Abstract
Evidence from the literature indicates that mitochondrial dysfunction occurs in schizophrenia and other psychiatric disorders. To produce an animal model that simulates psychotic symptoms analogous to those seen in schizophrenic patients, sub-anesthetic doses of N-methyl-D-aspartate (NMDA) receptor antagonists (such as ketamine) have been used. The aim of this study was to evaluate behavioral changes and mitochondrial dysfunction in rats administered ketamine for 7 consecutive days. Behavioral evaluation was performed using an activity monitor 1, 3 and 6 h after the last injection. The activities of mitochondrial respiratory chain complexes I, II, I-III and IV in multiple brain regions (prefrontal cortex, striatum and hippocampus) were also evaluated. Our results showed that hyperlocomotion occurred in the ketamine group 1 and 3 h after the last injection. Stereotypic movements were elevated only when animals were evaluated 1 h after receiving ketamine. In addition, we found that ketamine administration affects the respiratory chain, altering the activity of respiratory chain complexes in the striatum and hippocampus after 1 h, those in the prefrontal cortex and hippocampus after 3 h and those in the prefrontal cortex and striatum 6 h after the last administration of ketamine. These findings suggest that ketamine alters the behavior of rats and changes the activity of respiratory chain complexes in multiple brain regions at different time points.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Schizophrenia is a heterogeneous neuropsychiatric disorder that consists of positive symptoms (delusions and hallucinations), negative symptoms (blunted affect and social withdrawal) and cognitive impairments (Bowie and Harvey 2006). It typically manifests in adolescence or early adulthood and continues to produce symptoms to varying degrees throughout the patient’s lifetime (Tien and Eaton 1992). The estimated prevalence of this disease is 1.0–1.5% of the world population, and only half of those patients are likely to obtain treatment (De Padua et al. 2005).
The complete pathophysiology of schizophrenia remains unknown, but it is clear that anatomical and biochemical brain alterations are present during its genesis (Swerdlow et al. 1998). The disorder usually appears due to a combination of genetic and environmental factors, such as neurodevelopment, environmental stresses/stimuli and the age at which such stimuli are received, resulting in a complex nervous disorder (Farber et al. 1995; Lewis and Lieberman 2000). The clinical manifestations of schizophrenia include delusions, hallucinations and agitation, which are caused by changes in sensory perception; as well as cognitive impairments such as difficulties in attention, memory and behavior, which interfere with interpersonal relationships and work. Lack of motivation, social isolation, blunted affect, impulsivity and a low sense of responsibility may be involved in this disorder, creating a negative impact on the patient’s quality of life (Bowie and Harvey 2006; Robertson et al. 2006).
Previous studies have demonstrated an imbalance in several neurotransmitter systems in the pathophysiology of schizophrenia (Marcotte et al. 2001; Wood et al. 2009). The dopaminergic system is the oldest pathway studied in schizophrenia, and a hypothesis of dopaminergic hyperfunction has arisen wherein the positive symptoms (delusions and hallucinations) are triggered by the increased occupancy of D2 receptors by dopamine (Bressan and Pilowsky 2003). This theory also derives from the fact that the first antipsychotic drugs were dopaminergic antagonists that demonstrated efficacy against the positive symptoms of schizophrenia, as well as against amphetamine-induced psychotic symptoms (dopamine release inducers). It has been observed that the chronic use of antipsychotic drugs is very effective at treating the positive symptoms, but not the negative cognitive and affective symptoms (Meltzer et al. 1989; Meyer 2007; Nikam and Awasthi 2008).
In addition to dopamine, glutamate has been widely studied in schizophrenia because it is well-known as one of the main neurotransmitters involved in its pathophysiology. Among the scientific evidence concerning the involvement of glutamate in the pathophysiology of schizophrenia is the finding of decreased levels of glutamate in the cerebrospinal fluid of schizophrenic patients and the fact that phencyclidine (PCP) and ketamine, two N-methyl-D-aspartate (NMDA) glutamatergic receptor antagonist drugs, cause severe symptoms similar to those observed in schizophrenia (Hitri et al. 1993; Park and Holzman 1992).
