Abstract
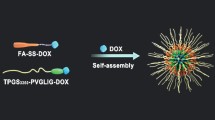
Stimuli-responsive nanomedicine shows high therapeutic effects and low side effects to tumor cells and tissues, representing a preferable therapeutics for cancer therapy. Herein, we design an acid-stimuli-responsive doxorubicin polymeric prodrug (OM@DOX), and this amphiphilic prodrug has a unique chemical structure with prominent advantages, including high drug loading rate (as high as 61.5 wt%), pH-triggered drug release and targeted access to cells. This smart polymeric prodrug has a preferable size of ~40 nm and strong micellar stability in aqueous solution, which is benefited to the long blood circulation and efficient extravasation from tumor vessel. Moreover, the prodrug micelles showed a higher cytotoxicity against tumor cells (HeLa cells) than normal cells (L929 cells), likely suggesting the potential tumor-specific targeting ability. To render this prodrug micelles with targeting function, folic acid (FA) molecules conjugated prodrug (FA-OM@DOX) further showed selectively higher cytotoxicity to KB tumor cells (FA-receptor-positive) than A549 tumor cells (FA-receptor-negative). Considering the rapidly cell-penetrating ability and aforementioned features, we believe that the present prodrug strategy has the potential as a promising nanomedicine and providing inspired insights to design multifunctional drug delivery nanoplatforms.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Cancer has been being a prevailing threat to human health owing to high mortality and severe incidence [1]. The therapeutic strategy of tumor mainly includes chemotherapy, immunotherapy, surgical resection and radiation therapy [2, 3]. Compared with other therapeutics, chemotherapy is a preferential strategy due to the less body injuries and remarkable clinical curative effect [4, 5]. However, conventional anticancer drugs are always limited by their instability, poor solubility in water and severely toxic side effects to normal cells/tissues including emesis, fever, anaphylaxis, baldness and other clinical manifestation [6]. Nanosized drug carriers (NSDCs) (with 10–100 nm size) have attracted more attention due to those NSDCs can effectively overcome those chemotherapeutic obstacles by regulating the entering way and distribution of drugs in body [7,8,9,10]. However, the severe side effects to normal cells and tissues remain a serious issue, which is mainly attributed to the undesired and nonspecific release of drugs.
Especially, polymeric NSDCs with popular amphiphilic structure, high drug loading and controlled drug release behavior have obtained comprehensive interest and a series of polymeric nanostructures based on liposomes [11, 12], polymersomes [13], polymeric micelles [14,15,16,17,18,19,20,21,22,23,24] and nanogels [25, 26] have been reported. Notably, stimuli-responsive NSDCs in responded to the intrinsic microenvironment, such as low pH [27,28,29,30], high glutathione (GSH) concentration [31,32,33] and other stimulus [34], may offer an effective method by improving the drug efficacy while reducing the nonspecific toxicity. For this purpose, our group have previously reported a novel pH-responsive doxorubicin (DOX) prodrug which can effectively improve the drug loading content of polymeric prodrug and restrained the early release of drugs [28]. Recently, Hu and co-workers designed one self-reporting theranostic platform with reduction-sensitive drug release and intensive antitumor-capacity against tumor cells [31]. Duan and his co-workers recently reported a dual responsive drug delivery system which could effectively inhibit the propagation of tumor through controlling the drug release behaviors [35]. To render these theranostic platform with target function, targeting moieties, such as sugars, folate acid and peptides, could further realize targeted cancer therapy [36,37,38,39]. Especially, folic acid (FA) showed the specific binding interaction between FA molecules, and FA-receptor on the surface of cells has widely studied for targeted drug delivery since it firstly was extracted from yeast [40,41,42,43,44]. Guo and his co-workers designed a polymeric prodrug by attaching FA to the polymer of DOX-conjugated poly(ethylene glycol)-poly(ε-caprolactone), which presented favorable site-specific anticancer therapy [45]. These aforementioned therapeutic nanoplatforms could minimize the primitive drug-leakage at normal cells and selectively released drugs at tumor site, resulting a high promising strategy for cancer therapy.
To explore more resultful NSDCs, we presented herein the synthesis of acid-activatable amphiphilic polymeric prodrug via reversible addition–fragmentation chain transfer polymerization (RAFT). Compared with other previously reported method about polymeric micelles derived from amphiphilic block copolymer, the present design possesses some unique advantages as drug delivery systems: (1) the obtained prodrug have a ultra-high drug loading amount as high as 61.5 wt%; (2) the prodrug micelles show robust stability in physiological environment and pH-triggered drug release pattern; (3) the obtained prodrug show a selectively high toxicity against tumor cells than normal cells, indicating an instinctive tumor-specific targeting ability. Specifically, the resulting prodrug had a hydrophilic block of poly[(ethylene glycol) methyl ether methacrylate] (POEGMA) with/without FA decoration and hydrophobic block of DOX drug and was denoted as OM@DOX and FA-OM@DOX (Scheme 1), respectively. Obviously, the hydrophilic POEGMA block presented a potential to enable these prodrugs to form micelles in aqueous solution. The subsequent results also demonstrated the micelles possessing a high micellar stability and pH-triggered drug release due to the acid milieu-responsive hydrazine bond existed in the prodrugs. The collective cytotoxicity results revealed the OM@DOX prodrug showed a higher toxicity for the tumor cell of HeLa than the normal cell of L929. Excitingly, FA-OM@DOX further presented preferentially cytotoxicity for KB cells than A549 cells, and which might be due to the rich FA-receptor on membrane of the former. The subsequent in vitro cellular internalization and cellular uptake demonstrated the micelles could selectively realize the drug accumulation in tumor cells, resulting a promising nanoplatform for cancer therapy.
