Abstract
Sulforaphane (SFN), a component of dietary cruciferous vegetables has been characterized for its anti-proliferative properties. We have recently demonstrated that pancreatic CSCs display activation of sonic hedgehog pathway which are fundamental drivers of stem cell renewal, and SFN inhibits the self-renewal of pancreatic CSCs in vitro. Consistent with these observations, we sought to determine the chemopreventive potential of SFN in an in vivo setting. We show here for the first time that sulforaphane treatment resulted in a significant reduction in the tumor growth of orthotopically implanted primary pancreatic CSCs isolated from human pancreatic tumors into the pancreas of NOD/SCID/IL2Rgamma mice, which is mediated through the modulation of Sonic hedgehog–GLI signaling. Hedgehog pathway blockade by SFN at a dose of 20 mg/kg resulted in a 45 % reduction in growth of pancreatic cancer tumors and reduced expression of Shh pathway components, Smo, Gli 1, and Gli 2 in mouse tissues. Further, SFN inhibited the expression of pluripotency maintaining transcription factors Nanog and Oct-4 and angiogenic markers VEGF and PDGFRα which are downstream targets of Gli transcription. Furthermore, SFN treatment resulted in a significant reduction in EMT markers Zeb-1, which correlated with increase in E-Cadherin expression suggesting the blockade of signaling involved in early metastasis. Interestingly, SFN downregulated the expression of Bcl-2 and XIAP to induce apoptosis. These data demonstrate that, at a tolerable dose, inhibition of Shh pathway by SFN results in marked reduction in EMT, metastatic, angiogenic markers with significant inhibition in tumor growth in mice. Since aberrant Shh signaling occurs in pancreatic tumorigenesis, therapeutics that target Shh pathway may improve the outcomes of patients with pancreatic cancer by targeting CSCs, thus suggesting the use of sulforaphane to further improve preventive and therapeutic approaches in patients with this devastating disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pancreatic cancer (PC) is the fourth leading cause of cancer related deaths in Western countries, despite intense efforts directed toward improving the therapeutic success in treating pancreatic adenocarcinoma [1]. One of the hallmarks of this devastating disease is the extensive local tumor invasion and early systemic dissemination which very often precedes diagnosis, and is believed to be a major cause of treatment failure in PC [2]. The ability to predict, detect, and prevent aggressive lethal PC in people most at risk, remain as some of the greatest clinical challenges. Therefore, there is an urgent need to discover novel and effective chemopreventive approaches for PC.
Increasing evidence of the existence of cancer stem cells in different solid tumors including pancreatic tumors, offers a smart explanation why standard chemo- or radiotherapy regimens against PC are usually ineffective and result in further tumor recurrence and spreading [3–6]. Although CSCs comprise only a small fraction of a tumor, they have the capacity to self-renew and produce progeny that can expand or repopulate tumor bulk [7, 8]. The CSC hypothesis suggests a new understanding of pancreatic carcinogenesis thus offering new strategies for PC prevention and therapy [9]. Therefore, development of therapeutic strategies that specifically target pancreatic CSCs can be effective in eradicating tumors and in reducing the risk of relapse and metastasis.
It is well known that sonic hedgehog signaling pathway plays a vital role during embryonic development. Sonic hedgehog activates a signal transduction cascade that includes the action of membrane proteins Patched (PTCH1) and Smoothened (SMOH), which then activates the canonical Hh pathway through Gli-dependent transcription of multiple targets, including Nanog, Cyclin D1, Ptch, Gli1, and Gli2. Upregulation of sonic hedgehog pathway has been linked to the development of several cancers including PC [10, 11]. Activation of Shh signaling seems to precede transformation of pancreatic tissue stem cells to pancreatic cancerous stem cells, with Gli transcription factor functioning as a mediator of environmental signals and in the progression of pancreatic CSCs into metastatic tumor cells. Since Hh plays a critical role in the renewal of cancer stem cells, Hedgehog pathway blockade has evolved as a promising therapy for various types of cancers including PC [12–14].
Organosulfur compounds such as isothiocyanates (ITCs) are abundantly found in cruciferous vegetables and have been shown to exhibit several potential chemoprotective activities in cell and animal models [15–18]. ITCs have been shown to be potent inhibitors of mammary, lung, and liver carcinogenesis induced by environmental and dietary carcinogens in rodent models [19–22]. Based on the literature review, sulforaphane (SFN) is an ITC found to exist as conjugates in the genus Brassica of cruciferous vegetables, and has been shown to inhibit the malignant growth in cancer cells of various origins with little or no toxicity toward normal cells [16, 22–28]. Thus, SFN holds great promise for development as a chemopreventive/therapeutic agent.
Our previous work provided evidence for a role of HH–GLI signaling in PC stem cells [29, 30]. Gli RNA interference demonstrated the general requirement of Gli1 and Gli2 in pancreatic CSC proliferation; further, SFN inhibited the self-renewal of pancreatic CSCs in vitro [31] [23]. Consistent with these observations, we sought to determine the effects of SFN in an in vivo setting. In the present study, we have investigated the chemopreventive potential of sulforaphane to inhibit the growth of pancreatic CSCs orthotopically implanted in the pancreas of NOD/SCID/IL2Rgamma mice. These mice were administered SFN by oral gavage with 0–20 mg/kg SFN. Here we demonstrate that human PC stem cells require HH-GLI pathway activity for proliferation, survival, self-renewal, and tumorigenicity. Furthermore, SFN treatment resulted in a significant reduction in tumor growth and was asssociated with reduced cell proliferation. The immunohistochemical and molecular analysis of tumor tissue thus obtained suggest that the anti-cancer efficacy of SFN was mediated through the modulation of Sonic hedgehog–GLI signaling. Our results thus argue that for the development of sulforaphane as a novel strategy for PC prevention and therapy that specifically target pancreatic CSCs can be effective in eradicating tumors and in reducing the risk of relapse and metastasis.
These findings deepen the concept that Hedgehog signaling is a fundamental driver of tumor self-renewal in PC and that Hedgehog pathway blockade by SFN is a promising novel strategy for prevention as well as treatment of the deadly, recurrent, and unresectable forms of PC.
