Abstract
Platinum-based chemotherapeutic drugs, including cisplatin, carboplatin, and oxaliplatin, have been used to manage cancer in spite of dose-dependent side effects, including nephrotoxicity, neurotoxicity and ototoxicity. These disadvantages have prompted the development of new strategies for cancer therapy that utilize functionalized nanoparticles as nanomedicines. In the present investigation, we have synthesized platinum nanoparticles using tea polyphenol (TPP) as both a reducing and surface modifying agent. The crystalline nature and morphology of the prepared TPP-functionalized platinum nanoparticles (TPP@Pt) were analyzed using X-ray diffraction (XRD) and transmission electron microscopy (TEM). The XRD results revealed that the TPP@Pt had a crystalline nature with a face-centered cubic structure. TEM imaging suggested that the TTP@Pt are flower shaped with a well-dispersed 30–60 nm-sized TPP@Pt formation. Cervical cancer cells (SiHa) were then treated with different concentrations of TPP@Pt. The effects of TPP@Pt on cell viability, nuclear morphology and cell cycle distribution were investigated. A cell viability assay revealed that the proliferation of SiHa cells was inhibited by TPP@Pt. Propidium iodide nuclear staining indicated that TPP@Pt induced nuclear fragmentation and chromatin condensation. Treatment with TPP@Pt significantly increased the percentage of cells in the G2/M phase, which indicates induced cell cycle arrest in the G2/M phase and an increased number of cells in the subG0 cell death phase. These findings highlight a potential use of TPP@Pt in cervical cancer treatment.
Graphical Abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Nanomedicine is an emerging research area in nanotechnology, and the potential scope of newly designed functional nanomaterials and their unique interactions at the cellular and molecular levels is broad, particularly for applications in the diagnosis, treatment and prevention of complex diseases such as cancers [1]. A variety of functional nanomaterials are being evaluated in clinical trials as drug carriers and for imaging of specific targets, with the aim of increasing the efficiency of drug bioavailability, reducing side effects and preventing damage to other tissues [2, 3]. For example, silica quantum dots, superparamagnetic iron oxides (for in vivo molecular imaging and therapy), functionalized carbon nanotubes (agents and/or vaccine adjuvants) and polymer nanocarriers (containing conventional cancer drugs for specific tumor cells) have been developed [3–6].
For many years, platinum-based molecules have received considerable attention because of their electrocatalytic properties [7, 8]. For instance, platinum-based therapeutic drugs, notably cisplatin and carboplatin, have been exploited in chemotherapy to kill cancer cells [8]. Platinum alloys have been employed in the invasive treatment of coronary artery disease, neuromodulation devices and catheters for the treatment of brain aneurysms [9]. However, these drugs are not selective for cancer cells, because normal cells are also affected, leading to substantial dose-limiting acute and chronic toxicities.
Functional platinum nanoparticles have evoked keen interest in recent decades owing to their size- and shape-dependent optical, catalytic and therapeutic properties. These properties can overcome the limits of conventional medicine, including lack of selectivity, poor pharmacokinetics and undesirable side effects [10–14]. Few platinum-based nanomaterials have been notable for excellent therapeutic applications [15–25]. Functional platinum nanoparticles have shown apoptosis-inducing properties through target-specific pathways [7–9, 26–28]. Porcel et al. [29] reported that the combination of platinum nanoparticles with ion irradiation enhanced the efficiency of cancer therapy. In addition, Manikandan et al. [30] demonstrated that 5–6 nm platinum nanoparticles have excellent biocompatibility, while laser treatment induced cell death in Neuro2A cell lines.
It is generally believed that the development of efficient green chemistry methods for the synthesis of metal nanoparticles may offer a potential method to overcome the shortcomings of current synthetic routes. Natural phytochemicals are non-nutritive biologically active chemical compounds that have antimicrobial, anti-inflammatory, anticancer and antioxidant properties. Several studies have attempted to evaluate the anticarcinogenic properties of phytochemicals such as carotenoids, flavonoids and phenolic acids [31–33]. Phytochemicals have induced apoptosis and cell cycle arrest in cell and animal studies [34]. The anticancer properties of phytochemicals were studied as a monotherapy or accompanied by chemotherapeutic drugs. Fortunately, certain phytochemicals produced a synergistic effect in cancer treatment when combined with chemotherapeutic drugs. For example, resveratrol exhibited synergism against human malignant mesothelioma [35].
