Abstract
Remote preconditioning is a unique phenomenon in which brief episodes of ischemia and reperfusion to remote organ protect the target organ against sustained ischemia–reperfusion (I/R)-induced injury. Protective effects of remote renal preconditioning (RRPC) are well established in heart, but their mechanisms still remain to be elucidated. So, the present study was designed to investigate the possible role of oxygen-sensing hypoxia inducible factor-prolyl 4-hydroxylases (HIF-P4Hs) in RRPC-induced cardioprotection in rats. Remote renal preconditioning was performed by four episodes of 5 min renal artery occlusion and reperfusion. Isolated rat hearts were perfused on Langendorff apparatus and were subjected to global ischemia for 30 min followed by 120 min reperfusion. The levels of lactate dehydrogenase (LDH) and creatine kinase (CK) were measured in coronary effluent to assess the degree of myocardial injury. Extent of myocardial infarct size and coronary flow rate was also measured. Ethyl 3,4-dihydroxybenzoate (EDHB) and α-ketoglutarate (α-KG) were employed as HIF-P4Hs inhibitor and activator, respectively. Diethyldithiocarbamic acid (DDCA) was employed as NFkB inhibitor. Remote renal preconditioning prevented I/R-induced myocardial injury and produced cardioprotective effects. Pharmacological preconditioning with EDHB (100 mg kg−1 i.p.) mimicked the cardioprotective effects of RRPC. However, α-KG (200 mg kg−1 i.p.) and DDCA (150 mg kg−1 i.p.) abolished cardioprotective effects of RRPC and EDHB. So, it may be concluded that inhibition of HIF-P4H has a key role in RRPC-induced cardioprotection. Further, remote preconditioning-induced HIF-P4H inhibition may have triggered a transduction pathway involving activation of NFkB.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Remote preconditioning is a unique phenomenon whereby transient regional ischemic episodes to tissues, at a distance from the target organ, afford protection to heart against sustained ischemia and reperfusion injury with the same efficacy as local ischemic preconditioning [1]. Przyklenk et al. [2] demonstrated that four cycles of 5 min occlusion and reperfusion of left circumflex artery led to reduction in infarct size following sustained occlusion of left anterior descending coronary artery and described this phenomenon as intracardiac preconditioning [2]. In the later years, various reports have published indicating that short episodes of occlusion and reperfusion of arteries such as cerebral [3], mesenteric [4], intestinal [5], renal arteries [6], and abdominal aorta [7] produce preconditioning of myocardium against sustained ischemia and reperfusion in various animals like mice, rabbits, pigs, sheep, swine, and dogs [1, 3, 8]. Remote preconditioning has also been documented to produce cardioprotective effects in human beings [9].
Hypoxia Inducible Factor-Prolyl 4-hydroxylases (HIF-P4Hs), a novel family of cytoplasmic prolyl 4-hydroxylases, have been identified as O2 sensor and reported to play a central role in regulation of cellular and systemic O2 homeostasis [10]. During normoxia, HIF-P4H catalyzed prolyl hydroxylation of hypoxia-inducible factor (HIF-α] has been described to induce degradation of HIF-α [11, 12]. However, hypoxia has been documented to inhibit the enzymatic activity of HIF-P4H, thus allowing the levels of HIF-α to get elevated [10]. Further, dimerisation of HIF-α with HIF β and subsequently its translocation in nucleus has been reported to induce the expression of humoral factors such as erythropoietin, vascular endothelial growth factor, glycolytic enzymes, which subsequently increase ischemic tolerance at cellular tissue and organ level [13]. Pharmacological inhibition of HIF-P4H has been reported to produce tissue protective effects in ischemic diseases like myocardial infarction [14, 15] and stroke [16] etc. Though inhibition of HIF-P4H has been reported to confer resistance against sustained ischemic insult, and role of HIF-P4H has also been identified in ischemic preconditioning [17], yet the possible involvement of HIF-P4H in remote preconditioning is still unexplored.