Given this clinical and neurobiological diversity, the use of animal models is appropriate for studying intracellular changes and behavior alterations that may be involved in schizophrenia. The NMDA receptor antagonist model is being used as an animal model for schizophrenia, generally by the administration of substances such as PCP and ketamine (Krystal et al. 1994). Ketamine is an anesthetic drug that acts as an antagonist of NMDA. Several reports in the literature indicate that sub-anesthetic doses of ketamine can produce hallucinations and paranoia in humans, effects that are similar to the positive symptoms characteristic of schizophrenia; some reports have also demonstrated that this model reproduces both the positive and negative symptoms of this disorder, as well as its cognitive impairments (Hunt et al. 2006; Littlewood et al. 2006; Takeyama et al. 2006).
Along with the imbalance in neurotransmitter systems, some lines of evidence indicate a role of mitochondrial dysfunction in schizophrenia, which also contributes to neurodegenerative diseases such as Alzheimer’s, Huntington’s and Parkinson’s disease (Di Donato 2000). This is due to the fact that high-energy-demand tissues such as the brain contain a greater number of mitochondria and therefore are more vulnerable to energy metabolism impairment (Boekema and Braun 2007). In this context, Reddy (2008, 2009) has already shown that mitochondria are an important target in the treatment of Alzheimer’s and other neurodegenerative diseases.
Mitochondria are responsible for several essential processes in the development and normal function of the body, including energy production, apoptosis, and the generation of reactive oxygen species. Therefore, mitochondrial dysfunction can lead to a failure in one or more of these factors and thus to abnormal cellular activity or death (Ben-Shachar 2002).
Mitochondrial pathology resulting from biochemical cascade dysfunction and the associated damage to the electron transport chain has been suggested to be an important factor in the pathogenesis of a range of neuropsychiatric disorders such as bipolar disorder, depression and schizophrenia (Fattal et al. 2006; Rezin et al. 2008).
Considering that mitochondrial dysfunction may be involved in the pathophysiology of neuropsychiatric disorders, this study aimed to induce a chronic animal model of schizophrenia in order to assess both the mitochondrial respiratory chain and the resulting behavioral changes.
Materials and methods
This study was approved by the Ethics Committee (Ethics Committee in Animal usage of the Universidade do Extremo Sul Catarinense), and it was performed in accordance with the Brazilian Society for Neuroscience and Behavior’s (SBNeC) recommendations for animal care.
Animals
Adult male Wistar rats weighing 250–300 g were obtained from our breeding colony. The animals were housed five to a cage with food and water available ad libitum and were maintained on a 12-h light/dark cycle (lights on at 7:00 am).
Animal model of schizophrenia
Symptoms of schizophrenia were induced by chronic sub-anesthetic doses of 25 mg/kg of ketamine (Hunt et al. 2006; Van Den Buuse et al. 2005). Ketamine was administered once a day over seven consecutive days. The animals were evaluated on the 7th day of treatment using the behavioral tests described below and were divided into 4 groups: control (saline); 1, 3 and 6 h after the last injection. With this chronic treatment we hoped to observe whether the animals have cellular alterations even when their behavior has returned to normal.
The rats were killed by decapitation after the behavioral evaluation, and brain structures such as the prefrontal cortex, striatum and hippocampus were dissected and rapidly frozen at −80°C until the biochemical analysis. The animals were evaluated at three times (1, 3 and 6 h) (Fig. 1); each time included two groups of 10 animals each (Table 1).
Behavioral evaluation
Open-field task
The open-field evaluation was performed in a 50 × 25 × 50 cm arena. Locomotor activity was measured for 60 min using a computerized system (Activity Monitor—Insight laboratory equipment, Ribeirão Preto, SP). This equipment monitored locomotor activity via the distance traveled (cm) by the animal, dividing the evaluation time into blocks of 5 min. Locomotor activity was constantly monitored by a system installed in the arena containing six parallel bars, each of which contained 16 infrared sensors that detect the rat’s exact position and movement, enabling a detailed analysis of each animal’s behavior. Information detected by the sensors is transmitted to a computer in which the animal’s activity is recorded each 5 min by a dedicated program (database: Open Source version Interbase 6.01). The distance covered by the animal is considered to be the sum of the changes in position monitored by the activity arena; the software calculates the distance between two locations, plus the previously traveled distances.
Stereotypy
Stereotypy is defined as rapid, repetitive, forward movements (Battisti et al. 2000; Krystal et al. 1994). This parameter was analyzed at the same time and place as hyperlocomotor activity. Stereotypy is considered by the software as an unstable movement any time when repetitive movements are recorded in sequential readings without alterations in the animal’s mass center. The possible units of measurement to be considered are mm (millimeters), cm (centimeters) and in (inches).
