Abstract
The aim of this study is the formulation of a new radiopharmaceutical for imaging solid tumor bearing. Gemcitabine is a nucleoside analogue used as chemotherapeutic agent. Gemcitabine was formulated and radiolabeled with one of the most important diagnostic radioactive isotopes (technetium-99m) to be investigated in solid tumor imaging. The labeling parameters such as gemcitabine amount, stannous chloride amount, pH of the reaction mixture, and reaction time were optimized. 99mTc–gemcitabine was prepared at pH 9 with a maximum labeling yield of 96 ± 0.3 % without any notable decomposition at room temperature over a period of 8 h. The preclinical evaluation and biodistribution in solid tumor bearing mice showed that 99mTc–gemcitabine had solid tumor selectivity, preclinical high biological accumulation in tumor cells and high retention. Tumor/normal muscle (T/NT) ratios increased with time showing high T/NT ratio (T/NT = 4.9 ± 0.27 at 120 min post injection) and high Tumor/Blood ratio (3.4 ± 0.06), suggesting 99mTc–gemcitabine as a novel solid tumor imaging agent.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tumor is one of the main courses of death worldwide. In world health organization had reported that tumor affected about third of population and caused quarter of the deaths in the developed world during the year 2000 [1]. Tumor cells are normal cells lost their normal regulatory mechanism resulting in high multiplication rate. When tumor increases in size, the disruption of the tumor blood supply will start leading to unbalance between O2 supply and consumption [1, 2]. This O2 unbalance will create the hypoxic domain, which is expressed, in about 50–60 % of the solid tumor [3, 4]. The early and accurate diagnosis of tumor will intensively improve the treatment plans for the patient. Tumor could be imaged invasively or noninvasively. The invasive methods are not suitable for routine clinical use because of their invasive nature, inconvenience and inability to acquire repeated measures [5]. The noninvasive method based upon using targeted radiopharmaceutical which use the difference of the pathological and physiological processes between tumor cells and normal one [6–10]. The target/non target (T/NT) ratio of the radiopharmaceutical expresses the ability of this radiopharmaceutical to specific tumor receptor [7, 9]. In literature, it has been considered that T/NT ratio greater than 1.5 proves the potentiality of the diagnostic agents [10–12]. The nitroimidazole analogues have received great attention as solid tumor imaging agents. These analogues showed some defects such as: lower tumor uptakes and slow blood clearance [13–18].
Currently, the positron emission tomography (PET) tracer such as: [18F] Fluoromisonidazole ([18F] FMISO), 2-deoxy-2-18F-fluoro-d-mannose ([18F] FDM) and 2-[18F] fluoro-2-deoxy-d-glucose (18F-FDG), have been used to evaluate solid tumor hypoxia. However, the short half life and high cost of the [18F] isotope restrict their wide application in clinical nuclear medicine [19–32]. Single-photon emission tomography (SPET) imaging also represents one of the standard technologies for most nuclear medicine departments [8, 33].
Recently, several 99mTc labeled radiopharmaceuticals such as 99mTc-meropenem, 99mTc-bombesin, 99mTc-citro-folate, 99mTc-sunitinib, 99mTc-PyDA (99mTc-pyrimidine-4,5-diamine), 99mTc(CO)3-Labeled-tetra-Peptides, 99mTc (CO)3-VIP (vasoactive intestinal peptide), 99mTc(CO)3-labeled chlorambucil analog, 99mTc-DMSAmetronidazole, 99mTc-BnAO-NI (3,3,10,10-tetramethyl-1-(2-nitro-1H-imidazo-1-y1)-4,9-diazadodecane-2,11-dionedioxime), 99mTc-nitride-pyrazolo[1,5-a]pyrimidine, 99mTcN-MAG-AMCPP (7-(2-aminoethylamino)-5-methyl-3-cyanopyrazolo[1,5-a]pyrimidine-N-mercaptoacetylglycine), 99mTc-DETA (Diethylenetriamine), 99mTc-TETA (Triethylenetetramine) and 99mTc-TEPA (Tetraethylenepentamine) have been reported [6, 34–45]. Also radioiodinated radiopharmaceutical as radioiodinated somatostatin analogue [Tyr3]octreotide, [131I]Iodoerythronitroimidazole and [131I] Iodomisonidazole (IMISO) [32, 46–49]. 99mTc-sestamibi (99mTc-MIBI) was used to image tumor [50, 51]. It was tested in Ehrlich Ascites Carcinoma (EAC) model and showed many disadvantage such as: low tumor/blood (T/B) ratio, low tumor-to-muscle (T/NT) ratio [52], very rapid blood clearance (few minutes) [53] and low tumor uptake (2.8 % ID/g) [54].
