Abstract
Hepatic encephalopathy (HE) is a serious complication of liver failure. HE manifests as a series of neuropsychiatric and neuromuscular symptoms including personality changes, sleep abnormalities, asterixis and muscle rigidity progressing through stupor to coma. The pathophysiologic basis of HE remains unclear. There is general agreement that ammonia plays a key role. In recent years, it has been suggested that oxidative/nitrosative stress constitutes part of the pathophysiologic cascade in HE. Direct evidence for oxidative/nitrosative stress in the pathogenesis of HE has been demonstrated in experimental animal models of acute or chronic liver failure. However, evidence from studies in HE patients is limited. This review summarizes this evidence for a role of oxidative/nitrosative stress in relation to ammonia toxicity and to the pathogenesis of HE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatic encephalopathy (HE) manifests as a series of neuropsychiatric and neuromuscular symptoms and is a serious complication of liver failure. The pathophysiologic basis of HE remains unclear. However, there is general agreement that ammonia plays a key role (Butterworth 2002). Ammonia accumulates in the brain in both acute and chronic liver failure leading to impaired bioenergetics (Kosenko et al. 1994; Rao and Norenberg 2001), altered neurotransmission (Mousseau and Butterworth 1994; Norenberg et al. 1997; Szerb and Butterworth 1992), activation of peripheral benzodiazepine receptors (Desjardins and Butterworth 2002; Norenberg et al. 1997) leading to the synthesis of neurosteroids (Ahboucha et al. 2006) as well as glutamate-mediated excitotoxicity (Hermenegildo et al. 1996; Marcaida et al. 1992) and excessive production of glutamine (Hawkins et al. 1993; Takahashi et al. 1991).
In recent years, oxidative/nitrosative stress has also been suggested to be part of the pathophysiologic cascade in HE. Oxidative stress is a condition in which the production of free radicals is far in excess of their rate of detoxification by endogenous mechanisms (Rao 2002). The brain is absolutely dependent upon oxidative metabolism for cell survival and, being a highly aerobic tissue accounting for 20% of total oxygen consumed by the body, is prone to dysfunction due to oxidative stress.
More than a decade ago, O’Connor and Costell (1990) were among the first to postulate that oxidative stress is implicated in the pathophysiologic mechanisms responsible for HE. They reported that hyperammonemic mice displayed evidence of lipid peroxidation in the brain. Since then, evidence for a role of oxidative stress due to ammonia neurotoxicity has been confirmed from cell culture studies (Norenberg et al. 2007; Murthy et al. 2001; Rama Rao et al. 2003). However, direct evidence for oxidative/nitrosative stress in the pathogenesis of HE in either experimental animal models of liver failure or in material from patients is limited.
This short review will summarize evidence for a role of oxidative/nitrosative stress in relation to the pathogenesis of HE.
Acute liver failure
Several studies described evidence in support of a role of oxidative stress in HE due to acute liver failure (ALF). Selective increases in endothelial nitric oxide synthase (eNOS) mRNA expression in the frontal cortex of rats with ischemic liver failure were described (Sawara et al. 2009) as well as increased nitrite/nitrate and nitric oxide levels in these animals (Jiang et al. 2009a, b) and in other models of ALF (Sathyasaikumar et al. 2007; Master et al. 1999). Increased brain nitric oxide production was also reported in brain tissue from portacaval-shunted rats administered ammonia infusions to precipitate brain edema (Master et al. 1999). Heme oxygenase-1 (HO-1) mRNA expression was shown to be elevated in brain in experimental ALF due to azoxymethane administration (Fig. 1) (Bemeur et al. 2009) as well as in hepatic devascularized rats (Jiang et al. 2009a, b).