Tea polyphenol (TPP) is a phytochemical extracted from tea leaves. TPP are effective free radical and singlet oxygen scavengers, possessing the potential to prevent a variety of diseases including cardiovascular, hepatic, renal, neural, pulmonary and intestinal diseases, as well as cancer, diabetes, and arthritis [36]. TPP contains catechins such as (+)-catechin, (−)-epicatechin, (−)-gallocatechin, (−)-epicatechin gallate, (−)-epigallocatechin and (−)-epigallocatechin gallate. Recent studies by our group have demonstrated that a combination of TPP and cisplatin treatment synergistically induced apoptosis through both caspase-8 and caspase-9 activation in breast cancer cells and might not produce side-effects [37]. Cervical cancer is a malignant neoplasm of the cervical area and is a major factor in women health problems in developing countries, killing 270,000 women each year. It is the second most common cancer worldwide and highly radio-resistant. At least 370,000 new cases are identified each year (WHO, 2010) [38, 39]. In this present investigation, we used green chemistry methods for synthesizing platinum nanoparticles using TPP as both a reducing and surface-modifying agent. Furthermore, we assessed the anticancer properties of prepared TPP-functionalized platinum nanoparticles (TPP@Pt) in human cervical cancer cells by assaying cell viability and examining nuclear morphological changes and cell cycle distribution using in vitro models. These molecules show promise as cytotoxic agents.
2 Materials and methods
2.1 Preparation of platinum nanostructures
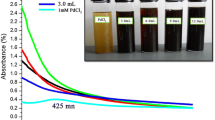
Platinum nanoparticles were fabricated using a green synthetic approach. Approximately 5 mL of tea polyphenol (Sigma, USA) was mixed with 25 mL of 0.001 M chloroplatinic acid (H2PtCl6–6H2O) (Sigma, India) solution under magnetic stirring. After a 1 h incubation at room temperature, the color of the precursor solution changed, indicating TPP@Pt formation. The products were purified by centrifugation. The isolated precipitate was washed twice with water.
2.2 Instrumentation
Shimadzu X 600 Powder X-Ray Diffractometer of Cu-Kα radiation 1.5414 Å was used in X-ray studies for phase identification of the TPP@Pt. For transmission electron microscopy (TEM) analysis, a drop of TPP@Pt nanostructures was dispensed directly onto a carbon-coated copper grid and allowed to dry completely in a vacuum desiccator. The prepared sample was analyzed using a JEOL TEM (Model JEM 2100, Japan).
2.3 Maintenance of SiHa cells
The cervical cancer cell line (SiHa) was provided by Prof. M.A. Akbarsha of the Mahatma Gandhi–Doerenkamp Center for Alternatives to Use of Animals in Life Science Education, Bharathidasan University, India. The cell line was maintained and propagated in 90 % DMEM containing 10 % fetal bovine serum (FBS) and 1 % penicillin/streptomycin. Cells were cultured as an adherent monolayer at approximately 70–80 % confluence and at 37 °C in a humidified atmosphere of 5 % CO2. Cells were harvested after brief trypsinization. Cells in the exponential growth phase were used in all experiments.
2.4 Cell viability assay
The MTT assay was performed as previously described by Blagosklonny and El-Diery [40]. Briefly, SiHa cells were plated to a density of 1 × 104 cells per well in 200 μL of fresh culture medium. After incubation overnight, the cells were treated with different concentrations (25–200 μg/mL) of TPP@Pt for 24 h. After incubation, 20 μL of MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide) solution [5 mg/mL in phosphate-buffered saline (PBS)] was added to each well. The plates were wrapped with aluminum foil and incubated at 37 °C for 4 h. The plates were centrifuged and the purple formazan product was dissolved by the addition of 100 μL of DMSO to each well. The absorbance was monitored at 570 nm (measurement) and 630 nm (reference) using a 96-well plate reader (Bio-Rad, CA, USA). Data collected for three replicates for each concentration of TPP@Pt were used to calculate the mean.