Tissue and homogenate preparation
The animals were killed by decapitation 60 min after the behavioral analyses. Brains were removed and prefrontal cortex, cerebellum, hippocampus, striatum and cerebral cortex were homogenized (1:10, w/v) in SETH buffer, pH 7.4 (250 mM sucrose, 2 mM EDTA, 10 mM Trizma base, 50 IU/ml heparin). Homogenates were centrifuged at 800 × g for 10 min and the supernatants were kept at −70°C until they were used for enzyme activity determination.
Respiratory chain enzyme activity
Complex I, or NADH dehydrogenase, was evaluated using the method described by Cassina and Radi (1996) by the rate of NADH-dependent ferricyanide reduction at λ = 420 nm. Complex II activity was determined by the method described by Fischer and colleagues (1985), and it was measured by following the decrease in absorbance due to the reduction of 2,6-DCIP at λ = 600 nm. Complex I-III activity was measured as cytochrome c reduction from succinate at λ = 550 nm and 37°C according to the method of Birch-Machin and colleagues (1994). The activity of cytochrome c oxidase (complex IV) was assayed according to the method described by Rustin and colleagues (1994), in which the decrease in absorbance due to the oxidation of previously reduced cytochrome c at λ = 550 nm is followed. The activity of the mitochondrial respiratory chain complexes were calculated as nmol/min.mg protein.
Protein content
Protein content was determined by the method described by Lowry and colleagues (1951) using bovine serum albumin as a standard.
Statistical analysis
Data were analyzed by Student’s t-test using the program SPSS (Statistical Package for the Social Sciences). In all comparisons, the statistical significance was set at p < 0.05.
Results
Animals that received ketamine injections for seven consecutive days and were then evaluated at 1 h after the last injection (7th day) presented a significant increase in locomotor activity when compared to animals that received saline. The evaluation period (1 h) was divided into blocks of 5 min, as shown in Fig. 2. Animals in the ketamine group that were evaluated 3 h after the last injection presented a significant increase in locomotor activity in 5 and 15 min of monitoring compared to the saline group. When the locomotor activity of the rats was evaluated 6 h after the last injection, no significant differences were detected between the saline and ketamine groups.
Locomotor activity at 1, 3 and 6 h. Distance traveled (cm) by rats subjected to behavioral evaluation was measured for 60 min using a computerized system (Activity Monitor) following the last ketamine administration. Comparison between the saline and ketamine groups. Bars represent means ± standard deviation (10 animals each group) *p < 0.05 according to Student’s t-test
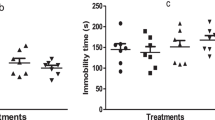
Stereotypic movements were significantly enhanced in the ketamine group rats when evaluated at 1 h; however, no difference was detected between the groups when the animals were evaluated at 3 and 6 h (Fig. 3).
Stereotypic evaluation at 1, 3 and 6 h. The number of stereotypic movements by rats subjected to behavioral evaluation was measured for 60 min using a computerized system (Activity Monitor) following the last ketamine administration. Comparison between the saline and ketamine groups. Bars represent means ± standard deviation (10 animals each group) *p < 0.05 according to Student’s t-test. Stereotypic movements at 1 h (F = 3,252 dF = 18), 3 h (F = 1,34 dF = 8), 6 h (F = 0,05 dF = 18)
In the biochemical assays, we observed in the prefrontal cortex that the activities of the mitochondrial respiratory chain complexes II, I-III and IV did not differ 1 h after the last ketamine administration, while different results were found with complex I, which showed a statistically significant increase. At the same time, in the striatum, the data showed a significant increase in the activities of complexes I, I-III and IV in rats that received ketamine compared to those that received saline. In addition, in the hippocampus, there was a statistically significant increase in the activities of complexes I and IV in animals from the ketamine group. The other complexes of the respiratory chain did not show any changes in this structure at this time (Fig. 4).
