Abstract
This study uses an event-based approach to examine individual, relationship, and contextual correlates of heterosexual condom use among homeless men. Structured interviews were conducted with a predominantly African American sample of 305 men recruited from meal lines in the Skid Row area of Los Angeles. Men reported on their most recent heterosexual event involving vaginal or anal intercourse. Adjusting for demographic characteristics only, condom use was more likely when men had higher condom use self-efficacy, greater HIV knowledge, or talked to their partner about condoms prior to sex. Condom use was less likely when men held more negative attitudes towards condoms, the partner was considered to be a primary/serious partner, hard drug use preceded sex, or sex occurred in a public setting. Condom attitudes, self-efficacy, partner type, and communication were the strongest predictors of condom use in a multivariate model that included all of the above-mentioned factors. Associations of unprotected sex with hard drug use prior to sex and having sex in public settings could be accounted for by lower condom self-efficacy and/or less positive condom attitudes among men having sex under these conditions. Results suggest that it may be promising to adapt existing, evidence-based IMB interventions for delivery in non-traditional settings that are frequented by men experiencing homelessness to achieve HIV risk reduction and thus reduce a significant point of disparity for the largely African American population of homeless men.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Individuals who are homeless have higher rates of HIV/AIDS than those who are stably housed [1]. A study of homeless and marginally housed individuals in San Francisco, for example, reported an overall seroprevalence of 10.5%—five times greater than in the general San Francisco population [2]. Homeless individuals typically reside in impoverished, urban areas with high HIV prevalence, and are more likely to engage in drug use, needle use, and sexual risk behavior than low-income housed individuals [3–8]. There is an urgent need for public health programs to develop strategies that address HIV risk among homeless individuals [9–11], and better understanding the determinants of HIV risk behavior in this stigmatized and vulnerable population can help inform these efforts. Both homelessness and HIV/AIDS disproportionately impact African American men [12, 13], contributing to the well-established racial disparities in morbidity among men.
In this study we focus specifically on understanding homeless men’s condom use with their female partners. Men who have sex with women (MSW) have been relatively understudied in the HIV epidemic in the U.S. compared to men who have sex with men (MSM), yet this group is a critical link in understanding and preventing the transmission of HIV [14]. Heterosexual contact accounts for approximately one-third of new annual HIV diagnoses in the United States [12]. Men who have sex with men and who self-identify as heterosexual or otherwise engage in sex with women are at high risk for both acquiring and transmitting HIV to their female sex partners [15–17]. An estimated 80% of new HIV infections among women in the US are due to high-risk heterosexual contact [18].
Studies examining the predictors of condom use have employed a variety of designs, but event-based approaches can be especially informative. By asking respondents to report on specific sexual events, it is possible to: (a) establish a temporal pairing between condom use and other behaviors occurring during the sexual event (e.g., substance use, communication about condoms) that is a necessary condition for inferring a causal link between the behaviors; and (b) identify other specific features of the event that may be important determinants of condom use and would otherwise be overlooked in global association studies. Identifying unique contextual characteristics of sexual events is especially important for marginalized populations, such as homeless men, that may differ from the general population in terms of the circumstances under which sex occurs. Homeless men who are living on the streets, for example, may be more likely to have sexual encounters that are unplanned, lacking in privacy, and with casual or sex trade partners. If these types of contextual characteristics predict condom use, it would suggest that a generic approach to HIV/AIDS prevention may be less effective than one that targets the specific needs and circumstances of this population.
The work of Tortu, McMahon and colleagues provides a useful framework for examining the event-based determinants of condom use in high-risk populations by simultaneously focusing on characteristics of the individual (e.g., demographics, attitudes), the relationship (e.g., type, qualities), and the sexual event itself (e.g., location, behaviors that occurred) [19, 20]. We have applied this framework to our own research examining the individual, relationship, and contextual correlates of condom use among sheltered homeless women and homeless youth [21, 22]. Across these and other event-based studies, condom use tends to be associated with the individual’s condom-related attitudes and whether the couple discussed condoms prior to having sex, consistent with the larger literature demonstrating the relevance of these factors across a range of populations [23, 24]. However, other important predictors of condom use to emerge from this literature include partner type [20–22, 25], the setting of the sexual event [19, 21], whether substances were used prior to having sex [19, 21, 25, 26], and what sexual activities occurred during the event [19, 20].
