Abstract
Heart failure (HF) is considered one of the most common diseases and one of the major causes of death. The latest studies show that HF is associated with an increase in oxidative stress. The use of antioxidants as therapy is effective in animal models, but not in humans. In this review, we analyse some emerging markers related to oxidative stress, evaluating their possible use as therapeutic targets: galectin-3, a β galactoside associated with myocardial fibrosis, α1-antitrypsin, an antiprotease and lectin-like oxidized low-density-lipoprotein receptor-1, the major receptor for ox-LDL. The up-regulation of galectin-3 appears to be associated with HF, atrial fibrillation, dilated cardiomyopathy, fibrogenesis and mortality, while in other cases it seems that galectin-3 may be protective in ischaemia–reperfusion injury. Serum α1-antitrypsin protein levels may increase in the presence of high concentrations of serum proteases, which are over expressed during reperfusion. The overexpression of α1-antitrypsin or the exogenous α1-antitrypsin treatment exhibits an anti-oxidative stress role, evaluated by increased eNOS expression and by decreased MMP9 expression, implicated in HF. The cardiac lectin-like oxidized low-density-lipoprotein receptor-1 is activated by oxidative stress in ischaemia–reperfusion injury, inducing apoptosis in cardiomyocytes through the deleterious NF-kB pathway, while the administration of anti-lectin-like oxidized low-density-lipoprotein receptor-1 antibody suppresses apoptosis and reduces the extent of myocardial infarction. In conclusion, α1-antitrypsin and lectin-like oxidized low-density-lipoprotein receptor-1 seem to represent two good markers in HF and therapeutic targets, whereas galectin-3 does not.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In recent decades, heart failure (HF) has become an epidemic in the western world.
HF is a pathological condition characterized by functional and structural cardiac changes, which progressively lead to mechanical cardiac dysfunction inducing multiple morphological, biochemical and molecular alterations referred to cardiac remodelling [1].
Many biological activities involved in this process include the interactions between endothelial cells, monocyte–macrophages, cardiomyocytes, fibrocytes and the neuro-endocrine system. In particular, systemic conditions such as diabetes, advanced age, hypertension, obesity, dyslipidemia and chronic kidney disease are involved in the onset of HF. These conditions increase oxidative stress through reactive oxygen species (ROS), leading to vascular endothelial damage, LV hypertrophy and heart interstitial fibrosis [2, 3].
Cardiac troponins and natriuretic peptides represent essential diagnostic biomarkers in HF [4]. A number of novel biomarkers are clinically available but not yet in routine use.
Here, we examine the biochemical events that characterize the initiation and progression of HF in relation to three markers sensitive to increased ROS as possible candidates in the diagnosis and treatment of HF: galactin-3 (GAL-3), α1-antitrypsin (AAT) and lectin-like oxidized low-density-lipoprotein receptor-1 (LOX-1). GAL-3 is involved in pathological myocardial fibrosis [5], AAT is a potent serine protease inhibitor [6], and LOX-1 is the major receptor for ox-LDL in human endothelial cells [7] (Fig. 1).
Effects of increased ROS in HF. The increment in ROS induced by altered metabolism, chronic kidney diseases and hypertension leads to electrophysiological, contractile, mitochondrial dysfunction and apoptosis in cardiomyocytes, fibrosis, inflammation and vascular dysfunction in the extracellular matrix; all events that characterize HF
Role of oxidative stress on HF
The main sources of ROS in the heart are the mitochondria, NADPH oxidases, xanthine oxidase and uncoupled nitric oxide synthase (NOS).
ROS are also produced by the increased expression and activity of NADPH oxidase due to pathological conditions leading to the increase in angiotensin II (Ang II), endothelin-1 and TNF alpha [8, 9]. In patients with HF, the production of xanthine oxidase is increased augmenting the ROS level [10]. In damaged heart tissue, NOS becomes structurally unstable inducing uncoupling and further increment of ROS levels. The deleterious effects of oxidants are partially due to their ability to induce modifications in subcellular organelles such as sarcoplasmic reticulum (SR), mitochondria and the nucleus, which are intimately involved in the regulation of cardiomyocyte Ca2+ homeostasis [11, 12]. Because contraction is mainly driven by Ca2+ released from the SR, this organelle plays a particularly important role in Ca2+ regulation, through the type two ryanodine receptors (RyR2), which are the major SR Ca2+ release channel in ventricular myocytes. Several studies showed that HF is associated with increased RyR2 activity and diastolic SR Ca2+ leak, leading to arrhythmias and contractile dysfunction [13,14,15] (Fig. 1).
Moreover, oxidative damage contributes to impairment of the electron transport chain in mitochondria inducing bio-energetic dysfunction by reduced ATP production and further accumulation of ROS [16].
Mitochondrial dysfunction has previously been reported in dilated cardiomyopathy and HF [17, 18]. However, several cellular strategies have evolved to limit or prevent mitochondria damage; for example, in the presence of overload pressure induced by left and right ventricular failure, the excessive mitochondrial ROS production [19] stimulates cardiomyocytes to activate mitophagy against cellular damage [20, 21].
Early myocardial reperfusion is an efficient strategy to avoid cell damage and to improve clinical outcomes, but subsequently, it causes tissue damage due to powerful oxidative stress. In fact after ischaemic events, oxidative stress can reduce the beneficial effects of the restored blood flow on the viability of cardiomyocytes inducing their death [22, 23]. Because of reperfusion injury, the incidence of cardiac failure is almost 10% at 1 year [24]. The generation of ROS can activate the intracellular proteolytic enzymes and induces cell death by initiating mitochondrial permeability transition [25].
Normally, production of free radicals by cellular respiration or by other biological processes in tissues is balanced by the presence of antioxidant molecules or enzymes.
As in other tissues, in the heart the main antioxidant components are catalase, superoxide dismutase (SOD), glutathione peroxidase (GPx), nicotinamide adenine dinucleotide (NAD+) and glutathione (GSH), which some studies showed to be reduced in the presence of HF [26, 27]. In dilated left ventricle tissue, GSH levels were decreased by 54% relative to controls and were shown to correlate with HF severity [28]. Recently, a study has shown that nicotinamide mononucleotide adenylyl transferase, a precursor of NAD+, is reduced in both a murine HF model and in patients affected by HF, suggesting that NAD+ , like GSH, is an important component in the elimination of ROS and lipoperoxides [29].
Studies from animal models indicated that both the inhibition of ROS-producing factors, the increase in antioxidant factors, such as vitamins, and the increase in antioxidant enzymes led to an improvement in the contractile capacity of myocardial tissue, a reduction in ventricular remodelling and fibrosis, as well as a reduction in the necrotic area after myocardial infarction (MI) [30,31,32,33,34,35,36,37]. These promising results have prompted some investigators to perform trials on humans, but, unfortunately, the data obtained from a large population were not positive [37,38,39].