Materials and methods
Reagents
Antibodies against GAPDH, Gli1, Gli2, and Smo, Nanog, VEGF, BCL2, Zeb1, E-Cadherin, and Ki-67 were purchased from Cell Signaling Technology, Inc. (Danvers, MA). SFN were purchased from LKT Laboratories, Inc. (St. Paul, MN). Enhanced chemiluminescence (ECL) Western blot detection reagents were from Amersham Life Sciences Inc. (Arlington Heights, IL). Terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling (TUNEL) assay kit was purchased from EMD Biosciences/Calbiochem. All other chemicals were purchased from Sigma-Aldrich (St Louis, MO).
Cell culture
Human PC stem cells (CD133+/CD44+/CD24+/ESA+) were obtained from Celprogen Inc. (San Pedro, CA). They were isolated from the primary tumors and have been described previously [27]. These CSCs consist of a bulk PC stem cell population, and thus cannot be considered as a cell line. The CSCs were cultured in DMEM supplemented with 1 % N2 Supplement (Invitrogen), 2 % B27 Supplement (Invitrogen), 20 ng/ml human platelet growth factor (Sigma-Aldrich), 100 ng/ml epidermal growth factor (Invitrogen), and 1 % antibiotic–antimycotic (Invitrogen) at 37 °C in a humidified atmosphere of 95 % air and 5 % CO2.
Orthotopic assays in NOD/SCID/IL2Rgamma mice
All the mice experiments were approved by University of Kansas Medical Center Institutional Animal Care and Use Committee. Male NOD/SCID/IL2Rgamma mice (4–6 weeks old) were purchased from Jackson Laboratories. The mice were anesthetized and the surgical site is shaved. The surgical site is scrubbed with three alternate scrubs of 70 % ethanol, followed by betadine, and placed in a supine position. The peritoneum is opened along the anatomical path given by the injection site and the pancreas is exposed. The wall of the pancreas is retracted with cotton tip to give slight pressure. In order to establish tumors, in vivo pancreatic CSC’s isolated from the human primary pancreatic tumors with CD133+/CD44+/CD24+/ESA+ immunophenotype (1 × 103 cells mixed with matrigel in 50 μl total volume, 50:50 ratio) were orthotopically implanted in the pancreas of NOD/SCID/IL2Rgamma mice to the insertion of a 27-gauge needle. A successful injection is defined by no apparent spillage of the cell suspension into the peritoneal cavity and the presence of a distinct tissue bleb at the injection site that contains the injected volume. The body wall is sutured using a running suture of 5-0 silk and the skin is then closed with surgical clips. One week post surgery, these mice were randomized into two groups of 8 mice each, and the following treatment protocols were implemented: group 1: vehicle control (0.1 ml normal saline containing 0.5 % DMSO) administered by gavage, everyday 5 days a week throughout the duration of experiment; group 2: sulforaphane (20 mg/kg in 0.1 ml normal saline containing 0.5 % DMSO) administered by gavage, everyday 5 days a week throughout the duration of experiment. After 6 weeks of treatment, the mice were sacrificed and the pancreatic tumors were harvested and the total weight of pancreatic tumors was measured.
Western blot analysis
Western blots were performed as we described elsewhere [32, 33]. In brief, cells were lysed in RIPA buffer containing 1× protease inhibitor cocktail, and protein concentrations were determined using the Bradford assay (Bio-Rad, Philadelphia, PA). Proteins were separated by 12.5 % SDS/PAGE and transferred to membranes (Millipore, Bedford, MA) at 55 V for 4 h at 4 °C. After blocking in 5 % non-fat dry milk in TBS, the membranes were incubated with the primary antibodies at 1:1,000 dilution in TBS overnight at 4 °C, washed three times with TBS-Tween 20, and then incubated with the secondary antibodies conjugated with horseradish peroxidase at 1:5,000 dilution in TBS for 1 h at room temperature. Membranes were washed again in TBS-Tween 20 for three times at room temperature. Protein bands were visualized on X-ray film using an enhanced chemiluminescence detection system.
Isolation of RNA
Tumor tissues were cryopreserved and the total RNA was extracted using Trizol (Life Technologies) according to the manufacturer’s instructions. The RNA pellets were then frozen and stored at −80 °C until use.
Evaluation of mRNA expression levels by quantitative real-time PCR
For the quantification of gene amplification, real-time PCR was performed using an ABI 7300 Sequence Detection System in the presence of SYBR- Green. Briefly, RNA was isolated and reverse transcribed. cDNA reactions were amplified with QPCR SYBR Green Mix (Applied Biosystems). The following gene-specific primers were used:
-
Nanog (5′-ACC TAC CTA CCC CAG CCT TT-3′, 5′-CAT GCA GGA CTG CAG AGA TT-3′)
-
Oct4 (5′-GGA CCA GTG TCC TTT CCT CT-3′, 5′-CCA GGT TTT CTT TCC CTA GC-3′)
-
Smothened (5′-TCG CTA CCC TGC TGT TAT TC-3′, 5′-GAC GCA GGA CAG AGT CTC AT-3′)
-
Gli1 (5′-CTG GAT CGG ATA GGT GGT CT-3′, 5′-CAG AGG TTG GGA GGT AAG GA-3′)
-
Gli2 (5′-GCC CTT CCT GAA AAG AAG AC-3′, 5′-CAT TGG AGA AAC AGG ATT GG-3′)
-
PDGFRα (5′-CCA GCA GTT TCC AGT CCT AA-3′, 5′-ACA GAT TGG CAG ACC ACA TT-3′)
-
Cyclin D1 (5′-TTC AAA TGT GTG CAG AAG GA-3′, 5′-GGG ATG GTC TCC TTC ATC TT-3′
-
ZEB1 (5′-GCA CAA CCA AGT GCA GAA GA-3′, 5′-CAT TTG CAG ATT GAG GCT GA-3′)
-
E-Cadherin (5′-TGC TCT TGC TGT TTC TTC GG-3′, 5′-TGC CCC ATT CGT TCA AGT AG-3′)
-
Bcl-2 (5′-AGA TGG GAA CAC TGG TGG AG-3′, 5′-TCT TCA CCT CCA GGC TCA GT-3′)
-
XIAP (5′-GGG TTT GTC TTG ACC TGG AA-3′, 5′-CTC CCA AAG TGC TGG GAT TA-3′)
-
HK-GAPD (5′-GAG TCA ACG GAT TTG GTC GT-3′, 5′-TTG ATT TTG GAG GGA TCT CG-3′)
Target sequences were amplified at 95 °C for 10 min, followed by 40 cycles of 95 °C for 15 s and 60 °C for 1 min. HK-GAPD was used as endogenous normalization control. All assays were performed in triplicate and were calculated on the basis of ΔΔCt method. The n-fold change in mRNAs expression was determined according to the method of 2−ΔΔCT.
