Abstract
We used samples from rheumatoid arthritis (RA) patients to examine whether Anti-citrullinated protein antibodies (ACPAs) alter macrophage subset distribution and promote RA development. Macrophage subset distributions and interferon regulatory factor 4 (IRF4) and IRF5 expressions were analyzed. ACPAs were purified by affinity column. After RA and osteoarthritis (OA) patients’ macrophages were cocultured with ACPAs, macrophage subsets and IRF4 and IRF5 expressions were measured. Small interfering RNAs (siRNAs) were transfected into ACPA-activated cells to suppress IRF4 or IRF5. Fluorescence-activated cell sorting (FACS), Western blot, and immunohistochemistry were performed. Macrophage subset disequilibrium occurred in RA patient synovial fluids. IRF4 and IRF5 were all expressed in the synovial fluid and synovium. ACPAs (40 IU/ml) could induce macrophages to polarize to M1 subsets, and the percentage of increased M1/M2 ratio of RA patients was higher than that of the OA patients. ACPAs also induce IRF4 and IRF5 protein expressions. IRF5 siRNA transfection impaired ACPA activity significantly. We demonstrated that macrophage subset disequilibrium occurred in RA patients. ACPAs induced IRF5 activity and led to M1 macrophage polarization.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Rheumatoid arthritis (RA) is a chronic immune-mediated disease marked by inflammation in joint linings (i.e., the synovium) and cartilage and bone destruction. Anti-citrullinated protein antibodies (ACPAs) are highly specific for RA and a powerful tool for its diagnosis and predicting disease severity [1]. These autoantibodies can be detected several years before clinical symptom onset, with titers increasing as disease onset approaches [2–4]. Citrullination is a posttranslational modification of proteins in which a peptidyl arginine is converted into the nonstandard amino acid peptidyl citrulline. The reaction is catalyzed by calcium-dependent peptidyl arginine deiminase (PAD). Five PADs have been identified in humans, and PAD-2 and PAD-4 are those found in rheumatoid synovial fluid cells [5] and in synovial membranes [6]. Citrullinated proteins have been detected in the synovial membranes and synovial fluid of patients with various forms of arthritis [7, 8], suggesting that citrullination is associated with inflammation in general.
Studies revealed that protein citrullination was involved in immune tolerance breakdown in experimental autoimmune arthritis [9]. Additionally, ACPAs are strongly associated with increased risk of healthy individuals developing RA. Among those with RA, their presence is associated with more severe structural damage, radiographic progression, and poorer response to therapy [10, 11]. Clavel et al. [12] demonstrated that immune complexes containing IgG ACPA (ACPA-IC) induce FcγR-mediated TNF-α secretion in macrophages. Lu et al. [13, 14] demonstrated that ACPAs could selectively activate extracellular signal-regulated protein kinases 1 and 2 (ERK1/2) and c-Jun N-terminal kinase (JNK) signaling pathways to enhance IκB kinase alpha (IKKα) phosphorylation, which leads to nuclear factor kappaB (NF-κB) activation and TNF-α production from monocytes/macrophages via binding to surface-expressed citrullinated glucose-regulated protein 78 (cit-GRP78).
RA pathogenesis is complex and includes many cell types, including T cells, B cells, and macrophages. Macrophages are of central importance in RA due to their prominent numbers in the inflamed synovial membrane and at the cartilage–pannus junction. Macrophages display a highly activated phenotype and produce a panoply of pro-inflammatory cytokines, chemokines, and growth factors [15]. One key feature of macrophages is their functional diversity. Depending on the microenvironment, macrophages are polarized into functionally distinct forms: classically activated (M1) macrophages and alternatively activated (M2) macrophages. M1 macrophages are engaged in inflammatory, microbicidal, and tumoricidal activities. By contrast, M2 macrophages dampen inflammation and promote tissue remodeling and repair [16]. Macrophage polarization is plastic, and M1 and M2 cell disequilibrium correlates with the disease [17]. However, the relationship between macrophage imbalances and RA pathogenesis is poorly understood. Based on these observations, we hypothesized that ACPAs may activate macrophages, alter macrophage subtype distribution, and correlate with RA development. In this study, we demonstrated that ACPAs activated interferon regulatory factor 5 (IRF5) and induced macrophages to polarize to M1 subtypes.
