Abstract
Tumor necrosis factor (TNF)-α exists in two bioactive forms, a 26-kDa transmembrane form (tmTNF-α) and a 17-kDa soluble form (sTNF-α). sTNF-α has been recognized as a key regulator of hepatitis; however, serum sTNF-α disappears in mice during the development of severe liver injury, and high levels of serum sTNF-α do not necessarily result in liver damage. Interestingly, in a mouse model of acute hepatitis, we have found that tmTNF-α expression on Kupffer cells (KCs) significantly increases when mice develop severe liver injury caused by lipopolysaccharide (LPS)/D-galactosamine (D-gal), and the level of tmTNF-α expression is positively related to the activity of serum transaminases. Therefore, we hypothesized that KC-expressed tmTNF-α constitutes a pathomechanism in hepatitis and have explored the role of tmTNF-α in this disease model. Here, we have compared the impact of KCstmTNFlow and KCstmTNFhigh on acute hepatitis in vivo and ex vivo and have further demonstrated that KCstmTNFhigh, rather than KCstmTNFlow, not only exhibit an imbalance in secretion of pro- and anti-inflammatory cytokines, favoring inflammatory response and exacerbating liver injury, but also induce hepatocellular apoptosis via tmTNF-α and the expression of another pro-apoptotic factor, Fas ligand. Our data suggest that KCtmTNFhigh is a major contributor to liver injury in LPS/D-gal-induced hepatitis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Liver injury caused by hepatitis is often associated with severe disorders of the immune response but not primary causes (Rolando et al. 2000). Kupffer cells (KCs) exert active roles in the immune regulation of hepatitis. Apart from their ability to produce immunosuppressive factors and metabolites to induce tolerance (Roland et al. 1994; You et al. 2008; Zhang et al. 2011), KCs are believed to promote liver injury through the secretion of proinflammatory cytokines and chemokines and the expression of death ligands (Bilzer et al. 2006). In murine models of hepatitis, the inhibition or deletion of KCs can attenuate or even completely suppress liver injury (Iimuro et al. 1994; Yamano et al. 2000). These data demonstrate that KCs are key targets for the immunomodulation of hepatitis.
Tumor necrosis factor-α (TNF-α) is a pleiotropic proinflammatory cytokine produced in the liver mainly by activated KCs. A growing body of evidence shows that soluble TNF-α (sTNF-α) is involved in various types of liver injury, including hepatitis and alcoholic and toxic liver injury (Hatano 2007; Antoniades et al. 2008). Upregulation of TNF-α in serum and hepatic tissue has been observed in lipopolysaccharide (LPS)/D-galactosamine (D-gal)-induced and Concanavalin A (Con A)-induced hepatitis models (Gantner et al. 1995; Mizuhara et al. 1994; Gonzalez-Teran et al. 2013; Yoshida et al. 2007). Pretreatment with anti-TNF-α neutralizing antibody can protect against liver damage (Gantner et al. 1995; Nakashima et al. 2008). Moreover, TNF receptor (TNFR) 1- or TNFR2-deficient mice exhibit resistance to Con A- or LPS/D-gal-induced liver injury (Kusters et al. 1997; Pfeffer et al. 1993). Collectively, these data suggest that sTNF-α is involved in the occurrence and development of hepatitis as a critical mediator produced by KCs. However, the reason that the reduction of TNF-α levels in serum and culture supernatants of liver tissues is accompanied by severe liver impairment at late stages of hepatitis is difficult to explain.
tmTNF-α is known to be the precursor of sTNF-α and has biological activities different from those of sTNF-α. tmTNF-α is often difficult to detect or can only be detected at low levels, even upon stimulation, as a result of being cleaved chiefly by TNF-α converting enzyme (TACE; Ware et al. 1992). Several studies have shown abnormally increased expression of tmTNF-α in neutrophils during acute inflammation (Wright et al. 2011), and in non-small cell lung carcinoma (Ardestani et al. 2013) as well as primary breast cancer (Yu et al. 2013). Therefore, both the roles of tmTNF-α in diseases and its therapeutic potential as a possible target have attracted growing interest. A few groups have reported the effect of tmTNF-α on acute hepatitis, but some transgenic studies have displayed diametrically opposed findings regarding the impact of tmTNF-α on hepatitis (Kusters et al. 1997; Olleros et al. 2010). Olleros et al. (2010) have reported protection from liver damage caused by BCG/LPS or D-GALN/LPS administration in TNF−/−, tmTNF knock-in, and sTNFR1-Fc transgenic mice, whereas Kusters et al. (1997) have demonstrated that Con-A-induced liver injury occurs in noncleavable tmTNF-α transgenic mice. tmTNF-α might exert different function in different hepatitis models. The increased expression of tmTNF-α on KCs by melphalan-induced TACE inhibition has been reported to mediate hepatocyte apoptosis notably in an in vitro primary mouse liver cell model and an ex vivo isolated perfused mouse liver model (Kresse et al. 2005). However, during the development of hepatitis, the kinetic expression of endogenous tmTNF-α in neither mouse models nor patients has as yet been reported. Do KCs express tmTNF-α at high level during the development of acute hepatitis? In particular, what is the in vivo role of KCs that express tmTNF-α at high level in the liver injury.
In the present study, we have found that increased endogenous tmTNF-α, but not sTNF-α, is consistent with the time at which obvious liver damage induced by LPS/D-gal occurs. KCs isolated from mice treated with LPS/D-gal for 6 h express tmTNF-α at high levels (KCstmTNFhigh), whereas KCs from mice treated for 2 h produce tmTNF-α at very low levels (KCstmTNFlow). KCstmTNFhigh, rather than KCstmTNFlow, have been shown ex vivo and in vivo to be mainly responsible for the imbalance between pro- and anti-inflammatory cytokines and the induction of hepatocyte apoptosis, contributing to LPS-induced liver injury.
Materials and methods
Animals
The animal study was approved by the Animal Care and Use Committee of Huazhong University of Science and Technology. Six- to 8-week-old male C57BL/6 mice were purchased from the Center for Animal Experiment and ABSL-3 Laboratory of Wuhan University. Animals were housed under specific pathogen-free conditions with a 12-h light–dark cycle and allowed free access to food and water.
Induction of hepatitis
Hepatitis was induced by intraperitoneal injection with 10 μg/kg LPS (Sigma-Aldrich; Escherichia coli 0111:B) plus 500 mg/kg D-gal (Sigma-Aldrich). Liver tissues and blood samples were then collected before (0 h) or after (2, 4, 6 h) injection. Hepatocellular damage was evaluated by liver histology and by serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST) activities.
