Abstract
Adolescents with gender dysphoria (GD) often face various associated social, emotional, and behavioral difficulties. In such a marginalized group, it is crucial to identify factors that may impact psychological functioning to better accommodate their needs. Therefore, the present study investigated the impact of two specific risk factors, poor peer relations and general family functioning, on the development of psychological problems in adolescents with GD, and their possible interaction effect. The Youth Self-Report, a Peer Relations Scale, and a General Family Functioning scale were assessed in a sample of n = 180 clinically referred adolescents (mean age 15.5; 146 transgender boys with a female birth-assigned sex, and 34 transgender girls with a male birth-assigned sex) with a complete GD diagnosis (fulfillment of the DSM 5 criteria A and B) at their initial admission to the Hamburg Gender Identity Service. Multiple linear regression analysis was conducted to examine the relationship between peer relations, family functioning, and psychological functioning outcomes. Adolescents with GD presented significantly higher Internalizing and Total Problem scores compared to the German reference norm. Externalizing problems were above the norm for transgender boys, but within the normal range for transgender girls. Multiple regression analysis revealed that, overall, adolescents with an advanced age, a female birth-assigned sex, poorer peer relations, and poorer family functioning showed more behavioral and emotional problems. Consequently, incorporating both the family and social environment in transgender care is of high importance to adequately tend to the needs of adolescents with GD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Peer relationships and family functioning that provide social support are two important protective factors for long-term mental health outcomes in young people [1]. Adolescents with gender dysphoria (GD) [2] often face a palette of associated (not only social, but also emotional and behavioral) difficulties or psychological problems [3,4,5,6]. However, it has not been sufficiently studied why adolescents with GD experience these problems and how they can best be accommodated. Poor peer relations (PPR) have been identified as one main risk factor that negatively impacts psychological functioning in adolescents with GD [4,5,6]. Family support has been identified as a protective factor against health risks in gender-diverse children and adolescents [7,8,9]. However, most studies lack the direct comparison of the positive or negative relationship or the interaction between peer relations, family functioning, and psychological functioning outcomes in adolescents with GD.
Adolescents with GD experience a distressing incongruence between their birth-assigned sex and the gender with which they identify [2]. Currently, gender identity clinics or specialized services worldwide are experiencing an increase of referrals for GD-related health care [10, 11]. While birth-assigned male children/transgender girlsFootnote 1 constituted the majority initially, there is a fairly recent development in which increase of clinically referred adolescent transgender boysFootnote 2 seeking help regarding gender identity has been observed in North American and Northern European clinics [12,13,14]. Most specialized gender identity clinics internationally furthermore report similar findings on psychological functioning: a higher prevalence of Internalizing problems (such as low self-worth, feelings of depression, self-harming behaviors/suicide attempts, and suicidal ideation) than Externalizing problems are reported in both children and adolescents with GD [4, 5, 15,16,17,18]. Adolescents seem to face significantly more behavioral and emotional problems, as measured by the Child Behavior Checklist (CBCL) or its equivalents Youth Self-Report (YSR) and Teacher’s Report Form (TRF), than do younger children with GD [17]. Most studies have reported an increased predominance of Internalizing problems in transgender girls compared to transgender boys, and the opposite for Externalizing problems [4, 5, 16, 17]. Clinical and population-based studies have also shown that children and adolescents who deviate from the socially defined gender norms report elevated rates of self-harming behavior and suicidal thoughts/tendencies [18,19,20]. In adolescents with a desire for gender-affirming medical interventions, these symptoms have been shown to diminish after treatment, though the treatment effects have not yet been researched sufficiently [21,22,23,24], and not all adolescents with GD express the need or desire for medical intervention [25, 26].
Despite risk, maintaining or rebuilding psychological well-being or mental health can be achieved with the help of various protective factors [1, 27, 28]. Social support can generally be defined as having someone outside the family, such as friends, peers, teachers or other caregivers, who listens and provides support. Social support has been investigated as one of the most important indicators of personal resources or protective factors of psychological well-being [1, 29, 30]. For adolescents in general, the peer group is of high importance for psychosocial development [31]. Two other well-established protective factors that have been identified as indicators of good mental health outcomes are self-efficacy and family climate [1, 30]. In well-functioning families, parents and children maintain close emotional relationships, support each other, and spend time together [1, 32,33,34]. The general functioning of a family (e.g., support, communication, acceptance, and connectedness) can be measured, e.g., via the general family functioning (GFF) scale of the McMaster’s Family Assessment Device (MFAD) [35, 36]. In German children and adolescents from the general population, positive changes in these protective factors over time were related to fewer symptoms of depression in the long term [1]. Furthermore, it has been argued that the potential interaction of these factors can protect or decrease the risk of poor mental health outcomes, e.g., that the family can promote emotional and behavioral resilience to negative peer experiences [32].
In gender-diverse children and adolescents, poor peer relations have been identified as one of the main factors impacting psychological or emotional and behavioral outcomes [5, 6, 17]. According to the Sexual Minority Stress Model postulated by Meyer [37], which was adapted to a gender-diverse population by Testa et al. [38], experiences of discrimination, violence, rejection, and victimization increase distress and subsequently negatively affect mental health in gender-diverse individuals. Peer problems often faced by adolescents with GD include negative reactions to gender-diverse behavior, varying from unwanted questions regarding one’s gender to physical abuse [19, 39]. For example, more strongly expressed gender diversity is linked to a greater likelihood of being victimized at school [39].
