Abstract
Nonalcoholic steatohepatitis (NASH) is a chronic inflammatory liver disease associated with insulin resistance and its metabolic consequences. Leukocyte mobilization, intrahepatic activation, and an exacerbated production of reactive oxygen species (ROS) and cytokines contribute to the development of NASH. Though alterations in peripheral blood (PB) T cell proportions and functionality remain unidentified, they might play a main role in NASH progression. We have compared the phenotype and Th1/Th2 commitment of peripheral immune cell reservoirs in adult patients and controls as well as the ability of neutrophils and monocytes to handle an ex vivo challenge. Also, we correlated those parameters with the main histological characteristics in NASH. Compared with controls, patients showed increased numbers of CD4+ cells and both CD4+ and CD8+ CD45RO subsets together with a higher frequency of IFN-γ-producing CD4+ and CD8+ T cells. We also found a decreased number of CD4+ and CD8+ CD45RA subsets. The distinctive production of IFN-γ highlights the significance of the observed skewed frequencies of PB T cells. Whereas ROS production by monocytes from NASH patients did not differ from controls, circulating neutrophils displayed a particularly higher phorbol myristate acetate-induced production of ROS. A negative correlation between oxidative burst and fibrosis grade was observed. This study reveals the presence of a characteristic profile of peripheral immune cells in NASH. We also discuss the probable influence of obesity on some of our present findings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The spectrum of nonalcoholic fatty liver diseases (NAFLD) ranges from simple fatty liver (hepatic steatosis) to nonalcoholic steatohepatitis (NASH) which is its more progressive form [1, 2]. The generation of intrahepatic oxidative stress and the activation of immune cells are important factors contributing to the pathogenesis of NAFLD [3, 4].
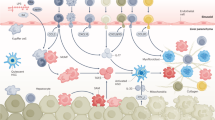
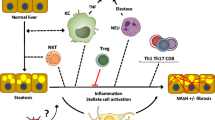
NASH occurs in a context defined by the presence of risk factors for the metabolic syndrome (Met S) and with insulin resistance as a well-identified etiological factor [5]. To be diagnosed as Met S, individuals may have central obesity plus two of four additional factors [6]. Visceral adipose tissue (VAT) from obese individuals is a source of soluble factors delivered to the liver via the portal vein. VAT is inflamed due to the influx of monocytes and the local activation into polarized proinflammatory macrophages termed M1. Also, the local expression of T cell chemokines is involved in the recruitment of inflammatory Th1 cells and effector CD8+ T cells. Inflammation causes insulin resistance, increased lipolysis, serum-free fatty acids flux, alteration of adipokine secretion, and consequently hepatic fat accumulation (steatosis) and hepatic insulin resistance.
NASH is histologically characterized by the presence of hepatic steatosis, ballooning, cell damage, and a mild portal and lobular infiltration of a small number of lymphocytes and polymorphonuclear leukocytes [7, 8]. Fibrosis progression on serial biopsies has been documented in approximately 30% of the cases [9, 10]. Even though the pathogenesis of NASH and especially the mechanisms involved in liver injury remain not fully understood, its current model is based on the “two-hit” hypothesis [11]. According to this hypothesis, an excessive accumulation of fat within hepatocytes represents the first hit [12]. This condition is believed to augment the sensitivity to a series of second multiple hits given by the complex interactions between liver resident cells, inflammatory mediators and reactive oxygen species (ROS) leading to cell death, inflammation, and fibrosis [13, 14]. Both hepatocytes and nonparenchymal cells, such as classically activated Kupffer cells (KC), along with newly recruited neutrophils and monocytes augment the sensitivity to second hits owing to their ability to secrete cytokines and to promote the influx of inflammatory cells and to produce ROS. As a consequence, the generation of oxidative stress speeds up the development and progression of NASH acting in a cooperative manner with proinflammatory cytokines [15]. In fact, the presence of by-products of lipid peroxidation within the liver in patients with NASH provides evidences for the involvement of the oxidative stress [16]. Those by-products promote the influx of inflammatory cells including lymphocytes as an additional source of proinflammatory cytokines in detriment to liver homeostasis [14]. The progression of NASH is assured because cytokines enhance the oxidative burst in resident and/or newly recruited cells [17].
The present study was designed to investigate the potential immunological alterations involving PB lymphocytes, monocytes, and neutrophils to gain information on the immunopathogenic aspects of NASH development. We aimed to examine the phenotype and Th1/Th2 commitment of PB T cells and the presence of hyper-responder monocytes and/or neutrophils in the blood. Also, we aimed to evaluate their potential correlation with histological features of NASH. To this end, we have studied the distribution of naïve (CD45RA) and memory (CD45RO) LT helper (CD4+) and cytotoxic (CD8+) peripheral subpopulations and assessed IFN-γ and IL-4 production by intracellular flow cytometry. We stimulated circulating monocytes and neutrophils with a protein kinase C activator to which cells respond in vitro [18] and evaluated the generation of ROS as an early marker of their inflammatory commitment [19].
