Abstract
Heart and kidney interactions are fascinating, in the sense that failure of the one organ strongly affects the function of the other. In this review paper, we analyze how principal driving forces for glomerular filtration and renal blood flow are changed in heart failure. Moreover, renal autoregulation and modulation of neurohumoral factors, which can both have repercussions on renal function, are analyzed. Two paradigms seem to apply. One is that the renin-angiotensin system (RAS), the sympathetic nervous system (SNS), and extracellular volume control are the three main determinants of renal function in heart failure. The other is that the classical paradigm to analyze renal dysfunction that is widely applied in nephrology also applies to the pathophysiology of heart failure: pre-renal, intra-renal, and post-renal alterations together determine glomerular filtration. At variance with the classical paradigm is that the most important post-renal factor in heart failure seems renal venous hypertension that, by increasing renal tubular pressure, decreases GFR. When different pharmacological strategies to inhibit the RAS and SNS and to assist renal volume control are considered, there is a painful lack in knowledge about how widely applied drugs affect primary driving forces for ultrafiltration, renal autoregulation, and neurohumoral control. We call for more clinical physiological studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is growing awareness that renal function determines outcome in heart failure (HF). Moreover, any combination of heart and renal failure is associated with worse outcomes [1–3]. Yet, how best to approach the interactions between the failing heart and the failing kidney, is not trivial. A categorization has been proposed, where order and chronicity in which the two organs fail are considered [2]. However, by design, this does not take into consideration the mechanisms involved. We previously emphasized that both hemodynamic and non-hemodynamic mechanisms are involved in cardiorenal crosstalk [1].
Regarding renal dysfunction in HF, classically, there has been very strong emphasis on arterial pressure and neurohumoral control (renin-angiotensin system, RAS, and the sympathetic nervous system, SNS). More recently, evidence from epidemiological and clinical studies supports a strong influence of central venous pressure on renal perfusion [4, 5]. In acute patients with advanced HF and worsening kidney function, increased central venous pressure was reported, as compared to patients in whom renal function remained stable [5]. In a chronic setting, lower GFR was strongly related to elevated central venous pressure [4]. These observations have revived interest in renal venous pressure as a determinant of renal function [6]. The goal of this review is to summarize current understanding of the pathophysiology of renal hemodynamics in HF, and explore areas that need further investigation.
Physiological regulation of RBF and glomerular filtration rate
One can analyze renal hemodynamics in a three-step approach: the primary driving forces for glomerular filtration, intrinsic renal mechanisms affecting these forces (autoregulation, pressure natriuresis), and finally neurohumoral factors. In principle, the GFR is determined by the permeability characteristics of the glomerular membrane, and hydrostatic and oncotic pressures in the glomerular capillary and in Bowman’s space. These driving forces, together with the structural integrity of the glomerulus, govern filtration and also dictate the pressure decline from the entry of the afferent arteriole into the glomerular capillary network, then to the beginning of the efferent arteriole, and finally the peritubular capillaries (Box 1).
Primary driving forces
Figure 1 depicts the process of filtration along the glomerular capillaries and the Starling forces in the glomerulus. In humans, the Starling forces in the glomerulus cannot be measured directly and are extrapolated from extensive micropuncture studies performed in rats [7–10].Single nephron GFR (whole kidney GFR divided by glomerular number) in humans is approximately 60–70 nl/min. Based on filtration fraction (GFR/RPF, about 20–25% in humans), plasma protein concentration at the end of the glomerulus can be estimated, and hence plasma oncotic pressure. Tubular hydrostatic pressure and Kf, the filtration coefficient, are not known in humans. Tubular protein concentration is not considered to be a relevant determinant of glomerular filtration, even in the presence of nephrotic-range proteinuria. Modeling of the process of glomerular filtration based on the Starling forces was first reported in a classical paper by Deen [7]. From the model, it is predicted that a decrease in mean arterial pressure, without adjustments in afferent and efferent arteriolar resistances, will lead to substantial changes in GFR. Similarly, plasma protein concentration and changes in tubular pressure will directly impact on the filtration process. It is immediately clear that HF can affect all of these factors.
Hydrostatic pressure decrease and oncotic pressure increase along the glomerular capillary network and filtration in normovolemic (solid lines) and hypovolemic (dashed lines) states a Estimated values for the primary determinants of glomerular filtration b Please note the relatively low value for net ultrafiltration pressure. Abbreviations: Pglom glomerular capillary hydrostatic pressure, πglom glomerular capillary oncotic pressure, Kf filtration coefficient, Part, mean systemic arterial pressure, Pven renal venous pressure, Ptub intratubular pressure, SNGFR single nephron GFR
In order to properly understand what impact changes in RBF will have on GFR, it is necessary to understand the concept of filtration equilibrium. Filtration equilibrium is the condition in which the sum of plasma oncotic pressure and tubular hydrostatic pressure equal glomerular capillary pressure before the end of the glomerular capillary network [7, 11]. The dependency of GFR on RBF is related to whether filtration equilibrium is reached or not. Unfortunately, we are not informed about this in healthy humans, or patients with reduced GFR. Nevertheless, independent of neurohumoral control or structural abnormalities, intrinsically to the basic mechanism of glomerular ultrafiltration, GFR can depend on RBF.
Autoregulation
Intrinsic to the vascular bed is the phenomenon of autoregulation. This is not specific for the kidney; however, the renal vasculature differs in several respects from the other tissues. First of all, it has not one, but two regulatory arteriolar regions, that serve to maintain glomerular pressure at a level that permits ultrafiltration. Second, RBF does not seem to be regulated by metabolic demand. Third, there are at least two systems that contribute to the stabilization of RBF, whereas regular capillary beds have one.
Historically, descriptions of stabilization of RBF upon fluctuations in renal perfusion pressure date back to the early years of the 20th century by Bayliss [12]. We now recognize that at least two mechanisms contribute to autoregulation in the kidney, a fast vasoconstriction mediated by increased wall tension in the vascular wall (“myogenic response”) and a slow vasoconstriction mediated by increased delivery of solutes to the macula densa (“tubuloglomerular feedback”, TGF) [13, 14]. The nature of a third mechanism to stabilize RBF upon changes in perfusion pressure is not yet clear, but both TGF and this 3rd mechanism seem to be slow [14, 15]. It is beyond the scope of this review to describe the components in detail [13].
Essentially, myogenic response is the intrinsic capability of the renal vasculature, in particular the small diameter vessels (arcuate arteries, cortical radial arteries and afferent arterioles) [16], to respond to an increase in wall tension with an increase in intracellular calcium, activation of myosin light chain kinase and vascular smooth muscle cell contraction. This mechanism is extremely fast [17]. The TGF system is a negative feedback system [13, 18–20]. In response to an increase in glomerular filtration, and consequently an increase in solute concentration, probably chloride, sensed by the macula densa, a mediator is released that constricts the afferent arteriole, which will stabilize the macula densa solute delivery [21]. The substance is still subject to investigation, but could be adenosine, which would then act via the adenosine A1 receptor on the afferent arteriole [22, 23]. As mentioned, this system is considerably slower than the myogenic response.
Of relevance to this review are three considerations. First, autoregulation primarily seems to be a pressure-mediated phenomenon and not a flow-mediated phenomenon. Second, since autoregulation is mediated primarily, if not entirely, by changes in afferent arteriolar tone, RBF and GFR are regulated in parallel. Finally, diuretics that decrease sodium reabsorption upstream of the macula densa will increase distal sodium delivery and will activate TGF, and consequently will lead to an afferent vasoconstriction [24, 25]; the typical example of such a diuretic is acetazolamide, acting on carbonic anhydrase in the proximal tubule. Parenthetically, such maneuvers will also increase proximal tubular pressure, and thereby decrease net ultrafiltration pressure [24]. Interestingly, the Na-2Cl-K cotransporter in the loop of Henle, that is blocked by furosemide, is also the sensor for TGF. Depending on the extent to which furosemide blocks the sensing of the TGF system, this drug can evoke a TGF-mediated decrease in GFR or induce a complete deactivation of the TGF system, and consequently an increase in GFR (see below).