Activities of mitochondrial respiratory chain complexes I, II, I-III and IV (nmol/min.mg protein) in brain structures at the 1-h time point. Comparison between the saline and ketamine groups. Bars represent means ± standard deviation (8 animals each group). *p < 0.05 according to Student’s t-test. Striatum: complex I (F = 1,166 dF = 7); complex II (F = 14,973 dF = 8); complex III (F = 3,842 dF = 8); complex IV (F = 4,248 dF = 8). Hippocampus: complex I (F = 3,025 dF = 8); complex II (F = 0,388 dF = 8); complex III (F = 1,613 dF = 8); complex IV (F = 3,782 dF = 10). Prefrontal cortex: complex I (F = 11,177 dF = 8); complex II (F = 4,677 dF = 10); complex III (F = 2,148 dF = 8); complex IV (F = 7,743 dF = 8)
In rats evaluated 3 h after the last ketamine administration, the prefrontal cortex presented a decrease in the activities of complexes I and II in the ketamine group relative to the saline group; however, there was no alteration in the other complexes in this structure. In the striatum, the activity of these complexes remained unchanged, and there was no difference between the groups (Fig. 5). The hippocampus also presented a decrease in the activities of complexes I and II in rats from the ketamine group.
Activities of mitochondrial respiratory chain complexes I, I, II-III and IV (nmol/min.mg protein) in brain structures at 3 h. Comparison between the saline and ketamine groups. Bars represent means ± standard deviation (8 animals each group). *p < 0.05 according to Student’s t-test. Striatum: complex I (F = 0,294 dF = 8); complex II (F = 0,056 dF = 10); complex III (F = 17.281 dF = 10); complex IV (F = 0,192 dF = 10). Hippocampus: complex I (F = 2,171 dF = 8); complex II (F = 8,885 dF = 10); complex III (F = 4,006 dF = 10); complex IV (F = 0,055 dF = 10). Prefrontal cortex: complex I (F = 0,847 dF = 8); complex II (F = 0,648 dF = 10); complex III (F = 0,260 dF = 10); complex IV (F = 0,047 dF = 9)
The evaluation at 6 h after the last ketamine administration indicated a decrease in the activities of complexes I and I-III in the prefrontal cortex and an increase in the activity of complex IV in animals in the ketamine group, while complex II remained unchanged. In both the striatum and the prefrontal cortex, we observed a decrease in the activities of complexes I and I-III in rats treated with ketamine; on the other hand, there was an increase in the activity of complex IV. The activities of complexes II, I-III and IV in the hippocampus were not significantly different between the saline and ketamine groups, although there was a significant decrease in these complexes in both groups (Fig. 6).
Activities of mitochondrial respiratory chain complexes I, II, I-III and IV (nmol/min.mg protein) in brain structures at 6 h. Comparison between the saline and ketamine groups. Bars represent means ± standard deviation (8 animals each group) *p < 0.05 according to Student’s t-test. Striatum: complex I (F = 1,281 dF = 8); complex II (F = 1,267 dF = 10); complex III (F = 1,331 dF = 12); complex IV (F = 7,933 dF = 8). Hippocampus: complex I (F = 3,026 dF = 8); complex II (F = 0,146 dF = 10); complex III (F = 1,778 dF = 14); complex IV (F = 0,565 dF = 10). Prefrontal cortex: complex I (F = 0,143 dF = 8); complex II (F = 2,370 dF = 10); complex III (F = 0,120 dF = 10); complex IV (F = 0,363 dF = 10)
Discussion
It is known that sub-anesthetic doses of ketamine induce schizophrenia-like manifestations. Littlewood and colleagues (2006) demonstrated that acute sub-anesthetic doses of ketamine (10 and 25 mg/kg) produce dose-dependent and specific localized changes in blood-oxygenation-level-dependent regions such as hippocampal, limbic and cortical areas. They also found that rats subjected to a sub-anesthetic dose of 25 mg/kg presented an increase in locomotor activity for up to 1 h and 50 min.
In this study, hyperlocomotion in rats that received ketamine was verified by behavioral evaluation at 1 h after the last injection, as well as in the first 15 min of the evaluation at 3 h after the last injection. Thus, we observed that ketamine-induced locomotor activity was present for up to 3 h and 15 min after the last administration of ketamine.
According to the neurodevelopmental animal model of schizophrenia, the administration of an NMDA receptor antagonist alters the behavior of adult rats. Behavior manifestations in rats that are related to the symptoms and neurobiological markers of this model include aspects such as hyperlocomotion, stereotypy, deficiency in information processing, and impairment of cognitive functions and social interactions (Bubeníková-Valešová 2008; Lipska and Weinberger 2000).
