Abstract
Purpose
It was reported from this laboratory that Kupffer cells (KCs) were activated in patients infected with HCV. Since dendritic cells, monocytes, and macrophages were activated by stimulation with HCV-related proteins, the specific aim of this study was to investigate the role of HCV-related proteins in activation of KCs, the signal pathway of activation of KCs mediated by Toll-like receptor (TLR) 4, and the influence of HCV infection on function of KCs.
Methods
Kupffer cells isolated from non-cancerous surgical specimen were co-cultured with HCV-related proteins (Core, NS3, NS4, and NS5), and production of cytokines (TNF-α, IL-1β, and IL-10) and hydrogen peroxide were assessed. Furthermore, effects of neutralization antibodies against the TLR2, TLR3, or TLR4, and cytochalasin B on the production TNF-α by KCs were investigated.
Results
Kupffer cells produced markedly a proinflammatory cytokine TNF-α by stimulation with all HCV-related proteins studied, and values were as same as production by KCs stimulated with LPS. Importantly, this production in the case of NS3 was significantly blunted by about 60% by neutralization antibodies against the TLR4, but not cytochalasin B. Production of TNF-α by isolated KCs stimulated with LPS was significantly greater in the HCV-infected livers than the HCV/HBV-negative livers.
Conclusions
These results indicated that HCV-related proteins may cause prolonged activation of KCs in the HCV-infected liver, leading to accumulation of inflammatory cytokines that contribute to DNA damage and carcinogenesis. Furthermore, function of KCs was difference between patients infected with and without HCV infection.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) is one of the most common cancers in the world, and hepatitis C virus (HCV) infection is the most frequent cause of HCC in Japan at present [1]. The incidence of HCC associated with HCV infection is also thought to be increasing elsewhere in the world; [2, 3], however, the long-term prognosis of HCC remains unsatisfactory because of the high incidence of multicentric or intrahepatic metastatic recurrences; therefore, the mechanisms underlying the development of HCC must be investigated in greater detail.
HCV infection increases the number of CD68-positive cells in the liver [4]. Previously, we reported that intrahepatic oxidative stress correlated to the number of CD68-positive cells in patients infected with HCV [5]. Furthermore, oxidative stress in the liver induced DNA damage in hepatocytes, and resulted in increases in the postoperative intrahepatic recurrence of HCC [5, 6]. Activated Kupffer cells, hepatic macrophages, increased in patients infected with HCV [7], and produced reactive oxygen species; [8, 9], however, the exact activation mechanism of Kupffer cells is still unclear.
Dendritic cells, monocytes, and macrophages were activated by stimulation with HCV-related proteins, such as core and NS3, and the signal pathway of this activation was regulated by Toll-like receptor (TLR) [10–12]. Accordingly, the specific purpose of this study was to investigate whether HCV-related proteins could activate Kupffer cells isolated from human liver tissues. Furthermore, effects of HCV infection on the function of Kupffer cells were also investigated.
Materials and Methods
Patients and Liver Tissues
Kupffer cells were isolated from patients who underwent surgical resection of a liver tumor at the University of Yamanashi Hospital (Yamanashi, Japan) between November 2004 and November 2007. The presence and identification of hepatitis C virus was determined by one or more of the following techniques: (1) presence of anti-HCV and anti-HBV reactive serum proteins, (2) reverse transcription-PCR for serum HCV-RNA or (3) branched DNA-HCV probe assay. Informed consent was obtained from all subjects who participated in the study and the study was approved by the Institutional Board on Ethics for Human Science at the University of Yamanashi.