Neurohumoral factors
The third layer of factors is neurohumoral control systems acting at systemic (integrative) level. The most relevant for heart and kidney interactions seem currently the RAS, natriuretic factors, the SNS, and nitric oxide (NO). At this point, we will only discuss briefly their impact on the basic driving forces for glomerular filtration and on the autoregulation systems. In particular, the actions of the RAS are complex. Although it is usually stated otherwise in textbooks, direct measurements of afferent and efferent arteriolar tone show that ANG II can constrict both arteriolar beds [26, 27]. Confusingly, this would result in an increase in filtration fraction, since filtration fraction is GFR/RPF, RPF decreases and GFR stays constant. This increase in filtration fraction is often incorrectly attributed to indicate efferent vasoconstriction, which is not necessarily the case [27]. A similar paradoxical situation can be found with respect to the actions of ANG II to enhance proximal tubular reabsorption, which might be expected to lead to a decrease in distal delivery, and consequently an increase in GFR mediated by TGF. However, the concomitant sensitization of TGF by ANG II leads to a stable GFR [28, 29]. This is illustrated in Fig. 2.
Synergistic actions of ANG II on proximal reabsorption and tubuloglomerular feedback (adapted from [28]. ANG II increases proximal tubular reabsorption, thereby decreasing the amount of fluid leaving the proximal tubule and reaching the macula densa. This would deactivate TGF, and increase single nephron GFR. However, ANG II also makes the TGF system more sensitive, so that single nephron GFR all together does not change
An acute increase in renal sympathetic nerve activity (RSNA) does not seem to affect net RBF very much under healthy conditions [30, 31], however, it does substantially affect tubular reabsorption [32]. Moreover, acute renal denervation does not seem to affect the function of the TGF system significantly [33, 34]. This seems to be different in (experimental) renal disease and HF (see below). Chronic manipulation of RSNA has important actions on blood pressure by affecting renin release. Since both renal failure and HF are characterized by inappropriate stimulation of the SNS, the SNS–RAS axis will be of relevance for our discussion.
The natriuretic peptide family, atrial natriuretic peptide (ANP), brain natriuretic peptide (BNP), C-type natriuretic peptide (CNP), and urodilatin, has well-defined renal hemodynamic effects. ANP and BNP (!) are secreted by the heart in response to increased wall stretch or stress [35] whereas CNP and urodilatin are produced by the kidney. Several receptors (Type A, B, and C) for the natriuretic peptide family have been identified. Receptors have been found in the glomerulus as well as in the afferent and efferent arterioles. The renal hemodynamic effects of all members of the natriuretic peptide bear a similar profile [36]. Therefore, here we discuss only results pertaining to ANP.
Exogenous administration of ANP in humans results in an increase in GFR, filtration fraction, and sodium excretion. Indeed in vitro ANP dilates pre-constricted vessels and in animals ANP induces pre-glomerular vasodilation through NO production, and increased guanylate cyclase activity and cGMP production. This is in agreement with the finding that ANP does not increase renal plasma flow [37]. The role of ANP in the regulation of GFR and renal plasma flow in (patho)physiologic conditions is illustrated in studies in which the ANP system was blocked. In conditions in which ANP and BNP levels are increased (high salt intake, hyperaldosteronism, diabetes) blockade of the ANP system decreases GFR suggesting a role for the natriuretic peptide family in regulating GFR and ERPF under these conditions. However, in rats with heart failure ANP seemed not to play a role in the regulation of renal hemodynamics [38].
Nitric oxide has well-described profound and tonic influence on the systemic and renal vasculature [39, 40]. Although hard to discriminate from the consequences on systemic hemodynamics transmitted to the renal vasculature, NO seems to dilate the afferent arteriole [41], thereby increasing glomerular capillary pressure and GFR. In both normal rats [42, 43] and in non-clipped kidneys of 2K1C Goldblatt hypertensive rats (model for renovascular hypertension), NO synthesis inhibition improves the efficacy and decreases the lower limit of autoregulation [44]. This likely is due to combined actions on myogenic response and TGF [45]. Responsiveness of the latter is enhanced during local NO synthesis inhibition, which indicates a stronger response to constrict the afferent arteriole upon increases in PGC [46, 47]. The actions of ANG II to increase TGF responsiveness are also enhanced by local NO synthesis inhibition [47].
Changes in primary driving forces for glomerular filtration in heart failure
Classically, renal failure in HF has been interpreted as pre-renal failure, where forward failure leads to a decrease in renal perfusion pressure, a decrease in glomerular capillary pressure and thereby a decrease in GFR. However, GFR would remain stable until a severe hypotension develops if autoregulation is intact. Severe hypotension that would be below the lower limit of autoregulation of healthy kidneys is uncommon in both patients with HF with preserved ejection fraction (HFPEF) and with reduced ejection fraction (HFREF). Distinction between an acute cardiorenal and a chronic cardiorenal syndrome has been proposed [2]. While this may be of some assistance in clinical management, it should not distract from discriminating the various mechanisms. We propose that in order to address worsening of renal function in HF, the following questions be addressed to support the understanding of the mechanism:
-
If blood pressure decreases, initially the kidney will dilate the afferent arteriole to maintain glomerular pressure. Is hypotension so severe that it exceeds the ability of the kidneys to autoregulate and maintain GFR?
-
Is (acute) HF occurring in the presence of pre-existing renal disease or atherosclerotic renovascular artery stenosis(ARAS)?
-
Are (intravenous) vasoconstrictors or other (vasodilator) drugs used that could compromise renal perfusion or renal autoregulation of RBF and GFR?
-
Does HF coincide with congestion, pulmonary hypertension [48], and an increase in central venous pressure? Is intra-abdominal pressure elevated?
-
Are there other causes suspected to impair renal function (e.g., interstitial nephritis or a primary kidney disease)?
Returning to the principal driving forces of glomerular filtration, these questions address predominantly glomerular pressure and tubular pressure, because plasma oncotic pressure will be reduced, and information about glomerular permeability is lacking. Using such an approach, worsening kidney function in HF can be discriminated as arterial, venous or intra-renal. This follows a classical approach used to diagnose renal failure in general, albeit that the post-renal axis generally is viewed as urological post-renal obstruction. Since current studies are not documenting these factors systematically, it can be suspected that outcome studies in general include very heterogeneous patient groups, and may fail to show consistent results.
One observation concerning GFR and RBF relationships deserves attention. In several studies, it has been noted that there is a strong positive correlation between GFR and RBF in cohorts of HF patients [49, 50]. In individual patients, this finding has been interpreted as GFR becoming strongly dependent upon RBF. There are, however, two interpretations possible. The first is that if GFR decreases due to progressive loss of nephrons, RBF declines also. In that case, the observation is not related to specific driving forces, autoregulation or neurohumoral factors. Alternatively, GFR is functionally dependent on RBF in each individual person. The latter may be true but is an untenable conclusion based upon the available data. If individuals have fluctuations in renal perfusion pressure within the autoregulatory range, GFR is not much dependent upon RBF, since they are stabilized together. In case renal perfusion pressure falls below the autoregulation range, as happened in a substantial number of patients in at least one report [50], GFR might become more and more dependent on RBF.
Because of its relevance, we would like to analyze further which physiological phenomena determine the coupling between cardiac output and RBF, and which factors determine the coupling between RBF and GFR. RBF, in principle, is determined by the renal perfusion pressure, RPP, and by intrarenal resistances. If a decrease in cardiac output occurs, and this coincides with a decrease in RBF, either renal perfusion pressure has decreased, intrarenal resistances have increased, or both. If the decrease in RBF is more pronounced than the decrease in cardiac output, this is likely due to the combination of a decrease in renal perfusion pressure and an increase in renal resistance. It should be remarked that a decrease in renal perfusion pressure within the autoregulatory range of a healthy kidney elicits a decrease in intrarenal resistances to stabilize RBF. A dissociation between cardiac output and RBF, therefore would implicate that the autoregulatory possibilities of the kidney are exhausted, or overruled by another mechanism (e.g., sympathetic nervous system). An example of a factor that could lead to a disproportional decrease in RBF upon a decrease in cardiac output is angiotensin II.
