Abstract
The aim of this study was to characterize the magnetic resonance imaging (MRI) features of PVNS. The radiographs and MR images of 23 pathologically proven cases of PVNS were retrospectively reviewed, with emphasis on MR images. There were 9 males and 14 females, mean age 36 years. Of 23 cases, 9 occurred in the hip, 8 in the knee, 3 in the ankle, 2 in the elbow and 1 in the wrist. Typical MRI findings included variable extent of nodular synovial proliferation, from mild proliferation to extensive masses, joint effusion in all cases, and multiple bony erosions in 15. Owing to the tight joint space, bone involvement was frequently seen in the hip, ankle, elbow and wrist. Although the knee joint had a loose capsule, bone involvement was rarely seen. Hemosiderin is a magnetic material, its deposit on proliferative synovial tissue resulting in a spotty low signal or extensive low signal area within the proliferative synovial masses on T1- (T1WI) and T2-weighted (T2WI) images, best seen on fast field echo (FFE) sequence MRI images. Fat-suppressed sequences obscured the deposit . This is diagnostic of PVNS. The MRI features of PVNS include variable extent of synovial proliferation, joint effusion and erosion of bone, and in particular the deposit of hemosiderin within the synovial masses. The deposit of hemosiderin, appearing as a low signal area best seen on FFE sequence, is diagnostic for PVNS.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Pigmented villonodular synovitis (PVNS) is now considered a joint inflammatory lesion of unknown etiology [1, 2]. It is a relatively rare disease that has a predilection for the lower extremities, particularly the knee and hip [1, 2, 3, 4]. The radiographic features of PVNS have been well documented in textbooks [1, 2] and articles [4, 5]. Soft tissue swelling within one joint typifies early PVNS on radiography. Classically, multiple soft tissue masses may be seen in underexposed radiographs: they may appear dense, owing to the intense deposits of hemosiderin. Bone involvement may be seen in the later stages [1, 2]. All of these radiographic features are non-specific, which means they are difficult to differentiate from simple synovitis; they may mimic tuberculosis or rheumatoid arthritis when bone erosion occurs. Furthermore, they may reveal normal X-rays in 32% of cases, and in 54% of PVNS cases in the knee [2].
The histology of PVNS has been best described by Jaffe et al [6]. The first stage, characterized by pigmentation (hemosiderin) with villous transformation of the synovial lining, is apparently caused by hyperplasia of undifferentiated connective tissue. Hemosiderin itself has ferromagnetic properties, which would be expected to alter the MRI signal [4]. Indeed, early studies confirmed this observation, and this may help diagnose PVNS [3, 4]. In general, MRI is superior to conventional radiographs for depicting abnormalities of the joint, and is able to depict the true extent of PVNS. For this paper we retrospectively reviewed the radiographs and MRI scans of 23 cases of PVNS, to assess the role of MRI in its evaluation.
Materials and methods
From September 1998 to March 2003, 23 patients with pathologically proven cases of PVNS underwent conventional radiography and MRI examination in our department. Each case had frontal and lateral X-rays of the involved joints. All MRI scans were performed with our Philips 1.0 T scanner. Various coils were used according to the joint under examination. T1WI, T2WI, FFE and fat-suppressed sequences were routinely acquired in one imaging plane, with fewer sequences in the other two planes, depending on the joint examined. Nine cases also had intravenous contrast injection of 0.1 mmol/kg GD-DTPA, and contrast-enhanced T1WI images were acquired in axial, coronal or/and sagittal planes. Scanning required half an hour to 45 min to complete. All X-rays and scans were retrospectively reviewed by two experienced musculoskeletal radiologists (X.C. and H.Q.).
Results
The study subjects consisted of 14 females and 9 males, with a mean age of 36 years, range 11–68 years. Of 23 cases, 9 occurred in the hip, 8 in the knee, 3 in the ankle, 2 in the elbow and 1 in the wrist.
