ABSTRACT
The safety and effectiveness of systemic and topical medical therapies for ocular disorders are limited due to poor ocular drug uptake, nonspecificity to target tissues, systemic side effects, and poor adherence to therapy. Intravitreal injections can enhance ocular drug delivery, but the need for frequent retreatment and potential injection-related side effects limit the utility of this technique. Sustained-release drug delivery systems have been developed to overcome these limitations; such systems can achieve prolonged therapeutic drug concentrations in ocular target tissues while limiting systemic exposure and side effects and improving patient adherence to therapy. A critical factor in the development of safe and effective drug delivery systems has been the development of biocompatible polymers, which offer the versatility to tailor drug release kinetics for specific drugs and ocular diseases. Ocular implants include nonbiodegradable and biodegradable designs, with the latter offering several advantages. The polymers most commonly used in biodegradable delivery systems are synthetic aliphatic polyesters of the poly-α-hydroxy acid family including polylactic acid, polyglycolic acid, and polylactic-co-glycolic acid. The characteristics of these polymers for medical applications as well as the pharmacological properties, safety, and clinical effectiveness of biodegradable drug implants for the treatment of ocular diseases are reviewed herein.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
INTRODUCTION
Topical drug therapy is the primary form of treatment for front-of-the-eye diseases, such as ocular surface diseases (e.g., conjunctivitis, dry eye), for elevated intraocular pressure, and for anterior uveitis (1–3). Anatomical and physiological barriers in the eye, including the corneal epithelium and conjunctival clearance mechanisms, afford protection against the entry of xenobiotics. These barriers also greatly impede the entry of drugs to the posterior segment, making it difficult to achieve therapeutic drug concentrations (1–4). Treatment of back-of-the-eye diseases such as diabetic retinopathy, neovascular age-related macular degeneration, and retinal venous occlusive disease is especially challenging with topical therapy given the greater diffusional distance (5). Although successful in rodent models (6,7), topical therapy for retinal diseases has yet to be proven successful in clinical trials. Systemically administered drugs can be used for treating front- and back-of-the-eye diseases. However, the accessibility of ocular tissues is greatly limited by the blood-aqueous and blood-retinal barriers. As a result, high systemic doses must be administered, which increases drug exposure in non-ocular tissues and, consequently, the risk of adverse systemic side effects (2,8).
Intravitreal drug injections have been used to deliver high drug concentrations to target tissues in the eye. However, the half-life of many intravitreally administered, low molecular-weight drugs, such as corticosteroids, ranges from 2 to 6 h (9), which results in transient efficacy and the need for frequent re-injections to maintain therapeutic drug concentrations (10). Larger molecular-weight compounds, such as vascular endothelial growth factor (VEGF) antibodies and antigen-binding fragments, have longer half-lives but still require monthly injections to maximize patient visual acuity potential (11–14). Frequent intravitreal injections increase the risk of serious adverse events including retinal detachment, endophthalmitis, and vitreous hemorrhage, as well as adverse manifestations in the anterior segment, such as cataract formation and intraocular pressure (IOP) elevation with corticosteroid use (15,16). Although the incidence rates of these serious side effects may be relatively low, they can be sight-threatening. Due to the anatomic and physiologic barriers to both topical and systemic drug therapy and the relatively short half-life of compounds administered by intravitreal injection (Table I), sustained drug delivery systems have evolved over the past decade to become an important approach for treating a variety of ocular diseases.
Sustained-release intrascleral and intravitreal drug implants and inserts have been developed for the treatment of ocular diseases. These polymer-based drug delivery systems are designed to achieve prolonged therapeutic drug concentrations in ocular target tissues that are not readily accessible by conventional means while limiting the side effects from systemic drug exposure, frequent intraocular injections, and high peak drug concentrations associated with pulsed dosing, as well as improving patient compliance (5,8,17,18).
Polymeric ocular drug delivery systems are classified as two basic types: nonbiodegradable and biodegradable (Table II) (5,10,19). The two most common nonbiodegradable device types include reservoir-type devices, in which a drug core is slowly released across a nonbiodegradable semipermeable polymer or is released from a nonbiodegradable polymer with an opening of fixed area, and implant-type devices, in which a nonbiodegradable free-floating pellet is injected intravitreally or a nonbiodegradable plug is anchored to the sclera. In a reservoir-type system, release kinetics can achieve a near-zero-order rate after establishing a steady-state concentration gradient across the nonbiodegradable semipermeable membrane. As long as solid drug remains within the core, the drug release will be relatively constant. Biodegradable systems are typically the matrix (monolithic) type, consisting of a homogeneous resin pellet made from drug and a biodegradable polymer; however, biodegradable core-shell and microcapsule systems have also been studied (20,21). Most of the clinically available ocular implants to date have been of the nonbiodegradable type, typically consisting of a combination of polyvinyl alcohol (PVA) and ethylene vinyl acetate (EVA) (21).
