Abstract
Glucocorticoids (GCs) are often prescribed in clinics but many adverse effects are also attributed to GCs. It is important to determine the role of GCs in the development of those adverse effects. Here, we investigated the impact of GCs on trivalent chromium (Cr) distribution in animals. Cr has been proposed to be important for proper insulin sensitivity, and deficits may lead to disruption of metabolism. For comparison, the effect of a high-fat diet on Cr modulation was also evaluated. C57BL/6JNarl mice were fed regular or high-fat diets for 12 weeks and further grouped for treatment with prednisolone or saline. Cr levels in tissues were determined 12 h after the treatments. Interestingly, prednisolone treatment led to significantly reduced Cr levels in fat tissue in mice fed regular diets; compared to the high-fat diet alone, prednisolone plus the high-fat diet led to a further reduction in Cr levels in the liver, muscle, and fat. Notably, a single dose of prednisolone was linked with elevated Cr levels in the thigh bones of mice fed by either regular or high-fat diets. In conclusion, this report has provided evidence that prednisolone in combination with a high-fat diet effects modulation of Cr levels in selected tissues.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glucocorticoid (GCs) hormones are secreted by the adrenal cortex, and they exert essential influences on glucose metabolism and energy homeostasis (Boyle and Cryer 1991; De Feo et al. 1989; McMahon et al. 1988). They also possess potent anti-inflammatory and immunosuppressive properties and are frequently used in the clinic to reduce inflammation or immune activation (Barnes 1998; Coutinho and Chapman 2011; Saklatvala 2002; Stahn et al. 2007). However, many adverse effects are also attributed to GCs. These include GC-induced osteoporosis (Bonacci et al. 2003; Mazziotti et al. 2006), central adiposity (Rockall et al. 2003), dyslipidemia (Taskinen et al. 1983; Wajchenberg 2000), skeletal muscle wasting (Khaleeli et al. 1983), insulin resistance (Schacke et al. 2002), tendency toward hyperglycemia (McMahon et al. 1988; van Raalte et al. 2009), glucose intolerance, and overt diabetes (Schacke et al. 2002). Of note, among these adverse effects, GC-induced osteoporosis, glucose intolerance, and diabetes can lead to severe medical problems (Schacke et al. 2002; Bonacci et al. 2003; Mazziotti et al. 2006). Excessive GC levels are known to contribute to some GC-related osteoporosis (Delany et al. 1994; Lukert and Raisz 1990), by stimulating bone resorption by osteoclasts, decreasing bone mass by inhibiting osteoblasts, and decreasing intestinal calcium resorption (Olbricht and Benker 1993; Lukert and Raisz 1994; Canalis 1996; Gulko and Mulloy 1996). In addition, insulin activity has been suggested to affect bone metabolism in that physiological insulin concentrations can stimulate collagen production by osteoblasts and insulin may reduce bone resorption by decreasing parathyroid hormone-stimulated osteoclast cell formation (McCarty 1995).
