Abstract
Enteropathogenic Escherichia coli (EPEC) is a leading cause of diarrhea among infants. Tight junction plays a vital role in intestinal paracellular permeability by forming physical intercellular barriers in epithelial cells. However, the impact of this enteric pathogen on tight junctions in vivo has not been fully investigated. In the present study, the alterations in tight junctions following EPEC infection in vivo were investigated. Western blot analysis revealed that the tight junction proteins, occludin and claudin-1, were displaced from tight junction membrane microdomains to Triton X-100 soluble fractions after EPEC infection. Changes in intestinal paracellular permeability were determined using the molecular tracer biotin, which was observed to penetrate the epithelia and extended into the lamina propria, indicating disruption in tight junction barrier function. Our results suggested that redistribution of tight junction proteins plays an important role in the disruption of epithelial barrier function induced by EPEC infection, which may provide new insight into the pathogenesis of diarrhea caused by EPEC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Enteropathogenic Escherichia coli (EPEC) infection triggers severe watery diarrhea which can lead to death in infants [1]. However, the pathological mechanisms leading to diarrhea during EPEC infection remain largely unknown. EPEC infection induces a typical intestinal lesion characterized by intimate adherence of bacteria to the epithelium, which is associated with microvilli destruction and reorganization of cytoskeletal actin [2]. The formation of attaching and effacing (A/E) lesions requires type III secretion system, which is encoded on a pathogenicity island called the locus of enterocyte effacement [3]. The bacterial proteins and effector molecules are injected into the host cell cytoplasm through the avenue formed by the secretion system apparatus [4].
The effectors delivered into the cells can function together to subvert host cellular processes [5, 6]. A great number of cellular responses occur following translocation of effectors into host cells, including induction of actin-rich pedestals underneath adherent bacteria, mitochondrial dysfunction, a weak inflammatory response, and tight junction (TJ) disruption [7–9]. They also induce changes in host cell signaling pathways that act in mediating the diarrheal response to EPEC infection [10].
TJs are the apical-most adhesive junctional complexes in mammalian epithelial cells, which function as permeability barriers by segregating luminal from adlumenal compartments [11]. TJs are formed of continuous strands of TJ proteins, consisting of occludin, claudins, and junctional adhesion molecule, all of which encircle the most apical aspect of the lateral plasma membrane [12]. There has been increasing recognition of an association between disrupted intestinal barrier function and the development of diseases including Crohn's disease, ulcerative colitis, and microbial infections [13–15]. It is well established that tight junctions are altered by EPEC in vitro. A decrease in transepithelial electrical resistance was observed during formation of attaching and effacing lesions, which was accompanied by an appearance of aberrant strands throughout the lateral membrane [16]. In addition to these morphological and physiological changes, EPEC has been shown to change the localization of occludin, zonula occludens-1, and the barrier forming claudin proteins [16, 17]. In addition to TER decline, molecular tracers have also indicated that the barrier is functionally compromised during these infections [18].
Although much work has investigated the effects of EPEC infection on tight junctions in tissue culture systems, there have been few investigations in relevant infection models. To investigate the mechanisms underlying whole animal disease, experiments in relevant infections are essential [19]. Until now, the most frequently used animal model was the murine infection model using the A/E mouse pathogen Citrobacter rodentium which could induce watery diarrhea. Similar results as the in vitro studies have been shown during animal infections with C. rodentium. In these animal models, alteration in TJ proteins localization and disruption of epithelial barrier integrity were revealed [19, 20]. A recent study has claimed that infection of EPEC in C57/BL6 mice caused destruction of enterocyte tight junctions [21].
To gain insight into the mechanism underlying the pathogenesis of EPEC infection, we used the in vivo A/E mouse infection model to investigate the effects of EPEC infection on tight junctions. We found that following wild-type EPEC infection, occludin and claudin-1 were displaced from the tight junction membrane microdomains to Triton X-100 soluble fractions. Moreover, tight junctions were functionally impaired.
MATERIALS AND METHODS
Animals
C57BL/6J mice were purchased from the Department of Experimental Animals, Medical College of Beijing University, China. Four- to 6-week-old male mice were used in this study. The animals were acclimatized to the new environment for 1 week. Mice were treated in accordance with the local animal protection legislation and were provided food and water ad libitum. Experimental protocols were approved by the Institutional Animal Care and Use Committee of Nanjing University, and the Principles of Laboratory Animal Care (NIH publication no. 86-23, revised in 1985) were followed.