Isolation of KCs and hepatocytes
Liver KCs and hepatocytes were isolated by the collagenase digestion technique with some modifications (Kuboki et al. 2007; Jung et al. 2012). Briefly, mouse liver was perfused in situ for 5 min with Hank’s buffered salt solution containing 0.05 % collagenase and then excised, minced, and passed through a 70-μm stainless steel mesh. To obtain the hepatocytes, the filtrates were centrifuged at 150g for 3 min, and then the cell pellet was washed three times and resuspended in RPMI 1640 medium supplemented with 10 % fetal bovine serum (FBS). To obtain the KCs, the initial cell suspension after collagenase digestion was resuspended in 40 % Percoll, then overlaid onto 70 % Percoll, and centrifuged at 750g for 20 min. The KC fraction was collected from the interface and overlaid onto Percoll gradient (25 %/50 %) for further purification and then centrifuged at 1800g for 30 min. KC-enriched monocytes located at the interface were harvested, washed, and suspended in RPMI 1640 containing 10 % FBS. After incubation for 30 min at 37 °C, non-adherent cells were removed, and adherent KCs were grown in RPMI 1640 containing 10 % FBS, 100 U/ml penicillin G, and 100 μg/ml streptomycin at 37 °C in a humidified atmosphere containing 5 % CO2.
KC culture in vitro
A total of 1 × 106 KCs isolated from LPS/D-gal-treated mice for 0 h (KCs-0h), 2 h (KCs-2h), 4 h (KCs-4h), or 6 h (KCs-6h) were seeded in a 24-well plate and incubated for 4 h at 37 °C, 5 % CO2. Culture supernatants were then collected and stored at −80 °C until tested. To measure the stability of tmTNF-α expression over time, KCs isolated from 2-h-treated (KCs-2h) or 6-h-treated (KCs-6h) mice were cultured for 0, 2, or 6 days at 37 °C, 5 % CO2. Then, KCs were collected, and tmTNF-α expression was analyzed by flow cytometry (FCM).
KC-hepatocyte coculture
For the determination of the coculture time, 1 × 106 liver KCs isolated from LPS/D-gal-treated mice for 2 h (KCs-2h) or 6 h (KCs-6h) were directly cocultured with 2 × 105 freshly isolated primary hepatocytes from normal mice for 6, 18, or 24 h at 37 °C, 5 % CO2. For transwell experiments, 1 × 106 liver KCs-6h were cocultured with hepatocytes at an effect/target (E/T) ratio of 1:1 or 5:1, either in contact or separated by a transwell membrane for 18 h. For neutralization of tmTNF-α, 1 × 106 KCs-6h were pretreated for 30 min with an anti-TNF-α antibody (10 μg/ml; BD Pharmingen) and then directly cocultured with 2 × 105 hepatocytes for 6 or 18 h. After coculture, hepatocyte apoptosis and AST activity were measured in the culture supernatants.
Adoptive transfer of KCs
KCs isolated from LPS/D-gal-treated mice for 2 h (KCs-2h) or 6 h (KCs-6h) were collected, respectively. Seven days after tail vein injection of 3 × 106 KCs-2h or KCs-6h into mice (Jung et al. 2012), LPS (10 μg/kg) plus D-gal (500 mg/kg) were intraperitoneally injected into each group of mice (n = 4). Liver tissues and blood samples were then collected 4 h post-injection.
RNA preparation and quantitative real-time polymerase chain reaction
Total cellular RNA was extracted from KCs by using Trizol reagents (Invitrogen). Of total RNA, 500 ng was reversely transcribed by using the Superscript Reverse Transcriptase kit (Invitrogen). The cDNA samples were then examined by quantitative real-time polymerase chain reaction (PCR) with the following primer pairs: FasL forward, 5’-AAGAAGGACCACAACACAAATCTG-3’, reverse, 5’-CCCTGTTAAATGGGCCACACT-3’; D-glyceraldehyde-3-phosphate dehydrogenase (GAPDH) forward, 5’-AAGGGCTCATGACCACAGTC-3’, reverse, 5’-GGATGCAGGGATGATGTTCT-3’. cDNA was amplified with the QuantiTect SYBRgreen PCR kit (Qiagen, Venio, The Netherlands) in an ABI 7500 Real-time PCR system (Applied Biosystems). The reactions were carried out in triplicate for 3 min at 95 °C, followed by 15 s at 95 °C, 20 s at 58 °C, and 20 s at 72 °C for 40 cycles. Results were analyzed by using the 2−ΔΔCt method and normalized with GAPDH.
Detection of transaminase activity and cytokines
ALT and AST activities in serum or culture supernatants were measured by using a Beckman Synchron CX5 system in the clinical laboratory of Tongji Hospital, Huazhong University of Science and Technology. The concentrations of sTNF-α, interleukin 4 (IL)-4, IL-6, and IL-10 were measured by using commercial enzyme-linked immunosorbent (ELISA) kits (eBioscience) according to the manufacturers’ protocols.
Flow cytometry
For the detection of tmTNF-α expression, KCs were collected and incubated for 1 h at 4 °C with an anti-TNF-α antibody (Abcam). Then, KCs were reacted at 4 °C with a fluorescein isothiocyanate (FITC)-conjugated secondary antibody for 40 min. Stained cells were analyzed on a FACS Calibur 440 E flow cytometer (Becton Dickinson). For the detection of hepatocyte apoptosis, hepatocytes were stained with FITC-conjugated annexin V and propidium iodide (PI) according to the manufacturer’s instructions (KeyGEN, Nanjing, China). The percentage of apoptotic (annexin V-positive) hepatocytes was determined by FCM.
Western blot
Total protein was extracted from isolated KCs or liver tissues in ice-cold lysis buffer (50 mmol/l TRIS–HCl pH 7.5, 150 mmol/l NaCl, 5 mmol/l EDTA, 1 % NP-40) containing a protease inhibitor cocktail (Sigma-Aldrich). A sample of 50 μg of extract protein was fractionated by 12 % polyacrylamide gel electrophoresis and transferred to polyvinylidene difluoride membranes by electroblotting. The membranes were blocked with 5 % skim milk in phosphate-buffered saline (PBS) containing 0.05 % Tween-20 for 1 h at room temperature and then incubated overnight at 4 °C with primary antibodies including anti-TNF-α (Abcam), anti-FasL (eBioscience), anti-caspase3 (Cell Signaling Technology), anti-β-actin, and anti-GAPDH (Santa Cruz), followed by corresponding horseradish-peroxidase-conjugated anti-rabbit or anti-mouse IgG secondary antibodies (Pierce) for 1 h at room temperature. Immunoreactive bands were detected by using an enhanced chemiluminescence kit (Pierce) and visualized with the Kodak Image Station 4000MM (Kodak).