BIODEGRADABLE OCULAR DRUG DELIVERY SYSTEMS
Biodegradable ocular drug delivery devices are composed of biocompatible polymers, which degrade into nontoxic byproducts, or polymers that solubilize in vivo and can be eliminated safely by the human body. Devices made from these polymers do not elicit permanent chronic foreign-body reactions (22) and do not require removal after the drug supply has been exhausted (1,23), which represents a distinct advantage over nonbiodegradable drug delivery systems. Biodegradable devices are typically constructed from synthetic aliphatic polyesters of the poly-α-hydroxy acid family, which include polyglycolic acid (PGA), polylactic acid (PLA), and the PGA/PLA copolymer, polylactic-co-glycolic acid (PLGA).
PLGA is synthesized by means of random ring-opening copolymerization of the cyclic dimers of glycolic acid and lactic acid. Successive monomeric units of glycolic or lactic acid are linked together in PLGA during polymerization by ester linkages. The ratio of lactide to glycolide used for the polymerization can be varied, and this will alter the biodegradation characteristics of the product (Fig. 1). The possibility to tailor the polymer degradation time by altering the ratio of the lactic acid and glycolic acid used during synthesis has made PLGA attractive for use in the production of a variety of biomedical devices since the 1970s. PLGA is relatively easy to construct into various shapes, such as rods, screws, plates, and pins for orthopedic and dental surgery; resorbable suture materials; vascular grafts and stents; and surgical meshes and scaffolding for tissue regeneration (22,24). Importantly, the rate of PLGA biodegradation, molecular weight and degree of crystallinity affects the drug release characteristics of drug delivery systems, thus giving polymer composition a significant role in the customization of implant characteristics.
The rate of drug release from biodegradable devices depends on the total surface area of the device, the percentage of loaded drug, the water solubility of drug, and the speed of polymer degradation (25). An advantage of PLGA-based delivery systems is that the rate and degree of drug release can be manipulated by altering the polymer composition to influence the degradation characteristics (24). The three main factors that determine the degradation rate of PLGA copolymers are the lactide:glycolide ratio (Fig. 1), lactide stereoisomeric composition (i.e., the amount of L- vs. DL-lactide), and molecular weight (22,24). The lactide:glycolide ratio and stereoisomeric composition are most important for PLGA degradation, as they determine polymer hydrophilicity and crystallinity. PLGA with a 1:1 ratio of lactic acid to glycolic acid degrades faster than PLA or PGA (5), and the degradation rate can be decreased by increasing the content of either lactide or glycolide (Fig. 1) (21). Polymers with degradation times ranging from weeks to years can be manufactured simply by customizing the lactide:glycolide ratio and lactide stereoisomeric composition (24). The versatility of PGA and PLA has enabled the construction of delivery systems to tailor drug release for treating a variety of front- and back-of-the-eye diseases.
Drug release from PLA- and PLGA-based matrix drug delivery systems generally follows pseudo first-order or square-root kinetics. Release is influenced by many factors, including polymer, drug load, implant morphology, and porosity. In general, drug release occurs in three phases (Fig. 2):
-
1:
Burst release: Drug release from the implant surface occurs, creating a short period of high drug release.
-
2:
Diffusion and chain scission: Diffusional drug release, which is governed by the inherent solubility of the drug in the surrounding media, occurs. Random chain scission of polymers occurs by hydrolytic cleavage, which increases the porosity and surface area for drug diffusion
-
3:
Biodegradation and mass loss: Drug release is associated with biodegradation of the polymer matrix, mass loss initially occurring in the central core of the implant, and a final burst in some delivery systems (Fig. 2) (1,3,5,19). The rapid achievement of high drug concentrations followed by a longer period of continuous lower-dose release makes such delivery systems ideally suited for acute-onset diseases that require a loading dose of drug followed by tapering doses over several months (20). More recent advancements in PLGA-based drug delivery systems have allowed for biphasic release characteristics with an initial high (burst) rate of drug release followed by sustained zero-order kinetic release; i.e. drug release rate from matrix is steady and independent of the drug concentration in the surrounding milieu over longer periods (10).
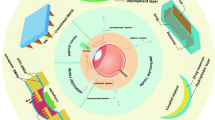
Drug-release mechanisms and biodegradation of matrix implant. a Schematic graph illustrating the cumulative release of drug from a PLGA implant at each phase of drug release and biodegradation. b Dry implant prior to implantation shows porous structure of PLGA. Magnified view (right) shows drug molecules (red spheres) interspersed in the pores and skeleton of the PLGA polymer. c Burst phase of drug release is the short phase occurring immediately after implantation. Magnified view (right) shows water penetrating the pores of PLGA (black curved arrows and squares) on the surface and drug molecules diffusing out of the implant on the surface (red arrows and red spheres). d Diffusion and random chain scission phase of drug release. Implant swells slightly as water molecules penetrate deeper into the core of the implant. The polymer is undergoing random chain scission, where the long PLGA chains are cleaved at random locations. Magnified view (right) shows water molecules (black curved arrows and squares) and drug molecules (red arrows and spheres) entering and exiting the implant from the core, respectively. e Biodegradation and mass loss phase is when the polymer begins to structurally break down from internal cavitation. Magnified view (right) shows that much of the drug molecules have diffused out from the cavity. f Continued biodegradation causes structural changes that alter the shape of the implant. Magnified view (right) shows that water is still passing through the polymer and less drug is available for release. g Implant fragments towards the end of biodegradation. Magnified view (right) shows that water is still passing through the smaller polymer skeleton and even less drug is available for release.