Mouse Infections
The wild-type EPEC 2348/69 was used in the experiment. Mice were orally infected with 2 × 108 EPEC suspended in 200 μl of sterile phosphate-buffered saline (PBS). Mice that received only sterile PBS served as control. Infections persisted for 1, 3, or 5 days at which point the mice were sacrificed by cervical dislocation.
Histological Analysis
The colon tissues were fixed in 10% neutrally buffered formalin, stained in hematoxylin and eosin (H&E), sectioned, and examined by light microscopy for the changes induced by EPEC infection.
Immunoblot Analysis
The previously reported method was followed to isolate tight junction membrane microdomains [22]. Briefly, tissue samples were homogenized in lysis buffer (50 mM Tris, 25 mM KCl, 5 mM MgCl2⋅6H2O, 2 mM EDTA, 40 mM NaF, 4 mM Na3VO4, pH 7.4) containing 1% Triton X-100 and protease inhibitor mixture solution. The resulted lysate was subjected to SDS-PAGE. Proteins were transferred electrophoretically onto PVDF membranes (Bio-Rad, Hercules, CA, USA). The membranes were blocked with 3% BSA in Tris-buffered saline containing 0.1% Tween-20 (TBS-T) for 20 min at room temperature. Membranes were then incubated overnight at 4°C with primary antibodies diluted in TBS-T buffer. Following three 5-min washes with TBS-T buffer, the membranes were incubated with appropriate secondary antibodies for 1 h at room temperature. The hybridized band was detected by ECL kit (Amersham Biosciences, Chalfont St Giles, UK) according to the manufacturer's instructions. Immunoblots were scanned using ChemiDOC XRS instrument (Bio-Rad), and densitometry was performed by Quantity One 1-d analysis software (Bio-Rad).
Assessment of Intestinal Mucosal Permeability
The previously reported method was adopted to assess the intestinal mucosal permeability [19]. In this method, EZ-link Sulfo-NHS-Biotin was used as a molecular tracer. In brief, tissues were fixed for 3 h in 3% paraformaldehyde and washed three times with PBS prior to cryoembedding and sectioning. Subsequently, tissues were embedded in optimal cutting temperature compound (Sakura Finetech, USA) and serial sections were cut at a thickness of 6 μm. Thereafter, tissues were permeabilized with 0.2% Triton X-100 in PBS for 20 min, and blocking was achieved by incubation with 5% goat serum in PBS containing 0.05% Tween-20 and 0.1% bovine serum albumin. Incubation with primary antibodies claudin-3 and 5 (Zymed Laboratories Inc., San Francisco, CA, USA) was performed overnight at 4°C. The primary antibodies were used at a dilution of 1:200. After three washes with PBS, the sections were incubated with Alexa 488-conjugated streptavidin (1:500) and Alexa 635-conjugated secondary antibodies (Molecular Probes, Eugene, OR, USA) (at 1:100 dilution) at room temperature for 1 h in the dark. Cell DNA was visualized by 4′, 6′-diamidino-2-phenylindole (DAPI; Molecular Probes). The stained sections were visualized and photographed using a Leica TCS SP2 laser confocal scanning microscope (Leica Microsystems, Heidelberg GmbH, Mannheim, Germany).
Statistical Analysis
Data were analyzed using paired Student's t test. Data were presented as mean ± SEM and were considered significant if P was <0.05.
RESULTS
Histological Assessment
We first examined the influence of EPEC infection on colonic mucosal architecture by H&E staining. The epithelial lining of the colon from control mice was intact and showed well-organized colonic mucosa (Fig. 1a). However, when mice were treated with EPEC for a 5-day period, loss of epithelial cells was seen and the surface epithelium had an irregular appearance (Fig. 1b–d). This infection also caused a mucosal hyperplasia in the colon accompanied by mild infiltration of inflammatory cells. Thus, this study revealed considerable tissue damages during EPEC infection in vivo.
