Abstract
The type I insulin-like growth factor (IGF) receptor (IGF1R) is a transmembrane tyrosine kinase involved in breast cancer proliferation, survival, and metastasis. Several monoclonal antibodies directed against the receptor are in clinical trials. In order to develop a methodology to detect and measure IGF1R levels in breast cancer cells, we covalently conjugated an IGF1R antibody, AVE-1642, with quantum dots (Qdots), which are nanocrystals that emit fluorescence upon excitation. AVE-1642 Qdots only bound to cells that express IGF1R, and measured IGF1R levels by fluorescence emission at 655 nm. After binding to the cell surface, AVE-1642 Qdots underwent receptor mediated endocytosis, localized to endosome, and later translocated into the nucleus. Treating MCF-7 cells with AVE-1642 Qdots, but not unconjugated Qdots alone, downregulated IGF1R levels and rendered cells refractory to IGF-I stimulation. Furthermore, cell proliferation was slightly inhibited by AVE-1642 Qdots, but not the unconjugated Qdots. Our data suggest that AVE-1642 Qdots can be used to detect IGF1R expression and measure changes in cell surface receptor levels. In addition, the inhibitory effect of AVE-1642 Qdots to cell proliferation implies that it may serve as a traceable therapeutic agent.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Targeted therapies against specific molecules relevant to cancer proliferation, motility and metastasis, have become “the wave of the future” for many types of cancer, including breast cancer [1]. One such target is the type I insulin-like growth factor receptor (IGF1R). IGF1R is a tyrosine kinase receptor that is activated by insulin-like growth factor (IGF)-I and IGF-II. Activated IGF1R recruits adaptor proteins, such as insulin-receptor substrate 1 (IRS-1) and IRS-2, leading to downstream activation of multiple signaling pathways including mitogen-activated protein kinase (MAPK) and phosphatidylinositol-3 kinase (PI-3 K) [2]. Increased expression and/or enhanced activity of IGF1R have been observed in breast cancer specimens [3]. It is well documented that IGF1R plays important roles in the proliferation, survival and metastasis of breast cancer cells [4]. Therefore, IGF1R has surfaced as an attractive target for breast cancer therapy. Several monoclonal antibodies directed against the receptor are in clinical trials.
Previous results from our laboratory have shown that a chimeric single chain antibody, scFv-Fc, downregulates the level of IGF1R both in cell lines and in an in vivo xenograft model [5]. Similar downregulation of IGF1R has been seen with other monoclonal antibodies, including EM-164, A12, and h7C10 [6–8]. Downregulation of IGF1R rendered cells refractory to further IGF-I and IGF-II stimulation and was associated with decreased tumor growth [7]. Thus, levels of IGF1R post therapy could be an excellent pharmacodynamic marker and potential indicator of response.
Although agents targeting IGF1R are in clinical trials, patient enrollment is not based on pre-selected levels of IGF1R in tumor specimens. To date, there has been little association between levels of IGF1R and response to anti-IGF1R therapies in preclinical model systems. For example, in prostate cancer cell lines with 4-fold differences in IGF1R expression, the anti-IGF1R monoclonal antibody A12 is equally effective in suppressing monolayer growth [9]. However, downregulation of IGF1R after A12 monoclonal antibody therapy is universally seen [10]. Methods to detect receptor downregulation in vivo could be useful in the clinical development of these anti-IGF1R antibodies.
Recently quantum dots (Qdots) detection of specific molecules has surfaced as a novel approach for molecular imaging and medical diagnostics [11–14]. Qdots are semiconductor nanocrystals that emit fluorescence from visible to infrared wavelengths, upon excitation by a light source. Among several differently composed Qdots, Cadmium/Selenide (Cd/Se) Qdots are the best studied. A Cd/Se Qdot is composed of a Cd/Se core, a ZnS shell, passivated with an outer layer of TOPO molecules. Compared with traditional fluorophore, Qdots have excellent optical properties including high brightness, resistance to photo-bleaching and tunable wavelength. Over the past few years, scientists have developed methodologies to covalently link Qdots to molecules such as peptides, antibodies, or small-molecule ligands for imaging applications as fluorescent probes [14, 15].
