigma, intrusive thoughts, posttraumatic growth, and QoL.
Results
As hypothesized, findings indicated a significant negative correlation between self-stigma and QoL. Findings from a path analysis indicated significant indirect effects of self-stigma on QoL through intrusive thoughts and posttraumatic growth—the negative correlation between self-stigma and QoL was completely mediated by more intrusive thoughts and less posttraumatic growth.
Conclusions
Our findings suggest that self-stigma may harm QoL among Chinese American breast cancer survivors by leading to more intrusive thoughts and not focusing on posttraumatic growth. To attenuate the negative impact of self-stigma on QoL among Chinese American breast cancer survivors, cognition-focused interventions should be utilized to reduce intrusive thoughts and foster posttraumatic growth.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Recent reviews indicate that it is common for Chinese American breast cancer survivors to believe that having cancer is a stigmatizing condition in their community [1, 2]. Although this past research sheds important light on the experiences of Chinese American breast cancer survivors, no known studies have investigated the consequences of perceiving one’s breast cancer as a stigmatizing condition on well-being among Chinese Americans. The current research aimed to begin to fill this gap in the literature by examining how internalizing stigma regarding one’s breast cancer may be associated with lower quality of life (QoL) for Chinese American breast cancer survivors.
Social stigma occurs when a person possesses an identity or attribute that causes that person to be negatively stereotyped, devalued, and discriminated against—resulting in unequal outcomes [3,4,5]. Indeed, decades of research have found that people who possess socially stigmatized identities have worse health outcomes than their non-stigmatized counterparts (see [6, 7] for reviews). These health disparities occur because stigmatized individuals are treated unfairly in a variety of different contexts (e.g., education, housing, healthcare; [6]), and also because they experience increased levels of stress as a result of their stigmatized status [8]. According to the minority stress model [8], stigmatized individuals are exposed to two unique types of stressors that increase their risk for negative health consequences: distal stressors and proximal stressors. Distal stressors are external to the individual, such as social rejection or perceiving discrimination from others; proximal stressors are internal to the individual, such as attempting to conceal a stigmatized status from others or self-stigma. Self-stigma occurs when one endorses negative stereotypes about people with one’s own stigmatized status and believes these negative stereotypes are true of one’s self [9], which can affect how stigmatized individuals interact with others (e.g., avoiding others, worrying about how others will view them).
To what extent are breast cancer survivors stigmatized? Although there is limited research on this topic, the existing research suggests that breast cancer survivors are stigmatized, but, perhaps, not as much as people with other types of cancer. The stigmatization of cancer, in general, is thought to originate from people’s fear of their own death—that interacting with cancer patients and survivors makes people uncomfortable because it reminds them of their own mortality, which can lead to cancer survivors being socially rejected and treated unfairly [10, 11]. Type of cancer can affect the degree of stigma—people with cancers that are perceived to be controllable (e.g., lung cancer) are more stigmatized than people with cancers that are perceived to be less controllable (e.g., breast cancer) [10, 12]. Thus, compared to people with lung cancer, people with breast cancer should be less stigmatized because unlike people with lung cancer, people with breast cancer are not perceived to have caused to their disease through their behavioral and lifestyle choices [13]. Moreover, it has recently been argued that the stigma of breast cancer is waning because of “pink ribbon” campaigns that have portrayed breast cancer survivors as courageous, inspirational, optimistic, and upbeat [10]. However, these campaigns may have not reduced the stigma of breast cancer among minority groups, including Chinese Americans.
Consistent with the minority stress model [8], even if societal perceptions of breast cancer survivors are becoming less negative, proximal stressors, such as self-stigma, may still harm the QoL of breast cancer survivors. Past research has found that more self-stigma is associated with worse QoL for cancer patients and survivors [14, 15]. The past research that has found evidence for this association, however, is limited in three ways. First, with a few exceptions [16, 17], the vast majority of this research has not focused on breast cancer survivors (e.g., [14, 15, 18],). Second, for the studies that examined breast cancer survivors, none specifically focused on the experiences of Chinese American breast cancer survivors [16]. Given that recent reviews have found that stigma is a common concern for Chinese American breast cancer survivors (e.g., [19, 20]), it is important to understand how stigma may be affecting their QoL. Finally, none of these past studies investigated the psychological mechanisms underlying the relationship between self-stigma and QoL. The current research attempts to address all three of these gaps.
