Abstract
There is a growing body of evidence showing that vitamin A induces toxic effects in several experimental models and in human beings. In the present work, we have investigated the effects of short-term vitamin A supplementation on the adult rat liver redox status. We have found that vitamin A at therapeutic doses induces a hepatic oxidative insult. Furthermore, we have observed increased antioxidant enzyme activity in the liver of vitamin-A-treated rats. Additionally, some mitochondrial dysfunction was found since superoxide anion production was increased in vitamin-A-treated rat liver submitochondrial particles, which may be the result of impaired mitochondrial electron transfer chain activity, as assessed here. We have also isolated rat liver mitochondria and challenged it with 75 μM CaCl2, a non-oxidant agent that is able to induce mitochondrial oxidative stress indirectly. We have found that mitochondria isolated from vitamin-A-treated rat liver are more sensitive to CaCl2 than control mitochondria regarding the redox status. Importantly, vitamin A seems to alter mitochondrial redox status independently of the participation of the mitochondrial permeability transition pore, which is activated by Ca2+ ions since cyclosporin A did not prevent the oxidative insult elicited by Ca2+ addition. Overall, we show here that mitochondria are a target of vitamin-A-associated toxicity also in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vitamin A is a micronutrient that is necessary in all stages of mammalian development. During adulthood, either vitamin A (retinol) or its derivatives (retinoids) also participate in the maintenance of mammalian organism homeostasis (Napoli 1999). The liver is the site where vitamin A is stored in an esterified form, namely retinyl palmitate (Olson and Gunning 1983; Napoli 1996). Vitamin A esters are more stable than free retinol and will be metabolized when retinol serum levels fall (Napoli 1996). In spite of this, there is a growing body of evidence suggesting that vitamin A may induce or facilitate liver toxicity. Low vitamin A doses might protect liver damage induced through CCl4 administration (Rosengren et al. 1995). However, chronic treatment with vitamin A alone induces liver damage (Russell et al. 1974) and fails in protecting liver against CCl4-induced toxicity (Elsisi et al. 1993a, b; Badger et al. 1996).
Therapeutically, vitamin A and retinoids are administrated in some pathological conditions at high doses, for instance leukemia and dermatological diseases (Norum 1993; Fenaux et al. 2001; Myhre et al. 2003). Short-term vitamin A exposition (i.e., days to weeks) at high doses is known to induce a myriad of side effects, including diarrhea and cognitive impairments (Geelen 1979; Myhre et al. 2003; O’Reilly et al. 2006). Additionally, vitamin A exposition as a food supplement or fortification may lead to intoxication, as recently published (Lam et al. 2006). However, the exact mechanism of such toxicity remains to be established. It is well established that retinoids are potent inducers of mitochondrial dysfunction, for instance mitochondrial swelling and leakage of cytochrome c (Rigobello et al. 1999; Klamt et al. 2005), with such an event culminating in increased reactive oxygen species (ROS) production (Klamt et al. 2005). Cytochrome c release to cytosol is a pro-apoptotic event, and ROS production is thought to participate positively in such event (Hengartner 2000; Ott et al. 2002; Kagan et al. 2004). Indeed, it has been shown that vitamin A and retinoids induce apoptosis in different cell types (Pfahl and Piedrafita 2003). However, excessive ROS or reactive nitrogen species production inhibit apoptosis progression since the caspases are dependent on a reduced thiol group in their active site to cleave their substrates (Hengartner 2000).
It has been demonstrated that vitamin A is a redox-active molecule whose behavior is pro- or antioxidant depending on its concentration. Recently, we have found that both short- and long-term vitamin A supplementation increased superoxide anion (O2 −•) production in submitochondrial particles (SMP) isolated from rat cerebral cortex and cerebellum (De Oliveira and Moreira 2007). Interestingly, we did not observe any adaptation to the insult promoted by vitamin A supplementation in the long-term exposition, showing that it is an important toxic effect of this vitamin A in those brain regions. Previously reported data also confirm the capacity of vitamin A (retinol) and its derivatives in inducing alterations in the cellular redox environment, including protein carbonylation, lipid peroxidation, and DNA damage induced by free radicals (Moreira et al. 1997; Dal-Pizzol et al. 2000; Klamt et al. 2000; Dal-Pizzol et al. 2001; Frota et al. 2004; De Oliveira et al. 2007a, b).
Therefore, we decided to investigate the effects of short-term vitamin A supplementation on rat liver regarding the redox effects of such treatment. Moreover, we have assessed mitochondrial electron transfer chain (METC) activity in the liver of vitamin-A-treated rats. We have also isolated liver mitochondria to analyze similar parameters. In addition, we have challenged isolated mitochondria with calcium, a non-oxidant agent, that is able to induce mitochondrial swelling and, indirectly, increases free radical production in mitochondria. The main objective of this work was to investigate whether a non-oxidant agent such as calcium ion was able to induce mitochondrial dysfunction in mitochondria isolated from vitamin-A-treated rats regarding redox environment parameters.
Materials and methods
Animals
We used adult male Wistar rats (90 days old; 250–320 g) obtained from our own breeding colony. They were caged in groups of five with free access to food and water and were maintained on a 12-h light–dark cycle (7:00–19:00 h) at 23 ± 1°C. All experimental procedures were performed in accordance with the National Institute of Health Guide for the Care and Use of Laboratory Animals recommendations for animal care. The Ethical Committee for animal experimentation of the Federal University of Rio Grande do Sul approved our research protocol.
Drugs and reagents
Arovit® (retinyl palmitate, a water soluble form of vitamin A) was purchased from Bayer, Sao Paulo, SP, Brazil. All other chemicals were purchased from Sigma, St. Louis, MO, USA. Vitamin A was prepared daily, and it occurred by protecting from light and by utilizing amber vials.
Drug administration
The animals were treated once a day for 3 or 7 days. All treatments were carried out at night (i.e., when the animals are more active and take a greater amount of food) in order to ensure maximum vitamin A absorption since this vitamin is better absorbed during or after a meal. The animals were randomly separated between groups and were treated with vehicle (0.15 M saline; control group), 1,000, 2,500, 4,500, or 9,000 IU/kg of retinyl palmitate (vitamin A) administered orally via a metallic gastric tube (gavage) in a maximum volume of 0.8 mL during each period of interest. We utilized six to seven animals in each experimental group. Vitamin A content in the diet of the animals was 12,500 IU/kg food. The daily vitamin A ingestion present only in the chow was calculated within the range of 350–400 UI/day. In the vitamin A supplementation groups, the rats were treated with vitamin A at doses ranging from 300 to 320 IU/day (1,000 IU/kg/day group), from 750 to 800 IU/day (2,500 IU/kg/day group), from 1,350 to 1,440 IU/day (4,500 IU/kg/day group), and from 2,700 to 2,880 IU/day (9,000 IU/kg/day group). Adequate measures were taken to minimize pain or discomfort.