Histology
Mouse liver tissues were excised and fixed with 10 % formalin in PBS for 24 h and then embedded in paraffin wax. Tissue sections (4 μm) were stained with hematoxylin-eosin (H&E) routinely for morphological evaluation.
Confocal microscopy
KCs were fixed with 4 % paraformldehyde at room temperature for 15 min and blocked with 3 % BSA in PBS for 1 h at room temperature. Immune staining was performed by incubation at room temperature for 1 h with a primary anti-TNF-α (Abcam) antibody from rabbit and FITC-anti-F4/80 from rat (Biolegand) and then with a secondary tetramethylrhodamine-isothiocyanate-labeled anti-rabbit IgG (Biovision). The cells were costained with 4,6-diamidino-2-phenyl indole (DAPI; 0.667 μg/ml, room temperature, 5 min) for nuclear staining and observed under a confocal microscope FU5000 (Olympus, Tokyo, Japan).
TUNEL staining
To evaluate hepatocyte apoptosis, the terminal deoxynucleotidyl transferase-mediated dUTP nick end-labeling (TUNEL) assay was carried out with a commercial kit (FITC-labeled POD, Boster, Wuhan, China) following the manufacturer’s recommended protocol.
TNF-α bioassay
Hepatocytes (105/well) as target cells were seeded in a 96-well microtiter plate. Supernatants from an 18-h culture of KCs-6h cells alone or their 18-h coculture with hepatocytes or 4 % paraformaldehyde-fixed KCs-6h cells (106) were added to target cells at an E/T ratio of 10:1 and incubated for 24 h. For the neutralization of TNF-α, the KCs-6h cells were pretreated with a specific antibody for 30 min before addition to the target cells without a wash step. Cell viability was then measured by staining for 4 h with 30 mM glucose-PBS containing 0.5 mg/ml 3-(4,5-dimethyl-thiazolyl-2)-2, 5-diphenol tetrazolium bromide (MTT; Sigma Chemical, St. Louis, Mo., USA), followed by cell lysis with 0.1 ml dimethylsulfoxide. The photometric measurement was performed at 570 nm on a microplate reader (Tecan, Austria). TNF-induced cytotoxicity was calculated by the following formula: cell death rate (%) = (1–ODsample/ODcontrol) × 100 %.
Statistical analysis
The differences were analyzed by the nonparametric Mann–Whitney U-test between two groups or the nonparametric one-way analysis of variance for more than two groups. Statistical correlation was assessed by the Pearson correlation coefficient. Data are presented as means ± SD. P values <0.05 were considered to be statistically significant.
Results
Increased tmTNF-α expression in KCs 6 h after LPS/D-gal treatment
First, we explored the changes in serum levels of TNF-α after the induction of hepatitis by LPS/D-gal, and the results showed that serum TNF-α levels increased rapidly and peaked at 2 h, but declined sharply 4 h post-treatment (Fig. 1a), similar to the observations of previous studies by others (Gonzalez-Teran et al. 2013; Yoshida et al. 2007). KCs isolated from mice treated with LPS/D-gal at 0 h (KCs-0h), 2 h (KCs-2h), 4 h (KCs-4h), or 6 h (KCs-6h) were then cultured for 4 h, and the sTNF-α content was detected in culture supernatants. Interestingly, the changes in sTNF-α release in the culture supernatants of isolated KCs (Fig. 1b) showed the same trend as those in the serum post-treatment. The results indicate that the changes in sTNF-α levels in local inflammatory lesions are in accordance with those in circulation.
Increased transmembrane tumor necrosis factor-α (tmTNF-α) expression in Kupffer cells (KCs) at 6 h after lipopolysaccharide (LPS)/D-galactosamine (D-gal) treatment. a Serum TNF-α levels at 0, 2, 4, or 6 h after intraperitoneal injection of LPS (10 μg/kg) plus D-gal (500 mg/kg) were measured by enzyme-linked immunosorbent assay (ELISA; n = 5). b KCs (1 × 106/well) isolated from mice at 0 h (KCs-0h), 2 h (KCs-2h), 4 h (KCs-4h), or 6 h (KCs-6h) after treatment were cultured in vitro for 4 h, and sTNF-α content in culture supernatants was analyzed by ELISA (n = 5). Total protein lysates of KCs-0h, KCs-4h, and KCs-6h were subjected to Western blot with anti-tmTNF-α or anti-D-glyceraldehyde-3-phosphate dehydrogenase (GAPDH) antibodies. c, c’ Representative immunoblots and histogram, respectively, showing densitometric analysis of tmTNF-α levels normalized to GAPDH (n = 3). Surface expression of tmTNF-α on KCs from the treated mice at various time-points was detected by flow cytometry (FCM; n = 6). d, d’ Representative FCM image and quantitative analysis of KCs, respectively. tmTNF-α expression (red) on F4/80-stained (green) KCs was observed by confocal microscope (e-g’’’). Nuclei were stained by DAPI (blue). Quantitative data represent means ± SD. **P < 0.01, ***P < 0.001 vs. 0 h
To investigate whether tmTNF-α is involved in the development of hepatitis, we detected the expression of tmTNF-α in KCs at various time-points after LPS/D-gal administration. As shown in Fig. 1c, c’, the expression of tmTNF-α in total cell lysates did not change significantly in KCs-4h but increased dramatically in KCs-6h, as compared with that in KCs-0h. Additionally, the surface expression of tmTNF-α on KCs (Fig. 1d, d’) isolated from LPS/D-gal-treated mice at various time-points also exhibited similar features. The confocal data showed evident tmTNF-α expression (red-stained) on F4/80-stained (green) KCs-6h (Fig. 1g, g’’’) rather than on KCs-2h (Fig. 1f, f’’’) or KCs-0h (Fig. 1e, e’’’). These results suggest that tmTNF-α is involved in the development of hepatitis induced by LPS/D-gal, although sTNF-α disappeared from the serum.
Level of tmTNF-α expression on KCs-6h was positively correlated with serum transaminase activity
To explore further the possible association of tmTNF-α expression on KCs with hepatocellular damage in LPS/D-gal-induced hepatitis, we evaluated the correlation between serum transaminase activity and tmTNF-α expression on KCs after 6-h treatment with LPS/D-gal (KCs-6h). As shown following H&E staining of liver sections (Fig. 2a, a’’’), hepatocytes were swollen at 2 h and 4 h after LPS/D-gal-treatment (Fig. 2a’, a’’), but significant hepatic sinus congestion, hepatic cords fracture, necrosis, and inflammatory cell infiltration were observed at 6 h post-injection (Fig. 2a’’’), indicating severe liver injury. In agreement with the results of H&E staining, the activities of serum ALT and AST were significantly elevated at 6 h but were maintained at normal levels at 2 and 4 h post-treatment (Fig. 2b, c). More remarkably, tmTNF-α expression levels on KCs-6h were positively correlated with serum ALT and AST activities (ALT, r = 0.818, P = 0.0004; AST, r = 0.848, P = 0.0001; Fig. 2d). These data strongly suggest that tmTNF-α, but not sTNF-α, is closely related to the liver injury.
