Abstract
Tissue bioengineering development is a global concern and different materials are studied and created to be safe, effective and with low cost. Nile Tilapia skin had shown its biological potential as covers for the burn wound. This study evaluates the tilapia skin histological, collagen properties and tensiometric resistance, after treatment by different sterilization methods. Tilapia skin samples were submitted to two sterilization processes: (1) chemical, which consisted in two 2% chlorhexidin baths, followed by sequential baths in increasing glycerol concentrations; and (2) radiation, when glycerolized skin samples were submitted to gamma radiation at 25, 30 and 50 kGy. Microscopic analyzes were performed through Haematoxylin–eosin and Picrosirius Red under polarized light. For tensiometric analysis, traction tests were performed. Glycerol treated skin presented a discrete collagen fibers disorganization within the deep dermis, while irradiated skin did not show any additional change. Throughout the steps of chemical sterilization, there was a higher proportion of collagen with red/yellow birefringence (type I) in the skin samples up to the first bath in chlorhexidin, when compared to samples after the first two glycerol baths (P < 0.005). However, there was no difference in relation to total collagen between groups. In irradiated skin, there was a larger total collagen preservation when using until 30 kGy (P < 0.005). Tensiometric evaluation did not show significant differences in relation to maximum load in the groups studied. We concluded that chemical and radiation (25 and 30 kGy) are efficient methods to sterilize Nile Tilapia skin without altering its microscopic or tensiometric characteristics.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Burn care has evolved over the years through a global endeavour in developing efficient and cost-effective treatment techniques and wound dressings. The main objective of treatment is the removal of the full thickness burn tissue and to close the wound, so avoiding serious septic, metabolic and functional complications, while allowing for tissue repair (Boateng and Catanzano 2015; Lineen and Namias 2008; Inoue et al. 2016).
Several materials have been suggested as biological covers for the burn wound, such as pig pericardium and skin, bovine peritoneal and amniotic membrane and others. Recently, Tilapia skin has also been suggested as a possible biological material due to its collagenous, histological and mechanical similarity to human skin and to other available biomaterials (Norbury et al. 2016; Guo et al. 2016; Mathangi et al. 2013).
Nile Tilapia (Oreochromis niloticus) belongs to the Cichlid family and originates from the Nile basin, in East Africa. It´s presence is now widespread in tropical and subtropical regions of the world. In the State of Ceara, it is abundantly found in fish farms along the Castanhao River which forms one of the main hydrographic basins in this state. Originally, Tilapia skin has been considered a noble commercial product after tanning; its possible usage as a biological dressing material would be of one with practically unlimited availability, low cost and excellent quality (Lineen and Namias 2008; Nunes Alves et al. 2015; Franco et al. 2013).
Another aspect to be considered is the fact that most of the biomaterials available in our country as wound dressings are imported and come at very high cost. To implement a novel biomaterial derived from the Nile Tilapia would produce great technological advancement with significant financial and social impact for the health system.
However, as there could be transmission of pathogens through these xenografts, these biomaterials must be submitted to severe handling (preservation, sterilization) protocols which will then result in safety, efficacy and biocompatibility of the material (Lineen and Namias 2008; Norbury et al. 2016; Kesting et al. 2008; Chiu and Burd 2005; Wasiak et al. 2008).
Glycerol at high concentration (85%) is an attractive option to prepare tissue since, besides its low cost, antiviral and antibacterial effects, it will also produce a less antigenic biological material, with non-viable cells, allowing for conservation in tissue banks for up to 5 years at – 4 °C (Paggiaro et al. 2010).
When considering sterilization options, chlorhexidine has been used in wound coverage procedures due to its activity against gram positive, gram negative and some fungi, as Pseudomonas aeroginosa and Candida albicans, respectively. Several studies present the usage of this topical agent in bone, tendon and amniotic membrane grafting procedures, although these same studies disagree about possible related micro-structural and inductive alterations that it could induce (Ülkür et al. 2005; Acar et al. 2011; Delgado et al. 2014; Versen-Hoeynck et al. 2008; Alomar et al. 2012).
