Abstract
Hypoxia-inducible factor-1 (HIF-1) could ameliorate renal ischemia reperfusion injury (IRI), but the underlying mechanism remains elusive. In the current study, we aim to investigate the possible role of prolyl hydroxylases inhibitor dimethyloxalylglycine (DMOG) in inducing delayed preconditioning-like effects against IRI. Mice were divided into four groups (n = 6): sham group; IRI group; DMOG group: pretreated with DMOG 24 h before IRI; and GW274150 + DMOG group: pretreated with DMOG followed by iNOS inhibitor GW274150 treatment 24 h before IRI. The results showed that the protein level of HIF-1a and the expression of its targets inducible nitric oxide synthase (iNOS), erythropoietin, and heme oxygenase-1 were obviously increased after administration of DMOG. Histological analysis of renal function showed improvement in tubulointerstitial injury due to ischemia by delayed preconditioning with DMOG. GW274150 antagonized the delayed renal protection afforded by DMOG as reflected by deteriorated renal dysfunction, aggravated histological injury, increased renal cell apoptosis, and increased vimentin expression in the kidney. In conclusion, our data demonstrate that DMOG pretreatment induces delayed renal protection against IRI in mice and the beneficial effects are mitigated by pharmacological inhibition of iNOS, suggesting that the protective effects derived from HIF-1 activation via DMOG in the kidney are partially mediated by iNOS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the kidney, ischemic injury leads to acute renal failure (ARF). Although renal function after episodes of ARF is thought to be restored, initial ischemic injury is associated with high morbidity and mortality [1]. Thus, great efforts have been taken to prevent ischemic renal injury, and the currently employed strategy is ischemic preconditioning, which can stimulate the endogenous cell protection mechanisms against renal ischemic reperfusion injury (IRI) [2]. Unfortunately, ischemia preconditioning cannot be widely used in the clinic, so pharmacological approaches that improve the ability of the kidney to tolerate ischemia and hypoxia would be more reasonable and practical [3].
Hypoxia-inducible factor (HIF) is the master regulator of a variety of processes during the adaptation to hypoxia. HIF is a heterodimer consisting of an oxygen-sensitive α-subunit HIF-α and a constitutively expressed β-subunit HIF-β [4]. Under a normoxia condition, the HIF-α subunit is hydroxylated by specific prolyl hydroxylases (PHD) and is rapidly degraded via the ubiquitin-proteasomal system. In a hypoxic environment, PHD-mediated hydroxylation is inhibited, leading to the accumulation of HIF-α in the nucleus, where it dimerizes with HIF-β to drive the transcription of target genes [5–7]. HIF regulates the expression of more than 100 genes, including erythropoietin (EPO), heme oxygenase-1 (HO-1), vascular endothelial growth factor (VEGF), glucose transporter-1 (Glut-1), and inducible nitric oxide synthase (iNOS), which control a variety of adaptive response to hypoxia, such as vasodilation, energy metabolism, glucose uptake, angiogenesis, erythropoiesis, cell viability, proliferation, and differentiation [8, 9].
PHD inhibitor has been shown to attenuate ischemic injury in many organs, including the kidney, heart, and brain [10–12], but the potential mechanism is still ambiguous. In this study, we aim to investigate the possible role of PHD inhibitor dimethyloxalylglycine (DMOG) in inducing delayed preconditioning-like effects against IRI. Specifically, we also identified the potential role of iNOS in ameliorating postischemic renal injury afforded by HIF-1α activation.
Materials and methods
Animals and grouping
Male C57BL/6 mice (weight from 22 to 26 g) were supplied by the Experimental Animal Center of Fudan University and randomized into the following 4 experimental groups: the sham group (n = 6), which received renal pedicles isolation alone; the IRI group (n = 6), which received 0.9% saline (ip) 24 h before IRI; the DMOG group (n = 6), which was pretreated with DMOG (Cayman Chemical, Ann Arbor, MI) (dissolved in 0.9% saline, ip) at a dose of 40 mg/kg 24 h before IRI; and the GW274150+DMOG group (n = 6), which received DMOG (40 mg/kg ip) 24 h before IRI followed by treatment with specific iNOS inhibitor GW274150 (Enzo Life Sciences International, PA) (10 mg/kg ip) 30 min before IRI. Animals were subjected to renal IRI as described below. All animal experiments were approved by the Institutional Animal Care Use Committee of Shanghai (No. SYXK [Hu] 2007-0002).