Materials and Methods
Patients
Twenty adult patients with NASH (>18 years) from the Hepatology division of the Gastroenterology Hospital “Dr. C.B. Udaondo” and the Italian Hospital of Buenos Aires were enrolled in this study. The diagnosis of NASH was based on the following criteria: (1) absence of other causes of liver disease such as alcoholic hepatitis, chronic viral hepatitis, toxic hepatitis, primary biliary cirrhosis, or autoimmune hepatitis, (2) daily alcohol consumption minor to 20 g, and (3) typical characteristic features of NASH in the liver biopsy, including macrovesicular steatosis, lobular inflammation together with ballooning degeneration [20, 21]. Thirty age-matched (52 years; range, 43–69) lean healthy individuals were recruited among members of the staff of Immunogenetics at the Clinical Hospital “José de San Martin”. To ensure the voluntary participation, all the staff was given information of the study and those who intended to participate were told to make contact with the investigators. None of the controls had used medications; the alcohol ingestion was less of 20 g/day; and the body mass index (BMI) was less than 25 kg/m2. They stated neither to suffer from any metabolic condition such as diabetes, hypertension, or insulin resistance nor to have abnormal values of total cholesterol within 6 months previous to the study. All subjects were informed of the aim of the study and gave their written informed consent. The study was approved by the respective local Ethics Committees informed of internationally endorsed standards for the application of the Helsinki Declaration. A clinical evaluation, an ultrasonography and laboratory tests including liver enzymes aspartate aminotransferase (AST) and alanine aminotransferase (ALT), triglycerides, and cholesterol were performed to all patients.
Histologic Analysis
The histologic diagnosis was established using hematoxylin and eosin (H & E) and Masson's trichrome stain of formalin-fixed paraffin-embedded liver samples according to the nonalcoholic fatty liver disease scoring system [20]. Slides from all biopsies were examined by two pathologists that scored the liver histology by using previously published criteria. Activity grade was semi quantitatively assessed using a 9-point scale (steatosis = 0–3; lobular inflammation = 0–3; and ballooning = 0–2). Fibrosis stage was measured using a 5-point scale.
Reagents and Antibodies
Ficoll-Hypaque was purchased from Pharmacia Biotech (Uppsala, Sweden). RPMI 1640 was obtained from Life Technologies (Gaithersburg, MD, USA). Gentamicin, glutamine, gelatin, ionomycin, brefeldin A, and phorbol myristate acetate (PMA) were purchased from Sigma Chemical Co. (Saint Louis, MO, USA). Lysis buffer was made up of 50 ml distilled water, 0.415 g of ammonium chloride, 0.084 g of sodium bicarbonate, and 0.1 ml of 0.5 M EDTA (pH 7.3). 2′7′-Dichlorofluorescin diacetate (DCFH-DA; Sigma) was made up daily by dissolving 0.8 mg of DCFH-DA in 84 μl of methanol and 750 μl of phosphate-buffered saline (PBS) containing 5 mM glucose and 0.1% gelatin (PBSg). PMA was dissolved in dimethyl sulfoxide to give a 25-μg/ml stock solution and stored at −20°C. Monoclonal antibodies (mAbs), Cytofix/Cytoperm and Perm Wash buffer were purchased from Becton–Dickinson (BD; Mountain View, CA, USA).
Cell Isolation Procedures
Blood samples were collected by venous puncture in heparin at the time of diagnosis and immediately processed to obtain monocytes and neutrophils. Peripheral blood mononuclear cells (PBMC) were prepared by Ficoll-Hypaque density gradient centrifugation at 2,000 rpm at room temperature for 20 min. PBMC were washed twice in PBS, counted, and resuspended in RPMI 1640 with 10% fetal bovine serum, 2 mmol/L l-glutamine, and 50 μg/ml gentamicin. For neutrophil assays, 10 ml of lysis buffer were added to propylene tubes and 1 ml of whole blood was then added to each tube. Tubes were mixed by inverting and after 10 min were spun at 1,200 rpm for 10 min. Total leukocytes were washed twice in PBS and resuspended in RPMI medium to yield a final concentration of 106 cells/ml.
Monoclonal Antibodies and Cell-Surface Staining
The following mAbs conjugated with fluorescein isothiocyanate (FITC) or Peridinin-Chlorophyll-Protein Complex (PerCP) were used for flow cytometry analysis of peripheral blood subpopulations: CD4 (Leu3a/PerCP), CD8 (Leu2/PerCP), CD45 RA (HI100/FITC), and CD45 RO (UCHL1/FITC). IgG1 isotypes (G1CL–FITC) were used at the same concentration to control for nonspecific binding. After incubation with surface-specific mAbs for 30 min at 4°C, PBMC were washed and resuspended in PBS.
