Abstract
For decades, cancer was associated with gap-junction defects. However, more recently it appeared that the gap junction proteins (connexins) could be re-expressed and participate to cancer cell dissemination during the late stages of tumor progression. Since primary tumors of prostate cancer (PCa) are known to be connexin deficient, it was interesting to verify whether their bone-targeted metastatic behaviour could be influenced by the re-expression of the connexin type (connexin43) which is originally present in prostate tissue and highly expressed in bone where it participates to the differentiation of osteoblastic cells. Thus, we investigated the effect of the increased Cx43 expression, by retroviral infection, on the metastatic behaviour of two well-characterized cell lines (PC-3 and LNCaP) representing different stages of PCa progression. It appeared that Cx43 differently behaved in those cell lines and induced different phenotypes. In LNCaP, Cx43 was functional, localized at the plasma membrane and its high expression was correlated with a more aggressive phenotype both in vitro and in vivo. In particular, those Cx43-expressing LNCaP cells exhibited a high incidence of osteolytic metastases generated by bone xenografts in mice. Interestingly, LNCaP cells were also able to decrease the proliferation of cocultured osteoblastic cells. In contrast, the increased expression of Cx43 in PC-3 cells led to an unfunctional, cytoplasmic localization of the protein and was correlated with a reduction of proliferation, adhesion and invasion of the cells. In conclusion, the localization and the functionality of Cx43 may govern the ability of PCa cells to metastasize in bones.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Metastasis remains the main cause of morbidity and death (90%) from solid tumors. It is thus important to elucidate the molecular mechanisms which are responsible for tumor cell mobility, homing and colonization of specific organ sites [1]. However, despite the fact that cell interactions are involved in those processes, only a few studies have examined what could be the role of proteins implicated in direct cellular interactions [2, 3]. Among possible candidates, gap junction proteins, named connexins (Cxs), are thought to enable cancer cells to adapt to different extracellular environments [4, 5]. Members of a multigene family, Cxs are involved in gap junctional intercellular communication (GJIC) and coordinate cell activities during development and differentiation [6]. Moreover, recent data demonstrated alternative functions for Cxs as hemichannels [7] or inducer of protein interactions [8]. Since loss of tissue homeostasis frequently accompanies tumor growth, gap junctions were suggested to be involved in carcinogenesis [9]. Such an assumption has been then confirmed by numerous data showing that cancer phenotype is indeed associated with a decreased capacity of GJIC in cancer cells both in vitro and in vivo [10–12]. In the context of primary solid tumor, Cxs (particularly Cx43) presented anti-proliferative effects in a wide range of cancer cell types and were frequently classified as tumor suppressor genes [13–15]. However, recent evidences suggest that the role of Cxs is more complex in cancer since they could be involved differently at different stages of tumor progression. For instance, Cx43 would play an active role in migration of cancer cells [16] by increasing their adhesion to the stroma. Moreover, they could also participate in breast cancer cell spreading by establishing heterocellular communication with vascular endothelial cells. This would increase the diapedesis needed for cancer cells to metastasize [17, 18]. Finally, as demonstrated for a human breast carcinoma cell line metastasizing to bones, it appears that heterocellular GJIC can occur with human osteoblastic (OB) cells [19]. Interestingly, transcriptome analyses of osteotropic breast cancer cells have revealed that Cx43 was up-regulated in metastatic cells that are believed to acquire bone cell-like properties (osteomimicry). This increased Cx43 expression was confirmed by immunohistochemistry in bone metastatic lesions from patients [20]. Then, Cxs could play multiple roles depending on the stage of carcinogenesis [4, 5]. However, contrary to their involvement in cell growth control, only few studies investigated so far the function of Cxs during the last steps of tumor progression.
Prostate cancer (PCa) is the most commonly diagnosed cancer in males and 80% of patients with advanced disease have bone metastasis mainly characterized by osteoblastic lesions [21, 22]. As seen in the majority of cancers, alterations in cellular interactions were demonstrated in PCa cells [2, 3]. In normal differentiated epithelial prostatic cells, Cx32 and Cx43 are the main Cxs expressed [23]. These Cxs were also localized at cell–cell contacts in epithelial cells of well differentiated prostate tumors, but presented either an alteration of expression or an impaired trafficking as the tumors progressed to more invasive and undifferentiated stages [23, 24]. In PCa cells, Cx43 was also involved in sensitivity to pro-apoptotic agents [25] and heterocellular coupling with fibroblasts controlling migration ability during invasion [26]. In bones, an essential role was also attributed to Cx43, while its expression was directly related to the differentiation state of osteogenic cells [27] and to the mineralization process [28]. Altogether, these data suggest that Cx43 may have a role in heterotypic interactions between PCa and OB cells during bone metastasis formation and/or progression.
In this study, after retroviral infection, we characterized Cx43-induced phenotypic changes in two PCa cell lines with different invasive characteristics (LNCaP and PC-3) and compared their bone impact in vivo after intratibial injection in Nude mice and in vitro after cocultures with OB cells. We found that Cx43 localization and function differ in those cell lines since GJIC is reestablished only in Cx43-expressing LNCaP cells. Interestingly, these communicating LNCaP cells exhibit increased aggressive characteristics whereas the more aggressive cells, PC-3, present a reduction of their tumor phenotype after Cx43 overexpression (proliferation, adhesion and invasion). In the bone xenograft model, Cx43 overexpression in LNCaP cells also induces a significant rise in the incidence of osteolytic metastasis that is associated with a PCa-induced reduction of OB cells number in coculture.
Materials and methods
Cell lines and stable transfection
LNCaP and PC-3 cell lines were purchased from ATCC (CRL-1435 and CRL-1740, Manassas, VA) and were grown in DMEM (Invitrogen, Cergy Pontoise, France) with high glucose 4.5 g/l supplemented with 10% Fetal Bovine Serum (FBS) (Lonza, Levallois-Perret, France), 100 IU/ml penicillin and 100 μg/ml streptomycin (Lonza). PCa cells overexpressing Cx43 (PC-3 Cx43 or LNCaP Cx43) were prepared as previously described [29] by means of retroviral particles containing human Cx43. Control cells were obtained using an empty pMSCV-puro vector (PC-3 mock or LNCaP mock). The stable Cx43 overexpression in the total cell population was checked over 10 passages at RNA and protein levels.
