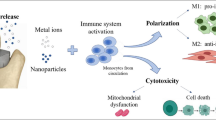
Abstract
It is generally accepted that periprosthetic bone resorption is initiated through aseptic inflammation aggravated by wear particles that are generated from artificial joint. However, some studies have demonstrated that “endotoxin-free” wear particles are almost completely unable to stimulate the macrophage-mediated production of proinflammatory cytokines. Here, we compare the titanium particles with different methods of endotoxin removal. The results indicated that different titanium particle preparation dosages did not significantly change particle size, morphology, and chemical composition. But it could cause variations in the endotoxin concentration of titanium particles and inflammatory responses in RAW264.7 macrophages. The particles with higher endotoxin levels correlated with more extensive inflammatory responses. When testing endotoxins using the supernatant of particle suspensions, it would lead to false negative results compared with testing the particle themselves. And when using the particles themselves, all the particles should be removed by centrifugation to avoid particle interference before the absorbance value was determined. Therefore, we suggest that research concerning wear particles should completely describe the endotoxin testing process, including endotoxin removal from particles and the details of endotoxin testing. Moreover, future research should focus on the surface of wear particles (the potential role of adherent endotoxin) rather than the particles themselves.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Total joint replacement has been a major success in surgery in terms of relieving pain and correcting deformities in patients with various joint diseases. However, aseptic loosening of prostheses remains a major problem for many patients. Because aseptic loosening is the result of implant-derived wear particles, it is commonly referred to as the ‘particle disease’ [1, 2]. However, research is conflicting concerning the detailed mechanisms involved in the generation of wear particles and the osteolytic response.
Although the exact mechanism underlying the pathogenesis of wear particles has yet to be elucidated, it is generally accepted that periprosthetic bone resorption is initiated by aseptic inflammation as a consequence of debris generated from the continuous wear, abrasion, or corrosion of implant components [3]. Fundamental to this process is the activation of the macrophages that produce pro-inflammatory cytokines, such as TNF-α, IL-1β, and IL-6, which recruit more cells (macrophages, osteoblasts, giant cells, and fibroblasts) that produce more cytokines and chemokines. However, in other studies, particles incubated with lipopolysaccharide (LPS, i.e., endotoxin) have been clearly demonstrated to elicit a strong inflammatory response from macrophages [4–7], while the “endotoxin-free” wear particles were almost completely unable to stimulate cytokine production by macrophages [4–6]. In addition, other studies have suggested a significant role for endotoxins in the induction of aseptic loosening [8, 9]. These data suggest that the endotoxins play an important role in the production of wear particles and the subsequent osteolysis around the arthroplasty.
Endotoxins are LPS derived from the cell membrane of Gram-negative bacteria. Bacteria can grow in nutrient poor environments, such as water, saline, and buffers, and thus, endotoxins are found almost everywhere. Moreover, endotoxins are highly heat stable and are not destroyed under regular sterilizing conditions which are usually used to clean joint implants and surgical instruments. However, endotoxins can be inactivated when exposed to temperatures of 250°C for more than 30 min or 180°C for more than 3 h. In addition, acids or alkaline solutions of at least 0.1 M can be used to destroy endotoxins in laboratories [10]. Previously, we reviewed the research concerning particle disease published since 2000. We found that many papers did not include detailed descriptions of sample preparation and endotoxin testing. In fact, some papers contain no specific methods for the removal of endotoxins from particles. Instead, these studies describe the use of 0.1 μm polycarbonate filter membranes [11–13], ethanol [14–17], autoclaving [14], UV light [14], gamma irradiation [18, 19] or sterilization without including detailed descriptions [20, 21]. However, these methods do not remove most of the endotoxins from particles. Similarly, there were few papers that detailed the endotoxin testing process. Many papers only state that after the samples preparation, the samples in the study are free of endotoxin under the endotoxin testing.
This paper focuses on methods that can be used for the removal of endotoxins from wear particles. It is important that to ensure that experimental results exclusively reflect the effects of wear particles rather than endotoxins. Thus, the aim of this paper is to determine effective methods for the removal of endotoxins from wear particles in research.
