Summary
The microtubule-targeting agents derived from natural products, such as vinca-alkaloids and taxanes are an important family of efficient anti-cancer drugs with therapeutic benefits in both haematological and solid tumors. These drugs interfere with the assembly of microtubules of α/β tubulin heterodimers without altering their expression level. The aim of the present study was to investigate the effect of thymoquinone (TQ), a natural product present in black cumin seed oil known to exhibit putative anti-cancer activities, on α/β tubulin expression in human astrocytoma cells (cell line U87, solid tumor model) and in Jurkat cells (T lymphoblastic leukaemia cells). TQ induced a concentration- and time-dependent degradation of α/β tubulin in both cancer cell types. This degradation was associated with the up-regulation of the tumor suppressor p73 with subsequent induction of apoptosis. Interestingly, TQ had no effect on α/β tubulin protein expression in normal human fibroblast cells, which were used as a non-cancerous cell model. These data indicate that TQ exerts a selective effect towards α/β tubulin in cancer cells. In conclusion, the present findings indicate that TQ is a novel anti-microtubule drug which targets the level of α/β tubulin proteins in cancer cells. Furthermore, they highlight the interest of developing anti-cancer therapies that target directly tubulin rather than microtubules dynamics.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Microtubules, the major cytoskeleton components in cells, are composed of α/β tubulin subunits. This structure is considered as one of the best targets in cancer chemotherapy [1]. Several natural compounds can target and inhibit successfully the normal function of microtubules [2]. The vinca-alkaloids and the taxanes are among the most important anti-microtubule drugs [2]. Indeed, microtubule-targeting drugs (MTDs) interfere with the assembly of microtubules of α/β tubulin heterodimers without altering their expression level [3]. Although MTDs have clinical therapeutic benefits against haematological and solid tumors, the development of resistance to these drugs, their specificity towards tumors, and the induction of neutropenia, myeloid and neurological toxicities are the major problems observed during their clinical applications [4–10]. Deficiency of MTDs-induced apoptotic pathways in different cancers has been suggested as a mechanism of resistance to these drugs [11]. In this context, it has been suggested that p53 might be a guardian of microtubules composition and that mutations in p53 are likely to contribute to the development of resistance to MTDs [11]. Thus, increasing the tissue specificity, reducing the side effects, especially the peripheral neuropathy and leukopenia, are major objectives in the current research for new MTDs.
Many studies have shown that thymoquinone (TQ), a natural product present in black cumin seed oil with anti-inflammatory and anti-cancer activities, is a potent cytotoxic agent against many types of human cancer cells [12, 13]. It has been reported that TQ exerts its anti-cancer effects through the inhibition of cell growth, cell cycle arrest with subsequent apoptosis [14–17]. TQ can induce apoptosis in cancer cells by p53-dependent and -independent pathways [12, 16]. The TQ-induced apoptosis in p53-null myeloblastic leukemia and human osteosarcoma cells involves an increase in the Bax/Bcl2 ratio and the activation of caspases [18, 19]. Recently, we have shown that TQ induces apoptosis in acute lymphoblastic leukemia cell line (Jurkat cells), a p53-deficient cell line, through activation of the tumor suppressor p73, the structural and functional homolog of p53, which targets the anti-apoptotic protein UHRF1 (Ubiquitin-like PHD Ring Finger 1) [12]. Unlike p53, which is mutated in 50% of cancer cells, the mutations of the p73 gene are very rare (less than 1%), making it as an alternative strategy for anti-cancer treatment, especially for those where p53 is deficient or mutated [20, 21]. Indeed, several studies have proposed that p73 is a novel promising target for cancer therapy [22–26].
The present study has indicated that TQ induces the degradation of α/β tubulin in human astrocytoma cells (cell line U87) and in the p53-deficient Jurkat cell line. This degradation is associated with p73 up-regulation in both cancer cell lines. Interestingly, TQ had no effect on α/β tubulin protein level in normal human fibroblast cells. Altogether, the present findings suggest that TQ is a new MTD exhibing specificity towards cancer cells.