Sterilization by radiation is one of the main methods in tissue engineering. Radiation presents high penetrability, low temperature rise, high efficacy in eliminating microorganisms and may be used in already packaged material. However, depending on the dosage, it may alter tissue architecture through physicochemical changes. It thus becomes important to define the appropriate microorganisms inactivation dosage, while preserving the biological characteristics of the xenograft (Kattz 2010; Conrad et al. 2013; Endres et al. 2009; Nguyen et al. 2013).
In this context, this study´s objective it to analyze Nile Tilapia skin microscopically as well as its tensiometric properties, while determining the its collagen Type I/III ratio after being prepared by different sterilization methods.
Materials and methods
Sample gathering
Nile Tilapia (Oreochromis niloticus) skin samples were obtained from fish farms on Castanhao (Jaguaribara-CE). Fish are raised in net pens and usually sacrificed when around 800 to 1000 grams. They are stunned by thermal shock (isothermal boxes with crushed ice and water [1:1]), and bled immediately after losing consciousness. Skins are removed with tile nippers and washed in running water to remove blood and other residues. For the final cleansing, they were cut in a 10 × 5 cm shape and placed on a 4 °C saline bath.
Chemical sterilization protocol for Nile Tilapia skin
Skin samples were submitted to chemical sterilization consisting of two sequential baths in 2% chlorhexidine for 30 min, followed by sequential baths in 50, 75 and 99% glycerol.
After cleanisng with saline (in natura skin–IN), samples were placed for 30 min in a sterile dish containing 2% chlorhexidine digluconate (tensoactive solution) (C1). After this first bath, skins were again washed with sterile saline and replaced in another sterile dish, with a fresh 2% chlorhexidine solution, where they remained for another 30 min (C2). Sequentially, these skins were washed with sterile saline and placed in another sterile dish containing a solution composed by glycerol (50%), saline (49%) and a penicilin/streptomycin/fungisol solution (1%) (G1). These containers were sealed and sent to the laboratory of Drug Research and Development Center of the Federal University of Ceará (Núcleo de Pesquisa e Desnvolvimento de Medicamentos–NPDM Universidade Federal do Ceará).
Upon or before completion of a 24 h period, these skins were removed from this bath and washed again in sterile saline, and sequentially placed into a solution containing glycerol (75%), saline (24%) and a solution of penicillin/streptomycin/fungisol (1%). They were then massaged individually on a sterile environment for 5 min (vertical laminar flow)(G2) and conditioned in sealed containers. These were then placed en bain marie (water bath) at 37 °C, on a rotation/agitation device at 15 rpm for 3 h. Later, the skins were removed and washed in sterile saline and placed into a solution containing glycerol (99%) and a solution composed by penicilin/streptomycin/fungisol (1%) when they were individually massaged for 5 min (G3) and again placed en bain marie at 37 °C, in the same device (at the same temperature and rotation speed [centrifuge]), for another 3 h. After these baths, the skins where individually placed in double plastic sterile envelopes with two year expiring periods.
Samples were sent for microbiological (bacteria and fungi) and for microscopic evaluation for each of these steps (IN, C1, C2, G1, G2 and G3) for contamination and possible collagen morphological collagen alterations analysis.
Microbiological testing
For each chemical sterilization step, three 1.5 × 1.5 cm samples were obtained, weighted and sent for culture and sensitivity (total of 18 samples). Each sample was imprinted into a Blood-Agar dish for quantitative culture.
Each skin sample was then placed in a sterile Petri dish to which 1 ml of sterile saline was added. The skin sample was then fragmented with a scalpel and mixed with the saline until a turbid solution was obtained. 0.1 ml of this solution was seeded into ASA, MacConkey and CPS (chromogenic medium), spreading it into the entire dish with a inoculation loop. The remaining material of each sample was then inoculated into a test tube containing 3 ml of Brain–Heart-Infusion–BHI
The dishes and the tubes were incubated at 35 °C (± 1) for 24 h. These cultures where then analysed quantitatively and qualitatively yielding microbiologial identification and sensitivity results after this incubation period.