Catalase and glutathione peroxidase activities are decreased in the brains of rats with ALF due to thioacetamide (TAA) administration (Túnez et al. 2007; Sathyasaikumar et al. 2007). This loss of antioxidant defenses was accompanied by a higher rate of lipid peroxidation (Túnez et al. 2007; Sathyasaikumar et al. 2007), an increase of superoxide-dismutase (SOD)-induced hydrogen peroxide production (Reddy et al. 2004) and increased vulnerability to reactive oxygen species due to iron accumulation (Halliwell 1992; Sathyasaikumar et al. 2007). It was recently demonstrated that the total antioxidant status was significantly decreased in the rat brain following TAA-induced ALF (Zarros et al. 2008).
Mitochondrial permeability transition (MPT) is another potential consequence of oxidative stress. MPT is a Ca2+-dependent mechanism associated with a collapse of the inner mitochondrial membrane potential due to a sudden opening of the permeability transition pore (PTP). Opening of the PTP results in enhanced free radical production (Miller et al. 2003). Ammonia has been shown to induce the MPT in cultured astrocytes (Bai et al. 2001), and the mechanism most likely involves oxidative stress as antioxidants completely inhibit its formation (Rama Rao et al. 2005). However, in vivo evidence of the involvement of MPT in HE awaits future studies.
Indomethacin, a nonsteroidal anti-inflammatory drug, has been reported to be beneficial in experimental ALF (Chung et al. 2001). Indomethacin is a non-selective cyclooxygenase inhibitor and thus would be expected to reduce the extent of oxidative stress by altering the arachidonate cascade. In addition, Asanuma et al. (2001) reported that indomethacin was able to scavenge nitric oxide radicals. In a single case report, indomethacin was shown to normalize the intracranial pressure in a patient with ALF (Clemmesen et al. 1997).
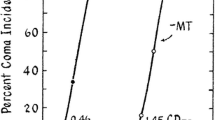
Our group recently demonstrated that the antioxidant N-acetylcysteine (NAC) significantly delayed the progression of encephalopathy in an experimental model of azoxymethane-induced ALF in the mouse (Bemeur et al. 2010a). NAC treatment decreased brain water content and proinflammatory cytokine levels and concomitantly restored both liver and brain GSH/GSSG ratios (Bemeur et al. 2010a). Treatment of experimental animals with HE with a range of agents with antioxidant properties including ascorbate, α-tocopherol, deferoxamine, butylated-hydroxyanisole, melatonin, L-carnitine, dimethylsulfoxide, and dimethylthiourea was also shown to have beneficial effects in ALF (Bruck et al. 1999; Guerrini 1994; Túnez et al. 2007).
Mild hypothermia improves the outcome of ALF in a wide range of experimental animal models (Cordoba et al. 1999; Rose et al. 2000; Schenker and Warren 1962; Traber et al. 1989; Jiang et al. 2009a; Bemeur et al. 2010b). While a number of mechanisms could explain this beneficial response, it is noteworthy that hypothermia has the potential to reduce free radical production (Globus et al. 1995). Jiang et al. (2009a) recently showed that mild hypothermia attenuates brain HO-1 mRNA and protein expression as well as eNOS and inducible NOS (iNOS) expression in the hepatic devascularized rat model of ALF. It was also shown that hypothermia led to normalization of eNOS mRNA expression in these animals (Sawara et al. 2009). Moreover, hypothermia delays the progression of encephalopathy, decreases proinflammatory cytokine levels, and increases GSH/GSSG ratios in the frontal cortex of mice with azoxymethane-induced ALF (Bemeur et al. 2010b).
To date, a limited number of studies have addressed the role of oxidative stress in the pathogenesis of HE in ALF patients. NAC was proven to be useful in the management of these patients (Harrison et al. 1991; Jones 1998; Wendon et al. 1994). Whether or not the beneficial effect of NAC relates simply to its antioxidant properties in the liver or to additional neuroprotective actions in the brain (NAC readily crosses the blood-brain barrier) remains to be established. Sodium benzoate, shown to be effective in the management of HE (Sushma et al. 1992) because of its ability to enhance the urinary excretion of ammonia (Brusilow et al. 1979), also has antioxidant properties (Haseloff et al. 1990; Upreti et al. 1991). Hypothermia has likewise been shown to be beneficial in humans with ALF due, at least in part, to its antioxidant effect (Jalan et al. 1999, 2003).