2 Materials and methods
2.1 Reagents
All mouse-specific ELISA kits were purchased from R&D Industries (Minneapolis, MN, USA). A commercial endotoxin detection kit (Chromogenic endpoint LAL with a Diazo coupling kit) was purchased from the Xiamen Houshiji Company, Fujian, China.
2.2 Titanium particle preparation
Commercial pure titanium (Ti) particles were purchased from Johnson Matthey (Catalog #00681; Ward Hill, MA, USA). It was demonstrated that such particles are similar to the wear particles retrieved from periprosthetic tissues. There were three groups in this assay: (1) In the high temperature group, the particles were sterilized by baking at 180°C for 6 h, followed by treatment with 70% ethanol for 48 h to remove the endotoxins [10]; (2) In the reference group [22], the first passivation was completed in 25% nitric acid at room temperature for 18–20 h. An additional incubation was conducted in a mixture of 0.1 N NaOH and 95% ethanol at 30°C for another 18–20 h. Subsequently, the particles were exposed to five cycles of alternating treatments with the two solutions. Between each treatment, the particles were washed five times with endotoxin-free water; and (3) 70% ethanol for 48 h. The Ti suspensions were sonicated for 30 min using a SB3200 Ultrasonic Generator (Shanghai Branson Ultrasonics Co. Ltd., Shanghai, China) prior to incubation with the cells. The concentration of the particles used for cell incubation was 0.1 mg/ml. It has been demonstrated that such particles are similar to the wear particles that have been retrieved from periprosthetic tissues [23, 24].
2.3 Particle morphology, chemical composition, and size determination
Because the size, morphology and chemical composition of the particles might affect the biological reaction with macrophages [25, 26] and other cells[27–29], we examined the size, morphology and chemical composition of the titanium particles after different endotoxin removal treatments. The surface morphology and chemical composition of the samples were investigated using a scanning electron microscope (SEM) equipped with energy-dispersive X-ray analysis (Instrumental Analysis Center of Shanghai Jiaotong University). The particle size distribution was determined by SICAS-4800 Photo-Sedimentometry (Shanghai Institute of Ceramics, Chinese Academy of Sciences). Prior to this analysis, ultrasonic wave dispersion was used for all samples.
2.4 Quantitative evaluation of endotoxin contamination in wear particles by limulus amebocyte lysate (LAL)-based assays
This assay was performed as recommended by the manufacturer LAL Assay Kit (detection limit = 0.01 endotoxin units/ml; Xiamen Houshiji, Fujian, China) with a standard curve of 0.01–1 endotoxin U of LPS/ml. A volume of 0.1 ml of known concentrations of particles (0.1 mg/ml) in endotoxin-free water, particle free supernatants or 0.01–1 unit/ml of endotoxin standards derived from Escherichia coli (Xiamen Houshiji, Fujian, China) was incubated with LAL reagent for 30 min at 37°C, and a volume of 0.1 ml endotoxin-free water as the control. After the initial incubation, the chromogenic substrate was added, and the incubation continued for an additional 6 min. The reaction was stopped by the addition of diazo reagents, and the particles should be removed by two rounds of centrifugation (600×g for 15 min) because the absorbance value can give incorrect readings with particle suspensions. Then the absorbance value was determined at 545 nm with a microplate reader. Because the assay is extremely sensitive to inhibition by test samples, all samples were measured with and without spikes containing a known amount of the endotoxin standard (0.05 endotoxin units/ml) as recommended by the manufacturer. The assays were considered reliable if the recovery of spikes was 50–200%. All samples (0.1 ml) were analyzed in duplicate. Only tests producing a correlation co-efficient for the standard curve of 0.95 or greater were accepted.
2.5 Cells and cell culture
The RAW264.7 murine monocytic/macrophagic cell line (ATCC, USA) was used in this experiments as an in vitro model of the macrophage inflammatory cytokine response to wear particles. This cell line has been used by previous investigators performing similar assays [30–32] and has the advantages of being a robust, stable, established cell line with predictable uniform cytokine responses. The RAW264.7 cells were grown, maintained, and assayed in DMEM with 10% heat-inactivated fetal bovine serum. The cells were seeded in a 24-well tissue culture plate (Costar, Corning, Lowell, MA) at a density of 2.5 × 105 cells/ml (1 ml/well).
