Abstract
Interleukin-17 (IL-17) is a proinflammatory cytokine that is expressed in the synovium T cells of rheumatoid arthritis (RA). This cytokine is implicated in the inflammation and destruction of the joint. However, the role of IL-17 on the production of vascular endothelial factor (VEGF) important to synovial proliferation has still not been identified. In this study, we investigated the effect on cultured rheumatoid fibroblast-like synoviocytes (FLS) of the IL-17 on the production and expression of VEGF, which play an important role in angiogenesis in rheumatoid synovium. IL-17 increased the production of VEGF dose dependently and the mRNA expression of VEGF. These results suggest that IL-17 might influence angiogenesis in RA by up-regulating the expression of VEGF in rheumatoid FLS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is a systemic autoimmune disease with chronic inflammation characterized by synovial cells proliferation in response to inflammatory stimuli, leading to formation of very aggressive tissue called the rheumatoid pannus. Expansion of pannus induces bone erosion and cartilage thinning, leading to loss of joint function. Neovascularization is required to maintain the chronic inflammatory state by transporting inflammatory cells to the site of synovitis as well as by supplying nutrients and oxygen to the pannus [1]. A number of angiogenic factors are involved in the neovascularization and include acidic and basic fibroblast growth factors, platelet-derived endothelial cell growth factor, transforming growth factor(TGF)-α, TGF-β, angiogenin, and vascular endothelial growth factor (VEGF) [2, 3].
VEGF is a heparin-binding, dimeric glycoprotein that induces endothelial cell proliferation, angiogenesis, and capillary permeability [4, 5]. It has been documented that VEGF may be involved in the pathogenesis of RA. Significantly greater quantities of VEGF are found in the synovial fluid of RA patients than in osteoarthritis or other forms of arthritis [6, 7], and VEGF protein and messenger RNA (mRNA) were expressed by subsynovial macrophages and synovial lining cells in RA joints [6, 8]. Hypoxia is an important stimulus for VEGF release in rheumatoid synovial cells [9–11]. In addition, prostaglandin (PG), IL-1 [12], IL-6 [13], TGF-β [10, 14], TNF-α [15] and CD40 ligand [16] have been describe to induce VEGF.
IL-17 is s T cell-derived cytokine produced by activated T cells, predominantly activated CD4+, CD45RO+ memory T cells [17, 18]. This cytokine stimulate stromal cells to secrete various cytokines and growth factors associated with inflammation [17–20]. Increased IL-17 expression was detected in several diseases, such as systemic sclerosis [21], nephritic syndrome [22], systemic lupus erythematosus [23], and RA [24, 25]. IL-17 is spontaneously produced by rheumatoid synovium [24], and high levels have been detected in the synovial fluid of patients with RA [24, 25]. IL-17 can stimulate the production of IL-1β and TNF-α from macrophages [20] and triggers human synoviocytes to produce IL-6, IL-8, granulocyte-macrophage colony-stimulating factor, and prostaglandin E2[18, 26] suggesting that IL-17 could be an important mediator in the pathogenesis of arthritis. Furthermore, IL-17 may be involved in tissue destruction. IL-17 has biologic activities similar to those of IL-1β, and additive/synergic effects with IL-1β and TNF-α have been reported [27]. IL-17 suppresses matrix synthesis by murine articular chondrocytes through nitric oxide (NO) production [28, 29], and promotes bone erosion through loss RANKL/OPG balance in collagen-induced arthritis (CIA) [30].
There is paucity of data regarding the effect of IL-17 on VEGF production in RA synoviocytes. In this study, we investigate the effect of IL-17 on the production and mRNA expression of VEGF in rheumatoid FLS.