Intracellular Cytokine Detection
PMBC were stimulated with 25 ng/ml of PMA and 1 mM ionomycin, in the presence of 1 mM Brefeldin A for 4 h at 37°C. After stimulation, cell-surface staining was performed using PerCP anti-CD4 or anti-CD8 as describe above. After that, the cells were fixed during 20 min at 4°C with a fixation kit (BD) and then washed with the suitable permeabilization buffer (BD). PE-conjugated anti-IFN-γ or anti-IL-4 or the corresponding isotypes were added to the cells and incubated at 4°C for 40 min in the presence of 50 μl of permeabilization buffer.
DCFH Oxidation
PBMC or total leukocytes (106 cells per milliliter) were incubated with 10 μl of DCFH-DA in PBSg, yielding a final concentration of 5 μM, for 15 min at 37° with shaking. After washing the cells twice with PBS, cell stimulation was initiated with the addition of 100 ng/ml of PMA at 37°C for 20 min (polymorphonuclear cells) or 60 min (mononuclear cells). Basal ROS production by resting cells was evaluated by analyzing saline-treated preparations. Following stimulation, PBMC were incubated with anti-CD14 (M5E2/PE; 5 μl/106 cells) for 20 min at 4°C.
Fluorescence Cytometric Analysis
Gates were separately set on lymphocytes, monocytes, or neutrophils according to their forward- and side-scatter properties and used to collect events from tubes stained with the control isotypes or the different fluorochrome-conjugated mAbs.
For lymphocytes analysis, cells were gated on the basis of side-scatter and simultaneous CD4 or CD8 expression. The expression of CD45RO and CD45RA isoforms was analyzed in a similarly selected CD4 or CD8 gates.
For monocytes analysis, cells were gated in a FSC/SSC dot plot (R1). In population R1, CD14-expressing monocytes were further gated in the SSC/FL2-PE dot plot (R2). Finally, this R2 population was analyzed regarding its DCF fluorescence in the FL1-FITC histogram. On the other hand, neutrophils were gated in a FSC/SSC dot plot and then analyzed for their DCF fluorescence. An isotype-matched negative control antibody was used in all cases to assess background fluorescence intensity. Acquisition and analysis were performed on a FACSCalibur flow cytometer (BD) using the WinMDI software version 2.9.
Statistical Analysis
GraphPad Prism© software (GraphPad, San Diego, CA, USA) was used for all analyses. Normality was assessed by the Kolmogorov–Smirnov test. Because the majority of the values showed a distribution different from normal, a nonparametric Mann–Whitney U test was used. All values are expressed as median±standard deviation. Spearman’s rank correlation coefficients were used to test the association between immunological parameters measured and histological characteristics in patients with NASH. Those patients with no signs of fibrosis were excluded from the correlation analysis between immunological parameters and stage of fibrosis. The level of significance was fixed in all cases at p < 0.05.
Results
Demographical Features and Clinical and Histological Characterization of Patients with NASH
A complete characterization of the enrolled patients is shown in Table I. Patient's median age was 55 years (range, 43 to 72 years), and gender distribution showed 30% of male and 70% of female. According to reference values [22], all 20 adult patients with NASH showed elevated BMI, being 85% obese (85% showing obesity type II) and 15% overweighted. The serum AST and ALT levels were elevated in 35% and 80% of the samples, respectively. Abnormal lipid profile (increased cholesterol and/or triglycerides) was found in 55% of patients with NASH. In addition, about 55% of NASH patients suffer from diabetes while 45% have hypertension (data not shown). The histological features of the patient population are described in Table I. The degree of steatosis was generally severe (40% of patients) or moderate (40% of patients). Mild lobular inflammation was observed in about 75% of patients while moderate inflammation was seen in 20% of patients with NASH. Only one patient showed a severe pattern of inflammation. Mild degree of ballooned hepatocytes was exhibited by 85% of patients while 10% have a moderate degree. Only one patient showed no evidence of ballooning. Fifty percent of NASH patients demonstrated signs of fibrosis, 40% showing mild, 40% moderate, and 20% severe stage of fibrosis.
Differential Expression of CD45RO and CD45RA Within CD4+ and CD8+ Subpopulations
The size of CD4+ and CD8+ lymphocyte subpopulations was measured at the peripheral compartment. While total percentage of CD4+ cells was increased in patients with NASH (36.33 ± 9.23 vs. 29.08 ± 9.61; p = 0. 02; vs. Co), no differences between the study groups were found for the CD8+ subpopulation (16.73 ± 5. 22 vs. 13.68 ± 5.60; p = 0.93) (Fig. 1). The percentage of the CD45RO within the CD8+ subpopulation was higher in patients than controls (56.66 ± 10.21 vs. 47.14 ± 6.76; p = 0.01). Reciprocally, CD45RA cells were significantly decreased within the CD8+ subpopulation from patients with NASH (42.23 ± 9.73 vs. 66.04 ± 10.24; p < 0.001; vs. Co). Similarly, when assessing the same naïve and memory markers on the CD4+ subpopulation, an increased percentage of CD45RO (72.99 ± 5.09 vs. 60.38 ± 5.88; p = 0.013; vs. Co) and, reciprocally, a decreased percentage of CD45RA (29.45 ± 8.90 vs. 43.29 ± 6.62; p = 0.008; vs. Co) were evidenced in patients with NASH (Fig. 2). No significant correlations were found between these immunological parameters and histological features in NASH.
