Abstract
In the present study, we investigated the protective mechanism of paeoniflorin (PF), a monoterpene glycoside extracted from Radix Paeoniae alba roots, on MPP+-induced neurotoxicity in cultured rat pheochromocytoma cells (PC12). Our work included examination of cell viability assessment, amounts of released lactic dehydrogenase (LDH), intracellular Ca2+ concentration, cell apoptosis, mitochondrial membrane potential, caspase-3 activity, and expression profiling of two apoptosis-related genes (Bcl-2 and Bax). It was shown that, PF functioned as an MPP+ antagonist, being able to suppress apoptosis, decrease LDH release and Ca2+ concentration, attenuate membrane potential collapse and, inhibit caspase-3 activation, decrease in Bax/Bcl-2 ratio. These observations suggest that PF could protect PC12 cells against MPP+-induced injury and the mechanism PF’s neuroprotective effect was closely associated with Bcl-2 up-regulation and Bax down-regulation. PF has neuroprotective effects on MPP+-induced apoptosis in PC12 cells via regulating mitochondrial membrane potential and Bcl-2/Bax/caspase-3 signaling pathways, and this new insight will help develop a PF-based therapeutic strategy for treatmenting neurodegenerative diseases and injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuronal death is the core component of neurodegenerative conditions, such as Parkinson’s disease (PD). PD is the second most common age-related neurodegenerative disease affecting millions of people worldwide. It is characterized by the selective and progressive degeneration of dopaminergic neurons in the substantia nigra pars compacta (SNpc) and subsequent decrease of the dopamine level in the striatum [1–6]. Although its molecular mechanism is not clear, oxidative stress, mitochondria dysfunction, apoptosis and caspase-mediated cell death are thought to be important mediators of neuronal death in acute and chronic neurodegenerative diseases [7–10]. Therefore, the suppression of dopaminergic neuronal cell death by regulation of the apoptotic cascade may control apoptotic events and provide new strategies in the prevention and treatment of PD. The traditional herbal medicine has been used for centuries in China for treating PD, and is still in current use, suggesting that medicinal herb may be a good source of drug candidates for the treatment of PD.
Peoniflorin (PF), a monoterpene glycoside isolated from the aqueous extract of the Chinese herb Radix Paeoniae alba, possesses wide pharmacological effects in the nervous system. It has been used in the treatment of cerebral ischemia [11], epilepsy [12], and neurodegenerative disorders such as Alzheimer’s disease [13] and Parkinson’s disease [14].Of importance, PF and its beneficial effects can be found in improvement of learning and memory, analgesia, conscious-sedation and antioxidation [15–17]. Previous studies have demonstrated that PF likely exerts a neuroprotective effect by activating adenosine A1 receptor, ameliorating the function of the cholinergic nerve, regulating ion channel homeostasis, retarding oxidative stress and apoptosis of neurons and promoting nerve growth [18–21]. However, the molecular mechanisms that underlie the protection effect of paeoniflorin on the neurotoxin have not been fully understood.
1-Methyl-4-phenylpyridinium (MPP+), the active metabolite of 1-metryl-4-phenyl-1, 2, 3, 6-tetrahydropyridine (MPTP), has been used extensively in various mammalian species to produce an experimental model of PD. MPP+ produces mitochondria-targeted injury [22], resulting in oxidative stress [23] and culminating in the loss of dopaminergic neurons [24]. MPP+ is a commonly used neurotoxin to produce neuronal cell apoptosis and neurodegenerative models [25].
PC-12 cell, a cell line derived from a pheochromo-cytoma of rat adrenal medulla which known to secrete dopamine neurotransmitters and contain high amounts of dopamine transporters is commonly used in the investigation of neurotherapeutics study for Parkinson’s disease (PD) [26].
Madopar (levodopa plus the peripherally acting decarboxylase inhibitor, benserazide) which was used in the clinical treatment of Parkinson’s disease and dopamine-responsive dystonia served as a positive control in the present study.
In the present study, we utilize PC12 cell and the neurotoxin, MPP+ to elucidate the molecular basis of PF as a potential PD prescription. The present study may also be useful for the establishment of a quantitative cell system for screening promising PD drugs.