Chronic liver failure
NOS activity is increased in the brains of portacaval-shunted rats (Rao et al. 1995). iNOS and nNOS protein expression is increased in the brains of these animals (Rao 2002; Suárez et al. 2005; 2006) whereas brain eNOS protein expression is increased in TAA-induced cirrhosis in the rat (Hernández et al. 2004). An increase in HO-1 mRNA expression as well as a decrease in copper/zinc-SOD gene expression have been reported in the brains of portacaval-shunted rats (Song et al. 2002). Protein tyrosine nitration, a consequence of oxidative/nitrosative stress, was demonstrated in the cerebral cortex of these animals (Schliess et al. 2002; Suárez et al. 2006).
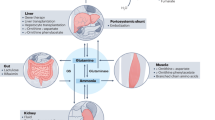
Exposure of brain to increased ammonia results in down regulation of the astrocytic glutamate transporter EAAT-2 leading to increased extracellular glutamate concentrations which activates NMDA receptors (NMDAr). This activation could cause production of superoxide, nitric oxide, nitric oxide-dependent cGMP and protein tyrosine nitration which leads to oxidative/nitrosative stress. Tyrosine nitration of the major ammonia-removing enzyme glutamine synthetase (GS) then results in increased brain ammonia and a vicious cycle
A distinctive neuropathologic finding in brains of patients with HE is the presence of Alzheimer type II astrocytes (Norenberg 1981). Characteristically, these cells contain increased amounts of lipofuscin pigment. These pigments consist of peroxidized lipids (Brunk 1989), consistent with their exposure to oxidative damage.
Table 1 summarizes evidence for oxidative/nitrosative stress in the brain in relation to the pathogenesis of HE in liver failure.
Cellular localization of oxidative/nitrosative stress in hepatic encephalopathy
Evidence supports the view that astrocytes are a major source of reactive oxygen species under simulated HE conditions (Schliess et al. 2006). Glutamine synthetase is predominantly expressed in astrocytes and the glutamine synthetase inhibitor methionine sulfoximine (MSO) reduces protein tyrosine nitration in ammonia-treated rats (Master et al. 1999; Schliess et al. 2002). Immunohistochemical analysis of brain slices from ammonia-treated rats reveals considerable co-localization of 3′-nitrotyrosine with glutamine synthetase and glial fibrillary acidic protein, indicating protein tyrosine nitration in astrocytes (Schliess et al. 2002; Görg et al. 2003, 2007).
In a rat model of chronic liver failure (portacaval anastomosis), neurons were immunoreactive to nNOS whereas iNOS was expressed in pyramidal-like cortical neurons and perivascular astrocytes (Suárez et al. 2006). In the same animals, nitrotyrosine immunoreactivity was found in pyramidal-like cortical neurons and in perivascular astrocytes. It was also demonstrated that nNOS and iNOS are produced in the Purkinje (neuronal) cells and Bergmann glial cells in rats following portacaval anastomosis (Suárez et al. 2005). TAA-cirrhotic rats showed nNOS immunoreactivity in stellate and basket neurons and eNOS immunoreactivity in perivascular glial cells of the white matter (Hernández et al. 2004). In the same experimental model of chronic liver failure, eNOS was located in Purkinje cell bodies and vessels endothelial cells (Hernández et al. 2004). Taken together, these data suggest that neuronal, glial and endothelial cells are all sources of nitric oxide in HE indicating that oxidative/nitrosative stress in HE is a multicellular phenomenon.
Oxidative/nitrosative stress in HE: ammonia or proinflammatory cytokines?