Regarding the RBF (or renal plasma flow for that matter) dependency of GFR, there is debate whether this could be relevant or not in humans. Again, in principle, perfusion pressure and intrarenal resistances determine RBF. Probably the best way to analyze RBF dependency of GFR is to look at (a) isolated changes in efferent resistance, (b) isolated changes in afferent resistance, (c) a concomitant unidirectional change in both resistances and (d) a change in renal perfusion pressure only. An isolated increase in efferent arteriolar resistance is generally associated with dissociation of RBF and GFR: RBF will tend to decrease and GFR will tend to increase. An isolated increase in afferent arteriolar resistance will generally decrease RBF and GFR in parallel. The debate is not closed at which level of vasoconstriction, and concomitantly low RBF, reduction of GFR will be more pronounced than reduction of RBF decrease. Simultaneous increases in afferent and efferent arteriolar resistances can be considered together with the scenario of a decrease in renal perfusion pressure. At higher blood flows (i.e., lower resistances or higher perfusion pressure), GFR will become less dependent upon RBF; conversely, low perfusion pressures or very high resistances will leave GFR very sensitive to blood flow[51]. This seems true in particular in circumstances of volume depletion (in rats). It must be remarked that this is not carved in stone, and direct data in humans is lacking.
Concluding, both structural and functional reasons may underlie the suggestion, from data in large cohorts of patients with HF, that GFR becomes quite RBF-dependent. This seems relevant in the perspective of selective renal vasodilator therapies.
Changes in neurohumoral control systems affecting renal function
This review does not provide a comprehensive list of all the factors that can contribute to alterations in GFR and RBF in heart failure. Instead, we will apply a classical framework: the triad RAS–SNS–extracellular volume.
First, the RAS is activated. At least three pathways are responsible for the activation of the RAS:
-
1.
Decreased systemic arterial pressure: If HF leads to a decrease in systemic and renal perfusion pressure, the RAS is activated in a classical way. It should be noted that both systemic and intrarenal levels of ANG II increase, and that renal angiotensinogen levels correlate with renal ANG II levels [52].
-
2.
Increased renal venous pressure (see below).
-
3.
Increased activity of the SNS
Second, the SNS is activated. The reasons for SNS activation in HF are also complex. Mechanisms leading to SNS activation partly overlap with the mechanisms activating the RAS:
-
1.
Decreased systemic arterial pressure, via the baroreceptor reflex
-
2.
Increased central stimulation of the SNS in the paraventricular nucleus (presumably by a combination of factors, increased ANG II, decreased NO, increased afferent renal sympathetic nerve activity) [53].
Increased SNS activity can affect renal function by increasing afferent arteriolar resistance, thereby decreasing RBF and GFR [54, 55]. If renal failure coexists, both the RAS and the SNS are inappropriately activated. This means that at normal blood pressure and normal volume status, there is increased renin release [56]. The SNS is activated by renal failure [57] and the baroreceptor curve is shifted to the right, indicating that at any blood pressure, sympathetic outflow is increased in renal patients compared to healthy controls; this effect seems to be strongly dependent upon ANG II [57]. The tight connection between the RAS and the SNS probably results in a vicious cycle in HF.
Third, volume control mechanisms will lead to extracellular volume expansion, and form the main reason for the congested state, eventually leading to further forward and backward failures. Besides the RAS and the SNS, both taking part in the volume retention, several other control mechanisms will function inappropriately:
-
1.
Decreased renal sensitivity to the natriuretic peptides lead to volume expansion. Levels of ANP, BNP, and CNP are elevated, yet there seems to be a renal insensitivity.
-
2.
Decreased levels of nitric oxide (NO) lead to volume expansion. NO leads to an integrated natriuretic response by decreasing tubular transport, and also decreases responsiveness of the TGF system [58].
-
3.
Increased adenosine A1 receptor activation leads to volume expansion. Adenosine A1 receptor activation can lead to a renal vasoconstriction [59, 60] and is probably the mediator of the TGF system [22, 23, 61]. Nevertheless, the hypothesis that targeting adenosine is beneficial for renal function is currently under strong dispute since clinical observations in patients with acute HF do not suggest any beneficial effect of adenosine A1 receptor blockade [62].
-
4.
Increased vasopressin-mediated volume control, leading to preferential water retention and hyponatremia [63]. It should be mentioned that ANG II can induce salt appetite and vasopressin release [64].
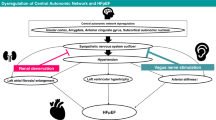
If one synthesizes this information, it seems that the RAS, SNS, and volume control, which are all intrinsically related, collectively disturb renal hemodynamic control. Figure 3 summarizes the role for the triad RAS–SNS–extracellular volume in determining GFR in HF.
Focus on renal venous hypertension and intratubular pressure
Several epidemiological and clinical studies have shown association between central venous pressure and eGFR in large cohorts, and have linked this to an increase in renal venous pressure [4]. Moreover, both paracentesis and ultrafiltration have been associated with a decrease in plasma creatinine [5]. The effect of volume removal was quite substantial, with a decrease in serum creatinine from about 3.4 to 2.4 mg/dL without significant changes in systemic hemodynamic measurements. A primary increase in renal venous pressure seems particularly relevant for observed changes in renal function in HF. As long ago as 1931, Winton observed in dogs the association of increased renal venous pressure with reduced RBF [65]. Later, renal venous pressure was shown to be elevated in subjects with HF [66]. In the last few years, there is revived interest for the importance of renal venous pressure. The mechanism is still under debate [67, 68]. Nevertheless, there is quite substantial literature to explain these observations.
From a theoretical point of view, an increase in renal venous pressure would decrease the arterio–venous pressure difference across the renal vasculature, which would lead to a decrease in RBF if resistances remained constant. Moreover, as all pressures within the renal bed would increase, glomerular pressure would also marginally increase. These events, however, would evoke an autoregulation response involving myogenic response and TGF, which would theoretically stabilize GFR. So, to a certain extent a perfectly functioning kidney should be able to stabilize the increase in renal venous pressure. In line with such a scenario is the observation that in dogs, GFR and RBF only decreased when RVP was substantially elevated [69]. Besides the consequences for the vascular pressure (gradients) in the renal vasculature, renal interstitial pressure would increase, because the interstitium has a low compliance and the kidney has a tight capsule. This will increase renal tubular pressure as a consequence and directly decrease the driving forces for GFR by decreasing the net hydrostatic pressure difference between the glomerular capillaries and the tubule. What do we know about the principal determinants of GFR upon an increase in RVP?
In a very beautiful study more than 50 years ago, the consequences of an increase in renal venous pressure for peritubular capillary and intratubular pressure were assessed [70]. Interestingly, the initial increase in pressure from about 0–15 mmHg did not result in any change in either peritubular capillary pressure or intratubular pressure. A further increase, though, resulted in a linear increase in pressure in both the tubules, and in small and larger capillaries. The transmission of the pressure increase to the tubules is of great importance: one of the main driving forces for filtration is affected, and directly decreases GFR. Furthermore, the only way this observation can be reconciled, is that the venous pressure raised interstitial pressure, which brings into play interstitial compliance and tubular compliance as factors as well. Several reports have indicated that GFR and RBF decrease when renal venous pressure is increased [65, 69, 71]. It should be stressed at this point that the decrease in GFR and the decrease in RBF have a different origin. The decrease in A–V pressure difference directly affects RBF but hardly GFR, the increase in intratubular pressure strongly affects GFR, but hardly affects RBF. Note that a strong decrease in GFR in the face of a mild decrease in RBF would result in a decreased FF, in this situation that could incorrectly be interpreted as a change in intrarenal resistances, i.e., a relatively large fall in efferent arteriolar resistance.