Reagents and Chemicals
PF isolation alba, identification and purification were done earlier by Yuchi Zhang from Changchun Normal University [27]. 1-Methyl-4-phenylpyridinium ion (MPP+) was purchased from Sigma-Aldrich (St Louis, MO, USA). Madopar (Shanghai Roche Led., Shanghai, China) was obtained at the institutional pharmacy. DMEM culture medium, Trizol reagent, fetal bovine serum, heat-inactivated horse serum, penicillin and streptomycin were purchased from Gibco BRL (Grand Island, NY, USA). Cell counting kit-8 (CCK-8), caspase-3 activity assay kit, lactate dehydrogenase (LDH) assay kit, mitochondrial membrane potential detection fluorescent dye JC-1 were purchased from Beyotime Biotechnology (Haimen, China), Ca2+-sensitive fluorescent probe Fluo-3AM was purchased from Sigma-Aldrich. Monoclonal antibodies to Bax, Bcl-2 and GAPDH were obtained from Santa Cruz (Santa Cruz, CA, USA). All other chemicals and reagents used in this study were analytical grade.
Cell Culture and Treatments
PC12 cells were purchased from Shanghai Institute of Cell Biology, Chinese Academy of Sciences (Shanghai) and were maintained in DMEM medium supplemented with penicillin (100 U/mL), streptomycin (100 μg/mL), 5 % fetal bovine serum and 5 % horse serum, at 37 °C in a humidified atmosphere with 5 % CO2. PC12 cells (1 × 104 per well) were seeded in 96-well plates. After overnight incubation PC12 cells were divided into six equal groups for the following treatments: non-treated control, MPP+ 500 μM, MPP+ 500 μM + Madopar 50 μg/mL, 500 μM MPP+ + PF-25 (PF 25 μM), 500 μM MPP+ + PF-50, and 500 μM MPP+ + PF-100. For both CCK-8 and LDH activity assays, n = 6 per group. At 48 h after the cells were seeded, cultures were refreshed with serum-free medium with respective drug regimes. After a further 48-h incubation, tests were performed.
Cell Viability Assay
Cell viability was assessed using CCK-8 kit (Beyotime Biotechno1ogy, Haimen, Jiangsu, China). After the 48 h cultivation, 10 µL CCK-8 solution was added to each sample. After 2 h of incubation at 37 °C, the absorbance was determined at A450 on a microplate reader (SpectraMax M5, Molecular Devices, Sunnyvale, CA).
Microscopy Observation
The morphological changes in neurons were monitored under an inverted phase-contrast microscope (Leica, Germany) before and after PF treatment.
LDH Release Assay
Aliquots of 1.5 × 105 cells/well were transferred to a 24-well cell culture plate for an overnight incubation. Supernatants were collected and 200 μL/well was added to a black 96-well culture plate. LDH release was measured using LDH cytotoxicity assay kit (Beyotime, Haimen, Jiangsu, China) as per the manufacturer’s instructions. A450 in each well was determined using an enzyme linked. Data were normalized to the LDH activity released from control cells.
Measurement of Intracellular Ca2+ Concentration
Ca2+ concentration was determined as described in the literature [20–22]. Briefly, at the end of each of the six treatments, cells were collected and then incubated with the complete medium containing 5 μM Fura-3/AM at 37 °C for 45 min. Subsequently, the cells were washed and re-suspended with cold balanced (PBS) containing 0.2 % bovine serum albumin. The cells were incubated at 37 °C for another 5 min, and Ca2+ concentration was determined using a fluorescence spectrophotometer by according to emission changes at 510 nm with an excitation switch from 340 to 380 nm (Spectra Max M5, Molecular Devices, Sunnyvale, CA). The concentration of intracellular Ca2+ was expressed as a percentage of non-treated control.
Detection of Apoptosis
At the end of the treatments, cells were collected by centrifuging at 1000 rpm for 5 min, followed by washing with PBS for three times. The cells were re-suspended with pre-cooled 70 % ethanol, and the preparation was stored at 4 °C between 18 h and 1 week before being used. Before the test, cells were washed with PBS, and re-suspend with 200 μL of propidium iodide (PI) and RNase mixture (final concentrations being 50 and 100 μg/mL, respectively). The stained cells were filtered and incubated in the dark at 4 °C for 30 min before the flow cytometric analysis. The PI fluorescence of individual nuclei was measured using a flow cytometer (Beckman-Coulter Co., Epics XL, USA). Ten thousand cells in each sample were analyzed and the percentage of apoptotic cells accumulated in the sub-G1 peak was calculated by the research software of the flow cytometer (Wincycle 3.2, Beckman Coulter, CA, USA).