One notable gap in the field’s understanding of condom use among MSW is the potential impact of men’s gender-related attitudes and beliefs, such as traditional masculine ideologies and power dynamics within sexual relationships [27–29]. The dominant social cognitive theories of HIV risk do not attend to norms about gender and power in relationships and for this reason may provide too limited an understanding of heterosexual risk behavior [30]. A small number of studies have shown that traditional gender role norms run counter to safer sex practices [31–33]. However, results from this literature are often based on student samples and thus may not generalize to men who are older, less educated, and impoverished.
Towards the goal of reducing health disparities surrounding HIV risk, the present study uses an event-based approach to better understand the factors that influence condom use during specific sexual events among homeless MSW. In a probability sample of mostly African American homeless men, systematically recruited from meal lines in Los Angeles, we examine key individual, relationship, and contextual characteristics that existing literature and our formative research suggest may be particularly relevant to heterosexual condom use in this population. This approach is intended to provide a more comprehensive understanding of risk and protective factors that influence condom use among homeless MSW, as well as factors that are not particularly relevant for this population.
Methods
Study Participants
Participants were 305 homeless men randomly sampled and interviewed in the Skid Row area of Los Angeles. This area is home to the highest concentration of homeless persons in Los Angeles County. Men were eligible if they were age 18 or older, could complete an interview in English, and experienced homelessness in the past 12 months (defined as spending at least one night on the street, or in a shelter, mission, vehicle, public or abandoned building, or voucher hotel because they did not have a home of their own or of a family member or friend to stay in). As this sample was collected as part of a study of heterosexual risk behavior, all participants reported having vaginal or anal sex with a female partner in the past 6 months. Computer-assisted structured interviews were conducted by trained male interviewers between July and October 2010. Men were paid $30 for participating in the interview, which lasted an average of 83 min. The research protocol was approved by the institutional review boards of the University of Southern California and RAND Corporation.
Study Design
To obtain a representative sample of heterosexually active homeless men from the Skid Row area of Los Angeles, we implemented a probability sample of homeless men recruited from meal lines in the study area. The list of meal lines in Skid Row was developed using existing directories of services for homeless individuals and conducting interviews with service providers. Our final list contained 13 meal lines (5 breakfasts, 4 lunches, and 4 dinners) offered by five different organizations. Each meal line was investigated extensively to obtain an estimate of the average number of men served daily, which was then used to assign an overall quota to each site which was approximately proportional to its size. The second stage of the adopted sampling design consisted of drawing a probability sample of homeless men from the 13 distinct meal lines. Men were selected for eligibility screening by their position in line using random number tables. Ninety-one percent of sampled men completed an interview.
Study Variables
Individual Characteristics
Demographic variables included age, race/ethnicity, and years of education. Separate questions asked about ethnicity and race, and men were classified into one of three groups for analysis: African American, Hispanic, and Other (which includes 73% non-Hispanic Whites, but also a small number of men who reported being Asian, American Indian/Alaska Native, or multi-racial). Individual characteristics also included attitudes about condoms, HIV knowledge, and gender-related beliefs, which were assessed with items from previously published measures. We used four items each to assess negative attitudes towards condoms (sample item: using condoms makes sex less enjoyable [34, 35]; α = 0.74) and condom use self-efficacy (sample item: it is too much trouble to carry around condoms [36]; α = 0.54). These items were rated on a 4-point scale (1 = strongly disagree to 4 = strongly agree). Basic knowledge about HIV and its transmission was assessed by five items (sample item: looking at a person is enough to tell if he or she has HIV/AIDS) [37, 38]. We classified men as having all correct responses vs. less than all correct. We assessed gender-related beliefs in terms of traditional masculine ideology or “machismo” specific to sexual relationships (10 items; sample item: the man should be more sexually experienced than the woman in a relationship [39]; α = 0.75) and sexual relationship power in men’s typical relationships with women (5 items; sample item: I always need to know where she is when she isn’t with me [40]; α = 0.62). All gender-related belief items were rated from 1 = strongly disagree to 4 = strongly agree.
