Abstract
Objective
To present a decision support system for optimising mechanical ventilation in patients residing in the intensive care unit.
Methods
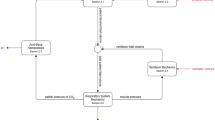
Mathematical models of oxygen transport, carbon dioxide transport and lung mechanics are combined with penalty functions describing clinical preference toward the goals and side-effects of mechanical ventilation in a decision theoretic approach. Penalties are quantified for risk of lung barotrauma, acidosis or alkalosis, oxygen toxicity or absorption atelectasis, and hypoxaemia.
Results
The system is presented with an example of its use in a post-surgical patient. The mathematical models describe the patient’s data, and the system suggests an optimal ventilator strategy in line with clinical practice.
Conclusions
The system illustrates how mathematical models combined with decision theory can aid in the difficult compromises necessary when deciding on ventilator settings.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Iotti GV (2001) Closed-loop control mechanical ventilation. Respir Care Clin N Am 7:341–515
Rudowski R, East TD, Gardener RM (1996) Current status of mechanical ventilation decision support systems: a review. Int J Clin Monit Comput 13:157–166
McKinley BA, Moore FA, Sailors RM, Cocanour CS, Marques A, Wright RB, Tonnesen AS, Wallace CJ, Morris AH, East TD (2001) Computerized decision support for mecnanical ventilation of trauma induced ARDS: results of a randomized clinical trial. J Trauma 50:415–425
Dojat M, Harf A, Touchard D, Lemaire F, Brochard L (2000) Clinical evaluation of a computer-controlled pressure support mode. Am J Respir Crit Care Med 161:1161–1166
Bouadma L, Lellouche F, Cabello B, Taillé S, Mancebo J, Dojat M, Brochard L (2005) Computer-driven management of prolonged mechanical ventilation and weaning: a pilot study. Intensive Care Med 31:1446–1450
Kwok HF, Linkens DA, Mahfouf M, Mills GH (2003) Rule-base derivation for intensive care ventilator control using ANFIS. Artif Intell Med 29:185–201
Keeney RL, Raiffa H. Decisions with multiple objectives. Cambridge University Press, 1993
Rutledge GW, Thomsen GE, Farr BR, Tovar MA, Polaschek JX, Beinlich IA, Sheiner LB, Fagan LM (1993) The design and implementation of a ventilator-management advisor. Artif Intell Med 5:67–82
Rudowski R, Kaye W, Garner CV, Greenburg AG. Clinical investigation of computerized decision support with coronary arterial bypass grafts patients. Biocyb Biomed Eng 1995; 15:81-2
Smith BW, Rees SE, Christensen TF, Karbing DS, Andreassen S. (2006) Getting the most from clinical data through physiological modelling and medical decision support. In: Rees S, ed, European Society for Computing and Technology in Anaesthesia and Intensive Care (ESCTAIC): Aalborg (Denmark), September 7–10, J Clin Monit Comput 2005; 20(2): 117-44
Kjærgaard S, Rees SE, Nielsen JA, Freundlich M, Thorgaard P, Andreassen S. Modelling of hypoxaemia after gynaecological laparotomy. Acta Anaesthesiol Scand 2001; 45:349-56
Rees SE, Andreassen S (2005) Mathematical models of oxygen and carbon dioxide storage and transport: The acid–base chemistry of blood. Crit Rev Biomed Eng 33(3):209–264
Andreassen S, Rees SE (2005) Mathematical models of oxygen and carbon dioxide storage and transport: interstitial fluid and tissue stores and whole body transport. Crit Rev Biomed Eng 33(3):265–298
Siggaard-Andersen O, Wimberly PD, Gøthgen I, Siggaard-Andersen M (1984) A mathematical model of the haemoglobin–oxygen dissociation curve of the human blood and of the oxygen partial pressure as a function of temperature. Clin Chem 30:1646–1651