Material and methods
Cell culture and treatment
The human astrocytoma cells (line U87, WHO grade IV) and human T lymphocyte cell line Jurkat were obtained from the America Type Culture Collection (Mannassa, VA, USA). Cell lines were maintained in a humidified incubator with 5% CO2 at 37°C, and were grown in EMEM (Biowhitaker, Lonza, Belgium) for human astrocytoma cells and RPMI 1640 (Sigma-Aldrich, St-Louis, MO) for Jurkat cells and human fibroblast cells. Both media were supplemented with 15% (v/v) fetal calf serum (FCS, Biowhitaker,), 2 mM glutamine, 100 U/ml penicillin and 50 mg/ml streptomycin (Sigma St. Louis, MO). For all treatments, a 100 mM solution of TQ (Sigma–Aldrich, St) was prepared in 100% DMSO (Dimethylsulfoxide; Millipore S.A.S., Molsheim, France) and appropriate working concentrations were prepared with cell culture medium. The final concentration of DMSO was less than 0.1% in both control and treated conditions.
Western blot analysis
Cells were treated with TQ at different concentrations and incubated for the indicated time. Cells were then harvested and centrifuged at 200 g for 5 min at room temperature. The pellets were resuspended in RIPA buffer (25 mM Tris pH 7.6, 150 mM NaCl, 1% NP-40, 1% sodium deoxycholate, 0.1% SDS) containing different protease inhibitors (Sigma-Aldrich) and incubated on ice for 20 min. The cell suspensions were then sonicated three times (30 s each) and the supernatants containing the proteins were collected after centrifugation at 10,000 g for 16 min at 4°C. The protein concentration was determined by the Bradford assay (Bio-Rad, Marnes la Coquette, France). Proteins were separated on 10% SDS-polyacrylamide gels and transferred to PVDF membranes (Millipore, Saint Quentin en Yvelines, France), as previously described [27]. Immunoblot was performed using either a mouse monoclonal anti-β tubulin antibody (Sigma–Aldrich), a purified monoclonal anti-α tubulin (Clone 10D8) antibody (Biolegend, San Diago, CA), a mouse monoclonal anti-p73 antibody (BD Biosciences Pharmingen), a mouse monoclonal anti-UHRF1 antibody (Proteogenix, Oberhausbergen, France), or a mouse monoclonal anti-β actin antibody (Abcam, Paris, France), according to the manufacturer’s instructions.
Apoptosis assay
For detection of apoptosis, the annexin V-binding capacity of treated cells was examined using the annexin V Binding Guava Nexin® Assay by capillary cytometry (Guava Easycyte Plus HP system, with absolute cell count and six parameters) following the manufacturer’s recommendations (Guava Technologies Inc, Hayward, CA, USA). Guava Nexin® Assay utilizes annexin V-Phycoerythrin (PE) to detect phosphatidylserine (PS) on the external membrane of apoptotic cells. The cell impermeant dye, 7-Amino-Actinomycin (7AAD), is used in the Guava Nexin® Assay as an indicator of cell membrane structural integrity. 7-AAD is excluded from viable cells as well as early apoptotic cells. Jurkat cells were seeded into 6-multiwell plates at a density of 2 × 106 cells/well, grown for 24 h and exposed to TQ at different concentrations for 24 h. Jurkat cells were stained directly in the 96-well microplate with 100 μl of Guava Nexin Reagent, a pre-made cocktail containing annexin V-PE and 7-AAD in buffer, in 200 μl final volume. After 20 min incubation at room temperature, the samples were analysed using Guava® System.
Statistical analysis
Data are presented in a bar graph form, expressed as means ± SEM from at least three independent experiments. Statistical analyses were performed using the one-way ANOVA. Significance levels were defined as **, P < 0.01; ***, P < 0.001 (versus the corresponding untreated group).