This study showed that stereotypic movements, which are rapid, repetitive, forward movements such as balancing the head and rotational activities, were elevated only in the evaluation at 1 h after the last injection. Ketamine has a relatively short effect that lasts between 20 and 45 min. It is distributed through tissues such as the heart, lungs and brain, and it has an elimination time of 2–3 h (Maxwell 2005). This information may explain the finding that hyperlocomotion was present in the more acute evaluation period, as were the stereotypic movements.
Examination of the post mortem brain tissues of schizophrenic patients has indicated that there are abnormalities in the functionality of the enzyme complexes of the mitochondrial respiratory chain (Maurer and Moller 1997). Mitochondrial dysfunction in schizophrenia includes mitochondrial hypoplasia, dysfunction of the oxidative phosphorylation system and altered mitochondrial-related gene expression (Karry et al. 2004). Abnormal mitochondrial morphology, proportion and density have been observed in the brains of schizophrenic individuals (Ben-Shachar 2002).
These mitochondrial abnormalities of schizophrenia were classified by Ben-Shachar and colleagues (2003) into three categories: mitochondrial morphological aberrations, oxidative phosphorylation dysfunction and genetic abnormalities (Ben-Shachar and Laifenfeld 2003). It is known that ketamine can be used to reproduce an animal model of schizophrenia (Bubeníková-Valešová et al. 2008). One study showed that ketamine administered for 5 days caused changes in dopaminergic, glutamatergic and serotoninergic neurotransmission. These changes produce an increase in the D2 hippocampal receptors, a decrease in glutamatergic receptors in the prefrontal cortex, and increases in the density of dopamine and serotonin transporters in the striatum, hippocampus and prefrontal cortex (Becker et al. 2003).
Our results show that 1 h after the last ketamine injection, the prefrontal cortex presented a change in the activity of complex I. Karry and colleagues (2004) assessed schizophrenic patients and controls in parallel for three parameters, including mRNA and protein levels and enzymatic activity in platelet mitochondria. The results showed a significant correlation among complex I activity and mRNA level, as well as among protein levels of the 24- and 51- kDa subunits in the prefrontal cortex.
Acutely, ketamine produces an increase in positive symptom expression, which may indicate a correlation with increases in complex I. According to these results, Ben-Shachar and colleagues (2007) observed that patients with high positive symptoms demonstrated an increase in complex I within their platelets.
In the striatum, we detected increases in the activities of complexes I and IV in the 1 h- evaluation. A study of postmortem tissue investigating the possibility of brain alterations in schizophrenia also showed that there was mitochondrial dysfunction within the striatum, and it additionally showed that schizophrenic patients presented a decrease in energy metabolism in this structure (Kung and Roberts 1999). We suggest that a compensatory mechanism mediated by respiratory chain complexes I and IV may have been activated to supply the energetic demand in this structure. In the hippocampus, complexes I and IV also showed a significant increase; however, in contrast to this result, Cavelier and colleagues (1995) showed that the activity of complex IV was significantly reduced in postmortem brain tissue, suggesting that this decrease may be due to a specific deficit in the subunits of complex IV or it may reflect a general decrease in mitochondrial capacity in oxidative phosphorylation. We suggest that the enhanced activity of the mitochondrial respiratory chain complexes 1 h after the last administration of ketamine reflects the necessity of increasing the electron transporters to supply the energetic demands of cellular function.
In the prefrontal cortex and hippocampus, the enzymatic activity of complex II at 3 h was significantly lower in the ketamine group than in the saline group. This suggests the possibility that a late effect of the ketamine due to chronic treatment and impairment may have been imparted to these structures. A study using neuroimaging techniques showed a decrease in the volume and number of mitochondria in schizophrenic patients (Uranova et al. 2001). Studies have also indicated that mitochondrial dysfunction may increase levels of calcium, thereby inducing pro-apoptotic stress, and that this dysfunction can also influence the apoptotic mechanisms present in schizophrenia (Karry et al. 2004). Complex I showed a significant increase compared with the control group, which suggests that the effect of ketamine persists in the hippocampus and the prefrontal cortex 3 h after its administration.
Considering that brain energy metabolism is altered in schizophrenia, Duncan and colleagues (1998) demonstrated that ketamine administration at 30 mg/kg increases metabolism, as evidenced by a significant increase of 2-deoxyglucose (2-DG) uptake in some brain areas including the medial prefrontal cortex, frontal cortex, hippocampus, nucleus accumbens and other areas. In this context, Bubber et al. (2010) recently published a paper showing a reduction in enzymes from the tricarboxylic acid cycle but an increase in succinate dehydrogenase (SDH), which is a part of complex II. This finding corroborates our results regarding increased complexes from the respiratory chain, and it suggests that there may be a compensatory effect caused by this primary decrease. Our results showed that in the setting of chronic ketamine administration, energy metabolism remained altered 3 h after the last injection, as evidenced by changes in mitochondrial respiratory chain complexes I and II.