Experimental section
Regents and materials
All biological reagents including Dulbecco’s Modified Eagle’s Medium (DMEM), TrypLE™ Express Enzyme, Penicillin–Streptomycin Solution, Triton X-100,Alexa Fluors®633 Phalloidin,DAPI and Lyso Tracker®Red were acquired from the Life Technologies of China. The chemicals embracing folate (FA), 1-(3-Dimethylaminopropyl)-3-ethylcarbodiimide hydrochloride (EDC·HCl), N–BOC-1,6-hexanediamine hydrochloride (NH2–BOC·HCl), methyl glycolate, N-Hydroxysuccinimide, methacryloyl chloride, trifluoroacetic acid (TFA), trimethylamine (TEA) and anhydrous solvent including dimethyl sulfoxide (DMSO), 1,4-dioxane, N, N-dimethylformamide (DMF) were acquired from Sigma-Aldrich (USA) except for doxorubicin hydrochloride (DOX·HCl), which was attained from Beijing HuaFeng United Technology CO. Ltd (China). The deionized (DI) water obtained from a water purification system of Millipore. The other solvents with analytical grade were used directly without any further treatment.
Instruments
A Bruker AV 600 NMR spectrometer (Rheinstetten, Germany) was used to record the 1H NMR spectra of the polymers; Gel permeation chromatography (GPC, Agilent 1260, USA) was employed to notarize the molecular weights (M w) and Polydispersity (PDI); Dynamic light scattering (DLS, Nano-ZS90, Malvern, UK) was used to determine the size distribution and stability of micelles. Transmission electron microscopy (TEM, JEM-2100, Japan) were employed to measure the size and morphology of micelles. A Tensor 27 Fourier transform infrared spectroscopy (FT-IR) was used to study the molecular structure and chemical bonds; A Cary Eclipse fluorescence spectrophotometer (RF-5301PC, Shimadzu, Japan) was used to measure fluorescence emission spectra and fluorescence excitation spectra, the latter could be used to analyze the critical micelle concentration; A Lambda 35spectrometer (UV-2550, Shimadzu, Japan) was used to record UV–vis absorbance spectra; A synergy H1 Microplate reader (Tecan SPARK-10M) was used to measure the accumulation of drug release and cell viability; a confocal laser scanning microscope (CLSM, Zeiss LSM 880, Germany) was used to record cellular imaging; A flow cytometry from ACEA biosciences (FAC, NovoCyte 2060R) was used to detect the cellular uptake at a certain concentration and different time points.
Synthesis of FA–NH2
Typically, folic acid (FA, 1.0 g, 2.3 mmol) was dispersed in a solvent of 40 mL anhydrous DMF under the protection of argon gas, and then a mixture of 1-(3-Dimethylaminopropyl)-3-ethylcarbodiimide hydrochloride (EDC·HCl, 440 mg, 2.4 mmol) and N-hydroxysuccinimide (NHS, 260 mg, 2.3 mmol) was added, and the mixture was stirred for 0.5 h under an ice bath. After that, a mixture of NH2–BOC.HCl (615 mg, 2.5 mmol) and TEA (2.4 mmol, 336 uL) in 5.0 mL DMF was added, and the reaction was further stirred for 12 h at room temperature. Finally, 200 mL deionized water was added slowly to precipitate the resultant, yielding a dark yellow solid (denoted as FA–NH2–BOC) (282 mg, 19.2% yields).
In order to remove the protection of t-butyloxycarbonyl, FA–NH2–BOC (282 mg, 0.4 mmol) was dispersed in a mixture solvent of 6 mL of DMF and 6 mL of TFA and stirred for 0.5 h. After evaporation of the solvent, methanol was added and further co-evaporated three times for removing residual solvent. The mixture was precipitated into the excess ether; after dried under vacuum oven, a dark yellow solid of FA–NH2 was obtained (48.8 mg, 17.3% yields).
Synthesis of POEGMA block polymer
The RAFT agent of CPPA-NHS (38 mg, 0.1 mmol), OEGMA (1.425 g, 2.8 mmol) and AIBN (3.2 mg, 0.02 mmol) were dissolved in 5 mL of anhydrous 1, 4-dioxane. Then, the formative mixture was stirred for 24 h at 70 °C after three degassed cycles. The reaction was terminated using liquid nitrogen and the obtained crude product were dialyzed against methanol to remove the unreacted OEGMA monomer. The liquid in dialysis tube was concentrated by a rotary evaporator and obtained the pure POEGMA block polymer, which would be as a RAFT agent for the subsequent reaction. The degree of polymerization (DP) of OEGMA was calculated as 30 based on the 1H NMR results (307.8 mg, 21.1% yield).
Synthesis of POEGMA-b-PMGMA diblock copolymer
Firstly, the ethyl glycinate methacrylamide (MGMA) monomer was synthesized according to the previous reference with some modification [45]. The POEGMA-b-PMGMA diblock copolymer were synthesized using POEGMA as the macroRAFT agent and MGMA as the monomer, concretely, POEGMA (170 mg, 0.01 mmol), MGMA (81 mg, 0.5 mmol) and AIBN (0.825 mg, 0.005 mmol) were dissolved in a mixture solvent of 1.5 mL DMSO and 1.5 mL dioxane; the formative mixture was degassed three times and stirred for 24 h at 70 °C. The reaction was terminated using liquid nitrogen, and the obtained crude product was dialyzed against methanol to remove the unreacted OEGMA monomer. The liquid in dialysis tube was concentrated by a rotary evaporator and obtained the pure P(OEGMA)30-b-P(MGMA)22 diblock copolymer. Similarly, the P(OEGMA)30-b-P(MGMA)60 copolymer was synthesized with the same method while the molar quantity of MGMA was 1.0 mmol.
Synthesis of FA-POEGMA-b-PMGMA diblock copolymer
Typically, a mixture of P(OEGMA)30-b-P(MGMA)60 (300 mg, 0.01 mmol) and FA–NH2 (6.7 mg, 0.01 mmol) was dissolved in 2 mL anhydrous DMSO, and then, 11.2 uL TEA was added into the above mixture and stirred 48 h at room temperature. At the end of reaction, excess diethyl ether was added and precipitated the resultant. After dried in vacuum, a viscous solid was obtained (101.3 mg, 33.0% yields).
