Abstract
Objectives
We recently demonstrated that fibrin-based tissue engineered blood vessels (TEV) exhibited vascular reactivity, matrix remodeling and sufficient strength for implantation into the veins of an ovine animal model, where they remained patent for 15 weeks. Here we present an approach to improve the mechanical properties of fibrin-based TEV and examine the relationship between mechanical strength and smooth muscle cell (SMC) function.
Materials and Methods
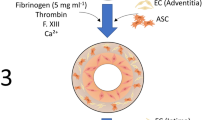
To this end, we prepared TEV that were composed of two layers: a cellular layer containing SMC embedded in fibrin hydrogel to provide contractility and matrix remodeling; and a second cell-free fibrin layer composed of high concentration fibrinogen to provide mechanical strength.
Results
The ultimate tensile force of double-layered TEV increased with FBG concentration in the cell-free layer in a dose-dependent manner. Double-layered TEV exhibited burst pressure that was ten-fold higher than single-layered tissues but vascular reactivity remained high even though the cells were constricting an additional tissue layer.
Conclusion
These results showed that mechanical strength results largely from the biomaterial but contractility requires active cellular machinery. Consequently, they may suggest novel approaches for engineering biomaterials that satisfy the requirement for high mechanical strength while preserving SMC function.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Due to the rise in cardiovascular disease throughout the world, there is increasing demand for small diameter blood vessels as replacement grafts. Although venous grafts are currently the golden standard, the ten-year failure rate is very high (1). In addition, limited availability, especially for repeat grafting procedures, and the pain and discomfort associated with the donor site necessitate the development of alternative technologies. Synthetic conduits of polytetra-flouroethylene (Teflon, ePTFE) or polyethylene terephthalate (Dacron) have been used extensively in replacement of large diameter (>6 mm) vessels (2–4), but small diameter synthetic grafts displayed high failure rates due to thrombus and plaque formation. On the other hand tissue engineered vascular grafts (TEV) are capable of remodeling in response to host signals and offer a clear alternative to existing technologies.
Several approaches have been proposed for tissue engineering of vascular grafts. They involve decellularized tissues, cell sheet engineering and biodegradable scaffolds. Scaffolds derived from decellularized tissues have been implanted directly or after addition of endothelial and smooth muscle cells to improve patency and vascular reactivity (5–7). Another approach that does not involve a scaffold, termed cell sheet engineering, employed sheets of smooth muscle cells and fibroblasts that were manually wrapped around a mandrel to form a multilayered cylindrical TEV (8, 9). These constructs displayed a well defined layered organization and reached mechanical strength that was comparable to native vessels.
The third approach employed synthetic or natural biomaterials as biodegradable scaffolds for seeding smooth muscle and endothelial cells. Synthetic materials such as polyglycolic acid (PGA) were used successfully to engineer contractile TEV that developed sufficient strength for implantation in vivo (10,11). However, the products of PGA hydrolysis induced dedifferentiation of smooth muscle cells in vivo, limiting the efficacy of PGA as a scaffold for cardiovascular tissue engineering (12). Natural biomaterials such as collagen and fibrin hydrogels have also been employed because they offer high density and uniform cell seeding during polymerization and contain inherent biological signals that affect cellular activity. SMC compacted both collagen and fibrin hydrogels to a large extent and the constraint of the central mandrel induced cellular alignment (13) that could be further improved through application of cyclic strain (14–16). Surprisingly, SMC in 3D collagen gels downregulated expression of smooth muscle α-actin and decreased collagen synthesis, suggesting a departure from the contractile phenotype (17–19). On the other hand, fibrin stimulated collagen and elastin synthesis (20–22), suggesting that fibrin may promote SMC differentiation into a more contractile phenotype than collagen.
We have recently demonstrated that fibrin-based small-diameter tissue engineered blood vessels (TEV) could be implanted in an ovine animal model. After two weeks in culture TEV exhibited significant vasoreactivity in response to several vasodilators and vasoconstrictors and developed considerable mechanical strength to withstand interpositional implantation in the jugular veins of lambs, where they remained patent for 15 weeks (23). Although these experiments clearly demonstrated implantability of fibrin-based TEV in the veins of a large animal model, implantation into the arterial circulation would require stronger TEV to withstand higher pressure.
Several approaches have been taken to improve the mechanical properties of TEV from natural biomaterials. Application of pulsatile pressure increased cellular alignment and tensile strength significantly but not to levels required for implantation (16,24). Crosslinking with gluteraldehyde or other chemical methods was toxic to cells but ribose mediated crosslinking showed promising results (25,26). Non-degradable Dacron sleeves have been also been used to reinforce collagen-based TEV and allowed in vivo implantation (27,28). More recently, a two layer collagen TEV, termed construct-sleeve hybrid, was demonstrated to increase tensile strength significantly when the collagen sleeve was crosslinking with chemical or physical methods (29).
Here we tested the hypothesis that a second, cell-free layer of fibrin hydrogel may improve the mechanical strength of TEV without compromising contractility, a measure of the smooth muscle cell function. To this end, we prepared TEV that were composed of two layers: a SMC-containing layer to promote matrix remodeling and contractility and a cell-free layer of high fibrinogen concentration to provide mechanical strength without chemical or physical crosslinking. We found that tensile strength increased in proportion to the concentration of fibrinogen in the cell-free layer without compromising the contractile function of V-SMC. As expected, contractility required the presence of cells with active actin cytoskeleton but the change in tensile strength was attributed mainly to the second layer of fibrin hydrogel. Since fibrin polymerizes within seconds this approach may allow for application of the second cell-free layer in situ to provide additional strength at the time of implantation.