Results
TQ induces a concentration-dependent degradation of α/β tubulin associated with p73 up-regulation in human astrocytoma cells (line U87)
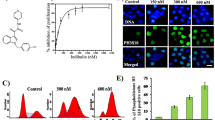
We first investigated the effect of TQ on α/β tubulin and p73 proteins in human astrocytoma cells (line U87 MG, Fig. 1). For this purpose, human astrocytoma cells were exposed to different concentrations of TQ for 24 h. We observed that TQ induces a concentration-dependent α/β tubulin down-regulation in U87 MG cells (Fig. 1). Indeed, TQ at 100 μM caused a pronounced decrease in α tubulin level, while β tubulin was undetectable (Fig. 1). TQ-induced α/β tubulin degradation in astrocytoma cells was associated with a concentration-dependent p73 up-regulation which started at 50 μM suggesting that α/β tubulin degradation is a downstream effect of p73 up-regulation in the mechanism of action of TQ. These results show that TQ induced α/β tubulin down-regulation associated with the up-regulation of p73 in human astrocytoma cells (line U87).
Effects of TQ on α/β tubulin and p73 expression in human astrocytoma cells (cell line U87). Cells were exposed to TQ at the indicated concentration and incubated for 24 h. Immunoblot analyses were performed as described in “Material and methods” with different antibodies. Specific bands were detected with their expected apparent molecular weight. All membranes were reblotted with an anti β actin probe to ensure equal protein loading and transfer. The data are representative of at least three independent experiments
TQ induces a concentration- and time-dependent degradation of α/β tubulin in acute lymphoblastic leukaemia cells (Jurkat cell line)
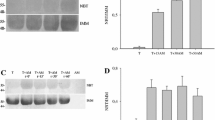
We have investigated the effect of TQ on the expression of α/β tubulin in the p53-deficient Jurkat cell line. Figure 2a shows that TQ induced β tubulin down-regulation and the appearance of a lower molecular weight form of α tubulin starting at 10 μM. Interestingly, at 50 μM of TQ, α/β tubulin protein level became undetectable (Fig. 2a). The apoptotic effect of TQ in Jurkat cells was also studied under the same experimental conditions. Cells were exposed to different concentration of TQ for 24 h and then apoptosis was assessed as described in “Material and methods”. As shown in Fig. 2b, increasing concentrations of TQ induced an increasing number of apoptotic cells. TQ began to trigger apoptosis at 10 μM, a concentration where α/β tubulin proteins were down-regulated. TQ at 50 μM, induced approximately apoptosis of 90% of cells (Fig. 2b), a response which was associated with a total loss of α/β tubulin proteins (Fig. 2a). In our previous study we have shown that p73 is expressed at a low level in untreated Jurkat cells and that TQ induced a marked up-regulation of its expression starting at concentrations of or greater than 10 μM [12]. Taken together, these results indicate that TQ like in human astrocytoma cells induced α/β tubulin down-regulation in acute lymphoblastic leukaemia cells and that this effect is associated with activation of the tumor suppressor p73 leading subsequently to apoptosis.