Synthesis of amphiphilic polymeric prodrug
A two-step procedure was used to prepare the DOX polymeric prodrug. 100 mg of POEGMA-b-PMGMA or FA-POEGMA-b-PMGMA was dispersed in a mixture anhydrous solvent of 6 mL of methanol and 3 mL of DMF, and hydrazine hydrate was added and stirred for 12 h at 25 °C. After the reaction, the mixture was dialyzed (MWCO = 3500) against DI water (200 ml × 3) for 24 h. After a freeze–drying process, a pale solid was obtained and further used to graft DOX drug.
Next, 47 mg of POEGMA-b-hydrazide or FA-POEGMA-b-hydrazide and DOX·HCl (2.0 equivalents to the molar amount of the NH2 group in POEGMA-b-hydrazide or FA-POEGMA-b-hydrazide) was added in a mixture solvent of 3 mL DMF and 3 mL methanol. After adding one drop of TFA, the mixture was stirred for 48 h in the dark, and then, the mixture were dialyzed against methanol (200 ml × 3) for 48 h to remove the Free DOX drug. Finally, the dark red solid denoted as POEGMA-b-PDOX (OM@DOX) or FA-POEGMA-b-PDOX (FA-OM@DOX) was obtained after a freeze–drying procedure.
Measurement of the critical micelle concentration (CMC)
The value of CMC is a crucial parameter to verify the stability of micelles. Typically, 2.0 mg of pyrene was dissolved in 10 mL acetone, after volatilizing the acetone completely, 3 mL of OM@DOX-1 and OM@DOX-2 micelles with different concentrations were added, respectively. After stirring in the dark for 12 h, the fluorescence of the solution were detected with a fixed emission wavelength at 390 nm, further plotted the concentration of micelles and fluorescence intensity ratio I338/I333; the CMC value was obtained based on the point of the curve.
Preparation and micellar stability of prodrug micelles
Briefly, OM@DOX-1, OM@DOX-2 or FA-OM@DOX prodrug micelles were prepared using a dialysis method. A mixture of prodrug (5 mg) and TEA (10 uL) was dissolved in 1 mL of DMSO and stirred about 1 h. Then, the prodrug solution was added dropwise into 8 mL deionized water and stirred for 0.5 h, the micellar solution was dialyzed against deionized water (500 ml × 3) for 48 h and the concentration was adjusted to 500 µg/mL for further experiment.
Dynamic light scattering (DLS) instrument was employed to access the micellar stability of OM@DOX-1 and OM@DOX-2 micelles by recording the size distribution of micelles. Specifically, 500 µg/mL of OM@DOX-1 and OM@DOX-2 micelles were placed at refrigerator set at 4 °C, and the average diameter at pre-determined time ranged from 1 day to 5 days, respectively.
Drug release of DOX from prodrug micelles
To estimate the loading content of DOX of OM@DOX-1 and OM@DOX-2 micelles, 1.0 mg of prepared OM@DOX-1 and OM@DOX-2 prodrug was added into 3.0 mL of diluted hydrochloric acid (0.01M) and stirred for 48 h in the dark. The fluorescent intensity of the above solution was measured, and the grafting DOX amount was calculated based on the standard cure of DOX.
The in vitro release of DOX from OM@DOX-1 and OM@DOX-2 micelles was measured using a dialysis method described as follow: Briefly, 1.0 mL of the prepared OM@DOX-1 or OM@DOX-2 micelles in water was transferred into a dialysis tube (MWCO3500) and dialyzed against different pH buffer solution (80 mL) including pH 7.4, pH 6.8 and pH 5.0 at 37 °C. Then, 3.0 mL of buffer solution was taken out and were replaced with 2.0 mL freshly buffer solution at a specific time interval. The corresponding fluorescent intensity at 555 nm was measured using a 488 excitation wavelength. The amounts of DOX in dialysate were determined using fluorescence spectroscopy based on the standard cure of DOX.
In vitro cytotoxicity
Cytotoxic analysis of OM@DOX-1 and OM@DOX-2 micelles was studied by PrestoBlue assay with HeLa cells. Firstly, 1 × 104 HeLa cells were added into the 96-well plates per well and cultured at 37 °C with 5% CO2 for 12 h, then phosphate buffered saline PBS (1×) was used to wash the metabolites of the cells, and 200 uL different concentrations of Free DOX,OM@DOX-1 and OM@DOX-2 micelles ranging from 0 to10 ug/mL were added, respectively. After being cultured for 24, 48 and 72 h at 37 °C with 5% CO2, the cells were washed with PBS (1×) and added 100 uL pre-prepared PrestoBlue solution, which were diluted 10 times with DMEM, after cultivated for 1 h, a Synergy H1 Microplate Reader was used to record the absorbance at 570 and 600 nm, the untreated cells were used as control and the measured data were analyzed. With the same method, the cytotoxicity of OM@DOX micelles to normal cells (L929) was detected, and the cells treated with Free DOX were used as control. To further study the selectively cytotoxicity of FA-OM@DOX micelles, the cell viability of Free DOX, OM@DOX-2 and FA-OM@DOX micelles to KB cells and A549 cells were measured and analyzed with the protocol.
Cellular uptake and intracellular localization
To examine the internalization of DOX in tumor cells, HeLa cells were incubated into 8-well plate with a density of 1 × 104 per well at 37 °C with 5% CO2, after 12 h adhesion of cells on the plates, Free DOX, OM@DOX-1 and OM@DOX-2 micelles (final DOX concentration: 30 μg/mL) were added and incubated with HeLa cells for 0.5, 2 and 6 h, respectively. Then, the drug outside of cells was washed for five times by PBS (1×) and treated with formalin solution for 0.5 h along with thrice washing using PBS (1×). After that, 0.1% (vol/vol) Triton X-100 in PBS (1×) was added to permeabilize the cells for 5 min, and then, the cells were fixed with 1% (wt/vol) BSA in PBS. Then, filamentous actin (F-actin) cytoskeleton was stained with Alexa Fluor® 633 phalloidin for 1 h. After thrice washing with PBS, DAPI was further used to stain the cell nucleus for 1 min. After removing residual DAPI using PBS washing, a few fresh PBS (1×) was left in the plate for fluorescent imaging. Lasers of 633, 488 and 405 nm were employed to excite Alexa Fluor®633 phalloidin, DOX and DAPI, respectively. The corresponding fluorescence emissions were recorded by a confocal laser scanning microscopy (LSM 800, Carl Zeiss, Germany) using a band-pass filter combination including 638–747 nm, 493–634 nm and 410–507 nm for imaging in three individual channels (Objective: EC Plan-Neofluar 10x/0.30 M27; dimension is 1024 × 1024.).
