Abstract
Microglia play a critical role in controlling the homeostasis of the brain, but over-activated microglia secrete pro-inflammatory mediators and cytokines, which induce neuronal cell death. Fucoxanthin (Fx), a marine carotenoid, has demonstrated a variety of beneficial health effects. Despite accumulating evidence supporting the immune-modulating effects of Fx in vitro, the underlying signaling pathways remain unknown. In the present study, Fx dose-dependently inhibited the secretion of lipopolysaccharide (LPS)-induced pro-inflammatory mediators including interleukin (IL)-6, tumor necrosis factor (TNF)-α, reactive oxygen species (ROS), prostaglandin (PG) E2, and nitric oxide (NO) productions, and also suppressed the expression of inducible NO synthase (iNOS) and cyclooxygenase (COX)-2 enzymes. Further, the reverse transcription-polymerase chain reaction (RT-PCR) analysis indicated IL-6, TNF-α, iNOS, and COX-2 mRNA expression were suppressed by treatment with Fx in a dose-dependently manner. The mechanism studies indicated that Fx blocks protein kinase B (Akt)/nuclear factor-kappaB (NF-κB) and mitogen-activated protein kinase (MAPKs)/transcription factor (AP)-1 pathways. In addition, we demonstrated that Fx increases nuclear factor erythroid 2-related factor (Nrf)-2 activation and heme oxygenase (HO)-1 expression in LPS-activated BV-2 microglia. Subsequently, we found that Fx also mediates the reactive oxygen species (ROS) by activating protein kinase A (PKA)/cyclic adenosine monophosphate (cAMP) response element binding protein (CREB) pathway, and promotes the production of brain-derived neurotrophic factor (BDNF). These results indicate that Fx may be more effective and potential than other candidates via either decreasing the pro-inflammatory factors production or increasing the neuroprotective molecules expression for therapy of neurodegenerative diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuro-inflammation is commonly involved in several neurodegenerative diseases including Parkinson’s disease and Alzheimer’s disease [1, 2]. Microglia, as resident central nervous system (CNS) immune cells, play an important role in the host defense and neuronal repair for the maintenance of CNS homeostasis through their strict activation [3, 4]. However, persistent microglial activation leads to neuronal cell death by the overproduction and accumulation of pro-inflammatory mediators such as nitric oxide (NO), reactive oxygen species (ROS), tumor necrosis factor (TNF)-α, interleukin (IL)-6, and prostaglandin (PG) E2. These factors are up-regulated by numerous intracellular pathways that involve several signal transduction molecules such as nuclear factor-kappa B (NF-κB), activator protein-1 (AP-1), and mitogen-activated protein kinases (MAPKs) [1, 2, 5]. Therefore, inhibitors of the specific pathway of microglial activation may act as therapeutic agents for neurodegenerative diseases.
Moreover, microglia also prevent damage to neighboring neurons by eliminating toxic materials by phagocytosis, and by expressing various detoxifying/antioxidant enzymes including heme oxygenase (HO)-1, cAMP response element binding protein (CREB), and brain-derived neurotrophic factor (BDNF) [6–8]. For example, HO-1 is considered a critical cellular response against the toxicity of oxidative stress and inflammatory responses both in vitro and in vivo for the catabolism of heme by a process that releases carbon monoxide, ferrous iron, and biliverdin to neutralize ROS, and NO production [9–12]. The expression of HO-1 is regulated by the nuclear factor erythroid 2-related factor (Nrf)-2, and CREB transcription factors [13, 14]. Thus, activation of both Nrf-2/HO-1 and PKA/CREB pathways also play crucial roles in the process of microglia de-activation [15, 16]. Furthermore, CREB facilitates the expression of a large and diverse group of genes including regulator of anti-oxidative and anti-inflammatory genes [17–20]. In summary, both the control of pro-inflammatory of factors and promotion of beneficial enzymes expression may be considered useful therapeutic strategies for neuro-inflammatory diseases.
Fucoxanthin (Fx), a marine carotenoid, is well-known to possess anti-oxidant, anti-cancer, anti-inflammatory, and anti-obesity properties [21]. Numerous studies have reported that Fx inhibits inflammatory mediators and pro-inflammatory cytokines in vitro and in vivo [22–26]. In vitro studies have reported that Fx exerts anti-inflammatory effects by inhibiting MAPKs including c-Jun N-terminal kinase (JNK), extracellular signal-regulated kinase (ERK), p38, and NF-κB in lipopolysaccharide (LPS)-induced RAW 264.7 macrophages and amyloid-β-induced microglia [22, 23, 25]. In vivo studies on Fx recently reported that it also inhibits inflammatory responses in LPS-induced uveitis and a carrageenan-induced paw edema model via inhibiting Akt, NF-κB, and MAPKs [25, 26]. These findings suggest that Fx may be a useful therapeutic candidate for inflammatory diseases owing to its inhibitory effects on NF-κB activation and MAPKs phosphorylation. Investigations of the anti-inflammatory mechanism of Fx have mostly been focused on the inhibition of pro-inflammatory factors via NF-κB and MAPKs molecules [22, 23]. In addition, Fx, which is an antioxidant increased the mRNA expression levels of superoxide dismutase (SOD) and glutathione (GSH) in hydrogen peroxide (H2O2)-stimulated BV-2 cells [23]. Furthermore, Fx also promoted the synthesis of glutamate-cysteine ligase catalytic subunit (GCLC) and glutathione synthetase (GSS) through the activation of the Akt/Nrf2 pathway in human skin cells [27]. However, the mechanism by which Fx reduces pro-inflammatory mediators, and activates beneficial enzymes remains to be clearly elucidated in a neuro-inflammatory model. In this study, we confirmed that Fx also inhibits NF-κB and MAPKs in LPS-activated BV-2 cells, and found that an upstream regulator of NF-κB, Akt is involved in microglial de-activation, and a downstream regulator of MAPKs, AP-1 was inhibited in LPS-activated BV-2 cells treated with Fx. Furthermore, Fx activates Nrf-2/HO-1 and PKA/CREB pathways in LPS-activated BV-2 cells.