Kupffer Cell Isolation
Kupffer cells were isolated according to the method of Heuff et al. [13], with some modifications. Tumor-free liver tissues were collected from surgical specimens during liver tumor surgery. Liver tissues were dissected with scissors and incubated with Liver Perfusion Medium (LPM) containing 8,000 mg/l NaCl, 400 mg/l KCl, 88.17 mg/l NaH2PO42H2O, 120.45 mg/l Na2HPO4, 2,380 mg/l 2-[4-(2-hydroxyethyl)-1-piperazinyl]ethanesulfonic acid (HEPES), 350 mg/l NaHCO3, 190 mg/l ethylene glycol-bis(2-aminoethylether)-N,N,N′,N′-tetraacetic acid (EGTA), 900 mg/l glucose, and 6 mg/l phenol red. Subsequently, they were ground manually through mesh (pore size 100 μm) and incubated in LPM with CaCl22H2O containing 0.05% collagenase (Sigma-Aldrich Co., St. Louis, MO) on a magnetic stirrer at 37°C for 30 min. After incubation, the suspension was filtered through mesh (pore size 100 μm) and the filtrate was centrifuged at 720 × g for 7 min. The pellet was resuspended in 50 ml Gey’s balanced salt solution (GBSS) and centrifuged at 720 × g for 7 min. After washing, the pellet was resuspended in 10 ml GBSS. Non-parenchymal cells were separated from nonviable cells, parenchymal cells and erythrocytes by centrifugation on a 16% Nycodenz (Nycomed, Oslo, Norway) gradient for 20 min, 1,900 × g at 4°C. The interface was collected, resuspended in 50 ml GBSS, and continuously centrifuged at 720 × g for 7 min. The final pellet was resuspended in Dulbecco’s modified Eagle’s medium (DMEM; Invitrogen, Carlsbad, CA) with 10% fetal bovine serum (Invitrogen) and 5 ml antibiotic–antimycotic solution (Sigma-Aldrich Co., St. Louis, MO) containing 100 U/ml penicillin, 100 μg/ml streptomycin and 0.25 μg/ml amphotericin B.
Assays for TNF-α, IL-1β, and IL-10
Isolated Kupffer cells were plated onto 24-well tissue culture plates and incubated in a humidified atmosphere of 5% CO2 at 37°C for 24 h. Subsequently, dish-adhering cells were incubated with or without recombinant HCV-related proteins (core (aa 2–192), NS3 (aa 1,192–1,456), NS4 (aa 1,916–1,947), or NS5 (aa 2,061–2,302); Virogen, Watertown, MA) or lipopolysaccharide (LPS; Sigma-Aldrich Co., St. Louis, MO). Isolated Kupffer cells were stimulated with 1, 5, or 10 μg/ml HCV-related proteins. Furthermore, the effects of neutralization antibodies against Toll-like receptor (TLR) 2, TLR3, TLR4, or cytochalasin B on the production TNF-α by Kupffer cells were investigated. Before administration of HCV-related protein, NS3 protein, Kupffer cells were pre-incubated with monoclonal antibody against human TLR 2 (Imgenex, San Diego, CA) 20 μg/ml for 1 h, monoclonal antibody against human Toll-like receptor 3 (IMGENEX) 20 μg/ml for 1 h, monoclonal antibody against human TLR 4 (Imgenex, San Diego, CA) 20 μg/ml for 1 h, cytochalasin B (Sigma-Aldrich) 20 μM for 1 h, dimethyl sulfoxide (DMSO; Sigma-Aldrich) 2 μl/ml for 1 h in a humidified atmosphere of 5% CO2 at 37°C. Supernatants were collected 24 h later and stored at −80°C until assay for TNF-α, IL-1β, and IL-10 using specific cytokine enzyme-linked immunosorbent assay kits (Biosource International, Inc., Camarillo, CA). Contamination of LPS was not detected in HCV-related proteins or other reagents. Kupffer cells were washed with residual cultured medium with PBS and solved with Cell Culture Lysis Reagent (Promega Co. Madison, WI). The solution was collected and stored at −80°C, until analyzed for protein concentration using a DC Protein Assay kit (Bio-Rad Laboratories, Heracles, CA). The concentration of cytokines was divided by the cell protein concentration.