Currently, many efforts are focused on understanding and diminishing GC-induced adverse effects (Stahn et al. 2007; Clore and Thurby-Hay 2009; van Raalte et al. 2009). Many previous reports have indicated a link between trivalent chromium (Cr) deficiency and type 2 diabetes or insulin resistance (Brown et al. 1986; Freund et al. 1979; Jeejeebhoy et al. 1977; Vincent 2000). Moreover, many Cr supplements can ease some type 2 diabetes-related disorders, especially in animal models. These models all indicate that Cr has a significant anti-diabetic potential (Chen et al. 2009b, 2010; Cefalu et al. 2002; Morris et al. 1993; Striffler et al. 1995; Krol and Krejpcio 2011; Sahin et al. 2011). Intriguingly, a recent report indicated that Cr is not an essential trace element in rats, and the same group concluded that supranutritional amounts of Cr in the diet had the pharmacological effect of increasing insulin sensitivity (Di Bona et al. 2011). However, in a human case report, Cr administration with i.v. decreased the insulin requirements, and this improves glucose control (Phung et al. 2010); this supplementations also enhance insulin sensitivity in patients with type 2 diabetes, and subject phenotypes have been shown to be very important when assessing the clinical responses to Cr (Wang et al. 2007). Moreover, many important reports also provide clues that Cr indeed plays a role in metabolism. For example, Cr supplementation protects against renal dysfunction by modulation of NF-kappa B pathway in high-fat and streptozotocin-induced diabetic rats (Selcuk et al. 2012); Cr supplement also modulates serotonergic properties and carbohydrate metabolism in a diabetic rat model (Komorowski et al. 2012). Moreover, another report indicates that Cr supplementation can lower blood levels of proinflammatory cytokines (TNF-alpha, IL-6, C-reactive protein), oxidative stress, and lipids levels in diabetic rats. (Jain et al. 2007). Taken together, these reports have supported that Cr is an important co-factor or pharmacological agent for proper carbohydrate metabolism and also for effective insulin responses. These influences could be more important in subjects suffering from impaired insulin activity or dietary carbohydrate stress. Moreover, high carbohydrate intake and some stressful dietary situations have also been reported to promote the excretion of Cr in the urine (Anderson 1997; Morris et al. 1988). Interestingly, our raw data also showed that a high-fat diet plays a role in deterioration of Cr accumulation in some insulin-sensitive tissues. Therefore, this study aimed to determine the influence of GCs or a high-fat diet on altered Cr distribution in tissues. This could further reveal the mechanisms underlying certain GCs-related disorders, and potentially explain some GC-induced side effects in terms of Cr modulation in animals.
Materials and methods
Animal, diet and tissue preparation
C57BL/6JNarl (C57BL) and KK/H1 J (KK) mice were used in this study. Animals were maintained in a room at a mean constant temperature of 22 ± 2 °C with a 12-hour light–dark cycle and free access to food and water. C57BL mice were grouped and fed a regular diet (5008 Rodent LabDiet) or a high-fat diet (high-fat Rodent TestDiet, 67 % of calories provided by fat) for 12 weeks. The KK mice were also grouped and fed a mouse diet (18.3 % protein, 25.8 % fat, 55.9 carbohydrates; gross energy, 4.35 kcal/mg) or a high-fat diet (16.3 % protein, 66.6 % fat, 17.1 % carbohydrate; gross energy, 7.1 kcal/mg) for 12 weeks. Each group was further divided into 2 groups and injected with prednisolone or saline (control) as described below. Number of animals in each experiment is indicated within each figure. In all animal experiments, the authors adhered to the guidelines for the Care and Use of Laboratory Animals, as recommended by the Taiwanese government.
Injections of prednisolone and biochemical analysis
After 12 weeks on a specific diet described above, feeding groups were divided into 2 groups. Mice were then intra-peritoneally injected with prednisolone (2 mg/kg body weight; Donison) or saline (control group). Twelve hours after injection, mice were fasted for another 12 h, and blood samples were collected from tail veins and subjected to biochemical analysis. Blood glucose was determined using glucose oxidase reaction; blood insulin levels were determined using a commercial kit (Rat Insulin ELISA kit, Crystal Chem Inc.). Serum triacetylglycerol levels were determined using clinical chemistry analyzers (Hitachi Autoanalyzer 7070 and Roche I 800). Mice were sacrificed under anesthesia, and the thigh bone, epididymal fat, liver, and quadriceps were collected and stored at −20 °C until further Cr analysis.
Cr analysis
After the experiments, the samples of blood and tissues (liver, muscle, fat, and bone) were collected. Then, the collected samples (250 μl of blood, 0.1 g of tissues) were digested in 65 % nitric acid (1 ml) and heated at 65 °C for 1 h. The digested solutions were diluted with distilled water up to 5 ml before measurement. The calibration solutions were prepared from 1,000 μl/ml stock solutions from Merck by dilution with distilled water. Chromium concentrations of standards and samples were determined using graphite furnace atomic absorption spectrophotometry (Hitachi Z-2000 series polarized Zeeman atomic absorption spectrophotometer). In this assay, no tissue retention studies were done. Therefore, the data represent not absolute chromium levels in tissue that can be compared to other literature values.
