Abstract
Insulin contributes to atherosclerosis, but the potential mechanisms are kept unclear. In this study, insulin promoted proliferation of A7r5 cells. Microarray analysis indicated that insulin significantly changed 812 probe sets of genes, including 405 upregulated and 407 downregulated ones (fold change ≥ 1.5 or ≤ − 1.5; p < 0.05). Gene ontology analysis showed that the differentially expressed genes were involved in a number of processes, including the regulation of cell proliferation/migration/cycle, apoptotic process, oxidative stress, inflammatory response, mitogen-activated protein kinase (MAPK) activity, lipid metabolic process and extracellular matrix organization. Moreover, Kyoto Encyclopedia of Genes and Genomes pathway analysis indicated that the genes were involved in biosynthesis of amino acids, fatty acid metabolism, glycolysis/gluconeogenesis, metabolic pathways, regulation of autophagy, cell cycle and apoptosis, as well as the PI3K-Akt, MAPK, mTOR and NF-κB signaling pathways. Additionally, insulin enhanced phosphorylation of MAPK kinase 1/2 and Akt, suggesting activation of the MAPK and PI3K-Akt signaling pathways. Inhibition of ERK1/2 reduced insulin-induced proliferation. This study revealed the proliferative effects of insulin and displayed global gene expression profile of A7r5 cells stimulated by insulin, suggesting new insight into the molecular pathogenesis of insulin promoting atherosclerosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes is a chronic metabolic disorder associated with a high risk of macrovascular complications. Patients with diabetes have a higher prevalence of atherosclerosis and atherosclerotic vascular disease events than subjects without diabetes [1]. Atherosclerosis is a pathophysiological basis of type 2 diabetic macrovascular complications. Abnormal proliferation and migration of vascular smooth muscle cells (VSMCs) play a key role in vascular remodeling and restenosis during the development of atherosclerosis. Indeed, diabetes promotes VSMC proliferation and accumulation in atherosclerotic lesions [2]. Type 2 diabetes, characterized by insulin resistance, often coexists with hyperinsulinemia. Insulin resistance is closely related to atherosclerosis in patients with type 2 diabetes [3]. High-dose insulin therapy adversely affects the risk of cardiovascular events in type 2 diabetes [4]. Studies revealed that insulin accelerates proliferation and migration of VSMCs [5, 6], suggesting a key role of insulin in diabetic atherosclerosis.
Insulin exerts a series of biological functions through activating at least two pathways including the mitogen-activated protein kinase (MAPK) and the PI3K-Akt signaling pathways [7, 8]. Upon insulin stimulation, activated insulin receptor (InsR) phosphorylates InsR substrate which in turn activates the small GTP-binding protein Ras through the binding of growth-factor receptor bound protein-2 (Grb2) and son-of-sevenless (SOS) [8]. Activated InsR phosphorylates Src-homology-2-containing protein, which also enhances the activity of Ras via the binding of Grb2 and SOS. Finally, Ras promotes activation of Raf, thus triggering MAPK cascades [8]. MAPK family mainly contains extracellular signal-regulated kinase 1 and 2 (ERK1/2), the JNKs, and the p38MAPK. The MAPK signaling pathway is involved with cell growth, proliferation, survival, and cellular differentiation. Inhibition of the MAPK signaling pathway blocks insulin-induced proliferation and migration of VSMCs [6]. Furthermore, activation of the PI3K-Akt signaling pathway by insulin impacts on metabolic effects of glucose, fat and protein [8]. However, the potential mechanisms of action through which insulin promotes atherosclerosis through VSMCs are kept unclear.
This study aimed to observe the effects of insulin on proliferation and the global gene expression profile of A7r5 rat aortic smooth muscle cells, which would reveal the potential mechanisms of action by which insulin promotes atherosclerosis.
Materials and methods
Cell culture
A7r5 cells were provided by the Cell Bank of Type Culture Collection of the Chinese Academy of Science (Shanghai, China) and cultured in high glucose DMEM (GIBCO, USA), supplemented with 10% FBS (GIBCO, USA). The cells were maintained in a humidified incubator with 7.5% CO2 at 37 °C.
Cell proliferation assay
A7r5 cells were cultured in DMEM containing 10% FBS. After 24 h, the cells were serum starved overnight in DMEM with 1% FBS, and then treated with various concentrations of insulin (Sigma, USA; 0–10 μM) or/and PD98059 (Sigma, USA; 10 μM). After incubation for 24, 48, or 72 h, the medium was replaced with serum-free DMEM, and CCK-8 solution (Dojingdo Molecular Technologies, USA) was added to each well. The optical absorbance was determined at 450 nm using a microplate reader (Infinite® 200 Pro NanoQuant, Tecan Group) after incubation for 1 h at 37 °C.