MATERIALS AND METHODS
Patients
Thirty-nine RA patients fulfilling the American College of Rheumatology criteria for RA [18] were involved in this study, including 32 women and 7 men. Patients were evaluated for tender and swollen joint counts, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), visual analog scale (VAS), and a disease activity score of 28 joints (DAS28) (mean DAS28 4.3 ± 1.4). The clinical and serological features, such as rheumatoid factor (RF) and anti-cyclic citrullinated peptide antibody (ACPA), were also recorded. In this study, 35 patients with osteoarthritis (OA) (28 women and 7 men) were studied as controls. The study protocol was approved by the Institutional Ethics Committee. All patients gave written informed consent to the study protocol.
For synovial fluid macrophage isolation, synovial fluid was cultured in a 12-well culture plate for 3 h, adherent cells were washed with PBS, resuspended, and then adjusted to 1 × 106/ml in Dulbecco’s modified Eagle’s medium (DMEM).
ACPA Purification from ACPA-Positive RA Sera
Serum samples with high ACPA titers (>200 IU/ml) were obtained from RA patients and pooled. The APCA activity of these serum samples was detected with a commercially available enzyme-linked immunosorbent assay (ELISA) kit (Pharmacia Diagnostics). We used a first-generation synthetic cyclic citrullinated peptide (CCP) antigen (QiangYao Co.) in the clinical test designed by Schellekens et al. [19] to show amino acid sequence HQCHQESTXGRSRGRCGRSGS (X designates citrulline, and C represents the chemical bond between two cysteines). The synthetic peptide was conjugated to normal human serum-activated HP column (GE Healthcare Life Sciences) according to the manufacturer’s instructions and then packed as a CCP affinity column. The pooled ACPA-containing RA sera were incubated with the CCP affinity column overnight at 4 °C. The column was washed with 0.02 M sodium phosphate, pH 7.0, and the unbounded fraction was collected. The bound ACPAs were washing with 0.05 M glycine-HCl, pH 3.0; the effluent was immediately neutralized with 1:10 volume of 1 M Tris buffer (pH 8.0) and concentrated through a Vivaspin 20 polyethersulfone 30,000 MWCO membrane (Sartorious). The citrullinated peptide-binding activity of the affinity-purified human ACPAs was measured with ELISA kits (Pharmacia Diagnostics). The endotoxin levels in purified ACPAs were confirmed to be <0.5 EU/ml with the limulus amebocyte lysate assay (Lonza).
Macrophages Cultured with Purified ACPAs
RA and OA patients’ peripheral blood mononuclear cells (PBMCs) were isolated from freshly drawn anti-coagulated blood using 1.077 g/ml Ficoll–Hypaque gradient centrifugation (2000 rpm for 20 min). The isolated PBMCs were cultured for 6 h and then discarded the nonadherent cell. To induce macrophages, the adherent cells were cultured with phorbol 12-myristate 13-acetate (PMA) (50 ng/ml) for 48 h, and then, the macrophages were cultured with or without purified ACPAs (40 IU/ml) for 48 h. After being cultured with ACPAs, the macrophages were harvested for assay. The following formula was used to analyze the fluorescence-activated cell sorting (FACS) results:
Flow Cytometry
Standard FACS analysis was performed to evaluate macrophage subsets. ACPA-induced macrophages or synovial fluid macrophages were stained and incubated at 4 °C for 30 min with Percp-cy5.5-conjugated anti-CD68 (BD Biosciences), which are human macrophage-specific markers. APC-conjugated anti-HLA-DR (BD Biosciences) and PE-conjugated anti-CD163 (BD Biosciences) were used to discriminate M1 and M2 macrophage populations. CD68+HLA-DR+ cells were identified as M1 macrophages and CD68+CD163+ cells as M2 macrophages.
Western Blot
Equal amounts of protein were resolved by 10 % SDS-PAGE and transformed onto a PVDF membrane. The membrane was blocked with 5 % nonfat dried milk and incubated with antibody specific for IRF4, IRF5, and Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) overnight at 4 °C. After washing with TBST, the membranes were incubated with horseradish peroxidase-linked secondary antibody. The proteins were visualized using ECL chemiluminescence and exposed to X-ray film. Bands were quantified with images. Protein expressions were determined by densitometry analysis of the target protein normalized to GAPDH.