Additional sterilization by radiation
After the above mentioned chemical sterilization process, skins were individually packaged into double plastic envelopes and sent to the Nuclear Energy Research Institute in Sao Paulo (Instituto de Pesquisas Energéticas Nucleares–IPEN) where different samples were irradiated on a Cobalt 60 Multipurpose Irradiator, at 25, 30, and 50 kGy. Irradiation protocol was based on ISO 11,137.
Histological analysis
Samples obtained during all sterilization steps were immersed in 10% buffered formaldehyde. After 24 h, any remaining muscle or adipose tissue was removed and these samples were automatically processed by the Lupe(R) device, being immersed in 58 °C paraffin. They were then cut with a Leica (R) microtome at 4 μm thicknesses and prepared with Haematoxilin-Eosin for analysis on the optical microscope.
Histochemical analysis
Skin samples from each step were submitted for collagen type I and III content analysis. 3 μm Nile Tilapia fragments were placed in glass slides and de-paraffinized at 60 °C for 3 h, followed by 3 five min xylol baths. They were then treated by alcohol sequential rehydration followed by incubation for 30 min in picrosirius red solution (ScyTek(R)) and washed in two fast 5% hydrochloric acid baths. The samples were stained by Harris haematoxilin for 45 s and mounted with Enhtellan(R). A polarized light microsocope (Leica DM 2000) was used to identify the Type I Collagen, tainted red-yellow and the Type III Collagen, tainted green-whitish.
Photomicrographs were taken with a DFC 295 camera coupled to the Leica DM 2000 microscope aiming at quantification the different types of collagen. These Color Treshold (Image > Adjust > Color Threshold) calibrated photomicrographs were analysed by Image J(R) (RSB) image analysing software on the RGB function for Red (71–255), Green (0–69) and Blue (71–92). After calibration, images were converted to an 8-bits color scale, then binarized (Process > Binary > Make Binary) and the red stained collagen area percentage was measured(Analyse > Analyse Particles) (von Versen-Hoeynck et al. 2008; Nunes Alves et al. 2015).
The same protocol was used after light polarization setting the colors in the RGB function to Red (0–255), Green (0–255) and Blue (0–32). After adjusting, the images were converted to an 8 bits color scale (Image > Type > 8-bit) and binarized (Process > Binary > Make Binary) and the yellow-redish collagen stained area percentage was measured (Collagen Type I).
The green whitish area correspondent to Collagen Type III, was measured after subtracting the percentage of the the red-yellowish stained area from the total red stained area.
Tensiometric properties analysis
Traction studies were performed with an Instron(R) 3345 device with a 500 N load cell with wedge mechanical claws. As irradiation was the final step of sterilization, this analysis was performed on irradiated skin comparing to control (non irradiated).
All samples (irradiated and control) were immersed in saline (3 baths, 5 min) and cut into rectangular 10.0 × 2.5 cm fragments. These were equally distributed in control, 25, 30 and 50 kGy groups. They were then cut into an hourglass shape, with a 1 cm wide center. A Mitutoyo® digital caliper was used to measure the thickness of the central part of the hourglass shaped sample during the traction test.
Maximum load (N), deformation to traction (%) and extension under traction (cm) were measured using the Bluehill 2(R) software. All testing was performed with a 5 mm/min dislocation speed.
Statistical analysis
All data was submitted to the Kolmogorov–Smirnov normality test. Collagen content tests were compared by the Student t test (significance level: 5%, parameter data described as: mean ± mean standard error (MSE).
Tensiometric data was analysed by the ANOVA test, followed by Bonferroni post = test (significance level: 5%), (significance level: 5%, parameter data described as: mean ± mean standard error (MSE).