Few studies to our knowledge have directly assessed the consequences of renal venous pressure for autoregulation of RBF. De Wardener [72] reported that an isolated increase in renal venous pressure reduced RBF, but an increase in both renal venous pressure and arterial pressure was associated with a stable RBF. Later, this was put into further perspective: increasing renal interstitial pressure (and thereby renal venous pressure) decreased RBF, even in the presence of furosemide (to block TGF), renal decapsulation (to permit interstitial expansion), or inhibition of the SNS using phentolamine [73]. Taken together, it seems that increases in renal venous and interstitial pressure decrease RBF but also strongly affect the myogenic response. TGF does not seem to be critically involved.
Experimental models have indicated that both an increase in abdominal pressure [74] and in renal venous pressure [75, 76] lead to a prompt increase in plasma renin activity. One study in swine also reported an increase in aldosterone levels [71]. Although two observations used pressure increases in the range of 25–30 mmHg, which would be in the high pathophysiological range, the study by Kishimoto also observed increases in renin release at very mild increases in renal venous pressure [75]. Studies investigating the role of this increase in RAS activity for renal and systemic hemodynamics, and exploring the mechanisms involved in the RAS activation are not available.
Altogether, all of these data support the idea that renal venous pressure is an important determinant of renal hemodynamics and RAS activation. Renal venous pressure obviously becomes increased when there is a renal venous outflow obstruction or when any of the vascular beds downstream of the kidney has increased venous pressure. Factors determining renal venous pressure are summarized in Table 1 and consequences of increased renal venous pressure are summarized in Box 2.
Special case: renal artery stenosis
Renal artery stenosis comes with several consequences for the renal circulation. First of all, the kidney behind the stenosis can experience lower perfusion pressure. This will elicit several responses: (a) autoregulation induced afferent arteriolar vasodilation due to myogenic response and TGF deactivation, and (b) an increase in renin release due to decreased perfusion pressure per se, decreased macula densa sodium delivery, and increased efferent SNS traffic. The increased renin will constrict the afferent and the efferent arterioles. However, any effects on the afferent arteriole are likely minimal due to autoregulatory vasodilatation. Together, these adaptations are directed at maintaining that kidney’s GFR and RBF. Thus, if systemic blood pressure falls to low values in HF (or is reduced from hypertensive levels to normal), the stenotic kidney’s adjusting capacity is exhausted, and renal perfusion pressure (behind the stenosis) will fall below the lower limit of autoregulation. The severity of the stenosis is clearly relevant, although it could well be that a minimal stenosis, only discernable by an asymmetry in left to right RBF, already affects renal regulation of blood pressure [77]. The other aspect involves both the stenotic and the contralateral kidney: enhanced actions of ANG II will lead to sodium retention directly and indirectly due to aldosterone formation, with increased extracellular fluid volume as a consequence. While good experimental or clinical evidence is lacking, this may further aggravate the renal venous congestion in HF and compromise GFR and RBF.
Renal artery stenosis is frequent in patients with HF. In both the STAR [78] and ASTRAL trials [79], which compared the renal consequences of angioplasty versus medication, about 50% of the patients had coronary artery disease and 10% had HF. When specifically studied in patients with ARAS, LV morphology and function was seldom normal and about 75% had diastolic dysfunction [80]. In a small group of patients with combined heart and renal failure, prevalence of ARAS was above 50% [81]. Therefore, consideration of ARAS in HF patients seems relevant. Nevertheless, success of angioplasty for the improvement of blood pressure control or renal failure seems limited [78, 79]. In addition, the angioplasty procedure comes with significant morbidity. Studies have been underpowered to judge whether intervention in the renal artery could be of benefit for the heart [82]. Support for beneficial actions of angioplasty with respect to HF (and thereby for the pathophysiological relevance of ARAS) comes from a small retrospective cohort. In this study, patients with HF and ARAS who underwent angioplasty had better survival than patients who were medically treated [83]. While the presence of ARAS might well be relevant for the management of the patient with HF, the high complication rate of the procedure per se and the inability to identify the patients in which an intervention would clearly improve renal and cardiac functions, currently form an obstacle. The latter problem includes the current inability to identify patients where the kidney behind the stenosis is so severely damaged (due to long standing high blood pressure or due to ischemic nephropathy) that an intervention cannot be helpful. With all these issues in mind, a study about renal and cardiac functions in cardiorenal patients with ARAS would be warranted.
How do medications affect the renal circulation in chronic heart failure?
Pharmacological manipulation of the RAS
Renin inhibitors, ACE inhibitors, and angiotensin receptor antagonists are different strategies to inhibit the actions of the main effector pathway of the RAS, ANG II binding to the AT1 receptor, and thereby inhibition of downstream events [84]. As abundantly emphasized in recent reviews, renin inhibition decreases Ang I and ANG II, and supposedly thereby activation of all AT receptors, and possibly the Mas, Ang [1–7] receptor [84–87]. ACE inhibitors also decrease ANG II, but increase Ang I, which might leave the Mas receptor activation via ACE2 untouched [88], and increase accumulation of vasodilator kinins [89], which seems to be relevant in physiological [90] and pathophysiological conditions [91]. Finally, AT1 receptor antagonists obviously leave the other receptors untouched, but these are now exposed to high ANG II levels, because of the interruption of the negative feedback loop that normally limits renin transcription [92]. Despite the wide speculation and arousal about these differences, solid clinical evidence for significantly different actions of the various modes of RAS inhibition on renal hemodynamics in general and in HF is lacking. Therefore, we will limit the discussion to renal hemodynamic consequences of decreased ANG II, AT1 receptor-mediated actions irrespective of the applied pharmacological approach.
That being said, two questions are of importance. The first is what the consequences are of angiotensin inhibition for glomerular hemodynamics and renal autoregulation in HF? Table 2 lists the general actions of ANG II on the determinants of GFR and on TGF. There are a few remarks pertinent to HF. Inhibition of ANG II may lead to hypotension, to levels below the lower limit of autoregulation with a decrease in glomerular capillary pressure and GFR as a consequence. Furthermore, the high prevalence of ARAS in cardiac patients will frequently lead to a situation where afferent arteriolar vasodilation is insufficient to buffer a decrease in renal perfusion pressure. While ANG II inhibition does not affect the autoregulation process per se [93], it assists in aligning the autoregulation process around the prevailing renal perfusion pressures [94, 95]. It goes beyond the purpose of this paper to discuss in detail the difficult phenomenon that ANG II inhibition can cause a (slight) dissociation between the efficiency of GFR (poorer) and RBF (better) autoregulation [93], and the relevance of this in clinical conditions is not known. So, in short, ANG II inhibition can specifically cause a decrease in GFR by hypotension in particular in the presence of ARAS. The second question is to what extent the effects of elevated renal venous and renal interstitial pressure (and almost certainly tubular pressure) are mediated via the RAS in HF? Although several studies have indicated that renal venous hypertension increases renin release, this remains to be addressed.
Pharmacotherapy affecting the SNS with emphasis on beta blockade
Despite the fact that beta-blockers are widely used in HF, and renal dysfunction is prevalent, there are very few studies directly assessing renal hemodynamics upon beta-blockade initiation in HF. One study documented a slightly less pronounced decrease in GFR (using MDRD) upon carvedilol versus metoprolol [96]. No RBF was measured. Another study assessed the renal response to carvedilol in HF and found a marginal increase in RPF after 4 months treatment and a marginal decrease in GFR [97]. One study has reported a decrease in renal vascular resistance upon selective α blockade using prazosin in HF patients [98]. Renal vascular resistance tended to decrease in HF patients in one study [99]. Besides acting directly, beta-blockers consistently decrease plasma renin activity. One can conclude that 1) the number of studies precisely assessing renal function in HF upon manipulation of the SNS is extremely limited and 2) no consistent clear changes in renal function have been reported in the few studies available.