Materials and methods
Isolation and culture of synoviocytes
Fibroblast-like synoviocytes (FLS) were isolated by enzymatic digestion of synovial tissues, obtained from RA patients undergoing total joint replacement surgery, as described previously [16]. Tissues were minced into 2- to 3-mm pieces and treated for 4 h with 4 mg/ml of collagenase (type I; Worthington Biochemical, Freehold, NJ) in Dulbecco’s modified Eagle’s medium (DMEM) at 37 ° C in 5% CO2. Dissociated cells were then centrifuged at ×500g, resuspended in DMEM supplemented with 10 % fetal calf serum (FCS, Life Technologies, Grand Island, NY), 2 mM glutamine, penicillin (100 units/ml), and streptomycin (100 μg/ml), and plated in 75-cm2 flasks. Cultures were kept at 37 ° C in 5% CO2, and the medium was replaced every 3 days. When cells approached confluence, they were passed by diluting 1:3 with fresh medium and were recultured until used.
VEGF production by cytokines
A homogeneous population of FLS from passage 4 to 8 was used for each experiment. FLS were seeded in 24-well plates at 6×104 cells/well in 1 ml DMEM supplemented with 5% FCS, and incubated at 37° C for 24 h. Cultures were washed with serum-free DMEM, and then incubated in serum-free DMEM supplements with insulin-transferrin-selenium A (ITSA, Life Technologies) for 48 h until the medium was replaced with fresh DMEM/ITSA. Subsequently, various concentrations of IL-17, IL-1β, TNF-α and TGF-β (5–400 pg/ml) were added to the each well, and cultures were incubated for 24 h. IL-17(20 pg/ml), IL-1β (20 pg/ml), TNF-α (20 pg/ml) and TGF-β (20 pg/ml), IL-17 with TNF-α, IL-17 with IL-β, and IL-17 with TGF-β were added to each well, and cultures were incubated for 12, 24, 48, and 72 h. Cell-free media were collected and stored at −20 ° C until used.
Enzyme-linked immunosorbent assay (ELISA) of VEGF
VEGF in culture supernatants was measured by sandwitch ELISA, as previously described [16]. Ninety-six-well microtiter plates were coated with 100μl/well of 0.4μg/ml goat anti-human VEGF165 (R&D systems, Minneapolis, MN) buffered with 50 mM of sodium carbonate (pH 9.6). After overnight incubation at 4 ° C, the plates were blocked with 1% bovine serum albumin (BSA) in phosphate buffered saline (PBS) for 1 h at room temperature. The human recombinant VEGF 165 (R&D Systems) or test samples were added to the wells and incubated for 2 h at room temperature. Plates were incubated with 0.2 μg/ml biotinylated goat anti-human VEGD165 (R&D Systems) for 2 h at room temperature. Peroxidase-labeled extravidin (Sigma), diluted 1:1000, was added to react with the plates at room temperature for 1 h. A color reaction was induced by the addition of substrate solution (TMB/H2O2) and was stopped 30 min later by the addition of 1 M phosphoric acid. An automated microplate reader was used to measure the OD at a wave-length of 450 nm. Between each of these steps, the plates were washed four times with PBS containing 0.05% Tween 20. Human recombinant VEGF 165 diluted in culture medium was used as a calibration standard, ranging from 10 pg/ml to 2,000 pg/ml. A standard curve was drawn by plotting OD versus the log of the recombinant VEGF 165 concentration.
Quantitation of VEGF mRNA by real-time reverse transcription-polymerase chain reaction (RT-PCR)
Total cellular RNA was extracted from synovial cells as described previously [31] and was treated with amplification-grade DNase I (GIBCO BRL, Life Techonologies). RNA was then subjected to reverse transcription (RT) using the SuperScript Preamplification System for First Strand cDNA Synthesis (GIBCO BRL, Life Technologies). Serial dilutions of the cDNA template were prepared and PCR was carried out using a Lightcycler System (Roche Molecular Biochemicals, Palo Alto, CA). After each elongation phase, the fluorescence of SYBR Green I (Roche Molecular Biochemicals), which binds double-stranded DNA, was measured. Reactions (20 μl) were performed in microcapillary tubes using 5 μl of diluted cDNA with SYBR Green I, master mis, upstream and downstream primers, and MgCl2. Sequences of primer pairs were as follows: VEGF:upstream, 5′-TTCATGGATGTCTATCAGCG-3′, downstream, 5′-GCTCATCTCTCCTATGTGCT-3′, β-actin : upstream, 5′-AACACCCCAGCCATGTACG-3′, downstream, 5′-ATGTCACGCACGATTTCCC-3′. Reactions containing water or cDNA synthesized without reverse transcriptase, as template, resulted in no PCR products. LightCycler quantification software v3 was used to compare amplification in experimental samples during the log-linear phase to the standard curve from the dilution series of acute tissue. All experimental samples were normalized to β-actin expression levels for that tissue. The expression levels of each gene were plotted relative to the levels in normal tissue.