The introduction of new radiopharmaceutical for solid tumor imaging based upon pharmaceutical having specific receptor to solid tumor could increase the selectivity and enhance the imaging ability of the radiotracer [55].
Gemcitabine is one of the selective antitumor. Gemcitabine (dFdCyd) is an analogue of deoxycytidine which is the drug of choice for various solid tumors such as non-small cell lung cancer, pancreatic cancer, bladder cancer and breast cancer. It is also under investigation for the use in oesophageal cancer and lymphomas. Approximately 92–98 % of gemcitabine was eliminated via renal pathway [56–68].
The triphosphate analogue of gemcitabine inhibits DNA replication and arrest tumor growth. This mechanism is most likely by which gemcitabine causes cell death and there by determine antitumor activity. The diphosphate analogue of gemcitabine binds to ribonucleotide reductase (RNR) active site and inactivates the enzyme irreversibly. Once RNR is inhibited, the cell cannot produce the deoxyribonucleotides required for DNA replication and repair, so cell apoptosis is induced as shown in Fig. 1 [66–71].
In this study, gemcitabine was labeled with 99mTc and the parameters affecting labeling yield were studied to select the optimum conditions required to get high labeling yield with high purity. Biological evaluation of the 99mTc–gemcitabine was carried out in tumor bearing mice.
Experimental
Materials and equipments
Gemcitabine 2′, 2′-difluorodeoxycytidine (C9H11F2N3O4, M.Wt = 263.198 g/mol) was purchased from Sigma to Aldrich laborchemikalien GmbH D-30918 seelze (Germany) with purity ≥98 %. All chemicals were of analytical grade and were used directly without further purification. Deionized water was used in all experiments for the preparation of all solutions. Albino mice, each of 20–25 g, were used for the biological distribution study. A NaI (Tl) γ-ray scintillation counter (Scaler Ratemeter SR7 model, England) was used for the measurement of γ-ray radioactivity. Whatman No.1 paper chromatography (PC), Whatman International Ltd, Maidstone, Kent, UK. Technetium-99 m was eluted as 99mTcO4 − from 99Mo/99mTc generator, Gentech, Turkey.
Preparation of 99mTc–gemcitabine complex
Labeling procedure study
Gemcitabine was dissolved in N2-purged DMSO in an evacuated penicillin vial. The required amounts (0.25–3 mg) of gemcitabine were transferred to 10 ml clean vials which were kept under positive N2-gas pressure. Exactly the required SnCl2·2H2O amounts (3–200 µg) were added. After gently swirling, 1 ml of freshly eluted 99mTcO4 − (400 MBq) was added through sterilized syringes to each vial. The pH of the preparations was studied in range 5.0–11.0 at different reaction time followed by incubation at room temperature before investigations then the in vitro stability were studied at the optimum condition.
Labeling yield assay
The labeling yield and in vitro stability of 99mTc–gemcitabine were determined by paper chromatography (PC) and high performance liquid chromatography (HPLC).
PC analysis
The labeling yield and the in vitro stability of 99mTc–gemcitabine complex were assessed by ascending PC to evaluate the percent of 99mTc–gemcitabine, free 99mTcO4 − and reduced hydrolyzed-99mTc colloid species as follows [72–74]:
For each labeling experiment, ascending chromatography was carried out using two strips of Whatman No.1 paper chromatography (13 cm long and 0.5 cm wide). Two drops of the reaction product were spotted on line (origin) at distance of 2 cm from the bottom. One strip was developed with acetone and other strip was developed with ethanol: water: ammonium hydroxide mixture (2:5:1, v/v/v). After complete development, the two strips were dried, cut into 1 cm pieces and separately counted using the NaI(Tl) γ-ray scintillation counter to determine the ratio of the hydrolyzed 99mTc, free 99mTcO4 − and 99mTc–gemcitabine complex. Each experiment was repeated three times.