In addition to investigating the possible association between self-stigma and QoL for Chinese American breast cancer survivors, the current research investigated the extent to which intrusive thoughts and posttraumatic growth (i.e., construing traumatic events, such as cancer, as opportunities for growth and positive change) mediate this association. The experience of self-stigma may serve as a filtering lens, coloring stigmatized individuals’ way of thinking, and the interpretation of their experience [21]. On one hand, past research indicates that more cancer-related intrusive thoughts can be associated with lower QoL for breast cancer survivors under certain conditions [22] and that coping with stigma by engaging in ruminative thought is associated with worse outcomes [23]. On the other hand, past research indicates that posttraumatic growth is a common experience for Chinese American breast cancer survivors [24]. Posttraumatic growth is generally associated with better health and psychological well-being [25, 26] and has been found to buffer against the harmful effects of stigma for lung cancer patients [27].
The present research
Using the minority stress model as a theoretical framework [8], the current research investigated the relationship between self-stigma and QoL and the possible psychological mechanisms underlying the relationship between self-stigma and QoL for Chinese American breast cancer survivors. It was hypothesized that self-stigma would predict lower QoL, and that this relationship would be mediated by more intrusive thoughts and less posttraumatic growth. The goal of this study is to fill an important gap in literature and inform interventions aimed at improving the QoL of Chinese American breast cancer survivors.
Method
Participants
One hundred thirty-six Chinese American breast cancer survivors participated in this study. Adult women were eligible if they (1) had been diagnosed with breast cancer, (2) had completed breast cancer surgery within 5 years, and (3) self-identified as comfortable speaking, reading, and writing in Chinese (i.e., Mandarin or Cantonese).
This study utilized data from the baseline assessment of a larger, intervention study [28]. The sample size was determined by power analysis so that the sample size would be sufficient to test the main hypotheses for the intervention study [28]. To determine the power in the proposed mediation analysis, a post hoc power analysis was conducted based on guidelines by Thoemmes et al. [29]. The Monte Carlo power analysis was conducted, and results indicated the current sample size yielded 94.1% power in testing the total indirect effect of self-stigma.
Procedure
This study was approved by the institutional review board. The entire study was conducted in Chinese. Participants were recruited from Los Angeles, New York, and Houston metropolitan areas, in collaboration with the Herald Cancer Association (HCA), a community-based Chinese cancer organization. Potential participants were introduced to the study at cultural events, educational conferences, and support groups. After participants indicated initial interest in the study, they were contacted by community researcher who screened them for eligibility over the phone. Eligible participants were invited to participate in the study. The informed consent and baseline assessment packet were sent to participants by mail. Participants received monetary compensation (US$20) for completing the baseline assessment. All study materials were presented in Chinese.
Measures
Chinese-language versions of all of the measures were available with the exception of the Posttraumatic Growth Inventory [30]. The Posttraumatic Growth Inventory was translated into Chinese by our bilingual research team using the backward translation method and procedure [31]. One team member translated the English items into Chinese, a second team member back-translated the Chinese items into English, and a third team member compared the back-translated English items with the original English items, and made suggestions for revision. The procedure was repeated until all translated Chinese items achieved equivalent meaning with the original English items.
