Abstract
Our aim was to study whether there is causal association between serum uric acid and metabolic syndrome (MetS). A cross-sectional study was performed, including a total of 27,009 subjects (23,345 subjects having uric acid data) from the Dongfeng-Tongji Cohort study. The MetS was defined by the International Diabetes Foundation criteria of 2005. Association analysis was performed by logistic regression. A genetic risk score was calculated by adding the uric acid increasing alleles in two SNPs (rs11722228 in SLC2A9 and rs2231142 in ABCG2) which were identified from our genome-wide association study on uric acid levels. The causal association was examined by mendelian randomization analysis. Among a middle- and old-age Chinese population, serum uric acid concentrations were strongly associated with the risk of MetS and its several components (P < 0.0001). The effects were stronger in women than in men. Despite the lack of statistical significance, both SNPs exhibited a trend with increased MetS risk (rs11722228, OR = 1.06, 95 % CI 0.99–1.14; rs2231142, OR = 1.02, 95 % CI 0.95–1.10), consistent with their increasing uric acid effects. Each additional uric acid increasing allele in the genetic risk score was associated with 3 % increased MetS risk (OR = 1.03, 95 % CI 0.98–1.09; P = 0.23). Further adjustment for serum uric acid attenuated the trend of individual SNP and genetic risk score with increased MetS risk (all OR < 1.0). These findings suggested that serum uric acid was associated with MetS risk in a middle- and old-age Chinese population. Whether this association was causal remained to be investigated in the future studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The metabolic syndrome (MetS) is characterized by a clustering of cardiovascular risk factors including abdominal obesity, elevated blood pressure, increased glucose levels, and dyslipidaemia. The prevalence of MetS has been increasing rapidly in the world. In the United States, the prevalence is estimated to be 27 % (25.2 % in men and 29 % in women) [1]; in China, the age-standardized prevalence of MetS was 9.8 % in men and 17.8 % in women [2] based on the data from a cross-sectional survey conducted in 2000–2001. MetS is related to an increased risk of diabetes, cardiovascular diseases, and kidney diseases [3–5], as well as an increased risk for mortality from cardiovascular diseases and all-cause mortality [6].
Hyperuricemia, the precursor of gout, is associated with a wide range of diseases including MetS [7–9]. Both cross-sectional [10, 11] and prospective studies [12–15] have consistently shown that uric acid levels were associated with the risk of MetS. Experimental studies also indicated that uric acid might play a role in insulin resistance [16], promoting secretion of inflammatory factors [17] and adipocytokine [18]. Evidence also suggested that uric acid might play a causal role in the fructose-induce MetS [19]. However, whether the uric acid has the causal effects on MetS still remained to be investigated [20]. In the present study, we used the baseline data of the Dongfeng-Tongji Cohort (DFTJ cohort) study [21] including 27,009 individuals to investigate the association between serum uric acid levels and MetS risk. Furthermore, we used the uric acid related SNPs which were identified in our genome wide association study (GWAS) as instruments to explore whether there were causal associations between uric acid levels and the risk of MetS.
Subjects and methods
Study population
The DFTJ cohort study was launched in 2008 among retirees of Dongfeng Motor Corporation (DMC) in Shiyan City, Hubei province [21]. DMC was founded in 1969 and is one of the 3 largest auto manufacturers in China. Between 2008 and 2010, we recruited 87 % (n = 27,009 out of 31,000) of retired employees who agreed to answer the questionnaires and provided baseline blood samples. Data allowing the determination of the status of MetS was available for 25,134 of the participants. Among them, after exclusion participants with age younger than 50 years old (n = 663) or those with missing serum uric acid levels (n = 1,169), 23,345 individuals (10,649 men, 12,696 women) having serum uric acid data were included in our analytic samples. The socio-demographic characteristics were similar between participants included in the present study and those excluded. The study has been approved by the Medical Ethics Committee of the School of Public Health, Tongji Medical College, and Dongfeng General Hospital, DMC. All participants provided written informed consent.
Data collection
Baseline data were collected by trained interviewers via semi-structured questionnaires during face-to-face interviews. Information on socio-demographic factors, health status, and lifestyle was included in the questionnaires. The general health examination was performed at the same time. Standing height, body weight, and waist circumference were measured with participants in light indoor clothing and without shoes. Body mass index (BMI) was calculated as weight in kilograms divided by height in meters squared.