MATERIALS AND METHODS
Cell Culture
Neonatal vascular smooth muscle cells (SMC) were isolated from pulmonary veins removed from 3-days old lambs. Vessels were placed in cold PBS and cut open longitudinally. Endothelial cells, adventitia and connective tissues were removed by vigorously scraping the luminal and outside surfaces respectively. After thoroughly rinsed in PBS, the vessels were minced into pieces, about 1 mm, and placed into a T-25 flask with 4 ml media. Cells were maintained in M199 media supplemented with 10% fetal bovine serum (FBS), 1% penicillin/streptomycin, 1% l-glutamine and 15 mM HEPES (all from Gibco, Gaithersburg, MD). SMC were cryo-preserved at passage 2 and used for experiments between passages 4–7.
Single-layered Constructs
Single layer constructs were formed in 48-well plates (10 mm in diameter) in which a 4-mm polydimethylsiloxane (PDMS) mandrel was placed in the center of each well. Bovine thrombin (Sigma, St. Louis, MO) solution containing SMC and CaCl2 was mixed 1:4 (volume ratio) with the indicated concentration of human plasminogen-free fibrinogen (Enzyme research Laboratories, South Bend, IN) to a total volume of 600 μl surrounding the mandrel. The final cell density was 106 SMC per ml. After complete fibrin formation, the constructs were covered with 1 ml M199 media supplemented with 10% fetal bovine serum (FBS), 1% penicillin/streptomycin, 1% l-glutamine and 15 mM HEPES, 300 μM ascorbic acid phosphate(Sigma), 5 ng/ml TGF-β1 (USBiological, Swampscott, MA), 2 μg/ml insulin (Sigma), and 20 μg/ml aprotinin (Invitrogen, Carlsbad, CA) when indicated. On day two, the gels were released from the walls to allow radial compaction around the mandrel. Culture medium was changed every two days for two weeks. In some experiments TEV were treated with cytochalasin D (10 μg/mL) or sodium azide (1% w/v) for 24 h during the last day of the experiment.
Bi-layered Constructs with Cell Layer Inside
The cell layer was formed first as described for single-layered constructs. After 3 days of compaction, the constructs were transferred into 96-well plates (diameter 6.4 mm) and positioned in the center of each well. At that time, fibrin (200 μl) with the indicated concentration of FBG (10, 20 or 30 mg/ml) was polymerized around the SMC layer. When polymerization was complete, the constructs were transferred in 48-well plates and covered with culture medium. The length of the constructs was approximately 1 cm and their thickness varied with the concentration of FBG in the cell-free layer, as shown in the results section.
Bi-layered Constructs with Cell Layer Outside
Cell-free fibrin was polymerized in 96-well plates (200 μl per well) with a 4 mm mandrel in the center. The final concentration of fibrinogen in the cell-free layer was 10, 20 or 30 mg/ml as indicated. After complete polymerization, each construct was transferred into the center of a well in 48-well plates and SMC-containing fibrin (600 μl) was polymerized around this layer. The final cell density was 106 SMC per ml and the final concentration of fibrinogen in the cellular layer was 2.5 mg/ml. The constructs were covered with culture media and after 24 h they were released from the walls to allow for radial compaction around the mandrel. The length of the constructs was approximately 1 cm and their thickness varied with the concentration of FBG in the cell-free layer, as shown in the results section.
Long Tubular Constructs with Cell Layer Outside
For burst pressure measurements we prepared long tubular constructs (length = 4 cm; diameter = 4.0 mm) as follows. Fibrin (4 ml) was polymerized around a 4-mm-diameter silastic tube into a plastic mold (1 cm in diameter × 6 cm in length). After polymerization was complete, the hydrogels were placed into 50 ml conicals and centrifuged at 1,500 rpm for 5 min to remove excess water and reduce the volume of hydrogels by ~50%. Then SMC-containing fibrin (2–3 ml with 106 SMC/ml) was polymerized between the first layer and the wall of the plastic mold. After polymerization was complete, each TEV was removed from the plastic tube, transferred into a 50 ml conical tube and incubated in 40 ml culture media. Cell culture medium was replenished every three days.
TEV Compaction
After two weeks in culture, the length and annular area of each cylindrical construct were recorded with a digital camera (Kodak DC290) and digital images were analyzed with software ImageJ (National Institutes of Health, Bethesda, MD). The volume of each construct was calculated as the product of the annular area times the length.
Vascular Reactivity
After 2 weeks in culture, TEV rings were removed from the mandrels and placed into an isolated tissue system (Radnoti, Monrovia, CA) with standard Krebs–Ringer solution and continuously bubbled with 94% O2, 6% CO2 to obtain a pH of 7.4, a Pco2of 38 mmHg, and a Po2 > 500 mm Hg. The temperature was kept at 37°C. Each construct was mounted on stainless steel hooks through the lumen, one was fixed, and the other one was connected to a Statham UC2 force transducer. Tissues were equilibrated at a basal tension of 1.0 g and constant length for 30 min.
Pharmacological agents were added to the bath to elucidate TEV function. Contractions were elicited by adding KCl (118 mM) for 15 min or until tension was stable or norepinephrine (NE; 3 × 10−6 M). Isometric contraction was recorded using a PowerLab data acquisition unit and analyzed by Chart5 software (ADInstruments, Colorado Springs, CO).
Ultimate Stress and Burst Pressure Measurements
We employed two methods to test the strength of fibrin hydrogels with high concentrations of FBG: ultimate tensile stress and burst pressure. We measured force/stress by extending the constructs using the isolated tissue bath. Briefly, a circular segment of each cylindrical TEV was mounted on two stainless steel hooks, one fixed and the other connected to a force transducer. The tissues were bathed in standard Krebs–Ringer solution, equilibrated at basal tension of 1.0 g and constant length for 30–60 min and then stretched incrementally at an average rate of 1.3 mm/min until failure. Ultimate tensile force (UTF) was defined as the maximum force withstood by the tissues at failure. Ultimate tensile stress (UTS) was calculated by dividing the ultimate force by the initial cross-sectional area, which was calculated as the product of (wall thickness) × (length) of each TEV.