Renal IRI
Animals were anesthetized with sodium pentobarbital (50 mg/kg ip) and then subjected to bilateral warm ischemic injury by simultaneous clamping of both renal pedicles with nontraumatic microvascular clamps for 30 min. Body temperature was maintained by placing mice on the heat pad during the surgery. After reperfusion for 24 h, blood samples and kidneys were collected. Sham-operated animals underwent the same anesthesia, laparotomy, and renal pedicles isolation as ischemic mice.
Blood urea nitrogen (BUN) and serum creatinine (Scr) measurement
BUN and Scr were measured by an enzymatic method with a commercial kit (Sysmex, Shanghai, China) on a HITACHI 7170A automatic biochemical analyzer (Hitachi, Shanghai, China).
Histological examination
Paraffin-embedded kidney sections (4 μm) were stained with hematoxylin and eosin. Morphological assessment was performed by an experienced renal pathologist, who was blind to the treatment groups. More than 10 high-power fields (magnification ×400) including both cortex and outer medulla were randomly selected. A grading scale of 0–4, as outlined by Jablonski et al. [13], was used for the histopathological assessment of ischemia and reperfusion-induced damage of the proximal tubules.
Immunocytochemistry
Formalin-fixed kidney sections (4 μm) were de-paraffinized in xylene and rehydrated through a graded ethanol series to water. After blocking with 10% normal horse serum in PBS, the slides were stained for vimentin in sequential incubation with mouse monoclonal antibody (clone V9; Dako, Carpinteria, CA), biotin-conjugated secondary antibody, and avidin–biotin peroxidase complex (Jackson Immunoresearch, West Grove, PA). Integral optical density of the vimentin-positive area in the tubulointerstitium was quantitatively measured by counting 20 randomly selected high-power fields (HPF, 400×) per section in the outer medulla. All quantification was performed in a blinded manner.
Detection of apoptotic cells
Formaldehyde-fixed paraffin sections were de-paraffinized, rehydrated, and incubated with proteinase K, and endogenous peroxidase activity was quenched. In situ labeling of fragmented DNA was performed with TUNEL staining with a commercially available in situ cell death detection kit (Roche Diagnostics, Mannheim, Germany), according to the manufacturer’s instructions. The number of TUNEL-positive cells in each section was calculated by counting the number of positive cells in 20 randomly selected fields of the entire sample. Quantification was made by a renal pathologist in a blind manner.
Real-time PCR analysis
Total RNA was extracted from kidney using Trizol Reagent (Invitrogen, Carlsbad, CA) according to the manufacturer’s instructions. cDNA was synthesized with a SuperScript first strand synthesis kit (Invitrogen) following the protocol supplied, and 1 μg cDNA was used for real-time PCR (Roche Diagnostics) utilizing SYBR Green PCR reagent (QIAGEN, Hilden, Germany) with the primers as follows: β-actin 5′-CCTCTATGCCAACACAGTGC-3′, 5′-GTACTCCTGCTTGCTGATCC-3′; iNOS 5′-TTGGAGCGAGTTGTGGATTG-3′, 5′-GTGAGGGCTTGGCTGAGTGA-3′; EPO 5′-AAAAGAATGGAGGTGGAAGAAC-3′, 5′-TACCCGAAGCAGTGAAGTGAG-3′; HO-1 5′-ACAGATGGCGTCACTTCGTC-3′, 5′-AGGCAAGATTCTCCCTTACAG-3′. After denaturation at 95°C for 15 min, the PCR samples were cycled 40 times at 95°C for 10 s, 58°C for 15 s, and 72°C for 20 s. All reactions were performed in triplicate. For quantitative analysis, iNOS, EPO, and HO-1 mRNA levels were normalized to the level of β-actin as the internal control.
