Abstract
Purpose
To assess the feasibility and safety of same-day discharge after S-ICD implantation by implementing a specific analgesia protocol and phone follow-up.
Methods
Consecutive patients presenting for outpatient S-ICD implantation were enrolled between 1/1/2018 and 4/30/2019. An analgesia protocol included pre-operative acetaminophen and oxycodone, intraoperative local bupivacaine, and limited use of oxycodone-acetaminophen at discharge. The primary outcome was successful same-day discharge. Numerical Pain Rating Scale (NPRS) on postoperative day (POD) 1, 3, 14, and 30 and any unplanned health care visits during the 1-month follow-up period were assessed.
Results
Out of 53 potentially eligible S-ICD patients, 49 patients (92.5%) were enrolled and successfully discharged on the same day. Mean age of these 49 patients was 47 ± 14 years. There were no acute procedural complications. Severe pain (NPRS ≥ 8) on POD 0, 1, and 3 was present in 14.3%, 14.3%, and 8.2% of patients, respectively. The total in-hospital stay was 534 ± 80 min. Four unplanned visits (8%) due to cardiac or device-related issues occurred during 1-month follow-up, including 2 patients with heart failure exacerbation, one patient with an incisional infection, and one patient with inappropriate shocks.
Conclusions
With the appropriate institutional protocol including specific analgesics and phone follow-up, same-day discharge after outpatient S-ICD implantation is feasible and appears safe for most patients.. Device-related pain can be severe in the first 3 days post-implantation and can be successfully treated with limited supply of narcotic medications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Various cardiovascular procedures are routinely performed on an outpatient basis, including percutaneous coronary intervention, transvenous pacemaker/defibrillator implantation, and catheter ablation of certain arrhythmias [1, 2]. Subcutaneous implantable defibrillator (S-ICD) is an established device therapy for the treatment of malignant ventricular tachyarrhythmias [3,4,5,6]. In patients without a pacing indication or at high risk for infection, S-ICD is a preferred device option as S-ICD is not associated with pneumo/hemothorax, cardiac perforation, tricuspid regurgitation or endocarditis [7].
The perioperative care for patients with S-ICD is still evolving and the patients are often monitored overnight after implantation due to a perceived need for parenteral pain medications for effective pain control associated with the larger device pocket, extensive soft tissue dissection, and subcutaneous tunneling. The feasibility and safety of outpatient S-ICD implantation has not been assessed in a prospective fashion.
The purpose of this study was to assess the feasibility and safety of the same-day discharge after S-ICD implantation using a specific analgesia strategy referred to as DASH protocol (same day subcutaneous defibrillator and send home).
2 Methods
2.1 Inclusion and exclusion criteria
Consecutive patients > 18 years of age presenting for outpatient S-ICD implantation (EMBLEM™, MRI S-ICD, Boston Scientific, Natick, MA, USA) were enrolled to a prospective registry between 1/1/2018 and 4/30/2019 at the Ohio State University Medical Center. The purpose of the study was to evaluate a specific analgesia protocol designed to allow for the same-day discharge after outpatient S-ICD implantation. S-ICD implantation for hospitalized patients was excluded. Eligible patients had to be accompanied by a companion to drive them home and the companion had to be present when discharge instructions were provided. Those who were unable or unwilling to provide informed consent and those with inotrope-dependent congestive heart failure (CHF) and/or implanted with left ventricular assist device were excluded. Patients were appropriately screened for S-ICD implantation using a proprietary automated ECG screening tool [8].
2.2 Pre-implantation preparation and prophylactic analgesics
All outpatient S-ICD implantations were scheduled in the morning or early afternoon to avoid late evening discharge. Acetaminophen 975 mg and oxycodone 10 mg were given orally 1–2 h prior to the procedure unless they had a known intolerance or allergy to either of the drugs. (Fig. 1) All patients were evaluated by the anesthesiologist in the pre-operative unit, including assessment of the American Society of Anesthesiologists (ASA) physical status classification and modified Mallampati scoring. Briefly, ASA I, II, III, and IV describe a normal healthy patient, a patient with mild systemic disease, a patient with severe systemic disease, and a patient with severe systemic disease that is a constant threat to life, respectively [9]. A radial arterial line was placed if necessary. An indwelling urinary catheter was not used. Direct oral anticoagulants were held for 24 h. Antiplatelet drugs, warfarin, and all cardiac medications were generally continued peri-procedurally. Intravenous prophylactic antibiotics (cefazolin and vancomycin) were administered pre-procedurally.
