Abstract
Background
We previously demonstrated that insulin-like growth factor-1 (IGF-1) regulates sodium/potassium adenosine triphosphatase (Na+/K+-ATPase) in vascular smooth muscle cells (VSMC) via phosphatidylinositol-3 kinase (PI3K). Taking into account that others’ work show that IGF-1 activates the PI3K/protein kinase B (Akt) signaling pathway in many different cells, we here further questioned if the Akt/mammalian target of rapamycin (mTOR)/ribosomal protein p70 S6 kinase (S6K) pathway stimulates Na+/K+-ATPase, an essential protein for maintaining normal heart function.
Methods and results
There were 14 adult male Wistar rats, half of whom received bolus injections of IGF-1 (50 μg/kg) for 24 h. We evaluated cardiac Na+/K+-ATPase expression, activity, and serum IGF-1 levels. Additionally, we examined the phosphorylated forms of the following proteins: insulin receptor substrate (IRS), phosphoinositide-dependent kinase-1 (PDK-1), Akt, mTOR, S6K, and α subunit of Na+/K+-ATPase. Additionally, the mRNA expression of the Na+/K+-ATPase α1 subunit was evaluated. Treatment with IGF-1 increases levels of serum IGF-1 and stimulates Na+/K+-ATPase activity, phosphorylation of α subunit of Na+/K+-ATPase on Ser23, and protein expression of α2 subunit. Furthermore, IGF-1 treatment increased phosphorylation of IRS-1 on Tyr1222, Akt on Ser473, PDK-1 on Ser241, mTOR on Ser2481 and Ser2448, and S6K on Thr421/Ser424. The concentration of IGF-1 in serum positively correlates with Na+/K+-ATPase activity and the phosphorylated form of mTOR (Ser2448), while Na+/K+-ATPase activity positively correlates with the phosphorylated form of IRS-1 (Tyr1222) and mTOR (Ser2448).
Conclusion
These results indicate that the Akt/mTOR/S6K signalling pathway may be involved in the IGF-1 regulating cardiac Na+/K+-ATPase expression and activity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The insulin-like growth factor-1 (IGF-1) is a polypeptide growth factor sharing structural similarities with insulin, which regulates cell differentiation, maturation, development, and proliferation in nearly all organs [1]. Numerous studies proposed that IGF-1 plays a role in cardiovascular physiology homeostasis [1]. IGF-1, in particular, regulates vascular vasoconstriction/vasodilation, cardiac apoptosis, and autophagy [2, 3]. Also, IGF-1 exerts anti-inflammatory and anti-oxidant effects in the vasculature by lowering atherosclerotic plaque burden [4]. Furthermore, IGF-1 has angiogenic properties, as indicated by its capacity to regulate endothelial junction protein levels and stimulate angiogenesis in endothelial cells [5]. With the rising prevalence of cardiovascular diseases, research into IGF-1’s role in cardiovascular system function is gaining attention.
The pivotal function of sodium/potassium adenosine triphosphatase (Na+/K+-ATPase) in cells is maintaining Na+ and K+ ions gradient across the membrane by utilizing the energy of hydroxylation of ATP molecule [6]. The Na+/K+-ATPase is required for rapid action potential upstroke and cardiomyocyte contractility by regulating ion exchange and cell membrane trafficking of many substances while maintaining proper cell function and cardiac output [7]. The Na+/K+-ATPase is a heterodimeric transmembrane protein with two essential subunits: a catalytic α subunit and a highly glycosylated β subunit. Additionally, α and β subunits can interact with the γ subunit belonging to the tissue-specific FXYD protein group [8]. The α subunit encompasses ten transmembrane segments responsible for ion transport, a significant intracellular domain with ATP-binding and phosphorylation sites, and an extracellular domain containing binding sites for cardiac glycosides [6]. The β subunit is essential for assembly and increases the stability of the α subunit and modulation of ions affinity [9]. Heart-specific γ subunit or phospholemman stabilizes the Na+/K+-ATPase and its kinetic and transport properties by modifying the affinity for ions and ATP [8].
The effects of IGF-1 are mediated by four types of tyrosine kinase membrane receptors [10]. IGF-1 acts primarily via its putative receptor (IGF-1R) and, with lower affinity, through the insulin receptor (IR), IGF-2 receptor and hybrid receptor with subunits of IGF-1 and IR (IGF-1R/IR) [11]. After interacting with its receptor, IGF-1 initiates autophosphorylation, which creates docking sites for recruiting and phosphorylating various adaptor proteins, including insulin receptor substrate (IRS) [1]. One of the major signalling pathways that are activated via IGF-1 receptors is phosphatidylinositol-3 kinase (PI3K)/protein kinase B (Akt)/mammalian target of rapamycin (mTOR) [1, 12, 13]. Multiple intracellular mediators, such as PI3K, phosphoinositide-dependent protein kinase-1 (PDK-1) and Akt, are involved in IGF-1 signalling across cell types. Despite its primary effect on PI3K, IGF-1 has also been associated with the activation of mTOR/ribosomal protein p70 S6 kinase (S6K) [14]. Another in vitro study showed the involvement of the S6K enzyme in regulating Na+/K+-ATPase protein expression using a model utilizing alveolar epithelial cells transfected with a dominant negative construct of p70S6K [15].
The IGF-1 causes vasorelaxation, which increases nitric oxide generation and Na+/K+-ATPase activation [16]. According to the literature, IGF-1 is a significant regulator of Na+/K+-ATPase in vitro, and its effects are mediated through the PI3K/Akt signalling cascade, which is associated with IGF-1-induced increased Na+/K+-ATPase messenger ribonucleic acid (mRNA) in vascular smooth muscle cells (VSMC) [12, 17, 18]. Through a signalling cascade involving IRS/PI3K/PDK/Akt/mTOR/S6K, this study sought to investigate the in vivo effect of IGF-1 on cardiac Na+/K+-ATPase expression/activity in rats. We hypothesize that a modification in the IRS/PI3K/PDK/Akt/mTOR/S6K signalling pathway, which regulates Na+/K+-ATPase expression and activity, is responsible for IGF-1’s enhanced capacity to activate cardiac Na+/K+-ATPase activity in vivo. An important consequence of this hypothesis is that IGF-1 in vivo increases expression and activity of Na+/K+-ATPase in the heart through a PI3K-dependent activation of the Akt/mTOR cascade, which in turn amplifies mTOR/S6K signalling and, consequently, Na+/K+-ATPase expression and activity.