Coculture with osteoblastic (OB) cells
OB cells were isolated from calvaria of 3–5 days-old mice after sequential digestions as previously described [30]. After 6 days of primary culture in DMEM with 20% FBS, OB cells were trypsinized in a 0.05% trypsin/0.15% EDTA solution, seeded at 25 × 103 cells/ml in a differentiating medium (DMEM supplemented with 10% FBS and 10 mM sodium β-glycerophosphate) and cultured at 37°C. All reagents were from Sigma (St. Louis, MO).
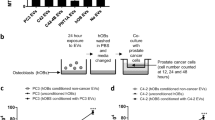
To study the impact of PCa cells (mock and Cx43) on OB cells proliferation and differentiation, cocultures with or without contact were carried out and compared to OB cells cultured alone. The initial ratio was 1:10 in favor of OB cells in both coculture conditions, but in the bilayer configuration (no contact), OB cells were separated from PCa cells with a cell culture insert (PET, 0.4 μm pore size, BD Biosciences, Pont-de-Claix, France), as illustrated in Fig. 4b.
Real-time quantitative RT-PCR
RNA extraction, reverse transcription and RT-qPCR were performed as previously detailed [31]. The primers are described in supplemental Data, Table 1. Results are displayed in the relative expression (percentage) compared to GAPDH expression and normalized relative to control cells. Primer validation and species specificity were checked using cDNA from human or mouse OB primary culture (data not shown).
Immunoblotting
As previously described [30], 50 μg of proteins were separated on 12% polyacrylamide-SDS gel and electroblotted on nitrocellulose membrane. Blots were probed overnight at 4°C with monoclonal antibody against Cx43 (1/1,000; Transduction Laboratories, Lexington, KY). Then, membranes were incubated with goat anti-mouse HRP-conjugated antibody (1/5,000) for 1 h at room temperature (Dako, Glostrup, Denmark). Bound antibodies were detected using an enhanced-ECL kit as specified by the manufacturer (ThermoScientific, Rockford, IL).
Immunocytochemistry
To detect Cx43, procedure was modified from Geneau et al. [30] using cold acetone fixation (10 min) and propidium iodide for nuclear counterstaining. Samples were observed on a confocal microscope (FV1000 Olympus IX-81, Tokyo, Japan). All controls performed by omitting the primary antibody were negative.
Proliferation and apoptotic assays
Proliferation assay was performed according to Geneau et al. [30]. One OD unit corresponds to 5 × 104, 3.3 × 104 and 2.8 × 104 cells for OB, PC-3 and LNCaP respectively. Results on PCa cells were also confirmed by XTT proliferation kit (Roche Diagnostics, Mannheim, Germany). Assessment of Cx43 impact on apoptosis was performed by means of the FITC-annexinV apoptosis detection kit according to recommendations of the manufacturer (BD Biosciences). After incubation with propidium iodide and FITC-conjugated annexinV, samples were analyzed on a FACSCanto-II flow cytometer using the FACSDiva-II software (BD Biosciences).
Adhesion and invasion assay
For adhesion assay, 3×103 PCa cells were seeded on vitronectin or fibronectin-coated (0.5 μg/ml) wells in 16-wells Lab-tek® chamber slide system (Nunc, Rochester, NY). Cells were allowed to attach for 2 h in DMEM with 10% FBS and processed as reported in [32]. Cell invasion through 25 μg Matrigel® (BD Biosciences) was assessed using Boyden chambers with 8 μm pores (PET, BD Biosciences). After 24 h incubation, cells on the upper surface were removed and cells attached to the lower surface were fixed, stained with eosin/haematoxylin. To ascertain the implication of Cx43 in invasive properties, control experiments were performed in the presence of 10 μM GM6001 (functional inhibitor of MMP1, 2, 3, 8 and 9; EMD chemicals, Giggstown, NJ). For both techniques, cell number was measured by means of ImageJ software.
Gap junction functionality
For qualitative GJIC evaluation, donor cells were labeled with a diffusible fluorescent dye (5 μM calcein/AM, Sigma) together with a non-diffusible membrane marker (10 μM DiL-C18(3), Invitrogen) as previously detailed [33]. After washing, cells were trypsinized, resuspended in culture medium and 103 fluorescent cells were laid on recipient cells. The transfer of dye was visualized after 4 h at 37°C on the Olympus confocal system.
The degree of homocellular GJIC between PCa cells was also measured by means of the gap-FRAP (Fluorescence recovery after photobleaching) method [34]. Briefly, cultured PCa cells were loaded with a diffusible fluorescent tracer (7 μg/ml 6-carboxyfluorescein, Sigma) and the fluorescence of investigated cells was dramatically decreased by a laser beam (photobleaching at 405 nm) in order to study the recovery by diffusion from adjacent cells and to measure the diffusion rate constant k.
Secretome analysis
Proteins (1 mg) from the serum-free medium of PCa cells were digested overnight with trypsin (1 μg/50 μg protein; Promega, Madison, WI). After purification through C18 columns, resulting peptides were isotopically labeled by peptide-level dimethylation induced by formaldehyde treatment [35]. In order to compare quantitatively the peptides according to their cell origin (mock and Cx43), two isotopologs of formaldehyde (200 mM) were used (15 μl/sample); a light one (CH2O) to label the peptides from Cx43-PCa cells and a heavy deuterated one (CD2O) to label the peptides from mock cells [35]. Labeled peptides were analyzed as described [35] on a linear trapping quadrupole-Orbitrap mass spectrometer with Xcalibur software (ThermoFisher). Fragments spectra were identified using Mascot (v.2.2, Matrix Science) and quantitative ratios were extracted using MSQuant (http://msquant.sourceforge.net/). For each type of secreted protein, results are presented as ratios of Cx43-transfected versus mock cells.
ALP activity
Intracellular alkaline phosphatase activity was measured by colorimetry as described [36] and normalized against total cellular protein content determined by DC Protein Assay (BioRad, Marnes-la-Coquette, France).