Effects of TQ on α/β tubulin expression and apoptosis in Jurkat cells. a Cells were exposed to TQ at different concentrations and incubated for 24 h. Immunoblot analyses were performed as described in “Material and methods” with different antibodies. The data are representative of at least three independent experiments. b Cell apoptosis rate was assessed by capillary cytometry using the annexin V-Phycoerythrin (PE) and 7-Amino-Actinomycin (7AAD) staining assay. Events in each of the four quadrants were: Lower-left quadrant: viable cells, not undergoing detectable apoptosis (Annexin V-PE negative and 7-AAD negative cells). Lower-right quadrant: cells in the early stage of apoptosis (Annexin V-PE positive and 7-AAD negative cells). Upper right quadrant: cells in the late apoptotic or dead (Annexin V-PE positive and 7-AAD positive cells, their number, expressed as percentage relative to the total cell number, is indicated on the right). Upper-left quadrant: mostly nuclear debris (Annexin V-PE negative and 7-AAD positive). The data are representative of at least three independent experiments
TQ has no effect on α/β tubulin protein expression in normal human fibroblast cells as compared to Jurkat cells
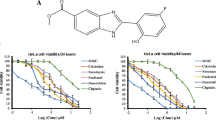
In order to determine the chronology of the molecular events induced by TQ leading to down-regulation of α/β tubulin proteins, we analyzed the time-course effect of TQ in Jurkat cells at 50 μM (concentration at which α/β tubulin proteins were completely depleted, Fig. 2a). Figure 3a shows that TQ induced a rapid α/β tubulin down-regulation in Jurkat cells at 3 h associated with a p73 up-regulation, this decrease in the α/β tubulin level was more pronounced at 6 h. In the next step, we have investigated the effect of TQ on α/β tubulin protein in normal human fibroblast cells as a non-cancerous cell model (Fig. 3b). Interestingly, in the same conditions, TQ had no effect on α/β tubulin protein expression in normal human fibroblast cells (Fig. 3b), even after 12 h of treatment (data not shown). All these findings indicate that TQ degrades α/β tubulin proteins in Jurkat cells without affecting their level in normal human fibroblast cells.
Time-course of the effects of TQ on α/β tubulin and p73 expression in Jurkat cells and in normal human fibroblast cells. Jurkat cells (a) and normal human fibroblast cells (b) were exposed to 50 μM of TQ for the indicated times. a, b show representative immunoblots. Similar observations were made in three independent experiments
Discussion
Because of their essential role in cell proliferation, microtubules are considered as one of the best targets for the development of anti-cancer drugs [2, 28]. It has been suggested that targeting tubulin level directly without manipulating microtubules dynamics could be an additional approach to induce apoptosis in cancer cells [28]. In the present study, we evaluated the effect of TQ on α/β tubulin protein level in human astrocytoma cells (line U87) and in p53-deficient acute lymphoblastic leukaemia cell line (Jurkat cells). Our results showed that TQ induces a concentration- and time-dependent degradation of α/β tubulin associated with the up-regulation of tumor suppressor p73 in both cancer cell lines. In human astrocytoma cells, TQ induced α/β tubulin down-regulation at 100 μM while in Jurkat cells this effect started at 10 μM suggesting that leukaemia cells are more sensitive to TQ than astrocytoma cells. Interestingly, TQ had no effect on the expression of α/β tubulin protein in normal human fibroblast cells as compared to Jurkat cells. The human astrocytoma cell line (U87 MG) is a high-grade invasive form of astrocytic brain tumors with a mean