Immunohistochemistry
Frozen synovium sections were stained with mouse anti-human IRF4 or IRF5 followed by a horseradish peroxidase-labeled anti-mouse secondary antibody and a 3,30-diaminobenzidine (DAB) substrate to detect IRF4 and IRF5 expressions. Section areas and positive cells were measured from digital images using IMAGE PRO PLUS software (Media Cybernetics, Silver Springs, MD). The results were averaged and expressed as integrated optical density (IOD)/positive cell.
IRF4 or IRF5 Suppression with siRNA
IRF4siRNAs or IRF5siRNAs were transfected into macrophages according to the manufacturer’s instructions (GenePharma). Briefly, adherent cells from RA patients’ PBMCs were cultured with PMA (50 ng/ml) for 48 h, and IRF4siRNAs or IRF5siRNAs were transfected into macrophages using transfection reagents (Gene Pharma). Six hours later, the transfection reagents were removed and macrophages cultured with ACPA (40 IU/ml). After 48 h, cells were harvested for FACS and Western blot assay. FACS was used to detect transfection efficiency and macrophage distribution. Western blot was used to determine if IRF4 or IRF5 protein expressions were inhibited. Protein expressions were determined by densitometry analysis of the target protein normalized to GAPDH. The following formula was used to analyze the FACS results:
Statistical Analysis
All statistical analyses were performed with SPSS 17.0 software (IBM, USA). Data are expressed as the means ± SD. Statistical significance was determined using the independent samples t test, and P < 0.05 was considered statistically significant.
RESULTS
Macrophage Subset Disequilibrium in Synovial Fluid
FACS was used to discriminate macrophage subsets in synovial fluid. To keep the same conditions, synovial fluid cells were not cultured with DMEM in vitro. Synovial fluids were only cultured 3 h to separate macrophages from other cells. As shown in Fig. 1, the M1/M2 macrophage ratio was 32.76 ± 11.02 in RA patients, while only 9.01 ± 5.35 in OA patients. The results show macrophage subset disequilibrium occurred in RA patient synovial fluids.
The macrophage subtype distribution in RA patient synovial fluid. Twelve synovial fluids from RA patients and nine synovial fluids from OA patients were analyzed independently by FACS. a The gate is CD68+ cell. b The CD68-positive cell. Bar graphs summarize the data. ***P < 0.001, versus OA patients. n = 12 (RA), n = 9 (OA).
IRF4 and IRF5 Overexpress in Synovial Fluid Cells
IRFs were originally described as type I IFN expression and signaling regulators. However, it is now well established that they have additional important functions, including regulating macrophages and DC ontogeny [20]. IRF5 is a crucial transcription factor in a number of immune and homeostatic processes. IRF5 activation downstream of Toll-like receptors (TLRs) and RIG-I-like RNA helicases, involving IRAK and IKK. IKKβ phosphorylated IRF5 at Ser462 and induced the dimerization of wild-type IRF5. IRF5−/− mice are resistant to lethal endotoxin-induced shock and show diminished production of pro-inflammatory mediators such as TNF-α, IL-6, and IL-12 in response to in vitro stimulation of macrophages with TLR agonists, and IRF5−/− macrophages are polarized to an anti-inflammatory M2 phenotype. IRF5 has the dual function of activating M1 genes while repressing M2 genes by binding to similar cis-acting elements in gene promoters [21, 22]. Macrophage M2 phenotype is promoted by several transcription factors, including STAT3, STAT6, IRF4, PPARγ, and KLF-4. IRF4 specifically regulates M2 macrophage polarization in response to parasites or the fungal cell wall component chitin. This pathway involves the histone demethylase JMJD3, which functions by removing an inhibitory histone modification, H3K27me [23]. In this study, IRF4 and IRF5 protein expressions were detected in synovial fluids. As shown in Fig. 2, IRF4 and IRF5 were expressed in synovial fluid, but IRF4 and IRF5 levels were higher in RA patients than in OA patients (P < 0.01). Although IRF5 protein expressions were higher than IRF4 protein expressions in RA patients, the difference was not significant.