Role of GAL-3 in HF
In HF, increased oxidative stress through ROS leads to cardiac fibrosis, especially after reperfusion [3, 40]. GAL-3, a beta galactoside binding lectin, is closely associated with MI and myocardial fibrosis in HF [41].
GAL-3 is mainly found in the cytoplasm of various types of cell, but can easily cross cell membranes entering the nucleus and the mitochondria and it can also be abundantly excreted in the extracellular space [42]. In the cytosol and mitochondria, it interacts with anti-apoptotic factors such as Bcl-2 [43], while in the extracellular compartment, it seems to regulate cellular adhesion. According to some authors, GAL-3 plays an important role in various physio-pathological processes such as in organogenesis, in the immune system and in tumour growth. These biological activities are due to particular interactions with various betagalactosides containing glycans, through a recognition domain composed of 135 amino acids (CRD) [44]. Lactose is an effective inhibitor of GAL-3 biological functions, but the addition of a glucose residue to the reducing end of galactose increases the affinity for galectin-3 considerably [45, 46].
Moreover, in the lactose molecule, exchange of a hydroxyl group for the more hydrophobic acetamide group (N-acetyllactosamine) increases affinity for galectin-3 by over sixfold, while a hydrophilic gal residue addition to the 3-hydroxyl group of lactose-N-acetyllactosamine increases the affinity for GAL-3 by over 23-fold [45].
Non-carbohydrate binding activities of GAL-3 include the interaction with the bacterial endotoxin lipopolysaccharide and with insoluble elastin, an extracellular matrix protein [47,48,49].
GAL-3 binds to intracellular and extracellular glycoproteins and activates fibroblast to produce fibres of connective tissue inducing fibrosis [50, 51]. Several clinical and experimental studies showed that up-regulation of GAL-3 was associated with HF, atrial fibrillation, dilated cardiomyopathy, fibrogenesis and mortality, implicating GAL-3 as a biomarker of heart disease [52,53,54,55,56,57]. GAL-3 has been shown to represent a strong predictive marker at 18 months if other risk factors, such as diabetes and renal insufficiency, are concurrent [58]. Moreover, some findings showed that low blood levels (< 11.8 ng/ml) of GAL-3 represent a good predictor of the absence of mortality and re-hospitalization at 6 months, whereas higher blood levels (> 17.8 ng/ml) indicate increased risk of being readmitted (2–3 times) [59, 60]. It has been observed that a genetic deficiency of GAL-3 or use of its inhibitors, like modified citrus pectin, attenuates cardiac fibrosis and inflammation [61]. Indeed, in experimental hyperaldosteronism, the increase in GAL-3 expression was associated with cardiac and renal fibrosis, and it was prevented by pharmacological inhibition (modified citrus pectin) or GAL-3 genic silencing [62]. In keeping with these findings, Yu et al. [63] found that genetic and pharmacological inhibition of GAL-3 prevents cardiac remodelling by interfering with myocardial fibrogenesis [63]. However, other studies are not in complete agreement with these observations. In fact, in an established mouse model of pressure-overloaded myocardium, a marked up-regulation of GAL-3 that correlated with adverse remodelling and dysfunction was found, but GAL-3 gene silencing had no effects on survival, systolic and diastolic dysfunction, or fibrosis [55]. Moreover, in a murine model with fibrotic cardiomyopathy attributable to cardiac overexpression of human β2-adrenoceptors (β2-TG), the treatment with N-acetyllactosamine which prevents GAL-3 upregulation did not reverse cardiac fibrosis, inflammation or cardiomyopathy [64].
Endomyocardial biopsies from HF patients revealed that the GAL-3 concentration in cardiac tissue did not reflect the concentration in plasma [53]. In many cases, the GAL-3 blood levels in HF patients before and after heart transplantation were unchanged, indicating that other organs were responsible for its high production [65].
Other hypotheses on the role of GAL-3 after ischaemia–reperfusion injury suggest that it could be protective. In fact, in GAL-3-KO rat group, troponin I and the proapoptotic proteins, cleaved caspase 3, cytochrome c and annexin V, were significantly higher than in GAL-3 wild-type group, which showed a significant increment in the antiapoptotic protein BCL2 and an increased antioxidant activity in the ischaemia reperfusion (IR)-injured myocardium [48].
Furthermore, after IR, heart immunohistochemically stained sections of the GAL-3 wild-type group showed higher expression of SOD, GSH reductase and catalase than those of the GAL-3 KO group [66, 67]. Glutathione and catalase specifically provide significant antioxidant protection of the myocardium against IR injury [68,69,70,71].
Regarding the relationship of ROS and GAL-3 in IR, Matarrese et al. [72] reported that GAL-3 might interfere with the early stages of cell death which are associated with perturbation of mitochondrial homeostasis and subsequent formation of ROS [72]. According to these data, the increase in GAL-3 in HF could be traced back to a compensatory protective mechanism. The contrasting findings present in the literature about the role of GAL-3 in HF reduce the possibility of using it as potential target for drug treatment [73,74,75].
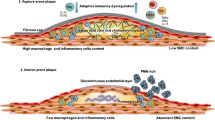
For some authors, Gal-3 it is still an emerging marker [76], but for others it is not.
Recent findings suggested that GAL-3, in combination with apoptotic endothelial cell-derived microvesicles (MVs) CD31+/annexin V+ MVs, was the best predictor of reduced ejection fraction (HFpEF) [76], while another author reported that it was not able to distinguish between preserved ejection fraction (HFrEF) and HFpEF patients, even if it demonstrated a prognostic role in subjects with HFpEF [77].
Role of AAT in HF
The increase in ROS in HF is associated with inflammation, and it is also related to the presence of proteases. In fact, it has been observed that some cytokines, such as IL-1 beta and IL-6, play an important role in cardiac remodelling and induction of metalloproteases [78, 79]. Serum AAT protein, the major component of the α-1 protein (A1-Pr) fraction, is an antiprotease, whose levels may increase in the presence of high concentrations of serum proteases over expressed during inflammation [80], so some authors suggested that it represents a promising therapeutic marker in HF and MI [81]. AAT action was previously studied in relation to its genetic deficiency in patients with chronic obstructive pulmonary disease, which did not show any protective protease activity and destruction of the elastin matrix within the lung, resulting in emphysema [82].
However, in addition to its presence in the lungs, circulating AAT also binds to the endothelium, limiting vascular damage and inflammatory pathways [83,84,85,86,87].