survival time of less than 1 year. As microtubules are essential components for cell division and intracellular transport, it is reasonable to suggest that α/β tubulin degradation which was observed in TQ-treated human astrocytoma cells is likely to limit tumor cells’ invasiveness. Indeed, previous studies have shown that TQ reduced colon tumor cell invasion as well as significantly inhibited the invasion of lung cancer cell [29, 30]. Presently, we dont have an explanation why TQ selectively induced α/β tubulin degradation in cancer cells without affecting their level in normal cells. Since α/β tubulin proteins are essential for cell proliferation, it is possible that because cancer cells multiply rapidly they are more sensitive to TQ compared to normal-growing cells. In agreement with such a hypothesis, we observed that TQ induced a dramatic decrease in the expression of UHRF1, an anti-apoptotic protein, which is over-expressed in numerous cancers and essential for cell proliferation [12, 13] in Jurkat cells without affecting its level in normal human fibroblast cells (Fig. 1A-B, supplementary data). Since previous studies have shown that TQ induces p73 up-regulation-dependent UHRF1 down-regulation [12, 14] and that UHRF1 down-regulation induces cell cycle arrest in G2/M and apoptosis [31], it is likely that TQ-induced p73 up-regulation in the present study leads to UHRF1 and α/β tubulin degradation resulting ultimately in extensive apoptosis. Although the present study indicates that α/β tubulin proteins are selectively degraded in human astrocytoma cells and leukaemia cells, the mechanism underlying the inhibitory effect of TQ remains to be clarified. Some studies have shown that MTDs such as paclitaxel (taxol) can induce caspase-independent mitotic death (CIMD) by up-regulating of p73 but not its homolog p53 [32–35]. In addition, high concentrations of TQ also induced the up-regulation of p73 with the subsequent induction of apoptosis independently of caspase 3 activation in Jurkat cells [12]. Thus, TQ might be able to induce the degradation of α/β tubulin proteins through a caspase-independent pathway, which is activated by the up-regulation of p73. Furthermore, isothiocyanates (ITCs), one of the best chemopreventive small molecules, have been shown to induce a selective degradation of α/β tubulin and that this degradation is initiated by their interaction resulting in the ubiquitination of α/β tubulin and their subsequent degradation by the proteasome [36]. It has also been shown that the small molecule T0070907 (a PPAR inhibitor) is able to decrease the protein level of α/β tubulin by activation of the proteasome pathway [37]. Since TQ is a small drug-like molecule [38, 39], it is likely that TQ decreases α/β tubulin level in cancer cells by increasing the rate of proteasomal degradation rather than by interfering with its synthesis. The present findings suggest that TQ is an attractive MTD with potent anticancer-activity, associated to low cytotoxic effects on normal human cells and which also has anti-inflammatory and neuroprotective activities as well as a sensitizing effect on cancer cells resistant to chemotherapy [15, 40–44]. In conclusion, we have shown that TQ causes in cancer cells α/β tubulin degradation associated with p73 up-regulation. These data support the idea that small molecules can be used to decrease α/β tubulin levels, and suggest that TQ might act as a novel and potent anti-microtubule drug.
References
Zhou J, Giannakakou P (2005) Targeting microtubules for cancer chemotherapy. Curr Med Chem Anticancer Agent 5:65–71. doi:10.2174/1568011053352569
Jordan MA, Wilson L (2004) Microtubules as a target for anticancer drugs. Nat Rev Cancer 4:253–265. doi:10.1038/nrc1317