Total RNA extraction
A7r5 cells were incubated in DMEM (containing 1% FBS) with insulin (10 μM) (mode group, MOD) or without insulin (control group, CON). After 24 h, total RNA was isolated using TRIzol® reagent (Life Technologies, USA) followed by purification with RNasey Mini Kit (Qiagen, Germany) according to the manufacturers’ instructions. The concentration of RNA was quantified using the NanoDrop® ND-2000 Spectrophotometer (NanoDrop Technologies). The integrity of RNA was checked using an Agilent Bioanalyzer 2100 (Agilent Technologies), and RNA purity fulfilled the criterium of A260/280 ≥ 1.8. The integrity met the following criteria: RNA Integrity Number ≥ 7 and 28S/18S ≥ 0.7.
Microarray analysis
Total RNA was converted into complementary DNA (cDNA) using GeneChip™ 3′ IVT PLUS Reagent kit (Affymetrix, USA). Then, cDNA was amplified and transcribed into biotin labeled complementary RNA (cRNA) using GeneChip® 3′ IVT Express Kit (Affymetrix) following the manufacturer’s instructions. Biotin-tagged cRNA was purified and fragmented to strands of 35–200 bases in length. The fragmented cRNA was mixed with control oligonucleotide B2, 20 × hybridization controls (bioB, bioC, bioD, cre), 2 × hybridization mix, DMSO and nuclease-free water. After incubation for 5 min at 99 °C and subsequently 5 min at 45 °C, the sample was hybridized to GeneChip® Rat Genome 230 2.0 Array Chips (Affymetrix). The hybridization was performed at 45 °C and rotated at 60 rpm for 16 h using a GeneChip Hybridization Oven 640 (Affymetrix). The chips were washed and stained using a Fluidics Station 450 (Affymetrix). Finally, the chips were scanned using a GeneChip Scanner 3000 (Affymetrix). Microarray analysis was performed in the Shanghai OE Biotech, Co., Ltd. (Shanghai, China).
Reverse transcription-quantitative PCR assays
RT-qPCR was used to confirm representative genes from the microarray analysis. Total RNA was reverse transcribed into cDNA using HiScript II Q RT SuperMix (Vazyme Biotech, China), which was performed in a GeneAmp® PCR System 9700 (Applied Biosystems). qPCR was performed using a LightCycler® 480 II Real-time PCR Instrument (Roche Diagnostics). The reaction conditions were as follows: initial stage, 95 °C for 30 s; cycling stage, denaturation, 95 °C for 10 s; and anneal and extension, 60 °C for 30 s. The primer sequences used are shown in Table 1.
Western blotting
The protein expression and phosphorylation levels of MAPK kinase (MEK1/2) and Akt were analyzed using western blotting. After insulin treatment for 24 h, the cells were lysed in cold RIPA cell lysis buffer followed by ultrasonic lysis. The protein concentrations were quantified using a BCA Protein Assay kit (Thermo Fisher Scientific, USA). The proteins were separated using SDS-PAGE and electrophoretically transferred to PVDF membranes. The membranes were blocked using 5% non-fat dried milk and subsequently incubated with primary antibodies (Cell Signaling Technology, USA) overnight at 4 °C. After incubation of membranes with secondary antibodies (Jackson Immunoresearch, USA) for 1 h at room temperature, the targeted protein bands were detected using the ECL detection reagents (Shanghai Yi Sheng Biotechnology, China).
Statistical analysis
The data from cell proliferation, RT-qPCR assays and western blotting were analyzed using SPSS 16.0 for Windows and are presented as mean ± SD. The difference between two groups was identified using Student’s t-test, and comparisons among groups were performed using one-way ANOVA followed by Tukey’s test. A p value of < 0.05 was considered to indicate statistically significance. The chip-scanned images were analyzed to generate raw data using an Affymetrix GeneChip Command Console (Version 4.0). The array data were normalized using an Affymetrix Transcriptome Analysis Console (TAC Version 4.0) based on the robust multichip average and subsequently analyzed using the TAC Software. The differentially expressed genes between two groups were identified through fold changes and p-value from t-test as follows: fold change ≥ 1.5 or ≤ − 1.5, and p < 0.05. Afterwards, gene ontology (GO) analysis was employed to determine the roles of the genes. Molecular pathways enriched by differentially expressed genes were identified using the Kyoto Encyclopedia of Genes and Genomes (KEGG). Finally, unsupervised hierarchical clustering was performed to display the distinguishable genes expression pattern between groups and a volcano plot was constructed using TAC Software.