On the other hand, family support [7,8,9] and the overall family connectedness [8, 34] seem to be related to significantly better psychological outcomes in transgender or gender-diverse children and adolescents. In a Canadian study assessing the mental health of 923 gender-diverse adolescents and young adults, the feeling of family connectedness was the strongest protective predictor of better outcomes among those aged 14–18 years [34]. However, while family can function as a protective factor for children and adolescents with GD and for young people in general, families can also act as potential stressors or risk factors. For example, Grossman and D’Augelli reported in their study of 55 gender-diverse adolescents that approximately 50% of subjects said they had “sometimes” or “often” been insulted, made to feel guilty, and embarrassed in front of others for their gender expression by their parents. Additionally, 13–36% of subjects reported “sometimes” or “often” being physically abused by their parents in relation to their gender identity [19]. Although one of the main reasons for poor outcomes in adolescents with GD may be social ostracism [39, 40] or poor peer relations, several experts suggest that there might be other sources of distress and that the experience of GD itself may be inherently distressing [18, 19, 41]. Furthermore, variance in transitioning socially (and thus, the degree of variation in gender presentation among adolescents, in how far they have “outed” themselves to others, or live in their preferred gender role) might impact peer relationship patterns [6]. Not only do peers seem to be responsible for experiences of discrimination and related distress, but also both family and peers may possibly act, and also interact, in the relationship with positive or negative health outcomes.
Therefore, the present study investigates the impact of two specific potential protective or risk factors on psychological problems in adolescents with GD: poor peer relations and general family functioning. Potential effects of the interaction between the risk factors (peer problems and impaired family functioning) are investigated. Their possible interaction is examined as a protective factor to provide prevention strategies. To be able to draw conclusions about the overall psychological functioning of this sample compared to the German norm, comparisons with the age-equivalent German T-scores of the YSR will be made. Additionally, the study includes control factors that may also impact psychological functioning: gender, age, the degree of cross-gender identification (or GD), the degree to which adolescents have undergone a social transition, the families' socioeconomic status, and their living situation (parents' marital status).
Methods
Study design
The present study followed a cross-sectional, questionnaire-based, single-subject study design. Data were collected between September 2013 and June 2017 from clinically referred adolescents at the Hamburg Gender Identity Service for Children and Adolescents. This clinic at the University Medical Center Hamburg-Eppendorf offers specialized services for children and adolescents with gender identity issues with a possibility of a referral to an endocrinology specialist for further medical (hormonal) treatment. Diagnostic and treatment procedures conform to the international guidelines provided by the World Professional Associations for Transgender Health (WPATH) [21] and are performed by psychosocial staff (e.g., clinical psychologists). All families who attended the Hamburg Gender Identity Service were invited to complete a set of self- and parent-report questionnaires during their first visit to the clinic and thus before undergoing any psychosocial or medical treatment. The local ethical committee in Hamburg approved the study. Participation was voluntary, and written informed consent was obtained from all study participants (parents as well as the participating adolescents) according to institutional guidelines.
Participants
This study assessed clinically referred adolescents living in Germany complying with the diagnostic criteria for GD according to the DSM 5 [2]. All families with initial visits to the clinic between September 2013 and June 2017 (n = 434 gender-diverse children and adolescents; 72% birth-assigned females and 28% birth-assigned males) were invited to complete a set of questionnaires during their first appointment (see Fig. 1). Information was obtained at baseline (upon clinical entry) from adolescents (aged 11 and above), parents, and clinicians. Adolescents’ self-reporting was voluntary (which resulted in n = 124 dropouts due to lack of participation and n = 40 missing questionnaire sets or informed consent forms). Because self-reporting was performed by those aged 11 and above, parental reports of n = 38 children (aged 5–10) were excluded from the present analyses. Further inclusion criteria for the study were a sufficient command of the language as well as an absence of a severe psychiatric diagnosis, such as psychosis (which resulted in the exclusion of another n = 8 individuals), and no prior medical treatment (which resulted in the exclusion of another n = 2 individuals). Additionally, the present study focused on adolescents with complete diagnostic criteria of GD (fulfilling both A- and B-criteria according to the DSM 5, assessed by specialized clinicians from the Gender Identity Service around 6 months after clinical entry, and thus, after participation in the study). Therefore, during the process of data cleaning, an additional n = 42 adolescents, who did not, or not by the time of analysis, receive a complete diagnosis were excluded from the analysis. Thus, for the present study, the complete data of n = 180 clinically referred adolescents (aged 11–18 years), who fulfilled all the DSM 5 diagnostic criteria for GD at the time of data analysis and their families were included in the final analyses (see Fig. 1).
To compare socio-demographic characteristic and psychological functioning between selected participants (n = 180) and participants who were not included in the analysis (because they did not fulfill diagnostic criteria; n = 42), t tests for age and psychological functioning outcomes (Internalizing problems, Externalizing problems, and Total Problem scores) were carried out. The included and excluded adolescents did not significantly differ in age or any of the psychological outcome measures. To compare categorical variables, such as gender and socio-demographic measures, Chi-squared tests (χ2) were applied. The relation between socio-demographic characteristics and inclusion/exclusion was not significant. Compared to birth-assigned females/transgender boys (30 out of 176), slightly more birth-assigned males/transgender girls were excluded from the analysis because they did not fulfill diagnostic criteria (12 out of 46). Thus, the sex ratio of the analysis sample favored transgender boys (81%) compared to transgender girls (19%) even more strongly than upon clinical entry (72% vs. 28%). However, neither the relation between gender and inclusion/exclusion nor the relation between gender and the fulfillment of diagnostic criteria was statistically significant.
Measures
Socio-demographic and clinical features
The following socio-demographic measures were included in the analyses: gender, age at assessment, parent’s marital status, and parental socioeconomic status (SES). The parent’s marital status variable was based on the parent’s current living situation and relationship status. The parent filling out the questionnaire was asked whether she or he lived together in the same household as the mother/father of the child concerned. Parent’s marital status and living situation were divided into two subgroups: “both parents (living together or married) vs. “other” (parents living as single parent, separated, divorced, widowed, or living with new spouse or partner). For the regression analysis, the two dichotomous items, gender and parent’s marital/living situation, were dummy coded (0 = transgender boys, 1 = transgender girls; and 0 = parents not living together/married, 1 = parents living together/married, respectively).