Xenograft model and bone impact analyses
All these procedures were conducted in accordance with the guidelines of the European Union (CEE 86-609) and verified by the local Animal Care Committee. PCa cells (6 × 105 in 5 μl PBS) were injected into the right tibia of male Balb/c Nude mice (7 weeks old; Charles River Laboratories, Wilmington, MA) under anesthesia (100 mg/kg ketamine and 10 mg/kg xylazine, Sigma). The left tibia received a control injection with PBS. After 20–40 days, anesthetized mice were imaged by means of micro X-ray computed tomography (μCT) with a CT 120 (GE Healthcare, France). 360 X-ray projections were collected in 1° increments (80 kVp; 450 μA; 120 ms exposure time for 26 min total scan time). Projection images were reconstructed into 3D volumes (10,243 voxels, 93 μm resolution) on a 4PCreconstruction cluster using a modified tent-FDK conebeamalgorithm (GE Healthcare reconstruction software). Three-dimensional data were processed and rendered (isosurface/maximum intensity projections) using MicroView (GE Healthcare). The procedure for bone volume measurement after tibia injection is detailed in supplemental Data, Fig. 2.
Osteogenic sites were analyzed by Single Photon Emission Computed Tomography (SPECT). [99mTc]-MDP (Methylene Di Phosphonate) is a conventional bone scintigraphic agent that selectively concentrates in bone thanks to its chemical adsorption onto, and into, the crystalline structure of hydroxyapatite. After 3–6 weeks, mice were injected in the tail vein with [99mTc]-MDP with 18 MBq. Images were recorded 60 min after injection of [99mTc]-MDP. Mice were anesthetized with 1.5–2% isoflurane in air and transferred to a Nano SPECT/CT (Bioscan, Washington, DC). Image acquisition parameters were 24 projections and 30–60 s/image depending upon activity injected in the animals. Dedicated software (InVivoScope) was used to reconstruct 3D images and to quantify radioactivity. Image analysis was qualitative (comparison with μCT), and quantitative by drawing volumes of interest around tumors in both legs, with results expressed as percentage of injected doses.
Statistical analysis
All reported data are expressed as mean ± SEM. One-way analysis of variance followed by Tukey’s test was performed for RT-qPCR, whereas Student’s t-test for unpaired data was used in other cases. *P < 0.05; **P < 0.01; ***P < 0.001.
Results
Cx43 leads to functional communication only in LNCaP cells
Cx43 overexpression in PC-3 (PC-3 Cx43) and LNCaP (LNCaP Cx43) cells was confirmed by RT-qPCR and western blotting (Fig. 1a, b). Native and mock PC-3 and LNCaP cells presented low level of Cx43 expression (mRNA and protein level; Fig. 1a, b; not shown for native cells) and no functional GJIC (Fig. 1d). Western blot analyses revealed that retroviral infection induced a stable physiological increase of Cx43 by 3.09 ± 0.34 and 3.35 ± 0.57 fold over the endogenous expression in the total population of PC-3 and LNCaP cells, respectively (Fig. 1b). No compensation or alteration of expression was demonstrated for other Cxs previously described in PCa cells including Cx26, Cx32, Cx45 (Supplemental Data, Fig. 1a). In terms of localization, LNCaP Cx43 cells exhibited a characteristic punctuate immunostaining at appositional membranes and inside cells whereas Cx43 immunofluorescence was restricted to the cytoplasmic compartment in PC-3 Cx43 cells (Fig. 1c). This differential localization of Cx43 leads to functional divergences as confirmed by preloading and gap-FRAP experiments showing GJIC only between LNCaP Cx43 cells (Fig. 1d and supplemental Data, Fig. 1b). All data obtained for LNCaP Cx43 correspond to a functional GJIC quantitatively similar to intercellular coupling of other epithelial or normal cells in terms of permeability (diffusion rate constant k = 0.225 ± 0.04 min−1) and of percentage of coupled cells [30, 34].
Cx43 presents different patterns of localization and function in PCa cells. Stable retroviral Cx43 expression in PC-3 and LNCaP cells was confirmed by RT-qPCR (a) and immunoblotting normalized to GAPDH (b). c Cx43 immunolocalization (green) and counterstaining of nuclei by Propidium Iodide (PI, red) demonstrated a cytoplasmic localization for PC-3 Cx43 cells and a characteristic punctuate immunostaining at cell–cell boundaries for LNCaP Cx43 cells. Enlarged images marked by the white boxes (Box) are shown on the right. d Functional homocellular coupling between PCa cells evaluated by gap-FRAP method. Top: Digital images of fluorescence distribution in LNCaP Cx43 cells at different times: Prebleach, just after photobleach (T = 0 min), and after fluorescence redistribution (T = 5 min). Polygon1 represents the photobleached tested cell; Polygon2 is an unbleached control cell for fluorescence correction. Representative example of fluorescence recovery curves were expressed as the percentage of prebleach value vs. time in LNCaP mock (white circles), LNCaP Cx43 (black circles) and control unbleached cell (black squares). Bottom: Percentage of coupled cells with corresponding diffusion rate constants k determined from recovery curves for LNCaP Cx43 (n > 20). White and black bars correspond to mock and Cx43-transfected cells respectively. *P < 0.05, **P < 0.01, ***P < 0.001. (c–d Scale bars = 100 μm; for Box, scale bars = 20 μm)
Cx43 induces contrasting phenotypic changes in LNCaP and PC-3 cells
The contribution of Cx43 expression level on tumoral characteristics of PCa cells was analyzed in vitro after overexpression in both cell lines. Cx43 decreases the proliferation rate of PC-3 cells by half after 4 days of culture. In contrast, no significant effects could be demonstrated during a 1–6 days period for LNCaP cells (Fig. 2a). This effect on cell number was not associated with increased apoptosis since the viability of PCa cells was not affected by retroviral infection in Cx43 and mock cells (Fig. 2b and supplemental Data, Fig. 1c). The aggressive phenotype of PCa cells was evaluated by means of adhesion to different matrix components and by invasion ability in Boyden chambers (Fig. 2c, d). As expected, PC-3 presented a more pronounced adhesive and invasive properties than LNCaP cells in our conditions. Interestingly, PC-3 Cx43 cells presented a significant reduction of adhesion on vitronectin (−35%) and fibronectin (−31%) as well as of the invasion ability (−44%). On the contrary, the aggressiveness of LNCaP cells was clearly increased after Cx43 overexpression. Indeed, LNCaP Cx43 displayed an increased adhesion on vitronectin and fibronectin compared to mock cells and were more invasive through Matrigel® (+70% compared to mock cells). In our experimental conditions, the significant effects on invasive ability were not linked to migration properties because of their abolition in the presence of GM6001, a functional blocker of MMPs (supplemental Data, Fig. 1d). To complete the characterization of PCa Cx43 cells, comparative proteomic approach was made for identifying secreted molecules implicated in invasion or metastatic processes (Fig. 2e, f). The layout of secreted molecules by functional groups (Supplemental Data, Table 2) showed that molecules implicated in collagen degradation (MMP13, PLAT and TIMP2) exhibited variations in LNCaP Cx43 cells towards an invasive phenotype. Furthermore, in LNCaP Cx43 cells (Fig. 2f), a high proportion of factors that were already described in prostate cancer progression or bone metastasis (PTX3, DAG-1, BMP3 and LGALS1) presented the same hostile profile. Finally, consistently with cell viability assays, PC-3 Cx43 cells presented an increased expression of antimitotic factors like NOV (Fig. 2e). Altogether, in vitro data indicate that aggressive properties of PC-3 cells are reduced by Cx43 overexpression whereas they are augmented in LNCaP cells.