Insulin resistance analysis
The homeostasis model assessment-estimated insulin resistance (HOMA-IR) has been widely used for the estimation of insulin resistance in research (Albreda et al. 2000, Mao et al. 2007, Vogeser et al. 2007). Therefore, insulin resistance of mice was evaluated using homeostasis model assessment (HOMA-IR). Fasting plasma glucose (FPG: mmol/l) and fasting plasma insulin concentration (FPI: mU/l) were determined. Insulin resistance was calculated as follows: FPI × FPG/22.5 as reported previously (Matthews et al. 1985).
Statistical analysis
Data are expressed as mean ± standard deviation (±S.D.), and statistical analyses were performed by the Student’s t test using Microsoft Excel. A P value of less than 0.05 or 0.01 was considered significant. Otherwise, data from four groups were analyzed by using the one-way ANOVA with a post hoc comparison analysis.
Results
The effects of prednisolone in combination with a high-fat diet on Cr distribution in C57BL/6 J mice
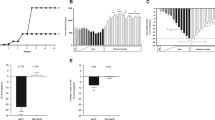
To determine the role of prednisolone in modulation of Cr levels in tissues, the effects of prednisolone on Cr mobilization or accumulation in the epididymal fat, quadriceps, liver, blood, and thigh bone were evaluated. First, in mice fed regular diets, Cr levels in fat (epididymal fat) were significantly reduced after a single dose of prednisolone (Fig. 1). However, Cr accumulation in the liver, muscle (quadriceps), bone (thigh bone), and blood were unaffected by this treatment. This result implies that prednisolone treatments indeed have an impact on Cr accumulation in certain tissues. The high-fat diet, in our preliminary data, has been found to reduce Cr accumulation in the liver, muscle, and bone tissues (data not shown). Here, in line with our previous data, a long-term high-fat diet (12 weeks) significantly reduced Cr levels in the liver, muscle, and bone (Fig. 2a). Intriguingly, prednisolone treatment can further diminish Cr accumulation in tissues, and prednisolone plus the high-fat diet led to considerably reduced Cr accumulation in the liver, fat and muscle (Fig. 2b). Therefore, these findings indicate that prednisolone and high-fat diets all tended to reduce Cr levels in selected insulin-sensitive tissues.
Chromium concentrations in fat are reduced by a single dose of prednisolone in mice fed regular diets. C57BL/6 J mice (n = 20) were grouped and fed regular diets for 12 weeks. Mice were further divided into two groups and injected either with saline or prednisolone as described in Materials and methods section. Tissue samples were harvested 24 h after injection and chromium levels were determined. Values are expressed as mean ± S.D. *P < 0.05 versus control
Prednisolone treatment worsens Cr levels in the liver, muscle, and fat in mice fed a high-fat diet. a C57BL/6JNarl mice (n = 18) were grouped and fed normal or high-fat diets for 12 weeks. Tissue samples were collected, and chromium levels were determined. b C57BL/6JNarl mice (n = 18) were fed high-fat diets for 12 weeks. Mice were further divided into groups and injected either with saline (control) or prednisolone as described in Materials and methods section. Tissue samples were harvested 24 h after injection and chromium levels were determined. Values are expressed as mean ± S.D. *P < 0.05, **P < 0.01, ***P < 0.001 versus normal diets or control group
GC treatment has been linked to GC-induced osteoporosis. Thus, the impact of prednisolone and the high-fat diet on Cr levels in the thigh bones was also evaluated in this study. Interestingly, prednisolone treatment seems to exert profound effects on Cr levels; Cr levels in the thigh bones were increased moderately (Fig. 1) or significantly (Fig. 2b) in 2 different animal models. In this study, Cr levels were considerably promoted in C57BL/6 J mice (Fig. 2a, b) and KK mice (Fig. 4a, b) by prednisolone treatment. In contrast, Cr levels in the thigh bone were reduced considerably by the high-fat diet in both animal models (Fig. 2a; data in KK model are not shown). These findings indicate that prednisolone affects Cr levels in the thigh bone.