Acetone, as developing solvent, was used to develop one paper strip where the free 99mTcO4 − moved with the solvent front (R f = 1), while 99mTc–gemcitabine and reduced hydrolyzed technetium colloid remained at the origin.
A mixture of ethanol: water: ammonium hydroxide (2:5:1, v/v/v) as developing solvent to develop another paper strip where reduced hydrolyzed technetium colloid remained at the origin (R f = 0) while free 99mTcO4 − and 99mTc–gemcitabine species migrated with the solvent front (R f = 1).
The labeling yield percent of 99mTc–gemcitabine complex was determined as follows:
The labeling procedure using P.C. is a valid procedure showing precision as have acceptable degree of repeatability where percent of relative standard deviation less than 1 (%RSD < 1 %), intermediate precision as fulfill the acceptance criterion of pooled %RSD < 3 % defined in validation plan and showing linearity (R2 ≥ 0.99) as results proved a linear relationship between the measured activity vs. calculated activity.
HPLC analysis
The labeling yield was further confirmed by a Shimadzu HPLC system, which consists of pumps LC-9A and UV spectrophotometer detector (SPD-6A) operated at a wavelength of 234 nm. Chromatographic analysis was performed by injection of 40 mL from the reaction mixture of 99mTc–gemcitabine into a reversed-phase column (Lichrospher RP18, 4 mm × 250 mm; 5 µm). The column was eluted with mobile phase of (acetonitrile: water) (55:45 v/v) and the flow rate was adjusted to 0.5 mL/min. Then fractions of 0.5 mL were collected separately using a fraction collector up to 20 mL and counted in a well-type NaI (Tl) γ-scintillation counter.
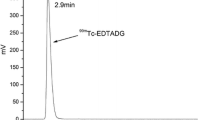
An HPLC chromatogram was presented in Fig. 2 showing two peaks, one at fraction No. 1, which corresponds to 99mTcO4 −, while the second peak was collected at fraction No. 3.8 for 99mTc–Gemcitabine which was found to coincide with the UV signal at retention time 3.5 min.
In-vitro stability of 99mTc–gemcitabine in serum
Stability of 99mTc–gemcitabine was studied in serum by mixing 1.8 ml of serum and 0.2 ml of 99mTc–gemcitabine complex and incubated at 37 °C for 12 h. Exactly 0.2 ml aliquots were withdrawn during the incubation at different time intervals up to 12 h and assayed using P.C. for determination of the in vitro stability of 99mTc–gemcitabine in serum.
Biodistribution study
The study was approved by the animal ethics committee and was in accordance with the guidelines set out by the Egyptian Atomic Energy Authority.
Tumor hypoxia induction in mice
The biodistribution study was done in tumor hypoxia bearing mice. The parent tumor line (Ehrlich Ascites Carcinoma) was withdrawn from 7 days old donor female Swiss Albino mice and diluted with sterile physiological saline solution to give 12.5 × 106 cells/ml. Exactly 0.2 ml solution was then injected intramuscularly in the right thigh to produce a solid tumor evaluated in female Albino Swiss mice weighting 20–25 g. The animals were maintained till the tumor development was apparent (4–6 days).
Biodistribution assay
A volume of 0.15 ml of 99mTc–gemcitabine complex containing 185–1,850 kBq was intravenously injected in the tail vein of mice. The animals were anesthetized by chloroform at the predesigned time interval and their body organs and fluids were separated, weighted and their radioactivities were assayed using a NaI(Tl) γ-ray scintillation counter. Biological distribution of 99mTc–gemcitabine complex in mice organs and fluids was studied as a function of time 20, 30, 60, 90, 120, 180 and 240 min post injection (p.i.). The percentages of the injected dose/g organ or fluids were calculated.