In the vasculature, low levels of AAT could cause the local degradation of elastin and consequently increase collagen deposition, contributing to arterial stiffness in atherosclerosis [83,84,85,86,87]. It is known that ROS plays a critical role in IR events. Indeed, during reperfusion the high production of ROS cannot be completely neutralized by antioxidant systems [88, 89].
Feng et al. [89] found that in HUVECs the overexpression of AAT or exogenous AAT treatment significantly increased the activity of SOD reduced by IR, whereas the knockdown of AAT did not [89]. Similarly, other findings showed that AAT exhibited an antioxidative stress role, evaluated by increased expression of eNOS and vascular endothelial growth factor-1 (VEGFR1) and by decreased expression of matrix metalloproteinase-9 (MMP-9) [90].
eNOS is known to protect cells against various injurious states, whereas the enhanced activity of MMP-9 is implicated in a variety of cardiovascular pathological states, such as ischaemic heart disease and HF [91]. Other studies have shown that patients with a reduced increment of the anti-protease AAT after MI were more likely to die, or had a worse clinical outcome than patients who had a normal increase in anti-protease AAT [92]. In fact, in vivo, the increment in AAT is sufficient to inhibit the high concentration of proteases [92]. However, it is known that AAT undergoes oxidation in HF patients, leading to protein dysfunction and loss of its activity against elastase and other proteases, events that can induce myocardial damage [93]. Based on these observations, the overexpression of AAT could represent a compensatory response to the loss of AAT activity [94].
Our recent study showed that serum A1-Pr concentration, measured through serum protein electrophoresis (SPE), identified patients with clinically overt HF in NYHA class III [6].
Recently, in a large population of HF patients, we observed a high positive correlation between A1-Pr and AAT (unpublished data). Therefore, an increase in A1-Pr, observed during a simple SPE, might represent a warning signal in patients not yet identified as HF.
Finally, a series of preclinical studies have provided evidence that AAT therapy is effective in several diseases, such as diabetes mellitus and organ transplant rejection, suggesting that medical applications of AAT can be expanded to pathologies other than pulmonary emphysema [94]. Using a model wherein endothelial cell monolayers are exposed to IR, exogenous AAT was found to alleviate IR injury in a dose- and time-dependent manner, demonstrating that overexpression of AAT decreased cell apoptosis and promoted proliferation via inhibition of Rac1/PAK/p38 signalling and ROS production [90]. In a clinical study, a single administration of Prolastin C, a plasma-derived AAT, given 12 h after reperfusion in patients with ST-Segment Elevation MI (STEMI), led to a significant inhibition of CK-MB, supporting the hypothesis that Prolastin C reduces the ischaemia–reperfusion injury time in STEMI patients. These preliminary data suggest that AAT treatment may be therapeutically beneficial to reduce IR-induced vascular injury [95].
Role of LOX-1 in HF
Reperfusion is associated with a large amount of ROS that converts LDL in ox-LDL and over-expression of LOX-1 in myocardial tissue. LOX-1 is considered the major receptor for ox-LDL in human endothelial cells, and it is also expressed in smooth muscle cells, cardiomyocytes and macrophages, in atherosclerotic lesions and in plaque neovascularization [96,97,98,99]. Our previous studies showed that the measurement of soluble LOX-1 in serum could potentially be useful in predicting progression of atherosclerotic disease in humans, as it is closely correlated with atherosclerotic plaque formation [100].
In HF, LOX-1 levels were found to correlate directly with brain natriuretic peptide and inversely with the ejection fraction [101]. Supporting these observations, mice with LOX-1 gene deletion showed improvement in cardiac function, myocardial inflammation and fibrosis, after treatment with doxorubicin [102].
Moreover, the cardiac LOX-1 pathway was activated by oxidative stress in vitro and by IR injury in vivo, inducing apoptosis in cardiomyocytes, while the administration of anti-LOX-1 antibody was able to suppress apoptosis in vitro and to reduce the extent of MI in vivo [7, 103].
In addition, the up-regulation of this receptor increases the production of proteases that are involved in HF [104]. In fact, one of the characteristics of HF is the large accumulation of collagen fragment induced by metalloproteinases, such as collagenases and gelatinases [104].
Hu et al. [105] reported the regulation of TGFbeta1-mediated collagen formation by LOX-1 underlying signalling in mouse cardiac fibroblasts. Transfection of wild-type mouse cardiac fibroblasts with AAV/TGFbeta1 markedly enhanced the expression of NADPH oxidases (p22(phox), p47(phox) and gp91(phox) subunits), LOX-1, ROS and collagen synthesis, concomitant with an increase in the activation of p38 and p44/42 mitogen-activated protein kinases (MAPK). The TGFbeta(1)-mediated increase in collagen synthesis was markedly attenuated in cardiac fibroblasts from/of LOX-1 knock-out mice, as well as in similar wild-type fibroblasts treated with an anti-LOX-1-specific antibody [105].
LOX-1 expression was markedly increased during IR. Simultaneously, the expression of MMP-1 and adhesion molecules (P-selectin, VCAM-1 and ICAM-1) was also increased in the IR area [106], together with leukocyte accumulation. Treatment of rats with LOX-1 antibody prevented IR-induced upregulation of LOX-1 and reduced MMP-1 and adhesion molecule expression, as well as leukocyte recruitment. These findings indicate that myocardial IR upregulates LOX-1 expression, which increases the expression of MMP-1 and adhesion molecules through p38 MAPK activation. Inhibition of LOX-1 exerts an important protective effect against myocardial IR injury [106]. However, the utility of the serum LOX-1 assay was shown not only in the diagnosis of left ventricular systolic HF after episodes of post-ischaemic reperfusion, but also in the diagnosis of HF, for example in patients with ischaemic cardiomyopathy indicating a link between LOX-1 and HF in patients with chronic ischaemia supported by oxidative stress and inflammation [107].
In cultured neonatal rat cardiac myocytes, noradrenaline and endothelin were able to upregulate LOX-1 expression inducing apoptosis through p38 MAPK, a component of oxidant stress-sensitive signalling pathways [103].
Moreover, in Dahl salt sensitive rats, with HF, it has been observed that eplerenone, a selective aldosterone blocker, stimulated endothelial eNOS through AKT and inhibited iNOS via nuclear factor kB(NF-kB) after activation of LOX-1 pathway, suggesting that the suppression of NF-kB- LOX-1 activation could improve cardiac function and remodelling [108].