Materials and methods
Animals
The research was conducted on adult male Wistar rats that were nurtured at the Institute of Nuclear Sciences in Vinca, Belgrade. The animals were kept in cages in optimal laboratory conditions (22 ± 2 °C and 12-hour light-dark cycle) and supplied with food and water ad libitum. Animals were provided with a well-balanced meal specifically designed for laboratory rats, prepared by Veterinarski zavod Subotica in Serbia. The official Vinca Institute’s Ethical Committee for Experimental Animals approved the experimental protocols under Veterinary Directorate No. 323-07-02710/2017-05.
Experimental treatment
A total of 14 animals were divided into 2 groups (n = 7), whereas 24 h before decapitation, the group of rats, labelled as “IGF-1”, was treated intraperitoneally with a bolus injection of 50 µg/kg of IGF-1 (Sigma-Aldrich, I3769-50UG) dissolved in saline. This specific IGF-1 dosage was selected following previously published results [19]. At the same time, the other group of rats (labelled as “Control”) were treated with saline. Animals were anaesthetized with a mixture of ketamine and xylazine (80 mg/kg of ketamine (VetViva Richter GmbH, Austria) and 12 mg/kg xylazine (VET-AGRO Multi trade Company Sp. z.o.o. Poland)), and sacrificed. The blood was collected through cardiac puncture and centrifuged, and obtained serum samples were stored at -80 °C until analysis. The hearts were removed, frozen in liquid nitrogen, and preserved at -80 °C.
Heart lysate preparation
Rat hearts were chopped and homogenized on ice using a homogenizer (Witeg Homogenizer HG-16D) in buffer (1 M Tris, 1.5 M NaCl, 0.1 M EDTA; 10% glycerol, 1% Triton X-100, pH 7.4) using Complete ULTRA protease inhibitor cocktail tablets (Roche, Mannheim, Germany). Homogenates were incubated at 4 °C for 1 h with steady rotation before being ultracentrifuged for 20 min at 100,000 × g, and the resulting lysate was stored at -80 °C, as we previously described [20].
Protein extraction from the heart plasma membrane
Plasma membranes were prepared using the method described by Luiken et al. [21]. Rat hearts were cut on ice and incubated for 30 min in a high-salt solution (20 mM HEPES, 2 M NaCl, and 5 mM sodium azide, pH 7.4) at 4 °C. Following the incubation period, the suspension was centrifugation at 1,000 × g for 5 min. The pellet was homogenized on ice using a Witeg Homogenizer in a TES buffer containing 20 mM Tris, 250 mM sucrose, and 1 mM EDTA at pH 7.4, supplemented with complete ULTRA protease inhibitor cocktail tablets from Roche (Mannheim, Germany). After homogenization, the homogenate was centrifuged a few times, and the isolated plasma membrane fraction was stored at -80 °C, as we previously described [20].
Measurement of serum IGF-1 concentration
The IGF-1 concentration in serum was measured using the radioimmunoassay method with a commercially available kit and IGF-1 standards. The method involved IGF-1 labelled with 125I and polyclonal rabbit antibodies to IGF-1, as was shown previously [22]. The results for IGF-1 were expressed in nM.
Na+/K+-ATPase assay
The Na+/K+-ATPase assay was done in two sets of epruvetes, whereas one set contained 50 µl of incubation mixture (2 M NaCl, 400 mM KCl, 100 mM MgCl2, 1 M Tris pH 7.4 and ddH2O), 105 µl of ddH2O and 25 µl of the sample (1 µg/µl), while other set contained 50 µl of incubation mixture, 20 µl of ouabain, 85 µl of ddH2O and 25 µl of the sample (1 µg/µl), as we previously described [20].
SDS-PAGE and Western blotting
Total protein lysates and plasma membrane protein extracts (40 µg per well) were separated using SDS-polyacrylamide gel electrophoresis and then transferred to polyvinylidene difluoride membranes. Membranes were further blocked in 5% bovine serum albumin. Heart lysate fractions were probed with antibodies (Cell Signaling) directed IRS, phospho-IRS (Ser307) and phospho-IRS (Tyr1222), PDK-1 and phospho-PDK-1 (Ser241) Akt and phospho-Akt (Ser473), mTOR, phospho-mTOR (Ser2481) and phospho-mTOR (Ser2448), S6K and phospho - S6K (Ser241). Plasma membrane fractions were probed with antibodies against the phosphorylated (Ser23) form of α subunit of Na+/K+-ATPase, α1 and α2 subunit of Na+/K+-ATPase (Santa Cruz Biotechnology). After the incubation, membranes were washed and incubated with the appropriate secondary HRP-conjugated anti-rabbit or anti-mouse secondary antibody (Santa Cruz Biotechnology). After 2 h of incubation with secondary antibodies, membranes were washed and used for subsequent detection using an ECL method. Membranes incubated with phosphorylated proteins were stripped and reblotted with antibodies directed against non-phosphorylated forms of the same proteins. All membranes were probed with mouse anti-actin monoclonal antibody (Santa Cruz Biotechnology) and HRP-conjugated secondary antibody as loading control. The signals were quantified using Image J 1.45s software (National Institutes of Health, USA).