Measurement of Net, Total Hydrogen Peroxide Generation by Kupffer Cells
Isolated Kupffer cells 2.0 × 105 were placed in a 96-well microplate and incubated in a humidified atmosphere of 5% CO2 at 37°C for 24 h. After incubation, the culture medium in each well was replaced with 200 μl HBSS buffer with 2′,7′-dichlorofluorescein diacetate (DCF-DA; Sigma-Aldrich; 50 μmol/l) as intracellular reactive oxygen species marker for 30 min. Subsequently, the dish adherent cells (Kupffer cells) were washed out DCF-DA with HBSS. Before and after incubation with or without HCV-related proteins (core, NS3, NS4, or NS5) or t-Butyl hydroperoxide (Sigma-Aldrich) in a humidified atmosphere of 5%CO2 at 37°C for 6 h, the fluorescence in each cell was measured in a fluorescence microplate reader (Molecular Devices Co; SpectraMax®340PC384) using an excitation of 485 nm and an emission detection of 535 nm. Values after 6 h of administration subtracted from former value were shown.
Statistics
The STATVIEW software (ver. 5.0, SAS Institute, Cary, NC) was used for statistical analysis. Categorical variables were compared using the Fisher exact test or Chi-square test as appropriate. Inter-experiment comparisons in cytokine concentrations for the different culture conditions were analyzed by means of Student’s t test or Mann–Whitney’s U test as appropriate. All values were reported as means ± SE and a p value <0.05 was considered to be significant.
Results
HCV-Related Proteins Activated Kupffer Cells Isolated from Human Liver Tissues
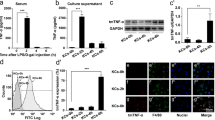
In this study, a total of 37 consecutive patients were enrolled and assigned to the HCV/HBV negative group (n = 22), HCV group (n = 15; Table 1). There were no significant differences between groups in all parameters traditionally evaluated in patients with the exception of pathology and histology of liver. The production of TNF-α by isolated Kupffer cells was minimal without stimulation (Fig. 1a). On the other hand, TNF-α production increased significantly by stimulation with HCV-related proteins in a dose-dependent manner, except for NS4. Furthermore, HCV-related protein induced a large amount of TNF-α production by Kupffer cells as same as those production with LPS stimulation.
Production of cytokines by isolated Kupffer cells isolated from patients without HCV/HBV infection. Kupffer cells isolated from patients without HCV/HBV infection were stimulated with HCV-related proteins or LPS for 24 h. Supernatants were collected and analyzed for TNF-α (a), IL-1β (b), and IL-10 (c) by ELISA. Core protein, core; nonstructural 3 protein, NS3; nonstructural 4 protein, NS4; nonstructural 5 protein, NS5; lipopolysaccharide, LPS. Data represent the mean ± SE. †, P < 0.05 compared to medium; and *, P < 0.01 compared to medium by Student’s t-test
Production of IL-1β by isolated Kupffer cells was minimal without stimulation (Fig. 1b). On the other hand, IL-1β production increased significantly by stimulation with HCV-related proteins, except for core proteins. Although the greatest production was observed in Kupffer cells incubated with 5 μg/ml of NS5, this production was much lower than TNF-α production by Kupffer cells.
IL-10 production by isolated Kupffer cells was minimal without stimulation (Fig. 1c). On the other hand, IL-10 production increased significantly by stimulation with HCV-related proteins, except for core proteins. Furthermore, the greatest production was observed in Kupffer cells incubated with 1 μg/ml of NS5. Although HCV-related proteins induced IL-10 production by isolated Kupffer cells, the values were much lower than TNF-α production by Kupffer cells.
The Signal Pathway of Activation of Kupffer Cells by HCV-Related Proteins Was Partially Mediated by TLR4
TNF-α production by isolated Kupffer cells was minimal without stimulation (Fig. 2). Production was markedly increased in Kupffer cells co-incubated with NS3 proteins and DMSO. Furthermore, the production was not blunted by treatment with a phagocytosis blockade, cytochalasin B.
Effect of cytochalasin B on production of TNF-α by isolated Kupffer cells. TNF-α production by isolated Kupffer cells stimulated with NS3 protein (10 μg/ml) in the presence or absence of cytochalasin B was measured by ELISA. dimethyl sulfoxide, DMSO; nonstructural 3 protein, NS3. Data represent the mean ± SE
Production was markedly increased in Kupffer cells co-incubated with NS3 proteins (Fig. 3). This increase was significantly, but not totally, blunted by antagonists for TLR4, but not TLR2 or TLR3. Neutralization antibodies against TLR4 also inhibited the production of IL-10, and the results were similar to those of TNF-α (Fig. 4).
