Abstract
Goals
The aim of this study was to analyze recent trends in emergency department (ED) visits for diverticulitis between 2006 and 2013.
Background
Acute diverticulitis is a serious medical condition that frequently leads to ED visits, hospitalizations, and surgeries resulting in a significant health care burden.
Methods
Data were obtained from the National Emergency Department Sample (NEDS) records in which diverticulitis (ICD-9-CM codes 562.11 and 562.13) was the primary diagnosis in the ED between 2006 and 2013. The NEDS collects data from more than 25 million visits in over 950 hospital emergency departments and is weighted to provide national estimates. Our findings reflected patient and hospital characteristics such as demographics, geographical region, and total charges for ED and inpatient stays.
Results
Between 2006 and 2013, the rate of diverticulitis-related ED visits increased by 26.8% from 89.8 to 113.9 visits per 100,000 population. The aggregate national cost of diverticulitis-related ED visits increased by 105%, from approximately $822 million in 2006 to over $1.6 billion in 2013. Cost data were adjusted for inflation and reported in 2015 dollars. The percentage of individuals admitted to the same hospital from the ED decreased from 58.0 to 47.1% from 2006 to 2013, respectively, while the rate of bowel surgeries per 100,000 ED visits for diverticulitis decreased by 33.7% from 2006 to 2013.
Conclusions
The number of ED visits due to diverticulitis and associated costs continued to rise between 2006 and 2013, while the rate of bowel surgeries and inpatient admissions through the ED for diverticulitis decreased.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diverticular disease is one of the most common gastrointestinal diseases in the US population [1], particularly among the elderly [2–4]. Diverticulitis is the most common complication of diverticular disease with previous estimates varying between 10 and 25% of individuals with diverticulosis [5, 6]; however, recent estimates suggest that the rate may be significantly lower [7]. Among individuals in Olmstead County, the incidence of diverticulitis increased by 50% between 1990–1999 and 2000–2007, with a particularly notable rise in younger individuals [8]. The development of acute diverticulitis is associated with obesity, smoking, diet, lack of physical activity, and the use of nonsteroidal anti-inflammatory drugs [9]. Younger individuals with diverticulitis tend to have similar or less severe disease, though they tend to be re-admitted more frequently [8, 10, 11].
The emergency department (ED) is a common point of entry to the hospital for patients [9, 12]. Diverticulitis is the third most common GI discharge diagnosis from the ED [1]. From 2000 to 2009, there was a 41% increase in hospital admissions for diverticulitis without hemorrhage, representing 219,133 discharges totaling $2.1 billion dollars in inpatient costs in 2009 [1]. In addition, it was estimated that approximately 13–36% of patients with diverticulitis require readmission [9]. Between 1998 and 2005, the average number of elective surgeries for diverticulitis in the USA increased by 29%, and the rise in elective surgeries for diverticulitis increased by 73% for patients between the ages of 18 and 44 [13]. More recently, the rate of surgeries for diverticulitis has decreased by 1.8% between 2006 and 2011 [14].
The purpose of this study was to analyze the nationwide trends in diverticulitis in the ED, including admissions, surgical data, patient characteristics, and the associated cost burden from 2006 to 2013. No previous studies have looked at these data across these years.
Methods
This study utilized the Nationwide Emergency Department Sample (NEDS) [15] from the Healthcare Utilization Project (HCUP) [16], which is supported by the Agency for Healthcare Research and Quality (AHRQ). The NEDS is the largest publicly available emergency department all-payer database in the USA. The 2006 NEDS contains data from about 26 million ED visits from over 950 hospitals weighted to approximate over 120 million ED visits, and the 2013 NEDS contains data from 30 million ED visits at 947 hospitals that are weighted to provide national estimates for 135 million ED visits [16]. The NEDS includes national ED information regarding patient and hospital demographics, as well as inpatient admissions rates, and ED and inpatient procedures and associated costs, among others [16]. Summary statistics on trends and population rates for these data are available at no cost on HCUPnet, offered by AHRQ. Individual years of the NEDS are available for purchase and include patient-specific ED data such as inpatient length of stay, associated costs, and procedures performed. We analyzed ED trends for diverticulitis from 2006 to 2013 using International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) codes 562.11 (diverticulitis of colon without mention of hemorrhage) and 562.13 (diverticulitis of colon with hemorrhage).