Experiment studying was repeated five times and differences in the data were evaluated with one way ANOVA test. Results for p are reported and all the results are given as mean ± SEM. The level of significance was set at p > 0.05.
Results and discussion
Factors affecting the percent labeling yield of 99mTc–Gemcitabine complex
Effect of gemcitabine amount
The gemcitabine was labeled with technetium-99 m using the direct technique, in which the Sn(II) chelate react with the reduced technetium-99m at pH 9 to form the labeled chelate according to the following equations [75]:
As shown in Fig. 3, at low gemcitabine amount (0.25 mg) the labeling yield was small to 46 ± 0.6 %. This low labeling yield was due to the gemcitabine amount was insufficient to react with the reduced form of technetium-99 m forming 99mTc–gemcitabine complex so; the remaining reduced form of technetium-99m was converted to reduced hydrolyzed technetium colloid (35 ± 0.1 %). By increasing the gemcitabine amount to 2 mg, the labeling yield was maximized to become 96.3 ± 0.03 % which was significantly higher than other yields (p < 0.001). By increasing the gemcitabine amount over the optimum values, the labeling yield was slightly decreased to 93.7 ± 0.019 % at 3 mg gemcitabine.
Effect of pH of the reaction mixture
Data presented in Fig. 4 reflects the results obtained from the labeling of gemcitabine with technetium-99m at different pH values (5–11). The labeling yield of the 99mTc–gemcitabine is maximum and significantly higher than other yields (p < 0.001) at pH 9 (96.3 ± 0.03 %). At pH below or above the optimum pH, the labeling yield is significantly decreased by forming reduced hydrolyzed technetium-99m which is the main radiochemical impurity.
Effect of SnCl2·2H2O amount
SnCl2·2H2O is the best reducing agent for reduction of 99mTc from (VII) to lower valence state, which facilitates its chelation with different organic molecules [70]. The results in Fig. 5 showed that, the maximum labeling yield of 99mTc–gemcitabine complex (96.3 ± 0.3 % at 10 µg of SnCl2·2H2O) was significantly higher than other yield (p < 0.001). Below this value, the percentage of free pertechnetate increased to 43.3 ± 0.012 % at 3 µg SnCl2·2H2O because SnCl2·2H2O is not sufficient for complete reduction of pertechnetate to form 99mTc–gemcitabine complex. By increasing the stannous chloride amount more than 10 µg, the labeling yield decreased again. This may be due to the fact that most of the gemcitabine were consumed in the formation of complexes, so the pertechnetate is reduced to insoluble technetium (IV) TcO2·xH2O in the absence of gemcitabine [75–77].
Effect of reaction time
The labeling yield of 99mTc–gemcitabine complex was studied at different reaction times (5–60 min). Figure 6 shows that the formation of 99mTc–gemcitabine complex was started relatively slowly with labeling yield of 80.9 ± 0.19 % at 5 min. The maximum yield of 99mTc–gemcitabine complex (96.3 ± 0.03 % at 30 min) had significantly higher than yields at 5 min and 15 min (p < 0.001) and not significantly difference with yields at 45 and 60 min (p > 0.05) because the labeling yield reaches the saturation value and not affected by increasing the reaction time above 30 min.
In-vitro stability of 99mTc–gemcitabine complex
The stability of 99mTc–gemcitabine complex was studied in order to determine the suitable time for injection to avoid the formation of the undesired products that result from the radiolysis and oxidation of the labeled compound during storage time post labeling with technetium, besides to the effect of ionizing γ-radiation (radiolysis). These undesired radioactive products may be accumulated in non-target organs.
The results show that 99mTc–gemcitabine complex was stable at a maximum yield of 96.3 ± 0.3 % with no significant decrease up to 8 h (p > 0.05).
In-vitro stability of 99mTc–gemcitabine in serum
The stability of 99mTc–gemcitabine complex in serum was determined by PC at different time. The results showed that, 99mTc–gemcitabine complex was stable in serum showing maximum labeling yield of 96.3 ± 0.3 % with no significant decrease up to 6 h (p > 0.05) then the stability decreased slightly showing labeling yield of 87.1 ± 0.3 % at 12 h.