Materials and Methods
Chemicals
The Fx (>98% purity), LPS (Escherichia coli 055:B5), and other chemicals were purchased from Sigma-Aldrich (St. Louis, MO, USA). All the primary antibodies including those against iNOS, COX-2, HO-1, Nrf-2, BDNF, phosphorylated (p)-CREB, CREB, p-PKA, PKA, p-JNK, JNK, p-ERK, ERK, p-p38, p38, p-Akt (Ser308), p-Akt (Thr473), Akt, p-NF-κB, LiminB1, and glyceraldehyde 3-phosphate dehydrogenase (GAPDH), as well as the anti-rabbit horseradish peroxidase (HRP)-linked IgG antibodies were purchased from Cell Signaling Technology (Beverly, MA, USA) while the primers were ordered from Cosmogenetech (Seoul, Korea). The Alexa Fluor 488-labled goat anti-rabbit IgG antibody, Superscript Ш reverse transcriptase kit, and Trizol reagent were purchased from Invitrogen (Eugene, OR, USA).
Cell Culture and Viability
The BV-2 cells were generously provided by Dr. Sung Joong Lee (Seoul National University, Seoul, Korea), and maintained in Dulbecco’s modified Eagle’s medium (DMEM, Gibco, USA) supplemented with 5% heat-inactivated fetal bovine serum (FBS, Gibco) and 1% penicillin–streptomycin at 37 °C under a humidified atmosphere of 5% CO2. To determine the effects of Fx on cell viability, the cells (2.5 × 104 cells/well) were seeded into 96-well plates at 37 °C incubation for 24 h, and then were treated with various concentration of Fx (5, 10, and 20 μM) in the presence or absence of LPS (100 ng/mL) for 12 h. The cell viability was measured by adding the EZ-Cytox (1:10; DAEILLAB Co., Ltd., Seoul, Korea) followed by incubation at 37 °C for 30 min. Then, the absorbance of the reaction solution was determined using a micro-plate reader (BIO-TEK@ Dower Wave XS, Winooski, VT, USA) at 450 nm.
Determination of ROS
To detect the effects of Fx on ROS production, the cells (5 × 105 cells/well) were seeded for 24 h, pre-treated with various concentration of Fx for 1 h, and then co-treated with LPS (100 ng/mL) for 12 h. The culture medium was removed and the cells were gently washed twice with 1 mL phosphate buffered saline (1× PBS). Then, the cells were incubated with 2′,7′-dichlorofluorescin diacetate (DCF-DA) at a concentration of 20 μΜ diluted with FBS-free DMEM protected from light at 37 °C for 1 h. After washing, the cells were collected using 0.5 mL trypsin for each well, the reaction was stopped by adding 0.8 mL DMEM with 5% FBS, and then the cells were centrifuged at 2000 rpm for 2 min, followed by suspension in PBS. The intracellular ROS was determined by measuring the mean fluorescence intensity of 10,000 cells using a flow cytometer (BD FACSCablibur, USA) at excitation and emission wavelengths 480 and 520 nm, respectively.
Enzyme-Linked Immunosorbent Assay (ELISA)
The cells (5 × 105 cells/well) were seeded for 24 h, pre-treated with various concentration of Fx for 1 h, and then co-treated with LPS (100 ng/mL) at 37 °C for 12 h. The culture medium was collected and centrifuged at 13,000 rpm for 5 min. The levels of PGE2, IL-6, and TNF-α in the culture medium were quantified using ELISA kits from R&D System Inc. (Minneapolis, MN, USA), according to the manufacturer’s instructions.