α-Ketoglutarate has been employed as an activator of HIF-P4H [18]. Ethyl 3, 4-dihydroxybenzoate (EDHB) has been characterized as a cell-permeable inhibitor that competitively binds to both the ascorbate and α-ketoglutarate-binding sites of the prolyl hydroxylase active domain and has been employed as selective inhibitor of HIF-P4H enzyme [19]. Nuclear factor kappa-B (NFkB) is hypoxia-activated, redox-sensitive, pro-survival transcription factor and its key role has become apparent in the pathophysiology of myocardial infarction, and unstable angina [20]. Moreover, the possible role of NFkB in ischemic preconditioning has also been suggested and pharmacological inhibition of NFkB has abolished cardioprotection in both classic and delayed models of preconditioning [21, 22]. Diethyldithiocarbamic acid (DDCA) has been employed as a specific inhibitor of NFkB [22]. Recently, it has been reported that inhibition of HIF-P4H is associated with activation of NFkB in HeLa cell lines [23]. However, no such pathway is explored in HIF-P4H inhibition induced preconditioning. So, the present study was designed to investigate the possible role and transduction pathway of HIF-P4H in remote renal preconditioning (RRPC)-induced cardioprotection in rats.
Materials and methods
Wistar albino rats (150–200g) were employed for the present study. They were fed on standard laboratory diet (Kisan Feeds Ltd., Chandigarh, India) and had free access to water and food. The experimental protocol was approved by Institutional Animal Ethics Committee and care of the animals was carried out as per the guidelines of Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA), Ministry of Environment and Forest, Government of India (Reg. No.-107/1999/CPCSEA).
Drugs and chemicals
EDHB and DDCA were procured from Sigma-Aldrich, USA. α-ketoglutarate was procured from Merck. Kits for CK estimation were purchased from Human Diagnostics, Germany, marketed in India by Medsource Ozone. All other chemicals were of analytical grade and obtained from S.D. Fine chemicals, Mumbai, India. All the drugs were dissolved in distilled water except EDHB, which was dissolved in PEG 400.
Remote renal preconditioning (RRPC)
Rat was anesthetized with thiopental sodium (35 mg kg−1 i.p.). A 2-cm-long incision was given on the abdomen. The renal artery was isolated and a silken suture (numbered 5/0) was used to make a shoelace knot to occlude left renal artery and knot was untied for reperfusion. Four episodes of ischemia and reperfusion, each comprising 5 min occlusion and 5 min reperfusion, were used for RRPC.
Isolated rat heart preparation
Rat was heparinized (500 IU kg−1 i.p.) about 20 min before sacrificing the animal. After sacrificing rat by cervical dislocation, heart was rapidly excised and mounted immediately on Langendorff apparatus [24]. The isolated heart was perfused retrogradely at constant pressure of 70 mm Hg with Kreb’s Henseleit (KH) solution of pH 7.4 bubbled with 95% O2 and 5% CO −2 . Flow rate was maintained at 7–9 ml/min. The heart was enclosed in a double wall jacket, the temperature of which was maintained at 37°C by circulating warm water. After 10 min stabilization, global ischemia was produced for 30 min by blocking the inflow of KH solution and it was followed by reperfusion for 120 min. Coronary effluent was collected at different time intervals, i.e., basal (immediately after stabilization), 0 min, 5 min, and 30 min after reperfusion for biochemical estimations. Coronary flow rate was measured at different time intervals to assess the degree of injury to coronary vasculature.
Assessment of infarct size
After 120 min reperfusion, heart was removed from Langendorff apparatus. The atria and the root of aorta were excised and heart was kept overnight at 0°C. Frozen heart was sliced into uniform sections of 2–3-mm thickness. The slices were incubated in 1% triphenyl tetrazolium chloride (TTC) at 37°C in 0.2 M Tris buffer (pH 7.4) for 20 min. The extent of myocardial infarct size was estimated macroscopically by volume and weight method [25].
Estimation of lactate dehydrogenase (LDH)
The levels of LDH were estimated in samples of coronary effluent collected after stabilization (basal), immediately and 30 min after reperfusion using 2, 4 DNPH method [26].
Estimation of creatine kinase (CK)
The levels of CK were estimated in coronary effluent samples after stabilization (basal) and 5 min after reperfusion using method described by Swanson and Wilkinson [27].
Experimental protocol
Eight groups, each comprising six wistar albino rats, were employed in the present study.
Group I (Sham control)
Rat was subjected to surgical procedure to isolate left renal artery, but artery was not occluded. Heart was isolated and perfused on Langendorff apparatus 40 min after the isolation of left renal artery. After 10 min stabilization, heart was subjected to global ischemia for 30 min followed by reperfusion for 120 min.