For measurements of burst pressure, long TEV (4 cm) were removed from the mandrel and cannulated at each end and secured with silk ties. The constructs were then placed in line with a fluid (PBS) filled tubing. Attached at one end of the tubing was a physiologic pressure transducer (Gould-Spectrum, Cleveland, OH) connected to a recording device. The other end was connected to a syringe filled with PBS which was used to pressurize the TEV simultaneously while the pressure was recorded. The TEV was pressurized until it broke, at which point the pressure was taken as the Burst Pressure (mmHg).
Histology and Immunohistochemistry
Tissue samples were fixed in 10% buffered formalin, dehydrated through graded concentrations of ethanol and Hemo-De (Scientific Safety Solvents, Keller, TX) and embedded in paraffin. Tissue morphology and collagen synthesis were evaluated by staining 5 μm paraffin sections with hematoxylin and eosin (H&E) as described previously [30–32]. For immunohistochemistry, tissue sections were deparaffinized and incubated in a tissue section retriever (PickCell Laboratories BV, Amsterdam, Netherlands) for antigen unmasking. Tissue sections were permeabilized with 0.1% triton X-100 for 1 h, blocked with 1% BSA in PBS for 30 min and incubated with monoclonal antibodies overnight at 4°C. The following antibodies were used: mouse monoclonal anti-human smooth muscle actin (1:50 dilution; SeroTec, Oxford, UK) , anti-human smooth muscle calponin (1:50 dilution; DakoCytomation, Carpinteria, CA) or anti-human smooth muscle myosin heavy chain (1:250 dilution; Lab Vision, Fremont, CA,) in PBS containing 1% BSA and 0.01% triton X-100. The tissue sections were washed three times and incubated with Alexa Fluor488 goat anti-mouse IgG (1:100 dilution; Molecular Probes, Eugene, OR) for 1 h at room temperature. Images of tissue sections were acquired at 100× magnification using an inverted microscope (Diaphot-TMD; Nikon Instruments, Melville, NY) and a Retiga 1300 digital camera (QImaging, Burnaby, BC, Canada).
Statistical Analysis
Data were expressed as mean ± standard deviation and statistical significance (defined as p < 0.05) was determined using Student’s t-test.
RESULTS
Mechanical Strength of Cell-free Fibrin Hydrogels is Proportional to Fibrinogen Concentration
Previous work demonstrated that increasing the fibrinogen (FBG) concentration increased the number of fiber bundles at the expense of fiber bundle thickness (33). To examine the effects of these structural changes on mechanical properties, we measured the ultimate tensile force (UTF) and burst pressure of cylindrical, cell-free fibrin hydrogels as a function of FBG concentration. We found that increasing FBG concentration increased UTF and ultimate tensile stress (UTS) of fibrin hydrogels in a dose dependent way (Fig. 1A).
High fibrinogen concentration increased the mechanical strength of fibrin hydrogels. Ultimate tensile force and stress (A) and burst pressure (B) of cell-free fibrin hydrogels as a function of FBG concentration. Data are mean ± standard error of four independent experiments. The symbols (* and ×) indicate p < 0.05 compared to samples containing 2.5 mg/mL FBG.
We also prepared longer TEV (4 cm in length) and measured the pressure to burst by filling the lumen with PBS and record the pressure using a pressure transducer. Similar to UTF, we found that the burst pressure increased significantly (Fig. 1B; black bars) and in a FBG dose dependent manner. Interestingly, when water was removed by centrifugation of fibrin constructs, the burst pressure increased further, reaching approximately 160 mmHg at the highest FBG concentration of 30 mg/ml.
High Fibrinogen Concentration Decreases TEV Compaction and Smooth Muscle Contractility
Next we examined whether embedding smooth muscle cells (SMC; 106 cells/mL) in fibrin hydrogels of high FBG concentration would increase TEV strength even further. Similar to our data with larger diameter mandrel (6.4 mm) (31), we observed that increasing FBG concentration decreased fibrin hydrogel compaction in a dose dependent manner (Fig. 2A). Specifically, for 2.5 mg/mL FBG, TEV compacted to less than 5% of their original volume after 2 weeks culture, but compaction decreased at higher FBG concentrations and was diminished at a FBG concentration of 15 mg/ml (Fig. 2A). As expected higher FBG concentrations increased UTF by two-fold and decreased UTS mainly due to increased tissue thickness (Fig. 2C). However, vascular reactivity in response to KCl decreased in a dose dependent manner suggesting that cellular function might be compromised at high FBG concentrations (Fig. 2B). Indeed, a colorimetric proliferation assay (MTT assay) showed reduced viability of cells in gels with 30 mg/ml FBG compared to those with 2.5 mg/ml FBG (data not shown).
High fibrinogen concentration decreased hydrogel compaction and vascular reactivity of TEV. SMC were embedded in fibrin gels and cultured around a 4.0 mm cylindrical mandrel with the indicated concentrations of FBG. The fibrin gels contained 106 cells/mL, Ca2+ (2.5 mM) and thrombin (2.5 U/mL). After 2 weeks in culture the tissues were photographed to measure compaction and mounted on a force transducer to measure mechanical strength and reactivity. (A) Fibrin hydrogel compaction; (B) ultimate tensile force and stress; (C) vascular reactivity in response to KCl. Data are presented as mean ± standard deviation of triplicate samples in a representative experiment (n = 3). The symbols (* and ×) indicate p < 0.05 compared to samples containing 2.5 mg/mL FBG.