Reverse Transcription-Polymerase Chain Reaction (RT-PCR)
The cells were seeded for 24 h, pre-treated with various concentrations of Fx for 1 h, and subsequently co-treated with 100 ng/mL LPS at 37 °C for 6 h. The total RNA was extracted using Trizol reagent and quantified using an ultraviolet–visible (UV–Vis) spectrophotometer (Thermo Fisher Scientific Inc, Lafayette, CA, USA), and 5 μg of RNA was converted to cDNA by using a Superscript Ш reverse transcriptase kit according to the manufacturer’s instructions. The target DNA bands were amplified by using 2 μL of primer pairs and 2 μL cDNA template, which were mixed with Novelzyme Taq Plus Premix (Noble Bio, Suwon, Korea), according to the manufacturer’s instructions. Then, the cDNAs were separated by electrophoresis on 1.5% agarose gels and stained using ethidium bromide buffer. The intensity of the PCR product was measured using the CoreBio i-MAX Gel Image Analysis System (CoreBio System, Seoul, Korea) and analyzed using the ImageJ software (National Institutes of Health, NIH Image in the public domain, USA). The following primer sets were used: IL-6 (sense: CCACTTCACAAGTCGGAGGCTT and anti-sense: CCAGCTTATCTGTTAGGAGA), TNF-α (sense: CATCTTCTCAAAATTCGAGTGACAA and anti-sense: ACTTGGGCAGATTGACCTCAG), iNOS (sense: CCCTTCCGAAGTTTCTGGCAGCAGC and anti-sense: GGCTGTCAGAGCCTCGT GGCTTTGG), COX-2 (sense: TTGAAGACCAGGAGTACAGC and anti-sense: GGTACAGTTCCATGACATCG). GAPDH (sense: TGATGACATCAAGAAGGTGGTGAAG and anti-sense: TCCTTGGAGGCCATGTAGGCCAT).
Quantification of NO Production
The concentration of NO produced in the culture supernatant was measured using Griess reagents (1% sulfanilamide, and N-[1-naphthyl]-ethylenediamine dihydrochloride in 2.5% H3PO4). Each 50 μL culture medium sample was reacted with equal volume of mixed Griess reagent (1:1) for 10 min under the dark condition. Different concentrations of sodium nitrite (0–100 μM) were used as the standard to assess nitrite concentration, and all of samples were detected at wavelength 540 nm.
Immunocytochemistry
For the immunohistochemistry analysis, the cells (5 × 104 cells/well) were seeded on poly-l-lysine coated glass coverslips in 24-well plates at 37 °C for 24 h, pre-treated with various concentrations of Fx for 1 h, and then incubated with LPS (100 ng/mL) for 12 h. Then, the cells were fixed with 3.8% paraformaldehyde in PBS at room temperature for 20 min, permeabilized with 0.5% Triton X-100 in PBS for 30 min, and then blocked in 5% bovine serum albumin (BSA) in PBS plus 0.1% Tween 20 (PBST) for 30 min. The cells were incubated in blocking buffer containing anti-Nrf-2 or p-CREB antibody (1:100) for 2 h at room temperature. After washing, the cells were reacted with Alexa Fluor 488-labeled secondary goat anti-rabbit IgG antibody (1:200). For nuclear staining, the cells were incubated with 25 μg/mL of 4′-6-diamidino-2-phenylindole (DAPI) in PBST at 37 °C for 30 min. The fluorescence images were captured and analyzed by using a confocal microscope (Leica, Solms, Germany).
Western Blot Analysis
The cells (5 × 105 cells/well) were seeded for 24 h, pre-treated with various concentration of Fx for 1 h, and then co-treated with LPS (100 ng/mL) for 12 h. Then, the cells were collected, lysed in ice-cold lysis buffer (Cell Signaling) containing 1× protease inhibitor cocktail (PIC, Roche, Penzberg, Germany) and 1× PMSF. The total protein was quantified using Bradford reagent (Bio-Rad, Hercules, CA, USA), and various concentrations of BSA as standard. The proteins in each sample were separated using 8 or 10% sodium dodecyl sulfate polyacrylamide (SDS–PAGE), and transferred to a polyvinylidene difluoride (PVDF, Millipore, USA) membrane, which was subsequently blocked with 5% BSA in TBST and incubated with the appropriate primary antibodies (1:1000) overnight at 4 °C. After washing with TBST, the membrane was incubated with the HRP-conjugated secondary antibodies (1:1500) for 1 h at room temperature. The blots were visualized using enhance chemiluminescence (ECL) Reagents (Thermo Fisher Scientific Inc., Lafayette, CA, USA). Densitometry analysis of bands was performed using the LAS4000 system (Fujifilm, Tokyo, Japan).
Statistical Analysis
The data were analyzed using the software Prism 5 software (Graph-Pad Software Inc, San Diego, CA, USA). All the data are expressed as mean ± standard error of the mean (SEM). The statistical comparisons between the different treatments were performed using a one-way analysis of variance (ANOVA) with the Newman–Keuls multiple comparison test and p < 0.05 was considered statistically significant.