Distribution of CD4+ and CD8+ T cell subpopulations in peripheral blood. Patients 2–5, 8–12, and 19 (Table I) were studied. Representative dot plots of CD4 or CD8 expression vs. SSC for gating purpose (upper panels). The relative proportion of CD4+ in total cells in patients (NASH; n = 10) was higher than in healthy controls (Co; n = 10). The relative proportion of CD8+ in total cells did not differ between patients and controls. The box and whiskers show non-parametric statistics: median, lower and upper quartiles and confidence interval around the median (lower panel). The Mann–Whitney U test was used to determine significant differences between the two groups. *p < 0.05 was considered statistically significant
Distribution of naïve (CD45RA) and memory (CD45RO) T cell subsets within CD4+ and CD8+ peripheral blood subpopulations. Patients 2–5, 8–12, and 19 (Table I) were studied. Representative dot plots of CD45RA or CD45RO expression on CD4 or CD8 T cells in a NASH patient (upper panels). The proportion of CD4+ T cells expressing CD45RO was higher in patients (NASH; n = 10) than in healthy controls (Co) and, reciprocally, proportion of CD4+ T Cells expressing CD45RA was lower in NASH compared with controls. Likewise, the proportion of CD8+ T cells expressing CD45RO was higher in patients whereas the proportion of CD8+ expressing CD45RA was decreased in comparison to healthy controls. The box and whiskers show non-parametric statistics: median, lower and upper quartiles, and confidence interval around the median (lower panels). The Mann–Whitney U test was used to determine significant differences between the two groups. *p < 0.05 was considered statistically significant
An Increased Percentage of CD4+ IFN-γ+ and CD8+ IFN-γ+ T Cells in Patients with NASH
We used intracellular staining to study the expression of the most representative cytokines of Th1 (IFN-γ) and Th2 (IL-4) profiles in PBMC (Fig. 3). An increased frequency of IFN-γ-producing CD4+ T cells was detected in patients with NASH (21.97 ± 7.61) related to Co (3.78 ± 3.61; p = 0.011). In contrast, no differences were found for the frequency of IL-4-producing CD4+ cells between both groups. A higher frequency of IFN-γ-producing CD8+ T cells was also found in patients with NASH (35.15 ± 4.81 vs. 16.66 ± 3.75; p = 0.001; vs. Co). No significant correlations were found between the increased percentages of CD4+ IFN-γ+ and CD8+ IFN-γ+ T cells and histological features in NASH.
Percentage of IFN-γ- and IL-4-producing CD4+ and CD8+ cells in peripheral blood. Patients 8–10, 13, and 15–20 (Table I) were studied. Cells were gated on CD4 or CD8 vs. side-scatter dot plots. Representative dot plots of CD4 or CD8 cells showing intracellular IFN-γ and IL-4 in a NASH patient (upper panel). The percentages of IFN-γ-producing cells in total CD4+ and IFN-γ-producing cells in total CD8+ cells, respectively, were higher in patients (NASH; n = 10) compared with controls (Co; n = 10). No differences were found between both groups regarding IL-4-producing cells in CD4+ cells. The box and whiskers show non-parametric statistics: median, lower, and upper quartiles and confidence interval around the median values (lower panel). The Mann–Whitney U test was used to determine significant differences between the two groups. p value of <0.05 was considered statistically significant
Increased ROS Production in Circulating Neutrophils but Not in Monocytes from Patients with NASH
We compared the mean channel fluorescence intensities of the signals generated by monocytes or neutrophils on the basis of a stimulation index (SI) defined by the ratio between PMA-stimulated monocytes (or neutrophils) and non-stimulated monocytes (or neutrophils). After PMA stimulation, monocytes showed similar mean SI in patients and controls (2.99 ± 2.86 vs. 4.42 ± 3.02; p = 0.562) (Fig. 4). On the contrary, neutrophils from patients with NASH produced a higher amount of ROS as evidenced by their increased mean SI (21.01 ± 6.41 vs. 3.6 ± 1.45; p < 0.001; vs. Co) (Fig. 5). We found a negative correlation between SI generated by neutrophils and the stage of fibrosis (r = −0.91; p = 0.016). No significant correlations were found between SI generated by neutrophils and other histological features in NASH.