Dumontet C, Jordan MA (2010) Microtubule-binding agents: a dynamic field of cancer therapeutics. Nat Rev Drug Discov 9:790–803. doi:10.1038/nrd3253
Huisman MT, Chhatta AA, van Tellingen O, Beijnen JH, Schinkel AH (2005) MRP2 (ABCC2) transports taxanes and confers paclitaxel resistance and both processes are stimulated by probenecid. Int J Cancer 116:824–829. doi:10.1002/ijc.21013
Hopper-Borge E, Chen ZS, Shchaveleva I, Belinsky MG, Kruh GD (2004) Analysis of the drug resistance profile of multidrug resistance protein 7 (ABCC10): resistance to docetaxel. Cancer Res 64:4927–4930. doi:10.1158/0008-5472.CAN-03-3111
Canta A, Chiorazzi A, Cavaletti G (2009) Tubulin: a target for antineoplastic drugs into the cancer cells but also in the peripheral nervous system. Curr Med Chem 16:1315–1324
Argyriou AA, Koltzenburg M, Polychronopoulos P, Papapetropoulos S, Kalofonos HP (2008) Peripheral nerve damage associated with administration of taxanes in patients with cancer. Crit Rev Oncol Hematol 66:218–228. doi:10.1016/j.critrevonc.2008.01.008
Vats T, Buchanan G, Mehta P, Ragab A, Hvizdale E, Nitschke R, Link M, Beardsley GP, Maybee D, Krischer J (1992) A study of toxicity and comparative therapeutic efficacy of vindesine-prednisone vs. vincristine-prednisone in children with acute lymphoblastic leukemia in relapse. Invest New Drugs 10:231–234
Bellmunt J, Théodore C, Demkov T, Komyakov B, Sengelov L, Daugaard G, Caty A, Carles J, Jagiello-Gruszfeld A, Karyakin O, Delgado FM, Hurteloup P, Winquist E, Morsli N, Salhi Y, Culine S, von der Maase H (2009) Phase III trial of vinflunine plus best supportive care compared with best supportive care alone after a platinum-containing regimen in patients with advanced transitional cell carcinoma of the urothelial tract. J Clin Oncol 27:4454–4461. doi:10.1200/JCO.2008.20.5534
Mielke S, Sparreboom A, Mross K (2006) Peripheral neuropathy: a persisting challenge in paclitaxel-based regimes. Eur J Cancer 42:24–30. doi:10.1016/j.ejca.2005.06.030
Galmarini CM, Kamath K, Vanier-Viornery A, Hervieu V, Peiller P, Falette N, Puisieux A, Ann Jordan M, Dumontet C (2003) Drug resistance associated with loss of p53 involves extensive alterations in microtubule composition and dynamics. Br J Cancer 88:1793–1799. doi:10.1038/sj.bjc.6600960
Alhosin M, Abusnina A, Achour M, Sharif T, Muller CM, Peluso JP, Chataigneau T, Lugnier C, Schini-Kerth VB, Bronner C, Fuhrmann G (2010) Induction of apoptosis by thymoquinone in lymphoblastic leukemia Jurkat cells is mediated by a p73-dependent pathway which targets the epigenetic integrator UHRF1. Biochem Pharmacol 79:1251–1260. doi:10.1016/j.bcp.2009.12.015
Alhosin M, Sharif T, Mousli M, Etienne-Selloum N, Fuhrmann G, Schini-Kerth VB, Bronner C (2011) Down-regulation of UHRF1, associated with re-expression of tumor suppressor genes, is a common feature of natural compounds exhibiting anti-cancer properties. J Exp Clin Cancer Res 30:41. doi:10.1186/1756-9966-30-41
Abusnina A, Alhosin M, Keravis T, Muller CM, Fuhrmann G, Bronner C, Lugnier C (2011) Down-regulation of cyclic nucleotide phosphodiesterase PDE1A is the key event of p73 and UHRF1 deregulation in thymoquinone-induced acute lymphoblastic leukemia cell apoptosis. Cell Signal 23:152–160. doi:10.1016/j.cellsig.2010.08.015
Banerjeea S, Padhyea S, Azmia A, Wanga Z, Philipa PA, Kucukb O, Sarkara FH, Mohammada RM (2010) Review on Molecular and Therapeutic Potential of Thymoquinone in Cancer. Nutrition and Cancer 62:938–946. doi:10.1080/01635581.2010.509832
Gali-Muhtasib H, Roessner A, Schneider-Stock R (2006) Thymoquinone: a promising anti-cancer drug from natural sources. Int J Biochem Cell Biol 38:1249–1253. doi::10.1016/j.biocel.2005.10.009