Data
Data were taken from at least three repeated experiments performed with each sample obtained from the three RA patients. Statistical analysis was performed using the SPSS statistical software package (version 10.0 for Windows). Comparisons among groups were performed by Mann–Whitney test. A 5% significance levels was accepted as showing statistical significance.
Results
IL-17 dose-dependently increased the production of VEGF in FLS
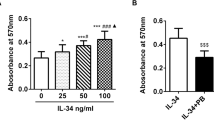
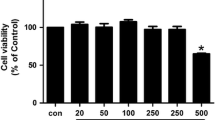
Stimulation of FLS by IL-17, IL-1β, TNF-α and TGF-β with 5, 10, 20, 50, 100, 200, 400 pg/ml increased VEGF production dose-dependently (Fig. 1).
Vascular endothelial growth factor (VEGF) production was dose-dependently increased by IL-17, IL-1β, tumor necrosis factor- α (TNF-α) and transforming growth factor-β (TGF-β). Human rheumatoid arthritis synoviocytes were stimulated with IL-17, IL-1β, TNF-α and TGF-β (5–400 pg/ml) and cultured for 24 h. Data were taken from at least three repeated experiments performed with each sample obtained from the three RA patients. The amount of VEGF in the supernatant was determined by sandwitch ELISA. Data were expressed as log scale of mean concentration (C : concentration of with IL-17, IL-1β, TNF-α and TGF-β, V : concentration of VEGF)
IL-17 had additive effect with TNF-α, IL-1β and TGF-β on the production and expression of VEGF in FLS
VEGF production of FLS stimulated by PBS, IL-17 (20 pg/ml), IL-1β (20 pg/ml), TNF-α(20 pg/ml), TGF-β (20 pg/ml), IL-17 (20 pg/ml)+IL-1β (20 pg/ml), IL-17 (20 pg/ml)+TNF-α (20 pg/ml) and IL-17 (20 pg/ml)+TGF-β (20 pg/ml) was 190±21 pg/ml, 456±52, 547±35, 487±42, 423±46, 820±54, 680±43 and 676±54 pg/ml after 12 h culturing, 213±25, 497±38, 587±58, 587±47, 467±35, 880±57, 750±46, 840±78 pg/ml after 24 h culturing, 220±31, 492±32, 652±45, 610±66, 580±57, 1043±87, 1044±68 and 986±57 pg/ml after 48 h culturing, 232±37, 543±46, 663±35 and 578±35, 612±57, 1259±89, 1162±74 and 979±74 pg/ml after 72 h culturing (Table 1).
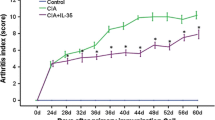
The mRNA VEGF/β-actin relative density of FLS untstimulated, stimulated by IL-17 (20 pg/ml), IL-1β (20 pg/ml), TNF-α (20 pg/ml), TGF-β (20 pg/ml), IL-17 (20 pg/ml)+IL-1β (20 pg/ml), IL-17 (20 pg/ml)+TNF-α(20 pg/ml) and IL-17 (20 pg/ml)+TGF-β (20 pg/ml) was 1, 2.2±0.6, 3±1, 1.8±0.3, 2±0.5, 3.4±0.8, 3.2±1 and 2.8±1.3 after 24 h culturing (Fig. 2).