2.5 Detection of apoptosis by fluorescence microscopy
The nuclear morphology of treated SiHa cells was analyzed by exposing the cells to TPP@Pt (IC50 = 18.34 µg/mL; IC75 = 11.4 µg/mL) for 24 h. Control cells were grown in the same manner, but in the absence of TPP@Pt. Cells were trypsinized and fixed with 70 % ethanol. Cell nuclei were then stained by treatment with 1 mg/mL propidium iodide (PI) (Sigma) at 37 °C for 15 min in the dark. Stained cells were examined under a fluorescence inverted microscope (Carl Zeiss, Jena, Germany).
2.6 Cell cycle analysis
SiHa cells were plated at 2 × 105 cells/mL in a 6-well plate. After culturing for 24 h (37 °C, 5 % CO2), the cells were treated with IC50 (18.34 µg/mL) and IC75 (11.4 µg/mL) of TPP@Pt for 24 h. Following trypsinization, the cells were centrifuged at 1000×g for 10 min, and the pellet was resuspended in 0.5 mL PBS. Fixation was completed by adding 4.5 mL of cold 70 % ethanol and incubating at 4 °C for 16 h. The fixed cells were centrifuged at 1000×g for 10 min, and the pellet was suspended in 5 mL PBS. After being washed with PBS, the pellet was resuspended in 1 mL PI staining solution. After incubation at 37 °C for 15 min, the cells were analyzed to determine the cell cycle stage by a flow cytometer (BD FACSCanto™ II, San Jose, CA, USA) with an excitation wavelength of 488 nm and emission at 670 nm. The presented data are representative of those data obtained in at least three independent experiments conducted in triplicate.
2.7 Statistical analysis
Results are expressed as mean ± standard error (SE). All data were derived from at least three independent experiments with a similar pattern. For these calculations Calcusyn (Biosoft, UK) and Microsoft Excel software (Microsoft Corp., KY, USA) were used. For all comparisons, differences were considered statistically significant at P < 0.05.
3 Results and discussion
3.1 Physico-chemical properties of TPP@Pt
In recent years, green synthetic methods have been used for synthesizing many well-characterized metal nanoparticles. Green synthetic methods are eco-friendly routes of nanoparticle fabrication that mainly represent an alternative to chemical and physical methods, and can be used to increase selectivity, pharmacokinetics and desirable synergistic effects. Various metal nanoparticles have been synthesized using plant phytochemicals as reducing and stabilizing agents and also without the use of toxic and expensive chemicals [41, 42]. In this investigation, we developed a technique for synthesizing Pt-nanoparticles using TPP as reducing and stabilizing agents to obtain desired size- and shape-specific functionalized Pt nanoparticles. TPPs contain a variety of polyphenols, including epigallocatechin-3-gallate, (−)-epigallocatechin, epicatechin-3-gallate, and other catechins. Earlier studies have demonstrated that polyphenols have the potential to form chelating complexes with metal ions [43]. Very few studies have reported tea polyphenols being exploited for metal nanoparticle synthesis including silver, gold, palladium and iron [44, 45]. Similarly, our results revealed that TPP have the potential to reduce platinum ions at ambient temperatures. The crystalline nature of the prepared platinum nanoparticles was analyzed using an X-ray diffractometer (Fig. 1). The XRD pattern of prepared samples showed a peak at 39.4 ° (1 1 1), which corresponds to face-centered cubic platinum nanoparticles. This XRD result is well matched with previous reports [46]. Morphology and particle size of the prepared TPP@Pt were analyzed using TEM. Figure 2 shows TEM images of TPP@Pt, whose size varied between 30 and 60 nm (Fig. 2a and b). The TEM images suggested a well-dispersed TPP@Pt formation with a flower shape. The elemental profile of the prepared nanostructures was analyzed using TEM with an EDX setup. The EDX results (Fig. 3) showed Pt, C and Cu peaks, which suggested the presence of platinum nanoparticles. The Cu and C peaks correspond to the copper grid and TPP, respectively. Thus, these observations suggest that TPP reduced the platinum ions to platinum nanoparticles at ambient temperatures. Earlier studies have demonstrated that nanomaterials display size- and shape-dependent optical, catalytic and biological properties [47]. In addition, it is most important to minimize particle aggregation, because aggregated particles will affect not only particle delivery to the targeted cancer cells but also particle circulation inside the human body. The biological properties of flower-shaped platinum nanoparticles were analyzed on cervical cancer cell lines.