The SES was measured based on the Winkler Index [42], which considers education, income, and job position of both parents, resulting in a sum score that ranges from 3 to 21. In the present study, the score was based on 3 three-point variables and thus ranged from 3 to 9: educational background of the parent with the highest status (1 = no or lower education; 2 = middle or technical school; 3 = higher education or university); household income (1 = less than 2.000€ per month; 2 = 2.000 - 4.000€ per month; 3 = more than 4.000€ per month); and job position of the parent with the highest status (1 = lower occupation or unemployed; 2 = skilled occupation or self-employed; 3 = executive or academic occupation). In the socio-demographic description, participants were categorized into groups with low (scores from 1 to 3), middle (scores from 4 to 6), and high SES (scores from 7 to 9).
Additionally, to measure “cross-gender” identification (experiences of belonging to the “other” gender), a sum score assessed in previous studies (e.g., [5]) was used: in the YSR, items 5 and 110 relate to cross-gender experiences (“I act like the opposite gender”, and “I wish I were of the opposite gender”). Although it was excluded from the Total Problem score, this sum score can be used independently as a measure to calculate the degree of GD (with a binary understanding of cross-gender identification). It has a range from 0 to 4, rated on two scales ranging from 0 = “not true” to 2 = “very true or often true”.
Social transitioning was measured using a self-constructed item that assessed the degree to which adolescents had undergone a complete social transition, or lived in their preferred gender role in three different life areas, respectively: at home, with friends/in their peer group, and at school. Since multiple answers were possible, the combination of the different answers were recoded as follows: 1 = “no social transition, yet (living in birth-assigned gender role)”; 2 = “partial social transition in at least 1 out of 3 life areas (or in-between gender roles)”; 3 = almost complete social transition (living in the new gender role in at least 2 out of 3 life areas; e.g., at home and with friends, but not in school)”; 4 = “complete social transition in all life areas (living in the new gender role of the preferred gender at home, with friends/peers and at school)”. Resulting in a four-point scale, this measure allows for the assessment of the gradual degree to which a child/adolescent has transitioned to another gender role, socially.
Psychological functioning
Behavioral and emotional problems were assessed via the 1991 German version of the Youth Self-Report (YSR) for adolescents aged 11–18 years [43,44,45]. The YSR consists of 120 items, which are rated on a 3-point scale ranging from 0 = “not true” to 2 = “very true or often true”. Thus, a higher score reflects a greater degree of the respective problems. The total sum of all problems’ scores is reflected in the Total Problem score, whereas two main scales can be conducted (Internalizing and Externalizing problems). Additionally, clinical range scores (> 90th percentile; T-scores > 63) can be reported for these three indices. The adolescent German norm population (aged 11–18) based on the birth-assigned sex-specific T-scores for all three scales are provided by Döpfner et al. [44]. These population-based converted T-scores were birth assigned, sex and age adjusted, and assigned and calculated for each scale in addition to sum scores in the present study. These norm scores allow to determine whether the scores of our sample lie within the norm range of the respective German population. The decision to match T-scores based on the sex-assigned at birth was made to control for possible normative (birth-assigned) sex effects.
The following items were excluded from the Total Problem score (resulting in 102 items): 2 health-related items (“allergies” and “asthma”), 16 items regarding socially desirable behavior, and 2 items measuring cross-gender identification. Item 85 (“strange ideas”) was excluded from the Total Problem score if the answer given was related to intense or obsessive feelings that could be related to GD (e.g., “belonging to the opposite gender”). In our sample, Cronbach’s alpha for the Internalizing, Externalizing and Total Problem scales was between α = 0.83 and 0.93.
Poor peer relations (PPR)
The degree of problems experienced in social interactions with peers were measured via three items from the YSR: item 25 (“I don’t get along with other kids”), item 38 (“I get teased a lot”), and item 48 (“I am not liked by other kids”). The PPR has been used in various studies investigating young people referred for GD (e.g., [4,5,6, 17, 46]). In the present sample, Cronbach’s alpha of the scale was α = 0.72. A higher score on the PPR scale indicates poorer peer relations, or higher levels of peer related problems, respectively (range 0 - 6).
General family functioning (GFF)
The McMasters’ Family Assessment Device (MFAD) is a questionnaire designed to evaluate the functioning of a family based on the McMasters’ Model of Family Functioning using seven different scales measuring the structural, organizational, and transactional characteristics of families [36]. The seventh scale consists of 12 items on a 4-point measure and evaluates family functioning, such as family support (“In times of crisis we can turn to each other for support”) and acceptance (“Individuals are accepted for what they are”). The reliability and validity of the general family functioning (GFF) scale has been confirmed [35]. In the present study, Cronbach’s alpha was α = 0.89. A higher score on the GFF scale of the MFAD indicates lower levels of family functioning, or poorer/ impared experienced support from the family (range 1 - 4), while the cutoff for categorical analysis (meaning “problematic” family functioning) is set at 2.17 [35].
Statistical analysis
Individual missing values were ascribed to by using the expectation–maximization (EM) algorithm [47]. To test for gender group differences or relationships in the demographic and clinical characteristics, either t-tests or Chi-squared tests (χ2) were used. The statistical power of results was evaluated using Phi (ϕ) or the effect size given by Cohen’s d [48].
The further statistical analysis was divided into two steps. First, behavioral and emotional problems of the participating adolescents with GD were evaluated using mean raw scores, T-scores, and confidence intervals. T-scores were assigned for each raw score of the three YSR Scales (Internalizing, Externalizing and Total Problem score) to allow a comparison with the age-equivalent population-based German norm [44]. Presuming the T-distribution to be normal (M = 50; SD = 10), confidence intervals that are not within the normal range (and therefore do not include the mean norm M = 50) differ significantly from the reference group of the same-aged birth-assigned sex [49]. If confidence intervals of two groups overlap, it can be assumed that the results do not significantly differ from one another [49]. Therefore, statements about the sample’s possible deviations from the norm population can be made.