All subjects were examined in the morning after overnight fasting. For each individual, fifteen miniliters of fasting blood were drawn and distributed into three tubes: two ethylenediaminetetraacetic acid anticoagulant tubes for plasma and DNA, and a coagulation tube for serum. Uric acid, creatinine, triglyceride, total cholesterol, low density lipoprotein (LDL) cholesterol, high density lipoprotein (HDL) cholesterol, and blood glucose levels were measured by the hospital’s laboratory with ARCHITECT Ci8200 automatic analyzer (ABBOTT Laboratories. Abbott Park, Illinois, USA) using the Abbott Diagnostics reagents according to the instructions of the manufacturer.
Assessment of uric acid and covariates
Serum uric acid levels were categorized into five groups according to the quintiles of gender-specific distribution: <261, 261–300, 301–338, 339–389 and ≥390 μmol/l for men; <207, 207–240, 241–274, 275–318, and ≥319 μmol/l for women, respectively. According to the respondents’ self-reported smoking status, participants were grouped as current smokers, ex-smokers, and nonsmokers. Based on the self-reported drinking status, participants were classified as current drinkers, ex-drinkers, and nondrinkers. The amount of meat and seafood intake was assessed according to the following formula: frequency (times per week) × the amount of each time (gram). The frequency of alcohol consumption was assessed as <1 servings/week, 2–4 servings/week, 5–7 servings/week, 8–10 servings/week, and >10 servings/week. Other variables were dichotomized as yes or no on the basis of the responses to questions on physical activity, past history of coronary heart diseases (CHD), diabetes and hypertension, and the use of lipid and/or blood pressure lowering drugs and diuretics.
Genotyping
Two SNPs (rs11722228 and rs2231142) mapping to two genes (SLC2A9 and ABCG2) were genotyped in 7,827 subjects with the iPLEX system (Sequenom, San Diego, USA) in 384-well format. These two SNPs were previously reported to be associated with serum uric acid levels both in Asians [22] and Europeans [23, 24] and were also validated in our GWAS and proved to be associated with serum uric acid independently (unpublished data). Finally, genotyping failed 36 (0.5 %) and 0 for SNPs rs11722228 and rs2231142, respectively owing to DNA quantity or quality. The two SNPs were in Hardy-Weinberg equilibrium (P > 0.05).
Definition of metabolic syndrome
We used the International Diabetes Foundation (IDF) criteria of 2005 [25] to define the MetS in the present study. These criteria are similar to the modified US National Cholesterol Education Program’s Adult Treatment Panel III criteria (NCEP) [26]. The IDF definition of MetS includes central obesity (waist circumference ≥90 cm in Chinese men and ≥80 cm in Chinese women) plus any 2 of the following 4 factors: (1) high blood pressure: systolic ≥130 mm Hg, diastolic ≥85 mm Hg, or known treatment for hypertension; (2) hypertriglyceridemia: fasting serum triglycerides ≥1.7 mmol/l; (3) low HDL cholesterol: fasting HDL cholesterol <1.0 mmol/l in men and <1.3 mmol/l in women; and (4) hyperglycemia: fasting glucose level of ≥5.6 mmol/l (≥100 mg/dl) or known treatment for diabetes.
Data analysis
All statistical analyses were performed using SPSS 13.0 software. The Quanto software package was used for statistical power calculation [27]. Categorical variables were expressed in percentages and continuous variables in mean ± SD unless otherwise specified. We computed the simple and multivariable adjusted odds ratios (ORs) and 95 % confidence intervals (CIs) for the MetS and its components using the logistic regression. In the multivariable model, we adjusted for age (continuous), gender (male, female) plus smoking (never smoking, quit smoking, smoking), drinking (never drinking, quit drinking, drinking), physical activity (yes/no), and concentrations of creatinine (continuous). We used the simple count method to calculate the genetic risk score. For associations of individual SNP or the genetic score with MetS, analyses were further adjusted for uric acid to examine whether the associations of individual SNP or genetic risk score with MetS was mediated by their effects on uric acid levels. The attenuation of the associations between the SNPs or genetic risk score with MetS risk after adjustment for uric acid suggested the potential causal association between uric acid and MetS [28]. We calculated the expected effect sizes (βE) of the individual SNP or genetic risk score on MetS risk based on the effect sizes of individual SNP or genetic score on uric acid (βGB) and the effect sizes of uric acid on MetS (βBD). The formula is βE = βGB × βBD, as previously reported [29]. The differences between expected effects sizes of individual SNP or genetic score on MetS and observed effect sizes were compared by student’s t test [30]. A two-sided P value <0.05 was considered significant.