Cx43 leads to different and opposite phenotypic changes in PC-3 and LNCaP cells. a Proliferation rate was assessed by means of methylene blue staining in PC-3 and LNCaP cells. Data represent means ± SEM of 3 independent experiments performed in triplicate. Proliferation status of mock (white circles) and Cx43-transfected (black circles) were compared until 6 days. b Mean values of apoptotic cells for each cell type after 4 days of culture. Bars represent percentages of annexinV-positive cells from three independent experiments. c Adhesion assay on fibronectin and vitronectin for PC-3 (left) and LNCaP (right) transfected or not with Cx43. Controls were performed with PBS. d Invasion assay on Matrigel®. For adhesion and invasion assays data are presented as mean ± SEM of 4 different experiments performed in triplicate. e–f Secretome analysis for PC-3 and LNCaP cells respectively. Top: Identified proteins were gathered into 3 categories (stimulated, inhibited or unmodified by Cx43 expression). Bottom: Comparative abundance of secreted proteins detected in culture media of PC-3 (e) and LNCaP (f) cells and presented according to the value of their ratio of Cx43:Mock for secreted proteins present in 3 independent experiments. Arrows underline the main secreted factors already implicated in prostate cancer progression and bone metastasis. White and black bars correspond to mock and Cx43-transfected cells respectively. *P < 0.05, **P < 0.01, ***P < 0.001
Cx43 increases the aggressiveness of LNCaP in the bone context
To evaluate the influence of Cx43 on the bone lesions due to PCa cells, we generated intra-osseous xenografts of PCa cells and followed in parallel the bone integrity and remodeling by micro computed tomography (μCT) and scintigraphy (SPECT-CT), respectively. After intratibial injection of 6 × 105 cells, tumor incidence for LNCaP Cx43 cells was greatly increased compared to mock cells (85 vs 22%) while PC-3 cells induced tumor growth in bone context whatever the genotype (Fig. 3a). However, no difference in tumor size was measured between the PCa cell types (1 cm diameter before euthanasia). When a tumor developed, tomographic analysis demonstrated osteolysis in all cases after 20 days (arrow heads in Fig. 3b) requiring euthanasia as early as day 31 and day 40 for PC-3 and LNCaP cells respectively. Quantitative μCT analysis allowed measuring the tibia bone volume (Supplemental Data, Fig. 2b). No significant difference was measured between PC-3 Cx43 and mock cells, but enhanced osteolysis was demonstrated for LNCaP Cx43 compared to mock cells (Fig. 3c). For the osteogenic aspect, no Cx43 effects on the number of mineralization sites were revealed by means of SPECT-CT analyses (Fig. 3b, d). Thus, in vivo data confirm that enhanced Cx43 expression and function in LNCaP cells induced an increased metastatic ability leading to osteolytic lesions.
Effects of Cx43 expression on bone impact in vivo. a Tumor incidence of PCa Cx43 cells compared to PCa mock cells after intratibial injection in Nude mice. b Representative experiments of μCT and SPECT-CT at days 20 and 31 for PC-3 cells and days 20 and 40 for LNCaP cells. Note the absence of tibia osteolysis with LNCaP mock cells compared to large bone destruction with LNCaP Cx43 cells. Arrow heads represent osteolytic lesions in right tibiae. c Bone volume of tibia injected with PCa cells compared to control with PBS following the procedure detailed in supporting information Fig. 2. Cx43 overexpression in LNCaP increased the development of osteolytic tumor. d Analysis of osteogenic sites corresponding to percentage of [99mTc]-MDP activity in tibia injected with PCa cells compared to control. 3 mice were examined for PC-3 cells, 9 for LNCaP mock and 13 for LNCaP Cx43. White and black bars correspond to mock and Cx43-transfected cells respectively. **P < 0.01
Cx43 could modify the PCa cell impact on OB proliferation in vitro
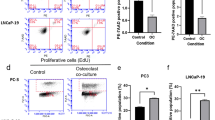
Osteoblasts, the key cells of bone remodeling, also present functional GJIC due to Cx43 expression [30]. Therefore, the specific OB/PCa cell interaction was investigated in vitro both in direct contact and in bilayer configuration. Preloading assay demonstrated functional GJIC only between LNCaP Cx43 and OB cells (Fig. 4a). Cocultures with two different configurations (Fig. 4b) were employed at a ratio of 1:10 for PCa and OB cells, respectively. In the contact configuration, PCa cells presented a clonal expansion (Fig. 4b) leading to restricted areas of heterocellular contact with OB cells. In these conditions, an evolution of the PCa:OB cell ratio was determined only for PC-3 mock cells (twofold increase) leading to appropriate correction during proliferation assays. In the bilayer configuration, only communication by soluble factors can occur.