Results
Effects of insulin on the proliferation of A7r5 cells
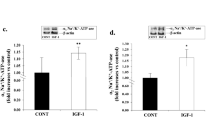
As shown in Fig. 1, treatment with insulin (0.1–10 μM) for 24 h significantly increased absorbance (Fig. 1a) and number (Fig. 1b) of A7r5 cells in a dose-dependent manner when compared with the control group (0 μM insulin; p < 0.05 or p < 0.01). Moreover, the absorbance was enhanced by insulin incubation for 48 h (Fig. 1c, all p < 0.01) and 72 h (Fig. 1d) in an insulin dose-dependent fashion. Additionally, the peak of cell proliferation induced by insulin was at 24 h or 48 h because 10 μM insulin promoted cell proliferation to 223.38%, 235.71%, 192.01% of the control group (0 μM insulin) for 24, 48, 72 h, respectively. The data indicated that insulin promotes proliferation of A7r5 cells. Li et al. reported that insulin at 10 μM causes maximum proliferation of rat aortic smooth muscle cells among 0.001–100 μM insulin [7], and that insulin promotes cell proliferation in a time-dependent fashion (0–48 h), to 24 h to the peak [7]. Therefore, we chose the optimum level of insulin at 10 μM and the optimum intervention time of 24 h to do the microarray analysis.
Effects of insulin on the global gene expression profile of A7r5 cells
To reveal the potential mechanisms of action by which insulin promotes proliferation, the effects of insulin on the gene expression profile of A7r5 cells was observed using microarray analysis. Compared with the control group (without insulin treatment), 812 probe sets of genes in the model group (10 μM insulin treatment for 24 h) were found to be differentially expressed, of which 405 were upregulated and 407 were downregulated (Supplementary Table 1). The differentially expressed genes were selected for clustering according to their similarity, and the results are shown in Fig. 2a with the vertical axis representing the clustering of genes based on their expression profile, and the horizontal axis indicating the clustering in the light of the sample. Additionally, the microarray data were used to construct volcano plots (Fig. 2b). In the volcano plots, the vertical axis shows the statistical significance, which was equal to the negative log10 of p-value; thus, low p-values are located at the top of the plot. The horizontal axis corresponds to fold change, and the changes in both directions are symmetric from the center. Red points represent the upregulated genes (Fig. 2b), fold change ≥ 1.5 with p < 0.05, whereas green points represent the downregulated genes, fold change ≤ − 1.5 with p < 0.05.
Hierarchical cluster analysis and a volcano plot in A7r5 cells. a After treatment with insulin (10 μM) for 24 h, the genes differentially expressed between the control group (CON, n = 4; without insulin treatment) and the model group (MOD, n = 4; with insulin treatment) were visualized as a heat map after unsupervised hierarchical clustering. Color tags display the levels of gene expression, the blue and the red spectrum indicates the downregulated and the upregulated genes, respectively. b A volcano plot was constructed according to biological and statistical significance using the microarray data from the control group and the model group. The vertical axis represents the statistical significance and horizontal axis exhibits the fold change. The downregulated genes with fold change ≤ − 1.5 and p < 0.05 were labelled as green points, while the upregulated ones with fold change ≥ 1.5 and p < 0.05 were marked as red points
Verification of differentially expressed genes
RT‑qPCR was used to validate the microarray data by determining the relative mRNA levels of 14 representative genes. Compared with the control group, insulin significantly increased mRNA levels of genes including Myc (Fig. 3a), Jun (Fig. 3b), Cd44 (Fig. 3c), Ccnd1 (Fig. 3d), Il1r1 (Fig. 3k), Socs3 (Fig. 3l) and Rad18 (Fig. 3n), while reducing gene expression levels of Cdkn1b (Fig. 3e), Gas6 (Fig. 3f), Sox4 (Fig. 3g), Gadd45a (Fig. 3h), Bcl2l11 (Fig. 3i), Ulk1 (Fig. 3j) and Pdgfrb (Fig. 3m). These results were consistent with the microarray data.