Effect of TLR2, TLR3, or TLR4 antagonist on cytokine production by Kupffer cells isolated from patients without HCV/HBV infection. Production of TNF-α by Kupffer cells isolated from patients without HCV/HBV infection by stimulation with NS3 protein (5 μg/ml) was investigated in the presence or absence of TLR2 antagonist, TLR3 antagonist, or TLR4 antagonist. Monoclonal antibody against human toll-like receptor 2, TLR2 antagonist; monoclonal antibody against human toll-like receptor 3, TLR3 antagonist; monoclonal antibody against human toll-like receptor 4, TLR4 antagonist; and nonstructural 3 protein, NS3. Data represent the mean ± SE
Effect of TLR4 antagonist on cytokine production by Kupffer cells isolated from patients without HCV/HBV infection. Production of TNF-α (a) and IL-10 (b) by Kupffer cells isolated from patients without HCV/HBV infection by stimulation with NS3 protein (10 μg/ml) was investigated in the presence or absence of TLR4 antagonist. Monoclonal antibody against human toll-like receptor 4, TLR4 antagonist; and nonstructural 3 protein, NS3. Data represent the mean ± SE. *, P < 0.05 compared to the absence of TLR4 antagonist by the means of Mann–Whitney’s U test
Effects of HCV Infection on the Function of Kupffer Cells
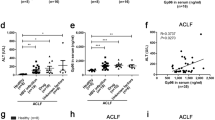
In Kupffer cells isolated from livers in patients infected with HCV or without HCV/HBV infection, significant production of TNF-α was induced by stimulation with LPS (Fig. 5a). These values were significantly greater in Kupffer cells isolated from livers infected with HCV compared to Kupffer cells isolated from livers without HCV/HBV infection. Although HCV-related protein also induced production of TNF-α by Kupffer cells isolated from both HCV-infected and HCV/HBV non-infected livers, there were no significant differences in the production of TNF-α by stimulation with all HCV-related proteins studied.
Functional heterogeneity of the Kupffer cell between liver infected with HCV and the non-infected liver. Production of TNF-α (a) and hydrogen peroxide (b) by Kupffer cells isolated from patients infected with HCV (striped bar) or without HCV/HBV (solid bar) was investigated. Production of TNF-α and hydrogen peroxide was measured as described in "Materials and Methods". Core protein, core; nonstructural 3 protein, NS3; nonstructural 4 protein, NS4; nonstructural 5 protein, NS5; lipopolysaccharide, LPS; and t-Butyl hydroperoxide, t-BOOH. Data represent mean ± SE. *, p < 0.05 compared to Kupffer cells isolated from patients without HCV/HBV infection; †, p < 0.05 compared to the medium; and ‡, P < 0.01 compared to the medium by Student’s t-test
Hydrogen peroxide production by isolated Kupffer cells was not different between HCV-infected livers and HCV/HBV non-infected livers (Fig. 5b). Although hydrogen peroxide production increased in both HCV-infected and HCV/HBV non-infected livers after stimulation with t-BOOH, this production was significantly greater in HCV/HBV non-infected livers compared to HCV-infected livers. The production of hydrogen peroxide by Kupffer cells stimulated with each of NS3, NS4, or NS5 increased in HCV/HBV non-infected livers; however, this event was not observed by stimulation with core proteins. On the other hand, the production did not increase in Kupffer cells isolated from HCV-infected livers after stimulation with core, NS3, NS4, or NS5 proteins.
Discussion
In the present study, the activation of Kupffer cells by stimulation with HCV-related proteins was investigated. This is the first report to document the activation of human Kupffer cells by stimulation with HCV-related proteins. Furthermore, the signal was partially regulated by TLR4.