Results
Effects of Fx on Viability and ROS Production in LPS-Activated BV-2 Microglial Cells
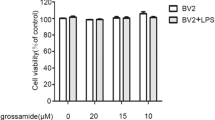
Our initial experiments revealed that treatment with Fx at concentrations of 5, 10, and 20 μM did not affect the viability of unstimulated and LPS (100 ng/mL)-stimulated BV-2 cells, respectively (Fig. 1a). Therefore, these results indicated that these concentrations of Fx could be used in all the subsequent experiments. Since ROS play an important role in neuronal cell death, we investigated the effects of Fx on intracellular ROS production by using a fluorescence sensitive probe DCF-DA. As shown in Fig. 1b, the level of intracellular ROS decreased by 28.3, 44.7, and 59.0% compared to that in the LPS-treated group at 5, 10, and 20 μM Fx, respectively. These results suggest that Fx may alleviate ROS-induced neuronal cells death, which is consistent with the results of previous study [23].
Effects of Fx on viability and ROS production in LPS-activated BV-2 microglial cells. a Viability of cells stained by EZ-Cytox for 30 min with absorbance determined at 450 nm. Results are percentage of control group. b Levels of intracellular ROS from three independent experiments were quantified. c Intracellular ROS levels measured by FACS. Values are mean ± standard error of the mean (SEM) of three independent experiments; ### p < 0.001 compared to control group, **p < 0.01, ***p < 0.001 compared to LPS group
Effects of Fx on Pro-Inflammatory Cytokines in LPS-Activated BV-2 Microglial Cells
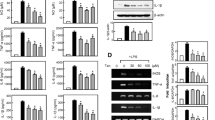
Next, we assessed the inhibitory effects of Fx on LPS-induced pro-inflammatory cytokines TNF-α and IL-6 by determining their secretory concentration in the cell culture supernatants using specific ELISA kit. Figure 2a shows that the secretion of TNF-α and IL-6 was significantly increased by stimulation with LPS. However, both cytokines were dose-dependently inhibited by treatment with Fx, which reduced TNF-α and IL-6 by 69.4 and 49.3% at 20 μM, respectively. Moreover, we analyzed the effects of Fx on mRNA expression of TNF-α and IL-6 by RT-PCR analysis. We found that LPS induced 7.8-fold and 14.3-fold increases in the synthesis of TNF-α and IL-6 mRNA, respectively (Fig. 2d), while pre-treatment with Fx significantly inhibited this effect dose-dependently (46.7, and 43.3%, decrease, respectively).
Effects of Fx on pro-inflammatory mediators, upstream regulator mRNA, and protein expression in LPS-activated BV-2 microglial cells. a Levels of TNF-α and IL-6 were measured using ELISA. b Production of NO was measured using Griess reagents. c Level of PGE2 was measured using ELISA. d The mRNA levels of TNF-α and IL-6 were measured using RT-PCR analysis. The mRNA level of GAPDH was loading control. e The mRNA levels of iNOS and COX-2 were measured using PCR analysis. The mRNA level of GAPDH was loading control. f Protein levels of iNOS and COX-2 were measured using western blot analysis. GAPDH protein was loading control. Values are mean ± SEM of three independent experiments; ### p < 0.001 compared to control group, **p < 0.01, and ***p < 0.001 compared to LPS group
Effects of Fx on NO and PGE2 Production, and iNOS and COX-2 Expression in LPS-Activated BV-2 Microglial Cells
The effect of Fx on NO and PGE2 production was assessed by assaying the conditioned medium from the treated cells. The LPS-stimulated microglia released a large amount of NO and PGE2 (Fig. 2b, c), which were dose-dependently reduced by treatment with Fx. Especially, pre-treatment with Fx at 20 μM significantly inhibited the productions of NO and PGE2 by 61.9, and 65%, respectively. Since the secretion of NO and PGE2 are regulated by the expression of iNOS and COX-2, respectively, we examined whether Fx has any effect on mRNA and protein expressions of iNOS and COX-2. As shown in Fig. 2e, f, pre-treatment with Fx significantly and dose-dependently decreased the levels of iNOS and COX-2 mRNA and protein, respectively. These results indicate that Fx can suppress LPS-induced NO and PGE2 by down-regulating iNOS and COX-2 at mRNA and protein expression in LPS-activated BV-2 microglia.
Effects of Fx on Expression of Akt/NF-κB Pathway in LPS-Activated BV-2 Microglial Cells
NF-κB is a key upstream regulator for production of pro-inflammatory mediators [28]. Thus, we tested whether Fx affects NF-κB activation by detecting the phosphorylation of NF-κB in LPS-activated microglia. Figure 3a showed that LPS-induced NF-κB phosphorylation was reduced in the presence of Fx, and similar data was observed in LPS-induced RAW 264.7 macrophages [22]. In attempt to investigate the upstream modulator of NF-κB, and confirm the relation between the Akt and NF-κB activation, we found that Fx significantly inhibits LPS-induced Akt (Thr308) phosphorylation, not significant for Akt (Ser473) in Fig. 3b. We also used a specific Akt inhibitor, LY294002 of 5 μM to partly abolish the LPS-induced p-NF-κB in nuclear of cells, which was reduced more by co-treatment of LY294002 and Fx (data not shown). These data indicate that Fx regulates NF-κB activation by blocking Akt phosphorylation.