2.6 Cell cytotoxicity: MTT assay
The cytotoxicity of the RAW264.7 macrophages in response to Ti particles was examined using the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay. The RAW264.7 macrophages (5 × 103 cells/well) were cultured in 96-well tissue culture plates for 24 h and incubated with 0.5 mg/ml of MTT at 37°C for 4 h. Following the removal of the supernatant, the insoluble formazan crystals were dissolved in 200 μl dimethyl sulfoxide, and the absorbance was measured using a 570 nm wavelength Synergy HT microtiter plate reader (BioTek Instruments, Inc., Vermont, USA).
2.7 Measurement of proinflammatory cytokines by ELISA
The RAW264.7 cells, with different treatments, were cultured in DMEM with 10% heat-inactivated fetal bovine serum for 24 h. The cell culture supernatants were collected. Mouse-specific ELISA kits were used to analyze the amounts of TNF-α, IL-1β, and IL-6 produced by the cells in accordance with the manufacturer’s instructions. The intensity of the color detected at 450 nm was measured.
2.8 NF-κB luciferase reporter gene assay
There were many studies that indicate that wear particles can activate NF-κB nuclear translocation. These results have minimized the influence of endotoxins on the particles because all particle preparations were shown to be free of endotoxin by LAL-based assay [33–35].However, other research has also demonstrated that the titanium-alloy particles without endotoxins did not induce NF-κB activation [36]. To examine NF-κB activation, RAW264.7 cells that were stably transfected with a luciferase reporter gene p-NF-κB-TA-Luc [37] were plated in 24-well plates at a density of 1 × 105 cells/well and treated with three groups of particles for 8 h. The cells were harvested, and the luciferase activity was measured using the Promega Luciferase Assay System according the manufacturer’s instructions (Promega).
2.9 Statistical analysis
The data are expressed as the means ± SD of triplicate determinations. The differences between the groups were analyzed using analysis of variance (ANOVA). Statistical significance was defined as P < 0.05. The statistical analyses were performed using SPSS, version 11.0 (SPSS, Chicago, IL, USA).
3 Results
3.1 Different titanium particle preparation dosages did not significantly change particle size, morphology, and chemical composition
Using SEM, we observed that the particle preparation dosages did not significantly change the surface morphology of the particles. The particles appeared round, oval, and irregular in all samples (Fig. 1a). We observed that the particles in group 1 (mean diameter = 5 μm) were slightly larger than the others (group 2: 4 μm; group 3: 4.7 μm). The particle size distribution was also similar in all samples (Fig. 1d). From the EDX, we observed that all of the surfaces of the samples had similar chemical compositions after different particle preparations (Fig. 1b). In Fig. 1c, we randomly selected three points in one sample and selected three samples from each group because the different positions in the sample might have different chemical compositions. There were a total of six chemical elements (O, Al, Si, K, Ca, and Ti) present on the surface of the samples, and there were no differences among all six chemical elements (P > 0.05).
Particle morphology, chemical composition, and size determination. Using SEM, we observe that the particles are round, oval, and irregular in all groups (Fig. 1a). The particle size distribution is also similar in all samples (Fig. 1d). From the EDX, we observe that all of the sample surfaces have similar chemical compositions after different particle preparation methods (Fig. 1b). In Fig. 1c, we have randomly selected three points in one sample and selected three samples from one group to evaluate different positions. The sample may have a different chemical composition. There are a total of six chemical elements in all samples, and there are no differences among all six chemical elements (P > 0.05)
3.2 Testing the supernatant produced a negative result in endotoxin detection
In endotoxin testing (Fig. 2), we observed that different preparations of titanium particles yielded different results. Group 2 had a more positive effect on endotoxin removal compared with group 1 (P < 0.05) and group 3 (P < 0.01); however, we observed that the endotoxin still adhered to the particles. When testing the supernatant, we obtained the expected negative result (the supernatants of all groups are endotoxin-free) compared with the control (P > 0.05).