Redistribution of Tight Junction Proteins Induced by EPEC Infection
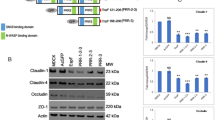
To investigate whether EPEC infection affected tight junction, we examined the expression of tight junction proteins in membrane microdomains of tight junction. A previous report has suggested that tight junctions are specific lipid raft [23]. The detergent-resistant tight junction membrane microdomains were isolated using detergent extraction and sucrose density gradient centrifugation, and the extracted tight junction proteins were analyzed by Western blot analysis. Using this method, we found that the lipid raft marker protein caveolin-1 was localized in fractions 2–5 in control, corresponding to tight junction membrane microdomains (Fig. 2a). EPEC infection affected the distribution of caveolin-1 in tight junction membrane microdomains. There was an 80.1% decrease in caveolin-1 localization in tight junction membrane microdomains after 1 day of infection with EPEC, and the expression of caveolin-1 declined by 37.8% and 18.4% following 3 and 5 days of infection, respectively (Fig. 2b). Moreover, Western blot analysis revealed that EPEC infection induced a movement of occludin and claudin-1 out of tight junction membrane microdomains. In control mice, 19.6% occludin was found in tight junction membrane microdomains (Fig. 2c, d). However, after EPEC infection, occludin was displaced from the low-density fractions to the bottom of the gradient. Another tight junction protein claudin-1 was also redistributed after EPEC infection (Fig. 2e, f).
Effect of EPEC infection on the distribution of occludin and claudin-1 in tight junction membrane microdomains. Tight junction membrane microdomains were isolated by sucrose density gradient centrifugation and analyzed by immunoblotting, probing with antibodies against caveolin-1 (a, b), occludin (c, d), or claudin-1 (e, f). The results of densitometric analysis were shown in b, d, and f. Asterisks indicated significant difference as compared with control (*P < 0.05; **P < 0.01; ***P < 0.001).
EPEC Infection Induced Mucosal Barrier Dysfunction
To determine whether the altered distribution of tight junction proteins induced functional disruption of tight junctions, we utilized biotin as a molecular tracer to assess the integrity of the epithelial barrier, and claudin-3 and 5 were double-labeled with the biotin tracer. Biotin was found to be restricted to the luminal boundary of the colon epithelium in control (Fig. 3a, c), which is in consistent with our previous study [24]. After EPEC infection, biotin was no longer held to the luminal bounder, and it permeated the epithelium and extended into the lamina propria. The biotin was observed to pass into the epithelium through areas of altered claudin location (Fig. 3b, d). It indicated that the tight junction was functionally altered by EPEC infection.
Tight junction barrier were disrupted by EPEC infection. The control (a, c) and EPEC-infected (b, d) colon tissues were stained with claudin antibodies and the cell tracer biotin to examine barrier permeability. DAPI was used to label the nucleus. a, b Claudin-3 and biotin staining. c, d Claudin-5 and biotin staining.
DISCUSSION
Enteropathogenic E. coli infection is a main cause of infantile diarrhea in developing countries, which leads to several hundred thousand infant deaths each year [25]. Until now, the underlying mechanisms by which EPEC triggers the severe watery diarrhea are unclear. Previous studies have suggested that this disease is in part dependent on EPEC interaction with enterocytes [26, 27]. This intimate attachment of bacteria to the host cell membrane results in loss of absorptive microvilli, which is called an A/E lesion. Thus, understanding how A/E bacterial pathogens colonize their hosts is of great importance in combating these infections. Our previous in vitro study demonstrated that EPEC infection caused disruption of tight junction structure and function [15]. Furthermore, our results indicated that the tight junction membrane microdomains were key sites of EPEC entry. To further our study, in the present report, we infected mice with a wild-type EPEC 2348/69 and investigated changes in the distribution of occludin and claudins in tight junction membrane microdomains and alteration in intestinal barrier function. We found that EPEC induced tight junction barrier dysfunction which was accompanied by redistribution of occludin and claudins in tight junction membrane microdomains.
Tight junctions form a regulatable semipermeable barrier at the boundary between the apical and the basolateral membrane domains [28, 29]. The key role of tight junction is acting as a regulatory barrier to the movement of molecules. Tight junctions are constituted of an array of tight junction proteins. The regulation of tight junction barrier function is a very intricate process and many transmembrane and intracellular proteins are involved [30]. It is increasingly recognized that tight junctions are altered both physiologically and pathophysiologically. Perturbation of tight junction was found to be involved in several disease states including enteric infection [16], Crohn's disease [29], and experimental colitis [22]. The impaired integrity of the intestinal barrier has been observed in patients with Crohn's disease [31]. A recent study reported that the expression pattern of claudins was altered in Crohn's disease [32].