Preparations of the samples
The animals were sacrificed by decapitation at 24 h after the last vitamin A administration. The liver was dissected out in ice immediately after the sacrifice and stored at −80°C for posterior biochemical analyses. The liver was homogenized in ice-cold 0.1 M phosphate buffer (pH 7.4). The homogenates were centrifuged (700×g, 5 min) to remove cellular debris. Supernatants were used for all biochemical assays described herein. SMP and intact mitochondria were isolated as described below. The results regarding liver redox state were normalized by the protein content using bovine albumin as standard (Lowry et al. 1951).
Isolation of submitochondrial particles (SMP)
Briefly, to obtain SMP, liver was dissected and homogenized in 230 mM mannitol, 70 mM sucrose, 10 mM Tris–HCl, and 1 mM EDTA (pH 7.4). Freezing and thawing (three times) the mitochondrial solution gave rise to superoxide dismutase-free SMP. The SMP solution was also washed (twice) with 140 mM KCl, 20 mM Tris–HCl (pH 7.4) to ensure Mn–superoxide dismutase (SOD) release from mitochondria (Poderoso et al. 1996; De Oliveira and Moreira 2007).
Isolation of intact mitochondria
Mitochondria from fresh rat liver were isolated as described elsewhere (Klamt et al. 2005). Briefly, liver of Wistar rats suspended in ice-cold isolation buffer A (220 mM mannitol, 70 mM sucrose, 5 mM HEPES (pH 7.4), 1 mM EGTA, and 0.5 mg/mL fatty-acid free bovine serum albumin) was gently homogenized with a glass-homogenizer and centrifuged at 2000×g for 10 min at 4°C. Approximately three quarters of the supernatant was further centrifuged at 10,000×g for 10 min at 4°C in a new tube. The fluffy layer of the pellet was removed by gently shaking with buffer A, and the firmly packed sediment was resuspended in the same buffer without EGTA and centrifuged at 10,000×g for 10 min at 4°C. The mitochondrial pellet was resuspended in buffer B (210 mM mannitol, 70 mM sucrose, 10 mM HEPES–KOH (pH 7.4), 4.2 mM succinate, 0.5 mM KH2PO4, and 4 μg/mL rotenone). This procedure, which was designed to isolate intact mitochondria rather than to recover all of that present in the liver, yielded about 20 mg of mitochondrial protein per gram of liver.
Incubation of intact rat liver mitochondria
After the end of the in vivo treatments, the animals were killed as mentioned above. Liver mitochondria were isolated as described, and 1 mg/mL mitochondria were incubated (in the presence of O2) for 10 min at 25°C with or without CaCl2 and/or co-treatments. Co-treatments consisted of 1 mM dithiothreitol (DTT), 1 mM reduced glutathione (GSH), 200 U/mL native purified superoxide dismutase (SOD), 50 U/mL catalase (CAT), 850 nM cyclosporine A (CsA), 50 μM bongkrekic acid (BKA), or 10 μM Trolox™ (an analogue of vitamin E). Co-treatments, when used, were added to the incubation buffer with or without CaCl2 in the beginning of the assay. After the ending of the incubation period, the samples were centrifuged at 10,000×g for 10 min at 4°C, and the mitochondrial pellet was resuspended in phosphate-buffered saline (pH 7.4) or in 140 mM KCl, 20 mM Tris–HCl (pH 7.4) buffer to assess oxidative stress markers or superoxide anion (O2 −•) production, respectively. To assess O2 −• production in intact mitochondria, we froze and thawed mitochondria three times to obtain mitochondrial membranes without mitochondrial matrix so that mitochondrial SOD did not interfere with the assay as mentioned above.
Antioxidant enzyme activity estimations
SOD activity was assessed by quantifying the inhibition of superoxide-dependent adrenaline auto-oxidation in a spectrophotometer at 480 nm, as previously described (Misra and Fridovich 1972). Catalase (CAT) activity was assayed by measuring the rate of decrease in H2O2 absorbance in a spectrophotometer at 240 nm (Aebi 1984). A ratio between SOD activity and CAT activity (SOD/CAT ratio) was applied to better understand the effect of vitamin A supplementation upon these two oxidant-detoxifying enzymes that work sequentially converting the superoxide anion to water (Halliwell 2006). An imbalance between their activities is thought to facilitate oxidative-dependent alterations in the cellular environment, which may culminate in oxidative stress.
Thiobarbituric acid reactive species (TBARS)
As an index of lipid peroxidation, we detected hepatic and mitochondrial thiobarbituric acid reactive species (TBARS) formation through a hot and acidic reaction. This is widely adopted as a method for measurement of lipid redox state, as previously described (Draper and Hadley 1990). Briefly, the samples were mixed with 0.6 mL of 10% trichloroacetic acid (TCA) and 0.5 mL of 0.67% thiobarbituric acid and then heated in a boiling water bath for 25 min. TBARS were determined by absorbance in a spectrophotometer at 532 nm. We have obtained TBARS concentration in the samples from a calibration curve that was performed using 1,1,3,3-tetramethoxypropane as standard, which was subjected to the same treatment as that applied to the supernatants of the samples. Results are expressed as nanomoles TBARS per milligram protein.