Protein isolation and western blot
Preparation of nuclear extract
Kidney tissue (100 mg) was homogenized using polytron homogenizer (Fluko, Shanghai, China) in 200 μL ice-cold homogenization buffer (10 mmol/L Hepes, pH 7.9, 2 mmol/L MgCl2 0.1 mmol/L EDTA, and 10% NP-40) with a cocktail of protease inhibitors (Roche Diagnostics). The mixture was vortexed 10 times for 1 min each and was centrifuged at 12,000g for 30 min at 4°C. The pellet was lysed in 60 μL ice-cold lysis buffer (50 mmol/L Hepes, 10% glycerol, 300 mmol/L NaCl, and 50 mmol/L KCl) with a cocktail of protease inhibitors and vortexed vigorously five times for 2 min each, and the mixture was centrifuged at 12,000g for 30 min at 4°C. The supernatant was taken as nuclear extract, which was diluted to a standard concentration of 3 μg/μL and stored in aliquots at −70°C. The protein concentration was determined by Bradford method (BioRad protein assay; Bio-Rad Laboratories, Hercules, CA).
Immunoblotting analysis
Total cell lysate was extracted using RIPA lysis buffer. About 100 μg nuclear extract or cell lysate was separated on SDS–polyacrylamide gels and transferred onto nitrocellulose membrane. Membranes were stained with Ponceau S solution (0.2% w/v in 1% acetic acid; Sigma-Aldrich) to verify equal protein loading and transfer and then blotted with HIF-1α antibody (clone α67; Novus Biologicals, Littleton, CO), iNOS antibody (Cell Signaling Technology, Danvers, MA), or actin antibody (Sigma-Aldrich). The membranes were incubated with horseradish peroxidase–conjugated secondary antibodies (Jackson Immunoresearch) and developed using ECL kit (Pierce, Rockford, IL) and exposed to X-ray film. Bands on X-ray films were quantified with Image plus 5.1 software.
Statistical analysis
Data were presented as mean ± SD. One-way analysis of variance (ANOVA) followed by the least significant difference (LSD) method was used to determine differences among more than two groups for all continuous parameters while Student’s t test was used for two-group data. Statistical analysis was performed using SPSS13.0 software, and P < 0.05 was considered significant.
Results
Stabilization and activation of HIF-1α in mice kidney after DMOG treatment
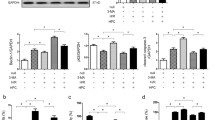
To evaluate the capacity of DMOG to stabilize HIF-1α protein, we detected the protein level of HIF-1α in the kidney of mice treated with DMOG. Immunoblotting analysis showed that DMOG treatment significantly increased the protein level of HIF-1α compared to vehicle-treated control kidney. As a positive control, CoCl2, a known HIF-1α activator, induced a high protein level of HIF-1α (Fig. 1a). These results prove that pretreatment with DMOG promotes the stabilization of HIF-1α protein.
DMOG promotes the stabilization and activation of HIF-1α in mice kidney. Mice kidney was subjected to different treatments. Control: treated with vehicle; DMOG: treated with 40 mg/kg DMOG; CoCl2: treated with 30 mg/kg CoCl2. a HIF-1α protein level was detected by immunoblotting. The samples were loaded in duplicate. b Expression of HIF-1α target genes iNOS, EPO, and HO-1 at mRNA level was determined by real-time polymerase chain reaction. mRNA fold changes of iNOS, EPO, and HO-1 were calculated using β-actin as an internal control. Quantitative data are expressed as mean ± standard error of mean; n = 6 animals/group. *P < 0.05 versus control
To explore the biological effects of DMOG-induced HIF-1α stabilization, next we detected the expression of HIF-1α target genes in mice kidney. Real-time PCR analysis demonstrated that the expressions of iNOS, EPO, and HO-1 at mRNA level were significantly increased in the DMOG-treated kidney compared to the vehicle-treated control kidney (Fig. 1b). Collectively, these data confirm that DMOG stabilizes HIF-1α and promotes the expression of HIF-1α targets in the kidney.
DMOG promotes iNOS expression in postischemia kidney
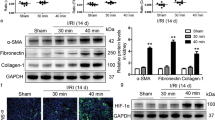
iNOS is one of the target genes of HIF-1α and is implicated in IRI although its role remains controversial. Thus, we focussed on iNOS and examined its expression in different experimental groups of mice. A modest induction of iNOS was observed in saline vehicle-treated kidney exposed to IRI compared with sham kidney. DMOG-pretreated IRI kidney showed significantly higher expression of iNOS compared with saline vehicle-treated kidney after IRI. The increase in iNOS expression was partially inhibited in animals treated by iNOS inhibitor GW274150 after DMOG pretreatment (Fig. 2).