Quantitative evaluation of endotoxin contamination in wear particles by LAL-based assays. Group 2 has a more positive effect on endotoxin removal compared with group 1 (P < 0.05) and group 3 (P < 0.01); however, we also find that adherent endotoxins remain on particles of this group compared with the control (P < 0.01). When testing the supernatant, we obtain negative results (P > 0.05) compared with the control. *Significantly different (P < 0.05), **Significantly different (P < 0.01). Data represent the means ± SD of three independent experiments with duplicate measurements in each experiment
3.3 Different titanium particle preparation dosages did not change cell cytotoxicity
From the MTT results (Fig. 3a), we observed that the phagocytosed particles really have the cytotoxic effect on the RAW264.7 compared with the control (P < 0.05). However, there were no observed differences between groups 1, 2 and 3 regarding cell cytotoxicity (P > 0.05).
Measurement of cell viability, proinflammatory cytokines and luciferase activity in NF-κB nuclear translocation. a The MTT assay results demonstrate that RAW264.7 cells have decreased proliferation after macrophages phagocytose the particles compared with the control (P < 0.05). However, group 1, group 2 and group 3 have no differences in cell proliferation (P > 0.05). b–d In group 3, the particles with adherent endotoxin can significantly stimulate IL-1β, TNF-α and IL-6 secretion by RAW264.7 cells compared with other groups in 48 h (P < 0.01). We observe that the particles in group 2 are almost unable to stimulate cytokine production by macrophages compared with the control (P > 0.05). However, in group 1, the TNF-α and IL-6 secretion are different compared with the control (P < 0.05). Although the particle in group 1 can induce increased proinflammatory cytokine production, there is no difference between group 1 and group 2 (P > 0.05). e Group 3 exhibits more active NF-κB nuclear translocation compared with other groups (P < 0.01). In addition, there are differences (P < 0.05) between group 1 and group 2. *Significantly different (P < 0.05), **Significantly different (P < 0.01). Data represent the means ± SD of three independent experiments with duplicate measurements in each experiment
3.4 Adherent endotoxins on particles induce a proinflammatory reaction and NF-κB activation in RAW264.7 cells
Using ELISA (Fig. 3b–d), we observed that the particles from group 2 were almost unable to stimulate proinflammatory cytokine (TNF-α, IL-1β, and IL-6) production by the RAW264.7 cells. The particles with a higher endotoxin concentration induced more proinflammatory cytokine production in groups 1 (TNF-α, IL-6; P < 0.05) and 3 (TNF-α, IL-1β, and IL-6; P < 0.01) compared with the control. We also examined the effect of adherent endotoxins on NF-κB nuclear translocation (Fig. 3e), and we observed that increased adherent endotoxins on the particles increased active NF-κB nuclear translocation.
4 Discussion
In 1998, Ragab and colleagues demonstrated that Ti particles without endotoxins were almost completely unable to stimulate cytokine production by murine marrow cells [22]. Since then, all research concerning particle disease should focus on endotoxin detection testing on particles. Because there are several ways to remove adherent endotoxin from particles, including the most commonly used method of high temperature or the circulatory use of nitric acid and NaOH, our results demonstrated that the circulatory use of nitric acid and NaOH was most effective for removing endotoxin from particles. The high temperature method still resulted in a relatively high endotoxin concentration. It is likely that when the particle solution is incubated at high temperatures, the particles deposit on the glass tube wall upon water evaporation. We found that the particles were bunched so tightly that it was difficult to separate them, and oxide film composed of TiO2 was formed on the surface of agglomerative particles, which was so protective that the further oxidation of titanium was prevented in various circumstances [38]. So oxide film on the surface might protect the inner endotoxins from removal. Therefore, the methods employed in group 2 might be the best way to remove the endotoxin from particles although it is relatively time consuming. However, different particles respond differently to methods of endotoxin removal. Many studies have reported that cobalt chrome, commercially pure titanium, titanium alloy, and ultra-high molecular weight polyethylene are the most potent types of particles that cause osteolysis [1, 2]. In addition, adherent endotoxins are responsible for many of the biological responses induced by commercially pure titanium, titanium alloy, titanium nitride, polymethylmethacrylate, cobalt chrome, and high-density polyethylene [8]. Therefore, it is important to use different methods to remove adherent endotoxins according to the type of particles. For example, high temperatures could not be used to remove endotoxins from ultra-high molecular weight polyethylene because high temperatures affect the chemical character of ultra-high molecular weight polyethylene.