It has been proposed that oxidative/nitrosative stress results from NMDA-receptor activation (Fig. 2) (Hermenegildo et al. 1996; Kosenko et al. 1999; Marcaida et al. 1992). In a rodent model of ammonia neurotoxicity, Kosenko et al. (1997) showed decreased activity of several antioxidant enzymes, including glutathione peroxidase, manganese SOD and catalase. The same articles also described an increase in lipid peroxidation as well as glutathione depletion. The precise free radical specie(s) generated by ammonia is not certain, although increased production of superoxide (Kosenko et al. 1997, 2003) as well as increased nitric oxide production (Master et al. 1999) have been proposed. Hilgier et al. (2003) showed that infusion of ammonia into the striatum of rats resulted in the production of hydroxyl radicals. Moreover, ammonia toxicity increases the cerebral production of superoxide, nitric oxide and nitric oxide-dependent cGMP synthesis, as well as protein tyrosine nitration in an NMDA receptor-dependent manner (Hermenegildo et al. 1996; Kosenko et al. 1999, 2004; Master et al. 1999; Hermenegildo et al. 2000; Larsen et al. 2001; Schliess et al. 2002, 2006). However, evidence for similar mechanisms in the pathogenesis of HE in chronic liver failure in vivo is lacking.
In addition to ammonia, the inflammatory cascade generated by circulating and brain cytokines is also a potential source of oxidative stress. It is well known that inflammation is associated with free radical production (Laroux et al. 2001; Bemeur et al. 2005). Bemeur et al. (2010a) showed that administration of the antioxidant NAC in an experimental model of ALF prevented the increase in cytokines and the concomitant decrease in brain GSH/GSSG in the frontal cortex. Protective effects of the anti-inflammatory drug minocycline were also reported in rats with ALF due to hepatic devascularization (Jiang et al. 2009b). It was proposed that synergism between the neurotoxic effects of ammonia and proinflammatory cytokines could explain the neurological complications in ALF Microglial activation and consequent oxidative/stress could be central to this synergism.
In summary, experimental evidence for oxidative/nitrosative stress in brain in experimental models of HE due to acute or chronic liver failure is increasing and several reports suggest that oxidative/nitrosative stress participates in the pathophysiologic cascade responsible for HE. Antioxidant therapy such as NAC is already being used in the management of ALF and its complications. Other antioxidants could prove to be a valuable adjunct to traditional HE therapies such as ammonia lowering strategies or anti-inflammatory drugs. Further studies are needed in order to assess these possibilities.
Abbreviations
- HE:
-
hepatic encephalopathy
- ALF:
-
acute liver failure
- eNOS:
-
endothelial nitric oxide synthase
- HO-1:
-
heme oxygenase-1
- TAA:
-
thioacetamide
- SOD:
-
superoxide dismutase
- MPT:
-
mitochondrial permeability transition
- PTP:
-
permeability transition pore
- NAC:
-
n-acetylcysteine
- iNOS:
-
inducible nitric oxide synthase
- nNOS:
-
neuronal nitric oxide synthase
- NMDAr:
-
n-methyl-d-aspartic acid receptors
- GS:
-
glutamine synthetase
- MSO:
-
methionine sulfoximine
References
Ahboucha S, Pomier-Layrargues G, Mamer O, Butterworth RF (2006) Increased levels of pregnenolone and its neuroactive metabolite allopregnanolone in autopsied brain tissue from cirrhotic patients who died in hepatic coma. Neurochem Int 49:372–378