These results suggested that while vascular reactivity requires active contractile cellular machinery, mechanical strength may depend primarily on the fibrin hydrogel. To test this hypothesis, TEV were cultured for two weeks and then treated with the actin polymerization inhibitor, cytochalasin D, or the cytotoxic agent, sodium azide for 24 h. Then vascular reactivity was measured in response to two agonists that cause contraction by different mechanisms: KCl, which opens the l-type, slow calcium potential dependent channels and NE, which acts through alpha1 and alpha2 receptors. Indeed, treatment of TEV with cytochalasin D or sodium azide diminished vascular reactivity to both KCl and NE without significantly affecting the magnitude of UTS (Fig. 3A, B).
Contribution of SMC to TEV contractility vs. mechanical strength. SMC were embedded in fibrin gels (106 cells/mL) and cultured around 4.0 mm cylindrical mandrels for two weeks before treatment with cytochalasin D (CytoD; 10 μg/mL) or sodium azide (NaN3; 1% w/v) for 24 h. The next day, the tissues were removed from the mandrels to measure (A) ultimate tensile force and stress; and (B) vascular reactivity in response to KCl or NE. The Krebs–Ringer solution was supplemented with cytochalasin D (10 μg/mL) or sodium azide (1% w/v) during the measurements of vascular contractility. Data are presented as mean ± standard deviation of triplicate samples in a representative experiment (n = 3).
Bi-layered TEV Exhibit Increased Strength Without Compromising Smooth Muscle Contractile Function
These results prompted us to hypothesize that double-layered TEV may show increased strength while maintaining the contractile function of embedded cells. To this end, we prepared TEV that were composed of two layers: a cellular layer containing SMC to provide compaction and vascular reactivity and a cell-free layer to provide mechanical strength. SMC (106 cells/mL) were embedded in fibrin hydrogels containing low concentration of FBG (2.5 mg/mL) and allowed to polymerize around 4.0 mm mandrels. After 3 days in culture, fibrin hydrogels compacted to approximately 5% of their initial volume indicating that the cells had developed active contractile machinery. At that time, a second layer of cell-free fibrin hydrogel containing high concentrations of FBG (ranging from 10–30 mg/mL) was added around the first layer. After two weeks in culture, the second gel layer was partially degraded (~50%) when FBG concentration was 10 or 20 mg/mL, possibly due to conversion of plasminogen to plasmin by the cells of the inner layer. In contrast, degradation of the second layer was minimal at 30 mg/ml FBG. The thickness of bi-layered TEV with 10, 20 or 30 mg/ml FBG in the outer layer was 0.649 ± 0.109 mm (n = 5), 0.773 ± 0.083 mm (n = 5), or 0.926 ± 0.066 mm (n = 5), respectively. The thickness of single-layered TEV was significantly lower at 0.305 ± 0.051 mm (n = 8).
We also examined the effect of the time of addition of the second layer on the properties of the resulting TEV. We found that addition of the second cell-free fibrin layer (30 mg/mL of FBG) at 3, 5 or 7 days after the first layer had no effect on strength or vascular reactivity (data not shown). However, addition of the cell-free layer after 13 days prevented integration of the two layers and resulted in delamination. Therefore, in all experiments shown here, the second layer of fibrin was added on day 3 after the first layer.
Mechanical Properties and Contractility of Bi-layered TEV
Next we measured mechanical strength of single and bi-layered TEV. In agreement with our data using cell-free constructs (Fig. 1), the UTF of double-layered TEV increased significantly with increasing FBG concentration in the outer layer (Fig. 4A). Specifically, the UTF of bi-layered TEV with 30 mg/ml FBG in the outer layer increased by five-fold as compared to single-layer TEV. On the other hand, UTS remained unchanged with addition of the second layer (Fig. 4A), suggesting that UTF increased in proportion to tissue thickness.
A second layer of fibrin increased strength and maintained vascular reactivity. Bi-layered TEV were constructed by sequential layering of two fibrin hydrogels in a concentric cylindrical arrangement. The first layer was formed around a 4.0-mm cylindrical mandrel and contained SMC (106 cells/mL) in fibrin hydrogel (FBG, 2.5 mg/mL). After 3 days in culture, a second layer of cell-free fibrin gel with the indicated FBG concentration was added around the first layer. After 2 weeks in culture, the tissues were removed from the mandrel to measure mechanical strength and reactivity. (A) Ultimate tensile force and stress; (B) vasoconstriction in response to KCl. Data are presented as means ± standard deviation of triplicate samples in a representative experiment (n = 3). The symbol (×) indicates p < 0.05 compared with single-layered TEV containing 2.5 mg/mL FBG.
We also measured smooth muscle contractility in response to KCl, a vasoconstrictor that causes contraction by opening the L-type, slow calcium potential dependent channels. Interestingly, the contractile force of bi-layered constructs was similar to that of single layered tissues (Fig. 4B), suggesting that smooth muscle contractility was not affected by addition of the second fibrin layer. As expected when the force of contraction was divided by area, the resulting stress decreased with increasing FBG concentration, mainly due to increased thickness of tissue constructs (Fig. 4B).
Burst pressure measurements of longer TEVs (~4 cm) showed that addition of the second cell-free fibrin layer increased burst pressure by approximately ten-fold. Specifically, the burst pressure increased from 18 ± 7.7 mmHg (n = 4) for single-layered TEV to 177 ± 5.3 mmHg (n = 4) for bi-layered TEV with 30 mg/mL FBG in the cell-free layer.
Bi-layered TEV with SMC in the Outer Layer
Next we examine whether the position of cells in the inner or outer layer would affect TEV contractility. To this end, we prepared TEV with a cell-free inner layer and a second layer containing cells. The first layer was polymerized around a 4.0 mm mandrel for one hour and a second layer of fibrin (2.5 mg/ml of FBG) containing SMC (106 cells/ml) was polymerized around the first one. The next day the second layer was detached from the wall of the tube to allow the cells to compact the matrix. After two weeks in culture, the second layer compacted significantly and the two layers appeared indistinguishable. At that time the thickness of bi-layered TEV with 10, 20 or 30 mg/ml FBG in the inner layer was 0.44 ± 0.11 mm (n = 5), 0.75 ± 0.088 mm (n = 5), or 1.207 ± 0.39 mm (n = 5), respectively.