The effects of prednisolone in combination with a high-fat diet on blood insulin, fasting glucose, triacetylglycerol, and insulin resistance
Blood insulin, fasting glucose, triacetylglycerol, and insulin resistance index (assessed by HOMA-IR) were examined in prednisolone-treated C57BL mice that were fed regular or high-fat diets. Compared to the mice fed a regular diet (Fig. 3), mice fed a high-fat diet exhibited significantly increased blood insulin (Fig. 3a), fasting blood glucose (Fig. 3b), and triacetylglycerol (Fig. 3c), and higher insulin resistance values (Fig. 3d). These data confirmed the adverse effects of high-fat diet in terms of diabetogenic-related indices (Fig. 3). High-fat diet plus prednisolone treatment worsened blood insulin, triacetylglycerol, and insulin resistance index.
Levels of blood insulin, triacetylglycerol, and insulin resistance are elevated by the combination of prednisolone and a high-fat diet. C57BL/6JNarl mice were grouped and fed normal diets or high-fat diets for 12 weeks. Mice were then treated either with saline or prednisolone for 24 h. Samples were harvested and blood insulin (a), fasting blood glucose (b), triacetylglycerol (c), and insulin resistance (d) were determined as described in Materials and methods section. Values are expressed as mean ± S.D. A one-way ANOVA with a post hoc comparison analysis were conducted to analyze the four groups. a, b, c different superscript letters indicate significant difference between two groups (P < 0.05)
The effects of prednisolone in combination with a high-fat diet on Cr distribution in KK/H1 J mice
High-fat diets have been shown to significantly promote the development of hyperglycemia, dyslipidemia, hyperinsulinemia, and insulin-resistant C57BL mice (Fig 3). Moreover, prednisolone treatment further diminished Cr accumulation in insulin-sensitive tissues in high-fat diet fed C57BL mice (Fig. 2b). Thus, we used genetically insulin-resistant KK/HlJ mice to explore whether the prednisolone treatment aggravated the diminution of Cr accumulation in high-fat diet fed KK mice. In KK mice fed the mouse diet (about 25 % fat, Fig. 4a), prednisolone treatment resulted in significantly decreased Cr levels in muscle but an increase in bone (Fig. 4a). Moreover, prednisolone lowered Cr accumulation in KK mice fed a high-fat diet (about 66 % fat), significantly reducing Cr concentrations in muscle and fat (Fig. 4b). Therefore, these findings are similar to those obtained using C57BL mice. Compared to KK mice fed normal mouse diet, high-fat diet significantly decreased Cr concentration in the liver, epididymal fat, and thigh bone. However, Cr levels in muscle and blood were unaffected by the high-fat diet (data not shown). Thus, the findings from KK mice also support the contention that the high-fat diet tends to reduce Cr accumulation in insulin-sensitive tissues and the thigh bone.
Chromium distribution in tissues is modulated by a single dose of prednisolone in KK/H1 J mice. a KK/H1 J mice (n = 20) were grouped and fed a mouse diet (25.8 % fat) for 12 weeks. Mice were further divided into 2 groups and injected with either saline or prednisolone as described in Materials and methods section. Tissue samples were harvested 24 h after injection and chromium levels determined. b KK/H1 J mice (n = 16) were fed a high-fat diet (66.6 % fat) and were processed as described in (a). Values are expressed as mean ± S.D. *P < 0.05 and **P < 0.01 versus control
Discussion
We have demonstrated here that prednisolone treatment in animals fed high-fat diets can lead to reduced Cr levels in insulin-sensitive tissues, while tending to elevate Cr levels in the thigh bone. To our knowledge, this is the first study to examine the effects of prednisolone on Cr distribution in animals. Since the tested animals received a single dose of prednisolone, we believe that the impact of prednisolone on Cr modulation could be augmented in subjects receiving multiple doses of prednisolone. Therefore, the effects of different dosages, durations, or types of steroids on Cr mobilization should be further investigated.
Intriguingly, a recent report demonstrated that Cr is not an essential trace element for rats and concluded that effects of supranutritional Cr in the diet should be regarded as pharmacological effects (Di Bona et al. 2011). However, as described in the introduction section, many previous reports have provided evidences that Cr is a co-factor, especially in subjects that have suffered certain disorders. For more clues, Cr has been reported to activate glucose transporter 4 trafficking and enhance insulin-stimulated glucose transport in an in vitro cell assay (Chen et al. 2006). Moreover, Cr supplementation can attenuate hepatic damage in a rat model of chronic cholestasis (Chen et al. 2009a) and help to attenuate high-fat diet-induced non-alcoholic fatty liver disease in KK/HlJ mice (Chen et al. 2010). Furthermore, Cr supplementation enhances insulin signaling in skeletal muscle in obese KK/HlJ diabetic mice (Chen et al. 2009b). Thus, the beneficial effects of Cr on insulin-related functions are more convincingly revealed in rodent models and also in several recent human reports (Phung et al. 2010; Wang et al. 2007).