Immunohistochemistry
Tumor samples were formalin fixed and paraffin embedded. Serial sections of 5 μM were deparaffinized and rehydrated through an alcohol gradient to water and subject to heat-induced antigen retrieval in 10 mM citrated for 20 min. The primary antibodies to human GLI1, GLI2, Smo, Nanog, VEGF, BCL2, Zeb1, E-Cadherin, and Ki-67 were incubated overnight at 4 °C. IGg antibody were used on control sections. Antibody binding was detected with DAB. TUNEL staining was used to detect apoptotic cells in tissue sections, using the DeadEnd™ Colorimetric TUNEL System, (Promega, Madison, WI) detection kit, according to the manufacturer’s instructions and proliferation was evaluated by immunostaining using antibodies against Ki-67.
Statistical analysis
The mean and SD were calculated for each experimental group. Differences between groups were analyzed by one- or two-way ANOVA followed by Bonferroni’s multiple comparison tests using PRISM statistical analysis software (GraphPad Software). Significant differences among groups were calculated at P < 0.05.
Results
Sulforaphane inhibits the growth of pancreatic CSCs orthotopically implanted in NOD/SCID mice by inhibiting Shh pathway
We have recently demonstrated the characterization of pancreatic CSC’s isolated from human pancreatic tumors [32]. Pancreatic CSC’s with CD133+ CD44+ CD24+ ESA+ immunophenotype were highly tumorigenic and formed tumors when sc injected into NOD/SCID mice. In another study we have recently shown that in an in vitro cell culture model, pancreatic CSCs derived spheres were significantly inhibited on treatment with SFN, suggesting the clonogenic depletion of the cancer stem cells by SFN. The clonogenic assay showed that SFN (0–10 μM) inhibited the pancreatic CSC growth in vitro in a dose-dependent manner [23]. We next validated our in vitro data in a pancreatic CSC orthotopic model, to further understand the regulation of Shh pathway in pancreatic CSCs by SFN in an in vivo setting.
To this end, pancreatic CSC’s isolated from the human primary pancreatic tumors with CD133+ CD44+ CD24+ ESA+ immunophenotype (1 × 103 cells mixed with matrigel in 50 μl total volume) were orthotopically implanted in NOD/SCID/IL2Rgamma mice and eight mice per group were treated with SFN (0–20 mg/kg body weight) administered through oral gavage once daily, five times a week for 6 weeks. Based on our previously reported in vitro study, that SFN inhibited pancreatic CSC spheroid formation and induced apoptosis [23] and other published literature examining the effects of sulforaphane in PC [34, 35], we elected to test 20 mg/kg dose of SFN in the current study. After 6 weeks of treatment, the mice were sacrificed and the pancreatic tumors were harvested and the total weight of the pancreatic tumors was measured. No apparent toxicity in SFN treated mice to normal organs was noted. Further, no insignificant effect in the overall weight or health of the mice treated with SFN compared to saline treated controls was observed in this study.
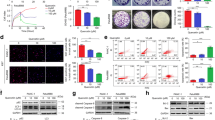
As shown in Fig. 1a, SFN significantly inhibited the growth of pancreatic tumor upon implantation of pancreatic CSC’s in the pancreas of NOD/SCID/IL2Rgamma mice. Treatment of mice with SFN at a dose of 20 mg/kg resulted in a 45 % reduction in growth of PC tumors. We next examined the effects of SFN on cell proliferation and apoptosis in tumor tissues derived from control and SFN treated mice (Fig. 1b, c) using Ki-67 and Tunnel antibodies, respectively. The data demonstrate that SFN inhibits the cell proliferation and induces apoptosis in tumor tissues.
Effect of SFN on the tumorigenic potential of human pancreatic CSC’s isolated from human primary pancreatic tumors. SFN inhibits the growth of PCSC tumors orthotopically implanted in NOD/SCID mice by inhibiting Shh pathway. a CSCs were orthotopically implanted into the pancreas of NOD/SCID mice. Tumor bearing mice were treated with SFN (0–20 mg/kg body weight) through gavage (Monday to Friday, once daily) for 6 weeks. At the end of the experiment, pancreatic tumor weights were recorded. Data represents the mean ± SD. $Significantly different from control, P < 0.05. The mean and SD were calculated for each experimental group. Differences between groups were analyzed by one- or two-way ANOVA followed by Bonferroni’s multiple comparison tests using PRISM statistical analysis software (GraphPad Software). Significant differences among groups were calculated at P < 0.05. b, c Effects of SFN on cell proliferation and apoptosis in tumor tissues. Immunohistochemistry was performed in tumor tissues obtained from control and SFN treated mice. Cell proliferation was measured by Ki67 staining, and apoptosis was measured by TUNEL assay. The total number of Ki-67 positive and TUNEL positive cells were quantified in tissues of both groups. Data represents mean ± SD. *Significantly different from control, P < 0.05
With the aim to investigate whether the effects of SFN is mediated by the inhibition of Shh pathway in vivo in a pancreatic CSC orthotopic model by modulating the expressions of Gli transcription factors, rather than noncanonical effects on Hh signaling or nonspecific toxicity, we next measured the mRNA levels of Gli transcription factors in the pancreatic tumor tissues obtained from the Control and SFN treated mice. Hedgehog pathway blockade by SFN inhibited the mRNA expression levels of Gli1 and Gli2 (Fig. 2a). Interestingly, the mRNA level of Smo was also significantly reduced in pancreatic tumor tissues obtained from SFN treated mice (Fig. 2a). Furthermore, pancreatic tumor tissues obtained from the Control and SFN treated mice were examined to measure the protein expression of Gli1 and Gli2 and Smo using immuno-histochemistry and western blotting. As shown in (Fig. 2b, c), we observed a significant inhibition in expression of these proteins in tissues obtained from SFN treated mice as compared to control mice. We thus conclude that Hedgehog pathway blockade by SFN significantly inhibits growth of pancreatic CSC’s to form tumors in NOD/SCID/IL2Rgamma mice.