To obtain the FA-medicated cellular uptake, OM@DOX and FA-OM@DOX micelles were detected, and the procedure was similar to the above-narrated without any staining. Concretely, KB cells and A549 cells were incubated into 8-well plate with a density of 1 × 104 per well at 37 °C with 5% CO2; after 12 h adhesion of cells on the plates, OM@DOX-2 and FA-OM@DOX micelles (final DOX concentration: 30 μg/mL) were added and incubated with HeLa cells for 0.5, 1 and 2 h, respectively. Then, the drug outside of cells were washed for five times by PBS (1×) and a few fresh PBS (1×) was left in the plate for fluorescent imaging. Laser of 488 nm was employed to excite DOX, the fluorescence emissions were recorded by CLSM.
To evaluate the intracellular localization of cells in vitro, Lyso Tracker® Red was used to label lysosomes. Briefly, 8-well plates were used to add 1 × 104 HeLa cells per well, after 12 h adhesion of cells on the plates at 37 °C with 5% CO2, Free DOX, OM@DOX-1 and OM@DOX-2 micelles (final DOX concentration: 30 μg/mL) were added and incubated for 0.5, 1 and 2 h, respectively, then the drugs had not entered the cells were washed for five times with PBS(1×); 400uL Lyso Tracker® Red was added and cultured for 0.5~1 h. After that, the residual Lyso Tracker® Red was washed three times with PBS(1×) and replaced with 100 uL DMEM to record the fluorescence imaging with CLSM and lasers of 577 nm were employed to excite Lyso Tracker®Red.
Quantification of cellular uptake by flow cytometry
six-well plates were used to add 1 × 105 HeLa cells per well and cultured for 12 h at 37 °C with 5% CO2, then OM@DOX-1 and OM@DOX-2 micelles (final DOX concentration: 30 μg/mL) were added 2 mL per well and incubated with HeLa cells for 0.5, 2 and 6 h, respectively, then the drugs had not entered the cells were washed and substituted with 500uL PBS (1×), after that the cells were collected and used a flow cytometry to detect the fluorescence intensity of DOX (PE channel was used and the incident was set as 1 × 105 cells with intermediate speed), among which, the cells without any treatment were served as control.
Results and discussion
Synthesis and characterization of pH-responsive DOX prodrug
The synthesis routes of amphiphilic OM@DOX and FA-OM@DOX prodrug were depicted in Fig. 1. Firstly, the block of POEGMA was synthesized by reversible addition–fragmentation chain transfer (RAFT) reaction of OEGMA using the CPPA-NHS as the RAFT agent and AIBN as the initiator at 70 °C. The diblock copolymer of POEGMA-b-PMGMA was further prepared using POEGMA as the macroinitiator. After reacted with FA–NH2, the targeted prodrug of FA-POEGMA-b-PMGMA was harvested. The obtained POEGMA-b-PMGMA or FA-POEGMA-b-PMGMA copolymer was further cultivated with hydrazine hydrate and subsequently conjugated with DOX, and then the OM@DOX and FA-OM@DOX polymeric prodrugs were obtained, respectively.
The representative 1HNMR spectra of polymer including POEGMA, POEGMA-b-PMGMA, FA-POEGMA-b-PMGMA and FA-OM@DOX were monitored and showed in Fig. 2. The marked peak 1 (3.24 ppm) and peak 2 (3.60 ppm) were the typical peaks of methoxy and methylene group of POEGMA block, while the characteristic peak of CPPA-NHS were also present at 3 (7.83~7.18 ppm). The degree of polymerization (DP) of OEGMA was determined on the base of the integral ratio of peak 3 (phenyl group) and 1 (methyl group). After extending the chain using MGMA monomer, the peaks at 4 (3.73 ppm) and 5 (4.55 ppm) were present in the 1HNMR spectra of POEGMA-b-PMGMA as shown in Fig. 2b. The DP of MGMA was determined on the base of the integral ratio of peak 1 (methyl group) and 5 (methylene group). After reacted with FA-NH2 (Figure S1) by an amidation reaction, FA signals (6.63~8.60 ppm) were present in the 1HNMR spectra of FA-POEGMA-b-PMGMA, indicating the successful synthesis. Finally, FA-POEGMA-b-PMGMA were treated with hydrazine hydrate and further conjugated with DOX drug to obtain amphiphilic polymeric prodrug of FA-OM@DOX, and its 1HNMR spectrum also confirmed the existence of DOX drug.
The molecular weights (M n ,NMR, M n,GPC, g mol−1) of aforementioned polymers were traced using gel permeation chromatography (GPC) technology. As shown in Fig. 3, after further polymerization of POEGMA, the molecular weights present obviously increase from 7100 to 8000 or 10800 for P(OEGMA)30-b-P(MGMA)22 or P(OEGMA)30-b-P(MGMA)60 diblock copolymer, respectively. Additionally, the PDI of above-mentioned polymers were all below 1.2 and indicated a satisfying controlled polymerization. Table 1 summarized the structural information of two targeted polymers and their precursors. In addition, the FT-IR spectra of POEGMA-b-PMGMA, Free DOX and OM@DOX were detected and showed in Figure S2, the stretch-vibration of C–O (OEGMA) and C=O (MGMA) appeared at 1109 and 1731 cm−1, respectively. After grafting DOX, a strong vibrating peak at 1670 cm−1 corresponding to hydrazide group were present in the FT-IR spectrum of OM@DOX, indicated the successful conjugated of DOX.