In this study, an IGF1R monoclonal antibody, AVE-1642 (humanized version of EM-164), was conjugated to Cd/Se Qdots. We show that AVE-1642 conjugated Qdots (AVE-1642 Qdots) bind specifically to breast cancer cells that express IGF1R. In addition, the impact of conjugated Qdots on IGF signaling and cell proliferation was assessed. Our results suggest that AVE-1642 Qdots can be used to identify IGF1R in breast cancer cells, which provide a step towards the application of Qdots in detecting IGF1R in vivo and predicting the response post therapy.
Materials and methods
Reagents
All chemical reagents were purchased from Sigma (St. Louis, MO, USA) unless otherwise indicated. IGF-I was purchased from GroPep, Thebarton, SA, Australia. AVE-1642 is a humanized form of EM164 [16) antibody from Sanofi-Aventis, Paris, France and anti-CD20 antibody was from ImmunoGen, Cambridge, MA, USA. ScFv-Fc is an humanized IGF1R antibody, which has been described elsewhere [5]. Alexa-488 labeled transferrin, 4′,6-diamidino-2-phenylindole (DAPI) and Qdot (Quantum dots) antibody conjugation kit were from Invitrogen, Carlsbad, CA, USA. Antibodies used for Western blotting are IGF1Rβ polyclonal antibody (C-20) (Santa Cruz, Santa Cruz, CA, USA), actin monoclonal antibody (Sigma, St. Louis, MO, USA), Akt and phospho-Akt (Ser473) antibodies, MAPK and phospho-MAPK antibodies (Cell signaling, Danvers, MA, USA), and HRP-conjugated secondary antibodies (Biorad, Hercules, CA, USA).
Cell lines and culture
MCF-7 cells (human breast cancer cell line), R- cells (mouse fibroblast cells with a homozygous disruption of IGF1R gene), and R-/IGF1R cells (cell line derived from R- cells with re-introduced IGF1R gene) were cultured according to literature [16]. R-cells were a gift from Renato Baserga (Thomas Jefferson University, Philadelphia, PA).
Conjugation of antibody with quantum dots
Antibodies were conjugated to Cd/Se Qdots (emission at 655 nm) through a heterobifunctional cross-linker, succinimidyl-4-(N-maleimidomethyl) cyclohexane-1-carboxylate (SMCC). The NHS ester end of SMCC was reacted with the amine groups on the Cd/Se Qdots, and the maleimide end of SMCC coupled to the sulfhydryls on the DTT-reduced antibody according to the instructions of the manufacturer (Invitrogetn, Carlsbad, CA, USA). Conjugate concentration was determined using the extinction coefficient (Qdot 655 nm Ext coef. at 800,000 M−1 cm−1) measured at 638 nm.
Fluorescence microscopy
Cells were incubated with antibody-conjugated Qdots (10 nM) for 1 h, then cells were washed three times with PBS briefly. Cells were observed under an Olympus BX60 Upright Microscope to obtain bright field image and fluorescent Qdots image using a band pass filter at 600/90 nm (200× magnification).
Confocal microscopy
Cells were incubated with antibody-conjugated Qdots (10 nM) for various times, with or without the addition of Alexa 488-labeled tranferrin. Cells were fixed using methanol for 10 min at −20°C. In some experiments, cells were rehydrated and stained with DAPI for 1 min, and then dehydrated with increasing concentrations of ethanol. Cells were mounted using SlowFade Gold anti-fade mounting media (Invitrogen, Carlsbad, CA, USA). Cell fluorescence was observed using an Olympus Fluoview FV500 laser scanning confocal system (600× magnification).
Flow cytometry
Cells were trypsinized and resuspended in PBS/1% BSA/0.1% sodium azide (FACS buffer). Cells were incubated with anti-CD20 antibody or AVE-1642 Qdots in FACS buffer for 1 h at 4°C. Cells were washed twice and resuspended with 400 μl FACS buffer. IGF1R levels on cell surface were measured using a LSRII flow cytometer (BD Biosciences, San Jose, CA, USA) with an excitation laser at Violet and emission at 650/20 nm.