Pharmacologic control of extracellular fluid volume
Loop diuretics inhibit the Na+2Cl−K+-cotransporter, NKCC2, which, within the nephron, is expressed in the loop of Henle. This same Na+2Cl−K+-cotransporter is responsible for the sensing of sodium in the macula densa (at the end of the thick ascending limb) pivotal for both renin release and the TGF system [100]. Loop diuretics can affect renal hemodynamics in several ways:
-
Stimulation of renin release, activation of the RAS by inhibition of macula densa sodium transport, which would mimic a situation of low sodium delivery to the macula densa; this would elicit renin secretion (see above).
-
Activation or inhibition of the TGF system resulting in a decrease or an increase in GFR. Incomplete blockade of the macula densa transport, in concert with increased sodium delivery to the macula densa could increase TGF activity. Strong blockade of macula densa transport, however, could desensitize the macula densa and decrease TGF activity. Although it is unknown at which systemically applied dose of furosemide this occurs, one probably needs very substantial dosages to inhibit TGF significantly. Altogether, in the clinical setting effects of loop diuretics on TGF could both decrease or increase GFR, depending upon whether TGF sensing becomes inhibited.
-
Increased tubular pressure: in particular if there is already venous congestion, a further increase in tubular pressure would directly affect glomerular filtration pressure and decrease GFR.
-
Direct vasodilation: Loop diuretics inhibit the NKCC1 transporter, which is expressed widely outside the nephron. Inhibition of NKCC1 in the vasculature has been shown to result in vasodilation [101]. Afferent vasodilation has been convincingly shown to be independent from the TGF mechanism in the hydronephrotic in vitro perfused kidney model, which lacks a TGF response [102].
In an elegant study in rats, the team of Schnermann demonstrated the relevance of all of the above-mentioned mechanisms, except for TGF activation [101]. Furosemide dilated isolated afferent arterioles, however, decreased RBF in vivo. The latter was accompanied by increases in proximal tubular pressure; decapsulation, and RAS inhibition diminished the impact of furosemide on RBF. It will therefore not come as a great surprise that both decreases and increases in RBF and GFR have been reported in the literature.
A trial in stage IV HF patients with mild renal failure showed that patients maintained on a high water intake, the lower dose of furosemide in the study together with a low sodium intake had the highest number of adverse events, and had the most pronounced increase in aldosterone and BNP [103]. Patients were all treated with a low to intermediate dose of captopril and most of them with spironolactone 25 mg once a day. These results are hard to explain, other than that further volume expansion affected renal interstitial and renal venous pressures, i.e., CVP. The study illustrates how complex the response to salt, water and diuretics is in this patient group. Moreover, incomplete RAS and aldosterone blockade may have triggered the responses in BNP, due to volume retention. Indeed, more pronounced diuretic effects of furosemide have been reported in HF patients when they were receiving high doses, or really low doses of ACEi [104, 105]. To complicate the matter further, furosemide has direct systemic vasodilator properties [106], as mentioned, and dose-dependently diminishes the concentration gradient in the renal medulla, thus diminishing vasopressin-mediated water retention [107]. In this respect, the studies reporting that higher dosages of (loop) diuretics are associated with worse renal function are extremely hard to interpret. One would not use very high dosages of diuretics in a euvolemic state, and more extensive extracellular fluid volume expansion is associated with poorer cardiac function, more venous congestion etc. In a similar manner, an RCT would not be able to discriminate the patients, who would have a benefit for their GFR versus patients in whom renal function would be further compromised, unless it were specifically designed for that purpose. It is doubtful that simply calling loop diuretics “nephrotoxic” is going to be of any help for the treatment of individual patients. Rather, the physiological characterization of the cardiac patient should be improved to better predict the response to treatment with loop diuretics [108]. In that respect, two different issues still need a comment. The first is that when one compares the effects of ACE inhibitor therapy and other therapies, the functional (or cosmetic) decrease in GFR should not be confused with a real decline in renal function. This issue has been discussed elsewhere[109, 110].The other issue is that the current knowledge does not allow us to decide, whether continuous infusion versus bolus injection of furosemide is better for renal and cardiac outcome: one recent trial was unable to discriminate differences between continuous and bolus, and low and high dose of furosemide regarding outcome and renal function[111]. From a physiologic perspective, this is not surprising, if one does not stratify patients according to relevant parameters such as central venous pressure.
Regarding thiazides, direct renal hemodynamic consequences are not prominent, and are also not to be expected. A more recent study indicates that one year treatment with thiazide in hypertensives has no effect on RBF, GFR or serum creatinine [112]. However, there will be hemodynamic effects via activation of the RAS. It should be emphasized that thiazides induce the RAS mainly by inducing a decrease in extracellular fluid volume, and not by directly interacting with the control mechanisms of renin release. A head-to-head comparison of thiazides versus loop diuretics has not been done (and is complicated by the difference in natriuretic action) in HF patients. Because thiazides principally act beyond the macula densa, in principle, they interfere less with renal hemodynamics than loop diuretics.
Other pharmacologic approaches (calcium antagonists, adenosine A1 antagonists, AVP antagonists, and endothelin antagonists) and non-pharmacologic approaches
Precise reporting of renal hemodynamic effects of other strategies is scarce. Regarding calcium antagonists, minimal decreases in renal vascular resistance, and increases in RBF have been reported [113–115]. Despite the well-described adenosine A1 receptor-mediated renal vasoconstriction, also via the TGF system, A1 antagonism has clinically not been shown clearly to improve renal outcome. In one uncontrolled study, an improvement of renal function was observed as assessed by cystatin C, used as marker for GFR [116]. In a recent large placebo-controlled trial, however, worsening of renal failure was described during the first 7 days of treatment with the A1 antagonist rolofyline [62], and no clear benefit for overall outcome was reported. This is surprising, given the expectations from experimental studies. Vasopressin V2 receptor antagonists are an extremely interesting class of drugs in HF, since one could consider part of the volume retention the consequence of an appropriate stimulation of vasopressin. Although the V2 receptor probably does not play an important direct role in glomerular hemodynamics, V2 antagonism better preserved GFR than furosemide in rats with heart failure induced by cardiomyositis [117]. In humans, a V2 receptor antagonist did not affect GFR [118]. Finally, the enthusiasm for the use of endothelin antgonists in heart failure has declined considerably, since they are associated with volume retention and pulmonary edema [119] and liver function abnormalities.
This last section about therapeutic options considers non-pharmacological manipulation of water and sodium balance. From the above, it emerges that maneuvers to diminish extracellular fluid volume expansion are far from neutral in hemodynamic terms. Therefore, decreased intake of salt and water is an obvious therapeutic option. As mentioned above, one of the most systematic studies about diuretics, sodium and water intake has left us with many questions [103]. This study reported the most pronounced adverse (renal) outcome in the lower dose of furosemide and low sodium diet group, which can possibly only be explained by incomplete RAS blockade. Because of the difficulties associated with removal of excess fluid and water, follow-up studies are warranted.
Clinical translation and further research need
The key message of the present review is a call for application of clinical physiology to perform carefully designed studies to better understand the pathophysiology of renal failure coinciding with heart failure. We propose two strategies to view renal hemodynamics in heart failure. One is to analyze glomerular hemodynamics by systematically addressing (a) principal driving forces of glomerular filtration, (b) autoregulation, and (c) neurohumoral control mechanisms. The second is that both systemic and renal hemodynamics in HF are strongly determined by the triad RAS–SNS–volume control (Fig. 3).
All in all, a number of important questions regarding disturbed renal hemodynamics emerge regarding renal hemodynamics in patients with congestive HF.
-
1.
Pre-renal: Is ARAS more frequent in combined heart and renal failures than in CKD or HF separately? At which level does ARAS become relevant for the function of the kidneys in HF? Does resolution of ARAS improve cardiac function? Does ARAS accentuate the relations between renal venous pressure and GFR or RBF in patients with congestive heart failure?