Cx43 expression affects osteoblastic proliferation in coculture conditions. a Demonstration of heterocellular coupling between OB cells and PCa-Cx43 cells by preloading assay. Only LNCaP Cx43 established GJIC with OB cells as shown by calcein diffusion (green) from donor cells tagged by DiL-C18(3) (red). b Left: Configuration of cocultures in contact and in a bilayer condition (no contact). Right: Phase-contrast photomicrograph of LNCaP Cx43 cells in contact with OB cells after 4 days of coculture. Arrows point the islets of LNCaP Cx43 cells. c OB cell number after 4 days of coculture with PC-3 (top) or LNCaP (bottom). Gray bars represent OB cells cultured alone while white and black bars correspond to OB cells cocultured with mock and Cx43-transfected PCa cells respectively. *P < 0.05, **P < 0.01. (a–b, Scale bars = 50 μm)
In the contact configuration, Cx43 in PC-3 cells produced a slight increase of the OB cell number, whereas in the bilayer configuration it was ineffective (Fig. 4c, top). On the contrary, LNCaP Cx43 exhibited a positive effect on OB cell number compared to mock cells in the bilayer configuration (Fig. 4c, bottom). Importantly, these effects were reversed in the contact configuration and especially, a significant decrease of the proliferation rate was demonstrated when OB cells could interact with communicating LNCaP Cx43 (Fig. 4c, bottom). These data were consistent with a reduction of the bone–forming cell number when Cx43 was overexpressed in LNCaP cells.
PCa cells in direct contact with OB cells increase their osteoclastic potential
To examine the effect of the prostatic Cx43 level on the OB differentiation potential, we analyzed the osteogenic capacity of individual OB cells cocultured with PCa cells. Commonly used differentiation markers like Cbfa-1, osteocalcin (OCN), Cx43 and osteopontin (OPN) were drastically decreased whatever the configuration and the level of Cx43 expression in prostatic cells, as demonstrated by RT-qPCR (Fig. 5 and supplemental Data, Fig. 3). Only ALP expression and activity presented an increased profile in the contact configuration. As bone resorption and osteoclastic differentiation are tightly orchestrated via the RANK/receptor activator of NF-kappaB ligand (RANKL)/osteoprotegerin (OPG) system, we investigated these osteoblastic criteria in presence of PCa cells. Significant variations were demonstrated only in contact configuration with increased RANKL (Fig. 5). We also demonstrated decreased OPG expression in presence of PCa cells whatever the configuration and the cell line (Supplemental Data, Fig. 3). The absence of significant differences between mock and transfected cells suggest a contact effect implicating adhesion molecules without a direct involvement of Cx43.
Effects of PCa cells on OB cell differentiation in vitro in the contact and bilayer configurations. Impact of PCa cells on OB cell differentiation status was evaluated by ALP activity after 2 days and by RT-qPCR on Cbfa1, OCN and RANKL after 4 days of coculture. Each bar represents mean ± SEM of 3 different experiments performed in triplicate. Gray bars represent OB cells cultured alone while white and black bars correspond to cocultures with mock and Cx43-transfected PCa cells respectively. For RT-qPCR, data correspond to the relative expression compared to GAPDH before normalization with OB cells alone. *P < 0.05, **P < 0.01, ***P < 0.001
In summary, cocultures demonstrated that the presence of PCa cells induce a drastic inhibition of the osteogenic status of OB cells together with an increase of their osteolytic ability due to soluble factors and/or physical contact. In this heterocellular context, Cx43 overexpression only generates an alteration of the proliferation rate of OB cells. However, contrary to the in vivo situation with bone marrow, the in vitro approach focuses on the unique dialogue between mesenchymal and prostatic cells.
Discussion
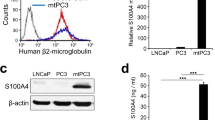
Given the central role of Cx43 in bone physiology and its altered expression in PCa primary tumors, we investigated the role of this Cx in bone-targeted metastasis of PCa cells. To do so, Cx43 expression was increased in two PCa cell lines representing different stages of cancer progression (PC-3 and LNCaP cells). Firstly, cellular characterization revealed a differential distribution and functionality of Cx43 in the two cell lines despite a similar increased level of expression. Consistently with previous studies [24, 25], Cx43 expression was restricted to cytoplasmic compartments in PC-3 Cx43 cells whereas it was localized at the plasma membrane in LNCaP Cx43 cells leading to the restoration of GJIC. In vitro analyses demonstrated significant differences between the cell lines in term of adhesion, invasion, proliferation and secretome profile. As described in other cellular models, data on PC-3 cells illustrate the suppressive role of Cx43 on cell growth and invasion [37–40] whereas no modification of the proliferation rate was measured in LNCaP cells. Controversially, previous studies using retroviral infection with rat Cx43 cDNA [13, 24] have shown an inhibition of growth and colonies formation with LNCaP cells. However, it should be noted that some experimental conditions differ from the present study especially the use of individual selected clones instead of total population of transfected cells. If this latter aspect fit better to the heterogeneous situation of the tumor, it could minimize the measured modification of cellular proliferation. Interestingly, for LNCaP cells, our data further demonstrated that Cx43 enhances cell aggressiveness as invasion and adhesion. These unexpected observations were supported by secretome analyses that suggest increased capabilities for collagen degradation and cell invasion (MMP13 and reduced TIMP-2) and for bone metastasis (β2-microglobulin, BMP3 and galectin-1). Moreover, contrary to the PC-3 situation, no significant Cx43 effects on LNCaP growth were demonstrated after 6 days of culture. These later results were in accordance with previous data obtained in similar conditions [25]. In normal and tumor cells a link between Cx43 expression and apoptotic status was demonstrated [41, 42]. However, in both PCa cell types tested, spontaneous apoptosis evaluated by annexinV/IP labeling was not affected by Cx43 as previously described [25]. Thus, in our cell models like in other cancer types, aberrant localizations of Cxs in addition to reduced expression in PCa cells could be responsible for their aggressive characteristics as previously demonstrated for androgen-independence [24].