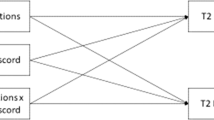
Second, a multiple linear regression analysis was conducted, using the raw scores of the YSR Total Problem score as an outcome, to identify predictors of behavioral and emotional problems. For the regression analysis, an adapted version of the YSR Total Problem score was used, excluding peer-related problems (items 25, 38, and 48) and cross-gender identification (items 5 and 110; resulting in a sum score of 97 items). The predictors were entered blockwise into the regression model via direct entry in four steps. In the first step, the control variables age, gender, cross-gender identification, social transition, SES, and parent’s marital/living situation were included in the model to account for possible confounding effects. Gender and parent’s marital/living situation were the only dichotomous variables in the model. In the second step, PPR was added to the model to identify the impact of poor peer relations on the outcome of our German sample. In the third step, the GFF Scale was introduced to the model to determine whether and to what extent family functioning explained further variance of the model. Both scales, the PPR and GFF, were centered at the mean to avoid possible problems with multicollinearity. In the fourth step, the interaction of PPR and GFF (PPR × GFF) was introduced to account for the possibility of both aspects influencing each other, or of the family acting as a protective factor for poor peer relations. In a multiple regression with n = 180 cases and 9 predictors, an average effect (f = 0.15) can be tested with a power of 97% (calculated with GPower).
Results
Socio-demographic and clinical features
Table 1 provides an overview of all socio-demographic and clinical characteristics. In total, more transgender boys were referred to the clinic and included in the analyses (n = 146, 81%) than transgender girls (n = 34, 19%). There was no significant age difference between transgender boys (mean age = 15.5, SD = 1.33) and transgender girls (mean age = 15.5, SD = 1.47), and no relationship between age and diagnosis could be found. Furthermore, there was no significant difference between transgender boys and transgender girls with regard to parent’s marital status as well as the families' SES. The majority of the sample, however, came from a family with a medium (53%) or high (44%) socioeconomic background.
The only two scales revealing a significant difference between the two gender groups was the scale measuring cross-gender identification/GD and the degree of social transition, in which transgender boys reported stronger cross-gender identification and a higher degree of (complete) social transition than did transgender girls.
Poor peer relations (PPR) and general family functioning (GFF)
An overview of the mean PPR and GFF scores are presented in Table 1. The present sample of adolescents reported high levels of peer-related difficulties. There was no signficant discrepancy between transgender boys and girls: for gender group comparisons, according to Cohen’s proposition for the classification of effect sizes [48], the effect size was low (d = 0.29). The majority of adolescents (63.9%) reported having experienced peer-related problems to at least some degree in the preceding 6 months (measured as agreement with any of the three items). Of the three items, item 48 “I am not liked by other kids” was among the two most frequently rated items (50.6%).
On average, transgender adolescents reported GFF leveling just below the cutoff at 2.17. However, one-third (34%) of the participants scored above the cutoff for “problematic” GFF. There was no gender disparity, Cohen’s effect size was observed to be d = 0.00.
Psychological functioning compared to the German norm
All the results of the three YSR scales are presented in Table 2. Looking at the confidence intervals, significant (non-overlapping 95% confidence intervals) deviations of T-scores from the German norm population (M = 50; SD = 10) were found with regard to almost all scales for the total sample, with the one exception being Externalizing problems in transgender girls. In total, Internalizing problems were far more common among transgender adolescents than Externalizing problems. On average, the present sample scored more than 1.5 SD higher for Internalizing problems than same-aged adolescents from the German reference group. Externalizing problems were within the normal range for transgender girls, but slightly elevated for transgender boys. The Total Problem score ranged more than a full standard deviation above that of the German reference group. The majority of the adolescents struggled with Internalizing problems within the clinical range (> 90th percentile; T-scores > 63; 55%). Transgender girls reported a higher percentage of clinically significant Internalizing problems (67.6%) than did transgender boys (52.1%). The clinical range for the Total Problem score showed no gender discrepancy with the overall percentage of 44.4%.
Multiple linear regression analysis: predictors of psychological functioning
Table 3 provides an overview of the multiple linear regression and the results of the final model. The results of the preceding steps were: first model (adjusted R2 = 0.036, F(6) = 2.112, p < 0.54), second model (adjusted R2= 0.233, F(7) = 8.754, p < 0.001) and third model (adjusted R2= 0.330, F(8) = 12.012, p < 0.001). The overall model fit was satisfactory, explaining 33% of the variance for the Total Problem score (and thus emotional and behavioral problems). The variance of inflation (VIF = 1.12) was not substantially greater than 1. The Durbin–Watson statistic was 1.96, indicating independence of distributions; a value of 2 would indicate perfect independence. With regard to multicollinearity or autocorrelation, no potential biases were evident: the highest correlations between two of the independent variables included were r = 0.44 between GFF and the YSR Total Problem score, and r = 0.44 between PPR and the YSR Total Problem score.
Significant predictors for the Total Problem score of the YSR in the final model were the following: a female birth-assigned sex and a higher age. The other control variables, cross-gender identification, social transition, SES, and the parent’s marital/living situation, were not significantly related to the outcome. In addition, both poor peer relations (PPR) and general family functioning (GFF) were significant predictors for higher Total Problem scores. After including GFF in the model, the adjusted R2 increased from 23 to 33%, implying that higher scores of (and thus, poorer) family functioning predicted poorer psychological functioning. However, the interaction between both factors (GFF and PPR; see fourth model) did not significantly predict the outcome.
Discussion
The present study is one of the first analyses in Germany to examine the standardized measures of psychological functioning in a large, systematically assessed sample of clinically referred adolescents with a GD diagnosis at baseline. The main aim of this study was to increase the understanding of how both peer relations and family functioning predicted psychological functioning in adolescents with GD. In addition, this study aimed at examining whether these two potential risk factors interacted, and whether this interaction might function as another risk or protective factor against perceived stress. To account for the potential confounding effect of gender, age, the degree of GD, and to which degree adolescents have already undergone social transitioning, the families' SES and living situation were included in the present analysis.