Regulation of Shh pathway by SFN in pancreatic CSCs in vivo. a Effects of SFN on components of Shh components in tumor tissues. Real-time PCR (q-RT-PCR) was performed to examine the expression of Smo, Gli1, and Gli2 and normalized with GAPDH in tissues derived RNA from control and SFN treated mice. Data represents mean ± SD. #Significantly different from control, P < 0.05. The results are an average of two independent experiments carried out in triplicate. b, c Effects of SFN on the protein expression of Smo, Gli1, and Gli2 were examined in tumor tissues by immunohistochemistry and western blotting obtained from control and SFN treated mice
SFN inhibits the expression of downstream targets genes of Shh pathway involved in maintaining pluripotency
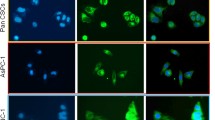
In an attempt to identify a link between HH–GLI signaling and stemness, we further characterized the effects of SFN on downstream transcription targets of Shh signaling pathway in vivo. The mRNA expression level of Hh target genes Oct4 and Nanog, involved in maintaining the pluripotency, was analyzed in the tumor tissues from control and SFN treated mice. As shown in (Fig. 3a, b), SFN inhibited the mRNA expression of Oct4 and Nanog in pancreatic CSCs orthotopic tumors. These data suggest that Oct4 and Nanog, which are essential for pluripotency, are also critical for PC stem cells and may be susceptible to Hh blockade.
Regulation of Hh target genes involved in the maintenance of pluripotency, proliferation, and invasion by SFN in pancreatic cancer stem cells. a–d Effects of SFN on expression of Hh target genes in the tumor tissues. Real-time PCR (q-RT-PCR) was performed to examine the expression of Oct4 and Nanog, involved in the maintenance of pluripotency, as well as expression of PDGFRα and VEGF involved in proliferation and invasion, respectively, in the tumor tissues from control and SFN treated mice and normalized with GAPDH. Data represents mean ± SD. #Significantly different from control, P < 0.05. The results are an average of two independent experiments carried out in triplicate. e Effects of SFN on the protein expression of Oct4, Nanog, PDGFRα, and VEGF were assessed by Immunohistochemical analysis of tumor tissues derived from control and SFN treated mice
SFN inhibits the expression of downstream targets genes of Shh pathway involved in maintaining cell proliferation, angiogenesis, and induction of apoptosis in tumor tissues
Furthermore, the expression of Hh target genes PDGFRα and VEGF involved in the proliferation and invasion was analyzed in the tumor tissues from control and SFN treated mice. The expression of PDGRFα and VEGF in tissues obtained from SFN treated group was significantly inhibited as compared to the control group (Fig. 3c, d), suggesting that sulforaphane can regulate pancreatic carcinogenesis by inhibiting Shh pathway and its downstream targets involved in proliferation and angiogenesis. The protein expression of downstream targets of Gli transcription, Oct4, Nanog, PDGFRα, and VEGF was further confirmed by immunohistochemistry of the mice tissues obtained from both the groups as shown in Fig. 3e.
As previously described in (Fig. 1b, c), we had observed that SFN inhibits the cell proliferation and induces apoptosis in tumor tissues derived from control and SFN treated mice using Ki-67 and tunnel antibodies, respectively. Since Bcl-2 and members of the IAP play important roles in cell survival and apoptosis [36], we sought to examine the effects of SFN on the expression of BCL2 and XIAP in pancreatic CSCs derived pancreatic tumors. Real-time PCR (q-RT-PCR) was performed to examine the expression of BCL2 and XIAP in the tumor tissues from control and SFN treated mice. As shown in Fig. 4a, the expression of BCL2 and XIAP was significantly inhibited in SFN treated mice as compared to control mice. The expression of BCL2 in pancreatic tumor tissues from both the group of mice was further confirmed by immunohistochemistry (Fig. 4c). These data suggest that SFN can induce apoptosis in CSCs by engaging cell-intrinsic pathway of apoptosis.
Regulation of apoptosis-related proteins and epithelial-mesenchymal transition factors by SFN in Pancreatic CSCs in vivo. a Real-time PCR (q-RT-PCR) was performed to examine the expression of BCL2 and XIAP involved in apoptosis, in the tumor tissues derived from control and SFN treated mice. RNA obtained from the tumor tissues was analyzed using Sybr Green for the expression of BCl2 and XIAP and normalized with GAPDH. Data represents mean ± SD. #Significantly different from control, P < 0.05. The results are an average of two independent experiments carried out in triplicate. b Regulation of epithelial-mesenchymal transition by SFN in pancreatic CSCs in vivo. In order to examine the effects of SFN on EMT markers, real-time PCR (q-RT-PCR) was performed to examine the expression of Zeb1 and E-Cadherin in the tumor tissues from control and SFN treated mice and normalized with GAPDH. Data represent mean ± SD. #Significantly different from control, P < 0.05. The results are an average of two independent experiments carried out in triplicate. c Effects of SFN on the protein expression of BCl2, Zeb1, and E-Cadherin was examined by immunohistochemical analysis of tumor tissues derived from control and SFN treated mice
Sulforaphane inhibits the marker of epithelial–mesenchymal transition markers (EMT) in human pancreatic CSCs
EMT plays a crucial role in tumorigenesis and cancer progression [37]. Recent studies have revealed that there is a direct link between the EMT program and the gain of epithelial stem cell properties. EMT is sufficient to induce a population with stem cell characteristics from well-differentiated epithelial cells and cancer cells [38]. Cancer stem cells undergoing metastasis usually express EMT markers. We, therefore, examined the effects of SFN on the mRNA and protein expression of EMT markers in pancreatic tumor tissues derived from SFN treated and control mice. The mRNA expression of Zeb-1 in the mouse tissue obtained from the SFN treated group as compared to that obtained from the control group was significantly reduced, as determined by qRT-PCR (Fig. 4b). Since these transcription factors impact on cell–cell contact formation as well as cell migration [39–41] and are a transcriptional repressor of E-cadherin, we thus reasoned that sulforaphane may regulate the metastasis of pancreatic CSCs by inhibiting the expression of Zeb-1 transcription factor which is involved in the epithelial-to-mesenchymal transition in CSCs by regulating E-Cadherin expression. Thus, we examined the effects of sulforaphane on the expression of E-cadherin. Interestingly, SFN induced the mRNA expression of E-cadherin (Fig. 4b). The changes of Zeb1 and E-Cadherin protein levels were further confirmed by immunohistochemical analysis of the tumor tissue obtained from SFN treated and control mice (Fig. 4c). These data thus suggest that SFN can inhibit early metastasis of pancreatic CSCs.