Other data have shown that LOX-1 can also act on cardiomyocyte contraction. This effect was observed by oxidation of tropomyosin in cardiomyocyte culture. The inhibition of LOX-1 with antisense RNA voided this effect [107]. The intracellular increment of oxidative stress induced activation of the p38 MAP kinase, responsible for pro-protein convertase subtilisin/kexin-9 (PCSK9). The authors described that ox-LDL significantly impaired contractile function via induction of PCSK9 [109]. The presence of LOX-1 has also been reported in fibroblasts of cardiac tissue, and its expression was induced by the increase in angiotensin II (Ang II levels), a neuro-hormone that contributes to cardiac remodelling [110, 111]. The infusion of Ang II in wild-type mice induces cardiac remodelling, while in mice with no-functioning LOX-1 the effect was less evident [110]. The incorporation of LOX-1 in cardiac fibroblast exposed to ox-LDL enhanced production of adhesion molecules and metalloproteinases [112].
Comments and criticisms on the use of GAL-3, AAT and LOX-1
In this review, we wanted to highlight the characteristics of GAL-3, AAT and LOX-1 as biomarkers for the diagnosis of HF and as potential targets of therapy.
In fact, precise early diagnosis could improve the life quality of these patients.
As we have described, few clinical studies have been performed on these markers regarding the diagnosis of HF. For GAL-3, enough data have been collected in clinical studies [52,53,54, 58,59,60] even if they are sometimes contradictory. For AAT and LOX-1, the published clinical data are insufficient to affirm their validity.
Recently, regarding AAT serum levels, we evaluated the trend in affected patients by indirectly measuring the serum concentrations of α-1 protein [6]. Correlation with NT-pro-BNP, NYHA class and other significant data led us to directly evaluate AAT in a larger population. However, some authors have already suggested in clinical studies that AAT represents a promising therapeutic marker in HF and in MI [82], and patients with low levels of AAT had a worse clinical outcome [92]. Several studies performed in animal models and in vitro suggest the implication of LOX-1 in HF, indicating the utility to investigate this relationship also in humans. Some clinical studies showed LOX-1 association with the development and progression of atherosclerotic plaques [101], and animal studies showed that LOX-1 levels correlated inversely with EF% and directly with natriuretic peptides [102]. LOX-1 association with apoptosis, inflammation and fibrosis leads us to believe that it is an important factor in the development of HF.
There are numerous markers of oxidative stress and inflammation that could be implicated in the development of HF, which are widely described in the literature. However, few of them have been introduced into clinical practice. In fact, in addition to their involvement in the disease, a marker must be sensitive, specific and, above all, easily measurable. The markers previously mentioned have good analytical characteristics and are easy to apply in clinical laboratories. With the ELISA methods, it is possible to have very accurate data, and from our studies the A1-Pr electrophoresis analysis provides an accurate estimate of the significant increase in AAT for an immediate evaluation of subjects at risk.
MicroRNAs (miRNAs) have been shown to participate in a variety of cardiovascular diseases through post-transcriptional regulation of target gene proteins: for instance, the miR-30 family can participate in ventricular remodelling through a variety of mechanisms, including autophagy, apoptosis, oxidative stress and inflammation. Although clinical studies can be performed by detecting miRNAs, not all clinical laboratories have molecular biology technologies and the costs and times for this analysis would be much higher to those incurred with the previously mentioned methods [113].
Conclusion
In conclusion, there are some accepted valid markers, like NT-proBNP, for the diagnosis of HF, while others are still being studied such as those described in this review. Considering the contradictory findings of the literature, GAL-3 does not appear to be a good marker in the diagnosis and characterization of HF, while in our experience, both A1-p, AAT and LOX-1 appear to be effective markers.
There are no studies on LOX-1 and AAT regarding HFpEF and HFrEF differentiation capacity. In our opinion, given the strong link that exists between these factors and the oxidative stress damage exerted on myocardial tissue in HF, a discriminatory capacity is to be expected. This evaluation will be considered in future studies.
Concerning the therapeutic use, being a non-specific method, antioxidant systems are not very effective, while therapies based on AAT treatment or on the inhibition of LOX-1 activity may be beneficial in reducing IR injury.
In particular, LOX-1 is susceptible to the presence of many macromolecules such as ox-LDL, Ang II, ROS and some cytokines, involved in several pathological processes (Fig. 2), by triggering the deleterious NF-kB pathway. Therefore, anti-LOX-1 antibodies could represent a useful therapy for HF patients.
Main effects of LOX-1 overexpression in cardiomyocytes. Activation of lectin-like oxidized low-density lipoprotein receptor-1 by ox-LDL and other stimuli leads to cascade of intracellular signalling pathways inducing cardiomyocytes injury and modification of extracellular matrix; events that lead to HF
References
Palazzuoli A, Nuti R (2010) Heart failure: pathophysiology and clinical picture. Contrib Nephrol 164:1–10. https://doi.org/10.1159/000313714
Lim S, Lam CS, Segers VF et al (2015) Cardiac endothelium-myocyte interaction: clinical opportunities for new heart failure therapies regardless of ejection fraction. Eur Heart J 36:2050–2060. https://doi.org/10.1093/eurheartj/ehv132