Relative mRNA levels of the differentially expressed genes in A7r5 cells. The cells were seeded at a density of 2.5–4.0 × 104/ml. After 24 h, the cells were starved overnight and then incubated with insulin (10 μM) for 24 h, the mRNA levels of Myc (a), Jun (b), Cd44 (c), Ccnd1 (d), Cdkn1b (e), Gas6 (f), Sox (g), Gadd45a (h), Bcl2l11 (i), Ulk1 (j), Il1r1 (k), Socs3 (l), Pdgfrb (m), and Rad (n) in A7r5 cells from the control group (CON, n = 4; without insulin treatment) and the model group (MOD, n = 4; with insulin treatment) were analyzed using RT-qPCR as materials and methods described. *p < 0.05 and **p < 0.01 vs. the control (0 μM insulin)
Functional classification of the differentially expressed genes
GO analysis was used to display the potential functions of the genes. The functions were divided into three large categories, namely, molecular function, biological process and cellular component. Figure 4a indicates the top 20 GO terms in molecular function ranked according to a negative log10 of p-value, including ‘protein homodimerization activity’, ‘collagen binding’, ‘calcium ion binding’, ‘1-phosphatidylinositol binding’, ‘protein binding’, ‘peroxidase activity’, and ‘receptor binding’. Furthermore, the molecular function of the differentially expressed genes still referred to ‘protein kinase binding’, ‘signaling adaptor activity’, ‘chemokine activity’, ‘receptor agonist activity’, ‘phosphatidylinositol 3-kinase binding’ and ‘protein tyrosine kinase activator activity’ (Supplementary Table 2). For biological process, the differentially expressed genes mainly involved in ‘response to drug’, ‘cell adhesion’, ‘cellular sodium ion homeostasis’, ‘response to hypoxia’, ‘response to nutrient’, ‘extracellular matrix organization’ and ‘memory’ (Fig. 4b). Additionally, the genes were still related to ‘positive regulation of cell migration’, ‘negative regulation of apoptotic process’, ‘cell growth’, ‘positive regulation of cell cycle’, ‘positive regulation of MAPK activity’, ‘positive regulation of ERK1/ERK2 cascade’, ‘positive regulation of cell proliferation’, ‘positive regulation of collagen biosynthetic process’, ‘response to oxidative stress’, and ‘regulation of inflammatory response’ (Supplementary Table 3). The most significantly enriched cellular component categories were ‘cytoplasm’, ‘membrane’ and ‘extracellular space’ (Fig. 4c and Supplementary Table 4).
GO and molecular pathway analysis for the differentially expressed genes. a–c The results from GO enrichment analysis were divided into three large function categories, including molecular function, biological process and cellular component. The figure indicates the top 20 GO functions regulated in molecular function (a), biological process (b) and cellular component (c) categories based on a negative log10 of P value, respectively. The vertical axis indicates the GO term description, and the horizontal axis represents statistical evidence. d Pathway analysis was performed based on the Kyoto Encyclopedia of Genes and Genomes (KEGG). The figure displays the top 20 KEGG pathways regulated sorting by a negative log10 of P value. The vertical axis shows the pathway term description, and the horizontal axis means the statistical evidence
Effects of insulin on molecular pathways
Figure 4d shows the top 20 molecular pathways in A7r5 cells, including ‘ECM-receptor interaction’, ‘hypertrophic cardiomyopathy (HCM)’, ‘PI3K-Akt signaling pathway’, ‘protein digestion and absorption’ and ‘pathways in cancer’. Moreover, the differentially expressed genes also enriched in ‘biosynthesis of amino acids’, ‘TNF signaling pathway’, ‘FoxO signaling pathway’, ‘metabolic pathways’, and involved in ‘TGF-β signaling pathway’, ‘fatty acid metabolism’, ‘regulation of autophagy’, ‘MAPK signaling pathway’, ‘mTOR signaling pathway’, ‘cell cycle’, ‘apoptosis’, ‘NF-κB signaling pathway’ and ‘type II diabetes mellitus’ (Supplementary Table 5).
Insulin increases phosphorylation of MEK1/2 and Akt, and PD98059 inhibits insulin-induced proliferation of A7r5 cells
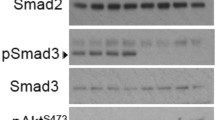
GO analysis indicated that A7r5 cell proliferation induced by insulin was related to positive regulation of MAP kinase activity and ERK1 and ERK2 cascade. KEGG pathway analysis also revealed the close relationship between insulin-induced proliferation of A7r5 cells and MAPK signaling pathway or PI3K-Akt signaling pathway. Here, insulin treatment for 24 h did not change the protein expression of MEK1/2 in A7r5 cells, but significantly increased phosphorylation of MEK1/2 (Fig. 5a), which is responsible for activation of ERK1/2. Specific inhibition of ERK1/2 by PD98059 significantly decreased insulin-induced absorbance in A7r5 cells (Fig. 5c; p < 0.01). Similarly, insulin did not affect the protein expression of Akt, but significantly promoted its phosphorylation (Fig. 5b), indicating the activation of the PI3K-Akt signaling pathway.