Self-stigma
The current study measured self-stigma of breast cancer using an adapted four-item version of the Self-Stigma Scale, which assesses affective, behavioral, and cognitive dimensions of self-stigma [32]. This scale was originally developed and tested in Chinese in samples of people with mental illness, sexual minorities, and immigrants [32], and it has been adapted to assess self-stigma in clinical samples such as people with diabetes [33] and people living with HIV [34]. In the current study, four items from the Self-Stigma Scale were adapted to the context of breast cancer survivorship, including “I fear that others would know that I am a breast cancer survivor,” “I estrange myself from others because I am a breast cancer survivor,” “The identity of being a breast cancer survivor taints my life,” and “I avoid interacting with others because I am a breast cancer survivor.” Participants’ responses to these items were measured on scales ranging from 1 (strongly disagree) to 4 (strongly agree). Higher scores indicate greater self-stigma. These items were chosen based on findings from a qualitative study that examined the psychosocial challenges of Chinese American breast cancer survivors [35]. In addition, our research team conducted a confirmatory factor analysis on this 4-item self-stigma scale in the present sample—results indicated a satisfactory model fit for a single factor, \(\chi^{ 2}_{(2)}\) = 0.970, p = .616, CFI = 1.000; TLI = 1.012; RMSEA = .000. Moreover, the 4-item self-stigma scale displayed excellent internal reliability (α = .93) in the present sample.
Intrusive thoughts
The seven-item intrusion subscale of the Impact of Event Scale (IES) [36] was used to measure how frequently participants have cancer-related intrusive thoughts. A sample item is “I thought about it when I didn’t mean to.” Participants’ responses were measured on scales ranging from 0 (not at all) to 5 (often). The IES has been validated in a Chinese sample [37]. Higher scores indicate greater intrusive thoughts. In the present sample, the intrusion subscale displayed excellent internal reliability (α = .89).
Posttraumatic growth
The 21-item posttraumatic growth inventory (PTGI) [30] was used to assess participants’ positive changes after experiencing negative life events. The PTGI consists of 5 subscales (i.e., new possibilities, relating to others, personal strength, spiritual change, and appreciation of life). Participants responded using 6-point scales ranging from 0 (I did not experience this change as a result of my crisis) to 5 (I experienced this change to a very great degree as a result of my crisis). Participants had a general understanding that “crisis” referred to their breast cancer diagnosis and treatment. Sample items for each subscale are, “I established a new path for my life” (new possibilities), “A sense of closeness with others” (relating to others), “Knowing I can handle difficulties” (personal strength), “A better understanding of spiritual matters” (spiritual change), and “An appreciation for the value of my own life” (appreciation of life). All 21 items from the PTGI were summed to create a total score, with higher numbers indicating more posttraumatic growth. In the present sample, PTGI displayed excellent internal reliability (α = .96).
Quality of life
The Chinese version of the Functional Assessment of Cancer Therapy-Breast (FACT-B) [38, 39] was used to measure different facets of participants’ QoL, including physical (e.g., “I have a lack of energy”), emotional (e.g., “I am losing hope in the fight against my illness”), social/family (e.g., “I feel close to my friends”), and functional well-being (e.g., “I am able to work”), as well as their other concerns about breast cancer. Participants’ responses were measured on scales ranging from 0 (not at all) to 4 (extremely). The FACT-B total score was used. Higher scores indicate better QoL. In the present sample, FACT-B displayed excellent internal reliability (α = .90).
Data analysis
Descriptive statistics were calculated for demographic and medical variables. Chi-square tests were used to examine the relationship between demographic and medical variables and QoL. Bivariate correlations were examined among self-stigma, intrusive thoughts, posttraumatic growth, and QoL. Path analysis was used to examine the goodness of fit of the mediation model. The indicators of model fit included (1) root mean square error of approximation (RMSEA) [40], an absolute index of overall model fit; (2) Tucker–Lewis Index (TLI) [41]; and (3) Comparative Fit Index (CFI) [41], relative indexes of model fit compared to the null model. RMSEA fit index values less than .05 are indicative of good model fit [42]. TLI and CFI descriptive index values greater than .95 are indicative of good model fit [43]. Bootstrapping was employed to estimate the statistical significance of the indirect effects; absence of zero in the 95% confidence interval suggests significant indirect effects [44].
