Abstract
Low-level laser irradiation (LLLI) and recombinant human bone morphogenetic protein type 2 (rhBMP-2) have been used to stimulate bone formation. LLLI stimulates proliferation of osteoblast precursor cells and cell differentiation and rhBMP-2 recruits osteoprogenitor cells to the bone healing area. This in vivo study evaluated the effects of LLLI and rhBMP-2 on the bone healing process in rats. Critical bone defects were created in the parietal bone in 42 animals, and the animals were divided into six treatment groups: (1) laser, (2) 7 μg of rhBMP-2, (3) laser and 7 μg of rhBMP-2, (4) 7 μg of rhBMP-2/monoolein gel, (5) laser and 7 μg rhBMP-2/monoolein gel, and (6) critical bone defect controls. A gallium-aluminum-arsenide diode laser was used (wavelength 780 nm, output power 60 mW, beam area 0.04 cm2, irradiation time 80 s, energy density 120 J/cm2, irradiance 1.5 W/cm2). After 15 days, the calvarial tissues were removed for histomorphometric analysis. Group 3 defects showed higher amounts of newly formed bone (37.89%) than the defects of all the other groups (P < 0.05). The amounts of new bone in defects of groups 1 and 4 were not significantly different from each other (24.00% and 24.75%, respectively), but were significantly different from the amounts in the other groups (P < 0.05). The amounts of new bone in the defects of groups 2 and 5 were not significantly different from each other (31.42% and 31.96%, respectively), but were significantly different from the amounts in the other groups (P < 0.05). Group 6 defects had 14.10% new bone formation, and this was significantly different from the amounts in the other groups (P < 0.05). It can be concluded that LLLI administered during surgery effectively accelerated healing of critical bone defects filled with pure rhBMP-2, achieving a better result than LLLI alone or the use of rhBMP-2 alone.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The use of osteogenic agents has become the target of many investigations. Several studies, both experimental and clinical, have investigated the effects of laser therapy on the recovery of tissue lost for different reasons, especially bone tissue [1]. Low-level laser irradiation (LLLI) stimulates proliferation of osteoblast precursor cells and also cell differentiation leading to an increase in the number of osteoblastic cells, and consequently new bone formation [2].
There are several types of material that can be used for bone recovery including bone grafts of different origins, biomembranes, biomaterials with osteoconductive properties [3], and especially nowadays with the advances in tissue engineering techniques, proteins with osteoinductive potential, such as bone morphogenetic protein type 2 (BMP-2). This osteoinductive protein is usually used combined with a material carrier with the aim of providing a sustainable delivery system. An ideal carrier should increase the exposure of host tissues to the growth factor substance and ensure its uniform distribution without allowing the implanted material to exceed the site limits and allowing it to be absorbed as bone formation occurs. Furthermore, it should be safe, biocompatible, biodegradable and formulated in different sizes and shapes for adequate implantation [4].
Several experimental models for bone repair evaluation using osteogenic materials have been described in the literature, using different areas, as critical bone defects in long bones [5], spinal cord [6], mandible [7, 8] and calvaria [9], and involving surgical techniques such as distraction osteogenesis [10, 11]. Thus, the aim of the present study was to evaluate histomorphometrically the action of LLLI and recombinant human BMP-2 (rhBMP-2) with or without a carrier on the process of healing of critical bone defects.
Material and methods
Formulation of rhBMP-2
The rhBMP-2 (Biozentrum, Germany) was diluted 1:1 with a neutral solution of phosphate buffer, pH 7.4. A sufficient amount of monoolein gel at a monoolein/water ratio of 7:3 to completely cover the critical bone defect was combined with 7 μg of protein.
Laser irradiation
The low-level laser source used was a gallium-aluminum-arsenide (GaAlAs) semiconductor diode device (Twin-Laser; MM Optics, São Carlos, SP, Brazil), with the laser beam delivered via an optical fiber. The irradiation parameters are presented in Table 1.
Animals
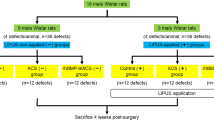
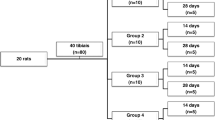
The animals used were 42 female Wistar rats (300–350 g body weight, 10–12 weeks of age) from the Ribeirão Preto Central Vivarium of the University of São Paulo. The animals were kept under standard conditions and fed ad libitum under an experimental protocol approved by the Animal Care and Use Committee of the Ribeirão Preto Campus of the University of São Paulo (protocol 08.1.224.53.6). The animals were housed in cages with five animals in each cage, and allowed to acclimatize for 1 week before surgery. The temperature was maintained at 24 ± 1°C with a light/dark cycle of 12/12 h with the light period initiated at 7:00 a.m. Animals were divided into six treatment groups of seven animals each (Table 2).