Shoieb AM, Elgayyar M, Dudrick PS, Bell JL, Tithof PK (2003) In vitro inhibition of growth and induction of apoptosis in cancer cell lines by thymoquinone. Int J Oncol 22:107–113
El-Mahdy MA, Zhu Q, Wang QE, Wani G, Wani AA (2005) Thymoquinone induces apoptosis through activation of caspase-8 and mitochondrial events in p53-null myeloblastic leukemia HL-60 cells. Int J Cancer 117:409–417. doi:10.1002/ijc.21205
Roepke M, Diestel A, Bajbouj K, Walluscheck D, Schonfeld P, Roessner A, Schneider-Stock R, Gali-Muhtasib H (2007) Lack of p53 augments thymoquinone-induced apoptosis and caspase activation in human osteosarcoma cells. Cancer Biol Ther 6:160–169. doi:10.4161/cbt.6.2.3575
Irwin MS, Kaelin WG (2001) Role of the newer p53 family proteins in malignancy. Apoptosis 6:17–29. doi:10.1023/A:1009663809458
Melino G, De Laurenzi V, Vousden KH (2002) p73: Friend or foe in tumorigenesis. Nat Rev Cancer 2:605–615. doi:10.1038/nrc861
Kravchenko JE, Ilyinskaya GV, Komarov PG, Agapova LS, Kochetkov DV, Strom E, Frolova EI, Kovriga I, Gudkov AV, Feinstein E, Chumakov PM (2008) Small-molecule RETRA suppresses mutant p53-bearing cancer cells through a p73-dependent salvage pathway. Proc Natl Acad Sci 105:6302–6307. doi:10.1073/pnas.0802091105
Bykov VJ, Zache N, Stridh H, Westman J, Bergman J, Selivanova G, Wiman KG (2005) PRIMA-1(MET) synergizes with cisplatin to induce tumor cell apoptosis. Oncogene 24:3484–3491. doi:10.1038/sj.onc.1208419
Ambrosini G, Sambol EB, Carvajal D, Vassilev LT, Singer S, Schwartz GK (2007) Mouse double minute antagonist Nutlin-3a enhances chemotherapy-induced apoptosis in cancer cells with mutant p53 by activating E2F1. Oncogene 26:3473–3481. doi:10.1038/sj.onc.1210136
Peirce SK, Findley HW (2009) The MDM2 antagonist nutlin-3 sensitizes p53-null neuroblastoma cells to doxorubicin via E2F1 and TAp73. Int J Oncol 34:1395–1402. doi:10.3892/ijo_00000267
Sampath D, Calin GA, Puduvalli VK, Gopisetty G, Taccioli C, Liu CG, Ewald B, Liu C, Keating MJ, Plunkett W (2009) Specific activation of microRNA106b enables the p73 apoptotic response in chronic lymphocytic leukemia by targeting the ubiquitin ligase Itch for degradation. Blood 113:3744–3753. doi:10.1182/blood-2008-09-178707
Achour M, Jacq X, Rondé P, Alhosin M, Charlot C, Chataigneau T, Jeanblanc M, Macaluso M, Giordano A, Hughes AD, Schini-Kerth VB, Bronner C (2008) The interaction of the SRA domain of ICBP90 with a novel domain of DNMT1 is involved in the regulation of VEGF gene expression. Oncogene 27:2187–2197. doi:10.1038/sj.onc.1210855
Schaefer KL (2008) PPARgamma Inhibitors as Novel Tubulin-Targeting Agents. PPAR Res 2008:785405. doi:10.1155/2008/785405
Gali-Muhtasib H, Kuester D, Mawrin C, Bajbouj K, Diestel A, Ocker M, Habold C, Foltzer-Jourdainne C, Schoenfeld P, Peters B, Diab-Assaf M, Pommrich U, Itani W, Lippert H, Roessner A, Schneider-Stock R (2008) Thymoquinone triggers inactivation of the stress response pathway sensor CHEK1 and contributes to apoptosis in colorectal cancer cells. Cancer Res 68:5609–5618. doi:10.1158/0008-5472.CAN-08-0884
Jafri SH, Glass J, Shi R, Zhang S, Prince M, Kleiner-Hancock H (2010) Thymoquinone and cisplatin as a therapeutic combination in lung cancer: In vitro and in vivo. J Exp Clin Cancer Res 29:87. doi:10.1186/1756-9966-29-87
Tien AL, Senbanerjee S, Kulkarni A, Mudbhary R, Goudreau B, Ganesan S, Sadler KC, Ukomadu C (2011) UHRF1 depletion causes a G2/M arrest, activation of DNA damage response and apoptosis. Biochem J 435:175–185. doi:10.1041/BJ20100840
DeLuca JG, Moree B, Hickey JM, Kilmartin JV, Salmon ED (2002) hNuf2 inhibition blocks stable kinetochore-microtubule attachment and induces mitotic cell death in HeLa cells. J Cell Biol 159:549–555. doi:10.1083/jcb.200208159