IRF4 and IRF5 protein expression detected by Western blotting in RA patient synovial fluid. Protein expressions were determined by densitometry analysis of the target protein normalized to GAPDH. a IRF4 protein expression. Bar graphs summarize the data. b IRF5 protein expression. Bar graphs summarize the data. **P < 0.01, versus OA patients. n = 9 (RA), n = 6 (OA).
Increased IRF5 Expression in RA Patient Synovium Tissues
The synovium from RA and OA patients were processed as indicated in the MATERIALS AND METHODS section to detect IRF4 and IRF5 by immunohistochemistry. IRF5 expression in RA patients’ synovium (21.10 ± 3.51 IOD/positive cell) versus OA patients’ (13.88 ± 1.99 IOD/positive cell) was significantly increased (Fig. 3, P < 0.01). IRF4 expressions in synovium were lower than IRF5 expressions, but the difference between RA and OA was not significant (Fig. 3).
IRF4 and IRF5 expression analyzed by immunohistochemistry in RA patient synovium. Protein expressions were measured from digital images using IMAGE PRO PLUS software. The results were averaged and expressed as IOD/positive cell. a IRF4 protein expression. Arrows show the positive cell. Bar graphs summarize the data. b IRF5 protein expression. Arrows show the positive cell. Bar graphs summarize the data. **P < 0.01, versus OA patients. n = 6.
ACPAs Altered Macrophage Subtype Distributions in RA Patients
To determine whether ACPAs correlate with macrophage subset imbalances in RA patients, ACPAs were purified from RA sera by CCP affinity columns, then cultured with macrophages from RA and OA patients in vitro. As shown in Fig. 4, ACPAs (40 IU/ml) could induce macrophages to polarize to M1 subsets. After culturing with ACPAs, the M1/M2 ratio increased 61.03 ± 15.90 % in OA patients, while it increased 158.62 ± 26.91 % in RA patients.
ACPAs altered the macrophage subtype distribution in RA patients. Adherent cells from RA and OA patients’ PBMCs were cultured with PMA to induce macrophage, and then, the macrophages were untreated or treated with purified ACPAs (40 IU/ml) for 48 h. Macrophages from OA patients were studied as controls. a The gate is CD68+ cell. b The CD68-positive cell. Bar graphs summarize the data. NEG cells were untreated with ACPAs. ***P < 0.001, versus OA patients. n = 10.
ACPAs Promote IRF4 and IRF5 Expressions in RA Patients
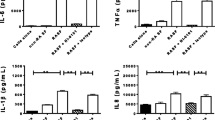
Since IRF4 and IRF5 were overexpressed in synovial fluid cells, we next detected whether ACPAs induce macrophages to polarize to M1 subsets through IRF signaling pathways. As shown in Fig. 5, ACPAs significantly promote IRF4 and IRF5 expression in macrophages. Without ACPAs, IRF4 and IRF5 relative expressions were 0.006 ± 0.0007 and 0.007 ± 0.0009, respectively. Adding ACPAs, IRF4 and IRF5 relative protein expressions increased to 0.084 ± 0.008 and 0.155 ± 0.013 in RA patients, respectively (P < 0.01).
ACPAs upregulated IRF4 and IRF5 protein expression in RA patients. Adherent cells from RA and OA patients’ PBMCs were cultured with PMA to induce macrophage, and then, the macrophages were untreated or treated with purified ACPAs (40 IU/ml) for 48 h. Macrophages from OA patients were studied as controls. a IRF4 protein expression. Bar graphs summarize the data. b IRF5 protein expression. Bar graphs summarize the data. NEG cells were untreated with ACPAs. ***P < 0.001, versus NEG. n = 6.