Moreover, the size or shape of commercially pure titanium particles might affect the biology of macrophages [25, 26] and other cells [27–29]. In this assay, we also used SEM and photo-sedimentometry to determine the size and shape of the particles after the sample preparation. We did not observe any significant changes in the size or shape of the particles. In addition to the common use of metal-to-metal arthroplasty, research [20, 39] has revealed that the surface change of the chemical composition on the particle could produce different biological effects on cells. Therefore, we also compared the surface chemical composition between the different endotoxin removal treatments. Similarly, we did not observe any significant changes in the chemical composition on the particles’ surfaces upon different endotoxin removal treatments. We suggest that changes in proinflammatory cytokine production and NF-κB activation result from different concentrations of endotoxins on the particles.
Most of the papers reviewed in the introduction did not describe the detailed testing process, and only two papers described their method of endotoxin testing using the particle supernatant [13, 40]. However, from our assays, we demonstrated that when we use the particle supernatant without removing the endotoxin for endotoxin testing, we also obtain negative results (the supernatants of all groups are endotoxin-free). However, when we use the particles with adherent endotoxins, we obtain positive results. Ragab also demonstrated particle suspension not the supernatant should be used in the endotoxin testing in their study [22]. Another important point Ragab also mentioned was when the reaction was stopped by the addition of diazo reagents; the particles should be removed by two rounds of centrifugation to avoid particle interference with the LAL-based chromagenic assay which can give incorrect readings with particle suspensions. So here we again remind that it is important for all particle research studies to describe the detailed process used for endotoxin testing. We should ensure that the particles supernatant as well as the particle surface are endotoxin-free because metal particles have a high affinity for endotoxins.
Because both particles [41, 42] and endotoxins [43] can cause cytotoxicity in macrophages, we used the MTT assay to analyse cytotoxicity. In our study, we demonstrated that titanium particles really have the cytotoxic effect on the RAW264.7 compared with the control. However, there is no difference among all the particles that were treated with different endotoxin removal treatments. We observed the presence of endotoxins on particles that did not inhibit RAW264.7 macrophage proliferation in the particles that were sterilized by ethanol.
Our present research demonstrated that the method for endotoxin removal from particles could significantly affect proinflammatory cytokine production. We also found that particles after endotoxin removal (in group 1 and group 2) could induce NF-κB activation in RAW264.7 cells because endotoxins were still adhered to the particles. The particles with circulatory use of nitric acid and NaOH could not induce proinflammatory cytokine production. However, the particles treated with high temperature could slightly induce proinflammatory cytokine production because more endotoxin was present on the particles compared with the particles treated with the circulatory use of nitric acid and NaOH. As for the ethanol-treated particles, the activation of NF-κB nuclear translocation and the production of proinflammatory cytokines are significantly greater than in the other groups when more endotoxins present on the particles. This observation is the reason that many studies have indicated that the wear particles could activate NF-κB nuclear translocation even when all particle preparations were shown to be free of endotoxin by LAL-based assay in their studies [33–35]. However, another paper also demonstrated that titanium-alloy particles without endotoxin did not induce NF-κB activation [36]. Although this paper reported that NF-κB translocation activity, as determined by immunohistochemistry, was similar to other tests, methods, such as the electron mobility sift assay, western blotting and luciferase reporter gene assays, may be more sensitive than immunohistochemical analysis for the detection of NF-κB nuclear translocation. Therefore, it is important to consider the surface (the potential role of adherent endotoxin) of the particles when examining the influence of wear particles.
In this paper, we only use the RAW264.7 murine monocytic/macrophagic cell line for these experiments as an in vitro model of the macrophage inflammatory cytokine response to wear particles. Although this cell line has the advantages of being a robust, stable, established cell line with predictable uniform cytokine responses, it is not a primary cell, which has limitations in the mimic of pathophysiology in vivo. Further experiments in primary cells or animal models are needed in future investigations. And here we only use commercial pure titanium (Ti) particles for the experiments, which may have different characteristics compared to the wear particles from patients with aseptic loosening. However, endotoxins could also accumulate on endotoxin-free commercial pure titanium particles and/or in the surrounding tissue after implantation in the calvaria of mice [8]. Therefore, we propose that commercial pure Ti particles are suitable for wear particle research. However, we only used one kind of wear particle in this study. It is possible that this result may not be applicable to other types of wear particles because different particles have different affinities to endotoxins.
