Abstract
Purpose
The aim was to elucidate if the nuclear size and number are indicative of aberrant chromosome content in human blastomeres and embryos.
Methods
The number of nuclei and the nucleus and blastomere size were measured by a computer controlled system for multilevel analysis. Then the nuclei were enumerated for 13 chromosomes by a combination of PNA and DNA probes.
Results
In the mononucleated embryos there was no difference in the mean size of chromosomally normal and abnormal nuclei but a significant difference in the mean nuclei size of nuclei that had gained chromosomes compared to nuclei that had lost chromosomes. The nuclei from multinucleated blastomeres had a significant smaller mean size and the frequency of chromosomally aberrant blastomeres was significantly higher.
Conclusion
The mean nuclear size is not a marker for the chromosome content in mononucleated embryos. However, it seems that the nuclei size can be related to multinucleation and maybe to the chromosome content.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Significant proportions of human embryos do not reach the blastocyst stage or implant after transfer. One possible cause of this early developmental arrest could be high incidence of nuclear and chromosomal abnormalities observed in embryos at these stages [1, 2].
A common nuclear abnormality observed at early cleavage stages is the presence of binucleated blastomeres often caused by failure of cytokinesis [3]. Other abnormalities include multi- or micronucleated blastomeres [4, 5]. Bi- and multinucleated blastomeres in general are more frequent in embryos with poor morphology [6] and quality and development [7] and are associated with lower pregnancy rates [8, 9, 10]. However, they may frequently occur in morphological good quality embryos too [3, 11].
Two studies have found the incidence of multinuclearity to vary between 14% and 33% in four-cell embryos obtained after controlled ovarian hyperstimulation [9, 12]. In addition, Hnida et al. [12] showed that multinucleate blastomeres are significantly larger than their non-multinucleated sibling blastomeres and Hardarson et al. [13] has found that embryos with uneven sized blastomeres have a higher degree of aneuploidy and multinuclearity.
Other investigations of cleavage stage embryos have indicated that aneuploidy errors could be the main cause of low implantation rate of human embryos [14, 15]. Previous studies have shown that only about 25–33% of cleavage stage embryos were chromosomally normal in all blastomeres [1, 16]. Unfortunately, the aneuploidy is not always reflected in the morphology or viability of the embryo, so additional selection criteria is needed.
In the present study we used a computer-controlled system for multilevel and non-invasive embryo morphology analysis to measure the size of nuclei and blastomeres in the individual separated blastomeres. Subsequently, the nuclei were analyzed for the composition of 13 chromosomes by the use of sequential Fluorescence In Situ Hybridization (FISH) with PNA and DNA probes (Fig. 1).
The embryo was morphological assessed. Then it was separated in individual blastomeres and the nuclei sizes were measured by computer controlled multilevel analysis. Then the individual nuclei were fixated and FISH analysis performed. The chromosome complement was then correlated to the size of each individual nucleus
The aim of the study was to characterize the blastomere and nuclei size in four-cell embryos and to evaluate the size of the nuclei and blastomeres in the separated blastomeres in relation to their nuclear and chromosomal status.
Materials and methods
Patients
The study included 35 IVF patients, who donated 35 surplus four cell-embryos. The inclusion criteria were indication for IVF or ICSI treatment and female age between 25 and 40 years. The embryos were donated 50–52 h after oocyte aspiration.
Patients were treated with the long protocol, using GnRH- agonist (Synarela®, Pharmacia, Denmark; Suprefact®, Aventis Pharma, Denmark) for down-regulation and recombinant FSH (Gonal-F®, Serono, Denmark or Puregon®, Organon, Denmark) for ovarian stimulation. HCG (Profasi®, Serono, Denmark) was given 36 h before oocyte retrieval.
