Abstract
Background
Though anemia is a sign of poor renal prognosis in chronic kidney disease (CKD), hemoglobin (Hb) levels are typically higher in autosomal dominant polycystic kidney disease (ADPKD) than in other kidney diseases, and anemia has not been examined as a potential prognosticator. Thus, we investigated anemia as a factor for renal prognosis in ADPKD.
Methods
In total, 115 non-dialysis patients, 48 men and 67 women, with ADPKD were evaluated. The renal outcome of a 50% reduction in the estimated glomerular filtration rate or renal replacement therapy was examined using the Cox regression analysis and Kaplan–Meier analysis.
Results
Patients were followed for a median of 5.5 years and 50 patients had reached the end point. The mean age of the patients at the first visit was 45.9 ± 13.3 years. The overall mean Hb was 12.90 ± 1.85 g/dL, and the mean Hb in men and women was 13.82 ± 1.72 g/dL and 12.25 ± 1.65 g/dL, respectively. Hb levels and uric protein content were statistically significant factors for poor renal prognosis, while hypertension and genetic mutations failed to reach significance. Furthermore, statistical significance was found in men with Hb < 12 g/dL and in women with Hb < 11 g/dL. Anemia had significant association with kidney disease progression in patients with ADPKD.
Conclusions
We found that anemia might be a factor for poor renal prognosis in ADPKD. Furthermore, a sex difference was found, wherein men with Hb < 12 g/dL and women with Hb < 11 g/dL were at risk of renal disease progression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
PKD1 and PKD2 have been identified as causative genes for autosomal dominant polycystic kidney disease (ADPKD), which is the most common inherited kidney disease [1]. Mutations in these genes cause the formation and growth of renal cysts, which gradually enlarge the kidneys, decrease parenchymal volume, and decrease renal function, leading to end-stage renal disease. With the PKD1 truncating mutation, factors such as a history of hypertension before age 35 years, microhematuria, urinary tract infections, and increased total kidney volume can lead to poor renal prognosis [2, 3].
Among most CKD patients, renal anemia is a complication of renal failure [4, 5] and has been reported to be associated with renal functional prognosis, vascular complications, and death [6]. A study on 603 CKD patients showed that those with controlled Hb levels of 13.0–15.0 g/dL had poorer renal prognosis than those with Hb levels of 10.5–11.5 g/dL [7]. In another study, CKD progression was worse in patients with Hb < 10 g/dL than patients with Hb > 12 g/dL [8]. A follow-up study showed an association between Hb and renal prognosis [9, 10]. Accordingly, anemia is considered a factor of poor renal prognosis in CKD, associated with hypoxia-induced interstitial failure, tubular cell apoptosis, oxidative stress-related injury, inflammation, and fibrosis [11].
The Kidney Disease Improving Global Outcomes (KDIGO) have set the Hb cutoff values at < 13.0 g/dL for men and < 12.0 g/dL for women, because sex differences in anemia are well known (KDIGO Guidelines). A cross-sectional study on 15,419 patients found that men with Hb < 12 g/dL or women with Hb < 11 g/dL accounted for approximately 1% of those with an estimated glomerular filtration rate (eGFR) of 60 ml/min/1.73 m2 and approximately 9% of those with an eGFR of 30 ml/min/1.73 m2, but men with Hb < 12 g/dL and women with Hb < 11 g/dL accounted for 33% and 67% of patients with an eGFR of 15 ml/min/1.73 m2, respectively [12]. Furthermore, the urinary albumin-to-creatinine ratio was the only factor of poor renal prognosis in CKD in men, but Hb levels were an additional prognosticator in women. These studies suggest that even a mild drop in Hb or mild anemia, considered within the normal range for CKD, should be treated early [13].
However, to date, there are no studies that have investigated anemia as a factor of poor renal prognosis in ADPKD. Thus, we investigated anemia as a prognostic factor in a cohort of ADPKD patients.