Study Variables
This study analyzed the trends in diverticulitis ED visits (ICD-9-CM diagnosis codes 562.11 and 562.13) from 2006 through 2013, with a focus on associated costs and surgical procedures in 2006 and 2013. We only included patients with a primary diagnosis of diverticulitis, defined by HCUP as the first-listed diagnosis on a medical record, as this was determined to be the principal reason for the ED visit. From HCUPnet, we retrieved patient statistics including age, sex, primary payer, residence (large, medium, or small metropolitan, large fringe (suburb) or micropolitan), and median income for zip code (low or not low). Hospital characteristics obtained from HCUPnet included ownership (government or private), region (Northeast, Midwest, South, or West), location (metropolitan or non-metropolitan), trauma center designation, and teaching status. We used STATA/MP 14.1 (College Station, TX) to analyze the 2006 and 2013 NEDS datasets for associated costs, surgical procedures, inpatient admission information, and secondary diagnoses. Much of the data reported in Table 1 and Figs. 1, 2, 3, 4 were retrieved directly from HCUPnet. US population data were collected from the US Census [17] for the respective years.
a Rate of emergency department (ED) visits with a primary discharge diagnosis of diverticulitis in each age group per 100,000 ED visits in respective age groups in 2006 and 2013. b The rate of ED visits with a primary discharge diagnosis of diverticulitis in each age group per 100,000 population in respective age groups in 2006 and 2013
The variables included in this study are defined according to HCUPnet. Demographic data by zip code, collected by Claritas, defined the median income of a patient’s zip code. The lowest yearly income quartile ranged from $1 to $37,999 (low), while the three highest income quartiles were defined as $38,000 and above (not low). A “large central” residence specifies metro areas considered cores of large cities with a population of 1 million or more. A “large fringe” residence specifies suburbs of large cities with a population of 1 million or more. “Medium and small metro” residences specify metro areas that have a population less than 1 million but greater than 50,000. “Micropolitan and non-core” residences refer to rural counties that have a population below 50,000. The American Hospital Association (AHA) Annual Survey determines teaching hospital status if a hospital has an AMA-approved residency program, Council of Teaching Hospitals (COTH) membership, or 0.25 or higher ratio of residents and full-time equivalent interns to beds. The American Hospital Association (AHA) Annual Survey of Hospitals determines hospital ownership.
The surgical procedures included in this study are consistent with clinical practice and previous surgical studies [18]. We included the following ICD-9-CM procedure codes: 45.71 (open and other multiple segmental resection of large intestine), 45.79 (other and unspecified partial excision of large intestine), 45.8 (total intra-abdominal colectomy), 45.81 (laparoscopic total intra-abdominal colectomy), 45.82 (open total intra-abdominal colectomy), 45.83 (other and unspecified total intra-abdominal colectomy), 48.63 (other anterior resection of rectum), 17.3 (laparoscopic partial excision of large intestine), 17.31 (laparoscopic multiple segmental resection of large intestine), 17.39 (other laparoscopic partial excision of large intestine), 17.35 and 45.75 (left hemicolectomy), 17.36 and 45.76 (sigmoid colectomy), 46.1X (colostomy), and 46.2X (ileostomy).
Statistical Analysis
The rate of diverticulitis ED visits per 100,000 ED visits in 2006 was calculated for all patient and hospital characteristics by dividing the number of diverticulitis ED visits in each category by the total number of ED visits within that respective category and then multiplying by 100,000. For example, the rate of diverticulitis visits per 100,000 ED visits for the 18–44 age group in 2006 was calculated by dividing the number of diverticulitis ED visits in the 18–44 age group (58,379) by the total number of ED visits for the 18–44 age group (48,547,041 visits) and then multiplying by 100,000.
The cost data for 2006 and 2013 were calculated from the source files of the respective NEDS databases using STATA/MP14.1. Total diverticulitis ED costs were calculated by multiplying the mean ED cost per ED visit for diverticulitis by the total number of ED visits for diverticulitis. All costs were adjusted for inflation and reported in terms of 2015 dollars using the consumer price index inflation calculator [19].