Effects of HCV-Related Proteins on Kupffer Cell Activation
Previous study reported that activated Kupffer cells produced reactive oxygen species and inflammatory cytokines [14], which induced liver injury. Furthermore, monocytes [11] and macrophages [12] were activated by stimulation with HCV core or NS3 proteins. In the present study, Kupffer cells were activated by HCV-related proteins, and produced a significant amount of TNF-α (Fig. 1a). TNF-α signals increase the expression of adhesion molecules such as ICAM-1 and chemokines such as MIP, and increase the number of infiltrating inflammatory cells in the liver [4], leading to liver injury. Thus, HCV-related proteins are most likely involved in the mechanism of liver injury in the HCV-infected liver.
Previous work has shown that the intrahepatic mRNA expression of IL-1β was greater in patients suffering from liver cirrhosis than chronic hepatitis. Furthermore, the mRNA expression of IL-1β positively correlated with the mRNA expression of TNF-α only in chronic HCV-infected patients [4]. In the present study, IL-1β production by stimulation with HCV-related proteins was low, and not correlated with TNF-α production (Fig. 1b). Thus, Kupffer cells activated by HCV-related proteins were not a predominant source of IL-1β in the chronic HCV-infected liver. Furthermore, in the present study, production of IL-10 by Kupffer cells stimulated with HCV-related proteins was also significantly lower compared to the production of TNF-α (Fig. 1c). Taken together, activated Kupffer cells by HCV-related proteins produced predominantly pro-inflammatory cytokine TNF-α.
It was reported that tetraspanin CD81 and scavenger receptor Class B type Ι were receptors for HCV envelope glycoprotein E2 in HCV entry [15, 16], and TLR2 was a receptor for core and NS3, as for dendritic cells, monocytes, and macrophages [10, 11]. The present study reported that TLR4 was the receptor for NS3 in Kupffer cells, however, production of TNF-α by Kupffer cells stimulated with core, NS4, or NS5 proteins did not blunt in the presence of antagonists for TLR4 (data not shown). Since truncated part of NS3 used in the present study was different from the part of NS3 used in the previous study [10], this may be a cause of inconsistent results. Indeed, TNF-α production by isolated Kupffer cell stimulated with the part of NS3 used in the previous study was not blocked by antagonist for TLR-2 or TLR-4 (data not shown).
Involvement of Kupffer Cells in Carcinogenesis in HCV-Infected Livers
Kupffer cells have been linked primarily to a pathological role in liver injury induced by hepatotoxins, including CCl4 [17], ethanol [18], and acetaminophen [19]. On the other hand, Kupffer cells may also have hepato-protective functions in acetaminophen-induced liver injury [20]. Under this condition, TNF-α induces the release of inflammatory mediators, and causes liver damage [21]. In addition, TNF-α causes proliferation, regeneration [21], and apoptosis [22, 23] in hepatocytes. On the other hand, TNF-α increases the IL-18R expression in HCC, and the promotion of anti-apoptotic effects on HCC in vitro [24]. Furthermore, TNF-α related to carcinogenesis was induced by the inactivation of p53, which was induced by the production and promotion of macrophage migration inhibitory factor induced by TNF-α signaling [25]. In addition, TNF-α which was elevated in patients infected with HCV, induced liver damage [26] and DNA damage [27]. Thus, large amount production of TNF-α by activated Kupffer cells stimulated with HCV-related proteins (Fig. 1a) may contribute to aggravation of hepatitis and carcinogenesis in the liver infected with HCV.
HCV Infection's Affects on the Function of Kupffer Cells
Kupffer cells act as antigen-presenting cells in the chronic viral infected liver and phagocytes in the non-infected liver [7]. Furthermore, in the physiological condition, Kupffer cells are CD14-negative. On the other hand, CD14 is induced under the pathophysiological condition, such as inflammation [28], suggesting that function of the Kupffer cell may be affected by infection with HCV. Therefore, the functional heterogeneity of Kupffer cells was investigated in livers infected with or without HCV in the present study (Fig. 5). Indeed, there were no significant differences in production of pro-inflammatory cytokine TNF-α by isolated Kupffer cells between HCV-infected liver and non-infected liver after stimulation with HCV-related proteins. In contrast, the production of hydrogen peroxide by isolated Kupffer cells stimulated with core or NS3 was significantly lower in the chronic HCV-infected liver compared to HCV-negative liver (Fig. 5b). Thus, chronic infection of HCV affects the function of the Kupffer cells.