IVF and ICSI-procedure
IVF and ICSI were performed according to the clinics routine procedures. Briefly, oocytes were aspirated 36 h after hCG injection and the IVF or ICSI procedure was performed 4–6 h later. On the following morning (18–20 h after insemination) the oocytes were checked for fertilization and cultured for a further 24 h. Embryo transfer was carried out 50–52 h after aspiration. Immediately prior to transfer, all the embryos were evaluated according to cleavage stage and quality score in accordance with the normal procedures at the clinic. Embryos were considered suitable for donation based on this morphology evaluation. The selection of embryos for transfer was done independently of this study and prior to embryo donation.
Embryo donation
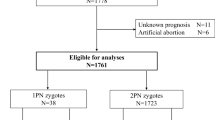
Only mono- or binucleated embryos that had developed to four-cell stage 48 h after aspiration with less than 20 percent fragmentation were included in this study. The donated embryos were surplus embryos that otherwise would have been frozen. Only patients having at least six surplus embryos were asked to donate. Informed consent was obtained from all patients before donation. In total 35 four-cell embryos was donated. One embryo had no pictures of the nuclei and was excluded before the FISH analysis. In the FISH evaluation only embryos with conclusive FISH signals in 75% or more of the blastomeres were included. Two embryos were excluded after the FISH analysis. One due to FISH failure and one due to inconclusive FISH result in two nuclei. This leaves a total of 32 embryos divided in 21 mononucleated embryos and 11 binucleated embryos.
The FISH analysis included a total of 128 blastomeres. Six blastomeres were excluded because of missing nuclei during fixation and three due to inconclusive FISH signals. Of the remaining 119 blastomeres 81 came from mononucleated embryos and 38 from binucleated embryos. The binucleated embryos comprised of 24 mononucleated blastomeres and nuclei and 14 binucleated blastomeres providing 28 nuclei.
Recording of digital images
The imaging was done as previously described by Hnida et al. [17]. In brief, the FertiMorph computer system for multilevel embryo morphology analysis (Image House Medical A/S, Copenhagen, Denmark) was used to record image sequences in the included embryos immediately after donation. Additionally, image sequences of the individual blastomeres were recorded after dissolving the zona pellucida and segregation of the blastomeres. The images from the individual blastomeres were used in this study. Each sequence consisted of 26 images of the same blastomere with the FertiMorph System automatically focusing in 5 μm intervals through the blastomere. All recordings were performed at 400 times magnification with Hoffman modulation contrast illumination.
Computer controlled morphometric analysis of the blastomeres and nuclear structures
Based on the digital image sequences, blastomere size and nuclear structures were analyzed in a semiautomatic manner using the morphology analysis software of the FertiMorph System as described in Hnida et al. [17]. In the individual blastomeres a nucleus was defined as a circular structure surrounded by a membrane and containing nuclear precursor bodies. All images of one sequence could be viewed in detail, enabling us to select the pictures where the different structures were in focus. For all blastomeres, the outer border and all visible nuclear structures were outlined.
Morphometric values describing the size of the blastomeres and nuclear structures (area, diameter and volume) were calculated automatically.
Definition of mono- and binucleated embryos
Based on the multilevel analysis, mononucleate embryos were defined as embryos having only blastomeres with no or one nuclear structure. Binucleate embryos were defined as embryos with at least one blastomere having two visible nuclear structures. The binucleated embryos included both mononucleated blastomeres and binucleated blastomeres. The nuclear status was confirmed by the fixation of the nuclei but only embryos with conclusive FISH signals in at least 75% of the blastomeres were included.
Segregation of the individual blastomeres
At 50 h (±2 h) after oocyte aspiration the embryos were transferred for about 1 min to culture medium containing pronase (5 mg/ml; Sigma, St. Louis, MO, USA) to dissolve the zona pellucida followed by incubation in Ca2+/Mg2+-free medium (EB-10; Vitrolife, Gothenburg, Sweden) for 1 to 4 min until segregation of the individual blastomeres. The individual blastomeres were transferred to separate wells containing IVF- medium (Medi-Cult, Jyllinge, Denmark).