Surgical procedure
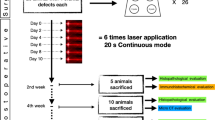
The animals were weighed and anesthetized by an intramuscular injection of xylazine 2% (10 mg/kg; Syntec do Brasil, Hortolândia, São Paulo, Brazil) and ketamine 10% (75 mg/kg; Agibrands do Brasil, Campinas, São Paulo, Brazil). Gauze soaked in physiological saline solution (0.9%) was applied onto both eyes during surgery to avoid corneal drying. To expose the calvaria, a 1-cm sagittal incision was made in the central region of the calvaria using a number 15 blade mounted on a number 3 scalpel. The critical bone defect (5 mm wide, 1 mm deep) was made in the right region (parietal bone) of the exposed calvaria using just one trephine drill (Neodent, Curitiba, PR, Brazil) for all animals. The trephine drill was adapted to a counter-angle head with the aid of an electric implant motor (Dentscler, Ribeirão Preto, SP, Brazil) at 35 Ncm torque and 1,490 rpm. The depth of drilling was controlled by a stop that was made and adapted to the trephine drill to avoid injury to the brain of the animal. The bone defect was made under constant irrigation with sterile saline solution (0.9%). Immediately after creation, the critical bone defect was irradiated according to the specified parameters, followed by skin closure. When the rhBMP-2 protein was combined with the laser, irradiation was always done before placement of the protein.
The animals were killed 15 days after treatment by an intramuscular injection of xylazine 2% (10 mg/kg; Syntec do Brasil, Hortolândia, São Paulo, Brazil) and ketamine 10% (75 mg/kg; Agibrands do Brasil, Campinas, São Paulo, Brazil), followed by rupture of the diaphragm. The animals were perfused via the heart through the left ventricle with 0.1 M phosphate buffered saline (pH 7.4) to wash the tissue and then with 4% formaldehyde solution for fixation. An infusion pump (550 T2 Samtronic, Brazil) was used to assist perfusion. The calvaria was removed after perfusion and the soft tissues were carefully detached from the bone. These fragments were immersed in the perfusion fixing solution (4% formaldehyde) for 24 h and later decalcified using 0.5 M EDTA, changing the solution every 2 days. After decalcification, which required from 15 to 30 days, the acidity was neutralized by a 24-h treatment in a 5% sodium sulfate solution. The tissue blocks were dehydrated through gradual exposure to ethanol: 70% (overnight), 80, 85, 90, 95, and 100% (2 h in each concentration). Bone blocks were immersed in equal parts of alcohol and xylol overnight and cleared in xylol, with three changes each for 2 h. All blocks were then embedded in paraffin. Semi-serial sections of thickness 6 μm were prepared from each sample and stained with Masson’s trichrome for later analysis under a light microscope.
Qualitative analysis by light microscopy
The light microscope (Leica DM 4000B) connected to a digital camera (Leica EC3) was used to capture images at a magnifications of ×10, ×20 and ×40. The newly formed bone in the area of the critical bone defect was evaluated qualitatively and the existing bone was differentiated from the newly formed bone in the experimental groups.
Histomorphometric analysis
Images of the histological sections of the critical bone defect were obtained using the microscope equipped with the digital camera. A total of 28 sections per group were analyzed (four per animal), this being the number sufficient for statistical analysis. The number of sections was calculated from the formula:
Where RSE is relative standard error, Vv is the volume density of the structure under analysis, and n is the number of points to be counted [12].
ImageJ software (http://rsb.info.nih.gov/ij) was used to generate a grid test system consisting of horizontal and vertical lines on each photomicrograph (Fig. 1). The points of intersection of these lines, total 80, were counted to determine the area of newly formed bone [13].
The volume density (Vv) of a structure can be determined by counting the points of a test system that fall on the section of the structure [13]. The parameter used in this study was a measure of the area of the test system occupied by the structure, with a similar interpretation to the volume density, as the basic law of stereology states that the number of points that touch the structure is related to the area of the structure between the points of the test system, or the volume of the structure within the volume of the test system [14].