Discussion
Pancreatic adenocarcinoma is almost universally unresponsive to many conventional therapies. In attempts to treat the disease, the tumor becomes chemoresistant resulting in the poor prognosis of most PC patients [42, 43]. The existence of rare subset of cancer stem cells in pancreatic tumors, offers a plausible explanation for the development of the resistance to standard therapies and tumor recurrence, which eventually tend to dominate the content of the tumor [3, 44, 45]. The most beneficial aspect of applying the stem cell biology to PC research is the resulting conceptual advance with respect to discovering therapeutics targeting specifically the tumorigenic CSCs to result in tumor eradication and prevention of metastasis. This will require identification of realistic drug targets unique to cancer stem cells.
Sonic hedgehog (Shh) is one of the three HH ligands of the Hedgehog (Hh) family of secreted signaling proteins reported to play an essential role in the progression and maintenance of pancreatic adenocarcinomas [46]. Pancreatic CSCs expressing stem cell markers CD133, CD44, CD24, and ESA express high levels of pluripotency maintaining factors, and drug resistance genes MDR1 and ABCG2 as compared to normal pancreatic cells and PC cells [29, 32, 47]. We have recently shown that activation of Shh signaling pathway is involved in regulating the proliferation of the human pancreatic CSCs. In the present study, we demonstrate that blockade of the Shh pathway by SFN suppressed the tumor self-renewal of human pancreatic CSCs orthotopically implanted in pancreas of NOD/SCID/IL2R gamma mice, which resulted in 45 % inhibition in the growth of tumors in SFN treated group of mice as compared to control group. No apparent toxicity to CNS, liver, and kidneys in mice treated with SFN were noted as well as no insignificant effect in the overall weight or health of the mice treated with SFN compared to saline treated controls was observed in this study. The Gli family is one of the target gene consistently induced whenever the Shh pathway is activated, making this transcript a reliable marker of both physiologic and pathologic Shh signaling activity [48]. Therefore, we examined the expression of Gli 1 and Gli 2 in the pancreatic tumor tissues obtained from the control and SFN treated mice. Sulforaphane inhibited the mRNA and protein expression levels of Gli1 and Gli2 (Fig. 2a–c). Interestingly, the mRNA level of Smo was also significantly reduced in pancreatic tumor tissues obtained from SFN treated mice. These findings deepen the concept that Hedgehog signaling is a fundamental driver of tumor self-renewal in PC, thus Hedgehog pathway blockade by SFN is a promising novel treatment strategy for deadly, recurrent, and unresectable forms of PC.
Epithelial-to-mesenchymal transition (EMT) is an embryonic program in which epithelial cells lose their characteristics and gain mesenchymal features. Accumulating evidence suggests that EMT plays an important role during malignant tumor progression [49, 50]. Furthermore, transformed epithelial cells can activate embryonic programs of epithelial plasticity and switch from a sessile, epithelial phenotype to a motile, mesenchymal phenotype. Induction of EMT can, therefore, lead to invasion of surrounding stroma, intravasation, dissemination, and colonization of distant sites. It is believed that sustained metastatic growth requires the dissemination of a CSC from the primary tumor followed by its re-establishment in a secondary site. Thus, EMT can confer metastatic ability on carcinomas. In the present study, SFN inhibited the expression of transcription factor ZEB1 required for inducing EMT in pancreatic CSCs. This transcription factor impact on cell–cell contact formation as well as cell migration and is a transcriptional repressor of E-cadherin [51]. Thus we examined the effect of SFN on the expression of E-Cadherin. We observed an induced expression of E-cadherin in tumor tissues obtained from SFN treated mice, suggesting a potential role of SFN in the blockade of signaling involved in early metastasis. This was consistent with the inhibition of epithelial-to-mesenchymal transition and was mirrored by a striking reduction in the invasive capacity of tumor cells as exhibited with a marked reduction in expression of Hh target genes PDGFRα, VEGF, and cyclin D involved in the proliferation and invasion. Furthermore, SFN treatment led to an increased rate of apoptotic death. SFN induced apoptosis by inhibiting Bcl-2 and XIAP as demonstrated from the decreased expression of the antiapoptotic proteins. These studies strongly suggest that SFN is a potent biologic inhibitor of human pancreatic carcinogenesis, reducing their proliferative and invasive activities.
Thus, agents that inhibit Shh pathway have the potential to prevent disease progression and metastatic spread. As well as drugs that selectively target CSCs offer a greater promise for cancer prevention and therapy. Sulforaphane is a naturally occurring isothiocyanate with promising chemopreventive activity [52–55]. It acts as an antioxidant, antiproliferative, antitumor, and anti-angiogenic agent, and thus a novel candidate for chemoprevention [27, 28]. SFN has been shown to inhibit progression and retard the growth of tumors of various origins including breast, prostate, pancreas and multiple myeloma and has been shown to inhibit HDAC activity in human subjects [18, 26, 35, 53, 56, 57]. To the best of our knowledge this is the first study to show that sulforaphane can inhibit the growth of pancreatic tumors in mice upon orthotopic implantation of the primary pancreatic CSC derived from human tumors. Our present studies strongly suggest that sulforaphane can modulate the expression of genes known to play roles in the carcinogenesis process involved in PC and, therefore, may be a potential agent for chemoprevention against PC. Elucidation of the mechanism(s) for antiproliferative activity of SFN is critical to overall assessment for their potential clinical utility. Since CSCs/progenitor cells play major roles in cancer initiation, progression, recurrence, and drug resistance, inhibition of CSC growth and their self-renewal capacity in vivo by sulforaphane could be significant for the management of PC.