This study showed that 6 h after the last ketamine administration, the prefrontal cortex, striatum and hippocampus showed changes in the transport of electrons in complexes I, I-III and IV. Our results also indicate that in a 6 h-time frame, there was an increase in the activity of complexes I and IV in the prefrontal cortex and striatum. This increased activity of complexes I and IV has been observed in neurodegenerative diseases (Strazielle et al. 2003), acting as a compensatory mechanism to promote cellular and neuronal survival. Some studies have reported changes in certain components of the mitochondrial oxidative phosphorylation system in schizophrenia, such as in the activities of complexes I and I-III in the postmortem brain (Maurer and Moller 1997), the activity of complex IV (Cavelier et al. 1995) and the activity of complex II in the postmortem brain (Prince et al. 1997).
These alterations in the main enzymatic complexes of the mitochondria in schizophrenia may be caused by cellular reactions that result in hypoxia or by primary dysfunction of the mitochondria in schizophrenic patients (Prabakaran et al. 2004).
In conclusion, our results show that the ketamine treatment alters the behavior of animals and changes the activity of the respiratory chain complexes in multiple regions at different times. Chronic administration of ketamine triggers a number of alterations in rats that may be compared to those seen in schizophrenic patients. An animal model can be used to study the alterations and the pathophysiological mechanisms of this disease. However, it is important to conduct further studies aiming to investigate other parameters of energy metabolism that may be involved in the pathogenesis of schizophrenia.
References
Battisti JJ, Shreffler CB, Uretsky NJ, Wallace LJ (2000) NMDA antagonists block expression of sensitization of amphetamine-and apomorphuneinduced stereotypy. Pharmacol Biochem Behav 67:241–246. doi:10.1016/S0091-3057(00)00324-5
Becker A, Peters B, Schroeder H, Mann T, Huether G, Grecksch G (2003) Ketamine-induced changes in rat behavior: a possible animal model of schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry 27:687–700. doi:10.1016/S0278-5846(03)00080-0
Ben-Shachar D (2002) Mitochondrial dysfunction in schizophrenia: a possible linkage to dopamine. J Neurochem 83:1241–1251. doi:10.1046/j.1471-4159.2002.01263
Ben-Shachar D, Laifenfeld D (2003) Mitochondria, synaptic plasticity, and schizophrenia. Int Rev Neurobiol 59:273–296. doi:10.1016/S0074-7742(04)59011-6
Ben-Shachar D, Bonne O, Chisin R, Klein E, Lester H, Aharon-Peretz J et al (2007) Cerebral glucose utilization and platelet mitochondiral complex I activity in schizophrenia: a FDG-PET study. Prog Neupsychopharmacol Biol Psychiatry 31:807–813. doi:10.1016/j.pnpbp.2006.12.025
Birch-Machin MA, Briggs HL, Saborido AA, Bindoff LA, Turnbull DM (1994) An evaluation of the measurement of the activities of complexes I–IV in the respiratory chain of human skeletal muscle mitochondria. Biochem Med Metab Biol 51:35–42. doi:0885-4505/94
Boekema EJ, Braun HP (2007) Supramolecular structure of the mitochondrial oxidative phosphorylation system. J Biol Chem 282:1–4. doi:10.1074/jbc.R600031200
Bowie CR, Harvey PD (2006) Schizophrenia from a neuropsychiatric perspective. Mt Sinai J Med 73:993–998
Bressan RA, Pilowsky LS (2003) Hipótese glutamatérgica da esquizofrenia. Rev Bras Psiq 25:177–183. doi:10.1590/S1516-44462003000300011
Bubber P, Hartounian V, Gibsin GE, Blass JP (2010) Abnormalities in the tricarboxylic acid (TCA) cycle in the brains of schizophrenia patients. Eur Neuropsychopharmacol 21:254–260. doi:10.1016/j.euroneuro.2010.10.007
Bubeníková-Valešová V, Horáček J, Vrajová M, Höschl C (2008) Models of schizophrenia in humans and animals based on inhibition of NMDA receptors. Neurosci Biobehav Rev 38:1014–1023. doi:10.1016/j.neubiorev.2008.03.012
Cassina A, Radi R (1996) Differential inhibitory action of nitric oxide and peroxynitrite on mitochondrial electron transport. Arch Biochem Biophys 328:309–316. doi:10.1006/abbi.1996.0178
Cavelier L, Jazin E, Eriksson I, Prince J, Bave U, Oreland L, Gyllensten U (1995) Decreased cytochrome c oxidase activity and lack of age related accumulation of mtDNA in brain of schizophrenics. Genomics 29:217–228. doi:10.1006/geno.1995.1234
De Padua AC, Gama CS, Lobato MI. Psicofármacos. Artmed POA. 2005.