So:
Where:
- P :
-
number of points
- A :
-
area
- V :
-
volume
- str:
-
analyzed structure
- test:
-
test system as a whole (total)
The formula used to quantify the area of newly formed bone was:
Statistical analysis
A normal distribution was found for all the data (Shapiro Wilk, P > 0.05). The data were analyzed by ANOVA and Duncan’s test to compare the groups. The SPSS (17.0) statistical software package was used, and the significance level was set at α = 5%.
Results
Qualitative analysis
After 15 days, the bone defects treated with the laser (group 1) and the critical bone defects (group 6) exhibited a small area of trabecular bone surrounded by osteoblasts close to the bone defect walls. Osteocytes were observed in wide osteocytic lacunae, indicating bone immaturity, and also abundant organized connective tissue. The new bone tissue in group 1 defects was more organized than that in group 6 defects (Figs. 2a, e and f). Group 5 defects (laser plus rhBMP-2/monoolein gel) showed the same characteristics as defects of groups 1and 6, but the amount of trabecular bone was higher and the new bone tissue was more organized.
a Photomicrograph of a group 1 defect (laser) showing the remaining bone and the newly formed bone with small trabeculae. b Photomicrograph of a group 2 defect (pure rhBMP-2) showing the newly formed bone with a trabecular appearance and abundant medullary cavities, with bone marrow and connective tissue as an extension of the periosteum layer. c Photomicrograph of a group 3 defect (laser and pure rhBMP-2) showing the remaining bone, the newly formed bone with a trabecular appearance and a small amount of connective tissue. d Photomicrograph of a group 4 defect (rhBMP-2/monoolein gel) showing the periosteum, the newly formed bone and the connective tissue with blood vessels. e Photomicrograph of a group 5 defect (laser and rhBMP-2/monoolein gel) showing the remaining bone, the connective tissue interspersed in the newly formed bone and the periosteum. f Photomicrograph of a group 6 defect (critical bone defect control) showing the remaining bone, the newly formed bone and a large amount of organized connective tissue (BV blood vessels, CT connective tissue, MC medullary cavities, NB newly formed bone, P periosteum, RB remaining bone)
In the animals treated with pure rhBMP-2 (group 2), new trabecular bone tissue was found close to the old bone walls with a great number of medullary cavities containing bone marrow. Osteoblastic cells and osteocytes in lacunae were was also evident on this trabecular bone. The adjacent connective tissue represented a continuation of the periosteum layer (Fig. 2b). This group showed the best bone tissue organization. In the defects treated with the laser plus pure rhBMP-2 placement (group 3) and rhBMP-2/monoolein gel (group 4), trabecular bone formation was observed near the old bone walls containing osteoblasts, osteocytes in lacunae, blood vessels and connective tissue, but in group 4 defects the amount of connective tissue was greater. In group 3 defects the bone tissue was more organized than in those of group 4 (Figs. 2c and d).
Quantitative analysis
The results are presented in Fig. 3 as means and standard errors. Group 3 defects (laser and pure rhBMP-2) showed higher amounts of newly formed bone than defects of all the other groups (P < 0.05). Defects of groups 2 (pure rhBMP-2) and 5 (laser and rhBMP-2/monoolein gel) were not significantly different, but were significantly different from defects of the other groups (P < 0.05). Defects of groups 1 (laser) and 4 (rhBMP-2/monoolein gel) were not significantly different, but were significantly different from defects of the other groups (P < 0.05). The smallest area of new bone formation was seen in defects of group 6 (critical bone defect control) and the difference in relation to defects of the other groups was significant (P < 0.05).
Discussion
This study aimed to evaluate the influence of LLLI and rhBMP-2 (pure or with a carrier substrate) on healing of calvarial bone defects in rats. LLLI and rhBMP-2 have been reported to stimulate new bone formation [15, 16]. In the present study, they were employed alone or in combination using the Wistar rat as an experimental animal model. Histomorphometric analysis revealed that defects of group 3 (laser and pure rhBMP-2) showed the greatest area of bone formation. The use LLLI for different treatments and indications, such as pain control and tissue recovery, including mineralized tissues, has been reported [17, 18]. BMPs, especially the BMP-2, have osteoinductive properties, causing mesenchymal cells to differentiate into osteoblastic cells [19, 20].