Measurement of protein carbonyls
The oxidative damage to proteins was measured by the quantification of carbonyl groups based on the reaction with dinitrophenylhydrazine (DNPH) as previously described (Levine et al. 1990). Briefly, tissue homogenates or mitochondria were divided into two aliquots of 200 μl. Proteins were precipitated by the addition of 100 μl 20% TCA for 5 min on ice and centrifuged at 4,000×g for 5 min. The pellet was redissolved in 100 μl 0.2 M NaOH, and 100 μl of 2 M HCl or 10 mM 2,4-DNPH in 2 M HCl was added to duplicate aliquots for blanks or the derivatizing of carbonyl groups, respectively. Samples were left for 30 min at room temperature. Proteins were reprecipitated with 20% TCA and washed three times with 500 μl 1:1 ethanol/ethyl acetate with 15-min standing periods to remove excess DNPH. Samples were redissolved in 1 mL 8 M urea, pH 2.3, and the absorbance was read at 370 nm. The carbonyl content in nanomoles per milligram protein was calculated using a molar extinction coefficient of 22,000 M−1 cm−1 at 370 nm after subtraction of the blank absorbance according to the following equation: \({{\left\{ {{{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {22,000}}} \right. \kern-\nulldelimiterspace} {22,000}}} \right) \times V} \right]} \mathord{\left/ {\vphantom {{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {22,000}}} \right. \kern-\nulldelimiterspace} {22,000}}} \right) \times V} \right]} {1,000}}} \right. \kern-\nulldelimiterspace} {1,000}}} \right\}} \mathord{\left/ {\vphantom {{\left\{ {{{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {22,000}}} \right. \kern-\nulldelimiterspace} {22,000}}} \right) \times V} \right]} \mathord{\left/ {\vphantom {{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {22,000}}} \right. \kern-\nulldelimiterspace} {22,000}}} \right) \times V} \right]} {1,000}}} \right. \kern-\nulldelimiterspace} {1,000}}} \right\}} Q}} \right. \kern-\nulldelimiterspace} Q}\), where V is the volume (in milliliters) of the sample utilized in the assay, and Q is the amount of protein (in milligrams) in the volume utilized to perform the carbonyl assay.
Measurement of protein and non-protein thiol content
Briefly, a supernatant aliquot of 20% TCA precipitated homogenates was diluted in SDS 0.1%, and 0.01 M 5,5′-dithionitrobis 2-nitrobenzoic acid (DTNB) in ethanol was added, and the intense yellow color was developed and read at 412 nm after 20 min (Ellman 1959). A blank sample was run simultaneously, except for the absence of DTNB. Protein thiol content was calculated after subtraction of the blank absorbance through the following equation utilizing the molar extinction coefficient of 13,600 M−1 cm−1 \({{\left\{ {{{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {13,600}}} \right. \kern-\nulldelimiterspace} {13,600}}} \right) \times V} \right]} \mathord{\left/ {\vphantom {{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {13,600}}} \right. \kern-\nulldelimiterspace} {13,600}}} \right) \times V} \right]} {1,000}}} \right. \kern-\nulldelimiterspace} {1,000}}} \right\}} \mathord{\left/ {\vphantom {{\left\{ {{{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {13,600}}} \right. \kern-\nulldelimiterspace} {13,600}}} \right) \times V} \right]} \mathord{\left/ {\vphantom {{\left[ {\left( {{{Final\;Absorbance} \mathord{\left/ {\vphantom {{Final\;Absorbance} {13,600}}} \right. \kern-\nulldelimiterspace} {13,600}}} \right) \times V} \right]} {1,000}}} \right. \kern-\nulldelimiterspace} {1,000}}} \right\}} Q}} \right. \kern-\nulldelimiterspace} Q}\), where V is the volume (in milliliters) of the sample utilized in the assay, and Q is the amount of protein (in milligrams) in the volume utilized to perform the carbonyl assay. The free sulfhydryl (–SH) content (non-protein thiol content) was estimated in supernatants of 20% TCA precipitated homogenates by the same method and was calculated according to the same equation described above. Results are expressed as nano- or micromoles SH per milligram protein, depending on the sample analyzed (rat tissue or mitochondria).
Quantification of O2 −• production
To quantify superoxide (O2 −•) production, SMP was incubated in reaction medium consisting of 230 mM mannitol, 70 mM sucrose, 10 mM HEPES–KOH (pH 7.4), 4.2 mM succinate, 0.5 mM KH2PO4, 0.1 μM catalase, and 1 mM epinephrine, and the increase in the absorbance (auto-oxidation of adrenaline to adrenochrome) was read in a spectrophotometer at 480 nm at 32°C, as previously described (Poderoso et al. 1996; De Oliveira and Moreira 2007).
Mitochondrial electron transfer chain (METC) enzyme activities
To obtain SMP from rat liver in order to assess METC activity, we homogenized the tissue in 250 mM sucrose, 2 mM EDTA, 10 mM Tris, pH 7.4, and 50 IU/mL heparin buffer. The samples were centrifuged 1,000×g, and the supernatants were colleted. Then, the samples were frozen and thawed three times, and METC activity detection was performed as described below.
Complex I–CoQ-III activity
Complex I–CoQ-III activity was determined by following the increase in absorbance due to reduction of cytochrome c at 550 nm with 580 nm as reference wavelength (∈ = 19.1 mM−1 cm−1). The reaction buffer contained 20 mM potassium phosphate, pH 8.0, 2.0 mM KCN, 10 μM EDTA, 50 μM cytochrome c, and 20–45 μg supernatant protein. The reaction started by addition of 25 μM NADH and was monitored at 30°C for 3 min before the addition of 10 μM rotenone, after which the activity was monitored for an additional 3 min. Complex I–III activity was the rotenone-sensitive NADH/cytochrome c oxidoreductase activity (Shapira et al. 1990).
Complex II–CoQ-III activity
Complex II–CoQ-III activity was measured by following the increase in absorbance due to the reduction of cytochrome c at 550 nm with 580 nm as the reference wavelength (∈ = 21 mM−1 cm−1). The reaction mixture consisting of 40 mM potassium phosphate, pH 7.4, and 16 mM succinate was preincubated with 50–100 μg supernatant protein at 30°C for 30 min. Subsequently, 4.0 mM sodium azide and 7.0 μM rotenone were added, and the reaction was started by the addition of 0.6 μg/mL cytochrome c and was monitored for 5 min at 30°C (Fisher et al. 1985).
Complex IV activity
Complex IV activity was measured by following the decrease in absorbance due to the oxidation of previously reduced cytochrome c at 550 nm with 580 nm as reference wavelength (∈ = 19.15 mM−1 cm−1). The reaction buffer contained 10 mM potassium phosphate, pH 7.0, 0.6 mM n-dodecyl-β-d-maltoside, 2–4 μg supernatant protein, and the reaction was started with addition of 0.7 μg reduced cytochrome c. The activity of complex IV was measured at 25°C for 10 min (Rustin et al. 1994).
Statistical analyses
Biochemical data are expressed as means ± SEM. All analyses were performed using the Statistical Package for the Social Sciences (SPSS 12.0) software. p values were considered significant when p < 0.05. Differences in experimental groups were determined by the Student’s t test or the one-way ANOVA followed by the post hoc Duncan’s test.
Results
Hepatic oxidative damage parameters
Lipid peroxidation
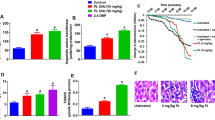
As depicted in Fig. 1a, we found increased lipid peroxidation in the liver of the rats that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day for 3 days (1.4- to 1.7-fold; p < 0.01). However, hepatic lipid peroxidation levels did not change after vitamin A supplementation for 7 days (Fig. 1a).