Results
Descriptive statistics
Participants’ ages ranged between 34 and 84 years old (M = 57.75, SD = 9.22), 61.5% received college education or above, 65.7% were married; the majority (67.9%) were diagnosed with breast cancer at stage I or II, and the mean time since diagnosis was 27.17 months (SD = 19.31 months). The majority of the sample (71.8%) reported a household income of $45,000 or less annually, with 37.1% reporting an annual household income of $15,000 or less. Table 1 displays demographic and medical variables for the current sample.
Correlational analyses
Results from a series of correlation analysis (for continuous variables) and Chi-square tests (for ordinal and nominal variables) indicated that, of these demographic and medical variables, only education level (\(\upchi^{ 2}_{(1)}\) = 4.66, p = 0.03) and annual household income (\(\upchi^{ 2}_{(1)}\) = 14.52, p < 0.001) were significantly associated with QoL. Based on these findings, educational level and household income were used on covariates in the later mediation analysis. Table 2 displays descriptive statistics and bivariate correlations for the variables of interest. Findings from these correlational analyses revealed that, consistent with study hypotheses, self-stigma was positively associated with intrusive thoughts, negatively associated with posttraumatic growth, and negatively associated with QoL. Additionally, intrusive thoughts were negatively associated with QoL. Finally, posttraumatic growth was positively associated with QoL.
Mediation analysis
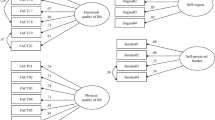
It was hypothesized that both intrusive thoughts and posttraumatic growth would mediate the relationship between self-stigma and QoL—specifically, that self-stigma would be positively related to intrusive thoughts, which in turn, would be negatively related to QoL, and that self-stigma would be negatively related to posttraumatic growth, which in turn, would be positively related to QoL. A single path-analytic model, displayed in Fig. 1, was run to test these mediation hypotheses using MPlus 7.0 [43]. As mentioned above, education level and income were controlled in analysis.
Results indicated that this path-analytic model explained 54.5% of the variability in QoL and fit the data well, \(\chi^{ 2}_{(1)}\) = 0.54, p = .46, CFI = 1.00, TLI = 1.03, RMSEA = .00.
Consistent with hypotheses, the total indirect effect of self-stigma on QoL—through intrusive thoughts and posttraumatic growth simultaneously—was statistically significant (standardized total indirect effect = − .43, p < .001, 95% CI − .54 to − .31). The indirect effect of self-stigma on QoL through intrusive thoughts was significant (standardized indirect effect = − .34, p < .001, 95% CI − .45 to − .24)—specifically, more self-stigma was associated with more intrusive thoughts, which in turn, was associated with lower QoL. The indirect effect of self-stigma on QoL through posttraumatic growth was also significant (standardized indirect effect = − .08, p = .02, 95% CI − .15 to − .02)—specifically, more self-stigma was associated less posttraumatic growth, which in turn, was associated with lower QoL. As expected, when controlling for intrusive thoughts and posttraumatic growth, the direct effect of self-stigma on QoL was not significant (standardized indirect effect = − .01, p = .92, 95% CI − .14 to .12)—indicating that intrusive thoughts and posttraumatic growth mediated the relationship between self-stigma on QoL.
Discussion
This study is the first study to examine the relationship between self-stigma and QoL in a sample of Chinese American breast cancer survivors, and to explore the potential psychological processes (i.e., intrusive thoughts and posttraumatic growth) that may underlie this relationship. Overall, the research hypotheses were supported. Self-stigma was found to be negatively associated with QoL, and this association was mediated by more intrusive thoughts and less posttraumatic growth. These findings suggest that self-stigma may lead to altered cognitions, either increased negative thoughts (i.e., intrusive thoughts) and/or reduced positive thoughts (i.e., posttraumatic growth), which have an impact on Chinese American breast cancer survivors’ QoL. An alternative way to interpret the present findings are that having less intrusive thoughts and more posttraumatic growth can serve as protective factors against the negative effect of self-stigma on QoL. Thus, interventions that aim to boost the QoL of Chinese American breast cancer survivors may attempt to reduce self-stigma and intrusive thoughts and/or foster posttraumatic growth.