Fixation
The nuclear structures from each blastomere were fixed separately on a silianized slide (Cat. No. S1308; Oncor, USA) in an HCL/Tween-20 solution (0.01 M/0.1%) as described in Coonen et al. [18], but using a microscope with 10 times magnification and Hoffman modulation contrast illumination. The fixed nuclear structures were located by drawing a circle around them, using a diamond objective. After fixation the slides was washed in phosphate-buffered saline (PBS) and dehydrated in a series of 70%, 90% and 99% ethanol and dried at room temperature. The slides were packed in slide boxes with silica gel, covered with paraffin and stored at −20°C until FISH analyze.
Pretreatment to FISH analysis
Before FISH analysis the slides were incubated with 0.1 mg/ml RNase (Sigma, St Louis, MO, USA) solution in 30 min at 37°C, washed in 2× sodium chloride, sodium citrat (SSC) and incubated with 0.005% pepsin for 3 min at 37°C. Post fixation was done in a formaldehyde solution for 2 min at room temperature and the slides were rinsed in PBS and dehydrated through an ethanol series.
FISH analysis
The sequential FISH analysis was performed by a combination of peptide nucleic acid (PNA) probes (Applied Biosystem, Bedford, MA, USA) including the principle of competitive displacement and DNA probes (Vysis, Abbort Park, IL, USA) as previously described by Agerholm et al. [19]. Briefly, on slides with fixed blastomere nuclei 2 μl probe mixture consisting of 20 mM Tris–HCl, pH 7.5, 70% Formamide (Invitrogen, USA), 1× Denharts solution (USB, USA), 10 mM NaCl, 100 μg/ml tRNA (Sigma), 100 μg/ml Salmon Sperm DNA (Sigma, USA), pH 7.0–7.5, and different concentrations of PNA oligomers was applied. After applying a coverslip the slide was denatured at 55°C in 4 min in the first cycle and 1 min in the following three cycles. Subsequent the slide was hybridized in 30–45 min in all cycles. Following the hybridization the coverslip was removed and the slide washed in 50% formamid/2× SCC in 2 min at 41°C and 4× SCC/Tween 20 at room temperature (RT) in 1 min. The slide was finally stained with 4′, 6 diamidino-2-phenylidole (DAPI; Vysis DAPI II antifade) and mounted with coverslip.
PNA probes
In total four FISH cycles with PNA probes were performed on each nucleus. The first FISH cycle was done by the use of PNA probes mixtures specific for chromosome 1, 16 and 17. The second FISH cycle for enumeration of chromosome 9 and 11 and included excess of unlabelled probe for chromosome 1, 16 and 17. The third FISH cycles included labeled probes for enumeration of chromosome 7 and 15 and unlabelled for chromosome 9 and 11. The last PNA FISH cycle enumerated chromosome 18, X and Y and had unlabelled probes for chromosome 15. Chromosome 7 was not available as unlabelled but no signal leftover from this probe was observed.
DNA probes
The fifth FISH cycle was done with the PB probe set from Vysis including DNA probes for enumeration of chromosome 13, 16, 18, 21 and 22.
FISH with DNA probes
The procedure for the DNA probes in the PB probe set was done according to the protocol described by Vysis but with a denaturation temperature of 69°C in 8 min and a hybridization for 4 h at 37°C with the slide covered by Para film followed by a washing step in 0.7× SSC/0.3% non-ionic detergent (NP-40) at 72°C for 7 min and in 2× SSC/0.1% NP-40 for 1 min at RT. The slide was mounted with Antifade II (Vysis, USA) and a coverslip.