Effects of Fx on Akt/NF-κB signaling pathway inhibition in LPS-activated BV-2 microglial cells. a Levels of p-NF-κB in nuclear fraction were measured using western blot analysis, and LiminB1 protein was loading control. b Level of phosphorylated Akt (Thr308 and Ser473) was measured using western blot. Total Akt was loading control. Values are mean ± SEM of three independent experiments; ## p < 0.01 compared to control group, *p < 0.05, **p < 0.01 compared to LPS group
Effects of Fx on Expression of MAPKs/AP-1 Pathway in LPS-Activated BV-2 Microglial Cells
Accumulating evidence has revealed that mitogen-activated protein kinases (MAPKs) signaling pathway play key regulatory roles in the production of pro-inflammatory mediators. Hence, whether the inhibition of pro-inflammatory mediators by Fx is mediated through the MAPKs signaling was examined in LPS-stimulated BV-2 cells. Figure 4a showed that Fx of 20 μM significantly inhibit the LPS-induced phosphorylation of three types of MAPKs which is consistent with previous reports [22, 23]. It is noteworthy that inhibitory effect of Fx on p38 is the largest among MAPKs. Furthermore, Fx also attenuated the downstream regulator of MAPKs, AP-1 activation (Fig. 4b). To confirm that Fx inhibits pro-inflammatory mediator through Akt/NF-κB and MAPKs (JNK/ERK/p38)/AP-1 pathways, specific inhibitors were used to abolish specific enzymes. As shown in Fig. 4c, NO production was significantly reduced by treatment of inhibitors, and co-treatment with Fx attenuated much more NO production. These data indicate that Fx inhibits pro-inflammatory mediators through suppressing Akt/NF-κB and MAPKs/AP-1 pathways.
Effects of Fx on MAPKs/AP-1 signaling pathway inhibition in LPS-activated BV-2 microglial cells. a Expression of three types of p-MAPKs (JNK, ERK, and p38) in total lysates were measured using western blot analysis with specific antibodies, and normalized by total MAPKs. b Expression levels of p-AP-1 (c-jun) in total lysates were measured using western blot analysis and normalized with total c-jun. c Microglial cells were pre-treated with specific inhibitors (JNK inhibitor: SP600125, ERK inhibitor: PD98059, p38 inhibitor: SB202190, Akt inhibitor: LY294002, NF-κB inhibitor: PDTC) for 30 min, and co-treated with Fx of 20 μM for 1 h, then co-treated with 100 ng/ml of LPS at 37 °C for 12 h. The NO production was detected using griess reagents. Values are mean ± SEM of three independent experiments; ### p < 0.01 compared to control group, ***p < 0.001 compared to LPS group
Effects of Fx on Expression of Nrf-2 and HO-1 in LPS-Activated BV-2 Microglial Cells
Previous studies showed that Nrf-2 is directly associate with the inhibition of the pro-inflammatory response, and activates HO-1, which is a key molecule for mediating the therapy of neuro-inflammation and cytoprotective effects [6, 11, 30]. Thus, we determined if the expression of Nrf-2 and HO-1 are involved in the anti-inflammatory mechanism of Fx by western blot analysis. A typical result is shown in Fig. 5a, and 20 μM of Fx significantly increased the expression of HO-1 and Nrf-2 by 1.4- and 2.2-fold, respectively. In addition, the translocation of Nrf-2 was promoted in the nuclei as shown in Fig. 5b, and this finding was supported by the immunofluorescence assay, which detected the Nrf-2 staining (Fig. 5c). Fx has been known to activate the Nrf-2-mediated pathway by increasing phosphorylation of Akt in human keratinocyte cells [27]. But phosphorylation of Akt was inhibited by treatment with Fx in LPS-induced BV-2 microglia. This difference indicates that the underlying mechanism by which Fx induce changes in Nrf-2 signaling may vary depending on the cell type.
Effects of Fx on Nrf-2/HO-1 signaling pathway activation is independent Akt in LPS-activated BV-2 microglial cells. a Levels of Nrf-2 in cytoplasmic fraction and HO-1 in total lysates were measured using western blot analysis with specific antibodies. GAPDH protein was loading control. b Levels of Nrf-2 in nuclear fraction were measured using western blot analysis and LimB1 was loading control. c Translocation of Nrf-2 (green) was visualized using confocal microscopy, and DAPI staining (blue) indicated the nuclei (bar 40 μm). Values are mean ± SEM of three independent experiments; *p < 0.05, **p < 0.01 significantly different. (Color figure online)
Effects of Fx on Activation of the PKA/CREB Pathway in LPS-Activated BV-2 Microglial Cells
Several studies reported that CREB plays a role as a key upstream regulator of neuroprotective signaling against ROS-mediated cell death in vivo by activating anti-oxidant gene expression/ROS detoxifying enzyme expression [7, 14, 19, 30]. Thus, we examined whether the Fx-induced ROS reduction was mediated via the activation of PKA/CREB pathway. As the shown in Fig. 6a, treatment with Fx significantly increased the p-PKA, p-CREB and BDNF expression in LPS-activated BV-2 cells. To evaluate the involvement of the PKA/CREB pathway in the Fx-mediated ROS induction, a specific PKA inhibitor (H89, 10 μM) was used to abolish the effects of CREB. The results showed that H89 significantly inhibited the expression of p-CREB, which was dose-dependently reversed by pretreatment with Fx (Fig. 6c). Moreover, the immunofluorescence data indicated that pretreatment of Fx increased phosphorylation and translocation of CREB (Fig. 6b). While co-treatment with H89 and the LPS-stimulation significantly increased the production of ROS by 53.0% compared to stimulation with LPS alone (Fig. 6d). However, the ROS production was concentration-dependently reduced by pre-treatment with Fx. These results suggest that Fx partially suppressed LPS-induced ROS, and recovered the expression of BDNF through the PKA/CREB pathway.