2.3 Implantation technique
Either general anesthesia or monitored anesthesia care was provided at the discretion of the anesthesiologist [10, 11]. An S-ICD system (EMBLEM™, MRI S-ICD, Boston Scientific, Natick, MA, USA) was implanted using a standard 2-incision technique. Pre-incisional infiltration of 0.25% bupivacaine (maximum dose, 2.5 mg/kg or 175 mg/dose) was given and repeated as necessary to the subxiphoid and lateral pockets. (Fig. 1) A standard conversion test (defibrillation threshold test (DFT)) was performed using 50-Hz burst pacing to induce ventricular fibrillation (VF) unless contraindicated. When the risk of VF induction was deemed prohibitive, a 10 J synchronized shock was delivered to measure impedance.
2.4 Post-anesthesia care
Those who were intubated for the procedure were extubated in the electrophysiology lab. Patients were monitored on cardiac telemetry in the post-anesthesia care unit. Postero-anterior and lateral chest X-ray was obtained in all patients. Self-reported pain using the 0–10 Numerical Pain Rating Scale (NPRS) was assessed approximately 2 h after the procedure. NPRS 0–5, 6–7, ≥ 8 were classified as mild, moderate, and severe pain, respectively [12]. Pain medications, either intravenous or oral narcotics, were administered as necessary. Discharge readiness was assessed using the Aldrete score, which assigns 0–2 points to the following criteria with a maximum total score of 10: activity, respiration, circulation, consciousness, and color. Patients with an Aldrete score of 9 or greater were considered appropriate for discharge [13].
2.5 Post-discharge care and follow-up
Ten tablets of oxycodone-acetaminophen 5/325 mg were prescribed at the time of discharge. No refill rule was strictly enforced. Self-reported pain using the 0–10 NPRS and the number of oxycodone-acetaminophen taken were assessed on the postoperative days (POD) 1, 3, and 14 by phone interview and approximately in 1 month at the time of in-person device check. Any device-related complications, inappropriate and appropriate device discharges, unplanned clinic and hospital visits were evaluated during the 1-month follow-up period (Fig. 1).
2.6 Informed consent and funding source
The Ohio State University Institutional Review Board approved the study, and all patients provided informed consent before pre-procedural pain medications were administered. The study was funded by Boston Scientific Corporation (Natick, MA, USA). The funding source did not have any involvement in the study design, in the collection, analysis and interpretation of data, in the writing of the report, or in the decision to submit the article for publication.
2.7 Statistical analysis
Continuous variables are presented as mean ± standard deviation (SD) and categorical variables are expressed as percentages. Total procedure time is defined as time interval between skin incision and skin closure. Total in-room time is defined as time interval from the patient’s arrival to the procedure room to departure from the procedure room. Total time in post recovery room is defined as time interval between arrival to the post anesthesia recovery unit to discharge from the hospital. Total in-hospital stay is defined as time interval from patient’s arrival to the hospital to discharge from the hospital. The mean NPRS in the first 3 days is the sum of NPRS at POD#0, #1, and #3 divided by 3. The mean NPRS in the first 3 days and NPRS at POD #14 were compared using paired sample t test.
3 Results
3.1 Study population
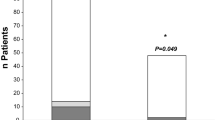
Sixty-two patients presented to the Ohio State University Medical Center for outpatient S-ICD implantation between 1/1/2018 and 4/30/2019. Five patients failed automated electrocardiographic screening for the S-ICD system and received a transvenous device. Four patients declined to participate in the DASH protocol due to their preference for overnight observation post-procedurally. After excluding these 9 patients, 53 patients were potentially eligible for the DASH protocol. However, three patients were subsequently deemed ineligible pre-procedurally for same-day discharge due to CHF exacerbation (N = 2) and uncontrolled diabetes (N = 1) and hospitalized for medical management. One patient received an S-ICD as planned; however, it was removed and replaced by a transvenous device due to unsuccessful DFT testing. Consequently, out of 53 patients potentially eligible for same day discharge, a total of 49 patients ultimately enrolled in the DASH protocol and were successfully discharged on the same day. Therefore, the rate of successful completion of the DASH protocol was 92.5%. (Fig. 2).