3.2 Cytotoxic effect of TPP@Pt
Generally, it is believed that malignant tumors develop due to deregulation of cellular proliferation, which is invariably associated with the inability of cells to undergo apoptosis. Most drug candidates induce cell death by modulating key elements of the apoptosis program and/or the cellular stress response [26–28]. Therefore, it is necessary to investigate the cytotoxicity, target specificity (apoptosis induction), and biocompatibility of the synthesized TPP@Pt. Therefore, the primary objective of the present study was to determine if a newly fabricated TPP@Pt would be cytotoxic to cervical cancer cells. Different assays were performed on TPP@Pt to measure cell death (apoptosis and necrosis). The SiHa cells were exposed to different concentrations (12.5, 25, 50, 100 and 200 µg/mL) of TPP@Pt for 24 and 48 h (Fig. 4). The TPP@Pt exhibited significant cell viability at lower concentrations from 12.5 to 200 μg/mL (at 24 and 48 h). On increasing the TPP@Pt concentration (12.5, 25, 50, 100 and 200 µg/mL), a noticeable dose-dependent decrease in relative cell viability was observed. The decreased cell viability in the presence of a high concentration of the nanoparticles might be due to their large surface area, although the dependency of cytotoxicity on the nature of the attached functional group cannot be ruled out. It is also evident from the literature that the factors contributing to cytotoxicity may include particle size (diameter) and surface functionalization of the materials. The TPP@Pt exhibited a cytotoxic effect on SiHa cells in both a dose- and time-dependent manner, as shown in Fig. 4. The prepared TPP@Pt showed IC50 and IC75 values were varied time dependently. For instance, the IC50 value of TPP@Pt is 18.34 µg/mL and <8 µg/mL for 24 and 48 h exposure respectively, whereas IC75 of TPP@Pt is 11.4 µg/mL and <8 µg/mL. Therefore, for consequent studies, we attained IC50 (18.34 µg/mL) and IC75 (11.4 µg/mL) correspondingly.
3.3 Effect of TPP@Pt on nuclear morphology
To confirm the mode of cell death, a PI-based nuclear staining assay was performed to observe nuclear fragmentation and other morphological changes in cells. Many experts have suggested that PI-based nuclear staining is a better method to interpret cell apoptosis/cytotoxicity measurements compared to the MTT assay; this staining also measures nuclear abnormalities such as fragmentation of the nucleus, a hallmark of late apoptosis. In our study, cells were treated with IC50 (18.34 µg/mL) and IC75 (11.4 µg/mL) concentrations of TPP@Pt for 24 and 48 h. The nuclear morphology of cells was examined using PI staining under a fluorescence microscope. In the treated cells, chromatin fragmentation, mitotic phase chromosome arrangements, binucleation, chromatin condensation and nuclear swelling were observed. The fluorescence microscopic images of TPP@Pt in treated and untreated (control) SiHa cells is shown in Fig. 5. This result indicates that TPP@Pt induced nuclear morphological changes (Fig. 5) via apoptosis. When compared to controls, the treated cells showed a higher percentage of cells with abnormal nuclear patterns following treatment with increasing concentrations of TPP@Pt. Data collected from the manual counting of cells with normal and abnormal nuclear features are shown in Fig. 5, showing that the number of apoptotic cells increased in both a time- and dose-dependent manner. Platinum-based therapeutic drugs, notably cisplatin and carboplatin, have been exploited in chemotherapy to kill cancer cells [26–28]. Hikosaka et al. [26] demonstrated that platinum nanoparticles showed similar activity to that of oxidizing nicotinamide adenine dinucleotide (NADH) and reducing ubiquinone (CoQ10). Moreover, Kajita et al. [27] reported platinum nanoparticles have unveiled antioxidant properties that scavenge ROS, including superoxide anion (O2 −), hydrogen peroxide (H2O2) and free radicals. In addition, recent studies have reported that nanomaterials induced cell death based on their size, shape and surface area [48, 49]. TPP were mainly used as both a reducing and stabilizing agent for TPP@Pt fabrication; these molecules contain several polyphenols and exhibit potential chemo preventive and antioxidant properties on the platinum nanoparticles surfaces. Moreover, tea catechin compounds have been shown to exhibit cytostatic properties in many tumor models [50, 51]. Furthermore, TPP have been shown to induce apoptosis in U937 cells and to enhance apoptosis in human colon cancer (HCT116) cells [52]. Catechin hydrate (CH) exhibits anticancer effects by blocking the proliferation of MCF7 cells and inducing apoptosis [37, 53]. The dose- and time-dependent cytotoxic effects clearly indicate that TPP@Pt can interact with the intracellular environment via binding to DNA and proteins. Our results demonstrated that flower shaped TPP@Pt induce cytotoxicity on human cervical cancer cells.