The survivorship issues of Chinese American breast cancer survivors, and survivors from other ethnic minority populations, may differ from those of the non-Hispanic White breast cancer survivors because of different understandings of the disease, language barriers, societal stigmas, and cultural and religious beliefs and values [2, 45]. Whereas breast cancer survivorship may be becoming less stigmatized for non-Hispanic White women due to “pink ribbon” campaigns, these benefits may not extend to ethnic minority women [13]. Indeed, recent qualitative studies show that stigma is still a common concern for Chinese American breast cancer survivors [19, 20]. The findings from the present quantitative study compliment and extend the findings from these recent qualitative studies, suggesting that more self-stigma of breast cancer may harm the QoL of Chinese American breast cancers survivors. Future research should continue to examine the experiences of breast cancer survivors from other minority populations.
The findings from present study also compliment and extend previous quantitative research examining the relationship between stigma and QoL. Specifically, previous research has found a negative relationship between self- and perceived stigma and QoL among cancer survivors (e.g., [14, 15]). The current study adds to this literature by finding evidence for a negative relationship between self-stigma and QoL in a sample of Chinese American breast cancer survivors—a relatively understudied population. Moreover, the present study also contributes to literature by investigating possible psychological mechanisms that may underlie the relationship between stigma and QoL—specifically, greater intrusive thoughts and less posttraumatic growth. Future research should continue to explore psychological mechanisms that link stigma to worse health and QoL, particularly in samples from understudied populations.
Study limitations
The present study is subject to limitations. First, the cross-sectional nature of data prevents us from drawing causal inferences. Future studies should adopt a longitudinal or experimental design to examine the causal relationships among self-stigma, intrusive thoughts, posttraumatic growth, and QoL. Second, while participants were recruited from geographically distant metropolitan areas, recruitment occurred at selected social events which may have led to self-selection bias. These participants may feel less stigmatized than others who would not attend these events. Future research should explore alternative channels to recruiting participants. Third, given the demographic characteristics of the current sample, it is possible that the relationships found in this study may be specific to older, educated, and married Chinese American breast cancer survivors and may not be generalized to other minority populations that have a different cultural view of breast cancer. Future studies should use samples of greater diversity in terms of age, education, income, ethnicity, and cancer type.
Clinical implications
Despite these limitations, the findings from the current study have clinical implications. Based on the current findings, it may make sense to screen Chinese American breast cancer survivors for self-stigma. Those experiencing high levels of self-stigma as a result of their breast cancer should be offered interventions that target cognitive processes [27]—interventions aimed at reducing the impact of intrusive thoughts and promoting posttraumatic growth. Indeed, interventions that have focused on cognitive reframing (e.g., Cognitive Behavioral Therapy [46]) and detaching from repetitive, negative thoughts (e.g., Mindfulness-based interventions, Acceptance and Commitment Therapy [46, 47]) have been found to be successful in facilitating adjustment among Chinese breast cancer survivors [48, 49].
Conclusion
Taken together, by examining the psychological factors that could be harming the QoL of Chinese American breast cancer survivors, an understudied population, the present study makes an important contribution to literature. Identifying harmful psychological processes allows researchers and clinicians to utilize and develop targeted psychosocial interventions that may benefit the QoL of breast cancer survivors. It is our hope that the current research will stimulate additional research in this area that will ultimately improve the lives of people contending with breast cancer.
References
Tam Ashing, K., Padilla, G., Tejero, J., & Kagawa-Singer, M. (2003). Understanding the breast cancer experience of Asian American women. Psycho-Oncology, 12(1), 38–58.
Ashing-Giwa, K. T., Padilla, G., Tejero, J., Kraemer, J., Wright, K., Coscarelli, A., et al. (2014). Understanding the breast cancer experience of women: A qualitative study of African American, Asian American, Latina and Caucasian cancer survivors. Psycho-Oncology, 13(6), 408–428.
Crocker, J., Major, B., & Steele, C. (1998). Social stigma. In D. Gilbert, S. T. Fiske, & G. Lindzey (Eds.), The handbook of social psychology (4th ed., pp. 504–553). Boston, MA: McGraw-Hill.