Level of tmTNF-α expression on KCs-6h was positively correlated with serum transaminase activity. a-a’’’ Representative H&E-stained liver sections at various time-points after LPS/D-gal injection. Original magnification, ×200. b, c Serum alanine aminotransferase (ALT, b) and aspartate aminotransferase (AST, c) activities at corresponding time-points were measured (n = 5). d Correlation analysis between serum ALT and AST activities at 6 h post-injection, and percentages of tmTNF-α-positive KCs from 6-h-treated group (KCs-6h; n = 13). Correlations were calculated by using the Pearson coefficient; r and P values are presented. Data represent means ± SD. ***P < 0.001 vs. 0 h
KCstmTNFhigh were involved in LPS-induced liver injury via imbalanced secretion of pro- and anti-inflammatory cytokines
The dysregulated production of inflammatory cytokines is an important cause of severe liver injury. Therefore, after LPS/D-gal administration, we analyzed the changes in content of serum IL-6, IL-4, and IL-10, representing the pro- and anti-inflmmatory cytokines, respectively, and used the ratios of serum IL-6 to IL-10 to assess the balance between pro- and anti-inflammatory cytokines. As shown in Fig. 3a-c, levels of serum IL-6 and IL-10 increased remarkably, peaked at 4 h and 2 h post-treatment, respectively, but markedly decreased at 6 h. However, the serum levels of IL-4 were only slightly elevated at 6 h. Although the decrease of serum IL-6 did not match the severity of liver injury, the dropped level of IL-6 was still 87.8 % of its peak, in contrast to the attenuate level of IL-10 being 23.6 % of its peak. Therefore, serum IL-6/IL-10 ratios significantly increased 6 h post-treatment (Fig. 3d), at which time the treated mice developed serious liver damage. In addition, the levels of tmTNF-α expression on KCs-6h were positively correlated with serum IL-6/IL-10 ratios in the 6-h-treated group (r = 0.9808, P = 0.0032; Fig. 3i).
Changes in interleukin-6 (IL-6) and IL-10 levels and ratios of IL-6/IL-10 in culture supernatants of KCs were consistent with those in serum. Levels of serum IL-4 (a), IL-6 (b), and IL-10 (c) were measured by ELISA, and the ratios of IL-6 to IL-10 (d) were calculated at various time-points after LPS/D-gal injection (n = 5). Concentrations of IL-4 (e), IL-6 (f), and IL-10 (g) were analyzed, and the ratios of IL-6 to IL-10 (h) were calculated in 4-h culture supernatants of KCs isolated from mice at 0 h (KCs-0h), 2 h (KCs-2h), 4 h (KCs-4h), or 6 h (n = 5) after treatment. Correlation analysis between IL-6/IL-10 ratios in serum at 6 h post-injection (i) or in 4-h culture supernatants of KCs-6h (j) and percentages of tmTNF-α-positive KCs from the 6-h-treated group (KCs-6h; n = 5). Correlations were calculated by using the Pearson coefficient; r and P values are presented. Data represent means ± SD. *P < 0.05, ***P < 0.001 vs. 0 h
Since activated KCs are important sources of serum inflammatory cytokines, we suspected that the dysfunction of tmTNF-α-expressing KCs play a considerable role in the imbalance of serum inflammatory cytokines. To testify this hypothesis, we cultured KCs isolated from mice at 0 h (KCs-0h), 2 h (KCs-2h), 4 h (KCs-4h), or 6 h (KCs-6h) after treatment and kept in vitro for 4 h, and the content of IL-4, IL-6, and IL-10 was measured in the culture supernatants. In contrast to the increased levels of serum IL-4, KCs-6h released less IL-4 compared with KCs from other time points (Fig. 3e), indicating that KCs-6h did not contribute to the elevated serum levels of IL-4 at 6 h. However, the content of IL-6 (Fig. 3f) and IL-10 (Fig. 3g) in the culture supernatants of KCs displayed the same tendency that was observed in serum after an LPS/D-gal challenge. Although the peak of IL-10 was observed in the supernatants of KCstmTNFlow-2 h and the peak of IL-6 in the supernatants of KCstmTNFlow-4 h, IL-6/IL-10 ratios were less than 4. In contrast, IL-6/IL-10 ratios in culture supernatants of KCstmTNFhigh-6 h were markedly increased over 15 (Fig. 3h), and tmTNF-α expression levels on KCs-6h were positively correlated with IL-6/IL-10 ratios either in KC-6 h culture supernatants (r = 0.9510, P = 0.0129, Fig. 3j) or in serum from 6-h-treated mice (r=0.9808, P = 0.0032; Fig. 3i). The above results verify our hypothesis and further indicate that KCstmTNFhigh are responsible for the imbalanced secretion of pro- and anti-inflammatory cytokines, and that the ratio of IL-6/IL-10 is a suitable indicator of the severity of acute hepatitis.
KCstmTNFhigh induced rapid hepatocellular apoptosis via cell-cell contact
Since hepatocyte apoptosis is known to be a major cause of hepatocellular injury in a variety of liver diseases, we assumed that the expression of tmTNF-α at a high level on KCs might induce hepatocyte apoptosis via cell-cell contact. To demonstrate this hypothesis, we investigated hepatocyte apoptosis and supernatant AST activity when freshly isolated liver cells from normal mice were cocultured with KCs from LPS/D-gal-treated mice. As shown in Fig. 4a, a’, the apoptotic hepatocytes rapidly increased at 6 h and peaked at 24 h after coculture of liver cells with KCs-6h that expressed tmTNF-α at a high level. However, no obvious change occurred in hepatocyte apoptosis over time after coculture of liver cells with KCs-2h that expressed tmTNF-α at low levels but secreted sTNF-α at high levels (Fig. 4c). Similarly, a significant increase of AST activity was observed in KC-6 h, but not in KCs-2h, and hepatocyte coculture supernatant (Fig. 4b).