Asanuma M, Nishibayashi-Asanuma S, Miyazaki I, Kohno M, Ogawa N (2001) Neuroprotective effects of non-steroidal anti-inflammatory drugs by direct scavenging of nitric oxide radicals. J Neurochem 76:1895–1904
Bai G, Rama Rao KV, Murthy CR, Panickar KS, Jayakumar AR, Norenberg MD (2001) Ammonia induces the mitochondrial permeability transition in primary cultures of rat astrocytes. J Neurosci Res 66:981–991
Bemeur C, Ste-Marie L, Desjardins P, Vachon L, Butterworth RF, Hazell AS, Montgomery J (2005) Dehydrascorbic acid normalizes several markers of oxidative stress and inflammation in acute hyperglycemic focal cerebral ischemia in the rat. Neurochem Int 46:399–407
Bemeur C, Jiang W, Desjardins P, Butterworth RF (2009) Mild hypothermia attenuates oxidative/nitrosative stress and cytotoxic brain edema in experimental acute liver failure. XXIVth International Symposium on Cerebral Blood Flow, Metabolism and Function & IXth International Conference on Quantification of Brain Function with PET, Chicago, IL, USA
Bemeur C, Vaquero J, Desjardins P, Butterworth RF (2010a) N-Acetylcysteine attenuates cerebral complications of non-acetaminophen-induced acute liver failure in mice: antioxidant and anti-inflammatory mechanisms. Metab Brain Dis (in press)
Bemeur C, Desjardins P, Butterworth RF (2010b) Antioxidant and anti-inflammatory effects of mild hypothermia in the attenuation of liver injury due to azoxymethane toxicity in the mouse. Metab Brain Dis (in press)
Bruck R, Aeed H, Shirin H, Matas Z, Zaidel L, Avni Y, Halpern Z (1999) The hydroxyl radical scavengers dimethylsulfoxide and dimethylthiourea protect rats against thioacetamide-induced fulminant hepatic failure. J Hepatol 31:27–38
Brunk UT (1989) On the origin of lipofuscin; the iron content of residual bodies, and the relation of these organelles to the lysosomal vacuome. A study on cultured human glial cells. Adv Exp Med Biol 266:313–320
Brusilow SW, Valle DL, Batshaw M (1979) New pathways of nitrogen excretion in inborn errors of urea synthesis. Lancet 2:452–254
Butterworth RF (2002) Pathophysiology of hepatic encephalopathy: a new look at ammonia. Metab Brain Dis 17:221–227
Chung C, Gottstein J, Blei AT (2001) Indomethacin prevents the development of experimental ammonia-induced brain edema in rats after portacaval anastomosis. Hepatology 34:249–254
Clemmesen JO, Hansen BA, Larsen FS (1997) Indomethacin normalizes intracranial pressure in acute liver failure: a twenty-three-year-old woman treated with indomethacin. Hepatology 26:1423–1425
Cordoba J, Crespin J, Gottstein J, Blei AT (1999) Mild hypothermia modifies ammonia- induced brain edema in rats after portacaval anastomosis. Gastroenterology 116:686–693
Desjardins P, Butterworth RF (2002) The “peripheral-type” benzodiazepine (omega 3) receptor in hyperammonemic disorders. Neurochem Int 41:109–114
Globus MY, Alonso O, Dietrich WD, Busto R, Ginsberg MD (1995) Glutamate release and free radical production following brain injury: effects of posttraumatic hypothermia. J Neurochem 65:1704–1711
Görg B, Foster N, Reinehr R, Bidmon HJ, Höngen A, Häussinger D, Schliess F (2003) Benzodiazepine-induced protein tyrosine nitration in rat astrocytes. Hepatology 37:334–342