Results
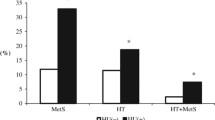
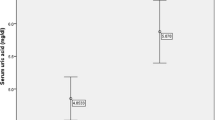
A total of 23,345 individuals (10,649 men, 12,696 women) were included in this study. The prevalence of MetS in our sample was 31.0 % in the total sample, 22.9 % in men, and 37.8 % in women. The mean (SD) of concentrations of uric acid was 328.2(81.5) μmol/l for males and 265.7 (72.9) μmol/l in females. The prevalence of the MetS raised from 17.4 % among the individuals with concentrations of serum uric acid <261 μmol in males and <207 μmol/l in females to 45.8 % among those with concentrations ≥390 μmol/l in males and ≥319 μmol/l in females (Fig. 1). Characteristics of the study population according to quintiles of serum uric acid levels were summarized in Table 1. Individuals with higher levels of uric acid were less likely to be current smokers and have higher levels of blood pressure, waist circumstance, BMI, fasting glucose, triglyceride, total cholesterol, LDL, and creatinine, and, lower HDL levels. Also, individuals with higher serum uric acid have higher prevalence of hypertension, type 2 diabetes, and CHD as well as higher percentage of medications use (lipid lowering drugs, blood pressure lowering drugs, and diuretics).
Prevalence (95 % CI) of the metabolic syndrome by quintiles of serum uric acid concentration among 23,345 participants. The quintiles of serum uric acid concentration were calculated by gender respectively. In male, the cutoff of serum uric acid concentration is <261, 261–300, 301–338, 339–389, and ≥390 μmol/l respectively; in female, the concentration of serum uric acid is <207, 207–240, 241–274, 275–318, and ≥319 μmol/l, respectively
Associations between serum uric acid levels and MetS
The association between serum uric acid levels and MetS was displayed in Table 2. Individuals in the highest uric acid quintile had higher odds of MetS compared with individuals in the lowest quintile (Q5 vs. Q1: OR, 3.69 [95 % CI: 3.35–4.06]; P for trend <0.0001) after adjustment for age and sex. Further adjustment for lifestyle parameters including smoking, drinking, physical activity, and creatinine levels did not materially change the association (Q5 vs. Q1: 3.68 [3.34–4.05]; P for trend <0.0001). Additional adjustment for the past history (yes/no) of hypertension, type 2 diabetes, CHD, and medication history got the similar results. When uric acid was entered in the model as a continuous variable, the fully adjusted OR was 1.005 (95 % CI: 1.004–1.005) per 1 μmol/l or 1.33 (95 % CI: 1.30–1.36) per 59.4 μmol/l (1 mg/dl). The statistical power to demonstrate OR equals to 1.33 per 1 mg/dl increase in uric acid was more than 99 %. We further used the modified NCEP criteria [26] to define the MetS and investigate the association of serum uric acid with MetS risk, the results were similar with the IDF criteria (Supplementary Table 1). The association in women was stronger than in men, and significant interaction with sex was found (P for interaction <0.0001). Exclusion of participants using diuretic and uric-acid-lowering drugs (n = 596; 2.55 % of all participants) did not materially changed the results. Individuals in the highest uric acid quintile had higher odds of MetS compared with the individuals in the lowest quintile (Q5 vs. Q1: OR = 3.02, 95 % CI: 2.73–3.35; P for trend <0.0001) after full adjustment (data not shown).
Associations between serum uric acid levels and MetS components
We further examined the associations between serum uric acid levels and MetS components (Table 3). The serum uric acid levels were significantly associated with five individual components of MetS after adjustment for age, sex, smoking, drinking, physical activity, and creatinine levels (P for trend <0.0001). Additional adjustment for the other components of the MetS reduced the effects of uric acid on individual component but still remained significant (P for trend <0.0001).