Results
The number of ED visits for diverticulitis in the USA increased from 268,767 in 2006 to 360,272 in 2013, a 34.1% increase (Fig. 1). The rate of diverticulitis ED visits per 100,000 ED visits increased from 223.9 per 100,000 (95% CI 223.0–224.8) in 2006 to 267.1 per 100,000 (95% CI 266.2–268.0) in 2013, a 19.3% increase (95% CI 19.28–19.30). The rate of diverticulitis ED visits per US population also increased, from 89.8 per 100,000 (95% CI 89.5–90.1) to 113.9 per 100,000 (95% CI 113.5–114.3) from 2006 to 2013 (Fig. 2), a 26.8% increase (95% CI 26.8–26.8), and an average of 3.8% per year over this period.
Costs
ED visits with a primary diagnosis of diverticulitis also had a substantial increase in the mean cost (inflation adjusted 2015 dollars) from $3061 (95% CI 3033–3090, s.d. = 2960.1) in 2006 to $4765 (95% CI 4749–4781, s.d. = 4408.2) in 2013, a 56% increase (Fig. 3). In comparison, the mean cost of all ED visits (regardless of reason) in the USA increased from $1540 (95% CI 1539–1541, s.d. = 2204.7) in 2006 to $2724 (95% CI 2723–2725, s.d. = 4132.4) in 2013, a 76.9% increase over the 7-year period. The aggregate national cost (in 2015 dollars) of diverticulitis ED visits increased by 105% from $822,838,234 in 2006 (95% CI 815,238,382–830,405,608) to $1,687,176,000 in 2013 (95% CI 1,681,538,000–1,692,815,000). Between 2006 and 2013, the total charges for combined inpatient and ED costs per patient with diverticulitis increased as well, from $33,525 (95% CI 33,500–33,549) in 2006 to $49,007 (95% CI 48,973–49,042) in 2013, a 46.2% increase. However, the average length of stay for inpatients decreased by 5.9% from 5.1 days (95% CI 5.1–5.2) in 2006 to 4.8 days (95% CI 4.80–4.81) in 2013. Resulting in an average cost per day of $5306 (95% CI $5255–$5357) in 2006 and $7821 (95% CI 7760–7882) in 2013 in 2013, an increase of 47% in inpatient cost per day.
Demographics
Age
Table 1 shows the patient demographics for ED visits and hospital admissions. The average age of patients presenting to the ED with diverticulitis was fairly consistent at 58.6 (95% CI 58.5–58.6) years in 2006 and 58.3 (95% CI 58.2–58.3) years in 2013. The average age for women was 62.2 (95% CI 62.1–62.3) in 2006 and 61.2 (95% CI 61.1–61.3) in 2013, while the average age for men was 54.0 (95% CI 53.9–54.1) in 2006 and 54.4 (95% CI 54.3–54.4) in 2013. The 65–84-year age group had the highest rate of ED visits for diverticulitis with 524/100,000 visits in 2006 and 571/100,000 visits in 2013, followed by the 45–64-year age group with 449.2/100,000 visits in 2006 and 515/100,000 visits in 2013 (Fig. 4a). The lowest rate of ED visits for diverticulitis was for the 18–44-year age group with 120/100,000 in 2006 and 138/100,000 in 2013. All of the age groups displayed increases in rates of ED visits for diverticulitis per 100,000 ED visits except the 85+ year age group which had a 2.3% decrease from 358.1/100,000 in 2006 to 350/100,000 in 2013. The percent of patients admitted to the same hospital through the ED for diverticulitis decreased across all age groups, with the greatest decrease in the 18–44-year age group, at 20.3%. The 85+ age group had the lowest decrease (12.8%) and the greatest percentage of admissions in both 2006 and 2013 (81.2 and 70.8%, respectively).
Mortality
Deaths per 100,000 patients admitted for diverticulitis decreased by 41.8% from 879.2/100,000 in 2006 to 511.8/100,000 in 2013. All age groups showed a decline, but the greatest decrease was among the 85+ age group from 3000/100,000 in 2006 to 2237/100,000 in 2013, a 25.4% decrease in deaths among these patients admitted through the ED.
Gender
Women presented to the ED for diverticulitis at a higher rate than men in both 2006 and 2013. Both genders showed an increase in rates of ED visits for diverticulitis per 100,000 ED visits between 2006 and 2013 (women: 228/100,000 to 274/100,000; men: 220/100,000 to 259/100,000, respectively) representing a 20.3% increase for women and a 17.9% increase for men. A greater percent of women were admitted to the hospital through the ED than men in both 2006 and 2013: 60.7 and 47.7% for women and 54.6 and 46.3% for men, respectively. Women had a 21.4% decrease in admission, and men had a 15.2% decrease in admission.