KCstmTNFhigh-6 h induced rapid hepatocellular apoptosis via cell-cell contact. a, b Liver KCs (1 × 105) isolated from 2-h (KCs-2h) or 6-h (KCs-6h) LPS/D-gal-treated mice were directly cocultured with 2 × 104 freshly isolated hepatocytes from normal mice for 0, 6, 18, or 24 h. Hepatocytes were stained with fluorescein isothiocyanate (FITC)-conjugated annexin V and propidium iodide (PI). The percentage of apoptotic (annexin V-positive) hepatocytes is shown. a, a’ Representative FCM image and quantitative analysis as a histogram, respectively. b Supernatant AST activities were measured at various time-points after coculture. c, f sTNF-α in supernatants was detected by ELISA. d, e Liver KCs-6h (1 × 105) were cocultured with hepatocytes at an E/T ratio of 1:1 or 5:1, either in contact or separated by a transwell memberane for 18 h. Hepatocytes were stained with FITC-conjugated annexin V and PI. The percentage of apoptotic hepatocytes is shown. d, d’ Representative FCM image and quantitative analysis as a histogram, respectively. e Supernatant AST activities were measured after coculture. Data represent means ± SD of three independent experiments. **P < 0.01, ***P < 0.001 vs. 0 h
Next, to determine the importance of cell contact in the apoptosis-inducing effect of KCs-6h, we cultured primary liver cells either in direct contact with KCs-6h or separated from them by a transwell membrane. As expected, after 18 h of coculture, only when hepatocytes were in direct contact with KCs-6h that expressed tmTNF-α at high levels but secreted a small amount of sTNF-α at an E/T ratio of 5:1 (Fig. 4f) were there significant increases in hepatocyte apoptosis (Fig. 4d, d’) and supernatant AST activity (Fig. 4e), respectively. These data suggest that KCstmTNFhigh induce apoptosis in liver cells via cell-cell contact.
KCstmTNFhigh induced hepatocellular apoptosis because of expression of tmTNF-α and FasL
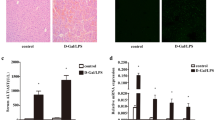
To explore further the role of tmTNF-α in hepatocyte apoptosis induced by KCstmTNFhigh, we used a neutralizing anti-TNF-α antibody to inhibit tmTNF-α-TNFR signaling. The results showed that the apoptosis-inducing effect of KCstmTNFhigh-6 h on hepatocytes after direct coculture could be partly blocked by pretreatment with an anti-TNF-α antibody (Fig. 5a, a’). In agreement with this, AST activity in coculture supernatants displayed the same phenomena (Fig. 5b). The detectability of a small amount of sTNF-α in cocultures maintained for 18 h indicated that TACE was not activated in KCstmTNFhigh-6 h (Fig. 5c). To investigate whether this small amount of sTNF-α in the coculture system could affect tmTNF-α-mediated cytotoxicity, we performed a cytotoxic bioassay for both forms of TNF-α. In contrast to the cytotoxic effect of fixed KCs-6h alone, supernatants from neither KCs-6h alone nor its coculture with hepatocytes could kill hepatocytes. Only the addition of fixed KCs-6h to these two supernatants did the cytotoxicity to hepatocytes occur, but the sTNF-containing supernatants could not affect the cytotoxicity of tmTNF-α on KCs-6h (Fig. 5d). These data suggest that tmTNF-α on KCs-6h, but not sTNF-α released by these cells, was cytotoxic to hepatocytes.
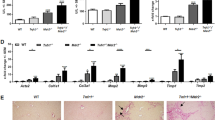
KCstmTNFhigh-6 h induced hepatocellular apoptosis caused by tmTNF-α and the induction of FasL. a, b Liver KCs (1 × 106) isolated from 6-h LPS/D-gal-treated mice (KCs-6h) were directly cocultured with 2 × 105 freshly isolated hepatocytes from normal mice for 6 or 18 h. For neutralization of tmTNF-α, KCs-6h were treated for 30 min with an anti-TNF-α antibody (α-TNF-α, 10 μg/ml) prior to the addition to hepatocytes. Hepatocytes were stained with FITC-conjugated annexin V and PI. The percentage of apoptotic hepatocytes is shown. a, a’ Representative FCM image and quantitative analysis as a histogram, respectively. b Supernatant AST activities measured 6 or 18 h after coculture. c Amount of sTNF-α in supernatants as detected by ELISA. d Cytotoxicity of sTNF-α in supernatants from culture of KCs-6h or their coculture with hepatocytes or/and cytotoxicity of tmTNF-α on fixed KCs-6h to hepatocytes as determined by bioassay (SN supernatant, Hep. hepatocyte). e KCs isolated from 2-h-treated (KCs-2h) or 6-h-treated (KCs-6h) mice were collected. Levels of mRNA for FasL were determined by real-time reverse transcription and the polymerase chain reaction and normalized to GAPDH (top). Total protein from lysates of isolated KCs-2h and KCs-6h were subjected to Western blot with anti-FasL or anti-GAPDH antibodies (bottom). Data represent means ± SD of three independent experiments. **P < 0.01, ***P < 0.001 vs. hepatocyte alone
Because (1) the Fas/FasL pathway has been implicated as an important known cellular pathway mediating apoptosis in hepatocytes (Jung et al. 2012), and (2) the rate of hepatocyte apoptosis remained at a relatively high level, especially after a 18 h-coculture, despite being reduced to some extent after TNF-α neutralization, we assumed that KCs-6h might induce hepatocyte apoptosis by expressing other apoptosis-related factors such as FasL. In agreement with our expectations, KCstmTNFhigh-6 h promoted the expression of FasL at both mRNA and protein levels (Fig. 5e). The data described above suggest that both tmTNF-α and FasL might be related to hepatocyte apoptosis induced by KCs-6h.
Adoptive transfer of KCstmTNFhigh accelerated liver injury induced by LPS/D-gal
To examine further the regulatory effect of KCstmTNFhigh in the development of hepatitis in vivo, LPS/D-gal-induced liver damage was compared between the adoptive transfer of KCstmTNFlow-2 h and the transfer of KCstmTNFhigh-6 h. At 1 week after adoptive transfer of carboxyfluorescein succinimidyl ester-labeled KCs via tail vein injection, about 45 % of KCs have been reported to be located in the liver (Jung et al. 2012). Our results showed that tmTNF-α expression remained stable when KCs-6h were cultured in vitro for up to 6 days (Fig. 6a, a’), an observation that supported the validity of adoptive transfer.