Relationship Characteristics
Four variables were used to characterize men’s relationships with their most recent female sex partner. Partner type was defined as primary vs. non-primary partner, with a primary partner defined as someone the respondent considered a wife, girlfriend, or other “steady” partner. Men reported how long they had known the partner (converted to number of years), how much they trusted that their partner would not give them a sexually transmitted infection (dichotomized as: 0 = less than completely, 1 = completely), and their relationship commitment. Relationship commitment was assessed with three items (You were extremely committed to this relationship; You depended on this person for money, food a place to stay, or something else; Your life would have been very disrupted if the relationship ended [41]; α = 0.64) rated on a scale from 1 = strongly disagree to 4 = strongly agree.
Contextual Characteristics
In an earlier stage of this project, we conducted qualitative interviews with a separate sample of 30 men recruited from meal lines in which they described two recent sexual events with women in order to identify important contextual features of sexual events that may be relevant to men’s engagement in unprotected sex [42]. Based on these narratives, as well as existing literature, we developed the following four closed-ended questions for the present study (each coded as 0 = no, 1 = yes): was the partner on contraceptives (“don’t know” was combined with “no”); was it a chance or unplanned meeting; was there something different or special about this event (e.g., they had not seen each other in a long time, one of them was going away for awhile, one of them had just gotten paid); and did they talk about whether to use a condom before they had sex that time. We also asked about the setting of the sexual event and coded responses into three categories: apartment or house; motel/hotel room; or a public place (e.g., park, alley, tent set up on the street, vehicle). Finally, contextual features included four separate questions about whether a man or his partner had consumed alcohol or used drugs within an hour or so prior to having sex that time (0 = no, 1 = yes). We derived measures that combined respondent use and partner use to avoid multicollinearity in our models due to significant overlap in these reports: corresponding alcohol use (i.e., both partners used, both partners did not use) was reported in 79.6% of events, and corresponding drug use was reported in 90.0% of events. We used two dummy-coded variables to assess drug use: whether the event involved marijuana use only (vs. no drug use) and whether the event involved any hard drug use (vs. no drug use) by either partner.
Condom Use
The outcome variable was whether a condom was properly used at the most recent sexual event involving vaginal or anal intercourse with a female partner. All reported events occurred within the past 6 months. The event was coded as one where a condom was used if the couple used a condom, did not take it off until intercourse had been completed, and (if applicable) used a new condom for each insertive act.
Statistical Methods
All analyses incorporate design and differential nonresponse weights (to represent the target population from the sample of respondents) and account for the modest design effect that they induce using the linearization method [43]. The small amount of missing data for some variables (generally <1%) was accounted for by mean or modal value imputation. We first checked the correlations among predictor variables to avoid multicollinearity problems in our models. We then conducted separate logistic regression analyses for each predictor variable to examine its association with unprotected sex, adjusting for demographic characteristics. All predictor variables associated with unprotected sex at p < 0.10 in these analyses were included in a multivariate model, which also adjusted for demographic characteristics. Analyses were conducted using the statistical package SAS 9.2.
Results
Participants were 45.6 years old on average, 72% were African American, and 86% reported not having a regular place to stay (see Table 1 for further sample description). All men reported on sexual events occurring within the past 6 months, with 73% of these events occurring within a month of the interview. When asked how well they remembered their last sexual event, 64% reported “very well,” 26% “fairly well,” and 9% “not very well.” Fifty percent of men reported condom use at the event. The 309 most recent events typically involved a partner that the men had known for awhile (median length = 1.5 years). Sex most often occurred in a house or apartment (47%), followed by a motel or hotel (34%) and public setting (18%). Substance use prior to sex was common, with 50% of the events involving alcohol use, 12% marijuana use, and 26% hard drug use (79% of the hard drug use events involved crack). Thirty-one percent of couples talked, prior to having sex, about whether to use a condom.