5 Conclusions
The current results document that different methods for endotoxin removal cause differences in endotoxin concentrations on titanium particles and inflammatory responses in RAW264.7 macrophages. Therefore, we should use the particles themselves not the supernatant of the particles in endotoxin testing, which will affect the results in wear particle research. We suggest that research on wear particles should describe the detailed methods for endotoxin testing, including endotoxin removal from particles and the endotoxin testing process, which will affect the readers’ judgement about whether the wear particles or the surfaces of the wear particles cause the proinflammatory response of macrophages. Based upon these findings, we believe that more attention should be paid to the surface (the potential role of adherent endotoxin) of wear particles than to the particles themselves. Future studies should also research other types of particles that may require different methods for endotoxin removal.
References
Gallo J, Kaminek P, Ticha V, Rihakova P, Ditmar R. Particle disease. A comprehensive theory of periprosthetic osteolysis: a review. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2002;146(2):21–8.
Kolundzic R, Orlic D. Particle disease–aseptic loosening of the total hip endoprosthesis. Lijec Vjesn. 2008;130(1–2):16–20.
Purdue PE, Koulouvaris P, Nestor BJ, Sculco TP. The central role of wear debris in periprosthetic osteolysis. HSS J. 2006;2(2):102–13.
Bi Y, Seabold JM, Kaar SG, Ragab AA, Goldberg VM, Anderson JM, et al. Adherent endotoxin on orthopedic wear particles stimulates cytokine production and osteoclast differentiation. J Bone Miner Res. 2001;16(11):2082–91.
Cho DR, Shanbhag AS, Hong C-Y, Baran GR, Goldring SR. The role of adsorbed endotoxin in particle-induced stimulation of cytokine release. J Orthop Res. 2002;20(4):704–13.
Brooks RA, Wimhurst JA, Rushton N. Endotoxin contamination of particles produces misleading inflammatory cytokine responses from macrophages in vitro. J Bone Joint Surg Br. 2002;84(2):295–9.
Smith RA, Hallab NJ. In vitro macrophage response to polyethylene and polycarbonate-urethane particles. J Biomed Mater Res A. 2010;93(1):347–55.
Greenfield EM, Bi Y, Ragab AA, Goldberg VM, Nalepka JL, Seabold JM. Does endotoxin contribute to aseptic loosening of orthopedic implants? J Biomed Mater Res B Appl Biomater. 2005;72(1):179–85.
Nalepka JL, Lee MJ, Kraay MJ, Marcus RE, Goldberg VM, Chen X, et al. Lipopolysaccharide found in aseptic loosening of patients with inflammatory arthritis. Clin Orthop Relat Res. 2006;451:229–35.
Magalhaes PO, Lopes AM, Mazzola PG, Rangel-Yagui C, Penna TCV, Pessoa A Jr. Methods of endotoxin removal from biological preparations: a review. J Pharm Pharm Sci. 2007;10(3):388–404.
Ren W, Yang S-Y, Fang H-W, Hsu S, Wooley PH. Distinct gene expression of receptor activator of nuclear factor-kappaB and rank ligand in the inflammatory response to variant morphologies of UHMWPE particles. Biomaterials. 2003;24(26):4819–26.
Fisher J, McEwen HMJ, Tipper JL, Galvin AL, Ingram J, Kamali A, et al. Wear, debris, and biologic activity of cross-linked polyethylene in the knee: benefits and potential concerns. Clin Orthop Relat Res. 2004;428:114–9.
Ingram J, Matthews JB, Tipper J, Stone M, Fisher J, Ingham E. Comparison of the biological activity of grade GUR 1120 and GUR 415HP UHMWPE wear debris. Biomed Mater Eng. 2002;12(2):177–88.
St Pierre CA, Chan M, Iwakura Y, Ayers DC, Kurt-Jones EA, Finberg RW. Periprosthetic osteolysis: characterizing the innate immune response to titanium wear-particles. J Orthop Res. 2010;28(11):1418–24.