Cytogenetic evaluation
The cytogenetic evaluation was done as describe by Ziebe et al. [1]. In Brief, the evaluation included classification of each blastomere as normal (diploid constitution) or abnormal (aneuploid constitution). Based on the result in the blastomeres a classification was applied to each embryo. The classification included; uniformly normal (all blastomeres had a diploid constitution); uniformly abnormal (all blastomeres had the same aneuploid constitution), overall normal (more than 50% of the blastomeres had diploid constitution) and overall abnormal (more than 50% of all the blastomeres and aneuploidy constitution). In addition, the overall normal and overall abnormal were further classified as one of the following; mosaic aneuploide (some blastomeres with a single chromosome added or deleted e.g. 2n/2n ± 1); mosaic ploidy (some blastomeres with normal chromosomal constitution in combination with a multiplied cell line, e.g. 2n/3n) or chaotic (some blastomeres with nuclei showing randomly different chromosome complement representing more than two cell lines in total). In a separate series, the aneuploid nuclei from the mononucleated embryos were also classified as hyper- or hypo-diploid depending on whether chromosomes were added or lacking. The nuclei with both added and lacking chromosomes were considered as mixed. A binucleated blastomere was regarded abnormal irrespectively if the two nuclei had a normal chromosomal constitution.
Ethical approval
Ethical approval for this study was obtained from the regional ethical committee for Copenhagen before initiation of the study.
Statistical analysis
Test for normal distribution was performed in STATA software. Comparison of means was performed by t-test in Excel (Microsoft, Redmund, WA, USA). A two-tailed test at p < 0.05 was considered significant.
Results
For chromosome content 133 nuclei from 119 blastomeres were included. Based on the 13 chromosomes envisioned, we found that 45 nuclei (34%) had normal chromosome content while 88 nuclei (66%) had abnormal chromosome content.
Chromosomal classification of mono and binucleated embryos and blastomeres
Mononucleated embryos
Four of the 21 mononucleated embryos were uniformly normal and seven were overall normal. All the overall normal embryos were mosaic aneuploid. Three embryos were uniformly abnormal and seven were overall abnormal. Of the seven overall abnormal one was mosaic aneuploid, one was mosaic ploid and five were mosaic chaotic (Table 1). In total 81 nuclei from 81 blastomeres were analyzed and 38 (47%) were chromosomally normal for the tested chromosomes.
Binucleated embryos
One of the 11 binucleated embryos included only diploid nuclei but was referred as overall normal due to the presence of a binucleated blastomere. No binucleated embryos were uniformly abnormal but 10 embryos were overall abnormal. All the overall abnormal embryos were mosaic chaotic (Table 1). In total 52 nuclei from 38 blastomeres were analyzed. Of the 52 nuclei 24 originated from mononucleated blastomeres and 28 nuclei from binucleated blastomeres. Five (21%) of the 24 nuclei from mononucleated blastomeres and 2 (7%) of the 28 nuclei from binucleated blastomeres were chromosomally normal for the tested chromosomes.
Chromosome content and mean diameter of nuclei and blastomeres in mono and binucleated embryos
Mononucleated embryos
There was no difference in the mean diameter of the chromosomally normal (18.94 ± 2.65 μm) and the chromosomally abnormal nuclei (18.05 ± 2.45 μm; p = 0.12). Neither was there any difference in the mean diameter of the blastomeres of chromosomally normal and chromosomally abnormal blastomeres (p = 0.92) or in the nuclei/cell ratio between the chromosomally normal and abnormal blastomeres (p = 0.15; Table 2).
Binucleated embryos
For the mononucleated blastomeres from binucleated embryos we found no difference between the mean diameter of the chromosomally normal nuclei (16.34 ± 2.85 μm) and the chromosomally abnormal nuclei (17.64 ± 2.67 μm, p = 0.34). No difference in the mean diameter of chromosomally normal and chromosomally abnormal blastomeres (p = 0.61) or in the nuclei/cell ratio between the chromosomally normal and abnormal blastomeres was observed (p = 0.64).