Morphology and size of prodrug micelles
The amphiphilic OM@DOX prodrug provided a capacity to form polymeric micelles in water solution. We used dynamic light scattering (DLS) and transmission electron microscopy (TEM) to verify the potential micellization. As shown in Fig. 4, OM@DOX micelles exhibited spherical morphology and had an average diameter of 37.8 ± 3.2 and 24.5 + 2.8 nm, which were revealed by TEM results as shown in Fig. 4b and e. Due to the relatively compact morphology, OM@DOX-2 had a small diameter in comparison with OM@DOX-1, although the former had a high more molecular weight. Furthermore, the DLS results of OM@DOX-1 and OM@DOX-2 micelles were determined as 44.5 and 28.8 nm, which were all larger than that of TEM, this might be due to the hydration of the amphiphilic structure of OM@DOX prodrug. The diameters detected by DLS were larger about 5 nm than TEM observed, this appearance maybe due to the swelling of micelles in water media or contraction of micelles in the absence of water media [46, 47]. Additionally, the DLS result indicated that FA-OM@DOX micelles showed an average diameter of 32.8 nm (Figure S3), indicating a desirable micellar size for biological application. The stability of micelles was a crucial parameter to evaluate its in vivo application. Herein, the dynamic change of diameter of OM@DOX-1 and OM@DOX-2 micelles were monitored(the time interval was 24 h)and showed in Fig. 4(c and f), obviously, no distinct change appeared within 5 days, which demonstrated the excellent stability of OM@DOX-1 micelles and OM@DOX-2 micelles in water media, leading to an enhanced drug efficiency.
As presented in Fig. 5a, the UV–vis spectra of Free DOX, OM@DOX-1 and OM@DOX-2 micelles in water showed a representative absorption of DOX at 488 nm, while the peak in OM@hydrazide was absent. Additionally, the fluorescence intensity of representative polymers was tested and presented in Fig. 5b, and it was obvious that Free DOX, OM@DOX-1 and OM@DOX-2 micelles in water with a proper emissive fluorescence corresponding to DOX at 557 nm while OM@hydrazide was absent once again. The above results provided sufficient evidence to support the grafting of DOX molecules. After FA molecules grafted on the end of POEGMA-b-PMGMA polymer, the obtained FA-POEGMA-b-PMGMA polymer in DMF shown the feature absorption peak of FA at 358 nm (Fig. 5c), demonstrating the successful modification of FA in FA-POEGMA-b-PMGMA polymer. In Fig. 5d, pyrene was used as fluorescence probe to monitor the critical micelles concentration (CMC) values of OM@DOX-1 and OM@DOX-2, and the CMC values of which were 0.0087 and 0.0102 mg/mL, respectively, indicating that the prodrugs could assemble into micelles at a low concentration (above the corresponding CMC value).
aUV–vis spectra and b fluorescence spectra of Free DOX, OM@hydrazide, OM@DOX-1 and OM@DOX-2 micelles in water. The insets of a, b and c were the digital photographs of Free DOX, OM@DOX-1 and OM@DOX-2 micelles in water. c UV–vis spectra of POEGMA-b-PMGMA and FA-POEGMA-b-PMGMA in DMF; d The fluorescence intensity ratio I3/I1 of pyrene as a function of OM@DOX-1 and OM@DOX-2 concentration
In vitro release of DOX from prodrug micelles
To obtain the information about the potential of OM@DOX prodrug as the drug carrier,the in vitro release of DOX from OM@DOX-1 and OM@DOX-2 micelles was detected under three simulated buffer solution (pH = 7.4, 6.8 or 5.0) at 37 °C. As shown in Fig. 6, the cumulative release of DOX was only 20.3% from OM@DOX-1micelles while was 11.4% from OM@DOX-2 micelles after 96 h. however, at an acid buffer of pH 5.0,the release rate of DOX within 36 h increased sharply to 63.2 and 71.5% for OM@DOX-1 and OM@DOX-2 micelles, respectively, ultimately, the cumulative release rate were 75.8 and 90.0% within 96 h. In brief, the release results could endow the potential of OM@DOX prodrug as a pH-responsive drug carrier delivering DOX drug into cells with a controlled drug release model.
In vitro cytotoxicity
The cytotoxicity of OM@DOX-1, OM@DOX-2 and FA-OM@DOX micelles were evaluated against HeLa cells (cancer cells) and L929 cells (normal cells) using PrestoBlue assay, and the DOX concentration was ranged from 0 to 10.0 μg/mL. In Fig. 7a–c, after being incubated in HeLa cell for 72 h, the cytotoxicity of OM@DOX-2 micelles with DOX concentration of 10.0 ug/mL presented a higher cytotoxicity than OM@DOX-1 micelles, and the cell viability were 25.6 and 16.2%, respectively, indicating a higher toxicity against tumor cells. Interestingly, the cytotoxicity of OM@DOX-1 and OM@DOX-2 micelles against the normal cells of L929 were 36.4 and 37.1% after 72 h incubation, which is infrequently reported in previously DOX drug delivery systems [16, 30]. The cytotoxicity results further demonstrated that the OM@DOX prodrug shown an obviously high cytotoxicity against tumor cells (HeLa) than normal cells (L929), suggesting a spontaneous tumor-specific targeting ability. In consideration of high drug loading feature and pH-triggered drug release process, the obtained prodrug could simultaneously meet high therapeutic efficiency and low side effect in one system.