Surprisingly, UTF did not increase to the same extent in this configuration. Specifically, for 30 mg/ml FBG in the inner layer UTF increased by 2.5-fold as compared to five-fold when cells were in the inner layer. As a result, UTS decreased with increasing FBG concentration in the cell-free layer (Fig. 5A). On the other hand, vascular contractility was unaffected by the addition of the second cell-free layer (Fig. 5B).
Bi-layered TEV with cell-free fibrin gel in the inner layer. Bi-layered TEV were constructed by sequential layering of two fibrin hydrogels in a concentric cylindrical arrangement. The cell-free fibrin layer was formed around a 4.0-mm cylindrical mandrel and contained different FBG concentrations as indicated. The outer layer contained SMC (106 cells/mL) in low FBG (2.5 mg/ml) fibrin. After 2 weeks in culture TEV were removed from the mandrel to measure (A) ultimate tensile force and stress; and (B) vasoconstriction in response to KCl. Data are presented as mean ± standard deviation of triplicate samples in a representative experiment (n = 3). The symbols (* and ×) indicate p < 0.05 compared to samples containing 2.5 mg/mL FBG.
Morphological Evaluation of Bi-layered TEV
Histological evaluation showed that SMC were distributed uniformly in the inner layer and did not migrate into the outer fibrin layer (Fig. 6A). In addition, immunostaining showed that SMC in bi-layered TEV expressed α-actin, calponin and myosin heavy chain, which represent early, intermediate and late markers of SMC differentiation respectively (Fig. 6B–D). Similar results were obtained when SMC were added in the outer layer (data not shown).
Histological organization and immunostaining of bi-layered TEV. After 2 weeks in culture, single or bi-layered TEV were removed from the mandrels and processed for histology and immunohistochemistry. Paraffin sections of (A) single-layered or (B) bi-layered TEV were stained with hematoxylin and eosin (bar = 20 μm). The dotted line demarcates the boundary between cell-free and cell-containing layers. Paraffin sections of bi-layered TEV were also stained for SMC differentiation markers (C) α-actin; (D) calponin; or (E) myosin heavy chain (bar = 10 μm).
DISCUSSION
Several studies demonstrated that application of mechanical forces and careful selection of biomaterials increased mechanical strength of TEV. Mechanical forces have been shown to modulate the SMC phenotype in two dimensional cultures (34–36) and cyclic mechanical loading was shown to increase the function of three-dimensional engineered smooth muscle tissues (10,16,37,38). Synthetic biomaterials have been designed to provide strength and elasticity. Specifically, polyglycolic acid has been copolymerized with several other polymers such as poly-L-lactic acid (39), polycaprolactone (40–42), poly-4-hydroxybutyrate (43) or polyethylene glycol (44) with various degrees of success. On the other hand, natural biomaterials such as collagen have been cross-linked with various chemicals e.g. gluteraldehyde or carbodiimide (45,46), which increased mechanical strength albeit at the expense of cell viability (47,48).
Here we demonstrated a simple method to increase mechanical strength without compromising cellular function. Specifically, we engineered TEV with two fibrin layers: a cellular layer to provide vasoreactivity and matrix remodeling and a cell-free layer to provide mechanical strength. Our results showed that the UTF of bi-layered TEV increased with increasing FBG concentration in the cell-free layer but KCl-induced vasoconstriction was similar to that of single-layered tissues, suggesting that SMC maintained their contractile properties. Interestingly, mechanical strength increased to a lesser extent when cells were added in the outer layer of bi-layered TEV. A potential explanation may be found by examining the state of cells when the second layer was added. When SMC were placed in the outer layer, they started to compact the fibrin matrix immediately, possibly causing partial degradation of the inner cell-free layer by converting plasminogen to plasmin. On the other hand, when SMC were placed in the inner layer, the second cell-free layer was added three days later, when compaction of the first layer was almost complete. At that time, the proteolytic activity of cells might be lower, thus affecting the structure of the cell-free layer to a lesser extent and resulting in higher UTF. Further experiments are required to address this hypothesis and determine a possible link between fibrin compaction and proteolytic activity of the embedded SMC.
It may be possible to polymerize the second fibrin layer in situ during TEV implantation. After securing the TEV in place by sutures, fibrin may be polymerized around the implant to provide a reinforcing layer. The angiogenic properties of fibrin may promote fast vascularization (49–52) and since fibrin also promotes collagen synthesis (20–22), the outer layer may be remodeled by the incoming cells to resemble the adventitia. At the same time the fibrin cell-free layer can be used as a device to deliver growth factors or genes to enhance the function of implanted TEV. Genetic engineering and chemical methods have already been developed to conjugate growth factors or genes into fibrin hydrogels and release them in a cell-controlled manner (53,54). This approach has been used for release of several growth factors including VEGF (55,56), NGF (57) or KGF (32) both in vitro and in vivo. In this case, matrix-mediated gene delivery may be used to improve matrix production, angiogenesis or patency of the implanted TEV.
In single layered TEV with SMC embedded in hydrogels of high FBG concentration, compaction and KCl-induced vasoconstriction decreased in a dose dependent manner, suggesting that fibrin remodeling may be necessary for development of functional TEV. SMC bind to fibrinogen and fibrin through integrin αvβ3 eliciting a series of biological responses including degradation of fibrin and synthesis of new extracellular matrix such as collagen and elastin (20–22,58,59). Blocking fibrin degradation with aprotinin decreased compaction and vasoreactivity in a dose dependent manner similar to increasing the concentration of FBG (31). However, addition of TGF-β1 and insulin induced collagen synthesis and counteracted the negative effects of aprotinin on vascular reactivity (31). Taken together these data suggests that remodeling of the fibrin matrix may be necessary for development of SMC contractility as measured by compaction and vascular reactivity.