Goffman, E. (1963). Stigma: Notes on the management of spoiled identity. New York: Simon and Schuster.
Link, B. G., & Phelan, J. C. (2001). Conceptualizing stigma. Annual Review of Sociology, 27(1), 363–385.
Hatzenbuehler, M. L., Phelan, J. C., & Link, B. G. (2013). Stigma as a fundamental cause of population health inequalities. American Journal of Public Health, 103(5), 813–821. https://doi.org/10.2105/AJPH.2012.301069.
Major, B., & O’Brien, L. T. (2005). The social psychology of stigma. Annual Review of Psychology, 56, 393–421. https://doi.org/10.1146/annurev.psych.56.091103.070137.
Meyer, I. H. (2003). Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: Conceptual issues and research evidence. Psychological Bulletin, 129(5), 674–697. https://doi.org/10.1037/0033-2909.129.5.674.
Corrigan, P. W., Larson, J. E., & Ruesch, N. (2009). Self-stigma and the “why try” effect: Impact on life goals and evidence-based practices. World Psychiatry, 8(2), 75–81. https://doi.org/10.1002/j.2051-5545.2009.tb00218.x.
Else-Quest, N. M., & Jackson, T. L. (2014). Cancer stigma. In P. W. Corrigan (Ed.), The stigma of disease and disability: Understanding causes and overcoming injustices (pp. 165–181). Washinton, DC: American Psychological Association.
Knapp, S., Marziliano, A., & Moyer, A. (2014). Identity threat and stigma in cancer patients. Health Psychology Open. https://doi.org/10.1177/2055102914552281.
Lebel, S., & Devins, G. M. (2008). Stigma in cancer patients whose behavior may have contributed to their disease. Future Oncology, 4(5), 717–733. https://doi.org/10.2217/14796694.4.5.717.
Bell, K. (2014). The breast-cancer-ization of cancer survivorship: Implications for experiences of the disease. Social Science and Medicine, 110, 56–63. https://doi.org/10.1016/j.socscimed.2014.03.031.
Kim, M. A., & Yi, J. (2014). Life after cancer: How does public stigma increase psychological distress of childhood cancer survivors? International Journal of Nursing Studies, 5(12), 1605–1614.
Williamson, T. J., Choi, A. K., Kim, J. C., Garon, E. B., Shapiro, J. R., Irwin, M. R., et al. (2018). A longitudinal investigation of internalized stigma, constrained disclosure, and quality of life across 12 weeks in lung cancer patients on active oncologic treatment. Journal of Thoracic Oncology, 13(9), 1284–1293.
Ernst, J., Mehnert, A., Dietz, A., Hornemann, B., & Esser, P. (2017). Perceived stigmatization and its impact on quality of life-results from a large register-based study including breast, colon, prostate and lung cancer patients. BMC cancer, 17(1), 741.
Tripathi, L., Datta, S. S., Agrawal, S. K., Chatterjee, S., & Ahmed, R. (2017). Stigma perceived by women following surgery for breast cancer. Indian Journal of Medical and Paediatric Oncology, 38(2), 146–152.
Cho, J., Choi, E. K., Kim, S. Y., Shin, D. W., Cho, B. L., Kim, C. H., et al. (2013). Association between cancer stigma and depression among cancer survivors: A nationwide survey in Korea. Psycho-Oncology, 22(10), 2372–2378.
Wong-Kim, E., Sun, A., Merighi, J. R., & Chow, E. A. (2005). Understanding quality-of-life issues in Chinese women with breast cancer: A qualitative investigation. Cancer Control, 12, 6–12.
Warmoth, K., Cheung, B., You, J., Yeung, N. C., & Lu, Q. (2017). xploring the social needs and challenges of Chinese American immigrant breast cancer survivors: A qualitative study using an expressive writing approach. International Journal of Behavioral Medicine, 24(6), 827–835.