Psychological functioning (YSR)
Overall, transgender adolescents with poorer peer relations, poorer family functioning, more advanced age, as well as transgender boys overall, showed more behavioral and emotional problems. These findings are consistent with previous research focusing on various aspects of possible risk and protective factors in transgender children and adolescents [e.g. 9, 20, 52]. In particular, the Total Problem scores and Internalizing problems (measured via the YSR) were elevated compared to the adolescent German norm, whereas the Externalizing scale was only elevated in adolescent transgender boys. Furthermore, both PPR and GFF positively predicted psychological functioning. The GFF did not significantly interact with PPR, and thus no conclusions can be drawn with regard to the possible function of the family as a protective factor against peer problems [1, 32]. However, possible mediating effects would need to be assessed in longitudinal designs applying different statistical methods to draw sufficient conclusions about risk and protective factors and how they interact over time [1, 9].
Similar to previous analyses which found high prevalence of associated psychiatric diagnoses [3], Internalizing problems, and impaired quality of life [50] in previous samples from the Gender Identity Service in Hamburg, psychological functioning was significantly lower in adolescents with GD than in their reference group in the German norm. The results obtained by using standardized measures on emotional and behavioral problems revealed patterns in psychosocial difficulties similar to those reported by most of the existing international literature [4], such as displaying more Internalizing than Externalizing problems [5, 16, 17]. The participants scored above the clinical cutoff on the mean Total Problem score and were within the clinical range on Internalizing problems. Consistent with prior research, Internalizing (e.g., being anxious/depressed or reporting somatic complaints) problems were far more common than Externalizing (e.g., rule-breaking and aggression) problems. Furthermore, transgender boys showed elevated tendencies for Externalizing problems, while transgender girls did not differ significantly from the norm [4, 5, 16]. The results on gender differences call for further investigation, especially considering the current increase of clinically referred transgender boys, and the resulting shift in the sex ratio of clinically referred adolescents favoring transgender boys [12,13,14].
Poor peer relations (PPR)
The majority of both transgender boys and transgender girls in the present study reported having experienced peer-related difficulties at least to some extent in the preceding 6 months, which also significantly predicted the outcome, overall psychosocial functioning. Previous studies assessing adolescents with GD found that the quality of peer relations plays a vital role in the gender-diverse adolescents’ psychosocial functioning: the 3-item metric of PPR was the strongest predictor of YSR emotional and behavioral problems in most of these studies [5, 6, 17, 18, 46]. This is possibly also due to the social ostracism resulting from their marked gender-diverse behavior. Among adolescents with GD, (gender) bullying, a smaller number of same-gender friends at school, or peer-related difficulties, social isolation, and stigmatization are significantly linked to emotional and behavioral problems (or stress, respectively) [5, 6, 17, 39,40,40]. The sense of well-being in school inevitably intersects with peer relations, as young people spend much of their time in school [50]. Therefore, it is worrisome that many adolescents with GD perceive their peer relations as rather poor. This observation indicates that collaboration with pedagogical staff and school management (e.g., to reduce bullying, or help with questions regarding which changing area to use, etc.) may be required to support young transgender people in daily school life [21, 39, 50, 51].
General family function (GFF)
Next to peer relations, in the present study, the functioning level of the families, in regard to how far they generally supported their child or in how accepted adolescents felt by their families, was positively related with overall psychological functioning outcomes: A higher GFF score, and thus, poorer family functioning, significantly predicted a higher problem score, and thus impaired psychological functioning. The GFF Scale explained another 10% of the total variance within the Total Problem score. A few previous studies have indicated that parental support regarding the gender identity of a child was related to lower psychosocial difficulties in children [8] and higher quality of life in adolescents [7]. Among adolescents from the general population [1, 32] as well as among transgender adolescents, parental support [7, 9] and family connectedness [52] can act as protective factors against distress or mental health issues, including depression. On the other hand, parental abuse is significantly related to suicide attempts in transgender adolescents [19]. Considering the heightened vulnerability and poor peer relations, parental support may potentially act as a buffer against the experiences of minority stress and thus emphasizes the importance of benevolent support by the community throughout childhood and adolescence [7, 9, 53, 54]. Although this interaction was not significantly supported by the present results, the relationship between these addressed determinants may need to be assessed further in future research, possibly via the application of better validated measures.
Limitations
One of the limitations of this study was the difference in sample sizes of transgender boy and transgender girl participants. A significantly higher percentage of birth-assigned female (72%) than birth-assigned male children and adolescents (28%) was referred to the Hamburg Gender Identity Service. Similarly, more adolescent transgender boys (81%) than transgender girls (19%) were included in the analysis sample. However, the number of male-assigned children referred to the service exceeded that of female-assigned children, while the opposite held for adolescents (which explains the relative increase in birth-assigned females in the older adolescent sample). Although consistent with current developments, this shift in gender ratio from childhood to adolescence appears to be exceptionally high compared to other samples [12,13,14] and might thus result in a sample bias in the present study. Therefore, the conclusions drawn from our sample need to be further investigated in future research to account for possible different needs of adolescent transgender boys and girls. It remains difficult to conclude whether such differences are related to greater societal tolerance or really a result of higher prevalence, although a German study on adolescent school children aged 10–16 years showed that gender variant experiences were more prevalent among birth-assigned female adolescents from the general population, as well [55].