Interestingly, the strength of fibrin gels increased significantly in the presence of cells. Specifically, UTF increased by ~80% and UTS increased by more than ten-fold, as the cells compacted the gels to less than 5% of their original volume resulting in significantly thinner vascular rings. It is not clear how the presence of cells improved the strength of fibrin hydrogels but several possibilities may be worth investigating. One possibility may be that gel compaction decreased the water content thereby increasing the density of fibrin fibers and mechanical strength. Indeed, our results showed that reducing the water content by centrifugation of fibrin tubes improved the burst pressure by ~50%, suggesting that this mechanism may account at least in part for improved mechanical properties. Alternatively, SMC have been shown to remodel the fibrin matrix and deposit new extracellular matrix including collagen and to a lesser extent elastin (22,60). Such matrix remodeling may have also contributed to increased strength. Further investigation is required to assess the relative contribution of each mechanism or identify additional mechanisms that may be at work.
Interestingly, the UTF of bi-layered TEV was similar to that of cell-free high FBG hydrogels, suggesting that mechanical strength may result from the high concentration hydrogel. On the other hand, vascular reactivity of bi-layered TEV was comparable to single layer constructs, suggesting that reactivity may be the contribution of cells alone. Indeed, treatment of TEV with cytochalasin D or sodium azide diminished vasoconstriction without affecting the magnitude of UTF significantly, suggesting that the cell-free layer provides mechanical strength while the cell-containing layer provides vascular reactivity and matrix remodeling. This finding may suggest that the ideal scaffold for vascular tissue engineering may be a hybrid biomaterial composed of a porous natural or polymeric scaffold infiltrated with fibrin hydrogel. In this composite the polymer may provide mechanical strength that satisfies the requirement for arterial implantation while fibrin may promote contractility and extracellular matrix synthesis thereby supporting SMC function. Such biomaterials are currently under investigation in our laboratory.
References
M. Gaudino, C. Cellini, C. Pragliola, C. Trani, F. Burzotta, G. Schiavoni, G. Nasso, and G. Possati. Arterial versus venous bypass grafts in patients with in-stent restenosis. Circulation 112:I265–269 (2005).
J. K. Drury, T. R. Ashton, J. D. Cunningham, R. Maini, and J. G. Pollock. Experimental and clinical experience with a gelatin impregnated Dacron prosthesis. Ann. Chir. Vasc 1:542–547 (1987).
M. Pasic, W. Muller-Glauser, B. Odermatt, M. Lachat, B. Seifert, and M. Turina. Seeding with omental cells prevents late neointimal hyperplasia in small-diameter Dacron grafts. Circulation 92:2605–2616 (1995).
M. Deutsch, J. Meinhart, T. Fischlein, P. Preiss, and P. Zilla. Clinical autologous in vitro endothelialization of infrainguinal ePTFE grafts in 100 patients: a 9-year experience. Surgery 126:847–855 (1999).
T. Huynh, G. Abraham, J. Murray, K. Brockbank, P. O. Hagen, and S. Sullivan. Remodeling of an acellular collagen graft into a physiologically responsive neovessel. Nat. Biotechnol 17:1083–1086 (1999).
A. Bader, G. Steinhoff, K. Strobl, T. Schilling, G. Brandes, H. Mertsching, D. Tsikas, J. Froelich, and A. Haverich. Engineering of human vascular aortic tissue based on a xenogeneic starter matrix. Transplantation 70:7–14 (2000).
S. Kaushal, G. E. Amiel, K. J. Guleserian, O. M. Shapira, T. Perry, F. W. Sutherland, E. Rabkin, A. M. Moran, F. J. Schoen, A. Atala, S. Soker, J. Bischoff, and J. E. Mayer, Jr. Functional small-diameter neovessels created using endothelial progenitor cells expanded ex vivo.[comment]. Nat. Med 7:1035–1040 (2001).
N. L’Heureux, S. Paquet, R. Labbe, L. Germain, and F. A. Auger. A completely biological tissue-engineered human blood vessel. [comment]. FASEB J 12:47–56 (1998).
N. L’Heureux, J. C. Stoclet, F. A. Auger, G. J. Lagaud, L. Germain, and R. Andriantsitohaina. A human tissue-engineered vascular media: a new model for pharmacological studies of contractile responses. FASEB J 15:515–524 (2001).
L. E. Niklason, J. Gao, W. M. Abbott, K. K. Hirschi, S. Houser, R. Marini, and R. Langer. Functional arteries grown in vitro. Science 284:489–493 (1999).
L. E. Niklason, W. Abbott, J. Gao, B. Klagges, K. K. Hirschi, K. Ulubayram, N. Conroy, R. Jones, A. Vasanawala, S. Sanzgiri, and R. Langer. Morphologic and mechanical characteristics of engineered bovine arteries. J. Vasc. Surg 33:628–638 (2001).
S. P. Higgins, A. K. Solan, and L. E. Niklason. Effects of polyglycolic acid on porcine smooth muscle cell growth and differentiation. J. Biomed. Mater. Res 67A:295–302 (2003).
V. H. Barocas, T. S. Girton, and R. T. Tranquillo. Engineered alignment in media equivalents: magnetic prealignment and mandrel compaction. J. Biomech. Eng 120:660–666 (1998).
D. Seliktar, R. A. Black, R. P. Vito, and R. M. Nerem. Dynamic mechanical conditioning of collagen-gel blood vessel constructs induces remodeling in vitro. Ann. Biomed. Eng 28:351–362 (2000).