Stimulation Index in peripheral blood monocytes after challenge with PMA. Patients 1–8, 14, and 16 (Table I) were studied. PBMC were stimulated with PMA (100 ng/ml) for 60 min and stained with anti-CD14 to gate the monocyte population in forward-side scattering. Monocytes were selected in a FSC vs. SSC dot plot, and CD14+ monocytes were further gated in the SSC-H vs. CD14-PE dot plot (not shown). The resulting population was analyzed regarding its DCF fluorescence in the FL1-FITC histogram (upper panel, gated on monocytes). A Stimulation Index for monocytes was defined by the ratio between DCF fluorescence intensity (DCF-FI) in PMA-stimulated and non-stimulated (basal) monocytes. No differences were found for the stimulation index between patients (NASH; n = 10) and controls (Co; n = 13). Horizontal bars indicate median values (lower panel). A two-tailed Mann–Whitney U test was used to determine significant differences between the two groups
Stimulation Index in peripheral blood neutrophils after challenge with PMA. Patients 6–14 and 17 (Table I) were studied. Neutrophils were stimulated with PMA (100 ng/ml) for 20 min. A gate was made for the neutrophil subpopulation in a FSC vs. SSC dot plot and then analyzed for DCF fluorescence intensity (DCF-FI; upper panel, gated on neutrophils). A Stimulation Index for neutrophils was defined by the ratio between DCF-FI in PMA-stimulated and non-stimulated (basal) neutrophils. A higher median value for the stimulation index was found in patients (NASH; n = 10) than controls (Co; n = 10). Horizontal bars indicate median values (lower panel). A two-tailed Mann–Whitney U test was used to determine significant differences between the two groups
Discussion
Some immunological alterations involving circulating lymphocytes and neutrophils were found in patients with NASH revealing the presence of a particular profile of peripheral immune cells. Concerning PB we found in first place, a similar percentage of total CD8+ LT but increased CD8+ CD45RO and decreased CD8+ CD45RA subpopulations; second, increased percentages of total CD4+ and CD4+ CD45RO together with decreased CD4+ CD45RA subpopulation and third, an increased percentage of IFN-γ-producing CD4+ and CD8+ T cells. Concerning neutrophils, patients with NASH were characterized by an augmented production of ROS following stimulation with PMA. In those patients with NASH characterized by the presence of fibrosis, a negative correlation was found between the SI of neutrophils and fibrosis stage. Conversely, monocytes were not committed to an inflammatory phenotype in NASH.
Naïve and memory T cells can be phenotypically distinguished based on the expression of CD45 isoforms. Whereas memory T cells display CD45RO after the stimulation by antigens, naïve T cells carry CD45RA [23, 24]. The expression of CD45 isoforms on the surface of LT helpers and cytotoxic cells was extensively studied in healthy individuals [25, 26] and also searching for the establishment of the immunologic background in a large range of diseases. For instance, an altered profile of CD45 isoforms expression has been associated with metabolic diseases such as hypothyroidism and diabetes type 2 [27] and in many chronic hepatitis including hepatitis C and alcoholic cirrhosis [28, 29]. An abnormal distribution of circulating naïve and memory CD4+ T cells was also found in patients with primary biliary cirrhosis compared with controls. Notwithstanding the concomitantly analyzed liver infiltrating lymphocytes showed the same abnormality than PB lymphocytes, differences between patients and controls were markedly greater in the liver of those patients [30]. It remains as a possibility that the local proportion of lymphocyte subsets in patients with NASH might also differ from control livers.
NAFLD are considered the hepatic manifestation of the MetS. Accordingly, previously reported correlation between increased numbers of CD4+ and CD4+ CD45RO PB cells with clustered features of the MS [31] agrees with our present observations in patients with NASH. The increases of CD45RO together with the reciprocal decreases of CD45RA proportions at both CD4+ and CD8+ peripheral compartments might reflect an intrahepatic stimulatory process concerning the transition of CD45RA into CD45RO, which is well matched with the prevalence of autoimmune phenomena reported in NAFLD [32]. Alternatively, our results might reflect an imbalanced migration of lymphocyte subsets into the liver, but a complete analysis of signals that govern the lymphocyte recruitment into the liver remain to be performed.
The faint division between obesity and liver disease was demonstrated in a study of the hepatic expression patterns of inflammatory/immune response genes associated with obesity without steatosis (OWS), obesity with severe steatosis (OSS) and obesity in the context of NASH. The upregulation of a number of specific genes in NASH and not in OWS and OSS was revealed. Other genes are upregulated in OWS and OSS, and further increased in NASH. This study clearly indicates that some hepatic characteristics of obesity non NASH extends beyond established NASH. The majority of those NASH markers identified in the liver did not show a differential expression in the VAT of NASH patients vs. OWS and OSS [33]. This finding underlines the notion that the VAT constitutes an autonomous source of regulator molecules that might influence hepatic and/or systemic metabolic and immunological functions. Given that our study patients were obese or overweighed, we cannot completely rule out that our findings are influenced by an overall increase in body fat.