Studies investigating the use of BMPs in association with laser irradiation have shown similar findings, with better results when LLLI and BMPs are combined, despite using different experimental models [15, 21, 22] from that used in the present work. The laser irradiation used in this study was in continuous emission mode, but in an in vitro study, it was observed that superpulsed laser irradiation has osteogenic properties, inducing the expression of molecules known to be important mediators of bone formation and, as a consequence, increasing calcium deposition in human cells [23].
In this study, the GaAlAs diode laser in continuous mode was used, with the following parameters: wavelength 780 nm, output power 60 mW, beam spot area 0.04 cm2, irradiation time 80 s, energy density 120 J/cm2 and irradiance 1.5 W/cm2. These laser parameters were chosen because of the good results obtained in a previous study of bone regeneration after biostimulation by LLLI and rhBMP-2 in ovariectomized rats [16]. In addition, the GaAlAs laser with a wavelength of 780 nm is used in dental practice in the Faculty of Dentistry of Ribeirão Preto of University of São Paulo (FORP/USP).
Following Pretel et al. [24], our intention was also to establish an immediate intraoperative protocol involving a single laser application in contact with the surgically injured tissue, which would provide better clinical effectiveness as all the energy would be delivered to the wound area. Our aim was to confirm the beneficial effects of a single dose of radiation to the bone defect on bone healing, seeking to show that this kind of treatment could be feasible and could be standardized in a new faster easily applied protocol. In the present study, when the laser was applied alone, the presence of organizing connective tissue, with blood capillaries and fibroblasts was observed, a result similar to those of others [17, 24–26]. Small amounts of trabecular bone were also observed, as found by Gerbi et al. [21], indicating acceleration of the tissue repair process, as reported by Ozawa et al. [2], who found an increase in cell proliferation and differentiation after laser irradiation. According to Karu et al. [27], the irradiation increases the amount of ATP and cell mitotic activity.
Defects of group 5, treated with a combination of laser and rhBMP-2 plus monoolein gel, also showed trabecular bone, which was more organized than bone tissue in defects of group 1. Defects of group 6 also showed new bone tissue, but not as organized as the new bone tissue in defects of groups 1 and 5. There were significant differences in the amounts of new bone tissue among the groups. In the present experimental model, the dose used led to the formation of new bone tissue and improved the bone healing process when combined with rhBMP-2. The findings of the present study agree with the results of Pretel et al. [24], who used a GaAlAs diode laser at 178 J/cm2, Khadra et al. [28], who used 23 J/cm2, and Renno et al. [29], who used 120 J/cm2 in ovariectomized rats.
In the present study, 7 μg of rhBMP-2 was used in each critical bone defect. The amounts of rhBMP-2, which aim to cover the area of the bone defect, are the subject of much discussion in the literature, and are dependent on several factors including the experimental model used, the size of the bone defect and time [30–33]. Different amounts of rhBMP-2 have been reported in the literature [7, 9, 34, 35]. However, there is consensus that the use of a carrier material is necessary to improve delivery of the protein, considering that it is very expensive and expands quickly from the site where it is placed. Thus, the monoolein gel in cubic phase was used as an atoxic and biodegradable matrix [36] with the ability to incorporate different lipophilic and hydrophilic substances [37], including BMPs, and to release them sustainably [11]. Although this vehicle has good properties as a delivery system for different substances, in the present study, no significant differences in the amounts of new bone tissue formed were observed between group 2 defects (pure rhBMP-2) and group 4 defects (rhBMP-2/monoolein gel), although the new bone tissue in group 2 defects was more organized than that in group 4 defects.
Different periods of time for bone evaluation have been presented in the literature, but considering the experimental conditions of this study and the analyzed literature, the authors decided to use 15 days until the animals were killed to observe the initial bone healing process response. Recent authors have found that 15, 45 and 60 days are adequate to observe new bone tissue formation in a critical bone defect area, because these periods correspond to the initial, medium and late bone healing process response [24].
Conclusion
We conclude that LLLI administered during surgery effectively accelerates healing of critical bone defects filled with pure rhBMP-2, achieving a better result than laser irradiation alone or the use of rhBMP-2 alone, which makes the clinical procedure easier, faster and cheaper.