Effects of insulin on the protein expression and phosphorylation levels of MEK1/2 and Akt, and inhibition of PD98059 on insulin-induced proliferation. The cells were seeded at a density of 2.5–4.0 × 104/ml. After 24 h, the cells were starved overnight and then treated with insulin for protein expression analysis or insulin and PD98059 for cell proliferation assay. After treatment for 24 h, the protein expression and phosphorylation of MEK1/2 (a) and Akt (b) were analyzed by western blotting, and cell proliferation (c) was analyzed using CCK-8 assays. *p < 0.05 and **p < 0.01 vs. the control (0.0 μM insulin); ##p < 0.01 vs. insulin (1.0 μM)
Discussion
Insulin resistance is associated with increased atherosclerosis. Study indicated that the thoracic aortic medial wall area increased more quickly in non-insulin-dependent diabetic rats with hyperinsulinemia compared with non-diabetic rats [9]. Insulin treatment accelerates the development of atherosclerotic plaques and increases the thickness of the aortic walls of animals [10, 11], suggesting a key role of insulin in promoting atherosclerosis. VSMCs are required for the pathophysiological process of atherosclerosis. In this study, insulin promoted proliferation of A7r5 cells, which is consistent with previous reports [5, 6]. And insulin altered 812 probe sets of genes, of which 405 were upregulated and 407 were downregulated. GO analysis showed that certain genes, such as Myc, Jun, Ccnd1, Pdgfrb, Gas6 and Cdkn1b were involved in the positive regulation of cell proliferation; Cdkn1b, Gadd45a, Myc and Bcl2l11 were involved in the regulation of cell cycle; and Pdgfrb and Cd44 were associated with cell migration. RT-qPCR verified that insulin increased mRNA levels of Myc, Jun and Ccnd1. Inhibition of Myc, Jun and Ccnd1 blocks proliferation of VSMCs [12,13,14]. Moreover, insulin decreased gene expression of Cdkn1b and Gadd45a. Inhibition of cell growth and G1-phase cell cycle arrest are associated with the upregulation of Cdkn1b expression in VSMCs [15], and activation of Gadd45a is beneficial for the inhibition of cell cycle [16]. Moreover, insulin enhanced Cd44 mRNA levels in A7r5 cells. Upregulation of Cd44 was associated with VSMC migration [17]. Insulin treatment triggers at least two signaling pathways, including the MAPK and the PI3K signaling pathways. Activation of the MAPK signaling pathway by growth factors, including insulin, controls the proliferation and migration of VSMCs [6, 7]. GO and KEGG analysis revealed that insulin positively regulates MAPK activity and ERK1/2 cascade, thus associating with the MAPK signaling pathway. Indeed, insulin promoted phosphorylation of MEK1/2 which is responsible for the activation of ERK1/2. Inhibition of ERK1/2 by PD98059 decreased insulin-induced proliferation of A7r5 cells. These results suggest that insulin promotes proliferation and migration of VSMCs, at least in part by regulating the MAPK signaling pathway. Just as GO and KEGG analysis demonstrated, in response to insulin, the PI3K-Akt signaling pathway mainly contributes to the regulation of substance metabolism including glucose, protein and fatty, but the pathway also mediates the proliferation of VSMCs [18]. In this study, insulin increased the phosphorylation of Akt, suggesting activation of the PI3K-Akt signaling pathway. Inhibition of the pathway significantly reduces insulin-induced proliferation of VSMCs [18]. Additionally, GO and KEGG analysis also indicated the close relationship between insulin and cell death/apoptosis. Increased evidence has confirmed the anti-apoptotic effect of insulin on VSMCs via the PI3K-Akt signaling pathway [19]. Because of the mitogenic properties, insulin is often used to treat external wounds including diabetic foot ulcers [20].
In this study, insulin reduced the mRNA levels of Ulk1 and gene expression of Atg14, implying an inhibitory effect of insulin on autophagy. Similarly, insulin downregulates autophagy in human skeletal muscle [21]. Studies have indicated that autophagy plays a crucial role in regulating VSMC homeostasis in atherogenesis and atherosclerotic plaque stability [22]. Elevated autophagy prevents the proliferation of coronary arterial myocytes [23], inhibits VSMC senescence and stabilizes atherosclerotic plaques [24]. By contrast, defective autophagy in VSMCs promotes VSMC senescence, enhances atherosclerotic plaque instability and the risk of plaque rupture, thus accelerating development of atherosclerosis [25, 26]. Moreover, activation of the PI3K-Akt/mTOR pathway or the MAPK/mTOR pathway inhibited autophagy in VSMCs [27, 28], while triggering the AMPK/mTOR signaling pathway induced autophagy in VSMCs [29]. In this study, insulin activated the MAPK and the PI3K-Akt signaling pathways in A7r5 cells. KEGG analysis indicated the close relationship between insulin and the AMPK signaling pathway. Hence, insulin may inhibit autophagy in A7r5 cells by regulating the MAPK, the PI3K-Akt signaling pathways or the AMPK signaling pathways.