This study demonstrated that prednisolone challenge leads to reduced Cr levels in insulin-sensitive tissues, especially in mice fed a high-fat diet. This kind of treatment may gradually impair insulin responses, especially in patients who receive long-term GC treatment. On the other hand, a high-fat diet has also been shown here to severely reduce Cr concentrations in insulin-sensitive tissues, and this manifests a link between impaired insulin responses and a high-fat diet. Indeed, through the studies of some diabetogenic indexes of mice fed high-fat diets, we have learned that this kind of diet contributes to elevated levels of blood insulin, fasting glucose, and triacetylglycerol, and to insulin resistance. Consistent with those observations, this report indicates here that the combination of a high-fat diet and prednisolone led to considerable decreased Cr levels in some insulin-sensitive tissues, accompanied by decreased blood insulin, fasting glucose, triacetylglycerol, and insulin resistance. Therefore, this study also partially supports a link between Cr and some kinds of metabolic disorders. Interestingly, Cr has been suggested to play a role in preservation of bone density through anabolic effects of insulin on bone metabolism (McCarty 1995). Therefore, it is assumed here that the mechanisms by which GCs elicit osteoporosis may include Cr modulation, and in some way the indirect reduction of insulin sensitivity.
Some nutrients, macronutrients, and several trace minerals are linked with the constitution of the bone matrix (Saltman and Strause 1993; Heaney et al. 1982; Arnaud and Sanchez 1990; Gur et al. 2002). However, direct role of Cr in the bone matrix is limited. Although a recent report shows that Cr is not an essential element for rats in terms of body composition, glucose metabolism, or insulin sensitivity (Di Bona et al. 2011), the effect of Cr on bone quality was not addressed in that study. Our data show that prednisolone treatment can lead to considerably increased Cr levels within bone. Possibly, these elevated levels of Cr in bone may affect the interaction between Cr and other bone minerals that may indirectly modulate bone density. Nevertheless, the relationship between bone Cr levels and bone quality should be further investigated.
Physiological insulin has been reported previously to indirectly affect Cr mobilization in insulin-sensitive tissues; this may affect the role of insulin in glucose transport or the transferrin-recycling pathway (Borguet et al. 1990; Clodfelder et al. 2001; Clodfelder and Vincent 2005; Sun et al. 2000; Vincent 2000). This study shows that prednisolone treatment plays a role in controlling Cr levels in insulin-sensitive tissues or the thigh bone. Thus, it is assumed that other hormones that physiologically modulate carbohydrate metabolism may partially contribute to Cr mobilization or distribution.
In conclusion, this study has demonstrated that prednisolone treatment can alter Cr levels both in insulin-sensitive tissues and in the thigh bone, and these affects can be augmented in mice fed a high-fat diet. These influences are suggested to partially contribute to some of the adverse effects of GCs, and we believe that the effects of prednisolone on Cr modulation could accumulate in animals undergoing long-term GCs therapy. The findings of this study should motivate further investigations of the influences of dose, duration of treatment, and type of steroids on Cr modulation. Moreover, whether Cr supplementation can partially overcome adverse effects of GC treatments should be further investigated.