Protein carbonylation
We found a 1.3- to 1.7-fold increase of protein carbonylation levels in the liver of the rats that received vitamin A at any dose tested for 3 days (p < 0.01; Fig. 1b). Vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day induced a 1.3- to 1.4-fold increase of hepatic protein carbonylation levels in the rats that were treated for 7 days (p < 0.01; Fig. 1b).
Protein thiol content
As shown in Fig. 1c, we detected decreased protein thiol content (1.2- to 1.3-fold) in the liver of the rats that were treated with vitamin A at 2,500, 4,500, or 9,000 IU/kg/day for 3 days (p < 0.01). However, protein thiol content did not change in the liver of the rats that were treated with vitamin A for 7 days (Fig. 1c).
Non-protein thiol content
Hepatic non-protein thiol content did not change in the rats that received vitamin A supplementation for 3 days (Fig. 1d). We found that vitamin A at 2,500, 4,500, or 9,000 IU/kg/day induced a 1.4- to 1.5-fold decrease of hepatic non-protein thiol content (p < 0.01; Fig. 1d).
Antioxidant enzyme activities
SOD activity
Vitamin A supplementation at 9,000 IU/kg/day induced a 1.3-fold increase of SOD activity in the liver of the rats that were treated for 3 days (p < 0.05; Fig. 2a). Sustained vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day for 7 days induced a 1.2- to 1.4-fold increase in hepatic SOD activity (p < 0.05; Fig. 2a).
CAT activity
We found increased (1.4-fold) CAT activity in the liver of the rats that received vitamin A supplementation at 9,000 IU/kg/day for 3 days (p < 0.05; Fig. 2b). CAT enzyme activity did not change in the liver of the rats that received vitamin A supplementation for 7 days (p < 0.05; Fig. 2b).
SOD/CAT
Hepatic SOD/CAT increased in the animals that received vitamin A supplementation at 4,500 or 9,000 IU/kg/day for 7 days (p < 0.05; Fig. 2c).
Hepatic submitochondrial particles (SMP) oxidative parameters
Superoxide anion (O2 −•) production
We found increased (1.3- to 1.6-fold; p < 0.01) O2 −• production in hepatic SMP of the rats that were treated with vitamin A at 2,500, 4,500, or 9,000 IU/kg/day for 3 days (Fig. 3a). Vitamin A supplementation at any dose tested induced a 1.3- to 1.7-fold increase of O2 −• production in hepatic SMP isolated from the rats that were treated for 7 days (p < 0.01; Fig. 3a).
Effects of short-term vitamin A supplementation on superoxide anion production (a), lipid peroxidation (b), protein carbonylation (c), and protein thiol content (d) in SMP isolated form rat liver. Data are mean ± SEM (n = 7 per group). *p < 0.01 (one-way ANOVA followed by the post hoc Duncan’s test)
SMP lipid peroxidation
As depicted in Fig. 4b, we found increased (1.7- to 2.7-fold) lipid peroxidation levels in hepatic SMP of the rats that received vitamin A at 2,500, 4,500, or 9,000 IU/kg/day for 3 days (p < 0.01). Vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day increased (1.6- to 2.7-fold) hepatic SMP lipid peroxidation levels in the rats that were treated for 7 days (p < 0.01; Fig. 3b).
SMP protein carbonylation
Vitamin A supplementation at 9,000 IU/kg/day induced a 1.5-fold increase of SMP protein carbonylation levels in the rats that were treated for 3 days (p < 0.01; Fig. 3c). Sustained vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day for 7 days induced a 1.5- to 1.8-fold increase of SMP protein carbonylation levels (Fig. 3c).
SMP protein thiol content
Hepatic SMP protein thiol content did not change in this experimental model (Fig. 3d).
Hepatic mitochondrial electron transfer chain (METC) enzyme activities
As depicted in Fig. 4a, vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg/day for 3 days induced an increase (1.3 to 1.5-fold) in hepatic complex I–III enzyme activity. We observed that vitamin A supplementation at any dose tested for 7 days induced an increase (1.3- to 1.6-fold) in hepatic complex I–III enzyme activity (Fig. 4a). In spite of this, we did not find any change in complex II–III and IV enzyme activities in the liver of vitamin-A-treated rats (Fig. 4b and c).
Incubated hepatic mitochondria
Lipid peroxidation
As shown in Table 1, mitochondria that were isolated from the liver of the rats that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 3 days present higher lipid peroxidation levels when incubated for 10 min with buffer C (p < 0.05). Interestingly, 75 μM CaCl2 induced a 2.5- to 2.9-fold increase of lipid peroxidation in liver mitochondria from the animals that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 3 days when compared with mitochondria isolated from the liver of the animals that received saline (vitamin A vehicle) for 3 days (p < 0.01). A co-treatment with GSH, SOD, CAT, or Trolox™ decreased lipid peroxidation levels induced by CaCl2 (p < 0.05; Table 1).
A very similar effect was observed when mitochondria were isolated from the liver of the rats that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 7 days (Table 1). Co-treatment with mitochondrial permeability transition pore (MPTP) inhibitors did not prevent the oxidative damage induced by 75 μM CaCl2 in mitochondria isolated from vitamin-A-treated rats (Table 2). The co-treatments alone did not alter mitochondrial lipid peroxidation levels (data not shown).
Protein carbonylation
We found increased protein carbonylation levels in incubated mitochondria (in the absence of CaCl2) that were isolated from the liver of the rats that were treated with vitamin A at 9,000 IU/kg for 3 days (p < 0.05; Table 3). CaCl2 at 75 μM induced a 1.7- to 2.0-fold increase of protein carbonylation in the mitochondria that were isolated from the liver of the rats that received vitamin A supplementation at 4,500 or 9,000 IU/kg for 3 days (p < 0.01; Table 2). CaCl2-induced protein carbonylation was decreased by a co-treatment with GSH, SOD, or Trolox™ (p < 0.05; Table 3).