In the bi-nucleated blastomeres there were only two nuclei in one blastomere that were chromosomally normal and no difference were observed (20.25 ± 0.35 μm vs 16.21 ± 2.85 μm; p < 0.59; Table 2).
Hyper- and hypo-diploid in mononucleated embryos
The chromosomally abnormal mononucleated blastomeres from mononucleated embryos were further divided into nuclei with chromosomes added (hyper-diploid) or chromosomes missed (hypo-diploid). The mean sizes of hypo-diploid nuclei (17.72 ± 2.63 μm) were significant smaller than the hyper-diploid nuclei (19.525 ± 0.88 μm; p = 0.003; Table 3).
Mean diameter of nuclei and blastomeres in mono and binucleated embryos
Mean nuclei size
Binucleated blastomeres had significantly smaller nuclei compared to the mononucleated blastomeres from mononucleated embryos (16.5 ± 2.57 μm vs 18.47 ± 2.94 μm, p = 0.001) but were not different compared to the mean nuclei size in the mononucleated sibling blastomeres (Table 4).The mean nuclei size in mononucleated blastomeres from mononucleated and binucleated embryos were not different.
Mean blastomere size
The mean blastomere size for binucleated blastomeres was significantly larger than their non-binucleated sibling blastomeres. In addition, the binucleated blastomere mean sizes were also significantly larger than the mononucleated blastomeres from mononucleated embryos. The nuclei/cell ratio in binucleated blastomeres was significantly different from the nuclei/cell ratio from the mononucleated blastomeres from mononucleated and binucleated embryos (Table 4).
Discussion
In the present communication the number and size of the nuclei in the blastomeres are combined with in situ estimates of chromosome composition of individual nuclei using probes representing in total 13 chromosomes. The combination of these parameters was done to elucidate to what extent the nuclei size and the number of nuclei is indicative of an aberrant chromosome content of blastomeres and embryos.
In the mononucleated embryos we compared the mean size of the nuclei in the different embryo classification and found no correlation. McKenzie et al. [20] demonstrated an altered localization of chromosomes in aneuploide blastomeres. Such an altered localization could be reflected in the size of the nuclei but this was not confirmed in the present study.
However, in a separate analysis we investigated the relationship between nuclear sizes and the gain or loss of chromosomes in mononucleated but aneuploid nuclei from mononucleated embryos (Table 3). The mean size showed a significant difference with the hypo-diploid nuclei being significantly smaller than the hyper-diploid nuclei. The observed size difference in hyper- and hypo-diploid nuclei shows that the nuclei sizes do reflect the chromosome content in some abnormalities. The mean size difference in hyper- and hypo-diploid could also explain why the overall mean diameter of the aneuploid nuclei including both hyper and hypo-diploid nuclei did not differ from the mean diameter of the chromosomally normal nuclei as described above.
Our classification of mononucleated embryos as embryos with none or one nuclear structure could bias the result but due to our definition to include only embryos containing nuclei with a conclusive FISH signal in at least 75% of their blastomeres the percentage of blastomeres with no nuclei is only 5%.
In the binucleated blastomeres no difference was found in the mean nuclei size between the diploid and aneuploid nuclei. However, the nuclei from binucleated blastomeres are significantly smaller than the nuclei from mononucleated blastomeres from mononucleated embryos. It has been speculated that bi-nucleated blastomeres originate from an uncoupling of the processes controlling karyokinesis and cytokinesis, resulting in duplication of the nuclear material without a subsequent cell cleavage [3, 13, 21]. Hnida et al. [17] described that the mean size of the nuclei in mononucleated embryos decreased 15% from a two cell- to a four cell-embryo. This indicates that the nuclear size is reduced at each karyokinesis and a similar reduction could be expected from the four-cell to eight-cell stage. If binucleation in the actual generation is a result of failed cytokinesis after a normal karyokinesis [3, 22] the binucleated blastomeres should be expected to have nuclei sizes comparable with the nuclei size in the following cell generation. The consequence for binucleation arisen in the four-cell embryo would be nuclei that are smaller compared to the nuclei in the mononucleated four-cell embryo. In this study the binucleated were 11% smaller than the mononucleated nuclei from mononucleated embryos which could be the reduction expected from a four-cell to an eight-cell embryo. The actual size of the nuclei could therefore document at what cleavage stage the multinuclearity had occurred. However, other mechanisms as errors in chromosomal replication and segregation may be involved in the formation of binucleated blastomeres [5, 21].