In summary, in this study we have demonstrated for the first time that cancer preventive agent SFN potently eliminates the self-renewal characteristics of pancreatic CSC isolated from the human primary tumors in vivo, by significantly inhibiting the growth of tumors on orthotopically implanting human pancreatic CSC’s in the pancreas of NOD/SCID/IL2Rgamma mice. We have shown that the inhibitory effects of SFN are mediated by the modulation of Shh pathway. SFN inhibits the expression of Smo, as well as effector molecule Gli 1 and 2, suggesting the clinical significance of Shh pathway in PC. Further, SFN inhibited the expression of transcription factors Nanog and Oct-4 which are required for maintaining stem-cell pluripotency and are downstream targets of Gli. Moreover, SFN inhibited expression of proteins downstream of Gli, involved in the apoptosis resistance, proliferation, angiogenesis, and EMT, thus suggesting the blockade of signaling involved in early metastasis. These findings deepen the concept that Hedgehog signaling is a fundamental driver of tumor self-renewal in PC, thus Hedgehog pathway blockade by non-toxic agent SFN could be considered as a novel strategy for the treatment and/or prevention of PC. Taken together our present studies strongly suggest that SFN is a potent biologic inhibitor of human pancreatic carcinogenesis, reducing their proliferative and invasive activities.
References
Jemal A, Siegel R, Xu J, Ward E (2010) Cancer statistics, 2010. CA Cancer J Clin 60:277–300. doi:10.3322/caac.20073
Rosewicz S, Wiedenmann B (1997) Pancreatic carcinoma. Lancet 349:485–489
Hermann PC, Huber SL, Herrler T, Aicher A, Ellwart JW, Guba M, Bruns CJ, Heeschen C (2007) Distinct populations of cancer stem cells determine tumor growth and metastatic activity in human pancreatic cancer. Cell Stem Cell 1:313–323. doi:10.1016/j.stem.2007.06.002
Shah AN, Summy JM, Zhang J, Park SI, Parikh NU, Gallick GE (2007) Development and characterization of gemcitabine-resistant pancreatic tumor cells. Ann Surg Oncol 14:3629–3637. doi:10.1245/s10434-007-9583-5
Hermann PC, Bhaskar S, Cioffi M, Heeschen C (2010) Cancer stem cells in solid tumors. Semin Cancer Biol 20:77–84. doi:10.1016/j.semcancer.2010.03.004
Hermann PC, Mueller MT, Heeschen C (2009) Pancreatic cancer stem cells—insights and perspectives. Expert Opin Biol Ther 9:1271–1278. doi:10.1517/14712590903246362
Reya T, Morrison SJ, Clarke MF, Weissman IL (2001) Stem cells, cancer, and cancer stem cells. Nature 414:105–111. doi:10.1038/35102167
Al-Hajj M, Clarke MF (2004) Self-renewal and solid tumor stem cells. Oncogene 23:7274–7282. doi:10.1038/sj.onc.1207947
Ischenko I, Seeliger H, Kleespies A, Angele MK, Eichhorn ME, Jauch KW, Bruns CJ (2010) Pancreatic cancer stem cells: new understanding of tumorigenesis, clinical implications. Langenbecks Arch Surg 395:1–10. doi:10.1007/s00423-009-0502-z
Thayer SP, di Magliano MP, Heiser PW, Nielsen CM, Roberts DJ, Lauwers GY, Qi YP, Gysin S, Fernandez-del Castillo C, Yajnik V, Antoniu B, McMahon M, Warshaw AL, Hebrok M (2003) Hedgehog is an early and late mediator of pancreatic cancer tumorigenesis. Nature 425:851–856
Tian H, Callahan CA, DuPree KJ, Darbonne WC, Ahn CP, Scales SJ, de Sauvage FJ (2009) Hedgehog signaling is restricted to the stromal compartment during pancreatic carcinogenesis. Proc Natl Acad Sci USA 106:4254–4259. doi:10.1073/pnas.0813203106
Chen X, Horiuchi A, Kikuchi N, Osada R, Yoshida J, Shiozawa T, Konishi I (2007) Hedgehog signal pathway is activated in ovarian carcinomas, correlating with cell proliferation: it’s inhibition leads to growth suppression and apoptosis. Cancer Sci 98:68–76. doi:10.1111/j.1349-7006.2006.00353.x
Chen JK, Taipale J, Cooper MK, Beachy PA (2002) Inhibition of Hedgehog signaling by direct binding of cyclopamine to smoothened. Genes Dev 16:2743–2748. doi:10.1101/gad.1025302
Olive KP, Jacobetz MA, Davidson CJ, Gopinathan A, McIntyre D, Honess D, Madhu B, Goldgraben MA, Caldwell ME, Allard D, Frese KK, Denicola G, Feig C, Combs C, Winter SP, Ireland-Zecchini H, Reichelt S, Howat WJ, Chang A, Dhara M, Wang L, Ruckert F, Grutzmann R, Pilarsky C, Izeradjene K, Hingorani SR, Huang P, Davies SE, Plunkett W, Egorin M, Hruban RH, Whitebread N, McGovern K, Adams J, Iacobuzio-Donahue C, Griffiths J, Tuveson DA (2009) Inhibition of Hedgehog signaling enhances delivery of chemotherapy in a mouse model of pancreatic cancer. Science 324:1457–1461. doi:10.1126/science.1171362
Jeong WS, Kim IW, Hu R, Kong AN (2004) Modulatory properties of various natural chemopreventive agents on the activation of NF-kappaB signaling pathway. Pharm Res 21:661–670
Clarke JD, Dashwood RH, Ho E (2008) Multi-targeted prevention of cancer by sulforaphane. Cancer Lett 269:291–304. doi:10.1016/j.canlet.2008.04.018