References
Albreda M, Rodriguez-Espinosa J, Murugo M, Leiva AD, Corcoy R (2000) Assessment of insulin sensitivity and beta-cell function from measurements in the fasting state and during an oral glucose tolerance test. Diabetologia 43:1507–1511
Anderson RA (1997) Chromium as an essential nutrient for humans. Regul Toxicol Pharmacol 26(1):S35–S41
Arnaud CD, Sanchez SD (1990) The role of calcium in osteoporosis. Annu Rev Nutr 10:397–414. doi:10.1146/annurev.nu.10.070190.002145
Barnes PJ (1998) Anti-inflammatory actions of glucocorticoids: molecular mechanisms. Clin Sci (Lond) 94(6):557–572
Bonacci JV, Harris T, Wilson JW, Stewart AG (2003) Collagen-induced resistance to glucocorticoid anti-mitogenic actions: a potential explanation of smooth muscle hyperplasia in the asthmatic remodelled airway. Br J Pharmacol 138(7):1203–1206
Borguet F, Cornelis R, Lameire N (1990) Speciation of chromium in plasma and liver tissue of endstage renal failure patients on continuous ambulatory peritoneal dialysis. Biol Trace Elem Res 26–27:449–460
Boyle PJ, Cryer PE (1991) Growth hormone, cortisol, or both are involved in defense against, but are not critical to recovery from, hypoglycemia. Am J Physiol 260(3 Pt 1):E395–E402
Brown RO, Forloines-Lynn S, Cross RE, Heizer WD (1986) Chromium deficiency after long-term total parenteral nutrition. Dig Dis Sci 31(6):661–664
Canalis E (1996) Clinical review 83: mechanisms of glucocorticoid action in bone: implications to glucocorticoid-induced osteoporosis. J Clin Endocrinol Metab 81(10):3441–3447
Cefalu WT, Wang ZQ, Zhang XH, Baldor LC, Russell JC (2002) Oral chromium picolinate improves carbohydrate and lipid metabolism and enhances skeletal muscle Glut-4 translocation in obese, hyperinsulinemic (JCR-LA corpulent) rats. J Nutr 132(6):1107–1114
Chen G, Liu P, Pattar GR, Tackett L, Bhonagiri P, Strawbridge AB, Elmendorf JS (2006) Chromium activates glucose transporter 4 trafficking and enhances insulin-stimulated glucose transport in 3T3-L1 adipocytes via a cholesterol-dependent mechanism. Mol Endocrinol 20(4):857–870. doi:10.1210/me.2005-0255
Chen WY, Chen CJ, Liao JW, Mao FC (2009a) Chromium attenuates hepatic damage in a rat model of chronic cholestasis. Life Sci 84(17–18):606–614. doi:10.1016/j.lfs.2009.02.003
Chen WY, Chen CJ, Liu CH, Mao FC (2009b) Chromium supplementation enhances insulin signalling in skeletal muscle of obese KK/HlJ diabetic mice. Diabetes Obes Metab 11(4):293–303
Chen WY, Chen CJ, Liu CH, Mao FC (2010) Chromium attenuates high-fat diet-induced nonalcoholic fatty liver disease in KK/HlJ mice. Biochem Biophys Res Commun 397(3):459–464
Clodfelder BJ, Vincent JB (2005) The time-dependent transport of chromium in adult rats from the bloodstream to the urine. J Biol Inorg Chem 10(4):383–393
Clodfelder BJ, Emamaullee J, Hepburn DD, Chakov NE, Nettles HS, Vincent JB (2001) The trail of chromium(III) in vivo from the blood to the urine: the roles of transferrin and chromodulin. J Biol Inorg Chem 6(5–6):608–617
Clore JN, Thurby-Hay L (2009) Glucocorticoid-induced hyperglycemia. Endocr Pract 15(5):469–474
Coutinho AE, Chapman KE (2011) The anti-inflammatory and immunosuppressive effects of glucocorticoids, recent developments and mechanistic insights. Mol Cell Endocrinol 335(1):2–13
De Feo P, Perriello G, Torlone E, Ventura MM, Fanelli C, Santeusanio F, Brunetti P, Gerich JE, Bolli GB (1989) Contribution of cortisol to glucose counterregulation in humans. Am J Physiol 257(1 Pt 1):E35–E42
Delany AM, Dong Y, Canalis E (1994) Mechanisms of glucocorticoid action in bone cells. J Cell Biochem 56(3):295–302. doi:10.1002/jcb.240560304