Patenting
A Tilapía Skin patent was filed before the National Institute of Industrial Property (Instituto Nacional da Propriedade Industrial) under protocol number INPI: BR 10 2015 021435 9.
Results
Microbiolgical testing
All six chemical sterilization steps testing showed no growth upon microbiological testing, in the seeding and re-seeding samples.
Histological analysis
Chemical sterilization
Microscopic analysis of all samples throughout the five chemical sterilization steps (C1, C2, G1, G2 and G3) demonstrated horizontally and longitudinally distributed collagen bundles within the dermis. Focal epithelial covering and superficial melanophores were occasionally seen.
There was a discrete difference in the collagen fibers disposition pattern in samples through the Glycerol steps (G1, G2 and G3), which remained organized on the superficial portion and disorganized on the deep portion. However, there was no evidence of fiber disaggregation.
Radiosterilization
Non-irradiated Tilapia skin epidermis presented a small stratified squamous epithelium layer with numerous melanophores. Superficial dermis consisted of organized and thick collagen fibers, in a horizontal disposition. Deep dermis consisted of thick collagen fibers distributed in horizontal and transversal bundles.
Irradiated skin at 25, 30 and 50 kGy presented without epidermis but with melanophores. Superficial dermis consisted of fibrous connective tissue, with compacted, parallel collagen fibers. Deep dermis consisted of thick collagen fibers, distributed in an alternating parallel or transversal fashion. In this location (deep), the collagen fibers were more disorganized in the groups of irradiated skin at 50 kGy.
Histochemical analysis
Chemical sterilization
Collagen with red/yellow birefringence (type I) and green/whitish birefringence (type III) analysis throughout the chemical sterilization steps did not show significant statistical differences in relation to total collagen composition. However, skin samples submitted to the first immersion in chlorhexidine (C1) presented a higher percentage of collagen with red/orange birefringence (type I) and a decreased percentage in collagen green/whitish birefringence (type III). This difference was statistically significant only in relation to the G1 and G2 steps. (P < 0005/2-way ANOVA/Bonferroni) (Figs. 1 and 2).
Percentage Total Collagen and Collagen red/orange birefringence (type I) and green/whitish birefringence (type III) evaluation in Tilapia skin connective tissue submitted to the different chemical sterilization steps. Collagen analysis throughout the chemical sterilization steps did not show significant statistical differences in relation to total collagen composition. However, skin samples submitted to the first immersion in chlorhexidine (C1) presented a higher percentage of collagen with red/orange birefringence (type I) and a decreased percentage in collagen green/whitish birefringence (type III). This difference was statistically significant only in relation to the G1 and G2 steps. (P < 0005/2-way ANOVA/Bonferroni)
Photomicrograph of Collagen profile Tilapia Skin with and without light polarization (Picrosirius Red stain, 400x), demonstrating Collagen birefringence yellow-redish (type I) and Collagen birefringence green-whitish (type III). Picrossirius stain showing total collagen marked in red without polarization of light, and birefringence yellow-redish (type I–Black arrow) and green-whitish (type III- Blue arrow) after polarization. There was a discrete difference in the collagen fibers disposition pattern in samples through the Glycerol steps (G1 and G2), which remained organized on the superficial portion and disorganized on the deep portion (white asterisk). However, there was no evidence of fiber disaggregation. (Color figure online)
Radiosterilization
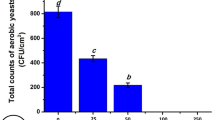
Total collagen analysis demonstrated a higher collagen preservation in samples submitted to 30 kGy when compared to control, with statistical significance (P < 0.001; 2-way ANOVA/Bonferroni). However, when comparing different collagen types, there was no difference in Collagen with red/yellow birefringence (Type I) and Collagen with green/whitish birefringence (Type III) expression within irradiated (25, 30 and 50 kGY) and control groups. All of them showing a larger quantity of Collagen with red/yellow birefringence (Type I) in relation to Collagen with green/whitish birefringence (Type III). Despite of this expression demonstrate more desorganization in the skin irradiated with 50 kGy. (P = 0.258 e P = 0.183, respectively; 2-way ANOVA/Bonferroni) (Fig. 3).