3.2 Patient characteristics
Baseline patient characteristics for the enrolled patients (N = 49) are listed in Table 1. Briefly, 27 (45%) patients were male, and the mean age was 47 ± 14 years. Four (8.1%) patients were over the age of 65. The mean body mass index (BMI) was 31 ± 7 kg/m2, and body weight ranged from 40.6 kg to 145 kg. The number of patients with BMI < 30, 30–35, 35–40, and > 40 kg/m2 were 22, 13, 9, and 5, respectively. Forty-four (90%) received S-ICD for a primary prevention indication. The most common cardiac etiology was non-ischemic cardiomyopathy (N = 20, 40.8%), followed by ischemic cardiomyopathy (N = 14, 28.6%). The mean left ventricular ejection fraction was 38 ± 15%. Three patients previously underwent transvenous defibrillator removal due to infection (N = 2) and lead malfunction (N = 1). Nine patients were receiving oral anticoagulation agent including warfarin (N = 3, mean INR at implantation = 1.8), apixaban (N = 5), and rivaroxaban (N = 1). Acetaminophen 975 mg and oxycodone 10 mg were given prior to the procedure to all patients except for one patient who did not receive oxycodone due to the reported drug intolerance to oxycodone.
3.3 Procedural characteristics and anesthetic care
Table 2 outlines the procedural characteristics. Two (4%) patients reported moderate to severe pain pre-procedurally due to underlying chronic pain syndrome. Twenty-three (47%) patients received general anesthesia while monitored anesthesia care was provided to 26 (53%) patients. Total 39.6 ± 10.6 ml bupivacaine (99 ± 26.5 mg) was used. DFT was attempted and successful in 42 patients. As previously mentioned, 1 patient failed DFT and received a transvenous ICD instead (NICM EF 20%, NYHA class II). This patient was not included in the analysis. Four patients received a 10 J synchronized shock for impedance measurement without VF induction due to patient refusal (N = 1), electrolyte imbalance (N = 1), and severe CHF (N = 2). Three patients underwent neither DFT nor 10 J shock due to an intracardiac thrombus. Total skin-to-skin procedure time, including DFT, was 80 ± 39 min. Patients remained in the post anesthesia recovery room for 248 ± 71 min. The total in-hospital stay, from arrival to the hospital to discharge, was 534 ± 80 min. There were no acute procedural complications.
3.4 Pain assessment
Figure 3 describes the pain level at immediately post-implantation (POD #0), 1 day, 3 days, 14 days, and 30 days after implantation. Notably, 14.3%, 14.3%, and 8.2% of patients on POD #0, #1, and #3 reported severe pain (NPRS ≥ 8). The mean NPRS in the first 3 days was 4.1 ± 1.6. The difference of the average NPRS in the first 3 days and the NPRS at POD #14 was 2.5 ± 1.9 (95% CI, 1.9–3.1; P < 0.01).
3.5 Post-discharge narcotics use and unplanned hospitalization
In the first 3 postoperative days, five patients took no oxycodone-acetaminophen and 43 patients took the mean 4.9 ± 2.9 tablets of oxycodone-acetaminophen. One patient did not report the number of tablets taken. Five patients took all 10 tablets by day 3. No narcotics refills were provided. Seven patients had unscheduled healthcare visits within 30 days of the S-ICD implantation, including 3 visits unrelated to S-ICD or cardiac conditions, 2 visits due to CHF exacerbation, 1 visit due to S-ICD incisional infection treated with oral antibiotics, and 1 visit due to inappropriate shocks. The last patient (NICM EF 27%, primary prevention, BMI = 42 kg/m2) received inappropriate shocks due to oversensing 3 days post-implant and S-ICD was removed due to the patient’s request. He declined any further ICD therapy.
4 Discussion
4.1 Main findings
Same-day discharge after outpatient S-ICD implantation is feasible and safe. The DASH protocol was completed in 49/53 (92.5%) eligible S-ICD patients. None of the 49 patients who were discharged on the same day after outpatient S-ICD implantation needed to be readmitted within 24 h of the discharge to manage post-operative pain. The analgesic protocol was simple and easy to implement, only incorporating pre-procedural oral medications, a change of intraoperative local anesthetic drug, a prescription for discharge pain medications, and post-discharge phone follow up from a nurse.
4.2 Development of the same-day discharge protocol
To our knowledge, this is the first prospective and systematic study to assess the feasibility and safety of the same-day discharge specifically for outpatient S-ICD implantation using the specific analgesic protocol. S-ICDs have been implanted at our institution since 2009, and all previous patients had been monitored at least overnight following the S-ICD implantation. The DASH protocol (same day subcutaneous defibrillator and send home) was devised to achieve effective pain control in the outpatient setting.