Rees SE, Kjaergaard S, Thorgaard P, Toft E, Andreassen S (2002) The automatic lung parameter estimator (ALPE) system: non-invasive estimation of pulmonary gas exchange parameters in 10–15 minutes. J Clin Monit Comput 17:43–52
Andreassen S, Rees SE, Kjaergaard S, Thorgaard P, Winter SM, Morgan CJ, Alstrup P, Toft E (1999) Hypoxia after coronary by-pass surgery modelled by resistance to oxygen diffusion. Crit Care Med 27:2445–2453
Kjaergaard S, Rees SE, Malczynski J, Nielsen JA, Thorgaard P, Toft E, Andreassen S (2003) Non-invasive estimation of pulmonary shunt and ventilation-perfusion mismatch. Intensive Care Med 29:727–734
Rees SE, Malczynski J, Korup E, Kjaergaard S, Thorgaard P, Andreassen S, Toft E. Assessing pulmonary congestion in left sided heart failure using pulmonary gas exchange parameters. 25th Conference of the IEEE Engineering in Medicine and Biology Society (EMBS), 2003, 435-38
Kjaergaard S, Rees SE, Grønlund J, Lambert P, Nielsen EM, Thorgaard P, Andreassen S (2004) Hypoxaemia after cardiac surgery – clinical application of a model of pulmonary gas exchange. Eur J Anaesthesiol 4:296–301
Rasmussen BS, Sollid J, Rees SE, Kjaergaard S, Murley D, Toft␣E (2006) Oxygenation within the first 120 h following coronary artery bypass grafting. Influence of systemic hypothermia (32 degrees C) or normothermia (36 degrees C) during the cardiopulmonary bypass: a randomized clinical trial. Acta Anaesthesiol Scand 50(1):64–71
Rees SE, Kjærgaard S, Andreassen S, Hedenstierna G. Reproduction of MIGET retention and excretion data using a simple model of gas exchange in lung damage caused by oleic acid infusion. J Appl Physiol 2006; 101:826-32
Laffey JG, Kavanagh BP (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury, the acute respiratory distress syndrome. The acute respiratory distress network. N Engl J Med 342:1301–1308
Sakka SG, Reinhart K, Wegschneider K, Meier-Hellmann A (2000) Is the placement of a pulmonary artery catheter still justified solely for the measurement of cardiac output? J Cardiothorac Vasc Anesth 14:119–124
Rees SE, Allerød C, Kjærgaard S, Toft E, Thorgaard P, Andreassen S. Diagnosing patient state in intensive care patients using the Intelligent Ventilator (INVENT) system. In: Quagalini S, Barahona P, Andreassen S, eds, Artificial intelligence in using in medicine, 8th Conference on Artificial Intelligence in Medicine in Europe, AIME, Springer, 2001: 131-35
Reinhart K, Rudolph T, Bredle DL, Hannemann L, Cain SM (1989) Comparison of central-venous to mixed oxygen saturation during changes in oxygen supply/demand. Chest 95:1216–1221
Chawla LS, Zia H, Gutierrez G, Katz NM, Seneff MG, Shah M (2004) Lack of equivalence between central and mixed venous oxygen saturation. Chest 126:1891–1896
Farr B. Assessment of preference through simulated decisions scenarios. Ph.D. thesis, Section on Medical Informatics, Stanford University, Stanford, CA, 1991
Acknowledgements
This work was partially supported by a grant awarded by the IT-committee under the Danish Technical Research Council.
Author information
Authors and Affiliations
Corresponding author
Additional information
Rees SE, Allerød C, Murley D, Zhao Y, Smith BW, Kjærgaard S, Thorgaard P, Andreassen S. Using physiological models and decision theory for selecting appropriate ventilator settings.
Rights and permissions
About this article
Cite this article
Rees, S.E., Allerød, C., Murley, D. et al. Using physiological models and decision theory for selecting appropriate ventilator settings. J Clin Monit Comput 20, 421–429 (2006). https://doi.org/10.1007/s10877-006-9049-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-006-9049-5