Abstract
The majority of deaths from carcinoma are caused by secondary growths that result from tumour invasion and metastasis. The importance of epithelial-to-mesenchymal transition (EMT) as a driver of invasion and metastasis is increasingly recognised, and recent evidence has highlighted a link between EMT and the cancer stem cells that initiate and maintain tumours and have also been implicated in invasion and metastasis. Here, we review cancer stem cells and their link with EMT, and explore the importance of this link in metastasis and therapeutic resistance of tumours. We also discuss new evidence from our laboratory demonstrating that cancer stem cells display a remarkable phenotypic plasticity that enables them to switch between an epithelial phenotype that drives tumour growth and an EMT phenotype that drives metastasis. As successful therapies must eradicate cancer stem cells in all their guises, the identification of sub-types of cancer stem cells that display therapeutic resistance and phenotypic plasticity has important implications for the future design of therapeutic strategies. The ability to assay the responses of different cancer stem cell phenotypes in vitro holds promise for the rapid development of a new generation of targeted therapies that fulfil this objective.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction—adult stem cells and cancer stem cells
The discovery of a population of breast cancer stem cells that have undergone epithelial-to-mesenchymal transition (EMT) [1] has opened up an exciting new front in the study of cancer stem cells. It had previously been proposed that cancer stem cells in carcinomas undergo an EMT to gain a migratory, mesenchymal phenotype that enables them to migrate out from the primary tumour to colonize distant sites, where they then undergo mesenchymal-to-epithelial transition (MET) to establish a metastatic tumour of the same epithelial character as the parent tumour [2]. Evidence is now accumulating in support of this hypothesis [3, 4]. As well as being implicated in metastasis, cancer stem cells that have undergone EMT exhibit therapeutic resistance [5] and may therefore also form a reservoir of surviving cells that is responsible for tumour recurrence after apparently successful initial therapy. For these reasons, cancer stem cells that have undergone EMT (EMT cancer stem cells) are now an important focus for research aimed at preventing tumour metastasis and recurrence [6].
The key attributes of cancer stem cells, and indeed any stem cell, are self-renewal and the ability to give rise to more differentiated cell types [7]. For the vast majority of tumours, the cancer stem cells lack the pluripotency that is a characteristic of embryonic stem cells, being generally limited to the lineage(s) of the tissue from which they arose [8]. In this regard, cancer stem cells are more similar to the adult stem cells that drive tissue regeneration and repair throughout adult life [9] (Fig. 1). Adult tissue stem cells have been identified in many organs, including skin (basal) [10], muscle (satellite cells) [11] and breast (in the myoepithelial compartment) [12]. They are characterised by two key attributes; self-renewal and the ability to reconstitute all of the lineages that make up the tissue of origin. In this latter regard, adult stem cells from all but the simplest tissues might be regarded as multipotent (as opposed to the pluripotency of embryonic stem cells), in that they possess a limited degree of developmental plasticity that enables differentiation into each of the required lineages. For example, breast tissue comprises two distinct cell lineages; the luminal cells that form the alveoli and are responsible for milk production, and the myoepithelial cells that line the branching ductal structures. Normal breast stem cells (CD44highCD24low) reside in the myoepithelial compartment, but can differentiate into both luminal and myoepithelial lineages [12]. Breast cancer stem cells also display a CD44highCD24low marker profile and are also multipotent, being able to differentiate into both epithelial and mesenchymal lineages [1, 13].
Types of stem cell. Pluripotent embryonic stem cells self-renew and can produce every single adult cell type. They express embryonic stem cell markers. Adult stem cells also self-renew, but their differentiation potential is restricted to the lineage(s) that make up the tissue in which they reside. They are characterised by various markers, such as CD44 in squamous epithelial and breast tissue. Cancer stem cells have the characteristics of adult stem cells, and often share the same markers. Tumour cells often display the range of lineages and patterns of differentiation that characterise the tissue of origin
The concept of cancer stem cells has been discussed for many years, but the first firm evidence came in 1997 when it was demonstrated that the ability to initiate tumour growth upon transplantation into NOD/SCID mice was limited to a CD34+/CD38− subpopulation of leukaemic cells [14]. Subsequently, cancer stem cells have also been identified using various markers in brain tumours (CD133+) [15], breast cancer (CD44highCD24lowESA+) [16], oral squamous cell carcinoma (CD44high) [17, 18], pancreatic cancer (CD44+CD24+ESA+) [19], prostate cancer (CD44+) [20] and other carcinomas. In breast cancer and oral squamous cell carcinoma, cancer stem cells have also been identified by high activity of the detoxifying enzyme ALDH1 [21, 22]. In addition to their ability to drive tumour growth, cancer stem cells have also been implicated in therapeutic resistance of tumours [5, 23, 24]. This therapeutic resistance presents considerable challenges for cancer therapy, as cancer stem cells that survive chemo or radiotherapy have the ability to regrow the whole tumour [25]. Cancer stem cells have also been implicated in tumour invasion and metastasis [26, 27], suggesting that surgical intervention may often come too late to enable successful excision of the cancer stem cell population. Therefore, new therapeutic regimens that target cancer stem cells are required.