Group II (Remote renal preconditioning)
Rat was subjected to surgical procedure to isolate left renal artery. Four episodes, each comprising 5 min renal artery occlusion and 5 min reperfusion, were carried out for RRPC. Immediately after the last episode of remote preconditioning, heart was isolated and subjected to 30 min global ischemia followed by 120 min reperfusion as described in group I.
Group III (α-ketoglutarate in RRPC)
Rat was administered α-ketoglutarate (200 mg kg−1 i.p.) 30 min prior to performing RRPC. After RRPC, heart was subjected to ischemia and reperfusion (I/R) as described in group I.
Group IV (Ethyl 3,4-dihydroxybenzoate-induced pharmacological preconditioning)
Rat was pharmacologically preconditioned with ethyl 3,4-dihydroxybenzoate (EDHB, 100 mg kg−1 i.p.) 30 min before subjecting the heart to I/R as described in group I.
Group V (α-ketoglutarate in EDHB-induced pharmacological preconditioning)
Rat was administered α-ketoglutarate (200 mg kg−1 i.p.) 30 min prior to pharmacological preconditioning with EDHB (100 mg kg−1 i.p.). Heart was subjected to I/R as described in group I, 40 min after EDHB-induced preconditioning.
Group VI (Diethyldithiocarbamic acid in RRPC)
Rat was administered diethyldithiocarbamic acid (150 mg kg−1 i.p.) 30 min prior to performing RRPC. After RRPC, heart was subjected to I/R as described in group I.
Group VII (Diethyldithiocarbamic acid in EDHB-induced pharmacological preconditioning)
Rat was administered diethyldithiocarbamic acid (150 mg kg−1 i.p.) 30 min prior to pharmacological preconditioning with EDHB (100 mg kg−1 i.p.). Heart was subjected to I/R as described in group I, 40 min after EDHB-induced preconditioning.
Group VIII (Vehicle control, PEG 400)
Rat was administered PEG 400, 70 min prior to isolation of the heart and subjected to I/R as described in group I.
Statistical analysis
The results were expressed as mean ± standard error of means (S.E.M.). The results of LDH, CK, and coronary flow rate were analyzed using two way repeated ANOVA, while the results of infarct size were analyzed by one-way ANOVA. Tukey’s multiple range test was employed for post-hoc analysis after ANOVA. A value of P < 0.05 was considered to be statistically significant.
Results
Effects of pharmacological interventions on infarct size
Remote renal preconditioning (RRPC) significantly attenuated I/R-induced myocardial infarct size measured by volume method. Pharmacological preconditioning with ethyl 3,4-dihydroxybenzoate (EDHB, 100 mg kg−1 i.p.) also attenuated I/R-induced infarction in a significant manner. Administration of α-ketoglutarate (α-KG, 200 mg kg−1 i.p.) abolished infarct-sparing effects of RRPC and EDHB. Further, diethyldithiocarbamic acid (DDCA, 150 mg kg−1 i.p.) administration also abolished RRPC- and EDHB-induced decrease in infarct size (Fig. 1). Similar results were obtained when infarct size was measured by volume method.
Effect of pharmacological interventions on myocardial infarct size by volume method. Values are mean ± S.E.M. for six animals. RRPC: Remote Renal Preconditioning; Alpha-KG: Alpha-ketoglutarate; EDHB: Ethyl 3, 4- dihydroxybenzoate; DDCA: Diethyldithiocarbamic acid; PEG 400: Polyethylene glycol 400. a: P < 0.05 vs. Control; b: P < 0.05 vs. RRPC
Effects of pharmacological interventions on release of LDH and CK in coronary effluent
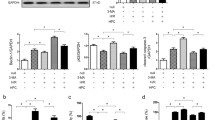
Thirty min ischemia followed by 120 min reperfusion (I/R) resulted in a significant increase in release of LDH, noted immediately and 30 min after reperfusion, and CK, noted 5 min after reperfusion, in coronary effluent as compared to basal. Remote renal preconditioning and pharmacological preconditioning with EDHB significantly attenuated I/R-induced increase in release of LDH and CK in coronary effluent. Administration of α-KG abolished RRPC- and EDHB-induced decrease in release of LDH and CK. Further, DDCA administration also abolished RRPC- and EDHB-induced decrease in LDH and CK release in coronary effluent in a significant manner (Figs. 2, 3).