Bone is the predominant site of distant metastasis for prostate tumor. Consequently the in vivo effects of Cx43 overexpression were evaluated on PCa cell-induced bone metastasis after intratibial injection. For the first time, the present data reveal an increased incidence of tumors for LNCaP Cx43 compared to mock cells, whereas no significant impact due to Cx was demonstrated in PC-3 cells. This in vivo assay confirmed the enhanced aggressiveness exhibited in vitro for LNCaP cells. Once PCa cells have metastasized to bone marrow, tumor cells are suspected to interact with OB cells, osteoclastic cells and stromal cells through both soluble factors and direct physical contact [43]. To further investigate the influence of Cx43 in this heterocellular interaction, we cocultured PCa cells with the key cells of bone remodeling (OB cells) in contact and bilayer configuration. Our data demonstrated an exclusive action of Cx43 on osteoblastic proliferation. However, in the present study, the presence of PCa cells in the microenvironment of OB cells always induced a drastic decrease of the differentiation ability as demonstrated for conventional OB markers. The fact that this inhibitory effect was observed either in contact or in bilayer configuration for both cell lines argues for an action of soluble factors independently from GJIC. Indeed, PCa cells can alter bone homeostasis by secreting factors that directly affect osteoblast functions like BMP3 and Galectin-1 [21, 44]. Interestingly, galectin-1, increased in secretome of LNCaP Cx43 cells, was previously implicated in the differentiation of human stromal cells [45] with effects similar to our in vitro data (stimulated ALP activity and inhibited OCN production).
Although PCa cells mainly induce osteoblastic lesions, bone resorption is known to be a key step for bone metastasis [46] and long term inhibition of osteolytic lesions may prevent skeletal complications in patients with metastatic PCa [47]. Therefore, we analyzed the expression level of OB cytokines implicated in the regulation of osteoclastic activity. Our in vitro results established that the presence of PCa cells induced a significant increase of the RANKL/OPG balance only in coculture with contact configuration of OB cells. These results suggest that Cx43 could be an important partner of the interacting complex between arrested cancer cells and cells of the microenvironment in which adhesion probably occurs before the establishment of functional gap junction channels. Moreover, robust links between cadherins and Cx expression were demonstrated during cancer progression [48, 49]. Among the cadherin family, cadherin-11 was recently implicated in the osteolytic potential of PCa cells [2]. The enhancement of osteoclastic activity by physical contact of PCa with OB cells was also described in a coculture model and was blocked by N-cadherin and cadherin-11 neutralization [43].
The link between connexin expression level and metastatic behaviour was suggested by in vitro studies in which Cx43 level and heterocellular GJIC between tumor cells and environmental cells may control tumor cell motility, homing and diapedesis. Indeed, in the rat Dunning model, migration capacities of a highly metastatic cell line (MAT-LyLu) was greater than those of cells with low metastatic potential (AT-2) and correlated with high Cx43 expression. Interestingly, this motility was increased when PCa cells were cocultured on a fibroblast-coated surface but independently from GJIC [26]. Moreover, the induction of Cx43 in a GJIC-deficient mammary tumor cell line was able to double the diapedesis efficiency [18]. In the breast cancer context, Cx43 was also demonstrated to facilitate the tumor cell attachment to lung endothelial cells and to take part in the metastatic homing [50]. The metastatic potential of breast cancer cells was also correlated to increased heterocellular GJIC between cancer and OB cells [19]. However, it should be mentioned that during breast cancer progression to the lung, a protective effect of Cx43 was demonstrated [51, 52]. These data and the present study suggest that during the multistage scheme of metastasis, Cx43 could be implicated at different points including crosstalk initiated at secondary sites in the bone. Finally, other connexins like Cx26 have been also associated with the progression of prostate cancer [53]. The increased Cx26 expression measured during the PCa progression was related to a role in adhesion regulation through its interaction with focal adhesion kinase. As shown in the present study for Cx43, Tate et al. also demonstrated that Cx26 and GJIC could have a role on PCa cell invasive behavior.
Conclusion
The effects of Cx43 on PCa cell characteristics depend on its localization and function. In LNCaP cells, these modifications lead to an increased incidence of bone metastasis in vivo and a decreased proliferation of bone-forming cells in vitro. To our knowledge, the present study is the first demonstration of the increased metastatic potential of PCa cells due to Cx43. From these results, it would be interesting to check whether the metastatic cells generally communicate with cells of their target organs and if these direct interactions do play a role in the dormancy of metastasis. In other words, it would be interesting to understand if the level of heterotypic GJIC with normal host cells would play a role in the growth control of metastasized cells. Moreover, additional investigations on heterocellular interactions between osteoclastic and PCa cells are required to further identify the role of Cx43 in the severity of osteolytic bone metastasis.