DMOG promotes iNOS expression in postischemia kidney. iNOS protein level was detected by immunoblotting in the kidney lysate from different groups of mice. Actin served as loading control. The sham kidneys exhibited no detectable iNOS. Three independent experiments all led to iNOS expressions. DMOG pretreatment (DMOG+IRI) significantly increased iNOS expression compared with ischemia/reperfusion injury (IRI) kidneys. Administration with selective iNOS inhibitor GW274150 after DMOG pretreatment (DMOG+GW+IRI) decreased the expression of iNOS compared with DMOG-pretreated group. Data are expressed as mean ± standard error of mean; n = 6 animals/group. *P < 0.05
iNOS inhibitor antagonizes the protective effects of DMOG on the kidney of IRI mice
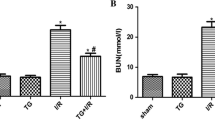
Renal IRI mice exhibited a significant increase in serum creatinine level compared to sham-operated animals, suggesting a severe renal dysfunction. Mice pretreated with DMOG before renal ischemia showed a significantly decreased serum creatinine level compared with untreated mice, indicating ameliorated renal function. Nevertheless, serum creatinine level was significantly higher in IRI mice treated with both DMOG and iNOS inhibitor GW274150 compared to IRI mice treated with DMOG alone (Fig. 3). These results suggest that DMOG has protective effects on kidney function during IRI, which could be attenuated by iNOS inhibitor.
DMOG and GW274150 have antagonistic effect on serum creatinine level after ischemia/reperfusion injury. Serum creatinine level was dramatically increased in IRI mice, which was reduced by DMOG treatment (DMOG+IRI), while pretreatment with GW274150 before DMOG administration (DMOG+GW+IRI) blunt this reduction. Data are expressed as mean ± standard error of mean; n = 6 animals/group. *P < 0.05
To provide more evidence that DMOG and iNOS inhibitors have antagonistic effects on renal function during IRI, we examined histological morphology of the kidney. Representative HE-stained sections showed reduced cast formation and less extensive tubular necrosis after DMOG treatment in comparison with the controls (Fig. 4a). Jablonski grading semi-quantitative scoring of HE stains showed that mice treated with GW274150 after DMOG pretreatment exhibited significantly higher Jablonski scores in the kidney (Fig. 4b).
DMOG and GW274150 have antagonistic effect on kidney morphology after ischemia/reperfusion injury. a Animals subjected to sham operation (A), ischemia/reperfusion injury (B), pretreated with DMOG before IRI (C), treated with GW274150 after DMOG administration before IRI (D). b Jablonski grading scale score was estimated based on hematoxylin and eosin staining. Data represent mean ± standard error of mean; n = 6 animals/group. *P < 0.05. Original magnification, ×200
Next, we employed a TUNEL assay to assess the apoptosis of renal cells (Fig. 5). As expected, TUNEL-positive epithelial cells were rarely observed in the kidneys of sham-operated animals. In contrast, ischemia caused a marked increase in apoptotic cells (26.0 ± 3.6%). DMOG significantly reduced the number of apoptotic cells (8.2 ± 1.5%). Treatment with iNOS inhibitor GW27415 before renal ischemia abated the reduction in apoptotic cells induced by DMOG pretreatment (17.3 ± 2.5%).
DMOG and GW274150 have antagonistic effect on renal cell apoptosis after ischemia/reperfusion injury (IRI). Apoptosis in different groups of mice was detected by TUNEL. a Sham-operated mice demonstrated almost no positive cells. b After IRI, TUNEL-positive cells appeared in the out medulla. c Pretreatment of mice with DMOG before IRI led to a decrease in the number of TUNEL-positive cells. d Treatment with GW27415 after DMOG administration led to an increase in the number of TUNEL-positive cells. Original magnification, ×200
Vimentin, an intermediate filament protein that is expressed almost exclusively in mesenchymal cells, has been shown to be detected in mitotically active proximal tubular cells after IRI [14]. As a marker for tubulointerstitial injury, vimentin was also detected in this study (Fig. 6). While weak vimentin staining was detected in the tubulointerstitium in sham-operated mice kidneys (5.4 ± 3.1), strong vimentin staining was predominantly detected in tubular epithelial cells and peritubular cells after ischemia/reperfusion (89.2 ± 22.7). Pretreatment with DMOG significantly reduced vimentin expression after 24 h of reperfusion (13.6 ± 4.2). However, GW274150 administration antagonized DMOG-induced down-regulation of vimentin expression (63.7 ± 18.5).