Percentage evaluation of total Collagen area and different birefringence of Collagen Tilapia skin in connective tissue submitted to different radiation dosages. (*P < 0.05/2-way anova/Bonferroni). a Total collagen analysis demonstrated a higher collagen preservation in samples submitted to 30 kGy when compared to control (P < 0.001; 2-way ANOVA/Bonferroni). b, c There was no difference in Collagen with red/orange birefringence (Type I) and Collagen with green/whitish birefringence (Type III) expression within irradiated (25, 30 and 50 kGY) and control groups. All of them showing a larger quantity of Collagen with red/orange birefringence (Type I) in relation to Collagen with green/whitish birefringence (Type III) (P = 0.258 e P = 0.183, respectively; 2-way ANOVA/Bonferroni)
Analysis of tensiometric properties
Rupture to traction in all groups occurred at the central region of the hourglass shaped sample, where thickness ranged from 0.66 to 1.38 mm.
In relation to maximum load, there was no statistical difference between control and samples irradiated at 25, 30 and 50 kGy, with values ranging from 23.473 to 56.455 N (P = 0.052).
However, deformation to maximum load traction showed a variation of 21.592% to 30.358% for samples irradiated at 30 kGy, 21.909 to 27.250% for samples irradiated at 50 kGy, and 32.233 to 37.700% for control. This data showed, with statistical significance (P = 0.004), that irradiated Tilapia skin samples (30 and 50 kGy) present a lesser deformation capacity to traction than the non-irradiated skin. Values obtained with samples irradiated at 25 kGy (26.100 and 33.142%) were not statistically significantly different in relation to control and the other irradiated groups (Fig. 4b).
Radio sterilized Tilapia sking tensiometric properties, presented in Maximun Load (a), Maximun Load Deformation to Traction (b) and Breaking Extension under Traction (c), compared to Control (CTRL), 25, 30 and 50 kGy (P < 0.005/ANOVA/Bonferroni). The maximum load showed no statistical difference between control and samples irradiated at 25, 30 and 50 kGy (P = 0.052). However, irradiated Tilapia skin samples (30 and 50 kGy) present a lesser deformation capacity to traction than the non-irradiated skin (P = 0.004). In addiction, irradieted Tilapia skins at 30 and 50 kGy showed lower extension under traction with statistically significant difference (P = 0.002; ANOVA/Binferroni) when compared to control and samples irradiated at 25 kGy
When considering extension under traction in the different dosages irradiated skin groups, samples irradiated at 30 kGy presented extensions from 2.16 to 3.09 cm and those irradiated at 50 kGy, 2.2 to 2.75 cm. The samples with these dosages presented a statistically significant difference when compared to control (3.32 to 3.83 cm) and samples irradiated at 25 kGy, (2.68 to 3.36 cm) (P = 0.002; ANOVA/Binferroni) (Fig. 4c)
Discussion
Tilapia skin has been shown histologically to be very similar to human skin, present dense fibrous connective tissue layer. As such, it can constitute a possible graft material similar to other xenografts which work as anti-bacterial barrier, reduce wound fluid and protein losses and contribute to ideal conditions for would healing processes to progress satisfactorily (Chiu and Burd 2005).
However, human or animal biological material could become potential pathogenic microorganisms carriers which could result in causing infectious diseases. To reduce this risk to a minimum, these materials must be submitted to rigorous disinfection and sterilization protocols, since a possible bacterial invasion would hinder wound healing since it would perpetuate and augment local inflammatory processes.