2 Cancer stem cells and EMT
EMT is the process by which epithelial cells detach from the epithelial sheet and acquire a motile mesenchymal phenotype. This is important for formation of the mesoderm during gastrulation, which involves individual cells acquiring a mesenchymal (mesodermal) phenotype and migrating from the ectoderm to the centre of the embryo [28]. EMT is also important for wound healing, where stromal signals trigger the surrounding epithelial cells to undergo EMT and migrate into the wound site [29]. Upon wounding, the epithelial cells at the edge of the wound are immediately exposed to a variety of EMT-inducing stromal signalling factors that they were previously isolated from. These include PDGF from platelets, FGF from fibroblasts and transforming growth factor beta (TGF-β) and tumour necrosis factor-alpha (TNF-α) from immune cells [30]. Tissue inflammation associated with wounding facilitates recruitment of EMT-inducing immune cells to the wound site [31]. The third occasion where EMT occurs is in cancer, where it drives migration of tumour cells from the primary site and formation of metastases [32, 33]. Cancer cells that have undergone EMT exhibit therapeutic resistance [5, 34, 35], including resistance to EGFR inhibitors [36], and evade the host immune response to the tumour [33, 37]. EMT is therefore an important process in tumour progression. The tumour cells undergoing EMT appear to borrow heavily from the EMT mechanisms involved in wound healing, including response to the same signals and promotion by the inflammatory tumour environment [30, 31]. Oncogenic changes in cancer cells, including mutations in receptor tyrosine kinase or Wnt signalling pathways, render them especially responsive to EMT-inducing signals originating in the tumour stroma [38]. The tumour environment is often viewed as a “wound that never heals”, with a chronic inflammatory environment that continually drives EMT of cancer cells at the tumour–stroma interface [39, 40]. The induction of EMT is mediated by key transcription factors within the cell, including Slug, Snail and Twist. These are activated in response to the aforementioned signalling pathways, and orchestrate intracellular changes including upregulating expression of vimentin, downregulating expression of E-cadherin and nuclear import of β-catenin (normally kept at the plasma membrane by E-cadherin in epithelial cells) [41]. The transcription factor Zeb1, which represses the EMT-inhibiting miR-200 family of microRNAs, is also an important inducer of EMT [42].
As detailed above, it is clear that the process of EMT plays an important role in tumour invasion and metastasis, and may also be responsible for the ability of tumours to evade and subvert the body's immune response. Cells that have undergone EMT are also resistant to many of the chemotherapeutic and adjuvant drugs that are used to treat epithelial tumours, and may therefore form a reservoir of cells that survive the initial treatment and drive tumour recurrence. This chemotherapeutic resistance is also a feature of cancer stem cells, and the discovery of a population of CD44highCD24low breast cancer stem cells that have undergone EMT has now united these two phenomena [1]. The technology of flow cytometric cell sorting (FACS), which revolutionised the study of cancer stem cells by enabling heterogeneous cell populations to be separated based on expression of protein markers and analysed separately, is now increasingly important to the study of EMT. Until recently, many studies of EMT have treated tumours as a homogenous population of cells that were assumed to be identical in their behaviour and underlying molecular mechanisms. The cellular and molecular heterogeneity present in most tumours required a change in approach, and FACS sorting is now used as a basis for study of the EMT features of cancer cells, and how these features relate to the issue of stemness. Using this approach, we have recently identified a population of cancer stem cells that have undergone EMT in squamous cell carcinoma, where they are CD44highESAlow [3].
3 Plasticity of the cancer stem cell phenotype
It is not yet clear whether EMT is restricted to the processes of embryogenesis, wound healing and tumourigenesis, or whether adult stem cells also display attributes of EMT in their normal state. CD24highCD24low cells from normal mammary tissue express EMT markers [1], a possible link between stemness and EMT in normal tissue. However, mammary stem cells reside in the myoepithelial part of the tissue, and unipotent non-stem myoepithelial cells share the CD24highESAlow phenotype exhibited by the stem cells [12] and might also express genes related to EMT. Therefore, there is still a question over whether there is a meaningful link between EMT and stemness in normal breast tissue. Stem cells in other tissues do not necessarily express an EMT phenotype; the self-renewing stem cells in skin display a distinctly epithelial phenotype and form tightly bound epithelial colonies known as holoclones in culture [43]. There is evidence that these holoclone-forming stem cells also exist in epithelial tumours [3, 17, 44, 45], suggesting that stem cells having undergone EMT are not always the necessary drivers of epithelial tumourigenesis. Nevertheless, it is clear that at least a portion of the cancer stem cells in many tumour types have undergone EMT. Our recent evidence suggests that cancer stem cells can undergo both EMT and the reverse process of MET to switch between EMT and epithelial phenotypes [3], and this plasticity of the cancer stem cell phenotype supports a model whereby cancer stem cells in carcinomas undergo an EMT that enables them to migrate out from the primary tumour and colonize distant sites, where they then undergo MET to enable growth of a metastatic tumour of the same epithelial character as the parent tumour [2] (Fig. 2).