PLA, PGA, and PLGA are cleaved predominantly by nonenzymatic hydrolysis of their ester linkages throughout the matrix, in the presence of water in the surrounding tissues. This process, referred to as bulk erosion, is distinguished from surface erosion of the drug/polymer matrix surface (5) occurring with polymers such as polyanhydrides (PAH) and polyorthoesters (POE). PLA, PGA, and PLGA polymers are biocompatible because they undergo hydrolysis in the body to produce the original monomers, lactic acid and/or glycolic acid. Lactic and glycolic acids are nontoxic and eliminated safely via the Krebs cycle by conversion to carbon dioxide and water (23,24).
Safety of Biodegradable Polymers
The safety and biocompatibility of PLGA polymers was first demonstrated through their use in the production of the biodegradable sutures Dexon® (PGA; Covidien AG, Switzerland) and Vicryl® (L-PLGA; Johnson & Johnson Corp., New Brunswick, NJ), which have been used successfully in the clinical setting for more than 30 years (24). The biocompatibility of PLA and PLGA polymers has been further examined in both non-ocular and ocular tissues of animals and humans. The findings indicate that the polymers are generally well tolerated. In a long-term follow-up study of patients who had received PLA- and PLGA-containing resorbable-plate osteosyntheses for maxillary and mandibular fracture/reconstruction, radiographic imaging and histopathological assessments showed reliable biocompatibility and disintegration for both polymers: 85:15 PLGA degraded within 12 months and 70:30 PLA within 24 months (26). Acceptable biocompatibility of PLA and/or PLGA polymers has been demonstrated based on in vitro studies in dura, spinal cord, Schwann cells, brain tissue, and peripheral nerves (27).
The host response to polymeric implants is multifactorial and is affected by the physical and chemical properties of the polymer and by the physical properties of the implant (volume, shape, and surface characteristics). The response can be categorized to be tissue-dependent, organ-dependent, and species-dependent (25). Implantation of PLGA in bone or soft tissue of animals causes no inflammatory response, or only a mild response that diminishes with time, and is not associated with toxicity or allergy. In addition, the biocompatibility of PLGA-containing sutures and fracture fixation devices (rods, pins, screws, and plates) has been confirmed in human clinical trials (24). Examples of implantable PLGA-containing products marketed to date include Vicryl® (Ethicon) and Polysorb® (U.S. Surgical, North Haven, CT) sutures; Biologically Quiet (Instrument Makar, Okemos, MI) and SD sorb (Surgical Dynamics, Norwalk, CT) suture anchors; orthopedic fixation devices such as Lactosorb® (Biomet, Warsaw, IN) and BiosorbPDX (Bionx Implants, Bluebell, PA) screws for craniomaxillofacial fixation, Biologically Quiet staples (Instrument Makar) for ACL reconstruction, SD sorb meniscal staples (Surgical Dynamics) for meniscus repair, and SmartPinPDX pins (Bionx) for fracture fixation; and non-ocular drug delivery implants such as Zoladex (goserelin acetate, AstraZeneca UK Ltd., UK) for prostate cancer, Nutropin® Depot (human growth hormone; Genentech, Inc., South San Francisco, CA) for growth deficiencies, Trelstar® Depot (triptorelin pamoate) for prostate cancer, and Sandostatin LAR® (octreotide; Novartis AG, Switzerland) for acromegaly (24).
PLA and PLGA biocompatibility has also been studied in ocular tissues, and the polymers have been suggested to display even better tolerability than when placed in nonocular tissues. The anterior chamber, vitreous cavity, and subretinal space are known to display immune privilege. The features that account for the immune privilege of the eye include the blood-ocular barrier as well as the absence of lymphatic drainage pathways, soluble immunomodulatory factors in aqueous humor, immunomodulatory ligands on the surface of ocular parenchymal cells, and indigenous tolerance-promoting antigen-presenting cells (28). Based on these features, it has been speculated that polymers implanted into the vitreous cavity would provoke less of an inflammatory reaction than in other tissues. Biodegradable PLA/PLGA polymers have been experimentally implanted in various tissues of the eye and have been shown to be well tolerated (5,29–31).