Abbreviations
- μCT:
-
Micro-Computed Tomography
- ALP:
-
Alkaline phosphatase
- BMP3:
-
Bone morphogenic protein-3
- Cx43:
-
Connexin43
- DAG1:
-
Dystroglycan-1
- Gap-FRAP:
-
Gap-fluorescence recovery after photobleaching
- GJIC:
-
Gap junctional intercellular communication
- LGALS1:
-
Galectin-1
- MDP:
-
Methylene diphosphonate
- MMP13:
-
Matrix metalloproteinase-13
- NOV/CCN3:
-
Nephroblastoma overexpressed gene/connective tissue growth factor3
- OB:
-
Osteoblastic
- OCN:
-
Osteocalcin
- OPG:
-
Osteoprotegerin
- OPN:
-
Osteopontin
- PCa:
-
Prostate cancer
- PLAT:
-
Plasminogen activator tissue-type
- PTX-3:
-
Pentraxin-related protein-3
- RANKL:
-
Receptor activator of nuclear factor-kappaB ligand
- TIMP2:
-
MetalloProteinase inhibitor-2
References
Gupta GP, Massague J (2006) Cancer metastasis: building a framework. Cell 127(4):679–695
Huang CF, Lira C, Chu K, Bilen MA, Lee YC, Ye X, Kim SM, Ortiz A, Wu FL, Logothetis CJ, Yu-Lee LY, Lin SH (2010) Cadherin-11 increases migration and invasion of prostate cancer cells and enhances their interaction with osteoblasts. Cancer Res 70(11):4580–4589
Ito A, Koma Y, Uchino K, Okada T, Ohbayashi C, Tsubota N, Okada M (2006) Increased expression of connexin 26 in the invasive component of lung squamous cell carcinoma: significant correlation with poor prognosis. Cancer Lett 234(2):239–248
Cronier L, Crespin S, Strale PO, Defamie N, Mesnil M (2009) Gap junctions and cancer: new functions for an old story. Antioxid Redox Signal 11(2):323–338
Naus CC, Laird DW (2010) Implications and challenges of connexin connections to cancer. Nat Rev Cancer 10(6):435–441
Kumar NM, Gilula NB (1996) The gap junction communication channel. Cell 84(3):381–388
Evans WH, De Vuyst E, Leybaert L (2006) The gap junction cellular internet: connexin hemichannels enter the signalling limelight. Biochem J 397(1):1–14
Herve JC, Bourmeyster N, Sarrouilhe D (2004) Diversity in protein–protein interactions of connexins: emerging roles. Biochim Biophys Acta 1662(1–2):22–41
Loewenstein WR (1979) Junctional intercellular communication and the control of growth. Biochim Biophys Acta 560(1):1–65
Mesnil M, Crespin S, Avanzo JL, Zaidan-Dagli ML (2005) Defective gap junctional intercellular communication in the carcinogenic process. Biochim Biophys Acta 1719(1–2):125–145
Avanzo JL, Mesnil M, Hernandez-Blazquez FJ, Mackowiak II, Mori CM, da Silva TC, Oloris SC, Garate AP, Massironi SM, Yamasaki H, Dagli ML (2004) Increased susceptibility to urethane-induced lung tumors in mice with decreased expression of connexin43. Carcinogenesis 25(10):1973–1982
Pointis G, Fiorini C, Gilleron J, Carette D, Segretain D (2007) Connexins as precocious markers and molecular targets for chemical and pharmacological agents in carcinogenesis. Curr Med Chem 14(21):2288–2303
Mehta PP, Perez-Stable C, Nadji M, Mian M, Asotra K, Roos BA (1999) Suppression of human prostate cancer cell growth by forced expression of connexin genes. Dev Genet 24(1–2):91–110
Fukushima M, Hattori Y, Yoshizawa T, Maitani Y (2007) Combination of non-viral connexin 43 gene therapy and docetaxel inhibits the growth of human prostate cancer in mice. Int J Oncol 30(1):225–231
Xu HT, Li QC, Zhang YX, Zhao Y, Liu Y, Yang ZQ, Wang EH (2008) Connexin 43 recruits E-cadherin expression and inhibits the malignant behaviour of lung cancer cells. Folia Histochem Cytobiol 46(3):315–321
Oliveira R, Christov C, Guillamo JS, de Bouard S, Palfi S, Venance L, Tardy M, Peschanski M (2005) Contribution of gap junctional communication between tumor cells and astroglia to the invasion of the brain parenchyma by human glioblastomas. BMC Cell Biol 6(1):7
Zhang W, DeMattia JA, Song H, Couldwell WT (2003) Communication between malignant glioma cells and vascular endothelial cells through gap junctions. J Neurosurg 98(4):846–853
Pollmann MA, Shao Q, Laird DW, Sandig M (2005) Connexin 43 mediated gap junctional communication enhances breast tumor cell diapedesis in culture. Breast Cancer Res 7(4):R522–R534
Kapoor P, Saunders MM, Li Z, Zhou Z, Sheaffer N, Kunze EL, Samant RS, Welch DR, Donahue HJ (2004) Breast cancer metastatic potential: correlation with increased heterotypic gap junctional intercellular communication between breast cancer cells and osteoblastic cells. Int J Cancer 111(5):693–697
Bellahcene A, Bachelier R, Detry C, Lidereau R, Clezardin P, Castronovo V (2007) Transcriptome analysis reveals an osteoblast-like phenotype for human osteotropic breast cancer cells. Breast Cancer Res Treat 101(2):135–148
Logothetis CJ, Lin SH (2005) Osteoblasts in prostate cancer metastasis to bone. Nat Rev Cancer 5(1):21–28
Jin JK, Dayyani F, Gallick GE (2011) Steps in prostate cancer progression that lead to bone metastasis. Int J Cancer 128(11):2545–2561
Mehta PP, Lokeshwar BL, Schiller PC, Bendix MV, Ostenson RC, Howard GA, Roos BA (1996) Gap-junctional communication in normal and neoplastic prostate epithelial cells and its regulation by cAMP. Mol Carcinog 15(1):18–32
Govindarajan R, Zhao S, Song XH, Guo RJ, Wheelock M, Johnson KR, Mehta PP (2002) Impaired trafficking of connexins in androgen-independent human prostate cancer cell lines and its mitigation by alpha-catenin. J Biol Chem 277(51):50087–50097
Wang M, Berthoud VM, Beyer EC (2007) Connexin43 increases the sensitivity of prostate cancer cells to TNFalpha-induced apoptosis. J Cell Sci 120(Pt 2):320–329
Miekus K, Czernik M, Sroka J, Czyz J, Madeja Z (2005) Contact stimulation of prostate cancer cell migration: the role of gap junctional coupling and migration stimulated by heterotypic cell-to-cell contacts in determination of the metastatic phenotype of Dunning rat prostate cancer cells. Biol Cell 97(12):893–903
Schiller PC, D’Ippolito G, Balkan W, Roos BA, Howard GA (2001) Gap-junctional communication mediates parathyroid hormone stimulation of mineralization in osteoblastic cultures. Bone 28(1):38–44
Lecanda F, Warlow PM, Sheikh S, Furlan F, Steinberg TH, Civitelli R (2000) Connexin43 deficiency causes delayed ossification, craniofacial abnormalities, and osteoblast dysfunction. J Cell Biol 151(4):931–944