Furthermore, the selection of the sample might have implications for the generalizability of the present findings. For example, because these data were solely derived from German adolescents with a medium to high socioeconomic background, a complete diagnosis of GD (fulfillment of both criteria A and B) and the wish to undergo medical treatment, findings of this study might not translate to different countries or more diverse populations, as previous research has for example identified possible cultural differences [4]. The findings may also not translate to all gender-diverse samples, including self-identified transgender, or non-binary adolescents [52, 40]. Lastly, the available data may over- or underestimate the true picture of mental health in this population and the effects of peer relations and family context. Another limitation can be linked to the use of some of the measures in the present study: both the peer relations scale and the cross-gender identification scale were derived from the YSR; the cross-gender identification scale has not been validated in this population. Due to the possible lack of measurement of the multiple dimensions of peer relations and support, intensity of GD, or the degree of transitioning socially, other measures might provide more accurate representations of these concepts. There are alternatives for measuring GD, such as the Utrecht Gender Dysphoria Scale [46], which are mostly applicable to binary identified samples, as well. However, there is a lack of validated alternatives for measuring the unique experiences of peer relation problems, peer support, non-binary identification, or the degree of transitioning socially in young transgender populations.
Implications
In a marginalized group, such as adolescents with GD, it is crucial to identify factors that may impact psychological functioning to better accommodate their needs. Regardless, similar to studies from the USA [7, 8], Canada [6, 11, 52], The Netherlands [5, 15, 17], and various European countries [4, 16], the present study highlights the importance of relationships with peers. Additionally, it highlights the role of the family and the possible negative outcomes if any of these relationships are impaired or problematic, in a direct comparison to each other. As this is the first study from Germany to directly assess psychosocial outcomes and these associations with each other in a sample of clinically referred adolescents with GD, the results add to the general knowledge of possible risk and protective factors among transgender or gender-diverse populations. The next step should be a long-term assessment of such outcomes in relation to treatment experiences, as both psychosocial support and gender-affirming medical interventions are likely to affect psychological functioning in the long term [21,22,23,24]. To sufficiently predict the development of long-term psychosocial outcomes for transgender populations, the unidirectional analysis of the influence of parents and peers on the mental health in a cross-sectional design is insufficient. Longitudinal assessments over multiple time points and analyses of bidirectional associations between transgender adolescents and their social environments, and possible mediators, are urgently needed to be able to predict the mental health in the long term. Similar to parents, adolescents also shape the relationships with their peers and families and may thus also affect their reactions. Therefore, an important future research goal would be to identify additional possible factors that help empower gender-diverse adolescents in growing into self-confident adults and help them navigate through their social surroundings. Researching the impact of family support, authors such as Pullen Sansfaçon et al. [54] urge practitioners to recognize the challenges that families encounter in supporting their transgender or gender-diverse children. The cited authors note the need for services that account for individual experiences of gender-diverse children and encourage parents to support each other [54]. Accordingly, approaches that focus on family and/or parental self-help groups should be beneficial to the overall well-being of the whole family. Resilience factors, such as coping or social support, can alleviate the negative impact of potential stressors and risk factors [9, 37]. Individual treatment concepts, which aim to strengthen the resilience of a member of a minority [37, 53], such as coping and social support, may buffer the effect of potential stressors and aim to encourage young people with GD to mature into self-assured and confident individuals [21]. However, further research is needed to study the correlation between the specific needs of this population and other possible factors, such as self-efficacy [1].
The present study showed that, similar to poor peer relations, a poorer family functioning strongly predicted impaired psychological outcomes. Therefore, both factors may increase the risk of impaired psychological functioning in adolescents with GD. However, these two risk factors did not significantly interact and may thus be regarded as independent factors. Although peer- and family-related difficulties might not pertain equally to all treatment- and non-treatment-seeking adolescents and gender-diverse adolescents, the results obtained here suggest that, when present, they have a strong impact on the adolescents’ overall psychological well-being and will very likely have consequences for future treatment outcomes and adjustment. The important roles both peers and families play with regard to the mental health of adolescents with GD point toward the need for a holistic and integrated approach to transgender health [21, 41]. Beyond the support of transitioning both medically and socially, mental health professionals may play a role in assisting the whole family regarding the overall development and should therefore aim at equally including the entire social environment in the care for adolescents with GD.
Notes
Male birth-assigned sex, identifying as female.
Female birth-assigned sex, identifying as male.
References
Klasen F, Otto C, Kriston L et al (2015) Risk and protective factors for the development of depressive symptoms in children and adolescents: results of the longitudinal BELLA study. Eur Child Adolesc Psychiatry 24:695–703. https://doi.org/10.1007/s00787-014-0637-5