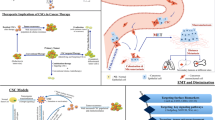
Metastasis of cancer stem cells. A model of the processes that occur during metastatic dissemination from a primary tumour, based on our results in squamous cell carcinoma [3]. Cancer stem cells undergo EMT in the primary tumour, and the resulting motile cancer stem cells invade through the stroma to reach the circulatory and lymphatic systems through which they travel to distant sites. At these secondary sites, they undergo MET to resume their proliferative phenotype and produce a metastatic growth. Differentiated epithelial cells contribute to tumour bulk, whereas the role of the newly-discovered differentiated EMT cells is currently unknown. It is possible that they may contribute to the tumour stroma, which signals to promote EMT and invasion at the tumour edge. It is not yet known what signals drive MET at the metastatic site. Marker expression for the different tumour cell types in squamous cell carcinoma is shown in the key
4 Different differentiation states within the population of cancer cells that have undergone EMT
An important question is whether all cancer cells exhibiting EMT characteristics are cancer stem cells, or are some actually more differentiated? This question is particularly important in consideration of the ability to undergo the reverse process of MET required to seed a new epithelial tumour, as it would be expected that more differentiated cells would lose the requisite lineage plasticity. Work using normal breast tissue [46] has shown that, as well as containing the bipotent breast stem cells, the myoepithelial population also contains cells that are committed to a myoepithelial lineage, which as discussed earlier is likely to share features of EMT. In squamous cell carcinoma, it has been demonstrated that some cells having undergone EMT can reverse this process through MET, but this ability is not shared by all EMT cancer cells. Further, the EMT cells that are capable of undergoing MET can be isolated from more differentiated EMT cells in FACS by their ESAlow/+ALDH1+ expression pattern [3]. The population of cancer cells that have undergone EMT and become fixed in the mesenchymal lineage, such that they can no longer return to the epithelial phenotype, represent a more differentiated EMT phenotype. What role, if any, these cells play in tumour progression is unknown. It is possible that they may make an important contribution to the tumour stroma. The ability to differentiate between these two different classes of EMT cell is likely to be an important consideration, both to ensure that the correct cells are being characterised in cancer stem cell research and for any efforts at diagnosis based on the prevalence of EMT cancer stem cells.
5 EMT, MET and metastasis of cancer stem cells
One area of controversy is whether it is necessary for cancer stem cells to undergo EMT in order to seed metastases. In in vitro models, EMT cancer stem cells are much more invasive than their epithelial counterparts [3, 47]. The special ability to survive and grow in attachment-free conditions, which some studies suggest is unique to the EMT cancer stem cells [1, 48], is also likely to be of benefit to a cancer cell that has to survive in situations far removed from their parent tumour and surrounding stroma. In addition, evidence from in vivo experiments also suggests a crucial role for EMT cancer stem cells in metastasis [3, 32]. There are, however, some alternative models of metastasis that do not require a role for EMT cancer stem cells. The first is that stromal fibroblasts, or possibly cancer cells that have undergone an irreversible EMT, drag non-EMT cancer stem cells out of the tumour and into the circulatory and lymphatic systems, from where they travel around the body and seed new tumours [49]. Alternatively, recent evidence suggests that non-EMT breast cancer cells can collectively invade into the lymphatic system, but not the blood system, without the aid of cells that have undergone EMT [50]. Despite questions remaining over whether EMT is absolutely essential for metastasis, it is clear that it plays a very important role.
Another question concerns the role of MET in formation of metastases. Clearly, if metastasising cells have undergone EMT, then subsequent MET would be required for formation of a metastasis with the same epithelial characteristics as the original tumour. Therefore, the fact that most metastatic tumours mirror the phenotype of their primary counterpart [2] suggests a role for MET in their formation. Why are EMT cancer stem cells unable to form metastatic tumours directly, without recourse to the epithelial phenotype? It is possible that this happens in some cases, and indeed it may explain the highly mesenchymal nature of some metastatic tumours [51]. However, it has been observed that the EMT cancer stem cells in squamous cell carcinoma grow very slowly [3]. Therefore, the reemergence of non-EMT cancer stem cells may be required simply to enable the heightened rates of proliferation required to drive tumour growth. It has been shown that selection through multiple rounds of metastasis forms cell lines with a more epithelial character, and that these lines seed more bone metastases when injected intracardiacally or intratibially (but, crucially, not orthotopically) in a mouse model [4]. More recently, it has been demonstrated that the Mir-200 family of microRNAs promotes MET, decreased ability to escape from primary tumours and increased ability to colonize metastatic sites in breast cancer cell lines [52]. Thus, the evidence points to a requirement for EMT in the early stages and MET in the later stages of metastasis. There is as yet little information on what signals drive MET in cancer, although the fibroblast growth factor receptor-2 FGFR2IIIc has been implicated [4]. Two effects of the Mir-200 family also drive MET in cancer—downregulation of the secretome with consequent reduction of the secreted proteins Igfbp4 and Tinagl1 [52], and direct targeting of the E-cadherin repressors Zeb1 and Zeb2 [53].
6 Promotion of EMT by the tumour stroma
It has become increasingly evident that the stromal tissue surrounding a tumour plays an important role in enabling and sustaining tumour development [54]. Recent work has demonstrated that TGF-β produced by tumour cells induces the conversion of fibroblasts into myofibroblasts known as carcinoma-associated fibroblasts, and that these cells then maintain themselves in this state through autocrine TGF-β signalling and greatly promote tumour development [55]. Promotion of tumour development by these cells may be at least partly through TGF-β signalling back to the tumour that aids production of EMT cancer stem cells. Indeed, it is known that TGF-β signalling induces production of EMT cancer stem cells in tumour cell lines [3]. Nuclear β-catenin, a marker of EMT, is restricted to those tumour cells that are at the tumour–stroma interface in colorectal cancer [2], further indicating a role for the tumour stroma in the production of EMT cancer stem cells. The fact that TGF-β signalling appears to work in both directions, from tumour to stroma and vice versa, suggests a positive feedback loop that results in continuous EMT at the tumour–stroma interface as the “wound that never heals” model described earlier would predict. This would be particularly so if, as seems possible, the EMT cancer stem cells produce greater amounts of TGF-β than the non-EMT cancer cells, thus reinforcing the feedback loop. The questions of which cancer cells signal most strongly to the stroma, and whether the process is initiated by stromal signalling to the tumour or vice versa, are currently unanswered. In addition, the recent demonstration that some cancer cells undergo an irreversible EMT [3] suggests that the tumour may actually be able to create its own stroma that signals back to the tumour to promote EMT and tumour development. In addition to TGF-β, the inflammatory stromal microenvironment in which the tumour resides also produces TNF-α, IL-6 and other inflammatory mediators. These signals also induce EMT in tumour cells and further enhance inflammation, and crosstalk between the different signalling molecules including TGF-β sustains and upregulates their production [56].