The production of TNF-α by monocytes stimulated with LPS was greater on chronic-HCV patients compared to healthy controls [11]. It was previously reported that the mRNA expression of CD14 and MD-2, which are co-receptors for LPS, were upregulated in monocytes in patients infected with HCV compared with healthy controls [29]. Furthermore, in the present study, the production of TNF-α by isolated Kupffer cells stimulated with LPS was significantly greater in the chronic HCV-infected liver compared to the HCV-negative liver (Fig. 5a). Thus, Kupffer cells in HCV-infected livers were more susceptible for endotoxin. A previous study reported that endotoxin levels in the systemic circulation elevated in chronic hepatitis patients, and the plasma endotoxin levels progressively related to the severity of liver dysfunction [30]. Furthermore, there was a positive correlation between portal and systemic circulation LPS [31]. Thus, the enhanced susceptibility to endotoxin in Kupffer cells may be one cause of deterioration of inflammation in the HCV-infected liver.
In the present study, HCV-related proteins activated Kupffer cells isolated from human liver tissues. Furthermore, the signal pathway of TNF-α production by isolated Kupffer cells stimulation with HCV-related proteins was partially mediated by TLR4. Moreover, HCV infection enhanced susceptibility to endotoxin in the Kupffer cell. These results indicated that HCV infection and HCV-related proteins may be one cause of prolonged activation of Kupffer cells, leading to the accumulation of inflammatory cytokines that may contribute to DNA damage and carcinogenesis.
Kupffer cells isolated from patients without HCV/HBV infection were stimulated with HCV-related proteins or LPS for 24 h. Supernatants were collected and analyzed for TNF-α (A), IL-1β (B), and IL-10 (C) by ELISA. Core protein, core; nonstructural 3 protein, NS3; nonstructural 4 protein, NS4; nonstructural 5 protein, NS5; lipopolysaccharide, LPS. Data represent the mean ± SE. †, p < 0.05 compared to medium; and *, p < 0.01 compared to medium by Student’s t test.
TNF-α production by isolated Kupffer cells stimulated with NS3 protein (10 μg/ml) in the presence or absence of cytochalasin B was measured by ELISA. Dimethyl sulfoxide, DMSO; nonstructural three protein, NS3. Data represent the mean ± SE.
Production of TNF-α by Kupffer cells isolated from patients without HCV/HBV infection by stimulation with NS3 protein (5 μg/ml) was investigated in the presence or absence of TLR2 antagonist, TLR3 antagonist, or TLR4 antagonist. Monoclonal antibody against human Toll-like receptor 2, TLR2 antagonist; monoclonal antibody against human Toll-like receptor 3, TLR3 antagonist; monoclonal antibody against human Toll-like receptor 4, TLR4 antagonist; and nonstructural 3 protein, NS3. Data represent the mean ± SE.
Production of TNF-α (A) and IL-10 (B) by Kupffer cells isolated from patients without HCV/HBV infection by stimulation with NS3 protein (10 μg/ml) was investigated in the presence or absence of TLR4 antagonist. Monoclonal antibody against human Toll-like receptor 4, TLR4 antagonist; and nonstructural 3 protein, NS3. Data represent the mean ± SE. *, p < 0.05 compared to the absence of TLR4 antagonist by the means of Mann–Whitney’s U test.
Production of TNF-α (A) and hydrogen peroxide (B) by Kupffer cells isolated from patients infected with HCV (striped bar) or without HCV/HBV (solid bar) was investigated. Production of TNF-α and hydrogen peroxide was measured as described in “Materials and Methods”. Core protein, core; nonstructural 3 protein, NS3; nonstructural 4 protein, NS4; nonstructural 5 protein, NS5; lipopolysaccharide, LPS; and t-Butyl hydroperoxide, t-BOOH. Data represent mean ± SE. *, p < 0.05 compared to Kupffer cells isolated from patients without HCV/HBV infection; †, p < 0.05 compared to the medium; and ‡, p < 0.01 compared to the medium by Student’s t test.