Görg B, Qvartskhava N, Voss P, Grune T, Häussinger D, Schliess F (2007) Reversible inhibition of mammalian glutamine synthetase by tyrosine nitration. FEBS Lett 581:84–90
Guerrini VH (1994) Effect of antioxidants on ammonia induced CNS-renal pathobiology in sheep. Free Radic Res 21:35–43
Halliwell B (1992) Reactive oxygen species and the central nervous system. J Neurochem 59:1609–1623
Harrison PM, Wendon JA, Gimson AE, Alexander GJ, Williams R (1991) Improvement by acetylcysteine of hemodynamics and oxygen transport in fulminant hepatic failure. N Engl J Med 324:1852–1857
Haseloff RF, Blasig IE, Meffert H, Ebert B (1990) Hydroxyl radical scavenging and antipsoriatic activity of benzoic acid derivatives. Free Radic Biol Med 9:111–115
Hawkins RA, Jessy J, Mans AM, De Joseph MR (1993) Effect of reducing brain glutamine synthesis on metabolic symptoms of hepatic encephalopathy. J Neurochem 60:1000–1006
Hermenegildo C, Marcaida G, Montoliu C, Grisolia S, Minana MD, Felipo V (1996) NMDA receptor antagonists prevent acute ammonia toxicity in mice. Neurochem Res 21:1237–1244
Hermenegildo C, Monfort P, Felipo V (2000) Activation of N-methyl-D-aspartate receptors in rat brain in vivo following acute ammonia intoxication: characterization by in vivo brain microdialysis. Hepatology 31:709–715
Hernández R, Martinez-Lara E, Del Moral ML, Blanco S, Cañuelo A, Siles E, Esteban FJ, Pedrosa JA, Peinado MA (2004) Upregulation of endothelial nitric oxide synthase maintains nitric oxide production in the cerebellum of thioacetamide cirrhotic rats. Neuroscience 126:879–887
Hilgier W, Anderzhanova E, Oja SS, Saransaari P, Albrecht J (2003) Taurine reduces ammonia- and N-methyl-D-aspartate-induced accumulation of cyclic GMP and hydroxyl radicals in microdialysates of the rat striatum. Eur J Pharmacol 468:21–25
Jalan R, Olde Damink SW, Deutz NE, Lee A, Hayes PC (1999) Moderate hypothermia for uncontrolled intracranial hypertension in acute liver failure. Lancet 354:1164–1168
Jalan R, Olde Damink SW, Deutz NE, Davies NA, Garden OJ, Machavan KK, Hayes PC, Lee A (2003) Moderate hypothermia prevents cerebral hyperemia and increase in intracranial pressure in patients undergoing liver transplantation for acute liver failure. Transplantation 75:2034–2039
Jiang W, Desjardins P, Butterworth RF (2009a) Hypothermia attenuates oxidative/nitrosative stress, encephalopathy and brain edema in acute (ischemic) liver failure. Neurochem Int 55:124–128
Jiang W, Desjardins P, Butterworth RF (2009b) Minocycline attenuates oxidative/nitrosative stress and cerebral complications of acute liver failure in rats. Neurochem Int 55:601–605
Jones AL (1998) Mechanism of action and value of n-acetylcysteine in the treatment of early and late acetaminophen poisoning: a critical review. J Toxicol Clin Toxicol 36:277–285
Kosenko E, Kaminsky Y, Grau E, Miñana MD, Marcaida G, Grisolía S, Felipo V (1994) Brain ATP depletion induced by acute ammonia intoxication in rats is mediated by activation of the NMDA receptor and Na+, K(+)-ATPase. J Neurochem 63:2172–2178
Kosenko E, Kaminsky Y, Kaminsky A, Valencia M, Lee L, Hermenegildo C, Felipo V (1997) Superoxide production and antioxidant enzymes in ammonia intoxication in rats. Free Radic Res 27:637–644
Kosenko E, Kaminski Y, Lopata O, Muravyoy N, Felipo V (1999) Blocking NMDA receptors prevents the oxidative stress induced by acute ammonia intoxication. Free Radic Biol Med 26:1369–1374