Effects of Fx on PKA/CREB signaling pathway activation in LPS-activated BV-2 microglial cells. a Expression levels of p-PKA, p-CREB, and BDNF were measured using western blot. b p-CREB (green) was enhanced by treatment with Fx, and visualized using confocal microscopy, DAPI staining (blue) indicated the nuclei (bar 40 μm). c BV-2 cells were pretreated with H89 (PKA inhibitor, 10 μM) for 30 min, incubated with Fx for 1 h, and then co-treated with or without LPS (100 ng/mL) for 12 h. Expression of p-CREB was normalized by total CREB. d Levels of intracellular ROS from three independent experiments were quantified. e Intracellular ROS levels were measured using FACS. Values are mean ± SEM of three independent experiments; *p < 0.05, **p < 0.01, ***p < 0.001 significantly different. (Color figure online)
Discussion
In this study, we sought to demonstrate the pharmacological activity of Fx against LPS-activated neuroinflammatory responses and explain the underlying molecular signaling mechanisms of these effects. Previous studies showed that Fx suppresses NO, ROS, and pro-inflammatory cytokines production in LPS-induced RAW 264.7 cells and Aβ-induced BV-2 microglia [22–26,], which is similar to our findings. The results of our present study also proved that Fx dose-dependently attenuates the protein and mRNA expression of pro-inflammatory mediators in LPS-activated BV-2 microglial cells. The anti-neuroinflammatory mechanism of Fx involved classical NF-κB and MAPKs pathways including JNK, ERK, and p38 in LPS-activated microglia as previous studies reported [22, 23, 25, 26]. Moreover, we first found that Fx inhibits phosphorylation of Akt (Thr308) and AP-1 in LPS-activated BV-2 microglial cells. To prove the involvement of these molecules in the anti-inflammatory activity of Fx in LPS-activated microglial cells, specific inhibitors were applied. The data confirmed that the anti-inflammatory activity of Fx partly depended on these key molecules. These results support the notion that Fx is a promising agent for preventing neuro-inflammatory diseases by inhibiting the Akt/NF-κB and MAPKs/AP-1 pathways. Furthermore, the mechanism by which Fx regulates the protective factors, and the associated underlying molecular signaling pathways remain to be elucidated. Here, Fx promoted the expression of the Nrf-2 and HO-1, which are critical factors that exert neuroprotective effects by their anti-neuroinflammatory activities [31]. These data were consistent with those of a previous study showing that Fx increased the expression of Nrf-2 and HO-1 in human skin cells [27]. Interestingly, we found that Akt, one of the regulatory molecules in the Nrf-2/HO-1 pathway, was not activated by treatment with Fx in LPS-activated BV-2 microglia. Compared with Fx-activated Akt in human skin cells, Fx-inhibited Akt in LPS-induced microglia, which may depend on the cell type, and Akt in microglia was mainly involved in the process of NF-κB de-activation, which induced the expression of pro-inflammatory genes by binding to promoters of various inflammatory genes [32]. Thus, further studies would be needed to clarify the mechanisms of the Fx-activated Nrf-2/HO-1 pathway in microglia.
In addition, transcription factor CREB is known to be involved in modulating the relative activities of NF-κB and Nrf-2 [33]. In this study, we first addressed the important roles of PKA and CREB signaling molecules in the Fx-mediated anti-neuroinflammatory activities. Our findings showed that Fx induces the phosphorylation of CREB by increasing the p-PKA level. These data were also confirmed by using PKA inhibitor (H89) to abrogate effects of PKA, ROS production significantly increased, and this inhibition was dose-dependently reversed following treatment with Fx. These data indicate that Fx exerts anti-inflammatory activity through activating PKA/CREB signaling. Thus, the PKA/CREB signaling pathway was also involved in the Fx-mediated anti-inflammatory activities. Moreover, it has been reported that the expression of HO-1 is mediated via activation of PKA/CREB pathway [33]. In this study, the increase of HO-1 level may be also regulated by the activation of PKA/CREB. Further studies would be required to confirm the production of HO-1 via PKA/CREB signaling pathway in the actions of Fx.