Abbreviations
- DMSO:
-
Dimethyl sulfoxide
- ELISA:
-
Enzyme-linked immunosorbent assay
- HCC:
-
Hepatocellular carcinoma
- HCV:
-
Hepatitis C virus
- ICAM-1:
-
Intercellular adhesion molecule-1
- IL:
-
Interleukin
- KC:
-
Kupffer cell
- LPS:
-
Lipopolysaccharide
- MIP:
-
Macrophage inflammatory protein
- NS3:
-
Nonstructural 3 protein
- NS4:
-
Nonstructural 4 protein
- NS5:
-
Nonstructural 5 protein
- t-BOOH:
-
t-Butyl hydroperoxide
- TLR:
-
Toll-like receptor
- TNF:
-
Tumor necrosis factor
References
Kiyosawa K, Tanaka E. Characteristics of hepatocellular carcinoma in Japan. Oncology. 2002;62(1):5–7.
Yoshizawa H. Hepatocellular carcinoma associated with hepatitis C Virus infection in Japan: projection to other countries in the foreseeable future. Oncology. 2002;62(Suppl 1):8–17.
Tanaka Y, Hanada K, Mizokami M, et al. Inaugural article: a comparison of the molecular clock of hepatitis C virus in the United States and Japan predicts that hepatocellular carcinoma incidence in the United States will increase over the next two decades. Proc Natl Acad Sci USA. 2002;99:15584–15589.
McGuinness PH, Painter D, Davies S, McCaughan GW. Increases in intrahepatic CD68 positive cells, MAC387 positive cells, and proinflammatory cytokines (particularly interleukin 18) in chronic hepatitis C infection. Gut. 2000;46:260–269.
Maki A, Kono H, Gupta M, et al. Predictive power of biomarkers of oxidative stress and inflammation in patients with hepatitis C virus-associated hepatocellular carcinoma. Ann Surg Oncol. 2007;14:1182–1190.
Matsumoto K, Satoh Y, Sugo H, et al. Immunohistochemical study of the relationship between 8-hydroxy-2′-deoxyguanosine levels in noncancerous region and postoperative recurrence of hepatocellular carcinoma in remnant liver. Hepatol Res. 2003;25:435–441.
Burgio VL, Ballardini G, Artini M, Caratozzolo M, Bianchi FB, Levrero M. Expression of co-stimulatory molecules by Kupffer cells in chronic hepatitis of hepatitis C virus stiology. Hepatology. 1998;27:1600–1606.
Wheeler MD, Kono H, Yin M, et al. The role of Kupffer cell oxidant production in early ethanol-induced liver disease. Free Radic Biol Med. 2001;31:1544–1549.
Rusyn I, Kadiiska MB, Dikalova A, et al. Phthalates rapidly increase production of reactive oxygen species in vivo: role of Kupffer cells. Mol Pharmacol. 2001;59:744–750.
Dolganiuc A, Oak S, Kodys K, et al. Hepatitis C core and nonstructural 3 proteins trigger toll-like receptor 2-mediated pathways and inflammatory activation. Gastroenterology. 2004;127:1513–1524.
Dolganiuc A, Kodys K, Kopasz A, et al. Hepatitis C virus core and nonstructural protein 3 proteins induce pro-and anti-inflammatory cytokines and inhibit dendritic cell differentiation. J Immunol. 2003;170:5615–5624.
Chang S, Dolganiuc A, Szabo G. Toll-like receptors 1 and 6 are involved in TLR2-mediated macrophage activation by hepatitis C virus core and NS3 proteins. J Leukoc Biol. 2007;82:479–487.
Heuff G, Meyer S, Beelen RHJ. Isolation of rat and human Kupffer cells by a modified enzymatic assay. J Immunol Meth. 1994;174:61–65.
Decker K. Biologically active products of stimulated liver macrophages (Kupffer cells). Eur J Biochem. 1990;192:245–261. Review.