Biodistribution
The results of biodistribution of 99mTc–gemcitabine in tumor bearing Albino mice are summarized in Table 1. Solid tumor and different body organ were assayed at different time intervals (20, 30, 90, 120, 180 and 240 min) (p.i.), and the results were expressed as the average percent of injected dose per gram of organ or fluid (% ID/g organ ± SEM) for five mice per group. The solid tumor uptake of 99mTc–gemcitabine (11.2 ± 0.38 % ID/g) was significant high at 120 min p.i. which clearly indicates the ability of 99mTc–gemcitabine to accumulate and localize selectively in solid tumor sites. The whole-body clearance of radioactivity was fast as the radioactivity level for 99mTc–gemcitabine in the blood was 5.9 ± 0.1 % ID/g at 60 min p.i. followed by a steady declining to 2.6 ± 0.06 % at 240 min p.i. 99mTc–gemcitabine has high Tumor/Blood ratio (T/B) (3.4 ± 0.06 at 120 min p.i.). The high radioactivity in kidney reflects that urinary pathway is the main elimination route for 99mTc–gemcitabine [68]. 99mTc–gemcitabine has significant high tumor-to-muscle (T/NT) ratio 4.9 ± 0.27 at 120 min p.i. as shown in Fig. 7.
As, the main important properties of diagnostic radiopharmaceutical to be used as a potential targeting for solid tumor are high tumor uptake, high T/NT and high T/B ratio [6, 10, 11]. 99mTc–gemcitabine has the advance over some radiopharmaceuticals for solid tumor imaging as follows:
99mTc–gemcitabine has higher solid tumor uptake than other radio-labeled pharmaceuticals such as [131I] Iodoerythronitroimidazole (1.28 % ID/g at 2 h p.i.), 99mTc (CO)3-VIP (0.4–1 % ID/g at 1 h p.i.), 99mTc-sestamibi (MIBI) (2.8 % ID/g at 1 h), 18F-FDM (2.17 % ID/g at 1 h p.i.) and 18F-FDG (2.4 % ID/g at 1 h p.i.) [19–32, 44].
The T/NT ratio of 99mTc–gemcitabine is higher than other radio-labeled pharmaceuticals such as 99mTc-meropenem (3.5 at 1 h p.i.), 99mTc-bombesin (4.5 at 4 h p.i.), 99mTc-citro-folate (4.3 at 4 h p.i.), 99mTc-sunitinib (3 at 1 h p.i.), 99mTc-PyDA (3 at 1 h p.i.), 99mTc(CO)3-labeled-tetra-peptides (3.95 at 2 h p.i.), 99mTc(CO)3-labeled chlorambucil analog (3.2 at 3 h p.i.), 99mTc-DMSAmetronidazole (2.57 at 4 h p.i.), 99mTc-BnAO-NI (2.59 at 2 h p.i.), 99mTcN-MAG-AMCPP (1.83 at 1 h p.i.), 99mTc-DETA (2.47 at 4 h p.i.), 99mTc-TETA (2.45 at 4 h p.i.), 99mTc TEPA (2.91 at 4 h p.i.), 99mTc-nitride-pyrazolo[1,5-a]pyrimidine (2.2 at 1 h p.i.) and 18F-FMISO (3.4 at 4 h p.i.) [6, 34–45]. Some labeled pharmaceuticals such as [131I] Iodomisonidazole (IMISO) and radioiodinated somatostatin analogue [Tyr3]octreotide showed high T/NT ratio with low tumor/blood ratio (0.75–1) restricting their potentiality as tumor hypoxia imaging agents [32, 46–49].
These data suggest that 99mTc–gemcitabine could be used as a potential agent for tumor imaging. Further studies will be carried out to evaluate the real potentiality of 99mTc–gemcitabine for the diagnosis of the human solid tumors.
Conclusion
In this study, novel 99mTc–gemicitabin can be easily prepared with high labeling yield of 96.3 ± 0.03 %, in vitro stability up to 8 h and in vitro stability in serum up to 6 h. 99mTc–gemicitabin accumulated specifically in the solid tumor with high T/NT ratio (4.9 ± 0.27) and high T/B ratio (3.4 ± 0.06) and was quickly cleared from most of the body organs suggesting that it could be used as potential diagnostic agent for solid tumor.