Paulus WJ, Tschope C (2013) A novel paradigm for heart failure with preserved ejection fraction: comorbidities drive myocardial dysfunction and remodelling through coronary microvascular endothelial inflammation. J Am Coll Cardiol 62:263–267. https://doi.org/10.1016/j.jacc.2013.02.092
Sun RR, Lu L, Liu M et al (2014) Biomarkers and heart disease. Eur Rev Med Pharmacol Sci 18:2927–2935
De Boer RA, Van der Velde AR, Mueller C et al (2014) Galectin-3: a modifiable risk factor in heart failure. Cardiovasc Drugs Ther 28:237–246. https://doi.org/10.1007/s10557-014-6520-2
Lubrano V, Papa A, Pingitore A et al (2017) Alpha-1 protein evaluation to stratify heart failure patients. J Cardiovasc Med 18:774–776. https://doi.org/10.2459/JCM.0000000000000016
Kataoka K, Hasegawa K, Sawamura T et al (2003) LOX-1 pathway affects the extent of myocardial ischemia-reperfusion injury. Biochem Biophys Res Commun 300:656–660. https://doi.org/10.1016/s0006-291x(02)02905-4
Doughan AK, Harrison DG, Dikalov SI (2008) Molecular mechanisms of angiotensin II-mediated mitochondrial dysfunction: linking mitochondrial oxidative damage and vascular endothelial dysfunction. Circ Res 102:488–496. https://doi.org/10.1161/CIRCRESAHA.107.162800
Heymes C, Bendall JK, Ratajczak P et al (2003) Increased myocardial NADPH oxidase activity in human heart failure. J Am Coll Cardiol 41:2164–2171. https://doi.org/10.1016/s0735-1097(03)00471-6
Cappola TP, Kass DA, Nelson GS et al (2001) Allopurinol improves myocardial efficiency in patients with idiopathic dilated cardiomyopathy. Circulation 104:2407–2411. https://doi.org/10.1161/hc4501.098928
Dhalla NS, Das PK, Sharma GP (1978) Subcellular basis of cardiac contractile failure. J Mol Cell Cardiol 10:363–385
Dhalla NS, Temsah RM, Netticadan T (2000) Role of oxidative stress in cardiovascular diseases. J Hypertens 18:655–673. https://doi.org/10.1097/00004872-200018060-00002
Blayney LM, Lai FA (2009) Ryanodine receptor-mediated arrhythmias and sudden cardiac death. Pharmacol Ther 123:151–177. https://doi.org/10.1016/j.pharmthera.2009.03.006
Mochizuki M, Yano M, Oda T et al (2007) Scavenging free radicals by low-dose carvedilol prevents redox-dependent Ca2+ leak via stabilization of ryanodine receptor in heart failure. J Am Coll Cardiol 49:1722–1732. https://doi.org/10.1016/j.jacc.2007.01.064
Terentyev D, Györke I, Belevych AE et al (2008) Redox modification of ryanodine receptors contributes to sarcoplasmic reticulum Ca2+ leak in chronic heart failure. Circ Res 103:1466–1472. https://doi.org/10.1161/CIRCRESAHA.108.184457
Indo HP, Davidson M, Yen HC et al (2007) Evidence of ROS generation by mitochondria in cells with impaired electron transport chain and mitochondrial DNA damage. Mitochondrion 7:106–118. https://doi.org/10.1016/j.mito.2006.11.026
Hayashi D, Ohshima S, Isobe S et al (2013) Increased (99 m)Tc-sestamibi washout reflects impaired myocardial contractile and relaxation reserve during dobutamine stress due to mitochondrial dysfunction in dilated cardiomyopathy patients. J Am Coll Cardiol 61:2007–2017. https://doi.org/10.1016/j.jacc.2013.01.074
Ahuja P, Wanagat J, Wang Z et al (2013) Divergent mitochondrial biogenesis responses in human cardiomyopathy. Circulation 127:1957–1967. https://doi.org/10.1161/CIRCULATIONAHA.112.001219
Redout EM, Wagner MJ, Zuidwijk MJ et al (2007) Right-ventricular failure is associated with increased mitochondrial complex II activity and production of reactive oxygen species. Cardiovasc Res 75:770–781. https://doi.org/10.1016/j.cardiores.2007.05.012
Kubli DA, Gustafsson ÅB (2012) Mitochondria and mitophagy: the yin and yang of cell death control. Circ Res 111:1208–1221. https://doi.org/10.1161/CIRCRESAHA.112.265819
Wang K, Klionsky DJ (2011) Mitochondria removal by autophagy. Autophagy 7:297–300. https://doi.org/10.4161/auto.7.3.14502
Piper HM, García-Dorado DM et al (1998) A fresh look at reperfusion injury. Cardiovasc Res 38:291–300. https://doi.org/10.1016/s0008-6363(98)00033-9
Buja LM (2005) Myocardial ischemia and reperfusion injury. Cardiovasc Pathol 14:170–175. https://doi.org/10.1016/j.carpath.2005.03.006
Bulluck H, Yellon DM, Hausenloy DJ (2016) Reducing myocardial infarct size: challenges and future opportunities. Heart 102:341–348. https://doi.org/10.1136/heartjnl-2015-307855
Raedschelders K, Ansley DM, Chen DD (2012) The cellular and molecular origin of reactive oxygen species generation during myocardial ischemia and reperfusion. Pharmacol Ther 133:230–255. https://doi.org/10.1016/j.pharmthera.2011.11.004
Khaper N, Singal PK (1997) Effects of after load-reducing drugs on pathogenesis of antioxidant changes and congestive heart failure in rats. J Am Coll Cardiol 9:856–861. https://doi.org/10.1016/s0735-1097(96)00574-8
Khaper N, Kaur K, Li T et al (2003) Antioxidant enzyme gene expression in congestive heart failure following myocardial infarction. Mol Cell Biochem 251:9–15
Adamy C, Mulder P, Khouzami L et al (2007) Neutral sphingomyelinase inhibition participates to the benefits of N-acetylcysteine treatment in post-myocardial infarction failing heart rats. J Mol Cell Cardiol 43:344–353. https://doi.org/10.1016/j.yjmcc.2007.06.010
Townsend DM, Tew KD, Tapiero H (2003) The importance of glutathione in human disease. Biomed Pharmacother 57:145–155
Minhas KM, Saraiva RM, Schuleri KH et al (2006) Xanthine oxidoreductase inhibition causes reverse remodeling in rats with dilated cardiomyopathy. Circ Res 98:271–279. https://doi.org/10.1161/01.RES.0000200181.59551.71
Ukai T, Cheng CP, Tachibana H et al (2001) Allopurinol enhances the contractile response to dobutamine and exercise in dogs with pacing-induced heart failure. Circulation 103:750–755. https://doi.org/10.1161/01.cir.103.5.750
Takimoto E, Champion HC, Li M et al (2005) Oxidant stress from nitric oxide synthase-3 uncoupling stimulates cardiac pathologic remodelling from chronic pressure load. J Clin Invest 115:1221–1231. https://doi.org/10.1172/JCI21968