Quantitative real-time PCR (qPCR)
According to the manufacturer’s instructions, RNA was extracted from the heart tissue using a Trizol reagent (Life Technologies, USA). RNA purity and concentrations were measured using BioSpec-nano-Spectrophotometer (Shimazu, USA). RNA sample degradation was checked using 1.2% agarose electrophoresis. cDNK was synthesized with commercially available RevertAid H minus First Strand cDNK Synthesis Kit (Thermo Scientific, USA), using 1 µg of heart RNA and following the manufacturer’s instructions. The quantitative polymerase chain reaction (qPCR) assay was conducted using the 7500 Real-Time PCR System (Applied Biosystems) in 96-well reaction plates (MicroAmp Optical, ABI Foster City, CA Each well contained 10 µl of reaction mix (Brilliant III Ultra-Fast SYBR Green) and appropriate sample volume and pairs of primers (forward and reverse) resupplied to total volume of 20 ml with demineralized, RNase-free water. The primers were designed using the Primer Express1 software v2.0 from Applied Biosystems. These are the forward primer 5′-CACGGCCTTCTTTGTCAGTA-3′ and the reverse primer 5′-TTGTTCTTCATTCCCTGCTG-3′ for the α1 subunit of Na+/K+-ATPase (GenBank accession number: NM_031144). Furthermore, the PCR product length for the rat β-Actin gene (GenBank accession number: NM_031144) was 76 bp, and the forward primer was 5′-CCCTGGCTCCTAGCACCAT-3′, while the reverse primer was 5′-GAGCCACCAATCCACACAGA-3′. The conditions for the α1 subunit of Na+/K+-ATPase were 95 °C for 3 min, which was followed by 40 cycles run for 15 s at 95 °C and 32 s at 61 °C. Once the reaction ended, the 2−ΔΔCt technique was used to analyze the relative quantification of mRNA expression, and the cycle threshold values (Ct) were calculated. Next, the α1 subunit of Na+/K+-ATPase ‘s expression level was adjusted relative to the β-Actin gene found in the same sample.
Statistical analysis
The values were presented as mean ± SEM. Student’s t-test for independent samples and Pearson parametric correlation was used to assess the significance of differences and correlations between groups. Statistical analysis was performed using the SPSS program for Windows (SPSS, Chicago, IL, USA), with p-values < 0.05 considered significant.
Results
Anthropometric and biochemical parameters
The results of anthropometric and biochemical parameters are presented in Table 1. First, we assessed the effects of IGF-1 treatment on body mass, heart mass, body mass differential, and heart/body mass ratio. After bolus injection of IGF-1, there was no significant change in body and heart mass, body mass differential, or heart/body mass ratio as compared to control animals. Following the IGF-1 treatment, we assessed IGF-1 concentration in rat serum 24 h after the bolus injection. The results show that IGF-1 concentrations in the serum of IGF-1-treated animals were higher than in control rats (p < 0.01).
In vivo effects of IGF-1 on rat cardiac Na+/K+-ATPase activity and expression
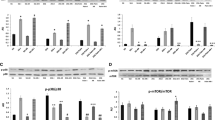
To deepen our comprehension of the in vivo impact of IGF-1 on the Na+/K+-ATPase regulation, we evaluated the activity, protein phosphorylation, and protein expression of the cardiac Na+/K+-ATPase subunits. First, we looked at the dynamic characteristics of cardiac Na+/K+-ATPase: activity and subunit phosphorylation. IGF-1 treatment significantly increased Na+/K+-ATPase activity (p < 0.05) (Fig. 1a), and the ratio p-α Na+/K+-ATPase (Ser23)/total α1 Na+/K+-ATPase (p < 0.05) (Fig. 1b). We examined Na+/K+-ATPase subunits α1 and α2 protein expression in the cardiac plasma membrane extract. IGF-1-treated rats had significantly higher protein expression of α1 and α2 Na+/K+-ATPase subunits (p < 0.01 and p < 0.05, respectively) in their hearts compared to control rats (Fig. 1c and d). To further understand how IGF-1 regulates Na+/K+-ATPase, we investigated the mRNA expression of the α1 subunit in rat hearts. IGF-1 therapy significantly raised the expression of α1 subunit mRNA in rat hearts compared to control rats by 5.6 fold (p < 0.001) (Fig. 1e).
Effects of IGF-1 on Na+/K+-ATPase activity and expression. (a) Specific activities of Na+/K+-ATPase are expressed in mmol Pi/h/mg of protein and represent mean ± SEM. (b) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents Na+/K+-ATPase phosphorylated on Ser23 (p-α Na+/K+-ATPase) as fold changes vs. total α1 Na+/K+-ATPase (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (c) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents α1 Na+/K+-ATPase protein level as fold increase vs. control (CONT: arbitrarily net at 1), and the x-axis represents treatment. Inserts: representative western blots. (d) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents α2 Na+/K+-ATPase protein level as fold increase vs. control (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (e) mRNA expression of α1 subunit of Na+/K+-ATPase. The results for phosphorylation and expression are expressed as a percentage of the value obtained for the control. CONT-control group, IGF-1 - IGF-1-treated group, Na+/K+-ATP-ase - sodium/potassium adenosine triphosphatase, *p < 0.05, **p < 0.01, ***p < 0.001
In vivo effects of IGF-1 on IRS-1, PDK-1, and Akt phosphorylation in rat heart
The following experiments were conducted to evaluate the role of the IRS-1/PDK-1/Akt signalling pathway in IGF-1-regulated Na+/K+-ATPase. IGF-1 treatment resulted in enhanced IRS-1 phosphorylation on Tyr1222 (p < 0.01) and decreased IRS-1 phosphorylation on Ser307 (p < 0.01) (Fig. 2a and b). Additionally, IGF-1 treatment significantly elevated PDK-1 phosphorylation on Ser241 (p < 0.05) and Akt phosphorylation on Ser473 (p < 0.05) compared to the control group (Fig. 3a and b).
Effects of IGF-1 on the phosphorylation of IRS-1 on Tyr1222 and Ser307 (a) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents IRS-1 phosphorylated on Tyr1222 as fold changes vs. total IRS-1 (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (b) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents IRS-1 phosphorylated on Ser307 as fold changes vs. total IRS-1 (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. The results for phosphorylation and expression are expressed as a percentage of the value obtained for the control. CONT-control group, IGF-1 - Insulin-like growth factor 1-treated group, IRS-1 - Insulin receptor substrate – 1, Tyr-tyrosine, Ser-serine, *p < 0.05, **p < 0.01
Effects of IGF-1 on the phosphorylation of PDK1 on Thr421/Ser241 and Akt on Ser473 in cell lysates of rat heart (a) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents PDK-1 phosphorylated on Thr421/Ser241 as fold changes vs. total PDK-1 (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (b) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents Akt phosphorylated on Ser473 as fold changes vs. total Akt (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. The results for phosphorylation and expression are expressed as a percentage of the value obtained for the control. CONT-control group, IGF-1 - Insulin-like growth factor 1-treated group, Akt – protein kinase B, Thr-threonine, Ser-serine, *p < 0.05
IGF-1 effects on mTOR and S6K phosphorylation in the rat heart
The study also investigated the mTOR involvement in Na+/K+-ATPase regulation by IGF-1 through the phosphorylation of mTOR on Ser2481 and Ser2448. IGF-1 treatment significantly elevated mTOR phosphorylation on Ser2448 (p < 0.01) and Ser2481 (p < 0.05) (Fig. 4a and b). Furthermore, our study showed that IGF-1 increased the degree of S6K (Thr421/Ser424) phosphorylation (p < 0.05) in rat cardiac lysate compared to non-treated control rats (Fig. 4c).