Assessment of Mitochondrial Membrane Potential
Mitochondrial membrane potential was assessed by fluorescent dye JC-1 (Beyotime Biotechno1ogy, Haimen, China) [16]. Briefly, after 48 h of cultivation, cells were incubated with 5 µg/mL JC-1 at 37 °C for 20 min.Then cells were rinsed twice with buffer. The fluorescence intensity of JC-1 aggregates was detected using a micro-plate reader at excitation of 525 nm and emission of 590 nm, whereas the JC-1 monomer was measured at an excitation of 490 nm and emission of 530 nm emission using a Softmax Pro 5 fluorescence plate reader (Molecular Devices, Sunnyvale, CA.USA). The fluorescence intensity ratio of aggregates to monomers was calculated as an indicator of mitochondrial membrane potential.
Determination of Caspase-3 Activity
Cellular caspase-3 activity was measured with commercially available colorimetric assay kit (Beyotime Biotechnology, Haimen, China) [23]. PC12 cells were lysed with lysis buffer supplied with the kit. The soluble fraction of the cell lysate was then assayed for caspase-3 activity using Ac-DEVD-pNA, a colorimetric substrate for caspase-3 as described in the manufacturer’s protocol.
Expression of Bcl-2 and Bax mRNAs
Total RNA was extracted using the Trizol® reagent according to the manufacturer’s instructions. RNA concentration was estimated at 260 nm using a UV spectrophotometer (Shimadzu, Japan). RNA purity was indicated by the ratio of A260 and A280 (between 1.7 and 2.0).
Transcript abundances of the B cell lymphoma 2 (Bcl-2) and Bcl-2 associated X protein (Bax) genes were examined by real-time RT-PCR. Primers and probes (Table 1) were designed on Primer Express 2.0 (Dalian Bio-engineering, Dalian, China). The glyceraldehyde-3-phosphate dehydrogenase (GAPDH) gene was used as an internal reference. For each RT reaction, RNA (1 μg) was added into a 10-μL reaction system containing dNTP (10 mM), random hexamer primer, Oligo-dT, RNase inhibitor (40 U/μL) and RT-PCR buffer, and the reaction was run at 42 °C for 40 min and 99 °C for 5 min. For PCR, the RT product, the forward and reverse primers, and the probes, along with the internal reference were included. The reaction was run on ABI PRISM 7000 Real Time PCR with 40 cycles of 94 °C for 15 s,57 °C for 15 s, 72 °C for 30 s.
Western Blot Analysis
Cytosolic protein extracts were prepared as described by Sugawara et al. [25]. Briefly, treated and untreated cells were lysed and denatured in a sample buffer (Complete Lysis-M, Roche). Equal amounts of proteins were seperated by 10 % SDS–polyacrylamide gels, transferred onto nitrocellulose membranes. The nitrocellulose membranes were blocked with 5 % nonfat milk in Tris-buffered saline (TBS, 150 mM NaCl, 20 mM Tris–HCl, pH 7.4), immunebloted with primary antibodies in TBS (All the antibodies purchase from Abcam,B-cell lymphoma 2(Bcl-2) (1:500), Bcl-2 associated X protein (Bax) (1:1000) and β-actin (1:1000)), 0.1 % Tween 20 for 2 h at room temperature or overnight at 4 °C. After washing, the blots were reacted with peroxidase-conjugated secondary antibodies for 45 min and the protein concentrations were determined by the ECL detection system. Optical density of each band was analyzed using Gel-Pro analyzer 4.0 software (Gel Media System, China).
Statistical Analysis
All data were expressed as mean ± SEM. To compare experimental and control groups, we used one- or two-way ANOVA, followed by post hoc Dunnett’s test using the SPSS software (SPSS Inc., Chicago, USA). A value of P < 0.05 was considered statistically significant for analysis. The figures were obtained by the Statistical Analysis System (GraphPad Prism 4, GraphPad Software, Inc.,San Diego, CA).
Results
PF Prevents MPP+-Induced Cell Death
To exclude the possibility that PF itself affected the survival of PC12 cells, different concentrations of PF (25, 50, 100 μM) were added to the cells for 48 h. PF-induced loss of cell viability in PC12 cells was negligible below the concentration of 100 μM (Fig. 1a).