DMOG and GW274150 have antagonistic effect on vimentin expression in ischemia/reperfusion kidney. Vimentin expression in different groups of mice was detected by immunohistochemical staining. Very few scattered vimentin intermediate filaments were observed in the out medulla of sham-operated mice (a) or mice pretreated with DMOG before ischemia (c). However, strong staining of vimentin was detected in mice subjected to ischemia/reperfusion injury alone (b) or mice that had been pretreated with iNOS inhibitor GW274150 after DMOG administration before ischemia (d). Original magnification, ×200
Discussion
Since renal parenchymal hypoxia evidently plays an important role in the development of acute kidney injury, induction of hypoxia adaptation has been proposed as a novel interventional strategy in such high-risk patients [8, 15]. Although it is well known that acute systemic hypoxia/ischemia induces delayed preconditioning in the kidney [16, 17], the potential protection provided by chemical induction of a hypoxia response with DMOG has not been investigated. Here, we demonstrate that a single dose of DMOG (40 mg/kg) induced a delayed preconditioning that has protective effects on the kidney as evidenced by the reduction in serum creatinine, histological score, the number of apoptotic cells, and the expression of vimentin in the kidney 24 h after IRI.
HIF-1α is a key transcription factor that mediates tissue adaptive response to hypoxia by directly regulating the expression of a large number of target genes. DMOG is an effective inhibitor of PHD, and the inhibition of PHD by DMOG has been shown to promote the stabilization of HIF-1α and other beneficial factors, prevent IRI injury, and attenuate the acute inflammatory response [18–21]. Additionally, DMOG has an anti-apoptotic activity in different cell types under ischemia/hypoxia conditions. The mechanism of the protective effects could be mediated by mitochondrial pathway involving reduced cytochrome c release and caspase-3 activation [22, 23]. In this study, we employed DMOG to obtain the long-lasting stability and activity of HIF-1α in murine kidney that was sustained under normoxic condition for 24 h. In addition, our results showed that mRNA level of iNOS, EPO and HO-1 was significantly increased after pretreatment with DMOG, which paralleled HIF-1α activation. These data prove that DMOG stabilizes HIF-1α and promotes its biological activity.
While previous evidence has shown that both EPO and HO-1 could protect the kidney against the injury caused by ischemia reperfusion [24, 25], the role of iNOS in IRI remains controversial [26, 27]. On the one hand, increased activity of NOS is associated with IRI, and iNOS was considered as a proinflammatory factor in ischemia reperfusion injury [26]. On the other hand, nonselective NOS inhibitors are known to worsen the postischemic renal function, whereas l-arginine, a nitric oxide (NO) precursor, can reverse NOS inhibitor–induced deterioration of renal function. GW274150 ([(S)-2-Amino-(1-iminoethylamino)-5-thioheptanoic acid]) has recently been identified as a novel, highly selective, potent, and long-acting inhibitor of iNOS. GW274150 is a sulfur-substituted acetamine amino acid derivative of l-lysine, which, like 1400 W, has a very high selectivity for iNOS versus eNOS (>250-fold) or nNOS (>80-fold) [27]. In the current study, we demonstrate the up-regulation of iNOS in DMOG-pretreated IRI kidney, which was partially inhibited by GW274150. Next, we provide evidence that iNOS inhibitor GW274150 antagonized the protective effects of DMOG on the kidney of IRI mice, suggesting that iNOS plays protective function in kidney IRI. These results are consistent with the overwhelming opinion that iNOS plays a role in protection induced by mild sublethal ischemic preconditioning against a secondary exposure to ischemia reperfusion in retina, heart, brain, and kidney [28–31]. Notably, renal protective effects of delayed preconditioning were attenuated by a selective inhibitor of iNOS L-NII, and delayed ischemic preconditioning was not observed in iNOS knockout mice [16].