Associations between uric acid levels related SNPs and MetS risk
In our GWAS of serum uric acid in 1,452 individuals from DFTJ-cohort we replicated the associations between variants in genes of SLC2A9 and ABCG2 with uric acid concentrations which were reported in Asians and Europeans before [24, 31–33] (unpublished data). In the present study we then genotyped the two SNPs (rs11722228 in SLC2A9 and rs2231142 in ABCG2) that were independently associated with uric acid levels in our GWAS. As Table 4 showed, the effect sizes of individual SNP on uric acid ranged from 0.202 to 0.226 mg/dl (11.0–13.4 μmol/l). Each additional uric acid-increasing allele in the genetic risk score was associated with 0.218 (95 % CI 0.188–0.247) mg/dl [12.9 (95 % CI 11.2–14.7) μmol/l] (P = 1.98 × 10−47) uric acid. In order to investigate the causal association of uric acid levels and MetS, we further explored the associations of the two SNPs with MetS risk. Unfortunately, we did not find significant associations of the two SNPs with MetS risk, however, the two SNPs showed a trend with increased risk of MetS, directionally consistent with their increasing uric acid effects (OR range 1.02–1.06; Table 4; Supplementary Table 2). We then used the genetic risk score to calculate the combination of risk alleles of the two SNPs. Each additional uric acid increasing allele in the genetic risk score was associated with 3 % increased risk of MetS (OR = 1.03, 95 % CI 0.98–1.09; P = 0.23). However, compared with those without risk alleles, individuals with 4 genetic score had 1.99-fold increased risk of MetS (95 % CI 1.22–3.27, P = 0.006; Supplementary Table 3). The associations of individual SNP or genetic risk score with the risk of MetS were not different from the expected associations based on the observed associations between these SNPs (or genetic score) and serum uric acid levels and the association between uric acid levels and MetS (P range 0.11–0.80; Table 4).
Discussion
In the present study we found a graded positive association between serum uric acid and the prevalence of MetS. This association was stronger in females than in males. The mendelian randomization analysis provided limited support for the causal association between serum uric acid levels and the risk of MetS. This might be due to the relative small sample size and limited statistical power in the present study.
The findings that increased serum uric acid levels associated with increased risk of MetS were in accordance with previous studies including cross-sectional [10, 11] and prospective studies [12–15, 20]. In addition, in the present study the association of uric acid levels and MetS risk was more robust among women than men, consistently with the previous reported findings [10, 13, 14]. Future investigations are needed to examine the underlying mechanisms of the sex-related association between serum uric acid levels and MetS risk.
Although the epidemiology studies [10–15, 20] consistently found the positive associations between serum uric acid and MetS and the animal study indicated that uric acid had a cause role in the fructose-induced MetS, using of uric acid-lowering medications such as benzbromarone and allopurinol could reduce the blood pressure, TG and insulin levels, and body weight [19], however, whether the uric acid has the causal effects on MetS still remained to be investigated [20]. Cause-and-effect relationship between biomarkers and diseases such as the serum uric acid levels and MetS risk can be studied using the mendelian randomization analysis [34], which is based on the random assortment of alleles/genotypes transferred from parent to offspring at the time of gamete formation [35]. For the mendelian randomization analysis, three conditions must be fulfilled [28]. First, uric acid associated variants (instrumental variable) must be associated with the exposure variable of the serum uric acid. In the present study, the two independent SNPs of rs11722228 and rs2231142 were associated with uric acid levels and explained 1.03 and 1.09 % of the total variation of serum uric acid levels, respectively; Also, the serum uric acid levels were associated with increased MetS risk (Tables 2, 4); therefore, the two variants of uric acid could serve as instruments in a mendelian randomization study. Second, genetic variants must be independent of confounders. As supplementary Table 4 showed, no associations were found for genetic risk score with these confounders (P value = 0.36–0.68). Finally, the individual SNP and genetic risk score of uric acid must not affect MetS risk by other pathways except for serum uric acid. In the present study, the two SNPs showed a trend with increased Mets risk and further adjustment for serum uric acid attenuated this trend. In addition, the associations of the individual SNP (or the genetic risk score) with the risk of MetS were not different from the expected associations. However, the lack of statistical significance between the genetic variants of uric acid and the MetS risk did not lend the evidences for the causal association between the serum uric acid levels and Mets. This might be due to the small contribution of each SNP to the total variation of the serum uric acid levels. For example, the two SNPs of rs11722228 and rs2231142 explained 1.03 and 1.09 % of the total variation of serum uric acid levels, respectively. In addition, although the present study had more than 99 % power to detect the OR which equals to 1.25 of the individual SNP associated with the MetS risk; however, it had only 71.4 % statistical power when the OR equals to 1.10. The present study had limited power to detect the minor effects of the individual SNP (OR ranged from 1.02 to 1.06) on the MetS risk. Studies with larger sample size are warranted to validate the results. Although we did not provide solid evidence for the causal role of serum uric acid on the development of MetS, the expected direction of a null association might provide new clue for the future studies. Studies with larger sample size or a meta-analysis combined studies that were directionally concordant but statistically null findings will enable us to achieve a conclusion about whether there was a causal association of uric acid with MetS.