Cell stimulation and cell lysates
Cells were grown in Dulbecco’s Modified Eagle’s Medium (DMEM). When cells reached 50% confluence, they were serum-deprived for 24 h in serum free media as described previously [17]. Cells were treated with various concentrations of antibody or antibody-conjugated Qdots for times as indicated in figure legends. The next day, medium was replaced with serum free media with or without IGF-I (5 nM) for 10 min. Cells were washed twice with ice-cold PBS on ice and lysed as previously described [17]. Protein concentration of cell lysates was determined using the bicinchoninic acid protein assay reagent kit (Pierce, Rockford, IL, USA).
Gel electrophoresis and Western blotting
Proteins from lysates were resolved by SDS-PAGE and transferred to nitrocellulose membranes. The membranes were immunoblotted using IGF1Rβ antibody (1:2,000 dilution), MAPK antibody (1:2,000 dilution), phospho-MAPK antibody (1:2,000 dilution), Akt antibody (1:2,000 dilution), phospho-Akt antibody (1:2,000 dilution), or actin antibody (1:5,000 dilution) followed by the appropriate horseradish peroxidase-conjugated secondary antibody (Biorad, Hercules, CA, USA). Western blots were developed by the chemiluminescence method.
Cell proliferation assay
Assays were performed as previously described [18]. Briefly, cells were plated in triplicate in 24-well tissue culture plates at a density of 20,000 cells per well in growth media. After 24 h, cells were washed twice with PBS and switched to serum free media for 24 h. Cells were then treated with or without unconjugated Qdots (10 nM), AVE-1642 Qdots (10 nM), or AVE-1642 antibody (10 nM) in growth media and incubated for 5 days. 60 μl of 5 mg/ml MTT reagent in PBS was added to each well and plates were incubated for 3 h at 37°C. Wells were then aspirated and 0.5 ml of solubilizing solution (95% DMSO + 5% IMEM) was added to solubilize the formazan crystals. Absorbance was measured at 570 nm with a 650 nm differential filter.
Results
Specific binding of AVE-1642 Qdots to cells that express IGF1R
Cd/Se Qdots were conjugated with the IGF1R antibody (AVE-1642), through a heterobifunctional chemical linker SMCC. The same protocol was used to conjugate Qdots with an irrelevant anti-CD20 antibody, directed against the B-cell expressed CD20 protein. AVE-1642, or anti-CD20 conjugated Qdots were incubated with MCF-7 cells, a breast cancer cell line that expresses high levels of IGF1R as previously shown [17]. In Fig. 1a, AVE-1642, but not anti-CD20 conjugated Qdots, bound to MCF-7 cells and emitted fluorescence upon excitation. To confirm that AVE-1642 Qdots bound only to IGF1R expressing cells, we used the IGF1R deficient cell line, R- cells, and its derivative cell line in which IGF1R gene was re-introduced (R-/IGF1R). Figure 1b shows that AVE-1642 Qdots only bound to R-/IGF1R cells, but not R- cells, although R- cells express the related insulin receptor [16). Therefore, expression of IGF1R was necessary for AVE-1642 Qdots binding.
AVE-1642 Qdots bound to cells that express IGF1R specifically. (a) MCF-7 cells were incubated with AVE-1642 Qdots (top panels) or anti-CD20 Qdots (bottom panels) for 1 h, and then washed with PBS. Cells were observed under fluorescent microscope. The left panels show the bright field image of cells, and the right panels show the Qdots fluorescence at 655 nm. (b) R- cells (top panels) or R-/IGF1R cells (bottom panels) were incubated with AVE-1642 Qdots for 1 h, and then washed with PBS. Cells were observed under microscope
Measurement of changes of IGF1R levels on cell surface
In order to confirm the specific binding of AVE-1642 Qdots, we performed flow cytometry analysis to measure the fluorescent intensity bound to cells. Several cell lines were incubated with either anti-CD20 Qdots, or AVE-1642 Qdots in vitro. When R- cells were incubated with AVE-1642 Qdots, no specific fluorescence was detected on the cell surface (Fig. 2a). In contrast, incubation of AVE-1642 Qdots to R-/IGF1R cells produced a dramatic increase of fluorescence compared with that of the anti-CD20 Qdots (Fig. 2b). This suggested specific binding of AVE-1642 Qdots to cell surface IGF1R. Since IGF1R antibodies downregulate IGF1R levels, we determined whether AVE-1642 Qdots were able to detect changes of surface IGF1R levels. As shown in Fig. 2c, AVE-1642 Qdots, but not anti-CD20 Qdots, bound to MCF-7 cells with high fluorescent intensity. When cells were pretreated with a separate IGF1R scFv-Fc antibody, the fluorescent intensity decreased dramatically to 11% of baseline, consistent with the antibody-induced down-regulation of IGF1R level in cells. While we cannot rule out the possibility that scFv-Fc interfered with AVE-1642 Qdots binding, the decrease in IGF1R detected by fluorescence was equivalent to the scFv-Fc mediated receptor downregulation detected by immunoblot [5]. Therefore, AVE-1642 Qdots could detect downregulation of IGF1R after antibody treatment.