Examples of Biodegradable Ocular Drug Delivery Systems
Lacrisert® (Aton Pharma, Inc., Lawrenceville, NJ), introduced in 1981, is a sterile, translucent, rod-shaped, water-soluble, biodegradable ophthalmic insert made of hydroxypropyl cellulose (HPC), a physiologically inert substance, for daily administration into the inferior cul-de-sac of the eye. The sustained release of HPC (5 mg) stabilizes and thickens the precorneal tear film and prolongs tear breakup time. The implant is approved to relieve the signs and symptoms of moderate to severe dry eye syndrome, including keratitis sicca, and is indicated especially for patients who remain symptomatic after therapy with artificial tears (32). Once-daily treatment with Lacrisert was shown to be more effective in relieving dry eye symptoms than 4-times-daily treatments with topical artificial tears (32). The implant, which can be self-administered up to twice daily using a specially designed applicator, is generally well tolerated. Side effects, which are typically mild and transient, include blurred vision, ocular discomfort/irritation, matting/stickiness of eyelashes, photophobia, hypersensitivity, eyelid edema, and hyperemia. The results of patient surveys regarding comfort and product preference favored Lacrisert over artificial tears (32).
Surodex™ (Allergan, Inc., Irvine, CA) is a rod-shaped biodegradable matrix implant (1.0 × 0.5 mm) consisting of dexamethasone and PLGA with hydroxypropyl methylcellulose (HPMC) which provides sustained drug release at a constant rate (60 μg over 7–10 days) (20). The implant is inserted in the anterior chamber following cataract surgery to control postoperative inflammation (33–36). Surodex does not require suture fixation and is well tolerated (18,20). In cataract patients, Surodex was shown to reduce anterior chamber cells and flare in the postoperative period and to have an anti-inflammatory effect at least as good as that of topical steroids (33–35).
A dexamethasone posterior-segment drug delivery system (Ozurdex®, formerly Posurdex, Allergan Inc, Irvine, CA) has recently been introduced into clinical practice. Ozurdex is a biodegradable implant consisting of 0.7 mg dexamethasone within a solid, rod-shaped PLGA copolymer (Novadur™, Allergan, Inc.) matrix (Figs. 3 and 4). The implant is designed to release dexamethasone biphasically, with peak doses for the initial 2 months, followed by lower therapeutic doses for up to 6 months. A novel single-use applicator is used to insert the drug pellet (6.5 mm × 0.45 mm) into the vitreous through a 22-gauge pars plana injection (Fig. 3). The procedure is performed in-office rather than in a surgical setting and does not require sutures for wound closure. Ozurdex was approved by the FDA in June 2009 for the treatment of macular edema (ME) associated with retinal vein occlusion, and it is currently being evaluated in clinical trials for the treatment of macular edema secondary to diabetic retinopathy (Clinicaltrials.gov ID# NCT00168337; NCT00168389) and for the treatment of uveitis (NCT00333814). In a phase 2 clinical trial, patients treated with the 700-μg implant showed marked improvement in vision—up to a 3-line increase in visual acuity as compared with a control group, with therapeutic effects persisting up to 180 days in some eyes. The treatment was not associated with sterile endophthalmitis or an increased incidence of retinal detachment (37). A clinical safety evaluation of Ozurdex following intravitreal insertion by sclerotomy in a 6-month phase 2 study in patients with persistent ME showed a mild increase in the incidence of adverse events in the treatment groups relative to the observation groups on day 8, which was expected as a result of the surgical procedure (i.e., hyperemia, pruritus, vitreous hemorrhage, and anterior chamber cells and flare) (38). As of October 2009, more than 2,500 patients have been enrolled in Ozurdex studies.
A Novadur-based implant for the delivery of brimonidine tartrate is in the early stages of development. It is currently being evaluated in clinical trials of patients with retinitis pigmentosa (phase 1 and 2; ID NCT00661479), glaucomatous optic neuropathy (phase 2; NCT00693485), age-related macular degeneration (phase 2; NCT00658619), and rhegmatogenous macula-off retinal detachment (phase 2; ID NCT00972374).
Verisome™ (Ramscor, Inc., Menlo Park, CA) is a zero-order sustained-release, intraocular drug delivery technology for the formulation of drugs as long-acting biodegradable solids, gels, or liquids that can be administered intravitreally via a standard 30-gauge injection. The technology is nonpolymer-based and proprietary. It can be adapted for a variety of drugs, including small molecules, peptides, proteins, and monoclonal antibodies, to allow custom tailoring of the duration of action (http://www.iconbioscience.com/Technology-Overview.html). An investigational triamcinolone acetonide (TA) formulation using the Verisome system (IBI 20089) was shown in rabbits to provide sustained delivery of TA at a mean daily dose of 1.1 μg/mL for up to 1 year from a single injection (39). IBI 20089 was also recently evaluated for safety and efficacy in a phase 1 trial in 10 patients with cystoid macular edema associated with retinal vein occlusion (40). A formulation of IBI 20089 that delivers 13.8 mg TA was found to significantly reduce macular thickness at 120 days post-treatment and was more effective than a 6.9-mg formulation. The delivery system visibly reduced in size as the drug was released, and it was well tolerated, with the exception of one case of IOP elevation that required surgery.