Cytotoxic effect and protective effect of PF in cultured PC12 cells. a Effects of PF on cell survival in cultured PC12 cells. Cells were treated with different concentrations of PF for 48 h, after which the cell viability was measured by MTT assay. b Neuroprotective effects of PF on MPP+-induced cytotoxicity in cultured PC12 cells. Cells were treated With 500 μM MPP+ plus either Madopar (50 μg/mL) or PF (25, 50 and 100 μM) for 48 h, after which the cell viability was measured by MTT assay. Values mean ± SEM (n = 6). ## P < 0.01 as compared with control group; *P < 0.05; **P < 0.01 as compared with MPP+ treated group
To further determine the neuroprotective effects of PF on MPP+-induced cell deaths, PC12 cells were treated for 48 h with 25, 50 or 100 μM of PF exposure to 500 μM MPP+. Figure 1b shows a significant decrease of the cell viability in MPP+-induced group compared to control group (P < 0.001) and significant increase of the cell viability [F (4, 25) = 83.97, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01).
Effect of PF on MPP+-Induced Changes in Cellular Morphology
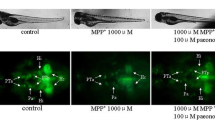
Visual inspection by phase-contrast microscopy showed that those normal PC12 cells showed round cell bodies and the cell edges were intact and clear (Fig. 2). After treatment with 500 μM MPP+ for 48 h, PC12 cells displayed obvious cell body shrinkage and nuclear condensation. Co-treatment with PF (25, 50 or 100 μM) or Madopar drastically prevented morphological deterioration of cells, most of which showed normal cell morphology with normal nuclear size and integrity.
Effect of PF on MPP+-induced changes in cellular morphology Normal PC12 cells showed round cell bodies and the cell edges were intact and clear. Photographs were taken with an inverted microscope at ×400 magnification. a Control; b 500 μM MPP+ treated alone; c 500 μM MPP+ with Madopar (50 μg/mL); d–f 500 μM MPP+ with PF (25, 50 and 100 μM)
PF Inhibits LDH Release from Cells Treated with MPP+
We also observed a significant increase of LDH leakage in MPP+-induced group compared to control group (P < 0.001) and a significant decrease of LDH leakage [F (4, 25) = 53.8, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01) (Fig. 3).
PF Reduces MPP+-Induced Increase of Ca2+ Load
In addition, a significant increase of intracellular Ca2+ concentration in MPP+-induced group compared to control group (P < 0.001), and a significant decrease of Ca2+ concentration [F (4, 25) = 62, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01) (Fig. 4).
PF Reduces Apoptotic Rate in Cells Treated with MPP+
After treatment with 500 μM MPP+, the S period of the cells reduced significantly (Table 1). With 500 μM MPP+ plus either Madopar (50 μg/mL) or PF (12.5, 25 and 50 μM) the S period upgrade and G0/G1 period lengthened [F (4, 25) = 52.9, P < 0.01]. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01).
PF Inhibits Caspase-3 Activity in Cells Treated with MPP+
Figure 5 showed that a significant increase of caspase-3-like activity in MPP+-induced group compared to control group (P < 0.001) and a significant decrease of caspase-3-like activity [F (4, 25) = 66.56, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01) (Fig. 5). These results indicate that PF was able to inhibit MPP+-induced caspase-3 activation.
Effect of PF on MPP+- treated mitochondrial membrane potential loss in PC12 cells. The fluorescence intensity ratio of JC-1 aggregates to monomers was used as an indicator of mitochondrial membrane potential. Data are expressed as mean ± SEM (n = 6). ## P < 0.01 compared to the control group; *P < 0.05, **P < 0.01 compared to the MPP+ treated group
PF Prevented MPP+-induced Membrane Potential Loss
Figure 6 showed that a significant loss of mitochondrial membrane potential (MMP) in MPP+-induced group compared to control group (P < 0.001) and a significant increase of MMP [F (4, 25) = 66.56, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01).
Effect of PF on mRNA Levels of Bcl-2/Bax Genes in MPP+-Induced PC12 Cells
MPP+ treatment led to an increase in Bax mRNA level and a decrease in Bcl-2 mRNA level (Fig. 7a, b), reducing a ratio of Bcl-2/Bax significantly being 0.2 compared to that of unexposed control (P < 0.05). But the ratios for cells pretreated with PF and Madopar were 0.39, 0.68, 1.29 and 1.108, significantly higher than that of the MPP+ treatment (P < 0.05, 0.01, 0.0001, and <0.05) (Fig. 7c; Table 2).
PF Down Regulates the Bcl-2/Bax Ratio in MPP+-Induced PC12 Cells
Figure 7 showed that MPP+ exposure reduced a ratio of Bcl-2/Bax compared to control group (P < 0.001) and a significant high ratio of Bcl-2 to Bax [F (4, 25) = 61.2, P < 0.01] in MPP+-induced groups treated with Madopar, PF (25, 50 or 100 μM) compared to MPP+ group. Also, post hoc analyses revealed significant differences among PF-treated groups (25, 50 or 100 μM) (P < 0.01). The results suggested that PF treatment shifted the balance between pro- and anti-apoptotic members toward cell survival (Fig. 8).