References
Stein A, Benayahu D, Maltz L, Oron U (2005) Low-level laser irradiation promotes proliferation and differentiation of human osteoblasts in vitro. Photomed Laser Surg 23:161–166
Ozawa Y, Shimizu N, Kariya G, Abiko Y (1998) Low-energy laser irradiation stimulates bone nodule formation at early stages of cell culture in rat calvarial cells. Bone 22:347–354
Shegarfi H, Reikeras O (2009) Review article: bone transplantation and immune response. J Orthop Surg 17:206–211
Toriumi DM, Robertson K (1993) Bone inductive biomaterials in facial plastic and reconstructive surgery. Facial Plast Surg 9:29–36
Bostrom MP, Saleh KJ, Einhorn TA (1999) Osteoinductive growth factors in preclinical fracture and long bone defects models. Orthop Clin N Am 30:647–658
Canto FRT, Garcia SB, Issa JPM, Marin A, Guimarães EABB, Defino HLA (2008) Influence of decortication of the recipient graft bed on graft integration and tissue neoformation in the graft-recipient bed interface. Eur Spine J 17:706–714
Arosarena O, Collins W (2005) Comparison of BMP-2 and -4 for rat mandibular bone regeneration at various doses. Orthod Craniofac Res 8:267–276
Issa JPM, Nascimento C, Bentley MV, Guimarães EABB, Iyomasa MM, Sebald W, Albuquerque RF Jr (2007) Bone repair in rat mandible by rhBMP-2 associated with two carriers. Micron 39:373–379
Issa JP, Defino HL, Netto JC, Volpon JB, Regalo SC, Iyomasa MM, Siéssere S, Tiossi R (2010) Evaluation of rhBMP-2 and natural latex as potential osteogenic proteins in critical size defects by histomorphometric methods. Anat Rec 293:794–801
Albuquerque RF Jr, Oliveira MTM, Guimarães EABB, Brentegani LG, Issa JPM (2008) Trigeminal nitric oxide synthase expression correlates with new bone formation during distraction osteogenesis. Calcif Tissue Int 82:309–315
Issa JPM, Nascimento C, Lamano-Carvalho TL, Iyomasa MM, Sebald W, Albuquerque RF Jr (2009) Effect of recombinant human bone morphogenetic protein-2 on bone formation in the acute distraction osteogenesis. Clin Oral Implant Res 20:1286–1292
Hally A (1964) A counting method for measuring the volumes of tissue components in microscopical sections. Q J Microsc Sci 105:503–517
Weibel ER, Kistler GS, Scherle WF (1966) Practical stereological methods for morphometric cytology. J Cell Biol 30:23–38
Mandarim-de-Lacerda CA (1995) Métodos quantitativos em morfologia. Eduerj, Rio de Janeiro
Carvalho PTC, Silva IS, Reis FA, Belchior ACG, Facco GG, Guimarães RN, Fernandes GHC, Denadai AS (2006) Effect of 650 nm low-power laser on bone morphogenetic protein in bone defects induced in rat femors. Acta Cir Bras 21:63–68
Siéssere S, Sousa LG, Issa JP, Iyomasa MM, Pitol DL, Barbosa AP, Semprini M, Sebald W, Bentley MV, Regalo SC (2011) Application of low-level laser irradiation (LLLI) and rhBMP-2 in critical bone defect of ovariectomized rats: histomorphometric evaluation. Photomed Laser Surg 29:453–458. doi:10.1089/pho.2010.2917
Guzzardella GA, Fini M, Torricelli P, Giavaresi G, Giardino R (2002) Laser stimulation on bone defect healing: an in vitro study. Lasers Med Sci 17:216–220
Iyomasa DM, Garavelo I, Iyomasa MM, Watanabe IS, Issa JP (2009) Ultrastructural analysis of the low level laser therapy effects on the lesioned anterior tibial muscle in the gerbil. Micron 40:413–418
Spector JA, Luchs JS, Mehrara BJ, Greenwald JA, Smith LP, Longaker MT (2001) Expression of bone morphogenetic proteins during membranous bone healing. Plast Reconstr Surg 107:124–134
Ruhe PQ, Kroese-Deutman HC, Wolke JG, Spauwen PH, Jansen JA (2004) Bone inductive properties of rhBMP-2 loaded porous calcium phosphate cement implants in cranial defects in rabbits. Biomaterials 25:2123–2132
Gerbi ME, Marques AM, Ramalho LM, Ponzi EA, Carvalho CM, Santos RC, Oliveira PC, Nóia M, Pinheiro AL (2008) Infrared laser light further improves bone healing when associated with bone morphogenic proteins: an in vivo study in a rodent model. Photomed Laser Surg 26:55–60