Other biodegradable polymers, such as glycolide-co-lactide-co-caprolactone copolymers (PGLC), polycaprolactones (PCL), polyorthoesters (POE), and polyanhydrides (PAH), have been explored for ocular drug delivery systems (1,5,17,19), but these technologies are still in the early stages of development, and none have yet been marketed commercially. PGLC has been used in combination with cyclosporine to treat experimental uveitis (41), in an intracameral dexamethasone implant to prevent corneal graft rejection in an animal model (42), and with FK506 to prolong corneal allograft survival (43). Polymers that degrade by surface erosion, such as POE and PAH (e.g. 1,3-bis-carboxyphenoxypropane), are biocompatible and may reduce drug burst effects when they are not required clinically (1). POE, which is hydrophobic and degrades by surface erosion, has been used to deliver 5-fluorouracil (44). PAH, which also undergoes surface erosion, has been used in implants to deliver 5-fluorouracil, 5-fluorouridine, mitomycin C, taxol, and etoposide as adjuncts in glaucoma-filtration surgery in animals (5,23).
The naturally occurring biopolymers chitosan and gelatin have been used in ocular inserts to deliver levofloxacin and gatifloxacin for the treatment of conjunctivitis. These systems provide prolonged drug release with zero-order kinetics (45).
In addition to their use in sustained-release implants and inserts, biodegradable polymers can be used in a variety of other ways to increase the residence time of drugs, slow drug clearance, and enhance drug absorption. Biodegradable polymers have been employed experimentally as viscosity enhancers, as mucoadhesive agents, in drug-releasing contact lenses, and in injectable formulations (e.g. hydrogels and liposomes as well as microemulsions, microsuspensions, microspheres, microcapsules and their nanoscale counterparts). These therapeutic strategies and examples of such ocular drug delivery systems have been discussed in depth in several recent reviews (1–3,17,19). Microsomes are spherical liposomal structures, ranging in size from roughly 0.01 to 10 μm that consist of vesicular lipid bilayers separated by water or an aqueous buffer compartment (1,2,8). Microsomes allow for the circumvention of cell membrane barriers and protection of the delivered drug from metabolic or immune attack, thereby reducing drug toxicity and enhancing the therapeutic effect. Several studies have examined the feasibility of using microspheres composed from PLGA, PLA, and other biodegradable polymers as biodegradable systems for the sustained ocular delivery of therapeutic drugs (29,31,46) including progesterone (47), adriamycin (30), and pegaptanib (48). Microspheres composed of the biodegradable biopolymer chitosan have been used to deliver acyclovir through the rabbit cornea (49) and have been shown to enhance ocular delivery of ofloxacin from erodible inserts constructed from polyethylene oxide (50). Smaller-sized particulate drug delivery systems include nanoparticles, which are polymeric colloidal particles (ranging in size from 10 to 1,000 nm) consisting of macromolecular materials in which the drug is dissolved, entrapped, encapsulated, and/or to which the drug is adsorbed or attached; nanospheres, which are solid spheres containing drug bound in a matrix or adsorbed on the surface of a colloidal carrier; and nanocapsules, which are small capsules with a central cavity surrounded by a polymeric membrane (1,2,8). Biodegradable PLA nanoparticles (140 nm) administered intravitreally have been shown to localize in the retinal pigment epithelium (51), and coating nanoparticles with polyethylene glycol (PEG) has been reported to enhance the therapeutic efficacy of treatment for ocular diseases such as autoimmune uveoretinitis (52). Drug-impregnated contact lenses have been widely investigated for the sustained release of ocular drugs (53–55). Soft contact lenses are typically composed of nonbiodegradable hydrogels of poly(2-hydroxyethylmethacrylate) (PHEMA) or hydroxyethylmethacrylate (HEMA) copolymerized with other monomers such as methacrylic acid, acetone acrylamide, and vinyl pyrrolidone. Typically, the amount of drug that can be loaded into such systems is low, and release is usually rapid and poorly controlled; however, entrapping the drug in a biodegradable nanoparticle prior to incorporation into the contact lens can be used to sustain the release (1).
NONBIODEGRADABLE OCULAR DRUG DELIVERY SYSTEMS
In nonbiodegradable reservoir-type devices, PVA, a permeable polymer, is typically used as a structural element, while the device’s drug-restricting membrane is composed of EVA, a hydrophobic polymer that is relatively impermeable to hydrophilic drugs (1,3,5). Drug release from reservoir-type devices occurs when water diffuses through the outer EVA coating and partially dissolves the enclosed drug, forming a saturated drug solution that is then released into the surrounding tissue via diffusion (1,3). Drug release occurs at a constant rate, and the duration of release is limited primarily by the rate of drug dissolution within the reservoir. The drug release rate can be slowed by increasing the surface area or thickness of the drug-restricting polymer, and drug delivery can be increased by maximizing the surface area available for drug diffusion or by using a more permeable membrane. Nonbiodegradable reservoir-type devices are typically designed to release drug over a span of months or years for the treatment of chronic conditions that require long-term drug therapy.