Wang P, Chen H, Qin H et al (1998) Overexpression of human copper, zinc-superoxide dismutase (SOD1) prevents post ischemic injury. Proc Natl Acad Sci USA 95:4556–4560. https://doi.org/10.1073/pnas.95.8.4556
Qin F, Lennon-Edwards S, Lancel S et al (2010) Cardiac-specific overexpression of catalase identifies hydrogen peroxide-dependent and -independent phases of myocardial remodelling and prevents the progression to overt heart failure in G(alpha)q-overexpressing transgenic mice. Circ Heart Fail 3:306–313. https://doi.org/10.1161/CIRCHEARTFAILURE.109.864785
Hamblin M, Smith HM, Hill MF (2007) Dietary supplementation with vitamin E ameliorates cardiac failure in type I diabetic cardiomyopathy by suppressing myocardial generation of 8-iso-prostaglandin F2 alpha and oxidized glutathione. J Card Fail 13:884–892. https://doi.org/10.1016/j.cardfail.2007.07.002
Li W, Tang R, Ouyang S et al (2017) Folic acid prevents cardiac dysfunction and reduces myocardial fibrosis in a mouse model of high-fat diet-induced obesity. Nutr Metab 14:68. https://doi.org/10.1186/s12986-017-0224-0
Cunnington C, Van Assche T, Shirodaria C et al (2012) Systemic and vascular oxidation limits the efficacy of oral tetrahydrobiopterin treatment in patients with coronary artery disease. Circulation 125:1356–1366. https://doi.org/10.1161/CIRCULATIONAHA.111.038919
Freudenberger RS, Schwarz RP, Brown J et al (2004) Rationale, design and organisation of an efficacy and safety study of oxypurinol added to standard therapy in patients with NYHA class III-IV congestive heart failure. Expert Opin Investig Drugs 13:1509–1516. https://doi.org/10.1517/13543784.13.11.1509
Hare JM, Mangal B, Brown J et al (2008) Impact of oxypurinol in patients with symptomatic heart failure. J Am Coll Cardiol 51:2301–2309. https://doi.org/10.1016/j.jacc.2008.01.068
Louzao-Martinez L, Vink A, Harakalova M et al (2016) Characteristic adaptations of the extracellular matrix in dilated cardiomyopathy. Int J Cardiol 220:634–646. https://doi.org/10.1016/j.ijcard.2016.06.253
Al-Salam S, Hashmi S (2018) Myocardial ischemia reperfusion injury: apoptotic, inflammatory and oxidative stress. Role of galectin-3. Cell Physiol Biochem 50:1123–1139. https://doi.org/10.1159/000494539
Ochieng J, Furtak V, Lukyanov P (2002) Extracellular functions of galectin-3. Glycoconj J 19:527–535. https://doi.org/10.1023/B:GLYC.0000014082.99675.2f
Akahani S, Nangia-Makker P, Inohara H et al (1997) Galectin-3: a novel antiapoptotic molecule with a functional BH1 (NWGR) domain of Bcl-2 family. Cancer Res 57:5272–5276
Seetharaman J, Kanigsberg A, Slaaby R et al (1998) X-ray crystal structure of the human galectin-3 carbohydrate recognition domain at 2.1-A resolution. J Biol Chem 273:13047–13052. https://doi.org/10.1074/jbc.273.21.13047
Bachhawat-Sikder K, Thomas CJ, Surolia A (2001) Thermodynamic analysis of the binding of galactose and poly-N-acetyllactosamine derivatives to human galectin-3. FEBS Lett 500:75–79. https://doi.org/10.1016/s0014-5793(01)02586-8
Ochieng J, Fridman R, Nangia-Makker P et al (1994) Galectin-3 is a novel substrate for human matrix metalloproteinases-2 and -9. Biochemistry 33:14109–14114. https://doi.org/10.1021/bi00251a020
Mey A, Leffler H, Hmama Z et al (1996) The animal lectin galectin-3 interacts with bacterial lipopolysaccharides via two independent sites. J Immunol 156:1572–1577
Ochieng J, Warfield P, Green-Jarvis B et al (1999) Galectin-3 regulates the adhesive interaction between breast carcinoma cells and elastin. J Cell Biochem 75:505–514
Sciacchitano S, Lavra L, Morgante A et al (2018) One molecule for an alphabet of diseases, from A to Z. Int J Mol Sci 19(2):E379. https://doi.org/10.3390/ijms19020379
Rabinovich GA, Toscano MA (2009) Turning “sweet” on immunity: galectin glycan interactions in immune tolerance and inflammation. Nat Rev Immunol 9:338–352. https://doi.org/10.1038/nri2536
Arad U, Madar-Balakirski N, Angel-Korman A et al (2015) Galectin-3 is a sensor-regulator of toll-like receptor pathways in synovial fibroblasts. Cytokine 73:30–35. https://doi.org/10.1016/j.cyto.2015.01.016
De Boer RA, Daniels LB, Maisel AS et al (2015) State of the art: newer biomarkers in heart failure. Eur J Heart Fail 17:559–569. https://doi.org/10.1002/ejhf.273
Besler C, Lang D, Urban D et al (2017) Plasma and cardiac galectin-3 in patients with heart failure reflects both inflammation and fibrosis: implications for its use as a biomarker. Circ Heart Fail 10(1–9):e003804. https://doi.org/10.1161/CIRCHEARTFAILURE.116.003804
Frunza O, Russo I, Saxena A et al (2016) Myocardial galectin-3 expression is associated with remodeling of the pressure-overloaded heart and may delay the hypertrophic response without affecting survival, dysfunction and cardiac fibrosis. Am J Pathol 186:1114–1127. https://doi.org/10.1016/j.ajpath.2015.12.017
Nguyen MN, Su Y, Vizi D et al (2018) Mechanisms responsible for increased circulating levels of galectin-3 in cardiomyopathy and heart failure. Sci Rep 8(8213):1–12. https://doi.org/10.1038/s41598-018-26115-y
Hernández-Romero D, Vílchez JA, Lahoz Á et al (2017) Galectin-3 as a marker of interstitial atrial remodelling involved in atrial fibrillation. Sci Rep 7:40378. https://doi.org/10.1038/srep40378
Jaquenod De Giusti C, Ure AE, Rivadeneyra L et al (2015) Macrophages and galectin 3 play critical roles in CVB3-induced murine acute myocarditis and chronic fibrosis. J Mol Cell Cardiol 85:58–70. https://doi.org/10.1016/j.yjmcc.2015.05.010
Peacock WF (2003) Rapid optimization: strategies for optimal care of decompensated congestive heart failure patients in the emergency department. Rev Cardiovasc Med 3:41–48
Meijers WC, De Boer RA, Van Veldhuisen DJ et al (2015) Biomarkers and low risk in heart failure, data from COACH and TRIUMPH. Eur J Heart Fail 17:1271–1282. https://doi.org/10.1002/ejhf.407
Meijers WC, Januzzi JL, Adourian AS et al (2014) Elevated plasma galectin-3 is associated with near-term rehospitalisation in heart failure: a pooled analysis of 3 clinical trials. Am Heart J 167:853–860. https://doi.org/10.1016/j.ahj.2014.02.011