Effect of PF on the expression of Bcl-2 and Bax in PC12 cells. Cells were treated with MPP+ (500 μM) and Madopar (50 μg/mL)/PF (25, 50 or 100 μM) for 48 h, and then cell lysate were subject to Western blot analysis. The levels of Bax and Bcl-2 were quantified by densitometric analysis (a) and the Bax/Bcl-2 ratio was determined (b). Data are mean ± SEM (n = 6). ## P < 0.01 compared to the control group; *P < 0.05, **P < 0.01 compared to the MPP+ treated group
Discussion
Parkinson’s disease is a chronic, neurodegenerative disorder that results from the gradual and progressive loss of dopaminergic neurons in the substantia nigra. There is abundant evidence suggesting that MPP+-induced cell death is a useful representation for studying dopaminergic degeneration modeling Parkinson’s disease both in vitro and in vivo [28–31]. PC12 cells possess many of the characteristics of human neurons and therefore have served as a well-established PD model. In the present study, we provide direct evidence that PF protects PC12 cells against MPP+-induced cytotoxicity in several aspects.
Consistent with previous studies [32–34], the present study clearly demonstrated that PF possesses robust neuroprotective effects, as evidenced by the fact that PF significantly ameliorated the MPP+ induced decrease of cell viability, cellular apoptotic alternations and prevented morphological changes of neurons. The robust protective effect of PF is also reflected in its suppression of the neurotoxin-induced over release of LDH. Increased release of LDH has been observed in cultured neuronal cells exposed to neurotoxins [32] and brain injury [35].Therefore, the suppression of LDH release seems to be a consequence of the protective effects of PF against neurotoxicity and neural injury.
The intracellular Ca2+ concentration plays a fundamental role in the development of neurons. However, in a variety of pathologic conditions, intracellular Ca2+ overoad may excessively activate Ca2+/calmodulin-dependent pathways and lead to neuronal cell damage [36]. Previous studies have reported that MPP+-induced apoptotic cell death in PC12 cells was related to intracellular Ca2+ overload [37]. Our study further revealed that exposure of cells to the neurotoxin resulted in intracellular calcium overflow; treatment with PF remarkably blocked the calcium influx. Similar results also have been extensively observed in other in vitro and animal experiments [32, 38]. It is well known that excessive cytosolic calcium causes a wide range of subcellular pathological responses, in particular dysfunction of mitochondrial membrane permeability [39]. It appears that the effect of PF in maintaining mitochondrial membrane integrity is related to its capacity of regulating cytosolic calcium homeostasis.
Mitochondria play a central part in neurodegeneration and neuronal death [40]. A key feature of mitochondrial apoptosis is disruption of the membrane potential mainly caused by increased membrane permeability [41]. It is known that that MPP+ treatment caused a significant decrease in MMP levels [42, 43], and our study revealed that co-treatment with PF could inhibit MMP declining, suggesting that PF could maintain mitochondrial membrane integrity by preventing the membrane permeability from neurotoxicity.
Disruption of the mitochondrial membrane potential is one of the earliest intracellular events that occur following induction of apoptosis. During the process of caspase cascade activation, caspase-3 is the main executioner caspase. Caspase-3 has been demonstrated to participate in MPP+-induced apoptosis and is regulated by mitochondria dysfunction-mediated ROS overproduction [44]. The present results indicated that caspase-3 activities in PC12 cells increased dramatically following the 48-h treatment with 500 μM MPP+, but treatment with 100 μM PF effectively attenuated MPP+-induced caspase-3 activity by 43 %. PF may functions as an MPP+ antagonist.