AVE-1642 Qdots measured changes of IGF1R levels by flow cytometry analysis. (a and b) Cells were trypsinized, resuspended in FACS buffer, and incubated with either AVE-1642 Qdots or anti-CD20 Qdots. The fluorescence of bound Qdots was analyzed by flow cytometry. The horizontal axis of the diagram represents the fluorescent intensity of Qdots, and the vertical axis shows the percentage of maximum cell number. (a) R- cells. Light line-defined region represents fluorescence of bound anti-CD20 Qdots, and dark line-defined region represents fluorescence of bound AVE-1642 Qdots. (b) R-/IGF1R cells. Light line-defined region represents fluorescence of bound anti-CD20 Qdots, and shaded region represents fluorescence of bound AVE-1642 Qdots. (c) MCF-7 cells were pretreated with 250 nM of scFv-Fc, or remain untreated for 24 h, and then cells were trypsinized, and incubated with or without anti-CD20 Qdots or AVE-1642 Qdots. The light shaded region represents background from no Qdots incubated cells. The light line-defined region represents fluorescence of bound CD-20 Qdots. The dark shaded region represents fluorescence of bound AVE-1642 Qdots without scFv-Fc treatment, and the dark line-defined region represents fluorescence of bound AVE-1642 Qdots after scFv-Fc treatment
Dynamic trafficking of AVE-1642 Qdots in MCF-7 cells
Fluorescent microscopy revealed that AVE-1642 Qdots bound to cells within 10 min of exposure, but persistent detection of Qdots could be seen for as long as 24 h and beyond (data not shown). In order to assess the cellular fate of AVE-1642 Qdots, we simultaneously added AVE-1642 Qdots and Alexa 488-labeled transferrin in MCF-7 cells. Fluorophore-labeled transferrin has been used to trace receptor-mediated endocytosis [19]. As shown in Fig. 3a, when cells were exposed to AVE-1642 Qdots for 10 min, they were mainly localized to the plasma membrane. By 1 h of incubation, a large portion of Qdots were co-localized with transferrin in early endosome, suggesting that Qdots were internalized through IGF1R mediated endocytosis as we have previously suggested [5]. Surprisingly, after 6 h, Qdots showed a juxta-nuclear staining pattern, and a small portion of Qdots were actually localized in the DAPI stained nucleus. By 24 h, the majority of the Qdots were localized inside the nucleus. Therefore, the uptake of Qdots in cells follows a dynamic trafficking path, from cell membrane, to endosome, and then to the nucleus.
Trafficking of AVE-1642 Qdots was dynamic in MCF-7 cells. (a) MCF-7 cells were incubated with AVE-1642 Qdots and Alexa 488-labeled transferrin for 10 min (top panels) or 1 h (lower panels), and then cells were fixed. The subcellular distribution of Qdots and transferrin was observed under confocal microscope. The bar in each image represents 20 μm in length. (b) MCF-7 cells were incubated with AVE-1642 Qdots for 6 h (top panels) or 24 h (bottom panels), and then cells were fixed and stained with DAPI. The fluorescence of Qdots and DAPI was analyzed by confocal microscope
Time-dependent degradation of IGF1R by AVE-1642 Qdots
We and others have shown that downregulation of IGF1R by antibodies occurs through endocytosis [5–8]. We assessed whether antibody-conjugated Qdots also downregulated IGF1R in cells. As shown in Fig. 4a, IGF1R levels were downregulated by IGF1R antibodies after 24 h, including scFv-Fc and AVE-1642, but not anti-CD20, consistent with our previous results [5, 16]. When cells were incubated with AVE-1642 Qdots, but not anti-CD20 Qdots, the level of IGF1R decreased dramatically. Our results suggest that AVE-1642 Qdots not only bound to IGF1R, but also retained the function of downregulating IGF1R through receptor mediated endocytosis. In addition, the IGF1R level decreased in a time dependent manner; as by 6 h, the IGF1R level was reduced by more than 50% (Fig. 4b).