Trindade MC, Lind M, Sun D, Schurman DJ, Goodman SB, Smith RL. In vitro reaction to orthopaedic biomaterials by macrophages and lymphocytes isolated from patients undergoing revision surgery. Biomaterials. 2001;22(3):253–9.
Kanaji A, Caicedo MS, Virdi AS, Sumner DR, Hallab NJ, Sena K. Co–Cr–Mo alloy particles induce tumor necrosis factor alpha production in MLO-Y4 osteocytes: a role for osteocytes in particle-induced inflammation. Bone. 2009;45(3):528–33.
Yang S-Y, Yu H, Gong W, Wu B, Mayton L, Costello R, et al. Murine model of prosthesis failure for the long-term study of aseptic loosening. J Orthop Res. 2007;25(5):603–11.
Zysk SP, Gebhard HH, Kalteis T, Schmitt-Sody M, Jansson V, Messmer K, et al. Particles of all sizes provoke inflammatory responses in vivo. Clin Orthop Relat Res. 2005;433:258–64.
Utzschneider S, Becker F, Grupp TM, Sievers B, Paulus A, Gottschalk O, et al. Inflammatory response against different carbon fiber-reinforced PEEK wear particles compared with UHMWPE in vivo. Acta Biomater. 2010;6(11):4296–304.
Kovacik MW, Mostardi RA, Neal DR, Bear TF, Askew MJ, Bender ET, et al. Differences in the surface composition of seemingly similar F75 cobalt-chromium micron-sized particulates can affect synovial fibroblast viability. Colloids Surf B Biointerfaces. 2008;65(2):269–75.
Germain MA, Hatton A, Williams S, Matthews JB, Stone MH, Fisher J, et al. Comparison of the cytotoxicity of clinically relevant cobalt-chromium and alumina ceramic wear particles in vitro. Biomaterials. 2003;24(3):469–79.
Ragab AA, Van De Motter R, Lavish SA, Goldberg VM, Ninomiya JT, Carlin CR, et al. Measurement and removal of adherent endotoxin from titanium particles and implant surfaces. J Orthop Res. 1999;17(6):803–9.
von Knoch M, Jewison DE, Sibonga JD, Sprecher C, Morrey BF, Loer F, et al. The effectiveness of polyethylene versus titanium particles in inducing osteolysis in vivo. J Orthop Res. 2004;22(2):237–43.
Lee S-S, Woo C-H, Chang J-D, Kim J-H. Roles of Rac and cytosolic phospholipase A2 in the intracellular signalling in response to titanium particles. Cell Signal. 2003;15(3):339–45.
Gonzalez O, Smith RL, Goodman SB. Effect of size, concentration, surface area, and volume of polymethylmethacrylate particles on human macrophages in vitro. J Biomed Mater Res. 1996;30(4):463–73.
Sterner T, Schutze N, Saxler G, Jakob F, Rader CP. Effects of clinically relevant alumina ceramic, zirconia ceramic and titanium particles of different sizes and concentrations on TNF-alpha release in a human macrophage cell line. Biomed Tech (Berl). 2004;49(12):340–4.
Matthews JB, Besong AA, Green TR, Stone MH, Wroblewski BM, Fisher J, et al. Evaluation of the response of primary human peripheral blood mononuclear phagocytes to challenge with in vitro generated clinically relevant UHMWPE particles of known size and dose. J Biomed Mater Res. 2000;52(2):296–307.
Choi MG, Koh HS, Kluess D, O’Connor D, Mathur A, Truskey GA, et al. Effects of titanium particle size on osteoblast functions in vitro and in vivo. Proc Natl Acad Sci USA. 2005;102(12):4578–83.
Sommer B, Felix R, Sprecher C, Leunig M, Ganz R, Hofstetter W. Wear particles and surface topographies are modulators of osteoclastogenesis in vitro. J Biomed Mater Res A. 2005;72(1):67–76.
Illgen RL, Forsythe TM, Pike JW, Laurent MP, Blanchard CR. Highly crosslinked vs conventional polyethylene particles—an in vitro comparison of biologic activities. J Arthroplasty. 2008;23(5):721–31.