Nonbiodegradable implants, although useful in some clinical situations, have several distinct drawbacks (Table I). Some designs require relatively large incisions for implantation, may require sutures or some other form of anchoring, and require re-implantation once the drug is completely released to maintain efficacy and optional removal of the prior implant. The implantation and removal of nonbiodegradable implants can be associated with serious side effects such as retinal detachment, vitreous hemorrhage, and cataract formation (1,3,5,10,22,23,56).
CONCLUSIONS
Biodegradable polymer-based drug delivery systems show considerable promise for the treatment of ocular diseases. Such systems offer a potential solution to many of the limitations of conventional methods for the administration of ophthalmic drugs, especially for treating sight-threatening retinal diseases. Some polymers used in biodegradable drug delivery systems offer well-documented biocompatibility and an acceptable ocular safety profile, while other polymers are investigational and are in varying stages of development. The versatility of biodegradable polymers allows for construction of delivery systems to tailor the drug release for treating a variety of front- and back-of-the-eye diseases. In addition, biodegradable drug delivery systems can also be used to repurpose well-established drugs that may be ineffective by conventional administration routes and provide a sustained-release platform to be practical and effective for treating eye diseases. Clinical studies are in progress examining the efficacy and safety of such delivery systems in a variety of ocular diseases.
REFERENCES
Conway BR. Recent patents on ocular drug delivery systems. Recent Pat Drug Deliv Formul. 2008;2(1):1–8.
Ghate D, Edelhauser HF. Ocular drug delivery. Expert Opin Drug Deliv. 2006;3(2):275–87.
Kearns VR, Williams RL. Drug delivery systems for the eye. Expert Rev Med Devices. 2009;6(3):277–90.
Myles ME, Neumann DM, Hill JM. Recent progress in ocular drug delivery for posterior segment disease: emphasis on transscleral iontophoresis. Adv Drug Deliv Rev. 2005;57(14):2063–79.
Yasukawa T, Ogura Y, Kimura H, Sakurai E, Tabata Y. Drug delivery from ocular implants. Expert Opin Drug Deliv. 2006;3(2):261–73.
Tanito M, Li F, Elliott MH, Dittmar M, Anderson RE. Protective effect of TEMPOL derivatives against light-induced retinal damage in rats. Invest Ophthalmol Vis Sci. 2007;48(4):1900–5.
Ni Z, Hui P. Emerging pharmacologic therapies for wet age-related macular degeneration. Ophthalmologica. 2009;223(6):401–10.
Ghate D, Edelhauser HF. Barriers to glaucoma drug delivery. J Glaucoma. 2008;17(2):147–56.
Kwak HW, D’Amico DJ. Evaluation of the retinal toxicity and pharmacokinetics of dexamethasone after intravitreal injection. Arch Ophthalmol. 1992;110:259–66.
Kiernan DF, Mieler WF. The use of intraocular corticosteroids. Expert Opin Pharmacother. 2009;10(15):2511–25.
Spaide RF, Chang LK, Klancnik JM et al. Prospective study of intravitreal ranibizumab as a treatment for decreased visual acuity secondary to central retinal vein occlusion. Am J Ophthalmol. 2009;147:298–306.
Pieramici DJ, Rabena M, Castellarin AA et al. Ranibizumab for the treatment of macular edema associated with perfused central retinal vein occlusions. Ophthalmology. 2008;115:e47–54.
Dafer RM, Schneck M, Friberg TR, Jay WM. Intravitreal ranibizumab and bevacizumab: a review of risk. Semin Ophthalmol. 2007;22(3):201–4.
Rosenfeld PJ, Rich RM, Lalwani GA. Ranibizumab: phase III clinical trial results. Ophthalmol Clin N Am. 2006;19(3):361–72.
Jager RD, Aiello LP, Patel SC, Cunningham Jr ET. Risks of intravitreous injection: a comprehensive review. Retina. 2004;24(5):676–98.
Berinstein DM. New approaches in the management of diabetic macular edema. Tech Ophthalmol. 2003;1:106–13.
Wadhwa S, Paliwal R, Paliwal SR, Vyas SP. Nanocarriers in ocular drug delivery: an update review. Curr Pharm Des. 2009;15(23):2724–50.
Lee SY, Chee SP. Surodex after phacoemulsification. J Cataract Refract Surg. 2005;31(8):1479–80.
Gaudana R, Jwala J, Boddu SH, Mitra AK. Recent perspectives in ocular drug delivery. Pharm Res. 2009;26(5):1197–216.
Lee SS, Yuan P, Robinson MR. Ocular implants for drug delivery. In: Wnek GE, Bowlin GL, editors. Encyclopedia of biomaterials and biomedical engineering. New York: Informa Healthcare USA, Inc; 2008. p. 2259–69.
Davis JL, Gilger BC, Robinson MR. Novel approaches to ocular drug delivery. Curr Opin Mol Ther. 2004;6(2):195–205.
Chu C-C. Biodegradable polymers: an overview. In: Wnek GE, Bowlin GL, editors. Encyclopedia of biomaterials and biomedical engineering. New York: Informa Healthcare USA, Inc; 2008. p. 195–206.