Atherosclerosis is a chronic inflammatory process. Inflammation contributes to the progression of atherosclerosis by modifying the morphology and composition of atherosclerotic plaques. In this study, some differentially expressed genes, including Il1r1 and Socs3, were enriched in the regulation of inflammatory response and monocyte chemotaxis. Insulin resistance promotes a pro-inflammatory and pro-oxidant state, thereby boosting the formation of atherosclerotic plaque in apolipoprotein E knock out (ApoE-KO) mice [30]. Insulin treatment increases plasma inflammatory cytokines in type 2 diabetic patients, including IL-6, TNF-α, monocyte chemoattractant protein (MCP-1) and vascular cell adhesion molecule [31]. Further studies revealed that insulin promotes monocyte migration to and infiltration of the arterial wall [32], and facilitates inflammatory cytokine production from monocyte [33]. High insulin enhances the mRNA levels of IL-6 and MCP-1 in VSMCs which are linked to the activation of the MAPK/NF-κB pathways [34]. Suppression of the MAPK/NF-κB signaling pathways reduces insulin-induced inflammatory cytokine [34]. In accordance, insulin increases the expression of matrix metalloproteinase-9 (MMP-9) via the phosphorylation of ERK1/2, thus potentiating monocyte chemotaxis [32].
Oxidative stress, resulting from the excess production of ROS and reactive nitrogen species, also contributes to atherosclerosis, and accelerates development of diabetic atherosclerosis [35]. ROS can directly damage vascular cells through oxidative modification of protein, DNA strand breakage and cellular lipid oxidation. Insulin resistance promotes oxidative stress in fructose-fed ApoE-KO mice [30] and elevated doses insulin therapy induces oxidative stress in type 2 diabetic patients [36]. A high insulin level augments the excessive production of ROS by enhancing NADPH oxidase activity and NADPH oxidase 1 mRNA expression, thus leading to proliferation and migration of VSMCs [37]. Antioxidant treatment using N-acetylcysteine and diphenyleneiodonium blocks insulin-induced proliferation and migration of VSMCs [37, 38]. In this study, insulin treatment was associated with oxidative stress and ROS production, which were compliant with previous reports [37, 38].
Atherosclerosis is characterized by atherosclerotic plaque. VSMCs synthesize and secrete ECM components such as collagen, fibronectin, proteoglycans and elastin [39]. ECM affects not only vascular stiffness but also the formation of fibrous cap, which cover the fatty streak lesions. Vascular stiffness and the expression of fibronectin and collagen IV alpha 3 are increased in the aorta of type 2 diabetic rats [40]. Insulin also promotes collagen synthesis and elastin production in VSMCs [41, 42]. In this study, the differentially expressed genes were enriched in ‘positive regulation of collagen biosynthetic process’ and ‘ECM organization’, suggesting the importance of insulin in regulating the ECM composition and the stability of atherosclerotic plaque.
Additionally, insulin resistance increases the risk of dementia [43]. Chronic insulin stimulation causes dysfunction of insulin-associated signaling pathways, including the PI3K-Akt signaling pathway, thereby resulting in insulin resistance and a reduction in glucose metabolism [44]. Due to the disorder of glucose metabolism, vascular disease and neuron cell death, cognitive function is easily impaired in type 2 diabetes.