Woods CM, Zhu J, McQueney PA, Bollag D, Lazarides E (1995) Taxol-induced mitotic block triggers rapid onset of a p53-independent apoptotic pathway. Mol Med 1:506–526
Niikura Y, Dixit A, Scott R, Perkins G, Kitagawa K (2007) BUB1 mediation of caspase-independent mitotic death determines cell fate. J Cell Biol 178:283–296. doi:10.1083/jcb.200702134
Kitagawa K, Niikura Y (2008) Caspase-independent mitotic death (CIMD). Cell Cycle 7:1001–1005. http://dx.doi.org/10.4161/cc.7.8.5720
Mi L, Gan N, Cheema A, Dakshanamurthy S, Wang X, Yang DC, Chung FL (2009) Cancer preventive isothiocyanates induce selective degradation of cellular alpha- and beta-tubulins by proteasomes. J Biol Chem 284:17039–17051. doi:10.1074/jbc.M901789200
Harris G, Schaefer KL (2009) The microtubule-targeting agent T0070907 induces proteasomal degradation of tubulin. Biochem Biophys Res Commun 388:345–349. doi:10.1016/j.bbrc.2009.08.009
Reindl W, Yuan J, Krämer A, Strebhardt K, Berg T (2008) Inhibition of polo-like kinase 1 by blocking polo-box domain-dependent protein-protein interactions. Chem Bio l 15:459–466. doi:10.1016/j.chembiol.2008.03.013
Effenberger-Neidnicht K, Breyer S, Mahal K, Diestel R, Sasse F, Schobert R (2011) Cellular localisation of antitumoral 6-alkyl thymoquinones revealed by an alkyne-azide click reaction and the streptavidin-biotin system. ChemBioChem 12:1237–1241. doi:10.1002/cbic.201000762
Tekeoglu I, Dogan A, Ediz L, Budancamanak M, Demirel A (2007) Effects of thymoquinone (volatile oil of black cumin) on rheumatoid arthritis in rat models. Phytother Res 21:895–897. doi:10.1002/ptr.2143
Chehl N, Chipitsyna G, Gong Q, Yeo CJ, Arafat HA (2009) Anti-inflammatory effects of the Nigella sativa seed extract, thymoquinone, in pancreatic cancer cells. HPB (Oxford) 11:373–381. doi:10.1111/j.1477-2574.2009.00059.x
Al-Majed AA, Al-Omar FA, Nagi MN (2006) Neuroprotective effects of thymoquinone against transient forebrain ischemia in the rat hippocampus. Eur J Pharmacol 543:40–47. doi:10.1016/j.ejphar.2006.05.046
Kanter M (2011) Protective effects of thymoquinone on the neuronal injury in frontal cortex after chronic toluene exposure. J Mol Histol 42:39–46. doi:10.1007/s10735-010-9305-3
Gurung RL, Lim SN, Khaw AK, Soon JF, Shenoy K, Mohamed Ali S, Jayapal M, Sethu S, Baskar R, Hande MP (2010) Thymoquinone induces telomere shortening, DNA damage and apoptosis in human glioblastoma cells. PLoS One 5:e12124. doi:10.1371/journal.pone.0012124
Acknowledgments
Abdulkhaleg Ibrahim is supported by a fellowship from the Libyan Higher Education Ministry and Tanveer Sharif from the Association pour la Recherche sur le Cancer (ARC), France. We thank Dr Dominique Wachsmann and Dr Ghada Alsaleh, University of Strasbourg, France for kindly gift for providing us normal human fibroblast cells.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Fig. 1
Time-course of the effects of TQ on UHRF1 expression in Jurkat cells and in normal human fibroblast cells. Jurkat cells (A) and normal human fibroblast cells (B) were exposed to 50 μM of TQ for the indicated times. Specific band of UHRF1 was detected with its expected apparent molecular weight. The data are representative of at least three independent experiments (PDF 23 kb)
Rights and permissions
About this article
Cite this article
Alhosin, M., Ibrahim, A., Boukhari, A. et al. Anti-neoplastic agent thymoquinone induces degradation of α and β tubulin proteins in human cancer cells without affecting their level in normal human fibroblasts. Invest New Drugs 30, 1813–1819 (2012). https://doi.org/10.1007/s10637-011-9734-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-011-9734-1