Mitochondria that were isolated from the liver of the rats that were treated with vitamin A at 2,500, 4,500, or 9,000 IU/kg for 7 days showed increased (1.4- to 1.5-fold) protein carbonylation levels even when incubated in the absence of CaCl2 (p < 0.05; Table 2). However, the addition of CaCl2 increased (1.7- to 2.0-fold) protein carbonylation levels in mitochondria that were isolated from the animals that received vitamin A at 2,500, 4,500, or 9,000 IU/kg when compared with mitochondria isolated from the animals that received saline (p < 0.01; Table 2). Only the co-treatment with GSH, SOD, or Trolox™ prevented the increase in protein carbonylation induced by CaCl2 (p < 0.05; Table 3). Co-treatment with MPTP inhibitors did not prevent the oxidative damage induced by 75 μM CaCl2 in mitochondria isolated from vitamin-A-treated rats (Table 4). The co-treatments alone did not interfere in the mitochondrial protein carbonylation levels (data not shown).
Protein thiol content
As depicted in Table 5, protein thiol content of mitochondria isolated from control or vitamin-A-treated rats did not change when incubated in the absence of CaCl2. However, CaCl2 induced a 1.3- to 1.4-fold decrease of protein thiol content in the mitochondria isolated from the animals that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 3 days when compared to mitochondria isolated from control animals (p < 0.05). A co-treatment with GSH, SOD, or Trolox™ prevented the decrease in protein thiol content induced by CaCl2 (p < 0.05; Table 5).
We did not detect any change in liver mitochondria isolated from 7-day vitamin-A-treated rats when incubated without CaCl2 regarding the redox state of protein thiol content (Table 5). However, CaCl2 at 75 μM induced a decrease (1.5- to 1.6-fold) in the protein thiol content of the mitochondria that were isolated from the animals that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 7 days when compared to control animals (p < 0.05; Table 5). A co-treatment with GSH, SOD, or Trolox™ prevented the decrease in protein thiol content induced by CaCl2 (p < 0.05; Table 5). Co-treatment with MPTP inhibitors did not prevent the oxidative damage induced by 75 μM CaCl2 in mitochondria isolated from vitamin-A-treated rats (Table 6). The co-treatments alone did not alter mitochondrial protein thiol content (data not shown).
Superoxide anion (O2 −•) production
As shown in Table 7, mitochondria that were isolated from the liver of the rats that received vitamin A supplementation at 2,500, 4,500, or 9,000 IU/kg for 3 days produced more O2 −• after incubation without CaCl2 when compared to mitochondria isolated from the liver of control animals (p < 0.05). The addition of CaCl2 increased (2.0- to 2.45-fold) O2 −• production in mitochondria isolated from vitamin-A-treated rats (2,500, 4,500, or 9,000 IU/kg vitamin A, 3 days; p < 0.01). A co-treatment with GSH, SOD, or Trolox™ prevented the increase in O2 −• production induced by CaCl2 (p < 0.05; Table 7).
We detected increased O2 −• production in mitochondria isolated from the animals that received vitamin A supplementation at any dose tested for 7 days after incubation without CaCl2 when compared to mitochondria isolated from the liver of control animals treated during the same period (p < 0.05; Table 7). The addition of CaCl2 increased O2 −• production (2.0- to 2.7-fold) in mitochondria isolated from the rats that received vitamin A supplementation at any dose tested when compared to saline-treated animals (control animals; p < 0.01; Table 7). A co-treatment with GSH, SOD, or Trolox™ prevented the increase in O2 −• production induced by CaCl2 (p < 0.05; Table 7). Co-treatment with MPTP inhibitors did not prevent the oxidative damage induced by 75 μM CaCl2 in mitochondria isolated from vitamin-A-treated rats (Table 8). The co-treatments alone did not alter mitochondrial O2 −• production levels (data not shown).
Discussion
In this work, we investigated the short-term effects of vitamin A supplementation on rat liver redox parameters. In addition, we have isolated SMP and intact mitochondria from the liver of the animals that received vitamin A at different doses and analyzed the effects of vitamin A supplementation on the mitochondrial redox state. We have found that vitamin A supplementation for 3 or 7 days exerts a pro-oxidant state on rat liver and on isolated hepatic mitochondria, as well as on mitochondria that were incubated with CaCl2, a non-oxidant agent that is able to, indirectly, induce oxidative stress in mitochondria through mitochondrial dysfunction, for instance mitochondrial swelling (Cai and Jones 1998).
Vitamin A is, as previously mentioned, a redox-active molecule, which is able to induce—or facilitate—oxidative stress in several experimental models. We have recently reported increased superoxide anion (O2 •−) production in SMP isolated from rat cerebral cortex and cerebellum (De Oliveira and Moreira 2007). Furthermore, we have previously reported that retinol induces mitochondrial swelling in vitro and, consequently, induces cytochrome c release from mitochondria (Klamt et al. 2005). In the present work, we demonstrate, for the first time, that mitochondria isolated from the livers of rats that received vitamin A at therapeutic doses for 3 or 7 days is more sensitive to CaCl2 regarding the redox effects of this challenge.
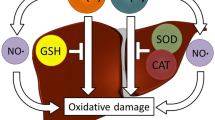
Vitamin A supplementation induced lipid peroxidation, protein carbonylation, and oxidation of protein thiol groups in rat liver in vivo (Fig. 1a,b,c, and d). Interestingly, we did not find any change in lipid peroxidation levels in the liver of the rats that received vitamin A supplementation for 7 days (Fig. 1a). Also, we did not find any change in CAT enzyme activity in the same period (Fig. 2b). At least in part, the non-altered lipid peroxidation levels may be due to decreased rates of hydrogen peroxide production in rat liver in such period since CAT enzyme is not altered. Hydrogen peroxide is a diffusible reactive oxygen species, which is capable of inducing oxidative damage mainly to lipids due to its capacity to cross biological membranes (Halliwell 2006). Non-protein thiol content was decreased only in the animals that receive vitamin A supplementation for 7 days (Fig. 1d), showing that this treatment is able to, at least in part, consume some liver glutathione (GSH), which might facilitate the pro-oxidant effects that were observed in both SMP and intact mitochondria isolated from rat liver (Fig. 3a,b,c, and d; Tables 1, 3, 5, and 7). We found increased SOD and CAT enzyme activities in the liver of the rats that received vitamin A (Fig. 2a, and b). These results indicate an increased O2 •− production since this pro-oxidant agent allosterically activates SOD, which in turn produces H2O2 by dismutation of O2 •− (Halliwell 2006). Actually, we found increased O2 •− production in SMP isolated from the livers of the animals that received vitamin A supplementation (Fig. 3a). According to Fig. 4, we observed increased complex I–III enzyme activity, but unaltered complexes II–III and IV enzyme activities, suggesting mitochondrial uncoupling and, consequently, gave rise to increased O2 •− production, as mentioned above.