Di Donato S (2000) Disorders related to mitochondrial membranes: phatology of the respiratory chain and neurodegeneration. J Inheret Metab Dis 23:247–263. doi:10.1023/A:1005684029429
Duncan GE, Leipzig JN, Mailman RB, Lieberman JA (1998) Differential effects of clozapine and haloperidol on ketamine-induced brain metabolic activation. Brain Res 812:65–75. doi:10.1016/S0006-8993(98)00926-3
Farber NB, Wozniak DF, Price MT, Labruyere J, Huss J, Peter HS, Olney JW (1995) Age-specific neurotoxicity in the rat associated with NMDA receptor blockade: potential relevance to schizophrenia? Biol Psychiat 38:788–796. doi:10.1016/0006-3223(95)00046-1
Fattal O, Budur K, Vaughan AJ, Franco K (2006) Review of the literature on major mental disorders in adult patients with mitochondrial diseases. Psychosomat 47:1–7. doi:10.1176/appi.psy.47.1.1
Fischer JC, Ruitenbeek W, Berden JA, Trijbels JM, Veerkamp JH, Stadhouders AM et al (1985) Differential investigation of the capacity of succinate oxidation in human skeletal muscle. Clin Chim Acta 153:23–26
Hitri A, O’Connor DA, Cohen JM, Keuler DJ, Deutsch SI (1993) Differentiation between MK-801-and apomorphine-induced stereotyped behaviors in mice. Clin Neuropharmacol 16:220–236
Hunt MJ, Raynaud B, Garcia R (2006) Ketamine dose-dependently unduces high-frequency oscillations in the nucleus accumbens in freely moving rats. Biol Psychiat 60:1206–1214. doi:10.1016/j.biopsych.2006.01.020
Karry R, Klein E, Ben-Shachar D (2004) Mitochondrial complex I subunits expression is altered in schizophrenia: a postmortem study. Biol Psychiatry 55:676–684. doi:10.1016/j.biopsych.2003.12.012
Krystal JH, Karper LP, Seibyl JP, Freeman GF, Delaney R, Bremner JD (1994) Subanesthetic effects of the noncompetitive NMDA antagonists, ketamine, in humans. Arch Gen Psychiatry 51:199–214
Kung L, Roberts RC (1999) Mitochondrial pathology in human schizophrenic striatum: a postmortem ultrastructural study. Synapse 31:67–75
Lewis DA, Lieberman JA (2000) Catching up on schizophrenia: natural history and neurobiology. Neuron 28:325–334. doi:10.1016/S0896-6273(00)00111-2
Lipska BK, Weinberger DR (2000) To model a psychiatric disorder in animals: schizophrenia as a reality test. Neuropsychopharmacol 23:223–239. doi:10.1038/sj.npp.1395545
Littlewood CL, Jones N, O’Neill MJ, Mitchell SN, Tricklebank M, Williams SCR (2006) Mapping the central effects of ketamine in the rat using pharmacological MRI Psychopharmacol 186:64–81. doi:10.1007/s00213-006-0344-0
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–267
Marcotte ER, Pearson DM, Srivastava LK (2001) Animal models of schizophrenia: a critical review. J Psychiatry Neurosci 26:395–410
Maurer I, Moller HJ (1997) Inhibition of complex I by neuroleptics in normal human brain cortex parallels the extrapyramidal toxicity of neuroleptics. Mol Cell Biochem 174:255–259. doi:10.1023/A:1006872911332
Maurer I, Zierz S, Möller HJ (2001) Evidence for a mitochondrial oxidative phosphorylation defect in brains from patients with schizophrenia. Schizophr Res 48:125–136. doi:10.1016/S0920-9964(00)00075-X
Maxwell JC (2005) Party Drugs: properties, prevalence, patterns and problems. Subst Use Misus 40:1203–1240. doi:10.1081/JA-200066736
Meltzer HY, Bastani B, Ramirez L, Matsubara S (1989) Clozapine: new research on efficacy and mechanism of action. Eur Arch Psychiatry Neurol Sci 238:332–339