The important role ascribed to IFN-γ in hepatic damage is based on its capability to prime KC upon the co- recruitment of monocytes and lymphocytes into the inflamed liver, and also on its increased expression observed in experimental models of TNF-α related liver injury [34]. NASH is not considered a Th1-polarized disease; however, several studies have shown that an excessive production of Th1 proinflammatory cytokines and a deficit of anti-inflammatory cytokines are key players in its development [35, 36]. Among adaptive cells of the immune system, T lymphocytes play a major role in the inflammatory response and thus we hypothesized that an unregulated function might be critical for NASH. Our present data showing an increased Th1 phenotype within the peripheral CD4+ T cell population in NASH is intriguing. T cells as well as macrophages are recruited into human VAT [37]. Given that IFN-γ promotes macrophage activation in human adipose tissue [38], we can hypothesize that a potential vicious circle could be established, in which IFN-γ produced by the incoming CD4+ T cell population and probably also by effectors CD8+ T cells into the VAT might be capable to further sustain the M1 phenotype development of macrophages [39]. In addition, insulin sensitivity might be attenuated and human adipocyte differentiation might be suppressed by IFN-γ [40]. Thus, our results suggest that an intriguing interplay between M1 and Th1 polarization states might represent an interaction between the innate and adaptive immune systems in NASH.
IL-4 production, on the other hand, appeared to be related to a constitutional feature of the investigated individuals. Activation of innate immunity in NASH involves sequestration of both neutrophils and monocytes from blood into the liver [41–43].
The observed infiltration of neutrophils [44] led us to consider the probable involvement of PMN cells as potential causative factor within the complex pathophysiology of NASH. Innate cytokines like TNF-α and IL-1α are inducers of inflammatory chemokines produced not only by local sources but also by peripheral blood cells. These cytokines were recognized as sensitizing factors acting upon leukocyte infiltration of the liver [44]. Neutrophil recruitment can also be promoted by factors of the complement cascade triggered by hepatocyte apoptosis. These factors can further stimulate neutrophil respiratory burst thereby causing formation and diffusion of ROS into nearby cells. The resulting intracellular oxidative stress induces mitochondrial dysfunction and cell death amplifying hepatocytes damage and cytokines release [45–47] and contributes to stellate cell activation and hepatic fibrosis [48].
Our results suggest for the first time that the ability of peripheral neutrophils to handle the challenge provided by PMA is less in NASH patients than in control subjects. The negative correlation between SI generated by neutrophils and the stage of fibrosis demonstrates a relationship between a greater activation status of peripheral neutrophils and early fibrosis. In agreement, smaller amount of ROS were observed in liver cirrhosis patients compared with healthy subjects [49].
Through a functional study based on ROS generation we showed that oxygen metabolism of circulating monocytes was within the same range of values in patients with NASH and controls. The evaluation of additional markers of monocyte activation was out of our scope and remains to be examined. Once within the liver, the pivotal role reported for KC in NASH is not only the consequence of ROS production, but also by one or more steps of KC activation [50]. By instance, the lipid composition of the liver probably in addition with extra factors associated with obesity in NASH influences the oxidative burst in KC.
Conclusions
We clearly demonstrated the presence of an altered phenotype and functionality of circulating immune cells as a distinctive characteristic in adult patients with NASH. However, we cannot completely exclude the influence of an overall increase in body fat on some of our present findings.
References
Paschos P, Paletas K. Non alcoholic fatty liver disease and metabolic syndrome. Hippokratia. 2009;13:9–19.
Vuppalanchi R, Chalasani N. Non-alcoholic fatty liver disease and non-alcoholic steatohepatitis. Hepatology. 2009;49(1):306–17.
Zhan YT, An W. Role of liver innate immune cells in nonalcoholic fatty liver disease. World J Gastroenterol. 2010;16(37):4652–60.
Videla L. Oxidative stress signaling underlying liver disease and hepatoprotective mechanisms. World J Hepatol. 2009;1:72–8.
Pascale A, Pais R, Ratziu V. An overview of nonalcoholic steatohepatitis: past, present and future directions. J Gastrointestin Liver Dis. 2010;19(4):415–23.
Alberti GMM, Zimmet PM, Shaw J. Metabolic syndrome—a new world-wide definition. A consensus statement from the International Diabetes Federation. Diabet Med. 2006;23:469–80.
Brunt EM. Pathology of nonalcoholic steatohepatitis. Hepatol Res. 2005;33:68–71.
Brunt EM. Histopathology of non-alcoholic fatty liver disease. Clin Liver Dis. 2005;13(4):533–44.
Adams LA, Sanderson S, Lindor KD, Angulo P. The histological course of nonalcoholic fatty liver disease: a longitudinal study of 103 patients with sequential liver biopsies. J Hepatol. 2005;42:132–8.
Fassio E, Alvarez E, Dominguez N, Landeira G, Longo C. Natural history of nonalcoholic steatohepatitis: a longitudinal study of repeat liver biopsies. Hepatology. 2004;40:820–6.
Day C, James OFW. Steatohepatitis: a tale of two “hits”? Gastroenterology. 1998;114:842–5.