The diarrhea induced by EPEC infection was once thought to be caused by the loss of absorptive microvilli [33]. Recently, a growing number of in vitro studies have demonstrated that EPEC infection affected tight junction barrier function. Infection of the intestinal cell monolayers induced a time-dependent decrease in transepithelial electrical resistance which was correlated with the dissociation of occludin from intestinal epithelial tight junctions [17]. Despite extensive studies on the effect of EPEC infection on tight junction function in vitro, little is known about the changes of tight junction during EPEC infection in vivo. In the present study, we demonstrated that tight junction barrier function was altered during EPEC infection. Similar with what has been reported for Campylobacter jejuni, our findings showed that EPEC infection induced a translocation of occludin and claudin-1 from the TJ platform [34]. We also observed that the cell tracer could pass between cells through the tight junctions during EPEC infection. These findings indicated that EPEC disrupted multiple host tight junction proteins in vivo resulting in a functionally deficient epithelial barrier. In summary, our study demonstrated the underlying molecular mechanisms of tight junction barrier disruption triggered by EPEC infection. These results may provide critical information on the pathogenesis of EPEC infection.
REFERENCES
Guttman, J.A., F.N. Samji, Y.L. Li, W.Y. Deng, A. Lin, and B.B. Finlay. 2007. Aquaporins contribute to diarrhoea caused by attaching and effacing bacterial pathogens. Cellular Microbiology 9: 131–141.
Phillips, A.D., J. Giròn, S. Hicks, D. Gordon, and G. Frankel. 2000. Intimin from enteropathogenic Escherichia coli mediates remodelling of the eukaryotic cell surface. Microbiology 146: 1333–1344.
Clarke, S.C., R.D. Haigh, P.P. Freestone, and P.H. Williams. 2003. Virulence of enteropathogenic Escherichia coli, a global pathogen. Clinical Microbiology Reviews 16: 365–378.
Muza-Moons, M.M., A. Koutsouris, and G. Hecht. 2003. Disruption of cell polarity by enteropathogenic Escherichia coli enables basolateral membrane proteins to migrate apically and to potentiate physiological consequences. Infection and Immunity 71: 7069–7078.
Ruchaud-Sparagano, M.H., M. Maresca, and B. Kenny. 2007. Enteropathogenic Escherichia coli (EPEC) inactivate innate immune responses prior to compromising epithelial barrier function. Cellular Microbiology 9: 1909–1921.
Matsuzawa, T., A. Kuwae, S. Yoshida, C. Sasakawa, and A. Abe. 2004. Enteropathogenic Escherichia coli activates the RhoA signaling pathway via the stimulation of GEF-H1. The EMBO Journal 23: 3570–3582.
Dean, P., and B. Kenny. 2009. The effector repertoire of enteropathogenic E. coli: ganging up on the host cell. Current Opinion in Microbiology 12: 101–109.
Chen, H.D., and G. Frankel. 2005. Enteropathogenic Escherichia coli: unravelling pathogenesis. FEMS Microbiology Reviews 29: 83–98.
Dean, P., M. Maresca, and B. Kenny. 2005. EPEC's weapons of mass subversion. Current Opinion in Microbiology 8: 28–34.
Vallance, B.A., and B.B. Finlay. 2000. Exploitation of host cells by enteropathogenic Escherichia coli. Proceedings of the National Academy of Sciences of the United States of America 97: 8799–8806.
Groschwitz, K.R., and S.P. Hogan. 2009. Intestinal barrier function: molecular regulation and disease pathogenesis. The Journal of Allergy and Clinical Immunology 124: 3–20.
Weflen, A.W., N.M. Alto, and G.A. Hecht. 2009. Tight junctions and enteropathogenic E. coli. Annals of the New York Academy of Sciences 1165: 169–174.
Gassler, N., C. Rohr, A. Schneider, J. Kartenbeck, A. Bach, N. Obermuller, et al. 2001. Inflammatory bowel disease is associated with changes of enterocytic junctions. American Journal of Physiology. Gastrointestinal and Liver Physiology 281: G216–G228.
Tummala, S., S. Keates, and C.P. Kelly. 2004. Update on the immunologic basis of Helicobacter pylori gastritis. Current Opinion in Gastroenterology 20: 592–597.
Li, Q.R., Q. Zhang, C.Y. Wang, N. Li, and J.S. Li. 2008. Invasion of enteropathogenic Escherichia coli into host cells through epithelial tight junctions. The FEBS Journal 275: 6022–6032.
Muza-Moons, M.M., E.E. Schneeberger, and G.A. Hecht. 2004. Enteropathogenic Escherichia coli infection leads to appearance of aberrant tight junctions strands in the lateral membrane of intestinal epithelial cells. Cellular Microbiology 6: 783–793.
Simonovic, I., J. Rosenberg, A. Koutsouris, and G. Hecht. 2000. Enteropathogenic Escherichia coli dephosphorylates and dissociates occludin from intestinal epithelial tight junctions. Cellular Microbiology 2: 305–315.