Region
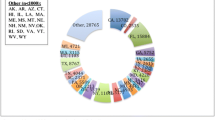
Patients in the Northeast had the highest rates of ED visits for diverticulitis per 100,000 ED visits in both 2006 and 2013 (262/100,000 and 301/100,000, respectively). The South had the lowest rate in 2006 (207/100,000), and the Midwest had the lowest rate in 2013 (246/100,000).
Primary Payer
Medicare as the primary payer for the ED visit had the highest rate of diverticulitis ED visits per 100,000 ED visits in 2006 and 2013 (416/100,000 in 2006 and 436/100,000 in 2013), while Medicaid as the primary payer had the lowest rate of diverticulitis ED visits (59/100,000 in 2006 and 85/100,000 in 2013). Patients living in large fringe metro regions (suburbs) had the highest rate of diverticulitis ED visits per 100,000 visits in both 2006 and 2013 (258/100,000 and 320/100,000), while in 2006, micropolitan and non-core (rural) regions had the lowest rate at 195/100,000 and in 2013 the lowest rate was large central metro at 242/100,000.
Inpatient Stay and Surgical Procedures
Table 2 shows the number of patients undergoing any of the selected bowel resections, as well as the breakdown of sigmoid colectomies, which constituted the majority of bowel surgeries for diverticulitis in this study (78% in 2006 and 81% in 2013). The total number of patients undergoing any of the bowel resections for diverticulitis decreased from 19,561 in 2006 to 17,393 in 2013, an 11.1% decrease. Overall, the rate of patients undergoing bowel surgeries per 100,000 ED visits for diverticulitis decreased by 33.7% between 2006 and 2013 from 7278/100,000 to 4827/100,000, respectively. The 65–84-year age group had the highest rates of bowel surgeries per 100,000 ED visits for diverticulitis at 8658/100,000 in 2006 and 5943/100,000 in 2013, a 31.4% decrease. The 18–44-year age group had the lowest rates of bowel surgeries per 100,000 ED visits for diverticulitis at 5126/100,000 in 2006 and 3207/100,000 in 2013, a 37.5% decrease. The rate of admitted patients undergoing a bowel surgery decreased from 12,553/100,000 in 2006 to 10,256/100,000 in 2013, an 18.5% decrease. Average length of stay among all patients decreased from 5.1 to 4.6 days from 2006 to 2013, a trend that continued across all categories and demographics.
Discussion
This study showed several important recent trends. First, consistent with previous studies [8, 20] showing a rise in the incidence of diverticulitis, we found the rate of ED visits with a primary diagnosis of diverticulitis per 100,000 ED visits increased by 19.3% between 2006 and 2013. Second, the aggregate national cost (in 2015 dollars) of diverticulitis ED visits in 2013 was over $1.6 billion representing a 105% increase in cost from 2006. Third, the percent of patients being admitted to the hospital from the ED for diverticulitis between 2006 and 2013 decreased as did the average length of stay and the number of patients who underwent bowel surgeries.
Consistent with previous studies showing the elderly having the highest rate of diverticulitis [2, 4, 21], our results also found the greatest rates of ED visits for diverticulitis among the elderly. Our results also showed that the younger population had the lowest rates of ED visits for diverticulitis. Our analysis indicates that there was an increase in the number ED visits between 2006 and 2013 in the younger age group. This is in contrast to other studies which show the rate per 100,000 ED visits did not increase significantly among the younger population [8, 13, 22]. Our study also found that the younger age group had the lowest rate of bowel surgeries of all age groups, which contrasts other studies suggesting that the younger age group may have more severe disease and more likely to require immediate surgical intervention due to complications [10, 21, 23].
The decreased rates of inpatient admission and surgeries for diverticulitis in our study are consistent with other studies emphasizing outpatient management for uncomplicated diverticulitis [24–29]. Several studies have found that outpatient care providing oral antibiotics for patients with uncomplicated acute diverticulitis was safe and efficacious in over 90% of cases [25, 26]. Both ambulatory care and homecare have been demonstrated to produce significant cost savings without compromising quality of care for patients [24–27]. In addition, we found both the absolute numbers and rates of mortality in hospitalized patients were lower, suggesting advancements in surgical techniques. Several studies have shown reduced mortality and complication rates and shorter length of inpatient stays in patients undergoing laparoscopic versus open colectomy for sigmoid diverticular disease [30–32].