Materials and methods
Study design
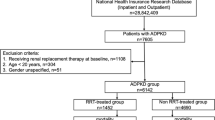
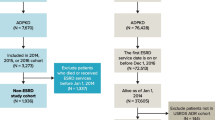
Patients who underwent genetic analysis for investigation of genetic and environmental factors of renal prognosis in ADPKD were included in the study, and prognosis of the kidney was examined in 115 ADPKD patients (48 men and 67 women). Regarding selection of participants, first, we recruited 134 patients with ADPKD who presented at the Kidney Center at Tokyo Women’s Medical University Hospital, Japan, and received genetic analyses [14] between 2003 and 2017. Patients without available Hb data (n = 11) and whose duration of follow-up was less than 2 months (n = 8) were excluded from the study. The remaining 115 patients were enrolled. We calculated the length of the kidney based on the axial slices of CT or MRI by multiplying the slice thickness by the number of slices between the superior and inferior tips of the kidneys. The average value of the left and right kidney lengths was used for analyses. All procedures were approved by the research ethics committee of Tokyo Women’s Medical University (No. 196B) in accordance with the 1964 Declaration of Helsinki and its later amendments, or with comparable ethical standards. Written informed consent was obtained from all participants included in the study.
Definition of comorbidities
The impact of concomitant treatments and comorbidities at baseline was assessed [15]. The comorbidities were recorded as positive according to the following criteria. Hypertension was defined as systolic BP ≥ 140 mmHg or diastolic BP ≥ 90 mmHg, or taking an antihypertensive agent; hyperuricemia was defined as serum uric acid level ≥ 7.0 mg/dL, or taking an anti-hypouricemic agent; hypertriglyceridemia was defined as serum TG level ≥ 150 mg/dL or taking an anti-dyslipidemic agent; low HDL-C was defined as a serum HDL-C level ≤ 40 mg/dL in men and ≤ 50 mg/dL in women, or taking an anti-dyslipidemic agent; high LDL-C was defined as a serum LDL-C level ≥ 140 mg/dL, or taking an anti-dyslipidemic agent; and diabetes was defined as HbA1c (NGSP) ≥ 6.5%, or taking oral antidiabetic agents or insulin therapy. Anemia was divided into three types: anemia type I was defined as an Hb level < 11 g/dL, or taking iron or erythropoiesis-stimulating agents (ESA); anemia type II was defined as an Hb level < 12 g/dL in men and < 11 g/dL in women, or taking iron or ESAs; and anemia type III was defined as an Hb level < 13 g/dL in men and < 12 g/dL in women, or taking iron or ESAs.
Outcome evaluation
Kidney disease progression, which was defined as a ≥ 50% decline in the eGFR from baseline, or progression to renal replacement therapy (RRT), which was defined as initiation of chronic dialysis or kidney transplantation, was the end points of this study. The subjects were followed up until June 2018.
Statistical analyses
Continuous variables are reported as the mean ± standard deviation or as medians (quartile 1, quartile 3). Categorical variables are reported as percentages, unless otherwise stated. Data were evaluated using unpaired t tests, Mann–Whitney U tests, Chi-squared tests, or Fisher’s exact tests, as appropriate. Prognostic variables for renal outcomes were assessed using the univariate and multivariate Cox proportional hazard method. Variables with P values < 0.1 in the univariate model were included in the multivariate analyses. Survival curves were plotted using the Kaplan–Meier method and were evaluated using the log-rank test. Twenty-five patients who were prescribed tolvaptan during the observation period were right-censored in the survival analyses. All statistical tests were two-tailed, and P < 0.05 was considered statistically significant. All statistical analyses were performed using the JMP Pro ver.14.1.0 software program (SAS Institute, Cary, NC, USA).
Results
Patient characteristics
Baseline patient characteristics are shown in Table 1. The median follow-up duration was 5.5 years. The PKD 1 truncating mutation was present in 56.1% of patients, and the PKD 1 non-truncating mutation was present in 25.2%. The PKD 2 mutation was present in 18.7% of patients. The mean Hb level among all patients was 12.90 ± 1.85 g/dL; 13.82 ± 1.72 g/dL in men and 12.25 ± 1.65 g/dL in women. The proportion of patients using ESAs was 5.2%. The most common clinical comorbidity was hypertension, with a rate of 64.6% (73 patients). Angiotensin-converting enzyme inhibitors (ACEI) and/or angiotensin receptor blockers (ARBs) were used by 42.6% (49 patients). One patient was treated with an aquaretic drug (tolvaptan). The kidney length examined in 76 patients with ADPKD was 17.8 ± 3.9 cm among men and 16.6 ± 4.4 cm among women.