Kranz I, Gonzalez JB, Dorfel I, Gemeinert M, Griepentrog M, Klaffke D, et al. Biological response to micron- and nanometer-sized particles known as potential wear products from artificial hip joints: part II: Reaction of murine macrophages to corundum particles of different size distributions. J Biomed Mater Res A. 2009;89(2):390–401.
Geng DC, Xu YZ, Yang HL, Zhu XS, Zhu GM, Wang XB. Inhibition of titanium particle-induced inflammatory osteolysis through inactivation of cannabinoid receptor 2 by AM630. J Biomed Mater Res A. 2010;95(1):321–6.
Nakashima Y, Sun DH, Trindade MC, Maloney WJ, Goodman SB, Schurman DJ, et al. Signaling pathways for tumor necrosis factor-alpha and interleukin-6 expression in human macrophages exposed to titanium-alloy particulate debris in vitro. J Bone Joint Surg Am. 1999;81(5):603–15.
Fritz EA, Jacobs JJ, Glant TT, Roebuck KA. Chemokine IL-8 induction by particulate wear debris in osteoblasts is mediated by NF-kappaB. J Orthop Res. 2005;23(6):1249–57.
Wei X, Zhang X, Flick LM, Drissi H, Schwarz EM, O’Keefe RJ. Titanium particles stimulate COX-2 expression in synovial fibroblasts through an oxidative stress-induced, calpain-dependent, NF-kappaB pathway. Am J Physiol Cell Physiol. 2009;297(2):C310–20.
Akisue T, Bauer TW, Farver CF, Mochida Y. The effect of particle wear debris on NFkappaB activation and pro-inflammatory cytokine release in differentiated THP-1 cells. J Biomed Mater Res. 2002;59(3):507–15.
Wang C, Steer JH, Joyce DA, Yip KHM, Zheng MH, Xu J. 12-O-tetradecanoylphorbol-13-acetate (TPA) inhibits osteoclastogenesis by suppressing RANKL-induced NF-kappaB activation. J Bone Miner Res. 2003;18(12):2159–68.
Hiromoto S, Hanawa T, Asami K. Composition of surface oxide film of titanium with culturing murine fibroblasts L929. Biomaterials. 2004;25(6):979–86.
Mostardi RA, Kovacik MW, Ramsier RD, Bender ET, Finefrock JM, Bear TF, et al. A comparison of the effects of prosthetic and commercially pure metals on retrieved human fibroblasts: the role of surface elemental composition. Acta Biomater. 2010;6(2):702–7.
Ingram JH, Stone M, Fisher J, Ingham E. The influence of molecular weight, crosslinking and counterface roughness on TNF-alpha production by macrophages in response to ultra high molecular weight polyethylene particles. Biomaterials. 2004;25(17):3511–22.
Hallab NJ, Anderson S, Caicedo M, Brasher A, Mikecz K, Jacobs JJ. Effects of soluble metals on human peri-implant cells. J Biomed Mater Res A. 2005;74(1):124–40.
Yamamoto A, Honma R, Sumita M, Hanawa T. Cytotoxicity evaluation of ceramic particles of different sizes and shapes. J Biomed Mater Res A. 2004;68(2):244–56.
Yamamoto Y, He P, Klein TW, Friedman H. Endotoxin induced cytotoxicity of macrophages is due to apoptosis caused by nitric oxide production. Innate Immun. 1994;1(3):181–7.
Acknowledgments
This work was supported by the National High Technology Research and Development Program of China (863 Program) (Grant No. 2006AA02A137), Program for the Shanghai Key Laboratory of Orthopaedic Implant (Grant No. 08DZ2230300) and the National Natural Science Foundation of China (Grant No. 81001529). We also thank Prof. Jiake Xu from the University of Western Australia for his donation of the RAW264.7 cells that were stably transfected with a luciferase reporter gene.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ding, H., Zhu, Z., Tang, T. et al. Comparison of the cytotoxic and inflammatory responses of titanium particles with different methods for endotoxin removal in RAW264.7 macrophages. J Mater Sci: Mater Med 23, 1055–1062 (2012). https://doi.org/10.1007/s10856-012-4574-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10856-012-4574-x