Martínez-Martínez E, Calvier L, Fernández-Celis A et al (2015) Galectin-3 blockade inhibits cardiac inflammation and fibrosis in experimental hyperaldosteronism and hypertension. Hypertension 66:767–775. https://doi.org/10.1161/HYPERTENSIONAHA.115.05876
Calvier L, Martinez-Martinez E, Miana M et al (2015) The impact of galectin-3 inhibition on aldosterone-induced cardiac and renal injuries. JACC Heart Fail 3:59–67. https://doi.org/10.1016/j.jchf.2014.08.002
Yu L, Ruifrok WP, Meissner M et al (2013) Genetic and pharmacological inhibition of galectin-3 prevents cardiac remodeling by interfering with myocardial fibrogenesis. Circ Heart Fail 6:107–117. https://doi.org/10.1161/CIRCHEARTFAILURE.112.971168
Nguyen MN, Su Y, Kiriazis H et al (2018) Upregulated galectin-3 is not a critical disease mediator of cardiomyopathy induced by β2-adrenoceptor overexpression. Am J Physiol Heart Circ Physiol 314:1169–1178
Grupper A, Nativi-Nicolau J, Maleszewski JJ et al (2016) Circulating galectin-3 levels are persistently elevated after heart transplantation and are associated with renal dysfunction. JACC Heart Fail 4:847–856. https://doi.org/10.1016/j.jchf.2016.06.010
Jolly SR, Kane WJ, Bailie MB et al (1984) Canine myocardial reperfusion injury. Its reduction by the combined administration of superoxide dismutase and catalase. Circ Res 54:277–285. https://doi.org/10.1161/01.res.54.3.277
Nakamura H, Nakamura K, Yodoi J (1997) Redox regulation of cellular activation. Annual Rev Immunol 15:351–369. https://doi.org/10.1146/annurev.immunol.15.1.351
Ceconi C, Curello S, Cargnoni A et al (1988) The role of glutathione status in the protection against ischaemic and reperfusion damage: effects of N-acetyl cysteine. J Mol Cell Cardiol 20:5–13
Singh A, Lee KJ, Lee CY et al (1989) Relation between myocardial glutathione content and extent of ischemia-reperfusion injury. Circulation 80:1795–1804. https://doi.org/10.1161/01.cir.80.6.1795
Chen Z, Siu B, Ho YS et al (1998) Overexpression of MnSOD protects against myocardial ischemia/reperfusion injury in transgenic mice. J Mol Cell Cardiol 30:2281–2289. https://doi.org/10.1006/jmcc.1998.0789
Woo YJ, Zhang JC, Vijayasarathy C et al (1998) Recombinant adenovirus-mediated cardiac gene transfer of superoxide dismutase and catalase attenuates post ischemic contractile dysfunction. Circulation 98:II255–II260
Matarrese P, Tinari N, Semeraro ML et al (2000) Galectin-3 overexpression protects from cell damage and death by influencing mitochondrial homeostasis. FEBS Lett 473:311–315. https://doi.org/10.1016/s0014-5793(00)01547-7
Fernandes Bertocchi AP, Campanhole G, Wang PH et al (2008) A role for galectin-3 in renal tissue damage triggered by ischemia and reperfusion injury. Transpl Int 21:999–1007. https://doi.org/10.1111/j.1432-2277.2008.00705.x
Yamaoka A, Kuwabara I, Frigeri LG et al (1995) A human lectin, galectin-3 (epsilon bp/Mac-2), stimulates superoxide production by neutrophils. J Immunol 154:3479–3487
Dong R, Zhang M, Hu Q et al (2018) Galectin-3 as a novel biomarker for disease diagnosis and a target for therapy. Int J Mol Med 41:599–614. https://doi.org/10.3892/ijmm.2017.3311
Berezin AE, Kremzer AA, Samura TA et al (2019) Altered signature of apoptotic endothelial cell-derived microvesicles predicts chronic heart failure phenotypes. Biomark Med 13:737–750. https://doi.org/10.2217/bmm-2018-0449
Beltrami M, Ruocco G, Dastidar AG et al (2016) Additional value of Galectin-3 to BNP in acute heart failure patients with preserved ejection fraction. Clin Chim Acta 457:99–105. https://doi.org/10.1016/j.cca.2016.04.007
Li M, Georgakopoulos D, Lu G et al (2005) p38 MAP kinase mediates inflammatory cytokine induction in cardiomyocytes and extracellular matrix remodeling in heart. Circulation 111:2494–2502. https://doi.org/10.1161/01.CIR.0000165117.71483.0C
Moore L, Fan D, Basu R et al (2012) Tissue inhibitor of metalloproteinases (TIMPs) in heart failure. Heart Fail Rev 17:693–706. https://doi.org/10.1007/s10741-011-9266-y
Lewis EC (2012) Expanding the clinical indications for α (1)-antitrypsin therapy. Mol Med 18:957–970. https://doi.org/10.2119/molmed.2011.00196
Abbate A, Van Tassell BW, Christopher S et al (2015) Effects of prolastin C (plasma-derived alpha-1 antitrypsin) on the acute inflammatory response in patients with ST-segment elevation myocardial infarction (from the VCU-alpha 1-RT pilot study). Am J Cardiol 115:8–12. https://doi.org/10.1016/j.amjcard.2014.09.043
Duckers JM, Shale DJ, Stockley RA et al (2010) Cardiovascular and muscle skeletal co-morbidities in patients with alpha 1 antitrypsin deficiency. Respir Res 11:173. https://doi.org/10.1186/1465-9921-11-1
Forsyth KD, Talbot V, Beckman I (1994) Endothelial serpins-protectors of the vasculature? Clin Exp Immunol 95:277–282. https://doi.org/10.1111/j.1365-2249.1994.tb06523.x
Ortiz-Muñoz G, Houard X, Martín-Ventura JL et al (2009) HDL antielastase activity prevents smooth muscle cell anoikis, a potential new antiatherogenic property. FASEB J 23:3129–3139. https://doi.org/10.1096/fj.08-127928
Aldonyte R, Janssson L, Janciauskiene S (2004) Concentration-dependent effects of native and polymerised alpha1-antitrypsin on primary human monocytes, in vitro. BMC Cell Biol 5:1–11. https://doi.org/10.1186/1471-2121-5-11
Laurent S, Cockcroft J, Van Bortel L et al (2006) Expert consensus document on arterial stiffness: methodological issues and clinical applications. Eur Heart J 27:2588–2605. https://doi.org/10.1093/eurheartj/ehl254
Willum-Hansen T, Staessen JA, Torp-Pedersen C et al (2006) Prognostic value of aortic pulse wave velocity as index of arterial stiffness in the general population. Circulation 113:664–670. https://doi.org/10.1161/CIRCULATIONAHA.105.579342
Rana A, Goyal N, Ahlawat A et al (2014) Mechanisms involved in attenuated cardio-protective role of ischemic preconditioning in metabolic disorders. Perfusion 30:94–105. https://doi.org/10.1177/0267659114536760