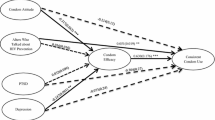
Table 2 shows results from the analyses that predicted condom use during the men’s most recent sexual event. Adjusting for demographic characteristics only, results indicated that condom use was more likely when men had higher condom use self-efficacy, greater knowledge about HIV, or talked with their partner about condom use right before sex. Men were less likely to use condoms when they held more negative attitudes towards condoms, either partner engaged in hard drug use, or sex occurred in a public place. In addition, men were marginally less likely to use a condom with a primary sex partner compared to a non-primary partner (p = 0.07). When all of these variables were included in the same model, condom use was more likely when men felt more efficacious about using condoms and talked with their partner about condom use right before sex, but less likely among men who held more negative condom attitudes or had sex with a primary partner.
We conducted secondary analyses to better understand why hard drug use prior to sex and having sex in a public place did not remain significant risk factors for unprotected sex when controlling for non-demographic factors. As shown in Table 3, hard drug use prior to sex was significantly associated with the setting in which sex occurred. Specifically, hard drug use was less likely when men had sex in a house or apartment vs. elsewhere, but more likely when they had sex in a public place vs. elsewhere. Further, men whose most recent sexual event involved hard drug use had more negative attitudes about condoms and lower self-efficacy for condom use, although they were not less likely to discuss condom use with their partner. There was a marginal association between the setting in which men had sex and their negative attitudes towards condoms, but the setting of the event was unrelated to men’s condom use self-efficacy or whether they talked about condom use with their partner.
Discussion
In our predominantly African American sample of homeless men, only 50% reported condom use at their most recent sexual event. In examining a wide range of individual, relationship, and contextual characteristics to better understand the determinants of condom use in this population, results indicated that the strongest barriers included men’s negative attitudes about condoms, their low self-efficacy for condom use, and not talking with their partner about condom use before having sex. These barriers have been highlighted as among the most important in the larger literature on heterosexual condom use based on relatively more advantaged samples [23, 44, 45] and are targeted in information-motivation-behavioral skills (IMB) approaches to HIV prevention [46]. Their relevance to condom use among homeless men is an important finding in that it suggests that the putative mechanisms of change targeted in most IMB-based interventions are also reasonable targets for interventions with homeless men. We are aware of no evidence-based HIV sexual risk reduction interventions specifically for homeless men, yet there may be promise in adapting existing evidence-based HIV risk reduction interventions designed for men of color for this highly vulnerable population “in situ”. For example, promising results have been reported for an IMB-based intervention for African American MSW that is brief (one 45–50 min session) and delivered by a lay health advisor in a clinic setting [47]. This type of intervention may be suitable for adaptation in community settings frequented by homeless men.
Results from this study highlight the considerable diversity in the context of homeless men’s sexual events, despite their shared experience of being homeless on Skid Row. Some men reported sexual encounters that were drug-involved and occurred in sidewalk tents or other public places. More often, however, their sexual events occurred in a setting that afforded greater privacy such as a rented motel room, the home of a more stably housed partner, or their own place (such as the single room occupancy housing that is available to some homeless individuals in the Skid Row area). Results from this study suggest that the contextual factors of setting and drug use are relevant to understanding men’s condom use, but not in a direct way that one might expect (e.g., caused by the disinhibiting effects of substance use on sexual behavior). The greater risk of unprotected sex when events occurred in a public place or involved hard drug use was due more to negative condom attitudes among men having sex under these conditions than to these contextual factors per se. This further points to the potential relevance of IMB-based interventions for this population, even among homeless men who engage in furtive, drug-involved sexual relations in public places. However, some tailoring may be useful to address their unique needs, consistent with the results of recent meta-analyses showing the advantages of tailored HIV risk reduction interventions [48, 49].
In terms of relationship characteristics and attitudes, men’s condom use was more strongly related to whether the partner was considered a “primary” partner (defined for men as a wife, girlfriend, or other steady partner) than how long they had known the partner, their level of commitment to the relationship, or their gender-related beliefs regarding traditional masculine ideology and sexual relationship power. The greater importance of partner type over relationship length is consistent with findings from other research on predictors of condom use among homeless women [22] and homeless youth [21]. However, it is interesting that partner type was more predictive of condom use than relationship commitment given the strong link between commitment and condom use in studies of homeless women [41, 50]. Our qualitative research with homeless men suggests that designating a partner as a “primary” partner means that she is low risk and can be trusted [42]. However, the same may not necessarily be true of partners to whom men feel more “committed.” This may be due in part to how we defined commitment in this study, which included an element of dependency on the partner for tangible support. Thus, this measure may not have been capturing the sort of emotional commitment to a partner that often leads to the cessation of condom use.