IL-17 increased the vascular endothelial growth factor (VEGF) mRNA expression and had additive effect with TNF-α, IL-1β, and TGF-β on VEGF mRNA expression. Human rheumatoid arthritis synoviocytes were stimulated with IL-17, IL-1β, TNF-α, transforming growth factor-β (TGF-β) (20 pg/ml), IL-17+IL-1β, IL-17+TNF-α, and IL-17+TGF-β and cultured for 24 h. Data were taken from at least three repeated experiments performed with each sample obtained from the three RA patients. The VEGF mRNA expression was determined by real-time RT-PCR. Data were expressed as mean±SD *, **, *** ; P<0.05 by Mann–Whitney test
Discussion
In this study, we demonstrated that IL-17 increased the production and mRNA expression of VEGF, and had additive effect with TNF-α, IL-1β and TGF-β on the production of VEGF in RA synoviocytes.
IL-17 may contribute to joint inflammation and destruction in RA. In vivo studies, IL-17 increased joint inflammation, cartilage destruction and bone erosion [30, 31] in CIA. It promotes bone erosion through loss of receptor activator NF-κB ligand/osteoprotegerin balance. Blocking of IL-17 reduced joint inflammation, cartilage destruction and bone erosion [32–34] and these results suggest blocking of IL-17 may provide a therapeutic strategy for RA.
Apart from inflammatory and destructive responses, IL-17 has been shown to promote angiogenesis in tumor models and correlates well with the numbers of blood vessels in human ovarian cancers [35]. IL-17 promotes tumorgenicity of human cervical tumors in nude mice and is associated with an increased level of IL-6 expression at the tumor sites [36]. Increased levels of IL-6 correlate well with the invasiveness of cervical tumors [37]. IL-17 promotes angiogenesis and tumor growth [38].
IL-17 had synergic effect with IL-1 on the production of IL-6, leukemia inhibitory factor (LIF) [39], and had synergic effects with TNF-α on the production of macrophage inhibitory protein −3α (MIP-3α) and IL-6 in rheumatoid arthritis synoviocytes [40]. In our study, IL-17 had no synergic but rather additive effect with TNF-α, IL-1β and TGF-β on the production and expression of VEGF in RA synoviocytes.
In summary, we have demonstrated that IL-17 increase the production and expression of VEGF and had additive effect with TNF-α, IL-1β and TGF-β on the production of VEGF in RA synoviocytes. Our data strongly suggest that IL-17 is implicated in the angiogenesis of RA synovium.
References
Koch AE (1998) Angiogenesis: implications for rheumatoid arthritis. Arthritis Rheum 41:951–962
Walsh DA (1999) Angiogenesis and arthritis. Rheumatology 38:103–112
Klagsbrun M, D’Amore PA (1991) Regulators of angiogenesis. Annu Rev Physiol 53:217–239
Dvorak HF, Brown LF, Detmar M, Dvorak AM (1995) Vascular permeability factor/vascular endothelial growth factor, microvascular hyperpermeability, and angiogenesis. Am J Pathol 146:1029–1039
Conn G, Soderman DD, Schaeffer MT, Wile M, Hatcher VB, Thomas KA (1990) Purification of a glycoprotein vascular endothelial cell mitogen from a rat glioma-derived cell line. Proc Natl Acad Sci USA 87:1323–1327
Fava RA, Olsen NJ, Spencer-Green G, Yeo KT, Yeo TK, Berse B et al (1994) Vascular permeability factor/endothelial growth factor (VPF/VEGF): accumulation and expression in human synovial fluids and rheumatoid synovial tissue. J Exp Med 180:341–346
Koch AE, Harlow LA, Haines GK, Amento EP, Unemori EN, Wong WL et al (1994) Vascular endothelial growth factor: a cytokine modulating endothelial function in rheumatoid arthritis. J Immunol 152:4149–4156
Nagashima M, Yoshino S, Ishiwata T, Asano G (1995) Role of vascular endothelial growth factor in angiogenesis of rheumatoid arthritis. J Rheumatol 22:1624–1630