The pattern of mitochondrial inheritance has a profound impact on development and reproductive performance [45]. Previous studies and our experiment showed that MPP+ treatment caused a significant decrease in the level of MMP. However, we found that co-treatment of PF could inhibit reduction of MMP on PC12 cells, suggesting that the neuroprotective effect of PF may be related to the mitochondrial death pathway. While there is more than one pathway to apoptosis, the Bcl-2 family members play an important role in MPP+-induced apoptotic cell death [43]. In addition, O’Malley et al. [43] reported that the overexpression of Bcl-2 attenuated MPP+-induced cell death. Moreover, we investigated the expression profiles of two apoptosis-related proteins including Bcl-2 and Bax [46]. Apoptosis is associated with the activation of a genetic program in which apoptosis effector genes promote cell death. It is regulated by the action of the Bcl-2 family of proteins, which includes anti- and pro-apoptotic members such as Bcl-2 and Bax [47–51]. It was reported that Bcl-2 binds to the mitochondrial membrane, competitive binding with Bax and forming Bcl-2/Bax heterodimer, which leads to closing mitochondrial permeability transition pore and preventing the release of cytochrome C, thereby inhibiting apoptosis. As a proapoptotic molecule, Bax can be combined into a Bax–Bax homodimer to form the composition of the mitochondrial membrane permeable channels, through which cytochrome C can transfer from mitochondrial into cytoplasm, which activate the caspase-related apoptosis cascade, resulting in mitochondrial-dependent apoptosis. In the present study, the expression level and mRNA level of Bcl-2 was significantly decreased when treated with MPP+ alone and significantly increased when treated with a combination of MPP+ at 500 μM plus PF at different concentration (10, 50, 100 μM) for 48 h as compared with the control group. However, the expression level and mRNA level of Bax was just the opposite. The current study revealed that PF significantly reversed a MPP+-induced decrease of Bcl-2/Bax ratio. In this regard, the Bcl-2/Bax ratio may be a better predictor of apoptotic fate than the absolute expression of either Bax or Bcl-2 alone [42]. Any changes in the balance between the pro- and anti-apoptotic proteins will affect cell death. The present results showed that MPP+ had a profound effect on the expression of Bcl-2 family members in PC12 cells. Treatment with Madopar and PF reduced the expression of pro-apoptotic Bax and increased the expression of anti-apoptotic Bcl-2, thereby increasing the MPP+-induced Bcl-2/Bax ration elevation in PC12 cells.
In conclusion, our results provided novel insights into the cellular mechanisms of PF’s biological functions. Neuroprotection of PF may be associated with alleviating LDH leakage, decreasing [Ca2+]i and regulating mitochondrial membrane potential and Bcl-2/Bax/caspase-3 signal pathway. These results suggest that PF might be a promising candidate for the prevention or treatment of neurodegenerative diseases such as Parkinson’s disease, but further studies to understand the basic mechanism are required.
References
Braak H, Del Tredici K, Rüb U et al (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24:197–211
Chaturvedi RK, Shukla S, Seth K et al (2006) Neuroprotective and neurorescue effect of black tea extract in 6-hydroxydopamine lesioned rat model of Parkinson’s disease. Neurobiol Dis 22(2):421–434
Ciobica A, Hritcu L, Artenie V et al (2009) Effects of 6-OHDA infusion into the hypothalamic paraventricular nucleus in mediating stress-induced behavioral responses and oxidative damage in rats. Acta Endocrinol (Bucharest) (4):425–436
Hritcu L, Foyet HS, Stefan M et al (2011) Neuroprotective effect of the methanolic extract of Hibiscus asper leaves in 6-hydroxydopamine-lesioned rat model of Parkinson’s disease. J Ethnopharmacol 137(1):585–591
Gerlach M, Double KL, Ben-Shachar D et al (2003) Neuromelanin and its interaction with iron as a potential risk factor for dopaminergic neurodegeneration underlying Parkinson’s disease. Neurotox Res 5(1–2):35–44
Lang AE, Lozano AM (1998) Parkinson’s disease. N Engl J Med 339:1044–1053