Gills JJ, Jeffery EH, Matusheski NV, Moon RC, Lantvit DD, Pezzuto JM (2006) Sulforaphane prevents mouse skin tumorigenesis during the stage of promotion. Cancer Lett 236:72–79. doi:10.1016/j.canlet.2005.05.007
Hunakova L, Sedlakova O, Cholujova D, Gronesova P, Duraj J, Sedlak J (2009) Modulation of markers associated with aggressive phenotype in MDA-MB-231 breast carcinoma cells by sulforaphane. Neoplasma 56:548–556
Nguyen N, Sharma A, Sharma AK, Desai D, Huh SJ, Amin S, Meyers C, Robertson GP (2011) Melanoma chemoprevention in skin reconstructs and mouse xenografts using isoselenocyanate-4. Cancer Prev Res (Phila) 4:248–258. doi:10.1158/1940-6207.CAPR-10-0106
Wang LG, Chiao JW (2010) Prostate cancer chemopreventive activity of phenethyl isothiocyanate through epigenetic regulation (review). Int J Oncol 37:533–539
Tang L, Zirpoli GR, Jayaprakash V, Reid ME, McCann SE, Nwogu CE, Zhang Y, Ambrosone CB, Moysich KB (2010) Cruciferous vegetable intake is inversely associated with lung cancer risk among smokers: a case-control study. BMC Cancer 10:162. doi:10.1186/1471-2407-10-162 1471-2407-10-162[pii]
Kang L, Wang ZY (2010) Breast cancer cell growth inhibition by phenethyl isothiocyanate is associated with down-regulation of oestrogen receptor-alpha36. J Cell Mol Med 14:1485–1493. doi:10.1111/j.1582-4934.2009.00877.x
Srivastava RK, Tang SN, Zhu W, Meeker D, Shankar S (2011) Sulforaphane synergizes with quercetin to inhibit self-renewal capacity of pancreatic cancer stem cells. Front Biosci (Elite Ed) 3:515–528
Hahm ER, Singh SV (2010) Sulforaphane inhibits constitutive and interleukin-6-induced activation of signal transducer and activator of transcription 3 in prostate cancer cells. Cancer Prev Res (Phila) 3:484–494. doi:10.1158/1940-6207.CAPR-09-0250
Haristoy X, Angioi-Duprez K, Duprez A, Lozniewski A (2003) Efficacy of sulforaphane in eradicating Helicobacter pylori in human gastric xenografts implanted in nude mice. Antimicrob Agents Chemother 47:3982–3984
Myzak MC, Tong P, Dashwood WM, Dashwood RH, Ho E (2007) Sulforaphane retards the growth of human PC-3 xenografts and inhibits HDAC activity in human subjects. Exp Biol Med (Maywood) 232:227–234
Srivastava RK, Tang SN, Zhu W, Meeker D, Shankar S (2011) Sulforaphane synergizes with quercetin to inhibit self-renewal capacity of pancreatic cancer stem cells. Front Biosci (Elite Ed) 3:515–528
Yu D, Sekine-Suzuki E, Xue L, Fujimori A, Kubota N, Okayasu R (2009) Chemopreventive agent sulforaphane enhances radiosensitivity in human tumor cells. Int J Cancer 125:1205–1211. doi:10.1002/ijc.24480
Tang SN, Fu J, Nall D, Rodova M, Shankar S, Srivastava RK (2012) Inhibition of sonic hedgehog pathway and pluripotency maintaining factors regulate human pancreatic cancer stem cell characteristics. Int J Cancer 131:30–40. doi:10.1002/ijc.26323
Singh BN, Fu J, Srivastava RK, Shankar S (2011) Hedgehog signaling antagonist GDC-0449 (Vismodegib) inhibits pancreatic cancer stem cell characteristics: molecular mechanisms. PLoS One 6:e27306. doi:10.1371/journal.pone.0027306
Rodova M, Fu J, Nalls D, Srivastava RK, Shankar S (2012) Sonic hedgehog signaling inhibition provides opportunities for targeted therapy by sulforaphane in regulating pancreatic cancer stem cell self-renewal. PLoS One 7:e46083
Shankar S, Nall D, Tang SN, Meeker D, Passarini J, Sharma J, Srivastava RK (2011) Resveratrol inhibits pancreatic cancer stem cell characteristics in human and kras transgenic mice by inhibiting pluripotency maintaining factors and epithelial–mesenchymal transition. PLoS One 6:e16530. doi:10.1371/journal.pone.0016530
Tang SN, Singh C, Nall D, Meeker D, Shankar S, Srivastava RK (2010) The dietary bioflavonoid quercetin synergizes with epigallocathechin gallate (EGCG) to inhibit prostate cancer stem cell characteristics, invasion, migration and epithelial–mesenchymal transition. J Mol Signal 5:14. doi:10.1186/1750-2187-5-14
Li Y, Zhang T, Schwartz SJ, Sun D (2011) Sulforaphane potentiates the efficacy of 17-allylamino 17-demethoxygeldanamycin against pancreatic cancer through enhanced abrogation of Hsp90 chaperone function. Nutr Cancer 63:1151–1159. doi:10.1080/01635581.2011.596645
Kallifatidis G, Labsch S, Rausch V, Mattern J, Gladkich J, Moldenhauer G, Buchler MW, Salnikov AV, Herr I (2011) Sulforaphane increases drug-mediated cytotoxicity toward cancer stem-like cells of pancreas and prostate. Mol Ther 19:188–195. doi:10.1038/mt.2010.216
Chen X, Thakkar H, Tyan F, Gim S, Robinson H, Lee C, Pandey SK, Nwokorie C, Onwudiwe N, Srivastava RK (2001) Constitutively active Akt is an important regulator of TRAIL sensitivity in prostate cancer. Oncogene 20:6073–6083
Iwatsuki M, Mimori K, Yokobori T, Ishi H, Beppu T, Nakamori S, Baba H, Mori M (2010) Epithelial–mesenchymal transition in cancer development and its clinical significance. Cancer Sci 101:293–299. doi:10.1111/j.1349-7006.2009.01419.x