3.4 Cell cycle analysis
The cell cycle is a vital regulator of the cell proliferation and growth process, which protects the cell from DNA damage. DNA damage-induced cell cycle arrest can activate cell death via apoptosis. We evaluated the effect of TPP@Pt on the cell cycle of human cervical cancer cells by flow cytometry. SiHa cells were exposed to different concentrations (IC50 = 18.34 µg/mL and IC75 = 11.4 µg/mL) of TPP@Pt for 24 h. The cell cycle distribution is shown in Fig. 6a, b and c. The proportion of cells in G0/G1 and S phase significantly decreases (P < 0.05), accompanied by an increase in the proportion of cells in the G2/M phase (Fig. 6d). TPP@Pt induced a dose-dependent cell phase distribution in SiHa cells, which indicates G2/M phase cell cycle arrest due to the DNA damage. The cell cycle results are consistent with nuclear morphological changes. Our present investigation clearly indicates that TPP@Pt inhibit cell proliferation via induction of apoptotic cell death. In addition, this present study suggests that TPP@Pt produce a cytotoxic effect by reducing cell viability and causing internucleosomal DNA fragmentation, G2/M cell cycle arrest and hypo-diploid accumulation, and they should be applicable as a potential therapeutic agent for human cervical cancer. Earlier studies demonstrated that the platinum-based therapeutic agent satraplatin induced apoptosis via G2/M phase cell cycle arrest [50]. Moreover, Shingu et al. [54] synthesized a polynuclear platinum compound that induced early G2/M phase arrest, accompanied by later apoptosis. A previous study demonstrated that G2/M phase arrest in response to DNA damage can lead to a variety of fates, including apoptosis, prolonged permanent arrest, and recovery after repair of DNA damage or adaptation to the damage, allowing progression through the cell cycle with the DNA damage that initially evoked the arrest [55]. The cells emerging from G2 arrest either progress through the cell cycle or apoptotic cell death [56]. In the future, the effects of functionalized TPP@Pt in in vitro and in vivo cancer models will be evaluated at cellular and molecular levels.
Effects of TPP@Pt on cell cycle distribution. (a–c) Histogram representing the propidium iodide (PI) staining of TPP@Pt-treated and untreated SiHa cells for 24 h [a Control, b IC50 and c IC75] d Bar diagram showing the cell distribution in the sub-G0, G0/G1, S, and G2/M phases for SiHa cells treated with and without TPP@Pt. The data represent the mean ± SE of triplicate
4 Conclusion
Biosynthesis of TPP@Pt using tea polyphenols is a cheap, simple and eco-friendly process. In this present investigation, TPP@Pt were synthesized using TPP as both a reducing and surface modifying agent. The synthesized TPP@Pt were characterized by various techniques, including UV–Vis spectroscopy, TEM, XRD, and EDX. TEM images showed well dispersed 30–60 nm-sized TPP@Pt with flower shapes. The TPP@Pt have cytotoxic properties that inhibit cell proliferation and induce apoptosis in human cervical cancer cells. In the cell cycle phase distribution, TPP@Pt triggered the G2/M phase cell cycle arrest. These findings emphasize that the TPP@Pt have potential anticancer properties and can be applied as cancer therapeutics. In the future, the molecular-level mechanism of TPP@Pt action on cancer cells will be studied. Furthermore, target-specific functionalization of TPP@Pt may lead to their application cancer therapy.
References
Jee J, Na JH, Lee S, Kim SH, Choi K, Yeo Y, Kwon IC. Cancer targeting strategies in nanomedicine: design and application of chitosan nanoparticles. Curr Opin Solid State Mater Sci. 2012;16:333–42.