Kosenko E, Venediktova N, Kaminsky Y, Montoliu C, Felipo V (2003) Sources of oxygen radicals in brain in acute ammonia intoxication in vivo. Brain Res 98:193–200
Kosenko E, Montoliu C, Giordano G, Kaminsky Y, Venediktova N, Buryanov Y, Felipo V (2004) Acute ammonia intoxication induces an NMDA receptor-mediated increase in poly(ADP-ribose) polymerase level and NAD metabolism in nuclei of rat brain cells. J Neurochem 89:1101–1110
Laroux FS, Pavlick KP, Hines IN, Kawachi S, Harada H, Bharwani S, Hoffman JM, Grisham MB (2001) Role of nitric oxide in inflammation. Acta Physiol Scand 173:113–118
Larsen FS, Gottstein J, Blei AT (2001) Cerebral hyperemia and nitric oxide synthase in rats with ammonia-induced brain edema. J Hepatol 34:548–554
Marcaida G, Felipo V, Hermenegildo C, Manama MD, Grisolia S (1992) Acute ammonia toxicity is mediated by the NMDA type of glutamate receptors. FEBS Lett 296:67–68
Master S, Gottstein J, Blei AT (1999) Cerebral blood flow and the development of ammonia-induced brain edema in rats after portacaval anastomosis. Hepatology 30:876–880
Miller TJ, Phelka AD, Tjalkens RB, Dethloff LA, Philbert MA (2003) CI-1010 induced opening of the mitochondrial permeability transition pore precedes oxidative stress and apoptosis in SY5Y neuroblastoma cells. Brain Res 963:43–56
Mousseau DD, Butterworth RF (1994) Current theories on the pathogenesis of hepatic encephalopathy. Proc Soc Exp Biol Med 206:329–344
Murthy CR, Rama Rao KV, Bai G, Norenberg MD (2001) Ammonia-induced production of free radicals in primary cultures of rat astrocytes. J Neurosci Res 66:282–288
Norenberg MD (1981) The astrocyte in liver disease. Adv Cell Neurobiol 2:303–352
Norenberg MD, Huo Z, Neary JT, Roig-Cantesano A (1997) The glial glutamate transporter in hyperammonemia and hepatic encephalopathy: relation to energy metabolism and glutamatergic neurotransmission. Glia 21:124–133
Norenberg MD, Jayakumar AR, Rama Rao KV, Panickar KS (2007) New concepts in the mechanism of ammonia-induced astrocyte swelling. Metab Brain Dis 22:219–234
O’Connor JE, Costell M (1990) New roles of carnitine metabolism in ammonia cytotoxicity. Adv Exp Med Biol 272:183–195
Rama Rao KV, Jayakumar AR, Norenberg MD (2003) Ammonia neurotoxicity: role of the mitochondrial permeability transition. Metab Brain Dis 18:113–127
Rama Rao KV, Jayakumar AR, Norenberg MD (2005) Role of oxidative stress in the ammonia-induced mitochondrial permeability transition in cultured astrocytes. Neurochem Int 47:31–38
Rao VL (2002) Nitric oxide in hepatic encephalopathy and hyperammonemia. Neurochem Int 41:161–170
Rao KV, Norenberg MD (2001) Cerebral energy metabolism in hepatic encephalopathy and hyperammonemia. Metab Brain Dis 16:67–78
Rao VL, Audet RM, Butterworth RF (1995) Increased nitric oxide synthase activities and L-[3H]arginine uptake in brain following portacaval anastomosis. J Neurochem 65:677–678
Reddy PV, Murthy CR, Reddanna P (2004) Fulminant hepatic failure induced oxidative stress in nonsynaptic mitochondria of cerebral cortex in rats. Neurosci Lett 368:15–20
Rose C, Michalak A, Pannunzio M, Chatauret N, Rambaldi A, Butterworth RF (2000) Mild hypothermia delays the onset of coma and prevents brain edema and extracellular brain glutamate accumulation in rats with acute liver failure. Hepatology 31:872–877