Di Bona KR, Love S, Rhodes NR, McAdory D, Sinha SH, Kern N, Kent J, Strickland J, Wilson A, Beaird J, Ramage J, Rasco JF, Vincent JB (2011) Chromium is not an essential trace element for mammals: effects of a “low-chromium” diet. J Biol Inorg Chem 16(3):381–390
Freund H, Atamian S, Fischer JE (1979) Chromium deficiency during total parenteral nutrition. JAMA 241(5):496–498
Gulko PS, Mulloy AL (1996) Glucocorticoid-induced osteoporosis: pathogenesis, prevention and treatment. Clin Exp Rheumatol 14(2):199–206
Gur A, Colpan L, Nas K, Cevik R, Sarac J, Erdogan F, Duz MZ (2002) The role of trace minerals in the pathogenesis of postmenopausal osteoporosis and a new effect of calcitonin. J Bone Miner Metab 20(1):39–43. doi:10.1007/s007740200005
Heaney RP, Gallagher JC, Johnston CC, Neer R, Parfitt AM, Whedon GD (1982) Calcium nutrition and bone health in the elderly. Am J Clin Nutr 36(5 Suppl):986–1013
Jain SK, Rains JL, Croad JL (2007) Effect of chromium niacinate and chromium picolinate supplementation on lipid peroxidation, TNF-alpha, IL-6, CRP, glycated hemoglobin, triglycerides, and cholesterol levels in blood of streptozotocin-treated diabetic rats. Free Radic Biol Med 43(8):1124–1131. doi:10.1016/j.freeradbiomed.2007.05.019
Jeejeebhoy KN, Chu RC, Marliss EB, Greenberg GR, Bruce-Robertson A (1977) Chromium deficiency, glucose intolerance, and neuropathy reversed by chromium supplementation, in a patient receiving long-term total parenteral nutrition. Am J Clin Nutr 30(4):531–538
Khaleeli AA, Edwards RH, Gohil K, McPhail G, Rennie MJ, Round J, Ross EJ (1983) Corticosteroid myopathy: a clinical and pathological study. Clin Endocrinol 18(2):155–166
Komorowski JR, Tuzcu M, Sahin N, Juturu V, Orhan C, Ulas M, Sahin K (2012) Chromium picolinate modulates serotonergic properties and carbohydrate metabolism in a rat model of diabetes. Biol Trace Elem Res. doi:10.1007/s12011-012-9393-x
Krol E, Krejpcio Z (2011) Evaluation of anti-diabetic potential of chromium(III) propionate complex in high-fat diet fed and STZ injected rats. Food Chem Toxicol 49(12):3217–3223. doi:10.1016/j.fct.2011.09.006
Lukert BP, Raisz LG (1990) Glucocorticoid-induced osteoporosis: pathogenesis and management. Ann Intern Med 112(5):352–364
Lukert BP, Raisz LG (1994) Glucocorticoid-induced osteoporosis. Rheum Dis Clin North Am 20(3):629–650
Mao XQ, Wu Y, Wu K, Liu M, Zhang JF, Zou F, Ou-Yang JP (2007) Astragalus polysaccharide reduces hepatic endoplasmic reticulum stress and restores glucose homeostasis in a diabetic KKAy mouse model. Acta Pharmacol Sin 28:1947–1956
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419
Mazziotti G, Angeli A, Bilezikian JP, Canalis E, Giustina A (2006) Glucocorticoid-induced osteoporosis: an update. Trends Endocrinol Metab 17(4):144–149
McCarty MF (1995) Anabolic effects of insulin on bone suggest a role for chromium picolinate in preservation of bone density. Med Hypotheses 45(3):241–246
McMahon M, Gerich J, Rizza R (1988) Effects of glucocorticoids on carbohydrate metabolism. Diabetes Metab Rev 4(1):17–30
Morris BW, Griffiths H, Kemp GJ (1988) Effect of glucose loading on concentrations of chromium in plasma and urine of healthy adults. Clin Chem 34(6):1114–1116
Morris BW, MacNeil S, Stanley K, Gray TA, Fraser R (1993) The inter-relationship between insulin and chromium in hyperinsulinaemic euglycaemic clamps in healthy volunteers. J Endocrinol 139(2):339–345
Olbricht T, Benker G (1993) Glucocorticoid-induced osteoporosis: pathogenesis, prevention and treatment, with special regard to the rheumatic diseases. J Intern Med 234(3):237–244