Basaranoglu M, Kayacetin S, Yilmaz N, Kayacetin E, Tarcin O, Sonsuz A. Understanding mechanisms of the pathogenesis of nonalcoholic fatty liver disease. World J Gastroenterol. 2010;16(18):2223–6.
Jasen PML. Nonalcoholic steatohepatitis. J Med. 2004;62:217–24.
Brunt EA, Kleiner DE, Wilson L, Unalp A, Behling CE, Lavine JE, et al. Portal chronic inflammation in nonalcoholic fatty liver disease. Hepatology. 2009;49(3):809–20.
Jaeschke H, Gores GJ, Cederbaum AI, Hinson JÁ, Pessayre D, Lemasters JJ. Mechanisms of hepatotoxicity. Toxicol Sci. 2002;65:166–76.
Seki S, Kitada T, Yamada T, Sakaguchi H, Nakatani K, Wakasa K. In situ detection of lipid peroxidation and oxidative DNA damage in non-alcoholic fatty liver diseases. J Hepatol. 2002;37:56–62.
Abdelmalek MF, Diehl AM. Mechanisms underlying nonalcoholic steatohepatitis. Drug Discov Today Dis Mech. 2006;3(4):479–88.
Vowells SJ, Sekhsaria S, Malech HL, Shalit M, Fleisher TA. Flow cytometric analysis of the granulocyte respiratory burst: a comparison study of fluorescent probes. J Immunol Methods. 1995;178:89–97.
Morel F, Doussiere JV, Vignais PV. The superoxide-generating oxidase of phagocytic cells. Physiological, molecular and pathological aspects. Eur J Biochem. 1995;201:523–46.
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology. 2005;41(6):1313–21.
Brunt EM, Janney CG, Di Bisceglie AM, Neuschwander-Tetri BA, Bacon BR. Nonalcoholic steatohepatitis: a proposal for grading and staging the histological lesions. Am J Gastroenterol. 1999;94:2467–74.
World Health Organization (WHO. Preventing and managing the global epidemic of obesity. Report of the World Health Organization Consultation of Obesity. World Health Organ Tech Rep Ser. 2000;894:i–xii. 1–253.
Berard M, Tough DF. Qualitative differences between naïve and memory T cells. Immunology. 2002;106:127–38.
Linton JP, Haynes L, Tsui L, Zhang X, Swain S. From naive to effector – alterations with aging. Immunol Rev. 1997;160:9–18.
Kimmig S, Przybylski GK, Schmidt CA, Laurisch K, Mowes B, Radbruch A, et al. Two subsets of naive T helper cells with distinct T cell receptor excision circle content in human adult peripheral blood. J Exp Med. 2002;195(6):789–94.
Richards SJ, Jones RA, Roberts BE, Patel D, Scott CS. Relationships between 2H4 (CD45RA) and UCHLl (CD45RO) expression by normal blood CD4+ CD8−, CD4− CD8+, CD4− CD8dim+, CD3+ CD4−CD8− and CD3− CD4−CD8− lymphocytes. Clin Exp Immunol. 1990;81:149–55.
Li QF, Li YP, Cheng PS. Peripheral T-lymphocyte subsets changes in patients with endocrine and metabolic diseases. Zhonghua Nei Ke Za Zhi. 1989;28(7):410–2.
Romo EM, Muñoz-Robles JA, Castillo-Rama M, Meneu JC, Moreno-Elola A, Perez-Saborido B, et al. Peripheral blood lymphocyte populations in end-stage liver diseases. J Clin Gastroenterol. 2007;41(7):713–21.
Arizcorreta A, Márquez M, Fernández-Gutiérrez C, Guzmán EP, Brun F, Rodríguez-Iglesias M, et al. T cell receptor excision circles (TRECs), CD4+, CD8+ and their CD45RO+ and CD45RA+ subpopulations in hepatitis C virus (HCV)-HIV-co-infected patients during treatment with interferon alpha plus ribavirin: analysis in a population on effective antiretroviral therapy. Clin Exp Immunol. 2006;146:270–7.
Leon MP, Spickett G, Jones DEJ, Bassendine MF. CD4+ T cell subsets defined by isoforms of CD45 in primary biliary cirrhosis. Clin Exp Immunol. 1995;99:233–9.
Tanigawa T, Iso H, Yamagishi K, Muraki I. Association of lymphocyte sub-populations with clustered features of metabolic syndrome in middle-aged Japanese men. Atherosclerosis. 2004;173:295–300.
Yatsuji S, Hashimoto E, Kaneda H, Taniai M, Tokushige K, Shiratori K. Diagnosing autoimmune hepatitis in nonalcoholic fatty liver disease: is the International Autoimmune Hepatitis Group scoring system useful? J Gastroenterol. 2005;40:1130–8.