Additionally, many studies have demonstrated that iNOS is an essential mediator of the delayed phase of preconditioning induced by a number of pharmacological agents [32, 33]. But little is known about the role of iNOS in hypoxia preconditioning mediated by HIF-1 in any organ. Since iNOS is primarily regulated by HIF-1α in the kidney, we hypothesized that iNOS contributes to the protective effects of DMOG in the kidney. Our data show that serum creatinine level, apoptosis, vimentin expression, and histological injury in the kidney were significantly increased in mice treated by both DMOG and GW274150 compared to DMOG-treated mice. Thus, we speculate that renal protection achieved by the pharmacological activation of HIF-1α is at least partially mediated by iNOS, which may act as the downstream effector of DMOG. In agreement with our speculation, Xi et al. demonstrated that CoCl2-induced delayed cardioprotection is dependent on iNOS because the infarct limiting effect was absent in the iNOS-deficient mice [34]. In addition, Natarajan et al. reported that the cardioprotective effects achieved by PHD2 silencing and HIF-1 stabilization were lost in iNOS knockout mice and wild-type mice treated with iNOS inhibitor 1400W [19].
As demonstrated previously, the up-regulation of iNOS may increase renal NO generation. The role of NO in IRI is controversial [35–37]. Low levels of NO may be protective, but higher levels may be detrimental [38]. A delicate balance so as to allow the production of physiologically relevant amounts of NO but at the same time block the generation of reactive nitrogen species through repressing excessive NO levels is extremely required for therapeutic interference with iNOS [39]. Therefore, we suppose that preconditioning with DMOG has induced moderate iNOS/NO, which initiates cytoprotection signaling to defend against subsequent injury in renal tubule cells. Interestingly, previous report indicated that NO donors could induce HIF-1α expression under normoxic conditions [40]. Although our study did not address the direct role of NO in stabilization of HIF-1α in the kidney, such a possibility exists because DMOG activated HIF-1α and GW274150 blocked the DMOG-induced protection. Thus, it is plausible that increased iNOS expression after HIF-1α activation with DMOG might trigger further HIF-1α activity and extend its renoprotective effects via a positive feedback mechanism.
In summary, our study demonstrates that DMOG pretreatment induces delayed renal protection against IRI in mice by improving renal function and inhibiting apoptosis of renal cells. These beneficial effects are antagonized by selective iNOS inhibitor, suggesting that the protective effects derived from HIF-1 activation via DMOG in the kidney are partially mediated by iNOS.
References
Basile DP, Donohoe D, Roethe K, Osborn JL (2001) Renal ischemic injury results in permanent damage to peritubular capillaries and influences long-term function. Am J Physiol Renal Physiol 281:F887–F899
Reutzel-Selke A, Pratschke J, Martins PN, Denecke C, Jurisch A, Kotsch K, Pascher A, Neuhaus P, Tullius SG (2008) Ischemic preconditioning produces systemic protective and adoptively transferable effects. Kidney Int 74:622–630
Bonventre JV (2002) Kidney ischemic preconditioning. Curr Opin Nephrol Hypertens 11:43–48
Wang GL, Semenza GL (1993) General involvement of hypoxia inducible factor 1 in transcription response to hypoxia. Proc Natl Acad Sci USA 90:4304–4308
Ivan M, Kondo K, Yang H, Kim W, Valiando J, Ohh M, Salic A, Asara JM, Lane WS, Kaelin WG Jr (2001) HIF targeted for VHL-mediated destruction by proline hydroxylation: implication for O2 sensing. Science 292:464–468
Jaakkola P, Mole DR, Tian Y, Wilson MI, Gielbert J, Gaskell SJ, Kriegsheim Av, Hebestreit HF, Mukherji M, Schofield CJ, Maxwell PH, Pugh CW, Ratcliffe PJ (2001) Targeting of HIF-α to the von Hippel-Lindau ubiquitylation complex by O2-regulated prolyl hydroxylation. Science 94:468–472