7 Cancer stem cells and therapeutic resistance
A big problem for cancer therapy is the occurrence of resistance in tumours, and this therapeutic resistance has been attributed to cancer stem cells [23]. Typically, initially successful treatment kills the bulk of the tumour but leaves the cancer stem cells still alive, and these then drive tumour regrowth and disease relapse. This often results in a more aggressive tumour, possibly due to a higher content of cancer stem cells. It has been demonstrated that EMT cancer stem cells exhibit resistance to common chemotherapy drugs [5], and breast cancer cells remaining after conventional therapy display both features of EMT and the CD44highCD24−/low signature of breast cancer stem cells [57]. Other work demonstrates therapeutic resistance of the holoclone-forming, epithelial-phenotype cancer stem cells in squamous cell carcinoma [58]. At present, the mechanism governing resistance of cancer stem cells to therapy is unclear. Drug efflux transporters of the ABC family have been implicated in therapeutic resistance as they pump drugs out of the cell, with ABCC2 and ABCB1 being associated with resistance to cisplatin and paclitaxel, respectively [59, 60]. Recent studies have uncovered a link between the Oct4 transcription factor, PI3K/Akt and ABCG2-mediated resistance of cancer stem cells to cisplatin in hepatocellular carcinoma [61] and oral squamous cell carcinoma [62], and ABCB5 has been implicated in the resistance of cancer stem cells to doxorubicin in hepatocellular carcinoma [63] and melanoma [64]. Therefore, the ABC family of transporters appears to be heavily involved in the mechanism of cancer stem cell therapeutic resistance. Undoubtedly, the key molecular drivers of cancer stem cell therapeutic resistance remain to be uncovered, but will hopefully in the future provide molecular targets through which cancer stem cell resistance may be abrogated, thus enabling their eradication. The antibiotic salinomycin has already been demonstrated to specifically kill EMT cancer stem cells in breast cancer cell lines [5], although the mechanism for this is not yet known.
8 The role of EMT in enabling cancer stem cells to evade the immune response
Another feature of cancer stem cells is their ability to evade the immune response to the tumour, and actively suppress the T cell response [65]. In melanoma, this feature has been linked to cancer stem cells that exhibit features of EMT [66]. A direct link between EMT and immune evasion has been demonstrated through the knockdown of Axl, a receptor tyrosine kinase that is required for EMT [33]. When injected into normal BALB/c mice, with a functioning immune system, control breast cancer cells formed tumours that were initially subjected to a vigorous immune response that caused tumour regression, but then regrew and metastasised. Axl-knockdown breast cancer cells (depleted of EMT cancer stem cells) initially behaved in the same manner, but were not able to overcome the immune response and regrow. Thus, it seems that EMT cancer stem cells survive the initial immune response to the tumour, then drive regrowth of a tumour that is no longer subject to an effective immune response. This feature of EMT cancer stem cells is of particular significance to mouse models used to assess the presence of cancer stem cells, as any model that retains an immune system may present a more favourable environment for growth of EMT cancer stem cells than epithelial-phenotype cancer stem cells that are less able to evade the immune response. Therefore, new mouse models with more complete immune compromisation will be important for accurate assessment of cancer stem cell properties. For example, using the new NOD/SCID Il2rg −/− mouse model, the proportion of tumour initiating cells in melanoma increases to 1 in 4 compared to 1 in 111,000 when transplanted into standard NOD/SCID mice [67], demonstrating that the use of more immunocompromised mice enables a far greater proportion of cancer stem cells to display tumour-initiating ability.
9 Diagnostic potential of cancer stem cells
The presence of cancer cells in the circulation has been investigated as a possible indicator of metastasis, but looking specifically for circulating cancer stem cells or EMT cancer stem cells in the primary tumour may give a better indication as these are the cells that will drive the formation of secondary tumours. Expression of CD26, a marker of EMT cancer stem cells in primary colorectal cancer, is a predictor of subsequent metastasis [68], and the EMT marker smooth muscle actin is a strong prognostic marker for poor outcome in oral squamous cell carcinoma [69]. It is hoped that assaying for cancer stem cell features will give a better indication of the likely disease course, including the likelihood of metastasis, and thus enable more tailored therapeutic management.
10 Conclusion—important implications for therapeutic strategies
EMT enables metastasis, evasion of the immune response,and tumour recurrence after chemotherapy (due to resistance of the EMT cancer stem cells) and surgery (due to motility of the EMT cancer stem cells). The self-renewal endowed on these cells by their stemness is key to their ability to drive new tumour growth, and underlines the central importance of understanding how cancer stem cells are controlled and sustained in order that future therapies might successfully target both the non-EMT cancer stem cells that drive tumour growth and the EMT cancer stem cells that drive tumour metastasis and recurrence. It is hoped that the recent development of sophisticated in vitro cancer stem cell assays [3] will greatly facilitate both mechanistic studies and efforts at high throughput drug screening, and thus drive rapid progress in the development of cancer stem cell therapies.