Effects of IGF-1 on the phosphorylation of mTOR on Ser2448and Ser2481 and S6K on Thr421/Ser424. (a) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents mTOR phosphorylated on Ser2448 as fold changes vs. total mTOR (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (b) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents mTOR phosphorylated on Ser2481 as fold changes vs. total mTOR (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. (c) Western blot densitometry results (each bar is mean ± SEM). The y-axis represents S6K kinase phosphorylated on Thr421/Ser424 as fold changes vs. total S6K (CONT: arbitrarily set at 1), and the x-axis represents treatment. Inserts: representative western blots. The results for phosphorylation and expression are expressed as a percentage of the value obtained for the control. CONT-control group, IGF-1 – Insulin-like growth factor 1-treated group, mTOR - Mammalian target of rapamycin, S6K - ribosomal protein p70 S6 kinase, Thr-threonine, Ser-serine, *p < 0.05, **p < 0.01
Correlation between the concentration of IGF-1 in serum with Na+/K+-ATPase activity and phosphorylation of mTOR on Ser2448
A correlation has been noted between the serum IGF-1 concentration and the Na+/K+-ATPase activity and phosphorylation of mTOR (Fig. 5). The Na+/K+-ATPase activity shows a significant (p < 0.05) correlation (r = + 0.607) with the concentration of IGF-1 in serum (Fig. 5a). The concentration of IGF-1 and mTOR phosphorylation on Ser2448 show a significant positive correlation (r = + 0.646, p < 0.05) (Fig. 5b).
Correlation between the concentration of IGF-1 in serum with Na+/K+-ATPase activity and phosphorylation of mTOR (a) Correlation between the concentration of IGF-1 in serum and Na+/K+-ATPase activity. (b) Correlation between the concentration of IGF-1 and changes in phosphorylation of mTOR on Ser2448. IGF-1 – Insulin-like growth factor-1, Na+/K+-ATP-ase - sodium/potassium adenosine triphosphatase, mTOR - Mammalian target of rapamycin, Ser-serine
Correlation between the activity of Na+/K+-ATPase with phosphorylation of IRS-1 and mTOR
A significant correlation (r = + 0.712, p < 0.05) was detected between Na+/K+-ATPase activity and IRS-1 phosphorylation on Tyr1222 (Fig. 6a). Furthermore, we observed a significant (p < 0.01) positive correlation (r = + 0.841) between Na+/K+-ATPase activity and phosphorylation of mTOR on Ser2448 (Fig. 6b).
Correlation between the activity of Na+/K+-ATPase with phosphorylation of IRS-1 and mTOR. (a) Correlation between the activity of Na+/K+-ATPase and phosphorylation of IRS-1 on Tyr1222. (b) Correlation between the Na+/K+-ATPase activity and phosphorylation of mTOR on Ser2448. IRS-1 - Insulin receptor substrate – 1, Na+/K+-ATP-ase - sodium/potassium adenosine triphosphatase, mTOR - Mammalian target of rapamycin, Tyr-tyrosine, Ser-serine
Discussion
It is well documented that IGF-1, produced locally by cardiomyocytes, exerts a key physiological role in the heart via multiple processes that promote cardiomyocyte survival and proliferation [1]. One of the important actions of IGF-1 includes the simulative effects on Na+/K+-ATPase function that was established in vitro [12, 17, 18]. IGF-1 has been demonstrated to stimulate Na+/K+-ATPase activity in VSMC in vitro [18], implying that locally produced IGF-1 has a vasodilatory role via autocrine/paracrine activities [23]. Literature data indicate that IGF-1 enhances blood circulation by acting as a vasodilator [1, 23].
The IGF-1 produced locally can function as an autocrine and/or paracrine agent, promoting vasodilation through activation of Na+/K+-ATPase, which elevates the Na+ gradient across the membrane, leading to Ca2+ efflux via Na+/Ca2+ exchange [24, 25]. Alterations in the transcriptional and translational profiles of Na+/K+-ATPase isoforms have been documented in numerous tissues in response to diverse agonists and disease conditions [9, 26]. The IGF-1 was reported to selectively induce the α1 isoform in astrocytes [27], an effect that tyrosine kinase inhibitors could block. Different hormones regulate Na+/K+-ATPase activity, stimulating cardiomyocytes’ function [28]. The literature data regarding the effect of IGF-1 on different subunits’ expression of the Na+/K+-ATPase in the heart is limited. Most studies mainly explore the α1 subunit expression or activity of Na+/K+-ATPase under IGF-1 treatment [12, 17, 18]. However, the current study detected a significant increase in α1 protein and mRNA and α2 protein expression in IGF-1-treated rats. In addition, we found that the concentration of IGF-1 in serum increases in IGF-1-treated rats, which positively correlated with Na+/K+-ATPase activity. Our results also showed that treating rats with IGF-1 increases cardiac Na+/K+-ATPase activity and phosphorylation of the α subunit of Na+/K+-ATPase on Ser23. These results align with in vitro studies where IGF-1 positively affects the expression and activity of Na+/K+-ATPase [12, 17, 18]. In addition, oral administration of IGF-1 (3.5 mg/kg/day for 4 days) increases Na+/K+-ATPase activity in the enterocytes of pigs [29]. Our results indicate that IGF-1 stimulates not only Na+/K+-ATPase activity present on the plasma membrane but also increases the number of available Na+/K+-ATPase molecules since phosphorylation of α1 subunit of Na+/K+-ATPase on Ser23 stimulates subunit trafficking from intracellular compartments to the plasma membrane [30]. Furthermore, two separate investigations examined the impact of IGF-1 on the regulation of Na+/K+-ATPase and observed stimulatory effects of IGF-1 on Na+/K+-ATPase activity in salmon gills [31, 32]. Additionally, Shimomura et al. discovered a positive correlation between serum IGF-1 levels and Na+/K+-ATPase activity in the gills of non-treated salmon [32], a similar correlation observed in our study.