Previously, it was presumed that the large S-ICD generator pocket, extensive soft tissue dissection, and subcutaneous tunneling would require inpatient administration of potent parenteral analgesics such as morphine and hydromorphone post-operatively to achieve adequate pain control. Consequently, patients following the elective outpatient S-ICD implantation were hospitalized to a cardiac telemetry unit. In devising a specific analgesic protocol for S-ICD implantation, a wide range of prophylactic pain medications were considered, including NSAIDs, opioid, gabapentinoid (gabapentin and pregabalin), and acetaminophen, as well as adjuvant peripheral regional anesthesia [14, 15]. Given the wide availability and cardiovascular safety profile, a simple combination of oral acetaminophen 975 mg and oxycodone 10 mg 1–2 h prior to the incision was chosen. With regard to the choice of local anesthetics, lidocaine, bupivacaine, liposomal bupivacaine, and a mixture of lidocaine and bupivacaine were considered. Previously, lidocaine had been used in our institution for all S-ICD implantation. It has a rapid onset but duration of only up to 2 h. Bupivacaine provides an intermediate onset and a longer duration of analgesia for up to 14 h [16]. Lidocaine and bupivacaine can be mixed in order to merit from the immediate onset of lidocaine and longer effects of bupivacaine. However, 0.25% (2.5 mg/ml) bupivacaine alone was selected to simplify the protocol so as to avoid dose miscalculation that may arise from mixing lidocaine and bupivacaine. Liposomal bupivacaine is a new formulation of bupivacaine that provides slow and sustained release of bupivacaine, and its local effect can last up to 3 days. It is, however, expensive, and cost-effectiveness data of this formulation compared with plain bupivacaine are lacking [17].
The DASH protocol was predicated on the extensive prior S-ICD experience and availability of the multidisciplinary team at our institution. More than 300 S-ICDs have been implanted at our institution. The multidisciplinary care team, including anesthesiologists, nurse anesthetists, and device clinic nurses, have had extensive clinical experience caring for patients with S-ICD implantation. Follow-up phone calls from the experienced electrophysiology nurses likely reassured our patients and prevented unnecessary hospital or clinic visits solely for pain control.
4.3 Self-reported pain scale and medication use
Up to 14% of our patients reported severe pain (NPRS ≥ 8) on day 1 through day 3 post-operatively. Accordingly, most patients (88%) took at least 1 oxycodone-acetaminophen tablet by day 3. However, the pain was controlled with oral medications and no patients returned to the hospital for intravenous pain control. With regard to opioid prescription, only 10 tablets of low-dose oxycodone-acetaminophen were prescribed at the time of discharge and no refill rule was strictly enforced. It is reassuring to note that the risk of opioid abuse and dependence associated with a low dose and short-term use is considerably lower than high dose and/or long-term opioid use [18].
4.4 Complications
There were 2 unplanned healthcare visits (4%) within 30 days of implantation conclusively related to S-ICD implantation due to incisional infection successfully treated with oral antibiotics and inappropriate shocks due to oversensing, leading to S-ICD removal. Neither of these complications, however, would have been prevented even if they had stayed overnight in the hospital following outpatient S-ICD implantation.
4.5 DFT testing
The current guidelines give a class I indication for DFT testing during S-ICD implantation, and it is our routine practice to perform DFT unless contraindicated. [19] In this study, the vast majority of patients underwent DFT testing (43 out of 50, 86%) and 4 patients (8%) received a 10 J shock to insure S-ICD system integrity. Only 3 patients (6%) underwent neither DFT nor 10 J shock testing. Overall, DFT testing did not impede patients from being discharged on the same day.
4.6 Limitations
Several limitations of the study should be noted. First, by the study design, this is a single arm prospective study without a control group. Therefore, it is unknown whether outpatient S-ICD patients could have been discharged safely with adequate pain control without the specific analgesic protocol. Based on our shared experience with S-ICD implantation, pain associated with the larger device pocket, extensive soft tissue dissection, and subcutaneous tunneling was felt to be more severe than that of small pectoral devices. It was therefore deemed unethical to randomize patients or assign eligible patients to a control group. Second, only outpatients were included in this study and the majority of the subjects were for primary prevention SCD indication. Hence, the findings are not entirely applicable to inpatients, who are generally sicker and medically complex. We have, however, adopted the same prophylactic analgesic protocol as the standard of care for all S-ICD implantation in our clinical practice. Third, this is a small single-center study, and implementation of the same-day discharge protocol may not be applicable or safe in hospitals with limited S-ICD experiences. There is a significant learning curve for physicians newly adopting the S-ICD [20].