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (DSM-5®). American Psychiatric Pub
Becker I, Gjergji-Lama V, Romer G, Möller B (2014) Merkmale von Kindern und Jugendlichen mit Geschlechtsdysphorie in der Hamburger Spezialsprechstunde. [Characteristics of Children and Adolescents with Gender Dysphoria Referred to the Hamburg Gender Identity Clinic.] Prax Kinderpsychol Kinderpsychiatr 63:486–509. https://doi.org/10.13109/prkk.2014.63.6.486
de Graaf NM, Cohen-Kettenis PT, Carmichael P, et al (2017) Psychological functioning in adolescents referred to specialist gender identity clinics across Europe: a clinical comparison study between four clinics. Eur Child Adolesc Psychiatry. https://doi.org/10.1007/s00787-017-1098-4
de Vries ALC, de Steensma TD, de Cohen-Kettenis PT et al (2016) Poor peer relations predict parent- and self-reported behavioral and emotional problems of adolescents with gender dysphoria: a cross-national, cross-clinic comparative analysis. Eur Child Adolesc Psychiatry 25:579–588. https://doi.org/10.1007/s00787-015-0764-7
Shiffman M, VanderLaan DP, Wood H et al (2016) Behavioral and emotional problems as a function of peer relationships in adolescents with gender dysphoria: A comparison with clinical and nonclinical controls. Psychol Sex Orientat Gend Divers 3:27–36. https://doi.org/10.1037/sgd0000152
Simons L, Schrager SM, Clark LF et al (2013) Parental support and mental health among transgender adolescents. J Adolesc Health Off Publ Soc Adolesc Med. https://doi.org/10.1016/j.jadohealth.2013.07.019
Olson KR, Durwood L, DeMeules M, McLaughlin KA (2016) Mental health of transgender children who are supported in their identities. PEDIATRICS 137:e20153223–e20153223. https://doi.org/10.1542/peds.2015-3223
Birkett, McConnell, Mustanski (2016) Families matter: social support and mental health trajectories among lesbian, gay, bisexual, and transgender youth. J Adolesc Health 59:674–680. https://doi.org/10.1016/j.jadohealth.2016.07.026
Arcelus J, Bouman WP, Van Den Noortgate W et al (2015) Systematic review and meta-analysis of prevalence studies in transsexualism. Eur Psychiatry J Assoc Eur Psychiatr 30:807–815. https://doi.org/10.1016/j.eurpsy.2015.04.005
Zucker KJ, Bradley SJ, Owen-Anderson A et al (2008) Is gender identity disorder in adolescents coming out of the closet? J Sex Marital Ther 34:287–290. https://doi.org/10.1080/00926230802096192
Aitken M, Steensma TD, Blanchard R et al (2015) Evidence for an altered sex ratio in clinic-referred adolescents with gender dysphoria. J Sex Med 12:756–763. https://doi.org/10.1111/jsm.12817
de Graaf NM, de Giovanardi G, Zitz C, Carmichael P (2018) Sex ratio in children and adolescents referred to the gender identity development service in the UK (2009–2016). Arch Sex Behav 47:1301–1304. https://doi.org/10.1007/s10508-018-1204-9
Steensma TD, Cohen-Kettenis PT, Zucker KJ (2018) Evidence for a change in the sex ratio of children referred for gender dysphoria: data from the center of expertise on gender dysphoria in amsterdam (1988–2016). J Sex Marital Ther. https://doi.org/10.1080/0092623X.2018.1437580
Cohen-Kettenis PT, Owen A, Kaijser VG et al (2003) Demographic characteristics, social competence, and behavior problems in children with gender identity disorder: A cross-national, cross-clinic comparative analysis. J Abnorm Child Psychol 31:41–53
Skagerberg E, Davidson S, Carmichael P (2013) Internalizing and externalizing behaviors in a group of young people with gender dysphoria. Int J Transgenderism 14:105–112. https://doi.org/10.1080/15532739.2013.822340
Steensma TD, Zucker KJ, Kreukels BPC et al (2014) Behavioral and emotional problems on the teacher’s report form: A cross-national, cross-clinic comparative analysis of gender dysphoric children and adolescents. J Abnorm Child Psychol 42:635–647. https://doi.org/10.1007/s10802-013-9804-2
Aitken M, VanderLaan DP, Wasserman L et al (2016) Self-harm and suicidality in children referred for gender dysphoria. J Am Acad Child Adolesc Psychiatry 55:513–520
Grossman AH, D’Augelli AR (2007) Transgender youth and life-threatening behaviors. Suicide Life Threat Behav 37:527–537
Taliaferro LA, McMorris BJ, Rider GN, Eisenberg ME (2018) Risk and protective factors for self-harm in a population-based sample of transgender youth. Arch Suicide Res Off J Int Acad Suicide Res. https://doi.org/10.1080/13811118.2018.1430639
Coleman E, Bockting W, Botzer M et al (2012) Standards of care for the health of transsexual, transgender, and gender-nonconforming people, Version 7. Int J Transgenderism 13:165–232. https://doi.org/10.1080/15532739.2011.700873
Costa R, Dunsford M, Skagerberg E et al (2015) Psychological support, puberty suppression, and psychosocial functioning in adolescents with gender dysphoria. J Sex Med 12:2206–2214. https://doi.org/10.1111/jsm.13034
de Vries ALC, de McGuire JK, Steensma TD et al (2014) Young adult psychological outcome after puberty suppression and gender reassignment. Pediatrics 134:696–704. https://doi.org/10.1542/peds.2013-2958
Hembree WC, Cohen-Kettenis PT, Gooren L et al (2017) Endocrine treatment of gender-dysphoric/gender-incongruent persons: An endocrine society clinical practice guideline. J Clin Endocrinol Metab 102:3869–3903. https://doi.org/10.1210/jc.2017-01658
Clark BA, Veale JF, Townsend M, et al (2018) Non-binary youth: Access to gender-affirming primary health care. Int J Transgenderism 0:1–12. https://doi.org/10.1080/15532739.2017.1394954
Frohard-Dourlent H, Dobson S, Clark BA et al (2017) “I would have preferred more options”: accounting for non-binary youth in health research. Nurs Inq 24:e12150. https://doi.org/10.1111/nin.12150
Masten AS, Cutuli JJ, Herbers JE, Gabrielle-Reed MJ (2009) Resilience in development. Handb Posit Psychol 117–131
Rutter M (2000) Psychosocial influences: critiques, findings, and research needs. Dev Psychopathol 12:375–405
Schwarzer R, Knoll N (2007) Functional roles of social support within the stress and coping process: A theoretical and empirical overview. Int J Psychol 42:243–252. https://doi.org/10.1080/00207590701396641
Wille N, Bettge S, Ravens-Sieberer U, BELLA study group (2008) Risk and protective factors for children’s and adolescents’ mental health: results of the BELLA study. Eur Child Adolesc Psychiatry 17 Suppl 1:133–147. https://doi.org/10.1007/s00787-008-1015-y
Rubin KH, Bukowski WM, Laursen B (2009) Handbook of peer interactions, relationships, and groups. Guilford Press, New York, NY, US