The effects seen here when mitochondria were challenged with CaCl2 might be a consequence of increased levels of markers of oxidative stress that were found in vivo in SMP, which represent mitochondrial membranes without mitochondrial matrix content (Poderoso et al. 1996). We found increased lipid peroxidation and protein carbonylation and decreased protein thiol content in SMP isolated from rat liver (Fig. 3a–d). This in vivo oxidative insult might facilitate the in vitro observed impairment in the mitochondrial redox state that was triggered by CaCl2 treatment. Indeed, it was previously reported that oxidation of thiol groups induces mitochondrial dysfunction in several experimental models (Kowaltowski et al. 1998; Kim et al. 2003; Aon et al. 2007). It is important to mention that the CaCl2 concentration used here is considered to be low to moderate when compared to other reports (Borutaite et al. 1999; Duchen 2000). Higher CaCl2 concentrations, for instance 150–300 μM, could induce effects not associated with the ability of calcium ions to open the MPTP.
In Tables 1 and 2, we observed that a co-treatment with DTT, CsA, or BKA did not protect isolated mitochondria against the pro-oxidant state induced by CaCl2 regarding lipid peroxidation. However, the absence of effect of DTT is expected since this thiol reducer agent does not pass through biological membranes. Interestingly, addition of reduced glutathione (GSH), SOD, CAT, or Trolox™ effectively promote mitochondrial protection against CaCl2-induced redox impairment (Table 1, 3, 5, and 7). It is important to mention, again, that CaCl2 induces a pro-oxidant state in mitochondria through indirect action since this molecule did not present an intrinsic capacity to induce oxidative stress directly. The redox effects induced by CaCl2 is very likely to be consequence of CaCl2-dependent MPTP induction, as previously reported (Zamzami and Kroemer 2001). In spite of this, our data indicate a potential toxic effect of vitamin A upon rat liver mitochondria that is independent of MPTP activation. It is noteworthy that neither CsA nor BKA, two inhibitors of the MPTP, did protect mitochondria against CaCl2 pro-oxidant effects (Tables 2, 4, 6, and 8). Protein carbonylation, oxidation of protein thiol content, and O2 •− production were prevented when GSH, SOD, or Trolox™ were added to the incubation buffer, but CAT was ineffective in preventing those oxidant insults induced by CaCl2 (Tables 3, 5, and 7, respectively), suggesting that H2O2 did not participate in altering those redox parameters in this experimental model. Taken together, these data reinforce our hypothesis that vitamin A is able to induce a mitochondrial impairment that is, at least in part, dependent on the redox environment. However, it was also demonstrated that vitamin A is a membranolytic agent (Goodall et al. 1980). This effect might be responsible for all the other effects that were seen in the present work since the doses applied here are considered to be high, even though therapeutically used (Norum 1993; Fenaux et al. 2001). Mitochondrial membrane breakage in vivo could facilitate, for example, O2 •− production since increased mitochondrial cytochrome c leakage facilitates electron transfer chain uncoupling (Borutaite et al. 1999; Klamt et al. 2005). Consequently, it could induce increased oxidative stress parameters in mitochondrial membranes.
Other important research groups have demonstrated that short-term vitamin A supplementation attenuated CCl4-induced liver toxicity through increased CYP4502E1 protein levels (Inder et al. 1999). However, in a previous study, it was demonstrated that vitamin A facilitates acetaminophen-induced hepatotoxicity (Rosengren and Sipes 1995). Indeed, we have recently demonstrated that both short- and long-term vitamin A supplementation have induced a pro-oxidant insult in some rat brain regions and also altered the behavior of the animals, for instance, inducing anxiety-like behavior and decreasing both locomotion in and exploration of an open-field apparatus (De Oliveira and Moreira 2007; De Oliveira et al. 2007b).
Vitamin A supplementation, either therapeutically or inadvertently, is a cause of concern among researchers since this vitamin is promptly delivered to several human tissues through its binding proteins (Napoli 1999). This feature favors the induction of early signs of vitamin A toxicity. However, in some cases, some side effects are very difficult to be diagnosed since it alters, for example, cognition (Myhre et al. 2003). Indeed, some reports have been published showing that vitamin A or some of its derivatives induces depression in humans (Jick et al. 2000; Hull and D’Arcy 2003).
Based on the results presented here and also in previously reported data, we conclude that vitamin A is able to induce a pro-oxidant state in rat liver by, at least in part, inducing an in vivo impairment in the mitochondrial redox state (as assessed through hepatic SMP isolation), which might be responsible for the effects seen when CaCl2 was used as an in vitro challenging agent against mitochondrial integrity. The results shown here indicate that liver mitochondria isolated from vitamin-A-treated rats are more sensitive to a non-oxidant agent when compared to saline-treated rats, i.e., the in vivo vitamin-A-induced oxidative damage favors the in vitro observed mitochondrial redox impairment. Unfortunately, it is almost impossible to indicate the vitamin A metabolite responsible for the observed effects, given the vast number of vitamin A metabolites existing. Additionally, some vitamin A derivatives are very unstable molecules and would exert its effects too fast to be detected due to its high reactivity (Napoli 1999). Also, case reports of vitamin A toxicity have shown serum retinol concentrations within normal limits (Ellis et al. 1986; Croquet et al. 2000; Mills and Tanumihardjo 2006), indicating that serum retinol is not a good measure of vitamin A status during toxicity. Our data could be useful to explain some previously reported studies showing that the liver of rats that received vitamin A supplementation are more sensitive to some chemically stressful conditions. In addition, the herein observed impairment in METC activity may culminate in increased rates of superoxide anion production in the liver of patients treated under high vitamin A doses even acutely. We have observed here increased superoxide anion production levels in the liver of the rats that received vitamin A. Increased rates of superoxide anion production would lead to decreased hepatic function if persistent. Then, the results presented here may be useful to elucidate, at least in part, the mechanism by which vitamin A interferes with tissue homeostasis even during short-term exposure to high levels of this vitamin.
Abbreviations
- CsA:
-
Cyclosporin A
- METC:
-
Mitochondrial electron transfer chain
- MPTP:
-
Mitochondrial permeability transition pore
- SMP:
-
Submitochondrial particles
References
Aebi H. Catalase in vitro. Methods Enzymol 1984;105:121–6
Aon MA, Cortassa S, Maack C, O’Rourke B. Sequential opening of mitochondrial ion channels as a function of glutathione redox thiol status. J Biol Chem 2007;282:21889–900. doi:10.1074/jbc.M702841200.
Badger DA, Sauer JM, Hoglen NC, Jolley CS, Sipes IG. The role of inflammatory cells and cytochrome P450 in the potentiation of CCl4-induced liver injury by a single dose of retinol. Toxicol Appl Pharmacol 1996;141:507–19. doi:10.1006/taap.1996.0316.