A number of publications have documented that the number of nuclei in the blastomeres can to some extent predict the pregnancy rates [9, 23]. In the present study the number of nuclei in the blastomere is clearly associated with the presence of chromosome aberrations. In the binucleated embryos the frequency of chromosomally abnormal nuclei was significantly higher both in the binucleated and their non-binucleated sibling blastomeres. This is in concordance to Kligman et al. [6] who found that more multinucleated embryos are chromosomal abnormal than non-multinucleated. The same was demonstrated by Hardarson et al. [13] who found that 86% of embryos with multinucleation were chromosomally abnormal in >50% of their constitutive blastomeres. We observed that 47% of the blastomeres from mononucleated embryos were diploid compared to only 15% of the blastomeres from binucleated embryos. This means that the abnormalities at the chromosomal level are not limited to the binucleated blastomere but are observed in the embryos in general.
The presence of binucleated blastomeres in an embryo does therefore indicate an increased risk of chromosome aberrations in the mononucleated blastomeres as well.
The fact that binucleated blastomeres are significantly larger than the mononucleated blastomeres from mononucleated embryos and significantly larger than their non-binucleated sibling blastomeres indicates that unevenness in the blastomere size can be linked to multinucleation. This is in concordance to Hardarson et al. [13] who described that embryos with uneven blastomere size were correlated with aneuploidy and multinucleation.
In conclusion, the nuclei diameter from mononucleated four cell embryos is not indicative for the chromosomal status of the nuclei. However, the significant difference between the hyper-diploid and hypo-diploid nuclei size indicate that the nuclei size do reflect the chromosome content in subgroups. In addition, the binucleated embryos are chromosomally abnormal both in the binucleated and mononucleated blastomeres and the nuclei size in the bi-nucleated blastomeres seems to be predictive for the generation of the blastomere when the multinucleation occurs.
References
Ziebe S, Lundin K, Loft A, Bergh C, Nyboe Andersen AN, Selleskog U, et al. FISH analysis for chromosomes 13, 16, 18, 21, 22, X and Y in all blastomeres of IVF pre-embryos from 144 randomly selected donated human oocytes and impact on pre-embryo morphology. Hum Reprod. 2003;18:2575–81.
Kats-Jaffe MG, Trounson AO, Cram DS. Mitotic errors in chromosome 21 of human preimplantation embryos are associated with non-viability. Mol Hum Reprod. 2004;10:143–7.
Hardy K, Winston RM, Handyside AH. Binucleate blastomeres in preimplantation human embryos in vitro; failure if cytokinesis during early cleavage. Fertil Steril. 1993;70:60–6.
De Scisciolo C, Wright DL, Mayer JF, Gibbons W, Muasher AJ, Lanzendorf SE. Human embryo derived from in vitro and in vivo matured oocytes: analysis for chromosomal abnormalities and nuclear morphology. J Ass Reprod Gen. 2000;17:284–92.
Meriano J, Clark C, Cadesky K, Laskin C. Binucleated and micronucleated blastomeres ind embryos derived from human assisted reproduction cycles. Reprod BioMed Online. 2004;9:511–20.
Kligman I, Bendiva C, Alikani M, Munne S. The presence of multinucleated blastomeres in human embryos is correlated with chromosomal abnormalities. Hum Reprod. 1996;11:1492–8.