References
Harrison L, Blackwell K (2004) Oncologist 9(Suppl 5):31–40
Chapman JD, Engelhardt EL, Stobbe CC, Schneider RF, Hanks GE (1998) Radiother Oncol 46:229–237
Vaupel P, Mayer A (2007) Cancer Metastasis Rev 26:225–239
Hu M, Polyak K (2008) Curr Opin Genet Dev 18:27–34
Fukumoto M (2004) Ann Nucl Med 18(2):79–95
Zhang J, Yu Q, Huo J, Pang Y, Yang S, He Y, Tang T, Yang C, Wang X (2010) J Radioanal Nucl Chem 283:481–485
Schottelius M, Wester H (2009) Methods 48:161
Andre Lues BB, Luciene GM, Carolina AF, Monica CO, Alfredo MG, Valbert NC (2010) Bioorg Med Chem Lett 20(21):6182–6184
Santos-Cuevas CL, Ferro-Flores G, Murphy CA, Ramrez F, Luna-Gutiérrez MA, Pedraza-Lpez M, Garca-Becerra R, Ordaz-Rosado D (2009) Int J Pharm 375:75–83
Kanchan K, Sudhanand P, Aruna K, Archana M, Manu J, Meera V, Ambikalmajan MRP, Rama M, Natesan R (2007) Appl Radiat Isot 65(4):382–396
De Barros AL, Cardoso VN, Mota LD, Leite EA, de Oliveira MC, Alves RJ (2010) Bioorg Med Chem Lett 20(8):2478–2480
De Barros AL, Cardoso VN, Mota LG, Alves RJ (2010) Bioorg Med Chem Lett 20(1):315–317
Yang DJ, Kim C, Schechter NR, Azhdarinia A, Yu D, Oh C, Bryant JL, Won J, Kim EE, Podoloff DA (2003) Radiology 226(2):465–473
Chu TW, Li RJ, Hu SW, Liu XQ, Wang XY (2004) Nucl Med Biol 31(2):199–203
Kong DJ, Lu J, Ye SZ, Wang XB (2007) J Label Compd Radiopharm 50(21):420–449
Mallia MB, Mathur A, Subramanian S, Banerjee S, Sarma HD, Venkatesh M (2005) Bioorg Med Chem Lett 15(14):3398–3401
Mallia MB, Subramanian S, Banerjee S, Sarma HD, Venkatesh M (2006) Bioorg Med Chem 14(23):7666–7670
Mallia MB, Subramanian S, Mathur A, Sarma HD, Venkatesh M, Banerjee S (2008) Bioorg Med Chem Lett 18(19):5233–5237
Zhang Y, Chu TW, Gao XG, Liu XQ, Yang Z, Guo ZQ, Wang XY (2006) Bioorg Med Chem Lett 16(7):1831–1833
Faintuch BL, Teodoro R, Duatti A, Muramoto E, Faintuch S, Smith CJ (2008) Nucl Med Biol 35(4):401–411
Yang DJ, Wallace S, Cherif A, Li C, Gretzer MB, Kim EE, Podoloff DA (1995) Radiology 194(3):795–800
Bakheet SM, Powe J (1998) Semin Nucl Med 28(4):352–358
Kubota R, Yamada S, Kubota K, Ishiwata K, Tamahashi N, Ido T (1992) J Nucl Med 33(11):1972–1980
Kubota R, Kubota K, Yamada S, Tada M, Takahashi T, Iwata R, Tamahashi N (1995) J Nucl Med 36(3):484–492
Yamada S, Kubota K, Kubota R, Ido T, Tamahashi N (1995) J Nucl Med 36(7):1301–1306
Sugawara Y, Gutowski TD, Fisher SJ, Brown RS, Wahl RL (1999) Eur J Nucl Med 26(4):333–341
Reinhard MJ, Kubota K, Yamada S, Iwata R, Yaegashi H (1997) J Nucl Med 38(2):280–287
Gutowski TD, Fisher SJ, Moon R, Wahl RL (1992) J Nucl Med 33:925
Brown RS, Fisher SJ, Wahl RL (1993) J Nucl Med 34(1):75–82
Furumoto S, Shinbo R, Iwata R, Ishikawa Y, Yanai K, Yoshioka T, Fukuda H (2013) J Nucl Med 54(8):1354–1361