References
Mani, S. A., Guo, W., Liao, M. J., Eaton, E. N., Ayyanan, A., Zhou, A. Y., et al. (2008). The epithelial-mesenchymal transition generates cells with properties of stem cells. Cell, 133(4), 704–715. doi:10.1016/j.cell.2008.03.027.
Brabletz, T., Jung, A., Spaderna, S., Hlubek, F., & Kirchner, T. (2005). Opinion: Migrating cancer stem cells—An integrated concept of malignant tumour progression. Nature Reviews. Cancer, 5(9), 744–749. doi:10.1038/nrc1694.
Biddle, A., Liang, X., Gammon, L., Fazil, B., Harper, L. J., Emich, H., et al. (2011). Cancer stem cells in squamous cell carcinoma switch between two distinct phenotypes that are preferentially migratory or proliferative. Cancer Research. doi:10.1158/0008-5472.CAN-11-1059.
Chaffer, C. L., Brennan, J. P., Slavin, J. L., Blick, T., Thompson, E. W., & Williams, E. D. (2006). Mesenchymal-to-epithelial transition facilitates bladder cancer metastasis: Role of fibroblast growth factor receptor-2. Cancer Research, 66(23), 11271–11278. doi:10.1158/0008-5472.CAN-06-2044.
Gupta, P. B., Onder, T. T., Jiang, G., Tao, K., Kuperwasser, C., Weinberg, R. A., et al. (2009). Identification of selective inhibitors of cancer stem cells by high-throughput screening. Cell, 138(4), 645–659. doi:10.1016/j.cell.2009.06.034.
Wang, Z., Li, Y., Ahmad, A., Azmi, A. S., Kong, D., Banerjee, S., et al. (2010). Targeting miRNAs involved in cancer stem cell and EMT regulation: An emerging concept in overcoming drug resistance. Drug Resistance Updates, 13(4–5), 109–118. doi:10.1016/j.drup.2010.07.001.
Clarke, M. F., Dick, J. E., Dirks, P. B., Eaves, C. J., Jamieson, C. H., Jones, D. L., et al. (2006). Cancer stem cells–perspectives on current status and future directions: AACR Workshop on cancer stem cells. Cancer Research, 66(19), 9339–9344. doi:10.1158/0008-5472.CAN-06-3126.
Gu, G., Yuan, J., Wills, M., & Kasper, S. (2007). Prostate cancer cells with stem cell characteristics reconstitute the original human tumor in vivo. Cancer Research, 67(10), 4807–4815. doi:10.1158/0008-5472.CAN-06-4608.
Mackenzie, I. C. (2008). Cancer stem cells. Annals of Oncology, 19(Suppl 5), v40–v43. doi:10.1093/annonc/mdn306.
Mackenzie, I. C. (2006). Stem cell properties and epithelial malignancies. European Journal of Cancer, 42(9), 1204–1212. doi:10.1016/j.ejca.2006.01.041.
Morgan, J. E., & Partridge, T. A. (2003). Muscle satellite cells. The International Journal of Biochemistry & Cell Biology, 35(8), 1151–1156.
Stingl, J. (2009). Detection and analysis of mammary gland stem cells. The Journal of Pathology, 217(2), 229–241. doi:10.1002/path.2457.
Battula, V. L., Evans, K. W., Hollier, B. G., Shi, Y., Marini, F. C., Ayyanan, A., et al. (2010). Epithelial-mesenchymal transition-derived cells exhibit multilineage differentiation potential similar to mesenchymal stem cells. Stem Cells, 28(8), 1435–1445. doi:10.1002/stem.467.
Bonnet, D., & Dick, J. E. (1997). Human acute myeloid leukemia is organized as a hierarchy that originates from a primitive hematopoietic cell. Nature Medicine, 3(7), 730–737.
Singh, S. K., Clarke, I. D., Terasaki, M., Bonn, V. E., Hawkins, C., Squire, J., et al. (2003). Identification of a cancer stem cell in human brain tumors. Cancer Research, 63(18), 5821–5828.
Al-Hajj, M., Wicha, M. S., Benito-Hernandez, A., Morrison, S. J., & Clarke, M. F. (2003). Prospective identification of tumorigenic breast cancer cells. Proceedings of the National Academy of Sciences of the United States of America, 100(7), 3983–3988. doi:10.1073/pnas.0530291100.
Locke, M., Heywood, M., Fawell, S., & Mackenzie, I. C. (2005). Retention of intrinsic stem cell hierarchies in carcinoma-derived cell lines. Cancer Research, 65(19), 8944–8950. doi:10.1158/0008-5472.CAN-05-0931.
Prince, M. E., Sivanandan, R., Kaczorowski, A., Wolf, G. T., Kaplan, M. J., Dalerba, P., et al. (2007). Identification of a subpopulation of cells with cancer stem cell properties in head and neck squamous cell carcinoma. Proceedings of the National Academy of Sciences of the United States of America, 104(3), 973–978. doi:10.1073/pnas.0610117104.