Kimura H, Ogura Y. Biodegradable polymers for ocular drug delivery. Ophthalmologica. 2001;215(3):143–55.
Avgoustakis K. Polylactic-co-glycolic acid (PLGA). In: Wnek GE, Bowlin GL, editors. Encyclopedia of biomaterials and biomedical engineering. New York: Informa Healthcare USA, Inc; 2008. p. 2259–69.
Shive MS, Anderson JM. Biodegradation and biocompatibility of PLA and PLGA microspheres. Adv Drug Deliv Rev. 1997;28(1):5–24.
Landes C, Ballon A, Roth C. Maxillary and mandibular osteosyntheses with PLGA and P(L/DL) LA Implants: a 5-year inpatient biocompatibility and degradation experience. Plast Reconstr Surg. 2006;117(7):2347–60.
Holmes R, Cohen S, Cornwall G, Thomas K, Kleinhenz K, Beckett M. MacroPore resorbable devices in craniofacial surgery. Clin Plast Surg. 2004;31:393–406.
Streilein JW. Ocular immune privilege: the eye takes a dim but practical view of immunity and inflammation. J Leukocyte Biol. 2003;74:179–85.
Moritera T, Ogura Y, Honda Y, Wada R, Hyon SH, Ikada Y. Microspheres of biodegradable polymers as a drug-delivery system in the vitreous. Invest Ophthalmol Vis Sci. 1991;32:1785–90.
Moritera T, Ogura Y, Yoshimura N, Honda Y, Wada R, Hyon SH et al. Biodegradable microspheres containing adriamycin in the treatment of proliferative vitreoretinopathy. Invest Ophthalmol Vis Sci. 1992;33:3125–30.
Giordano GG, Chevez-Barrios P, Refojo MF, Garcia CA. Biodegradation and tissue reaction to intravitreous biodegradable poly(D, L-lactic-co-glycolic)acid microspheres. Curr Eye Res. 1995;9:761–8.
Lacrisert [prescribing information]. Lawrenceville, NJ, USA: Aton Pharma, Inc; 2007. Available at: http://www.lacrisert.com/pdfs/Lacrisert_PI.pdf. Accessed 04/07/2010.
Chang D, Garcia I, Hunkeler J, Minas T. Phase II results of an intraocular steroid delivery system for cataract surgery. Ophthalmology. 1999;106:1172–7.
Tan DT, Chee SP, Lim L, Lim AS. Randomized clinical trial of a new dexamethasone delivery system (Surodex) for treatment of post-cataract surgery inflammation. Ophthalmology. 1999;106(2):223–31.
Tan DT, Chee SP, Lim L, Theng J, Van Ede M. Randomized clinical trial of Surodex steroid drug delivery system for cataract surgery: anterior versus posterior placement of two Surodex in the eye. Ophthalmology. 2001;108:2172–81.
Seah SK, Husain R, Gazzard G, Lim MC, Hoh ST, Oen FT et al. Use of Surodex in phacotrabeculectomy surgery. Am J Ophthalmol. 2005;139(5):927–8.
Haller JA, Dugel P, Weinberg DV, Chou C, Whitcup SM. Evaluation of the safety and performance of an applicator for a novel intravitreal dexamethasone drug delivery system for the treatment of macular edema. Retina. 2009;29(1):46–51.
Kuppermann BD, Blumenkranz MS, Haller JA, Williams GA, Weinberg DV, Chou C et al. Randomized controlled study of an intravitreous dexamethasone drug delivery system in patients with persistent macular edema. Arch Ophthalmol. 2007;125(3):309–17.
Hu M, Huang G, Karasina F, Wong VG. Verisome™, a novel injectable, sustained release, biodegradable, intraocular drug delivery system and triamcinolone acetonide. Invest Ophthalmol Vis Sci. 2008;49:E-Abstract 5627. http://abstracts.iovs.org/cgi/content/abstract/49/5/5627.
Lim JI, Wieland MR, Fung A, Hung DY, Wong V. A phase 1 study evaluating the safety and evidence of efficacy of IBI-20089, a triamcinolone intravitreal injection formulated with the Verisome™ drug delivery technology, in patients with cystoid macular edema. Invest Ophthalmol Vis Sci. 2009;50:E-Abstract 5395. http://abstracts.iovs.org/cgi/content/abstract/50/5/5395.
Dong X, Shi W, Yuan G, Xie L, Wang S, Lin P. Intravitreal implantation of the biodegradable cyclosporin a drug delivery system for experimental chronic uveitis. Graefes Arch Clin Exp Ophthalmol. 2006;244(4):492–7.
Kagaya F, Usui T, Kamiya K, Ishii Y, Tanaka S, Amano S et al. Intraocular dexamethasone delivery system for corneal transplantation in an animal model. Cornea. 2002;21(2):200–2.
Shi W, Liu T, Xie L, Wang S. FK506 in a biodegradable glycolide-co-clatide-co-caprolactone polymer for prolongation of corneal allograft survival. Curr Eye Res. 2005;30(11):969–76.