Bowes L, Maughan B, Caspi A et al (2010) Families promote emotional and behavioural resilience to bullying: evidence of an environmental effect. J Child Psychol Psychiatry 51:809–817. https://doi.org/10.1111/j.1469-7610.2010.02216.x
Phillips T (2012) The influence of family structure vs. family climate on adolescent well-being. Child Adolesc Soc Work J. https://doi.org/10.1007/s10560-012-0254-4
Youngblade LM, Theokas C, Schulenberg J et al (2007) Risk and promotive factors in families, schools, and communities: a contextual model of positive youth development in adolescence. Pediatrics 119(Suppl 1):S47–53. https://doi.org/10.1542/peds.2006-2089H
Byles J, Byrne C, Boyle MH, Offord DR (1988) Ontario Child Health Study: reliability and validity of the general functioning subscale of the McMaster Family Assessment Device. Fam Process 27:97–104
Epstein NB, Baldwin LM, Bishop DS (1983) The McMaster family assessment device. J Marital Fam Ther 9:171–180. https://doi.org/10.1111/j.1752-0606.1983.tb01497.x
Meyer IH (2015) Resilience in the study of minority stress and health of sexual and gender minorities. Psychol Sex Orientat Gend Divers 2:209–213. https://doi.org/10.1037/sgd0000132
Testa RJ, Habarth J, Peta J et al (2015) Development of the gender minority stress and resilience measure. Psychol Sex Orientat Gend Divers 2:65–77. https://doi.org/10.1037/sgd0000081
Toomey RB, Ryan C, Diaz RM et al (2010) Gender-nonconforming lesbian, gay, bisexual, and transgender youth: School victimization and young adult psychosocial adjustment. Dev Psychol 46:1580–1589. https://doi.org/10.1037/a0020705
Baams L, Beek T, Hille H et al (2013) Gender nonconformity, perceived stigmatization, and psychological well-being in Dutch sexual minority youth and young adults: A mediation analysis. Arch Sex Behav 42:765–773. https://doi.org/10.1007/s10508-012-0055-z
Bockting WO (2016) Vulnerability and resilience among gender-nonconforming children and adolescents: mental health professionals have a key role to play. J Am Acad Child Adolesc Psychiatry 55:441–443. https://doi.org/10.1016/j.jaac.2016.04.008
Winkler J, Stolzenberg H (1999) Der sozialschichtindex im bundes-gesundheits survey [Social class index in the Federal health survey]. Gesundheitswesen 61:178–183
Achenbach TM (1991) Manual for the youth self-report and 1991 profile. University of Vermont, Burlington, VT, Dept. of Psychiatry
Döpfner, M., Plück, J., Bölte, S., et al (1998) Fragebogen für Jugendliche; deutsche Bearbeitung der Youth Self-Report Form der Child Behavior Checklist (YSR). Einführung und Anleitung zur Handauswertung mit deutschen Normen: Arbeitsgruppe Deutsche Child Behavior Checklist. [Questionnaire for Adolescents; German Version of the Youth Self Report Form of the Child Behavior Checklist (YSR). Introduction and Manual for the Evaluation using German norm data: Work Group of the German Child Bheavior Checklist.] Arbeitsgruppe Kinder-, Jugend- und Familiendiagnostik (KJFD), Köln
Döpfner M, Berner W, Lehmkuhl G (1995) Reliabilität und faktorielle Validität des Youth Self-Report der Child Behavior Checklist bei einer klinischen Stichprobe. [Reliability and factorial validity of the Youth Self-Report of the Child Behavior Checklist in a clinical sample.] Diagnostica 41:221–244
Zucker KJ, Bradley SJ, Owen-Anderson A et al (2012) Demographics, behavior problems, and psychosexual characteristics of adolescents with gender identity disorder or transvestic fetishism. J Sex Marital Ther 38:151–189. https://doi.org/10.1080/0092623X.2011.611219
Little RJA, Rubin DB (2014) Statistical analysis with missing data. John Wiley & Sons
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Routledge, New York, NY
Cumming G, Finch S (2005) Inference by eye: confidence intervals and how to read pictures of data. Am Psychol 60:170–180. https://doi.org/10.1037/0003-066X.60.2.170
Röder M, Barkmann C, Richter-Appelt H, et al (2018) Health-related quality of life in transgender adolescents: Associations with body image and emotional and behavioral problems. Int J Transgenderism 0:1–14. https://doi.org/10.1080/15532739.2018.1425649
Holt V, Skagerberg E, Dunsford M (2016) Young people with features of gender dysphoria: Demographics and associated difficulties. Clin Child Psychol Psychiatry 21:108–118. https://doi.org/10.1177/1359104514558431
Veale JF, Peter T, Travers R, Saewyc EM (2017) Enacted stigma, mental health, and protective factors among transgender youth in Canada. Transgender Health 2:207–216. https://doi.org/10.1089/trgh.2017.0031
Breslow AS, Brewster ME, Velez BL et al (2015) Resilience and collective action: exploring buffers against minority stress for transgender individuals. Psychol Sex Orientat Gend Divers 2:253–265. https://doi.org/10.1037/sgd0000117
Pullen Sansfaçon A, Robichaud M-J, Dumais-Michaud A-A (2015) The experience of parents who support their children’s gender variance. J LGBT Youth 12:39–63. https://doi.org/10.1080/19361653.2014.935555
Becker I, Ravens-Sieberer U, Ottová-Jordan V, Schulte-Markwort M (2017) Prevalence of adolescent gender experiences and gender expression in Germany. J Adolesc Health 61:83–90. https://doi.org/10.1016/j.jadohealth.2017.02.001
Schneider C, Cerwenka S, Nieder TO et al (2016) Measuring gender dysphoria: A multicenter examination and comparison of the utrecht gender dysphoria scale and the gender identity/gender dysphoria questionnaire for adolescents and adults. Arch Sex Behav 45:551–558. https://doi.org/10.1007/s10508-016-0702-x
Acknowledgements
We thank all the participants who contributed to this study by providing important personal data on many levels, and the clinicians for their contribution to the data collection in the care unit, especially Saskia Fahrenkrug.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical standards statement
All human and animal studies have been approved by the appropriate local ethics committee and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Rights and permissions
About this article
Cite this article
Levitan, N., Barkmann, C., Richter-Appelt, H. et al. Risk factors for psychological functioning in German adolescents with gender dysphoria: poor peer relations and general family functioning. Eur Child Adolesc Psychiatry 28, 1487–1498 (2019). https://doi.org/10.1007/s00787-019-01308-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-019-01308-6