Hatzenbuehler, M. L. (2009). How does sexual minority stigma “get under the skin”? A psychological mediation framework. Psychological Bulletin, 135(5), 707–730. https://doi.org/10.1037/a0016441.
Lewis, J. A., Manne, S. L., DuHamel, K. N., Vickburg, S. M. J., Bovbjerg, D. H., Currie, V., et al. (2001). Social support, intrusive thoughts, and quality of life in breast cancer survivors. Journal of Behavioral Medicine, 24(3), 231–245. https://doi.org/10.1023/A:1010714722844.
Miller, C. T., & Kaiser, C. R. (2001). A theoretical perspective on coping with stigma. Journal of Social Issues, 57(1), 73–92. https://doi.org/10.1111/0022-4537.00202.
Gonzalez, P., Nuñez, A., Wang-Letzkus, M., Lim, J. W., Flores, K. F., & Nápoles, A. M. (2016). Coping with breast cancer: Reflections from Chinese American, Korean American, and Mexican American women. Health Psychology, 35(1), 19–28. https://doi.org/10.1037/hea0000263.
Taylor, S. E., Lichtman, R. R., & Wood, J. V. (1984). Attributions, beliefs about control, and adjustment to breast cancer. Journal of Personality and Social Psychology, 46(3), 489–502. https://doi.org/10.1037/0022-3514.46.3.489.
Helgeson, V. S., Reynolds, K. A., & Tomich, P. L. (2006). A meta-analytic review of benefit finding and growth. Journal of Consulting and Clinical Psychology, 74(5), 797–816. https://doi.org/10.1037/0022-006X.74.5.797.
Shen, M. J., Coups, E. J., Li, Y., Holland, J. C., Hamann, H. A., & Ostroff, J. S. (2015). The role of posttraumatic growth and timing of quitting smoking as moderators of the relationship between stigma and psychological distress among lung cancer survivors who are former smokers. Psycho-Oncology, 24(6), 683–690. https://doi.org/10.1002/pon.3711.
Lu, Q., Gallagher, M. W., Loh, A., & Young, L. (2018). Expressive writing intervention improves quality of life among Chinese-American breast cancer survivors: A randomized controlled trial. Annals of Behavioral Medicine. https://doi.org/10.1093/abm/kax067.
Thoemmes, F., Mackinnon, D. P., & Reiser, M. R. (2010). Power analysis for complex mediational designs using Monte Carlo Methods. Structural Equation Modeling, 17(3), 510–534.
Tedeschi, R. G., & Calhoun, L. G. (1996). The Posttraumatic Growth Inventory: Measuring the positive legacy of trauma. Journal of Traumatic Stress, 9(3), 455–471. https://doi.org/10.1007/BF02103658.
Brislin, R. W. (1970). Back-translation for cross-cultural research. Journal of Cross-Cultural Psychology, 1(3), 185–216. https://doi.org/10.1177/135910457000100301.
Mak, W. W., & Cheung, R. Y. (2010). Self-stigma among concealable minorities in Hong Kong: Conceptualization and unified measurement. American Journal of Orthopsychiatry, 80(2), 267–281.
Kato, A., Takada, M., & Hashimoto, H. (2014). Reliability and validity of the Japanese version of the Self-Stigma Scale in patients with type 2 diabetes. Health and Quality of Life Outcomes, 12(1), 179. https://doi.org/10.1186/s12955-014-0179-z.
Yang, X., & Mak, W. W. (2016). The differential moderating roles of self-compassion and mindfulness in self-stigma and well-being among people living with mental illness or HIV. Mindfulness, 8(3), 595–602. https://doi.org/10.1007/s12671-016-0635-4.
Yeung, N., Dai, J., Zheng, D., Man, J., Loh, A., Young, L., et al. (2011). Exploration of culturally unique needs and challenges experienced by chinese breast cancer survivors living in the United States: A qualitative study using expressive writing approach. Psycho-oncology, 20(Supplement 1), 92.
Horowitz, M., Wilner, N., & Alvarez, W. (1979). Impact of event scale: A measure of subjective stress. Psychosomatic Medicine, 41(3), 209–218. https://doi.org/10.1097/00006842-197905000-00004.