Strengths of this study include the large, probability sample of homeless men, event-based approach to understanding determinants of condom use, and wide range of individual, relationship, and contextual characteristics that were examined. However, the study also has several limitations. First, our results may not generalize to homeless men in other geographic areas or circumstances. Second, some measures had relatively low reliabilities, suggesting a need to develop more psychometrically sound measures of certain constructs for use with high-risk homeless men. Third, retrospective self-reports of sexual events are subject to the usual concerns regarding validity; however, our confidence in the accuracy of these reports is bolstered by the fact that most of the sexual events occurred within 1 month of the interview and were remembered “very well.” Finally, sampling multiple sexual events would have strengthened the study by allowing us to investigate within-subject associations [51, 52].
The principal finding of this study is that condom-related attitudes and talking about condoms prior to having sex are key predictors of homeless men’s condom use during specific sexual events with women. This finding is important in that it suggests that a promising prevention approach may be to adapt existing, evidence-based brief interventions for delivery in non-traditional settings that are frequented by men experiencing homelessness to achieve HIV risk reduction and thus reduce a significant point of disparity for the largely African American population of homeless men. The importance of housing, although not a focus of this study, must be highlighted as well in light of growing evidence that permanent supportive housing may be an effective means of HIV risk reduction for homeless persons [9, 53].
References
Martens WH. A review of physical and mental health in homeless persons. Public Health Rev. 2001;29(1):13–33.
Robertson MJ, Clark RA, Charlebois ED, et al. HIV seroprevalence among homeless and marginally housed adults in San Francisco. Am J Public Health. 2004;94(7):1207–17.
Aidala A, Cross JE, Stall R, Harre D, Sumartojo E. Housing status and HIV risk behaviors: implications for prevention and policy. AIDS Behav. 2005;9(3):251–65.
Wenzel SL, Tucker JS, Elliott MN, et al. Prevalence and co-occurrence of violence, substance use and disorder, and HIV risk behavior: a comparison of sheltered and low-income housed women in Los Angeles County. Prev Med. 2004;39(3):617–24.
Gorbach PM, Murphy R, Weiss RE, Hucks-Ortiz C, Shoptaw S. Bridging sexual boundaries: men who have sex with men and women in a street-based sample in Los Angeles. J Urban Health. 2009;86(Suppl 1):63–76.
Kidder DP, Wolitski RJ, Pals SL, Campsmith ML. Housing status and HIV risk behaviors among homeless and housed persons with HIV. J Acquir Immune Defic Syndr. 2008;49(4):451–5.
Kipke MD, Weiss G, Wong CF. Residential status as a risk factor for drug use and HIV risk among young men who have sex with men. AIDS Behav. 2007;11(Suppl 6):56–69.
Salazar LF, Crosby RA, Holtgrave DR, et al. Homelessness and HIV-associated risk behavior among African American men who inject drugs and reside in the urban south of the United States. AIDS Behav. 2007;11(Suppl 2):70–7.
Wolitski RJ, Kidder DP, Fenton KA. HIV, homelessness, and public health: critical issues and a call for increased action. AIDS Behav. 2007;11(Suppl 6):167–71.
Auerbach J. Transforming social structures and environments to help in HIV prevention. Health Aff. 2009;28(6):1655–65.
Shubert V, Bernstine N. Moving from fact to policy: housing is HIV prevention and health care. AIDS Behav. 2007;11(S2):172–81.
Hall HI, Song R, Rhodes P, et al. Estimation of HIV incidence in the United States. JAMA. 2008;300(5):520–9.
National Coalition for the Homeless. How many people experience homelessness? Available at: http://www.nationalhomeless.org/factsheets/who.html. Accessed 9 Dec 2011.
Malebranche DJ. Bisexually active Black men in the United States and HIV: acknowledging more than the “down low”. Arch Sex Behav. 2008;37(5):810–6.
Zule WA, Bobashev GV, Wechsberg WM, Costenbader EC, Coomes CM. Behaviorally bisexual men and their risk behaviors with men and women. J Urban Health. 2009;86(Suppl 1):48–62.