The radiographic features of PVNS varied according to which joint was involved. In the hip joint, the most striking findings were multiple erosions in the subchondral areas of the acetabulum and around the neck, seen in all 9 cases; joint space narrowing was noticed in five hips (Fig. 1a). The radiographic findings in the hip were highly suggestive of PVNS, although non-specific. In the knee joint swelling and effusion were usually seen, commonly located in the Hoffa pad, suprapatellar region and posterior joint space (Fig. 2a). These findings were non-specific, no different from joint swelling caused by other pathologies. Bone involvement was not found in the 8 knees of our series. Nodular masses were seen in two elbows and one ankle, which were suggestive of PVNS. Soft tissue masses were found in other two ankles and one wrist.
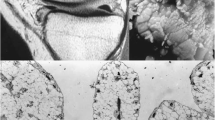
Male, 33 years old. Pelvis X-ray (a), T1-weighted (b), STIR (c) and FFE (d) coronal MRI images. X-ray showed multiple bone erosions (arrows) in the femoral neck and intertrochanteric regions and acetabulum of the right hip, with joint effusion (a). MR images of the hip showed multiple bone erosions and soft tissue masses around the joint (arrows b–d). Bone marrow edema on STIR (arrow c) and very low signal of hemosiderin deposits in the FFE images (arrows d)
Male, 30 years old. Lateral X-ray (a), T1-weighted (b), T2-weighted (c), STIR (d) and FFE (e) of MR. X-ray showed soft tissue masses in the posterior region of the knee joint without bone involvement (arrow a). Sagittal MR images of the knee showed nodular soft tissue masses in the Hoffa pad and the posterior region of the knee joint without bone erosion (arrows b–e), intermediate signal on T1- and T2-weighted scans (arrows b, c), high signal on STIR (arrows d) and very low signal of hemoderin deposits in the FFE images (arrow e)
Typical MRI findings included a variable extent of nodular synovial proliferation, from mild proliferation to extensive masses, with hemosiderin deposits in all cases. The hemosiderin deposits on proliferative synovial tissue resulted in a spotty low signal or extensive low signal area within the proliferative synovial masses on T1WI and T2WI, best seen on FFE sequence MRI scans. Although fat-suppressed sequences MR images showed proliferative synovial masses as very high signal, they obscured the hemosiderin deposits. This was diagnostic for PVNS. MRI demonstrated multiple bony erosions all cases except for 8 knees. Other findings included bone marrow edema in 10 cases, mostly in the hip, and joint effusion in 7 cases, mostly in the knee. Enhancement was seen in the proliferative synovial masses, however, GD-DTPA contrast-enhanced T1WI did not help the diagnosis.
Discussion
Imaging plays an important role in the diagnosis of PVNS, the radiographic features of which have been well documented [1, 2]. Our radiographic findings were consistent with those in the literature [1, 2, 5]. One common finding of PVNS on radiography is the swelling of the joint, as conventional radiography is insensitive to differentiate effusion from synovial thickening and proliferation; therefore, this finding is very non-specific and can be found in many joint abnormalities. In the hip joint, soft tissue masses and joint effusions are difficult to appreciate, as the thick soft tissue is superimposed around the hip joint. In the intermediate stage of PVNS characteristic villonodular masses appear, and these tend to coalesce, forming still larger masses. If multiple nodular soft tissue masses around a joint are seen on radiographs, particular if they appear dense owing to the intense deposits of hemosiderin within the mass, PVNS is highly likely. Unfortunately, these findings are rarely seen in the hip and knee, where PVNS most commonly occurs. Another important finding on radiography is bone erosion. These osseous changes are the result of pressure atrophy, the actual invasion of bone, or both. Bone erosion is rarely seen in the knee, except in the later stages: it is due to the large joint space of the knee, whereas in the hip joint, owing to the tight joint space, bone erosion is most commonly seen, as well as in the ankle and elbow. The bone erosion in the subchondral areas may be confused with other conditions, such as cystic changes of degenerative osteoarthritis, rheumatoid arthritis and tuberculosis [1, 2, 5]. Careful observation of radiographs may help differentiate them. PVNS is predominantly monoarticular, whereas rheumatoid arthritis involves multiple joints, particular the hands and feet. Usually, except for these bone defects, the remaining bone appears dense and healthy in texture, unless disuse atrophy ensues, whereas severe osteoporosis is commonly seen in rheumatoid arthritis. In addition to subchondral cysts, clearly subchondral sclerosis, joint space narrowing and osteophytes may help differentiate osteoarthritis from PVNS.