-
2.
Intrarenal: Is a real cardio–renal connection existent, i.e., does HF result in induction or acceleration of renal disease? Does this have any specific characteristics? How do common pharmacological strategies (RAS inhibition, SNS inhibition, natriuretics/diuretics) alone or in combination affect principal determinants of GFR, autoregulation, and neurohumoral control mechanisms.
-
3.
Post-renal: Is renal venous pressure inversely related to GFR and RBF in patients with congestive heart failure? Are the characteristics of this relationship (slope and intercept) blunted (i.e., shifted down and to the left) by RAS blockade? Is intra-abdominal pressure inversely related to GFR and RBF in patients with congestive heart failure? Is there a direct relation between renal venous pressure and renal interstitial pressure in patients with congestive HF? Is there a direct relation between renal venous pressure and activity of the RAS (and SNS) in patients with congestive HF?
There is a beauty in evolving concepts around the consequences of heart failure for renal function and vice versa, in the sense that epidemiological and physiological approaches take turns in leading in new directions. The call is now for physiology.
References
Bongartz LG, Cramer MJ, Doevendans PA, Joles JA, Braam B (2005) The severe cardiorenal syndrome: ‘Guyton revisited’. Eur Heart J 26:11–17
Ronco C, Haapio M, House AA, Anavekar N, Bellomo R (2008) Cardiorenal syndrome. J Am Coll Cardiol 52:1527–1539
El Nahas M (2010) Cardio-kidney-damage: a unifying concept. Kidney Int 78:14–18
Damman K, van Deursen VM, Navis G, Voors AA, van Veldhuisen DJ, Hillege HL (2009) Increased central venous pressure is associated with impaired renal function and mortality in a broad spectrum of patients with cardiovascular disease. J Am Coll Cardiol 53:582–588
Mullens W, Abrahams Z, Francis GS et al (2009) Importance of venous congestion for worsening of renal function in advanced decompensated heart failure. J Am Coll Cardiol 53:589–596
Udani SM, Koyner JL (2010) The effects of heart failure on renal function. Cardiol Clin 28:453–465
Deen WM, Robertson CR, Brenner BM (1972) A model of glomerular ultrafiltration in the rat. Am J Physiol 223:1178–1183
Gabbai FB, Gushwa LC, Peterson OW, Wilson CB, Blantz RC (1987) Analysis of renal function in the two-kidney Goldblatt model. Am J Physiol 252:F131–F137
Schnermann J, Wright FS, Davis JM, von Stackelberg W, Grill G (1970) Regulation of superficial nephron filtration rate by tubulo-glomerular feedback. Pflugers Arch 318:147–175
Braam B, Navar LG, Mitchell KD (1995) Modulation of tubuloglomerular feedback by angiotensin II type 1 receptors during the development of Goldblatt hypertension. Hypertension 25:1232–1237
Oken DE (1982) An analysis of glomerular dynamics in rat, dog, and man. Kidney Int 22:136–145
Bayliss WM (1902) On the local reactions of the arterial wall to changes of internal pressure. J Physiol 28:220–231
Cupples WA, Braam B (2007) Assessment of renal autoregulation. Am J Physiol Renal Physiol 292:F1105–F1123
Just A, Arendshorst WJ (2003) Dynamics and contribution of mechanisms mediating renal blood flow autoregulation. Am J Physiol Regul Integr Comp Physiol 285:R619–R631
Siu KL, Sung B, Cupples WA, Moore LC, Chon KH (2009) Detection of low-frequency oscillations in renal blood flow. Am J Physiol Renal Physiol 297:F155–F162
Carmines PK, Inscho EW, Gensure RC (1990) Arterial pressure effects on preglomerular microvasculature of juxtamedullary nephrons. Am J Physiol 258:F94–F102
Loutzenhiser R, Bidani A, Chilton L (2002) Renal myogenic response: kinetic attributes and physiological role. Circ Res 90:1316–1324
Braam B, Mitchell KD, Koomans HA, Navar LG (1993) Relevance of the tubuloglomerular feedback mechanism in pathophysiology. J Am Soc Nephrol 4:1257–1274
Schnermann J, Traynor T, Yang T et al (1998) Tubuloglomerular feedback: new concepts and developments. Kidney Int Suppl 67:S40–S45
Vallon V (2003) Tubuloglomerular feedback and the control of glomerular filtration rate. News Physiol Sci 18:169–174
Kriz W (2004) Adenosine and ATP: traffic regulators in the kidney. J Clin Invest 114:611–613
Schnermann J, Weihprecht H, Briggs JP (1990) Inhibition of tubuloglomerular feedback during adenosine1 receptor blockade. Am J Physiol 258:F553–F561
Sun D, Samuelson LC, Yang T et al (2001) Mediation of tubuloglomerular feedback by adenosine: evidence from mice lacking adenosine 1 receptors. Proc Natl Acad Sci U S A 98:9983–9988
Leyssac PP, Karlsen FM, Holstein-Rathlou NH, Skott O (1994) On determinants of glomerular filtration rate after inhibition of proximal tubular reabsorption. Am J Physiol 266:R1544–R1550
Skott P, Hommel E, Bruun NE, Arnold-Larsen S, Parving HH (1989) The acute effect of acetazolamide on glomerular filtration rate and proximal tubular reabsorption of sodium and water in normal man. Scand J Clin Lab Invest 49:583–587
Carmines PK, Morrison TK, Navar LG (1986) Angiotensin II effects on microvascular diameters of in vitro blood-perfused juxtamedullary nephrons. Am J Physiol 251:F610–F618
Carmines PK, Perry MD, Hazelrig JB, Navar LG (1987) Effects of preglomerular and postglomerular vascular resistance alterations on filtration fraction. Kidney Int Suppl 20:S229–S232
Mitchell KD, Braam B, Navar LG (1992) Hypertensinogenic mechanisms mediated by renal actions of renin-angiotensin system. Hypertension 19:I18–I27
Braam B, Koomans HA (1996) Renal responses to antagonism of the renin-angiotensin system. Curr Opin Nephrol Hypertens 5:89–96
DiBona GF, Sawin LL (2004) Effect of renal denervation on dynamic autoregulation of renal blood flow. Am J Physiol Renal Physiol 286:F1209–F1218
Rudenstam J, Bergstrom G, Taghipour K, Gothberg G, Karlstrom G (1995) Efferent renal sympathetic nerve stimulation in vivo. Effects on regional renal haemodynamics in the Wistar rat, studied by laser-Doppler technique. Acta Physiol Scand 154:387–394
DiBona GF, Kopp UC (1997) Neural control of renal function. Physiol Rev 77:75–197
Takabatake T (1982) Feedback regulation of glomerular filtration rate in the denervated rat kidney. Kidney Int Suppl 12:S129–S135
Hermansson K, Kallskog O, Wolgast M (1984) Effect of renal nerve stimulation on the activity of the tubuloglomerular feedback mechanism. Acta Physiol Scand 120:381–385
Martinez-Rumayor A, Richards AM, Burnett JC, Januzzi JL Jr (2008) Biology of the natriuretic peptides. Am J Cardiol 101:3–8
Levin ER, Gardner DG, Samson WK (1998) Natriuretic peptides. N Engl J Med 339:321–328
Gaillard CA, Koomans HA, Mees EJ (1988) Enalapril attenuates natriuresis of atrial natriuretic factor in humans. Hypertension 11:160–165
Nishikimi T, Miura K, Minamino N, Takeuchi K, Takeda T (1994) Role of endogenous atrial natriuretic peptide on systemic and renal hemodynamics in heart failure rats. Am J Physiol 267:H182–H186
Baylis C, Harton P, Engels K (1990) Endothelial derived relaxing factor controls renal hemodynamics in the normal rat kidney. J Am Soc Nephrol 1:875–881
Baylis C, Mitruka B, Deng A (1992) Chronic blockade of nitric oxide synthesis in the rat produces systemic hypertension and glomerular damage. J Clin Invest 90:278–281