AVE-1642 Qdots caused IGF1R downregulation and rendered cells refractory to further IGF-I stimulation. (a) MCF-7 cells were treated with scFv-Fc (250 nM), anti-CD20 (250 nM), AVE-1642 (120 nM), anti-CD20 Qdots (10 nM), or AVE-1642 Qdots (AVE-Qdots) (10 nM) for 24 h, and IGF1R levels were analyzed by Western blotting. (b) MCF-7 cells were treated with AVE-1642 Qdots (10 nM) for various time points, and IGF1R levels were analyzed by Western blotting. (c) MCF-7 cells were pre-treated with unconjugated Qdots (10 nM) or AVE-1642 Qdots (10 nM) for 1 h or 24 h, and then cells were treated with IGF-I (5 nM) for 5 min. The level of IGF1R, the phosphorylation and total level of Akt and MAPK were analyzed by Western blotting using their specific antibodies. The level of actin was used as a control
Effect of AVE-1642 Qdots on IGF-I stimulated cell signaling
To assess the impact of Qdots treatment on cell signaling, MCF-7 cells were pretreated with unconjugated Qdots, or AVE-1642 Qdots, treated with IGF-I, and then the phosphorylation of downstream signaling molecules, including Akt and MAPK was examined. Interestingly, when cells were pre-treated with AVE-1642 Qdots for just 1 h, the IGF-I stimulated phosphorylation of Akt and MAPK was dramatically decreased (Fig. 4c). At this early time point, the level of IGF1R had no significant changes when measured by immunoblot. However, confocal microscopy showed that the AVE-1642 Qdots were localized in the endosomes at 1 h. This suggests that IGF1R detected by immunoblotting was localized in endosome and was subsequently degraded. Decreased membrane IGF1R rendered cell refractory to further IGF-I stimulation. After 24 h of treatment, the level of IGF1R was downregulated and IGF-I stimulated phosphorylation of Akt and MAPK was diminished.
Impact of Qdots on MCF-7 cell proliferation
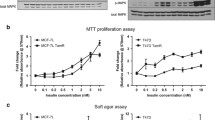
In order to examine whether Qdots, or conjugated Qdots affected MCF-7 cell proliferation, MCF-7 cells were cultured in full media in the presence or absence of unconjugated Qdots, AVE-1642 Qdots, or AVE-1642 antibody. After 5 days, cell growth rate was assessed using MTT assay. As shown in Fig. 5, Qdots themselves did not significantly affect cell growth. However, AVE-1642 inhibited MCF-7 cell growth and AVE-1642 Qdots also had a similar effect, but to a lesser extent.
AVE-1642 Qdots, but not unconjugated Qdots, affected MCF-7 cell proliferation. Cells were incubated with unconjugated Qdots, AVE-1642 Qdots (10 nM), or AVE-1642 antibody (10 nM) in full serum media for 5 days. Cell proliferation was analyzed by MTT assay as described in “Materials and methods”. Analysis of variance was used to compare the statistical significance among the data. Significant differences among data was denoted as P < 0.05 (one asterisk), and P < 0.001 (three asterisks)
Discussion
Given the increasing use and activity of molecular targeted therapy, a major challenge is to determine which patients benefit from specific target inhibition. The primary means of selecting patients is based upon the expression level of targeted molecules in primary tumors. Traditionally, ligand binding in the case of estrogen receptor, fluorescent in situ hybridization (FISH) for HER-2, and immunohistochemistry for both molecules, has been used to detect receptor levels. Recently, conjugated Qdots have been used to detect HER-2 levels in breast cancer cells [20, 21]. Herein, we show that antibody conjugated Qdots specifically detect the expression level of IGF1R in breast cancer cells. Direct conjugation of AVE-1642 with Qdots does not alter the ability of AVE-1642 to bind IGF1R. More importantly, AVE-1642 Qdots have the ability to detect changes of the IGF1R levels, after antibody downregulation of IGF1R. Since downregulation of IGF1R after monoclonal antibody therapy is commonly reported, the ability of AVE-1642 Qdots to detect receptor downregulation could be useful in predicting response post antibody therapies in clinical settings.