Spitz, J., R. Yuhan, A. Koutsouris, C. Blatt, J. Alverdy, and G. Hecht. 1995. Enteropathogenic Escherichia coli adherence to intestinal epithelial monolayers diminishes barrier function. American Journal of Physiology. Gastrointestinal and Liver Physiology 268: G374–G379.
Guttman, J.A., Y.L. Li, M.E. Wickham, W.Y. Deng, A.W. Vogl, and B.B. Finlay. 2006. Attaching and effacing pathogen-induced tight junction disruption in vivo. Cellular Microbiology 8: 634–645.
Guttman, J.A., F.N. Samji, Y.L. Li, A.W. Vogl, and B.B. Finlay. 2006. Evidence that tight junctions are disrupted due to intimate bacterial contact and not inflammation during attaching and effacing pathogen infection in vivo. Infection and Immunity 74: 6075–6084.
Shifflett, D.E., D.R. Clayburgh, A. Koutsouris, J.R. Turner, and G.A. Hecht. 2005. Enteropathogenic E. coli disrupts tight junction barrier function and structure in vivo. Laboratory Investigation 85: 1308–1324.
Li, Q.R., Q. Zhang, M. Zhang, C.Y. Wang, Z.X. Zhu, N. Li, and J.S. Li. 2008. Effect of n-3 polyunsaturated fatty acids on membrane microdomain localization of tight junction proteins in experimental colitis. The FEBS Journal 275: 411–420.
Nusrat, A., C.A. Parkos, P. Verkade, C.S. Foley, T.W. Liang, W. Innis-Whitehouse, et al. 2000. Tight junctions are membrane microdomains. Journal of Cell Science 113: 1771–1781.
Zhang, Q., Q.R. Li, C.Y. Wang, X.X. Liu, N. Li, and J.S. Li. 2010. Enteropathogenic Escherichia coli changes distribution of occludin and ZO-1 in tight junction membrane microdomains in vivo. Microbial Pathogenesis 48: 28–34.
Kaper, J.B., J.P. Nataro, and H.L. Mobley. 2004. Pathogenic Escherichia coli. Nature Reviews. Microbiology 2: 123–140.
Moon, H.W., S.C. Whipp, R.A. Argenzio, M.M. Levine, and R.A. Giannella. 1983. Attaching and effacing activities of rabbit and human enteropathogenic Escherichia coli in pig and rabbit intestines. Infection and Immunity 41: 1340–1351.
Ulshen, M.H., and J.L. Rollo. 1980. Pathogenesis of Escherichia coli gastroenteritis in man—another mechanism. New England Journal of Medicine 302: 99–101.
Balda, M.S., and K. Matter. 1998. Tight junctions. Journal of Cell Science 111: 541–547.
Förster, C. 2008. Tight junctions and the modulation of barrier function in disease. Histochemistry and Cell Biology 130: 55–70.
Tomson, F.L., V.K. Viswanathan, K.J. Kanack, R.P. Kanteti, K.V. Straub, M. Menet, et al. 2005. Enteropathogenic Escherichia coli EspG disrupts microtubules and in conjunction with Orf3 enhances perturbation of the tight junction barrier. Molecular Microbiology 56: 447–464.
Hollander, D. 1993. Permeability in Crohn's disease: altered barrier functions in healthy relatives? Gastroenterology 104: 1848–1851.
Weber, C.R., and J.R. Turner. 2007. Inflammatory bowel disease: is it really just another break in the wall? Gut 56: 6–8.
Nataro, J.P., and J.B. Kaper. 1998. Diarrheagenic Escherichia coli. Clinical Microbiology Reviews 11: 142–201.
Chen, M.L., Z.M. Ge, J.G. Fox, and D.B. Schauer. 2006. Disruption of tight junctions and induction of proinflammatory cytokine responses in colonic epithelial cells by Campylobacter jejuni. Infection and Immunity 74: 6581–6589.
ACKNOWLEDGMENTS
This work was supported by the Key Project of National Natural Science Foundation in China (30830098), the National Basic Research Program (973 Program) in China (Nos. 2007CB513005 and 2009CB522405), the National Natural Science Foundation in China (81070375), the Scientific Research Fund in Jiangsu Province (BK2009317), and the National Key Project of Scientific and Technical Supporting Programs funded by the Ministry of Science & Technology of China (2008BAI60B06).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Q., Li, Q., Wang, C. et al. Redistribution of Tight Junction Proteins During EPEC Infection In Vivo . Inflammation 35, 23–32 (2012). https://doi.org/10.1007/s10753-010-9285-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-010-9285-1