Feng Y, Hu L, Xu Q et al (2015) Cytoprotective role of alpha-1 antitrypsin in vascular endothelial cell under hypoxia/reoxygenation condition. J Cardiovasc Pharmacol 66:96–107. https://doi.org/10.1097/FJC.0000000000000250
Bhatt LK, Veeranjaneyulu A (2014) Enhancement of matrix metalloproteinase 2 and 9 inhibitory action of minocycline by aspirin: an approach to attenuate outcome of acute myocardial infarction in diabetes. Arch Med Res 45:203–209. https://doi.org/10.1016/j.arcmed.2014.01.008
Gilutz H, Siegel Y, Paran E et al (1983) Alpha1-antitrypsin in acute myocardial infarction. Br Heart J 49:26–29. https://doi.org/10.1136/hrt.49.1.26
Duranton J, Bieth GJ (2003) Inhibition of proteinase-3 by alpha1-antitrypsin in vitro predicts very fast inhibition in vivo. Am J Resp Cell Mol Biol 29:57–61. https://doi.org/10.1165/rcmb.2002-0258OC
Banfi C, Brioschi M, Barcella S et al (2008) Oxidized proteins in plasma of patients with heart failure: role in endothelial damage. Eur J Heart Fail 10:244–251. https://doi.org/10.1016/j.ejheart.2008.01.016
Stockley RA (2014) Alpha1-antitrypsin review. Clin Chest Med 35:39–50. https://doi.org/10.1016/j.ccm.2013.10.001
Abouzaki N, Christopher S, Benjamin CT et al (2018) Inhibiting the inflammatory injury after myocardial ischemia reperfusion with plasma-derived alpha-1 antitrypsin: a post hoc analysis of the VCU-α1RT Study. J Cardiovasc Pharmacol 71:375–379. https://doi.org/10.1097/FJC.0000000000000583
Aoyama T, Chen M, Fujiwara H et al (2000) LOX-1 mediates lysophosphatidylcholine induced oxidized LDL uptake in smooth muscle cells. FEBS Lett 467:217–220. https://doi.org/10.1016/s0014-5793(00)01154-6
Chen M, Kakutani M, Minami M et al (2000) Increased expression of lectin-like oxidized low density lipoprotein receptor-1 in initial atherosclerotic lesions of Watanabe heritable hyperlipidemic rabbits. Arterioscler Thromb Vasc Biol 20:1107–1115
Hu C, Dandapat A, Sun L et al (2008) Regulation of TGFbeta1-mediated collagen formation by LOX-1: studies based on forced overexpression of TGFbeta1 in wild-type and lox-1 knock-out mouse cardiac fibroblasts. J Biol Chem 283:10226–10331. https://doi.org/10.1074/jbc.M708820200
Kataoka H, Kume N, Miyamoto S et al (1999) Expression of lectin-like oxidized low-density lipoprotein receptor-1 in human atherosclerotic lesions. Circulation 99:3110–3117. https://doi.org/10.1161/01.cir.99.24.3110
Lubrano V, Del Turco S, Nicolini G et al (2008) Circulating levels of lectin-like oxidized low-density lipoprotein Receptor-1 are associated with inflammatory markers. Lipids 43:945–950. https://doi.org/10.1007/s11745-008-3227-9
Takaya T, Wada H, Morimoto T et al (2010) Left ventricular expression of lectin-like oxidized low-density lipoprotein receptor-1 in failing hearts. Circ J 74:723–729. https://doi.org/10.1253/circj.cj-09-0488
Yokoyama C, Aoyama T, Ido T et al (2016) Deletion of LOX-1 protects against heart failure induced by doxorubicin. PLoS ONE 11:e0154994. https://doi.org/10.1371/journal.pone.0154994
Iwai-Kanai E, Hasegawa K, Sawamura T et al (2001) Activation of lectin-like oxidized low-density lipoprotein receptor-1 induces apoptosis in cultured neonatal rat cardiac myocytes. Circulation 104:2948–2954. https://doi.org/10.1161/hc4901.100381
Cleutjens JP, Kandala JC, Guarda E et al (1995) Regulation of collagen degradation in the rat myocardium after infarction. J Mol Cell Cardiol 27:1281–1289
Hu C, Chen J, Dandapat A et al (2008) LOX-1 abrogation reduces myocardial ischemia-reperfusion injury in mice. J Mol Cell Cardiol 44:76–83. https://doi.org/10.1016/j.yjmcc.2007.10.009
Li D, Williams V, Liu L et al (2002) LOX-1 inhibition in myocardial ischemia-reperfusion injury: modulation of MMP-1 and inflammation. Am J Physiol Heart Circ Physiol 283:1795–1801. https://doi.org/10.1152/ajpheart.00382.2002
Besli F, Gullulu S, Sag S et al (2016) The relationship between serum lectin-like oxidized LDL receptor-1 levels and systolic heart failure. Acta Cardiol 71:185–190. https://doi.org/10.2143/AC.71.2.3141848
Kobayashi N, Yoshida K, Nakano S et al (2006) Cardioprotective mechanisms of eplerenone on cardiac performance and remodeling in failing rat hearts. Hypertension 47:671–679. https://doi.org/10.1161/01.HYP.0000203148.42892.7a
Schlüter KD, Wolf A, Weber M et al (2017) Oxidized low-density lipoprotein (oxLDL) affects load-free cell shortening of cardiomyocytes in a pro-protein convertase subtilisin/kexin 9 (PCSK9)-dependent way. Basic Res Cardiol 112:63. https://doi.org/10.1007/s00395-017-0650-1
Hu C, Dandapat A, Sun L et al (2008) Modulation of angiotensin II-mediated hypertension and cardiac remodeling by lectin-like oxidized low-density lipoprotein receptor-1 deletion. Hypertension 52:556–562. https://doi.org/10.1161/HYPERTENSIONAHA.108.115287
Chen J, Li D, Schaefer R et al (2006) Cross-talk between dyslipidemia and renin-angiotensin system and the role of LOX-1 and MAPK in atherogenesis studies with the combined use of rosuvastatin and candesartan. Atherosclerosis 184:295–301. https://doi.org/10.1016/j.atherosclerosis.2005.04.016
Chen K, Chen J, Liu Y et al (2005) Adhesion molecule expression in fibroblasts: alteration in fibroblast biology after transfection with LOX-1 plasmids. Hypertension 46:622–627. https://doi.org/10.1161/01.HYP.0000179045.95915.b0
Zhang X, Dong S, Jia Q et al (2019) The MicroRNA in ventricular remodeling: the miR-30 family. Biosci Rep 2:39. https://doi.org/10.1042/BSR20190788
Acknowledgements
The authors are grateful to Dr. Lucrecia Mota and Michael Minks for their English editing support.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lubrano, V., Balzan, S. Role of oxidative stress-related biomarkers in heart failure: galectin 3, α1-antitrypsin and LOX-1: new therapeutic perspective?. Mol Cell Biochem 464, 143–152 (2020). https://doi.org/10.1007/s11010-019-03656-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-019-03656-y