Effects of pharmacological interventions on release of lactate dehydrogenase (LDH) in coronary effluent at basal level, 0 min and 30 min after reperfusion. Values are mean ± S.E.M. for six animals. RRPC: Remote Renal Preconditioning; Alpha-KG: Alpha-ketoglutarate; EDHB: Ethyl 3,4- dihydroxybenzoate; DDCA: Diethyldithiocarbamic acid; PEG 400: Polyethylene glycol 400. a: P < 0.05 vs. Control; b: P < 0.05 vs. RRPC
Effects of pharmacological interventions on release of Creatine Kinase (CK) in coronary effluent at basal level and after 5 min of reperfusion. Values are mean ± S.E.M. for six animals. RRPC: Remote Renal Preconditioning; Alpha-KG: Alpha-ketoglutarate; EDHB: Ethyl 3,4- dihydroxybenzoate; DDCA: Diethyldithiocarbamic acid; PEG 400: Polyethylene glycol 400. a: P < 0.05 vs. Control; b: P < 0.05 vs. RRPC
Effect of pharmacological interventions on coronary flow rate
Thirty min ischemia followed by 120 min reperfusion resulted in a marked decrease in coronary flow rate immediately, 5 min and 30 min after reperfusion as compared to basal. Remote renal preconditioning and pharmacological preconditioning with EDHB markedly attenuated I/R-induced decrease in coronary flow rate. Administration of α-KG and DDCA also abolished RRPC- and EDHB-induced restoration of coronary flow rate in a significant manner (Table 1/Fig. 4).
Effects of pharmacological interventions on coronary flow rate (ml min−1) at basal level, 0 min, 5 min, and 30 min after reperfusion. Values are mean ± SEM for six animals. RRPC: Remote Renal Preconditioning; Alpha-KG: Alpha-ketoglutarate; EDHB: Ethyl 3,4- dihydroxybenzoate; DDCA: Diethyldithiocarbamic acid; PEG 400: Polyethylene glycol 400. a: P < 0.05 vs. Control; b: P < 0.05 vs. RRPC
Discussion
In the present study, short episodes of occlusion and reperfusion of renal artery attenuated sustained ischemia reperfusion (I/R)-induced myocardial injury assessed in terms of reduction in release of myocardial enzymes (LDH and CK), infarct size, and improvement in coronary flow rate. The noted cardioprotective effect of remote preconditioning is supported by studies from our laboratory using abdominal aorta [7] and from other laboratories using cerebral arteries [3], mesenteric arteries [4],and renal arteries [6] for remote preconditioning.
Hypoxia inducible factor-prolyl 4-hydroxylases (HIF-P4H], a family of dioxygenases, has been reported to act as oxygen sensor and to play a crucial role in O2 homoeostasis [10]. Short duration of hypoxia/ischemia has been known to inhibit the activity of HIF-P4H [10], allowing HIF-ά to escape from prolyl hydroxylation and subsequent degradation [11]. Elevated levels of HIF-ά, due to HIF-P4H inhibition, have been shown to upregulate the gene expression of humoral factors [13], which confer resistance to tissues against sustained ischemic insult in diseases like myocardial infarction, stroke, etc. [14–16]. Moreover, inhibition of HIF-P4H and subsequent elevation of HIF-ά has been reported to play a key role in preconditioning-induced protective effects in heart [28], brain [17], and kidney [29]. In the present investigation, α-ketoglutarate, a selective HIF-P4H activator, abolished the cardioprotective effects of RRPC suggesting that inhibition of HIF-P4H may be playing an important role in RRPC induced cardioprotective effects. Further, pharmacological preconditioning with ethyl 3,4-dihydroxybenzoate (EDHB), a selective HIF-P4H inhibitor, mimicked the cardioprotective effect of RRPC suggesting that inhibition of HIF-P4H may confer protection to heart against I/R injury. So, it may be proposed that short episodes of hypoxia/ischemia during remote preconditioning inhibit HIF-P4H and subsequently upregulate humoral factors, which trigger a transduction pathway leading to cardioprotection against I/R injury. However, nature of cardioprotective humoral factors elevated due to HIF-P4H inhibition needs further investigation. Nevertheless, it is the first report highlighting a key role of HIF-P4H in RRPC-induced cardioprotective effects.