D. Seliktar, R. M. Nerem, and Z. S. Galis. The role of matrix metalloproteinase-2 in the remodeling of cell-seeded vascular constructs subjected to cyclic strain. Ann Biomed Eng 29:923–934 (2001).
D. Seliktar, R. M. Nerem, and Z. S. Galis. Mechanical strain-stimulated remodeling of tissue-engineered blood vessel constructs. Tissue Eng 9:657–666 (2003).
J. P. Stegemann, and R. M. Nerem. Altered response of vascular smooth muscle cells to exogenous biochemical stimulation in two- and three-dimensional culture. Exp. Cell Res 283:146–155 (2003).
M. Thie, W. Schlumberger, R. Semich, J. Rauterberg, and H. Robenek. Aortic smooth muscle cells in collagen lattice culture: effects on ultrastructure, proliferation and collagen synthesis. Eur. J. Cell Biol 55:295–304 (1991).
R. A. Clark, L. D. Nielsen, M. P. Welch, and J. M. McPherson. Collagen matrices attenuate the collagen-synthetic response of cultured fibroblasts to TGF-beta. J. Cell Sci 108:1251–1261 (1995).
T. L. Tuan, A. Song, S. Chang, S. Younai, and M. E. Nimni. In vitro fibroplasia: matrix contraction, cell growth, and collagen production of fibroblasts cultured in fibrin gels. Exp. Cell Res 223:127–134 (1996).
E. D. Grassl, T. R. Oegema, and R. T. Tranquillo. A fibrin-based arterial media equivalent. J. Biomed. Mater. Res 66A:550–561 (2003).
J. L. Longand, and R. T. Tranquillo. Elastic fiber production in cardiovascular tissue-equivalents. Matrix Biol 22:339–350 (2003).
D. D. Swartz, J. A. Russell, and S. T. Andreadis. Engineering of fibrin-based functional and implantable small-diameter blood vessels. Am. J. Physiol. Heart Circ. Physiol 288:H1451–H1460 (2005)Epub 2004 Oct 1414.
B. C. Isenbergand, and R. T. Tranquillo. Long-term cyclic distention enhances the mechanical properties of collagen-based media-equivalents. Ann. Biomed. Eng 31:937–949 (2003).
T. S. Girton, T. R. Oegema, and R. T. Tranquillo. Exploiting glycation to stiffen and strengthen tissue equivalents for tissue engineering. J. Biomed. Mater. Res 46:87–92 (1999).
T. S. Girton, T. R. Oegema, E. D. Grassl, B. C. Isenberg, and R. T. Tranquillo. Mechanisms of stiffening and strengthening in media-equivalents fabricated using glycation. J. Biomech. Eng 122:216–223 (2000).
K. Ishibashiand, and T. Matsuda. Reconstruction of a hybrid vascular graft hierarchically layered with three cell types. Asaio. J 40:M284–290 (1994).
T. Matsudaand, and H. Miwa. A hybrid vascular model biomimicking the hierarchic structure of arterial wall: neointimal stability and neoarterial regeneration process under arterial circulation. J. Thorac. Cardiovasc. Surg 110:988–997 (1995).
J. D. Berglund, M. M. Mohseni, R. M. Nerem, and A. Sambanis. A biological hybrid model for collagen-based tissue engineered vascular constructs. Biomaterials 24:1241–1254 (2003).
D. J. Geer, D. D. Swartz, and S. T. Andreadis. In vivo model of wound healing based on transplanted tissue-engineered skin. Tissue Eng 10:1006–1017 (2004).
L. Yao, D. D. Swartz, S. F. Gugino, J. A. Russell, and S. T. Andreadis. Fibrin-based tissue-engineered blood vessels: differential effects of biomaterial and culture parameters on mechanical strength and vascular reactivity. Tissue Eng 11:991–1003 (2005).
D. J. Geer, D. D. Swartz, and S. T. Andreadis. Biomimetic delivery of keratinocyte growth factor upon cellular demand for accelerated wound healing in vitro and in vivo. Am. J. Pathol 167:1575–1586 (2005).
C. B. Herbert, C. Nagaswami, G. D. Bittner, J. A. Hubbell, and J. W. Weisel. Effects of fibrin micromorphology on neurite growth from dorsal root ganglia cultured in three-dimensional fibrin gels. J. Biomed. Mater. Res 40:551–559 (1998).
J. D. Smith, N. Davies, A. I. Willis, B. E. Sumpio, and P. Zilla. Cyclic stretch induces the expression of vascular endothelial growth factor in vascular smooth muscle cells. Endothelium 8:41–48 (2001).
W. Li, Q. Chen, I. Mills, and B. E. Sumpio. Involvement of S6 kinase and p38 mitogen activated protein kinase pathways in strain-induced alignment and proliferation of bovine aortic smooth muscle cells. J. Cell Physiol 195:202–209 (2003).
Q. Chen, W. Li, Z. Quan, and B. E. Sumpio. Modulation of vascular smooth muscle cell alignment by cyclic strain is dependent on reactive oxygen species and P38 mitogen-activated protein kinase. J. Vasc. Surg 37:660–668 (2003).
B. S. Kim, J. Nikolovski, J. Bonadio, and D. J. Mooney. Cyclic mechanical strain regulates the development of engineered smooth muscle tissue. Nat. Biotechnol 17:979–983 (1999).
J. Nikolovski, B. S. Kim, and D. J. Mooney. Cyclic strain inhibits switching of smooth muscle cells to an osteoblast-like phenotype. FASEB J 17:455–457 (2003)Epub 2003 Jan 2002.
B. S. Kim, J. Nikolovski, J. Bonadio, E. Smiley, and D. J. Mooney. Engineered smooth muscle tissues: regulating cell phenotype with the scaffold. Exp. Cell Res 251:318–328 (1999).