Bruick RM SLA (2001) A conserved family of prolyl-4-hydroxylases that modify HIF. Science 294:1337–1340
Semenza GL (2000) Surviving ischemia: adaptive responses mediated by hypoxia inducible factor 1. J Clin Invest 106:809–812
Haase VH (2006) Hypoxia-inducible factors in the kidney. Am J Physiol Renal Physiol 291:F271–F281
Rosenberger C, Rosen S, Shina A, Frei U, Eckardt KU, Flippin LA, Arend M, Klaus SJ, Heyman SN (2008) Activation of hypoxia-inducible factors ameliorates hypoxic distal tubular injury in the isolated perfused rat kidney. Nephrol Dial Transplant 23:3472–3478
Ockaili R, Natarajan R, Salloum F, Fisher BJ, Jones D, Fowler AA 3rd, Kukreja RC (2005) HIF-1 activation attenuates postischemic myocardial injury: role for heme oxygenase-1 in modulating microvascular chemokine generation. Am J Physiol Heart Circ Physiol 289:H542–H548
Harten SK, Ashcroft M, Maxwell PH (2010) Prolyl hydroxylase domain inhibitors: a route to HIF activation and neuroprotection. Antioxid Redox Signal 12:459–480
Jablonski P, Howden BO, Rae DA, Birrell CS, Marshall VC, Tange J (1983) An experimental model for assessment of renal recovery from warm ischemia. Transplantation 35:198–204
Witzgall R, Brown D, Schwarz C, Bonventre JV (1994) Localization of proliferating cell nuclear antigen, vimentin, c-Fos, and clusterin in the postischemic kidney: evidence for a heterogenous genetic response among nephron segments, and a large pool of mitotically active and dedifferentiated cells. J Clin Invest 93:2175–2188
Rosenberger C, Rosen S, Heyman SN (2006) Renal parenchymal oxygenation and hypoxia adaptation in acute kidney injury. Clin Exp Pharmacol Physiol 33:980–988
Joo JD, Kim M, D’Agati VD, Lee HT (2006) Ischemic preconditioning provides both acute and delayed protection against renal ischemia and reperfusion injury in mice. J Am Soc Nephrol 17:3115–3123
Yang CC, Lin LC, Wu MS, Chien CT, Lai MK (2009) Repetitive hypoxic preconditioning attenuates renal ischemia/reperfusion induced oxidative injury via upregulating HIF-1 alpha-dependent bcl-2 signaling. Transplantation 88:1251–1260
Hill P, Shukla D, Tran MG, Aragones J, Cook HT, Carmeliet P, Maxwell PH (2008) Inhibition of hypoxia inducible factor hydroxylases protects against renal ischemia-reperfusion injury. J Am Soc Nephrol 19:39–46
Natarajan R, Salloum FN, Fisher BJ, Ownby ED, Kukreja RC, Fowler AA 3rd (2007) Activation of hypoxia-inducible factor-1 via prolyl-4 hydoxylase-2 gene silencing attenuates acute inflammatory responses in postischemic myocardium. Am J Physiol Heart Circ Physiol 293:H1571–H1580
Natarajan R, Salloum FN, Fisher BJ, Kukreja RC, Fowler AA 3rd (2006) Hypoxia inducible factor-1 activation by prolyl 4-hydroxylase-2 gene silencing attenuates myocardial ischemia reperfusion injury. Circ Res 98:133–140
Ockaili R, Natarajan R, Salloum F, Fisher BJ, Jones D, Fowler AA 3rd, Kukreja RC (2005) HIF-1 activation attenuates postischemic myocardial injury: role for heme oxygenase-1 in modulating microvascular chemokine generation. Am J Physiol Heart Circ Physiol 289:H542–H548
Sasabe E, Tatemoto Y, Li D, Yamamoto T, Osaki T (2005) Mechanism of HIF-1alpha-dependent suppression of hypoxia-induced apoptosis in squamous cell carcinoma cells. Cancer Sci 96:394–402
Liu XB, Wang JA, Ogle ME, Wei L (2009) Prolyl hydroxylase inhibitor dimethyloxalylglycine enhances mesenchymal stem cell survival. J Cell Biochem 106:903–911
Yang CW, Li C, Jung JY, Shin SJ, Choi BS, Lim SW, Sun BK, Kim YS, Kim J, Chang YS, Bang BK (2003) Preconditioning with erythropoietin protects against subsequent ischemia reperfusion injury in rat kidney. FASEB J 17:1754–1755
Wagner M, Cadetg P, Ruf R, Mazzucchelli L, Ferrari P, Redaelli CA (2003) Heme oxygenase-1 attenuates ischemia/reperfusion induced apoptosis and improves survival in rat renal allografts. Kidney Int 63:1564–1573