Li XL, Cheng WD, Li J et al (2008) Protective effect of estrogen on apoptosis in a cell culture model of Parkinson’s disease. Clin Invest Med 31(5):258–264
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443(7113):787–795
Levy OA, Malagelada C, Greene LA (2009) Cell death pathways in Parkinson’s disease: proximal triggers, distal effectors, and final steps. Apoptosis 14(4):478–500
Olanow CW, Tatton WG (1999) Etiology and pathogenesis of Parkinson’s disease. Ann Rev Neurosci 22:123–144
Liu J, Jin DZ, Xiao L (2006) Paeoniflorin attenuates chronic cerebral hypoperfusion-induced learning dysfunction and brain damage in rats. Brain Res 1089:162–170
TsudaT Sugaya A, Ohguchi H et al (1997) Protective effects of peony root extract and its components on neuron damage in the hippocampus induced by the cobalt focus epilepsy model. J Neuropathol Exp Neurol 146:518–525
Zhong SZ, Ge QH, Li Q et al (2009) Peoniflorin attenuates Abeta((1-42))mediated neurotoxicity by regulating calcium homeostasis and ameliorating oxidative stress in hippocampus of rats. J Neurol Sci 280:71–78
Liu DZ, Zhu J, Jin DZ et al (2007) Behavioral recovery following sub-chronic paeoniflorin administration in the striatal 6-OHDA lesion rodent model of Parkinson’s disease. J Ethnopharmacol 112:327–332
Liu J, Jin DZ, Xiao L et al (2006) Paeoniflorin attenuates chronic cerebral hypoperfusion-induced learning dysfunction and brain damage in rats. Brain Res 1089(1):162–170
Wang D, Wong HK, Feng YB et al (2013) Paeoniflorin, a natura neuoprotective agent, modulates multiple anti-apoptotic and pro-apoptotic patways in differentiated PC12 cells. Cell Mol Neurobiol 33(4):521–529
Yu HY, Liu MG, Liu DN et al (2007) Antinociceptive effects of systemic paeoniflorin on bee venom-induced various ‘phenotypes’ of nociception and hypersensitivity. Pharmacol Biochem Behav 88:131–140
Liu DZ, Xie KQ, Ji XQ et al (2005) Neuroprotective effect of paeoniflorin on cerebral ischemic rat by activating adenosine A1 receptor in a manner different from its classical agonists. Br J Pharmacol 146(4):604–611
Liu DZ, Zhao FL, Liu J et al (2006) Potentiation of adenosine A1 receptor agonist CPA-induced antinociception by paeoniflorin in mice. Biol Pharm Bull 29(8):1630–1633
Hu S, Dong H, Zhang H et al (2012) Noninvasive limb remote ischemic preconditioning contributes neuroprotective effects via activation of adenosine A1 receptor and redox status after transient focal cerebral ischemia in rats. Brain Res 1459:81–90
Héron A, Lekieffre D, Le Peillet E et al (2007) Effects of an A1 adenosine receptor agonist on the neurochemical, behavioral and histological consequences of ischemia. Brain Res 641(2):217–224
Esteves AR, Domingues AF, Ferreira IL et al (2008) Mitochondrial function in Parkinson’s disease cybrids containing an nt2 neuron-like nuclear background. Mitochondrion 8:219–228
Chen PC, Vargas MR, Pani AK et al (2009) Nrf2-mediated neuroprotection in the MPTP mousemodel of Parkinson’s disease: critical role for the astrocyte. Proc Natl Acad Sci USA 106(8):2933–2938
Ourednik V, Ourednik J, Xu Y et al (2009) Cross-talk between stem cells and the dysfunctional brain is facilitated by manipulating the niche: evidence from an adhesion molecule. Stem Cells 27:2846–2856
Segura Aguilar J, Kostrzewa RM (2004) Neurotoxins and neurotoxic species implicated in neurodegeneration. Neurotox Res 6(7–8):615–630
Li P, Li Z (2015) Neuroprotective effect of paeoniflorin on H2O2-induced apoptosis in PC12 cells by modulation of reactive oxygen species and the inflammatory response. Exp Ther Med 9(5):1768–1772
Zhang Y, Liu C, Qi Y et al (2015) Circulating ultrasound-assisted extraction, countercurrent chromatography, and liquid chromatography for the simultaneous extraction, isolation, and analysis of the constituents of Uncaria tomentosa. J Chromatogr A 1388:36–42
Gerlach M, Riederer P, Przuntek H et al (1991) MPTP mechanisms of neurotoxicity and their implications for Parkinson’s disease. Eur J Pharmacol 208:273–286
Swerdlow RH, Parks JK, Miller SW et al (1996) Origin and functional consequences of the complex I defect in Parkinson’s disease. Ann Neurol 40:663–671
NicotraA Parvez S (2002) Apoptotic molecules and MPTP-induced cell death. Neurotoxicol Teratol 24:599–605
Dipasquale B, Marini AM, Youle RJ (1991) Apoptosis and DNA degradation induced by 1-methyl-4-phenylpyridinium in neurons. Biochem Bio-phys Res Commun 181:1442–1448