Denadai AS, Carvalho PTC, Reis FA, Belchior ACG, Pereira DM, Dourado DM, Silva IS, Oliveira LVF (2009) Morphometric and histological analysis of low-power laser influence on bone morphogenetic protein in bone defects repair. Laser Med Sci 24:689–695. doi:10.1007/s10103-008-0595-6
Saracino S, Mozzati M, Martinasso G, Pol R, Canuto RA, Muzio G (2009) Superpulsed laser irradiation increases osteoblast activity via modulation of bone morphogenetic factors. Lasers Surg Med 41:298–304
Pretel H, Lizarelli RF, Ramalho LT (2007) Effect of low-level laser therapy on bone repair: histological study in rats. Lasers Surg Med 39:788–796
Garavello-Freitas I, Baranauskas V, Joazeiro PP, Padovani CR, Dal Pai-Silva M, da Cruz-Hofling MA (2003) Low-power laser irradiation improves histomorphometrical parameters and bone matrix organization during tibia wound healing in rats. J Photochem Photobiol B 70:81–89
Pinheiro AL, Limeira Junior Fde A, Gerbi ME, Ramalho LM, Marzola C, Ponzi EA, Soares AO, De Carvalho LC, Lima HC, Gonçalves TO (2003) Effect of 830-nm laser light on the repair of bone defects grafted with inorganic bovine bone and decalcified cortical osseous membrane. J Clin Laser Med Surg 21:301–306
Karu T, Pyatibrat L, Kalendo G (1995) Irradiation with He-Ne laser increases ATP level in cells cultivated in vitro. J Photochem Photobiol B 27:219–223
Khadra M, Kasem N, Haanaes HR, Ellingsen JE, Lyngstadaas SP (2004) Enhancement of bone formation in rat calvarial bone defects using low-level laser therapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97:693–700
Renno AC, de Moura FM, dos Santos NS, Tirico RP, Bossini PS, Parizotto NA (2006) Effects of 830-nm laser light on preventing bone loss after ovariectomy. Photomed Laser Surg 24:642–645
Riley EH, Lane JM, Urist MR, Lyons KM, Lieberman JR (1996) Bone morphogenetic protein-2: biology and applications. Clin Orthop Relat Res 324:39–46
Okubo Y, Bessho K, Fujimura K, Kusumoto K, Ogawa Y, Iizuka T (2000) Osteogenesis by recombinant human bone morphogenetic protein-2 at skeletal sites. Clin Orthop Relat Res 375:295–301
Murakami N, Saito N, Horiuchi H, Okada T, Nozaki K, Takaoka K (2002) Repair of segmental defects in rabbit humeri with titanium fiber mesh cylinders containing recombinant human bone morphogenetic protein-2 (rhBMP-2) and a synthetic polymer. J Biomed Mater Res 62:169–174
Issa JP, Pitol DL, Iyomasa MM, Barbosa AP, Defino HL, Volpon JB, Shimano AC, Silva P (2009) Collagen fibers evaluation after rhBMP-2 insertion in critical-sized defects. Micron 40:560–562
Wang EA, Rosen V, D’Alessandro JS, Bauduy M, Cordes P, Harada T, Israel D, Hewick RM, Kerns KM, LaPan P, Luxenberg DP, Mcquaid D, Moutsatsos IK, Nove J, Wozney JM (1990) Recombinant human bone morphogenetic protein induces bone formation. Proc Natl Acad Sci USA 87:2220–2224
Abdala PM, Iyomasa MM, Sato S, Bentley MV, Pitol DL, Regalo SC, Siéssere S, Issa JP (2010) Osteoinductivity potential of rhBMP-2 associated with two carriers in different dosages. Anat Sci Int 85:181–188
D’Antona P, Parker WO, Zanirato MC, Esposito E, Nastruzzi C (2000) Rheologic and NMR characterization of monoglyceride-based formulations. J Biomed Mater Res 52:40–52
Boyd BJ, Whittaker DV, Khoo SM, Davey G (2006) Lyotropic liquid crystalline phases formed from glycerate surfactants as sustained release drug delivery systems. Int J Pharm 309:218–226
Acknowledgments
We acknowledge the support of grants from the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP - 2008/51480-4), Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) and Pró-Reitoria de Pesquisa da Universidade de São Paulo.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosa, A.P., de Sousa, L.G., Regalo, S.C.H. et al. Effects of the combination of low-level laser irradiation and recombinant human bone morphogenetic protein-2 in bone repair. Lasers Med Sci 27, 971–977 (2012). https://doi.org/10.1007/s10103-011-1022-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-011-1022-y