Our data have shown that AVE-1642 Qdots bind to IGF1R on the cell surface, undergo receptor-mediated endocytosis and co-localize with transferrin in the early endosome. This is analogous to the finding that EGF conjugated Qdots bind to and activate EGFR, and are internalized into the endosome [22]. In addition, similar results were obtained by Jaiswal et al., showing that dihydrolipoic acid-capped Qdots, which bind to positively charged proteins, were localized to juxta-nuclear endosomal region of HeLa cells [23]. We have previously shown that antibodies against IGF1R downregulate the level of IGF1R on the cell surface. Here we show that AVE-1642 Qdots, but not anti-CD20 Qdots, also specifically downregulated IGF1R level in cells. This is due to the internalization and subsequent degradation of the receptor in the endosome.
Our confocal microscopy data have shown that Qdots were localized in the juxta-nuclear region within 24 h after treatment. It is conceivable that Qdots translocate from endosome to nucleus after IGF1R-antibody complex are degraded in the endosome. It has been shown that other nanoparticles, such as silica, or gold nanoparticles, can translocate into nucleus through the nuclear pore complex (NPC), after entering cells [24, 25]. Although the diameter of the NPC is only 26 nm, Pante et al. indicated that gold particles with a size of 39 nm can translocate into nucleus through the NPC [25]. Since the size of unconjugated Qdots is around 15–19 nm [26], it is very likely Qdots translocate to the nucleus through the NPC as well. The long term effect of Qdots on the nucleus structure and function remains to be elucidated.
Beyond the intracellular fate of Qdots, their in vivo distribution needs to be understood. It has also been reported that in vivo intravenously delivered Qdots may be taken up by the reticuloendothelial system (RES), which consists of phagocytic cells located in the liver, spleen, lymph nodes and bone marrow [27–31]. The RES uptake not only prevents Qdots from targeting tumor, but also may bring toxicity concerns to the RES organs. Therefore, the long term metabolism of Qdots in vivo will need to be studied thoroughly.
Since the Qdots utilized here are made of heavy metals, one concern is that they may cause cytotoxicity to breast cancer cells. However, our data have shown that incubation of unconjugated Qdots with breast cancer cells didn’t affect cell proliferation significantly. This is consistent with previous reports that Qdots had minimal effect on cell growth [32, 33]. Interestingly, AVE-1642 Qdots inhibited cell growth to a smaller extent compared to unconjugated antibody. Binding of AVE-1642 Qdots caused receptor downregulation, and rendered cells refractory to IGF-I treatment, therefore inhibiting cell growth. In this regard, coupled with their fluorescence nature, AVE-1642 Qdots may be used to track the efficiency of antibody delivery and targeting of tumor in vivo.
Our data have shown that AVE-1642 Qdots are excellent agents to measure IGF1R level in cell lines with high specificity. This finding provides a step towards the in vivo application of AVE-1642 Qdots. Since breast cancer metastasizes to distant organs, it is often not feasible to measure levels of IGF1R in those sites. It may be problematic to use the level of IGF1R in primary tumors as a criterion to select patients for anti-IGF1R therapy as stability of IGF1R over time has not been studied. Certainly, there is little evidence of gene amplification of IGF1R in breast cancer [34], and the level of IGF1R could vary from the primary tumor to metastatic tumors. Therefore, it is necessary to develop non-invasive in vivo imaging technology to quantitatively measure IGF1R levels in metastasized tumors, and to be able to predict response post therapy. The efficiency and stability of the in vivo delivery and targeting of AVE-1642 Qdots to tumor is currently under investigation in our laboratory.