Cao BY, Yang YP, Luo WF et al (2010) Paeoniflorin, a potent natural compound, protects PC12 cells from MPP+ and acidic damage via autophagic pathway. J Ethnopharmacol 131(1):122–129
Wankun X, Wenzhen Y, Min Z et al (2011) Protective effect of paeoniflorin against oxidative stress in human retinal pigment epithelium in vitro. Mol Vis 17:3512–3522
Wang D, Wong HK, Feng YB et al (2013) Paeoniflorin, a natural neuroprotective agent, modulates multiple anti-apoptotic and pro-apoptotic pathways in differentiated PC12 cells. Cell Mol Neurobiol 33:521–529
Zandbergen EG, de Haan RJ, Hijdra A (2001) Systematic review of prediction of poor outcome in anoxic-ischaemic coma with biochemical markers of brain damage. Intensive Care Med 27(10):1661–1667
Lee CS, Park SY, Ko HH et al (2005) Inhibition of MPP+-induced mitochondrial damage and cell death by trifluoperazine and W-7 in PC12 cells. Neurochem Int 46:169–178
Li N, Liu B, Dluzen DE, Jin Y (2007) Protective effects of ginsenoside Rg2 against glutamate-induced neurotoxicity inPC12 cells. J Ethnopharmacol 111:458–463
Sugaya A, Suzuki T, Sugaya E et al (1991) Inhibitory effect of peony root extract on pentylenete-trazol-induced EEG power spectrum changes and extracellular calcium concentration changes in rat cerebral cortex. J Ethnopharmacol 33(1–2):159–167
Giorgi C, Baldassari F, Bononi A et al (2012) Mitochondrial Ca(2+) and apoptosis. Cell Calcium 52(1):36–43
Naoi M, Maruyama W, Yi H, Inaba K et al (2009) Mitochondria in neurodegenerative disorders: regulation of the redox state and death signaling leading to neuronal death and survival. J Neural Transm 116(11):1371–1381
Mayer B, Oberbauer R (2003) Mitochondrial regulation of apoptosis. News Physiol Sci 18:89–94
Cory S, Adams JM (2002) The Bcl-2 family: regulators of the cellular life-or-death switch. Nat Rev Cancer 2(9):647–656
O’Malley KL, Liu J, Lotharius J et al (2003) Targeted expression of Bcl-2 attenuates MPP+ but not 6-OHDA induced cell death in dopaminergic neurons. Neurobiol Dis 14(1):43–51
Nicotra A, Parvez S (2002) Apoptotic molecules and MPTP-induced cell death. Neurotoxicol Teratol 24(5):599–605
Mills JC, Wang S, Erecinska M et al (1995) Use of cultured neurons and neuronal cell lines to study morphological, biochemical, and molecular changes occurring in cell death. Methods Cell Biol 46:217–242
Blum D, TorchS Lambeng N et al (2001) Molecular pathways involved in the neurotoxicity of 6-OHDA, dopamine and MPTP: contribution to the apoptotic theory in Parkinson’s disease. Prog Neurobiol 65:135–172
Anvekar RA, Asciolla JJ, Missert DJ et al (2011) Born to be alive: a role for the BCL-2 family in melanoma tumor cell survival, apoptosis, and treatment. Front Oncol 1:1–4
MacGibbon GA, Lawlor PA, Sirimanne ES et al (1997) Bax expression in mammalian neurons undergoing apoptosis, and in Alzheimer’s disease hippocampus. Brain Res 750:223–234
Miller TM, Moulder KL, Knudson CM et al (1997) Bax deletion further orders the cell death pathway in cerebellar granule cells and suggests a caspaseindependent pathway to cell death. J Cell Biol 139:205–217
Yu J, Zhou X, He X et al (2011) Curcumin induces apoptosis involving bax/bcl-2 in human hepatoma SMMC-7721 cells. Asian Pac J Cancer Prev 12:1925–1929
Zhao J, Wang LP, Nie JS et al (2011) Effects of benzo(a)pryene on apoptosis of neuronal cells and expression of Bcl-2 and Bax proteins in rat brain tissue. Zhonghua Lao Dong Wei Sheng Zhi Ye Bing Za Zhi 29:820–824
Acknowledgments
This project was supported by the National Natural Science Foundation of China (31370374 and 31170326 and 31400453 and 81373899 and 31350003), the Natural Science Foundation of Jilin Province of China [(2014)D254 and 20130413043GH and 20130102063JC and 20130521013JH and 20140311032YY], and Natural Science Foundation of Changchun Normal University [(2012) D004].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Standards
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Zheng, M., Liu, C., Fan, Y. et al. Protective Effects of Paeoniflorin Against MPP+-induced Neurotoxicity in PC12 Cells. Neurochem Res 41, 1323–1334 (2016). https://doi.org/10.1007/s11064-016-1834-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-016-1834-z