Li, C., Heidt, D. G., Dalerba, P., Burant, C. F., Zhang, L., Adsay, V., et al. (2007). Identification of pancreatic cancer stem cells. Cancer Research, 67(3), 1030–1037. doi:10.1158/0008-5472.CAN-06-2030.
Patrawala, L., Calhoun, T., Schneider-Broussard, R., Li, H., Bhatia, B., Tang, S., et al. (2006). Highly purified CD44+ prostate cancer cells from xenograft human tumors are enriched in tumorigenic and metastatic progenitor cells. Oncogene, 25(12), 1696–1708. doi:10.1038/sj.onc.1209327.
Clay, M. R., Tabor, M., Owen, J. H., Carey, T. E., Bradford, C. R., Wolf, G. T., et al. (2010). Single-marker identification of head and neck squamous cell carcinoma cancer stem cells with aldehyde dehydrogenase. Head & Neck, 32(9), 1195–1201. doi:10.1002/hed.21315.
Ginestier, C., Hur, M. H., Charafe-Jauffret, E., Monville, F., Dutcher, J., Brown, M., et al. (2007). ALDH1 is a marker of normal and malignant human mammary stem cells and a predictor of poor clinical outcome. Cell Stem Cell, 1(5), 555–567. doi:10.1016/j.stem.2007.08.014.
Li, X., Lewis, M. T., Huang, J., Gutierrez, C., Osborne, C. K., Wu, M. F., et al. (2008). Intrinsic resistance of tumorigenic breast cancer cells to chemotherapy. Journal of the National Cancer Institute, 100(9), 672–679. doi:10.1093/jnci/djn123.
Bao, S., Wu, Q., McLendon, R. E., Hao, Y., Shi, Q., Hjelmeland, A. B., et al. (2006). Glioma stem cells promote radioresistance by preferential activation of the DNA damage response. Nature, 444(7120), 756–760. doi:10.1038/nature05236.
Singh, A., & Settleman, J. (2010). EMT, cancer stem cells and drug resistance: An emerging axis of evil in the war on cancer. Oncogene, 29(34), 4741–4751. doi:10.1038/onc.2010.215.
Charafe-Jauffret, E., Ginestier, C., Iovino, F., Tarpin, C., Diebel, M., Esterni, B., et al. (2010). Aldehyde dehydrogenase 1-positive cancer stem cells mediate metastasis and poor clinical outcome in inflammatory breast cancer. Clinical Cancer Research, 16(1), 45–55. doi:10.1158/1078-0432.CCR-09-1630.
Hermann, P. C., Huber, S. L., Herrler, T., Aicher, A., Ellwart, J. W., Guba, M., et al. (2007). Distinct populations of cancer stem cells determine tumor growth and metastatic activity in human pancreatic cancer. Cell Stem Cell, 1(3), 313–323. doi:10.1016/j.stem.2007.06.002.
Hay, E. D. (2005). The mesenchymal cell, its role in the embryo, and the remarkable signaling mechanisms that create it. Developmental Dynamics, 233(3), 706–720. doi:10.1002/dvdy.20345.
Savagner, P., Kusewitt, D. F., Carver, E. A., Magnino, F., Choi, C., Gridley, T., et al. (2005). Developmental transcription factor slug is required for effective re-epithelialization by adult keratinocytes. Journal of Cellular Physiology, 202(3), 858–866. doi:10.1002/jcp.20188.
Kalluri, R., & Weinberg, R. A. (2009). The basics of epithelial-mesenchymal transition. The Journal of Clinical Investigation, 119(6), 1420–1428. doi:10.1172/JCI39104.
Wu, Y., Deng, J., Rychahou, P. G., Qiu, S., Evers, B. M., & Zhou, B. P. (2009). Stabilization of snail by NF-kappaB is required for inflammation-induced cell migration and invasion. Cancer Cell, 15(5), 416–428. doi:10.1016/j.ccr.2009.03.016.
Yang, M. H., Wu, M. Z., Chiou, S. H., Chen, P. M., Chang, S. Y., Liu, C. J., et al. (2008). Direct regulation of TWIST by HIF-1alpha promotes metastasis. Nature Cell Biology, 10(3), 295–305. doi:10.1038/ncb1691.
Gjerdrum, C., Tiron, C., Hoiby, T., Stefansson, I., Haugen, H., Sandal, T., et al. (2010). Axl is an essential epithelial-to-mesenchymal transition-induced regulator of breast cancer metastasis and patient survival. Proceedings of the National Academy of Sciences of the United States of America, 107(3), 1124–1129. doi:10.1073/pnas.0909333107.
Skvortsova, I., Skvortsov, S., Raju, U., Stasyk, T., Riesterer, O., Schottdorf, E. M., et al. (2010). Epithelial-to-mesenchymal transition and c-myc expression are the determinants of cetuximab-induced enhancement of squamous cell carcinoma radioresponse. Radiotherapy and Oncology, 96(1), 108–115. doi:10.1016/j.radonc.2010.04.017.
Bandyopadhyay, A., Wang, L., Agyin, J., Tang, Y., Lin, S., Yeh, I. T., et al. (2010). Doxorubicin in combination with a small TGFbeta inhibitor: A potential novel therapy for metastatic breast cancer in mouse models. PLoS One, 5(4), e10365. doi:10.1371/journal.pone.0010365.
Fuchs, B. C., Fujii, T., Dorfman, J. D., Goodwin, J. M., Zhu, A. X., Lanuti, M., et al. (2008). Epithelial-to-mesenchymal transition and integrin-linked kinase mediate sensitivity to epidermal growth factor receptor inhibition in human hepatoma cells. Cancer Research, 68(7), 2391–2399. doi:10.1158/0008-5472.CAN-07-2460.