Zatz R, de Nucci G (1991) Effects of acute nitric oxide inhibition on rat glomerular microcirculation. Am J Physiol 261:F360–F363
Kramp RA, Fourmanoir P, Ladriere L et al (2000) Effects of Ca(2+) channel activity on renal hemodynamics during acute attenuation of NO synthesis in the rat. Am J Physiol Renal Physiol 278:F561–F569
Kramp R, Fourmanoir P, Caron N (2001) Endothelin resets renal blood flow autoregulatory efficiency during acute blockade of NO in the rat. Am J Physiol Renal Physiol 281:F1132–F1140
Turkstra E, Braam B, Koomans HA (2000) Impaired renal blood flow autoregulation in two-kidney, one-clip hypertensive rats is caused by enhanced activity of nitric oxide. J Am Soc Nephrol 11:847–855
Shi Y, Wang X, Chon KH, Cupples WA (2006) Tubuloglomerular feedback-dependent modulation of renal myogenic autoregulation by nitric oxide. Am J Physiol Regul Integr Comp Physiol 290:R982–R991
Braam B, Koomans HA (1995) Reabsorption of nitro-l-arginine infused into the late proximal tubule participates in modulation of TGF responsiveness. Kidney Int 47:1252–1257
Braam B, Koomans HA (1995) Nitric oxide antagonizes the actions of angiotensin II to enhance tubuloglomerular feedback responsiveness. Kidney Int 48:1406–1411
Haas GJ, Leier CV (2009) Are hemodynamic parameters predictors of mortality? Heart Fail Clin 5:229–240
Cody RJ, Ljungman S, Covit AB et al (1988) Regulation of glomerular filtration rate in chronic congestive heart failure patients. Kidney Int 34:361–367
Smilde TD, Damman K, van der Harst P et al (2009) Differential associations between renal function and “modifiable” risk factors in patients with chronic heart failure. Clin Res Cardiol 98:121–129
Robertson CR, Deen WM, Troy JL, Brenner BM (1972) Dynamics of glomerular ultrafiltration in the rat. 3. Hemodynamics and autoregulation. Am J Physiol 223:1191–1200
Schunkert H, Tang SS, Litwin SE et al (1993) Regulation of intrarenal and circulating renin-angiotensin systems in severe heart failure in the rat. Cardiovasc Res 27:731–735
Patel KP (2000) Role of paraventricular nucleus in mediating sympathetic outflow in heart failure. Heart Fail Rev 5:73–86
Myers BD, Deen WM, Brenner BM (1975) Effects of norepinephrine and angiotensin II on the determinants of glomerular ultrafiltration and proximal tubule fluid reabsorption in the rat. Circ Res 37:101–110
Fleming JT, Zhang C, Chen J, Porter JP (1992) Selective preglomerular constriction to nerve stimulation in rat hydronephrotic kidneys. Am J Physiol 262:F348–F353
Weidmann P, Beretta-Piccoli C, Steffen F, Blumberg A, Reubi FC (1976) Hypertension in terminal renal failure. Kidney Int 9:294–301
Ligtenberg G, Blankestijn PJ, Oey PL et al (1999) Reduction of sympathetic hyperactivity by enalapril in patients with chronic renal failure. N Engl J Med 340:1321–1328
Braam B (1999) Renal endothelial and macula densa NOS: integrated response to changes in extracellular fluid volume. Am J Physiol 276:R1551–R1561
Navar LG (1998) Integrating multiple paracrine regulators of renal microvascular dynamics. Am J Physiol 274:F433–F444
Osswald H, Spielman WS, Knox FG (1978) Mechanism of adenosine-mediated decreases in glomerular filtration rate in dogs. Circ Res 43:465–469
Osswald H, Hermes HH, Nabakowski G (1982) Role of adenosine in signal transmission of tubuloglomerular feedback. Kidney Int Suppl 12:S136–S142
Massie BM, O’Connor CM, Metra M et al (2010) Rolofylline, an adenosine A1-receptor antagonist, in acute heart failure. N Engl J Med 363:1419–1428
Oghlakian G, Klapholz M (2009) Vasopressin and vasopressin receptor antagonists in heart failure. Cardiol Rev 17:10–15
Fitzsimons JT (1998) Angiotensin, thirst, and sodium appetite. Physiol Rev 78:583–686
Winton FR (1931) The influence of venous pressure on the isolated mammalian kidney. J Physiol 72:49–61
Maxwell MH, Breed ES, Schwartz IL (1950) Renal venous pressure in chronic congestive heart failure. J Clin Invest 29:342–348
Jessup M, Costanzo MR (2009) The cardiorenal syndrome: do we need a change of strategy or a change of tactics? J Am Coll Cardiol 53:597–599
Joles JA, Bongartz LG, Gaillard CA, Braam B (2009) Renal venous congestion and renal function in congestive heart failure. J Am Coll Cardiol 54:1632; author reply 1632–1633
Blake WD, Wegria R et al (1949) Effect of increased renal venous pressure on renal function. Am J Physiol 157:1–13
Gottschalk CW, Mylle M (1956) Micropuncture study of pressures in proximal tubules and peritubular capillaries of the rat kidney and their relation to ureteral and renal venous pressures. Am J Physiol 185:430–439
Doty JM, Saggi BH, Sugerman HJ et al (1999) Effect of increased renal venous pressure on renal function. J Trauma 47:1000–1003
Semple SJ, De Wardener HE (1959) Effect of increased renal venous pressure on circulatory autoregulation of isolated dog kidneys. Circ Res 7:643–648
Clausen G, Oien AH, Aukland K (1992) Myogenic vasoconstriction in the rat kidney elicited by reducing perirenal pressure. Acta Physiol Scand 144:277–290
Gudmundsson FF, Gislason HG, Myking OL, Viste A, Grong K, Svanes K (2002) Hormonal changes related to reduced renal blood flow and low urine output under prolonged increased intra-abdominal pressure in pigs. Eur J Surg 168:178–186
Kishimoto T, Maekawa M, Abe Y, Yamamoto K (1973) Intrarenal distribution of blood flow and renin release during renal venous pressure elevation. Kidney Int 4:259–266
Bloomfield GL, Blocher CR, Fakhry IF, Sica DA, Sugerman HJ (1997) Elevated intra-abdominal pressure increases plasma renin activity and aldosterone levels. J Trauma 42:997–1004, discussion 1004–1005
van Onna M, Houben AJ, Kroon AA et al (2003) Asymmetry of renal blood flow in patients with moderate to severe hypertension. Hypertension 41:108–113
Bax L, Woittiez AJ, Kouwenberg HJ et al (2009) Stent placement in patients with atherosclerotic renal artery stenosis and impaired renal function: a randomized trial. Ann Intern Med 150(840–8):W150–W151
Wheatley K, Ives N, Gray R et al (2009) Revascularization versus medical therapy for renal-artery stenosis. N Engl J Med 361:1953–1962
Wright JR, Shurrab AE, Cooper A, Kalra PR, Foley RN, Kalra PA (2005) Left ventricular morphology and function in patients with atherosclerotic renovascular disease. J Am Soc Nephrol 16:2746–2753
Emans ME, Van Der Putten K, Velthuis BK et al (2009) High prevalence of atherosclerotic renal artery stenosis in the cardiorenal syndrome; negative association with diabetes mellitus posterpresentatie. European Society of Cardiology, Barcelona
Kalra PA (2010) Renal revascularization for heart failure in patients with atherosclerotic renovascular disease. Nephrol Dial Transplant 25:661–663
Kane GC, Xu N, Mistrik E, Roubicek T, Stanson AW, Garovic VD (2009) Renal artery revascularization improves heart failure control in patients with atherosclerotic renal artery stenosis. Nephrol Dial Transplant 25:813–820
Wolf G (2008) Novel aspects of the renin-angiotensin-aldosterone-system. Front Biosci 13:4993–5005