Cell viability of HeLa cells (a, b and c) and L-929 cells (d) incubated with Free DOX, OM@DOX-1 and OM@DOX-2 micelles with different drug concentrations. Cell viability of (e) KB and (f) A549 cell lines treated with Free DOX (1), OM@DOX-2 (2) and FA-OM@DOX (3) micelles for 72 h. The data were presented as mean ± SD (n = 3)
To confirm the FA-receptor specificity of OM@DOX prodrug, the cytotoxicity of FA-OM@DOX, OM@DOX and Free DOX were also calculated against the KB cells (FA-receptor-positive) and A549 cells (FA-receptor-negative). As shown in Fig. 7e and f, FA-OM@DOX shown a preferably cytotoxicity against KB cells in comparison with A549 cells, although the cytotoxicity of two cells was parallel under the high concentration of 10 µg/mL, this might be due to the maximum DOX release amount directed by the acid environment in term of tumor cells. Furthermore, OM@DOX prodrug showed high toxicity against tumor cells with passive-targeting pathway, after armed with FA targeting, the prodrug could further realize the tumor-targeting ability through the specific interaction with FA-receptor-positive tumor cells, which was beneficial to targeted cancer therapy [48, 49].
In vitro cellular uptake
The subcellular internalization of Free DOX, OM@DOX-1, OM@DOX-2 and FA-OM@DOX were investigated with a laser confocal scanning microscopy (LCSM). The green fluorescence of DOX, red fluorescence of Alexa Fluors®633 Phalloidin (F-actin) and blue fluorescence of DAPI were used to dye the F-actin and nuclei of cells. As shown in Fig. 8 and Figure S4, the fluorescence intensity of DOX was distinctly increased from 0.5 to 6 h, which suggested that OM@DOX- micelles with high permeability and further delivered DOX into the cells nuclei. Furthermore, OM@DOX-2 micelles with evidently increased fluorescence than OM@DOX-1 micelles at the same time points (0.5, 2 and 6 h), this might be related to the smaller diameter of OM@DOX-2 than OM@DOX-1 micelles. However, after 2 h incubation, Free DOX strong aggregated in the nuclei and shown brighter fluorescence intensity than that of OM@DOX-1 and OM@DOX-2 micelles.
The subcellular internalization of FA-OM@DOX micelles was also investigated and the fluorescence of DOX showed as red, OM@DOX micelles were used as a control against KB cells (Fig. 9). The fluorescence intensity of DOX delivered by FA-OM@DOX micelles with a sustained increasing from 0.5 to 2 h than that of OM@DOX micelles, which indicated that the FA molecular of FA-OM@DOX micelles could effectively interact with FA-receptors on the membrane of KB cells and then entered into the cells.
To further study the procedure of OM@DOX-1 and OM@DOX-2 micelles entered into cells, we estimated the subcellular co-localization of OM@DOX-1 and OM@DOX-2 micelles with Lyso Tracker@Red. As presented in Fig. 10a and Figure S5, the micelles could cross the cell membrane via endocytosis, and then released the drug triggered by the low pH of lysosome in cells. After incubated for 0.5 to 6 h, the increased fluorescence intensity of DOX derived from OM@DOX micelles delivered suggested a sustained entering process of micelles.
a CLSM images of HeLa cells treated with OM@DOX-2 micelles for 0.5, 2 and 6 h, respectively. For each row, images from left to right display the internalized DOX (green), lysosome (Lyso Tracker@Red, red), cell morphology in bright filed and the overlays of three images, respectively. Scale bars: 50 μm. b Quantitative analysis of intracellular uptake of OM@DOX-1 and OM@DOX-2 micelles incubated with control, 0.5, 2 and 6 h in HeLa cells using flow cytometry; c the mean fluorescence intensity (MFI) of OM@DOX-1 and OM@DOX-2 micelles at different time points, and the data were presented as mean ± SD (n = 3)
Quantitative cellular uptake of DOX at different time points was monitored with Flow cytometry. In Fig. 10b and Figure S6, HeLa cells treated with OM@DOX-2 micelles showed a considerable increase of fluorescence intensity due to the internalized DOX. Furthermore, the median fluorescence intensity (MFI) of which reached up to 8028 (87.04%) after 0.5 h, which suggested most drugs had been phagocytosed by cells, while OM@DOX-1 micelles with a lower intracellular uptake rate and after 0.5 h with the MFI of 5714 (58.50%). After 6 h incubation, the fluorescence of swallowed OM@DOX-2 micelles (MFI = 15765, 96.29%) was slightly higher than OM@DOX-1 micelles (MFI = 16914, 93.01%), and these results were consistent with the CLSM results and were partially related to its smaller diameter.
Conclusion
In conclusion, we have synthesized one new type of acid-activatable doxorubicin (DOX) polymeric prodrug with ultra-high drug loading for targeted cancer therapy. The amphiphilic FA-OM@DOX or OM@DOX prodrug could self-assemble into prodrug micelles in water solution and expressed high micellar stability even a 5 days storage. The size of prodrug micelles could control by adjusting the length of hydrophilic and hydrophobic chain. Additionally, the designed structure also endowed the prodrug a high drug loading up to 61.5 wt%. The following cytotoxicity results demonstrated that OM@DOX micelles exhibited a higher toxicity against HeLa cells (Cancer cells) than L929 cells (Normal cells), indicating a spontaneous tumor-specific targeting ability. Moreover, the targeted form of FA-OM@DOX micelles present a selective toxicity for FA-receptor-positive KB cells rather than the FA-receptor-negative A549 cells, showing a tumor-targeting ability. In consideration of high drug loading content, pH-triggered drug release behavior and fast cell-penetrating ability. We believe that the present prodrug could offer constructive idea for preparation of stimuli-responsive nanomedicine platform and further extruded its mission in the field of targeted cancer therapy.