Kudo-Saito, C., Shirako, H., Takeuchi, T., & Kawakami, Y. (2009). Cancer metastasis is accelerated through immunosuppression during Snail-induced EMT of cancer cells. Cancer Cell, 15(3), 195–206. doi:10.1016/j.ccr.2009.01.023.
Shin, S. Y., Rath, O., Zebisch, A., Choo, S. M., Kolch, W., & Cho, K. H. (2010). Functional roles of multiple feedback loops in extracellular signal-regulated kinase and wnt signaling pathways that regulate epithelial-mesenchymal transition. Cancer Research, 70(17), 6715–6724. doi:10.1158/0008-5472.CAN-10-1377.
Smith, G. R., & Missailidis, S. (2004). Cancer, inflammation and the AT1 and AT2 receptors. Journal of Inflammation (London), 1(1), 3. doi:10.1186/1476-9255-1-3.
Chang, H. Y., Nuyten, D. S., Sneddon, J. B., Hastie, T., Tibshirani, R., Sorlie, T., et al. (2005). Robustness, scalability, and integration of a wound-response gene expression signature in predicting breast cancer survival. Proceedings of the National Academy of Sciences of the United States of America, 102(10), 3738–3743. doi:10.1073/pnas.0409462102.
Thiery, J. P. (2003). Epithelial-mesenchymal transitions in development and pathologies. Current Opinion in Cell Biology, 15(6), 740–746.
Wellner, U., Schubert, J., Burk, U. C., Schmalhofer, O., Zhu, F., Sonntag, A., et al. (2009). The EMT-activator ZEB1 promotes tumorigenicity by repressing stemness-inhibiting microRNAs. Nature Cell Biology, 11(12), 1487–1495. doi:10.1038/ncb1998.
Barrandon, Y., & Green, H. (1987). Three clonal types of keratinocyte with different capacities for multiplication. Proceedings of the National Academy of Sciences of the United States of America, 84(8), 2302–2306.
Harper, L. J., Piper, K., Common, J., Fortune, F., & Mackenzie, I. C. (2007). Stem cell patterns in cell lines derived from head and neck squamous cell carcinoma. Journal of Oral Pathology & Medicine, 36(10), 594–603. doi:10.1111/j.1600-0714.2007.00617.x.
Li, H., Chen, X., Calhoun-Davis, T., Claypool, K., & Tang, D. G. (2008). PC3 human prostate carcinoma cell holoclones contain self-renewing tumor-initiating cells. Cancer Research, 68(6), 1820–1825. doi:10.1158/0008-5472.CAN-07-5878.
Keller, P. J., Lin, A. F., Arendt, L. M., Klebba, I., Jones, A. D., Rudnick, J. A., et al. (2010). Mapping the cellular and molecular heterogeneity of normal and malignant breast tissues and cultured cell lines. Breast Cancer Research, 12(5), R87. doi:10.1186/bcr2755.
Burk, U., Schubert, J., Wellner, U., Schmalhofer, O., Vincan, E., Spaderna, S., et al. (2008). A reciprocal repression between ZEB1 and members of the miR-200 family promotes EMT and invasion in cancer cells. EMBO Reports, 9(6), 582–589. doi:10.1038/embor.2008.74.
Chaffer, C. L., Brueckmann, I., Scheel, C., Kaestli, A. J., Wiggins, P. A., Rodrigues, L. O., et al. (2011). Normal and neoplastic nonstem cells can spontaneously convert to a stem-like state. Proceedings of the National Academy of Sciences of the United States of America, 108(19), 7950–7955. doi:10.1073/pnas.1102454108.
Gaggioli, C., Hooper, S., Hidalgo-Carcedo, C., Grosse, R., Marshall, J. F., Harrington, K., et al. (2007). Fibroblast-led collective invasion of carcinoma cells with differing roles for RhoGTPases in leading and following cells. Nature Cell Biology, 9(12), 1392–1400. doi:10.1038/ncb1658.
Giampieri, S., Manning, C., Hooper, S., Jones, L., Hill, C. S., & Sahai, E. (2009). Localized and reversible TGFbeta signalling switches breast cancer cells from cohesive to single cell motility. Nature Cell Biology, 11(11), 1287–1296. doi:10.1038/ncb1973.
Asiedu, M. K., Ingle, J. N., Behrens, M. D., Radisky, D. C., & Knutson, K. L. (2011). TGFbeta/TNF(alpha)-mediated epithelial-mesenchymal transition generates breast cancer stem cells with a claudin-low phenotype. Cancer Research, 71(13), 4707–4719. doi:10.1158/0008-5472.CAN-10-4554.
Korpal, M., Ell, B. J., Buffa, F. M., Ibrahim, T., Blanco, M. A., Celia-Terrassa, T., et al. (2011). Direct targeting of Sec23a by miR-200 s influences cancer cell secretome and promotes metastatic colonization. Nature Medicine, 17(9), 1101–1108. doi:10.1038/nm.2401.
Korpal, M., Lee, E. S., Hu, G., & Kang, Y. (2008). The miR-200 family inhibits epithelial-mesenchymal transition and cancer cell migration by direct targeting of E-cadherin transcriptional repressors ZEB1 and ZEB2. Journal of Biological Chemistry, 283(22), 14910–14914. doi:10.1074/jbc.C800074200.