Henley T, Reddy MP, Ramaswamy MR, Lilien DL (2004) Clin Nucl Med 29(5):322–323
Yang DJ, Ilgan S, Higuchi T, Zareneyrizi F, Oh CS, Liu CW, Kim EE, Podoloff DA (1999) Pharm Res 16(5):743–750
Larson SM (1994) J Nucl Med 35:1653–1655
Sakr TM, Motaleb MA, Ibrahim IT (2012) J Radioanal Nucl Chem 292(2):705–710
Sakr TM, El-Safoury DM, Awad GA, Motaleb MA (2013) J Label Compd Radiopharm 56(8):392–395
Sakr TM, Essa BM, El-Essawy FA, El-Mohty AA (2014) Radiochemistry 56(1):76–80
Wan W, Yang M, Pan S, Yu C, Wu N (2008) Drug Dev Res 69(8):520–525
Altiparmak B, Lambrecht FY, Bayrak E, Durkan K (2010) Int J Pharm 400(1–2):8–14
De Barros AL, Mota LD, Ferreira CdeA, Oliveira MC, Góes AM, Cardoso VN (2010) Bioorg Med Chem Lett 20(21):6182–6184
Mallia MB, Subramanian S, Mathur A, Sarma HD, Venkatesh M, Banerjee S (2010) J Label Comp Radiopharm 53(8):535–542
Wang J, Yang J, Yan Z, Duan X, Tan C, Shen Y, Wu W (2011) J Radioanal Nucl Chem 287(2):465–469
Ding R, He Y, Xu J, Liu H, Wang X, Feng M, Qi C, Zhang J, Peng C (2012) Med Chem Res 21(4):523–530
Machac J, Krynyckyi B, Kim C (2002) Semin Nucl Med 32(4):276–292
Hruska CB, Conners AL, Jones KN, Weinmann AL, Lingineni RK, Carter RE, Rhodes DJ, O’Connor MK (2014) EJNMMI Res 4(1):5–18
Hsia CC, Huang FL, Hung LH, Shen LH, Chen CL, Wang HE (2011) Appl Radiat Isot 69(4):649–655
Kuchar M, Oliveira MC, Gano L, Santos I, Kniess T (2012) Bioorg Med Chem Lett 22(8):2850–2855
Baishya R, Nayak DK, Chatterjee N, Halder KK, Karmakar S, Debnath MC (2014) Chem Biol Drug Des 83(1):58–70
Breeman WAP, Hofland LJ, Bakker WH, Pluij M, Koetsveld PM, Jong M, Setyono-Han B, Kwekkeboom DJ, Visser TJ, Lamberts SWJ, Krenning EP (1993) Eur J Nucl Med 20(11):1089–1094
Maecke HR, Reubi JC (2011) J Nucl Med 52:841–844
Khalkhali I, Cutrone JA, Mena IG, Diggles LE, Venegas RJ, Vargas HI, Jackson BL, Khalkhali S, Moss JF, Klein SR (1995) Radiology 196(2):421–426
Palmedo H, Gr¨unwald F, Bender H, Schomburg A, Mallmann P, Krebs D, Biersack HJ (1996) Eur J Nucl Med 23(8):940–946
Barbarics E, Kronauge JF, Davison A, Jones AG (1998) Nucl Med Biol 25(7):667–673
Wackers FJT, Berman DS, Maddahi J, Watson DD, Beller GA, Strauss HW, Boucher CA, Picard M, Holman BL, Fridrich R (1989) J Nucl Med 30(3):301–311
Del Vecchio S, Ciarmiello A, Potena MI, Carriero MV, Mainolfi C, Botti G, Thomas R, Cerra M, D’Aiuto G, Tsuruo T, Salvatore M (1997) Eur J Nucl Med 24(2):150–159
Du C, Ying H, Zhou J, Jiang J, Liu C, Chen J, Wang X, Hu C (2014) Med Oncol 31(2):833–842
Anderson H, Hopwood P, Stephens RJ, Thatcher N, Cottier B, Nicholson M, Milroy R, Maughan TS, Falk SJ, Bond MG, Burt PA, Connolly CK, McIllmurray MB, Carmichael J (2000) Br J Cancer 83:447–453