Hb had a significant correlation between kidney length (r = − 0.32, P = 0.0051) and age (r = − 0.31, P = 0.0008).
Prognostic indicators in ADPKD patients
At the follow-up examination, 50 patients had reached the end point (≥ 50% eGFR decline or RRT). The numbers of patients who achieved the renal outcome during the observation period were 12 (75%, anemia type 1), 14 (77.8%, anemia type 2), and 24 (68.6%, anemia type 3). Patients who were administered ESAs during the observation period were not right-censored. Among 34 patients who were administered ESAs during the observation period, 32 (94.1%) achieved the end point.
The univariate analyses showed that age (10-year increase) (HR, 1.47; 95% CI 1.19–1.82; P < 0.001); PKD1 truncating mutation (HR, 1.89; 95% CI 1.04–3.61, P = 0.037); hemoglobin (HR, 0.53; 95% CI 0.43–0.64; P < 0.001); eGFR (10 mL/min/1.73 m2 increase) (HR, 0.48; 95% CI 0.39–0.58; P < 0.001); urinary protein excretion (HR, 1.95; 95% CI 1.50–2.55; P < 0.001); hypertension (HR, 4.49; 95% CI 2.22–10.35.; P < 0.001); hyperuricemia (HR, 3.93; 95% CI 2.20–7.07; P < 0.001); use of ARB and/or ACEI (HR, 3.29; 95% CI 1.86–6.01; P < 0.001); and kidney length (1 cm increase) (HR, 1.19; 95% CI 1.10–1.29; P < 0.001) were significant risk factors associated with ≥ 50% decline in eGFR or RRT. All three types of anemia had significant association with progression of kidney disease in the univariate model (Table 2A).
The multivariate analysis showed that age (10 year increase) (HR, 0.50; 95% CI 0.33–0.73; P < 0.001); eGFR (10 mL/min/1.73 m2 increase) (HR, 0.44; 95% CI 0.32–0.59; P < 0.001); and hemoglobin (HR, 0.69; 95% CI 0.50–0.95; P = 0.023) were independently associated with a ≥ 50% eGFR decline or RRT (Table 2B). The other multivariate Cox regression analyses showed that anemia type II [HR 5.97, 95% CI (1.48–24.04), P = 0.012] had significant associations with kidney disease progression. Anemia type I [HR 3.08, 95% CI (0.84–12.09), P = 0.09] and anemia type III [HR 1.11, 95% CI (0.51–2.35), P = 0.79] did not have significant association with a ≥ 50% eGFR decline or RRT. Kaplan–Meier analysis showed that the kidney survival rate in patients with anemia type II was significantly lower than that among patients without (log-rank P < 0.001) (Fig. 1). Table 3 shows subgroup Cox analyses for cohort of patients with kidney length and without ESAs/iron/tolvaptan. Although kidney length had significant association with renal outcome in the univariate Cox analysis, the association was not seen in multivariate Cox analyses.
Discussion
In general, disease progression of ADPKD is associated with various prognostic indicators and is most commonly associated with age and kidney volume [16]. In the present study, though the genetic factors and kidney length had no significant association with renal outcome, multivariate Cox analysis revealed that Hb level and anemia type II (Hb < 12.0 g/dL in men, Hb < 11.0 g/dL in women) were risk factors of kidney disease progression. Furthermore, Cox analyses showed conflicting results regarding age between univariate and multivariate analyses. The hazard ratio was more than 1.0 in the univariate model and less than 1.0 in the multivariate models. We consider that these changes of the prognostic power of age and kidney length may be influenced by the correlation between Hb (age, r = − 0.31, P = 0.0008; kidney length, r = − 0.32, P = 0.0051).
In a recent systematic review, among the 16 studies that evaluated renal risk factors of ADPKD, only two mentioned baseline Hb levels [16]. Griveas et al. reported low Hb levels (13.4 vs. 13.7 g/dL) proportionate to increased initial eGFR (78.0 vs. 73.2 mL/min/1.73 m2) in patients with a high rate of eGFR decline (− 2.6 vs. − 0.2 mL/min/1.73 m2/year) [17]. Panizo et al. included data on baseline Hb levels (mean 15.8 ± 13.9 g/dL), but it was not investigated as a prognosticator [18].