Pileri P, Uematsu Y, Campagnoli S, et al. Binding of hepatitis C virus to CD81. Science. 1998;282:938–941.
Zeisel MB, Koutsoudakis G, Schnober EK, et al. Scavenger receptor class B type I is a key host factor for hepatitis C virus infection required for an entry step closely linked to CD81. Hepatology. 2007;46:1722–1731.
Muriel P, Alba N, Perez-Alvarez VM, Shibayama M, Tsutsumi VK. Kupffer cells inhibition prevents hepatic lipid peroxidation and damage induced by carbon tetrachloride. Comp Biochem Physiol C Toxicol Pharmacol. 2001;130:219–226.
Niemela O, Parkkila S, Bradford B, Iimuro Y, Pasanen M, Thurman RG. Effect of Kupffer cell inactivation on ethanol-induced protein adducts in the liver. Free Radic Biol Med. 2002;33:350–355.
Michael SL, Pumford NR, Mayeux PR, Niesman MR, Hinson JA. Pretreatment of mice with macrophage inactivators decreases acetaminophen hepatotoxicity and the formation of reactive oxygen and nitrogen species. Hepatology. 1999;30:186–195.
Ju C, Reilly TP, Bourdi M, et al. Protective role of Kupffer cells in acetaminophen-induced hepatic injury in mice. Chem Res Toxicol. 2002;15:1504–1513.
Schwabe RF, Brenner DA. Mechanisms of liver injury. I. TNF-alpha-induced liver injury: role of IKK, JNK, and ROS pathways. Am J Physiol Gastrointest Liver Physiol. 2006;290:583–589.
Kamata H, Honda S, Maeda S, Chang L, Hirata H, Karin M. Reactive oxygen species promote TNFα-induced death and sustained JNK activation by inhibiting MAP kinase phosphatases. Cell. 2005;120:649–661.
Pham CG, Bubici C, Zazzeroni F, et al. Ferritin heavy chain upregulation by NF-kappaB inhibits TNFalpha-induced apoptosis by suppressing reactive oxygen species. Cell. 2004;119:529.
Asakawa M, Kono H, Amemiya H, et al. Role of interleukin-18 and its receptor in hepatocellular carcinoma associated with hepatitis C virus infection. Int J Cancer. 2006;118:564–570.
Zhang H-Y, Nanji AA, Luk JM, et al. Macrophage migration inhibitory factor expression correlates with inflammatory changes in human chronic hepatitis B infection. Liver Int. 2005;25:571–579.
Kallinowski B, Haseroth K, Marinos G, et al. Induction of tumour necrosis factor (TNF) receptor type p55 and p75 in patients with chronic hepatitis C virus (HCV) infection. Clin Exp Immunol. 1998;111:269–277.
Farinati F, Cardin R, Bortolami M, Guido M, Rugge M. Oxidative damage, pro-inflammatory cytokines, TGF-alpha and c-myc in chronic HCV-related hepatitis and cirrhosis. World J Gastroenterol. 2006;12:2065–2069.
Tomita M, Yamamoto K, Kobashi H, Ohmoto M, Tsuji T. Immunohistochemical phenotyping of liver macrophages in normal and diseased human liver. Hepatology. 1994;20:317–325.
Dolganiuc A, Garcia C, Kodys K, Szabo G. Distinct Toll-like receptor expression in monocytes and T-cells in chronic HCV infection. World J Gastroenterol. 2006;12:1198–1204.
Lin RS, Lee FY, Lee SD, et al. Endotoxemia in patients with chronic liver diseases: relationship to severity of liver diseases, presence of esophageal varices, and hyperdynamic circulation. J Hepatol. 1995;22:165–172.
Plachouras D, Stamatakos M, Baziaka F, et al. Portal and systemic endotoxemia in abdominal operations: the significance of acute abdomen. J Surg Res. 2006;134:133–137.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hosomura, N., Kono, H., Tsuchiya, M. et al. HCV-Related Proteins Activate Kupffer Cells Isolated from Human Liver Tissues. Dig Dis Sci 56, 1057–1064 (2011). https://doi.org/10.1007/s10620-010-1395-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-010-1395-y