Borutaite V, Morkuniene R, Brown GC. Release of cytochrome c from heart mitochondria is induced by high Ca2+ and peroxynitrite and is responsible for Ca2+-induced inhibition of substrate oxidation. Biochim Biophys Acta 1999;1453:41–8.
Cai J, Jones DP. Superoxide in apoptosis. Mitochondrial generation triggered by citochrome c loss. J Biol Chem 1998;273:11401–4. doi:10.1074/jbc.273.19.11401.
Croquet V, Pilette C, Lespine A. Hepatic hypervitaminosis A: importance of retinyl ester level determination. Eur J Gastroenterol Hepatol 2000;12:361–4.
Dal-Pizzol F, Klamt F, Frota MLC Jr, Moraes LF, Moreira JCF, Benfato MS. Retinol supplementation induces DNA damage and modulates iron turnover in rat Sertoli cells. Free Radic Res 2000;33:677–87. doi:10.1080/10715760000301191.
Dal-Pizzol F, Klamt F, Benfato MS, Bernard EA, Moreira JCF. Retinol supplementation induces oxidative stress and modulate antioxidant enzyme activities in rat Sertoli cells. Free Radic Res 2001;34:395–404. doi:10.1080/10715760100300331.
De Oliveira MR, Moreira JCF. Acute and chronic vitamin A supplementation at therapeutic doses induces oxidative stress in submitochondrial particles isolated from cerebral cortex and cerebellum of adult rats. Toxicol Lett 2007;173:145–50. doi:10.1016/j.toxlet.2007.07.002.
De Oliveira MR, Pasquali MAB, Silvestrin RB, Mello e Souza T, Moreira JCF. Vitamin A supplementation induces a prooxidative state in the striatum and impairs locomotory and exploratory activity of adult rats. Brain Res 2007a;1169:112–9. doi:10.1016/j.brainres.2007.07.008.
De Oliveira MR, Silvestrin RB, Mello e Souza T, Moreira JCF. Oxidative stress in the hippocampus, anxiety-like behavior and decreased locomotory and exploratory activity of adult rats: effects of sub acute vitamin A supplementation at therapeutic doses. Neurotoxicology 2007b;28:1191–9. doi:10.1016/j.neuro.2007.07.008.
Draper HH, Hadley M. Malondialdehyde determination as an index of lipid peroxidation. Methods Enzymol 1990;186:421–31. doi:10.1016/0076-6879(90)86135-I.
Duchen MR. Mitochondria and Ca2+ in cell physiology and pathophysiology. Cell Calcium 2000;28:339–48. doi:10.1054/ceca.2000.0170.
Ellis JK, Russell RM, Makrauer FL, Schaefer EJ. Increased risk for vitamin A toxicity in severe hypertriglyceridemia. Ann Intern Med 1986;105:877–9.
Ellman GL. Tissue sulfhydryl groups. Arch Biochem Biophys 1959;82:70–7. doi:10.1016/0003-9861(59)90090-6.
Elsisi AED, Hall P, Sim WLW, Earnest DL, Sipes IG. Characterization of vitamin A potentiation of carbon tetrachloride-induced liver injury. Toxicol Appl Pharmacol 1993a;119:280–8. doi:10.1006/taap.1993.1070.
Elsisi AED, Earnest DL, Sipes IG. Vitamin A potentiation of carbon tetrachloride hepatotoxicity: enhanced lipid peroxidation without enhanced biotransformation. Toxicol Appl Pharmacol 1993b;119:289–94. doi:10.1006/taap.1993.1071.
Fenaux P, Chomienne C, Degos L. Treatment of acute promyelocytic leukaemia. Best Pract Res Clin Haematol 2001;14:153–74. doi:10.1053/beha.2000.0121.
Fisher JC, Ruitenbeek W, Berden JÁ, Trijbels JM, Veerkamp JH, Stadhouders M, Sengers RC, Janssen AJ. Differential investigation of the capacity of succinate oxidation in human skeletal muscle. Clin Chim Acta 1985;153:23–36. doi:10.1016/0009-8981(85)90135-4.
Frota MLC Jr, Klamt F, Dal-Pizzol F, Schiengold M, Moreira JCF. Retinol-induced mdr1 and mdr3 modulation in cultured rat Sertoli cells is attenuated by free radical scavengers. Redox Rep 2004;9:161–5. doi:10.1179/135100004225005192.
Geelen JAG. Hypervitaminosis A induced teratogenesis. CRC Crit Rev Toxicol 1979;6:351–75. doi:10.3109/10408447909043651.
Goodall AH, Fisher D, Lucy JA. Cell fusion, haemolysis and mitochondrial swelling induced by retinol and derivatives. Biochim Biophys Acta 1980;595:9–14. doi:10.1016/0005-2736(80)90242-4.
Halliwell B. Oxidative stress and neurodegeneration: where are we now. J Neurochem 2006;97:1634–58. doi:10.1111/j.1471-4159.2006.03907.x.
Hengartner MO. The biochemistry of apoptosis. Nature 2000;401:770–6. doi:10.1038/35037710.
Hull PR, D’Arcy C. Isotretinoin use and subsequent depression and suicide: presenting the evidence. Am J Clin Dermatol 2003;4:493–505. doi:10.2165/00128071-200304070-00005.
Inder RE, Bray BJ, Sipes IG, Rosengren RJ. Role of cytochrome P4502E1 in retinol’s attenuation of carbon tetrachloride-induced hepatotoxicity in the Swiss Webster mouse. Toxicol Sci 1999;52:130–9. doi:10.1093/toxsci/52.1.130.
Jick SS, Kremers HM, Vasilakis-Scaramozza C. Isotretinoin use and risk of depression, psychotic symptoms, suicide, and attempted suicide. Arch Dermatol 2000;136:1231–6. doi:10.1001/archderm.136.10.1231.
Kagan VE, Borisenko GG, Tyurina YY, Tyurin VA, Jiang J, Potapovich AI, Kini V, Amoscato AA, Fuji Y. Oxidative lipidomics of apoptosis: redox catalytic interactions of cytochrome c with cardiolipina and phosphatidylserine. Free Radic Biol Med 2004;37:1963–85. doi:10.1016/j.freeradbiomed.2004.08.016.
Kim TS, Yun BY, Kim IY. Induction of the mitochondrial permeability transition by selenium compounds mediated by oxidation of the protein thiol groups and generation of the superoxide. Biochem Pharmacol 2003;66:2301–11. doi:10.1016/j.bcp.2003.08.021.