Even though anemia is a factor of poor renal prognosis in CKD, it has not been investigated sufficiently in ADPKD. It is possible that anemia has been neglected in further studies because it does not manifest as frequently in ADPKD. Hb typically remains higher in ADPKD than in CKD of other etiologies [19] because erythropoietin (EPO) is produced in the cysts and parenchymal cells in ADPKD [20, 21]. However, our study showed that low Hb was associated with poor renal prognosis in ADPKD patients. This may be due to the involvement of the hypoxia-inducible factors (HIF-1, -2, and -3). Under hypoxic conditions, HIF-1α and HIF-2α production is promoted to activate EPO transcription [22]. When CKD progresses, myofibroblasts transformed from the EPO-producing pericytes increase, preventing the effects of HIF-2α stimulation [23]
However, in ADPKD, cyst formation occurs before renal function declines, and vessels compressed in renal tissue lead to hypoxia and stimulate HIF-1α and HIF-2α production. This results in EPO increase and high Hb levels due to continued increases in pericyte HIF-2α production. However, cyst fluid secretion is promoted by hypoxia-induced HIF-1α production in the cyst-lining epithelial cells [24,25,26]. Hypoxia in ADPKD with renal function decline does not lead to EPO production in myofibroblasts despite producing more HIF-2α, effectively lowering Hb. Furthermore, progression of ischemia of the cyst-lining epithelial cells causes interstitial disease, as well as HIF-1α increase and cyst growth, eventually leading to progression of renal dysfunction. This is one reason why anemia may predict poor renal prognosis.
In the multivariate analysis of factors of poor renal prognosis in the present study, there were no significant differences in type I (both sexes Hb < 11 g/dL) and type III (men < 13 g/dL, women < 12 g/dL) anemia, but there was a significant difference in type II (men Hb < 12 g/dL, women < 11 g/dL). This sex-specific difference is likely attributable to variation in changes in Hb (ΔHb g/dL) from the respective normal Hb levels for each sex, with Hb decreasing more in men than in women. It is possible that ischemia is induced by androgens, which promote vasoconstriction. Conversely, estrogens promote vasodilatation, thereby inhibiting ischemia [27]. Therefore, it is possible that production of EPO in the pericytes is promoted in men to increase Hb levels more than in women; however, concomitant increases in HIF-1α increase cyst growth. Furthermore, the degree of change in Hb levels was greater in men because they have higher basal Hb levels than women. Increased ischemia and cystic growth resulting from changes in Hb may be implicated in anemia-related decline in renal prognosis in men. It may be necessary to investigate different targets for treating anemia to set different Hb targets for men and women.
In the present study, anemia was a factor of poor renal prognosis in ADPKD. Recent clinical trials were conducted using prolyl-hydroxylase domain (PHD) inhibitors that inhibit breakdown of HIF as treatment for anemia [28, 29]. However, PHD inhibitors are likely to inhibit the breakdown of both HIF-2α and HIF-1α, which may promote cystic growth [24, 25]. Therefore, PHD inhibitors should be administered with caution.
While these findings may have several implications for patients with ADPKD, our study has several limitations. First, the study was observational in nature, and any observed associations do not prove causality. Second, only the patients’ baseline characteristics were considered, and their characteristics during the follow-up period were not considered. Third, though total kidney volume is a factor associated with renal prognosis, only 31 patients examined TKV in the present study. Therefore, we used kidney length for the analyses in the present study; however, it may underestimate the effect of kidney size. Fourth, the sample size was relatively small; hence, further studies with a larger sample size are warranted to understanding the mechanisms and determine clinical interventions to delay the progression of ADPKD.
In conclusion, this study is the first, to our knowledge, to show that anemia is a factor for poor renal prognosis in ADPKD. Though anemia is less likely to manifest in ADPKD than CKD of other causes, it may worsen renal prognosis, indicating that early introduction of anemia treatment might be recommended.
References
Mochizuki T, Tsuchiya K, Nitta K. Autosomal dominant polycystic kidney disease: recent advances in pathogenesis and potential therapies. Clin Exp Nephrol. 2013;17:317–26.
Johnson AM, Gabow PA. Identification of patients with autosomal dominant polycystic kidney disease at highest risk for end-stage renal disease. J Am Soc Nephrol JASN. 1997;8:1560–7.