Our study found the highest rates of hospital admissions in the Northeast, followed by the South and the Midwest. The reason for the regional differences is unclear, though it is likely to be multifactorial including differences in demographics such as obesity, a significant risk factor for diverticulitis [33], which tends to be higher in the Midwest and South [9, 34, 35]. We found slightly higher rates of women being admitted to the hospital and undergoing surgery for diverticulitis. Several studies have noted gender differences with diverticulitis as well, finding it more predominant in younger males and older women [21, 22]. However, some studies have found no differences or a slight female predominance, as we found in our study [36].
This study is in agreement with other studies that have found decreasing rates of admission and surgical procedures for patients with diverticulitis in recent years [14, 18], and our data show that this trend continues through 2013. Unlike these previous studies, we analyzed cost for ED visits as well as combined ED and inpatient stays showing marked increase in charges for diverticulitis visits. In contrast to our study which showed a decrease in inpatient admissions and surgical procedures, a previous study analyzing ED data from before 2006 found increased admission rates and surgical procedures [13].
While the admission and surgical rates of diverticulitis have gone down, there are still increasing rates of patients presenting to the ED with diverticulitis. Future care and policies may need to focus more on prevention of diverticulitis and diverticular disease, addressing risk factors like obesity, low-fiber diets, and chronic alcohol consumption [37].
This study has several limitations. First, our dataset does not include ambulatory data or inpatient data from patients who are not admitted through the ED. Additionally, the NEDS includes data from 950 hospitals, which may vary in their coding practices. Also, this dataset does not indicate repeat patients, but counts each visit as a unique patient. This dataset was also not controlled for data entry errors. Finally, this study includes only ED visits in which diverticulitis was the primary discharge diagnosis, which may underestimate the number of ED visits. Further studies that examine differences in institutional coding practices and patient specifics may further define the information in this study.
Conclusions
This study analyzed the ED trends for diverticulitis and found increasing rates of patients presenting with diverticulitis as well as increasing costs between 2006 and 2013. While the rate of patients being admitted to the hospital from the ED with diverticulitis had decreased and length of inpatient stay had decreased, further studies are needed to find ways to improve outpatient management of diverticular disease and cost-saving measures in both the ED and the inpatient and surgical areas.
References
Peery AF, Dellon ES, Lund J, et al. Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology. 2012;143:1179–87e1–1179–87e3.
Commane DM, Arasaradnam RP, Mills S, et al. Diet, ageing and genetic factors in the pathogenesis of diverticular disease. World J Gastroenterol. 2009;15:2479–2488.
Painter NS, Burkitt DP. Diverticular disease of the colon: a deficiency disease of Western civilization. Br Med J. 1971;2:450–454.
Comparato G, Pilotto A, Franze A, et al. Diverticular disease in the elderly. Dig Dis. 2007;25:151–159.
Janes SE, Meagher A, Frizelle FA. Management of diverticulitis. BMJ. 2006;332:271–275.
Heise CP. Epidemiology and pathogenesis of diverticular disease. J Gastrointest Surg. 2008;12:1309–1311.
Shahedi K, Fuller G, Bolus R, et al. Long-term risk of acute diverticulitis among patients with incidental diverticulosis found during colonoscopy. Clin Gastroenterol Hepatol. 2013;11:1609–1613.
Bharucha AE, Parthasarathy G, Ditah I, et al. Temporal trends in the incidence and natural history of diverticulitis: a population-based study. Am J Gastroenterol. 2015;110:1589–1596.
Humes DJ, Spiller RC. Review article: the pathogenesis and management of acute colonic diverticulitis. Aliment Pharmacol Ther. 2014;39:359–370.
Horesh N, Shwaartz C, Amiel I, et al. Diverticulitis and the age factor—does age matter? J Dig Dis. 2016;17:313–318.
Katz LH, Guy DD, Lahat A, et al. Diverticulitis in the young is not more aggressive than in the elderly, but it tends to recur more often: systematic review and meta-analysis. J Gastroenterol Hepatol. 2013;28:1274–1281.
van de Wall BJ, Poerink JA, Draaisma WA, et al. Diverticulitis in young versus elderly patients: a meta-analysis. Scand J Gastroenterol. 2013;48:643–651.
Etzioni DA, Mack TM, Beart RW Jr, et al. Diverticulitis in the United States: 1998–2005: changing patterns of disease and treatment. Ann Surg. 2009;249:210–217.