Crespin S, Bechberger J, Mesnil M, Naus CC, Sin WC (2010) The carboxy-terminal tail of connexin43 gap junction protein is sufficient to mediate cytoskeleton changes in human glioma cells. J Cell Biochem 110(3):589–597
Geneau G, Lamiche C, Niger C, Strale PO, Clarhaut J, Defamie N, Debiais F, Mesnil M, Cronier L (2010) Effect of endothelin-1 on osteoblastic differentiation is modified by the level of connexin43: comparative study on calvarial osteoblastic cells isolated from Cx43+/− and Cx43+/+ mice. Cell Tissue Res 340(1):103–115
Clarhaut J, Gemmill RM, Potiron VA, Ait-Si-Ali S, Imbert J, Drabkin HA, Roche J (2009) ZEB-1, a repressor of the semaphorin 3F tumor suppressor gene in lung cancer cells. Neoplasia 11(2):157–166
Potiron VA, Sharma G, Nasarre P, Clarhaut JA, Augustin HG, Gemmill RM, Roche J, Drabkin HA (2007) Semaphorin SEMA3F affects multiple signaling pathways in lung cancer cells. Cancer Res 67(18):8708–8715
Goldberg GS, Bechberger JF, Naus CC (1995) A pre-loading method of evaluating gap junctional communication by fluorescent dye transfer. Biotechniques 18(3):490–497
Cronier L, Bastide B, Herve JC, Deleze J, Malassine A (1994) Gap junctional communication during human trophoblast differentiation: influence of human chorionic gonadotropin. Endocrinology 135(1):402–408
Boersema PJ, Aye TT, van Veen TA, Heck AJ, Mohammed S (2008) Triplex protein quantification based on stable isotope labeling by peptide dimethylation applied to cell and tissue lysates. Proteomics 8(22):4624–4632
Majeska RJ, Rodan GA (1982) The effect of 1, 25(OH)2D3 on alkaline phosphatase in osteoblastic osteosarcoma cells. J Biol Chem 257(7):3362–3365
Krutovskikh VA, Troyanovsky SM, Piccoli C, Tsuda H, Asamoto M, Yamasaki H (2000) Differential effect of subcellular localization of communication impairing gap junction protein connexin43 on tumor cell growth in vivo. Oncogene 19(4):505–513
Olbina G, Eckhart W (2003) Mutations in the second extracellular region of connexin 43 prevent localization to the plasma membrane, but do not affect its ability to suppress cell growth. Mol Cancer Res 1(9):690–700
Bates DC, Sin WC, Aftab Q, Naus CC (2007) Connexin43 enhances glioma invasion by a mechanism involving the carboxy terminus. Glia 55(15):1554–1564
Lin JH, Takano T, Cotrina ML, Arcuino G, Kang J, Liu S, Gao Q, Jiang L, Li F, Lichtenberg-Frate H, Haubrich S, Willecke K, Goldman SA, Nedergaard M (2002) Connexin 43 enhances the adhesivity and mediates the invasion of malignant glioma cells. J Neurosci 22(11):4302–4311
Kandouz M, Batist G (2010) Gap junctions and connexins as therapeutic targets in cancer. Expert Opin Ther Targets 14(7):681–692
Tang M, Asamoto M, Ogawa K, Naiki-Ito A, Sato S, Takahashi S, Shirai T (2009) Induction of apoptosis in the LNCaP human prostate carcinoma cell line and prostate adenocarcinomas of SV40T antigen transgenic rats by the Bowman-Birk inhibitor. Pathol Int 59(11):790–796
Shiirevnyamba A, Takahashi T, Shan H, Ogawa H, Yano S, Kanayama H, Izumi K, Uehara H (2011) Enhancement of osteoclastogenic activity in osteolytic prostate cancer cells by physical contact with osteoblasts. Br J Cancer 104(3):505–513
Guise T (2010) Examining the metastatic niche: targeting the microenvironment. Semin Oncol 37(Suppl 2):S2–S14
Andersen H, Jensen ON, Moiseeva EP, Eriksen EF (2003) A proteome study of secreted prostatic factors affecting osteoblastic activity: galectin-1 is involved in differentiation of human bone marrow stromal cells. J Bone Miner Res 18(2):195–203
Dougall WC, Chaisson M (2006) The RANK/RANKL/OPG triad in cancer-induced bone diseases. Cancer Metastasis Rev 25(4):541–549
Saad F, Gleason DM, Murray R, Tchekmedyian S, Venner P, Lacombe L, Chin JL, Vinholes JJ, Goas JA, Zheng M (2004) Long-term efficacy of zoledronic acid for the prevention of skeletal complications in patients with metastatic hormone-refractory prostate cancer. J Natl Cancer Inst 96(11):879–882
Li Z, Zhou Z, Donahue HJ (2008) Alterations in Cx43 and OB-cadherin affect breast cancer cell metastatic potential. Clin Exp Metastasis 25(3):265–272
Haass NK, Smalley KS, Herlyn M (2004) The role of altered cell–cell communication in melanoma progression. J Mol Histol 35(3):309–318
Elzarrad MK, Haroon A, Willecke K, Dobrowolski R, Gillespie MN, Al-Mehdi AB (2008) Connexin-43 upregulation in micrometastases and tumor vasculature and its role in tumor cell attachment to pulmonary endothelium. BMC Med 6:20
Saunders MM, Seraj MJ, Li Z, Zhou Z, Winter CR, Welch DR, Donahue HJ (2001) Breast cancer metastatic potential correlates with a breakdown in homospecific and heterospecific gap junctional intercellular communication. Cancer Res 61(5):1765–1767
Plante I, Stewart MK, Barr K, Allan AL, Laird DW (2011) Cx43 suppresses mammary tumor metastasis to the lung in a Cx43 mutant mouse model of human disease. Oncogene 30(14):1681–1692
Tate AW, Lung T, Radhakrishnan A, Lim SD, Lin X, Edlund M (2006) Changes in gap junctional connexin isoforms during prostate cancer progression. Prostate 66(1):19–31
Acknowledgments
This work was supported by the French Society of Rheumatology (SFR); the “Ligue Nationale contre le Cancer” and The Canadian Institutes of Health Research (CCN, LJF). C. Lamiche is supported by grants from the region “Poitou–Charentes”. We are most grateful to Drs A. Le Pape and S. Lerondel (CIPA, CNRS, TAAM UPS 44, Orléans, France) for their expert assistance during in vivo experiments. The authors would like to thank Dr A.C. Balandre, N. Stoynov and L. Le Scouarnec for their technical support.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lamiche, C., Clarhaut, J., Strale, PO. et al. The gap junction protein Cx43 is involved in the bone-targeted metastatic behaviour of human prostate cancer cells. Clin Exp Metastasis 29, 111–122 (2012). https://doi.org/10.1007/s10585-011-9434-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-011-9434-4