Taken together, these results suggest that Fx not only inhibits classical pathways such as the Akt/NF-κB and MAPKs/AP-1 pathways, but it also activates beneficial molecules such as those involved in Nrf-2/HO-1 and PKA/CREB signaling pathways in LPS-activated BV-2 microglial cells. These results prove that Fx may be useful in protecting against cell-death in neurodegenerative diseases by down-regulating pro-inflammatory factors and up-regulating neurotrophin.
References
Teismann P, Tieu K, Cohen O, Choi DK, Wu DC, Marks D, Vila M, Jackson-Lewis V, Przedborski S (2003) Pathogenic role of glial cells in Parkinson’s disease. Mov Disord 18(2):121–129. doi:10.1002/mds.10332
Heneka MT, O’Banion MK, Terwel D, Kummer MP (2010) Neuroinflammatory processes in Alzheimer’s disease. J Neural Transm 117(8):919–947. doi:10.1007/s00702-010-0438-z
Kaur G, Han SJ, Yang I, Crane C (2010) Microglia and central nervous system immunity. Neurosurg Clin N Am 21(1):43–51. doi:10.1016/j.nec.2009.08.009
Graeber MB, Streit WJ (2010) Microglia: biology and pathology. Acta Neuropathol 119(1):89–105. doi:10.1007/s00401-009-0622-0
Dendorfer U, Oettgen P, Libermann TA (1994) Multiple regulatory elements in the interleukin-6 gene mediate induction by prostaglandin, cyclic AMP, and lipopolysaccharide. Mol Cell Biol 14(7):4443–4454
Lee TS, Chau LY (2002) Heme oxygenase-1 mediates the anti-inflammatory effect of interleukin-10 in mice. Nat Med 8(3):240–246. doi:10.1038/nm0302-240
Lee B, Cao R, Choi YS, Cho HY, Rhee AD, Hah CK, Hoyt KR, Obrietan K (2009) The CREB/CRE transcriptional pathway: protection against oxidative stress-mediated neuronal cell death. J Neurochem 108(5):1251–1265. doi:10.1111/j.1471-4159.2008.05864.x
Akaike A, Katsuki H, Kume T, Maeda T (1999) Reactive oxygen species in NMDA receptor-mediated glutamate neurotoxicity. Parkinsonism Related Disord 5(4):203–207
Vareille M, Rannou F, Thelier N, Glasser AL, de Sablet T, Martin C, Gobert AP (2008) Heme oxygenase-1 Is a Critical regulator of nitric oxide production in enterohemorrhagic Escherichia coli-infected human enterocytes. J Immunol 180(8):5720–5726. doi:10.4049/jimmunol.180.8.5720
Pae HO, Ae Ha Y, Chai KY, Chung HT (2008) Heme oxygenase-1 attenuates contact hypersensitivity induced by 2,4-dinitrofluorobenzene in mice. Immunopharmacol Immunotoxicol 30(2):207–216. doi:10.1080/08923970801946824
Syapin PJ (2008) Regulation of haeme oxygenase-1 for treatment of neuroinflammation and brain disorders. Br J Pharmacol 155(5):623–640. doi:10.1038/bjp.2008.342
Lee JW, Choi YJ, Park JH, Sim JY, Kwon YS, Lee HJ, Kim SS, Chun W (2013) 3,4,5-Trihydroxycinnamic acid inhibits lipopolysaccharide-induced inflammatory response through the activation of Nrf2 pathway in BV2 microglial cells. Biomol Ther 21(1):60–65. doi:10.4062/biomolther.2012.091
Kensler TW, Wakabayashi N, Biswal S (2007) Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annu Rev Pharmacol Toxicol 47:89–116. doi:10.1146/annurev.pharmtox.46.120604.141046
Bedogni B, Pani G, Colavitti R, Riccio A, Borrello S, Murphy M, Smith R, Eboli ML, Galeotti T (2003) Redox regulation of cAMP-responsive element-binding protein and induction of manganous superoxide dismutase in nerve growth factor-dependent cell survival. J Biol Chem 278(19):16510–16519. doi:10.1074/jbc.M301089200
Sandberg M, Patil J, D’Angelo B, Weber SG, Mallard C (2014) NRF2-regulation in brain health and disease: implication of cerebral inflammation. Neuropharmacology 79:298–306. doi:10.1016/j.neuropharm.2013.11.004
Jung JS, Shin JA, Park EM, Lee JE, Kang YS, Min SW, Kim DH, Hyun JW, Shin CY, Kim HS (2010) Anti-inflammatory mechanism of ginsenoside Rh1 in lipopolysaccharide-stimulated microglia: critical role of the protein kinase A pathway and hemeoxygenase-1 expression. J Neurochem 115(6):1668–1680. doi:10.1111/j.1471-4159.2010.07075.x
Shaywitz AJ, Greenberg ME (1999) CREB: a stimulus-induced transcription factor activated by a diverse array of extracellular signals. Annu Rev Biochem 68:821–861. doi:10.1146/annurev.biochem.68.1.821