References
Pegram MD, Pietras R, Bajamonde A, Klein P, Fyfe G (2005) Targeted therapy: wave of the future. J Clin Oncol 23:1776–1781
Sepp-Lorenzino L (1998) Structure and function of the insulin-like growth factor I receptor. Breast Cancer Res Treat 47:235–253
Cullen KJ, Yee D, Sly WS, Perdue J, Hampton B, Lippman ME, Rosen N (1990) Insulin-like growth factor receptor expression and function in human breast cancer. Cancer Res 50:48–53
Zhang H, Yee D (2004) The therapeutic potential of agents targeting the type I insulin-like growth factor receptor. Expert Opin Investig Drugs 13:1569–1577
Sachdev D, Li SL, Hartell JS, Fujita-Yamaguchi Y, Miller JS, Yee D (2003) A chimeric humanized single-chain antibody against the type I insulin-like growth factor (IGF) receptor renders breast cancer cells refractory to the mitogenic effects of IGF-I. Cancer Res 63:627–635
Maloney EK, McLaughlin JL, Dagdigian NE, Garrett LM, Connors KM, Zhou XM, Blattler WA, Chittenden T, Singh R (2003) An anti-insulin-like growth factor I receptor antibody that is a potent inhibitor of cancer cell proliferation. Cancer Res 63:5073–5083
Burtrum D, Zhu Z, Lu D, Anderson DM, Prewett M, Pereira DS, Bassi R, Abdullah R, Hooper AT, Koo H, Jimenez X, Johnson D, Apblett R, Kussie P, Bohlen P, Witte L, Hicklin DJ, Ludwig DL (2003) A fully human monoclonal antibody to the insulin-like growth factor I receptor blocks ligand-dependent signaling and inhibits human tumor growth in vivo. Cancer Res 63:8912–8921
Goetsch L, Gonzalez A, Leger O, Beck A, Pauwels PJ, Haeuw JF, Corvaia N (2005) A recombinant humanized anti-insulin-like growth factor receptor type I antibody (h7C10) enhances the antitumor activity of vinorelbine and anti-epidermal growth factor receptor therapy against human cancer xenografts. Int J Cancer 113:316–328
Wu JD, Odman A, Higgins LM, Haugk K, Vessella R, Ludwig DL, Plymate SR (2005) In vivo effects of the human type I insulin-like growth factor receptor antibody A12 on androgen-dependent and androgen-independent xenograft human prostate tumors. Clin Cancer Res 11:3065–3074
Rowinsky EK, Youssoufian H, Tonra JR, Solomon P, Burtrum D, Ludwig DL (2007) IMC-A12, a human IgG1 monoclonal antibody to the insulin-like growth factor I receptor. Clin Cancer Res 13:5549s–5555s
Ferrari M (2005) Cancer nanotechnology: opportunities and challenges. Nat Rev Cancer 5:161–171
Michalet X, Pinaud FF, Bentolila LA, Tsay JM, Doose S, Li JJ, Sundaresan G, Wu AM, Gambhir SS, Weiss S (2005) Quantum dots for live cells, in vivo imaging, and diagnostics. Science 307:538–544
Gao X, Yang L, Petros JA, Marshall FF, Simons JW, Nie S (2005) In vivo molecular and cellular imaging with quantum dots. Curr Opin Biotechnol 16:63–72
Jiang W, Papa E, Fischer H, Mardyani S, Chan WC (2004) Semiconductor quantum dots as contrast agents for whole animal imaging. Trends Biotechnol 22:607–609
Gao X, Cui Y, Levenson RM, Chung LW, Nie S (2004) In vivo cancer targeting and imaging with semiconductor quantum dots. Nat Biotechnol 22:969–976
Sachdev D, Singh R, Fujita-Yamaguchi Y, Yee D (2006) Down-regulation of insulin receptor by antibodies against the type I insulin-like growth factor receptor: implications for anti-insulin-like growth factor therapy in breast cancer. Cancer Res 66:1–12
Zhang H, Pelzer AM, Kiang DT, Yee D (2007) Down-regulation of type I insulin-like growth factor receptor increases sensitivity of breast cancer cells to insulin. Cancer Res 67:391–397
Byron SA, Horwitz KB, Richer JK, Lange CA, Zhang X, Yee D (2006) Insulin receptor substrates mediate distinct biological responses to insulin-like growth factor receptor activation in breast cancer cells. Br J Cancer 95:1220–1228