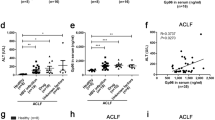
Adoptive transfer of KCstmTNFhigh accelerated liver damage induced by LPS/D-gal. KCs isolated from 2-h (KCs-2h) or 6-h (KCs-6h) LPS/D-gal-treated mice were cultured in vitro for 0, 2, or 6 days. Surface expression of tmTNF-α on KCs at various times was detected by flow cytometry (FCM). a, a’ Representative FCM image and quantitative analysis of three independent experiments as a histogram, respectively. b–h At 7 days after tail vein injection of 3 × 106 KCs-2h or KCs-6h into mice, LPS (10 μg/kg) plus D-gal (500 mg/kg) were intraperitoneally injected into each group of mice (n = 4). Treatment of mice with or without LPS/D-gal alone served as controls. Blood samples and livers were then collected at 4 h post-injection. b-b’’’ Representative H&E-stained liver sections from each group of mice. Original magnification, ×200. c Level of serum IL-6. d Level of serum IL-10. f Level of serum IL-4. g Level of serum sTNF-α. h Level of serum AST. e Serum IL-6/IL-10 ratios were calculated. i–i’’’ Representative TUNEL-stained liver sections from each group of mice. Original magnification, ×200. j Caspase 3 activation was determined by Western blot. Quantitative data represent means ± SD. *P < 0.05, **P < 0.01
Then, 7 days after adoptive transfer of KCs-2h or KCs-6h into normal mice, hepatitis was induced by injection of LPS/D-gal. At 4 h post-injection, KCs-2h transfer did not affect the pathological changes induced by LPS/D-gal, including hepatocyte swelling, inflammatory cell infiltration, and some necrosis, whereas KCs-6h transfer did indeed aggravate LPS-induced liver injury, which was manifested as significant hepatic sinus congestion, hepatic cords fracture, hydropic degeneration, and some necrosis (Fig. 6b-b’’’). Serum IL-6 levels (Fig. 6c) were much higher, and serum IL-10 levels (Fig. 6d) were notably lower in mice that had received KCs-6h compared with those that had received KCs-2h, resulting in extremely high IL-6/IL-10 ratios in the former group (Fig. 6e); this was in accordance with the results previously described. In addition, a trace of serum IL-4 (Fig. 6f) was only found in KCs-6h-transfer mice, whereas a slightly elevated serum concentration of sTNF-α (Fig. 6g) was found in KCs-2h-transfer mice, but no statistical significance was seen between the groups of transfer of KCs-2h and of KCs-6h. Moreover, increased serum ALT activity (Fig. 6h), significant apoptosis in hepatocytes (Fig. 6i-i’’’) and activation of caspase 3 (Fig. 6j) were also observed in the KCs-6h-transfer group compared with the KCs-2h-transfer group. Our results above suggest that KCstmTNFhigh accelerated the progression of liver damage.
Discussion
sTNF-α is widely accepted to play a crucial role in the pathomechanism of hepatitis (Pfeffer et al. 1993; Kresse et al. 2005; Rudiger and Clavien 2002; Lehmann et al. 1987; Mohler et al. 1994). However, some phenomena are difficult to explain: (1) initially elevated serum TNF-α disappears in mice developing severe liver injury (Gonzalez-Teran et al. 2013; Yoshida et al. 2007); (2) high serum levels of TNF-α do not necessarily result in liver damage (Leist et al. 1995); (3) although a combination of sTNF-α and D-gal by intravenous injection for 8 h induces severe liver damage, sTNF-α alone does not exert the same destructive effect (Gonzalez-Teran et al. 2013). In the present study, our data have also confirmed that sTNF-α fails directly to cause liver damage; this is supported by the following observations: (1) the dynamic changes in serum TNF-α are inconsistent with the severity of liver injury or, to be specific, the levels of serum TNF-α peak at 2 h and nearly disappear at 4 h after LPS/D-gal treatment, whereas significant liver impairment does not occur during this period; (2) the highest level of sTNF-α is produced by KCstmTNFlow-2 h, which are unable to induce hepatocyte apoptosis and AST release, either in direct or in indirect coculture with liver cells.
Our present results originally demonstrated that tmTNF-α expressing KCs could directly cause liver injury in vivo, on the basis of several lines of evidence. (1) Contrary to the changes in serum TNF-α, the levels of tmTNF-α expression on KCs were slightly upregulated at 2 h and 4 h but markedly increased at 6 h after LPS/D-gal challenge. Confocal data showed obvious tmTNF-α expression on the surface of F4/80+ KCs-6h rather than on KCs-2h. More importantly, tmTNF-α expression on KCs-6h was positively correlated with serum transaminase activity. (2) KCstmTNFhigh-6 h could only induce hepatocyte apoptosis via cell-cell contact but not kill the hepatocytes in an indirect coculture system, although a certain amount of sTNF-α was still detected in either KCs-6h culture or coculture supernatants. Furthermore, KCs-6h culture or coculture supernatants failed to kill hepatocytes and did not enhance the cytotoxicity of fixed KCs-6h. (3) Neutralization of tmTNF-α expressed on KCs could partly block the hepatocyte apoptosis. These data strongly suggest that tmTNF-α, but not sTNF-α, is directly involved in LPS/D-gal-induced liver impairment and related to the development of hepatitis.
The release of inflammatory cytokines and the interaction amongst these factors play crucial roles in the development of liver injury (Cressman et al. 1996; Louis et al. 2003; Sun et al. 2004). The imbalance between pro- and anti-inflammatory cytokines is closely associated with the severity of hepatitis (Antoniades et al. 2008). Because of the extremely unstable content and the lack of specificity of serum cytokines, they cannot effectively predict the severity of liver injury. In the present study, the levels of IL-4 were not significantly changed, and we used the changes in ratios of serum IL-6 to IL-10 to reflect the imbalance between pro- and anti-inflammatory cytokines. Our results revealed that the increased IL-6/IL-10 ratios were consistent with the severity of liver damage. The IL-6/IL-10 ratio reached a relative maximum when severe liver damage occurred. Our adoptive transfer experiments also showed that notably high IL-6/IL-10 ratios in serum occurred in KCs-6h-transferred mice, in which liver injury was aggravated at 4 h after LPS/D-gal injection. Taken together, these data demonstrate a correlation between the imbalance of pro- and anti-inflammatory cytokines and the development of acute hepatitis and further suggest that the ratio of serum IL-6/IL-10 might be a suitable indicator of disease severity.