Overall, this study indicated the proliferative effects of insulin and displayed the global gene expression profile of A7r5 cells following insulin treatment, suggesting new insights into the molecular pathways by which insulin promotes atherosclerosis.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Krempf M, Parhofer KG, Steg PG et al (2010) Cardiovascular event rates in diabetic and nondiabetic individuals with and without established atherothrombosis (from the REduction of Atherothrombosis for Continued Health [REACH] Registry). Am J Cardiol 105:667–671
Suzuki LA, Poot M, Gerrity RG et al (2001) Diabetes accelerates smooth muscle accumulation in lesions of atherosclerosis: lack of direct growth-promoting effects of high glucose levels. Diabetes 50:851–860
Park SW, Kim SK, Cho YW et al (2009) Insulin resistance and carotid atherosclerosis in patients with type 2 diabetes. Atherosclerosis 205(1):309–313
Stoekenbroek RM, Rensing KL, Bernelot Moens SJ et al (2015) High daily insulin exposure in patients with type 2 diabetes is associated with increased risk of cardiovascular events. Atherosclerosis 240:318–323
Yu C, Wang Z, Han Y et al (2014) Dopamine D4 receptors inhibit proliferation and migration of vascular smooth muscle cells induced by insulin via down-regulation of insulin receptor expression. Cardiovasc Diabetol 13:97
Su XL, Wang Y, Zhang W et al (2011) Insulin-mediated upregulation of K(Ca)3.1 channels promotes cell migration and proliferation in rat vascular smooth muscle. J Mol Cell Cardiol 51:51–57
Li F, Xia K, Sheikh MS et al (2014) Retinol binding protein 4 promotes hyperinsulinism-induced proliferation of rat aortic smooth muscle cells. Mol Med Rep 9:1634–1640
Taniguchi CM, Emanuelli B, Kahn CR (2006) Critical nodes in signalling pathways: insights into insulin action. Nat Rev Mol Cell Biol 7:85–96
Hosomi N, Noma T, Ohyama H et al (2002) Vascular proliferation and transforming growth factor-beta expression in pre- and early stage of diabetes mellitus in Otsuka Long-Evans Tokushima fatty rats. Atherosclerosis 162:69–76
Li F, Xia K, Sheikh SA et al (2015) Involvement of RBP4 in hyperinsulinism-induced vascular smooth muscle cell proliferation. Endocrine 48:472–482
Min J, Weitian Z, Peng C et al (2016) Correlation between insulin-induced estrogen receptor methylation and atherosclerosis. Cardiovasc Diabetol 15:156
Bennett MR, Anglin S, McEwan JR et al (1994) Inhibition of vascular smooth muscle cell proliferation in vitro and in vivo by c-myc antisense oligodeoxynucleotides. J Clin Invest 93:820–828
Li T, Song T, Ni L et al (2014) The p-ERK-p-c-Jun-cyclinD1 pathway is involved in proliferation of smooth muscle cells after exposure to cigarette smoke extract. Biochem Biophys Res Commun 453:316–320
Kim MH, Ham O, Lee SY et al (2014) MicroRNA-365 inhibits the proliferation of vascular smooth muscle cells by targeting cyclin D1. J Cell Biochem 115:1752–1761
Jung SM, Park SS, Kim WJ et al (2012) Ras/ERK1 pathway regulation of p27KIP1-mediated G1-phase cell-cycle arrest in cordycepin-induced inhibition of the proliferation of vascular smooth muscle cells. Eur J Pharmacol 681:15–22
Suzuki H, Tanabe H, Mizukami H et al (2011) Differential gene expression in rat vascular smooth muscle cells following treatment with coptisine exerts a selective antiproliferative effect. J Nat Prod 74:634–638
Yan D, Liu X, Hua L et al (2016) MMP-14 promotes VSMC migration via up-regulating CD44 expression in cardiac allograft vasculopathy. Pathol Res Pract 212:1119–1125
Isenovic ER, Fretaud M, Koricanac G et al (2009) Insulin regulation of proliferation involves activation of AKT and ERK 1/2 signaling pathways in vascular smooth muscle cells. Exp Clin Endocrinol Diabetes 117:214–219
Nakazawa T, Chiba T, Kaneko E et al (2005) Insulin signaling in arteries prevents smooth muscle apoptosis. Arterioscler Thromb Vasc Biol 25:760–765
Bhittani MK, Rehman M, Altaf HN et al (2020) Effectiveness of topical insulin dressings in management of diabetic foot ulcers. World J Surg 44:2028–2033
Fritzen AM, Madsen AB, Kleinert M et al (2016) Regulation of autophagy in human skeletal muscle: effects of exercise, exercise training and insulin stimulation. J Physiol 594:745–761
Wei YM, Li X, Xu M et al (2013) Enhancement of autophagy by simvastatin through inhibition of Rac1-mTOR signaling pathway in coronary arterial myocytes. Cell Physiol Biochem 31:925–937
Grootaert MOJ, Moulis M, Roth L et al (2018) Vascular smooth muscle cell death, autophagy and senescence in atherosclerosis. Cardiovasc Res 114:622–634
Luo Z, Xu W, Ma S et al (2017) Moderate autophagy inhibits vascular smooth muscle cell senescence to stabilize progressed atherosclerotic plaque via the mTORC1/ULK1/ATG13 signal pathway. Oxid Med Cell Longev 2017:3018190