To explore the possible transduction mechanism triggered due to HIF-P4H inhibition during remote/pharmacological preconditioning, nuclear factor kappa B (NFkB) modulator was employed. Administration of diethyldithiocarbamic acid (DDCA), a selective inhibitor of NFkB, attenuated cardioprotective effect of RRPC suggesting the possible role of NFkB in RRPC-mediated cardioprotection. These results of present study are supported by earlier reports, indicating the involvement of NFkB in remote preconditioning [30] and ischemic preconditioning [21, 22]. Further, NFkB inhibitor also abolished pharmacological preconditioning (EDHB)-induced cardioprotective effect indicating that NFkB may be the downstream mediator of transduction pathway, triggered due to HIF-P4H inhibition. Inhibition of HIF-P4H has been shown to trigger signaling pathway leading to activation NFkB in tumor cell lines [23]. So it may be suggested that as a consequence of inhibition of HIF-P4H in pharmacological preconditioning (due to EDHB) or remote preconditioning (due to hypoxia), a transducing pathway is triggered involving activation of NFkB with subsequent cardioprotection. To our best of knowledge, it is the first report indicating the possible involvement of NFkB activation in a transducing pathway triggered by HIF-P4H inhibition in both remote and pharmacological preconditioning.
Conclusion
It may be concluded that inhibition of HIF-P4H is playing an important role in remote renal preconditioning induced cardioprotection. Further, remote preconditioning induced HIF-P4H inhibition may trigger a transduction pathway involving activation of NFkB.
Abbreviations
- HIF-P4Hs:
-
Hypoxia-inducible factor-prolyl 4-hydroxylases
- HIF-α:
-
Hypoxia-inducible factor
- EDHB:
-
Ethyl 3,4-dihydroxybenzoate
- NFkB:
-
Nuclear factor kappa-B
- DDCA:
-
Diethyldithiocarbamic acid
- KH:
-
Kreb’s Henseleit
- TTC:
-
Triphenyl tetrazolium chloride
- LDH:
-
Lactate dehydrogenase
- CK:
-
Creatine kinase
- RRPC:
-
Remote renal preconditioning
- I/R:
-
Ischemia–reperfusion
References
Kharbanda RK, Mortensen UM, White PA et al (2002) Transient limb ischemia induces remote ischemic preconditioning in vivo. Circulation 106:2881–2883
Przyklenk K, Baurer B, Ovize M et al (1993) Regional ischaemic “preconditioning” protects remote virgin myocardium from subsequent sustained coronary occlusion. Circulation 87:893–899
Tokuno S, Hinokiyama K, Tokuno K et al (2002) Spontaneous ischaemic events in the brain and heart adapt the hearts of severely atherosclerotic mice to ischemia. Arterioscler Thromb Vasc Biol 22:995–1001
Patel HH, Moore J, Hsu AK et al (2002) Cardioprotection at a distance: mesenteric artery occlusion protects the myocardium via an opioid sensitive mechanism. J Mol Cell Cardiol 34:1317–1323
Wang YP, Xu H, Mizoguchi et al (2001) Intestinal ischemia induces late preconditioning against myocardial infarction: a role for inducible nitric oxide synthase. Cardiovasc Res 49:391–398
Takaoka A, Nakae I, Mitsunami K et al (1999) Renal ischemia/reperfusion remotely improves myocardial energy metabolism during myocardial ischemia via adenosine receptors in rabbits: effect of remote preconditioning. J Am Coll Cardiol 33:556–564
Singh M, Sharma A (2004) Mechanism of cardioprotective effect of remote aortic preconditioning. In: Dhalla NS, Angel RA, Pierce GN (eds) Pathophysiology of cardiovascular diseases. Kluwer Academic Publishers, Boston, pp 277–285
Xia Z, Herijgers P, Nishida T et al (2003) Remote preconditioning lessens the deterioration of pulmonary function after repeated coronary artery occlusion and reperfusion in sheep. Can J Anaesth 50:481–488
Loukogeorgakis SP, Donald A, Charakida M et al (2005) Remote ischaemic preconditioning provides early and late protection against endothelial ischemia reperfusion injury in humans. J Am Coll Cardiol 46:450–456
Semenza GL (2001) HIF-1, O2, and the 3 PHDs: how animal cells signal hypoxia to the nucleus. Cell 107:1–3