Klamt F, Dal-Pizzol F, Ribeiro NC, Bernard EA, Benfato MS, Moreira JCF. Retinol-induced elevation in ornithine decarboxylase activity in cultured Sertoli cells is attenuated by free radical scavenger and by iron chelator. Mol Cell Biochem 2000;208:71–6. doi:10.1023/A:1007081703928.
Klamt F, de Oliveira MR, Moreira JCF. Retinol induces permeability transition and cytochrome c release from rat liver mitochondria. Biochim Biophys Acta 2005;1726:14–20.
Kowaltowski AJ, Netto LES, Vercesi AE. The thiol-specific antioxidant enzyme prevents mitochondrial permeability transition. Evidence for the participation of reactive oxygen species in this mechanism. J Biol Chem 1998;273:12766–9. doi:10.1074/jbc.273.21.12766.
Lam HS, Chow CM, Poon WT, Lai CK, Chan KCA, Yeung WL, Hui J, Chan AYW, Ng PC. Risk of vitamin A toxicity from candy-like chewable vitamin supplements for children. Pediatrics 2006;118:820–4. doi:10.1542/peds.2006-0167.
Levine RL, Garland D, Oliver CN, Amici A, Climent I, Lenz AG, Ahn BW, Shaltiel S, Stadman ER. Determination of carbonyl content in oxidatively modified proteins. Methods Enzymol 1990;186:464–78. doi:10.1016/0076-6879(90)86141-H.
Lowry OH, Rosebrough AL, Randal RJ. Protein measurement with the folin phenol reagent. J Biol Chem 1951;193:265–75.
Mills JP, Tanumihardjo SA. Vitamin A toxicity in wild-caught African green vervet monkeys (Chlorocebus aethiops) after 2 years in captivity. Comp Med 2006;56:421–5.
Misra HP, Fridovich I. The role of superoxide anion in the autoxidation of epinephrine and a simple assay for superoxide dismutase. J Biol Chem 1972;247:3170–5.
Moreira JCF, Dal-Pizzol F, Von Endt D, Bernard EA. Effect of retinol on chromatin structure in Sertoli cells: 1,10-phenanthroline inhibit the increased DNAse I sensitivity induced by retinol. Med Sci Res 1997;25:635–8.
Myhre AM, Carlsen MH, Bohn SK, Wold HL, Laake P, Blomhoff R. Water-miscible, emulsified, and solid forms of retinol supplements are more toxic than oil-based preparations. Am J Clin Nutr 2003;78:1152–9.
Napoli JL. Biochemical pathways of retinoids transport, metabolism, and signal transduction. Clin Immunol Immunopathol 1996;80:S52–62. doi:10.1006/clin.1996.0142.
Napoli JL. Interactions of retinoids binding proteins and enzymes in retinoids metabolism. Biochim Biophys Acta 1999;1440:139–62.
Norum KR. Acute myeloid leukaemia and retinoids. Eur J Clin Nutr 1993;47:77–87.
Olson J, Gunning D. The storage form of vitamin A in rat liver cells. J Nutr 1983;113:2184–91.
O’Reilly KC, Shumake J, Gonzalez-Lima F, Lane MA, Bailey SJ. Chronic administration of 13-cis-retinoic acid increases depression-related behavior in mice. Neuropsychopharmacology 2006;31:1919–27. doi:10.1038/sj.npp.1300998.
Ott M, Robertson JD, Gogvadze V, Zhivotovsky B, Orrenius S. Cytochrome c release from mitochondria proceeds by a two-step process. Proc Natl Acad Sci U S A 2002;99:1259–63. doi:10.1073/pnas.241655498.
Pfahl M, Piedrafita FJ. Retinoid targets for apoptosis induction. Oncogene 2003;22:9058–62. doi:10.1038/sj.onc.1207109.
Poderoso JJ, Carreras MC, Lisdero C, Riobo N, Schopfer F, Boveris A. Nitric oxide inhibits electron transfer and increases superoxide radical production in rat heart mitochondria and submitochondrial particles. Arch Biochem Biophys 1996;328:85–92. doi:10.1006/abbi.1996.0146.
Rigobello MP, Scutari G, Friso A, Barzon E, Artusi S, Bindoli A. Mitochondrial permeability transition and release of cytochrome c induced by retinoic acids. Biochem Pharmacol 1999;58:665–70. doi:10.1016/S0006-2952(99)00149-5.
Rosengren RJ, Sipes IG. Retinol pretreatment potentiates acetaminophen-induced hepatotoxicity in the male Swiss Webster mouse. Toxicologist 1995;15:219.
Rosengren RJ, Sauer JM, Hooser SB, Sipes IG. The interactions between retinol and five different hepatotoxicants in the Swiss Webster mouse. Fundam Appl Toxicol 1995;25:281–92. doi:10.1006/faat.1995.1064.
Russell RM, Boyer JL, Bagheri SA, Hruban Z. Hepatic injury from chronic vitaminosis A resulting in portal hypertension and ascites. N Engl J Med 1974;291:435–40.
Rustin P, Chretien D, Bourgeron T, Gérard B, Rötig A, Saudubray JM, Munnich A. Biochemical and molecular investigations in respiratory chain deficiencies. Clin Chim Acta 1994;228:35–51. doi:10.1016/0009-8981(94)90055-8.
Shapira AH, Mann VM, Cooper JM, Dexter D, Daniel SE, Jenner P, Clark JB, Marsden CD. Anatomic and disease specificity of NADH CoQ1 reductase (complex I) deficiency in Parkinson’s disease. J Neurochem 1990;55:2142–5. doi:10.1111/j.1471-4159.1990.tb05809.x.
Zamzami N, Kroemer G. The mitochondrion in apoptosis: how Pandora’s box opens. Nat Rev Mol Cell Biol 2001;2:67–71. doi:10.1038/35048073.
Acknowledgments
This work was supported by grants of CNPq, FAPERGS, and PROPESQ-UFRGS. M.R. de Oliveira, M.W.S. Oliveira, R. Lorenzi, and R.F. da Rocha are recipients of CNPq fellowships.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Oliveira, M.R., Oliveira, M.W.S., Lorenzi, R. et al. Short-term vitamin A supplementation at therapeutic doses induces a pro-oxidative state in the hepatic environment and facilitates calcium-ion-induced oxidative stress in rat liver mitochondria independently from permeability transition pore formation. Cell Biol Toxicol 25, 545–560 (2009). https://doi.org/10.1007/s10565-008-9111-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-008-9111-9