Sathyasaikumar KV, Swapna I, Reddy PV, Murthy ChR, Dutta Gupta A, Senthilkumaran B, Reddanna P (2007) Fulminant hepatic failure in rats induces oxidative stress differentially in cerebral cortex, cerebellum and pons medulla. Neurochem Res 32:517–524
Sawara K, Desjardins P, Chatauret N, Kato A, Suzuki K, Butterworth RF (2009) Alterations in expression of genes coding for proteins of the neurovascular unit in ischemic liver failure. Neurochem Int 55:119–123
Schenker S, Warren KS (1962) Effect of temperature variation on toxicity and metabolism of ammonia in mice. J Lab Clin Med 60:291–301
Schliess F, Görg B, Fischer R, Desjardins P, Bidmon HJ, Herrmann A, Butterworth RF, Zilles K, Häussinger D (2002) Ammonia induces MK-801-sensitive nitration and phosphorylation of protein tyrosine residues in rat astrocytes. FASEB J 16:739–741
Schliess F, Görg B, Häussinger D (2006) Pathogenetic interplay between osmotic and oxidative stress: the hepatic encephalopathy paradigm. Biol Chem 387:1363–1370
Song G, Dhodda VK, Blei AT, Dempsey RJ, Rao VL (2002) GeneChip analysis shows altered mRNA expression of transcripts of neurotransmitter and signal transduction pathways in the cerebral cortex of portacaval shunted rats. J Neurosci Res 68:730–737
Suárez I, Bodega G, Rubino M, Felipo V, Fernández B (2005) Neuronal and inducible nitric oxide synthase expression in the rat cerebellum following portacaval anastomosis. Brain Res 1047:205–213
Suárez I, Bodega G, Arilla E, Felipo V, Fernández B (2006) The expression of nNOS, iNOS and nitrotyrosine is increased in the rat cerebral cortex in experimental hepatic encephalopathy. Neuropathol Appl Neurobiol 32:594–604
Sushma S, Dasarathy S, Tandon RK, Jain S, Gupta S, Bhist MS (1992) Sodium benzoate in the treatment of acute hepatic encephalopathy: a double-blind randomized trial. Hepatology 16:138–144
Szerb JC, Butterworth RF (1992) Effect of ammonium ions on synaptic transmission in the mammalian central nervous system. Prog Neurobiol 39:135–153
Takahashi H, Koehler RC, Brusilow SW, Traystman RJ (1991) Inhibition of brain glutamine accumulation prevents cerebral edema in hyperammonemic rats. Am J Physiol 261:H825–H829
Traber P, DalCanto M, Ganger D, Blei AT (1989) Effect of body temperature on brain edema and encephalopathy in the rat after hepatic devascularization. Gastroenterology 96:885–891
Túnez I, Muñoz MC, Medina FJ, Salcedo M, Feijóo M, Montilla P (2007) Comparison of melatonin, vitamin E and L-carnitine in the treatment of neuro- and hepatoxicity induced by thioacetamide. Cell Biochem Funct 25:119–127
Upreti KK, Das M, Khanna SK (1991) Role of antioxidants and scavengers on argemone oil-induced toxicity in rats. Arch Environ Contam Toxicol 20:531–537
Wendon JA, Harrison PM, Keays R, Williams R (1994) Cerebral blood flow and metabolism in fulminant liver failure. Hepatology 19:1407–1413
Zarros A, Theocharis S, Skandali N, Tsakiris S (2008) Effects of fulminant hepatic encephalopathy on the adult rat brain antioxidant status and the activities of acetylcholinesterase, (Na(+), K(+))- and Mg (2+)-ATPase: comparison of the enzymes’ response to in vitro treatment with ammonia. Metab Brain Dis 23:255–264
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bemeur, C., Desjardins, P. & Butterworth, R.F. Evidence for oxidative/nitrosative stress in the pathogenesis of hepatic encephalopathy. Metab Brain Dis 25, 3–9 (2010). https://doi.org/10.1007/s11011-010-9177-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-010-9177-y