5 Conclusions
With the appropriate institutional protocol, same-day discharge after outpatient S-ICD implantation is feasible and appears safe for most patients. Although device-related pain can be pronounced over the first 3 days post-implantation, this pain and patient anxiety was well-managed by a short course of narcotics and phone support provided by a nurse.
References
Marijon E, Albenque JP, Boveda S, Jacob S, Schmutz M, Bortone A, et al. Feasibility and safety of same-day home discharge after radiofrequency catheter ablation. Am J Cardiol. 2009;104(2):254–8. https://doi.org/10.1016/j.amjcard.2009.03.024.
Peplow J, Randall E, Campbell-Cole C, Kamdar R, Petzer E, Dhillon P, et al. Day-case device implantation-a prospective single-center experience including patient satisfaction data. Pacing Clin Electrophysiol. 2018;41(5):546–52. https://doi.org/10.1111/pace.13324.
Weiss R, Knight BP, Gold MR, Leon AR, Herre JM, Hood M, et al. Safety and efficacy of a totally subcutaneous implantable-cardioverter defibrillator. Circulation. 2013;128(9):944–53. https://doi.org/10.1161/CIRCULATIONAHA.113.003042.
Friedman DJ, Parzynski CS, Varosy PD, Prutkin JM, Patton KK, Mithani A, et al. Trends and in-hospital outcomes associated with adoption of the subcutaneous implantable cardioverter defibrillator in the United States. JAMA Cardiol. 2016;1(8):900–11. https://doi.org/10.1001/jamacardio.2016.2782.
Gold MR, Aasbo JD, El-Chami MF, Niebauer M, Herre J, Prutkin JM, et al. Subcutaneous implantable cardioverter-defibrillator post-approval study: clinical characteristics and perioperative results. Heart Rhythm. 2017;14(10):1456–63. https://doi.org/10.1016/j.hrthm.2017.05.016.
Burke MC, Gold MR, Knight BP, Barr CS, Theuns D, Boersma LVA, et al. Safety and efficacy of the totally subcutaneous implantable defibrillator: 2-year results from a pooled analysis of the IDE study and EFFORTLESS registry. J Am Coll Cardiol. 2015;65(16):1605–15. https://doi.org/10.1016/j.jacc.2015.02.047.
Al-Khatib SM, Stevenson WG, Ackerman MJ, Bryant WJ, Callans DJ, Curtis AB, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2018;72(14):e91–e220. https://doi.org/10.1016/j.jacc.2017.10.054.
Francia P, Ziacchi M, De Filippo P, Viani S, D'Onofrio A, Russo V, et al. Subcutaneous implantable cardioverter defibrillator eligibility according to a novel automated screening tool and agreement with the standard manual electrocardiographic morphology tool. J Interv Card Electrophysiol. 2018;52(1):61–7. https://doi.org/10.1007/s10840-018-0326-2.
Dripps RD, Lamont A, Eckenhoff JE. The role of anesthesia in surgical mortality. JAMA. 1961;178:261–6. https://doi.org/10.1001/jama.1961.03040420001001.
Essandoh MK, Otey AJ, Abdel-Rasoul M, Stein EJ, Turner KR, Joseph NC, et al. Monitored anesthesia care for subcutaneous cardioverter-defibrillator implantation: a single-center experience. J Cardiothorac Vasc Anesth. 2016;30(5):1228–33. https://doi.org/10.1053/j.jvca.2016.06.007.
Essandoh MK, Mark GE, Aasbo JD, Joyner CA, Sharma S, Decena BF, et al. Anesthesia for subcutaneous implantable cardioverter-defibrillator implantation: perspectives from the clinical experience of a U.S. panel of physicians. Pacing Clin Electrophysiol. 2018. https://doi.org/10.1111/pace.13364.
Boonstra AM, Stewart RE, Koke AJ, Oosterwijk RF, Swaan JL, Schreurs KM, et al. Cut-off points for mild, moderate, and severe pain on the numeric rating scale for pain in patients with chronic musculoskeletal pain: variability and influence of sex and catastrophizing. Front Psychol. 2016;7:1466. https://doi.org/10.3389/fpsyg.2016.01466.