References
Chen W, Zheng R, Zeng H, Zhang S (2015) Epidemiology of lung cancer in China. Thorac Cancer 6:209–215
Tibbitt M, Dahlman J, Langer R (2016) Emerging frontiers in drug delivery. J Am Chem Soc 3:704–717
Blum A, Kammeyer J, Rush A, Callmann C, Hahn M, Gianneschi N (2015) Stimuli-responsive nanomaterials for biomedical applications. J Am Chem Soc 137:2140–2154
Ban Q, Bai T, Duan X, Kong J (2017) Noninvasive photothermal cancer therapy nanoplatforms via integrating nanomaterials and functional polymers. Biomater Sci 5:190–210
Xu Z, Ma X, Gao Y, Hou M, Xue P, Li C, Kang Y (2017) Multifunctional silica nanoparticles as a promising theranostic platform for biomedical applications. Mater Chem Front 1:1257–1272
Holohan C, Van Schaeybroeck S, Longley D, Johnston P (2013) Cancer drug resistance: an evolving paradigm. Nat Rev Cancer 13:714–726
Mahmoudi M, Hofmann H, Rothen-Rutishauser B, Petri-Fink A (2012) Assessing the in vitro and in vivo toxicity of superparamagnetic iron oxide nanoparticles. Chem Rev 112:2323–2338
Chen G, Qiu H, Prasad P, Chen X (2014) Upconversion nanoparticles: design, nanochemistry, and applications in theranostics. Chem Rev 114:5161–5214
Tibbitt M, Dahlman J, Langer R (2016) Emerging frontiers in drug delivery. J Am Chem Soc 138:704–717
Lu Y, Aimetti A, Langer R, Gu Z (2016) Bioresponsive materials. Nat Rev Mater 2:16075
Kluza E, Jacobs I, Hectors S, Mayo K, Griffioen A, Strijkers G, Nicolay K (2012) Dual-targeting of αvβ3 and galectin-1 improves the specificity of paramagnetic/fluorescent liposomes to tumor endothelium in vivo. J Control Release 158:207–214
Pattni B, Chupin V, Torchilin V (2015) New developments in liposomal drug delivery. Chem Rev 115:10938–10966
Du J, Tang Y, Lewis A, Armes S (2011) Tailor-made dual pH-sensitive polymer-doxorubicin nanoparticles for efficient anticancer drug delivery. J Am Chem Soc 133:17560–17563
Wang Y, Wang J, Han H, Liu J, Zhao H, Shen M, Xu Y, Xu J, Li L, Guo X (2016) Self-assembled micelles of N-phthaloylchitosan-g-poly (N-vinylcaprolactam) for temperature-triggered non-steroidal anti-inflammatory drug delivery. J Mater Sci 51:1591–1599. doi:10.1007/s10853-015-9482-2
Lu S, Neoh K, Huang C, Shi Z, Kang E (2013) Polyacrylamide hybrid nanogels for targeted cancer chemotherapy via co-delivery of gold nanoparticles and MTX. J Colloid Interface Sci 412:46–55
Yang C, Huang S, Wang X, Wang M (2016) Theranostic unimolecular micelles of highly fluorescent conjugated polymer bottlebrushes for far red/near infrared bioimaging and efficient anticancer drug delivery. Polym Chem 7:7455–7468
Xu Z, Liu S, Liu H, Yang C, Kang Y, Wang M (2015) Unimolecular micelles of amphiphilic cyclodextrin-core star-like block copolymers for anticancer drug delivery. Chem Commun 51:15768–15771
Wang C, Wei H, Tan N, Boydston A, Pun S (2016) Sunflower polymers for folate-mediated drug delivery. Biomacromolecules 17:69–75
Zhang S, Xu J, Chen H, Song Z, Wu Y, Dai X, Kong J (2017) Acid-cleavable unimolecular micelles from amphiphilic star copolymers for triggered release of anticancer drugs. Macromol Biosci 17:1600258
Chen F, Chen H, Duan X, Jia J, Kong J (2016) Molecularly imprinted polymers synthesized using reduction-cleavable hyperbranched polymers for doxorubicin hydrochloride with enhanced loading properties and controlled release. J Mater Sci 51:9367–9383. doi:10.1007/s10853-016-0183-2
Duan X, Wu Y, Ma M, Du J, Zhang S, Chen H, Kong J (2017) Amphiphilic polymer–drug conjugates based on acid-sensitive 100% hyperbranched polyacetals for cancer therapy. J Mater Sci 52:9430–9440. doi:10.1007/s10853-017-1135-1
Xu Z, Xue P, Gao Y, Liu S, Shi X, Hou M, Kang Y (2017) pH-responsive polymeric micelles based on poly(ethyleneglycol)-b-poly(2-(diisopropylamino) ethyl methacrylate) block copolymer for enhanced intracellular release of anticancer drugs. J Colloid Interface Sci 490:511–519
Bui D, Maksimenko A, Desmaele D, Harrisson S, Vauthier C, Couvreur P, Nicolas J (2013) Polymer prodrug nanoparticles based on naturally occurring isoprenoid for anticancer therapy. Biomacromolecules 14:2837–2847
Wang H, Sun D, Zhao N, Yang X, Shi Y, Li J, Su Z, Wei G (2014) Fabrication of alginate–gelatin crosslinked hydrogel microcapsules and evaluation of the microstructure and physico-chemical properties. J Mater Chem B 2:1362–1370
Li H, Du J, Du X, Xu C, Sun C, Wang H, Cao Z, Yang X, Zhu Y, Nie S, Wang J (2016) Stimuli-responsive clustered nanoparticles for improved tumor penetration and therapeutic efficacy. Proc Natl Acad Sci USA 113:4164–4169
Liow S, Dou Q, Kai D, Li C, Sugiarto S, Yu C, Kwok R, Chen X, Wu Y, Ong S, Kizhakeyil A, Verm N, Tang B, Loh X (2016) Long-term real-time in vivo drug release monitoring with AIE thermogelling polymer. Small 13:1603404
Zhan F, Chen W, Wang Z, Lu W, Cheng R, Deng C, Meng F, Liu H, Zhong Z (2011) Acid-activatable prodrug nanogels for efficient intracellular doxorubicin release. Biomacromolecules 12:3612–3620