Rosenholm JM, Sahlgren C, Lindén M. Towards multifunctional, targeted drug delivery systems using mesoporous silica nanoparticles–opportunities & challenges. Nanoscale. 2010;2:1870–83.
Bourzac K. Nanotechnology: carrying drugs. Nature. 2012;491:S58–60.
Rosenblum LT, Kosaka N, Mitsunaga M, Choyke PL, Kobayashi H. In vivo molecular imaging using nanomaterials: general in vivo characteristics of nano-sized reagents and applications for cancer diagnosis (Review). Mol Membr Biol. 2010;27:274–85.
Pescatori M, Davide B, Enrica V, Cécili M, Camilla B, Elena M, Andrea P, et al. Functionalized carbon nanotubes as immunomodulator systems. Biomaterials. 2013;34:4395–403.
Delogu LG, Enrica V, Roberto M, Gérard AP, Ciriaco C, Roberto M, Luciano M, Francesco S, et al. Ex vivo impact of functionalized carbon nanotubes on human immune cells. Nanomedicine. 2012;7:231–43.
Stephens IEL, Bondarenko AS, Grønbjerg U, Rossmeisl J, Chorkendorff I. Understanding the electrocatalysis of oxygen reduction on platinum and its alloys. Energy Environ Sci. 2012;5:6744–62.
Kostova I. Platinum complexes as anticancer agents. Recent Pat Anti-Cancer Drug Discov. 2006;1:1–22.
Cowley A. On the use of platinum in biomedical applications. In: The 4th International Platinum Conference, Platinum in transition Boom or Bust, The Southern African Institute of Mining and Metallurgy, 2010.
Daniel MC, Astruc D. Gold nanoparticles: assembly, supramolecular chemistry, quantum-size-related properties, and applications toward biology, catalysis, and nanotechnology. Chem Rev. 2004;104:293–346.
Cuenya BR. Synthesis and catalytic properties of metal nanoparticles: size, shape, support, composition, and oxidation state effects. Thin Solid Films. 2010;518:3127–50.
Kelly KL, Coronado E, Zhao LL, Schatz GC. The optical properties of metal nanoparticles: the influence of size, shape, and dielectric environment. J Phys Chem B. 2003;107:668–77.
Pal S, Tak YK, Song JM. Does the antibacterial activity of silver nanoparticles depend on the shape of the nanoparticle? A study of the gram-negative bacterium escherichia coli. Appl Environ Microbiol. 2007;73:1712–20.
Park S, Xie Y, Weaver MJ. Electrocatalytic pathways on carbon-supported platinum nanoparticles: comparison of particle-size-dependent rates of methanol, formic acid, and formaldehyde electrooxidation. Langmuir. 2002;18:5792–8.
Bendale Y, Bendale V, Paul S, Bhattacharyya SS. Green synthesis, characterization and anticancer potential of platinum nanoparticles bioplatin. Chin J integr med. 2012;10:681–9.
Endo K, Ueno T, Kondo S, Wakisaka N, Murono S, Ito M, Kataoka K, Kato Y, Yoshizaki T. Tumor-targeted chemotherapy with the nanopolymer-based drug NC-6004 for oral squamous cell carcinoma. Cancer Sci. 2013;104:369–74.
Hou J, Shang J, Jiao C, Jiang P, Xiao H, Luo L, Liu T. A core cross-linked polymeric micellar platium(IV) prodrug with enhanced anticancer efficiency. Macromol Biosci. 2013;13:954–65.
Min Y, Li J, Liu F, Yeow EK, Xing B. NIR light mediated photoactivation pt based antitumor prodrug and simultanous cellular apoptosis imaging via upconversion nanoparticles. Angew Chem Int Ed Engl. 2014;53:1012–6.
Mironava T, Simon M, Rafailovich MH, Rigas B. Platinum folate nanoparticles toxicity: cancer vs. normal cells. Toxicol In Vitro. 2013;27:882–9.
Pandey A, Kulkarni A, Roy B, Goldman A, Sarangi S, Sengupta P, Phipps C, Kopparam J, Oh M, Basu S, et al. Sequential application of a cytotoxic nanoparticle and a PI3 K inhibitor enhances antitumor efficacy. Cancer Res. 2014;74:675–85.