Masuyama A, Mita T, Azuma K et al (2018) Defective autophagy in vascular smooth muscle cells enhances atherosclerotic plaque instability. Biochem Biophys Res Commun 505:1141–1147
Grootaert MO, da Costa Martins PA, Bitsch N et al (2015) Defective autophagy in vascular smooth muscle cells accelerates senescence and promotes neointima formation and atherogenesis. Autophagy 11:2014–2032
Montes DK, Brenet M, Muñoz VC et al (2013) Vasopressin activates Akt/mTOR pathway in smooth muscle cells cultured in high glucose concentration. Biochem Biophys Res Commun 441:923–928
Song Z, Wei D, Chen Y et al (2019) Association of astragaloside IV-inhibited autophagy and mineralization in vascular smooth muscle cells with lncRNA H19 and DUSP5-mediated ERK signaling. Toxicol Appl Pharmacol 364:45–54
Wu H, Song A, Hu W et al (2018) The anti-atherosclerotic effect of Paeonol against vascular smooth muscle cell proliferation by up-regulation of autophagy via the AMPK/mTOR signaling pathway. Front Pharmacol 8:948
Cannizzo B, Lujάn A, Estrella N et al (2012) Insulin resistance promotes early atherosclerosis via increased proinflammatory proteins and oxidative stress in fructose-fed ApoE-KO mice. Exp Diabetes Res 2012:941304
Antoniades C, Tousoulis D, Marinou K et al (2007) Effects of insulin dependence on inflammatory process, thrombotic mechanisms and endothelial function, in patients with type 2 diabetes mellitus and coronary atherosclerosis. Clin Cardiol 30:295–300
Kappert K, Meyborg H, Clemenz M et al (2008) Insulin facilitates monocyte migration: a possible link to tissue inflammation in insulin-resistance. Biochem Biophys Res Commun 365:503–508
Tsiotra PC, Boutati E, Dimitriadis G et al (2013) High insulin and leptin increase resistin and inflammatory cytokine production from human mononuclear cells. Biomed Res Int 2013:487081
Zhang BF, Jiang H, Chen J et al (2018) KDM3A inhibition attenuates high concentration insulin-induced vascular smooth muscle cell injury by suppressing MAPK/NF-κB pathways. Int J Mol Med 41:1265–1274
Yuan T, Yang T, Chen H et al (2019) New insights into oxidative stress and inflammation during diabetes mellitus-accelerated atherosclerosis. Redox Biol 20:247–260
Monnier L, Colette C, Michel F et al (2011) Insulin therapy has a complex relationship with measure of oxidative stress in type 2 diabetes: a case for further study. Diabetes Metab Res Rev 27:348–353
Abhijit S, Bhaskaran R, Narayanasamy A et al (2013) Hyperinsulinemia-induced vascular smooth muscle cell (VSMC) migration and proliferation is mediated by converging mechanisms of mitochondrial dysfunction and oxidative stress. Mol Cell Biochem 373:95–105
He R, Qu AJ, Mao JM et al (2007) Synergistic proliferation induced by insulin and glycated serum albumin in rat vascular smooth muscle cells. Sheng Li Xue Bao 59:1–7
Zeadin MG, Petlura CI, Werstuck GH (2013) Molecular mechanisms linking diabetes to the accelerated development of atherosclerosis. Can J Diabetes 37:345–350
Sista AK, O’Connell MK, Hinohara T et al (2005) Increased aortic stiffness in the insulin-resistant Zucker fa/fa rat. Am J Physiol Heart Circ Physiol 289:H845–H851
Ruiz-Torres A, Melón J, Muñoz FJ (1998) Insulin stimulates collagen synthesis in vascular smooth muscle cells from elderly patients. Gerontology 44:144–148
Shi J, Wang A, Sen S et al (2012) Insulin induces production of new elastin in cultures of human aortic smooth muscle cells. Am J Pathol 180:715–726
Bello-Chavolla OY, Antonio-Villa NE, Vargas-Vázquez A et al (2019) Pathophysiological mechanisms linking type 2 diabetes and dementia: review of evidence from clinical, translational and epidemiological research. Curr Diabetes Rev 15:456–470
Song J, Kang SM, Kim E et al (2015) Impairment of insulin receptor substrate 1 signaling by insulin resistance inhibits neurite outgrowth and aggravates neuronal cell death. Neuroscience 301:26–38
Funding
This study was supported by the National Natural Science Foundation of China (Nos. 81460711 and 81760852), the Guangxi National Natural Science Foundation (Nos. 2017GXNSFAA198284 and 2014GXNSFAA118264), the Innovation Project of Guangxi Graduate Education (No. JGY2018084), the Guangxi Key Laboratory of Chinese Medicine Foundation Research (No. 20-065-53), Guangxi University of Chinese Medicine, the Cultivation Program of 1000 Young and Middle-aged Backbone Teachers in Higher Education of Guangxi (No. Gui Teacher Education [2019]81), and the Guangxi Collabrative Innovation Center for Scientific Achievements Transformation and Application on Traditional Chinese Medicine (No. 05020058).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Duan, H., Feng, X. & Huang, X. Effects of insulin on the proliferation and global gene expression profile of A7r5 cells. Mol Biol Rep 48, 1205–1215 (2021). https://doi.org/10.1007/s11033-021-06200-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-06200-8