Amongst medical, dentistry and institutional use antiseptics, chlorhexidine has been highlighted due to its bactericidal and bacteriostatic actions, low toxicity and substantivity (Mann-Salinas et al. 2015). Also, studies have shown that chlorhexidine concentrations between 0.5 and 2.0% have not been associated with collagen fibriles dissociation in tendon grafts (Allomar et al. 2012). This data corroborates with this current study when sample immersion in 2.0% chlorhexidine did not cause collagen alterations on Tilapia skin analyzed through haematoxilin eosin tainted samples.
However, collagen composition changes were noted in skin samples submitted to 30 min chlorhexidine baths and sequential glycerol concentrations. When compared, skin samples submitted to the 30 min chlorhexidine bath showed better collagen Type I preservation than those who went through the complete glycerol sterilization process. As this particular evaluation is unprescedented in the literature, we did not find any related study. These changes were noticed at the early steps of chemical sterilization when the skin structure remains very similar to the skin in natura.
Literature has shown that glycerolized grafts form an anti-bacterial protective barrier probably due to their close adhesion to the wound resulting of local microcirculation recovery which would allow for increased supply of phagocytes and serum bacteriostatic factors (Maral et al. 1999).
Glycerol dehydrates skin through intracellular fluid removal. This alteration however does not lead to changes in the intracellular ionic concentration, so maintaining its structural integrity. This preserving method has been favorably described in the literature being that cellular characteristics are reconstituted by rehydration with saline (Zidan et al. 2014).
In the present study, Tilapia skin submitted to the glycerol protocol were rehydrated and found to be histologically similar to in natura tilapia skin. There was a discrete disorganisation of deeper collagen fibers but without disaggregation. Some studies in the literature also show this cellular architecture preservation for other grafts (Zidan et al. 2014; Ravishanker et al. 2003).
Despite glycerol acting as a potent fixating tissue agent as well as decreasing viable microorganisms, it is essential to combine this agent with other sterilization methods aiming at complete pathogen elimination (Chiu and Burd 2005). Radiosterilization is the method of choice in this situation since it effective in exterminating bacteria, fungi and viruses due to direct DNA damage (Singh et al. 2016).
Previous studies recommend trials for choosing the appropriate radiosterilization method for complete pathogen removal, while preserving mechanical and inductive material properties (Endres et al. 2009). Previous studies evaluating bone grafts have shown microstructural, biological and mechanical alterations with different radiation dosages (Nguyen et al. 2013; Singh et al. 2016; Burton et al. 2014).
Similarly, studies with allogenic tendon grafts have shown that materials irradiated at dosages ranging from 1.5 to 2.5 Mrads (15 to 25 kGy) have less elasticity and stress resistance when compared to the non irradiated control. This study with Tilapia skin has shown that traction deforming and load traction extension values were significant lower in those samples which received the larger irradiation dosages (30 and 50 kGy). Skin samples submitted to 25 kGy did not differ from non-irradiated samples.
In relation to collagen deposition, it was noted that it was higher in samples submitted to 25 kGy than non-irradiated samples. However, no differences between Collagen Type I and Type III ratios were noted in any of the analyzed groups. Data referring to collagen typification changes before gama irradiation is incospicuous in the literature.
However, previous studies in graft material have shown that although radiation dosages above 25 kGy do not alter collagen cross-linking, this could damage denatured collagen quantity (Ravishanker et al. 2003). Additionally, in a spectroscopy microstructural analysis, it was noted that irradiating skin grafts above 30 kGy would alter hydrogen bonds and collagen amide groups (Shah et al. 2009). These alterations could cause a fiber increase previously to denaturation, similarly to what happens in bone tissue when radiation dosage is 33 kGy or more. So, it could be that the total collagen increase noted when using 30 kGy could be due to the previous increase in the fiber volume, in a process before its denaturation.
Some authors related that bone tissue irradiation at 20 and 25 kGy dosages is sufficient to eliminate S. Epidermis and B. pulimilis, known to be resitant to gama radiation. It has also been described that these dosages would be safe without causing mechanical properties alterations in this material (Nguyen et al.2013).