Meyer JM (2007) Antipsychotic safety and efficacy concerns. J Clin Psychiatry 68:20–26
Nikam SS, Awasthi AK (2008) Evolution of schizophrenia drugs: a focus on dopaminergic systems. Curr Opin Investig Drugs 9:37–46
Park S, Holzman PS (1992) Schizophrenics show spatial working memory deficits. Arch Gen Psychiatry 49:975–982
Prabakaran S, Swatton JE, Ryan MM, Huffaker SJ, Huang JTJ, Griffin JL (2004) Mitochondrial dysfunction in schizophrenia: evidence for compromised brain metabolism and oxidative stress. Mol Psychiatry 9:684–697. doi:10.1038/sj.mp.4001511
Prince JA, Blennow K, Gottfries CG, Karlsson I, Oreland L (1997) Mitochondrial function in differentially altered in the basal ganglia of chronic schizophrenics. Neuropsychopharmacol 21:372–379. doi:S0893-133X(99)00016-0
Reddy PH (2008) Mitochondrial medicine for aging and neurodegenerative diseases. Neuromolecular Med 10:291–315
Reddy PH (2009) Role of mitochondria in neurodegenerative diseases: mitochondria as a therapeutic target in Alzheimer’s disease. CNS Spectr 14:8–13
Rezin GT, Amboni G, Zugno AI, Quevedo J, Streck EL (2008) Mitchondrial dysfunction and psychiatric disorders. Neurochem Res 34:1021–1029. doi:10.1007/s11064-008-9865-8
Robertson GS, Hori SE, Powell KJ (2006) Schizophrenia: an integrative approach to modelling a complex disorder. J Psyc Neurosci 31:157–167
Rustin P, Chretien D, Bourgeron T, Gérard B, Rötig A, Saudubray JM, Munnich A (1994) Biochemical and molecular investigations in respiratory chain deficiencies. Clin Chim Acta 228:35–51
Strazielle C, Sturchler-Pierrat C, Staufenbiel M, Lalonde R (2003) Regional brain cytochrome oxidase activity in beta-amyloid precursor protein transgenic mice with the Swedish mutation. Neurosc 118:1151–1163. doi:10.1016/S0306-4522(03)00037-X
Swerdlow NR, Bakshi V, Waikar M, Taad N, Geyer MA (1998) Seroquel, clozapine and chlorpromazine restore sensorimotor gating in ketamine-treated rats. Psychopharmacol 140:75–80. doi:10.1007/s002130050741
Takeyama K, Yoshikawa M, Oka T, Kawaguchi M, Suzuki T, Hashimoto A (2006) Ketamine enhances the expression of serine racemase and D-amino acid oxidase mRNAs in rat brain. Eur J Pharmacol 540:82–86. doi:10.1016/j.ejphar.2006.04.021
Tien AY, Eaton WW (1992) Psychopathologic precursors and sociodemographic risk factors for the schizophrenia syndrome. Arch Gen Psychiatry 49:37–46
Uranova N, Orlovskaya D, Vikhreva O, Zimina I, Kolomeets N, Vostrikov V et al (2001) Electron microscopy of oligodendroglia in severe mental illness. Brain Res Bull 55:597–610. doi:10.1016/S0361-9230(01)00528-7
Van Den Buuse M, Garner B, Gogos A, Kusljic S (2005) Importance of animal models in schizophrenia research. Aust N Z J Psychiatry 39:550–557
Wood SJ, Yücel M, Pantelis C, Berk M (2009) Neurobiology of schizophrenia spectrum disorders: the role of oxidative stress. Ann Acad Med Singapore 38:396–401
Acknowledgements
This research was supported by grants from CNPq, Instituto Cérebro e Mente, INCT and UNESC to AIZ, ELS, and JQ (CNPq Research Fellows).
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Oliveira, L., Fraga, D.B., De Luca, R.D. et al. Behavioral changes and mitochondrial dysfunction in a rat model of schizophrenia induced by ketamine. Metab Brain Dis 26, 69–77 (2011). https://doi.org/10.1007/s11011-011-9234-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-011-9234-1