The stimulative effects of IGF-1 in the heart are mediated via multiple signalling pathways, whereas IRS/PI3K/Akt is one of the significant pathways [1, 33]. The binding of IGF-1 to one of the IGF receptors at the plasma membrane leads to receptor autophosphorylation, which provides docking sites for IRS-1 molecules [11]. Further, phosphorylated IRS-1 initiates PI3K/Akt phosphorylation and activation of downstream signalling molecules mTOR/S6K [1]. The IRS molecules have multiple phosphorylation sites of serine, threonine, and tyrosine residues, that when phosphorylated lead to IRS activation or deactivation [34]. The IRS-1 phosphorylation on Ser307 leads to its inhibition and has an essential role in insulin resistance development [35], and IRS-1 phosphorylation on Tyr1222 provides its activation [36]. Our results showed decreased phosphorylation of IRS-1 on Ser307 and increased phosphorylation on Tyr1222 in the hearts of IGF-1-treated rats. In addition, our results show that the activity of Na+/K+-ATPase is positively correlated with stimulative phosphorylation sites of IRS-1 on Tyr1222, implying the involvement of IRS-1 in IGF-1 regulation of the Na+/K+-ATPase activity.
Activated IRS-1 acts as a protein scaffold for the recruitment and activation of downstream proteins such as PI3K/Akt [37]. Considering its significant role, Akt is tightly regulated by several phosphorylation sites, whereas phosphorylation on Ser473 is required for its maximal activation [38, 39]. Kim and Park have reported that IGF-1 induces Akt phosphorylation in human neuroblastoma cells exposed to highly potent and selective PDK-1 inhibitors [40]. This aligns with our results showing that IGF-1 treatment increased PDK-1 phosphorylation on Ser241 in rat hearts. Also, according to Hart and Vogt’s study [38], phosphorylation of Akt was increased in endothelial cells after stimulation with IGF-1 (50 ng/ml). Following treatment with IGF-1 at a concentration of 100 nM, our earlier research demonstrated that VSMC exhibited elevated levels of Akt phosphorylation on Ser473 and Na+/K+-ATPase activity [12]. Also, we have previously shown that IRS/PI3K/Akt signalling is involved in the up-regulation of cardiac Na+/K+-ATPase expression/activity of rats treated with estradiol [20]. A recent study showed that elevated levels of Akt phosphorylation lead to increased Na+/K+-ATPase α1 and β1 subunit protein expression in rat models of acute lung injury and alveolar epithelial cells (both in vivo and in vitro) after treatment with maresin conjugates in tissue regeneration 1 [41]. Results of our study are consistent with these results as we showed that IGF-1 treatment increased phosphorylation of Akt on Ser473, simultaneously with increased expression and activity of Na+/K+-ATPase.
The IGF-1-dependent Akt activation was shown to be involved in mTOR stimulation as a master regulator of many cell processes, including cell growth, proliferation and survival [42]. Thus, we further examined the participation of mTOR in IGF-1-induced stimulation of Na+/K+-ATPase. Phosphorylation of multiple sites on mTOR induces its activation under physiological conditions, with Ser2448 and Ser2481 being the most critical sites for kinase activity [43]. Additionally, the phosphorylation of Ser2448 is activated by Akt, while the phosphorylation of Ser2481 is considered an autocatalytic mTOR site [44]. The mTOR phosphorylated on Ser2448 is mainly involved in cell growth and proliferation, while the mTOR phosphorylated on Ser2481 acts as an Akt activator (Ser473 phosphorylation) [45]. Our results showed increased mTOR phosphorylation on both sites, Ser2448 and Ser2481, in the hearts of IGF-1-treated rats, indicating IGF-1-induced stimulation of mTOR. Wang et al. showed that the treatment with L-Tryptophan activated mTOR and enhanced mRNA expression of α1 subunit of Na+/K+-ATPase in intestinal epithelial cells, indicating the involvement of mTOR in Na+/K+-ATPase stimulation [46]. Results of correlation analysis show that the concentration of IGF-1 in serum positively correlates with phosphorylation of mTOR on Ser2448 and that the activity of Na+/K+-ATPase is positively correlated with simulative phosphorylation of mTOR on Ser2448.
To gain more insight into IGF-1 effects on Na+/K+-ATPase, we further analyzed S6K, one of the main mTOR and Akt effectors responsible for protein synthesis [47]. Bakker et al. showed that IGF-1 treatment (1, 10 and 100 ng/ml) dose-dependently increased Akt and S6K phosphorylation in osteocytes, while mTOR inhibitor rapamycin suppressed this IGF-1 stimulatory effects [48]. The same inhibitory effect of rapamycin was shown in a study by Pesce et al. [15], one of the rare studies exploring the involvement of S6K activation on Na+/K+-ATPase regulation. The same authors proposed that the long-term mechanism of regulation of Na+/K+-ATPase by β-adrenergic agonist isoproterenol is mediated via PI3K activation and subsequent downstream activation of mTOR/S6K in alveolar epithelial cells [15]. Results from our study show that IGF-1 treatment leads to increased phosphorylation of S6K in the hearts of rats, which may be at least partially involved in stimulating the expression of Na+/K+-ATPase subunits. The principal new finding of the present study is that the induction of Na+/K+-ATPase by IGF-1 in vivo is mediated by a mechanism that involves IRS/PI3K/PDK/Akt/mTOR/S6K signalling pathway. These data extend our previous finding that IGF-1 stimulate Na+/K+-ATPase activity in vitro in VSMC and that this stimulation is mediated through a pathway involving PI3K [12]. To illustrate our findings, we provide the following model of Na+/K+-ATPase regulation by IGF-1 in the heart in physiological conditions (Fig. 7). The IGF-1 binds to the receptor at the plasma membrane, which induces autophosphorylation and activation. Thus, the activated IGF receptor recruits and activates IRS-1 molecules, which further induces PI3K activation that stimulates downstream molecules PDK-1, Akt, mTOR and S6K, subsequently increasing Na+/K+-ATPase expression and activity in the heart.