Cornec-Le Gall E, Audrezet MP, Rousseau A, Hourmant M, Renaudineau E, Charasse C, Morin MP, Moal MC, Dantal J, Wehbe B, Perrichot R, Frouget T, Vigneau C, Potier J, Jousset P, Guillodo MP, Siohan P, Terki N, Sawadogo T, Legrand D, Menoyo-Calonge V, Benarbia S, Besnier D, Longuet H, Ferec C, Le Meur Y. The PROPKD score: a new algorithm to predict renal survival in autosomal dominant polycystic kidney disease. J Am Soc Nephrol JASN. 2016;27:942–51.
Kazmi WH, Kausz AT, Khan S, Abichandani R, Ruthazer R, Obrador GT, Pereira BJ. Anemia: an early complication of chronic renal insufficiency. Am J Kidney Dis. 2001;38:803–12.
Obrador GT, Ruthazer R, Arora P, Kausz AT, Pereira BJ. Prevalence of and factors associated with suboptimal care before initiation of dialysis in the United States. J Am Soc Nephrol JASN. 1999;10:1793–800.
Portoles J, Gorriz JL, Rubio E, de Alvaro F, Garcia F, Alvarez-Chivas V, Aranda P, Martinez-Castelao A, Group N-S. The development of anemia is associated to poor prognosis in NKF/KDOQI stage 3 chronic kidney disease. BMC Nephrol. 2013;14:2.
Drueke TB, Locatelli F, Clyne N, Eckardt KU, Macdougall IC, Tsakiris D, Burger HU, Scherhag A, Investigators C. Normalization of hemoglobin level in patients with chronic kidney disease and anemia. N Engl J Med. 2006;355:2071–84.
Chang WX, Asakawa S, Toyoki D, Nemoto Y, Morimoto C, Tamura Y, Ota T, Shibata S, Fujigaki Y, Shen ZY, Uchida S. Predictors and the subsequent risk of end-stage renal disease—usefulness of 30% decline in estimated GFR over 2 years. PLoS ONE ONE. 2015;10:e0132927.
Hoefield RA, Kalra PA, Baker P, Lane B, New JP, O'Donoghue DJ, Foley RN, Middleton RJ. Factors associated with kidney disease progression and mortality in a referred CKD population. Am J Kidney Dis. 2010;56:1072–81.
Eddington H, Hoefield R, Sinha S, Chrysochou C, Lane B, Foley RN, Hegarty J, New J, O'Donoghue DJ, Middleton RJ, Kalra PA. Serum phosphate and mortality in patients with chronic kidney disease. Clin J Am Soc Nephrol CJASN. 2010;5:2251–7.
Tsuruya K, Yoshida H, Suehiro T, Fujisaki K, Masutani K, Kitazono T. Erythropoiesis-stimulating agent slows the progression of chronic kidney disease: a possibility of a direct action of erythropoietin. Ren Fail. 2016;38:390–6.
Astor BC, Muntner P, Levin A, Eustace JA, Coresh J. Association of kidney function with anemia: the Third National Health and Nutrition Examination survey (1988–1994). Arch Intern Med. 2002;162:1401–8.
Okada K, Yanai M, Takeuchi K, Matsuyama K, Nitta K, Hayashi K, Takahashi S. Sex differences in the prevalence, progression, and improvement of chronic kidney disease. Kidney Blood Press Res. 2014;39:279–88.
Mochizuki T, Teraoka A, Akagawa H, Makabe S, Akihisa T, Sato M, Kataoka H, Mitobe M, Furukawa T, Tsuchiya K, Nitta K. Mutation analyses by next-generation sequencing and multiplex ligation-dependent probe amplification in Japanese autosomal dominant polycystic kidney disease patients. Clin Exp Nephrol. 2019. https://doi.org/10.1007/s10157-019-01736-3.
Ording AG, Sorensen HT. Concepts of comorbidities, multiple morbidities, complications, and their clinical epidemiologic analogs. Clin Epidemiol. 2013;5:199–203.
Woon C, Bielinski-Bradbury A, O'Reilly K, Robinson P. A systematic review of the predictors of disease progression in patients with autosomal dominant polycystic kidney disease. BMC Nephrol. 2015;16:140.