Several limitations in the present study need to be considered. First, this is a cross-sectional study and more cohort studies are warranted to validate our results. Second, the population stratification might bias our results. However, our study population is highly homogeneous by including only Chinese population. Third, our analyses were restricted to the middle- and old-age population and therefore may not be generalized to young people (<50 years old). Fourth, biological compensation (canalization) by other genes during development should be considered when we used the mendelian randomization analysis to infer causal relationship. However, canalization is difficult to be assessed and we are not aware of any such potential effects.
In summary, there was a graded positive association between serum uric acid and the MetS risk in a middle- and old-age Chinese population. The mendelian randomization analysis lent limited evidences for the causal roles of serum uric acid on the development of MetS. Further studies are warranted to validate these findings.
References
Ford ES, Giles WH, Mokdad AH. Increasing prevalence of the metabolic syndrome among U.S. Adults. Diabetes Care. 2004;27(10):2444–9.
Gu D, Reynolds K, Wu X, et al. Prevalence of the metabolic syndrome and overweight among adults in China. Lancet. 2005;365(9468):1398–405.
Isomaa B, Almgren P, Tuomi T, et al. Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care. 2001;24(4):683–9.
Haffner SM, Valdez RA, Hazuda HP, et al. Prospective analysis of the insulin-resistance syndrome (syndrome X). Diabetes. 1992;41(6):715–22.
Chen J, Muntner P, Hamm LL, et al. The metabolic syndrome and chronic kidney disease in U.S. adults. Ann Intern Med. 2004;140(3):167–74.
Trevisan M, Liu J, Bahsas FB, et al. Syndrome X and mortality: a population-based study. Risk factor and life expectancy research group. Am J Epidemiol. 1998;148(10):958–66.
Ford ES, Li C, Cook S, et al. Serum concentrations of uric acid and the metabolic syndrome among US children and adolescents. Circulation. 2007;115(19):2526–32.
Siu YP, Leung KT, Tong MK, et al. Use of allopurinol in slowing the progression of renal disease through its ability to lower serum uric acid level. Am J Kidney Dis. 2006;47(1):51–9.
Tuttle KR, Short RA, Johnson RJ. Sex differences in uric acid and risk factors for coronary artery disease. Am J Cardiol. 2001;87(12):1411–4.
Chiou WK, Wang MH, Huang DH, et al. The relationship between serum uric acid level and metabolic syndrome: differences by sex and age in Taiwanese. J Epidemiol. 2010;20(3):219–24.
Nan H, Qiao Q, Soderberg S, et al. Serum uric acid and components of the metabolic syndrome in non-diabetic populations in Mauritian Indians and Creoles and in Chinese in Qingdao, China. Metab Syndr Relat Disord. 2008;6(1):47–57.
Ryu S, Song J, Choi BY, et al. Incidence and risk factors for metabolic syndrome in Korean male workers, ages 30 to 39. Ann Epidemiol. 2007;17(4):245–52.
Sui X, Church TS, Meriwether RA, et al. Uric acid and the development of metabolic syndrome in women and men. Metabolism. 2008;57(6):845–52.
Yang T, Chu CH, Bai CH, et al. Uric acid level as a risk marker for metabolic syndrome: a Chinese cohort study. Atherosclerosis. 2012;220(2):525–31.
Zhang Q, Zhang C, Song X, et al. A longitudinal cohort based association study between uric acid level and metabolic syndrome in Han Chinese urban population. BMC Public Health. 2012;12(1):419.