Singh et al. (2016) and ISO 11137:2006 (Baker et al. 2005) recommend a dosage of 25 kGy for future use of the material as graft. In this study, this dosage did not alter the mechanical nor the histological properties of the tilapia skin.
Conclusion
Chemical sterilization as well as radiosterilization at the dosages of 25 kGy and 30 kGy are effective in preparing Nile Tilapia skin for usage as a biological dressing, and these methods do not alter their microscopical nor their tensiometric properties.
References
Acar A, Uygur F, Diktaş H et al (2011) Comparison of silver-coated dressing (Acticoat®), chlorhexidine acetate 0.5% (Bactigrass®) and nystatin for topical antifungal effect in Candida albicans-contaminated, full-skin-thickness rat burn wounds. Burns 37(5):881–884. https://doi.org/10.1016/j.burns.2011.01.024
Alomar ZA, Gawri R, Roughley PJ, Haglund L, Burman M (2012) The effects of chlorhexidine graft decontamination on tendon graft. Am J Sports Med 40(7):1646–1653. https://doi.org/10.1177/0363546512443808
Baker TF, Ronholdt CJ, Bogdansky S (2005) Validating a low dose gamma irradiation process for sterilizing allografts using ISO 11137 Method 2B. Cell Tissue Bank 6(4):271–275. https://doi.org/10.1007/s10561-005-7364-6
Boateng J, Catanzano O (2015) Advanced therapeutic dressings for effective wound healing - a review. J Pharm Sci 104(11):3653–3680. https://doi.org/10.1002/jps.24610
Burton B, Gaspar A, Josey D, Tupy J, Grynpas MD, Willett TL (2014) Bone embrittlement and collagen modi fi cations due to high-dose gamma-irradiation sterilization. Bone 61:71–81. https://doi.org/10.1016/j.bone.2014.01.006
Chiu T, Burd A (2005) “Xenograft” dressing in the treatment of burns. Clin Dermatol 23(4):419–423. https://doi.org/10.1016/j.clindermatol.2004.07.027
Conrad BP, Rappé M, Horodyski M, Farmer KW, Indelicato PA (2013) The effect of sterilization on mechanical properties of soft tissue allografts. Cell Tissue Bank 14(3):359–366. https://doi.org/10.1007/s10561-012-9340-2
Delgado LM, Pandit A, Zeugolis DI (2014) Influence of sterilisation methods on collagen-based devices stability and properties. Expert Rev Med Devices 11(3):305–314. https://doi.org/10.1586/17434440.2014.900436
Endres S, Kratz M (2009) Gamma irradiation. An effective procedure for bone banks, but does it make sense from an osteobiological perspective? J Musculoskelet Neuronal Interact 9(1):25–31
Franco MLRS, Franco NP, Gasparino E, Dorado DM, Prado M, Vesco APD (2013) Comparação das peles de tilápia do Nilo, PACU e Tambaqui: histologia, composição e resistência. Arch Zootec 62(237):21–32
Guo Z-Q, Qiu L, Gao Y et al (2016) Use of porcine acellular dermal matrix following early dermabrasion reduces length of stay in extensive deep dermal burns. Burns. https://doi.org/10.1016/j.burns.2015.10.018
Inoue Y, Hasegawa M, Maekawa T et al (2016) The wound/burn guidelines–1: wounds in general. J Dermatol. https://doi.org/10.1111/1346-8138.13276
Kattz J (2010) The effects of various cleaning and sterilization processes on allograft bone incorporation. J Long Term Eff Med Implants. 20(4):271–276. http://www.ncbi.nlm.nih.gov/pubmed/21488820. Accessed 18 Feb 2017
Kesting MR, Wolff K-D, Hohlweg-Majert B, Steinstraesser L (2008) The role of allogenic amniotic membrane in burn treatment. J Burn Care Res 29(6):907–916. https://doi.org/10.1097/BCR.0b013e31818b9e40
Lineen E, Namias N (2008) Biologic dressing in burns. J Craniofac Surg 19(4):923–928. https://doi.org/10.1097/SCS.0b013e318175b5ab