Griveas I, Bishop K, World M. Adult polycystic kidney disease: who needs hospital follow-up? Artif Organs. 2012;36:594–9.
Panizo N, Goicoechea M, Garcia de Vinuesa S, Arroyo D, Yuste C, Rincon A, Verdalles U, Ruiz-Caro C, Quiroga B, Luno J. Chronic kidney disease progression in patients with autosomal dominant polycystic kidney disease. Nefrologia. 2012;32:197–205.
de Almeida EA, Alho I, Marques F, Thiran C, Bicho MP, Prata M. Haemoglobin and erythropoietin levels in polycystic kidney disease. Nephrol Dial Transplant. 2008;23:412–3.
Chandra M, Miller ME, Garcia JF, Mossey RT, McVicar M. Serum immunoreactive erythropoietin levels in patients with polycystic kidney disease as compared with other hemodialysis patients. Nephron. 1985;39:26–9.
Eckardt KU, Mollmann M, Neumann R, Brunkhorst R, Burger HU, Lonnemann G, Scholz H, Keusch G, Buchholz B, Frei U, et al. Erythropoietin in polycystic kidneys. J Clin Investig. 1989;84:1160–6.
Semenza GL. Oxygen sensing, homeostasis, and disease. N Engl J Med. 2011;365:537–47.
Liu J, Wei Q, Guo C, Dong G, Liu Y, Tang C, Dong Z. Hypoxia, HIF, and associated signaling networks in chronic kidney disease. Int J Mol Sci. 2017;18(5):950.
Kraus A, Peters DJM, Klanke B, Weidemann A, Willam C, Schley G, Kunzelmann K, Eckardt KU, Buchholz B. HIF-1alpha promotes cyst progression in a mouse model of autosomal dominant polycystic kidney disease. Kidney Int. 2018;94:887–99.
Hofherr A, Busch T, Kottgen M. HIF-1alpha drives cyst growth in advanced stages of autosomal dominant polycystic kidney disease. Kidney Int. 2018;94:849–51.
Buchholz B, Schley G, Faria D, Kroening S, Willam C, Schreiber R, Klanke B, Burzlaff N, Jantsch J, Kunzelmann K, Eckardt KU. Hypoxia-inducible factor-1alpha causes renal cyst expansion through calcium-activated chloride secretion. J Am Soc Nephrol JASN. 2014;25:465–74.
Murphy WG. The sex difference in haemoglobin levels in adults - mechanisms, causes, and consequences. Blood Rev. 2014;28:41–7.
Sakashita M, Tanaka T, Nangaku M. Hypoxia-inducible factor-prolyl hydroxylase domain inhibitors to treat anemia in chronic kidney disease. Contrib Nephrol. 2019;198:112–23.
Maxwell PH, Eckardt KU. HIF prolyl hydroxylase inhibitors for the treatment of renal anaemia and beyond. Nat Rev Nephrol. 2016;12:157–68.
Acknowledgements
We express our sincere appreciation to all the patients, collaborating physicians, and other medical staff for their important contributions to the study. We particularly want to thank Ms. Naomi Iwasa for contributing to this study by collecting the clinical data. This study was supported in part by a Grant-in-Aid for Intractable Renal Diseases Research, Research on rare and intractable diseases, Health and Labour Sciences Research Grants from the Ministry of Health, Labour and Welfare of Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Toshio Mochizuki and Ken Tsuchiya received travel fees and honoraria for lectures from Otsuka Pharmaceutical Co. Toshio Mochizuki and Hiroshi Kataoka belong to an endowed department sponsored by Otsuka Pharmaceutical Co, Chugai Pharmaceutical Co, Kyowa Hakko Kirin Co, and JMS Co.
Research involving human participants and/or animals
All procedures were approved by the research ethics committee of Tokyo Women’s Medical University (No. 196B) in accordance with the 1964 Declaration of Helsinki and its later amendments, or with comparable ethical standards.
Informed consent
Written informed consent was obtained from all participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Ushio, Y., Kataoka, H., Sato, M. et al. Association between anemia and renal prognosis in autosomal dominant polycystic kidney disease: a retrospective study. Clin Exp Nephrol 24, 500–508 (2020). https://doi.org/10.1007/s10157-020-01856-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-020-01856-1