Chen LK, Lin MH, Lai HY, et al. Uric acid: a surrogate of insulin resistance in older women. Maturitas. 2008;59(1):55–61.
Kanellis J, Watanabe S, Li JH, et al. Uric acid stimulates monocyte chemoattractant protein-1 production in vascular smooth muscle cells via mitogen-activated protein kinase and cyclooxygenase-2. Hypertension. 2003;41(6):1287–93.
Tamba S, Nishizawa H, Funahashi T, et al. Relationship between the serum uric acid level, visceral fat accumulation and serum adiponectin concentration in Japanese men. Intern Med. 2008;47(13):1175–80.
Nakagawa T, Hu H, Zharikov S, et al. A causal role for uric acid in fructose-induced metabolic syndrome. Am J Physiol Renal Physiol. 2006;290(3):F625–31.
Santos RD. Elevated uric acid, the metabolic syndrome and cardiovascular disease: cause, consequence, or just a not so innocent bystander? Endocrine. 2012;41(3):350–2.
Wang F, Zhu J, Yao P, et al. Cohort profile: the Dongfeng-Tongji cohort study of retired workers. Int J Epidemiol. 2012;. doi:10.1093/ije/dys053.
Kamatani Y, Matsuda K, Okada Y, et al. Genome-wide association study of hematological and biochemical traits in a Japanese population. Nat Genet. 2010;42(3):210–5.
Wallace C, Newhouse SJ, Braund P, et al. Genome-wide association study identifies genes for biomarkers of cardiovascular disease: serum urate and dyslipidemia. Am J Hum Genet. 2008;82(1):139–49.
Dehghan A, Kottgen A, Yang Q, et al. Association of three genetic loci with uric acid concentration and risk of gout: a genome-wide association study. Lancet. 2008;372(9654):1953–61.
Alberti KG, Zimmet P, Shaw J. The metabolic syndrome—a new worldwide definition. Lancet. 2005;366(9491):1059–62.
Grundy SM, Cleeman JI, Daniels SR, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation. 2005;112(17):2735–52.
Gauderman W, Morrison J (2006) QUANTO 1.1: a computer program for power and sample size calculations for genetic-epidemiology studies. http://hydra.usc.edu/gxe.
Lawlor DA, Harbord RM, Sterne JA, et al. Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med. 2008;27(8):1133–63.
Li S, Zhao JH, Luan J, et al. Genetic predisposition to obesity leads to increased risk of type 2 diabetes. Diabetologia. 2011;54(4):776–82.
Freathy RM, Timpson NJ, Lawlor DA, et al. Common variation in the FTO gene alters diabetes-related metabolic traits to the extent expected given its effect on BMI. Diabetes. 2008;57(5):1419–26.
Vitart V, Rudan I, Hayward C, et al. SLC2A9 is a newly identified urate transporter influencing serum urate concentration, urate excretion and gout. Nat Genet. 2008;40(4):437–42.
Yamagishi K, Tanigawa T, Kitamura A, et al. The rs2231142 variant of the ABCG2 gene is associated with uric acid levels and gout among Japanese people. Rheumatology (Oxford). 2010;49(8):1461–5.
Woodward OM, Kottgen A, Coresh J, et al. Identification of a urate transporter, ABCG2, with a common functional polymorphism causing gout. Proc Natl Acad Sci USA. 2009;106(25):10338–42.
Smith GD, Ebrahim S. Mendelian randomization: prospects, potentials, and limitations. Int J Epidemiol. 2004;33(1):30–42.
Didelez V, Sheehan N. Mendelian randomization as an instrumental variable approach to causal inference. Stat Methods Med Res. 2007;16(4):309–30.
Acknowledgments
The authors would like to thank all study subjects for participating in the present DFTJ-cohort study as well as all volunteers for assisting in collecting the samples and data. This work was supported by the grant from the National Natural Science Foundation (grant NSFC-81172751 and NSFC-30711120579) and Program for the New Century Excellent Talents in University for Meian He.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dai, X., Yuan, J., Yao, P. et al. Association between serum uric acid and the metabolic syndrome among a middle- and old-age Chinese population. Eur J Epidemiol 28, 669–676 (2013). https://doi.org/10.1007/s10654-013-9829-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-013-9829-4