Danser AH (2007) Novel drugs targeting hypertension: renin inhibitors. J Cardiovasc Pharmacol 50:105–111
Ma TK, Kam KK, Yan BP, Lam YY (2010) Renin-angiotensin-aldosterone system blockade for cardiovascular diseases: current status. Br J Pharmacol 160:1273–1292
Muller DN, Luft FC (2008) Renin receptor blockade: a better strategy for renal protection than renin-angiotensin system inhibition? Curr Hypertens Rep 10:405–409
Burns KD (2007) The emerging role of angiotensin-converting enzyme-2 in the kidney. Curr Opin Nephrol Hypertens 16:116–121
Erdos EG, Yang HY (1967) An enzyme in microsomal fraction of kidney that inactivates bradykinin. Life Sci 6:569–574
Pellacani A, Brunner HR, Nussberger J (1994) Plasma kinins increase after angiotensin-converting enzyme inhibition in human subjects. Clin Sci (Lond) 87:567–574
Cruden NL, Witherow FN, Webb DJ, Fox KA, Newby DE (2004) Bradykinin contributes to the systemic hemodynamic effects of chronic angiotensin-converting enzyme inhibition in patients with heart failure. Arterioscler Thromb Vasc Biol 24:1043–1048
Haddad G, Amiri F, Garcia R (1997) Modulation of renal glomerular angiotensin II receptors by ace inhibition and AT1 receptor antagonism. Regul Pept 68:111–117
Rosivall L, Youngblood P, Navar LG (1986) Renal autoregulatory efficiency during angiotensin-converting enzyme inhibition in dogs on a low sodium diet. Ren Physiol 9:18–28
Cupples WA (1993) Angiotensin II conditions the slow component of autoregulation of renal blood flow. Am J Physiol 264:F515–F522
Sorensen CM, Leyssac PP, Skott O, Holstein-Rathlou NH (2000) Role of the renin-angiotensin system in regulation and autoregulation of renal blood flow. Am J Physiol Regul Integr Comp Physiol 279:R1017–R1024
Ito H, Nagatomo Y, Kohno T, et al (2010) Differential effects of carvedilol and metoprolol on renal function in patients with heart failure. Circ J 74:1578–1583
Heitmann M, Davidsen U, Stokholm KH, Rasmussen K, Burchardt H, Petersen EB (2002) Renal and cardiac function during alpha1-beta-blockade in congestive heart failure. Scand J Clin Lab Invest 62:97–104
Preston RA, O’Connor DT, Stone RA (1979) Prazosin and renal hemodynamics: arteriolar vasodilation during therapy of essential hypertension in man. J Cardiovasc Pharmacol 1:277–286
Magorien RD, Hermiller JB, Unverferth DV, Leier CV (1985) Regional hemodynamic effects of clonidine in congestive heart failure. J Cardiovasc Pharmacol 7:91–96
Schlatter E, Salomonsson M, Persson AE, Greger R (1989) Macula densa cells sense luminal NaCl concentration via furosemide sensitive Na+2Cl-K+ cotransport. Pflugers Arch 414:286–290
Oppermann M, Hansen PB, Castrop H, Schnermann J (2007) Vasodilatation of afferent arterioles and paradoxical increase of renal vascular resistance by furosemide in mice. Am J Physiol Renal Physiol 293:F279–F287
Wang X, Breaks J, Loutzenhiser K, Loutzenhiser R (2007) Effects of inhibition of the Na+/K+/2Cl− cotransporter on myogenic and angiotensin II responses of the rat afferent arteriole. Am J Physiol Renal Physiol 292:F999–F1006
Paterna S, Parrinello G, Cannizzaro S et al (2009) Medium term effects of different dosage of diuretic, sodium, and fluid administration on neurohormonal and clinical outcome in patients with recently compensated heart failure. Am J Cardiol 103:93–102
Good JM, Brady AJ, Noormohamed FH, Oakley CM, Cleland JG (1994) Effect of intense angiotensin II suppression on the diuretic response to furosemide during chronic ACE inhibition. Circulation 90:220–224
Motwani JG, Fenwick MK, Morton JJ, Struthers AD (1992) Furosemide-induced natriuresis is augmented by ultra-low-dose captopril but not by standard doses of captopril in chronic heart failure. Circulation 86:439–445
Dikshit K, Vyden JK, Forrester JS, Chatterjee K, Prakash R, Swan HJ (1973) Renal and extrarenal hemodynamic effects of furosemide in congestive heart failure after acute myocardial infarction. N Engl J Med 288:1087–1090
Beck FX, Sone M, Dorge A, Thurau K (1992) Effect of loop diuretics on organic osmolytes and cell electrolytes in the renal outer medulla. Kidney Int 42:843–850
MacFadyen RJ, Ng Kam Chuen MJ, Davis RC (2010) Loop diuretic therapy in left ventricular systolic dysfunction: has familiarity bred contempt for a critical but potentially nephrotoxic cardio renal therapy? Eur J Heart Fail 12:649–652
Slagman MC, Navis G, Laverman GD (2010) Reversible effects of diuretics added to renin-angiotensin-aldosterone system blockade: impact on interpretation of long-term kidney function outcome. Am J Kidney Dis 56:601–602
Bakris GL, Weir MR (2000) Angiotensin-converting enzyme inhibitor-associated elevations in serum creatinine: is this a cause for concern? Arch Intern Med 160:685–693
Felker GM, Lee KL, Bull DA et al (2011) Diuretic strategies in patients with acute decompensated heart failure. N Engl J Med 364:797–805
Sihm I, Thygesen K, Krusell LR, Lederballe O (2000) Long-term renal and cardiovascular effects of antihypertensive treatment regimens based upon isradipine, perindopril and thiazide. Blood Press 9:346–354
Walsh JT, Andrews R, Curtis S, Evans A, Cowley AJ (1997) Effects of amlodipine in patients with chronic heart failure. Am Heart J 134:872–878
Drexler H, Depenbusch JW, Truog AG, Zelis R, Flaim SF (1985) Effects of diltiazem on cardiac function and regional blood flow at rest and during exercise in a conscious rat preparation of chronic heart failure (myocardial infarction). Circulation 71:1262–1270
Binetti G, Rubino I, Varani E et al (1989) Felodipine in severe chronic congestive heart failure: acute effects on central hemodynamics and regional blood flow distribution. Cardiovasc Drugs Ther 3:903–911
Mitrovic V, Seferovic P, Dodic S et al (2009) Cardio-renal effects of the A1 adenosine receptor antagonist SLV320 in patients with heart failure. Circ Heart Fail 2:523–531
Veeraveedu PT, Watanabe K, Ma M et al (2008) Effects of V2-receptor antagonist tolvaptan and the loop diuretic furosemide in rats with heart failure. Biochem Pharmacol 75:1322–1330
Costello-Boerrigter LC, Boerrigter G, Cataliotti A, Harty GJ, Burnett JC Jr (2010) Renal and anti-aldosterone actions of vasopressin-2 receptor antagonism and B-type natriuretic peptide in experimental heart failure. Circ Heart Fail 3:412–419
Mathier MA, Ishizawar D (2010) Bosentan. Expert Opin Pharmacother 11:1023–1034
Hall JE, Coleman TG, Guyton AC, Kastner PR, Granger JP (1981) Control of glomerular filtration rate by circulating angiotensin II. Am J Physiol 241:R190–R197
Acknowledgments
Branko Braam is a New Investigator supported by the Heart and Stroke Foundation of Canada. This work has also been supported by a grant from the Dutch Heart Foundation. Current work on renal hemodynamics by Drs. Cupples and Braam is supported by the Canadian Institute of Health Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Braam, B., Cupples, W.A., Joles, J.A. et al. Systemic arterial and venous determinants of renal hemodynamics in congestive heart failure. Heart Fail Rev 17, 161–175 (2012). https://doi.org/10.1007/s10741-011-9246-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-011-9246-2