Phung OJ, Quercia RA, Keating K, Baker WL, Bell JL, White CM, Coleman CI (2010) Improved glucose control associated with i.v. chromium administration in two patients receiving enteral nutrition. Am J Health Syst Pharm 67(7):535–541. doi:10.2146/ajhp090109
Rockall AG, Sohaib SA, Evans D, Kaltsas G, Isidori AM, Monson JP, Besser GM, Grossman AB, Reznek RH (2003) Computed tomography assessment of fat distribution in male and female patients with Cushing’s syndrome. Eur J Endocrinol 149(6):561–567
Sahin K, Tuzcu M, Orhan C, Agca CA, Sahin N, Guvenc M, Krejpcio Z, Staniek H, Hayirli A (2011) The effects of chromium complex and level on glucose metabolism and memory acquisition in rats fed high-fat diet. Biol Trace Elem Res 143(2):1018–1030. doi:10.1007/s12011-010-8905-9
Saklatvala J (2002) Glucocorticoids: do we know how they work? Arthritis Res 4(3):146–150
Saltman PD, Strause LG (1993) The role of trace minerals in osteoporosis. J Am Coll Nutr 12(4):384–389
Schacke H, Docke WD, Asadullah K (2002) Mechanisms involved in the side effects of glucocorticoids. Pharmacol Ther 96(1):23–43
Selcuk MY, Aygen B, Dogukan A, Tuzcu Z, Akdemir F, Komorowski JR, Atalay M, Sahin K (2012) Chromium picolinate and chromium histidinate protects against renal dysfunction by modulation of NF-kappaB pathway in high-fat diet fed and Streptozotocin-induced diabetic rats. Nutr Metab (Lond) 9(1):30. doi:10.1186/1743-7075-9-30
Stahn C, Lowenberg M, Hommes DW, Buttgereit F (2007) Molecular mechanisms of glucocorticoid action and selective glucocorticoid receptor agonists. Mol Cell Endocrinol 275(1–2):71–78
Striffler JS, Law JS, Polansky MM, Bhathena SJ, Anderson RA (1995) Chromium improves insulin response to glucose in rats. Metabolism 44(10):1314–1320
Sun Y, Ramirez J, Woski SA, Vincent JB (2000) The binding of trivalent chromium to low-molecular-weight chromium-binding substance (LMWCr) and the transfer of chromium from transferrin and chromium picolinate to LMWCr. J Biol Inorg Chem 5(1):129–136
Taskinen MR, Nikkila EA, Pelkonen R, Sane T (1983) Plasma lipoproteins, lipolytic enzymes, and very low density lipoprotein triglyceride turnover in Cushing’s syndrome. J Clin Endocrinol Metab 57(3):619–626
van Raalte DH, Ouwens DM, Diamant M (2009) Novel insights into glucocorticoid-mediated diabetogenic effects: towards expansion of therapeutic options? Eur J Clin Invest 39(2):81–93
Vincent JB (2000) The biochemistry of chromium. J Nutr 130(4):715–718
Vogeser M, Kοnig D, Frey I, Predel HG, Parhofer KG, Berg A (2007) Fasting serum insulin and the homeostasis model of insulin resistance (HOM-IR) in the monitoring of lifestyle interventions in obese persons. Clin Biochem 40:964–968
Wajchenberg BL (2000) Subcutaneous and visceral adipose tissue: their relation to the metabolic syndrome. Endocr Rev 21(6):697–738
Wang ZQ, Qin J, Martin J, Zhang XH, Sereda O, Anderson RA, Pinsonat P, Cefalu WT (2007) Phenotype of subjects with type 2 diabetes mellitus may determine clinical response to chromium supplementation. Metabolism 56(12):1652–1655. doi:10.1016/j.metabol.2007.07.007
Acknowledgments
This work was partially supported by the National Science Council (grants NSC100-2320-B-562-001 and NSC 100-2313-B-562-001) and the Ministry of Education (Taiwan) under the ATU plan, and also supported by a Grant from St. Mary’s Medicine, Nursing and Management College (SMC100-I-14).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, PW., Lin, C., Chen, CD. et al. Chromium levels in insulin-sensitive tissues and the thigh bone are modulated by prednisolone and high-fat diets in mice. Biometals 26, 347–354 (2013). https://doi.org/10.1007/s10534-013-9621-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-013-9621-7