As IL-10 and IL-6 are mainly synthesized and secreted by KCs (Rolando et al. 2000; Bilzer et al. 2006), and as KCstmTNFhigh were closely related to liver injury, we hypothesized that these KCs were mainly responsible for the imbalance between IL-10 and IL-6. As expected, when KCs from LPS/D-gal-treated mice at different time-points were cultured in vitro for 4 h, the changes in supernatant IL-6 and IL-10 levels and the ratios of IL-6 to IL-10 were similar to the changes in serum. Although IL-6 and IL-10 released by KCstmTNFhigh-6 h were decreased, the decreased extent of IL-10 was much greater than that of IL-6, and thus the IL-6/IL-10 ratio reached a relative maximum. Therefore, we are tempted to speculate that the imbalance in secretion of pro- and anti-inflammatory cytokines, as a result of the dysfunction of KCstmTNFhigh, is one of the important reasons for the occurrence and development of hepatitis.
Our transwell experiments validated the idea that rapid apoptosis was induced in hepatocytes 6 h after direct coculture with KCstmTNFhigh-6 h, whereas no obvious apoptosis was found in the KCstmTNFlow-2 h-hepatocyte coculture system, even if sTNF-α was present in the culture supernatants. Furthermore, in LPS-induced hepatitis models, most mice show serious liver damage at 6 h after LPS treatment (Gonzalez-Teran et al. 2013; Yoshida et al. 2007), suggesting that rapid hepatocyte apoptosis induced by KCstmTNFhigh is closely associated with severe liver injury in mice developing hepatitis. Jung et al. (2012) reported that 1 week after adoptive transfer, 45 % of carboxyfluorescein-succinimidyl-ester-labeled adoptively transferred KCs were localized in liver. Therefore, we checked the length of time that tmTNF-α expression could persist on KCs-6h and found that tmTNF-α was stably expressed for at least 6 days on these cells. In vivo transfer of KCs further verified that mice receiving KCstmTNFhigh developed severe liver injury and exhibited notable hepatocyte apoptosis, activation of caspase 3, and the release of AST in serum at 4 h post LPS/D-gal treatment, indicating that the progression of liver damage caused by LPS/D-gal was accelerated through the adoptive transfer of KCstmTNFhigh. The expression of tmTNF-α on KCs induced in vitro by melphalan has been reported to mediate hepatocyte apoptosis, as the coculture and neutralization of tmTNF-α nearly totally prevents the induction of apoptosis (Kresse et al. 2005). However, our results have shown that the pretreatment of KCs-6h with an anti-TNF-α antibody only partly blocked hepatocyte apoptosis, suggesting that KCs-6h can directly induce hepatocyte apoptosis via tmTNF-α, and that other apoptosis pathways must also be involved in this apoptosis-inducing effect. Our study has confirmed that FasL expression was much higher in KCstmTNFhigh-6 h than in KCstmTNFlow-2 h. The liver is very sensitive to Fas-mediated apoptosis because Fas antigen is highly and constitutively expressed on hepatocytes (Pinkoski et al. 2000). Furthermore, in agreement with our results, LPS has been reported to induce the expression of FasL, rather than Fas, on KCs, whereas the expression of Fas, rather than FasL, can be upregulated in hepatocytes in response to LPS. The differential expression of FasL between KCstmTNFhigh and KCstmTNFlow suggests the possible effect of tmTNF-α signaling on KCs. Our previous study has shown that the activation of tmTNF-α-mediated reverse signaling by sTNFR1 boosts the expression of FasL in NK92 cells (Yu et al. 2009). The reverse signaling of tmTNF-α might also contribute to the induction of FasL expression in KCs. Taking these data together we suspect that the pro-apoptotic molecules tmTNF-α and FasL are the leading cause of rapid hepatocyte apoptosis induced by KCs-6h.
In summary, our findings initially demonstrated that KCstmTNFhigh could directly cause liver injury in LPS/D-gal-induced hepatitis, whose mechanisms of action might involve an imbalance in the secretion of pro- and anti-inflammatory cytokines and the induction of hepatocyte apoptosis. KCstmTNFhigh secreted more pro-inflammatory cytokines and less anti-inflammatory cytokine IL-10 and promoted FasL expression, whereas the release of pro- and anti-inflammatory cytokines was inverse, and the expression of FasL was very weak in KCstmTNFlow. The two subsets of KCs seem to have a different phenotype and might play distinct roles in LPS-induced hepatitis; this will form the basis of an attractive and challenging study in the future. Our study provides new insights into the role of KCstmTNFhigh in LPS/D-gal-induced hepatitis.
References
Antoniades CG, Berry PA, Wendon JA, Vergani D (2008) The importance of immune dysfunction in determining outcome in acute liver failure. J Hepatol 49:845–861
Ardestani S, Li B, Deskins DL, Wu H, Massion PP, Young PP (2013) Membrane versus soluble isoforms of TNF-alpha exert opposing effects on tumor growth and survival of tumor-associated myeloid cells. Cancer Res 73:3938–3950
Bilzer M, Roggel F, Gerbes AL (2006) Role of Kupffer cells in host defense and liver disease. Liver Int 26:1175–1186
Cressman DE, Greenbaum LE, DeAngelis RA, Ciliberto G, Furth EE, Poli V, Taub R (1996) Liver failure and defective hepatocyte regeneration in interleukin-6-deficient mice. Science 274:1379–1383
Gantner F, Leist M, Lohse AW, Germann PG, Tiegs G (1995) Concanavalin A-induced T-cell-mediated hepatic injury in mice: the role of tumor necrosis factor. Hepatology 21:190–198
Gonzalez-Teran B, Cortes JR, Manieri E, Matesanz N, Verdugo A, Rodriguez ME, Gonzalez-Rodriguez A, Valverde A, Martin P, Davis RJ, Sabio G (2013) Eukaryotic elongation factor 2 controls TNF-alpha translation in LPS-induced hepatitis. J Clin Invest 123:164–178
Hatano E (2007) Tumor necrosis factor signaling in hepatocyte apoptosis. J Gastroenterol Hepatol 22(Suppl 1):S43–S44
Iimuro Y, Yamamoto M, Kohno H, Itakura J, Fujii H, Matsumoto Y (1994) Blockade of liver macrophages by gadolinium chloride reduces lethality in endotoxemic rats—analysis of mechanisms of lethality in endotoxemia. J Leukoc Biol 55:723–728