Proposed mechanism of the in vivo effects of IGF-1 on Na+/K+-ATPase regulation in rat heart IGF-1 – Insulin-like growth factor-1, IGF-1R- IGF-1 receptor, IRS-1 - Insulin receptor substrate – 1, Y – Tyrosine amino acid, S – Serine amino acid, Na+/K+-ATP-ase - sodium/potassium adenosine triphosphates, PI3K - phosphatidylinositol-3 kinase, Akt - protein kinase B, mTOR - mammalian target of rapamycin, PDK − 1 - phosphoinositide-dependent kinase-1, S6K - ribosomal protein p70 S6 kinase, T – Threonine amino acid, ↑ increase
Conclusion
The present study showed that in vivo treating rats with IGF-1 leads to increased Na+/K+-ATPase activity, phosphorylation of α subunit, and gene and protein expression of α subunits. Our results also indicate the involvement of IRS/PDK-1/Akt/mTOR/S6K pathway in cardiac Na+/K+-ATPase regulation under IGF-1 treatment. The results of this study represent the basis for further studies directed toward clarifying the molecular mechanisms by which IGF-1 affects cardiac Na+/K+-ATPase and for developing new therapeutics in cardiac diseases.
Data availability
The data supporting this study’s findings are available from the corresponding author, [M.O.], upon reasonable request.
Abbreviations
- Akt:
-
protein kinase B
- ATP:
-
adenosine triphosphate
- CVD:
-
cardiovascular disease
- IGF-1:
-
insulin-like growth factor-1
- IGF-1R:
-
insulin-like growth factor-1 receptor
- IR:
-
insulin Receptor
- IRS:
-
insulin receptor substrate
- mTOR:
-
mammalian target of rapamycin
- mRNA:
-
messenger ribonucleic acid
- Na+/K+ATPase:
-
sodium/potassium adenosine triphosphatase
- PCR:
-
polymerase chain reaction
- PDK-1:
-
phosphoinositide-dependent kinase-1
- PI3K:
-
phosphatidylinositol-3 kinase
- S6K:
-
ribosomal protein p70 S6 kinase
- VSMC:
-
vascular smooth muscle cells
References
Higashi Y, Gautam S, Delafontaine P, Sukhanov S (2019) IGF-1 and cardiovascular disease. Growth Horm IGF Res 456 – 16. https://doi.org/10.1016/j.ghir.2019.01.002
Lin M, Liu X, Zheng H, Huang X, Wu Y, Huang A, Zhu H, Hu Y, Mai W, Huang Y (2020) IGF-1 enhances BMSC viability, migration, and anti-apoptosis in myocardial infarction via secreted frizzled-related protein 2 pathway. Stem Cell Res Ther 11(1):1–16. https://doi.org/10.1186/s13287-019-1544-y
Nederlof R, Reidel S, Spychala A, Gödecke S, Heinen A, Lautwein T, Petzsch P, Köhrer K, Gödecke A (2022) Insulin-like growth factor 1 attenuates the pro-inflammatory phenotype of neutrophils in myocardial infarction. Front Immunol 13908023. https://doi.org/10.3389/fimmu.2022.908023
Higashi Y, Quevedo HC, Tiwari S, Sukhanov S, Shai S-Y, Anwar A, Delafontaine P (2014) Interaction between insulin-like growth factor-1 and atherosclerosis and vascular aging. Front Horm Res 43:107–124. https://doi.org/10.1159/000360571
Higashi Y, Sukhanov S, Shai S-Y, Danchuk S, Snarski P, Li Z, Hou X, Hamblin MH, Woods TC, Wang M (2020) Endothelial deficiency of insulin-like growth factor-1 receptor reduces endothelial barrier function and promotes atherosclerosis in apoe-deficient mice. Am J Physiol Heart Circ Physiol 319(4):H730–H743. https://doi.org/10.1152/ajpheart.00064.2020
Clausen MV, Hilbers F, Poulsen H (2017) The structure and function of the Na,K-ATPase isoforms in Health and Disease. Front Physiol 8:371. https://doi.org/10.3389/fphys.2017.00371
Meyer MJ, Ottolia M, Bers DM, Blaustein MP, Boguslavskyi A, Bossuyt J, Bridge JH, Chen-Izu Y, Clancy CE, Edwards A (2015) Na+/Ca2 + exchange and Na+/K+‐ATPase in the heart. J Physiol 593(6):1361–1382. https://doi.org/10.1113/jphysiol.2014.282319
Meyer DJ, Bijlani S, de Sautu M, Spontarelli K, Young VC, Gatto C, Artigas P (2020) FXYD protein isoforms differentially modulate human Na/K pump function. J Gen Physiol 152(12):e202012660. https://doi.org/10.1085/jgp.202012660
Obradovic M, Sudar-Milovanovic E, Gluvic Z, Banjac K, Rizzo M, Isenovic ER (2023) The na(+)/K(+)-ATPase: a potential therapeutic target in cardiometabolic diseases. Front Endocrinol (Lausanne) 141150171. https://doi.org/10.3389/fendo.2023.1150171
Cai W, Sakaguchi M, Kleinridders A, Gonzalez-Del Pino G, Dreyfuss JM, O’Neill BT, Ramirez AK, Pan H, Winnay JN, Boucher J, Eck MJ, Kahn CR (2017) Domain-dependent effects of insulin and IGF-1 receptors on signalling and gene expression. Nat Commun 8:14892. https://doi.org/10.1038/ncomms14892
Hakuno F, Takahashi S-I (2018) 40 years of IGF1: IGF1 receptor signaling pathways. J Mol Endocrinol 61(1):T69–T86. https://doi.org/10.1530/JME-17-0311
Isenovic ER, Meng Y, Jamali N, Milivojevic N, Sowers JR (2004) Ang II attenuates IGF-1-stimulated Na+, K+-ATPase activity via PI3K/Akt pathway in vascular smooth muscle cells. Int J Mol Med 13(6):915–922. https://doi.org/10.3892/ijmm.13.6.915