Cuzzocrea S, Chatterjee PK, Mazzon E, Dugo L, De Sarro A, Van de Loo FA, Caputi AP, Thiemermann C (2002) Role of induced nitric oxide in the initiation of the inflammatory response after postischemic injury. Shock 18:169–176
Alderton WK, Angell AD, Craig C, Dawson J, Garvey E, Moncada S, Monkhouse J, Rees D, Russell LJ, Russell RJ, Schwartz S, Waslidge N, Knowles RG (2005) GW274150 and GW273629 are potent and highly selective inhibitors of inducible nitric oxide synthase in vitro and in vivo. Br J Pharmacol 145:301–312
Sakamoto K, Yonoki Y, Kubota Y, Kuwagata M, Saito M, Nakahara T, Ishii K (2006) Inducible nitric oxide synthase inhibitors abolished histological protection by late ischemic preconditioning in rat retina. Exp Eye Res 82:512–518
Shinmura K, Xuan YT, Tang XL, Kuwagata M, Saito M, Nakahara T, Ishii K (2002) Inducible nitric oxide synthase modulates cyclooxygenase-2 activity in the heart of conscious rabbits during the late phase of ischemic preconditioning. Circ Res 90:602–608
Cho S, Park EM, Zhou P, Frys K, Ross ME, Iadecola C (2005) Obligatory role of inducible nitric oxide synthase in ischemic preconditioning. J Cereb Blood Flow Metab 25:493–501
Park KM, Byun JY, Kramers C, Kim JI, Huang PL, Bonventre JV (2003) Inducible nitric-oxide synthase is an important contributor to prolonged protective effects of ischemic preconditioning in the mouse kidney. J Biol Chem 278:27256–27266
Wakeno-Takahashi M, Otani H, Nakao S, Imamura H, Shingu K (2005) Isoflurane induces second window of preconditioning through up-regulation of inducible nitric oxide synthase in rat heart. Am J Physiol Heart Circ Physiol 289:H2585–H2591
Zhao T, Xi L, Chelliah J, Levasseur JE, Kukreja RC (2000) Inducible nitric oxide synthase mediates delayed myocardial protection induced by activation of adenosine A(1) receptors: evidence from gene-knockout mice. Circulation 102:902–907
Xi L, Taher M, Yin C, Salloum F, Kukreja RC (2004) Cobalt chloride induces delayed cardiac preconditioning in mice through selective activation of HIF-1α and AP-1 and iNOS signaling. Am J Physiol Heart Circ Physiol 287:H2369–H2375
Yu L, Gengaro PE, Niederberger M, Burke TJ, Schrier RW (1994) Nitric oxide: a mediator in rat tubular hypoxia/reoxygenation injury. Proc Natl Acad Sci USA 91:1691–1695
Bertuglia S (2008) Intermittent hypoxia modulates nitric oxide-dependent vasodilation and capillary perfusion during ischemia-reperfusion-induced damage. Am J Physiol Heart Circ Physiol 294:H1914–H1922
Lopez-Neblina F, Paez AJ, Toledo-Pereyra LH (1995) Modulation of neutrophil infiltration through nitric oxide in the ischemic rat kidney. Transplant Proc 27:1883–1885
Goligorsky MS, Brodsky SV, Noiri E (2002) Nitric oxide in acute renal failure: NOS versus NOS. Kidney Int 61:855–861
Pannu R, Singh I (2006) Pharmacological strategies for the regulation of inducible nitric oxide synthase: neurodegenerative versus neuroprotective mechanisms. Neurochem Int 49:170–182
Kimura H, Weisz A, Kurashima Y, Hashimoto K, Ogura T, D’Acquisto F, Addeo R, Makuuchi M, Esumi H (2000) Hypoxia response element of the human vascular endothelial growth factor gene mediates transcriptional regulation by nitric oxide: control of hypoxia-inducible factor-1 activity by nitric oxide. Blood 95:189–197
Acknowledgments
This work was supported by a grant from the Project of Science and Technology Committee of Shanghai, China (No. 09410705800).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, XL., Yan, ZW., Sheng, WW. et al. Activation of hypoxia-inducible factor-1 ameliorates postischemic renal injury via inducible nitric oxide synthase. Mol Cell Biochem 358, 287–295 (2011). https://doi.org/10.1007/s11010-011-0979-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-011-0979-y