IRF5 Correlates with ACPA-Induced Macrophage Subset Disequilibrium in RA
To confirm that IRFs are involved in the ACPA-induced macrophage subset disequilibrium in RA, IRF4siRNAs or IRF5siRNAs were transfected into macrophages from RA patients. FACS results show that 45 % of macrophages were transfected with IRF4siRNA or IRF5siRNA. As shown in Fig. 6, IRF4siRNA or IRF5siRNA transfection reduced ACPA-induced IRF4 or IRF5 protein expression in macrophages, and IRF5siRNA transfection reduced ACPA-induced the increased M1/M2 ratio significantly (P < 0.001). ACPAs alone, the percentage of M1/M2 ratio was increased 161.01 ± 15.35 %, whereas transfected with IRF5siRNA, the percentage of M1/M2 ratio was only increased 54.97 ± 7.80 %. Although, transfected with IRF4siRNAs also influence ACPA function, but the effect of IRF4 was lower than that of IRF5, the percentage of M1/M2 ratio was increased 132.12 ± 13.12 %.
IRF4siRNA or IRF5siRNA transfection altered ACPA-induced macrophage subtypes distribution in RA patients. Adherent cells from RA patients’ PBMCs were cultured with PMA to induce macrophage, and then, IRF4siRNAs or IRF5siRNAs were transfected into macrophages. Six hours later, the transfection reagents were removed and macrophages cultured with ACPA (40 IU/ml) for 48 h. a IRF4 protein expression. Bar graphs summarize the data. b IRF5 protein expression. Bar graphs summarize the data. ***P < 0.001, versus ACPAs + siRNA. n = 4. c The gate is CD68+ cell. d The CD68-positive cells. Bar graphs summarize the data. NEG cells were untreated with ACPAs or/and siRNA. *P < 0.05, ***P < 0.001, versus ACPAs. n = 4.
DISCUSSION
Rheumatoid arthritis is characterized by synovial hyperplasia and inflammation, with increased numbers of macrophages, fibroblasts, and lymphocytes in the synovium. Evidence indicates that CD4+T cell-mediated autoimmune responses, especially Th cell imbalances, play a critical role in RA pathogenesis [24, 25]. The earliest attempts to delete CD4 + T cells in RA treatments were disappointing [26]. Macrophages are of central importance in to RA pathogenesis, and disease severity correlates with the number of activated macrophages in the inflamed tissues and in circulation [27]. Li et al. [28] demonstrated that anti-human DR5 antibody TRA-8 specifically eliminates inflammatory macrophages, leading to the IL-23/Th17 axis and Tregs rebalance and arthritis resolution in a mouse arthritis model. Macrophages are characterized by considerable diversity and plasticity. Depending on the microenvironment, macrophages are polarized into functionally distinct forms: M1 macrophages which are engaged in inflammation and M2 macrophages which dampen inflammation. M1 and M2 cell disequilibrium was associated with colitis development [17]. This study demonstrates that macrophage imbalances occur in RA patients’ synovial fluid cells, and the M1/M2 macrophage ratio was 32.76 ± 11.02 in RA patients.
IRFs were originally described as type I IFN expressions and signaling regulators. Recent studies show that IRFs were involved in RA pathogenesis. IRF4 has emerged as a crucial controller of both IL-17 and IL-21 production in RA. Satoh et al. [21] demonstrated that IRF4 specifically regulates M2 macrophage polarization, while Krausgruber et al. [22] detected that IRF5 promotes inflammatory macrophage polarization and TH1–TH17 responses. Weiss et al. [29] also demonstrated that IRF5 is highly expressed in pro-inflammatory macrophages and should be utilized as a reliable marker for macrophages at inflammation sites. In this study, consistent with macrophage subset ratio FACS results in synovial fluid, IRF5 protein expressions were higher than IRF4 protein expressions in synovial fluid and synovium.