Rout SR, Behera B, Maiti TK, Mohapatra S. Multifunctional magnetic calcium phosphate nanoparticles for targeted platin delivery. Dalton Trans. 2012;41:10777–83.
Sengupta P, Basu S, Soni S, Pandey A, Roy B, Oh MS, Chin KT, Paraskar AS, Sarangi S, Connor Y, et al. Cholesterol-tethered platinum II-based supramolecular nanoparticle increases antitumor efficacy and reduces nephrotoxicity. Proc Natl Acad Sci U S A. 2012;109:11294–9.
Wang J, Wang X, Song Y, Zhu C, Wang K, Guo Z. Detecting and delivering platinum anticancer drugs using fluorescent maghemite nanoparticles. Chem Commun (Camb). 2013;49:2786–8.
Yang J, Sun X, Mao W, Sui M, Tang J, Shen Y. Conjugate of Pt(IV)-histone deacetylase inhibitor as a prodrug for cancer chemotherapy. Mol Pharm. 2012;9:2793–800.
Yoshihisa Y, Zhao QL, Hassan MA, Wei ZL, Furuichi M, Miyamoto Y, Kondo T, Shimizu T. SOD/catalase mimetic platinum nanoparticles inhibit heat-induced apoptosis in human lymphoma U937 and HH cells. Free Radic Res. 2011;45:326–35.
Hikosaka K, Kim J, Kajita M, Kanayama A, Miyamoto Y. Platinum nanoparticles have an activity similar to mitochondrial NADH: ubiquinone oxidoreductase. Colloids Surf B. 2008;66:195–200.
Kajita M, Hikosaka K, Iitsuka M, Kanayama A, Toshima N, Miyamoto Y. Platinum nanoparticle is a useful scavenger of superoxide anion and hydrogen peroxide. Free Radic Res. 2007;41:615–26.
Nellore J, Pauline C, Amarnath K. Bacopa monnieri phytochemicals mediated synthesis of platinum nanoparticles and its neurorescue effect on 1-methyl 4-phenyl 1, 2, 3, 6 tetrahydropyridine-induced experimental parkinsonism in zebrafish. J Neurodegener Disord. 2013;2013:972391.
Porcel E, Liehn S, Remita H, Usami N, Koayashi K, Furusawa Y, Lesech C, Lacombe S. Platinum nanoparticles: a promising material for future cancer therapy? Nanotechnology. 2010;21:085103–10.
Manikandan M, Hasan N, Wu HF. Platinum nanoparticles for the photothermal treatment of Neuro 2A cancer cells. Biomaterials. 2013;34:5833–42.
Wang S, Meckling KA, Marcone MF, Kakuda Y, Tsao R. Can phytochemical antioxidant rich foods act as anti-cancer agents? Food Res Int. 2011;44:2545–54.
Liu RH. Potential synergy of phytochemicals in cancer prevention: mechanism of action. J Nutr. 2004;134:3479S–85S.
Marchand L, Murphy S, Hankin JH, Wikens LR, Kolonel LN. Intake of flavonoids and lung cancer. J Natl Cancer Inst. 2000;92:154–60.
Sun J, Liu RH. Cranberry phytochemical extracts induce cell cycle arrest and apoptosis in human MCF-7 breast cancer cells. Cancer Lett. 2006;241:124–34.
Lee YJ, Lee YJ, Im JH, Won SY, Kim YB, Cho MK, Nam HS, Choi YJ, Lee SH. Synergistic anti-cancer effects of resveratrol and chemotherapeutic agent clofarabine against human malignant mesothelioma MSTO-211H cells. Food Chem Toxicol. 2013;52:61–8.
Higdon JV, Frei B. Tea catechins and polyphenols: health effects, metabolism, and antioxidant functions. Crit Rev Food Sci Nutr. 2003;43:89.
Periasamy VS, Alshatwi AA. Tea polyphenols modulate antioxidant redox system on cisplatin-induced reactive oxygen species generation in a human breast cancer cell. Basic Clin Pharmacol Toxicol. 2013;112:374–84.
Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics. CA Cancer J Clin. 2005;55:74–108.
World d Health Organization (WHO)/InstitutCatalàd’Oncologia (ICO). Summary report. 3rd ed. London: WHO/ICO Information Centre; 2010.