Xu Z, Zhang K, Hou L, Wang D, Liu Y, Guan J, Zhang Y, Zhang H (2014) A novel nanoassembled doxorubicin prodrug with a high drug loading for anticancer drug delivery. J Mater Chem B 2:3433–3437
Xu X, Wu J, Liu Y, Yu M, Zhao L, Zhu X, Bhasin S, Li Q, Ha E, Shi J, Farokhzad O (2016) Ultra-pH-responsive and tumor-penetrating nanoplatform for targeted siRNA delivery with robust anti-cancer efficacy. Angew Chem Int Ed 55:7091–7094
Shi X, Ma X, Hou M, Gao Y, Bai S, Xiao B, Xue P, Kang Y, Xu Z, Li C (2017) pH-responsive unimolecular micelles based on amphiphilic star-like copolymer with high drug loading for effective drug delivery and cellular imaging. J Mater Chem B 5:6847–6859
Hu X, Liu G, Li Y, Wang X, Liu S (2015) Cell-penetrating hyperbranched polyprodrug amphiphiles for synergistic reductive milieu-triggered drug release and enhanced magnetic resonance signals. J Am Chem Soc 137:362–368
Xu Z, Liu Y, Kang J, Wang F (2015) Glutathione- and pH-responsive nonporous silica prodrug nanoparticles for controlled release and cancer therapy. Nanoscale 7:5859–5868
Zhang X, Liu K, Huang Y, Xu J, Li J, Ma X, Li S (2014) Reduction-sensitive dual functional nanomicelles for improved delivery of paclitaxel. Bioconjug Chem 25:1689–1696
Li Y, Xiao K, Zhu W, Deng W, Lam K (2014) Stimuli-responsive cross-linked micelles for on-demand drug delivery against cancers. Adv Drug Deliv Rev 66:58–73
Duan X, Chen H, Fan L, Kong J (2016) Drug self-assembled delivery system with dual responsiveness for cancer chemotherapy. ACS Biomater Sci Eng 2:2347–2354
Debbage P (2009) Targeted drugs and nanomedicine: present and future. Curr Pharm Des 15:153–172
Li R, Feng F, Wang Y, Yang X, Yang X (2014) Folic acid-conjugated pH/temperature/redox multi-stimuli responsive polymer microspheres for delivery of anti-cancer drug. J Colloid Interface Sci 429:34–44
Liu H, Xu Y, Wen S, Chen Q, Zheng L, Shen M, Zhao J, Zhang G, Shi X (2013) Targeted tumor computed tomography imaging using low-generation dendrimer-stabilized gold nanoparticles. Chem Eur J 19:6409–6416
Xu Z, Hou M, Shi X, Gao Y, Xue P, Liu S, Kang Y (2017) Rapidly cell-penetrating and reductive milieu-responsive nanoaggregates assembled from an amphiphilic folate-camptothecin prodrug for enhanced drug delivery and controlled release. Biomater Sci 3:444–454
Ross J, Chaudhuri P, Ratnam M (1994) Differential regulation of folate receptor isoforms in normal and malignant tissues in vivo and in established cell lines: physiological and clinical implications. Cancer 73:2432–2443
Kang M, Yoo H, Kwon Y, Yoon H, Lee S, Kim S, Yeom D, Kang M, Choi Y (2015) Design of multifunctional liposomal nanocarriers for folate receptor-specific intracellular drug delivery. Mol Pharm 12:4200–4213
Guo X, Shi C, Wang J, Di S, Zhou S (2013) pH-triggered intracellular release from actively targeting polymer micelles. Biomaterials 34:4544–4554
Chen Y, Cao W, Zhou J, Pidhatika B, Xiong B, Huang L, Tian Q, Shu Y, Wen W, Hsing I, Wu H (2015) Poly(l-lysine)-graft-folic acid-coupled poly(2-methyl-2-oxazoline) (PLL-g-PMOXA-c-FA): a bioactive copolymer for specific targeting to folate receptor-positive cancer cells. ACS Appl Mater Interfaces 7:2919–2930
Lu J, Zhao W, Huang Y, Liu H, Marquez R, Gibbs R, Li J, Venkataramanan R, Xu L, Li S (2014) Targeted delivery of doxorubicin by folic acid-decorated dual functional nanocarrier. Mol Pharm 11:4164–4178
Wang H, Xu F, Li D, Liu X, Jin Q, Ji J (2013) Bioinspired phospholipid polymer prodrug as a pH responsive drug delivery system for cancer therapy. Polym Chem 4:2004–2010
Xu Z, Wang D, Xu S, Liu Zhang X, Zhang H (2014) Preparation of a camptothecin prodrug with glutathione-responsive disulfide linker for anticancer drug delivery. Chem Asian J 9:199–205
Xu J, Tian K, Zhao X, Zhou T, Pei M, Liu P (2016) Fluorescent amphiphilic copolymer-based tumor theranostics for facile DOX-loading and tumor microenvironment-triggered release. Mater Des 105:333–340
Zhang Y, Sun Y, Xu X, Zhu H, Huang L, Zhang X, Qi Y, Shen Y (2010) Radiosynthesis and micro-SPECT imaging of 99mTc-dendrimer poly(amido)-amine folic acid conjugate. Bioorg Med Chem Lett 20:927–931
Xu Z, Shi X, Hou M, Xue P, Gao Y, Liu S, Kang Y (2017) Disassembly of amphiphilic small molecular prodrug with fluorescence switch induced by pH and folic acid receptors for targeted delivery and controlled release. Colloid Surf B 150:50–58
Acknowledgements
This work was supported by a star-up Grant (SWU115058, SWU115059), Fundamental Research Funds for Central Universities from Southwest University (XDJK2016A010) and Chongqing Research Program of Basic Research and Frontier Technology (cstc2016jcyjA0078) and National Natural Science Foundation of China (51703187, 31671037, 21602073).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ma, X., Shi, X., Bai, S. et al. Acid-activatable doxorubicin prodrug micelles with folate-targeted and ultra-high drug loading features for efficient antitumor drug delivery. J Mater Sci 53, 892–907 (2018). https://doi.org/10.1007/s10853-017-1546-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10853-017-1546-z