Jackson JR, Minton JA, Ho ML, Wei N, Winkler JD (1997) Expression of vascular endothelial growth factor in synovial fibroblasts is induced by hypoxia and interleukin 1β. J Rheumatol 24:1253–1259
Berse B, Hunt JA, Diegel RJ, Morganelli P, Yeo K, Brown F et al (1999) Hypoxia augments cytokine (transforming growth factor-β [TGF-β] and IL-1)-induced vascular endothelial growth factor secretion by human synovial fibroblasts. Clin Exp Immunol 115:176–182
Ikeda E, Achen MG, Breier G, Risau W (1995) Hypoxia-induced transcriptional activation and increased mRNA stability of vascular endothelial growth factor in C6 glioma cells. J Biol Chem 270:19761–19766
Ben-Av P, Crofford LJ, Wilder RL, Hla T (1995) Induction of vascular endothelial growth factor expression in synovial fibroblasts by prostaglandin E and interleukin-1: a potential mechanism for inflammatory angiogenesis. FEBS Lett 372:83–87
Cohen T, Nahari D, Cerem LW, Neufeld G, Levi BZ (1996) Interleukin 6 induces the expression of vascular endothelial growth factor. J Biol Chem 271:736–741
Pertovaara L, Kaipainen A, Mustonen T, Orpana A, Ferrara N, Saksela O et al (1994) Vascular endothelial growth factor is induced in response to transforming growth factor-β in fibroblastic and epithelial cells. J Biol Chem 269:6271–6274
Paleolog EM, Young S, Stark AC, McCloskey RV, Feldmann M, Maini RN (1998) Modulation of angiogenic vascular endothelial growth factor by tumor necrosis factor α and interleukin-1 in rheumatoid arthritis. Arthritis Rheum 41:1258–1265
Cho CS, Cho ML, Min SY, Kim WU, Min DJ, Lee SS et al (2000) CD40 engagement on synovial fibroblast up-regulates production of vascular endothelial growth factor. J Immunol 164:5055–5061
Yao Z, Painter SL, Fanslow WC, Ulrich D, Macduff BM, Spriggs MK et al (1995) Human IL-17: a novel cytokine derived from T cells. J Immunol 155:5483–5486
Fossiez F, Djossou O, Chomarat P, Flores-Romo L, Ait-Yahia S, Maat C et al (1996) T cell interleukin-17 induces stromal cells to produce proinflammatory and hematopoietic cytokines. J Exp Med 183:2593–2603
Yao Z, Fanslow WC, Seldin MF, Rousseau AM, Painter SL, Comeau MR et al (1995) Herpesvirus Saimiri encodes a new cytokine, IL-17, which binds to a novel cytokine receptor. Immunity 3:811–821
Jovanovic DV, Di Battista JA, Martel-Pelletier J, Jolicoeur FC, He Y, Zhang M et al (1998) IL-17 stimulates the production and expression of proinflammatory cytokines, IL-1β and TNF-α by human macrophages. J Immunol 160:3513–3521
Kurusawa K, Hirose K, Sano H, Endo H, Shinkai H, Nawata Y et al (2000) Increased interleukin-17 production in patients with systemic sclerosis. Arthritis Rheum 43:2455–2463
Matsumoto K, Kanmatsuse K (2002) Increased urinary excretion of interleukin-17 in nephrotic patients. Nephron 91:243–249
Wong CK, Ho CY, Li EK, Lam CW (2000) Elevation of proinflammatory cytokine (IL-18, IL-17, IL-12) and Th2 cytokine (IL-4) concentrations in patients with systemic lupus erythematosus. Lupus 9:589–593
Chabaud M, Durand JM, Buchs N, Fossiez F, Page G, Frappart L et al (1999) Human interleukin-17: a T cell derived proinflammatory cytokine produced by the rheumatoid synovium. Arthritis Rheum 42:963–970
Ziolkowska M, Koc A, Luszczykiewicz G, Ksiezopolska-Pietrzak K, Klimczak E, Chwalinska-Sadowska H et al (2000) High levels of IL-17 in rheumatoid arthritis patients: IL-15 triggers in vitro IL-17 production via cyclosporin A-sensitive mechanism. J Immunol 164:2832–2838
Chabaud M, Fossiez F, Taupin JL, Miossec P (1998) Enhancing effect of IL-17 on IL-1-induced IL-6 and leukemia inhibitory factor production by rheumatoid arthritis synoviocytes and its regulation by Th2 cytokines. J Immunol 161:409–414