Bertola A, Bonnafous S, Anty R, Patoraux S, Saint-Pauk MC, Iannelli A, et al. Hepatic expression patterns of inflammatory and immune response genes associated with obesity and NASH in morbidly obese patients. PLoS One. 2010;5(10):e13577.
Smith SR, Calzetta A, Bankowski J, Kenworthy-Bott L, Terminelli C. Lipopolysaccharide-induced cytokine production and mortality in mice treated with Corynebacterium parvum. J leukocyte Biology. 1993;54:23–9.
Maher J, Leon P, Ryan J. Beyond insulin resistance: Innate immunity in nonalcoholic steatohepatitis. Hepatology. 2008;48:670–8.
Guebre-Xabier M, Yang S, Lin HZ, Schwenk R, Krzych U, Diehl AM. Altered hepatic lymphocyte subpopulations in obesity-related murine fatty livers: potential mechanism for sensitization to liver damage. Hepatology. 2000;31:633–40.
Wu H, Ghosh S, Perrad XD, Feng L, Garcia GE, Perrad JL, et al. T-Cell accumulation and regulated on activation. normal T cell expressed and secreted upregulation in adipose tissue in obesity. Circulation. 2007;115:1029–38.
Kintscher U, Hartge M, Hess K, Foryst-Ludwig A, Clemenz M, Wabitsch M, et al. T-lymphocyte infiltration in visceral adipose tissue: a primary event in adipose tissue inflammation and the development of obesity-mediated insulin resistance. Arterioscler Thromb Vasc Biol. 2008;28:1304–10.
Mantovani A, Sozzani S, Locati M, Allavena P, Sica A. Macrophage polarization: tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol. 2002;23:549–55.
McGillicuddy FC, Chiquoine EH, Hinkle CC, Kim RJ, Shah R, Roche HM, et al. Interferon γ attenuates insulin signaling, lipid storage, and differentiation in human adipocytes via activation of the JAK/STAT pathway. J Biol Chem. 2009;284(46):31936–44.
Rensen SS, Slaats Y, Driessen A, Peutz-Kootstra CJ, Nijhuis J, Steffensen R, et al. Activation of the complement system in human nonalcoholic fatty liver disease. Hepatology. 2009;50(6):1809–17.
Leclerq LA. Antioxidant defence mechanisms: new players in the pathogenesis of non-alcoholic steatohepatitis? Clin Sci. 2004;106:235–7.
Lefkowitch JH, Haythe JH, Regent N. Kupffer cell aggregation and perivenular distribution in steatohepatitis. Mod Pathol. 2002;15:699–704.
Guo RF, Ward PA. Role of C5a in inflammatory responses. Annu Rev Immunol. 2005;23:821–52.
Mollnes TE, Brekke OL, Fung M, Fure H, Christiansen D, Bergseth G, et al. Essential role of the C5a receptor in E coli-induced oxidative burst and phagocytosis revealed by a novel lepirudin-based human whole blood model of inflammation. Blood. 2002;100:1869–77.
Jaeschke H, Smith CV, Clemens MG, Ganey PE, Roth RA. Mechanisms of inflammatory liver injury: adhesion molecules and cytotoxicity of neutrophils. Toxicol Appl Pharmacol. 1996;139:213–26.
Poniachik J, Csendes A, Díaz JC, Rojas J, Burdiles P, Maluenda F, et al. Increased production of IL-1alpha and TNF-alpha in lipopolysaccharide-stimulated blood from obese patients with non-alcoholic fatty liver disease. Cytokine. 2006;33(5):252–7.
Nieto N, Friedman SL, Cederbaum AI. Stimulation and proliferation of primary rat hepatic stellate cells by cytochrome P450 2E1-derived reactive oxygen species. Hepatology. 2002;35(1):62–73.
Panasiuk A, Wysocka J, Maciorkowska E, Panasiuk B, Prokopowicz D, Zak J, et al. Phagocytic and oxidative burst activity of neutrophils in the end stage of liver cirrhosis. World J Gastroenterol. 2005;11(48):7661–5.
Harte AL, da Silva NF, Creely SJ, McGee KC, Billyard T, Youssef-Elabd EM, et al. Elevated endotoxin levels in non-alcoholic fatty liver disease. J Inflamm. 2010;7(15):201.
Acknowledgments
We wish to thank the patients for their cooperation. We also thank Dr. A.E. Feldstein for proofreading our manuscript.
Source of Funding
This work was supported by the Buenos Aires University (UBACyT M010); CONICET (PIP 6104), and A.N.P.C.y T (06–257). The funding sources had no involvement in study design; in the collection, analysis, and interpretation of data; in the writing of the report; or in the decision to submit the paper for publication.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Inzaugarat, M.E., Ferreyra Solari, N.E., Billordo, L.A. et al. Altered Phenotype and Functionality of Circulating Immune Cells Characterize Adult Patients with Nonalcoholic Steatohepatitis. J Clin Immunol 31, 1120–1130 (2011). https://doi.org/10.1007/s10875-011-9571-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-011-9571-1