Blagosklonny MV, El-Deiry WS. In vitro evaluation of a p53-expressing adenovirus as an anti-cancer drug. Int J Cancer. 1996;67:386–92.
Mohanpuria P, Rana NK, Yadav SK. Biosynthesis of nanoparticles: technological concepts and future applications. J Nanopart Res. 2008;10:507–17.
Asmathunisha N, Kathiresan K. A review on biosynthesis of nanoparticles by marine organisms. Colloids Surf B. 2013;103:283–7.
Kim EY, Ham SK, Shigenaga MK, Han O. Bioactive dietary polyphenolic compounds reduce nonheme iron transport across human intestinal cell monolayers. J Nutr. 2008;138:1647–51.
Nadagouda MN, Varma RS. Green synthesis of silver and palladium nanoparticles at room temperature using coffee and tea extract. Green Chem. 2008;10:859–62.
Moulton MC, Braydich-Stolle LK, Nadagouda MN, Kunzelman S, Hussain SM, Varma RS. Synthesis, characterization and biocompatibility of “green” synthesized silver nanoparticles using tea polyphenols. Nanoscale. 2010;2:763–70.
Venu R, Ramulu TS, Anandakumar S, Rani VS, Kim CG. Bio-directed synthesis of platinum nanoparticles using aqueous honey solutions and their catalytic applications. Colloid Surf A. 2011;384:733–8.
Ray PC. Size and shape dependent second order nonlinear optical properties of nanomaterials and their application in biological and chemical sensing. Chem Rev. 2010;110:5332–65.
Jensen TR, Malinsky MD, Haynes CL, Van Duyne RP. Nanosphere lithography: tunable localized surface plasmon resonance spectra of silver nanoparticles. J Phys Chem B. 2000;104:10549–56.
Smitha SL, Nissamudeen KM, Philip D, Gopchandra KG. Studies on surface plasmon resonance and photoluminescence of silver nanoparticles. Spectrochim Acta A.Mol Biomol Spectrosc. 2008;71:186.
Kalimutho M, Minutolo A, Grelli S, Formosa A, Sancesario G, Valentini A, Federici G, Bernardini S. Satraplatin (JM-216) mediates G2/M cell cycle arrest and potentiates apoptosis via multiple death pathways in colorectal cancer cells thus overcoming platinum chemo-resistance. Cancer Chemother Pharmacol. 2011;67:1299–312.
Farabegoli F, Papi A, Bartolini G, Ostan R, Orlandi M. (-)-Epigallocatechin-3-gallate downregulates Pg-P and BCRP in a tamoxifen resistant MCF-7 cell line. Phytomedicine. 2010;17:356–62.
Ahmed K, Wei Z, Zhao Q, Nakajima N, Matsunaga T, Ogasawara M, Kondo T. Role of fatty acid chain length on the induction of apoptosis by newly synthesized catechin derivatives. Chem Biol Interact. 2010;185:182–8.
Alshatwi AA. Catechin hydrate suppresses MCF-7 proliferation through TP53/Caspase-mediated apoptosis. J Exp Clin Cancer Res. 2011;29:167–76.
Shingu T, Chumbalkar VC, Gwak HS, Fujiwara K, Kondo S, Farrell NP, Bogler O. The polynuclear platinum BBR3610 induces G2/M arrest and autophagy early and apoptosis late in glioma cells. Neuro-oncology. 2010;12:1269–77.
Passalaris TM, Benanti JA, Gewin L, Kiyono T, Galloway DA. The G2 checkpoint is maintained by redundant pathways. Mol Cell Biol. 1999;19:5872–81.
Sorenson CM, Barry MA, Eastman A. Analysis of events associated with cell cycle arrest at G2 phase and cell death induced by cisplatin. J Natl Cancer Inst. 1990;82:749–55.
Acknowledgments
We gratefully acknowledge the financial support of the Deanship of Scientific Research, King Saud University, Saudi Arabia (Project No.: RGP-VPP-276).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alshatwi, A.A., Athinarayanan, J. & Vaiyapuri Subbarayan, P. Green synthesis of platinum nanoparticles that induce cell death and G2/M-phase cell cycle arrest in human cervical cancer cells. J Mater Sci: Mater Med 26, 7 (2015). https://doi.org/10.1007/s10856-014-5330-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-014-5330-1