Lauby JL, Millett GA, LaPollo AB, Bond L, Murrill CS, Marks G. Sexual risk behaviors of HIV-positive, HIV-negative, and serostatus-unknown Black men who have sex with men and women. Arch Sex Behav. 2008;37(5):708–19.
Siegel K, Schrimshaw EW, Lekas H-M, Parsons JT. Sexual behaviors of non-gay identified non-disclosing men who have sex with men and women. Arch Sex Behav. 2008;37(5):720–35.
Centers for Disease Control and Prevention. Subpopulation estimates from the HIV incidence surveillance system—United States, 2006. Morb Mortal Wkly Rep. 2008;57(36):985–9.
McMahon JM, Tortu S, Pouget ER, Hamid R, Neaigus A. Contextual determinants of condom use among female sex exchangers in East Harlem, NYC: an event analysis. AIDS Behav. 2006;10(6):731–41.
Tortu S, McMahon J, Hamid R, Neaigus A. Drug-using women’s sexual risk: an event analysis. AIDS Behav. 2000;4:329–40.
Tucker JS, Ryan GW, Golinelli D, et al. Substance use and other risk factors for unprotected sex: results from an event-based study of homeless youth. AIDS Behav. 2011; doi:10.1007/s10461-011-0017-9.
Tucker JS, Wenzel SL, Golinelli D, et al. Is substance use a barrier to protected sex among homeless women? results from between- and within-subjects event analyses. J Stud Alcohol Drugs. 2010;7(1):86–94.
Sheeran P, Abraham C, Orbell S. Psychosocial correlates of heterosexual condom use: a meta-analysis. Psychol Bull. 1999;125(1):90–132.
Noar SM, Carlyle K, Cole C. Why communication is crucial: meta-analysis of the relationship between safer sexual communication and condom use. J Health Commun. 2006;11(4):365–90.
Vanable PA, McKirnan DJ, Buchbinder SP, et al. Alcohol use and high-risk sexual behavior among men who have sex with men: the effects of consumption level and partner type. Health Psychol. 2004;23(5):525–32.
Leigh BC, Ames SL, Stacy AW. Alcohol, drugs, and condom use among drug offenders: an event-based analysis. Drug Alcohol Depend. 2008;93(1–2):38–42.
Senn TE, Scott-Sheldon LA, Seward DX, Wright EM, Carey MP. Sexual partner concurrency of urban male and female STD clinic patients: a qualitative study. Arch Sex Behav. 2011;40(4):775–84.
Dworkin SL, Ehrhardt AA. Going beyond “ABC” to include “GEM”: critical reflections on progress in the HIV/AIDS epidemic. Am J Public Health. 2007;97(1):13–8.
Pulerwitz J, Michaelis A, Weiss E. Looking back, moving forward: promoting gender equity to fight HIV, horizons studies 1999 to 2007. Washington: Population Council; 2010.
Higgins JA, Hoffman S, Dworkin SL. Rethinking gender, heterosexual men, and women’s vulnerability to HIV/AIDS. Am J Public Health. 2010;100(3):435–45.
O’Sullivan LF, Hoffman S, Harrison A, Dolezal C. Men, multiple sexual partners, and young adults’ sexual relationships: understanding the role of gender in the study of risk. J Urban Health. 2006;83(4):695–708.
Shearer CL, Hosterman SJ, Gillen MM, Lefkowitz ES. Are traditional gender role attitudes associated with risky sexual behavior and condom-related beliefs? Sex Roles. 2005;52(5):311–24.
Bowleg L, Teti M, Massie JS, Patel A, Malebranche DJ, Tschann JM. ‘What does it take to be a man? What is a real man?’: ideologies of masculinity and HIV sexual risk among Black heterosexual men. Cult Health Sex. 2011;13(5):545–59.
Mutchler MG, Bogart LM, Elliott MN, McKay T, Suttorp MJ, Schuster MA. Psychosocial correlates of unprotected sex without disclosure of HIV-positivity among African-American, Latino, and White men who have sex with men and women. Arch Sex Behav. 2008;37(5):736–47.
Stall RD, Paul JP, Barrett DC, Crosby GM, Bein E. An outcome evaluation to measure changes in sexual risk-taking among gay men undergoing substance use disorder treatment. J Stud Alcohol. 1999;60(6):837–45.