Burris HA, Moore MJ, Andersen J, Green MR, Rothenberg ML, Modiano MR, Cripps MC, Portenoy RK, Storniolo AM, Tarassoff P, Nelson R, Dorr FA, Stephens CD, Von Hoff DD (1997) J Clin Oncol 15:2403–2413
Lorusso V, Pollera CF, Antimi M, Luporini G, Gridelli C, Frassineti GL, Oliva C, Pacini M, De Lena M (1998) Eur J Cancer 34:1208–1212
Spielmann M, Llombart Cussac A, Kalla S, Espié M, Namer M, Ferrero JM, Diéras V, Fumoleau P, Cuvier C, Perrocheau G, Ponzio A, Kayitalire L, Pouillart P (2001). Oncology 60:303–307
Lund B, Hansen OP, Theilade K, Hansen M, Neijt JP (1994) J Nat Cancer Inst 86:1530–1533
Einhorn LH, Stender MJ, Williams SD (1999) J Clin Oncol 17:509–511
Cormier Y, Eisenhauer E, Muldal A, Gregg R, Ayoub J, Goss G, Stewart D, Tarasoff P, Wong D (1994) Ann Oncol 5:283–285
Kubicka S, Rudolph KL, Tietze MK, Lorenz M, Manns M (2001) Hepatogastroenterology 48:783–789
Catimel G, Vermorken JB, Clavel M, Clavel M, de Mulder P, Judson I, Sessa C, Piccart M, Bruntsch U, Verweij J, Wanders J (1994) Ann Oncol 5:543–547
Mutch DG, Bloss JD (2003) Gynecol Oncol 90:S8–S15
Cerqueira NMFSA, Fernandes PA, Ramos MJ (2007) Chemistry 13(30):8507–8515
Matsuda A, Sasaki T (2004) Cancer Sci 95:105–111
Heinemann V, Xu YZ, Chubb S, Sen A, Hertel LW, Grindey GB, Plunkett W (1992) Cancer Res 52:533–539
Bouffard DY, Laliberte J, Momparler RL (1993) Biochem Pharmacol 45:1857–1861
Arpicco S, Lerda C, Dalla Pozza E, Costanzo C, Tsapis N, Stella B, Donadelli M, Dando I, Fattal E, Cattel L, Palmieri M (2013). Eur J Pharm Biopharm 85:373–380
Cosco D, Paolino D, Cilurzo F, Casale F, Fresta M (2012) Int J Pharm 422:229–237
Motaleb MA (2007) J Radioanal Nucl Chem 272:95–99
Hall AV, Solanki KK, Vinjamuri S, Britton KE, Das SS (1998) J Clin Pathol 51:215–219
Kashani R, Cooper MS, Das SS (2004) Nucl Med Commun 25(4):413–414
Motaleb MA, El-Kolaly MT, Ibrahim AB, Abd El-Bary A (2011) J Radioanal Nucl Chem 10:1058–1063
Srivastava SC, Richards P (1983) Technetium-labeled compounds. In: Rayudu GVS (ed) Radiotracers for medical applications, CRC series in radiotracers in biology and medicine. CRC Press, Boca Raton, pp 107–185
Wardell JL (1994) Tin: inorganic chemistry. In: King RB (ed) Encyclopedia of inorganic chemistry, vol 8. Wiley, New York, pp 4159–4197
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ibrahim, A.B., Sakr, T.M., Khoweysa, O.M.A. et al. Formulation and preclinical evaluation of 99mTc–gemcitabine as a novel radiopharmaceutical for solid tumor imaging. J Radioanal Nucl Chem 302, 179–186 (2014). https://doi.org/10.1007/s10967-014-3233-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10967-014-3233-8