Chabaud M, Lubberts E, Joosten L, van den Berg W, Miossec P (2001) IL-17 derived from juxta-articular bone and synovium contributes to joint degradation in rheumatoid arthritis. Arthritis Res 3:168–177
Lubberts E, Joosten LAB, van de Loo FAJ, van den Bersselaar LA, van den Berg WB (2000) Reduction of interleukin-17 induced inhibition of chondrocyte proteoglycan synthesis in intact murine articular cartilage by interleukin-4. Arthritis Rheum 43:1300–1306
Martel-Pelletier J, Mineau F, Jovanovic D, Di Battista JA, Pelletier JP (1999) Mitogen-activated protein kinase and nuclear factor κB together regulate interleukin-17-induced nitric oxide production in human osteoarthritic chondrocytes: possible role of transactivating factor mitogen-activated protein kinase-activated protein kinase (MAPKAPK). Arthritis Rheum 42:2399–2409
Lubberts E, van den Bersselaar L, Oppers-Wlagreen B, Schwarzenberger P, Coenen-de Roo CJJ, Kolls JK et al (2003) IL-17 promotes bone erosion in murine collagen-induced arthritis through loss of the receptor activator of NF-κB ligand/osteoprotegerin balance. J Immunol 170:2655–2662
Lubberts E, Joosten LAB, Oppers-Walgreen B, van den Bersselaar L, Chenen-de Roo CJJ, Kolls JK et al (2001) IL-1-independent role of IL-17 in synovial inflammation and joint destruction during collagen-induced arthritis. J Immunol 167:1004–1013
Lubberts E, Koenders MI, Oppers-Walgreen B, van den Bersselaar L, Coenen-de Roo CJ, Joosten LA et al (2004) Treatment with a neutralizing anti-murine interleukin-17 antibody after the onset of collagen-induced arthritis reduces joint inflammation, cartilage destruction, and bone erosion. Arthritis Rheum 50:650–659
Nakae S, Nambu A, Sudo K, Iwakura Y (2003) Suppression of immune induction of collagen-induced arthritis in IL-17-deficient mice. J Immunol 171:6173–6177
Kim JM, Ho SH, Hahn W, Jeong JG, Park EJ, Lee HJ et al (2003) Electro-gene therapy of collagen-induced arthritis by using an expression plasmid for the soluble p75 tumor necrosis factor receptor-Fc fusion protein. Gene Ther 10:1216–1224
Kato T, Furumoto H, Ogura T, Onishi Y, Irahara M, Yamano S et al (2002) Expression of IL-17 mRNA in ovarian cancer. Biochem Biophys Res Commun 282:735–738
Tartour E, Fowwiez F, Joyeux I, Galinha A, Gey A, Claret E et al (1999) Interleukin 17, a T-cell-derived cytokine, promotes tumorgenicity of human cervical tumors in nude mice. Cancer Res 59:3698–3704
Page F, Vives V, Stautes-Fridman C, Fossiez F, Berger A, Cugnenc PH et al (1999) Control of tumor development by intratumoral cytokines. Immunol Lett 68:135–139
Numasaki M, Fukushi J, Ono M, Narula SK, Zavodny PJ, Kudo T et al (2003) Interleukin-17 promotes angiogenesis and tumor growth. Blood 101:2620–2627
Chabaud M, Fossiez F, Taupin JL, Miossec P (1998) Enhancing effect of IL-17 on IL-1-induced IL-6 and leukemia inhibitory factor production by rheumatoid arthritis synoviocytes and its regulation by Th2 cytokine. J Immunol 161:409–414
Katz Y, Nadiv O, Beer Y (2001) Interleukin-17 enhances tumor necrosis factor alpha-induced synthesis of interleukin 1, 6, and 8 in skin and synovial fibroblasts: a possible role as a “fine-tuning cytokine” in inflammation process. Arthritis Rheum 44:2176–2184
Acknowledgements
This work was supported by a project grant from the Supported by grants from the Pusan National University Hospital Institute
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ryu, S., Lee, J.H. & Kim, S.I. IL-17 increased the production of vascular endothelial growth factor in rheumatoid arthritis synoviocytes. Clin Rheumatol 25, 16–20 (2006). https://doi.org/10.1007/s10067-005-1081-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-005-1081-1