Jemmott LS, Jemmott JB III. Applying the theory of reasoned action to AIDS risk behavior: condom use among black women. Nursing Res. 1991;40(4):228–34.
Nyamathi A. Decision-making regarding drug use among homeless women. Rockville: National Institute on Drug Abuse; 1994.
Carey MP, Schroder KE. Development and psychometric evaluation of the brief HIV Knowledge questionnaire. AIDS Educ Prev. 2002;14(2):172–82.
Caron SL, Davis CM, Halteman WA, Stickle M. Predictors of condom-related behaviors among first-year college students. J Sex Res. 1993;30(3):252–9.
Pulerwitz J, Gortmaker SL, DeJong W. Measuring sexual relationship power in HIV/STD research. Sex Roles. 2000;42(7):637–60.
Tucker JS, Elliott MN, Wenzel SL, Hambarsoomian K. Relationship commitment and its implications for unprotected sex among impoverished women living in shelters and low-income housing in Los Angeles County. Health Psychol. 2007;26(5):644–9.
Brown RA, Kennedy DP, Tucker JS, Wenzel SL, Golinelli D, Wertheimer SR, Ryan GW. Sex and relationships on the street: how homeless men judge partner risk on Skid Row. AIDS Behav. 2011; doi:10.1007/s10461-011-9965-3.
Skinner CJ. Domain means, regression and multivariate analyses. In: Skinner CJ, Holt D, Smith TMF, editors. Analysis of complex surveys. New York: Wiley; 1989.
Harvey SM, Henderson JT. Correlates of condom use intentions and behaviors among a community-based sample of Latino men in Los Angeles. J Urban Health. 2006;83(4):558–74.
Milam J, Richardson JL, Espinoza L, Stoyanoff S. Correlates of unprotected sex among adult heterosexual men living with HIV. J Urban Health. 2006;83(4):669–81.
Fisher JD, Fisher WA, Shuper PA. Emerging theories in health promotion practice and research. The information—motivation—behavioral skills model of HIV preventive behavior. 2nd ed. San Francisco: Jossey Bass Publishers; 2009.
Crosby R, DiClemente RJ, Charnigo R, Snow G, Troutman A. A brief, clinic-based, safer sex intervention for heterosexual African American men newly diagnosed with an STD: a randomized controlled trial. Am J Public Health. 2009;99(Suppl 1):96–103.
Crepaz N, Marshall KJ, Aupont LW, et al. The efficacy of HIV/STI behavioral interventions for African American females in the United States: a meta-analysis. Am J Public Health. 2009;99(11):2069–78.
Scott-Sheldon LA, Fielder RL, Carey MP. Sexual risk reduction interventions for patients attending sexually transmitted disease clinics in the United States: a meta-analytic review, 1986 to early 2009. Ann Behav Med. 2010;40(2):191–204.
Kennedy DP, Wenzel SL, Tucker JS, et al. Unprotected sex of homeless women living in Los Angeles County: an investigation of the multiple levels of risk. AIDS Behav. 2010;14(4):960–73.
Bailey SL, Gao W, Clark DB. Diary study of substance use and unsafe sex among adolescents with substance use disorders. J Adolesc Health. 2006;38(3):297.e13–20.
Leigh BC, Vanslyke JG, Hoppe MJ, Rainey DT, Morrison DM, Gillmore MR. Drinking and condom use: results from an event-based daily diary. AIDS Behav. 2008;12(1):104–12.
Holtgrave DR, Briddell K, Little E, et al. Cost and threshold analysis of housing as an HIV prevention intervention. AIDS Behav. 2007;11(Suppl 6):162–6.
Acknowledgments
This research was supported by Grant R01HD059307 from the National Institute of Child Health and Human Development. We thank the men who shared their experiences with us, the service agencies in the Skid Row area that collaborated in this study, and the RAND Survey Research Group for assistance in data collection.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tucker, J.S., Wenzel, S.L., Golinelli, D. et al. Understanding Heterosexual Condom Use among Homeless Men. AIDS Behav 17, 1637–1644 (2013). https://doi.org/10.1007/s10461-012-0165-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-012-0165-6