Mann-Salinas EA, Joyner DD, Guymon CH et al (2015) Comparison of Decontamination Methods for Human Skin Grafts. J Burn Care Res 36(6):636–640. https://doi.org/10.1097/BCR.0000000000000188
Maral T, Borman H, Arslan H, Demirhan B (1999) Efectiveness of human amnion preserved long-term in glycerol as a temporary biological dressing. Burns 25(7):625–635
Mathangi Ramakrishnan K, Babu M, Mathivanan Jayaraman V, Shankar J (2013) Advantages of collagen based biological dressings in the management of superficial and superficial partial thickness burns in children. Ann Burns Fire Disasters 26(2):98–104
Nguyen H, Cassady AI, Bennett MB et al (2013) Reducing the radiation sterilization dose improves mechanical and biological quality while retaining sterility assurance levels of bone allografts. Bone 57(1):194–200. https://doi.org/10.1016/j.bone.2013.07.036
Norbury W, Herndon DN, Tanksley J, Jeschke MG, Finnerty CC (2016) Infection in Burns. Surg Infect (Larchmt) 17(2):250–255. https://doi.org/10.1089/sur.2013.134
Nunes Alves APN, Lima Verde MEQ, Ferreira Júnior AEC et al (2015) Avaliação microscópica, estudo histoquímico e análise de propriedades tensiométricas da pele de tilápia do Nilo. Rev Bras Queimaduras 14(3):203–210
Paggiaro AO, Mathor MB, de Carvalho VF (2010) Estabelecimento de protocolo de glicerolização de membranas amnióticas para uso como curativo biológico. Rev Bras Queimaduras 9(4):2–6
Ravishanker R, Bath AS, Roy R (2003) “Amnion Bank”–The use of long term glycerol preserved amniotic membranes in the management of superficial and superficial partial thickness burns. Burns 29(4):369–374. https://doi.org/10.1016/S0305-4179(02)00304-2
Shah NB, Wolkers WF et al (2009) Fourier transform infrared spectroscopy investigation of native tissue matrix modifications using a gamma irradiation process. Tissue Eng Part C Methods 15(1):33–40. https://doi.org/10.1089/ten.tec.2008.0158
Singh R, Singh D, Singh A (2016) Radiation sterelization of tissue allografts: a review. World J Radiol 8(4):355–370. https://doi.org/10.4329/wjr.v8.i4.355
Ülkür E, Öncül O, Karagöz H, Çeliköz B, Çavuslu S (2005) Comparison of silver-coated dressing (acticoat), chlorhexidine acetate 0.5% (bactigrass), and silver sulfadiazine 1% (silverdin) for topical antibacterial effect in pseudomonas aeruginosa-contaminated, full-skin thickness burn wounds in rats. J Burn Care Rehabil 26(5):430–433. https://doi.org/10.1097/01.bcr.0000176879.27535.09
von Versen-Hoeynck F, Per A, Becker J (2008) Sterilization and preservation influence the biophysical properties of human amnion grafts. Biologicals 36(4):248–255. https://doi.org/10.1016/j.biologicals.2008.02.001
Wasiak J, Cleland H, Campbell F (2008) Dressings for treating superficial and partial thickness burns. Cochrane Database Syst Rev 8(4):CD002106. https://doi.org/10.1002/14651858.CD002106.pub3
Zidan SM, Eleowa SA (2014) Banking and use of glycerol preserved full-thickness skin allograft harvested from body contouring procedures. Burns 40(4):641–647. https://doi.org/10.1016/j.burns.2013.08.039
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alves, A.P.N.N., Lima Júnior, E.M., Piccolo, N.S. et al. Study of tensiometric properties, microbiological and collagen content in nile tilapia skin submitted to different sterilization methods. Cell Tissue Bank 19, 373–382 (2018). https://doi.org/10.1007/s10561-017-9681-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10561-017-9681-y