ACPAs are strongly associated with an increased risk of developing RA in healthy individuals and are detectable in healthy persons’ blood prior to clinical RA. Geneticists and epidemiologists hold ACPA-positive RA to be a homogeneous phenotype of severe RA. ACPA is strongly associated with the HLA-DRB1-shared epitope [30] and PTPN22 [31], strong genetic risk factors for RA. However, ACPAs’ roles in RA pathogenesis are poorly understood. Lu et al. [13, 14] demonstrated that ACPAs could bound to surface-expressed citrullinated Grp78 protein on monocyte/macrophages and selectively activate ERK1/2 and JNK signaling pathways, which leads to NF-κB activation and TNF-α production. Yoo et al. [32] demonstrated that RA synoviocytes expressed higher levels of GRP78 than OA synoviocytes. Downregulation of Grp78 transcripts increased the apoptosis of RA synoviocytes while abolishing TNF- or TGF-β-induced synoviocyte proliferation. Our research detected that macrophage subset imbalances occur in synovial fluid. We hypothesized that ACPAs may activate macrophages and polarize to M1 macrophages. ACPAs was purified from RA sera through an affinity columnand cultured with M-CSF-induced macrophages that were derived from RA and OA patients’ PBMCs. To investigate the effect of ACPAs on RA, macrophages from OA patients were also studied as controls. After culturing with ACPAs, the M1/M2 ratio increased 61.03 ± 15.90 % in OA patients, while it increased 158.62 ± 26.91 % in RA patients. We demonstrated that ACPAs could induce IRF4 and IRF5 protein expressions and lead macrophages to polarize to M1 subsets. Recent studies show that IRF4 regulates M2 macrophage polarization [21], while IRF5 regulates M1 macrophage polarization and represses anti-inflammatory cytokine transcription [22, 23]. In this study, ACPAs enhanced IRF4 protein expression but did not lead to M2 macrophage polarization. We deduced that repression of IRF5 function may be associated with it.
To confirm that IRFs were involved in ACPAs-induced macrophage polarization, IRF4siRNAs or IRF5siRNAs were transfected into macrophages and cultured with ACPAs. FACS results show that IRF5siRNA transfection reduced ACPAs-induced M1 macrophage polarization significantly. With ACPA alone, the M1/M2 ratio percentage increased to 161.01 ± 15.35 %. After IRF5siRNA transfection, the M1/M2 ratio percentage only increased to 54.97 ± 7.80 %. IRF4siRNA transfection also influenced ACPA function, but IRF4 effects were lower than those of IRF5. This demonstrated that IRF5 regulates M1 macrophage polarization in RA patients.
In summary, this study demonstrates that macrophage subset disequilibrium occurred in RA patients. ACPAs induce IRF5 activity and lead to M1 macrophage polarization.
REFERENCES
van Venrooij, W.J., J.J. van Beers, and G.J. Pruijn. 2008. Anti-CCP antibody, a marker for the early detection of rheumatoid arthritis. Annals of the New York Academy of Sciences 1143: 268–285.
Nielen, M.M., D. van Schaardenburg, H.W. Reesink, R.J. van de Stadt, I.E. van der Horst-Bruinsma, M.H. de Koning, et al. 2004. Specific autoantibodies precede the symptoms of rheumatoid arthritis: a study of serial measurements in blood donors. Arthritis and Rheumatism 50: 380–386.
Rantapaa-Dahlqvist, S., B.A. de Jong, E. Berglin, G. Hallmans, G. Wadell, H. Stenlund, et al. 2003. Antibodies against cyclic citrullinated peptide and IgA rheumatoid factor predict the development of rheumatoid arthritis. Arthritis and Rheumatism 48: 2741–2749.
Chibnik, L.B., L.A. Mandl, K.H. Costenbader, P.H. Schur, and E.W. Karlson. 2009. Comparison of threshold cutpoints and continuous measures of anti-cyclic citrullinated peptide antibodies in predicting future rheumatoid arthritis. Journal of Rheumatology 36: 706–711.
Vossenaar, E.R., T.R. Radstake, A. van der Heijden, M.A. van Mansum, C. Dieteren, D.J. de Rooij, et al. 2004. Expression and activity of citrullinating peptidylarginine deiminase enzymes in monocytes and macrophages. Annals of the Rheumatic Diseases 63: 373–381.
De Rycke, L., A.P. Nicholas, T. Cantaert, E. Kruithof, J.D. Echols, B. Vandekerckhove, et al. 2005. Synovial intracellular citrullinated proteins colocalizing with peptidyl arginine deiminase as pathophysiologically relevant antigenic determinants of rheumatoid arthritis-specific humoral autoimmunity. Arthritis and Rheumatism 52: 2323–2330.
Chapuy-Regaud, S., M. Sebbag, D. Baeten, C. Clavel, C. Foulquier, F. De Keyser, et al. 2005. Fibrin deimination in synovial tissue is not specific for rheumatoid arthritis but commonly occurs during synovitides. Journal of Immunology 174: 5057–5064.