Olumi, A. F., Grossfeld, G. D., Hayward, S. W., Carroll, P. R., Tlsty, T. D., & Cunha, G. R. (1999). Carcinoma-associated fibroblasts direct tumor progression of initiated human prostatic epithelium. Cancer Research, 59(19), 5002–5011.
Kojima, Y., Acar, A., Eaton, E. N., Mellody, K. T., Scheel, C., Ben-Porath, I., et al. (2010). Autocrine TGF-beta and stromal cell-derived factor-1 (SDF-1) signaling drives the evolution of tumor-promoting mammary stromal myofibroblasts. Proceedings of the National Academy of Sciences of the United States of America, 107(46), 20009–20014. doi:10.1073/pnas.1013805107.
Lopez-Novoa, J. M., & Nieto, M. A. (2009). Inflammation and EMT: An alliance towards organ fibrosis and cancer progression. EMBO Molecular Medicine, 1(6–7), 303–314. doi:10.1002/emmm.200900043.
Creighton, C. J., Li, X., Landis, M., Dixon, J. M., Neumeister, V. M., Sjolund, A., et al. (2009). Residual breast cancers after conventional therapy display mesenchymal as well as tumor-initiating features. Proceedings of the National Academy of Sciences of the United States of America, 106(33), 13820–13825. doi:10.1073/pnas.0905718106.
Harper, L. J., Costea, D. E., Gammon, L., Fazil, B., Biddle, A., & Mackenzie, I. C. (2010). Normal and malignant epithelial cells with stem-like properties have an extended G2 cell cycle phase that is associated with apoptotic resistance. BMC Cancer, 10, 166. doi:10.1186/1471-2407-10-166.
Surowiak, P., Materna, V., Kaplenko, I., Spaczynski, M., Dolinska-Krajewska, B., Gebarowska, E., et al. (2006). ABCC2 (MRP2, cMOAT) can be localized in the nuclear membrane of ovarian carcinomas and correlates with resistance to cisplatin and clinical outcome. Clinical Cancer Research, 12(23), 7149–7158. doi:10.1158/1078-0432.CCR-06-0564.
Theile, D., Ketabi-Kiyanvash, N., Herold-Mende, C., Dyckhoff, G., Efferth, T., Bertholet, V., et al. (2011). Evaluation of drug transporters' significance for multidrug resistance in head and neck squamous cell carcinoma. Head & Neck, 33(7), 959–968. doi:10.1002/hed.21559.
Wang, X. Q., Ongkeko, W. M., Chen, L., Yang, Z. F., Lu, P., Chen, K. K., et al. (2010). Octamer 4 (Oct4) mediates chemotherapeutic drug resistance in liver cancer cells through a potential Oct4-AKT-ATP-binding cassette G2 pathway. Hepatology, 52(2), 528–539. doi:10.1002/hep.23692.
Tsai, L. L., Yu, C. C., Chang, Y. C., Yu, C. H., & Chou, M. Y. (2011). Markedly increased Oct4 and Nanog expression correlates with cisplatin resistance in oral squamous cell carcinoma. Journal of Oral Pathology & Medicine. doi:10.1111/j.1600-0714.2011.01015.x.
Cheung, S. T., Cheung, P. F., Cheng, C. K., Wong, N. C., & Fan, S. T. (2011). Granulin-epithelin precursor and ATP-dependent binding cassette (ABC)B5 regulate liver cancer cell chemoresistance. Gastroenterology, 140(1), 344–355. doi:10.1053/j.gastro.2010.07.049.
Frank, N. Y., Margaryan, A., Huang, Y., Schatton, T., Waaga-Gasser, A. M., Gasser, M., et al. (2005). ABCB5-mediated doxorubicin transport and chemoresistance in human malignant melanoma. Cancer Research, 65(10), 4320–4333. doi:10.1158/0008-5472.CAN-04-3327.
Wei, J., Barr, J., Kong, L. Y., Wang, Y., Wu, A., Sharma, A. K., et al. (2010). Glioma-associated cancer-initiating cells induce immunosuppression. Clinical Cancer Research, 16(2), 461–473. doi:10.1158/1078-0432.CCR-09-1983.
Ramgolam, K., Lauriol, J., Lalou, C., Lauden, L., Michel, L., de la Grange, P., et al. (2011). Melanoma spheroids grown under neural crest cell conditions are highly plastic migratory/invasive tumor cells endowed with immunomodulator function. PLoS One, 6(4), e18784. doi:10.1371/journal.pone.0018784.
Quintana, E., Shackleton, M., Sabel, M. S., Fullen, D. R., Johnson, T. M., & Morrison, S. J. (2008). Efficient tumour formation by single human melanoma cells. Nature, 456(7222), 593–598. doi:10.1038/nature07567.
Pang, R., Law, W. L., Chu, A. C., Poon, J. T., Lam, C. S., Chow, A. K., et al. (2010). A subpopulation of CD26+ cancer stem cells with metastatic capacity in human colorectal cancer. Cell Stem Cell, 6(6), 603–615. doi:10.1016/j.stem.2010.04.001.
Marsh, D., Suchak, K., Moutasim, K. A., Vallath, S., Hopper, C., Jerjes, W., et al. (2011). Stromal features are predictive of disease mortality in oral cancer patients. The Journal of Pathology, 223(4), 470–481. doi:10.1002/path.2830.
Acknowledgements
This work was funded by the NC3Rs.