T. Shin’oka, Y. Imai, and Y. Ikada. Transplantation of a tissue-engineered pulmonary artery. N. England J. Med 344:532–533 (2001).
M. Watanabe, T. Shin’oka, S. Tohyama, N. Hibino, T. Konuma, G. Matsumura, Y. Kosaka, T. Ishida, Y. Imai, M. Yamakawa, Y. Ikada, and S. Morita. Tissue-engineered vascular autograft: inferior vena cava replacement in a dog model. Tissue Eng 7:429–439 (2001).
S. H. Lee, B. S. Kim, S. H. Kim, S. W. Choi, S. I. Jeong, I. K. Kwon, S. W. Kang, J. Nikolovski, D. J. Mooney, Y. K. Han, and Y. H. Kim. Elastic biodegradable poly(glycolide-co-caprolactone) scaffold for tissue engineering. J. Biomed. Mater. Res. A 66:29–37 (2003).
S. P. Hoerstrup, A. Kadner, C. Breymann, C. F. Maurus, C. I. Guenter, R. Sodian, J. F. Visjager, G. Zund, and M. I. Turina. Living, autologous pulmonary artery conduits tissue engineered from human umbilical cord cells. Ann. Thorac. Surg 74:46–52 (2002)discussion 52.
M. C. Wake, P. K. Gupta, and A. G. Mikos. Fabrication of pliable biodegradable polymer foams to engineer soft tissues. Cell Transplant 5:465–473 (1996).
M. E. Nimni, D. Cheung, B. Strates, M. Kodama, and K. Sheikh. Chemically modified collagen: a natural biomaterial for tissue replacement. J. Biomed. Mater. Res 21:741–771 (1987).
L.H. Olde Damink, P.J. Dijkstra, M.J. van Luyn, P.B. van Wachem, P. Nieuwenhuis, and J. Feijen. Cross-linking of dermal sheep collagen using a water-soluble carbodiimide. Biomaterials 17:765–773 (1996).
P. B. van Wachem, M. J. van Luyn, L. H. Olde Damink, P. J. Dijkstra, J. Feijen, and P. Nieuwenhuis. Biocompatibility and tissue regenerating capacity of crosslinked dermal sheep collagen. J. Biomed. Mater. Res 28:353–363 (1994).
M. J. van Luyn, P. B. van Wachem, L. O. Damink, P. J. Dijkstra, J. Feijen, and P. Nieuwenhuis. Relations between in vitro cytotoxicity and crosslinked dermal sheep collagens. J. Biomed. Mater Res 26:1091–1110 (1992).
H. F. Dvorak, V. S. Harvey, P. Estrella, L. F. Brown, J. McDonagh, and A. M. Dvorak. Fibrin containing gels induce angiogenesis. Implications for tumor stroma generation and wound healing. Lab. Invest 57:673–686 (1987).
A. Takei, Y. Tashiro, Y. Nakashima, and K. Sueishi. Effects of fibrin on the angiogenesis in vitro of bovine endothelial cells in collagen gel. In Vitro Cell Dev. Biol. Anim 31:467–472 (1995).
P. Hudlett, A. Neuville, A. Miternique, C. Griffon, D. Weltin, and D. Stephan. Angiogenesis and arteriogenesis are increased in fibrin gel chambers implanted in prehypertensive spontaneously hypertensive rats. J. Hypertens 23:1559–1564 (2005).
L. Martineauand, and C. J. Doillon. Angiogenic response of endothelial cells seeded dispersed versus on beads in fibrin gels. Angiogenesis 10:269–277 (2007).
J. C. Schense, J. Bloch, P. Aebischer, and J. A. Hubbell. Enzymatic incorporation of bioactive peptides into fibrin matrices enhances neurite extension. Nat. Biotechnol 18:415–419 (2000).
S. E. Sakiyama-Elbertand, and J. Hubbell. Development of fibrin derivatives for controlled release of heparin- binding growth factors. J. Control Release 65:389–402 (2000).
A. H. Zisch, U. Schenk, J. C. Schense, S. E. Sakiyama-Elbert, and J. A. Hubbell. Covalently conjugated VEGF-fibrin matrices for endothelialization. J. Control Release 72:101–113 (2001).
A. H. Zisch, M. P. Lutolf, M. Ehrbar, G. P. Raeber, S. C. Rizzi, N. Davies, H. Schmokel, D. Bezuidenhout, V. Djonov, P. Zilla, and J. A. Hubbell. Cell-demanded release of VEGF from synthetic, biointeractive cell ingrowth matrices for vascularized tissue growth. FASEB J 17:2260–2262 (2003).
S. E. Sakiyama-Elbertand, and J. A. Hubbell. Controlled release of nerve growth factor from a heparin-containing fibrin-based cell ingrowth matrix. J. Control Release 69:149–158 (2000).
S. L. Brown, C. H. Lundgren, T. Nordt, and S. Fujii. Stimulation of migration of human aortic smooth muscle cells by vitronectin: implications for atherosclerosis. Cardiovasc. Res 28:1815–1820 (1994).
J. I. Jones, T. Prevette, A. Gockerman, and D. R. Clemmons. Ligand occupancy of the alpha-V-beta3 integrin is necessary for smooth muscle cells to migrate in response to insulin-like growth factor. Proc. Natl. Acad. Sci. USA 93:2482–2487 (1996).
J. J. Rossand, and R. T. Tranquillo. ECM gene expression correlates with in vitro tissue growth and development in fibrin gel remodeled by neonatal smooth muscle cells. Matrix Biol 22:477–490 (2003).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yao, L., Liu, J. & Andreadis, S.T. Composite Fibrin Scaffolds Increase Mechanical Strength and Preserve Contractility of Tissue Engineered Blood Vessels. Pharm Res 25, 1212–1221 (2008). https://doi.org/10.1007/s11095-007-9499-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9499-6