MRI has superior tissue contrast, suitable for depicting the synovial proliferation, joint effusion, bone erosion and deposits of hemosiderin. In the early stage, PVNS is characterized by pigmentation (hemosiderin) with villous transformation of the synovial lining. Hemosiderin, a magnetic material, is expected to alter the MRI signal. In our series, deposits of hemosiderin were observed in all cases, appearing as low signal areas in T1WI and T2WI images. FFE is a gradient-recalled echo sequence and is best to show the deposits of hemosiderin, as noted by Lin et al. [4]. Our data also confirmed Lin’s observation that the lesions all showed diffuse increased signal intensity throughout, and obscured the hemosiderin deposits on short inversion time inversion recovery sequence, a fat-suppressed sequence [4]. The deposits of hemosiderin vary markedly in severity, from tiny low signal particles to large areas of low signal. Although hemosiderin deposits in the soft tissue are not exclusive for PVNS, they can be seen in hematomas, giant cell tumors, and pseudoaneurysms as the results of hemorrhage [7], but the combination of hemosiderin deposits, villonodular soft tissue masses and/or multiple bone erosion is highly diagnostic for PVNS. Joint effusion, synovial thickening and soft tissue masses are similar in density on radiographs, but they can be easily differentiated with MRI. There is thick soft tissue around the hip, which makes it difficult to show the soft tissue abnormalities on radiographs, but MRI can clearly show the soft tissue changes in the hip. In our series 9 cases had contrast-enhanced MRI scans, but these did not help the diagnosis.
In conclusion, our data clearly demonstrated that MRI is very good in depicting the extent of PVNS, and the combination of synovial proliferation, soft tissue masses, deposits of hemosiderin and bone erosion around the joint is highly diagnostic for PVNS. Contrast enhancement is not necessary. Therefore, when PVNS is suspected clinically or radiographically, MRI should be prescribed.
Abbreviations
- FFE:
-
Fast field echo
- PVNS:
-
Pigmented villonodular synovitis
References
Edeiken J, Hodes PJ (1973) Roentgen diagnosis of diseases of bone, 2nd edn. Williams & Wilkins, Baltimore, pp 827–834
Mulder JD, Schutte HE, Kroon HM, Taconis WK (1993) Radiologic atlas of bone tumors. Elsevier, Amsterdam, pp689–695
Hughes TH, Sartoris DJ, Schweitzer ME, Resnick DL (1995) Pigmented villonodular synovitis: MRI characteristics. Skel Radiol 24:7–12
Lin J, Jacobson JA, Jamadar DA, Ellis JH (1999) Pigmented villonodular synovitis and related lesions: the spectrum of imaging findings. AJR 172:191–197
Cotten A, Flipo RM, Chastanet P et al. (1995) Pigmented villonodular synovitis of the hip: review of radiographic features in 58 patients. Skel Radiol 24:1–6
Jaffe HL, Lichtenstein L, Sutro CJ (1941) Pigmented villonodular synovitis, bursitis and tenosynovitis: a discussion of the synovial and bursal equivalents of tenosynovial lesion commonly denoted as xanthoma, xanthogranuloma, giant cell tumor or myeloplaxoma of tendon sheath, with some consideration of this tendon sheath lesion itself. Arch Pathol 31:731
Burquist TH (2001) MRI of the musculoskeletal system, 4th edn. Lippincott Williams & Wilkins, Philadelphia, pp 838–909
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheng, X.G., You, Y.H., Liu, W. et al. MRI features of pigmented villonodular synovitis (PVNS). Clin Rheumatol 23, 31–34 (2004). https://doi.org/10.1007/s10067-003-0827-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-003-0827-x