Yakin K. Impact of the presence of one or more multinucleated blastomeres on the developmental potential of the embryo to the blastocyst stage. Fertil Steril. 2005;83:243–5.
Jackson KV, Ginsburg ES, Hornstein MD, Rein MS, Clark RN. Multinucleation in normally fertilized embryos is associated with an accelerated ovulation induction response and lower implantation and pregnancy rates in in vitro fertilization-embryo transfer cycles. Fertil Steril. 1998;70:60–6.
Van Royen E, Mangelschots K, Vercruyssen M, De Neubourg D, Valken burg M, Rychart G, Gerris J. Multinucleation in cleavage stage embryos. Hum Reprod. 2003;18:1062–9.
Moriwaki T, Suganuma N, Hayakawa M, Hibi H, Katsunata Y, Ogushi H, et al. Embryo evaluation by analysing blastomeres nuclei. Hum Reprod. 2004;19:152–6.
Munne S, Cohen J. Unsuitability of multinucleated human blastomeres for preimplantation genetic diagnosis. Hum Reprod. 1993;8:1120–5.
Hnida C, Engenheiro E, Ziebe S. Computer-controlled, multilevel, morphometric analysis of blastomere size as biomarker of fragmentation and multinuclearity in human embryos. Hum Reprod. 2004;19:288–93.
Hardarson T, Hanson C, Sjogren A, Lundin K. Human embryos with uneven sized blastomeres have lower pregnancy and implantation rates: indication for aneuploidy and multinucleation. Hum Reprod. 2001;16:313–8.
Munne S. Preimplantation genetic diagnosis and human implantation. A review. Placenta 2003;24:1–7.
Delhanty JD. Preimplantation genetics: an explanation for poor human fertility? Ann Hum Genet. 2001;65:331–8.
Wells D, Delhanty JD. Comprehensive chromosomal analysis of human preimplantation embryos using whole genome amplification and single cell comparative genomic hybridization. Mol Hum Reprod. 2000;6:1055–62.
Hnida C, Agerholm I, Ziebe S. Traditional detection versus computer-controlled multilevel analysis of nuclear structures from donated human embryos. Hum Reprod. 2005;20:665–71.
Coonen E, Dumoulin CM, Ramaekers FCS, Hopman AHN. Optimal preparation of preimplantation embryo interphase nuclei for analysis by fluorescence in-situ hybridization. Human Reprod. 1994;9:533–7.
Agerholm I, Ziebe S, Williams B, Berg C, Crüger DG, Bruun-Petersen G, et al. Sequential FISH analysis using competitive displacement of labelled peptide nucleic acid probes for eight chromosomes in human blastomeres. Hum Reprod. 2005;20:1072–7.
McKenzie LJ, Carson SA, Marcelli S, Rooney E, Cisneros P, Torsky S, et al. Nuclear chromosomal localization in human preimplantation embryos: correlation with aneuploidy and embryos morphology. Hum Reprod. 2004;19:2231–7.
Pickering SJ, Taylor A, Johnsom MH, Braude PR. An analysis of multinuclear blastomeres and their derivative daughter blastomeres. Hum Reprod. 1995;10:1912–22.
Delimetreva SM, Zhivkova RS, Vatev ITS, Toncheva DI. Chromosomal disorders and nuclear and cell destruction in cleaving human embryos. Int J Dev Biol. 2005;49:409–16.
Saldeen P, Sundstrom P. Nuclear status of for cell preembryos predicts implantation potential in in vitro fertilization treatment cycles. Fertil Steril. 2005;84:584–9.
Acknowledgments
This work has been supported by Danish Medical Council and Vejle Council.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agerholm, I.E., Hnida, C., Crüger, D.G. et al. Nuclei size in relation to nuclear status and aneuploidy rate for 13 chromosomes in donated four cells embryos. J Assist Reprod Genet 25, 95–102 (2008). https://doi.org/10.1007/s10815-008-9199-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-008-9199-0