Einmahl S, Behar-Cohen F, D’Hermies F, Rudaz S, Tabatabay C, Renard G et al. A new poly(ortho ester)-based drug delivery system as an adjunct treatment in filtering surgery. Invest Ophthalmol Vis Sci. 2001;42(3):695–700.
Gorle AP, Gattani SG. Design and evaluation of polymeric ocular drug delivery system. Chem Pharm Bull (Tokyo). 2009;57(9):914–9.
Wada R, Hyon SH, Ikada Y. Injectable microspheres with controlled drug release for glaucoma filtering surgery. Invest Ophthalmol Vis Sci. 1992;33:3436–41.
Beck LR, Cowsar DR, Lewis DH, Cosgrove Jr RJ, Riddle CT, Lowry SR et al. A new long-acting injectable microcapsule system for the administration of progesterone. Fertil Steril. 1979;31:545–51.
Carrasquillo KG, Ricker JA, Rigas IK et al. Controlled delivery of the anti-VEGF aptamer EYE001 with poly(lactic-co-glycolic)acid microspheres. Invest Ophthalmol Vis Sci. 2003;44:290–9.
Genta I, Conti B, Perugini P, Pavanetto F, Spadaro A, Puglisi G. Bioadhesive microspheres for ophthalmic administration of acyclovir. J Pharm Pharmacol. 1997;49(8):737–42.
Di Colo G, Zambito Y, Burgalassi S, Serafini A, Saettone MF. Effect of chitosan on in vitro release and ocular delivery of ofloxacin from erodible inserts based on poly(ethylene oxide). Int J Pharm. 2002;248(1–2):115–22.
Bourges J-L, Gautier SE, Delie F et al. Ocular drug delivery targeting the retina and retinal pigment epithelium using polylactide nanoparticles. Invest Ophthalmol Vis Sci. 2003;44:3562–9.
de Kozak Y, Andrieux K, Villarroya H et al. Intraocular injection of tamoxifen-loaded nanoparticles: a new treatment of experimental autoimmune uveoretinitis. Eur J Immunol. 2004;34:3702–12.
Alvarez-Lorenzo C, Hiratani H, Concheiro A. Contact lenses for drug delivery: achieving sustained release with novel systems. Am J Drug Deliv. 2006;4(3):131–51.
Schultz CL, Poling TR, Mint JO. A medical device/drug delivery system for treatment of glaucoma. Clin Exp Optom. 2009;92(4):343–8.
Xinming L, Yingde C, Lloyd AW et al. Polymeric hydrogels for novel contact lens-based ophthalmic drug delivery systems: a review. Cont Lens Anterior Eye. 2007;31(2):57–64.
Mohammad DA, Sweet BV, Elner SG. Retisert: is the new advance in treatment of uveitis a good one? Ann Pharmacother. 2007;41(3):449–54.
Mansoor S, Kuppermann BD, Kenney MC. Intraocular sustained-release delivery systems for triamcinolone acetonide. Pharm Res. 2009;26(4):770–84.
Arjona A, Vasiliou S, Cole P. Highlights from the Annual Meeting of the Association for Research in Vision and Ophthalmology (ARVO) 2009. Drugs Future. 2009;34(11):925.
Macoul KL, Pavan-Langston D. Pilocarpine Ocusert system for sustained control of ocular hypertension. Arch Ophthalmol. 1975;93:587–90.
Quigley HA, Pollack IP, Harbin Jr TS. Pilocarpine Ocuserts: long-term clinical trials and selected pharmacodynamics. Arch Ophthalmol. 1975;93:771–5.
Chien YW. Novel drug delivery systems. 2nd ed. New York: Marcel Dekker; 1992.
Kedhar SR, Jabs DA. Cytomegalovirus retinitis in the era of highly active antiretroviral therapy. Herpes. 2007;14:66–71.
Kane FE, Burdan J, Cutino A, Green KE. Iluvien: a new sustained delivery technology for posterior eye disease. Expert Opin Drug Deliv. 2008;5(9):1039–46.
Emerich DF, Thanos CG. NT-501: an ophthalmic implant of polymer-encapsulated ciliary neurotrophic factor-producing cells. Curr Opin Mol Ther. 2008;10(5):506–15.
Thanos CG, Bell WJ, O’Rourke P, Kauper K, Sherman S, Stabila P et al. Sustained secretion of ciliary neurotrophic factor to the vitreous, using the encapsulated cell therapy-based NT-501 intraocular device. Tissue Eng. 2004;10(11–12):1617–22.
Tao W, Wen R, Laties A, Aguirre GD. Cell-based delivery systems: development of encapsulated cell technology for ophthalmic applications. In: Jaffe GJ, Ashton P, editors. Intraocular drug delivery. New York: Taylor & Francis Group; 2006. p. 111–28.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, S.S., Hughes, P., Ross, A.D. et al. Biodegradable Implants for Sustained Drug Release in the Eye. Pharm Res 27, 2043–2053 (2010). https://doi.org/10.1007/s11095-010-0159-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-010-0159-x