Rothenberger S, Iacopetta BJ, Kuhn LC (1987) Endocytosis of the transferrin receptor requires the cytoplasmic domain but not its phosphorylation site. Cell 49:423–431
Wu X, Liu H, Liu J, Haley KN, Treadway JA, Larson JP, Ge N, Peale F, Bruchez MP (2003) Immunofluorescent labeling of cancer marker Her2 and other cellular targets with semiconductor quantum dots. Nat Biotechnol 21:41–46
Tada H, Higuchi H, Wanatabe TM, Ohuchi N (2007) In vivo real-time tracking of single quantum dots conjugated with monoclonal anti-HER2 antibody in tumors of mice. Cancer Res 67:1138–1144
Lidke DS, Nagy P, Heintzmann R, Arndt-Jovin DJ, Post JN, Grecco HE, Jares-Erijman EA, Jovin TM (2004) Quantum dot ligands provide new insights into erbB/HER receptor-mediated signal transduction. Nat Biotechnol 22:198–203
Jaiswal JK, Mattoussi H, Mauro JM, Simon SM (2003) Long-term multiple color imaging of live cells using quantum dot bioconjugates. Nat Biotechnol 21:47–51
Chen M, von Mikecz A (2005) Formation of nucleoplasmic protein aggregates impairs nuclear function in response to SiO2 nanoparticles. Exp Cell Res 305:51–62
Pante N, Kann M (2002) Nuclear pore complex is able to transport macromolecules with diameters of about 39 nm. Mol Biol Cell 13:425–434
Kobayashi H, Hama Y, Koyama Y, Barrett T, Regino CA, Urano Y, Choyke PL (2007) Simultaneous multicolor imaging of five different lymphatic basins using quantum dots. Nano Lett 7:1711–1716
Ballou B, Lagerholm BC, Ernst LA, Bruchez MP, Waggoner AS (2004) Noninvasive imaging of quantum dots in mice. Bioconjug Chem 15:79–86
Ballou B, Ernst LA, Andreko S, Harper T, Fitzpatrick JA, Waggoner AS, Bruchez MP (2007) Sentinel lymph node imaging using quantum dots in mouse tumor models. Bioconjug Chem 18:389–396
Cai W, Shin DW, Chen K, Gheysens O, Cao Q, Wang SX, Gambhir SS, Chen X (2006) Peptide-labeled near-infrared quantum dots for imaging tumor vasculature in living subjects. Nano Lett 6:669–676
Jackson H, Muhammad O, Daneshvar H, Nelms J, Popescu A, Vogelbaum MA, Bruchez M, Toms S. A. (2007) Quantum dots are phagocytized by macrophages and colocalize with experimental gliomas. Neurosurgery 60:524–529; discussion 529–530
Gao XH, Cui YY, Levenson RM, Chung LWK, Nie SM (2004) In vivo cancer targeting and imaging with semiconductor quantum dots. Nat Biotechnol 22:969–976
Derfus AM, Chan WCW, Bhatia SN (2004) Probing the cytotoxicity of semiconductor quantum dots. Nano Lett 4:11–18
Rhyner MN, Smith AM, Gao XH, Mao H, Yang LL, Nie SM (2006) Quantum dots and multifunctional nanoparticles: new contrast agents for tumor imaging. Nanomedicine 1:209–217
Berns EM, Klijn JG, van Staveren IL, Portengen H, Foekens JA (1992) Sporadic amplification of the insulin-like growth factor 1 receptor gene in human breast tumors. Cancer Res 52:1036–1039
Acknowledgments
We thank Dr. Renato Baserga for R- cells. We are grateful to the services from the University of Minnesota Cancer Center Flow Cytometry Shared Resource and Confocal Microscopy Facility.Grant support: Department of Defense Post-doctoral Grant BC050548 (HZ) and R01CA74285 (DY), and Cancer Center Support Grant P30 077598.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, H., Sachdev, D., Wang, C. et al. Detection and downregulation of type I IGF receptor expression by antibody-conjugated quantum dots in breast cancer cells. Breast Cancer Res Treat 114, 277–285 (2009). https://doi.org/10.1007/s10549-008-0014-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-008-0014-5