Greenwood-Ericksen MB, Havens JM, Ma J, et al. Trends in hospital admission and surgical procedures following ED visits for diverticulitis. West J Emerg Med. 2016;17:409–417.
HNEDS (NEDS). Healthcare Cost and Utilization Project (HCUP) Agency for Healthcare Research and Quality. Rockville, MD, 2006, 2013.
HCUPnet. Healthcare Cost and Utilization Project (HCUP) Agency for Healtcare Research and Quality Rockville, MD, 2006–2013.
U.S. Census Bureau, 2006, 2013.
Schneider EB, Singh A, Sung J, et al. Emergency department presentation, admission, and surgical intervention for colonic diverticulitis in the United States. Am J Surg. 2015;210:404–407.
Consumer Price Index Inflation Calculator 2015.
Matrana MR, Margolin DA. Epidemiology and pathophysiology of diverticular disease. Clin Colon Rectal Surg. 2009;22:141–146.
Schauer PR, Ramos R, Ghiatas AA, et al. Virulent diverticular disease in young obese men. Am J Surg. 1992;164:443–446 (discussion 446–448).
Acosta JA, Grebenc ML, Doberneck RC, et al. Colonic diverticular disease in patients 40 years old or younger. Am Surg. 1992;58:605–607.
Pautrat K, Bretagnol F, Huten N, et al. Acute diverticulitis in very young patients: a frequent surgical management. Dis Colon Rectum. 2007;50:472–477.
Biondo S, Golda T, Kreisler E, et al. Outpatient versus hospitalization management for uncomplicated diverticulitis: a prospective, multicenter randomized clinical trial (DIVER Trial). Ann Surg. 2014;259:38–44.
Alonso S, Pera M, Pares D, et al. Outpatient treatment of patients with uncomplicated acute diverticulitis. Colorectal Dis. 2010;12:e278–e282.
Moya P, Arroyo A, Perez-Legaz J, et al. Applicability, safety and efficiency of outpatient treatment in uncomplicated diverticulitis. Tech Coloproctol. 2012;16:301–307.
Rueda JC, Jimenez A, Caro A, et al. Home treatment of uncomplicated acute diverticulitis. Int Surg. 2012;97:203–209.
Schaffzin DM, Wong WD. Nonoperative management of complicated diverticular disease. Clin Colon Rectal Surg. 2004;17:169–176.
Etzioni DA, Chiu VY, Cannom RR, et al. Outpatient treatment of acute diverticulitis: rates and predictors of failure. Dis Colon Rectum. 2010;53:861–865.
Alves A, Panis Y, Slim K, et al. French multicentre prospective observational study of laparoscopic versus open colectomy for sigmoid diverticular disease. Br J Surg. 2005;92:1520–1525.
Purkayastha S, Constantinides VA, Tekkis PP, et al. Laparoscopic vs. open surgery for diverticular disease: a meta-analysis of nonrandomized studies. Dis Colon Rectum. 2006;49:446–463.
Dwivedi A, Chahin F, Agrawal S et al. Laparoscopic colectomy vs. open colectomy for sigmoid diverticular disease. Dis Colon Rectum. 2002;45:1309–1314 (discussion 1314–1315).
Strate LL, Liu YL, Aldoori WH, et al. Obesity increases the risks of diverticulitis and diverticular bleeding. Gastroenterology. 2009;136(115–122):e1.
Martel J, Raskin JB. Ndsg. History, incidence, and epidemiology of diverticulosis. J Clin Gastroenterol. 2008;42:1125–1127.
Singh GK, Kogan MD, van Dyck PC. A multilevel analysis of state and regional disparities in childhood and adolescent obesity in the United States. J Community Health. 2008;33:90–102.
Parks TG. Natural history of diverticular disease of the colon. Clin Gastroenterol. 1975;4:53–69.
Pisanu A, Vacca V, Reccia I, et al. Acute diverticulitis in the young: the same disease in a different patient. Gastroenterol Res Pract. 2013;2013:867961.
Financial support
This project was funded in part by R01AT008573.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Bollom, A., Austrie, J., Hirsch, W. et al. Emergency Department Burden of Diverticulitis in the USA, 2006–2013. Dig Dis Sci 62, 2694–2703 (2017). https://doi.org/10.1007/s10620-017-4525-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-017-4525-y