Jung K, Kang M, Park C, Hyun Choi Y, Jeon Y, Park SH, Seo SK, Jin D, Choi I (2012) Protective role of V-set and immunoglobulin domain-containing 4 expressed on Kupffer cells during immune-mediated liver injury by inducing tolerance of liver T- and natural killer T-cells. Hepatology 56:1838–1848
Kresse M, Latta M, Kunstle G, Riehle HM, van Rooijen N, Hentze H, Tiegs G, Biburger M, Lucas R, Wendel A (2005) Kupffer cell-expressed membrane-bound TNF mediates melphalan hepatotoxicity via activation of both TNF receptors. J Immunol 175:4076–4083
Kuboki S, Okaya T, Schuster R, Blanchard J, Denenberg A, Wong HR, Lentsch AB (2007) Hepatocyte NF-kappaB activation is hepatoprotective during ischemia-reperfusion injury and is augmented by ischemic hypothermia. Am J Physiol Gastrointest Liver Physiol 292:G201–G207
Kusters S, Tiegs G, Alexopoulou L, Pasparakis M, Douni E, Kunstle G, Bluethmann H, Wendel A, Pfizenmaier K, Kollias G, Grell M (1997) In vivo evidence for a functional role of both tumor necrosis factor (TNF) receptors and transmembrane TNF in experimental hepatitis. Eur J Immunol 27:2870–2875
Lehmann V, Freudenberg MA, Galanos C (1987) Lethal toxicity of lipopolysaccharide and tumor necrosis factor in normal and D-galactosamine-treated mice. J Exp Med 165:657–663
Leist M, Gantner F, Jilg S, Wendel A (1995) Activation of the 55 kDa TNF receptor is necessary and sufficient for TNF-induced liver failure, hepatocyte apoptosis, and nitrite release. J Immunol 154:1307–1316
Louis H, Le Moine O, Goldman M, Deviere J (2003) Modulation of liver injury by interleukin-10. Acta Gastroenterol Belg 66:7–14
Mizuhara H, O’Neill E, Seki N, Ogawa T, Kusunoki C, Otsuka K, Satoh S, Niwa M, Senoh H, Fujiwara H (1994) T cell activation-associated hepatic injury: mediation by tumor necrosis factors and protection by interleukin 6. J Exp Med 179:1529–1537
Mohler KM, Sleath PR, Fitzner JN, Cerretti DP, Alderson M, Kerwar SS, Torrance DS, Otten-Evans C, Greenstreet T, Weerawarna K et al (1994) Protection against a lethal dose of endotoxin by an inhibitor of tumour necrosis factor processing. Nature 370:218–220
Nakashima H, Kinoshita M, Nakashima M, Habu Y, Shono S, Uchida T, Shinomiya N, Seki S (2008) Superoxide produced by Kupffer cells is an essential effector in concanavalin A-induced hepatitis in mice. Hepatology 48:1979–1988
Olleros ML, Vesin D, Fotio AL, Santiago-Raber ML, Tauzin S, Szymkowski DE, Garcia I (2010) Soluble TNF, but not membrane TNF, is critical in LPS-induced hepatitis. J Hepatol 53:1059–1068
Pfeffer K, Matsuyama T, Kundig TM, Wakeham A, Kishihara K, Shahinian A, Wiegmann K, Ohashi PS, Kronke M, Mak TW (1993) Mice deficient for the 55 kD tumor necrosis factor receptor are resistant to endotoxic shock, yet succumb to L. monocytogenes infection. Cell 73:457–467
Pinkoski MJ, Brunner T, Green DR, Lin T (2000) Fas and Fas ligand in gut and liver. Am J Physiol Gastrointest Liver Physiol 278:G354–G366
Roland CR, Walp L, Stack RM, Flye MW (1994) Outcome of Kupffer cell antigen presentation to a cloned murine Th1 lymphocyte depends on the inducibility of nitric oxide synthase by IFN-gamma. J Immunol 153:5453–5464
Rolando N, Wade J, Davalos M, Wendon J, Philpott-Howard J, Williams R (2000) The systemic inflammatory response syndrome in acute liver failure. Hepatology 32:734–739
Rudiger HA, Clavien PA (2002) Tumor necrosis factor alpha, but not Fas, mediates hepatocellular apoptosis in the murine ischemic liver. Gastroenterology 122:202–210
Sun R, Tian Z, Kulkarni S, Gao B (2004) IL-6 prevents T cell-mediated hepatitis via inhibition of NKT cells in CD4+ T cell- and STAT3-dependent manners. J Immunol 172:5648–5655
Ware CF, Crowe PD, Grayson MH, Androlewicz MJ, Browning JL (1992) Expression of surface lymphotoxin and tumor necrosis factor on activated T, B, and natural killer cells. J Immunol 149:3881–3888
Wright HL, Chikura B, Bucknall RC, Moots RJ, Edwards SW (2011) Changes in expression of membrane TNF, NF-{kappa}B activation and neutrophil apoptosis during active and resolved inflammation. Ann Rheum Dis 70:537–543
Yamano T, DeCicco LA, Rikans LE (2000) Attenuation of cadmium-induced liver injury in senescent male Fischer 344 rats: role of Kupffer cells and inflammatory cytokines. Toxicol Appl Pharmacol 162:68–75
Yoshida T, Abe K, Ikeda T, Matsushita T, Wake K, Sato T, Inoue H (2007) Inhibitory effect of glycyrrhizin on lipopolysaccharide and D-galactosamine-induced mouse liver injury. Eur J Pharmacol 576:136–142
You Q, Cheng L, Kedl RM, Ju C (2008) Mechanism of T cell tolerance induction by murine hepatic Kupffer cells. Hepatology 48:978–990
Yu M, Shi W, Zhang J, Niu L, Chen Q, Yan D, Liu T, Jing W, Jiang X, Wei F, Yin B, Zhang W, Li Q, Li Z (2009) Influence of reverse signaling via membrane TNF-alpha on cytotoxicity of NK92 cells. Eur J Cell Biol 88:181–191
Yu M, Zhou X, Niu L, Lin G, Huang J, Zhou W, Gan H, Wang J, Jiang X, Yin B, Li Z (2013) Targeting transmembrane TNF-alpha suppresses breast cancer growth. Cancer Res 73:4061–4074
Zhang M, Xu S, Han Y, Cao X (2011) Apoptotic cells attenuate fulminant hepatitis by priming Kupffer cells to produce interleukin-10 through membrane-bound TGF-beta. Hepatology 53:306–316
Author information
Authors and Affiliations
Corresponding author
Additional information
Peng Yang and Wenjing Zhou contributed equally to this work.
This work was supported by grants from the National Natural Science Foundation of China (81272520), National Program on Key Basic Research Project (973 Program, 2013CB530505), and Major Research Plan of the National Natural Science Foundation of China (91029709).
The authors declare that they do not have any conflicting financial interests.
Rights and permissions
About this article
Cite this article
Yang, P., Zhou, W., Li, C. et al. Kupffer-cell-expressed transmembrane TNF-α is a major contributor to lipopolysaccharide and D-galactosamine-induced liver injury. Cell Tissue Res 363, 371–383 (2016). https://doi.org/10.1007/s00441-015-2252-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-015-2252-2