Bailey JM, Singh PK, Hollingsworth MA (2007) Cancer metastasis facilitated by developmental pathways: Sonic hedgehog, Notch, and bone morphogenic proteins. J Cell Biochem 102:829–839. doi:10.1002/jcb.21509
Shin JO, Nakagawa E, Kim EJ, Cho KW, Lee JM, Cho SW, Jung HS (2012) miR-200b regulates cell migration via Zeb family during mouse palate development. Histochem Cell Biol 137:459–470. doi:10.1007/s00418-012-0915-6
Drake JM, Strohbehn G, Bair TB, Moreland JG, Henry MD (2009) ZEB1 enhances transendothelial migration and represses the epithelial phenotype of prostate cancer cells. Mol Biol Cell 20:2207–2217. doi:10.1091/mbc.E08-10-1076
Liu Y, El-Naggar S, Darling DS, Higashi Y, Dean DC (2008) Zeb1 links epithelial–mesenchymal transition and cellular senescence. Development 135:579–588. doi:10.1242/dev.007047
Akada M, Crnogorac-Jurcevic T, Lattimore S, Mahon P, Lopes R, Sunamura M, Matsuno S, Lemoine NR (2005) Intrinsic chemoresistance to gemcitabine is associated with decreased expression of BNIP3 in pancreatic cancer. Clin Cancer Res 11:3094–3101
Arumugam T, Ramachandran V, Fournier KF, Wang H, Marquis L, Abbruzzese JL, Gallick GE, Logsdon CD, McConkey DJ, Choi W (2009) Epithelial to mesenchymal transition contributes to drug resistance in pancreatic cancer. Cancer Res 69:5820–5828. doi:10.1158/0008-5472.CAN-08-2819
Bednar F, Simeone DM (2009) Pancreatic cancer stem cells and relevance to cancer treatments. J Cell Biochem 107:40–45. doi:10.1002/jcb.22093
Du Z, Qin R, Wei C, Wang M, Shi C, Tian R, Peng C (2010) Pancreatic cancer cells resistant to chemoradiotherapy rich in “stem-cell-like” tumor cells. Dig Dis Sci. doi:10.1007/s10620-010-1340-0
Lau J, Kawahira H, Hebrok M (2006) Hedgehog signaling in pancreas development and disease. Cell Mol Life Sci 63:642–652. doi:10.1007/s00018-005-5357-z
Nalls D, Tang SN, Rodova M, Srivastava RK, Shankar S (2011) Targeting epigenetic regulation of miR-34a for treatment of pancreatic cancer by inhibition of pancreatic cancer stem cells. PLoS One 6:e24099. doi:10.1371/journal.pone.0024099
Kasper M, Regl G, Frischauf AM, Aberger F (2006) GLI transcription factors: mediators of oncogenic Hedgehog signalling. Eur J Cancer 42:437–445. doi:10.1016/j.ejca.2005.08.039
Katoh Y, Katoh M (2008) Hedgehog signaling, epithelial-to-mesenchymal transition and miRNA (review). Int J Mol Med 22:271–275
Sarkar FH, Li Y, Wang Z, Kong D (2009) Pancreatic cancer stem cells and EMT in drug resistance and metastasis. Minerva Chir 64:489–500 R06095168[pii]
Wellner U, Schubert J, Burk UC, Schmalhofer O, Zhu F, Sonntag A, Waldvogel B, Vannier C, Darling D, zur Hausen A, Brunton VG, Morton J, Sansom O, Schuler J, Stemmler MP, Herzberger C, Hopt U, Keck T, Brabletz S, Brabletz T (2009) The EMT-activator ZEB1 promotes tumorigenicity by repressing stemness-inhibiting microRNAs. Nat Cell Biol 11:1487–1495. doi:10.1038/ncb1998
Hanlon N, Coldham N, Gielbert A, Kuhnert N, Sauer MJ, King LJ, Ioannides C (2008) Absolute bioavailability and dose-dependent pharmacokinetic behaviour of dietary doses of the chemopreventive isothiocyanate sulforaphane in rat. Br J Nutr 99:559–564. doi:10.1017/S0007114507824093
Li Y, Zhang T, Korkaya H, Liu S, Lee HF, Newman B, Yu Y, Clouthier SG, Schwartz SJ, Wicha MS, Sun D (2010) Sulforaphane, a dietary component of broccoli/broccoli sprouts inhibits breast cancer stem cells. Clin Cancer Res. doi:10.1158/1078-0432.CCR-09-2937
Myzak MC, Karplus PA, Chung FL, Dashwood RH (2004) A novel mechanism of chemoprotection by sulforaphane: inhibition of histone deacetylase. Cancer Res 64:5767–5774
Park EJ, Pezzuto JM (2002) Botanicals in cancer chemoprevention. Cancer Metastasis Rev 21:231–255
Shankar S, Ganapathy S, Srivastava RK (2008) Sulforaphane enhances the therapeutic potential of TRAIL in prostate cancer orthotopic model through regulation of apoptosis, metastasis and angiogenesis. Clin Cancer Res 14:1–16
Kallifatidis G, Rausch V, Baumann B, Apel A, Beckermann BM, Groth A, Mattern J, Li Z, Kolb A, Moldenhauer G, Altevogt P, Wirth T, Werner J, Schemmer P, Buchler MW, Salnikov AV, Herr I (2009) Sulforaphane targets pancreatic tumour-initiating cells by NF-kappaB-induced antiapoptotic signalling. Gut 58:949–963. doi:10.1136/gut.2008.149039
Acknowledgments
We thank our lab members for critical reading of the manuscript.
Conflict of interest
The authors indicate no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, SH., Fu, J., Watkins, D.N. et al. Sulforaphane regulates self-renewal of pancreatic cancer stem cells through the modulation of Sonic hedgehog–GLI pathway. Mol Cell Biochem 373, 217–227 (2013). https://doi.org/10.1007/s11010-012-1493-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-012-1493-6