Kinloch, A., K. Lundberg, R. Wait, N. Wegner, N.H. Lim, A.J. Zendman, et al. 2008. Synovial fluid is a site of citrullination of autoantigens in inflammatory arthritis. Arthritis and Rheumatism 58: 2287–2295.
Kuhn, K.A., L. Kulik, B. Tomooka, K.J. Braschler, W.P. Arend, W.H. Robinson, et al. 2006. Antibodies against citrullinated proteins enhance tissue injury in experimental autoimmune arthritis. Journal of Clinical Investigation 116: 961–973.
Berglin, E., T. Johansson, U. Sundin, E. Jidell, G. Wadell, G. Hallmans, et al. 2006. Radiological outcome in rheumatoid arthritis is predicted by presence of antibodies against cyclic citrullinated peptide before and at disease onset, and by IgA-RF at disease onset. Annals of the Rheumatic Diseases 65: 453–458.
del Val del Amo, N., R. Ibanez Bosch, C. Fito Manteca, R. Gutierrez Polo, and E. Loza Cortina. 2006. Anti-cyclic citrullinated peptide antibody in rheumatoid arthritis: relation with disease aggressiveness. Clinical and Experimental Rheumatology 24: 281–286.
Clavel, C., L. Nogueira, L. Laurent, C. Iobagiu, C. Vincent, M. Sebbag, et al. 2008. Induction of macrophage secretion of tumor necrosis factor alpha through Fcgamma receptor IIa engagement by rheumatoid arthritis-specific autoantibodies to citrullinated proteins complexed with fibrinogen. Arthritis and Rheumatism 58: 678–688.
Lu, M.C., N.S. Lai, H.C. Yu, H.B. Huang, S.C. Hsieh, and C.L. Yu. 2010. Anti-citrullinated protein antibodies bind surface-expressed citrullinated Grp78 on monocyte/macrophages and stimulate tumor necrosis factor alpha production. Arthritis and Rheumatism 62: 1213–1223.
Lu, M.C., N.S. Lai, W.Y. Yin, H.C. Yu, H.B. Huang, C.H. Tung, et al. 2013. Anti-citrullinated protein antibodies activated ERK1/2 and JNK mitogen-activated protein kinases via binding to surface-expressed citrullinated GRP78 on mononuclear cells. Journal of Clinical Immunology 33: 558–566.
Li, J., H.C. Hsu, and J.D. Mountz. 2012. Managing macrophages in rheumatoid arthritis by reform or removal. Current Rheumatology Reports 14: 445–454.
Biswas, S.K., M. Chittezhath, I.N. Shalova, and J.Y. Lim. 2012. Macrophage polarization and plasticity in health and disease. Immunologic Research 53: 11–24.
Zhu, W., J. Yu, Y. Nie, X. Shi, Y. Liu, F. Li, et al. 2014. Disequilibrium of m1 and m2 macrophages correlates with the development of experimental inflammatory bowel diseases. Immunological Investigations 43: 638–652.
Arnett, F.C., S.M. Edworthy, D.A. Bloch, D.J. McShane, J.F. Fries, N.S. Cooper, et al. 1988. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis and Rheumatism 31: 315–324.
Schellekens, G.A., H. Visser, B.A. de Jong, F.H. van den Hoogen, J.M. Hazes, F.C. Breedveld, et al. 2000. The diagnostic properties of rheumatoid arthritis antibodies recognizing a cyclic citrullinated peptide. Arthritis and Rheumatism 43: 155–163.
Savitsky, D., T. Tamura, H. Yanai, and T. Taniguchi. 2010. Regulation of immunity and oncogenesis by the IRF transcription factor family. Cancer Immunology, Immunotherapy 59: 489–510.
Krausgruber, T., K. Blazek, T. Smallie, S. Alzabin, H. Lockstone, N. Sahgal, et al. 2011. IRF5 promotes inflammatory macrophage polarization and TH1-TH17 responses. Nature Immunology 12: 231–238.