Wang X-W, Yuan L-J, Yang Y, Zhang M, Chen W-F (2020) IGF-1 inhibits MPTP/MPP+-induced autophagy on dopaminergic neurons through the IGF-1R/PI3K-Akt-mTOR pathway and GPER. Am J Physiol Endocrinol Metab 319(4):E734–E743. https://doi.org/10.1152/ajpendo.00071.2020
Bibollet-Bahena O, Almazan G (2009) IGF-1-stimulated protein synthesis in oligodendrocyte progenitors requires PI3K/mTOR/Akt and MEK/ERK pathways. J Neurochem 109(5):1440–1451. https://doi.org/10.1111/j.1471-4159.2009.06071.x
Pesce L, Comellas A, Sznajder JI (2003) β-Adrenergic agonists regulate Na-K-ATPase via p70S6k. Am J Physiol Lung Cell Mol Physiol 285(4):L802–L807. https://doi.org/10.1152/ajplung.00266.2002
Obradovic M, Zafirovic S, Soskic S, Stanimirovic J, Trpkovic A, Jevremovic D, Isenovic ER (2019) Effects of IGF-1 on the Cardiovascular System. Curr Pharm Des 25(35):3715–3725. https://doi.org/10.2174/1381612825666191106091507
Li D, Sweeney G, Wang Q, Klip A (1999) Participation of PI3K and atypical PKC in Na+-K+-pump stimulation by IGF-I in VSMC. Am J Physiol 276(6):H2109–H2116. https://doi.org/10.1152/ajpheart.1999.276.6.H2109
Standley PR, Zhang F, Zayas RM, Muniyappa R, Walsh MF, Cragoe E, Sowers JR (1997) IGF-I regulation of na(+)-K(+)-ATPase in rat arterial smooth muscle. Am J Physiol 273(1 Pt 1):E113–E121. https://doi.org/10.1152/ajpendo.1997.273.1.E113
Kanno Y, Mitsui T, Kitta T, Moriya K, Tsukiyama T, Hatakeyama S, Nonomura K (2016) The inflammatory cytokine IL-1β is involved in bladder remodeling after bladder outlet obstruction in mice. Neurourol Urodyn 35(3):377–381. https://doi.org/10.1002/nau.22721
Obradovic M, Stewart AJ, Pitt SJ, Labudovic-Borovic M, Sudar E, Petrovic V, Zafirovic S, Maravic-Stojkovic V, Vasic V, Isenovic ER (2014) In vivo effects of 17β-estradiol on cardiac na(+)/K(+)-ATPase expression and activity in rat heart. Mol Cell Endocrinol 388(1–2):58–68. https://doi.org/10.1016/j.mce.2014.03.005
Luiken JJ, Koonen DP, Willems J, Zorzano A, Becker C, Fischer Y, Tandon NN, Van Der Vusse GJ, Bonen A, Glatz JF (2002) Insulin stimulates long-chain fatty acid utilization by rat cardiac myocytes through cellular redistribution of FAT/CD36. Diabetes 51(10):3113–3119. https://doi.org/10.2337/diabetes.51.10.3113
Baricevic-Jones I, Nedić O, Nikolić J, Nedeljković J (2004) The insulin-like growth factor system in the circulation of patients with viral infections. Clin Chem Lab Med 42(10):1127–1131. https://doi.org/10.1515/CCLM.2004.231
Sowers JR (1997) Insulin and insulin-like growth factor in normal and pathological cardiovascular physiology. Hypertension 29(3):691–699. https://doi.org/10.1161/01.hyp.29.3.691
Singh T, Garg S, Mishra S (2012) Evaluation of effects of eicosapentaenoic acid on Na+-K+-ATPase in sheep pulmonary artery. Hum Exp Toxicol 31(6):579–587. https://doi.org/10.1177/0960327111417909
Sowers JR (1996) Effects of insulin and IGF-I on vascular smooth muscle glucose and cation metabolism. Diabetes 45. https://doi.org/10.2337/diab.45.3.s47. Suppl 3S47-51
Therien AG, Blostein R (2000) Mechanisms of sodium pump regulation. Am J Physiol Cell Physiol 279(3):C541–C566. https://doi.org/10.1152/ajpcell.2000.279.3.C541
Matsuda T, Murata Y, Kawamura N, Hayashi M, Tamada K, Takuma K, Maeda S, Baba A (1993) Selective induction of alpha 1 isoform of (na + + K+)-ATPase by insulin/insulin-like growth factor-I in cultured rat astrocytes. Arch Biochem Biophys 307(1):175–182. https://doi.org/10.1006/abbi.1993.1576
Pirkmajer S, Chibalin AV (2019) Chapter ten - hormonal regulation of Na+-K+-ATPase from the evolutionary perspective Curr Top Membr. 83:315–351. https://doi.org/10.1016/bs.ctm.2019.01.009
Alexander AN, Carey HV (2001) Involvement of PI 3-kinase in IGF-I stimulation of jejunal Na+-K+-ATPase activity and nutrient absorption. Am J Physiol Gastrointest Liver Physiol 280(2):G222–G228. https://doi.org/10.1152/ajpgi.2001.280.2.G222
Massey Katherine J, Li Q, Rossi Noreen F, Mattingly Raymond R, Yingst Douglas R (2012) Angiotensin II-dependent phosphorylation at Ser11/Ser18 and Ser938 shifts the E2 conformations of rat kidney Na+/K+-ATPase. Biochem J 443(1):249–258. https://doi.org/10.1042/bj20111398
McCormick SD (1996) Effects of Growth hormone and insulin-like growth factor I on Salinity Tolerance and Gill Na+, K+-ATPase in Atlantic Salmon (Salmo salar): Interaction with Cortisol. Gen Comp Endocrinol 101(1):3–11. https://doi.org/10.1006/gcen.1996.0002
Shimomura T, Nakajima T, Horikoshi M, Iijima A, Urabe H, Mizuno S, Hiramatsu N, Hara A, Shimizu M (2012) Relationships between Gill Na+,K+-ATPase activity and endocrine and local insulin-like growth factor-I levels during smoltification of masu salmon (Oncorhynchus masou). Gen Comp Endocrinol 178(2):427–435. https://doi.org/10.1016/j.ygcen.2012.06.011
del Díaz S, Benaouicha M, Muñoz-Chápuli R, Carmona R (2022) The insulin-like growth factor signalling pathway in Cardiac Development and Regeneration. Int J Mol Sci 23(1):234. https://doi.org/10.3390/ijms23010234