Jaakkola P, Mole DR, Tian YM et al (2001) Targeting of HIF-α to the von Hippel–Lindau ubiquitylation complex by O2 regulated prolyl hydroxylation. Science 292:468–472
Bruick RK, McKnight SL (2001) A conserved family of prolyl 4-hydroxylases that modify HIF. Science 294:1337–1340
Kaelin WG (2005) Proline hydroxylation and gene expression. Annu Rev Biochem 74:115–128
Ockaili R, Natarajan R, Salloum F et al (2005) HIF-1 activation attenuates postischemic myocardial injury: role for heme oxygenase-1 in modulating microvascular chemokine generation. AJP—Heart and Circulatory Physiology 289:H542–H548
Natarajan R, Salloum FN, Fisher BJ et al (2006) Hypoxia inducible factor-1 activation by prolyl 4-hydroxylase-2 gene silencing attenuates myocardial ischemia reperfusion injury. Circ Res 98:133–140
Siddiq A, Ayoub IA, Chavez JC et al (2005) Hypoxia-inducible Factor Prolyl 4-Hydroxylase Inhibition. A target for neuroprotection in the central nervous system. ASBMB 280:41732–41743
Jones NM, Lee EM, Brown TG et al (2006) Hypoxic preconditioning produces differential expression of hypoxia-inducible factor-1alpha (HIF-1alpha) and its regulatory enzyme HIF prolyl hydroxylase 2 in neonatal rat brain. Neurosci Lett 404:72–77
Son ED, Choi GH, Kim H et al (2007) Alpha-ketoglutarate stimulates procollagen production in cultured human dermal fibroblasts and decreases UVB-induced wrinkle formation following topical application on the dorsal skin of hairless mice. Biol Pharm Bull 30:1395–1399
Sasaki T, Majamaa K, Uitto J (1987) Reduction of collagen production in keloid fibroblast cultures by ethyl-3,4-dihydroxybenzoate. Inhibition of prolyl hydroxylase activity as a mechanism of action. J Biol Chem 262:9397–9403
Valen G, Yan ZQ, Hansson GK (2001) Nuclear factor kappa-B and the heart. J Am Coll Cardiol 38:307–314
Kis A, Yellon DM, Baxter GF (2003) Role of nuclear factor-kappa B activation in acute ischemia–reperfusion injury in myocardium. Br J Pharmacol 138:894–900
Xuan YT, Tang XL, Banerjee S et al (1999) Nuclear factor KB plays an essential role in the late phase of ischemic preconditioning in conscious rabbits. Circ Res 84:1095–1099
Cummins EP, Berra E, Comerford KM et al (2006) Prolyl hydroxylase-1 negatively regulates IκB kinase-β, giving insight into hypoxia-induced NFκB activity. PNAS 103:18154–18159
Langendorff O (1885) Untersuchungen amuber lebenderer saugethierherzen. Pfluger Arch Gesmate Physiol 61:291–332
Klein HH, Pushman S, Schaper J et al (1981) The mechanism of the tetrazolium reaction in identifying experimental infarction. Virchows Arch 393:287–297
King JA (1959) A routine method for estimation of lactate dehydrogenase activity. J Med Lab Tech 16:265–272
Swanson JR, Wilkinson JH (1972) Measurements of creatine kinase in serum. Stand Methds Clin Chem 7:33
Belaïdi E, Béguin PC, Ribuot C et al (2006) Hypoxic preconditioning: role of transcription factor HIF-1alpha. Ann Cardiol Angeiol 55:70–73
Bernhardt WM, Câmpean V, Kany S et al (2006) Preconditional activation of hypoxia-inducible factors ameliorates ischemic acute renal failure. J Am Soc Nephrol 17:1970–1978
Li G, Labruto F, Sirsjo A et al (2004) Myocardial protection by remote preconditioning: the role of nuclear factor kappa-B p105 and inducible nitric oxide synthase. Eur J Cardiothorac Surg 26:968–973
Acknowledgments
The authors are grateful to Dr. Ashok Kumar Tiwary, Head, Department of Pharmaceutical Sciences and Drug Research, Punjabi University, Patiala, India for supporting this study and providing technical facilities for the work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kant, R., Diwan, V., Jaggi, A.S. et al. Remote renal preconditioning-induced cardioprotection: a key role of hypoxia inducible factor-prolyl 4-hydroxylases. Mol Cell Biochem 312, 25–31 (2008). https://doi.org/10.1007/s11010-008-9717-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-008-9717-5