Takaoka, A., H. Yanai, S. Kondo, G. Duncan, H. Negishi, T. Mizutani, et al. 2005. Integral role of IRF-5 in the gene induction programme activated by Toll-like receptors. Nature 434: 243–249.
Satoh, T., O. Takeuchi, A. Vandenbon, K. Yasuda, Y. Tanaka, Y. Kumagai, et al. 2010. The Jmjd3-Irf4 axis regulates M2 macrophage polarization and host responses against helminth infection. Nature Immunology 11: 936–944.
Wang, T., X. Sun, J. Zhao, J. Zhang, H. Zhu, C. Li, et al. 2014. Regulatory T cells in rheumatoid arthritis showed increased plasticity toward Th17 but retained suppressive function in peripheral blood. Annals of the Rheumatic Diseases. doi:10.1136/annrheumdis-2013-204228.
Jiao, Z., W. Wang, S. Hua, M. Liu, H. Wang, X. Wang, et al. 2014. Blockade of Notch signaling ameliorates murine collagen-induced arthritis via suppressing Th1 and Th17 cell responses. American Journal of Pathology 184: 1085–1093.
Moreland, L.W., P.W. Pratt, M.D. Mayes, A. Postlethwaite, M.H. Weisman, T. Schnitzer, et al. 1995. Double-blind, placebo-controlled multicenter trial using chimeric monoclonal anti-CD4 antibody, cM-T412, in rheumatoid arthritis patients receiving concomitant methotrexate. Arthritis and Rheumatism 38: 1581–1588.
Maruotti, N., F.P. Cantatore, E. Crivellato, A. Vacca, and D. Ribatti. 2007. Macrophages in rheumatoid arthritis. Histology and Histopathology 22: 581–586.
Li, J., H.C. Hsu, P. Yang, Q. Wu, H. Li, L.E. Edgington, et al. 2012. Treatment of arthritis by macrophage depletion and immunomodulation: testing an apoptosis-mediated therapy in a humanized death receptor mouse model. Arthritis and Rheumatism 64: 1098–1109.
Weiss, M., K. Blazek, A.J. Byrne, D.P. Perocheau, and I.A. Udalova. 2013. IRF5 is a specific marker of inflammatory macrophages in vivo. Mediators of Inflammation 2013: 245804.
Snir, O., M. Widhe, C. von Spee, J. Lindberg, L. Padyukov, K. Lundberg, et al. 2009. Multiple antibody reactivities to citrullinated antigens in sera from patients with rheumatoid arthritis: association with HLA-DRB1 alleles. Annals of the Rheumatic Diseases 68: 736–743.
Kokkonen, H., M. Johansson, L. Innala, E. Jidell, and S. Rantapaa-Dahlqvist. 2007. The PTPN22 1858C/T polymorphism is associated with anti-cyclic citrullinated peptide antibody-positive early rheumatoid arthritis in northern Sweden. Arthritis Research and Therapy 9: R56.
Yoo, S.A., S. You, H.J. Yoon, D.H. Kim, H.S. Kim, K. Lee, et al. 2012. A novel pathogenic role of the ER chaperone GRP78/BiP in rheumatoid arthritis. Journal of Experimental Medicine 209: 871–886.
ACKNOWLEDGMENTS
These studies were funded by National Natural Science Foundation Projects to Dr. Shaohong Fang (No. C080102) and by grants from Department of Education, funding to Dr. Shaohong Fang (No. Z2010008) and supported by Key Laboratory of Myocardial Ischemia, Harbin Medical University, Chinese Ministry of Education to Dr. Shaohong Fang (No. KF201006 and No. KF201203) and Dr. Wei Zhu (No. KF201415); supported by postdoctoral sustentation fund of Heilongjiang province government to Xiu Li (No. LRB 2010–393)
Conflict of Interest
The authors report no conflicts of interest. The authors alone are responsible for the paper’s content and writing.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Wei Zhu and Xiu Li contributed equally to this work.
Rights and permissions
About this article
Cite this article
Zhu, W., Li, X., Fang, S. et al. Anti-Citrullinated Protein Antibodies Induce Macrophage Subset Disequilibrium in RA Patients. Inflammation 38, 2067–2075 (2015). https://doi.org/10.1007/s10753-015-0188-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-015-0188-z