Peng J, He L (2018) IRS posttranslational modifications in regulating insulin signaling. J Mol Endocrinol 60(1):R1–R8. https://doi.org/10.1530/JME-17-0151
Liu Z, Patil IY, Jiang T, Sancheti H, Walsh JP, Stiles BL, Yin F, Cadenas E (2015) High-Fat Diet induces hepatic insulin resistance and impairment of synaptic plasticity. PLoS ONE 10(5):e0128274. https://doi.org/10.1371/journal.pone.0128274
Wu J, Wu D, Zhang L, Lin C, Liao J, Xie R, Li Z, Wu S, Liu A, Hu W, Xi Y, Bu S, Wang F (2019) NK cells induce hepatic ER stress to promote insulin resistance in obesity through osteopontin production. J Leukoc Biol 107(4):589–596. https://doi.org/10.1002/jlb.3ma1119-173r
Zheng M, Wang P (2021) Role of insulin receptor substance-1 modulating PI3K/Akt insulin signaling pathway in Alzheimer’s disease. 3 Biotech 11(4):179. https://doi.org/10.1007/s13205-021-02738-3
Hart JR, Vogt PK (2011) Phosphorylation of AKT: a mutational analysis. Oncotarget 2(6):467–476. https://doi.org/10.18632/oncotarget.293
Partovian C, Simons M (2004) Regulation of protein kinase B/Akt activity and Ser473 phosphorylation by protein kinase Cα in endothelial cells. Cell Signal 16(8):951–957. https://doi.org/10.1016/j.cellsig.2004.01.008
Kim C, Park S (2018) IGF-1 protects SH-SY5Y cells against MPP+-induced apoptosis via PI3K/PDK-1/Akt pathway. Endocr Connect 7(3):443–455. https://doi.org/10.1530/ec-17-0350
Han J, Li H, Bhandari S, Cao F, Wang X-Y, Tian C, Li X-Y, Zhang P-H, Liu Y-J, Wu C-H, Smith FG, Jin S-W, Hao Y (2020) Maresin conjugates in tissue regeneration 1 improves alveolar fluid clearance by up-regulating alveolar ENaC, na, K-ATPase in lipopolysaccharide-induced acute lung injury. J Cell Mol Med 24(8):4736–4747. https://doi.org/10.1111/jcmm.15146
Saxton RA, Sabatini DM (2017) mTOR Signaling in Growth, Metabolism, and Disease. Cell 168(6):960–976. https://doi.org/10.1016/j.cell.2017.02.004
Fletcher L, Evans TM, Watts LT, Jimenez DF, Digicaylioglu M (2013) Rapamycin treatment improves neuron viability in an in vitro model of stroke. PLoS ONE 8(7):e68281. https://doi.org/10.1371/journal.pone.0068281
Wataya-Kaneda M (2015) Mammalian target of rapamycin and tuberous sclerosis complex. J Dermatol Sci 79(2):93–100. https://doi.org/10.1016/j.jdermsci.2015.04.005
Garling RJ, Watts LT, Sprague S, Digicaylioglu M (2018) Progesterone modulates mTOR in the hippocampus of mice after traumatic brain injury. Neural Regen Res 13(3):434–439. https://doi.org/10.4103/1673-5374.228725
Wang H, Ji Y, Wu G, Sun K, Sun Y, Li W, Wang B, He B, Zhang Q, Dai Z, Wu Z (2015) L-Tryptophan activates mammalian target of Rapamycin and enhances expression of tight Junction proteins in Intestinal Porcine Epithelial cells. J Nutr 145(6):1156–1162. https://doi.org/10.3945/jn.114.209817
Morita M, Gravel S-P, Hulea L, Larsson O, Pollak M, St-Pierre J, Topisirovic I (2015) mTOR coordinates protein synthesis, mitochondrial activity and proliferation. Cell Cycle 14(4):473–480. https://doi.org/10.4161/15384101.2014.991572
Bakker AD, Gakes T, Hogervorst JMA, de Wit GMJ, Klein-Nulend J, Jaspers RT (2016) Mechanical stimulation and IGF-1 enhance mRNA translation rate in osteoblasts Via activation of the AKT-mTOR pathway. J Cell Physiol 231(6):1283–1290. https://doi.org/10.1002/jcp.25228
Acknowledgements
This work is part of the collaboration between the Department of Radiobiology and Molecular Genetics, “VINČA” Institute of Nuclear Sciences - National Institute of the Republic of Serbia, University of Belgrade, Belgrade, Serbia and Computational Bioscience Research Center (CBRC), King Abdullah University of Science and Technology (KAUST), Thuwal 23955-6900, Kingdom of Saudi Arabia.
Funding
This work was funded by the Ministry of Science Technological Development and Innovation of the Republic of Serbia (Contract No#451-03-66/2024-03/200017) KAUST grant OSR#4129 (awarded to E.R.I).
Author information
Authors and Affiliations
Contributions
Conception and supervision: M.O. and E.R.I.Performed the research: K.B., M.O., S.Z., and M.S.Interpretation or analysis of data: K.B., M.O., S.Z., Z.G. and E.R.I.Preparation of the manuscript: K.B., M.O., S.Z., M.E., Z.G., O.N. and E.R.I.All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Ethical approval
The official Vinca Institute’s Ethical Committee for Experimental Animals approved experimental protocols (Veterinary Directorate – No. 451-03-66/2024-03/ 200017).
Consent to participate
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Banjac, K., Obradovic, M., Zafirovic, S. et al. The involvement of Akt, mTOR, and S6K in the in vivo effect of IGF-1 on the regulation of rat cardiac Na+/K+-ATPase. Mol Biol Rep 51, 517 (2024). https://doi.org/10.1007/s11033-024-09451-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11033-024-09451-3