Aldrete JA, Kroulik D. A postanesthetic recovery score. Anesth Analg. 1970;49(6):924–34.
Droghetti A, Basso Ricci E, Scimia P, Harizai F, Marini M. Ultrasound-guided serratus anterior plane block combined with the two-incision technique for subcutaneous ICD implantation. Pacing Clin Electrophysiol. 2018;41(5):517–23. https://doi.org/10.1111/pace.13318.
Miller MA, Garg J, Salter B, Brouwer TF, Mittnacht AJ, Montgomery ML, et al. Feasibility of subcutaneous implantable cardioverter-defibrillator implantation with opioid sparing truncal plane blocks and deep sedation. J Cardiovasc Electrophysiol. 2019;30(1):141–8. https://doi.org/10.1111/jce.13750.
Manzoor S, Taneja R, Sood N, Puri A, Kadayaprath G. Comparative study to assess the quality of analgesia of bupivacaine and bupivacaine with dexmedetomidine in ultrasound-guided pectoral nerve block type I and II in breast surgeries. J Anaesthesiol Clin Pharmacol. 2018;34(2):227–31. https://doi.org/10.4103/joacp.JOACP_366_16.
Noviasky J, Pierce DP, Whalen K, Guharoy R, Hildreth K. Bupivacaine liposomal versus bupivacaine: comparative review. Hosp Pharm. 2014;49(6):539–43. https://doi.org/10.1310/hpj4906-539.
Edlund MJ, Martin BC, Russo JE, DeVries A, Braden JB, Sullivan MD. The role of opioid prescription in incident opioid abuse and dependence among individuals with chronic noncancer pain: the role of opioid prescription. Clin J Pain. 2014;30(7):557–64. https://doi.org/10.1097/AJP.0000000000000021.
Wilkoff BL, Fauchier L, Stiles MK, Morillo CA, Al-Khatib SM, Almendral J, et al. 2015 HRS/EHRA/APHRS/SOLAECE expert consensus statement on optimal implantable cardioverter-defibrillator programming and testing. Heart Rhythm. 2016;13(2):e50–86. https://doi.org/10.1016/j.hrthm.2015.11.018.
Knops RE, Brouwer TF, Barr CS, Theuns DA, Boersma L, Weiss R, et al. The learning curve associated with the introduction of the subcutaneous implantable defibrillator. Europace. 2016;18(7):1010–5. https://doi.org/10.1093/europace/euv299.
Funding
Boston Scientific Corporation (Natick, MA, USA) funded the study. The funding source did not have any involvement in the study design, in the collection, analysis and interpretation of data, in the writing of the report, or in the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
Conceptualization: Toshimasa Okabe, Emile G. Daoud, and Michael K Essandoh
Methodology: Toshimasa Okabe, Emile G. Daoud, and Michael K Essandoh
Data collection: Toshimasa Okabe, Adrianne Miller, Tanner Koppert, Rafael Cavalcanti, Diego Alcivar-Franco, Jemina Osei, and Omar Kahaly
Formal analysis and investigation: Toshimasa Okabe, Emile G. Daoud, Michael K Essandoh, and Muhammad R. Afzal
Writing - original draft preparation: Toshimasa Okabe, Emile G. Daoud.
Writing - review and editing: Muhammad R. Afzal, Jaret Tyler, Mahmoud Houmsse, Steven J. Kalbfleisch, Raul WeissJohn D. Hummel, Ralph S. Augostini, Sujatha Bhandary, Galina Dimitrova, Kasey Fiorini Hamdy Elsayed-Awad, Antolin Flores, MD#, Leonid Gorelik, Manoj H. Iyer, Samiya Saklayen, Erica Stein, Katja Turner, William Perez
Funding acquisition: Emile G. Daoud
Supervision: Emile G. Daoud, Michael K Essandoh, Michael J. Andritsos
Corresponding author
Ethics declarations
Conflict of interest
Drs Weiss and Essandoh have received consulting fees and speaking fees from Boston Scientific. The remaining authors have no conflicts to disclose.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Okabe, T., Miller, A., Koppert, T. et al. Feasibility and safety of same day subcutaneous defibrillator implantation and send home (DASH) strategy. J Interv Card Electrophysiol 57, 311–318 (2020). https://doi.org/10.1007/s10840-019-00673-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-019-00673-1