Chen, S. C., Lai, Y. H., Liao, C. T., & Lin, C. C. (2005). Psychometric testing of the Impact of Event Scale-Chinese Version (IES-C) in oral cancer patients in Taiwan. Supportive Care in Cancer, 13(7), 485–492. https://doi.org/10.1007/s00520-005-0775-x.
Cella, D. F., Tulsky, D. S., Gray, G., Sarafian, B., Linn, E., Bonomi, A., et al. (1993). The functional assessment of cancer therapy scale: Development and validation of the general measure. Journal of Clinical Oncology, 11(3), 570–579. https://doi.org/10.1200/JCO.1993.11.3.570.
Wan, C., Zhang, D., Yang, Z., Tu, X., Tang, W., Feng, C., et al. (2007). Validation of the simplified Chinese version of the FACT-B for measuring quality of life for patients with breast cancer. Breast Cancer Research and Treatment, 106(3), 413–418. https://doi.org/10.1007/s10549-007-9511-1.
Steiger, J. S. (1990). Structural model evaluation and modification: An interval estimation approach. Multivariate Behavioral Research, 25(2), 173–180.
Bentler, P. M. (1990). Comparative fit indexes in structural models. Psychological Bulletin, 107(2), 238–246.
Browne, M. W., & Cudeck, R. (1993). Alternative ways of assessing model fit. In K. Bollen & J. S. Long (Eds.), Testing structural equation models. Newbury Park, CA: Sage.
Muthén LK, & Muthén, B. O. (1998-2016) Mplus User’s Guide, 7th ed. Los Angeles, CA: Muthén & Muthén
Preacher, K. J., & Hayes, A. F. (2008). Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behavior Research Methods, 40(3), 879–891.
Lu, Q., Yeung, N. C., You, J., & Dai, J. (2016). Using expressive writing to explore thoughts and beliefs about cancer and treatment among Chinese American immigrant breast cancer survivors. Psycho-Oncology, 25(1), 13711374.
Abad, A. N. S., Bakhtiari, M., Kashani, F. L., & Habibi, M. (2016). The comparison of effectiveness of treatment based on acceptance and commitment with cognitive-behavioral therapy in reduction of stress and anxiety in cancer patients. International Journal of Cancer Research and Prevention, 9(3), 229–246.
Zhang, J., Xu, R., Wang, B., & Wang, J. (2016). Effects of mindfulness-based therapy for patients with breast cancer: A systematic review and meta-analysis. Complementary Therapies in Medicine, 26, 1–10. https://doi.org/10.1016/j.ctim.2016.02.012.
Qiu, H., Ren, W., Yang, Y., Zhu, X., Mao, G., Mao, S., et al. (2018). Effects of cognitive behavioral therapy for depression on improving insomnia and quality of life in Chinese women with breast cancer: Results of a randomized, controlled, multicenter trial. Neuropsychiatric Disease and Treatment, 14, 2665–2673.
Zhang, J. Y., Zhou, Y. Q., Feng, Z. W., Fan, Y. N., Zeng, G. C., & Wei, L. (2017). Randomized controlled trial of mindfulness-based stress reduction (MBSR) on posttraumatic growth of Chinese breast cancer survivors. Psychology, Health & Medicine, 22(1), 94–109.
Acknowledgements
The authors would like to thank the Herald Cancer Association for their support in recruiting participants and data collection.
Funding
This study was supported by the American Cancer Society MRSGT-10-011-01-CPPB (PI: Qian Lu).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors do not have any potential conflicts of interest to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards (University of Houston IRB Protocol number: 12559-02).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wong, C.C.Y., Pan-Weisz, B.M., Pan-Weisz, T.M. et al. Self-stigma predicts lower quality of life in Chinese American breast cancer survivors: exploring the mediating role of intrusive thoughts and posttraumatic growth. Qual Life Res 28, 2753–2760 (2019). https://doi.org/10.1007/s11136-019-02213-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-019-02213-w