Lonze BE, Ginty DD (2002) Function and regulation of CREB family transcription factors in the nervous system. Neuron 35(4):605–623. doi:10.1016/S0896-6273(02)00828-0
Kronke G, Bochkov VN, Huber J, Gruber F, Bluml S, Furnkranz A, Kadl A, Binder BR, Leitinger N (2003) Oxidized phospholipids induce expression of human heme oxygenase-1 involving activation of cAMP-responsive element-binding protein. J Biol Chem 278(51):51006–51014. doi:10.1074/jbc.M304103200
Wen AY, Sakamoto KM, Miller LS (2010) The role of the transcription factor CREB in immune function. J Immunol 185(11):6413–6419. doi:10.4049/jimmunol.1001829
Miyashita K (2009) Function of marine carotenoids. Forum Nutr 61:136–146. doi:10.1159/000212746
Kim KN, Heo SJ, Yoon WJ, Kang SM, Ahn G, Yi TH, Jeon YJ (2010) Fucoxanthin inhibits the inflammatory response by suppressing the activation of NF-kappaB and MAPKs in lipopolysaccharide-induced RAW 264.7 macrophages. Eur J Pharmacol 649(1–3):369–375. doi:10.1016/j.ejphar.2010.09.032
Pangestuti R, Vo TS, Ngo DH, Kim SK (2013) Fucoxanthin ameliorates inflammation and oxidative reponses in microglia. J Agric Food Chem 61(16):3876–3883. doi:10.1021/jf400015k
Heo SJ, Yoon WJ, Kim KN, Oh CH, Choi YU, Yoon KT, Kang DH, Qian ZJ, Choi IW, Jung WK (2012) Anti-inflammatory effect of fucoxanthin derivatives isolated from Sargassum siliquastrum in lipopolysaccharide-stimulated RAW 264.7 macrophage. Food Chem Toxicol 50(9):3336–3342. doi:10.1016/j.fct.2012.06.025
Shiratori K, Ohgami K, Ilieva I, Jin XH, Koyama Y, Miyashita K, Yoshida K, Kase S, Ohno S (2005) Effects of fucoxanthin on lipopolysaccharide-induced inflammation in vitro and in vivo. Exp Eye Res 81(4):422–428. doi:10.1016/j.exer.2005.03.002
Choi JH, Kim NH, Kim SJ, Lee HJ, Kim S (2016) Fucoxanthin inhibits the inflammation response in paw edema model through suppressing MAPKs, Akt, and NFkappaB. J Biochem Mol Toxicol 30(3):111–119. doi:10.1002/jbt.21769
Karin M, Delhase M (2000) The IκB kinase (IKK) and NF-κB: key elements of proinflammatory signalling. Semin Immunol 12(1):85–98. doi:10.1006/smim.2000.0210
Lee S, Suk K (2007) Heme oxygenase-1 mediates cytoprotective effects of immunostimulation in microglia. Biochem Pharmacol 74(5):723–729. doi:10.1016/j.bcp.2007.06.016
Pawate S, Shen Q, Fan F, Bhat NR (2004) Redox regulation of glial inflammatory response to lipopolysaccharide and interferongamma. J Neurosci Res 77:540–551
Zheng J, Piao MJ, Kim KC, Yao CW, Cha JW, Hyun JW (2014) Fucoxanthin enhances the level of reduced glutathione via the Nrf2-mediated pathway in human keratinocytes. Mar Drugs 12(7):4214–4230. doi:10.3390/md12074214
Innamorato NG, Rojo AI, Garcia-Yague AJ, Yamamoto M, de Ceballos ML, Cuadrado A (2008) The transcription factor Nrf2 is a therapeutic target against brain inflammation. J Immunol 181(1):680–689. doi:10.4049/jimmunol.181.1.680
Liu SY, Xu P, Luo XL, Hu JF, Liu XH (2016) (7R,8S)-Dehydrodiconiferyl alcohol suppresses lipopolysaccharide-induced inflammatory responses in BV2 microglia by inhibiting MAPK signaling. Neurochem Res 41 (7):1570–1577. doi:10.1007/s11064-016-1870-8
Ziady AG, Sokolow A, Shank S, Corey D, Myers R, Plafker S, Kelley TJ (2012) Interaction with CREB binding protein modulates the activities of Nrf2 and NF-kappaB in cystic fibrosis airway epithelial cells. Am J Physiol Lung Cell Mol Physiol 302(11):L1221–L1231. doi:10.1152/ajplung.00156.2011
Acknowledgements
This research study was supported by the Institutional Program of the Korea Institute of Science and Technology (2Z04690), the Bio-Synergy Research Project (NRF-2012M3A9C4048793) and the Bio & Medical Technology Development Program (NRF-2015M3A9A5030735) of the Ministry of Science, ICT, and Future Planning through the National Research Foundation, Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhao, D., Kwon, SH., Chun, Y.S. et al. Anti-Neuroinflammatory Effects of Fucoxanthin via Inhibition of Akt/NF-κB and MAPKs/AP-1 Pathways and Activation of PKA/CREB Pathway in Lipopolysaccharide-Activated BV-2 Microglial Cells. Neurochem Res 42, 667–677 (2017). https://doi.org/10.1007/s11064-016-2123-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-016-2123-6